03 March 2023: Review Articles
Evolution of Hybrid Intelligence and Its Application in Evidence-Based Medicine: A Review
Valentina Bellini1AEF, Marco Badino1AEF, Massimo Maffezzoni1AEF, Francesca Bezzi1AEF, Elena Bignami1AEF*DOI: 10.12659/MSM.939366
Med Sci Monit 2023; 29:e939366
Abstract
ABSTRACT: Modern medicine, both in clinical practice and research, has become more and more based on data, which is changing equally in type and quality with the advent and development of healthcare digitalization. The first part of the present paper aims to present the steps through which data, and subsequently clinical and research practice, have evolved from paper-based to digital, proposing a possible future of this digitalization in terms of potential applications and integration of digital tools in medical practice. Noting that digitalization is no more a possible future, but a concrete reality, there is a strong need for a new definition of evidence-based medicine, which must take into account the progressive integration of artificial intelligence (AI) in all decision-making processes. So, leaving behind the traditional research concept of human intelligence versus AI, poorly adaptable to real-world clinical practice, a Human and AI hybrid model, seen as a deep integration of AI and human thinking, is proposed as a new healthcare governance system. The second part of our review is focused on some of the major challenges the digitalization process has to face, particularly privacy issues, system complexity and opacity, and ethical concerns related to legal aspects and healthcare disparities. Analyzing these open issues, we aim to present some of the future directions that in our opinion should be pursued to implement AI in clinical practice.
Keywords: Artificial Intelligence, Big Data, digital technology, Evidence-Based Medicine, machine learning, Telemedicine, Humans, Intelligence, Health Facilities
Background
Several articles about artificial intelligence (AI) and its application in healthcare have been published in recent decades, with a hyperbolic fashion that is still far from reaching a plateau [1–5]. Just to present some numbers, we did a literature review on PubMed using the keywords “artificial intelligence”, “machine learning”, “big data”, and “hybrid model”, including only Reviews in English language in our search. There are 4994 studies that could be found that way, covering almost every medical field, and this trend can be easily explained with the rapid and progressive healthcare digitization process, with digital care being no longer a possible future, but a concrete reality.
This narrative review aims to review the development of this digitalization process, starting from the origins of patient data recording and passing through the major issues of that “digital revolution” in order to propose that an ideal, hybrid intelligence model in which AI and human thinking must be deeply embed in decision-making and applied to evidence-based medicine (EBM). Secondly, some of the major open issues of the digitalization process are analyzed, presenting some of the future directions of healthcare digitalization itself.
We performed a narrative review of the literature in Scopus and PubMed databases. First, relevant studies published from January 2021 were included. We used a reduced timeframe to compare studies that take into account homogeneous technologies, considering the exceptional development of digital technology in recent years. The research string comprised various combinations of “artificial intelligence”, “machine learning”, “big data”, “data evolution”, “digitalization”, and “hybrid model”. We mainly included papers in English language that were not specific to a single medical field. Because of the need to provide an overview of data evolution over time, we also had to include in our review some excellent articles published before January 2021.
Evidence-Based Medicine Digital Revolution
Since the beginning, and for the most of human history, medical practice was primarily heuristic and anecdotal, so patient data have been scant and mostly scattered [1]. Decision-making was based on clinical impression, and outcomes were difficult to correlate with the quality of the medical decisions made [1]. Now, medical practice has become evidence-based. EBM is defined as the use of the best evidence available in the literature, embed with clinical expertise, in order to make the best clinical decisions possible [6].
Both medical practice and clinical research are based on patient data. Initially, the major change in patient data collection came from separate files to document collection into folders after patient discharge [7]. Clearly, records’ content was limited and data were often scattered between wards, clinics, and ambulatories, so finding relevant details was difficult and often relied on the record’s author’s memory [7]. Progressive medical specialization produced more and more specialized health records, which required an increasing quantity of new diagnostic and therapeutic procedures and subsequent specific documentation [7]. Moreover, medical data originate from many different sources, including administrative health data, biomarker data, and imaging [2]. A common form of writing and archiving would have improved the aggregation and retrieval of so much information.
A drastic and revolutionary transition from paper-based to digital format began in the 1960s with the introduction of electronic health (eHealth) records [7]. Initially, data filling was a slow and dull process, but enabled data collection in a much more effective way than paper-based documentation [7]. In the 21st century we entered an era in which a major shift in patient data collection has occurred [8]. Thanks to the rapid increase in the amount of available medical information, the dissemination of eHealth records and Electronic Medical Records (EMRs) and other emerging data sources, such as wearable devices or biobanks, the creation of large datasets has become possible [2,8,9–12].
With technology advancement, another system helped increasing data collection quantity and quality, called the Internet of Things (IoT). IoT is defined as a process of connecting physical objects to the Internet, being able to collect, send, and store data over a network without requiring human-to-human or human-to-computer interaction [3,13].
The large volumes of rapidly captured digital data from earlier sources, called Big Data, were too large for standard analytical techniques; hence, an alternative analytical method, capable of analyzing, integrating, and storing all the available information was needed [3,14,15]. As in other scientific areas, AI application helped achieve this goal. AI, and more specifically data mining and machine learning (ML) techniques, are now used to process and learn automatically from Big Data [9,10,15]. Currently, the adaptation process to eHealth records must involve AI algorithms to make medical services more manageable and malleable, health prevention-oriented, and cost-effective [7,9].
EBM is evolving accordingly; instead of extrapolating evidence from data obtained from a small number of samples to draw conclusions about the researched population, we are now able to use clinical data coming from the whole population to provide a real-world picture [7,16–18]. These same changes have also occurred in clinical research. Compared to paper-based data collection, the introduction of Electronic Case Report Form (eCRF) systems, such as REDCap or OpenClinica, greatly improve patient data collection quality and organization while reducing error rates [19].
Although reporting guidelines for different types of study exist, mostly consisting of checklists, additional and different factors need to be evaluated for AI studies to allow correct and safe application of AI in clinical research [16]. At the same time, AI development is advancing rapidly in healthcare because of its ability to fully release Big Data potential, gain insights to support evidence-based clinical decisions, and enable more patient-tailored care [20] (Figure 1). The ability to correctly study all of these data would allow clinicians to predict patient’s different health trajectories, understanding the complex interactions between their past and present, and how these would affect their future [2]. The goal is to discover new pathogenesis, classification, diagnosis, treatment, and progression of the disease, aiming to improve our ability to understand human health from a global point of view [2,21].
Therefore, in our opinion, there is a real need to change our perspective in AI medical research, abandoning the common idea of a competition between Human and AI in favor of a Human and AI collaboration – the Human and AI hybrid model – which may provide better results than either AI or Human Intelligence alone and embody real medical practice [4,22] (Figure 2). In fact, AI systems have a type of intelligence that can be described as task-centered, instead of the inimitable human capacity of high-level reasoning, imagining, and anticipating [22].
Open Issues and Future Directions
The major hurdles perceived by physicians to EMR adoption are lack of privacy and security, high start-up costs, workflow changes, system complexity, lack of total reliability, and interoperability, with the addition of a stressful environment, frequent patient turnover, and the staff fluctuation [23,24]. In fact, several steps in clinical research workflow are burdened by unnecessary complexity, and it is a real problem considering that, to be an active part of the entire process, clinicians should benefit from data and healthcare digitalization in terms of reduced office work and improvement of clinical practice [19,23]. In reality, data must be extrapolated from the eCRF system, and imported back into data analysis software, and all these steps may lead to increased error rates, with subsequent need for repeated checks [19]. As result, much of the data collected can be wasted. Big Data can be widely exploited only if we apply suitable methods to store and analyze them [15], and also immutability and verifiability properties becomes necessary, together with secure data sharing [7,25,26]. Blockchain technology is one example that has been suggested, providing many benefits in terms of data quality and secure data sharing [7,25,27]. System functioning relies on peer-to-peer networks that make data decentralized and available to multiple people at the same time [7,27]. All data stored this way are encrypted by algorithms called cryptographic hash functions [7,27].
Another source of concern is that ML algorithms are notoriously opaque, similar to black boxes, with physicians being supposed to act according to outputs coming from those clinical decision-support systems without clearly understanding how these outputs are created [28,29]. Some authors pointed out legal issues if patient harm result caused by accepting and acting upon the outputs of these medical AI clinical support system [28,30]. ML opacity occurs for several reasons, including lack of relevant technical knowledge or a cognitive mismatch between human reasoning and AI algorithms [28]. Some authors suggested that making AI more explainable or “interpretable” may be achieved at the expense of loss of accuracy of these systems, emphasizing that the use of less accurate models carries risks for patient health [28]. More attention needs to be directed toward how AI clinical support systems will become integrated into the medical decision-making process, so clinicians will be able to understand the outputs of these systems and embed them into their own clinical decision-making procedures [28,29,31,32]. In this regard, attention is needed also because an algorithmic explanation of AI prediction could be very different from how that prediction has been made [31]. Another source of concerns are potential biases between different AI users, so research is needed to understand how different users interact with AI outputs in various clinical settings [31].
Another problem is that more data does not necessarily mean higher-quality data, so collecting standardized data properly is the most important task, ensuring quality and reliability of Big Data systems [33,34]. Additionally, concrete efforts have to be made to strictly separate those portions of the record that deal with the unique aspects of each patient’s clinical problems from the parts that tabulate demographic and other data that could be used for different purposes [35]. We must also consider that data is a powerful tool but does not represent or replace patients in their complexity and humanity.
Moreover, not all hospitals have sufficient funds or infrastructure to achieve complete digitalization. Hence, the digitalization process itself is shows a major gap between healthcare and the digital world; currently, eHealth records are common but are supported by paper-based elements to various degrees [7]. Moreover, although AI systems have repeatedly been shown to be successful in a wide variety of retrospective medical studies, and the US Food and Drug Administration (FDA) is approving AI and ML products at an accelerating rate, relatively few AI tools have been embedded into medical practice, and the adoption rate of EMR is still low [4,7,24]. Even if all things that surround us have become more and more digitalized, and technology has been deeply integrated into modern life, physicians find themselves locked in a pre-Internet era [36]. Physicians need to be taught the basics to understand AI and the outputs that are given them, in order to integrate them into their decision-making process [11,37,38].
Finally, important ethical concerns exist as regards the potential risk for new technologies to exacerbate existing disparities in healthcare as a result of social, economic, racial, or ethnic characteristics [4,39,40]. As healthcare has shifted to increasingly rely on digital tools for patient care, digital inclusion has become critical to promote healthcare equity; the emerging digital ecosystems have to be re-designed according to proactive engagement, planning, and implementation [39,41,42]. Furthermore, many digital health tools have been developed with homogeneous and advantaged populations in mind; as a result, difficulties in accessing technology, disparities in digital knowledge, and distribution of Internet coverage could create hurdles in accessing these new technologies [39,42]. Limiting health disparities is an component of achieving health equity, which is the ‘attainment of the highest level of health for all people, valuing everyone equally with focused and ongoing societal efforts to address avoidable inequalities, historical and contemporary injustices, and the elimination of health and healthcare disparities” [39]. The digital transformation is an impressive tool that can harm health equity or improve it [43]. Patients experiencing systemic, structural, institutional, and social barriers want and need better and more affordable healthcare access. Therefore, designing systems that address these critical needs should be prioritized as we build the digital tools and platforms that will transform healthcare for the next generation [42]. Used in a targeted way, AI can be a tool for leveling disparities, in order to help highlight and erase the many well-documented inequalities in health [43]. Only in this way can AI improve health, ensuring tailored healthcare for everyone everywhere [43].
Conclusions
In conclusion, healthcare digitization is no longer a possible future, but is a concrete reality; therefore, instead of discussing whether to adhere to this revolutionary change, we need to address the challenges previously debated and engage with this new technology to build a new kind of EBM, supported by a hybrid AI-Human model, in order to provide truly personalized and patient-tailored medicine. Efforts must be made to achieve shared digitalization, not only among AI producers, legislators, and health directors, but also and especially with physicians and clinical researchers, to reduce unnecessary workload and improve clinical practice.
Figures
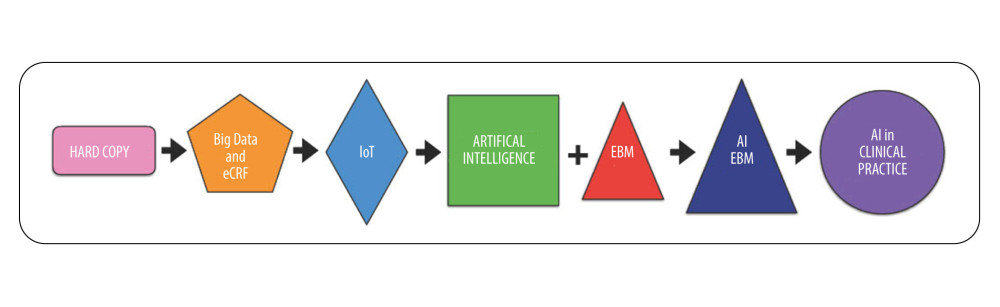 Figure 1. Data evolution’s steps, from paper-based model to application of AI in clinical practice. The first step is represented by data digitalization, both in clinical and research settings. The second step relies on IoT application, which allows interconnection of databases and devices. The third step consists of the collaboration between AI algorithm and EBM. The fourth step is formulation of proper guidelines for AI EBM, and will fully release AI potential in clinical practice. (AI – Artificial Intelligence; IoT – Internet of Things; EMB – Evidence-Based Medicine).
Figure 1. Data evolution’s steps, from paper-based model to application of AI in clinical practice. The first step is represented by data digitalization, both in clinical and research settings. The second step relies on IoT application, which allows interconnection of databases and devices. The third step consists of the collaboration between AI algorithm and EBM. The fourth step is formulation of proper guidelines for AI EBM, and will fully release AI potential in clinical practice. (AI – Artificial Intelligence; IoT – Internet of Things; EMB – Evidence-Based Medicine). 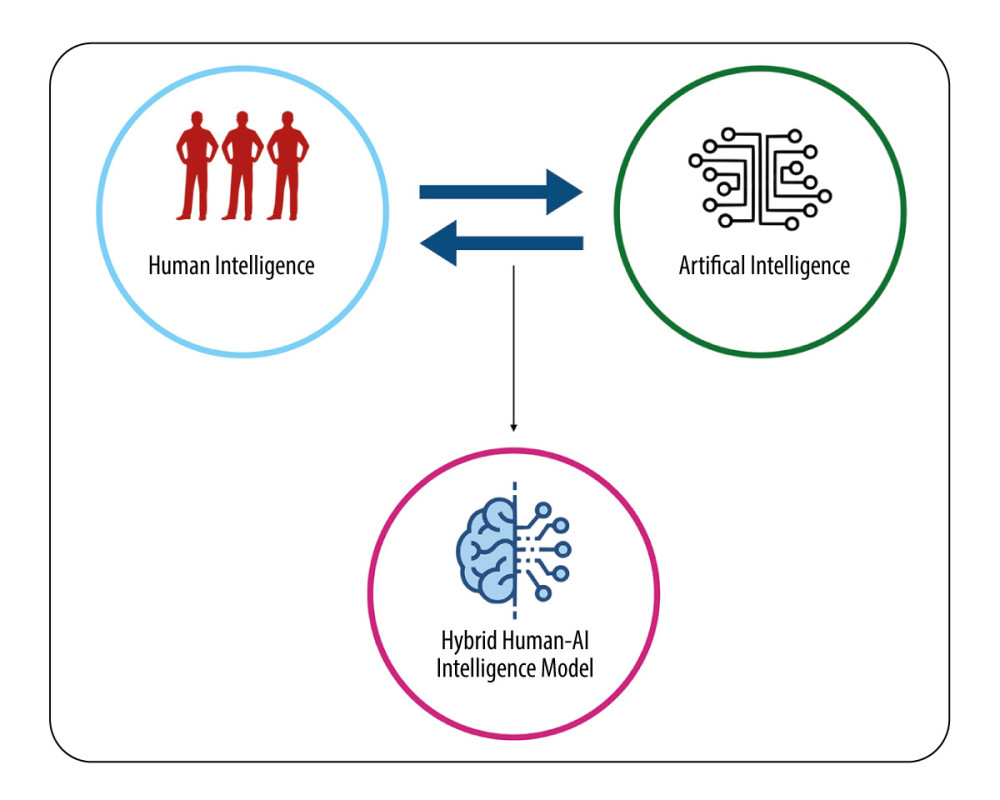 Figure 2. The concept of a Human and Artificial Intelligence (AI) hybrid model developed from the traditional concept of human and AI competition.
Figure 2. The concept of a Human and Artificial Intelligence (AI) hybrid model developed from the traditional concept of human and AI competition. References
1. Connor CW, Artificial intelligence and machine learning in anesthesiology: Anesthesiology, 2019; 131(6); 1346-59
2. Shilo S, Rossman H, Segal E, Axes of a revolution: Challenges and promises of Big Data in healthcare: Nat Med, 2020; 26(1); 29-38
3. Kelly JT, Campbell KL, Gong E, Scuffham P, The internet of things: Impact and implications for health care delivery: J Med Internet Res, 2020; 22(11); e20135
4. Rajpurkar P, Chen E, Banerjee O, Topol EJ, AI in health and medicine: Nat Med, 2022; 28(1); 31-38
5. Jiang F, Jiang Y, Zhi H, Artificial intelligence in healthcare: Past, present and future: Stroke Vasc Neurol, 2017; 2(4); 230-43
6. Sackett DL, Rosenberg WM, Gray JA, Evidence based medicine: What it is and what it isn’t: BMJ, 1996; 312(7023); 71-72
7. Lorkowski J, Pokorski M, Medical records: A historical narrative: Biomedicines, 2022; 10(10); 2594
8. Gillum RF, From papyrus to the electronic tablet: A brief history of the clinical medical record with lessons for the digital age: Am J Med, 2013; 126(10); 853-57
9. Subrahmanya SVG, Shetty DK, Patil V, The role of data science in healthcare advancements: Applications, benefits, and future prospects: Ir J Med Sci, 2022; 191(4); 1473-83
10. Pruneski JA, Williams RJ, Nwachukwu BU, The development and deployment of machine learning models: Knee Surg Sports Traumatol Arthrosc, 2022; 30(12); 3917-23
11. Cho B, Geng E, Arvind V, Understanding artificial intelligence and predictive analytics: A clinically focused review of machine learning techniques: JBJS Rev, 2022; 10(3); 21.00142
12. Naghdi T, Ardalan S, Asghari Adib Z, Moving toward smart biomedical sensing: Biosens Bioelectron, 2023; 223; 115009
13. Munir T, Akbar MS, Ahmed S, A systematic review of internet of things in clinical laboratories: Opportunities, advantages, and challenges: Sensors (Basel), 2022; 22(20); 8051
14. Tang R, Zhang S, Ding C, Artificial intelligence in intensive care medicine: Bibliometric analysis: J Med Internet Res, 2022; 24(11); e42185
15. Vincent JL, Creteur J, Big Data are here to stay!: Anaesth Crit Care Pain Med, 2019; 38(4); 339-40
16. Shelmerdine SC, Arthurs OJ, Denniston A, Sebire NJ, Review of study reporting guidelines for clinical studies using artificial intelligence in healthcare: BMJ Health Care Inform, 2021; 28(1); e100385
17. Ngiam KY, Khor IW, Big Data and machine learning algorithms for health-care delivery [published correction appears in Lancet Oncol. 2019;20(6):293]: Lancet Oncol, 2019; 20(5); e262-e73
18. Bellini V, Coccolini F, Forfori F, Bignami E, The AI evidence-based medicine pyramid: World J Crit Care Med, 2022 [article in press]
19. Installé AJ, Van den Bosch T, De Moor B, Timmerman D, Clinical data miner: An electronic case report form system with integrated data preprocessing and machine-learning libraries supporting clinical diagnostic model research: JMIR Med Inform, 2014; 2(2); e28
20. Ma B, Yang J, Wong FKY, Artificial intelligence in elderly healthcare: A scoping review: Ageing Res Rev, 2022; 83; 101808
21. Yoon JH, Pinsky MR, Clermont G, Artificial intelligence in critical care medicine: Crit Care, 2022; 26(1); 75
22. Hossein Jarrahi M, Lutz C, Newlands G, Artificial intelligence, human intelligence and hybrid intelligence based on mutual augmentation: Big Data Journal, 2022; 9(2); 20539517221142824
23. Montomoli J, Hilty MP, Ince C, Artificial intelligence in intensive care: Moving towards clinical decision support systems: Minerva Anestesiol, 2022; 88(12); 1066-72
24. Dutta B, Hwang HG, The adoption of electronic medical record by physicians: A PRISMA-compliant systematic review: Medicine (Baltimore), 2020; 99(8); e19290
25. Bellini V, Petroni A, Palumbo G, Bignami E, Data quality and blockchain technology: Anaesth Crit Care Pain Med, 2019; 38(5); 521-22
26. Bhatia J, Italiya K, Jadeja K, An overview of fog data analytics for IoT applications: Sensors (Basel), 2022; 23(1); 199
27. Kumar R, Arjunaditya , Singh D, AI-powered blockchain technology for public health: A contemporary review, open challenges, and future research directions: Healthcare (Basel), 2022; 11(1); 81
28. Hatherley J, Sparrow R, Howard M, The virtues of interpretable medical artificial intelligence: Camb Q Healthc Ethics, 2022 [Online ahead of print]
29. Bate A, Luo Y, Artificial intelligence and machine learning for safe medicines: Drug Saf, 2022; 45(5); 403-5
30. Nichol AA, Halley MC, Federico CA, Not in my AI: Moral engagement and disengagement in health care AI development: Pac Symp Biocomput, 2023; 28; 496-506
31. Kostick-Quenet KM, Gerke S, AI in the hands of imperfect users: NPJ Digit Med, 2022; 5(1); 197
32. Crossnohere NL, Elsaid M, Paskett J, Guidelines for artificial intelligence in medicine: Literature review and content analysis of frameworks: J Med Internet Res, 2022; 24(8); e36823
33. Simpao AF, Rehman MA, Anesthesia information management systems: Anesth Analg, 2018; 127(1); 90-94
34. Kim HS, Kim DJ, Yoon KH, Medical Big Data is not yet available: Why we need realism rather than exaggeration: Endocrinol Metab (Seoul), 2019; 34(4); 349-54
35. Reinus JF, The electronic medical record, Lawrence Weed, and the quality of clinical documentation: Am J Med, 2021; 134(3); e143-e44
36. Mandl KD, Kohane IS, Escaping the EHR trap – the future of health IT: N Engl J Med, 2012; 366(24); 2240-42
37. Chomutare T, Tejedor M, Svenning TO, Artificial intelligence implementation in healthcare: A theory-based scoping review of barriers and facilitators: Int J Environ Res Public Health, 2022; 19(23); 16359
38. Garvey KV, Thomas Craig KJ, Considering clinician competencies for the implementation of artificial intelligence-based tools in health care: Findings from a scoping review: JMIR Med Inform, 2022; 10(11); e37478
39. Samuels-Kalow M, Jaffe T, Zachrison K, Digital disparities: designing telemedicine systems with a health equity aim: Emerg Med J, 2021; 38(6); 474-76
40. London AJ, Artificial intelligence in medicine: Overcoming or recapitulating structural challenges to improving patient care?: Cell Rep Med, 2022; 3(5); 100622
41. Rodriguez JA, Shachar C, Bates DW, Digital inclusion as health care – supporting health care equity with digital-infrastructure initiatives: N Engl J Med, 2022; 386(12); 1101-3
42. Lyles CR, Wachter RM, Sarkar U, Focusing on digital health equity: JAMA, 2021; 326(18); 1795-96
43. Chen IY, Joshi S, Ghassemi M, Treating health disparities with artificial intelligence: Nat Med, 2020; 26(1); 16-17
Figures
 Figure 1. Data evolution’s steps, from paper-based model to application of AI in clinical practice. The first step is represented by data digitalization, both in clinical and research settings. The second step relies on IoT application, which allows interconnection of databases and devices. The third step consists of the collaboration between AI algorithm and EBM. The fourth step is formulation of proper guidelines for AI EBM, and will fully release AI potential in clinical practice. (AI – Artificial Intelligence; IoT – Internet of Things; EMB – Evidence-Based Medicine).
Figure 1. Data evolution’s steps, from paper-based model to application of AI in clinical practice. The first step is represented by data digitalization, both in clinical and research settings. The second step relies on IoT application, which allows interconnection of databases and devices. The third step consists of the collaboration between AI algorithm and EBM. The fourth step is formulation of proper guidelines for AI EBM, and will fully release AI potential in clinical practice. (AI – Artificial Intelligence; IoT – Internet of Things; EMB – Evidence-Based Medicine). Figure 2. The concept of a Human and Artificial Intelligence (AI) hybrid model developed from the traditional concept of human and AI competition.
Figure 2. The concept of a Human and Artificial Intelligence (AI) hybrid model developed from the traditional concept of human and AI competition. In Press
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








