29 October 2021: Clinical Research
Association of Diabetic Peripheral Neuropathy with Vitamin D Levels Depends on Vitamin D Status
Yang Ou1EF, Zhi Liang2B, Yang Yang3CD, Yi-kun Zhou1ABG*DOI: 10.12659/MSM.931244
Med Sci Monit 2021; 27:e931244
Abstract
BACKGROUND: Vitamin D deficiency has been reported to be associated with diabetic peripheral neuropathy (DPN). Our objective here was to evaluate the association between vitamin D levels and neuropathic symptoms in a Chinese population.
MATERIAL AND METHODS: A total of 4435 patients with type 2 diabetes (T2D) were recruited in this cross-sectional study. 25-dihydroxyvitamin D (25-(OH) D) serum concentration was measured by electrochemiluminescence assay (Cobas e601, Roche). DPN was clinically diagnosed by assessing neurological symptoms and performing current perception threshold (CPT) testing. Of all the patients, 2910 were CPT-positive and had assessed neurological symptoms.
RESULTS: In the vitamin D insufficiency group (<30 ng/mL 25-(OH) D), patients with neurological symptoms had higher serum 25-(OH) D levels than those without neurological symptoms (24.65±3.42 ng/mL vs 23.61±4.54 ng/mL, p≤0.001). The risk of numbness and pain increased by 0.5-fold for every 6 ng/mL increase in 25-(OH) D. In the vitamin D sufficiency group (≥30 ng/mL 25-(OH) D), patients with neurological symptoms had lower serum 25-(OH) D levels than those without neurological symptoms (32.96±3.18 ng/mL vs 33.45±4.27 ng/mL, p<0.01). For every 4 ng/mL decrease in 25-(OH) D, the risk of numbness and pain increased by 0.2-fold.
CONCLUSIONS: The association of neuropathy symptoms with 25-(OH) D levels differed depending on whether the patients had insufficient or sufficient vitamin D.
Keywords: 25-dihydroxyvitamin D, Diabetes Complications, Diabetic Neuropathies, Comorbidity, Cross-Sectional Studies, Female, Humans, Male, Risk Factors, Vitamin D, Vitamin D Deficiency, Vitamins
Background
Many disorders have been confirmed to be associated with vitamin D, such as cardiovascular diseases, metabolic syndrome, cancer, autoimmune diseases, and Alzheimer’s disease [1–3]. Vitamin D insufficiency (VDI) is common in diabetic patients [4]. Several studies have showed that adequate vitamin D intake can prevent or delay the onset of diabetes and reduce complications in diabetic patients [5–7].
Neuropathy is the most common chronic complication of diabetes; about 50% of diabetic patients have various types of neuropathies [8]. Approximately 50% of patients with diabetic neuropathy (DN) experience some degree of neuropathic pain [9]. Diabetic peripheral neuropathy (DPN) is an important cause of non-traumatic foot ulcers and amputations, and also contributes to recurrent hospitalizations, injuries, and decreased quality of life.
Although electrophysiological nerve conduction study (NCS) is the criterion standard of DPN diagnosis, it cannot detect early neurological injuries. Furthermore, NCS has some limitations in assessing DPN patients’ clinical manifestations. However, CPT can help distinguish NCS variables from clinical phenotypes according to the grade [10]. It also helps in understanding the functions of sensory fibers by evaluating the functions of Aβ, Aδ, and C from the early asymptomatic stage to the late stage of severe neuropathy [11].
The pathogenesis of DN is not fully understood thus far. Recently, studies have suggested that Vitamin D deficiency (VDD) contributes to the development of neuropathy complications [12–14]. VDD has also been shown to be an independent risk factor for DPN in a recent Chinese study [15]. The potential relationship between vitamin D levels and neuropathy warrants further study. Previous studies have mainly focused on the relation between vitamin D and DPN incidence, However, the relationship between vitamin D and neuropathic symptoms has not been well studied. Here, we aimed to evaluate the association between vitamin D levels and neuropathic symptoms in Chinese type 2 diabetes (T2D) patients with DPN from a different perspective.
Material and Methods
STUDY POPULATION AND NEUROPATHY ASSESSMENT:
This study included a total of 4435 patients with T2D hospitalized at the First People’s Hospital of Yunnan, Department of Endocrinology, during 2014–2017. Patients were diagnosed according to the 1999 World Health Organization criteria and the 2012 American Diabetes Association standards [16]. Patients with type 1 diabetes mellitus or specific types of diabetes mellitus, acute complications of diabetes, osteomalacia, history of cerebral infarction, degenerative changes in cervical vertebra, osteoporosis, parathyroid conditions including hyperparathyroidism and hypoparathyroidism, and patients receiving oral vitamin D supplements were excluded. We conducted this study in 2019 and had access to information that could identify individual participants during or after data collection. This study was approved by the Ethics Committee of the First People’s Hospital of Yunnan Province. Consent was obtained from each patient or subject after full explanation of the purpose and nature of all procedures used.
All patients underwent a neuropathic evaluation, including assessment of neurological symptoms and current perception threshold (CPT). All tests were carried out in a quiet room and performed by the same physician or technician. Positive neurological symptoms were defined as any pain, numbness, or tingling. CPT value was measured using a neurothesiometer (CPT/C, Neurotron, American). This device was applied at 2 different test sites: the right index finger and the right big toe. The test procedure used 3 different sinusoidal frequencies: 2000 Hz, 250 Hz, and 5 Hz. The stimulus was applied as a constant alternating current sinusoidal wave ranging in intensity from 0.01 mA to 9.99 mA. The measurements were selectively conducted on thick myelinated sensory nerve fibers (Aβ), fine myelinated sensory nerve fibers (Aδ), and unmyelinated sensory nerve fibers (c nerve fibers). The test results are expressed in CPT units. Normal CPT values measured at the hand were 2000 Hz 174–401, 250 Hz 26–183.5, and 5 Hz 17–104, and those measured at the toe were 2000 Hz 200–526, 250 Hz 62–211, and 5 Hz 18–173. An abnormal CPT value was defined as any value higher than the normal range. Of all the patients, 2910 were CPT-positive and clinically diagnosed as DPN according to the 2019 Expert consensus on diagnosis, treatment, and management of diabetic peripheral neuropathy in primary care [17]. Diagnostic criteria for DPN were: 1) history of diabetes mellitus (DM); 2) clinical manifestations and/or evidence of electrophysiological examination (CPT); and 3) exclusion of other causes.
DATA COLLECTION AND ANTHROPOMETRIC MEASUREMENT:
Information on sex, age, weight, height, and duration of diabetes was obtained through medical history inquiry and physical examination. Body mass index (BMI) was calculated as weight (kg) divided by height squared (m2).
2LABORATORY MEASUREMENTS AND VDI DIAGNOSIS: Blood samples were collected from an antecubital vein, and serum 25-dihydroxy vitamin D (25-(OH) D) concentration was measured by electrochemiluminescence assay (Cobas e601, Roche). VDI was defined as a serum circulating 25-(OH) D level of <30 ng/mL, and vitamin D sufficiency (VDS) as a 25-(OH) D level of ≥30 ng/mL. Patients were divided based on the presence of pain and/or numbness symptoms into a symptomatic group (SG) and an asymptomatic group (AG) (Figure 1).
STATISTICAL ANALYSIS:
SPSS v. 20.0 software was used for statistical analysis. Data are expressed as mean±standard deviation for continuous variables. Differences between the groups were analyzed using an independent-samples
Results
COMPARISON OF SYMPTOMATIC AND ASYMPTOMATIC STUDY GROUPS:
A total of 2910 people were enrolled in the study. The age, sex, diabetes duration, BMI, and 25-(OH) D levels were compared and analyzed. There were significant differences in sex, and diabetes duration between SG and AG. The SG patients had higher serum 25-(OH) D levels than AG patients (p≤0.001). A chi-square test showed significant differences according to sex and neurological symptoms (p≤0.001) (Table 1).
COMPARISON OF SYMPTOMATIC AND ASYMPTOMATIC STUDY GROUPS WITH DIFFERENT LEVELS OF 25-(OH) D:
Diabetic patients were divided into 2 groups according to 25-(OH) D levels: less than 30 ng/mL, and greater than or equal to 30 ng/mL. In the VDI group (<30 ng/mL 25-(OH) D), 1295 patients had no diabetic neurological symptoms and 566 patients had diabetic neurological symptoms. The SG patients had relatively higher serum 25-(OH) D levels than AG patients (24.65±3.42 ng/mL vs 23.61±4.54 ng/mL, p≤0.001). In contrast, the VDS group (≥30 ng/mL 25-(OH) D) showed the opposite association; the 326 SG patients had a lower 25-(OH) D level than the 728 AG patients (32.96±3.18 ng/mL vs 33.45±4.27 ng/mL, p<0.01) (Figure 2).
LOGISTIC REGRESSION ANALYSIS OF NEUROPATHIC SYMPTOM-RELATED RISK FACTORS:
There was a statistically significant difference between SG and AG in the VDI (25-(OH) D <30 ng/mL) group, so we performed further regression analysis of sex, course of disease, age, BMI, and 25-(OH) D levels. We found that in this 25-(OH) D range, the risk of neurological symptoms was higher with relatively higher 25-(OH) D levels. For every 6 ng/mL increase in 25-(OH) D, the risk of numbness and pain increased by 0.5-fold (Table 2). At the same time, we found that sex was related to neurological symptoms and women were more prone to neurological symptoms than men.
We also performed similar regression analysis in the VDS (≥30 ng/mL 25-(OH) D) group. We found that in this 25-(OH) D range, the risk of neurological symptoms was higher with relatively lower levels of 25-(OH) D. For every 4 ng/ml decrease in 25-(OH) D, the risk of numbness and pain increased by 0.2-fold (Table 3).
Discussion
In this study, we aimed to investigate the relationship between serum 25-(OH) D levels and neuropathic symptoms in T2D patients with DPN. This retrospective study revealed that the level 25-(OH) D was lower in AG patients than in SG patients. Additionally, in VDI patients (<30 ng/mL 25-(OH) D), the risk of neurological symptoms was higher with relatively higher levels of 25-(OH) D. For every 6 ng/mL increase in 25-(OH) D, the risk of numbness and pain increased by 0.5-fold. The opposite correlation was found in the VDS (≥30 ng/mL 25-(OH) D) group; the SG patients had relatively lower serum 25-(OH) D levels than AG patients. For every 4 ng/mL decrease in 25-(OH) D levels, the risk of numbness and pain increased by 0.2-fold. This suggests that relative vitamin D levels in different vitamin D states (VDI vs VDS) are reversely correlated with symptoms of diabetic neuropathy. As such, treating DPN patients with vitamin D may contribute to various degrees of diabetic peripheral neurological symptoms. These insights provide a new potential pathway for treating DPN.
Recent studies have reported that VDD is associated with the development of DPN in patients with T2D, and Asian diabetic patients with VDD are 1.22 times more likely to suffer from DPN [18]. Fan et al [19] also found that 25-(OH) D3 levels were lower in DPN and DN groups than in non-diabetic peripheral neuropathy (NDPN) and non-diabetic neuropathy (NDN) groups. VDD is an independent risk factor for DPN and DN [19].
The pathogenesis of DPN remains unclear. NGF deficiency can lead to the development of clinical diabetic small fiber neuropathy [20], and has been indicated as a potential therapeutic for peripheral neuropathies [21]. Vitamin D can promote NGF secretion. A vitamin D3 derivative was shown to induce NGF and prevent neurotrophic deficits in streptozotocin-diabetic rats [22–24]. 1,25-dihydroxyvitamin D3 regulates the synthesis of NGF in primary glial cultures [25], and vitamin D analogs have also been reported to be effective in inducing NGF in human cell lines [20,26].
There was a positive correlation reported between vitamin D and serum NGF in patients with type 1 diabetes and neuropathy recently [27]. Serum 25-(OH) D3 was inversely correlated with neuropathy, but positively correlated with NGF levels [28]. Vitamin D was deactivated by the CYP24A1 enzyme in the presence of glucotoxicity in Schwann cells, which can lead to decreased vitamin D-mediated NGF secretion [28], which can result in small nerve fiber neuropathy.
Our results in the VDS (≥30 ng/mL 25-(OH) D) group were consistent with many previous studies [18,19]. It was suggested that adequate 25-(OH) D can alleviate neurological symptoms. With the decrease of vitamin level, the cold detection threshold also was significantly reduced [29]. In addition, the decreased secretion of NGF mediated by vitamin D can also lead to small nerve fiber neuropathy [20]. Under the influence of the above factors, the lower the level of vitamin D, the more serious the symptoms of DPN.
The most unexpected finding was that the risk of diabetic neurological symptoms increased with relatively higher of vitamin D levels in the VDI group. Similarly, Abdelsadek et al found that serum levels of 25-(OH) D in patients with painless DPN were lower than in patients with painful DPN [30]. Also, the serum level of 25(OH) vitamin D had a statistically significant negative correlation with severity of DPN as regards to neuropathy disability score (NDS) and nerve conduction studies [30]. Blocking NGF activity has been to shown to have potential for normalizing neuronal hyperactivity and producing sustained clinical pain relief [31–35]. However, serum 25-(OH) D3 was positively correlated with NGF. We speculate that, in the VDI group, a slight increase in vitamin D levels led to severe symptomatic reactions because they may be more sensitive to NGF increases resulting from long-term VDI than VDS. Furthermore, vitamin D deficiency also impairs nociceptor function, worsens nerve damage, and lowers the pain threshold. As vitamin D levels increased, the risk of pain increased, and further investigation is needed to explore this. Alam et al found that high-dose intramuscular treatment with vitamin D3 improved neuropathy-specific quality of life in patients with painful diabetic neuropathy, particularly those with VDD, but did not change painful symptoms, paresthesia, loss of temperature sensation, or loss of touch sensation [36]. As vitamin D levels increased, the risk of pain increased, and more research on this is needed.
In previous studies [36–38], some subjects were DPN patients with VDI, and some studies did not group subjects according to vitamin D levels, but the proportion of DPN patients with VDD was more than 40%. Neurological symptoms were measured more than 1 week after vitamin D supplementation; however, these studies did not mention whether any of the symptoms actually worsened during the initial stage of treatment. Our results suggest that vitamin D supplementation can lead to worse diabetic peripheral neurological symptoms in diabetic peripheral neuropathy patients with VDI. Therefore, when type 2 diabetes patients are given vitamin D supplements, particularly for those with VDI, we should consider starting at lower vitamin D doses; or in the early stage of vitamin D treatment for patients with VDI, we should pay more attention to communicating with patients, informing them that pain may increase in short term, and advising them to persist in treatment for a long time.
This study also has some limitations. It was a cross-sectional study, lacking data about long-term supplementation of vitamin D in patients. Future follow-up studies should address whether supplementation with vitamin D aggravates neuropathic symptoms in patients with VDI. The effect of vitamin D supplementation on the symptoms of diabetic neuropathy should be observed after correcting the VDI. When VDI is corrected, will diabetic neurological symptoms decrease with higher levels of vitamin D?
Conclusions
Relative vitamin D levels in different vitamin D states were reversely correlated with symptoms of DPN. Relatively higher vitamin D levels are associated with neurological symptoms in VDI diabetes mellitus patients. We should consider that vitamin D supplementation may lead to increased neurological symptoms in diabetic patients with VDI; however, if VDI is corrected to sufficient levels, this risk of increased neurological symptoms may no longer exist.
Figures
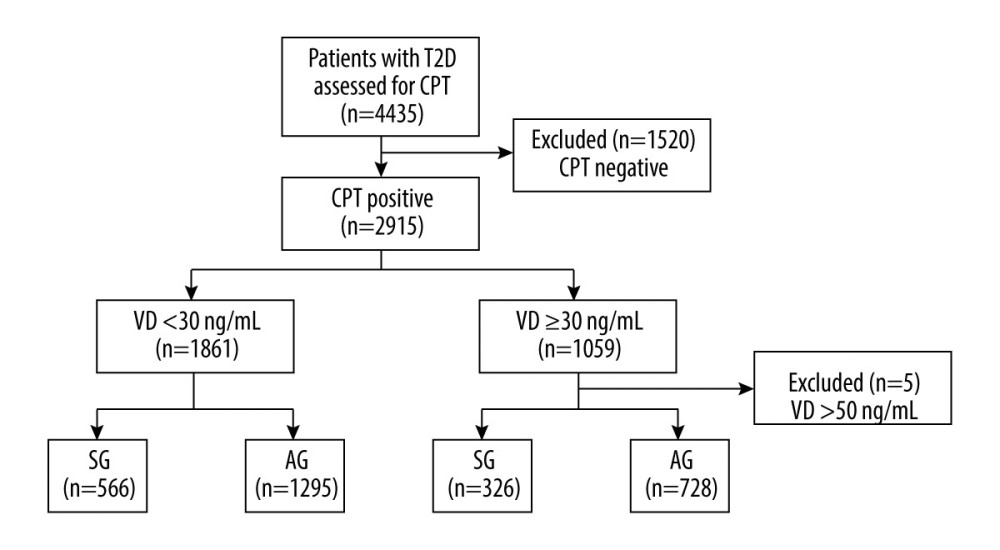 Figure 1. Flow chart.
Figure 1. Flow chart. 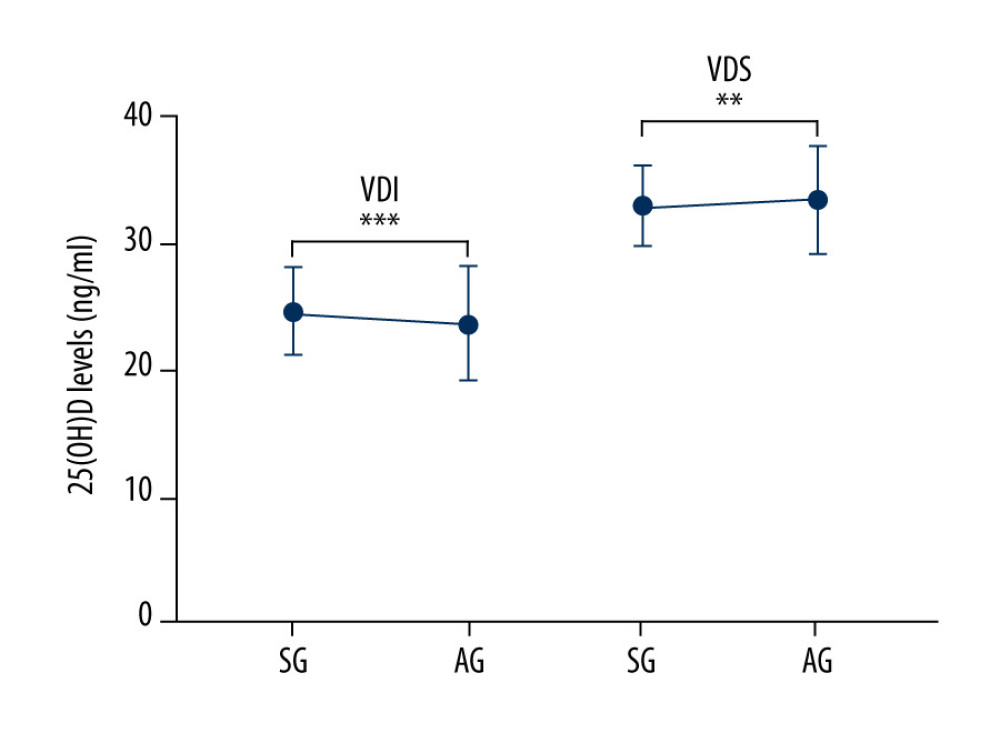 Figure 2. 25-hydroxy vitamin D levels in symptomatic and asymptomatic patients at varying states of vitamin D. Significance, *** p<0.001, ** p<0.01, VDI – vitamin D insufficiency; VDS – vitamin D sufficiency; SG – symptomatic group; AG – asymptomatic group; Figure 2 was made using Graphpad Prism 7 (GraphPad Software).
Figure 2. 25-hydroxy vitamin D levels in symptomatic and asymptomatic patients at varying states of vitamin D. Significance, *** p<0.001, ** p<0.01, VDI – vitamin D insufficiency; VDS – vitamin D sufficiency; SG – symptomatic group; AG – asymptomatic group; Figure 2 was made using Graphpad Prism 7 (GraphPad Software). Tables
Table 1. Characteristics of symptomatic and asymptomatic patients.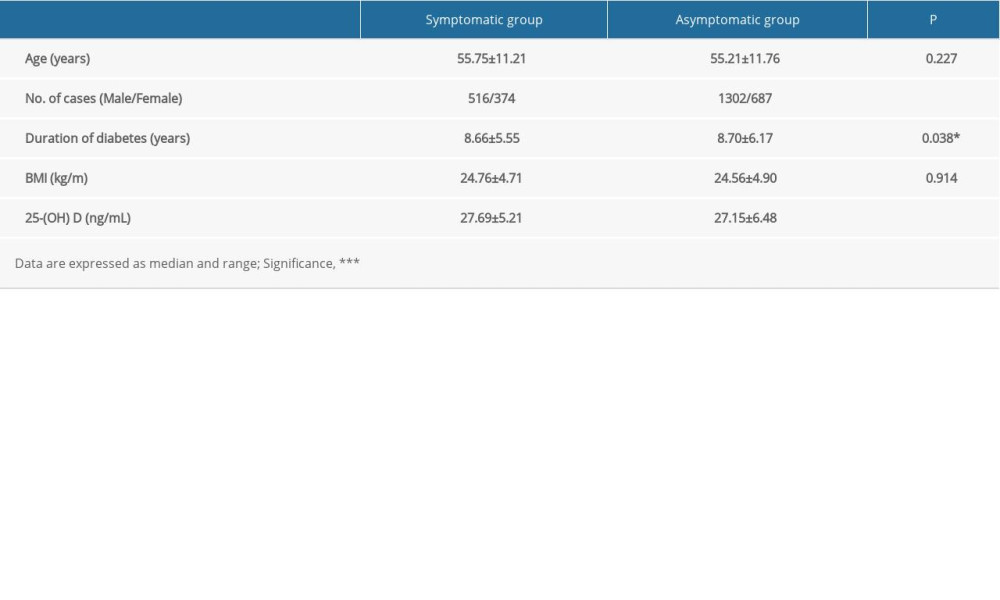 Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients.
Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients.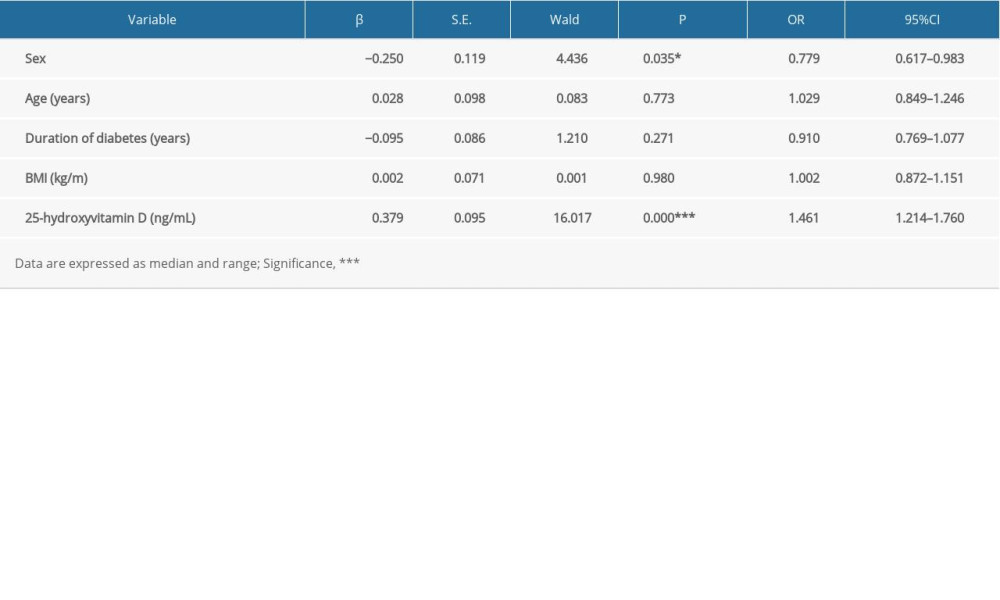 Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients.
Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients.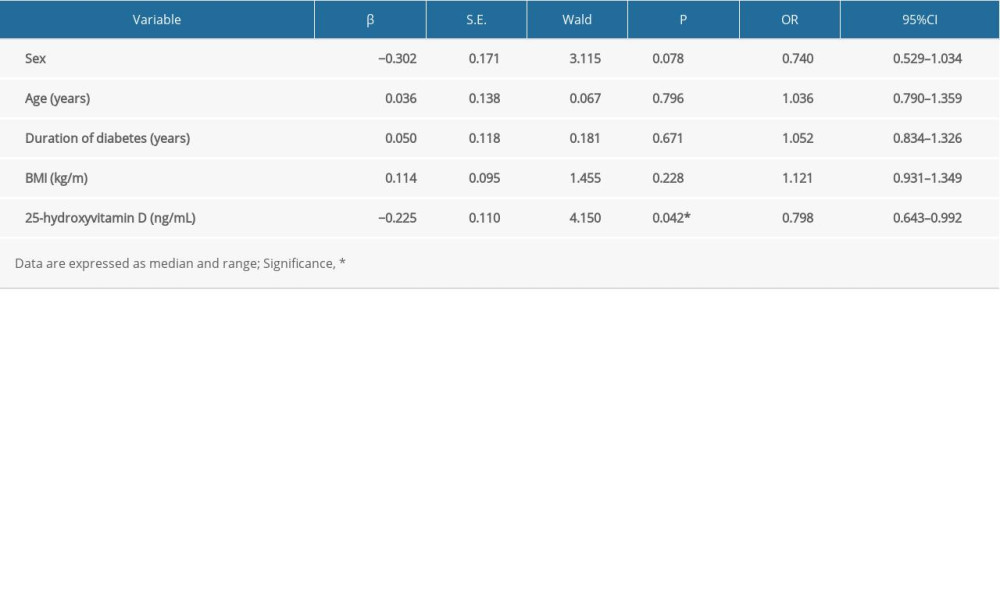
References
1. Holick MF, Vitamin D deficiency: N Engl J Med, 2007; 357(3); 266-81
2. Makariou S, Liberopoulos EN, Elisaf M, Challa A, Novel roles of vitamin D in disease: What is new in 2011?: Eur J Intern Med, 2011; 22(4); 355-62
3. Annweiler C, Dursun E, Feron F, Vitamin D and cognition in older adults: International consensus guidelines: Geriatr Psychol Neuropsychiatr Vieil, 2016; 14(3); 265-73
4. Sugden JA, Davies JI, Witham MD, Vitamin D improves endothelial function in patients with Type 2 diabetes mellitus and low vitamin D levels: Diabet Med, 2008; 25(3); 320-25
5. Pittas AG, Dawson-Hughes B, Li T, Vitamin D and calcium intake in relation to type 2 diabetes in women: Diabetes Care, 2006; 29(3); 650-66
6. Penckofer S, Kouba J, Wallis DE, Emanuele MA, Vitamin D and diabetes: Let the sunshine in: Diabetes Educ, 2008; 34(6); 939-40 944 passim
7. Danescu LG, Levy S, Levy J, Vitamin D and diabetes mellitus: Endocrine, 2009; 35(1); 11-17
8. Iqbal Z, Azmi S, Yadav R, Diabetic peripheral neuropathy: Epidemiology, diagnosis, and pharmacotherapy: Clin Ther, 2018; 40(6); 828-49
9. Argoff CE, Cole BE, Fishbain DA, Irving GA, Diabetic peripheral neuropathic pain: Clinical and quality-of-life issues: Mayo Clin Proc, 2006; 81(4 Suppl); S3-11
10. Park JH, Won JC, Patterns of nerve conduction abnormalities in patients with type 2 diabetes mellitus according to the clinical phenotype determined by the current perception threshold: Diabetes Metab J, 2018; 42(6); 519-28
11. Inceu GV, Veresiu IA, Measurement of current perception thresholds using the Neurometer((R)) – applicability in diabetic neuropathy: Clujul Med, 2015; 88(4); 449-52
12. Shehab D, Al-Jarallah K, Abdella N, Prospective evaluation of the effect of short-term oral vitamin d supplementation on peripheral neuropathy in type 2 diabetes mellitus: Med Princ Pract, 2015; 24(3); 250-56
13. Soderstrom LH, Johnson SP, Diaz VA, Mainous AG, Association between vitamin D and diabetic neuropathy in a nationally representative sample: Results from 2001–2004 NHANES: Diabet Med, 2012; 29(1); 50-55
14. Skalli S, Muller M, Pradines S, Vitamin D deficiency and peripheral diabetic neuropathy: Eur J Intern Med, 2012; 23(2); e67-68
15. He R, Hu Y, Zeng H, Vitamin D deficiency increases the risk of peripheral neuropathy in Chinese patients with type 2 diabetes: Diabetes Metab Res Rev, 2017; 33(2); dmrr.2820
16. American Diabetes Association, Standards of medical care in diabetes – 2012: Diabetes Care, 2012; 35(Suppl 1); S11-63
17. Expert consensus on diagnosis, treatment and management of diabetic peripheral neuropathy in primary care: Chinese Journal of General Practitioners, 2019; 18(6); 519-28 [in Chinese]
18. Qu GB, Wang LL, Tang X, The association between vitamin D level and diabetic peripheral neuropathy in patients with type 2 diabetes mellitus: An update systematic review and meta-analysis: J Clin Transl Endocrinol, 2017; 9; 25-31
19. Fan L, Zhang Y, Zhu J, Association of vitamin D deficiency with diabetic peripheral neuropathy and diabetic nephropathy in Tianjin, China: Asia Pac J Clin Nutr, 2018; 27(3); 599-606
20. Anand P, Terenghi G, Warner G, The role of endogenous nerve growth factor in human diabetic neuropathy: Nat Med, 1996; 2(6); 703-7
21. Apfel SC, Nerve growth factor for the treatment of diabetic neuropathy: What went wrong, what went right, and what does the future hold?: Int Rev Neurobiol, 2002; 50; 393-413
22. Riaz S, Malcangio M, Miller M, Tomlinson DR, A vitamin D(3) derivative (CB1093) induces nerve growth factor and prevents neurotrophic deficits in streptozotocin-diabetic rats: Diabetologia, 1999; 42(11); 1308-13
23. Riaz SS, Tomlinson DR, Clenbuterol stimulates neurotrophic support in streptozotocin-diabetic rats: Diabetes Obes Metab, 1999; 1(1); 43-51
24. Neveu I, Jehan F, Wion D, Alteration in the levels of 1,25-(OH)2D3 and corticosterone found in experimental diabetes reduces nerve growth factor (NGF) gene expression in vitro: Life Sci, 1992; 50(23); 1769-72
25. Neveu I, Naveilhan P, Jehan F, 1,25-dihydroxyvitamin D3 regulates the synthesis of nerve growth factor in primary cultures of glial cells: Brain Res Mol Brain Res, 1994; 24(1–4); 70-76
26. Fukuoka M, Sakurai K, Ohta T, Tacalcitol, an active vitamin D3, induces nerve growth factor production in human epidermal keratinocytes: Skin Pharmacol Appl Skin Physiol, 2001; 14(4); 226-33
27. Ozuguz U, Oruc S, Ulu MS, Does vitamin D have any role in the improvement of diabetic peripheral neuropathy in type 1 diabetic patients?: J Endocrinol Invest, 2016; 39(12); 1411-17
28. Zhou YK, Liang Z, Guo Y, High glucose upregulates CYP24A1 expression which attenuates the ability of 1,25(OH)2D3 to increase NGF secretion in a rat Schwann cell line RSC96: Mol Cell Endocrinol, 2015; 404; 75-81
29. Shillo P, Selvarajah D, Greig M, Reduced vitamin D levels in painful diabetic peripheral neuropathy: Diabet Med, 2019; 36(1); 44-51
30. Abdelsadek SE, El Saghier EO, Abdel Raheem SI, Serum 25(OH) vitamin D level and its relation to diabetic peripheral neuropathy in Egyptian patients with type 2 diabetes mellitus: Egypt J Neurol Psychiatr Neurosurg, 2018; 54(1); 36
31. Lane NE, Schnitzer TJ, Birbara CA, Tanezumab for the treatment of pain from osteoarthritis of the knee: N Engl J Med, 2010; 363(16); 1521-31
32. Schnitzer TJ, Lane NE, Birbara C, Long-term open-label study of tanezumab for moderate to severe osteoarthritic knee pain: Osteoarthritis Cartilage, 2011; 19(6); 639-46
33. Katz N, Borenstein DG, Birbara C, Efficacy and safety of tanezumab in the treatment of chronic low back pain: Pain, 2011; 152(10); 2248-58
34. Kivitz AJ, Gimbel JS, Bramson C, Efficacy and safety of tanezumab versus naproxen in the treatment of chronic low back pain: Pain, 2013; 154(7); 1009-21
35. Wild KD, Bian D, Zhu D, Antibodies to nerve growth factor reverse established tactile allodynia in rodent models of neuropathic pain without tolerance: J Pharmacol Exp Ther, 2007; 322(1); 282-87
36. Alam U, Fawwad A, Shaheen F, Improvement in neuropathy specific quality of life in patients with diabetes after vitamin D supplementation: J Diabetes Res, 2017; 2017; 7928083
37. Lee P, Chen R, Vitamin D as an analgesic for patients with type 2 diabetes and neuropathic pain: Arch Intern Med, 2008; 168(7); 771-72
38. Basit A, Basit KA, Fawwad A, Vitamin D for the treatment of painful diabetic neuropathy: BMJ Open Diabetes Res Care, 2016; 4(1); e000148
Figures
 Figure 1. Flow chart.
Figure 1. Flow chart. Figure 2. 25-hydroxy vitamin D levels in symptomatic and asymptomatic patients at varying states of vitamin D. Significance, *** p<0.001, ** p<0.01, VDI – vitamin D insufficiency; VDS – vitamin D sufficiency; SG – symptomatic group; AG – asymptomatic group; Figure 2 was made using Graphpad Prism 7 (GraphPad Software).
Figure 2. 25-hydroxy vitamin D levels in symptomatic and asymptomatic patients at varying states of vitamin D. Significance, *** p<0.001, ** p<0.01, VDI – vitamin D insufficiency; VDS – vitamin D sufficiency; SG – symptomatic group; AG – asymptomatic group; Figure 2 was made using Graphpad Prism 7 (GraphPad Software). Tables
 Table 1. Characteristics of symptomatic and asymptomatic patients.
Table 1. Characteristics of symptomatic and asymptomatic patients. Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients.
Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients. Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients.
Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients. Table 1. Characteristics of symptomatic and asymptomatic patients.
Table 1. Characteristics of symptomatic and asymptomatic patients. Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients.
Table 2. Logistic regression analysis of neuropathic symptom-related risk factors in VDI (<30 ng/mL 25-(OH) D) patients. Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients.
Table 3. Logistic regression analysis of neuropathic symptom-related risk factors in VDS (≥30 ng/mL 25-(OH) D) patients. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








