22 December 2020: Clinical Research
Characteristics and Effectiveness of the Coronavirus Disease 2019 (COVID-19) Prevention and Control in a Representative City in China
Ping Liu1ABCDEFG*, Zhoujun Ma2ABCDEFG, Yu Deng3BCDEF, Yongpu Li1BCDEF, Wei Xia1BCDE, Yu Liu1BCDE, Xiaolan Wu4BCDE, Junhuan Mou4BCDEF, Quan Li5BCDE, Jianghua Nie6BCDE, Wenxiu Zhou7BCDE, Xueqin Fu7BCDE, Fei Yu8BCDE, Yan Li8BCDE, Yaling Zhang8BCDE, Qin Xiang8BCDE, Xiaobin Peng2BCDE, Guangqun Jiang2ACGDOI: 10.12659/MSM.927472
Med Sci Monit 2020; 26:e927472
Abstract
BACKGROUND: SARS-CoV-2 has caused a pandemic. Control measures differ among countries. It is necessary to assess the effectiveness of these control measures.
MATERIAL AND METHODS: We collected the data of COVID-19 patients and control measures between January 18, 2020 and September 18, 2020 from the Changshou District and analyzed the clinical characteristics, epidemiological data, and the adjustment of policies to assess the effectiveness of control measures. The control of COVID-19 was divided into 2 stages, with the lifting of lockdown in Hubei province (March 25, 2020) as a dividing line.
RESULTS: We identified 32 patients through different means in the first stage. All the imported patients entered this area before the lockdown. In 93.1% of patients, the last exposure occurred before the implementation of the stay-at-home order and centralized isolation. Tracing of high-risk people and RT-PCR screening identified 56.3% of cases. In the second stage, all the high-risk people were under centralized isolation. Nine asymptomatic patients were identified. City lockdown and stay-at-home orders were not issued again, and no second-generation patients were found.
CONCLUSIONS: We have provided a successful model to control the transmission of COVID-19 in a short period.
Keywords: asymptomatic infections, COVID-19, Epidemiology, COVID-19, Cities, Risk Factors, SARS-CoV-2
Background
Novel coronavirus disease (COVID-19) was first reported in Wuhan, China, in December 2019 and rapidly spread to more than 200 countries and areas [1–4]. The confirmed cases and deaths increased rapidly [5,6], which far exceeded those with Severe Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS) [7]. On March 11, 2020, the WHO publicly announced that COVID-19 was a pandemic [5]. COVID-19 is difficult to prevent and control because of rapid person-to-person transmission and asymptomatic transmission [1,2,8–12]. There are no vaccines or effective therapeutic drugs for the disease right now. Compared to influenza, COVID-19 has longer hospital stay and higher mortality [6,13–17]. If it is not controlled at the early stage, it may lead to exhaustion of medical resources with the increase of cases and high mortality, just like the situations in Wuhan and Italy [6–8]. The SARS outbreak that began in southern China in 2003 was eventually able to be controlled through tracing contacts of suspected cases and isolating confirmed cases because most transmissions occurred after the onset of symptoms [7]. There was evidence of transmission before noticeable symptom onset in COVID-19 patients, which reminded us that contact tracing and confirmed case isolation might be insufficient to control outbreaks, and further interventions would be required to achieve control [8–12].
China is making great progress in the fight against the pandemic, and new cases have declined in recent months. Most newly reported patients are imported [18]. Changshou District is a city subordinate to Chongqing in the southwest of China, with a population of 903 000. The control of COVID-19 was divided into 2 stages based on the lifting of restrictions in Hubei Province on March 25, 2020. The first stage was before the lifting of restrictions, and the second stage was after the lifting of restrictions. We analyzed the clinical characteristics and epidemiological data of cases, and the process of adjustment of control measures in this district to show how these measures achieved control, and to provide a reference for countries and regions with ongoing community transmission.
Material and Methods
DATA SOURCES AND DEFINITION:
We collected the medical records of patients with COVID-19 between January 18, 2020 and September 18, 2020 from Changshou District. COVID-19 was diagnosed according to the WHO interim guidance [19], and confirmed by a positive result on real-time reverse-transcriptase polymerase-chain-reaction (RT-PCR) assay according to the protocol established by the WHO and the National Health Commission of China [19,20]. RT-PCR testing was initially performed at the CDC of Changshou District. After May 1, local hospitals and commercial testing agencies were authorized to carry out the test. The clinical diagnosis was based on epidemiology, clinical symptoms, CT scan, and serological results. All treatment programs were in accordance with the guidelines formulated by the National Health Commission of China and WHO [19,20].
The patients were divided into the first-stage group and the second-stage group based on the time of confirmation. The first-generation patients were defined having Wuhan exposure history, while second-generation patients were defined as infected by first-generation patients, and so on. Close contacts were defined as having close (within 2 meters) and prolonged (generally ≥30 minutes) contact with a confirmed patient [21]. Travelers coming from Wuhan (later expanded to other selected provinces, areas, and countries experiencing COVID-19 outbreaks) and close contacts were defined as high-risk people.
We also collected data about prevention and control of COVID-19 from the Center for Disease Control and Prevention (CDC) of Changshou District and government websites, including personnel input, epidemiological survey, and control measures.
STATISTICAL ANALYSIS:
Continuous variables are expressed as medians and interquartile ranges (IQR) or average, as appropriate. Categorical variables are summarized as counts and percentages. The differences between groups were analyzed with the use of non-parametric tests. A
Results
CONTROL MEASURES AND ADJUSTMENT PROCESS:
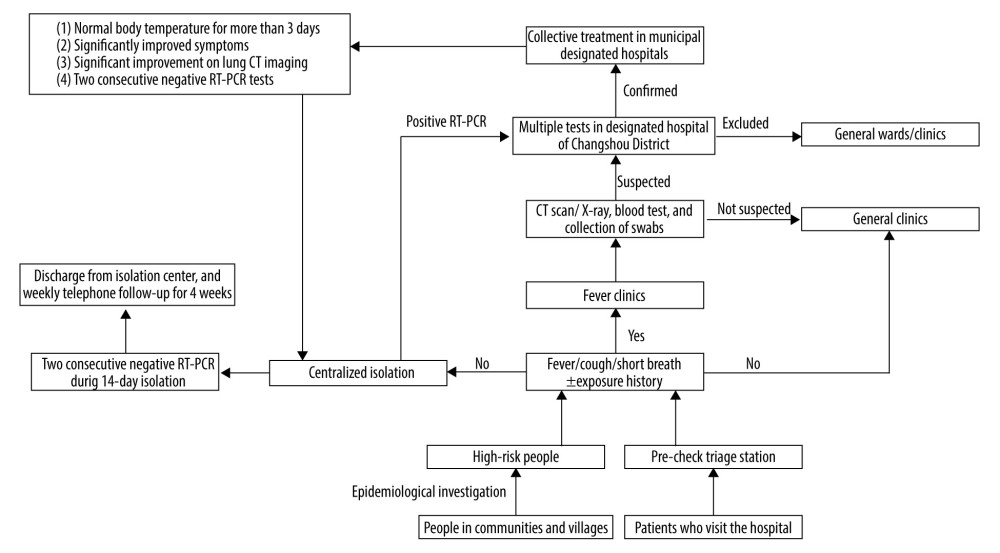
The Chongqing government activated the first-level public health emergency response on January 24, 2020, one day after the Wuhan shutdown, and formulated a series of prevention and control measures made up of 5 parts. First, city lockdowns, traffic restrictions, and stay-at-home orders were issued. Second, the government- designated hospitals and fever clinics to centralize treatment for COVID-19 patients. The work-flow is shown in Figure 1. Designated hospitals at the district level were responsible for screening and diagnosis, and designated hospitals at the municipal level were responsible for treatment. Fever clinics are the most important in the flow chart. All suspected patients had to be screened in the fever clinic. Each fever clinic was staffed with 1 doctor from the respiratory, infectious diseases, or general practice department. When the suspicious patients were younger than 14 years old or elderly with various complications, the clinicians in the fever clinic would consult with the corresponding specialists. The confirmed patients were transferred to the municipal designated hospital, where experts from various disciplines in the city were selected by Chongqing Municipal Health Commission to be responsible for the diagnosis and treatment of patients and could treat patients of all ages and with various complications. We have a multi-disciplinary team to discuss and treat the patients with negative RT-PCR but with an epidemiological history and/or typical clinical features. For these cases, retesting samples from other sites and using multiple methods (e.g., RT-PCR assay, viral gene sequence, antibody assay, chest CT scan) were encouraged to reduce the risk of misdiagnosis. Third, wearing masks, disinfection, ventilation, and body temperature monitoring were carried out in public areas such as hospitals, shopping malls, markets, airports, railway stations, and schools to slow the virus spread and identify as many potential patients as possible. Fourth, active monitoring of high-risk people and centralized isolation were widely implemented by the CDC of Changshou District. The high-risk people were transferred to designated hotels for isolation, where a group of doctors was staffed. Fifth, the scope of RT-PCR testing was expanded gradually. On January 28, 2020, Chongqing Municipal Health Commission allowed the clinicians to order RT-PCR tests based on clinical suspicion, regardless of the exposure history. On February 7, 2020, the CDC of Changshou District started to test all the high-risk people on the first day and last 3 days during their 14-day isolation period, or at any time according to the clinicians’ discretion. As the pandemic approached its end in China, the lockdown was lifted and all the people gradually returned to work and school. The cities face the possibility of a new round of virus transmission. The health code based on big data tracking has been developed to solve this problem. People are required to show the code when they travel between provinces. People from high-risk regions show the red code, and people from low-risk areas or with negative RT-PCR tests within 1 week show the green code. Those with the green code can move freely, while those with the red code need 14-day centralized isolation and tests for nucleic acid at least 2 times when they travel to another province or enter this city from outside. The RT-PCR screening gradually expanded to all the high-risk people, especially those with high-risk occupations such as medical staff, imported frozen food-related employees, and nursing staff in nursing homes, patients with fever and acute respiratory symptoms in the clinics, and all inpatients. City lockdowns, travel restrictions, and stay-at-home orders were not used in the second stage.
CLINICAL AND EPIDEMIOLOGIC CHARACTERISTICS:
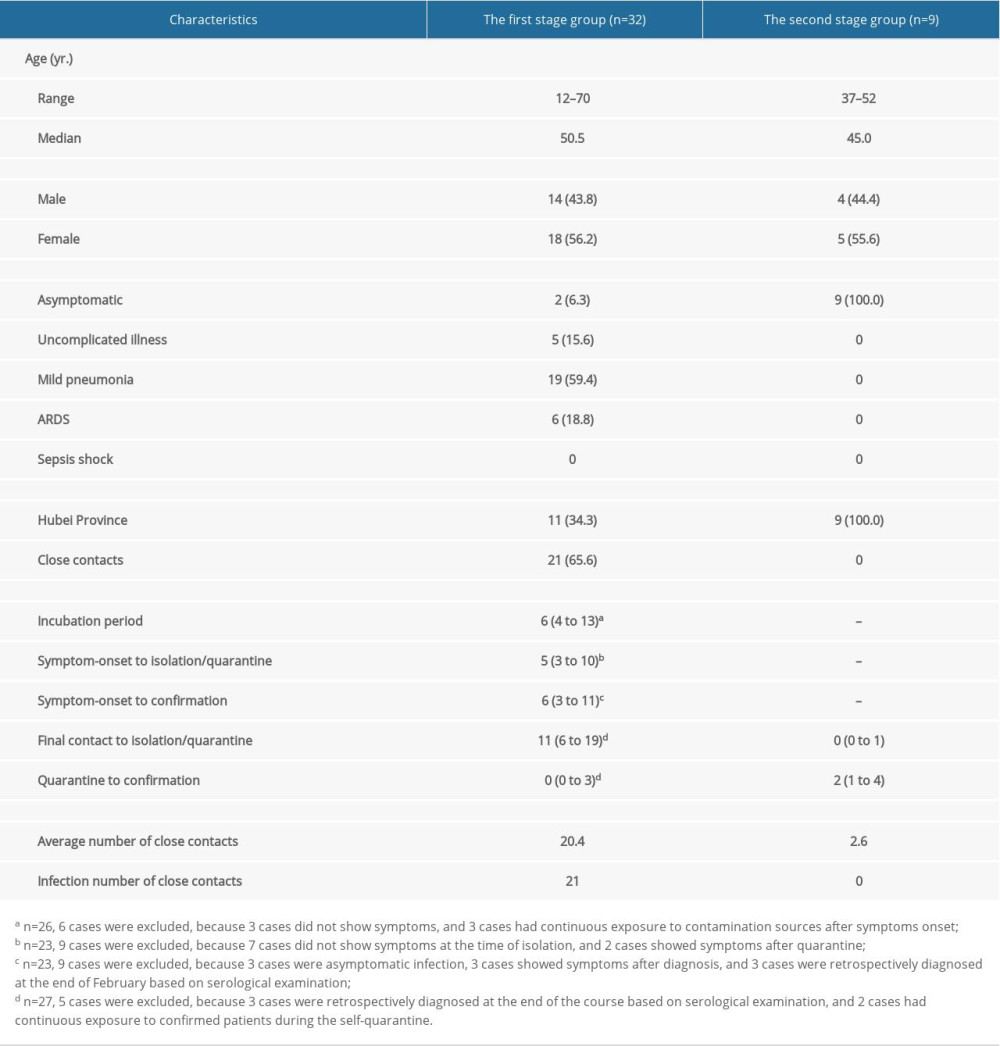
In the first stage, 32 patients were identified between January 18, 2020 and February 29, 2020. Twenty-nine patients were confirmed by positive RT-PCR tests, and 3 patients were clinical diagnosis cases, who were treated the same as the confirmed ones. Imported patients (the first generation) accounted for 34.4% (11/32) of cases. They entered this area from January 1, 2020 to January 23, 2020, the day of the Wuhan shutdown. The second and third generations accounted for 28.1% (9/32) and 37.5% (12/32) of cases, respectively. During the course of the disease, 6.3% (2/32) of cases did not show any symptoms or chest CT abnormalities. Of cases that developed into Acute Respiratory Distress Syndrome (ARDS), 78.1% (25/32) had pneumonia. Tracing of high-risk people and RT-PCR screening identified 18.8% (6/32) of cases that developed into Acute Respiratory Distress Syndrome (ARDS). Tracing of high-risk people and RT-PCR screening identified 56.3% (18/32) of cases and the ratio grew to 73.3% after February 7. Ten of the 18 cases were asymptomatic at the time of diagnosis. No intubations were needed and no deaths occurred. The last patient was discharged from the hospital on March 15, 2020 in the first stage. After 1 month without new cases, 9 imported patients were identified from April 4, 2020 to May 1, 2020 by tracing and centralized isolation of high-risk people. All were asymptomatic patients, and no second-generation cases were found. There have been no COVID-19 patients in our district for over 4 months. The demographic, clinical, and epidemiologic characteristics of the patients in the 2 stage are shown in Table 1.
In the first stage, the median duration from final contact to isolation was 11 days (IQR, 6 to 19), and the median duration from isolation to confirmation was 0 days (IQR, 0 to 3). The median duration from symptom onset to confirmation was 6 days (IQR, 3 to 11), which was shorter than that in South Korea [22]. In the second stage, all the high-risk people were required to enter centralized isolation as soon as possible. Most people were under isolation on the day they entered the district. The median duration from final contact to isolation was 0 days (IQR, 0 to 1), which was shorter than in the first stage (P<0.0001); the median duration from isolation to confirmation was 2 days (IQR, 1 to 4), which was not significantly different than in the first stages (P=0.1083).
In the first stage, 652 close contacts were traced. The average number of close contacts of confirmed patients was 20.4. Family members accounted for 40.7% of close contacts. Other common close contacts were colleagues (17.3%), neighbors (12.0%), passengers (9.9%), medical staff (5.9%), and friends (2.9%). Among all the close contacts, 15 patients were infected by family members (the highest proportion), 3 by colleagues, 2 by neighbors, 2 by friends, and 1 by a customer. Only 6.3% (2/32) of patients were infected after the implementation of the stay-at-home order and centralized isolation. There were 23 close contacts and no second-generation patients in the second stage. The average number of close contacts of confirmed patients was 2.6. Family members accounted for 47.8% of close contacts, 30.4% were colleagues, 8.7% were restaurant staff, and 4.3% were neighbors.
Over 1000 front-line health workers and community workers participated in COVID-19 patient diagnoses, screening, follow-up, and isolation in the first stage. There were 724 high-risk people under centralized isolation, and 5167 people received RT-PCR screening at isolation stations, fever clinics, and wards. In the second stage, about 300 front-line health workers participated in the control of COVID-19. Most community workers resumed their original work. Some personnel participated in the CDC monitoring and isolation of high-risk people within their jurisdiction. There were 140 high-risk people (including 44 people from Hubei province and 24 from abroad) under centralized isolation, and 37 627 people (including high-risk people, inpatients, and healthy people at their own expense) received RT-PCR screening.
Discussion
Since SARS-CoV-2 is a new virus, we did not know much about its biological behavior and pathogenicity at the beginning. The government swiftly adjusted the control measures according to the problems encountered and the deeper understanding of the virus. In the early stage of the pandemic, many patients in Wuhan were infected in the hospitals. To avoid nosocomial infection, patients with fever and/or acute respiratory symptoms were only allowed to seek medical advice in designated fever clinics and hospitals after January 24, 2020 (Figure 1). This measure ensured that there was no nosocomial infection in this district. Some patients did not have a clear COVID-19 exposure history, so they did not meet the conditions for a nucleic acid test, according to the early laboratory inspection policy, and this resulted in missed diagnoses. Clinicians were then allowed to order RT-PCR tests based on clinical suspicion, regardless of the exposure history, on January 28, 2020. Since then, no missed diagnoses of suspected patients have occurred. Asymptomatic patients were difficult to detect by self-reporting or contact tracing. An asymptomatic patient who came from Wuhan caused the largest patient cluster in the district, which also was the last cluster to be identified. To avoid this situation, all the high-risk people with or without symptoms were required to enter centralized isolation and undergo RT-PCR testing. Social distancing and self-quarantine were difficult to implement in low-income populations. People had to go to work or did not have separate rooms for self-quarantine. Few of the high-risk people in our district strictly followed the CDC instructions to take a 14-day self-quarantine at the first stage. They moved around and participated in public activities. Two patients were even infected by their family member during self-quarantine at home. The stay-at-home order and centralized isolation were implemented to solve this problem. Most close contact occurred before the implementation of the 2 measures in our district. Only 6.3% (2/32) of patients were infected after that. With strong control measures, the district temporarily controlled the outbreak within 2 months. No new cases were found in March. In the second stage, local patients were cleared and most newly-confirmed cases were imported [18]. We did not implement stay-at-home orders, traffic restrictions, or suspension of classes and work in this stage. Under the guaranty of accurate tracking of high-risk people based on big data, centralized isolation, and extensive RT-PCR screening, people could go to work and school normally.
In the first stage, when we diagnosed the first patient, COVID-19 had quietly spread in the communities for 18 days. Patients were confirmed in the emergency department, respiratory clinics, fever clinics, or by tracing high-risk people. The condition of patients ranged from asymptomatic to severe. People were in close contact with patients in different ways. In the second stage, we were actively involved in the prevention of COVID-19. All the imported patients were identified through high-risk people tracing and centralized isolation. All of them were asymptomatic infections since those with symptoms were restricted from traveling between provinces before being ruled out as infected with COVID-19 by doctors. At the beginning, when the people from high-risk areas and countries entered the district, some chose to go back home, eat something in a restaurant, or go to their companies to hand over work, before reporting to the designated hotel for isolation by themselves. This resulted in close contact with many people before isolation, such as family members, colleagues, neighbors, and restaurant employees. The patients stayed in the community for a longer time, resulting in more close contacts and more costs of prevention and control. To solve this problem, the high-risk people were sent directly to the designated hotel from the station or airport by negative-pressure emergency vehicle later. The duration from the final contact to isolation of patients in the first stage was much longer than that in the second stage.
All confirmed patients in China need to be hospitalized, and the discharge criteria are much stricter comparing to other countries (Figure 1). The asymptomatic and mild patients are important sources of infection. Home isolation is an alternative to hospitalization for them. But we did not choose this way, for 2 reasons. First, home isolation puts patients’ family members at risk. In China, most families cannot provide independent rooms and toilets for home isolation, and many cases were intra-family infections in the early stage of the outbreak in Wuhan, China [23]. Second, home isolation is unlikely to be fully effective because it cannot be strictly enforced. Our 2 cases were infected during isolation at home. Therefore, over 10 000 mild patients were admitted to fangcang shelter hospitals for centralized treatment in Wuhan, China, where medical staff could provide medical care, disease monitoring, food, shelter, and social activities [23]. When the number of cases decreases, asymptomatic and mild patients are isolated in local designated hospitals, as in our district. Although asymptomatic and mild patients do not need special treatment, centralized isolation or hospital isolation are very important for cutting off community transmission in many low-income countries when they cannot meet the conditions of home isolation. The patients cannot be discharged unless they have 2 consecutive negative RT-PCR test results according to the latest guideline of the National Health Commission of China (the 8th Edition) [24]. However, Wölfel et al. found that virus isolation success depended on high viral load and rapid isolation during the first week of symptoms from a considerable fraction of samples. No virus was isolated from samples taken after day 8, despite ongoing high viral loads [25]. This study suggested that the patient could be discharged from the hospital without being confirmed as PCR negative. Other countries and regions can adapt appropriate discharge criteria based on the latest research evidence and their sociological contexts.
Chest CT/X-ray has a high sensitivity for diagnosis of COVID-19 [26–28], the routine blood test is cheap and rapid and can distinguish between bacterial and viral infection in a certain patient, and the RT-PCR test is the standard method used to diagnose COVID-19; each patient in the fever clinic had to have these 3 tests. When we formulated prevention and control measures, the task of the fever clinic was to find suspected patients as far as possible, and the illness condition assessment was done after admission, so detection of pulse oxygen saturation (SpO2) was not included in the required measures in the fever clinic. Usually, shortness of breath and chest imaging abnormalities occur before, or in concert with, oxygen saturation drops for the patients of COVID-19, so checking the symptom of shortness of breath and chest CT scan/X-ray could reduce the risk of misdiagnosis of severe patients with low SpO2. Since SpO2 detection is simple and fast, we will add this test to the revised work-flow to screen out the severe patients more conveniently and quickly. Early detection, early isolation, early diagnosis, and early treatment could reduce the virus transmission and reduce the number of severe patients, thereby reducing mortality [29].
Joel et al. developed a stochastic transmission model and found that contact tracing and case isolation were more effective when there were fewer initial cases, lower R0, and less transmission before symptom onset, but these 2 measures alone were insufficient to control outbreaks [30]. Our findings support and expanded this model. Travel restrictions reduced the initial number of cases; stay-at-home orders and centralized isolation reduced close contacts and community transmission and so lowered the Ro; rapid and effective tracing of high-risk people and wide RT-PCR screening could find potential patients quickly, especially the asymptomatic patients, and reduced community transmission. The combination of these measures helped us to control the outbreak of COVID-19 in the first stage. Our control experience also provided another situation for this stochastic transmission model. When there were no local patients, active tracing of high-risk people and centralized isolation plus extensive RT-PCR screening measures could control the epidemic without affecting people’s normal work and lives.
There are 1.36 doctors, 2.26 nurses, and 6.04 beds per 1000 people in this district [31,32]. If extensive measures were not implemented before widespread community transmission, there might have been an exhaustion of medical resources, high mortality, and more economic losses. If COVID-19 turns into a chronic infectious disease, it will be a disastrous blow to the medical system and economic development of all countries in the world [33]. After confirming that the virus could be transmitted from person to person, the government and medical experts publicized professional popular COVID-19 knowledge for prevention and control measures by television, social media, text messages, wall newspapers, brochures, and other methods. Because of this extensive publicity about the virus, coupled with their experience from SARS in 2003, the Chinese people quickly realized the potential harm of COVID-19, so the vast majority of people supported and cooperated with the government to take strict prevention and control measures. The concept of early detection, early diagnosis, early isolation, and early treatment was widely known. We have a population of 0.9 million, only 824 km from Wuhan, Hubei province, which was the epidemic center in China, but at present we have only 41 patients, with no deaths, no hospital infection, and no medical staff infection. With the gradual control of the epidemic and the accumulation of knowledge about COVID-19, people’s desire for normal life and the worry about economic losses outweighed the panic about the pandemic. Therefore, in the second stage, the measures such as city lockdowns, traffic restrictions, and stay-at-home orders were not implemented, while the measures of centralized isolation of high-risk groups and extensive RT-PCR screening were retained. We gradually returned to work and school from March 10, 2020.
Through a detailed analysis of the measures and effectiveness of prevention and control in this region, we have provided a successful model to control the transmission of COVID-19 in a short period. However, this report has 4 limitations. First, this is a small descriptive study to evaluate the effectiveness of control measures. Second, the global infection has not reached its peak yet, so with the lifting of travel and work restrictions, this small city may face new rounds of pandemic for a long time. Whether the costs and benefits of these measures can be sustained for months or even years needs further assessment. Third, some strict control measures, such as centralized isolation of all high-risk people, may not be applicable to some countries and regions. Fourth, Changshou District is a city in the interior of China, and the generalizability of results is limited because of city scale and the small sample size. Effectiveness of the measures might vary in different climates and sociological contexts. Cities and nations with other characteristics might need to adapt and augment our measures to achieve the same level of effectiveness.
Conclusions
We implemented strong control measures, such as city lockdown, travel restrictions, stay-at-home orders, designated hospitals and fever clinics, centralized isolation, tracing of high-risk people, and extensive RT-PCR screening in the first stage to control the spread of COVID-19 within 2 months. Therefore, people’s lives gradually returned to normal. When facing the second round of virus transmission, we only performed active tracing of high-risk people based on big data, centralized isolation, and extensive RT-PCR screening measures, and successfully stopped community transmission of COVID-19 without affecting people’s normal work and lives. Our experience may serve as a reference for countries and areas with ongoing community transmission, helping them halt outbreaks or build long-term pandemic resilience.
References
1. Chan JF, Yuan S, Kok KH, A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: A study of a family cluster: Lancet, 2020; 395; 514-23
2. Li Q, Guan X, Wu P, Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia: N Engl J Med, 2020; 382; 1199-207
3. Chen N, Zhou M, Dong X, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study: Lancet, 2020; 395; 507-13
4. Huang C, Wang Y, Li X, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China: Lancet, 2020; 395; 497-506
5. World Health Organization (WHO): Rolling updates on coronavirus disease (COVID-19) https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen
6. World Health Organization (WHO): WHO Coronavirus Disease (COVID-19) Dashboard https://covid19.who.int/
7. Yang Y, Peng F, Wang R, The deadly coronaviruses: The 2003 SARS pandemic and the 2020 novel coronavirus epidemic in China: J Autoimmun, 2020; 109; 102434
8. Wu JT, Leung K, Leung GM, Nowcasting and forecasting the potential domestic and international spread of the 2019-nCoV outbreak originating in Wuhan, China: A modelling study: Lancet, 2020; 395; 689-97
9. Luo SH, Liu W, Liu ZJ, A confirmed asymptomatic carrier of 2019 novel coronavirus: Chin Med J (Engl), 2020; 133(9); 1123-25
10. Guan WJ, Ni ZY, Hu YChina Medical Treatment Expert Group for Covid-19, Clinical Characteristics of Coronavirus Disease 2019 in China: N Engl J Med, 2020; 382(18); 1708-20
11. Lai CC, Liu YH, Wang CY, Asymptomatic carrier state, acute respiratory disease, and pneumonia due to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2): Facts and myths: J Microbiol Immunol Infect, 2020; 53(3); 404-12
12. Li R, Pei S, Chen B, Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV-2): Science, 2020; 368(6490); 489-93
13. Wu Z, McGoogan JM, Characteristics of and important lessons from the Coronavirus Disease 2019 (COVID-19) outbreak in China: Summary of a report of 72 314 cases from the Chinese center for disease control and prevention: JAMA, 2020; 323(13); 1239-42
14. Ki MTask Force for 2019-nCoV, Epidemiologic characteristics of early cases with 2019 novel coronavirus (2019-nCoV) disease in Korea: Epidemiol Health, 2020; 42; e2020007
15. Akers IE, Weber R, Sax H, Influence of time to diagnosis of severe influenza on antibiotic use, length of stay, isolation precautions, and mortality: A retrospective study: Influenza Other Respir Viruses, 2017; 11; 337-44
16. Lee N, Choi KW, Chan PK, Outcomes of adults hospitalised with severe influenza: Thorax, 2010; 65; 510-15
17. American Centers for Disease Control: Disease burden of influenza http://www.cdc.gov/flu/about/burden/index.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fflu%2Fabout%2Fdisease%2Fburden.html
18. National Health Commission of China: Epidemic Bulletin http://www.nhc.gov.cn/xcs/yqtb/202004/185a308e4c66426190da0c4f2f9ab026.shtml
19. WHO: Clinical management of severe acute respiratory infection when Novel coronavirus (2019-nCoV) infection is suspected: Interim Guidance https://www.who.int/publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus-(ncov)-infection-is-suspected
20. National Health Commission of China: Novel coronavirus pneumonia prevention and control program (Fifth Edition) http://www.gov.cn/zhengce/zhengceku/2020-02/22/content_5482010.htm
21. Ng Y, Li Z, Chua YX, Evaluation of the effectiveness of surveillance and containment measures for the first 100 patients with COVID-19 in Singapore – January 2–February 29, 2020: MMWR Morb Mortal Wkly Rep, 2020; 69; 307-11
22. Peck KR, Early diagnosis and rapid isolation: Response to COVID-19 outbreak in Korea: Clin Microbiol Infect, 2020; 26(7); 805-7
23. Simiao C, Zongjiu Z, Juntao Y, Fangcang shelter hospitals: A novel concept for responding to public health emergencies: Lancet, 2020; 395; 1305-14
24. National Health Commission of China: Novel coronavirus pneumonia prevention and control program (Eighth Edition) http://www.nhc.gov.cn/yzygj/s7653p/202008/0a7bdf12bd4b46e5bd28ca7f9a7f5e5a/files/a449a3e2e2c94d9a856d5faea2ff0f94.pdf
25. Wölfel R, Corman VM, Guggemos W, Virological assessment of hospitalized patients with COVID-2019: Nature, 2020; 581(7809); 465-69
26. Xie X, Zhong Z, Zhao W, Chest CT for typical coronavirus disease 2019 (COVID-19) pneumonia: Relationship to negative RT-PCR testing: Radiology, 2020; 296(2); E41-45
27. Ai T, Yang Z, Hou H, Correlation of chest CT and RT-PCR testing for coronavirus disease 2019 (COVID-19) in China: A report of 1014 cases: Radiology, 2020; 296(2); E32-40
28. Kim H, Outbreak of novel coronavirus (COVID-19): What is the role of radiologists?: Eur Radiol, 2020; 30(6); 3266-67
29. Sun Q, Qiu H, Huang M, Lower mortality of COVID-19 by early recognition and intervention: experience from Jiangsu Province: Ann Intensive Care, 2020; 10(1); 33
30. Hellewell J, Abbott S, Gimma A, Feasibility of controlling COVID-19 outbreaks by isolation of cases and contacts: Lancet Glob Health, 2020; 8; e488-96
31. Chongqing Municipal Health Commission: Health statistics yearbook of Chongqing; Chapter 2; 27-57
32. Chongqing Municipal Health Commission: Health statistics yearbook of Chongqing; Chapter 3; 58-76
33. Ayittey FK, Ayittey MK, Chiwero NB, Economic impacts of Wuhan 2019-nCoV on China and the world: J Med Virol, 2020; 92; 473-75
In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387