16 August 2020: Clinical Research
The Evaluation of Bone Mineral Density based on Age and Anthropometric Parameters in Southeast Chinese Adults: A Cross-Sectional Study
Rongrong Xuan1ABCE, Yang Song2BCEF, Julien S. Baker3BCEF, Yaodong Gu2ACFG*DOI: 10.12659/MSM.923603
Med Sci Monit 2020; 26:e923603
Abstract
BACKGROUND: Osteoporosis is a chronic skeletal disease characterized by a reduction in bone density, resulting in high death rates and high costs among patients worldwide. This study investigated the associations among age, anthropometric parameters and bone mineral density (BMD) in southeast Chinese adults and evaluated the characteristics of southeast Chinese adults at high risk of osteoporosis.
MATERIAL AND METHODS: This study enrolled 424 female and 265 male volunteers. Height, weight and BMD were measured, and body mass index (BMI) was calculated. Based on their BMD T-scores, female and male participants were divided into groups with osteoporosis (OG1) and osteopenia (OG2) and a normal group (NG).
RESULTS: The findings revealed no significant correlations between BMD and anthropometric parameters in either gender. However, a significant negative correlation was noted between BMD and age in the female participants, and a significant positive correlation was observed between BMD and age in the male participants. Multiple comparisons between groups revealed that women in the OG1 and OG2 groups were significantly older than those in the NG group.
CONCLUSIONS: Age, anthropometric parameters and BMD correlate differently between groups and genders in southeast Chinese adults.
Keywords: Age Groups, Bone Density, Osteoporosis, Absorptiometry, Photon, Age Factors, Anthropometry, Cross-Sectional Studies
Background
Osteoporosis, also known as the “silent disease”, is a chronic skeletal disease characterized by low bone mass and deterioration of bone microarchitecture [1,2]. It has become a common major public health concern, with increasing incidence in both developing and developed countries [3,4]. Vertebral and hip fractures are the most frequent complications of the disease, resulting in a high risk of morbidity and early mortality [4,5]. An estimated 9 million cases of osteoporosis-related fractures are reported every year worldwide [6]. In addition, osteoporosis and its resulting complications are associated with significant economic costs related to hospitalizations, surgery, outpatient care, long-term care and disability [4]. Therefore, for the purpose of prevention and control, there is an urgent need to conduct epidemiological research on the prevalence of osteoporosis and related risk factors in large populations.
Bone mineral density (BMD) is regarded clinically as a significant determinant of osteoporosis and fracture risk [2]. BMD can be measured by several techniques, including dual energy X-ray absorptiometry and ultrasonic densitometry [7]. Although dual energy X-ray absorptiometry has been regarded as the gold standard for quantitatively estimating BMD [8,9], the application of this method is difficult because of its lack of portability and the risk of exposure to ionizing radiation [10]. As a result, ultrasonic densitometry, which is portable with no risk of exposure to harmful radiation [7], has gained in popularity for measuring the BMD of the peripheral skeleton [10]. Furthermore, this method was shown to be as sensitive as dual energy X-ray absorptiometry [7,10]. Therefore, ultrasonic densitometry may be a practical alternative measuring the prevalence of osteoporosis in large populations.
Because China has a very large population, many osteoporosis-related fractures and problems will likely occur in China [2]. It has been estimated that, by the year 2050, half of the world’s hip fractures will occur in Asia, with the majority occurring in China [11]. Thus, identifying factors that may contribute to the prevalence of osteoporosis in Asia, especially in China, could reduce the medical burden of this disease by formulating and implementing rational prevention and treatment programs based on prevalence.
Most large-scale epidemiological studies on osteoporosis have been conducted on Caucasians. Less is currently known about the associations between BMD and anthropometric parameters, such as height and weight, of Chinese adults, as a function of sex and age. Anthropometric measures differ among ethnic groups, suggesting the need for specific population studies in individual countries [12]. Moreover, most recent studies on osteoporosis prevalence in Chinese populations have focused on postmenopausal women [13–15], the elderly [2,16,17] and osteoporosis-related patients [18,19]. Less is available on Chinese participants over large age ranges, and the age ranges previously studied may be insufficient to characterize the prevalence of osteoporosis in this population. Therefore, the purpose of this study was to investigate the associations among age, anthropometric parameters and BMD in southeast Chinese adults and to evaluate the characteristics of southeast Chinese adults who are at high risk of osteoporosis.
Material and Methods
STUDY DESIGN AND PARTICIPANTS:
This cross-sectional study was performed in November 2018 in Ningbo, southeast China, and was approved by the Ethics Committee of Research Academy of Grand Health Interdisciplinary at Ningbo University (RAGH 20181013). The study population included volunteers who received test brochures from a health management research center affiliated with the University, during the period from November 2018 to December 2018. To maximize participation, the health staff fully explained the study and reminded participants of the time and date of the test when distributing the test brochures. A total of 689 participants were included. All participants were free from diseases that may have hindered them from participating in the test. Informed written consent was obtained from all participants prior to measurements and data collection.
ANTHROPOMETRIC MEASUREMENTS:
Anthropometric parameters included height, weight and body mass index (BMI). The measurements were recorded by trained technicians following international guidelines [3]. Height and weight were measured while participants were in a standing position, wearing light clothing, with no shoes, using a tape meter stadiometer with 1 mm accuracy. Weight was measured using a calibrated digital electronic weighing scale with an accuracy of ±100 grams. BMI was calculated as the ratio of weight (in kilograms) to height (in meters) squared.
BONE MINERAL DENSITY (BMD) MEASUREMENT:
BMD was assessed at the calcaneus of the non-dominant leg using ultrasonic densitometry (OsteoPro UBD 2002A, B. M. Tech Co., Ltd., Korea) by the same trained medical technician over the entire experimental period. Each instrument was standardized and calibrated before the first measurement on each test day in accordance with the manufacturer’s recommendations. BMD is a clinical determinant of osteopenia or osteoporosis and is calculated using each individual’s T-score according to the criteria established by the World Health Organization (WHO), in which a score of greater than −1 indicated normal bone density, a score from −1 to −2.5 indicated low bone mass or osteopenia, and a score of less than −2.5 indicated osteoporosis [20]. Following ultrasonic densitometry, female and male participants were divided into three groups, an osteoporosis group (OG1, n=29 and n=54, respectively), an osteopenia group (OG2, n=191 and n=138, respectively), and a normal group (NG, n=203 and n=72, respectively).
STATISTICAL ANALYSES:
All data were presented as mean±standard deviation (SD). Spearman’s rank-order correlation coefficient was applied to assess the linear correlations between age, anthropometric parameters and BMD in each gender. One-way analysis of variance with post hoc Tukey tests were used for multiple comparisons of age and anthropometric parameters between groups. All statistical analyses were performed using SPSS software, version 17.0 (SPSS Inc., Chicago, IL, USA), with
Results
Complete data sets were available for 689 participants, including 424 females (61.5%) and 265 males (38.5%). Characteristics of these participants are summarized in Table 1.
Correlation analysis (Table 2, Figures 1, 2) showed that, except for age, there were no significant correlations between BMD and height, weight and body mass index (BMI) in both genders. In contrast, age was found to be negatively correlated with BMD in female participants (r −0.24,
When comparing the means of age and anthropometric parameters and BMD categories, there were significant differences between groups (Table 3). Multiple comparisons using post-hoc analysis showed that age was significantly higher in the OG2 (
Discussion
The main purpose of this study was to identify whether there were any associations among age, anthropometric parameters and BMD in southeast Chinese adults. Our results demonstrated that there were no significant correlations between BMD and anthropometric parameters, including height, weight, and BMI, in either gender. However, BMD and age were significantly correlated in both males and females, with the correlations being positive in male but negative in female participants.
Recently, ultrasonic densitometry measurements of BMD at the calcaneus site have been proposed for identifying individuals at risk of osteoporotic fracture in large populations. This technique has been demonstrated to be an ideal experimental tool because of its portability and lack of the risk of radiation [7,10,21,22]. However, if a T-score less than −2.5 is defined as osteoporosis, the prevalence of osteoporosis may be underestimated when BMD of the heel is measured by ultrasonic densitometry [23]. This finding may partially explain why the correlations between anthropometric parameters and BMD observed in this study differed from those in previous studies, which have found that, in addition to age, BMD significantly correlated with height, weight, and BMI [1,7,24,25]. Because few studies have assessed correlations among age, anthropometric parameters and BMD in Asian populations, especially in Chinese, other factors may have contributed to the differences observed.
Results from this study also revealed that associations between age and BMD differed in females and males. In females, increased age was associated with a significantly increased risk of osteoporosis, a finding consistent with those observed previously [10,26,27]. Our results indicated that age was positively associated with BMD in males, suggesting that increased age may result in a decreased tendency toward osteoporosis. To our knowledge, this finding has not been observed in other populations, including Asian populations.
Several possible reasons could explain these differences. First, because of increasing social pressures from both family and work, young Chinese men are becoming more dependent on alcohol, with total per capita alcohol consumption of Chinese men being 17.0 liters in 2016, which is much higher than the world average [28]. Alcohol dependence would lead to several medical problems, such as liver dysfunction and vitamin D deficiency, which could increase the risk of osteoporosis [29]. In addition, alcohol itself can disturb bone remodeling and enhance bone fragility, which increase bone loss [30]. Fractures have been reported to be over four times more frequent in subjects with chronic alcoholism than in age-matched controls [31]. Second, a large proportion of the young participants recruited in this study were office workers, who tended to have sedentary lifestyles. In contrast, older participants are becoming more and more health-conscious and participate in more outdoor sports activities. Exercise has shown consistent benefits on BMD and has been widely recommended as a primary preventive strategy to reduce the risk of osteoporosis [32,33]. Third, this trend may be misleading, as few older participants were involved in this study. Although a significantly positive association was found between age and BMD in male participants, there were no significant differences in age when the three groups were compared. More interestingly, the mean age of the OG1 and OG2 groups was slightly greater than that of the NG group, indicating that the correlations observed in male participants may have been influenced by high leverage points on the extremes of the data set. Additional studies, however, are warranted to fully understand these inconsistences.
This study also attempted to summarize the characteristics of southeast Chinese adults who are at high risk of osteoporosis. Results of multiple comparisons showed that there were no significant differences in anthropometric parameters among groups of both genders. However, height, weight, and BMI tended to decrease from the NG to the OG1 group, indicating that both male and female subjects with osteoporosis were shorter, lighter and had a lower BMI. This finding is consistent with studies in Caucasian populations [34–36]. In addition, female osteoporosis patients in this study were older, as females in the OG2 and OG1 groups were significantly older than those in the NG group. However, the correlation between age and BMD of male participants and the age difference among male groups differed from results of other studies.
This study had several limitations. First, it was cross-sectional in design, making it difficult to fully explore the time course of bone loss. Moreover, several other parameters, such as family history and lifestyle, which may affect the risk of osteoporosis, were not measured in this study. Lastly, although this study included large numbers of males and females over a wide age range, none of the participants was aged 70–80 years. Further longitudinal studies with larger sample sizes and wider age ranges are warranted to explore the prevalence of osteoporosis and related factors in Chinese populations.
Conclusions
In conclusion, this study provides reference data for setting up national programs to prevent and control osteoporosis in China. The results showed that BMD was negatively correlated with age in females, and positively correlated with age in males. In addition, the anthropometric parameters of Chinese osteoporosis patients were consistent with those measured in Caucasians, except for the age of the male participants. Because few studies to date have focused on the onset of osteoporosis in China, further exploratory investigations are required to fully understand these differences and relationships.
Figures
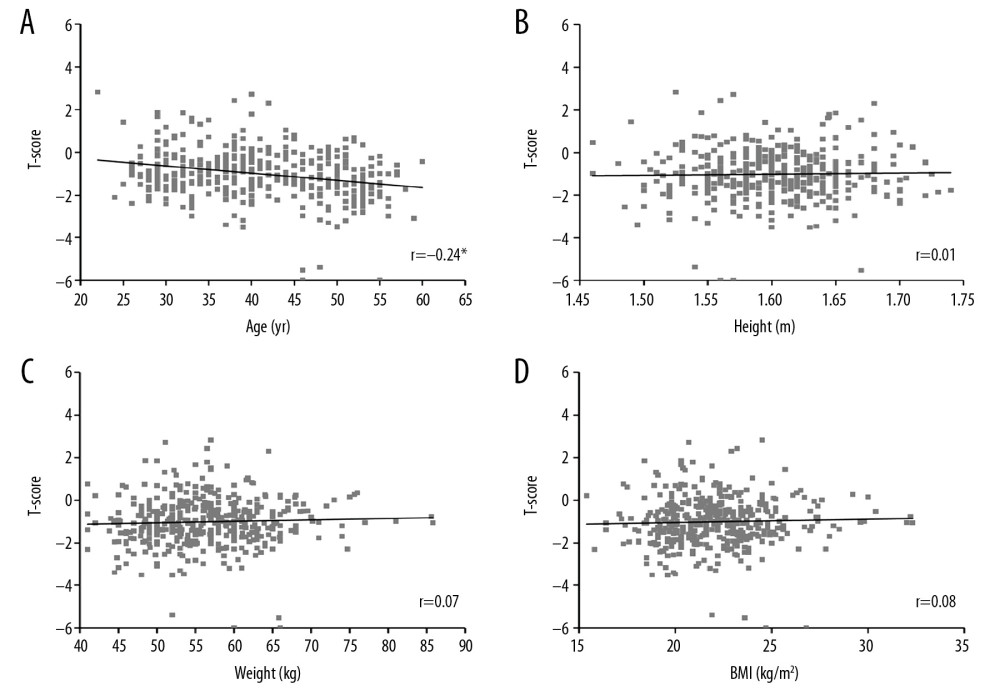 Figure 1. Correlations among age, anthropometric parameters and BMD of female participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05.
Figure 1. Correlations among age, anthropometric parameters and BMD of female participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05. 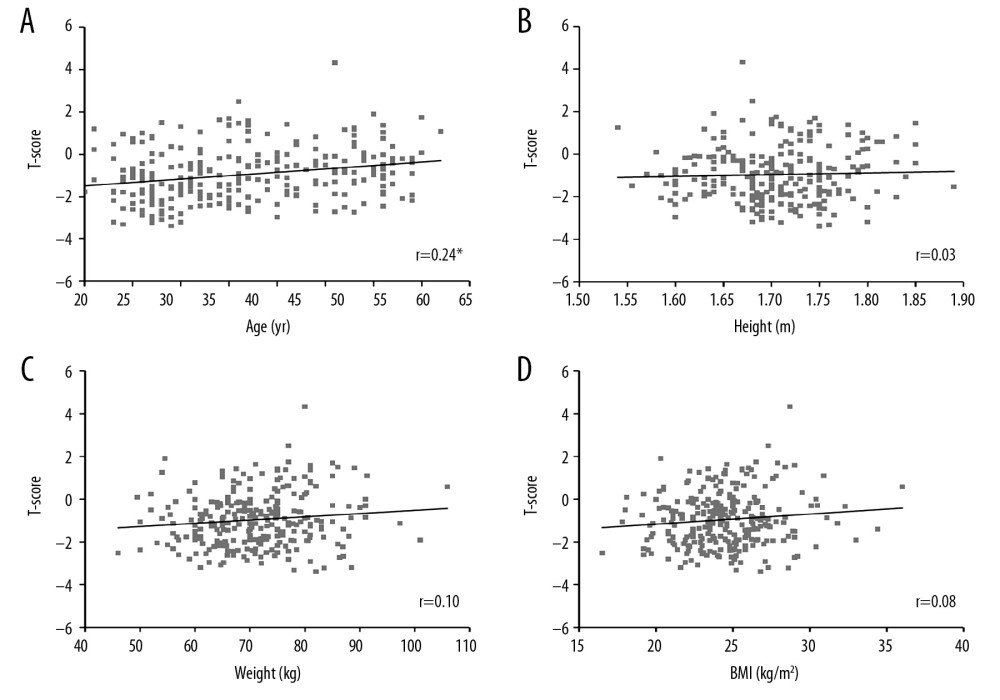 Figure 2. Correlations among age, anthropometric parameters and BMD of male participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05.
Figure 2. Correlations among age, anthropometric parameters and BMD of male participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05. References
1. Tariq S, Tariq S, Lone KP, Relationship of anthropometric measures with bone mineral density in postmenopausal non-osteoporotic, osteopenic and osteoporotic women: J Pak Med Assoc, 2017; 67; 590-94
2. Bian P, Li X, Ying Q, Factors associated with low femoral neck bone mineral density in very elderly Chinese males: Arch Gerontol Geriatr, 2015; 61; 484-88
3. Lewiecki EM, Silverman SL, Redefining osteoporosis treatment: Who to treat and how long to treat: Arq Bras Endocrinol Metab, 2006; 50; 694-704
4. Morales-Torres J, Gutiérrez-Ureña SOsteoporosis Committee of Pan-American League of Associations for Rheumatology, The burden of osteoporosis in Latin America: Osteoporos Int, 2004; 15; 625-32
5. Center JR, Nguyen TV, Schneider D, Mortality after all major types of osteoporotic fracture in men and women: an observational study: Lancet, 1999; 353; 878-82
6. Johnell O, Kanis JA, An estimate of the worldwide prevalence and disability associated with osteoporotic fractures: Osteoporos Int, 2006; 17; 1726-33
7. Annamalai R, Lal JS, Correlation of anthropometric measurements with bone mineral density in south Indian population: Int J Orthop Sci, 2018; 4(1); 221-24
8. Santos L, Romeu JC, Canhão H, A quantitative comparison of a bone remodeling model with dual-energy X-ray absorptiometry and analysis of the inter-individual biological variability of femoral neck T-score: J Biomech, 2010; 43; 3150-55
9. Fawzy T, Muttappallymyalil J, Sreedharan J, Association between body mass index and bone mineral density in patients referred for dual-energy X-ray absorptiometry scan in Ajman, UAE: J Osteoporos, 2011; 2011 876309
10. Hien VTT, Khan NC, Lam NT, Determining the prevalence of osteoporosis and related factors using quantitative ultrasound in Vietnamese adult women: Am J Epidemiol, 2005; 161; 824-30
11. Cooper C, Campion G, Melton LJ, Hip fractures in the elderly: A world-wide projection: Osteoporos Int, 1992; 2; 285-89
12. Kagawa M, Binns CW, Hills AP, Body composition and anthropometry in Japanese and Australian Caucasian males and Japanese females: Asia Pac J Clin Nutr, 2007; 16; 31-36
13. Han W, Bai XJ, Han LL, The relationship between serum fibroblast growth factor 23, Klotho, and lumbar spine bone mineral density in northern Chinese postmenopausal women: Menopause, 2019; 26; 546-53
14. Shi L, Mao C, Wang X, Association of chemerin levels and bone mineral density in Chinese obese postmenopausal women: Medicine, 2016; 95; e4583
15. Wei QS, Chen ZQ, Tan X, Serum serotonin concentration associated with bone mineral density in Chinese postmenopausal women: Scand J Clin Lab Invest, 2017; 77; 40-44
16. Yang XJ, Sang HX, Bai B: Med Sci Monit, 2018; 24; 7438-43
17. Cheung EYN, Ho AYY, Lam KF, Determinants of bone mineral density in Chinese men: Osteoporos Int, 2005; 16; 1481-86
18. Hou K, Lin C, Chen C, Association of probiotics and bone mineral density in Chinese patients with type 2 diabetes: Biomed Res, 2017; 28; 129-33
19. Zhao X, Zhang XM, Yuan N, Associations of bone mineral density and bone metabolism indices with urine albumin to creatinine ratio in Chinese patients with type 2 diabetes: Exp Clin Endocr Diab, 2019; 127; 50-55
20. Genant HK, Cooper C, Poor G, Interim report and recommendations of the World Health Organization Task-Force for Osteoporosis: Osteoporos Int, 1999; 10; 259-64
21. Greenspan SL, Cheng S, Miller PD, Orwoll ESQUS-2 PMA Trials Group, Clinical performance of a highly portable, scanning calcaneal ultrasonometer: Osteoporos Int, 2001; 12; 391-98
22. Boyanov M, Popivanov P, Prevalence of low forearm bone density in a Bulgarian female referral population: Osteoporos Int, 2002; 13; 288-95
23. Frost ML, Blake GM, Fogelman I, Contact quantitative ultrasound: an evaluation of precision, fracture discrimination, age-related bone loss and applicability of the WHO criteria: Osteoporos Int, 1999; 10; 441-49
24. Soltani A, Larijani B, Khashayar P, The relationship between anthropometric parameters and bone mineral density in an Iranian referral population: Acta Med Iran, 2014; 52; 505-10
25. Meybodi HA, Hemmat-Abadi M, Heshmat R, Association between anthropometric measures and bone mineral density: Population-based study: Iran J Public Health, 2011; 40; 18-24
26. Gregg EW, Kriska AM, Salamone LM, Correlates of quantitative ultrasound in the Women’s Healthy Lifestyle Project: Osteoporos Int, 1999; 10; 416-24
27. Yamaguchi J, Truman G, Cameron ID, Lifestyle factors affecting bone ultrasonometry of the calcaneus in Japanese women: Calcif Tissue Int, 2000; 66; 43-46
28. Liu R, Chen L, Zhang F, Trends in alcohol intake and the association between socio-demographic factors and volume of alcohol intake amongst adult male drinkers in China: Int J Environ Res Public Health, 2019; 16; 573
29. Pitts TO, Van Thiel DH, Disorders of divalent ions and vitamin D metabolism in chronic alcoholism: Recent developments in alcoholism, 1986; 357-77, Boston, Springer
30. Chakkalakal DA, Alcohol-induced bone loss and deficient bone repair: Alcohol Clin Exp Res, 2005; 29; 2077-90
31. Berg KM, Kunins HV, Jackson JL, Association between alcohol consumption and both osteoporotic fracture and bone density: Am J Med, 2008; 121; 406-18
32. Bonaiuti D, Shea B, Iovine R, Exercise for preventing and treating osteoporosis in postmenopausal women: Cochrane Database Syst Rev, 2002(3); CD000333
33. Benedetti MG, Furlini G, Zati A, Mauro GL, The effectiveness of physical exercise on bone density in osteoporotic patients: Biomed Res Int, 2018; 2018 4840531
34. Morin S, Tsang JF, Leslie WD, Weight and body mass index predict bone mineral density and fractures in women aged 40 to 59 years: Osteoporos Int, 2009; 20; 363-70
35. Barger-Lux MJ, Heaney RP, Calcium absorptive efficiency is positively related to body size: J Clin Endocr Metab, 2005; 90; 5118-20
36. Shapses SA, Riedt CS, Bone, body weight, and weight reduction: what are the concerns?: J Nutr, 2006; 136; 1453-56
Figures
 Figure 1. Correlations among age, anthropometric parameters and BMD of female participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05.
Figure 1. Correlations among age, anthropometric parameters and BMD of female participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05. Figure 2. Correlations among age, anthropometric parameters and BMD of male participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05.
Figure 2. Correlations among age, anthropometric parameters and BMD of male participants. Correlations between (A) age and BMD; (B) height and BMD; (C) weight and BMD; and (D) BMI and BMD. BMD, bone mineral density; * p<0.05. Tables
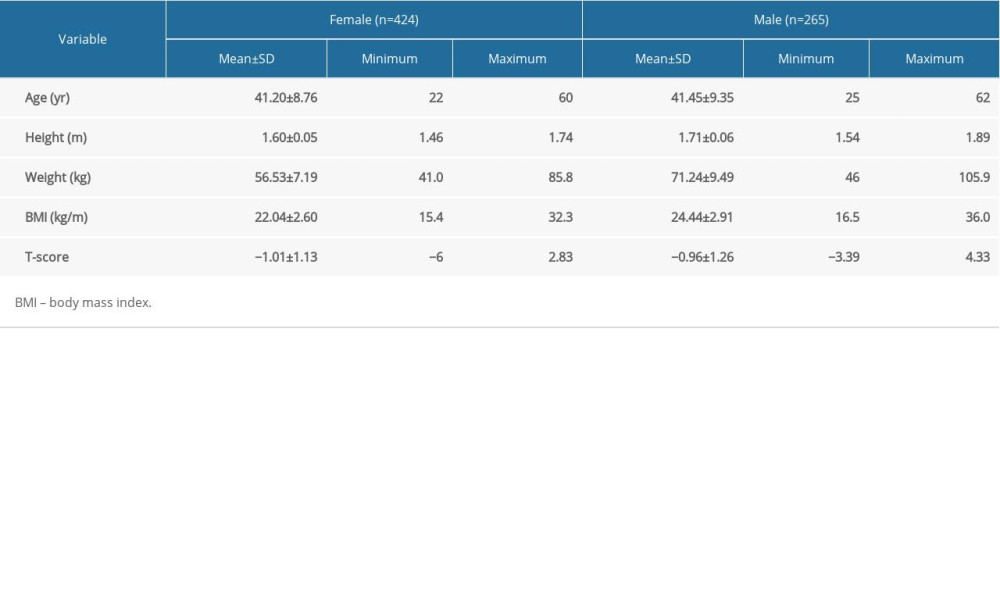 Table 1. Characteristics of the study population.
Table 1. Characteristics of the study population.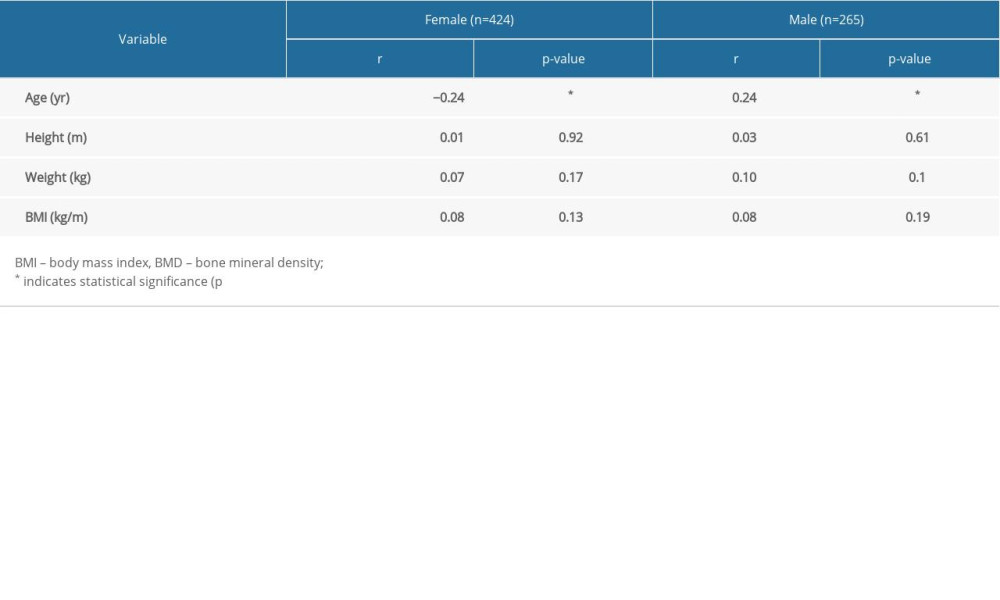 Table 2. Correlations between age, anthropometric parameters and BMD in female and male participants.
Table 2. Correlations between age, anthropometric parameters and BMD in female and male participants.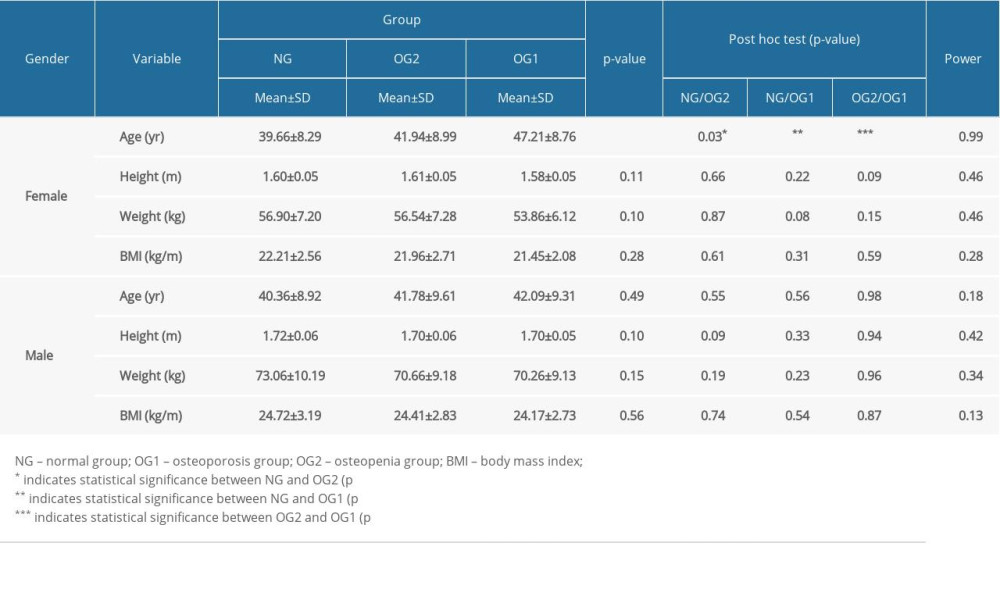 Table 3. Comparisons of age and anthropometric parameters between different groups of female and male participants.
Table 3. Comparisons of age and anthropometric parameters between different groups of female and male participants. Table 1. Characteristics of the study population.
Table 1. Characteristics of the study population. Table 2. Correlations between age, anthropometric parameters and BMD in female and male participants.
Table 2. Correlations between age, anthropometric parameters and BMD in female and male participants. Table 3. Comparisons of age and anthropometric parameters between different groups of female and male participants.
Table 3. Comparisons of age and anthropometric parameters between different groups of female and male participants. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








