16 June 2020: Clinical Research
Knowledge and Awareness of Venous Thromboembolism in Intensive Care Units in Zhejiang Province, China: A Cross-Sectional Survey
Jing Yan1AG, Jia Zhou1BC, Junhai Zhen1BC, Li Li1ABEG*, Zhejiang Provincial Critical Care Clinical Research Group1BEDOI: 10.12659/MSM.923378
Med Sci Monit 2020; 26:e923378
Abstract
BACKGROUND: The 2009 China Intensive Care Units (ICU) prevention guidelines lack venous thromboembolism (VTE) risk assessment. This survey was conducted to assess the risk of VTE, develop and establish a diagnosis, and provide prevention and treatment guidelines for ICU VTE.
MATERIAL AND METHODS: A cross-sectional questionnaire survey of ICU doctors ICUs was conducted online in the tertiary and secondary hospitals of Zhejiang province in China. The questionnaire included VTE-related hospital hardware information, VTE awareness, knowledge, and monitoring system.
RESULTS: The risk assessment rates at the time of admission and changed disease condition were 67.7% and 60.4%, respectively. D-dimer and ultrasound were commonly used for VTE screening. Heparin is preferred for short-term intravenous anticoagulant therapy, and warfarin is preferred for long-term therapy. We found that 23.53% of the ICUs have bedside ultrasound and staff for ultrasound examination, and 59.4% of the hospitals are equipped with VTE monitoring information systems. The VTE early identification specification is the key to whether the VTE assessment is performed after the patient enters the ICU.
CONCLUSIONS: The survey assessed the VTE risk and key VTE management elements. However, high heterogeneities were detected in the assessment. The ICU doctors have relatively limited awareness of VTE. Thus, there is an urgent need to update and standardize the ICU VTE guidelines for the prevention and treatment of VTE in China.
Keywords: Awareness, Intensive Care Units, Knowledge, venous thromboembolism, Anticoagulants, Clinical Competence, Critical Care, Cross-Sectional Studies, Early Diagnosis, Fibrin Fibrinogen Degradation Products, Heparin, Intermittent Pneumatic Compression Devices, Mass Screening, Personnel Management, Point-of-Care Systems, Practice Patterns, Physicians', Risk Assessment, Secondary Care Centers, Stockings, Compression, Surveys and Questionnaires, Tertiary Care Centers, Ultrasonography, Warfarin
Background
The incidence of venous thromboembolism (VTE) [1–5] ranks third among all cardiovascular diseases. It is estimated to annually affect 600 000 patients with deep vein thrombosis (DVT) [6–9] in the United States, and 50 000–200 000 deaths occur due to pulmonary thromboembolism (PTE) [10–12]. The incidence of post-thrombotic syndrome that affects the limbs is 35–69% and 49–100% at 3 and 5 years of DVT, respectively. According to the data, 10% of hospital deaths are caused due to VTE. In Europe, more than 500 000 people die each year due to VTE, which exceeds the combined death toll of acquired immune deficiency syndrome (AIDS), prostate cancer, breast cancer, and highway accidents. VTE is a common disorder in China and other Asian countries. Clinically, only 10–17% of patients with DVT have obvious symptoms of swelling of the lower extremities, local deep tenderness, and dorsiflexion. Severe clinical features and signs of DVT development include pulmonary embolism, with mortality rates of 9–50% and the vast majority of deaths occur within minutes to hours after symptom onset. The signs and symptoms of DVT commonly occur in patients after surgery, trauma, advanced cancer, coma, and prolonged bed rest. In China, the incidence of DVT after orthopedics and general surgery is 10–63% [13]. The exact incidence of VTE in ICU patients is unclear [14], but clinical observations and prospective studies suggest it to be 5–33%. These estimations are closely correlated to knowledge and awareness of the clinical nurses about venous thromboprophylaxis care.
The occurrence of VTE often involves oversight by various departments., and the prevention and treatment of VTE vary in different departments. Critically ill ICU patients are considered to be at high risk for VTE, thereby necessitating great attention [15]. VTE patients in the ICU share similar general risk factors with patients in other departments, such as age, immobilization, obesity, history of VTE, stroke, respiratory or heart failure, pregnancy, and recent surgery, [16–20]. Additionally, specific risk factors for VTE patients in the ICU have been reported [18,14], including mechanical ventilation, vasopressor use, and central venous catheter use. Although there are guidelines and consensus in China, including the China guidelines for the diagnosis and treatment of PTE (2018) and the Chinese patient service and the diagnosis and treatment of hospitalized patients with VTE, problems persist. First, VTE awareness at different levels of hospitals vary, leading to a high degree of heterogeneity in the implementation of guidelines. In addition, specialized guidelines for the ICU are lacking; only 1 China ICU patient DVT prevention guideline has been issued in 2009, but it does not address risk assessment of DVT. Therefore, the present study assessed the awareness of ICU physicians about VTE risk, as well as the current state of the system to provide reference information for promoting the establishment of VTE guidelines for ICUs.
The prevalence of VTE is often underestimated in ICUs, as it is often clinically unnoticeable and difficult to diagnose. Therefore, this study conducted a questionnaire survey on the knowledge and awareness of ICU VTE in Zhejiang province in China to enhance the awareness and perception of the clinical staff for improving VTE prevention and treatment in the ICU. These findings highlight the need to develop and implement new ICU VTE guidelines in China [21–26].
Material and Methods
STUDY DESIGN:
A cross-sectional survey of doctors currently working in ICUs in Zhejiang province, China, was conducted. Zhejiang province has 11 cities (Figure 1). The questionnaire was independently reviewed by 3 doctors (1 chief physician and 2 deputy-chief physicians) to ensure the clarity and readability of the questions. The questionnaires were obtained as online forms and directly sent to the ICU chief or deputy-chief physician of leading tertiary and secondary hospitals via the WeChat app.
QUESTIONNAIRES SETTING:
The questionnaire was developed after extensive literature review of current clinical practice based on Chinese guidelines for the diagnosis and treatment of PTE (2018) and Chinese patient service and the diagnosis and treatment of hospitalized patients with VTE. The contents included a total of 52 questions regarding doctor’s personal information, hospital hardware information, VTE awareness, and knowledge of VTE assessment, identification, and monitoring (Supplementary material). The components of the questionnaire covered the 4 key elements of ICU VTE management, including assessment, prevention, diagnosis and treatment, and improvement (Figure 2). All the questions must be answered and submitted online to enter the survey database.
DISTRIBUTION AND COLLECTION:
The questionnaires were distributed to 108 chief or deputy-chief physicians in the tertiary and secondary hospitals of Zhejiang province via online WeChat groups. Each ICU was represented by a doctor. After 1 week, the online questionnaire survey was closed, and the data were summarized and analyzed. In case of any repetitive answer sheets from 1 ICU, it was necessary to check whether the answers for the questionnaire were identical. One questionnaire was chosen if the answers are identical, and if not, 1 extra step of the phone call was made to the corresponding ICU department to confirm the answers.
STATISTICAL ANALYSIS:
SPSS 22.0 statistical software (IBM SPSS Inc.) was used for statistical analysis. The data were represented as frequency, percentage, mean, and standard deviation, and the rank-sum test was used to compare data between the 2 groups. The risk factors of VTE awareness were analyzed by multivariate logistic regression. The difference was statistically significant if P<0.05.
Results
BASELINE CHARACTERISTICS:
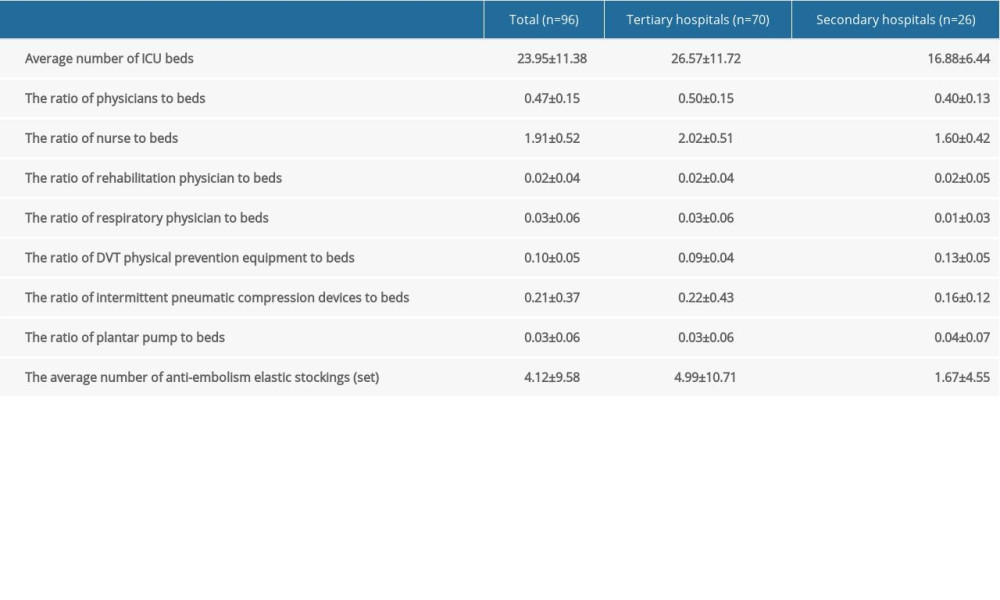
From July 6 to 12, 2019, a total of 172 questionnaires were distributed; of these, 96 were considered valid, with an effective recovery rate of 56%. A total of 96 questionnaires were completed, which encompassed 70 tertiary hospitals and 26 secondary hospitals. Among these, there were 88 general ICUs, 4 were emergency ICUs, and 4 were internal medicine or surgical ICUs. The 70 tertiary hospitals, including 63 general ICUs, 1 internal medical ICU, 2 surgical ICUs, and 4 emergency ICUs, were surveyed. The 26 hospitals surveyed included 25 general ICUs and 1 internal medical ICU. Together, all hospitals consisted of an average number of ICU beds of 23.95±11.38. The average number of beds in tertiary hospitals was 26.57±11.72, and that of secondary hospitals was 16.88±6.44. However, the ratio of physicians to beds, nurses to beds, rehabilitation physicians to beds, and respiratory physicians to beds was 0.47±0.15, 1.91±0.52, 0.02±0.04, and 0.03±0.06, respectively. In terms of DVT-related hospital hardware information, the ratio of DVT physical prevention equipment to beds, intermittent pneumatic compression devices to beds, and plantar pumps to beds was 0.10±0.05, 0.21±0.37, and 0.03±0.06, respectively. The average number of anti-embolism elastic stockings was 4.12±9.58 (Table 1).
Doctors are regarded as ICU directors or deputy directors for clinical work in the hospitals of Zhejiang province, consisting of 88% chief physicians and 12% deputy-chief physicians.
AWARENESS OF ASSESSMENT AND TREATMENT OF VTE:
D-dimer and early electrocardiogram screening are crucial for the analysis of the risk factors of VTE awareness. Strikingly, in the ICU departments of China, D-dimer and ultrasound are commonly used for screening, wherein 59.4% of 96 ICUs prefer ultrasound as their first choice of device, and 88.5% of the ICUs have bedside ultrasound equipment. Ultrasound plays a major role in early VTE screening, but only 80.21% of the ICUs have early ultrasound screening for VTE. The main reasons for the unavailability of ultrasound included no ultrasound qualification (57.89%), insufficient staff (42.11%), and no equipment (36.84%). The 96 ICUs with bedside ultrasound machines accounted for 88.54%. For ICUs with bedside ultrasound, only 23.53% (20) included professional staff responsible for bedside ultrasound examination, which might make it difficult to ensure the quality of inspection and quality control. Among the staff from 20 ICUs, 13 were ICU doctors (65%), 6 were sonographers (30%), and 1 was an ICU doctor and sonographer. All ICU doctors who performed bedside ultrasound examinations were qualified for the same, wherein 11.5% had general ultrasound training, and only 2.1% had ultrasound specialist training.
The criteria for VTE clinical risk assessment and awareness mainly focused on the admission and the condition of disease changes, which included patients with a risk assessment rate of 67.7% and 60.4%, respectively (Figure 3).
The VTE risk score plays a critical role in assessing disease. The Caprini scoring system was used in 69 (71.9%) ICUs, butthe Padua, Well, and Geneva scoring systems were not used routinely (Figure 4).
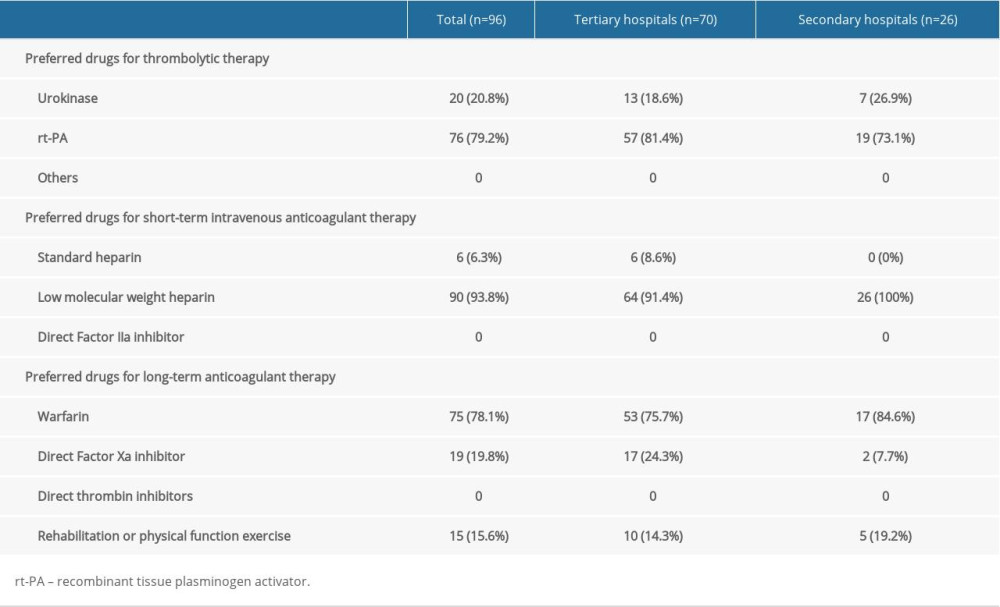
For VTE clinical treatment, recombinant tissue plasminogen activator (rt-PA) accounted for 80% of the preferred drugs for thrombolytic therapy, while the use of urokinase in secondary hospitals was slightly higher than that in tertiary hospitals (Table 2). The preferred drug for short-term intravenous anticoagulant therapy is low molecular weight heparin (LMWH), the preferred drug for anticoagulant therapy for long-term therapy is warfarin, and the use of new oral anticoagulant drugs is still relatively low (<30%), even in tertiary hospitals.
VTE MANAGEMENT RULES AND REGULATIONS:
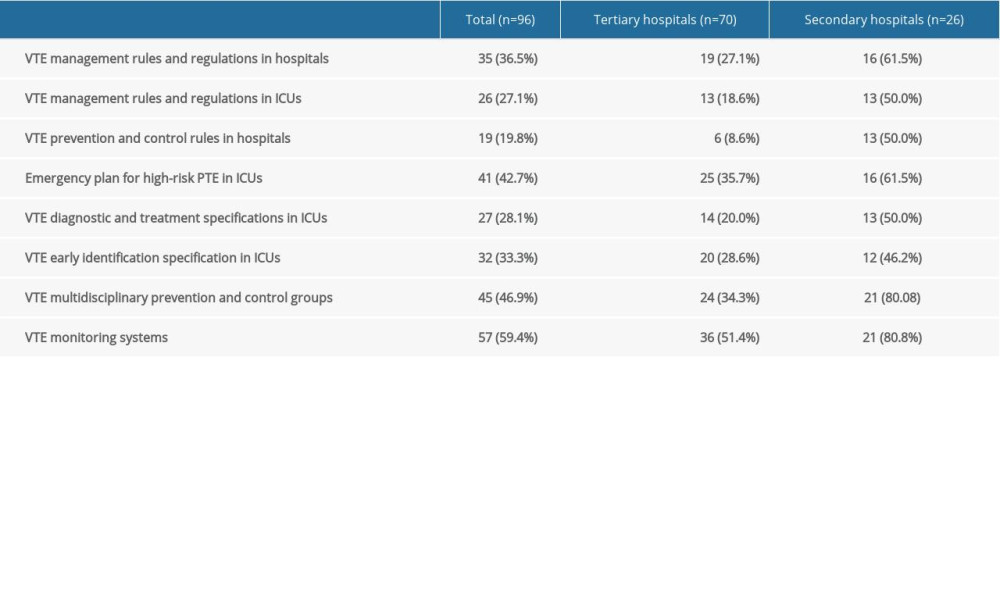
The management rules and regulations for VTE were established in 27.1% of the ICU departments, and multidisciplinary VTE prevention and control was performed in 46.9% of the ICU departments. In the VTE prevention and control team, the number of respiratory doctors remained relatively low, consisting mainly of doctors and nurses from the ICU department, followed by rehabilitation doctors. In the VTE multidisciplinary treatment team, the proportion of respiratory departments was relatively low. Also, there were fewer VTE monitoring information systems in the hospital (Table 3).
Although 76.04% of the ICUs included VTE assessment and prevention procedures, only 5.48% of the ICUs had dedicated staff to conduct the VTE assessment and prevention management. We found that 66.67% of the ICUs developed early VTE identification specifications, 71.88% of the ICUs developed VTE diagnostic and therapeutic specifications, and 57.29% of the ICUs developed high-risk PTE emergency plans. Only 40.63% of hospitals had VTE monitoring information systems, and 39.58% of the ICUs had dedicated staff for monitoring, analysis, and improvement of VTE (Figure 5).
RISK FACTORS OF VTE AWARENESS:
After multivariate regression analysis, the early identification of VTE remained the key factor determining whether the disease was assessed after the patient entered the ICU (OR=20.47, P=0.005).
Discussion
The awareness of VTE in the ICUs varies among hospitals. Significant differences were found regarding VTE knowledge, awareness, the formation of rules and regulations, and hardware conditions at different levels of hospitals. To prevent and treat VTE in ICUs, VTE awareness should be improved.
The number of beds in China’s ICUs is high, but the number of specialists and the amount of equipment remains low, which might in turn may affect the prevention and detection of conventional VTE. In recent years, the incidence of VTE has been increasing in critically ill ICU patients. A global ENDorse survey revealed that 41.5% of medically ill patients were deemed to be at risk for VTE in the ICU, ranging from 31.2% of patients with gastrointestinal/hepatobiliary diseases to 68.1% with ischemic stroke and up to 100% with acute heart failure, active non-infectious respiratory diseases, or pulmonary infections [1,2,27]. In China, VTE training and assessment showed rapid development in the prevention and treatment of VTE in the ICU. The current results demonstrated that VTE has become a routine assessment in ICUs. The Caprini scoring system has been adopted by most of the ICUs that are now focusing on VTE assessment during patient admission and are altered in the patient’s condition. Despite advances in the management of VTE, the knowledge of the Asian population regarding the incidence, prevalence, recurrence, and risk factors is limited, requiring an increase in the awareness of VTE. Although there are ICU VTE-related guidelines and consensus from 2009, there is no information regarding risk assessment. ICU physicians need to improve their awareness of VTE and need for prevention guidelines for Chinese ICU patients. The DVT prevention guidelines issued in 2009 for ICUs do not cover VTE risk assessment. Typically, the clinical assessment, diagnostic testing, therapeutic considerations, and risk factors for VTE are identical in Asian and Western populations [28].
Intriguingly, the treatment plans for VTE are not consistent among ICUs. LMWH is applied in 93.8% of ICUs. It is a crucial drug used as an anticoagulant therapy in ICUs, with a molecular weight between 3.5 and 5.0 kDa. Due to the low molecular weight, the biochemical and pharmacological properties are improved; thus, it has more advantages, such as good absorption, long half-life, high bioavailability, and no requirement for lab monitoring, in contrast to standard heparin [29]. The robust antithrombin effect of heparin has been the main cause of ICU hemorrhagic syndrome and thus is used in only 6.3% of ICUs. Since LMWH mainly induces anticoagulation activity factor Xa and has less effect on antithrombin, it can reduce adverse reactions such as hemorrhage caused by heparin and achieve effective anticoagulant function; thus, it primarily applied for anticoagulation in ICUs [30]. For VTE prophylaxis, there is no evidence suggesting that the bleeding risk in Asians using LMWH is higher than that in the Western population [28]. The conventional drug warfarin was used in 78.1% of the ICUs, while the usage ratio of novel oral anticoagulants (NOACs) was relatively low. Warfarin application requires monitoring of international normalized ratio (INR), which is a relatively cumbersome procedure. Moreover, the activity of metabolizing the enzyme of warfarin in the liver of Asians is quite different from that for the Western population; therefore, the dose should be lowered. The optimal INR range for Asians is narrower, between 0.7% and 1.1%, as compared to that for other populations, and the risk of intracranial hemorrhage is significantly higher than in the Western population, while the INR is lower [31,32]. Also, the NOACs might be more suitable for Asians [33]; nonetheless, the low proportion could be attributed to drug awareness and price. In the thrombolytic process, the use of recombinant tissue-type plasminogen activator (rt-PA) and LMWH also remained higher. However, this study did not investigate compliance with American College of Chest Physicians (CHEST) guidelines for antithrombotic therapy with respect to VTE disease guidelines [34].
Currently, Chinese hospitals are actively establishing VTE prevention and control systems. They are establishing active and effective risk assessment tools, developing effective prevention methods and strategies, and standardizing VTE prevention, diagnosis, and treatment. Despite these advances in the management of VTE, knowledge on the incidence, prevalence, recurrence, and risk factors is limited and requires increased awareness. At present, in China, the ICUs, hospitals, and administrative departments are focusing on VTE management and a comprehensive prevention and treatment system that involves the participation of management departments and multidisciplinary clinics. Although it takes a long time to implement this strategy, the VTE awareness of Chinese doctors and patients would be greatly improved, and a large number of treatments would be standardized.
Nevertheless, it is necessary to revise the guidelines for Chinese ICU patients, strengthen the promotion of guidelines, and improve the hospital equipment, software, information facilities, and the need for VTE system construction. In addition, national evidence-based clinical practice guidelines should be developed and implemented to reduce this variability and improve VTE management in China [28].
The other limitations of this study were as follows: Zhejiang is a developed province in China, albeit with limited representation. No random sampling was conducted, and hence, the sample collection of hospitals might be biased. In addition, the sample size was limited and does not encompass all ICUs of Zhejiang province, the questionnaire lacked standard questions, and the reliability and validity of the questionnaire were not strictly evaluated. Finally, this survey lacked VTE (DVT and PE) morbidity data.
Conclusions
AVAILABILITY OF DATA AND MATERIALS:
The completed questionnaires were collected and safely stored in the principal investigator’s office. Data were saved into an appropriately designed Excel spreadsheet. The datasets used and analyzed are available from the corresponding author on request.
Figures
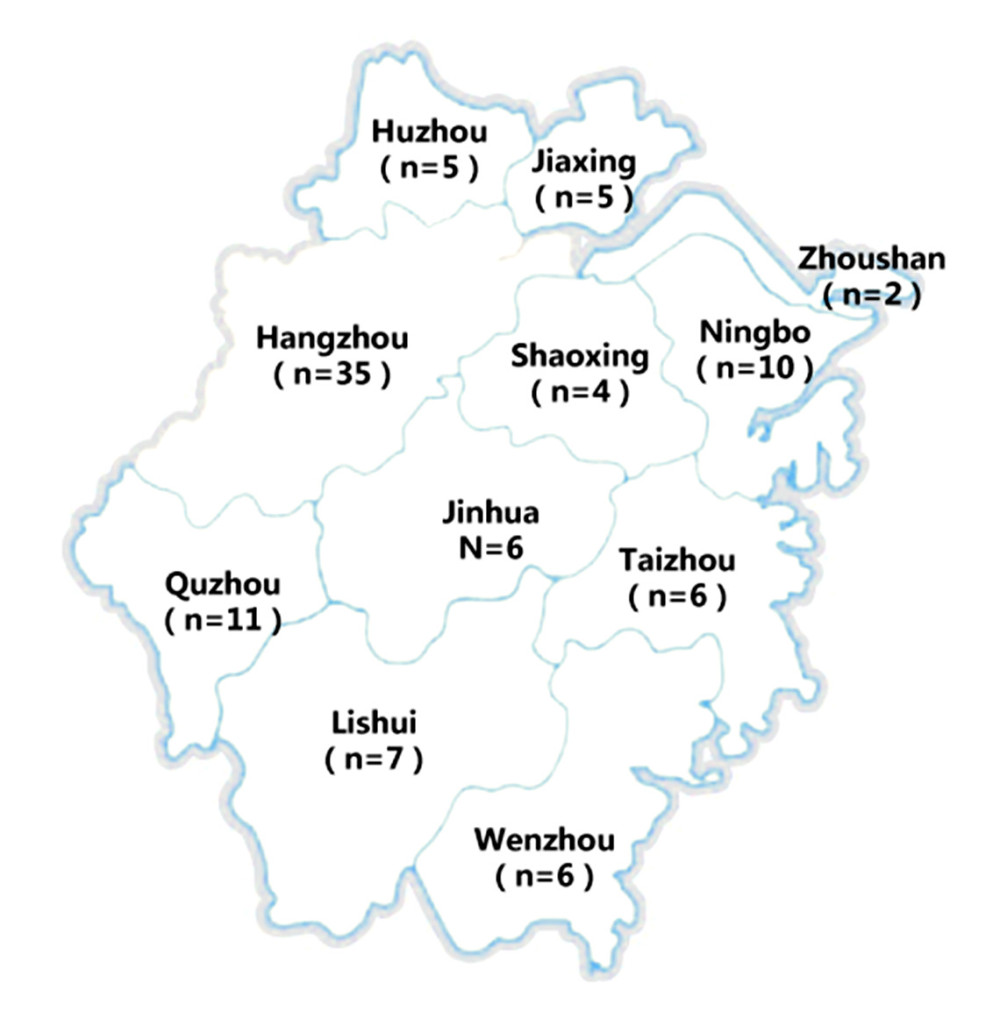 Figure 1. Map of Zhejiang province with 11 cities.
Figure 1. Map of Zhejiang province with 11 cities. 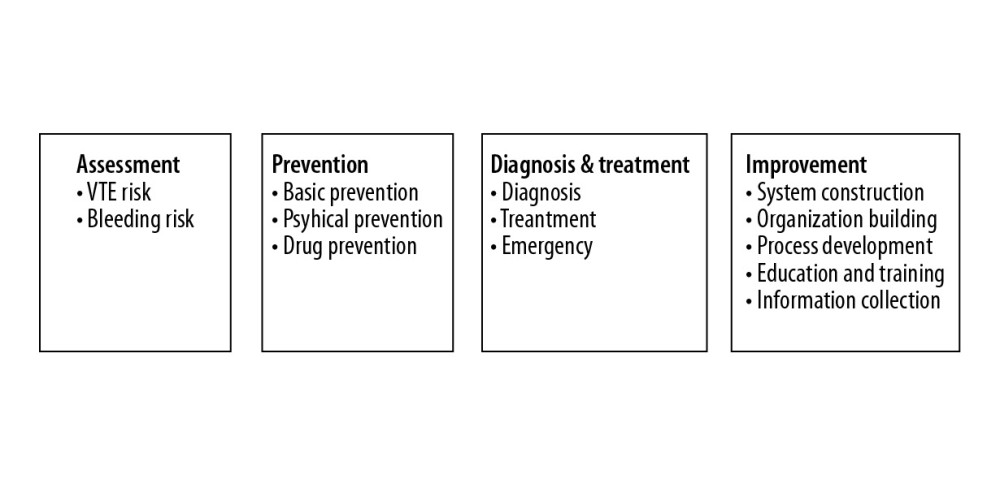 Figure 2. Key elements of VTE management in the Intensive Care Units (ICU).
Figure 2. Key elements of VTE management in the Intensive Care Units (ICU). 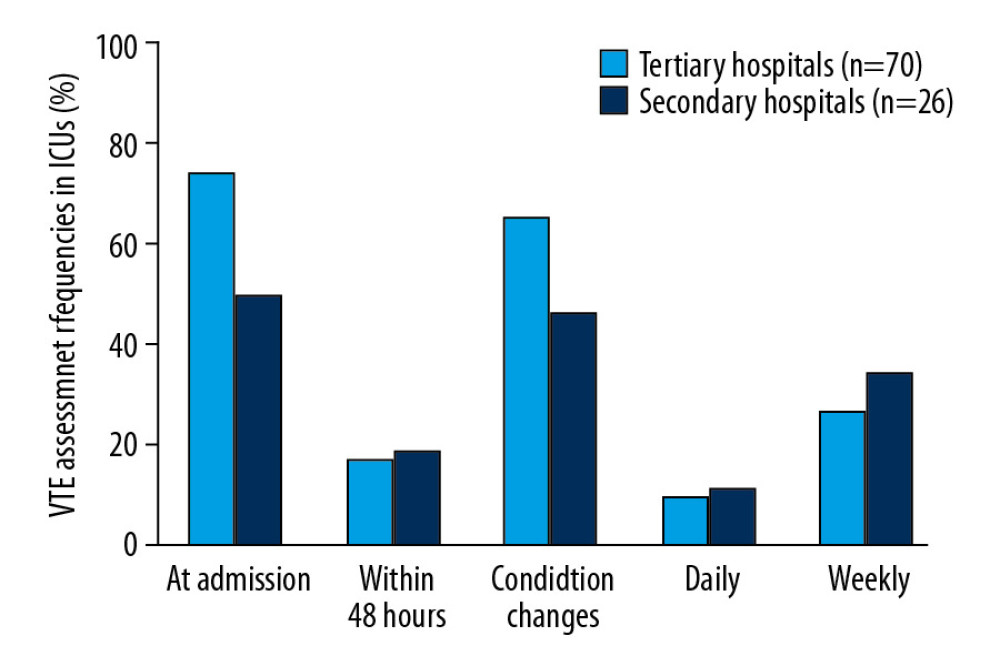 Figure 3. VTE assessment frequencies in the ICUs of Zhejiang province, China.
Figure 3. VTE assessment frequencies in the ICUs of Zhejiang province, China. 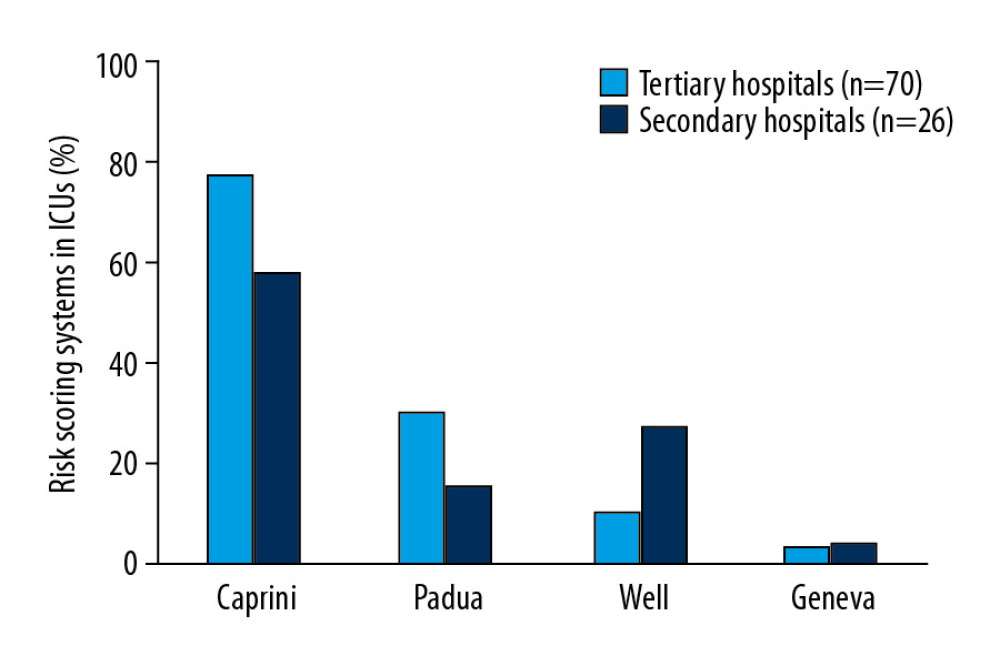 Figure 4. VTE risk scoring systems in the ICUs of Zhejiang province, China.
Figure 4. VTE risk scoring systems in the ICUs of Zhejiang province, China. 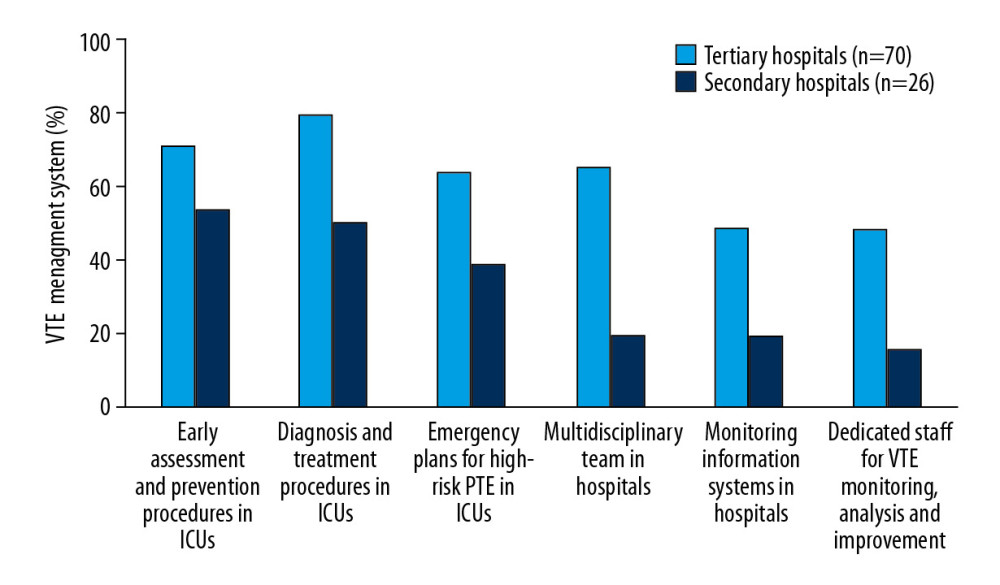 Figure 5. VTE management system in the ICUs of Zhejiang province, China.
Figure 5. VTE management system in the ICUs of Zhejiang province, China. References
1. Schulman S, Ageno W, Konstantinides SV, Venous thromboembolism: Past, present and future: Thromb Haemost, 2017; 117; 1219-29
2. Brenner B, Hull R, Arya R, Evaluation of unmet clinical needs in prophylaxis and treatment of venous thromboembolism in high-risk patient groups: Cancer and critically ill: Thromb J, 2019; 17; 6
3. Klok FA, Barco S, Siegerink B, Measuring functional limitations after venous thromboembolism: A call to action: Thromb Res, 2019; 178; 59-62
4. Serhal M, Barnes GD, Venous thromboembolism: A clinician update: Vasc Med, 2019; 24; 122-31
5. Stevens H, Tran H, Gibbs H, Venous thromboembolism: Current management: Aust Prescr, 2019; 42; 123-26
6. Thachil J, Deep vein thrombosis: Hematology, 2014; 19; 309-10
7. Di Nisio M, van Es N, Buller HR, Deep vein thrombosis and pulmonary embolism: Lancet, 2016; 388; 3060-73
8. Kafeza M, Shalhoub J, Salooja N, A systematic review of clinical prediction scores for deep vein thrombosis: Phlebology, 2017; 32; 516-31
9. Robert-Ebadi H, Righini M, Management of distal deep vein thrombosis: Thromb Res, 2017; 149; 48-55
10. Torbicki A, Perrier A, Konstantinides S, Guidelines on the diagnosis and management of acute pulmonary embolism: The Task Force for the Diagnosis and Management of Acute Pulmonary Embolism of the European Society of Cardiology (ESC): Eur Heart J, 2008; 29; 2276-315
11. Becattini C, Agnelli G, Risk stratification and management of acute pulmonary embolism: Hematology Am Soc Hematol Educ Program, 2016; 2016; 404-12
12. Handal-Orefice RC, Moroz LA, Pulmonary embolism management in the critical care setting: Semin Perinatol, 2019; 43; 205-12
13. Boddi M, Peris A, Deep vein thrombosis in intensive care: Adv Exp Med Biol, 2017; 906; 167-81
14. Minet C, Potton L, Bonadona A, Venous thromboembolism in the ICU: Main characteristics, diagnosis and thromboprophylaxis: Crit Care, 2015; 19; 287
15. Fumis RRL, Schettino GPP, Rogovschi PB, Correa TD, Would you like to be admitted to the ICU? The preferences of intensivists and general public according to different outcomes: J Crit Care, 2019; 53; 193-97
16. Cook D, Crowther M, Meade M, Deep venous thrombosis in medical-surgical critically ill patients: Prevalence, incidence, and risk factors: Crit Care Med, 2005; 33; 1565-71
17. Darze ES, Latado AL, Guimaraes AG, Incidence and clinical predictors of pulmonary embolism in severe heart failure patients admitted to a coronary care unit: Chest, 2005; 128; 2576-80
18. Geerts WH, Bergqvist D, Pineo GF: Chest, 2008; 133; 381s-453s
19. Shorr AF, Williams MD, Venous thromboembolism in critically ill patients. Observations from a randomized trial in sepsis: Thromb Haemost, 2009; 101; 139-44
20. Minet C, Lugosi M, Savoye PY, Pulmonary embolism in mechanically ventilated patients requiring computed tomography: Prevalence, risk factors, and outcome: Crit Care Med, 2012; 40; 3202-8
21. Lyman GH, Bohlke K, Falanga A, Venous thromboembolism prophylaxis and treatment in patients with cancer: American Society of Clinical Oncology clinical practice guideline update: J Oncol Pract, 2015; 11; e442-44
22. Jacobs B, Pannucci C, Scoring systems for estimating risk of venous thromboembolism in surgical patients: Semin Thromb Hemost, 2017; 43; 449-59
23. Young G, How I treat pediatric venous thromboembolism: Blood, 2017; 130; 1402-8
24. Bartlett MA, Bierle DM, Saadiq RA, Updates in venous thromboembolism management: Evidence published in 2017: Hosp Pract (1995), 2018; 46; 183-88
25. Lee AYY, Overview of VTE treatment in cancer according to clinical guidelines: Thromb Res, 2018; 164(Suppl 1); S162-67
26. Morgan J, Checketts M, Arana A, Prevention of perioperative venous thromboembolism in pediatric patients: Guidelines from the Association of Paediatric Anaesthetists of Great Britain and Ireland (APAGBI): Paediatr Anaesth, 2018; 28; 382-91
27. Bergmann JF, Cohen AT, Tapson VF, Venous thromboembolism risk and prophylaxis in hospitalised medically ill patients. The ENDORSE Global Survey: Thromb Haemost, 2010; 103; 736-48
28. Liew NC, Alemany GV, Angchaisuksiri P, Asian venous thromboembolism guidelines: Updated recommendations for the prevention of venous thromboembolism: Int Angiol, 2017; 36; 1-20
29. Fan Y, Jiang M, Gong D, Zou C, Efficacy and safety of low-molecular-weight heparin in patients with sepsis: A meta-analysis of randomized controlled trials: Sci Rep, 2016; 6; 25984
30. A-Lai GH, Zhu YK, Li G, Preoperative thromboprophylactic administration of low-molecular-weight-heparin significantly decreased the risk of intraoperative bleeding compared with heparin in patients undergoing video-assisted lobectomy for lung cancer: Ann Transl Med, 2019; 7; 90
31. Gan GG, Teh A, Goh KY, Racial background is a determinant factor in the maintenance dosage of warfarin: Int J Hematol, 2003; 78; 84-86
32. Ma C, Zhang Y, Xu Q, Influence of warfarin dose-associated genotypes on the risk of hemorrhagic complications in Chinese patients on warfarin: Int J Hematol, 2012; 96; 719-28
33. Bai Y, Guo SD, Shantsila A, Lip GYH, Modelling projections for the risks related with atrial fibrillation in East Asia: A focus on ischaemic stroke and death: Europace, 2018; 20; 1584-90
34. Kearon C, Akl EA, Ornelas J, Antithrombotic therapy for VTE disease: CHEST Guideline and Expert Panel Report: Chest, 2016; 149; 315-52
Figures
 Figure 1. Map of Zhejiang province with 11 cities.
Figure 1. Map of Zhejiang province with 11 cities. Figure 2. Key elements of VTE management in the Intensive Care Units (ICU).
Figure 2. Key elements of VTE management in the Intensive Care Units (ICU). Figure 3. VTE assessment frequencies in the ICUs of Zhejiang province, China.
Figure 3. VTE assessment frequencies in the ICUs of Zhejiang province, China. Figure 4. VTE risk scoring systems in the ICUs of Zhejiang province, China.
Figure 4. VTE risk scoring systems in the ICUs of Zhejiang province, China. Figure 5. VTE management system in the ICUs of Zhejiang province, China.
Figure 5. VTE management system in the ICUs of Zhejiang province, China. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387