06 August 2020: Review Articles
Extracorporeal Membrane Oxygenation (ECMO) in Critically Ill Patients with Coronavirus Disease 2019 (COVID-19) Pneumonia and Acute Respiratory Distress Syndrome (ARDS)
Xiaochun Ma1ABCDEF, Menglin Liang2B, Min Ding2B, Weiming Liu2B, Huibo Ma3BEF, Xiaoming Zhou4ABE, Hongsheng Ren2ABE*DOI: 10.12659/MSM.925364
Med Sci Monit 2020; 26:e925364
Abstract
ABSTRACT: Traced back to December 2019, an unexpected outbreak of a highly contagious new coronavirus pneumonia (COVID-19) has rapidly swept around China and the globe. There have now been an estimated 2 580 000 infections and more than 170 000 fatal cases around the world. The World Health Organization (WHO) estimated that approximately 14% of infections developed into severe disease, 5% were critically ill, and the mortality rate of critically ill patients is reported to be over 50%. The shortage of specific anti-viral treatment and vaccines remains a huge challenge. In COVID-19, refractory hypoxemia is common among the critically ill with acute respiratory distress syndrome (ARDS) despite invasive mechanical ventilation, and is further complicated by respiratory and circulatory failure. This difficult situation calls for the use of extracorporeal membrane oxygenation (ECMO) for assisting respiration and circulation if necessary. This article reviews the pertinent clinical literature, technical guidance, and expert recommendations on use of ECMO in critically ill cases of COVID-19. Here, we present basic knowledge and opinions about COVID-19 and ECMO, review the evidence on ECMO use in Middle East Respiratory Syndrome (MERS) and H1N1 influenza, share the technical guidance and recommendations on use of ECMO in COVID-19, summarize the current use of ECMO against COVID-19 in China, and discuss the issues in use of ECMO in COVID-19.
Keywords: COVID-19, Critical Illness, Extracorporeal Membrane Oxygenation, Respiratory Distress Syndrome, Adult, Betacoronavirus, COVID-19, Coronavirus Infections, Pandemics, Pneumonia, Viral, Practice Guidelines as Topic, SARS-CoV-2
Brief Introduction of 2019-nCoV
Since 8 December 2019, novel coronavirus (2019-nCoV)-infected pneumonia (COVID-19) cases were reported in Wuhan, Hubei province, China and afterwards spread across the entire world [1]. The 2019-nCoV is a single-strand, positive-sense RNA virus, and full-genome sequencing and phylogenic analysis suggests that this virus is closely related to bat coronaviruses [2]. 2019-nCoV also appears to be related to the coronaviruses causing Severe Acute Respiratory Syndrome (SARS-CoV) and Middle East Respiratory Syndrome (MERS-CoV) [3]. The initial reports suggested the transmission from wild animals to humans occurring in the Huanan Seafood Wholesale Market [4]. However, the origin of 2019-nCoV as well as the location of “Patient Zero” is still being explored. Evidence shows that 2019-nCoV uses angiotensin-converting enzyme II (ACE2) as a cellular entry receptor, which is also known to be a cell receptor for SARS-CoV [5].
Burden and Challenges of Critical Illness with COVID-19
CLINICAL CHARACTERISTICS OF COVID-19:
By 21 April 2020, the outbreak had grown to infect 82 788 subjects in China, with 4632 deaths, and infecting 2 498 661 people with 173 849 deaths in 184 other countries/regions [6]. The World Health Organization (WHO) has declared the outbreak a global health emergency and the regional and global risk levels have been upgraded to the highest level since 28 February 2020 [7]. COVID is a highly infectious respiratory disease primarily transmitted through contact, droplets, and possibly airborne in certain situations, although the precise mechanisms are not fully understood [8]. The trace of viral nucleic acid detected within stool and urine specimens hints at other possible transmission modes [9,10]. The diagnosis is established as confirmed or suspected COVID-19 by clinicians according to typical signs and symptoms and other major criteria, including rise in body temperature, decrease in counts of lymphocytes and white blood cells, detection of bilateral ground-glass opacity (GGO) or patchy shadows from chest computed tomography (CT), and positive result of testing by RT-PCR [11,12]. The typical signs and symptoms of patients include fever, fatigue, dry cough, anorexia, myalgia, and dyspnea, and some cases also manifest gastrointestinal and neurological symptoms [13,14]. Most cases have mild symptoms, with a good prognosis. Severe cases rapidly develop within 1 week into acute respiratory distress syndrome (ARDS), septic shock, refractory metabolic acidosis, coagulopathy, multiple organ dysfunction syndrome (MODS), and even death [4,15].
Gattinoni et al. proposed that COVID-19 is a specific disease with an inconsistency between the severity of the hypoxemia and respiratory system compliance. Depending on the median respiratory system compliance (50 ml/cmH2O), patients with COVID-19 are categorized into non-ARDS and ARDS subgroups [16]. ARDS is a clinical syndrome characterized by refractory hypoxemia and it has recently attracted much attention due to its high fatality rate. Although ARDS is triggered by various intrapulmonary and/or extrapulmonary causes, most cases manifest an acute onset of respiratory distress and hypoxemia that are difficult to correct with conventional oxygen therapy. Currently, the Berlin definition is used internationally to diagnose and stratify the severity of ARDS: (1) within 1 week of a known clinical insult or new or worsening respiratory symptoms; (2) chest imaging showing bilateral opacities not fully explained by effusions, lobar/lung collapse, or nodules; (3) origin of edema and respiratory failure not fully explained by cardiac failure or fluid overload and requiring objective assessment (e.g., echocardiography) to exclude hydrostatic edema if no risk factors are present; and (4) oxygenation, i) Mild, 200 mmHg <PaO2/FIO2 ≤300 mmHg with PEEP or CPAP ≥5 cmH2O; ii) Moderate, 100 mmHg <PaO2/FIO2 ≤200 mmHg with PEEP ≥5 cmH2O; iii) Severe, PaO2/FIO2 ≤100 mmHg with PEEP ≥5 cmH2O [17–19].
Mild cases are isolated for general anti-viral, symptomatic, and supportive therapies, whereas critically ill cases require admission to intensive care units (ICUs) for providing more aggressive treatment [20,21]. Of note, in endemic areas, infection ranges from asymptomatic infection, mild symptoms, to fatal respiratory syndromes, and re-infection with RNA tested positive after recovery has been sporadically reported in China [22,23].
SEVERE AND CRITICAL ILLNESS IN COVID-19:
Severe and critically ill cases in China currently account for approximately 7.8% of remaining confirmed cases based on the latest update. In Wuhan, China, 15.5% of cases are severe and critically ill, whereas outside Wuhan, China, this proportion is 6.9% of remaining confirmed cases [6]. The WHO estimated in a situation report that approximately 15% of cases developed into severe disease and 5% were critically ill around the world [24]. A recent meta-analysis of clinical characteristics of 50 466 hospitalized patients with COVID-19 in China estimated that the incidence of ARDS was 14.8% and severe and critically ill cases accounted for 18.1% of all infected cases [15]. The proportions of severe and critical infection are higher than with influenza infection [25]. Recent reports suggested that advanced age, comorbid conditions, and compromised immune function might predict ICU admission, poorer clinical outcomes, and even mortality [26]. Among these common preexisting health conditions are obesity, diabetes, malignant cancers, and cardiovascular diseases (CVD) [27].
MORTALITY OF COVID-19:
The mortality rate of COVID-19 is estimated to be approximately 6.9% across the globe, 5.6% in China, and 7.7% in Wuhan, as calculated from the latest reported data, which has proven to be higher than a previous rough estimation of 2.0% [6]. Mortality rates are variable in different epidemic countries and are much lower than those of SARS (SARS-CoV has a mortality rate of approximately 10.0%) and MERS (MERS-CoV, approximately 40.0% mortality rate) [28]. The above-mentioned meta-analysis calculated the mortality rate of COVID-19 as being approximately 4.3% in China [15]. However, the exact number of deaths due to COVID-19 has been over 10-fold higher than with the 2003 SARS epidemic, and the mortality rate of cases with critical illness has been reported as over 50% [29]. The mortality rate of COVID-19 seems high, considering that the mortality rate of seasonal influenza is commonly below 0.1%. Nevertheless, the current crude estimation of the COVID-19 mortality rate could be inflated and the true mortality rate has yet to be fully determined. It is hoped that the mortality rate will decline as the access to and quality of health care gradually improve [30].
TREATMENT OF COVID-19:
The treatment challenge is currently a lack of effective anti-viral therapy and vaccines for COVID-19. In response, a number of therapeutics are in clinical trials in China and more than 20 vaccines are in development for COVID-19 [31]. The most efficacious way for the general public to prevent disease is to avoid being unprotected from this infection and to boost immunity. The Recommendations for Diagnosis and Treatment of COVID-19 released by the National Health Commission of China (NHCC) states that all confirmed or suspected cases should be treated in isolation wards or hospitals. Severe and critical illness should be identified early and quickly transferred to ICUs for immediate optimized supportive care and treatment. For uncomplicated illness or mild pneumonia, oxygen therapy, anti-viral therapy, and symptomatic and supportive treatments are sufficient with close monitoring. For severe and critically ill cases, respiratory support is crucial in reversing the disease progression and decreasing the mortality and morbidity rates [32]. Particularly in cases of severe ARDS, refractory hypoxemia may gradually deteriorate despite protective mechanical ventilation or even prone ventilation. Considering that circulatory failure can further complicate the situation in COVID-19, what choice is left? The WHO and NHCC have suggested the use of extracorporeal membrane oxygenation (ECMO) for assisting respiration (and circulation if necessary) in critically ill patients with COVID-19 [32,33]. Within this article the pertinent clinical literature, technical guidance, and expert recommendations are reviewed for use of ECMO in critically ill patients with COVID-19. In this article we present basic knowledge about ECMO, review the evidence on use of ECMO in MERS and H1N1 influenza, share the technical guidance and recommendations of ECMO in COVID-19, summarize the current use of ECMO against COVID-19 in China, and discuss the issues in application of ECMO in COVID-19.
Basic Knowledge of ECMO
BASIC THEORY OF ECMO:
Cardiopulmonary bypass (CPB) is a technology that uses special artificial devices to mimic the human heart and lung to temporarily replace cardiopulmonary function and maintain the blood supply and gas exchange of the whole body. As a canonical example of technological expansion and extension of CPB, ECMO provides effective circulation and respiratory support in critically ill patients [34,35]. According to the report of the 3rd annual meeting of Chinese Society of Extracorporeal Support (CSECLS2019), there were 435 ECMO centers worldwide and ECMO treatment was performed in 13 394 cases in 2018 [36]. The Extracorporeal Life Support Organization (ELSO) estimated that in 2018 the survival rates of respiratory and circulatory support by ECMO were 58.7% to 73.2% and 42.7% to 52.6%, respectively [37]. Even with the continuous improvement of technology, the incidence of complications and mortality still remains high in ECMO treatment [38]. ECMO is a highly complex and sophisticated form of life support performed in specialized, experienced referral centers. ECMO is also very expensive, which to some extent hinders its rapid development [39].
The purpose of ECMO is to resolve hypoxemia and improve blood perfusion, ultimately gaining valuable time for recovery of the cardiopulmonary system or for organ transplantation. In ECMO, venous blood is drained out of the body, oxygenated by an extracorporeal membrane oxygenator, and transfused back into the body, with the entire process driven by a pump [40]. Unlike CPB used in open-heart surgery, the maintenance time of ECMO is much longer. ECMO equipment is relatively simple but must be high quality, with the core being the membrane oxygenator and the drive pump. The function of the pump, similar to the role of the heart, is to generate power that drives the blood to flow along the tube and lead out of or flow into the human body. The pumps currently used in ECMO are categorized into roller pumps and centrifugal pumps, both of which generate centrifugal force through the roller or motor to produce negative pressure and blood flow. The oxygenator, also called the “artificial lung”, is a gas exchange device for blood flow, and its function is mainly to absorb oxygen, dispose of carbon dioxide, and to regulate temperature [41].
For the patients with cardiopulmonary failure who require ECMO assistance, different assistance modes are used for different indications. According to the vessels that the blood is drained out of or injected into, the modes are classified as VA (venous to arterial)-ECMO, which draws the blood from the veins and injects it back into the arteries, and VV (venous to venous)-ECMO, which draws blood from and injects it back into the veins. There are also special forms of ECMO, such as VAV (venous to arterial and venous)- ECMO [42]. VV-ECMO is suited to patients with simple respiratory failure, and VA-ECMO and VAV-ECMO are capable of supporting both circulatory and respiratory failure [43].
VV-ECMO:
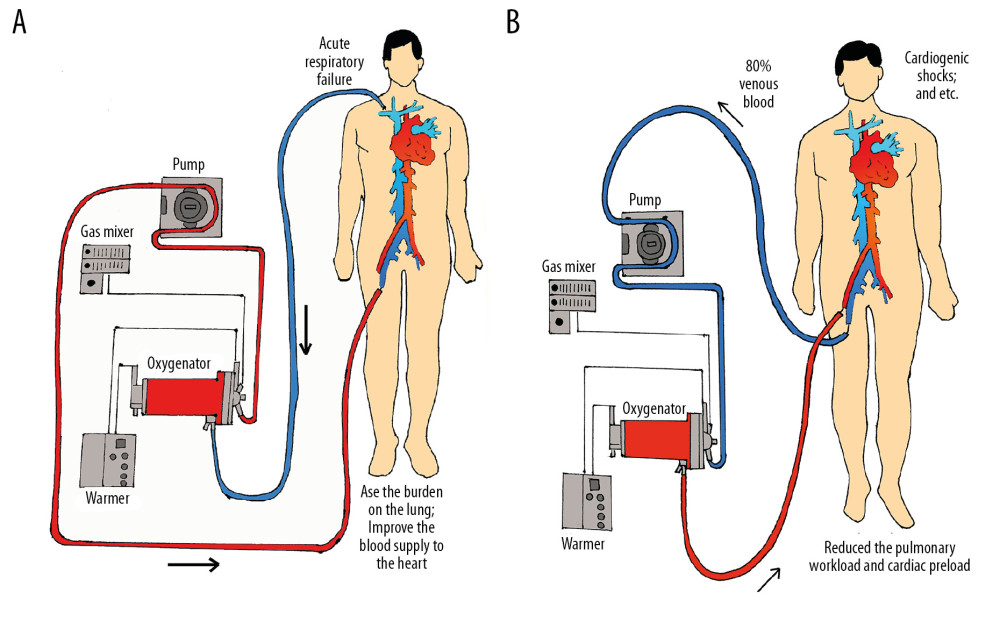
At present, the most frequently used modality of VV-ECMO is to drain venous blood out from the femoral vein and then infuse it back through the internal jugular vein [44]. When the VV mode is operating, the oxygen supply is from the extracorporeal oxygenator and autologous pulmonary circulation, which not only eases the burden on the lungs but also improves blood supply to the heart. The oxygenated blood directly enters the pulmonary artery to participate in the circulation, reducing pulmonary circulation resistance and right ventricular afterload (Figure 1A). Because of its unique cardiopulmonary-protective effect, VV-ECMO is considered as an assisting modality for reversible lung diseases with respiratory failure when traditional methods are not effective [45]. Thanks to advances in technology, its indications have been greatly expanded, and VV-ECMO can now be the preferred treatment option in patients with acute respiratory failure (ARF) who meet the indications [46].
VA-ECMO:
The traditional operation of VA-ECMO is to place the catheters in the femoral artery and femoral vein. About 80% of the venous blood is drained out, oxygenated, and then reinfused through the femoral artery [44], which reduces the pulmonary workload and cardiac preload to the greatest extent. VA-ECMO achieves the conversion of venous to arterial blood and supplies a large amount of oxygen to meet the needs of the body while maintaining low cardiac output (Figure 1B). At present, in the rescue of cardiogenic shocks due to conditions such as acute myocardial infarction and fulminant myocarditis, VA-ECMO provides prompt and efficacious support for gaining valuable time for recovery [47]. In addition, it also is associated with better outcomes in conditions such as acute heart failure caused by drowning, frostbite, and acute drug poisoning [48].
ECMO, as a life support for patients with cardiopulmonary failure, is a long-duration invasive respiratory and circulatory assisting system. During ECMO treatment, there are multiple risk factors that can lead to adverse complications, such as the long-term implantation of artificial devices, the non-physiological intervention in respiratory and circulatory systems, and the pathophysiological status of patients [40]. The complications are categorized into mechanical-related and patient-related according to the mechanisms. The mechanical-related complications of the ECMO system occur due to malfunction of mechanical devices, and include thrombosis, intubation problems, oxygenator dysfunction, and air embolism. Patient-related complications are a series of pathophysiological responses caused by factors such as invasive treatment or non-physiological intervention of ECMO, as well as preexisting diseases, during ECMO support. These complications mainly consist of bleeding, renal insufficiency, infection, hemolysis, hyperbilirubinemia, and certain complications of circulatory, respiratory, and nervous systems [49–51]. The most common complications of ECMO are bleeding and thrombosis, especially in patients with coagulopathy [52]. Particularly in COVID-19, the patients treated with ECMO are mostly sedated, which makes early detection and management of potentially fatal cerebral hemorrhage difficult [53]. In addition, patients receiving ECMO treatment often have drug-resistant bacterial infections.
In the treatment of COVID-19 patients, MODS is the most challenging problem, in which the kidneys and coagulation system are most commonly involved [54]. Thus, ECMO is often applied in conjunction with hemofiltration or plasmapheresis [55]. Patients treated with ECMO still need ventilator assistance, but at this time ECMO partially and temporarily replaces the cardiopulmonary function, and the ventilator parameters should be as low as possible to allow the lungs to fully rest. We suggest that the tidal volume should be reduced to 2–4 ml/kg, the FiO2 to 50%, the respiratory rate to 8–10 times/min, and the PEEP to 4–6 mmH2O. When ECMO is used, if there is carbon dioxide retention or respiratory acidosis, the ventilator should be adjusted to assist in removing excess carbon dioxide.
Evidence on ECMO Use in ARDS
Extracorporeal support techniques have been greatly improved and extensively applied in recent decades after several types of promising results were reported. Despite the growing use of VV-ECMO in ARDS, there is still a lack of clinical evidence supporting its use, and clinicians have been warned of its use in the treatment of severe ARDS. As early as 1979, Zapol and colleagues conducted the first multicenter, prospective, randomized study assessing the safety and efficacy of prolonged ECMO use in severe acute respiratory failure (ARF) in various conditions. No additional benefit for long-term survival was found, with the mortality being dismal at approximately 91.0% in both groups [56]. As a consequence of this disappointing result, ECMO was almost completely discarded for adult critical care for 3 decades until the encouraging outcome of its use as a rescue therapy in severe H1N1 infection in Australia and New Zealand (details shown below). Another example was a 2013 cohort study and propensity score analysis by Pham et al. exploring the role of ECMO in reducing ICU mortality in patients with severe H1N1 influenza-related ARDS. Nevertheless, the ICU mortality was comparable between the ECMO and non-ECMO groups [57]. Munshi et al. performed a meta-analysis in 2014 including 10 studies and 1248 patients and found no significant difference in hospital mortality between ECMO and mechanical ventilation; however, when restricted to higher-quality studies of VV-ECMO, a significant decrease in mortality was noted with ECMO compared with mechanical ventilation [58]. Supporting evidence of the efficacy of ECMO came from the second multicenter randomized controlled trial – the CESAR trial – reporting that treatment by ECMO significantly increased the rate of survival to 6 months without disability compared to conventional management [59].
In responding to the inconsistent results above, the American Thoracic Society/European Society of Intensive Care Medicine/Society of Critical Care Medicine Clinical Practice Guideline made no recommendation about use of ECMO in patients with ARDS due to insufficient evidence, and future research investigating clinical outcomes of ECMO in ARDS is needed. This guideline called for high-quality RCTs comparing VV-ECMO to conventional mechanical ventilation, such as the EOLIA trial (Extracorporeal Membrane Oxygenation for Severe Acute Respiratory Distress Syndrome) [60]. The EOLIA trial was a randomized trial evaluating the safety and efficacy outcomes of early application of ECMO in very severe ARDS, in comparison with conventional protective mechanical ventilation. The trial showed no statistically significant improvement in 60-day mortality by ECMO use. Nevertheless, the risk of a composite outcome was significantly decreased, which was defined as transfer to ECMO or death. Additionally, a post hoc Bayesian analysis of this RCT showed that ECMO is very likely to improve the outcome across a series of prior assumptions when applied early in severe ARDS [61–63].
Experience of ECMO in MERS and H1N1 Influenza
ECMO IN MERS:
In 2016, Rhee et al. reported the clinical implications of 5 severe cases of MERS in a South Korean outbreak, in which 1 patient (20%) required ECMO to treat refractory hypoxemia [64]. In the same year, Al-Dorzi et al. published an observational study of a hospital outbreak of MERS-CoV infection in Saudi Arabia, in which 1 in 8 patients (12.5%) requiring ICU admission received ECMO treatment [65]. In 2016, Choi et al. reported on the clinical presentation and outcomes of MERS in the Republic of Korea, in which ECMO was used in 3.8% of 186 patients [66]. In 2017, Arabi et al. reported that patients with MERS severe acute respiratory infection in Saudi Arabia were more likely to receive ECMO therapy than those with non-MERS severe acute respiratory infection (5.8% vs. 0.9%, p=0.003) [67]. In 2018, Shalhoub et al. published a multicenter study on critically ill healthcare workers (HCW) with MERS in Saudi Arabia, and found that non-surviving HCW were more likely to have received ECMO therapy compared to survivors – 5/8 (62.5%) versus 4/24 (16.7%), respectively [68]. In summary, ECMO was implemented among 12.5% to 28.1% of severe and critical illness with MERS in different centers, and among 3.8% to 5.8% of all MERS patients. However, clinical evidence has been sparse regarding the benefit or risk of ECMO in MERS, as revealed by our thorough search of pertinent studies in PubMed, Cochrane Library, and Embase. A 2018 comparative study by Alshahrani et al. assessed 35 critically ill patients with MERS with refractory hypoxemia in Saudi Arabia, among which 17 had received VV-ECMO, showing that use of ECMO significantly lowered the mortality rate of MERS compared with conventional respiratory care (100% vs. 65%), which was the only result supporting the benefit of ECMO for reducing mortality in patients with MERS [69]. This lack of evidence might be attributable to the small number of infections and deaths the disease has caused and the limited area in which MERS has spread. Severe cases with MERS remain at high risk of in-hospital death, although ECMO appeared to be somewhat effective.
ECMO USE IN H1N1:
ECMO was proven valuable in treating viral pneumonia during the H1N1 influenza pandemic in 2009. An early report of 68 severe cases with ARDS after H1N1 infection by the Australia and New Zealand Extracorporeal Membrane Oxygenation (ANZ ECMO) Influenza Investigators showed an encouraging result of 48 (71%) cases surviving to ICU discharge with the use of ECMO, and this resulted in the rebirth of ECMO technology in adult critical care [70]. Subsequently, several studies have focused on this issue and the results have been systematically reviewed and analyzed by 2 meta-analyses. A systematic review and meta-analysis in 2013 including 8 studies of patients with H1N1 influenza receiving ECMO has demonstrated that 266 (20.0%) patients were treated with ECMO with a median maintenance time of 10.0 days. The pooled estimate of in-hospital mortality suggested an overall in-hospital mortality rate of 28.0% in patients receiving ECMO, but the heterogeneity was obvious due to highly variable in-hospital mortality rates ranging between 8.0% and 65.0% among the included studies, and the patients underwent mechanical ventilation before ECMO implantation for a median of 2.0 days [71]. Recently, an updated meta-analysis of 13 studies on the same issue has reported that 494 patients receiving ECMO also had a median maintenance duration of 10.0 days, and the overall mortality rate was 37.1% despite a high level of heterogeneity. The median duration for mechanical ventilation was 19.0 days and ICU stay was 33.0 days [72]. Based on the data above, ECMO treatment appears to be feasible and effective as a salvage therapy for severe H1N1 pneumonia with respiratory failure. Despite this, it predicts a prolonged duration of ventilation and ICU stay and high mortality. Particularly, 1 group of authors highlighted that starting ECMO shortly after mechanical ventilation can improve survival rates [72].
The effectiveness of ECMO in improving survival in severe H1N1 pneumonia with respiratory failure is not clear. Evaluation of previous studies revealed debatable results with major methodological issues. Two quasi-RCTs evaluating ECMO in H1N1 were higher-quality studies but still yielded inconsistent outcomes. A 2011 matched-control observational study of 75 ARDS patients with H1N1 influenza in the UK showed a significantly lower mortality rate in the ECMO group compared to the non-ECMO group (23.7% vs. 52.5%) [73]. A meta-analysis by Munshi et al. of 3 studies and 364 patients found that ECMO was associated with a significantly lower in-hospital mortality rate in severe H1N1 infection, but its reliability was limited [74]. Hence, without high-quality data, use of ECMO in severe hypoxemic illness with H1N1 is still debatable.
Technical Guidance and Recommendations On Use of ECMO in COVID-19 Patients
Considering the reversibility of COVID-19 as a self-limited infection as well as the therapeutic effect of ECMO in MERS and influenza A H1N1, implementation of ECMO would to a large extent aid in the respiratory and circulatory support in critical illness with COVID-19. However, there are differences in the application ECMO in different centers regarding timing, indications, and patient management [75].
On 28 January 2020, the WHO released technical guidance for clinical management of severe acute respiratory infection when 2019-nCoV infection is suspected. This guidance uses a yellow exclamation mark to highlight conditional and careful recommendations on EMCO use in selected patients [33]. The National Institutes for Health (NIH) produced new treatment guidelines that acknowledge the use of ECMO in critical care [76]. In the third edition of Recommendations by NHCC, the use of ECMO is recommended in respiratory support to cure severe and critical illness when necessary, along with prone-position ventilation and lung recruitment [77]. In the sixth edition, ECMO is listed as a salvage therapy for severe ARDS after prone-position ventilation and lung recruitment becomes ineffective [78]. In the seventh edition, the indications of use of ECMO were supplemented as: (1) PaO2 <80 mmHg when FiO2 >0.9; and (2) airway plateau/pause pressure ≥35 cmH2O. For respiratory failure, VV mode is the preferred choice, and VA mode is applied when circulatory support is required [32].
The global panel in the ELSO prepared a detailed set of guidelines for ECMO use in patients with COVID-19. For VV-ECMO, the ELSO recommends against the initiation of ECMO prior to maximizing the traditional therapies for ARDS. VV-ECMO should be considered when: (1) PaO2/FiO2 <150 mmHg; (2) any of: i) PaO2/FiO2 <60 mmHg for >6 h; ii) PaO2/FiO2 <50 mmHg for >3 h; iii) pH <7.20 and PaCO2 >80 mmHg for >6 h; (3) no contraindication to ECMO; or (1) PaO2/FiO2 ≥150 mmHg; (2) pH <7.20 with PaCO2 >80 mmHg for >6 h; (3) no contraindication to ECMO [79].
The recommendations by the Chinese National Clinical Research Center for Respiratory Diseases suggest that ECMO should be considered when the standard respiratory support, such as lung-protective mechanical ventilation (tidal volume [VT] ≤6 ml/kg, airway plateau/pause pressure <30 cmH2O and positive end-expiratory pressure (PEEP) ≥10 cmH2O), lung recruitment, prone positioning, neuromuscular blockade, and sedation, fails to improve respiratory function in COVID-19. Specifically, ECMO should be implemented according to the following criteria: (1) PaO2/FiO2 <50 mmHg for more than 3 h; (2) PaO2/FiO2 <80 mmHg for more than 6 h; (3) arterial blood pH <7.25 and PaCO2 >60 mmHg for more than 6 h [75].
Consistently, the CSECLS suggests that ECMO should be initiated quickly before the refractory hypoxemia leads to MODS or the parameters of ventilators are adjusted to an improperly high level. With reference to the timing of ECMO for primary or secondary hypoxic respiratory failure due to any cause, the use of ECMO should be considered when the risk of death reaches or exceeds 50%, and ECMO treatment should be started when the risk of death reaches or exceeds 80%. Given that myocarditis has been reported in H1N1 influenza and MERS, myocarditis might also occur in COVID-19, and severe cases may manifest circulatory dysfunction. When these patients are complicated by cardiogenic shock or cardiac arrest, VA mode is needed for circulatory support. The indications of EMCO by CSECLS are similar to the above-mentioned ones except for: (1) PaO2/FiO2 <100 mmHg when FiO2=1.0; (2) severe thoracic air-leak syndrome; (3) cardiogenic shock or cardiac arrest [80].
Current Situation of Use of ECMO in COVID-19 in China
Data on use of ECMO in COVID-19 patients in China are sparse. Wang et al. published a cross-sectional study assessing the clinical characteristics of 138 hospitalized patients with COVID-19 in Wuhan, China, in which ECMO was used in 4 cases (2.9%), which accounted for 11.1% of ICU cases. Chest CT images showed the obvious absorption of bilateral GGO in a 52-year-old patient with critical illness 5 days after treatment with ECMO [13]. Chen et al. described the epidemiological and clinical characteristics of 99 cases of COVID-19 in Wuhan, China, and ECMO was provided in 3 cases (3.0%). A 69-year-old patient died of unresolved hypoxemia despite use of ECMO [1]. Huang et al. published a study on the clinical features of 41 patients infected with 2019-nCoV in Wuhan, China, and ECMO as salvage therapy was provided in 2 of 41 patients (4.9%) receiving ICU care due to refractory hypoxemia (15.4% of ICU patients) [4]. In the study by Yang et al. comparing clinical courses and outcomes in critically ill patients with COVID-19, 1 in 20 survivors (5.0%) and 5 in 32 (15.6) non-survivors received ECMO treatment, which means that 5 (83.3%) of 6 patients receiving ECMO failed to survive [81]. To sum up, the studies from Wuhan, China found that ECMO was used in 2.9% to 4.9% of hospitalized COVID-19 patients and in 11.1% to 15.4% of patients in the ICU. Zhong et al. summarized the clinical characteristics of 1099 COVID-19 patients in China recruited from 552 hospitals in 30 provinces, autonomous regions, and municipalities, among whom ECMO treatment was given in 5 patients (0.45%). These 5 patients accounted for 2.9% of 173 severe patients and 7.5% of 67 cases with the presence of a composite primary end-point of admission to ICU, use of mechanical ventilation, or death [82]. Given that more than 90% of severe and critical COVID-19 cases in China were treated in Wuhan, according to the latest data, the more frequent usage of ECMO in Wuhan is reasonable. After digital searching of relevant literature in PubMed, Cochrane Library, Embase, and other databases (such as medRxiv 2020), detailed information on use of ECMO in Wuhan, China, outside Wuhan, China, and in other countries is still missing. Zeng et al. recently published a case series of 12 patients, assessing the prognosis of ECMO usage for critical illness of COVID-19 in China, among which 3 patients were weaned successfully from ECMO, 5 died, and 4 remained alive with ECMO (but 2 were in a coma) [83]. However, the benefits and risks of ECMO in improving recovery and survival in COVID-19 remain unclear due to a shortage of solid evidence from high-quality comparative studies.
According to the EuroECMO-COVID Survey released on 18 April 2020, there were 820 patients with COVID-19 treated by ECMO [84]. A total of 515 ECMO-supported suspected or confirmed COVID-19 cases were reported by ELSO Chapter as of 22 April 2020. The median time of intubation before ECMO was 90 h, and the VV-ECMO mode was mostly used. There were 211 patients completing the ECMO regimen, among whom 90 were still in hospital. The median ECMO duration was 191 h and the mortality rate was 41% [85].
Vital Questions of ECMO in COVID-19
The very first dilemma is the absence of relevant clinical evidence from around the world. Although ECMO has been implemented in severe and critically ill patients with COVID-19 in China, few details are currently available for further analysis and interpretation. Hence, the role of ECMO in the management of COVID-19 remains elusive. There is a need for collaboration of registries and clinical research groups worldwide, as well as multicenter, high-quality, prospective, observational studies and randomized trials [86].
The second question is the benefit of ECMO in the management of COVID-19. Based on the lessons learned from MERS and H1N1 influenza, it is not difficult to speculate that even with the use of ECMO, the mortality rates of severe and critical patients with COVID-19 are still very high. Mechanically, ECMO is not a panacea for the MODS commonly observed in COVID-19 deaths; this is a difficult situation in which ECMO has shown limited efficacy [87]. In addition, ECMO does not provide direct support in the treatment of septic shock, coagulopathy, or other comorbid diseases. In addition to mortality, ECMO is associated with longer ICU stay and hospitalization, lower bed turnover, and higher medical expenses. Another core question in assessing the benefits of ECMO is whether ECMO is superior to traditional mechanical ventilation therapy in improving COVID-19 patient survival. Solving this problem requires high-quality prospective observational or randomized trials in the future, but obtaining such evidence from randomized trials is still challenging, even a decade after the H1N1 epidemic and 4 decades after the initial trial by Zapol et al.
The third question is when to apply ECMO in COVID-19 appropriately and what indications should be referred to. Some guidelines recommend the usage of ECMO as a rescue therapy after standard treatment fails [33]. Some authors suggest early implementation before MODS or severe ventilator-associated lung injury because studies have suggested that early initiation of ECMO in ARDS might be beneficial, especially among younger patients [88,89]. We have observed that if ECMO is initiated more than 10 days after invasive ventilator use in the treatment of COVID-19, the possibility of successful treatment is low. However, due to the shortage of ECMO equipment and experts, early application of ECMO might indeed be impractical in smaller or unqualified centers. Important ethical questions arise in deciding who receives ECMO treatment and who has priority.
The fourth question is choosing the best ECMO mode and position of catheterization. VV mode is preferred, but it is unknown in COVID-19 how many have or will develop myocarditis or circulatory failure. When should VA-ECMO or VAV-ECMO be activated in time for circulatory support and on what indications? Additionally, what strategies of ventilation and fluid management should be used when ECMO is running?
The fifth problem involves potential harm or complications of ECMO use in COVID-19 patients and how to prevent these complications in advance. Henry suggested that immunological indicators such as lymphocyte count and IL-6 should be closely monitored in patients receiving ECMO [90]. Because survivors and non-survivors of COVID-19 differ significantly in lymphocyte counts and IL-6 concentrations, these 2 indicators (lymphocyte count and IL-6) are to a large extent influenced by ECMO use [91–93]. Minimizing the risk of nosocomial infections is also pivotal because ECMO produces body fluid splashes and places medical staff at great risk. Hence, standardized protocols should be formulated, expert teams organized, and independent ICU wards established [75].
Conclusions
The highly contagious 2019-ConV has now infected tens of thousands of Chinese and has rapidly become a global pandemic, with health care systems overwhelmed with severe and critically ill patients in less well-resourced countries. ECMO is a sophisticated life support system supporting respiratory and circulatory failure and has been utilized in the management of severe infection with MERS and H1N1 influenza, with some evidence showing an additional survival benefit with use of ECMO. Much remains mysterious about the virus 2019-ConV, and solid clinical evidence is lacking on the role of ECMO in rescuing critical illness. Despite the application of ECMO in China and recommendations on ECMO by WHO and Chinese experts in COVID-19, several fundamental questions remain unanswered, including benefit, timing, indications, management, and risks of ECMO, as well as global sharing of evidence from trials.
References
1. Chen N, Zhou M, Dong X, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study: Lancet, 2020; 395(10223); 507-13
2. Zhou P, Yang XL, Wang XG, A pneumonia outbreak associated with a new coronavirus of probable bat origin: Nature, 2020; 579(7798); 270-73
3. Lu R, Zhao X, Li J, Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding: Lancet, 2020; 395(10224); 565-74
4. Huang C, Wang Y, Li X, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China: Lancet, 2020; 395(10223); 497-506
5. Brojakowska A, Narula J, Shimony R, Bander J, Clinical implications of SARS-Cov2 interaction with renin angiotensin system: J Am Coll Cardiol, 2020 [Online ahead of print]
6. National Health Commission of the People’s Republic of China: The latest situation of new coronavirus pneumonia by the end of April 21, 2020 Available from: 2020. Available from: http://www.nhc.gov.cn/xcs/yqtb/202004/965362945d96437da80117e53610fb3e.shtml
7. World Health Organization: The latest situation of new coronavirus pneumonia by the end of January 28, 2020 Available from: 2020. Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports
8. Wax RS, Christian MD, Practical recommendations for critical care and anesthesiology teams caring for novel coronavirus (2019-nCoV) patients: Can J Anaesth, 2020; 67(5); 568-76
9. Ling Y, Xu SB, Lin YX, Persistence and clearance of viral RNA in 2019 novel coronavirus disease rehabilitation patients: Chin Med J (Engl), 2020; 133(9); 1039-43
10. Li LY, Wu W, Chen S, Digestive system involvement of novel coronavirus infection: Prevention and control infection from a gastroenterology perspective: J Dig Dis, 2020; 21(4); 199-204
11. Zhang G, Hu C, Luo L, Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China: J Clin Virol, 2020; 127; 104364
12. Qi X, Lei J, Yu Q, CT imaging of coronavirus disease 2019 (COVID-19): From the qualitative to quantitative: Ann Transl Med, 2020; 8(5); 256
13. Wang D, Hu B, Hu C, Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China: JAMA, 2020; 323(11); 1061-69
14. Zhang JJ, Dong X, Cao YY, Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China: Allergy, 2020 [Online ahead of print]
15. Sun P, Qie S, Liu Z, Clinical characteristics of hospitalized patients with SARS-CoV-2 infection: A single arm meta-analysis: J Med Virol, 2020 [Online ahead of print]
16. Gattinoni L, Chiumello D, Rossi S, COVID-19 pneumonia: ARDS or not?: Crit Care, 2020; 24(1); 154
17. Matthay MA, Aldrich JM, Gotts JE, Treatment for severe acute respiratory distress syndrome from COVID-19: Lancet Respir Med, 2020; 8(5); 433-34
18. Force ADT, Ranieri VM, Rubenfeld GD, Acute respiratory distress syndrome: The Berlin Definition: JAMA, 2012; 307(23); 2526-33
19. Ramanathan K, Antognini D, Combes A, Planning and provision of ECMO services for severe ARDS during the COVID-19 pandemic and other outbreaks of emerging infectious diseases: Lancet Respir Med, 2020; 8(5); 518-26
20. Li L, Li R, Wu Z, Therapeutic strategies for critically ill patients with COVID-19: Ann Intensive Care, 2020; 10(1); 45
21. Cook DJ, Marshall JC, Fowler RA, Critical illness in patients with COVID-19: Mounting an effective clinical and research response: JAMA, 2020 [Online ahead of print]
22. Mao ZQ, Wan R, He LY, The enlightenment from two cases of asymptomatic infection with SARS-CoV-2: Is it safe after 14 days of isolation?: Int J Infect Dis, 2020; 95
23. Zhou L, Liu K, Liu HGCause analysis and treatment strategies of “recurrence” with novel coronavirus pneumonia (covid-19) patients after discharge from hospital: Zhonghua Jie He He Hu Xi Za Zhi, 2020; 43; 281-84 [in Chinese]
24. World Health Organization: The latest situation of new coronavirus pneumonia by the end of March 1, 2020 Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports
25. Wu D, Lu J, Liu Y, Positive effects of COVID-19 control measures on influenza prevention: Int J Infect Dis, 2020; 95; 345-46
26. Jordan RE, Adab P, Cheng KK, Covid-19: Risk factors for severe disease and death: BMJ, 2020; 368; m1198
27. Wang B, Li R, Lu Z, Huang Y, Does comorbidity increase the risk of patients with COVID-19: Evidence from meta-analysis: Aging (Albany NY), 2020; 12(7); 6049-57
28. Xie M, Chen Q, Insight into 2019 novel coronavirus – an updated intrim review and lessons from SARS-CoV and MERS-: CoV Int J Infect Dis, 2020; 94; 119-24
29. Han Q, Lin Q, Jin S, You L, Coronavirus 2019-nCoV: A brief perspective from the front line: J Infect, 2020; 80(4); 373-77
30. Wang W, Tang J, Wei F, Updated understanding of the outbreak of 2019 novel coronavirus (2019-nCoV) in Wuhan, China: J Med Virol, 2020; 92(4); 441-47
31. National Health Commission of the People’s Republic of China: The latest situation of vaccines for new coronavirus pneumonia by the end of April 14, 2020 Available from: http://www.nhc.gov.cn/xcs/xwbd/202004/e9dd56d9e1e344b7a83bc05b3cbcbfa0.shtml
32. National Health Commission of the People’s Republic of China: Diagnosis and Treatment Protocol for COVID-19 (Trial Version 7) Available from: http://en.nhc.gov.cn/2020-03/29/c_78469.htm
33. World Health Organization: Clinical management of severe acute respiratory infection when novel coronavirus (nCoV) infection is suspected Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/technical-guidance
34. Al-Fares A, Pettenuzzo T, Del Sorbo L, Extracorporeal life support and systemic inflammation: Intensive Care Med Exp, 2019; 7(Suppl 1); 46
35. Datzmann T, Trager K, Extracorporeal membrane oxygenation and cytokine adsorption: J Thorac Dis, 2018; 10(Suppl 5); S653-60
36. Available from: https://csecls2019.medmeeting.org/8735?lang=cn
37. : Extracorporeal Life Support Organization (ELSO) report in 2018 Available from: https://www.elso.org/
38. Vieira J, Frakes M, Cohen J, Wilcox S, Extracorporeal membrane oxygenation in transport part 2: Complications and troubleshooting: Air Med J, 2020; 39(2); 124-32
39. Lim JKB, Qadri SK, Toh TSW, Extracorporeal membrane oxygenation for severe respiratory failure during respiratory epidemics and pandemics: A narrative review: Ann Acad Med Singapore, 2020; 49(4); 1-34
40. Millar JE, Fanning JP, McDonald CI, The inflammatory response to extracorporeal membrane oxygenation (ECMO): A review of the pathophysiology: Crit Care, 2016; 20(1); 387
41. Ratnani I, Tuazon D, Zainab A, Uddin F, The role and impact of extracorporeal membrane oxygenation in critical care: Methodist Debakey Cardiovasc J, 2018; 14(2); 110-19
42. Napp LC, Kuhn C, Hoeper MM, Cannulation strategies for percutaneous extracorporeal membrane oxygenation in adults: Clin Res Cardiol, 2016; 105(4); 283-96
43. Camboni D, Philip A, Schmid C, Loforte A, Double, triple and quadruple cannulation for veno-arterial extracorporeal membrane oxygenation support: Is there a limit?: Ann Cardiothorac Surg, 2019; 8(1); 151-59
44. Jayaraman AL, Cormican D, Shah P, Ramakrishna H, Cannulation strategies in adult veno-arterial and veno-venous extracorporeal membrane oxygenation: Techniques, limitations, and special considerations: Ann Card Anaesth, 2017; 20(Suppl); S11-18
45. Mazzeffi M, Galvagno S, Menaker J, VV ECMO cannulation: Should i stay or should i go?: J Cardiothorac Vasc Anesth, 2019; 33(7); 1871-72
46. Del Sorbo L, Goffi A, Goligher E, Setting mechanical ventilation in ARDS patients during VV-ECMO: Where are we?: Minerva Anestesiol, 2015; 81(12); 1369-76
47. Li Y, Yan S, Cai L, Zhang Q, Does VA-ECMO plus impella work in refractory cardiogenic shock?: JACC Heart Fail, 2019; 7(4); 364
48. Behr CA, Strotmeyer SJ, Swol J, Gaines BA, Characteristics and outcomes of extracorporeal life support in pediatric trauma patients: J Trauma Acute Care Surg, 2020 [Online ahead of print]
49. Thomas J, Kostousov V, Teruya J, Bleeding and thrombotic complications in the use of extracorporeal membrane oxygenation: Semin Thromb Hemost, 2018; 44(1); 20-29
50. Ostermann M, Connor M, Kashani K, Continuous renal replacement therapy during extracorporeal membrane oxygenation: Why, when and how?: Curr Opin Crit Care, 2018; 24(6); 493-503
51. Schilcher G, Eisner F, Hackl G, Candida infection of membrane oxygenator during ECMO therapy: J Infect, 2019; 78(1); 75-86
52. Fong KM, Au SY, Wu HLH, Ng GWY, A potential source of cerebral emboli in patients supported with peripheral VA-ECMO: Intensive Care Med, 2019; 45(5); 702-3
53. Hartman ME, Hernandez RA, Patel K, COVID-19 respiratory failure: Targeting inflammation on VV-ECMO support: ASAIO J, 2020, 2020; 66(6); 603-6
54. Du Y, Tu L, Zhu P, Clinical features of 85 fatal cases of COVID-19 from Wuhan: A retrospective observational study: Am J Respir Crit Care Med, 2020; 201(11); 1372-79
55. Ronco C, Navalesi P, Vincent JL, Coronavirus epidemic: Preparing for extracorporeal organ support in intensive care: Lancet Respir Med, 2020; 8(3); 240-41
56. Zapol WM, Snider MT, Hill JD, Extracorporeal membrane oxygenation in severe acute respiratory failure. A randomized prospective study: JAMA, 1979; 242(20); 2193-96
57. Pham T, Combes A, Roze H, Extracorporeal membrane oxygenation for pandemic influenza A(H1N1)-induced acute respiratory distress syndrome: A cohort study and propensity-matched analysis: Am J Respir Crit Care Med, 2013; 187(3); 276-85
58. Munshi L, Walkey A, Goligher E, Venovenous extracorporeal membrane oxygenation for acute respiratory distress syndrome: A systematic review and meta-analysis: Lancet Respir Med, 2019; 7(2); 163-72
59. Peek GJ, Mugford M, Tiruvoipati R, Efficacy and economic assessment of conventional ventilatory support versus extracorporeal membrane oxygenation for severe adult respiratory failure (CESAR): A multicentre randomised controlled trial: Lancet, 2009; 374(9698); 1351-63
60. Fan E, Del Sorbo L, Goligher EC, An Official American Thoracic Society/European Society of Intensive Care Medicine/Society of Critical Care Medicine Clinical Practice Guideline: Mechanical ventilation in adult patients with acute respiratory distress syndrome: Am J Respir Crit Care Med, 2017; 195(9); 1253-63
61. Bartlett RH, Extracorporeal membrane oxygenation for acute respiratory distress syndrome: EOLIA and beyond: Crit Care Med, 2019; 47(1); 114-17
62. Grasselli G, Zanella A, Pesenti A, Veno-venous extracorporeal membrane oxygenation in acute respiratory distress syndrome: Should the EOLIA Study results change our clinical approach?: Minerva Anestesiol, 2019; 85(8); 909-13
63. Goligher EC, Tomlinson G, Hajage D, Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome and posterior probability of mortality benefit in a post hoc bayesian analysis of a randomized clinical trial: JAMA, 2018; 320(21); 2251-59
64. Rhee JY, Hong G, Ryu KM, Clinical implications of 5 cases of Middle East respiratory syndrome coronavirus infection in a South Korean outbreak: Jpn J Infect Dis, 2016; 69(5); 361-66
65. Al-Dorzi HM, Aldawood AS, Khan R, The critical care response to a hospital outbreak of Middle East respiratory syndrome coronavirus (MERS-CoV) infection: an observational study: Ann Intensive Care, 2016; 6(1); 101
66. Choi WS, Kang CI, Kim Y, Clinical presentation and outcomes of Middle East respiratory syndrome in the Republic of Korea: Infect Chemother, 2016; 48(2); 118-26
67. Arabi YM, Al-Omari A, Mandourah Y, Critically ill patients with the Middle East respiratory syndrome: A multicenter retrospective cohort study: Crit Care Med, 2017; 45(10); 1683-95
68. Shalhoub S, Al-Hameed F, Mandourah Y, Critically ill healthcare workers with the middle east respiratory syndrome (MERS): A multicenter study: PLoS One, 2018; 13(11); e0206831
69. Alshahrani MS, Sindi A, Alshamsi F, Extracorporeal membrane oxygenation for severe Middle East respiratory syndrome coronavirus: Ann Intensive Care, 2018; 8(1); 3
70. Davies A, Jones D, Bailey MAustralia and New Zealand Extracorporeal Membrane Oxygenation (ANZ ECMO) Influenza Investigators, Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome: JAMA, 2009; 302(17); 1888-95
71. Zangrillo A, Biondi-Zoccai G, Landoni G, Extracorporeal membrane oxygenation (ECMO) in patients with H1N1 influenza infection: A systematic review and meta-analysis including 8 studies and 266 patients receiving ECMO: Crit Care, 2013; 17(1); R30
72. Sukhal S, Sethi J, Ganesh M, Extracorporeal membrane oxygenation in severe influenza infection with respiratory failure: A systematic review and meta-analysis: Ann Card Anaesth, 2017; 20(1); 14-21
73. Noah MA, Peek GJ, Finney SJ, Referral to an extracorporeal membrane oxygenation center and mortality among patients with severe 2009 influenza A(H1N1): JAMA, 2011; 306(15); 1659-68
74. Zampieri FG, Mendes PV, Ranzani OT, Extracorporeal membrane oxygenation for severe respiratory failure in adult patients: A systematic review and meta-analysis of current evidence: J Crit Care, 2013; 28(6); 998-1005
75. Li M, Gu SC, Wu XJ, Extracorporeal membrane oxygenation support in 2019 novel coronavirus disease: Indications, timing, and implementation: Chin Med J (Engl), 2020; 133(9); 1115-17
76. National Institutes of Health (NIH). COVID-19 Treatment Guidelines Panel: Coronavirus diseases 2019 (COVID-19) treatment guidelines Available from: https://www.covid19treatmentguidelines.nih.gov/
77. National Health Commission of the People’s Republic of China: Diagnosis and treatment protocol for COVID-19 (Trial Version 3) Available from: http://www.nhc.gov.cn/xcs/zhengcwj/202001/f492c9153ea9437bb587ce2ffcbee1fa/files/39e7578d85964dbe81117736dd789d8f.pdf
78. National Health Commission of the People’s Republic of China: Diagnosis and treatment protocol for COVID-19 (Trial Version 6) Available from: http://www.nhc.gov.cn/yzygj/s7653p/202002/8334a8326dd94d329df351d7da8aefc2/files/b218cfeb1bc54639af227f922bf6b817.pdf
79. Extracorporeal Life Support Organization (ELSO): COVID-19 Interim Guidelines. A consensus document from an international group of interdisciplinary ECMO providers Available from: https://www.elso.org/Portals/0/Files/pdf/guidelines%20elso%20covid%20for%20web_Final.pdf
80. Recommendations on extracorporeal life support for critically ill patients with novel coronavirus pneumonia: Zhonghua Jie He He Hu Xi Za Zhi, 2020; 43(3); 195-98 [in Chinese]
81. Yang X, Yu Y, Xu J, Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study: Lancet Respir Med, 2020; 8(5); 475-81
82. Guan WJ, Ni ZY, Hu Y, Clinical characteristics of coronavirus disease 2019 in China: N Engl J Med, 2020; 382(18); 1708-20
83. Zeng Y, Cai Z, Xianyu Y, Prognosis when using extracorporeal membrane oxygenation (ECMO) for critically ill COVID-19 patients in China: A retrospective case series: Crit Care, 2020; 24(1); 148
84. Extracorporeal Life Support Organization: Euroelso Survey on ECMO use in adult COVID-19 patients in Europe by the end of April 18, 2020 Available from: https://www.euroelso.net/covid-19/covid-19-survey/
85. Extracorporeal Life Support Organization: ECMO in COVID-19 by the end of April 22, 2020 Available from: https://www.elso.org/Registry/FullCOVID19RegistryDashboard.aspx
86. MacLaren G, Fisher D, Brodie D, Preparing for the most critically ill patients with COVID-19: The potential role of extracorporeal membrane oxygenation: JAMA, 2020 [Online ahead of print]
87. Napp LC, Ziegeler S, Kindgen-Milles D, Rationale of hemoadsorption during extracorporeal membrane oxygenation support: Blood Purif, 2019; 48(3); 203-14
88. Crotti S, Bottino N, Spinelli E, Spontaneous breathing during veno-venous extracorporeal membrane oxygenation: J Thorac Dis, 2018; 10(Suppl 5); S661-69
89. Kurihara C, Walter JM, Singer BD, Extracorporeal membrane oxygenation can successfully support patients with severe acute respiratory distress syndrome in lieu of mechanical ventilation: Crit Care Med, 2018; 46(11); e1070-e3
90. Henry BM, de Oliveira MHS, Benoit S, Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): A meta-analysis: Clin Chem Lab Med, 2020 [Online ahead of print]
91. Terpos E, Ntanasis-Stathopoulos I, Elalamy I, Hematological findings and complications of COVID-19: Am J Hematol, 2020 [Online ahead of print]
92. Burrell AJC, Lubnow M, Enger TB, The impact of venovenous extracorporeal membrane oxygenation on cytokine levels in patients with severe acute respiratory distress syndrome: a prospective, observational study: Crit Care Resusc, 2017; 19(Suppl 1); 37-44
93. Yost G, Bhat G, Pappas P, Tatooles A, The neutrophil to lymphocyte ratio in patients supported with extracorporeal membrane oxygenation: Perfusion, 2018; 33(7); 562-67
In Press
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952