09 August 2020: Clinical Research
Locking Plates versus Locking Intramedullary Nails Fixation of Proximal Humeral Fractures Involving the Humeral Shaft: A Retrospective Cohort Study
Hui Song1BCDEF, Tao He1BCDEFG, Hui-Min Y. Guo1BCD, Zhan-Yu Li1ACD, Min Wei1ACD, Chao Zhang1ACD, Yu-Qi Dong1ACDEF*DOI: 10.12659/MSM.922598
Med Sci Monit 2020; 26:e922598
Abstract
BACKGROUND: For proximal humeral fractures (PHFs), locking intramedullary nails and locking plates have been widely used. However, few reports have been published on the therapy of complex PHFs accompanying humeral shaft fractures. Therefore, we performed this research to analyze the effectiveness of locking intramedullary nails and locking plates in the management of proximal humeral fractures involving the humeral shaft.
MATERIAL AND METHODS: We retrospectively reviewed 40 cases diagnosed with proximal humeral fractures involving the humeral shaft fixed with either locking intramedullary nails or locking plates with at least of 2 years’ follow-up. Clinical data were obtained from the medical records. Follow-up data included the Constant-Murley score, American Shoulder and Elbow Surgeons score (ASES), visual analog scale score (VAS), and the relative strength of the supraspinatus and deltoid muscles.
RESULTS: In total, 19 locking plate patients and 21 locking intramedullary nail patients were analyzed. The average follow-up period was 35 months in the locking plate group and 34 months in the locking intramedullary nail group. There were obvious differences in the intraoperative blood loss, time of operation, and the length of operative incision between the 2 groups (p<0.05). There were no significant differences between the groups in Constant-Murley score, ASES, VAS, or the relative strength of supraspinatus and deltoid muscles.
CONCLUSIONS: For PHFs involving the humeral shaft, both locking plates and locking intramedullary nails can achieve satisfactory functional results in the long-term follow-up assessment. The locking intramedullary nail group was superior with regards to intraoperative blood loss, time of operation, and length of incision.
Keywords: humeral fractures, Osteoporosis, Shoulder Fractures, Bone Nails, Fracture Fixation, Intramedullary, Postoperative Complications
Background
Proximal humeral fracture is one of the most frequent osteoporotic fractures that occur in the aged population, causing significant economic burden worldwide [1]. It has become more prevalent in the elderly population, with the incidence of displaced proximal humeral fractures (PHFs) requiring surgery also increased [2]. In 1970, 85% of PHF were either non-displaced or mildly displaced. However, owing to aging, this proportion had decreased to 42% by 2012 [3]. While the treatment of displaced PHFs has been well studied in the past decades [4–7], the optimal treatment of PHFs involving the humeral shaft was poorly discussed. The commonly used classification for PHFs in current clinical practice is the Neer or AO/OTA classifications [8,9]. However, they mainly focus on the fracture pattern proximal to the surgical neck of humerus, showing considerable limits in properly describing fracture patterns of PHFs involving the humeral shaft and are therefore insufficient for guiding the surgery plans in such cases [10]. Instead, the classification proposed by H.W. Stedtfeld in 2014 [11] addressed this issue and recommended dividing the humerus into 5 zones according to the anatomy structure, which takes into consideration the attachments of related muscles and the common fracture extensions. As such, this classification reveals superiority in guiding the application of suitable internal fixations in PHFs involving the humeral shaft.
PHFs involving the humeral shaft could be treated either intra-medullarily or extra-medullarily [5], including locking plates, locking intramedullary nails, hemiarthroplasty, and reverse shoulder arthroplasty [12–16]. However, debates persist in the selection of internal fixation methods. In clinical practice and the literature, the locking plates and the locking intramedullary nails have been more widely used. However, there were also some unsolved implant-related problems. For example, iatrogenic rotator cuff lesions may occur when the intramedullary locking nail is used, and whether the symptom would recover in the long-term follow-up remained unclear for the PHFs involving the humeral shaft patients. In addition, the locking plate required more surgical time and involved greater intraoperative blood loss, which can increase the perioperative complications. Locking plates and locking intramedullary nails have both been modified to overcome the problem of fixation failure concerning PHFs [17,18]. A recent prospective RCT study showed that in elderly patients, intramedullary nails had the same clinical effect and complication rates as locking plates [19]. Similarly, a meta-analysis revealed that both intramedullary nails and locking plates assured comparable effective results [20]. However, for more complex scenarios, such as those involving humeral shaft fractures, it remains unclear whether locking plates or locking intramedullary nails can be used to achieve a satisfactory prognosis and which method is better.
In this study, we aimed to investigate both the intraoperative parameters and the long-term functional outcomes of 40 patients with PHFs involving the humeral shaft, who had been treated with either locking plates or locking intramedullary nails.
Material and Methods
STUDY SUBJECTS:
We retrospectively analyzed all the patients diagnosed with PHFs involving the humeral shaft between January 2010 and December 2017 in Shanghai Renji Hospital. Inclusion criteria were as follows: (1) proximal humeral fractures involving the humeral shaft; (2) fresh fracture; and (3) no previous ipsilateral proximal humeral fracture. Exclusion criteria were as follows: (1) pathologic fractures; (2) accompanied with neurovascular damage; and (3) open fractures. In total, 43 cases were primarily included, 3 were eliminated in the final analysis, 2 were lost to follow-up (one in the long plate group and another in the long nail group), and 1 died due to unrelated medical reasons (in the plate group). X-ray and computed tomography were completed for all the objects and were classified by 2 orthopedic surgeons on the basis of the classification proposed by H.W. Stedtfeld [11].
SURGICAL PROCEDURES:
The operations were conducted by 3 surgeons with similar experience in the same trauma orthopedics department (Yu-Qi Dong, MD; Zhan-Yu Li, MD; Min Wei, MD). After induction of general anesthesia, patients were positioned in the beach chair position.
For the locking plate cases, the traditional deltopectoral approach was used. Correct restoration of the fracture parts was performed under C-arm fluoroscopy. Fracture fragments were stabilized by temporary Kirchner wires and reduction forceps. Then, a long proximal humeral locking plate (Smith & Nephew, Memphis, USA) was placed 8 mm under the peak of the greater tuberosity. The long locking plate was placed at the pronation direction according to the shape of the plate, and 1 special calcar screw was used to avoid varus collapse (Figure 1). The correct position of the plate and screws were confirmed by fluoroscopy in both the anteroposterior and axillary directions. The incision was sutured without vacuum drainage. The nerves, especially the radial nerve, were carefully protected during the operation [21].
For the locking intramedullary nail cases, we chose the anterolateral approach. The insert point was located at the tip of the humeral head, medial to the greater tuberosity, and lateral to the intertubercular sulcus. The insertion direction, which was along the axis of the humeral shaft, was confirmed by C-arm fluoroscopy. The nail (Smith & Nephew, Memphis, USA) was inserted nearly 5 mm under the cartilage surface of the humeral head (Figure 2). The distal and proximal screws were placed with the help of an ancillary system. The rotator cuff was then repaired, and the incision was sutured without vacuum drainage.
Allograft bone was used to address any significant bone defect. Five patients received bone allograft, 2 in the locking plate team and 3 in the locking intramedullary nail team. The intraoperative blood loss was recorded at the end of surgery.
POSTOPERATIVE MANAGEMENT AND REHABILITATION PROTOCOL:
For all the patients enrolled, the shoulder was fixed postoperatively using a sling. Early passive ROM exercises were started on postoperative day 1 with slight Codman rotation exercises. Three weeks postoperatively, rehabilitation exercises were initiated. At the beginning, passive exercises of the shoulder were initiated without causing any discomfort or pain. After 6 weeks, when the healing of the fracture was confirmed by X-ray, active exercises were applied to the shoulder. The training intensity was adjusted stepwise and the normal motion of the shoulder were pursued by 6 months after surgery.
POSTOPERATIVE EVALUATION:
Clinical follow-up was performed by 2 independent certified orthopedic trauma surgeons (Hui Song, MD; Tao He, MD) at 3, 6, 12, 24, and 36 months postoperatively. Plain radiographs were obtained postoperatively and at each follow-up time-point.
FUNCTIONAL EVALUATION OF SHOULDER:
Constant-Murley scores of the affected side were recorded as the primary outcome to evaluate shoulder function. Secondary outcomes included American Shoulder and Elbow Surgeons (ASES), visual analog scale (VAS), the relative strength of the supraspinatus and deltoid muscles, and active shoulder flexion and abduction range of motion (ROM).
RADIOGRAPHIC EVALUATION:
Plain radiographs of the anteroposterior and lateral direction of the shoulder were obtained and assessed for fragment reduction, postoperative implant position, tuberosity resorption, secondary migration of the humeral head, and failure of fixation. All radiographs were assessed by the same independent observers conducting follow-up.
STATISTICAL ANALYSIS:
All data were analyzed using SPSS software, version 19.0 (SPSS, Inc., Chicago, IL, USA). The t test was used for continuous data. When continuous data were non-normally distributed, the Mann-Whitney U test was used and results are represented by medians. The χ2 test or Fisher’s exact test was used to analyze the categorical variables. A p-value less than 0.05 was considered statistically significant.
Results
Demographic data were obtained from the medical records (Table 1). There were no differences in baseline parameters, and they were comparable between the 2 groups. According to the Neer classification for PHFs, there were 15 cases of 2-part fractures (7 cases in the locking plate group and 8 cases in the intramedullary nail group), 12 cases of 3-part fractures (5 cases in the locking plate group and 7 cases in the intramedullary nail group), and 13 cases of 4-part fractures (7 cases in the locking plate group and 6 cases in the intramedullary nail group). Stedtfeld classification is shown in Table 2. Of the 40 patients reviewed, 19 were fixed with locking plates and 21 were treated with locking intramedullary nails. The mechanism of injury was falling from height (n=32) or motor vehicle collisions (n=8). Fracture union was achieved for all the cases by 14 weeks postoperatively. At the last follow-up visit, there were no obvious differences in the Constant-Murley score or ASES score between the 2 groups. There was no significant difference in the relative strength of the supraspinatus or deltoid muscles between the groups (Table 3).
There was no wound infection, nerve damage, humeral head osteonecrosis, or humeral head varus collapse in this patient cohort. At the final follow-up visit, 4 patients (2 in the plate team and 2 in the nail team) complained of mild, occasional shoulder pain, but this improved with physical therapy.
Discussion
For PHFs involving the humeral shaft, the fracture lines are longer and more complex than in simple PHFs. The internal fixation devices frequently used for PHFs are normally too short and result in unstable fixation due to the fracture lines extending into the humeral shaft [17]. The devices, therefore, cannot sufficiently span the entire fracture area and maintain the stability during the period of bone union. Therefore, long locking plates and long locking intramedullary nails are the more appropriate choices. In our study, based on Stedtfeld’s categorization, the most common fracture type is Group B, consistent with reports by other groups. However, Stedtfeld et al. only reported the use of long intramedullary nails, without the application of long locking plates, and the long-term outcomes of either long locking intramedullary nails or plates were poorly investigated [11].
From our follow-up analysis, although good shoulder function was obtained with either long locking plates or long intramedullary nails, they have their own pearls and pitfalls. Locking plates are routine treatments for both PHFs and humeral shaft fractures. However, limitations are present owing to the longer incision compared with intramedullary nails and more interference with the regionally important structures [22]. To obtain correct restoration of the fracture parts under direct visualization, a longer skin incision was necessary, and a more comprehensive separation of the muscle was inevitable, subsequently causing more intraoperative blood loss [23,24]. Kozanek et al. reported that decreasing the operation time and the amount of blood loss reduced the need for transfusion, which related to inpatient adverse events such as surgical site infection and pulmonary embolism [25]. Thus, for elderly patients and those with chronic comorbidities, the long locking plates are less preferable than intramedullary nails owing to the greater intraoperative blood loss and the subsequent transfusion-associated complications. In some challenging cases, to obtain the ideal placement of the long locking plate in this kind of fracture, part of the deltoid muscle has to be cut, which interferes with the deltoid attachment on the humeral shaft, subsequently influencing shoulder abduction [26,27]. In the present study, all patients in the locking plates group received long locking plates, with the plates placed at the pronation direction of the humeral shaft to minimize the irritation and stripping of the deltoid muscle. From our 2-year analysis, the relative strength of the shoulder abduction showed no significant differences between the plates group and the nails group. In our opinion, pronation direction placement of the plate minimizes the plates-related influence on the biceps brachii and the deltoid muscles. Additionally, deltoid strength can be compensated for with proper rehabilitation postoperatively, even though a bundle of the deltoid muscle was cut.
In terms of the treatment with locking intramedullary nails, although various methods were used to protect the supraspinatus upon insertion, entry point-associated complications are still a primary concern when a proximal humeral antegrade nail is used [28,29]. It is noteworthy that the supraspinatus is more susceptible, which will affect shoulder abduction and the rotator cuff. A prospective randomized trial by Zhu et al. [30] showed that at 1 year, the locking nail group showed significantly reduced supraspinatus muscle strength (p=0.032) in the injured shoulder compared with the locking plate group. Nevertheless, there was no significant difference (p=0.106) between the groups at 3 years. The long-term effect on deltoid strength was not analyzed. In the present study, the long locking intramedullary nails were used to cover the span of the fracture lines and fracture fragments. Nevertheless, we found no statistically significant differences in shoulder strength and rotator cuff-related complications between the groups at 2-year follow-up.
In this study, no wound infections, neurologic damage, or humeral head osteonecrosis or varus collapse were noted. This should be attributed to our rigorous sterile operation and postoperative care, as well as careful exposure and protection of the nerves intraoperatively [31]. Furthermore, the soft tissues around the humeral head were cautiously protected, with minimal interference with arterial supply to the humeral head and the fracture ends [32], subsequently decreasing the risk of humeral head avascular necrosis. The exact placement of the calcar screw is also crucial to provide sufficient inferior stability of the humeral neck, reducing the incidence of humeral head varus. At the final follow-up visit, there were 4 patients who complained of rotator cuff problems. These patients were older than 65 years at the final follow-up visit and may have had imperfect rotator cuff repair or age-related degeneration.
There are several limitations in our study. While all follow-up examination data were collected by 2 independent observers, they were aware of the fixation method used, which may have caused information bias. Also, this study was retrospective in nature. Additionally, surgical skills may differ between surgeons. However, to minimize this bias, all surgeons engaged in this study were required to rigorously follow the standardized and structural surgical procedures for either intramedullary nail or plate fixation of PHFs involving the humeral shaft made by our department. Last but not least, the choice of fixation method made by surgeons could have caused selection bias.
Conclusions
Patients with PHF involving the humeral shaft can regain good shoulder function regardless of using either long locking plates or intramedullary nails. Similar recovery of the average strength of the supraspinatus and deltoid muscle were achieved by both modalities in the long-term follow-up. Elderly patients with chronic systemic disease or weakness may benefit from the use of locking intramedullary nails owing to shorter operation time, shorter incision, and less intraoperative blood.
Figures
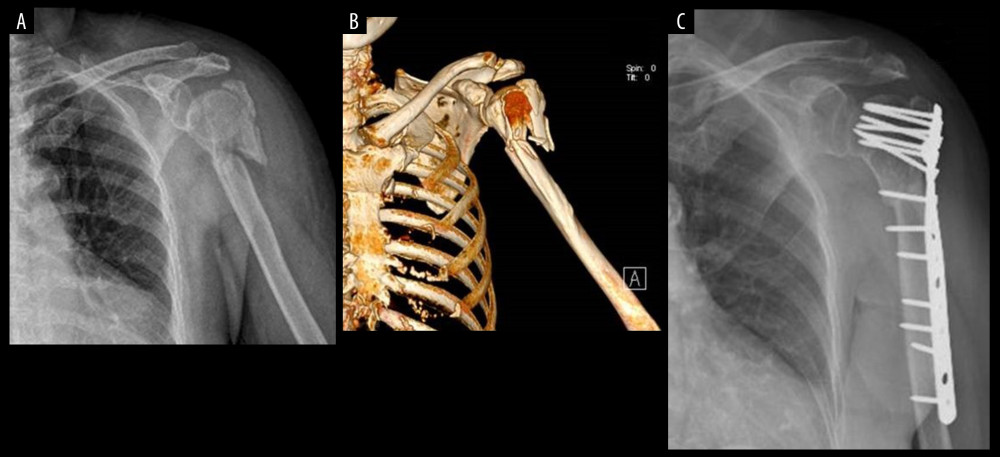 Figure 1. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking plate.
Figure 1. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking plate. 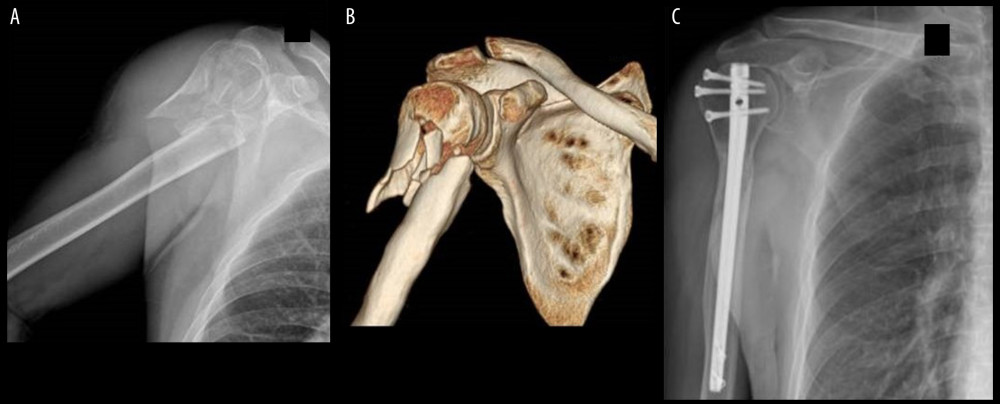 Figure 2. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking intramedullary nail.
Figure 2. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking intramedullary nail. Tables
Table 1. Demographics and clinical data of the patients.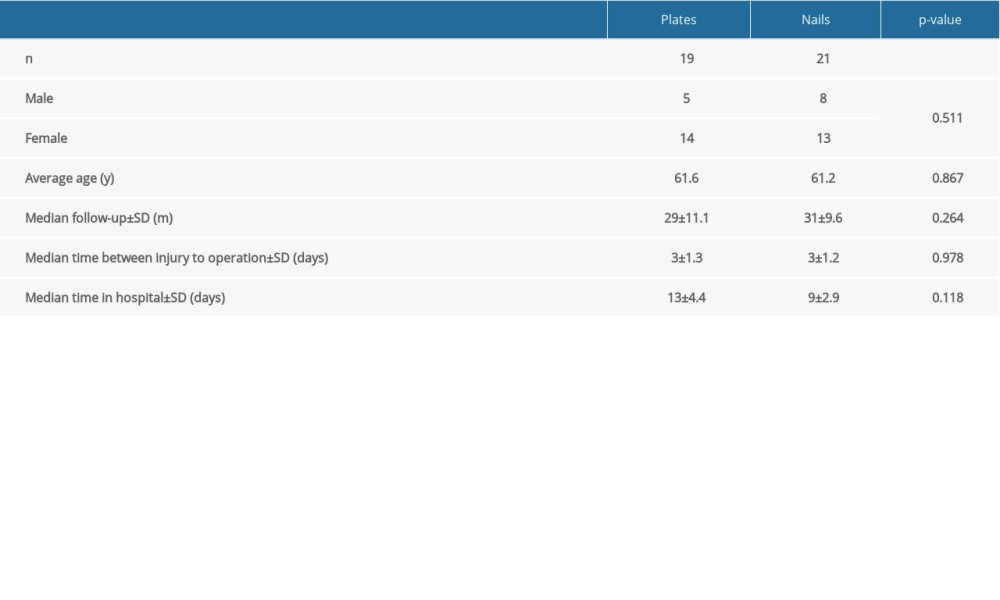 Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification.
Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification.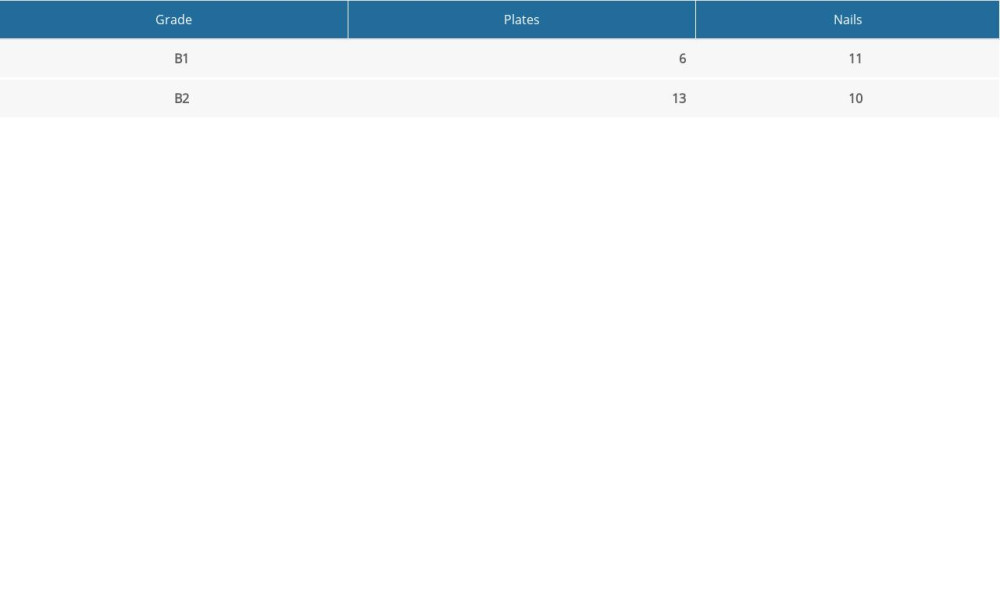 Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles.
Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles.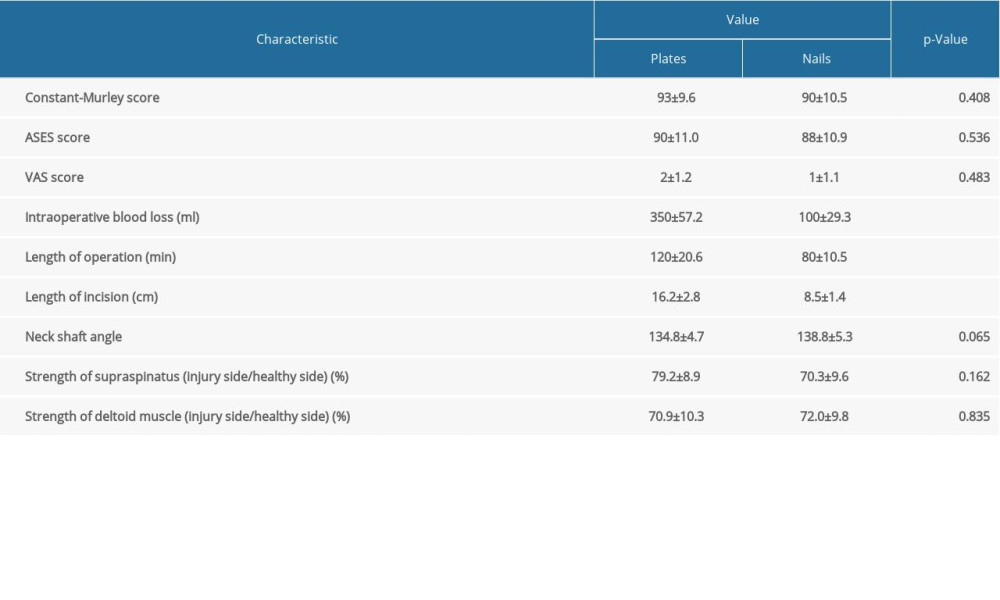
References
1. Namdari S, Voleti PB, Mehta S, Evaluation of the osteoporotic proximal humeral fracture and strategies for structural augmentation during surgical treatment: J Shoulder Elbow Surg, 2012; 21(12); 1787-95
2. Launonen AP, Lepola V, Saranko A, Epidemiology of proximal humerus fractures: Arch Osteoporos, 2115; 10; 209
3. Roux A, Decroocq L, El Batti S, Epidemiology of proximal humerus fractures managed in a trauma center: Orthop Traumatol Surg Res, 2012; 98(6); 715-19
4. Roberson TA, Granade CM, Hunt Q, Nonoperative management versus reverse shoulder arthroplasty for treatment of 3- and 4-part proximal humeral fractures in older adults: J Shoulder Elbow Surg, 2017; 26(6); 1017-22
5. Boudard G, Pomares G, Milin L, Locking plate fixation versus antegrade nailing of 3- and 4-part proximal humerus fractures in patients without osteoporosis. Comparative retrospective study of 63 cases: Orthop Traumatol Surg Res, 2014; 100(8); 917-24
6. Urda A, Gonzalez A, Colino A, Management of displaced surgical neck fractures of the humerus: Health related quality of life, functional and radiographic results: Injury, 2012; 43(Suppl 2); S12-19
7. Maier D, Jaeger M, Izadpanah K, Proximal humeral fracture treatment in adults: J Bone Joint Surg Am, 2014; 96(3); 251-61
8. Neer CS, Displaced proximal humeral fractures. Part I. Classification and evaluation: Clin Orthop Relat Res, 1987, 1970(223); 3-10
9. Brorson S, Eckardt H, Audige L, Translation between the Neer- and the AO/OTA-classification for proximal humeral fractures: Do we need to be bilingual to interpret the scientific literature?: BMC Res Notes, 2013; 6; 69
10. Wang Q, Hu J, Guan J, Proximal third humeral shaft fractures fixed with long helical PHILOS plates in elderly patients: Benefit of pre-contouring plates on a 3D-printed model-a retrospective study: J Orthop Surg Res, 2018; 13(1); 203
11. Stedtfeld HW, Biber R, Proximal third humeral shaft fractures – a fracture entity not fully characterized by conventional AO classification: Injury, 2014; 45(Suppl 1); S54-59
12. Wang G, Mao Z, Zhang L, Meta-analysis of locking plate versus intramedullary nail for treatment of proximal humeral fractures: J Orthop Surg Res, 2015; 10; 122
13. Konrad G, Audige L, Lambert S, Similar outcomes for nail versus plate fixation of three-part proximal humeral fractures: Clin Orthop Relat Res, 2012; 470(2); 602-9
14. Sebastia-Forcada E, Cebrian-Gomez R, Lizaur-Utrilla A, Gil-Guillen V, Reverse shoulder arthroplasty versus hemiarthroplasty for acute proximal humeral fractures. A blinded, randomized, controlled, prospective study: J Shoulder Elbow Surg, 2014; 23(10); 1419-26
15. Boyle MJ, Youn SM, Frampton CM, Ball CM, Functional outcomes of reverse shoulder arthroplasty compared with hemiarthroplasty for acute proximal humeral fractures: J Shoulder Elbow Surg, 2013; 22(1); 32-37
16. van der Merwe M, Boyle MJ, Frampton CMA, Ball CM, Reverse shoulder arthroplasty compared with hemiarthroplasty in the treatment of acute proximal humeral fractures: J Shoulder Elbow Surg, 2017; 26(9); 1539-45
17. Hymes RA, Levine MJ, Schulman JE, Mechanisms of failure of locked-plate fixation of the proximal humerus: Acoustic emissions as a novel assessment modality: J Orthop Trauma, 2013; 27(7); 392-98
18. Hessmann MH, Hansen WS, Krummenauer F, Locked plate fixation and intramedullary nailing for proximal humerus fractures: A biomechanical evaluation: J Trauma, 2005; 58(6); 1194-201
19. Plath JE, Kerschbaum C, Seebauer T, Locking nail versus locking plate for proximal humeral fracture fixation in an elderly population: A prospective randomised controlled trial: BMC Musculoskelet Disord, 2019; 20(1); 20
20. Sun Q, Ge W, Li G, Locking plates versus intramedullary nails in the management of displaced proximal humeral fractures: A systematic review and meta-analysis: Int Orthop, 2018; 42(3); 641-50
21. Stecco C, Gagliano G, Lancerotto L, Surgical anatomy of the axillary nerve and its implication in the transdeltoid approaches to the shoulder: J Shoulder Elbow Surg, 2010; 19(8); 1166-74
22. Clavert P, Adam P, Bevort A, Pitfalls and complications with locking plate for proximal humerus fracture: J Shoulder Elbow Surg, 2010; 19(4); 489-94
23. Vijayvargiya M, Pathak A, Gaur S, Outcome analysis of locking plate fixation in proximal humerus fracture: J Clin Diagn Res, 2016; 10(8); RC01-5
24. Malcherczyk D, Klasan A, Ebbinghaus A, Factors affecting blood loss and blood transfusion in patients with proximal humeral fractures: J Shoulder Elbow Surg, 2019; 28(6); e165-74
25. Kozanek M, Menendez ME, Ring D, Association of perioperative blood transfusion and adverse events after operative treatment of proximal humerus fractures: Injury, 2015; 46(2); 270-74
26. Robinson CM, Murray IR, The extended deltoid-splitting approach to the proximal humerus: Variations and extensions: J Bone Joint Surg Br, 2011; 93(3); 387-92
27. Rispoli DM, Athwal GS, Sperling JW, Cofield RH, The anatomy of the deltoid insertion: J Shoulder Elbow Surg, 2009; 18(3); 386-90
28. Gracitelli ME, Malavolta EA, Assuncao JH, Locking intramedullary nails compared with locking plates for two- and three-part proximal humeral surgical neck fractures: A randomized controlled trial: J Shoulder Elbow Surg, 2016; 25(5); 695-703
29. Dilisio MF, Nowinski RJ, Hatzidakis AM, Fehringer EV, Intramedullary nailing of the proximal humerus: Evolution, technique, and results: J Shoulder Elbow Surg, 2016; 25(5); e130-38
30. Zhu Y, Lu Y, Shen J, Locking intramedullary nails and locking plates in the treatment of two-part proximal humeral surgical neck fractures: A prospective randomized trial with a minimum of three years of follow-up: J Bone Joint Surg Am, 2011; 93(2); 159-68
31. Kennon JC, Smith JP, Crosby LA, Core decompression and arthroplasty outcomes for atraumatic osteonecrosis of the humeral head: J Shoulder Elbow Surg, 2016; 25(9); 1442-48
32. Patel S, Colaco HB, Elvey ME, Lee MH, Post-traumatic osteonecrosis of the proximal humerus: Injury, 2015; 46(10); 1878-84
Figures
 Figure 1. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking plate.
Figure 1. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking plate. Figure 2. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking intramedullary nail.
Figure 2. (A) Representative anteroposterior plain radiograph showing proximal humeral fractures involving the humeral shaft. (B) 3D CT showing proximal humeral fractures involving the humeral shaft. (C) Postoperative anteroposterior plain radiograph showing fracture fixation with a long locking intramedullary nail. Tables
 Table 1. Demographics and clinical data of the patients.
Table 1. Demographics and clinical data of the patients. Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification.
Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification. Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles.
Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles. Table 1. Demographics and clinical data of the patients.
Table 1. Demographics and clinical data of the patients. Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification.
Table 2. Classification of PHFs involving the humeral shaft according to the Stedtfeld classification. Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles.
Table 3. Follow-up data (nedian±SD) of the shoulder function, surgery associated data, and relative strength of the shoulder muscles. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








