09 September 2020: Clinical Research
Echo-Tracking Technique in Ultrasonography Can Monitor Changes in Carotid Artery Elastic Function at Early Stage of Intensity-Modulated Radiation Therapy for Nasopharyngeal Carcinoma
Wei Han12BDE, Junjie Liu3BC, Zhijie Liu1BEF, Xiaodong Zhu1AFG*DOI: 10.12659/MSM.926260
Med Sci Monit 2020; 26:e926260
Abstract
BACKGROUND: We used echo-tracking (ET) technique to observe short-term dynamic changes of the carotid artery in nasopharyngeal carcinoma (NPC) patients after intensity-modulated radiation therapy (IMRT).
MATERIAL AND METHODS: Sixty-one NPC patients received IMRT. In the irradiation group, the carotid artery was examined by ultrasonography before radiotherapy, at 2, 4, and 6 weeks after the start of radiotherapy, and at 3 and 6 months after the end of radiotherapy. In the control group, the carotid artery was examined by ultrasonography before radiotherapy of patients in the irradiation group, and at 3 and 6 months after the end of radiotherapy of patients in the irradiation group.
RESULTS: During radiotherapy for the 61 patients, the maximum dose on the carotid artery was 65.14±4.35 Gy, the average dose was 57.46±4.12 Gy, and the 50% volume dose was 51.80±5.32 Gy. At the end of irradiation, Ep (kPa) and β values were significantly different from those before treatment.
CONCLUSIONS: The present study demonstrates that the elastic function of the carotid artery can be significantly affected when the irradiation dose exceeds 45 Gy.
Keywords: Carotid Arteries, Cranial Irradiation, Radiation Injuries, Radiotherapy Dosage, Radiotherapy, Intensity-Modulated, Ultrasonography
Background
The incidence rate of nasopharyngeal carcinoma (NPC) is very high in southeast and southwest China, and radiotherapy is the main treatment for the disease, including traditional brachytherapy, stereotactic radiotherapy, and intensity-modulated radiation therapy (IMRT) [1]. The toxic effect of X-rays affects not only tumor cells, but also normal tissues and cells. Therefore, X-rays can cause radiation damage to normal tissues and organs to various degrees [1]. The carotid artery is one of the most exposed organs during radiotherapy. According to a report, 67% of patients with NPC have carotid artery narrowing of more than 70%, while endometrial injury occurs at about 4 weeks after radiotherapy [2]. Because the occurrence of clinical symptoms of vascular injury is usually little and late, the universality and severity of carotid artery injury after radiotherapy and the consequences caused by the injury have attracted less clinical attention. Moreover, the effects of radiotherapy dose and time after radiotherapy on carotid artery injury have not been well studied [3]. Therefore, it is necessary to follow up the injury of carotid artery in NPC patients after radiotherapy. The echo-tracking (ET) technique in ultrasonography is a new method to determine and evaluate the elastic function of the artery. In our preliminary studies, ET technique, especially Ep and β indices, is reliable in the evaluation of early arterial injury and reduction of arterial elasticity, and has accuracy in the clinical evaluation of carotid injury. In the present study, we used ET technique to observe short-term dynamic changes of the carotid artery in NPC patients after IMRT, so as to provide reference for improving NPC radiotherapy.
Material and Methods
SUBJECTS:
Sixty-one NPC patients who were hospitalized at the First Ward of Radiotherapy Department in the Tumor Hospital Affiliated to Guangxi Medical University between July 2015 and March 2016 and completed follow-ups were chosen as the irradiation group in the study. In the 61 patients, the carotid bifurcation on at least 1 side was located in the clinical target volume (CTV) or the lymph node prevention target area. In addition, 10 healthy adults were included into a control group (7 males and 3 females; age range, 25–62 years; mean age, 39.200±12.533 years; median age, 36.5 years). The subjects in the control group were randomly selected, including postgraduates, employees, or family members of the Tumor Hospital Affiliated to Guangxi Medical University. The inclusion criteria for the control group were that the subjects were healthy and able to express their wills. The present study was registered at the International Clinical Trial Registration Platform with a registration number of ChiCTR-OOC-16008853. All procedures performed in the study were approved by the Ethics Committee of the Tumor Hospital Affiliated to Guangxi Medical University. Written informed consent was obtained from all patients or their families.
RADIATION THERAPY:
All patients underwent radical IMRT on a linear accelerator (6MV-X; Varian, Palo Alto, CA, USA). During the treatment, all patients were in supine position, and then head, neck, and shoulder thermoplastics masks were fixed. Before treatment, all patients underwent computed tomography (CT)-simulated enhancement scanning. Scanning results were fused and matched on a 3-dimensional treatment planning system workstation (MIM Software, Cleveland, OH, USA). Target areas and organs at risk are delineated in accordance with the principles established by the International Commission on Radiation Units and Measurements (ICRU). The dosage of radiotherapy should be determined according to specific patients (ranges: PGTVnx, 70.06–72.32 Gy; PGTVnd, 66.24–70.4 Gy; PCTV, 50–66.24 Gy). Radiotherapy was performed 5 times a week for 6 weeks.
DOSIMETRIC ANALYSIS:
The patient planning data and physical data for the 61 patients in the first IMRT were exported from the Pinnacle system. Treatment planning system (TPS) in the doctors’ workstation was used to analyze the radiation dose for carotid artery in included patients, and a dose-volume histogram (DVH) was plotted. Maximum dose (Dmax), mean dose (Dmean), and 50% volume dose (D50) were calculated.
ULTRASONIC EXAMINATION:
In the irradiation group, the carotid artery was examined by ultrasonography before radiotherapy, at 2, 4, and 6 weeks after the start of radiotherapy, and at 3 and 6 months after the end of radiotherapy. In the control group, the carotid artery was examined by ultrasonography before the time at which the patients in irradiation group received radiotherapy, and at 3 and 6 months after the patients in the irradiation group completed radiotherapy. In the irradiation group, the carotid artery located on the same side with the CTV was selected for examination; if both sides were involved, the mean value of bilateral examinations was used. In the control group, the mean value of bilateral examinations was used. The Aloka full digital pure beam color Doppler ultrasound diagnostic system was used for the examination at a frequency of 5–13.3 MHz.
STATISTICAL ANALYSIS:
The results were analyzed using SPSS 22.0 statistical software (IBM, Armonk, NY, USA). The data were expressed as means±standard deviations. Results at different time points were compared with that before radiotherapy using the paired
Results
THE VALUES FOR CDFI:
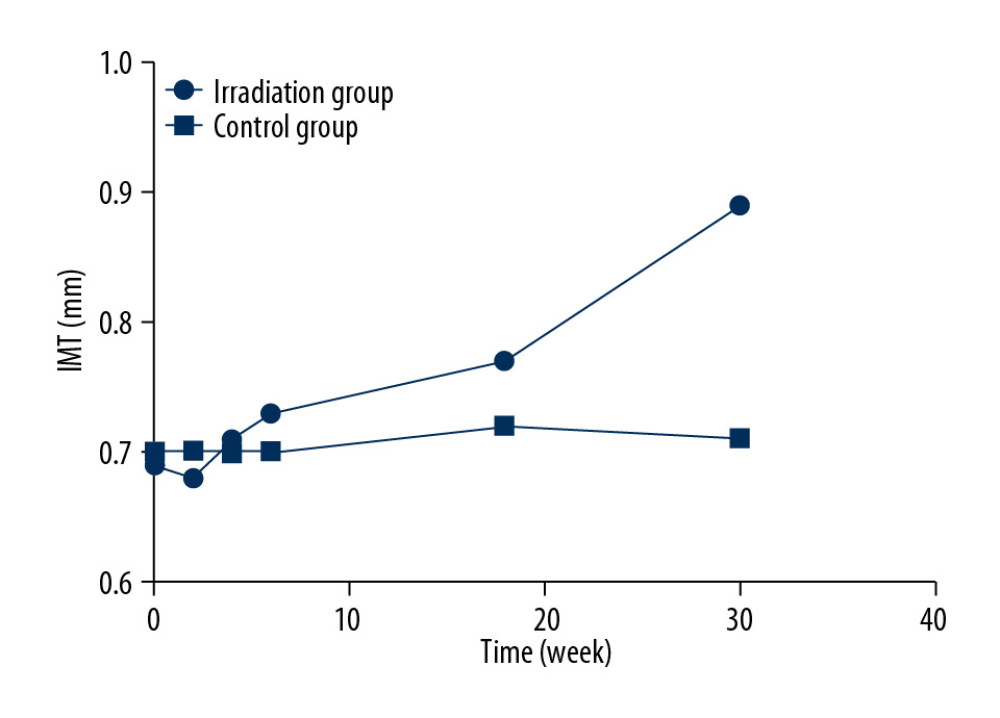
The carotid intima-media thickness (IMT) refers to the vertical dimension between carotid intima and media. The results of conventional CDFI parameters showed that there was no significant difference between IMT at the end of radiotherapy and that before radiotherapy, while statistical difference existed between IMT at 3 months and 6 months after the end of radiotherapy and IMT before radiotherapy (Table 1). In addition, IMT at week 18 after the start of radiotherapy was significantly different from that before radiotherapy (t=3.532, P=0.01), and IMT at week 30 after the start of radiotherapy was also significantly different from that before radiotherapy (t=6.548, P=0.00) (Table 1). RI at 6 months after the end of radiotherapy was significantly different from that before radiotherapy (t=2.548, P=0.01) (Table 1). Other values after the end of radiotherapy were not significantly different from those before radiotherapy (Table 1). IMT of the irradiation group at week 30 after the start of radiotherapy was significantly higher than that of the control group (P<0.05) (Table 2). Dynamic changes in IMT after irradiation are shown in Figure 1.
THE VALUES FOR ET:
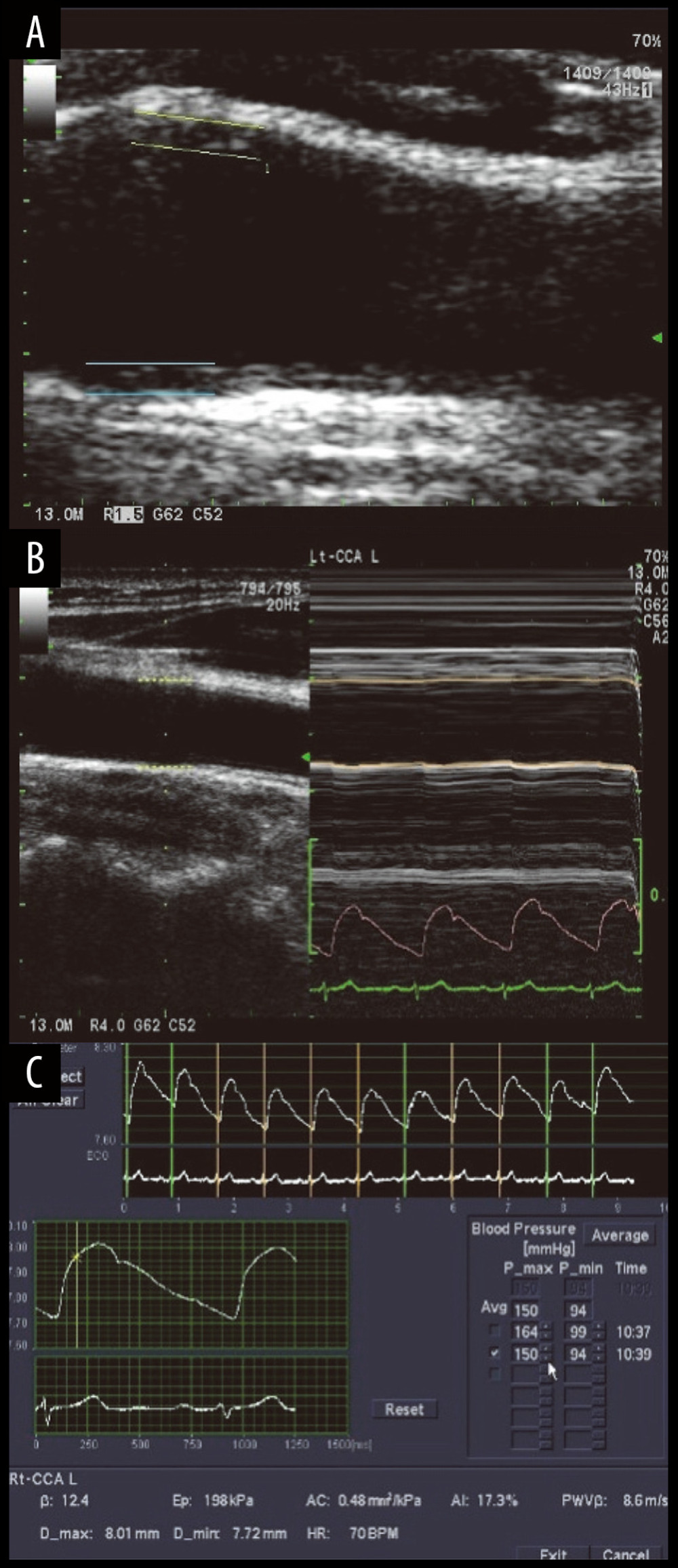
ET results showed that Ep (kPa) and β values at the end of radiotherapy were significantly different from those before radiotherapy (P<0.05). AC (mm2/kPa) and PWV-β (m/s) values at the end of radiotherapy were not different from those before radiotherapy (P>0.05), while those at 3 or 6 months after radiotherapy were significantly different from those before radiotherapy (P<0.05). AI value at the end of radiotherapy was not different from that before radiotherapy (Table 3). Ep (kPa), β, AC (mm2/kPa), and PWV-β (m/s) values of irradiation group at 3 or 6 months after radiotherapy were significantly different from those of the control group at the same time (P<0.05) (Table 3). Ultrasonic examination and ET elasticity curve of 3 patients are shown in Figure 2.
DOSIMETRIC RESULTS:
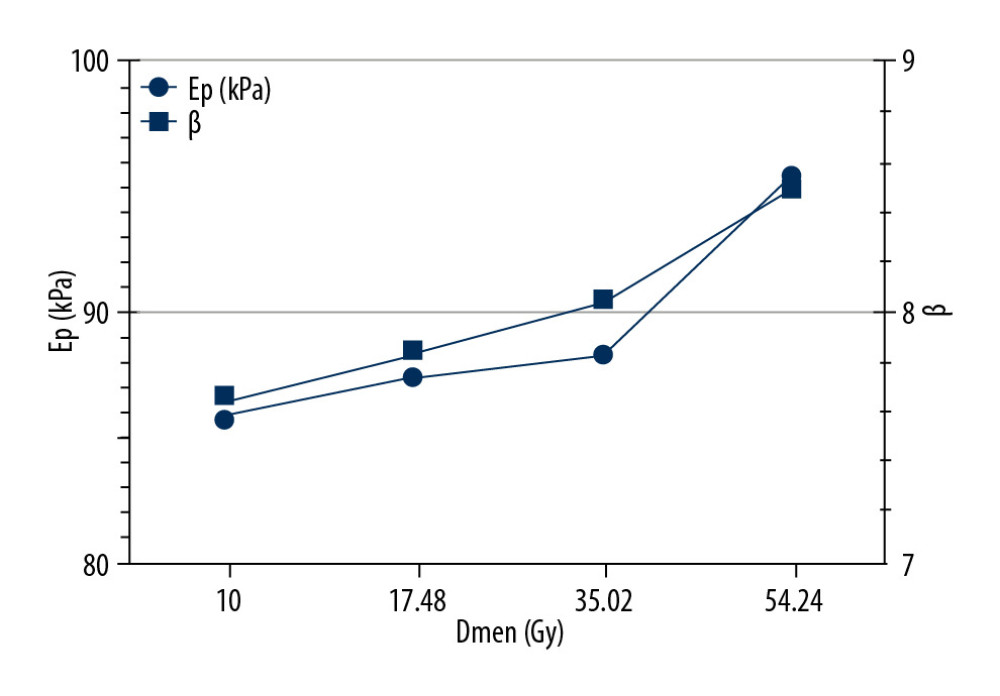
We chose 1 cm above and 2 cm below the carotid bifurcation for the study. During radiotherapy for the 61 patients, the maximum dose to the carotid artery was 65.14±4.35 Gy, the average dose was 57.46±4.12 Gy, and the 50% volume dose was 51.80±5.32 Gy (Figure 3). After the start of irradiation, Ep (kPa) and β values were slightly increased, and the increase was slow in the first 4 weeks after the start; from week 4, the increase became greater, and Dmean reached 45.02 Gy in week 4. At the end of irradiation, Ep (kPa) and β values were significantly different from those before treatment (Figure 3).
Discussion
After radiotherapy, the brain perfusion function of patients with head and neck radiotherapy often decreases, which is mainly caused by carotid artery injury, carotid artery stenosis, and carotid plaques [4,5]. Of note, the risks of stroke and cerebrovascular accidents are also increased significantly [4,5]. Radiotherapy can kill tumor cells and damage the large vessels of the neck, which will aggravate atherosclerosis of the carotid artery. In addition to indirect and direct injuries, radiotherapy also promotes the formation of arterial emboli and the risk of arterial rupture [1].
The thickness of the intima can reflect lumen change and is a reactive index of radiation injury. CDFI shows that the thickness of the intima in NPC patients with radiotherapy is significantly thicker than that in patients without radiotherapy [6]. Consistently, the present study showed similar effects on conventional CDFI parameters.
The elastic change of the artery appears earlier after injury, and reflects the change of artery function. Generally, structural change occurs after elastic change. Because the decrease of elasticity reflects the risk of atherosclerosis, carotid elasticity testing can be used as a predictor of cerebral infarction instead of IMT measurement. In recent years, using ultrasound technology of arterial elasticity detection (vascular ET technique), we can automatically obtain the change value of the diameter of blood vessels, calculate the relevant parameters of arteriosclerosis, and quantify the endothelial dysfunction before the appearance of morphological changes. In the present study, we used this technique to quantitatively analyze the changes in carotid artery elastic function at the early stage of radiotherapy. In the past, most studies showed that carotid artery injury caused by radiotherapy usually occurs late. However, the present study showed that that the changes in elastic function occurred at the early stage of radiotherapy, before morphological changes such as arterial wall thickening and lumen stenosis. Irradiation during radiotherapy can damage the endothelial cells of the carotid artery. After the injury, the endothelial cells synthesize and secrete a large amount of platelet-derived growth factor (PDGF) and fibroblast growth factor (FGF). These factors together lead to the proliferation, differentiation, and migration of vascular smooth muscle cells. Then, interleukin-1 (IL-1) and other factors begin to mediate the interaction among various cells, leading to fibrosis of vascular smooth muscle cells and decreased elastic function. In addition, irradiation also increases the permeability of endothelial cells in carotid nutrient capillaries and venous sinuses, resulting in cell edema and hyaline degeneration, as well as cellulosic necrosis of the tube wall. These will further accelerate arterial injury. It is reported that intima changes are very obvious at 4 weeks after radiotherapy, and the changes in media and adventitia begin to appear at 12 weeks after radiotherapy [7], which is consistent with the present study.
The present study also showed that with the increase of irradiation dose, β, EP, and PWVβ, which represented arterial elasticity, showed an upward trend, while AC value showed a downward trend. This suggested that the degree of vascular wall fibrosis increased with the increased dose of radiotherapy. Of note, the parameters β, EP, PWVβ, and AC in ET technique can reliably and sensitively reflect the change in arterial elastic function, while AI is of little value. EP (kPa) and β in the carotid artery increased slightly after irradiation, but did not change significantly within 4 weeks of treatment. After Dmean reached 45.02 Gy at the 4th week, the trend began to increase significantly. At the end of irradiation, EP (kPa) and β were significantly different from those before treatment. Dosimetric results showed that the self-healing function of the carotid artery began to be significantly affected after the patients received more than 45 Gy of irradiation. Therefore, we suggest to providing corresponding clinical treatment measures to prevent the occurrence of carotid atherosclerosis in advance after the patients receive more than 45 Gy of irradiation.
Conclusions
The earliest sign of carotid artery irradiation injury is decreased elastic function. The present study demonstrates that carotid artery elastic function can be significantly affected when irradiation doses exceed 45 Gy. Therefore, we suggest administering corresponding clinical treatment measures to prevent the occurrence of carotid atherosclerosis in advance, and to improve patient quality of life. ET technique can detect changes in carotid artery elastic function at the early stage of radiotherapy, and can be used as an adjunct examination method to monitor carotid artery injury in NPC patients after radiotherapy.
References
1. Su WH, Chiu CC, Yao Shugart Y, Heterogeneity revealed through meta-analysis might link geographical differences with nasopharyngeal carcinoma incidence in Han Chinese populations: BMC Cancer, 2015; 15; 598
2. Liang H, Wang D, Che G, Evaluation of carotid artery elasticity in patients with uremia by echo tracking: J Med Ultrason (2001), 2018; 45(4); 591-96
3. You M, Zhang L, Fang L, Evaluation of carotid arterial elasticity in patients with obstructive sleep apnea hypopnea syndrome by two-dimensional speckle tracking imaging: Medicine, 2017; 96(51); e8817
4. Farr KP, Kallehauge JF, Møller DS, Inclusion of functional information from perfusion SPECT improves predictive value of dose-volume parameters in lung toxicity outcome after radiotherapy for non-small cell lung cancer: A prospective study: Radiother Oncol, 2015; 117(1); 9-16
5. Pellegrini M, Derosa S, Tannoia A, Effects of superimposed tissue weight on regional compliance of injured lungs: Respir Physiol Neurobiol, 2016; 228; 16-24
6. Zhang P, Guo R, Wang C, Echo-tracking evaluation of changes in common carotid artery wall elasticity after smoking cessation: J Clin Ultrasound, 2019; 47(3); 144-49
7. Guchhait S, Banerjee B, Anisotropic linear elastic parameter estimation using error in the constitutive equation functional: Proceedings of the Royal Society of London, 2016; 472(2192); 20160213
Figures
Tables
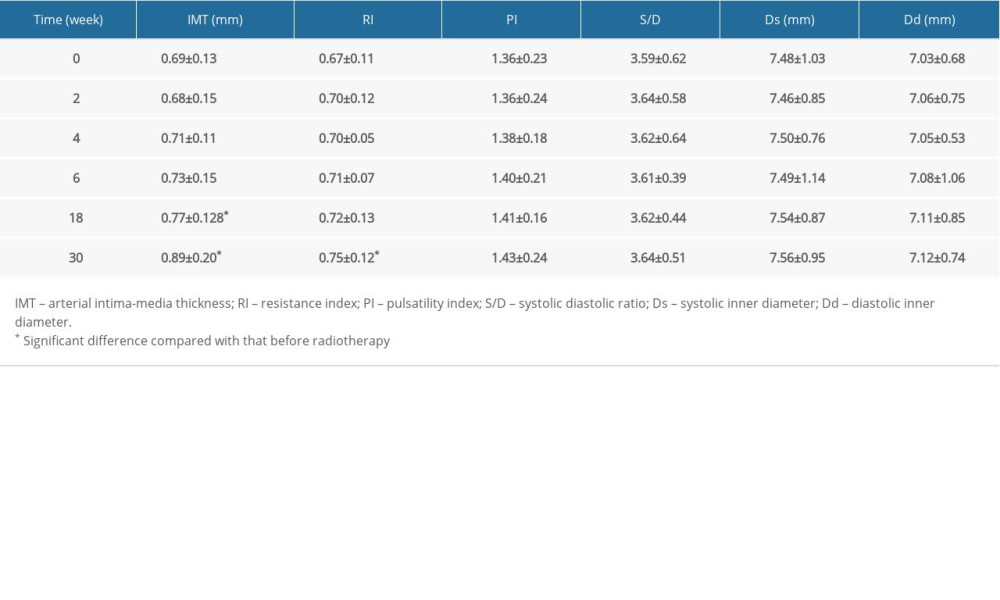 Table 1. Changes in conventional ultrasound values during radiotherapy.
Table 1. Changes in conventional ultrasound values during radiotherapy.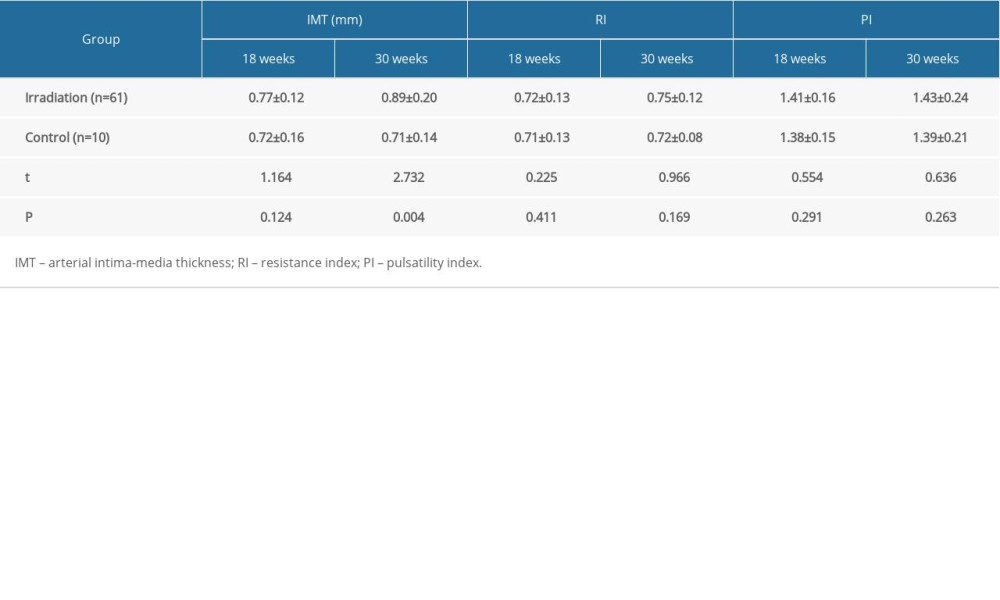 Table 2. Comparison of conventional ultrasound results between 18-week radiotherapy and 30-week radiotherapy.
Table 2. Comparison of conventional ultrasound results between 18-week radiotherapy and 30-week radiotherapy.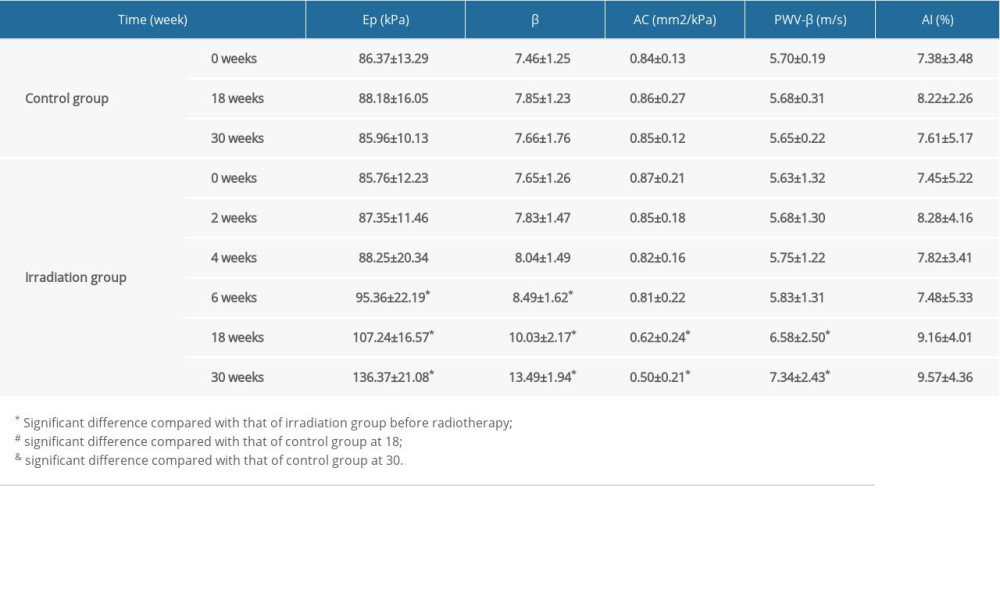 Table 3. Changes of ET ultrasound values during radiotherapy.
Table 3. Changes of ET ultrasound values during radiotherapy. Table 1. Changes in conventional ultrasound values during radiotherapy.
Table 1. Changes in conventional ultrasound values during radiotherapy. Table 2. Comparison of conventional ultrasound results between 18-week radiotherapy and 30-week radiotherapy.
Table 2. Comparison of conventional ultrasound results between 18-week radiotherapy and 30-week radiotherapy. Table 3. Changes of ET ultrasound values during radiotherapy.
Table 3. Changes of ET ultrasound values during radiotherapy. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387