21 June 2020: Clinical Research
Treatment of Temporomandibular Joint Disorders by Ultrashort Wave and Extracorporeal Shock Wave: A Comparative Study
Wenyan Li1ABCDEF, Junying Wu1ABCDEF*DOI: 10.12659/MSM.923461
Med Sci Monit 2020; 26:e923461
Abstract
BACKGROUND: This study was carried out to compare the therapeutic efficacy of extracorporeal shock wave (ESW) and ultrashort wave (UW) for temporomandibular joint disorder (TMD).
MATERIAL AND METHODS: A total of 80 patients with myofascial pain and TMD were enrolled in this study. The subjects were randomized to receive ESW or UW treatments. Patients in the ESW group received 1 ESW treatment for 4 weeks and patients in the US group were given US treatment once a day for 5 days per week for 4 weeks. The pain was measured using visual analog scale (VAS) and mouth opening was determined as pain-free maximum mouth opening (MMO) before and 4 weeks after the treatments. Other parameters assessed included functional indexes of temporomandibular joint such as mandibular movement (MM), joint noise (JN), joint press (JP), and disability index (DI).
RESULTS: After therapy, VAS, MMO, MM, JN, JP, and DI in ESW group, and VAS in UW group were significantly improved (P<0.05) as compared to before therapy. VAS, MMO, and the functional indexes of temporomandibular joint in the ESW group were significantly better than those in the UW group (1.79 vs. 2.00, 3.23 vs. 2.03, 1.79 vs. 2.41, 1.45 vs. 2.27, 1.55 vs. 2.59, and 3.30 vs. 4.79, respectively. P<0.05).
CONCLUSIONS: ESW significantly reduces pain and improves the functional indexes of temporomandibular joint and mouth opening limit for TMD patients as compared with UW therapy.
Keywords: High-Energy Shock Waves, pain management, Temporomandibular Joint, Electric Stimulation Therapy, Extracorporeal Shockwave Therapy, Pain Measurement, Range of Motion, Articular, Temporomandibular Joint Disorders, young adult
Background
Temporomandibular disorders (TMDs) are clinical conditions that affect the masticatory musculature, temporomandibular joint (TMJ), and associated structures [1]. The common symptoms of TMD include clicking of the joint, limited mouth opening, and muscle with joint pain, which is the most significant clinical symptom. The pain can be myogenic, arthrogenic, or mixed types [2]. A number of studies have examined the efficacy of physical therapies for the dysfunction of TMJ and pain, such as electrotherapy, massage, and physical and exercise therapy [3,4]. Among them, UW therapy is demonstrated to be able to reduce pain and inflammation, and improve the functions of the mouth [4,5]. However, this treatment is relatively slow in relieving pain [6].
Extracorporeal shock wave (ESW) has been widely recognized as a biological modulator that results in differentiation of mesenchymal stem cells, neovascularization, and release of angiogenetic factors [7,8]. Previous studies have shown that ESW is beneficial for musculoskeletal disorders, with a success rate between 65% and 91%, with few and negligible complications [9]. Some preliminary studies showed that ESW is effective in treating TMJ disorders [10]. However, a better understanding of the therapeutic effects of the physical therapy interventions is still required for rational use of this therapy for TMD treatment. In this study, we investigated the therapeutic effects of UW and ESW on reliving pain and increasing pain-free maximum mouth opening (MMO) in patients with myogenic or mixed TMD. Our results may help improve therapeutic management of the disease.
Material and Methods
SUBJECTS:
A total of 80 TMD patients treated at our hospital between July 2013 and September 2018 were included. Participants were included if they were older than 18 years and had diagnosed myofascial pain with or without mouth opening limitation based on the Research Diagnostic Criteria for TMD (RDC/TMD) [11]. They were also included if they had unilateral or bilateral joint impairment or disc displacement associated with myofascial pain. Those criteria are shown to have excellent intraclass correlation coefficient with TMD, especially for myofascial pain diagnosis [12]. Subjects were excluded if they had polyarthritis, acute trauma, joint infection, surgical treatment (physiotherapy, splint therapy, and acupuncture) within the 3 months prior to the study, depression, and other mental problems. Patients were asked not to take pain-relief medication or muscle relaxants at least 24 hours prior to the evaluations or during the treatment period. This study was approved by the Research Ethics Committee of Shanxi Medical University. Written informed consent was obtained from every patient before treatment.
PATIENT DATA AND INTERVENTIONS:
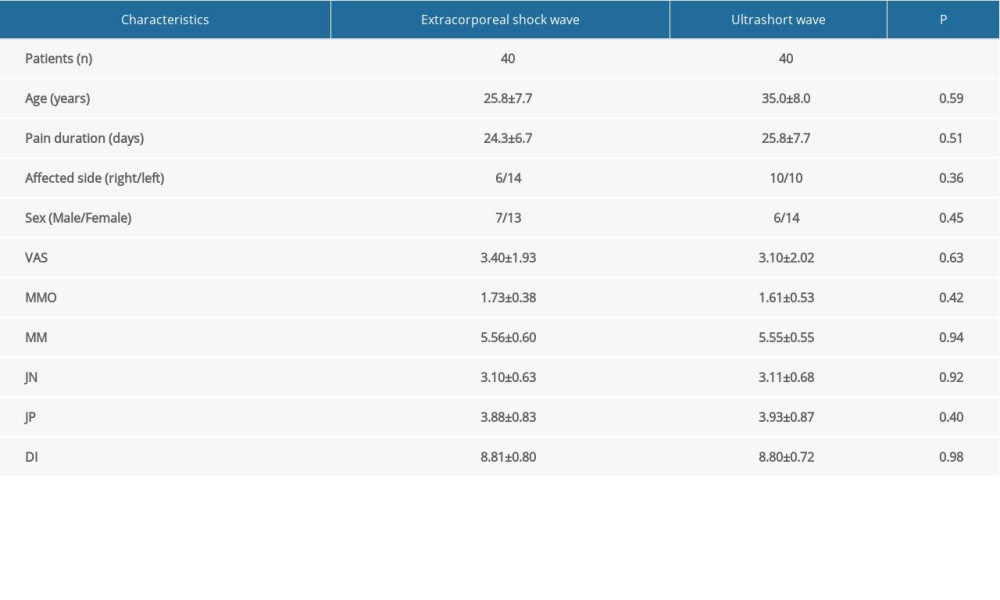
After detailed physical examinations, a specially-designed evaluation form was filled out for each patient. Demographic data such as age, sex, duration of pain, and other clinical data were collected (Table 1).
To compare the effectiveness of UW and ESW, patients were randomly assigned (using a simple randomization table) into 2 groups. Patients in the UW group received UW at an intensity of 45 W and wavelength of 6 meters using an ultra-short-wave emitter (Hannover, Germany). UW was applied by placing the electrodes 2 to 3 cm to the mandibular joint, and each treatment lasted 15 min once a day for 5 in a week for 4 weeks. Patients in the ESW group were given 1000 to 1500 shocks at 8 Hz frequency using a radial extracorporeal shock wave device (EMS, Swiss). The device was connected to a 15-mm diameter applicator according to the producer’s recommendations, and patients were treated once a week for 4 weeks.
OUTCOME ASSESSMENT:
Before and 4 weeks after the therapies, patients were assessed for pain using the visual analog scale (VAS), which uses a 10-cm ruler with left and right sides corresponding to no pain (0) and unbearable pain [13], respectively. The assessing physicians were blinded to the patients. The participants were asked to move the marker to indicate their pain level. Pain-free MMO was measured using an analog vernier caliper with a 0.05 mm precision, as previously described [14]. Participants were seated and asked to open their mouths as far as possible without pain. At the limit of mouth opening that was pain-free, the distance between the upper and lower central incisors (not considering the overbite) was determined. The temporomandibular index were assessed as described elsewhere [15,16], including mandibular movement (MM), joint noise (JN), joint press (JP), and disability index (DI).
STATISTICAL ANALYSIS:
Data are expressed as mean±standard derivation and analyzed using the Statistical Package for the Social Sciences (SPSS Inc., Chicago, IL, USA). The Wilcoxon rank test was used to compare intra-group differences for pain between before and 4 weeks after treatment, and the Mann-Whitney rank test was conducted for comparing the intergroup difference. Within-group comparisons for pain-free MMO were performed using the paired-sample
Results
BASELINE DATA:
Initially, 86 consecutive patients visiting the Physical and Rehabilitation Outpatient Clinic were selected for this study. Six patients refused to participate and the remaining 80 patients were randomized to receive UW or ESW treatments. No participants dropped out during the study. Basic characteristics of the patients are summarized in Table 1, and there was no difference in those characteristics between the 2 groups, including sex, age, duration of disease, VAS, MMO, MM, JN, JP, and DI.
VAS AND MMO:
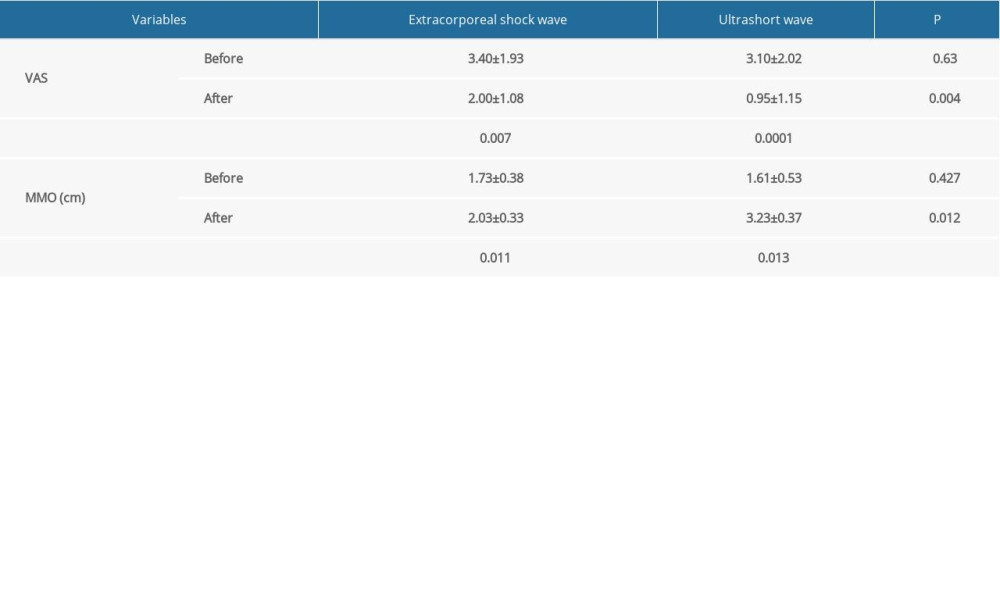
Before the therapies, there was no difference in VAS and MMO between the 2 groups (p>0.05). Four weeks after the therapies, VAS and MMO were better than before the therapies (p=0.004 and 0.012, respectively, Table 2). In addition, the improvements were greater in the ESW group than in the UW group (p=0.014 and 0.013, respectively, Table 2) after the treatments.
FRICTON INDEX:
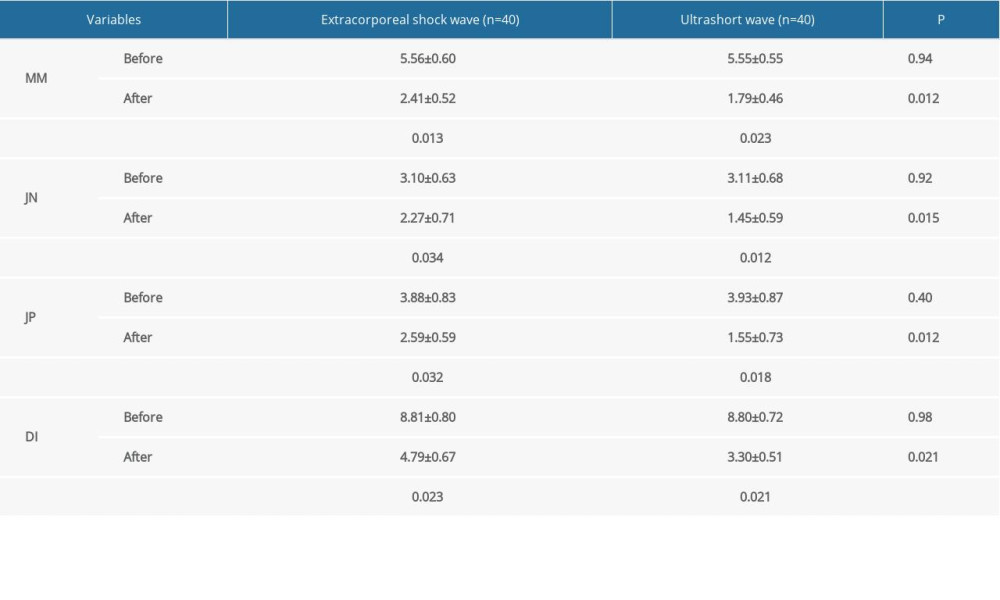
Before the therapies, the Fricton indexes measured as MM, JN, JP, and DI were similar between the 2 groups (p=0.012, 0.015, 0.012, and 0.021, respectively, Table 3). After the treatments, these parameters were better than before the treatments (p<0.05, Table 3). Furthermore, these indexes were better in the ESW than in the UW group (Table 3) after the treatments.
Discussion
TMD is a collective term for clinical disorders in the masticatory musculature, TMJs, and associated structures [17]. This dysfunction leads to impairments in chewing, swallowing, and speaking. The main signs include pain, joint noises, reduced range of motion, and mandibular deviation. Therefore, TMD patients should be treated from multiple perspectives, including pharmacological and physical treatment [18,19]. Although a number of methods are available [20], proper selection of treatment method is very important for better treatment of the disease [6,19]. The patients in our study had relatively long TMD duration, and were slow in response to UW therapy, which requires longer treatment time and often results in poor patient compliance.
Recently, ESW has become increasingly popular as a physical treatment for a number of disorders. Our comparison showed that ESW is more effective than UW in treating TMD, leading to better VAS, MMO, and Fricton indexes after treatment. ESW is a mechanical (acoustic) wave with a low-frequency pressure that propagates rapidly in space [21,22]. It is non-invasive and results in rapid patient response. Earlier studies showed that during the occurrence and development of TMD, cytokines such as IL-1, IL-6, and TNF-α are involved in inflammation of the synovium, leading to destruction of articular cartilage and excessive apoptosis of chondrocytes in the soft tissue of bone and joints as a result of increased NO content and the imbalance of local metabolism in the joint [23–25]. ESW can reduce NO content in the articular fluid, reduce the apoptosis of chondrocytes, promote the proliferation of articular cartilage and the repair of cartilage defects, and inhibit the secretion of inflammatory cytokines [26,27].
We found that the VAS scores of both groups declined after therapy, and the extent of decrease was greater in the ESW group than in the UW group. Furthermore, the pain-free MMO in both groups was improved after therapy, and the improvement was larger in the ESW group than in the UW group, demonstrating that ESW is better than UW for TMD treatment. The beneficial effect of shock waves is associated with micro-destruction [28,29], which is likely to result in micro-tears of non-vascularized or scantily vascularized tissues, and thus stimulate the revascularization by the local release of growth factors and mobilization of stem cells, leading to increased blood supply to the tissue [28,30]. Previous studies have suggested that these mechanisms also play a role in reducing the muscle tone for spasticity [31]. In addition, ESW may generate an analgesic effect during the treatment that blocks the activation and transmission of pain signals by non-invasive stimulation of cell membranes and nerve endings [32–34], which may be related to reduced pain and increased MMO.
UW therapy also is effective in treating TMD, although not as effective as ESW in our study. It induces changeable intracellular pressure, which acts as an „internal tissue massage”, leading to changes in the nervous conductivity, raising the threshold of pain, and improving muscle relaxation. Biochemical studies showed that UW increased the enzymatic activity that accelerates metabolism and regenerative processes [35,36].
Although our study provides valuable information regarding ESW in treating TMD, there are limitations. It was a single-center study with a limited number of participants. Patients were not stratified for treatments and the follow-up time was relatively short. Further studies are needed to validate our results with more patients and stratification is needed to optimize the patient conditions for better treatment outcomes.
Conclusions
The results showed that the efficacy of both treatments is comparable and substantially decreased pain and increased MMO. ESW is more effective, with fewer treatment sessions and requiring less time and cost for patients.
References
1. De Leeuw R, Klasser GD: Orofacial pain: Quidelines for assessment, diagnosis, and management, 2008, Chicago, Quintessence
2. Kothari SF, Baad-Hansen L, Oono Y, Somatosensory assessment and conditioned pain modulation in temporomandibular disorders pain patients: Pain, 2015; 156; 2545-55
3. Bae Y, Park Y, The effect of relaxation exercises for the masticator muscles on temporomandibular joint dysfunction (TMD): J Phys Ther Sci, 2013; 25; 583-86
4. Rashid A, Matthews NS, Cowgill H, Physiotherapy in the management of disorders of the temporomandibular joint – perceived effectiveness and access to services: A national United Kingdom survey: Br J Oral Maxillofac Surg, 2013; 51; 52-57
5. Sturdivant J, Fricton JR, Physical therapy for temporomandibular disorders and orofacial pain: Curr Opin Dent, 1991; 1; 485-96
6. Zhao YTreatment of temporomandibular joint disorders using acupuncture combined with Chinese and Western medicine: Journal of Traditional Chinese Medicine, 2011; 29; 1681-82 [in Chinese]
7. Notarnicola A, Moretti B, The biological effects of extracorporeal shock wave therapy (eswt) on tendon tissue: Muscles Ligaments Tendons J, 2012; 2; 33-37
8. Mattyasovszky SG, Langendorf EK, Ritz U: J Orthop Surg Res, 2018; 13; 75
9. Saggini R, Di Stefano A, Saggini A, Clinical application of shock wave therapy in musculoskeletal disorders: Part I: J Biol Regul Homeost Agents, 2015; 29; 533-45
10. Schenk I, Vesper M, Nam VCInitial results using extracorporeal low energy shockwave therapy ESWT in muscle reflex-induced lock jaw: Mund Kiefer Gesichtschir, 2002; 6; 351-55 [in German]
11. Dworkin SF, Research diagnostic criteria for temporomandibular disorders: Current status & future relevance: J Oral Rehabil, 2010; 37; 734-43
12. John MT, Dworkin SF, Mancl LA, Reliability of clinical temporomandibular disorder diagnoses: Pain, 2005; 118; 61-69
13. Heller GZ, Manuguerra M, Chow R, How to analyze the Visual Analogue Scale: Myths, truths and clinical relevance: Scand J Pain, 2016; 13; 67-75
14. Walker N, Bohannon RW, Cameron D, Discriminant validity of temporomandibular joint range of motion measurements obtained with a ruler: J Orthop Sports Phys Ther, 2000; 30; 484-92
15. Fricton JR, Schiffman EL, Reliability of a craniomandibular index: J Dent Res, 1986; 65; 1359-64
16. Fricton JR, Schiffman EL, The craniomandibular index: Validity: J Prosthet Dent, 1987; 58; 222-28
17. Calixtre LB, Grüninger BL, Haik MN, Effects of cervical mobilization and exercise on pain, movement and function in subjects with temporomandibular disorders: A single group pre-post test: J Appl Oral Sci, 2016; 24; 188-97
18. Liu F, Steinkeler A, Epidemiology, diagnosis, and treatment of temporomandibular disorders: Dent Clin North Am, 2013; 57; 465-79
19. Gauer RL, Semidey MJ, Diagnosis and treatment of temporomandibular disorders: Am Fam Physician, 2015; 91; 378-86
20. Mao Z, Zhang ZAdvance on treatment of termporomandibular disorders: Chin J Stomatol, 2012; 47; 2-5 [in Chinese]
21. Schmitz C, Császár NBM, Milz S, Efficacy and safety of extracorporeal shock wave therapy for orthopedic conditions: A systematic review on studies listed in the PEDro database: Br Med Bull, 2015; 116; 115-38
22. Sabeti-Aschraf M, Dorotka R, Goll A, Extracorporeal shock wave therapy in the treatment of calcific tendinitis of the rotator cuff: Am J Sports Med, 2005; 33; 1365-68
23. Cheng J, Wang Y, Wang Z, Differential regulation of proteoglycan-4 expression by IL-1alpha and TGF-beta1 in rat condylar chondrocytes: Tohoku J Exp Med, 2010; 222; 211-18
24. Kou XX, Wu YW, Ding Y, 17beta-estradiol aggravates temporomandibular joint inflammation through the NF-kappaB pathway in ovariectomized rats: Arthritis Rheum, 2011; 63; 1888-97
25. Jiao K, Niu LN, Wang MQ, Subchondral bone loss following orthodontically induced cartilage degradation in the mandibular condyles of rats: Bone, 2011; 48; 362-71
26. Kim YH, Bang JI, Son HJ: Osteoarthritis Cartilage, 2019; 27; 1692-701
27. Hazan-Molina H, Reznick AZ, Kaufman H, Assessment of IL-1beta and VEGF concentration in a rat model during orthodontic tooth movement and extracorporeal shock wave therapy: Arch Oral Biol, 2013; 58; 142-50
28. Contaldo C, Högger DC, Khorrami Borozadi M, Radial pressure waves mediate apoptosis and functional angiogenesis during wound repair in ApoE deficient mice: Microvasc Res, 2012; 84; 24-33
29. Wang C-J, Wang F-S, Yang KD, Shock wave therapy induces neovascularization at the tendon-bone junction. A study in rabbits: J Orthop Res, 2003; 21; 984-89
30. Mariotto S, Cavalieri E, Amelio E, Extracorporeal shock waves: From lithotripsy to anti-inflammatory action by NO production: Nitric Oxide, 2005; 12; 89-96
31. Park D-S, Kwon DR, Park G-Y, Therapeutic effect of extracorporeal shock wave therapy according to treatment session on gastrocnemius muscle spasticity in children with spastic cerebral palsy: A pilot study: Ann Rehabil Med, 2015; 39; 914-21
32. Visco V, Vulpiani MC, Torrisi MR, Experimental studies on the biological effects of extracorporeal shock wave therapy on tendon models. A review of the literature: Muscles Ligaments Tendons J, 2014; 4; 357-61
33. Hausdorf J, Lemmens MAM, Kaplan S, Extracorporeal shockwave application to the distal femur of rabbits diminishes the number of neurons immunoreactive for substance P in dorsal root ganglia L5: Brain Res, 2008; 1207; 96-101
34. Lin S-F, Chen Y-J, Tu H-P, The effects of extracorporeal shock wave therapy in patients with coccydynia: A randomized controlled trial: PLoS One, 2015; 10; e0142475
35. Kociuga N, Kociuga J, Woldańska-Okońska MPhysiotherapeutic proceeding in symptomatic calcaneal spur treatment: Wiad Lek, 2016; 69; 758-64 [in Polish]
36. Straburzyńska-Lupa A, Kornacka A, Ultrasound therapy in the treatment of calcar pedis – own experiences: Ortop Traumatol Rehabil, 2005; 7; 78-86
In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387