22 December 2020: Clinical Research
Comparison of Outcomes Following Thyroid Isthmusectomy, Unilateral Thyroid Lobectomy, and Total Thyroidectomy in Patients with Papillary Thyroid Microcarcinoma of the Thyroid Isthmus: A Retrospective Study at a Single Center
Zhiqiang Gui1ABCDEF, Zhihong Wang1AG*, Jingzhe Xiang1C, Wei Sun1ACDG, Liang He1A, Wenwu Dong1A, Jiapeng Huang1A, Dalin Zhang1A, Chengzhou Lv1A, Yuan Qin1A, Ting Zhang1A, Liang Shao1A, Ping Zhang1A, Hao Zhang1ADOI: 10.12659/MSM.927407
Med Sci Monit 2020; 26:e927407
Abstract
BACKGROUND: Papillary thyroid microcarcinoma (PTMC) measures less than 10 mm in diameter, is more common in the thyroid lobes, but rarely presents in the thyroid isthmus. This retrospective study aimed to compare patient outcomes following various types of surgery in patients with PTMC of the thyroid isthmus, at a single center in China.
MATERIAL AND METHODS: We analyzed the clinical data of patients with isthmus thyroid cancer treated at the First Hospital of China Medical University. Patients were divided into 2 groups according to the tumor diameter-PTMC of the thyroid isthmus and papillary thyroid carcinoma >10 mm. The clinicopathological features between the 2 groups were compared, and the effects of various surgical methods on the prognosis of patients were analyzed.
RESULTS: A total of 70 patients were included in this study: 29 with PTMC of the thyroid isthmus (41.4%) and 41 with papillary thyroid carcinoma >10 mm (58.6%). The rates of lymph node metastasis (10.3% vs. 34.1%) and extrathyroid extension (0% vs. 14.6%) in the PTMC of the thyroid isthmus were significantly lower than those in the papillary thyroid carcinoma >10 mm. The recurrence-free survival (RFS) rate was 97.1%. Survival analysis showed that there was no significant difference in RFS among patients with PTMC of the thyroid isthmus undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy.
CONCLUSIONS: These findings from a single center showed that for patients with PTMC of the thyroid isthmus, who had no comorbidities, there was no significant difference in outcome between the 3 types of thyroid surgery.
Keywords: Endocrine Surgical Procedures, Thyroid Gland, Carcinoma, Papillary, Follow-Up Studies, Thyroidectomy
Background
In recent years, the incidence of differentiated thyroid carcinomas has been the fastest-growing among all thyroid malignant tumors; most of them are papillary carcinomas and most have a good prognosis [1]. Papillary thyroid microcarcinoma (PTMC) measures less than 10 mm in diameter and is more common in the thyroid lobes, but is rarely present in the thyroid isthmus [2]. The thyroid isthmus is a very thin but important band of tissue connecting the glandular lobes on both sides and is mostly located in front of the 2nd–4th tracheal cartilage rings [3]. Thyroid malignant tumors located in the isthmus are relatively rare, accounting for about 3–9.2% of all thyroid malignant tumors reported in the literature [4,5]. Because of the specificity of the tumor’s location, the choice and scope of the surgical method are controversial. The American Thyroid Association (ATA) and British Thyroid Association (BTA) have not specified the method and scope of surgery for thyroid cancer in the isthmus [6–8]. Several studies have shown that thyroid carcinoma in the isthmus is more likely to show characteristic clinical features such as multifocality, capsule invasion, extra-glandular extension, and lymph node metastasis [9–11]. In the past, radical total thyroidectomy and preventive bilateral or ipsilateral central cervical lymph node dissection were considered most appropriate [12]. Recently, with increasing understanding of thyroid cancer, the mode of operation tends to be conservative. Some studies have suggested that for low-risk, differentiated, isthmus thyroid cancer, only isthmusectomy does not affect prognosis [13–15].
Some previous studies included all patients with isthmus thyroid tumors, including those with isthmus thyroid carcinoma further complicated with carcinoma of the lobe and some patients with multiple cancers on both lobes [12,16]. Moreover, mixed with other risk factors affecting prognosis, the existence of selective bias is not enough to explain the clinicopathological characteristics of simple cancer in the thyroid isthmus. As a more special type, PTMC of the thyroid isthmus also has its own characteristics in clinical manifestations and tumor biological behavior. For this group of patients, a different treatment approach is required than for those with non-microcarcinomas. To explore the clinical features and appropriate surgical methods of PTMC of the thyroid isthmus, we analyzed the clinical data of patients with isthmus thyroid carcinoma treated in our hospital, along with their clinical and pathological features, to explore the effects of various surgical methods on prognosis. Therefore, this retrospective study aimed to compare patient outcomes following thyroid isthmusectomy, unilateral thyroid lobectomy, and total thyroidectomy in patients with PTMC of the thyroid isthmus at a single center in China.
Material and Methods
INCLUSION AND EXCLUSION CRITERIA:
In this retrospective study, the clinical data of patients with isthmus thyroid cancer treated in the First Hospital of China Medical University from January 2012 to January 2019 were analyzed. Data collected included age, sex, complication, thyroid ultrasound report, operation record, diagnosis, operation method, pathology report, and postoperative complications. The inclusion criteria were as follows: postoperative pathological examination confirming differentiated thyroid cancer; limited cancer focus and only located in the thyroid isthmus; and treatment-naïve patients with no previous surgery, ablation, and other invasive procedures. The exclusion criteria were high-risk subtypes and family history, loss to follow-up, or incomplete information. Finally, 70 patients were included in our study.
The center point of the tumor is defined as the intersection of its longest and shortest diameters. When the center point of the tumor is within the lateral border of the trachea, it is considered to be isthmus thyroid cancer in isthmus. In addition, we considered the tumor to be located in the center of the isthmus when all tumors were within the 2 lateral borders of the trachea. When the central point of the tumor was within the 2 lateral borders, but the tumor itself was beyond both borders, it was defined as the tumor located in the isthmus, but deviating to one side. According to the diameter of the tumor, patients were divided into the PTMC of the thyroid isthmus and papillary thyroid carcinoma >10 mm, and the differences in prognosis-related clinicopathological features such as age, sex, lymph node metastasis, and extrathyroid extension were compared between groups. This study was approved by the Institutional Review Board of the First Hospital of China Medical University.
FOLLOW-UP:
Postoperative follow-up was carried out by telephonic contact and looking up the review records through the electronic medical records system. We recommended oral levothyroxine replacement therapy and thyroid-stimulating hormone (TSH) inhibition therapy after surgery to all patients with thyroid cancer. According to the recommendations of the ATA guidelines, some patients were treated with radioiodine (RAI) [6]. Thyroid function was reexamined 1 month after the operation to adjust the drug dosage; thyroid ultrasound was reperformed 12 months later to exclude any residual tumor, monitor recurrence, and evaluate the next step of treatment based on the examination results.
STATISTICAL ANALYSIS:
The effects of different surgical methods on the prognosis of patients were analyzed, and the main end point was RFS. The independent
Results
PATIENTS AND TUMOR CHARACTERISTICS:
After screening, 79 patients initially met the inclusion criteria; however, 9 patients with follow-up loss and incomplete clinical data were excluded. Thus, 70 patients (7 men and 63 women [1: 9]; median age, 47 years; age range, 18–47 years) were included in the final analysis. Briefly, 54 (77.1%) patients were <55 years old, and 16 (22.9%) were ≥55 years old. All patients underwent surgical treatment: 27 (38.6%), 20 (28.6%), and 23 (32.8%) patients underwent isthmusectomy, unilateral lobectomy with isthmusectomy, and total thyroidectomy, respectively. All patients underwent prophylactic central lymph node dissection. One patient underwent modified lateral cervical lymph node dissection because of high suspicion of lateral cervical lymph node metastasis by preoperative ultrasound and enhanced CT (Table 1).
CLINICOPATHOLOGICAL FEATURES:
All 70 patients had pathologically confirmed papillary carcinoma. According to the AMES stratification system, 70 patients were stratified for risk, of which only 2 were considered to be in the high-risk group and the rest were in the low-risk group. Tumors were divided into 2 groups based on the tumor diameter: 29 cases in PTMC of the thyroid isthmus (41.4%) and 41 cases in papillary thyroid carcinoma >10 mm (58.6%). Photomicrographs of the histopathology showed a well-circumscribed PTMC measuring less than 10 mm in the thyroid isthmus showing cuboidal and columnar cells, some with nuclear inclusions and nuclear grooves, and few mitoses. Hematoxylin and eosin (H&E) ×200 staining was performed (Figure 1). The median diameter of the tumor was 11.2 mm (range: 2–24.8 mm). The tumor was located in the center of the isthmus in 31 cases and deviated to one side of the isthmus in 39 cases. Overall, 17 patients (24.3%) had pathologically confirmed central cervical lymph node metastasis, 1 patient had cervical lateral lymph node metastasis, 13 (18.6%) had prelaryngeal lymph node metastasis, 13 (18.6%) had pretracheal lymph node metastasis, and 13 (18.6%) had paratracheal lymph node metastasis. Eighteen patients (25.7%) were complicated with Hashimoto’s thyroiditis. Extrathyroid invasion was found in 6 patients, including 4 cases of strap muscle invasion, 1 case of tracheal invasion, and 1 case of recurrent laryngeal nerve invasion by metastatic lymph nodes in the central area. All the 6 patients had papillary thyroid carcinoma >10 mm. There was no case of distant metastasis in our study.
The clinicopathological features of both groups of patients were compared (Table 2). The rates of lymph node metastasis (10.3% vs. 34.1%, p=0.022) and extrathyroid extension (0% vs. 14.6%, P=0.038) in PTMC of the thyroid isthmus were significantly lower than those with papillary thyroid carcinoma >10 mm. There was no significant difference in sex (89.7% vs. 90.2%, P=1.000), age (69.0% vs. 82.9%, p=0.171), or concomitant Hashimoto’s disease (27.6% vs. 24.4%, P=0.763). There was 1 case of recurrence in each group, but this was not significant. There was no significant difference (χ2=0.868, P=0.780) in the field of lymph node metastasis between the tumor located in the center of the isthmus and that which deviated to one side of the isthmus (Table 3).
FOLLOW-UP AND PROGNOSIS:
The median follow-up of 70 patients in this group was 41.5 months (range: 7–94 months). At the time of final follow-up, 2 patients, 1 each in PTMC of the thyroid isthmus and papillary thyroid carcinoma >10 mm, had recurrence at 7 months and 37 months after the operation, respectively. Unilateral lobectomy with isthmusectomy was performed in both these patients. The sites of recurrence were all residual glands; no further surgical treatment was performed, and the patients are currently being monitored. One patient experienced temporary hypoparathyroidism after total thyroidectomy.
The overall survival rate of all included patients was 100%, and the RFS rate was 97.1%. To study the effect of different surgical procedures on the prognosis of patients in PTMC of the thyroid isthmus, we plotted the survival analysis chart to evaluate the effect of different surgical procedures on recurrence in PTMC of the thyroid isthmus. The survival analysis is shown that there was no significant difference in the RFS rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in PTMC of the thyroid isthmus (Figure 2).
Discussion
The main purpose of our study was to compare the clinicopathological features between thyroid papillary microcarcinoma and papillary thyroid carcinoma >10 mm located in isthmus, and to explore the surgical method for thyroid papillary microcarcinoma located in the isthmus. Differentiated thyroid carcinoma in the isthmus is a relatively rare cancer because of the specificity of the tumor’s location. The incidence reported in some studies is between 3.0% and 9.2% [4,5]. However, the choice of surgical methods for thyroid cancer in the isthmus and the scope of prophylactic central lymph node dissection have been the focus of debate in China and internationally. Previous studies have shown that the isthmus is an important, thin, and narrow band of tissue of connecting the glandular lobes. Tumors developing in this area can easily breach the glandular capsule, invade the anterior cervical muscle and trachea, and show the characteristics of high lymph node metastasis and multifocality [9–11]. Total thyroidectomy should be used as the standard for surgical treatment of differentiated thyroid carcinoma of the isthmus [12]. However, some scholars opine that isthmusectomy may also be suitable for low-risk differentiated thyroid carcinoma in the isthmus. For low-risk thyroid isthmus carcinoma, isthmusectomy effectively avoids injury to the recurrent laryngeal nerve and parathyroid gland and retains more gland tissues, which has the advantages of good postoperative recovery, fewer postoperative complications, and high RFS rate [17,18]. However, at present, there is no national or global consensus on the standard of treatment of differentiated thyroid cancer in the isthmus, and the latest guidelines of the ATA have not given clear recommendations on the scope of surgery [6]. However, microcarcinomas have been the focus of debate since Ito et al. suggested the idea of active surveillance in 2014. The scope of treatment for microcarcinomas also tends to be conservative [19]. Huang et al. reported that the volume of thyroid isthmus is smaller than that of bilateral glandular lobes, and the tumors located there will display neck symptoms earlier and be easy to detect in the early stage [16]. Thus, most patients are diagnosed by microcarcinomas. The question remains,
In the report by Nixon et al., tumors limited to the thyroid isthmus without extra-glandular extension can be treated with isthmusectomy or extended isthmusectomy. They found that simple isthmusectomy or extended isthmusectomy do not expose the tracheo-esophageal groove and cause less damage to the recurrent laryngeal nerve and parathyroid glands [13]. The results of Park et al. also show that isthmusectomy is an appropriate treatment option for low- or medium-risk well-differentiated thyroid cancer limited to the isthmus [14]. Lim et al. also found that there was no difference in prognosis between unilateral lobectomy with isthmusectomy and total thyroidectomy for early-stage, lymph node-negative PTMC of the thyroid isthmus [20]. This study had 29 cases of PTMC of the thyroid isthmus, accounting for 41.4% of all patients whose cancer was located in the isthmus; of these, only 3 patients had cervical lymph node metastasis and no extra-glandular invasion. The incidence of lymph node metastasis and extra-glandular invasion in PTMC of the thyroid isthmus was significantly lower than that of papillary thyroid carcinoma >10 mm. The prognosis of 29 patients was good; only 1 patient had a relapse. Unilateral lobectomy with isthmusectomy and prophylactic ipsilateral central lymph node dissection were performed in the first time. Survival analysis showed that there was no significant difference in the RFS survival rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in PTMC of the thyroid isthmus. Therefore, for low-risk PTMC of the thyroid isthmus, the mode of surgery can be relatively conservative.
Some studies have found that papillary thyroid carcinoma >10 mm is more prone to prelaryngeal and pretracheal lymph node metastasis than other types of thyroid carcinomas, which may be related to the fact that prelaryngeal lymph nodes mainly receive lymphatic reflux from the isthmus and the upper one-third of the glandular lobes. Therefore, special attention should be paid to prelaryngeal and pretracheal lymph node metastasis when carrying out preventive dissection of central lymph nodes [21]. Song et al. reported that the most common lymph node metastasis of differentiated thyroid carcinoma in the isthmus is pretracheal lymph node metastasis. Papillary thyroid carcinoma located in the isthmus has a higher rate of lymph node metastasis than papillary thyroid carcinoma located in the lobe. They suggest that bilateral central lymph node dissection should be considered in the scope of cervical lymph node dissection [22]. Wang et al. analyzed the characteristics of central lymph node metastasis in 73 patients with clinical lymph node-negative (cN0), isolated papillary thyroid carcinoma >10 mm. They reported that tumor size >0.7 cm was associated with central lymph node metastasis, while tumor size >0.6 cm was significantly correlated with paratracheal lymph node metastasis [23]. In this study, according to the ultrasound and enhanced CT images, the 70 included patients were divided into 2 groups based on whether the tumor was located in the middle of the isthmus and deviated to one side of the isthmus; lymph node metastasis was evaluated and monitored in both groups. We found that there was no significant correlation between tumor location and the metastasis of prelaryngeal lymph nodes, pretracheal lymph nodes, and paratracheal lymph nodes. Among the 70 patients in this study, 17 had central lymph node metastasis; the lymph node metastasis rate in PTMC of the thyroid isthmus was only 10.3%, which was significantly lower than that in the papillary thyroid carcinoma >10 mm group (34.1%). This indicated that microcarcinoma in the isthmus could be detected earlier and showed characteristics of early-stage disease. As only 1 patient with total thyroidectomy and bilateral central lymph nodes developed postoperative hypoparathyroidism, we suggest that the extent of prophylactic central lymph node dissection should be determined to avoid accessory injury.
This study has some limitations, including the small number of cases and short follow-up duration. This was a retrospective study at a single center that relied on the content of medical records, had a small study size, with pathology diagnosis performed by different pathologists, and surgery may have been performed by surgeons with different levels of expertise. However, we followed strict inclusion criteria, and included only patients whose tumors were limited to the isthmus of the thyroid gland. According to previous reports, the incidence of thyroid isthmus cancer is between 3.0% and 9.2%. In this study, the incidence of thyroid isthmus cancer was 0.74% and much lower than even the lower rate reported in literature, which is likely related to our strict inclusion criteria. Our results show that we can better select the mode of surgery for thyroid cancer in the isthmus by studying patients with thyroid cancer limited to the thyroid isthmus, and avoid the influence of thyroid tumors in thyroid lobes on the choice of operation.
Conclusions
The incidence of lymph node metastasis and extra-glandular invasion in PTMC of the thyroid isthmus is significantly lower than that in papillary thyroid carcinoma >10 mm. These findings from a single center showed that, for patients with PTMC of the thyroid isthmus who had no comorbidities, there was no significant difference in outcome between the 3 types of thyroid surgery. The findings support current guidelines stating that conservative surgery should be performed where possible, and, when lymph node dissection is required, this should be performed with care to preserve vital structures in the neck.
Figures
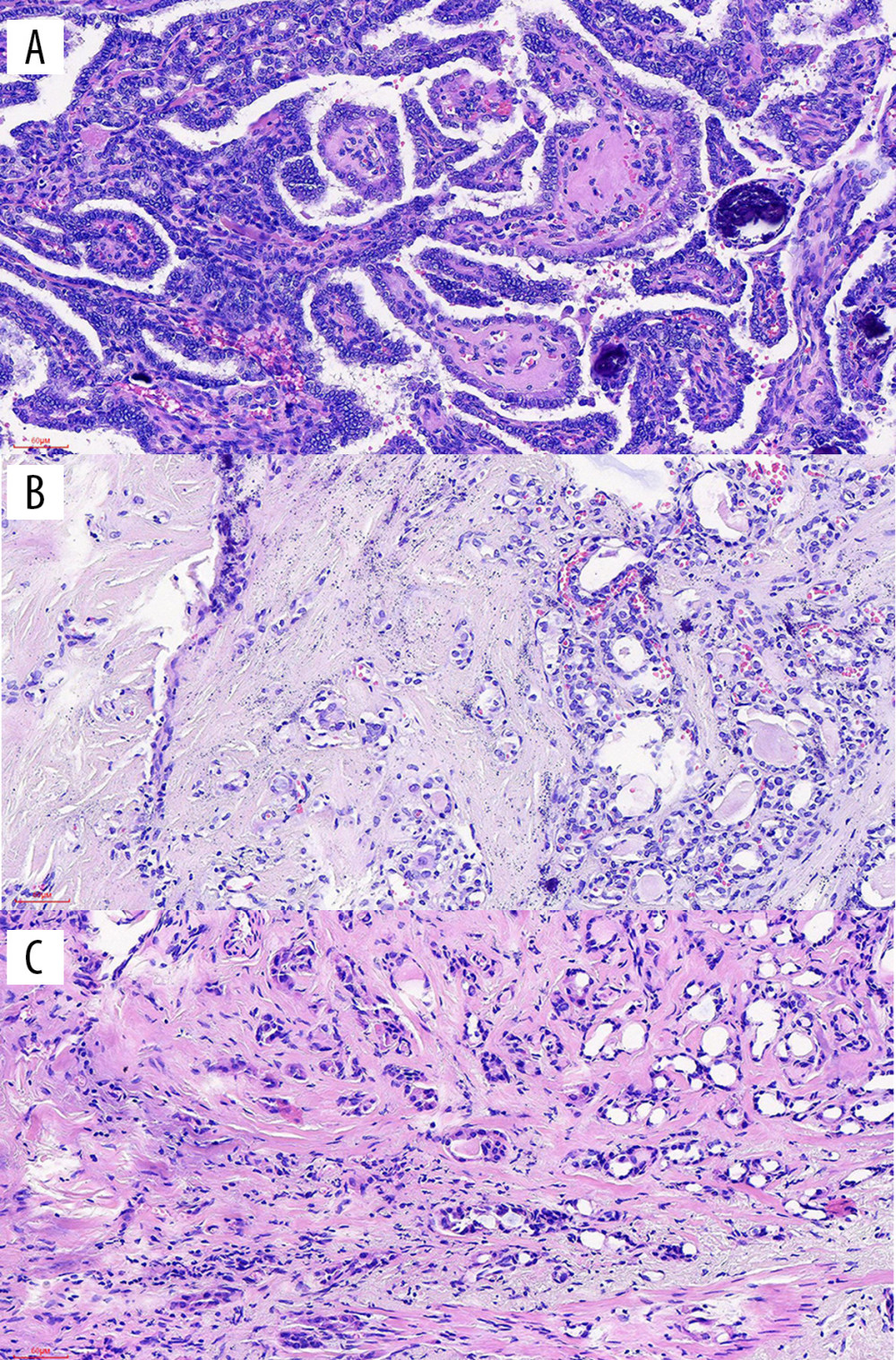 Figure 1. (A–C) Photomicrographs of the histopathology of a well-circumscribed papillary thyroid microcarcinoma (PTMC) measuring less than 10 mm in the thyroid isthmus showing cuboidal and columnar cells, some with nuclear inclusions and nuclear grooves, and few mitoses. Hematoxylin and eosin (H&E) ×200.
Figure 1. (A–C) Photomicrographs of the histopathology of a well-circumscribed papillary thyroid microcarcinoma (PTMC) measuring less than 10 mm in the thyroid isthmus showing cuboidal and columnar cells, some with nuclear inclusions and nuclear grooves, and few mitoses. Hematoxylin and eosin (H&E) ×200. 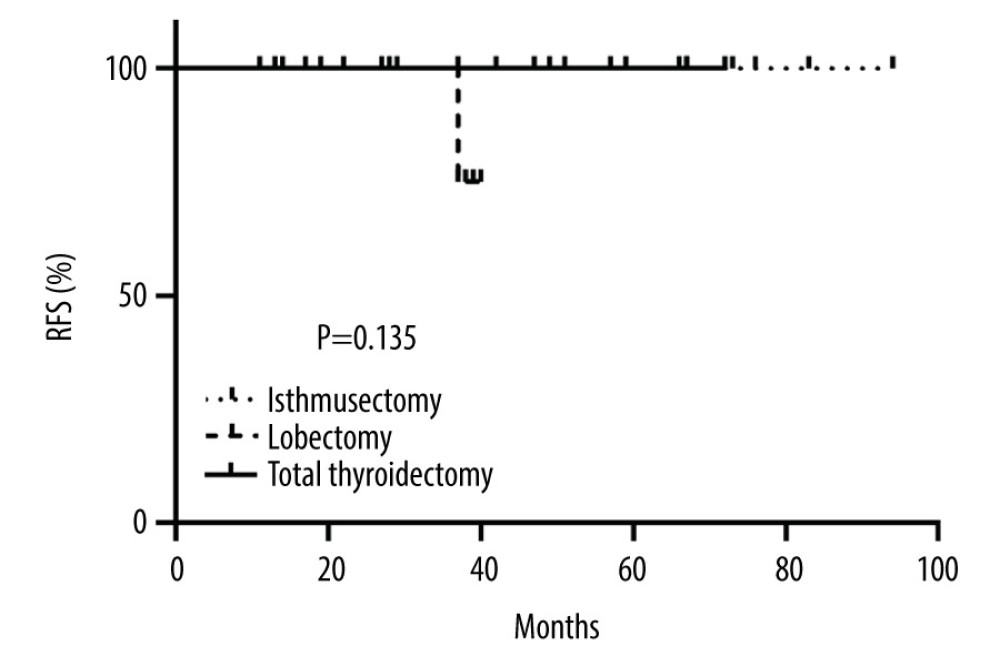 Figure 2. Kaplan-Meier survival curve of RFS for 29 PTMC of the thyroid isthmus patients. There was no significant difference in the RFS rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in the PTMC of the thyroid isthmus (P=0.135 >0.05).
Figure 2. Kaplan-Meier survival curve of RFS for 29 PTMC of the thyroid isthmus patients. There was no significant difference in the RFS rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in the PTMC of the thyroid isthmus (P=0.135 >0.05). References
1. Davies L, Welch HG, Increasing incidence of thyroid cancer in the United States, 1973–2002: JAMA, 2006; 295; 2164-67
2. Pakdaman MN, Rochon L, Gologan O, Incidence and histopathological behavior of papillary microcarcinomas: Study of 429 cases: Otolaryngol Head Neck Surg, 2008; 139; 718-22
3. Karatzas T, Charitoudis G, Vasileiadis D, Surgical treatment for dominant malignant nodules of the isthmus of the thyroid gland: A case control study: Int J Surg, 2015; 18; 64-68
4. Lee YS, Jeong JJ, Nam KH, Papillary carcinoma located in the thyroid isthmus: World J Surg, 2010; 34; 36-39
5. Sugenoya A, Shingu K, Kobayashi S, Surgical strategies for differentiated carcinoma of the thyroid isthmus: Head Neck, 1993; 15; 158-60
6. Haugen BR, Alexander EK, Bible KC, 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer: Thyroid, 2016; 26; 1-133
7. Watkinson JCBritish Thyroid Association, The British Thyroid Association guidelines for the management of thyroid cancer in adults: Nucl Med Commun, 2004; 25(9); 897-900
8. Mitchell AL, Gandhi A, Scott-Coombes D, Management of thyroid cancer: United Kingdom National Multidisciplinary Guidelines: J Laryngol Otol, 2016; 130; S150-60
9. Lee YC, Na SY, Chung H, Clinicopathologic characteristics and pattern of central lymph node metastasis in papillary thyroid cancer located in the isthmus: Laryngoscope, 2016; 126(10); 2419-21
10. Li G, Lei J, Peng Q, Jiang K, Lymph node metastasis characteristics of papillary thyroid carcinoma located in the isthmus: A single-center analysis: Medicine (Baltimore), 2017; 96; e7143
11. Goldfarb M, Rodgers SS, Lew JI, Appropriate surgical procedure for dominant thyroid nodules of the isthmus 1 cm or larger: Arch Surg, 2012; 147; 881-84
12. Lei J, Zhu J, Li Z, Surgical procedures for papillary thyroid carcinoma located in the thyroid isthmus: An intention-to-treat analysis: Onco Targets Ther, 2016; 9; 5209-16
13. Nixon IJ, Palmer FL, Whitcher MM, Thyroid isthmusectomy for well-differentiated thyroid cancer: Ann Surg Oncol, 2011; 18; 767-70
14. Park H, Harries V, McGill MR, Isthmusectomy in selected patients with well-differentiated thyroid carcinoma: Head Neck, 2020; 42; 43-49
15. Sugenoya A, Shingu K, Kobayashi S, Surgical strategies for differentiated carcinoma of the thyroid isthmus: Head Neck, 1993; 15(2); 158-60
16. Huang YQ, Wen QL, Cao JClinicopathological features of 120 cases with papillary thyroid carcinoma in isthmus: Journal of Chinese Oncology, 2018; 24(4); 308-12 [in Chinese]
17. Maser C, Donovan P, Udelsman R, Thyroid isthmusectomy: A rarely used but simple, safe, and efficacious operation: J Am Coll Surg, 2007; 204; 512-14
18. Skilbeck C, Leslie A, Simo R, Thyroid isthmusectomy: A critical appraisal: J Laryngol Otol, 2007; 121; 986-89
19. Kwon H, Jeon MJ, Kim WG, A comparison of lobectomy and total thyroidectomy in patients with papillary thyroid microcarcinoma: A retrospective individual risk factor-matched cohort study: Eur J Endocrinol, 2017; 176; 371-78
20. Lim ST, Jeon YW, Suh YJ, Correlation between surgical extent and prognosis in node-negative, early-stage papillary thyroid carcinoma originating in the isthmus: World J Surg, 2016; 40; 344-49
21. Chai YJ, Kim SJ, Choi JY, Papillary thyroid carcinoma located in the isthmus or upper third is associated with Delphian lymph node metastasis: World J Surg, 2014; 38; 1306-11
22. Song CM, Lee DW, Ji YB, Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus: Head Neck, 2016; 38(Suppl 1); E412-16
23. Wang J, Sun H, Gao L, Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients: Head Neck, 2016; 38(Suppl 1); E1510-14
Figures
 Figure 1. (A–C) Photomicrographs of the histopathology of a well-circumscribed papillary thyroid microcarcinoma (PTMC) measuring less than 10 mm in the thyroid isthmus showing cuboidal and columnar cells, some with nuclear inclusions and nuclear grooves, and few mitoses. Hematoxylin and eosin (H&E) ×200.
Figure 1. (A–C) Photomicrographs of the histopathology of a well-circumscribed papillary thyroid microcarcinoma (PTMC) measuring less than 10 mm in the thyroid isthmus showing cuboidal and columnar cells, some with nuclear inclusions and nuclear grooves, and few mitoses. Hematoxylin and eosin (H&E) ×200. Figure 2. Kaplan-Meier survival curve of RFS for 29 PTMC of the thyroid isthmus patients. There was no significant difference in the RFS rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in the PTMC of the thyroid isthmus (P=0.135 >0.05).
Figure 2. Kaplan-Meier survival curve of RFS for 29 PTMC of the thyroid isthmus patients. There was no significant difference in the RFS rate among patients undergoing isthmusectomy, unilateral lobectomy, and total thyroidectomy in the PTMC of the thyroid isthmus (P=0.135 >0.05). Tables
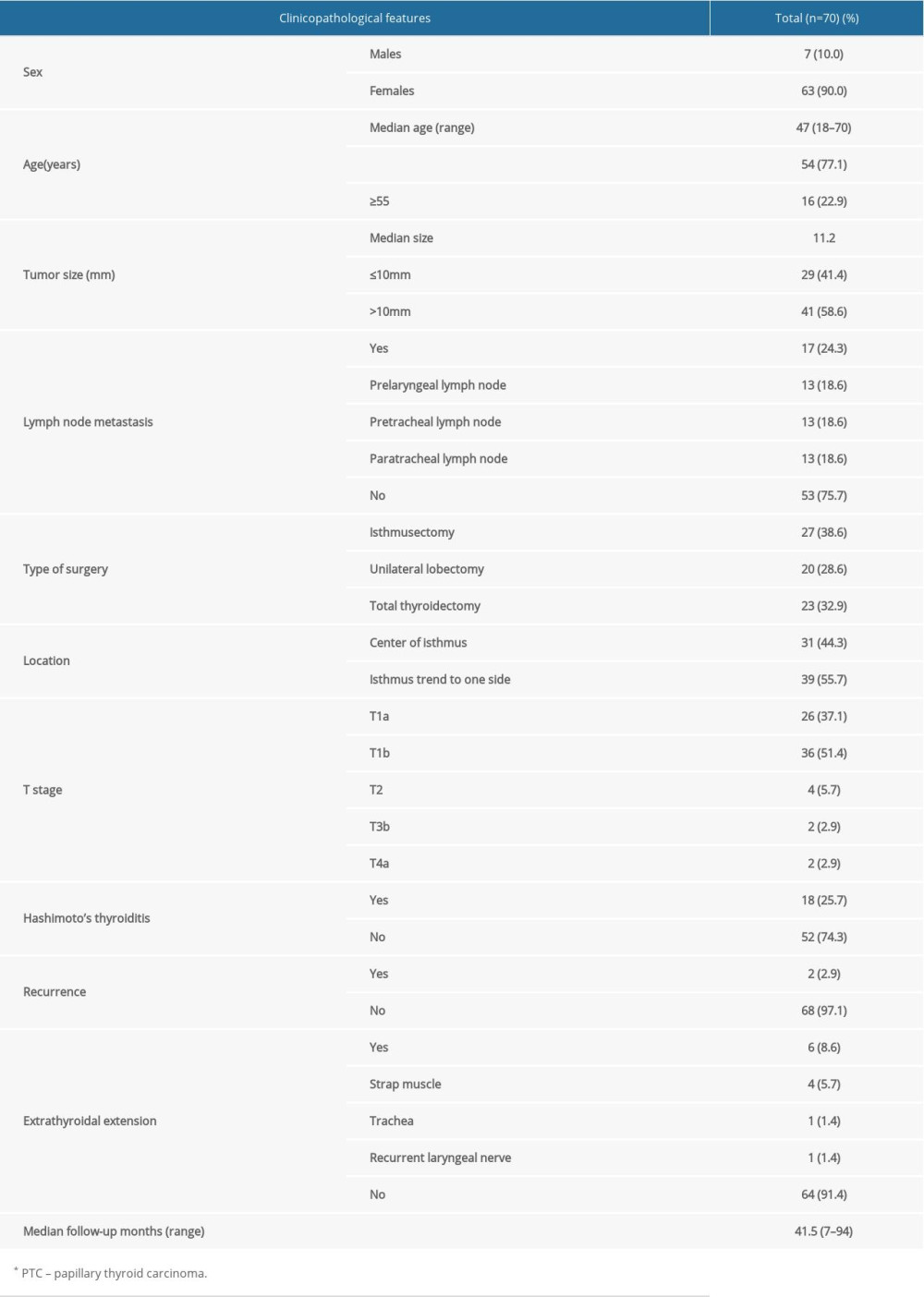 Table 1. Clinicopathological features of 70 isthmus PTC* patients.
Table 1. Clinicopathological features of 70 isthmus PTC* patients.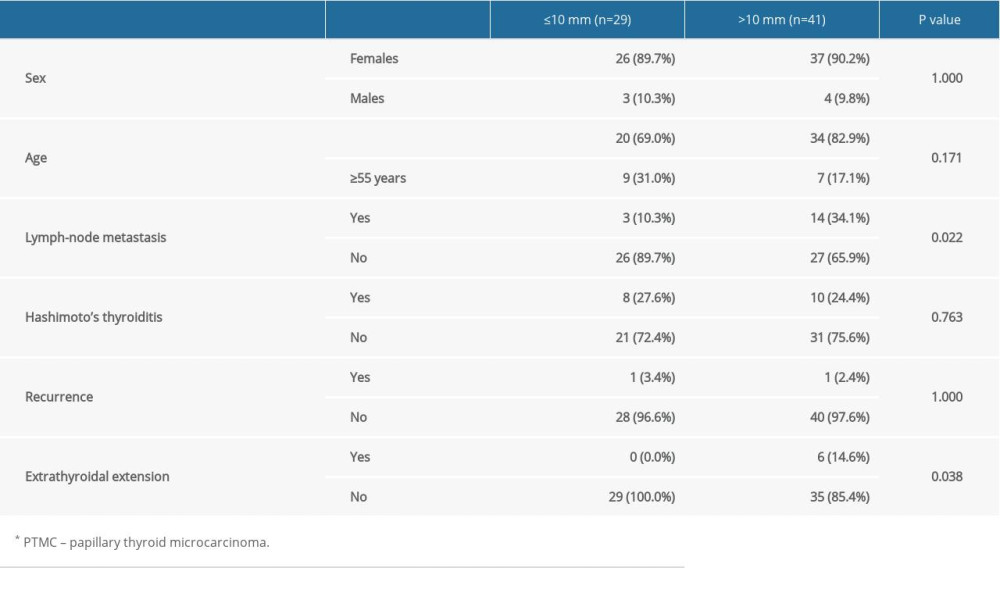 Table 2. Comparison of clinicopathological features between PTMC* of the thyroid isthmus and papillary thyroid carcinoma >10 mm.
Table 2. Comparison of clinicopathological features between PTMC* of the thyroid isthmus and papillary thyroid carcinoma >10 mm.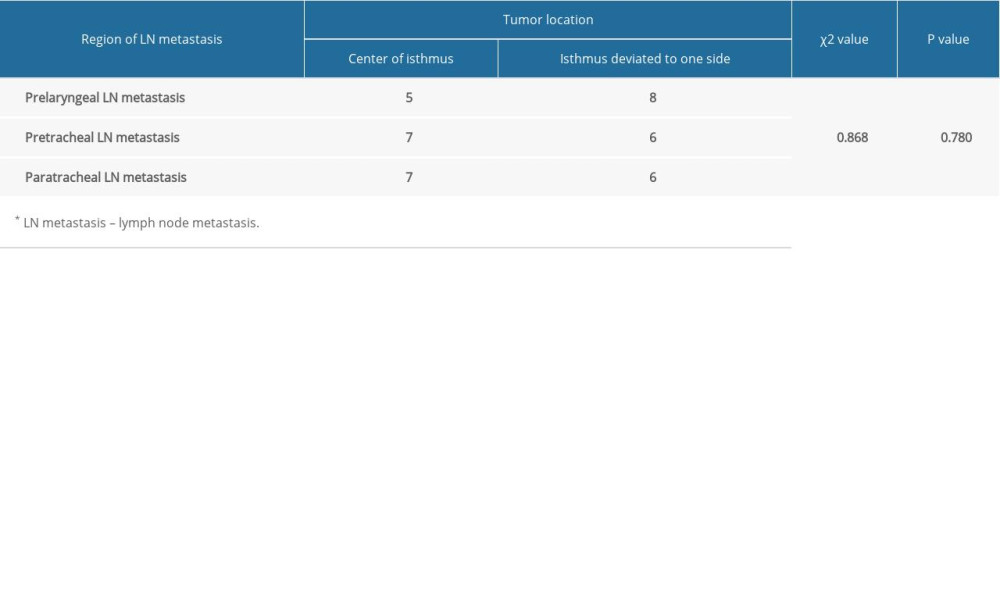 Table 3. The relationship between tumor location and the region of LN* metastasis.
Table 3. The relationship between tumor location and the region of LN* metastasis. Table 1. Clinicopathological features of 70 isthmus PTC* patients.
Table 1. Clinicopathological features of 70 isthmus PTC* patients. Table 2. Comparison of clinicopathological features between PTMC* of the thyroid isthmus and papillary thyroid carcinoma >10 mm.
Table 2. Comparison of clinicopathological features between PTMC* of the thyroid isthmus and papillary thyroid carcinoma >10 mm. Table 3. The relationship between tumor location and the region of LN* metastasis.
Table 3. The relationship between tumor location and the region of LN* metastasis. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








