06 April 2021 : Review article
Impact of Cardiovascular Diseases on COVID-19: A Systematic Review
Qingtai Cao1B*, HanYu Lei23E, MengLing Yang23B, Le Wei23A, YinMiao Dong2E, JiaHao Xu23F, Mi Nasser4C, MengQi Liu23F, Ping Zhu4G, LinYong Xu5G, MingYi Zhao2AGDOI: 10.12659/MSM.930032
Med Sci Monit 2021; 27:e930032
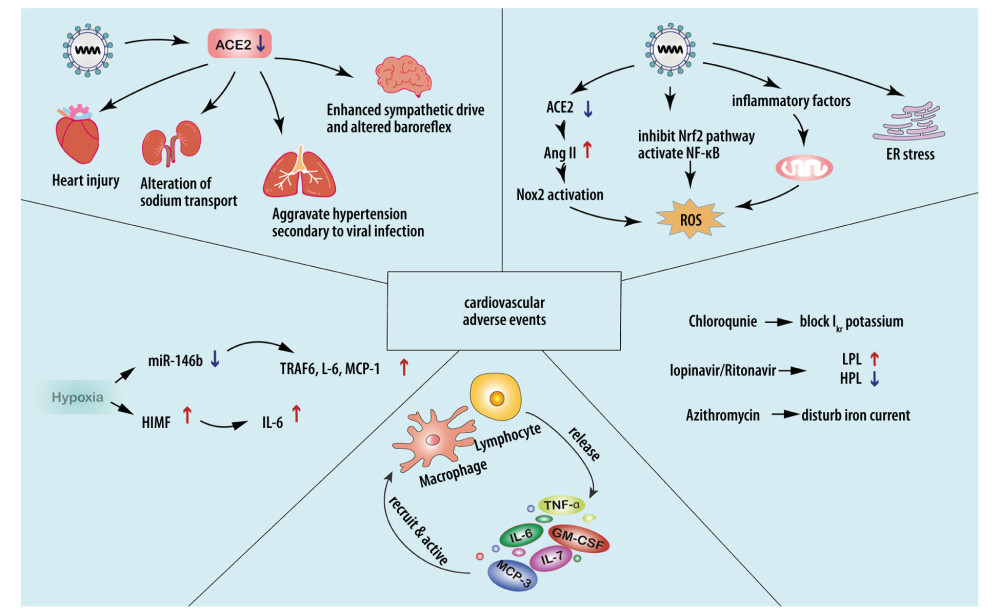
Figure 2 Possible mechanisms for cardiovascular injuries after SARS-CoV-2 infection. a) Stress: Downregulation of ACE2 could lead to excessive Nox2 activation, inducing ROS accumulation. High levels of TNF-α and IL-6 can increase mitochondrial stress, leading to higher levels of oxidative stress. ER stress can destabilize atherosclerotic plaque through increasing NF-κB-induced GM-CSF. b) Hypoxia: SARS-CoV-2-related hypoxemia can affect the miR-146b-TRAF6-IL-6/CCL2 (MCP-1) axis and induce expression of HIMF, promoting the production of proinflammatory cytokines. c) Accumulation of proinflammatory cytokines contributes to cardiovascular complications. d) Drug-related injuries: Drugs administered in treating SARS-CoV-2 can cause cardiovascular complications. Chloroquine, lopinavir/ritonavir, and azithromycin can affect the normal rhythm of the heart. Lopinavir/ritonavir can also increase LDL and suppress HDL, destabilizing atherosclerotic plaque. Pegylated interferon-α can lead to the upregulation of TNF-α.








