08 March 2023: Clinical Research
Treatment of Gingival Recession Defects with Pouch and Tunnel Technique Using Connective Tissue Graft and Lyophilized Chorion Membrane in Smokers
Aishwaraya Veerabadran LoganathanDOI: 10.12659/MSM.938865
Med Sci Monit 2023; 29:e938865
Abstract
BACKGROUND: The chorion membrane has been used for several decades as an allograft in tissue repair and various periodontal regenerative procedures. The present study, conducted at a single center in India, aimed to evaluate and compare the clinical outcomes of 26 gingival recession sites in chronic smokers treated using a pouch and tunnel technique with connective tissue graft (CTG) and lyophilized chorion membrane (LCM).
MATERIAL AND METHODS: The study included 22 smokers with 26 sites of recession defect, with Miller’s class I and class II gingival recession, which were allotted into control and test groups. The control group (13 sites) was treated with CTG, and the test group (13 sites) was treated with LCM. Clinical parameters like recession depth, recession width, relative clinical attachment level (RCAL), relative gingival position, width of attached gingiva, and width of keratinized gingiva were recorded at baseline and 6 months postoperatively. Visual analogue scores for pain and wound-healing index scores were assessed in the first week after surgery.
RESULTS: All clinical parameters showed significant improvements from baseline to 6 months postoperatively in the control and test groups. Recession width, RCAL, width of attached gingiva, and width of keratinized gingiva demonstrated significant differences, whereas mean root coverage percentage and recession depth did not show any significant differences between the study groups at 6 months postoperatively.
CONCLUSIONS: This study supports the role of LCM allograft as a scaffold to promote soft tissue regeneration and has demonstrated a favorable role for its use in root coverage procedures in patients who smoke.
Keywords: Chorion, Connective Tissue, gingival recession, smokers, Humans, Wound Healing, Gingiva
Background
Cigarette smoking has been shown to represent a strong and significant risk factor for periodontal disease [1,2]. The prevalence and severity of periodontitis seems to be greater in smokers than in non-smokers [3,4]. In particular, tobacco smoking is associated with increased periodontal bone and attachment loss [3–6], pocket formation [7], and tooth loss [8]. Gingival recession is defined as the apical displacement of the gingival margin from the cemento-enamel junction (CEJ) [9,10]. Gingival recession has generally been found to be more pronounced in smokers, regardless of variation in tooth type or site. Several cross-sectional studies have demonstrated that attachment loss and recession defects are more prevalent in smokers as compared with non-smokers [11–15]. Smoking also has a wide range of detrimental effects in the oral cavity. Cigarette smoking has been shown to represent a strong risk factor for the development of periodontal disease [16].
The clinical indications for exposed root coverage are esthetic need and management of root hypersensitivity, cervical abrasions, and shallow root caries lesions [17]. Various surgical methods to cover denuded root surfaces are available: these include the coronally positioned flap [18], laterally sliding flap [19], free gingival graft plus coronally positioned flap [20], acellular dermal matrix graft [21], and pouch and tunnel technique [22]. The impact of smoking on treatment outcomes is based on the dose-response relationship [23]. Smoking causes elevated complications in the wound-healing process by affecting various cell types and their ability to regenerate hard and soft tissues, either by altering their function or by diminishing their production [24]. However, precise mechanisms by which tobacco use interferes with healing of root coverage procedures is not fully understood.
As several clinical studies have shown that healing and root coverage outcomes are compromised in smokers, in terms of both quantity and stability [14,25,26], a more conservative technique for smoking cohorts is considered appropriate. Raetzke et al [27] suggested a bilaminar technique for management of isolated gingival recession defects by creating a pouch or an envelope around the gingival recession site. This achieved 80% of mean root coverage. However, for multiple gingival defects, Zabalegui et al [28] created a tunnel under the recessed area to receive the graft while preserving the interdental papilla, thus improving the gingival blood supply to the flap and achieving a mean root coverage of 91.6%. Successful outcomes were reported with a combination of these 2 techniques. A case report by Dani et al [22] showed about 100% of root coverage at the end of 1 year. Harris et al [29] and Zuhr et al [30] reported 90.5% and 98.4% root coverage using the pouch and tunnel technique. In the present study, we used the pouch and tunnel technique for root coverage in smokers as it does not involve vertical incisions and preserves the gingival blood supply and integrity of the interdental papilla, unlike other root coverage procedures. Due to minimal incisions and preservation of the blood supply at the surgical site, this technique is expected to accelerate wound healing and create less traction to the surrounding tissues, which may have favorable effects on smokers.
Since the introduction of the subepithelial connective tissue graft (CTG) in the 1980s [27,16], an enhanced predictability for obtaining esthetic root coverage has been reported [31,32], establishing this technique as a standard procedure for the treatment of gingival recession [31]. Although reliable, CTG is associated with pain, and acceptance of patients to undergo this surgical procedure is limited.
As a choice, there is a growing interest in the use of other biomaterials like placental allografts. Placental allografts have been used for more than 70 years in a variety of applications. Human amniotic membrane grafting is used as an adjunctive procedure across surgical specialties and in translational medicine to cultivate stem cells. It is easily available, and techniques of preparation and storage are relatively inexpensive. Lack of immunogenicity and the promotion of epithelial growth are favorable properties of amnion allografts. Amnion expresses anti-inflammatory, antimicrobial, and antifibrotic factors [33,34]. The use of amnion in regenerative medicine as a scaffold has been studied, and it has been found to be effective in many clinical trials [35]. The human placental layers consist of the inner amnion and the outer chorion. Chorion is an abundant source of collagen and non-collagenous proteins [36]. It contains anti-inflammatory and antimicrobial factors, cytokines, and growth factors, and acts as a scaffold that helps in the proliferation and differentiation of cells, thereby expediting the migration of cells to the defect area [37]. Collectively, these properties suggest that chorion may provide good root coverage outcomes.
To our knowledge, there are only very limited studies in the literature comparing different surgical techniques for root coverage outcomes between smoking cohorts [15,38–40]. However, there are no studies comparing the effect of different biomatrices in smokers for root coverage procedures. Hence, in light of the advantage of the pouch and tunnel technique, which has a positive effect on vascularization in smokers, the current study aimed to compare the effect of 2 different biomatrices for a root coverage procedure in smokers: CTG and lyophilized chorion membrane (LCM). The hypothesis of the study is that the effect of CTG and LCM on root coverage outcome would be comparable. To test this, the present study was conducted at a single center in India and aimed to evaluate outcomes of root coverage in smokers with Miller’s class I and class II gingival recession using a pouch and tunnel technique with LCM allograft tissue.
Material and Methods
STUDY POPULATION AND EXPERIMENTAL DESIGN:
This research study was conducted at a single center in India between March 2020 and July 2021. All the patients involved requested root coverage treatment for esthetic concerns or root hypersensitivity. Ethical approval was obtained from the Institutional Review Board (SRMDC/IRB/2019/MDS/No. 508). The study was conducted in accordance with the Helsinki Declaration of 1975, as revised in 2013. The study was registered in Clinical Trial Registry-India with the identifier number CTRI/2020/03/024159. Before participation, written informed consent was obtained from every participant, and detailed information about the nature of the study, the surgical protocol, potential treatment outcomes, and potential complications was given to the patient. The sample size calculation was done as follows: To have <5% alpha error and >90% power, a minimum of 26 sites in smoker patients (13 in each group) was required. The sample was then finalized on a total of 30 sites in smoker patients (15 in each group) to compensate for 10% anticipated dropouts. Pouch and tunnel technique was used as the surgical technique for root coverage management in both of the groups [22,27,28]. Patients in the control group received CTG and those in the test group received LCM (Tissue Bank, Tata Memorial Hospital, Mumbai, India; Figure 1).
PATIENT INCLUSION AND EXCLUSION CRITERIA:
The study population consisted of patients referred to the outpatient Department of Periodontology for periodontal treatment. Participants were recruited based on the following criteria: patients of age 25 to 45 years presenting with localized or multiple Millers class I and class II buccal tooth recessions; current cigarette smokers ≤10 cigarettes/day; patients not contraindicated for periodontal surgery; patients who are complying with oral hygiene instructions and periodontal recall; and patients with ≤20% of full mouth plaque scores [42] and full mouth bleeding scores [43] after phase I therapy. Pack-years were calculated at baseline for all the recruited patients. Heavy smokers, pregnant and lactating women, patients using medication affecting periodontal status, patients with a history of previous periodontal surgical treatment at the involved sites, and patients with immunodeficiency disorders, history of malignancy or carcinoma, or malposed or crowded teeth were excluded from this study.
RANDOMIZATION AND GROUP ALLOCATION:
One of the investigators (SS) randomly assigned the patients into control or test groups during the surgical appointment, according to the last digit of the outpatient card number. This number was written on a piece of paper, which was then placed in a sealed envelope and presented to the surgeon during the commencement of surgery. If the surgeon found an odd number on the paper, CTG was utilized as the biomatrix. If an even number was present on the paper, LCM was utilized as the biomatrix. The surgeon and the patient were aware of the biomatrix that was placed and hence were not blinded to the study. All of the surgical procedures were carried out by a single trained operator (PSG).
CLINICAL PARAMETERS AND OUTCOMES MEASURES:
The examiner (DA) who evaluated all the clinical parameters at baseline and 6 months postoperatively was blinded to the treatment protocol. All the parameters were recorded at 3 surfaces; mesiobuccal, midbuccal, and distobuccal, using a University of North Carolina periodontal probe. Clinical parameters evaluated were full mouth plaque score, full mouth bleeding score, recession depth, recession width, probing pocket depth, relative clinical attachment level (RCAL), relative gingival position, width of attached gingiva, and width of keratinized gingiva. Customized composite stents were prepared for each site using light cure composite material (Revotek LC™, Tokyo, Japan) along with vertical grooves to orient the probing angulations. Probing pocket depth, RCAL, and relative gingival position were measured with the help of the prepared stents at baseline. Further, the composite stents were kept on the study cast for followup measurements at 6 months postoperatively. Visual analogue scores (VAS) and wound-healing index scores were evaluated postoperatively at 1 week. Six months after surgery, the percentage of root coverage was evaluated. The primary outcome measures were recession depth and root coverage percentage. The remaining parameters were considered as secondary outcome measures.
PRESURGICAL PROCEDURE:
Patient recruitment was done based on the selection criteria. All the recruited patients underwent phase I therapy; that is, the nonsurgical phase, which included oral hygiene instructions, oral prophylaxis, root surface debridement, and removal of plaque retentive factors. Patients were recalled after 6 to 8 weeks and assessed for periodontal maintenance. Patients who demonstrated ≤20% of full mouth plaque scores and full mouth bleeding scores after phase I therapy were then allocated to control or test groups for phase II therapy (surgical phase).
SURGICAL PROCEDURE:
The surgical site was anaesthetized using 2% lignocaine hydrochloride (21.3 mg/mL) and adrenaline acid tartrate (22.7 mcg/mL) in a 1: 80,000 strength, after the surgical field had been properly isolated. After local anaesthesia, sulcular incisions were made around the neck of the tooth being treated. The incision was extended to the adjacent tooth, both on the mesial and distal aspect, using a 15c blade. The incision maintained the full thickness and height of the gingival component, thus enabling access beneath the buccal gingiva. The cutting side of the blade was directed towards the bone to dissect the connective tissue from the most apical part to the mucogingival line, thus enabling free access of the buccal flap around each tooth. Care was taken to not extend the incisions across the interdental region of the gingiva. The papilla was undermined carefully to maintain its integrity. The buccal gingiva could at this point move coronally since the connective tissue attachment is apical into the mucosal tissue. Care was taken not to perforate the buccal gingiva so as to avoid compromising the blood supply in that region. An envelope of full thickness pouch and tunnel was thus created using tunneling knives number 1 and 2 (Hu-Friedy, Chicago, Illinois, USA).
CTG for the control site was harvested from the palate, which was trimmed to remove the fatty glandular tissue and reduced to a uniform thickness of 1 to 1.5 mm. The incision was closed with simple interrupted sutures (3-0 silk suture material). CTG thus obtained was tunneled at the recipient site for the control group, and LCM was placed for the test group. The entire gingivopapillary complex, along with the CTG or LCM (Figure 2), was coronally positioned using 4-0 Vicryl sutures. It was suspended on the composite resin placed on a coronal point of the contact area. Periodontal dressing was placed over the surgical site (Figure 3).
POSTOPERATIVE MANAGEMENT:
Patients were prescribed analgesics for 5 days after surgery and, for ethical reasons, patients were advised to stop smoking for a week. They were instructed not to brush over the operated area, to avoid trauma to the surgical site. Chlorhexidine (0.2%) mouthwash was recommended for oral hygiene maintenance for 2 weeks. The periodontal dressing and the sutures were removed after 7 days. The wound-healing index scores were assessed at 1 week postoperatively. The pain, swelling, and discomfort experienced during and after the surgical procedure, and interference in daily activities, were assessed using a 10-cm VAS by the patient a week after the surgery. All the clinical parameters were recorded at the followup visits postoperatively and at 6 months.
STATISTICAL ANALYSIS:
Data analysis was performed using SPSS (IBM SPSS Statistics for Windows, Version 26.0, Armonk, NY: IBM Corp. Released 2019). Significance level was fixed at 5% (α≤0.05), and
Results
DESCRIPTIVE STATISTICS OF THE STUDY GROUPS:
Smokers with a total of 30 class I and class II recession sites were recruited for the present study. For both the study groups, pouch and tunnel technique was utilized. Fifteen sites were treated with CTG, and 15 sites were treated with LCM. Two patients having 2 sites each in both the groups were lost to followup after phase II therapy. One patient was not able to report back due to serious illness and another patient dropped out of the study due to relocating to a different city so a total of 4 sites (2 sites in each group) were lost during the 6-month evaluation. Hence, excluding those 4 sites, only 26 recession sites, with 13 recession sites each in control and test groups, were considered for statistical evaluation. Descriptive statistics for age, pack-years, and clinical parameters of patients recruited at baseline demonstrated no significant differences between the study groups (Table 1).
INTERGROUP COMPARISON OF VAS AND WOUND-HEALING INDEX SCORES BETWEEN THE CONTROL AND TEST GROUPS AFTER THERAPY:
VAS pain scale scores and wound-healing index scores between test and control groups were evaluated at 1 week postoperatively, using the Mann-Whitney U test. The results showed a highly significant difference in VAS pain scale scores in the test group in comparison with the control group. The wound-healing index scores did not demonstrate any significant difference between the study groups at 1 week postoperatively (Table 2).
INTRAGROUP ANALYSIS OF CLINICAL PARAMETERS FROM BASELINE TO 6 MONTHS AFTER THERAPY:
Clinical parameters like recession depth, recession width, relative gingival position, RCAL, probing pocket depth, width of attached gingiva, and width of keratinized gingiva were compared between baseline and 6 months postoperatively in the study groups. Both control and test groups showed significant improvement in all the parameters at 6 months (Table 3).
INTERGROUP ANALYSIS OF CLINICAL PARAMETERS BETWEEN THE STUDY GROUPS AT 6 MONTHS:
The clinical parameters evaluated at 6 months postoperatively were compared between the study groups. RCAL, width of attached gingiva, and width of keratinized gingiva showed significant differences in favor of the test group. On the other hand, recession width was significantly favorable towards the control group. The parameters, especially the recession depth and root coverage percentage, did not show any significant difference between the study groups when compared at 6 months postoperatively (Table 4).
Discussion
The present study aimed to compare the clinical outcomes of a pouch and tunnel technique using CTG or lyophilized chorion membrane to repair gingival recession defects.
The results of the study suggest that lyophilized chorion membrane provides almost comparable root coverage outcomes to CTG at 6 months postoperatively. Both groups showed significant improvements from baseline to 6 months in all clinical parameters. However, in terms of clinical attachment level gain and increase in width of attached and keratinized gingiva, there were significant differences at 6 months favoring the test group. When wound-healing index scores were assessed at 1 week postoperatively, both groups showed better healing with no signs of gingival edema, erythema, suppuration, patient discomfort, or flap dehiscence. VAS evaluated at week 1 indicated that patients reported slightly more pain in the control group compared with the test group.
Studies conducted to assess root coverage outcomes between smokers and non-smokers have always shown favorable results for non-smokers. In contrast, certain studies demonstrated clinically comparable outcomes in smokers and non-smokers. For instance, Harris et al [18] obtained about 96.65% of mean root coverage in smokers by using connective tissue with a double pellicle flap, and Tolmie et al [44] obtained about 96% of root coverage in smokers when treated with gingival autografts. Amarante et al [45] treated smokers with a coronally positioned flap and obtained about 62.5% of total root coverage. In our study, the root coverage percentage obtained was 59.77±18.59% in the guided tissue regeneration group and 56.31±18.60% in the chorion membrane group.
Most of the studies conducted on smokers showed low root coverage percentage, as obtained in our study. For instance, Trombelli and Scabbia et al [13] observed about 57% root coverage in smokers using the guided tissue regeneration technique. Studies by Souza et al [15] and Silva et al [14] utilized a coronally positioned flap technique in smokers, which resulted in about 58.02% and 69.3% of root coverage respectively. Certain studies were done to analyze root coverage outcomes when CTG was used in smokers. Martins et al [46] and Andia et al [24] showed about 58.84% and 50% root coverage whereas Erley et al [47] showed slightly better root coverage; about 82.3%.
Root coverage procedures with chorion membrane have shown promising results in nonsmokers. Case series conducted by Pundir et al [48] and Esteves et al [49] obtained about 77.93% and 89.92% of root coverage when chorion membrane was used. Clinical studies that utilized chorion membrane also demonstrated significant improvements in treatment outcomes [50,51]. There are no studies that used chorion membrane in smokers; hence, comparison of other studies with the current study is of limited value.
Smokers exhibited reduced root coverage outcomes due to nicotine accumulation on the root surfaces [52]. The impaired function of fibroblasts on the root surface when exposed to nicotine impedes wound healing with soft tissue grafts by changing cellular metabolism, including protein secretion and collagen formation. Studies have compared different techniques and biomatrices in heavy smokers and evaluated the root coverage outcomes. For instance, Reino et al 2015 [41] compared a coronally positioned flap and a new extended flap technique along with CTG in heavy smokers and obtained about 48.60% vs 54.28% of root coverage. Clinical trials that compared acellular dermal matrix with or without enamel matrix derivative in heavy smokers obtained about 44% vs 55.4% and 59.7% vs 52.8% root coverage [38,40]. From most of the above-mentioned studies, it was observed that root coverage percentage in smokers as reported in the literature closely matches with that obtained in our study groups.
Both control and test groups in our study showed significant improvement in recession depth reduction at 6 months postoperatively. The recession depth gain was about 1.62 mm and 1.81 mm in the in the control and test group, respectively. Although the control group showed slightly more reduction in recession depth, it was not significant when compared with the test group at 6 months postoperatively. These results were comparable to studies in smokers by Alves et al [40] and Pernambuco et al [38], in which they obtained about 1.52 mm of recession depth reduction in each of their control groups, and about 1.95 mm of recession depth reduction in their test groups. Studies by Silva et al [14], Souza et al [15], and Nanavati et al [53] showed recession depth improvement of about 1.9 mm in smokers. On the contrary, a study by Scabbia et al [54] showed increased recession depth compared with preoperative levels, to about an additional 0.7 mm, in smokers.
Two defect sites in the control group and 1 defect site in the test group obtained complete root coverage (CRC) in the present study. Various studies have also demonstrated that CRC in smokers is questionable. To cite a few studies, Silva et al [14], Andia et al [25], and Nanavati et al [53] reported that no tooth exhibited CRC in smokers, whereas Souza et al [15] and Erley et al [47] showed about 6.7% and 25% CRC, respectively. Also, Pernambuco et al [38] and Alves et al [40] reported only 3 instances of CRC in their test group.
The RCAL gain was about 1.05 mm and 0.98 mm in the control and test groups, respectively. Similarly, probing pocket depth also showed significant improvement, of about 1.23 mm and 0.91 mm in the control and test groups, respectively, from baseline to 6 months after the surgical treatment. The comparison between the study groups revealed that only parameters like recession width, RCAL, width of attached gingiva, and width of keratinized gingiva showed significant improvements postoperatively. RCAL gain was slightly in favor of the control group and parameters like recession width, width of attached gingiva, and width of keratinized gingiva were more favorable towards the test group. Other parameters, especially recession depth and percentage of root coverage, failed to show any significant difference between the study groups (Table 4). This observation revealed that lyophilized chorion membrane is comparable to that of CTG in achieving root coverage outcomes.
Smoking impairs vascularization of hard [30] and soft [31] tissues, which could be a major factor in impaired wound healing. For the CTG to revascularize, a sufficient blood supply is necessary. In smokers, a conservative approach like pouch and tunnel technique helps to provide favorable outcomes for management of gingival recessions, as it preserves the blood supply and integrity of the flap [55]. Scientific data have collectively highlighted that the root coverage procedures performed using CTG provide excellent esthetics and also favorably modulate the parameters associated with root coverage [56]. However, 1 major disadvantage of CTG is that it requires a second surgical site for procuring the graft. Hence, as an alternative approach, various biomaterials have been tried for root coverage procedures. One such biomaterial is chorion membrane, which has superior antibacterial properties and has diverse advantages attributed to its porous structure and composition. This membrane contains numerous growth factors like keratinocyte growth factor, transforming growth factor beta, and basic fibroblastic growth factor, as well as stem cells, which aid in the proliferation and differentiation of cells [37]. It also has tissue inhibitors of metalloproteinase, and may modulate inflammation by reducing inflammatory mediators [37].
The current study had limitations, including a low sample size and a followup period after therapy of only 6 months. In addition, gingival biotype was not considered as a parameter for assessing root coverage outcomes. Further studies are required to analyze the root coverage outcomes using various techniques and biomatrices in smokers, preferably with a larger sample size. Collectively, the findings of the present study suggested that the pouch and tunnel technique using lyophilized chorion membrane was effective and comparable to using CTG in improving the clinical parameters associated with root coverage procedures when utilized in smokers.
Conclusions
This study supports the role of lyophilized chorion membrane allograft as a scaffold to promote soft tissue regeneration. Our results demonstrated a favorable role for its use in root coverage procedures in smokers.
Figures
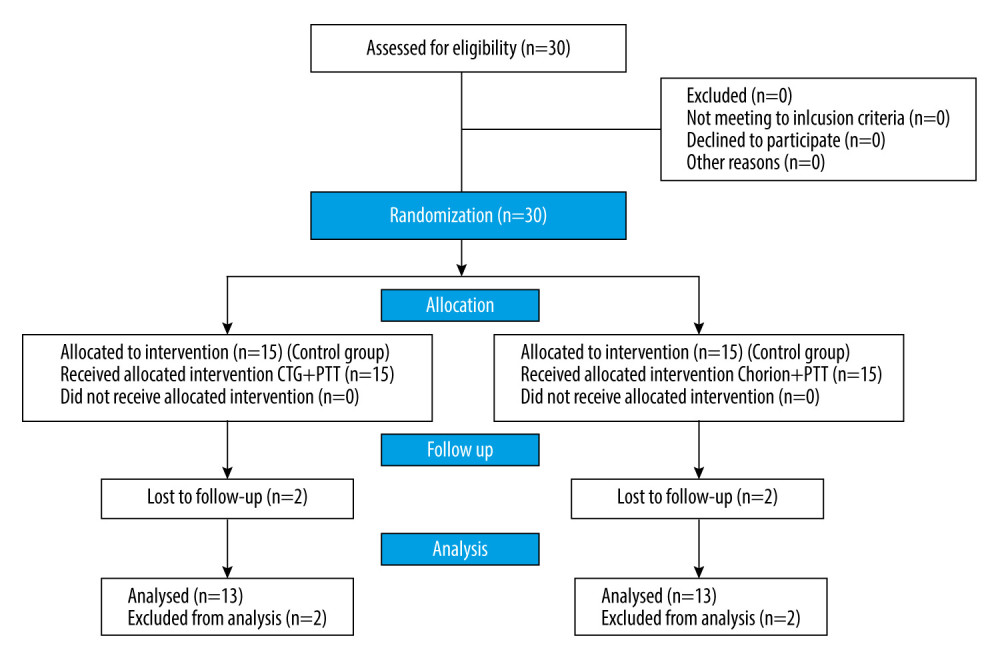 Figure 1. Consort flow chart of this study. CTG – connective tissue graft, PTT – pouch and tunnel technique.
Figure 1. Consort flow chart of this study. CTG – connective tissue graft, PTT – pouch and tunnel technique. 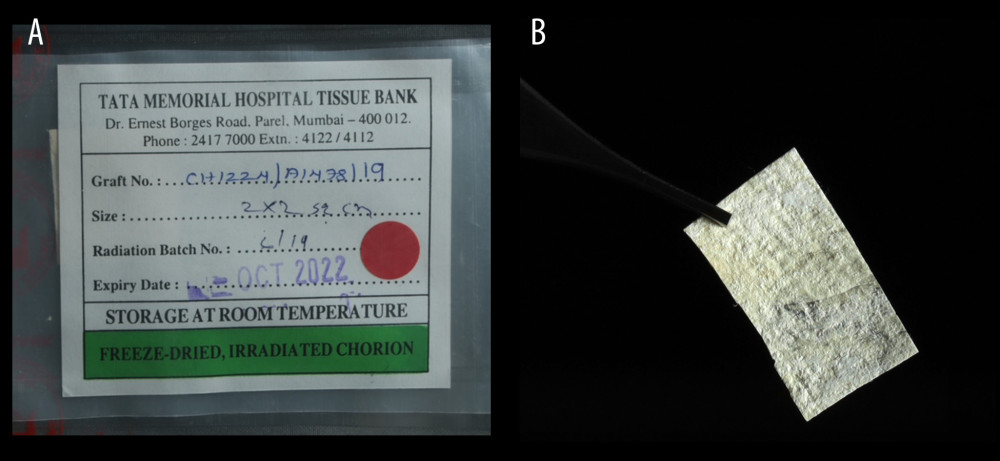 Figure 2. (A, B) Chorion membrane.
Figure 2. (A, B) Chorion membrane. 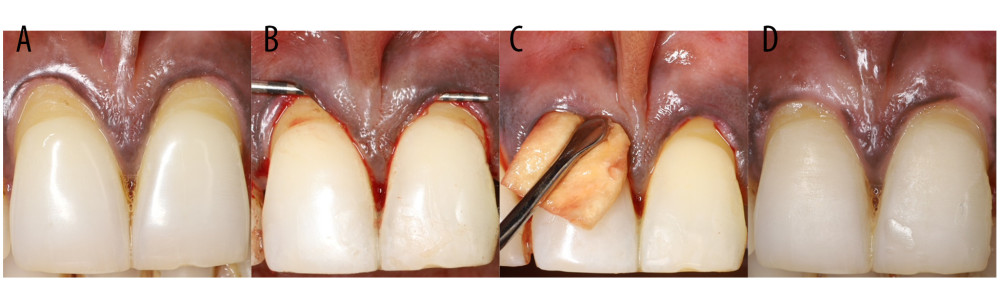 Figure 3. Root coverage procedure with chorion membrane. (A) Baseline, (B) Tunnel access, (C) Insertion of chorion membrane, (D) Post-operative 6 months.
Figure 3. Root coverage procedure with chorion membrane. (A) Baseline, (B) Tunnel access, (C) Insertion of chorion membrane, (D) Post-operative 6 months. Tables
Table 1. Descriptive statistics describing the parameters of the study groups at baseline.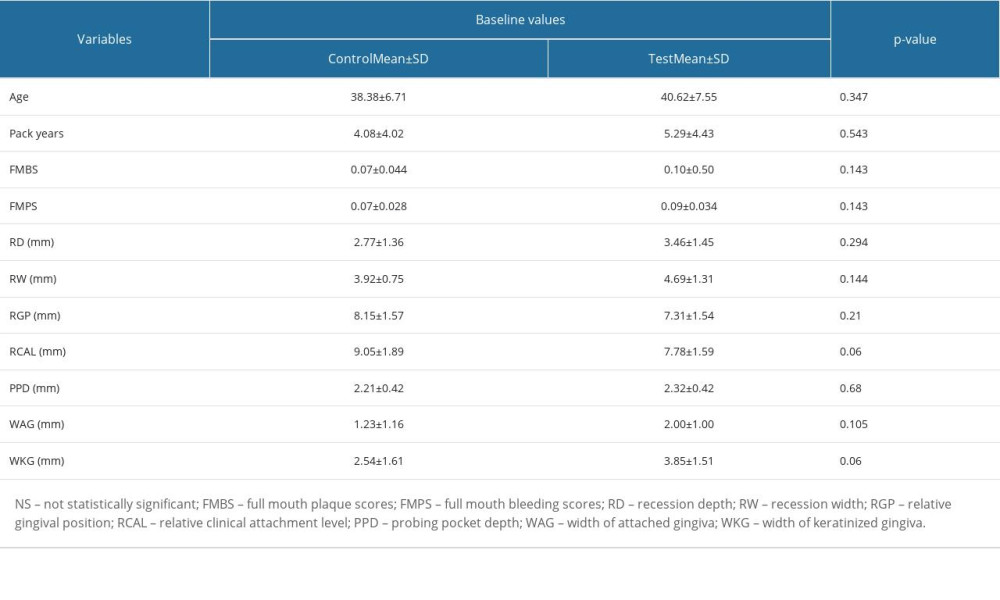 Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups.
Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups.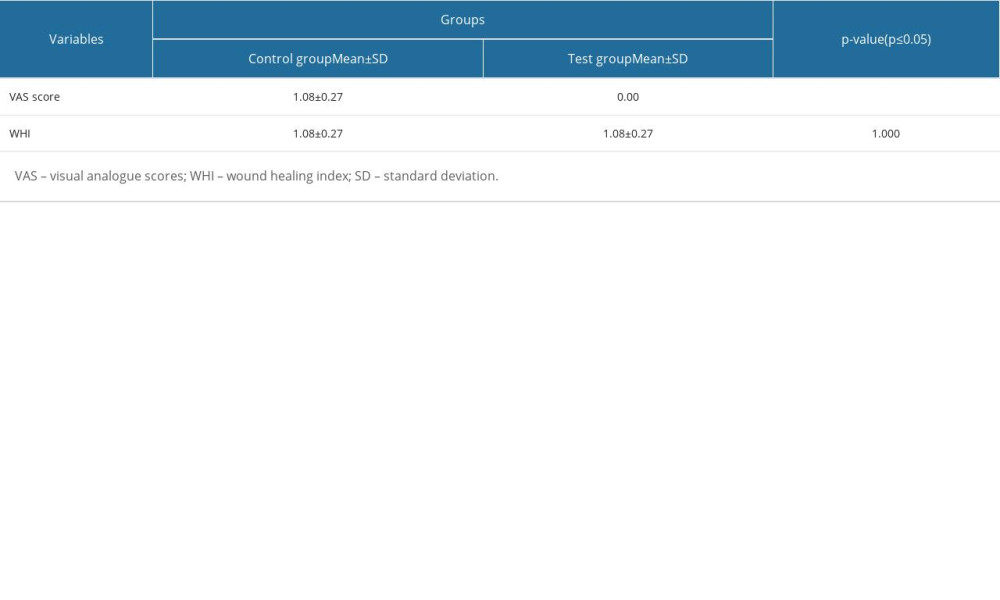 Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively.
Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively.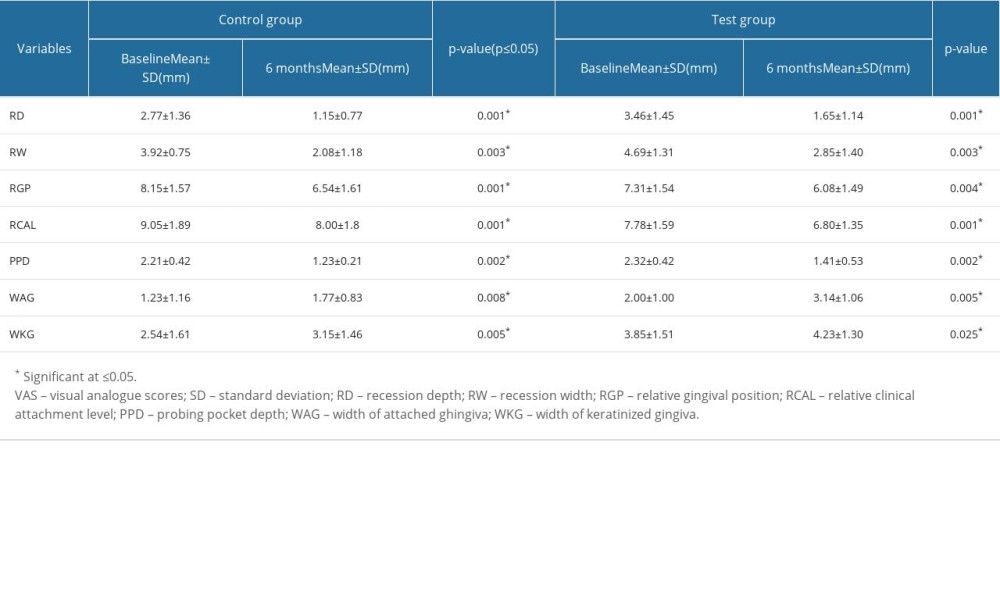 Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively.
Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively.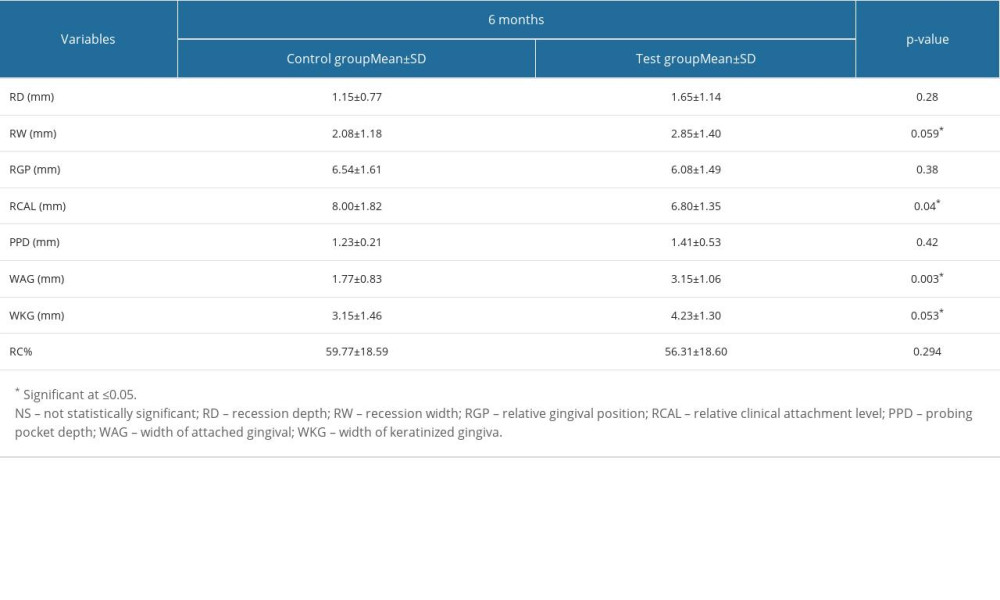
References
1. Grossi SG, Zambon JJ, Ho AW, Assessment of risk for periodontal disease. I. Risk indicators for attachment loss: J Periodontol, 1994; 65(3); 260-67
2. Bergström J, Cigarette smoking as risk factor in chronic periodontal disease: Community Dent Oral Epidemiol, 1989; 17(5); 245-47
3. Bergström J, Floderus-Myrhed B, Co-twin control study of the relationship between smoking and some periodontal disease factors: Community Dent Oral Epidemiol, 1983; 11(2); 113-16
4. Feldman RS, Bravacos JS, Rose CL, Association between smoking different tobacco products and periodontal disease indexes: J Periodontol, 1983; 54(8); 481-87
5. Bergström J, Eliasson S, Preber H, Cigarette smoking and periodontal bone loss: J Periodontol, 1991; 62(4); 242-46
6. Grossi SG, Genco RJ, Machtet EE, Assessment of risk for periodontal disease. II. Risk indicators for alveolar bone loss: J Periodontol, 1995; 66(1); 23-29
7. Machuca G, Rosales I, Lacalle JR, Machuca C, Bullón P, Effect of cigarette smoking on periodontal status of healthy young adults: J Periodontol, 2000; 71(1); 73-78
8. Ragnarsson E, Eliasson ST, Olafsson SH, Tobacco smoking, a factor in tooth loss in Reykjavik, Iceland: Eur J Oral Sci, 1992; 100(6); 322-26
9. Jati AS, Furquim LZ, Consolaro A, Gingival recession: Its causes and types, and the importance of orthodontic treatment: Dental Press J Orthod, 2016; 21(3); 18-29
10. Patel M, Nixon PJ, Chan MF, Gingival recession: Part 2. Surgical management using pedicle grafts: Br Dent J, 2011; 211(7); 315-19
11. Müller HP, Stadermann S, Heinecke A, Gingival recession in smokers and non-smokers with minimal periodontal disease: J Clin Periodontol, 2002; 29(2); 129-36
12. Tonetti MS, Pini-Prato G, Cortellini P, Effect of cigarette smoking on periodontal healing following GTR in infrabony defects: A preliminary retrospective study: J Clinical Periodontol, 1995; 22(3); 229-34
13. Trombelli L, Scabbia A, Healing response of gingival recession defects following guided tissue regeneration procedures in smokers and non-smokers: J Clin Periodontol, 1997; 24(8); 529-33
14. Silva CO, Sallum AW, de Lima AF, Tatakis DN, Coronally positioned flap for root coverage: Poorer outcomes in smokers: J Periodontol, 2006; 77(1); 81-87
15. Souza SL, Macedo GO, Tunes RS, Subepithelial connective tissue graft for root coverage in smokers and non-smokers: A clinical and histologic controlled study in humans: J Periodontol, 2008; 79(6); 1014-21
16. Langer B, Langer L, Subepithelial connective tissue graft technique for root coverage: J Periodontol, 1985; 56(12); 715-20
17. Wennström J, Pini Prato GP, Mucogingival therapy: Clinical periodontology and implant dentistry, 1997; 569-91, Copenhagen, Munksgaard
18. Harris RJ, Harris AW, The coronally positioned pedicle graft with inlaid margins: A predictable method of obtaining root coverage of shallow defects: Int J Periodontics Restorative Dent, 1994; 14(3); 228-41
19. Guinard EA, Caffesse RG, Treatment of localized gingival recessions. Part I: Lateral sliding flap: J Periodontol, 1978; 49; 351-56
20. Caffesse RG, Guinard EA, Treatment of localized gingival recessions. Part II: Coronally repositioned flap with a free gingival graft: J Periodontol, 1978; 49; 357-61
21. de Cortes AQ, Martins AG, Nociti FH, Coronally positioned flap with or without acellular dermal matrix graft in the treatment of Class I gingival recessions: A randomized controlled clinical study: J Periodontol, 2004; 75; 1137-44
22. Dani S, Dhage A, Gundannavar G, The pouch and tunnel technique for management of multiple gingival recession defects: J Indian Soc Periodontol, 2014; 18(6); 776-80
23. National Cancer Institute: Smoking and Tobacco Control Monograph 9, Cigars, Health Effects and Trends
24. Silverstein P, Smoking and wound healing: American J Med, 1992; 93; S22-24
25. Andia DC, Martins ÂG, Casati MZ, Root coverage outcome may be affected by heavy smoking: A 2-year follow-up study: J Periodontol, 2008; 79(4); 647-53
26. Silva CO, De Lima AF, Sallum AW, Tatakis DN, Coronally positioned flap for root coverage in smokers and non-smokers: Stability of outcomes between 6 months and 2 years: J Periodontol, 2007; 78(9); 1702-7
27. Raetzke PB, Covering localized areas of root exposure employing the “envelope” technique: J Periodontol, 1985; 56(7); 397-402
28. Zabalegui I, Sicilia A, Cambra J, Treatment of multiple adjacent gingival recessions with the tunnel subepithelial connective tissue graft: A clinical report: Int J Periodontics Restorative Dent, 1999; 19(2); 199-206
29. Harris RJ, Miller LH, Harris CR, Miller RJ, A comparison of three techniques to obtain root coverage on mandibular incisors: J Periodontol, 2005; 76(10); 1758-67
30. Zuhr O, Rebele SF, Schneider D, Tunnel technique with connective tissue graft versus coronally advanced flap with enamel matrix derivative for root coverage: A RCT using 3D digital measuring methods. Part I. Clinical and patient-centred outcomes: J Clin Periodontol, 2014; 41(6); 582-92
31. Bouchard P, Malet J, Borghetti A, Decision-making in aesthetics: Root coverage revisited: Periodontol, 2001; 27; 97-120
32. Harris RJ, The connective tissue and partial thickness double pedicle graft: A predictable method of obtaining root coverage: J Periodontol, 1992; 63; 477-86
33. Sridhar U, Tripathy K, Amniotic membrane graft: StatPearls [Internet] Feb 21, 2022, StatPearls Publishing
34. Koob TJ, Rennert R, Zabek N, Biological properties of dehydrated human amnion/chorion composite graft: Implications for chronic wound healing: Int Wound J, 2013; 10(5); 493-500
35. Silini AR, Cargnoni A, Magatti M, The long path of human placenta, and its derivatives, in regenerative medicine: Front Bioeng Biotechnol, 2015; 3; 162
36. Hao Y, Ma DH, Hwang DG, Identification of antiangiogenic and anti-inflammatory proteins in human amniotic membrane: Cornea, 2000; 19; 348-52
37. Kothiwale S, Ajbani J, Evaluation of anti-inflammatory effect of chorion membrane in periodontal pocket therapy: A clinical and biochemical study: J Indian Society Periodontol, 2018; 22; 433
38. Pernambuco R, Root coverage in smokers with acellular dermal matrix graft and enamel matrix derivative: A 12-month randomized clinical trial group: Int J Periodontics Restorative Dent, 2016; 36; 525-31
39. Reino DM, Novaes AB, Maia LP, Treatment of gingival recessions in heavy smokers using two surgical techniques: a controlled clinical trial: Brazilian Dent J, 2012; 23; 59-67
40. Alves LB, Costa PP, Scombatti de Souza SL, Acellular dermal matrix graft with or without enamel matrix derivative for root coverage in smokers: a randomized clinical study: J Clin Periodontol, 2012; 39(4); 393-99
41. Reino DM, Maia LP, Novaes AB, Souza SL, Comparative study of two surgical techniques for root coverage of large recessions in heavy smokers: Int J Esthet Dent, 2015; 10; 456-67
42. O’Leary TJ, Drake RB, Naylor JE, The plaque control record: J Periodontol, 1972; 43; 38
43. Ainamo J, Bay I, Problems and proposals for recording gingivitis and plaque: Int Dent J, 1975; 25; 229-35
44. Tolmie PN, Rubins RP, Buck GS, The predictability of root coverage by way of free gingival autografts and citric acid application: An evaluation by multiple clinicians: Int J Periodontics Restorative Dent, 1991; 11; 261-71
45. Amarante ES, Leknes KN, Skavland J, Lie T, Coronally positioned flap procedures with or without a bioabsorbable membrane in the treatment of human gingival recession: J Periodontol, 2000; 71; 989-98
46. Martins AG, Andia DC, Sallum AW, Smoking may affect root coverage outcome: A prospective clinical study in humans: J Periodontol, 2004; 75; 586-91
47. Erley KJ, Swiec GD, Herold R, Gingival recession treatment with connective tissue grafts in smokers and non-smokers: J Periodontol, 2006; 77; 1148-55
48. Pundir AJ, Agrawal V, Pundir S, Comparative evaluation of the efficacy of human chorion and amnion with coronally advanced flap for recession coverage: A case series: Clin Advances Periodont, 2016; 6; 118-26
49. Esteves J, Bhat KM, Thomas B, Efficacy of human chorion membrane allograft for recession coverage: A case series: J Periodontol, 2015; 86; 941-44
50. Dandekar SA, Deshpande NC, Dave DH, Comparative evaluation of human chorion membrane and platelet-rich fibrin membrane with coronally advanced flap in treatment of Miller’s class I and II recession defects: A randomized controlled study: J Ind Society Periodontol, 2019; 23; 152
51. Chopra P, Kassal J, Masamatti SS, Grover HS, Comparative evaluation of clinical efficacy of coronally advanced flap alone and in combination with placental membrane and demineralized freeze-dried bone allograft in the treatment of gingival recession: J Ind Society Periodontol, 2019; 23; 137
52. Aishwaraya VL, Subramanian S, Prakash PS, Role of immuno-inflammatory cells modified by smoking in periodontitis: J Pharm Neg Results, 2022; 15; 615-20
53. Nanavati B, Bhavsar NV, Jaydeepchandra M, Coronally positioned flap for root coverage: comparison between smokers and nonsmokers: J Int Oral health, 2013; 5; 21
54. Scabbia A, Cho KS, Sigurdsson TJ, Cigarette smoking negatively affects healing response following flap debridement surgery: J Periodontol, 2001; 72; 43-49
55. Chandra V, Bains VK, Jhingran R, Comparative evaluation of platelet-rich fibrin versus connective tissue grafting in treatment of gingival recession using pouch and tunnel technique: A randomized clinical study: Contemp Clin Dent, 2022; 13(3); 217-26
56. Savithri NK, Subramanian S, Prakash PS, Appukuttan D, Effect of microsurgical technique for root coverage using modified coronally advanced flap with connective tissue graft-Randomized controlled clinical trial: Dental Res J, 2022; 19(1); 87
Figures
Tables
 Table 1. Descriptive statistics describing the parameters of the study groups at baseline.
Table 1. Descriptive statistics describing the parameters of the study groups at baseline. Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups.
Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups. Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively.
Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively. Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively.
Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively. Table 1. Descriptive statistics describing the parameters of the study groups at baseline.
Table 1. Descriptive statistics describing the parameters of the study groups at baseline. Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups.
Table 2. Intergroup comparison of VAS scores and wound healing index scores between the control and test groups. Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively.
Table 3. Intragroup analysis of clinical parameters in the study groups from baseline to 6 months postoperatively. Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively.
Table 4. Intergroup analysis of clinical parameters between the study groups at 6 months postoperatively. In Press
08 Mar 2024 : Clinical Research
Evaluation of Foot Structure in Preschool Children Based on Body MassMed Sci Monit In Press; DOI: 10.12659/MSM.943765
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








