13 May 2021: Clinical Research
Ophthalmic Emergencies and Effects of Different Quarantine Models During the COVID-19 Pandemic
Berna Akova1ABCDEFG*, Sertaç Argun Kıvanç1ABCDEFGDOI: 10.12659/MSM.931967
Med Sci Monit 2021; 27:e931967
Abstract
BACKGROUND: The aim of this study was to evaluate the epidemiological features of the patients admitted to our emergency department (ED) during the COVID-19 pandemic in March, April, and May 2020, compare them with the patients in March, April, and May 2019, and to investigate the effect of various quarantine models.
MATERIAL AND METHODS: The records of 1206 eligible patients were reviewed. Age groups were divided according to their quarantine status. We recorded the reasons for patient presentation to the ED, the average number of patients in age groups according to quarantine days, and the problems reported by patients who presented to the ED according to quarantine days.
RESULTS: We enrolled 3016 of 3123 patients. The mean age was 36.4±17.3 years in 2019 and 37.8±16.4 years during the pandemic period (P=0.031). While 73.1% of the ED presentations were due to ocular trauma in 2019, it decreased to 70.7% in 2020. The proportion of those who presented to the ED during the weekend was 30.6% in 2019, but decreased to 23.9% in 2020 (<0.001). While 84.8% of trauma patients were ages 19-64 years in 2019, this rate increased to 88.9% during the pandemic (P=0.067). Non-trauma emergencies were more common than trauma emergencies in both periods in those over the age of 65 years. During the pandemic period, admissions to the ED were decreased in the quarantined age groups (P=0.001).
CONCLUSIONS: The changes in the number and characteristic of admissions for ophthalmic emergencies during the pandemic period may help planning allocation of healthcare personnel and resources in outpatient and emergency clinics.
Keywords: Coronavirus, COVID-19, Emergencies, Adolescent, COVID-19, Emergency Service, Hospital, Ophthalmology, Pandemics, Quarantine, young adult
Background
Coronavirus is one of the pathogens known to infect humans. It previously caused fatal respiratory system infections with MERS-CoV and SARS-CoV [1]. The new SARS-CoV-2, which emerged for the first time in Wuhan province China at the beginning of 2020, has caused a pandemic all over the world and, to date, more than 53 million people have been infected in 220 countries, according to the World Health Organization. During this pandemic, the lack of intensive care facilities and personal protective equipment has emerged all over the world [2–5]. However, due to the insufficient numbers of test kits and their low sensitivity, it was difficult to detect infection [6]. Therefore, health authorities of many countries decided to stop performing elective surgeries and providing routine outpatient services [7–9]. In addition to ceasing to perform elective surgeries, the Ministry of Health in Turkey also decided to perform only emergency surgeries and cancer surgeries. During this period, ophthalmology clinics in pandemic hospitals stopped routine patient admission and generally dealt only with emergency cases. During the pandemic period, many countries in the world have used different approaches. While some countries implemented a complete quarantine, others did not implement any special policies. From March, in which the first cases emerged, until the beginning of June in Turkey, only people 18 years old and under and those 65 years old and over were completely quarantined. The individuals between 19 and 64 years old had a full quarantine at weekends. In accordance with the rotational work policies of the workplaces, they worked rotationally during weekdays.
This study aims to investigate the effects of the pandemic and the related regulations on people with ophthalmic emergencies who presented to the ED of the tertiary reference hospital of Bursa Uludağ University, School of Medicine in Bursa with regard to the age groups, pandemic periods, and quarantine periods.
Material and Methods
GROUPS INCLUDED IN THE STUDY:
The subjects were separated into 3 age groups in terms of the quarantine status: 18 years and under, 19–64 years old, and 65 years and over. The full quarantine group consisted of patients aged 18 and under and 65 and over; the less-quarantined group consisted of the patients ages 19–64 years.
The groups were further divided into 5 subgroups, with 2 groups in 2019 and 3 groups in 2020. The year before the pandemic, the March, April, and May 2019 period was divided into 2 groups as weekdays and weekends. In the pandemic year (2020) in March, as the subjects 18 years age and under and 65 years and over were quarantined, weekdays in March were delineated as semi-quarantine weekdays group, and weekends in March were considered as semi-quarantine weekends group. In April and May 2020, weekdays were considered as semi-quarantine weekdays, while weekends and officially quarantined days for all age groups were considered full quarantine. Since quarantine was not applied to all groups on the last weekend of May, it was considered as a semi-quarantine weekend, like weekends in March. The groups are listed in Table 1.
STATISTICAL ANALYSIS:
SPSS 23 program (©IBM, International Business Machine, Armonk, NY, USA) was used for data analysis. The normality of distribution was determined by the one-sample Kolmogorov-Smirnov test. Descriptive statistical methods were used for demographic data. The Pearson chi-square test was used for comparison of age groups, patient-reported problems at time of presentation to the ED, and ED presentation times. The Kruskal-Wallis test was used for statistical comparison of the average number of patients admitted according to quarantine periods. The
Results
After detection of the first coronavirus case in March 2020, when the quarantine measures were implemented during the COVID-19 pandemic, the ED presentations of ophthalmic emergency patients were retrospectively compared with the presentations of the same months of the year before. We enrolled 3016 of 3123 patients in the study. While the number of presentations to the ED was 1855 in 2019, this number was 1161 in 2020, which was 37.4% lower. The mean age of patients who applied during the pandemic was 37.8±16.4 years, while the mean age of the patients who applied in same time interval in 2019 was 36.4±17.4 years. The groups were significantly different with respect to mean age (
From March to May, when the quarantine was actively applied, there was a decrease in the number of ophthalmologic emergency presentations in 2020 compared to the previous year. We compared the total number of patients in each month in 2019 vs 2020 (chi-square test). While the ED presentation rates were 37% (678 patients) in March, 29% (544 patients) in April, and 34% (633 patients) in May in 2019, the rates were 40% (465 patients) in March, 24% (283 patients) in April, and 36% (413 patients) in May in 2020. The change in distribution of the ED presentation rates was statistically significant (
Within the scope of pandemic measures, a curfew was imposed on individuals aged 18 and under and 65 and over on weekdays, and a curfew was imposed on all individuals on weekends. During the pandemic period, at the weekends when quarantine was implemented in all ages, a decrease was noted in the ED presentation rates at the weekend. When all ED presentations were evaluated, the weekend ED presentation rate was 30.6% in 2019, while it was 23.9% in 2020. This difference was significant between 2019 and 2020 (
The rate of ophthalmic ED presentation decreased in 2020 compared to 2019 in the groups aged 18 and under and 65 and over, who were permanently quarantined (
The rates of various reported eye problems among people presenting to the ED for ophthalmic diseases in both periods are given in Table 3. Ocular trauma was the most common problem in both periods in all age groups.
In 2019, 84.8% of ocular trauma cases were observed in the 19–64 age group, while this rate increased to 88.9% during the pandemic period (
In patients who were quarantined (<18 and >65 years), admission with ocular trauma was 15% in previous year, while this rate decreased significantly to 11% during the pandemic (
In 2019 and 2020, the most common cause of ophthalmic emergencies was ocular trauma followed by ocular infection in 2019 and followed by pain-stinging-burning problems in 2020 (Table 3).
While the patient concerns of pain-stinging-burning in the quarantine group accounted for 29% of the ED presentations in 2019, this rate decreased to 22% during the pandemic period (
While the ED presentation rate due to ocular infection was 39% before the pandemic in patients in the quarantine group, it decreased to 30% during the pandemic period, which was not statistically significant. Also, no significant difference was noted between 2019 and 2020 in the patients who constituted the quarantine group in terms of sudden vision loss and other problems (eg, diplopia, glaucoma, uveitis, flashing lights).
According to the quarantine days, the average daily number of patients presenting due to ophthalmic emergencies in different age groups is given in Table 4. The average daily number of patients was 20.6±4.9 patients in 2019 and 12.9±5.3 in 2020. Table 5 shows the average daily number of patients applying due to eye diseases and the average number of patients with different ED presentation problems according to the quarantine days.
Discussion
During extraordinary periods in our world, admissions to hospitals may increase and decrease. The coronavirus pandemic period, which started at the end of 2019 and continued throughout 2020, is such a period.
Wu et al investigated ophthalmic emergency admissions in 2020, when the pandemic started and stay-at-home measures were implemented. They compared the findings with the previous year and found that that the average number of patients per day decreased significantly from 49.0 to 36.4 [10]. A significant decrease was reported in the number of patients presenting for ophthalmic emergency during stay-at-home measures, and the incidence of ocular traumas were stable. Severe ocular trauma was noted in 87 (6.3%) of 1372 patients in 2019 and in 62 (5.9%) of 1058 patients in 2020. When the severe ocular trauma types were compared with those of the previous year, the difference was not statistically significant [10]. They evaluated a 1-month period between March 23 and April 20, while we evaluated a 3-month period. We also evaluated the days with a compulsory quarantine period. In our study, there was a decrease in the number of emergency visits during the pandemic regarding the number of ophthalmologic emergency patient admissions in March to May, when the stay-at-home measures were actively applied, compared to March to May in 2019. While the average daily number of ophthalmic emergency presentations was 20.6 in 2019, we observed that this number decreased to 12.9 during the pandemic period. The rate of ophthalmic emergency presentation decreased from 20% in 2019 to 15% in 2020, which is statistically significant, compared to the previous period in the age groups 18 and under and 65 and over, who were in continuous quarantine. Ocular trauma was the most frequent cause for presentation in both time periods. Ocular trauma constituted 73.1% of the ED presentations in 2019 and 70.7% in 2020. We think that the number of trauma presentations is high because our region is an organized industrial zone and we are the only reference tertiary hospital in the region.
A study conducted by Shah et al assessed and compared the frequency of pediatric ocular trauma in ophthalmological emergencies during the pandemic from March 22 to May 30 in 2020 found that the incidence of pediatric ocular trauma increased during the interval when quarantine measures were implemented [11]. In another study, Pellegrini et al observed 354 eye injuries (15.6% of emergency admissions) in 2019 between March 10 and April 10, while 112 eye injuries (19.9% of all ED presentations) were noted in the same interval in 2020. They found that during quarantine, the proportion of children and adolescents with ocular injuries decreased (from 14.7% to 8.0%) and that the proportion of men increased (from 66.7% to 75.0%). They showed a dramatic reduction in eye injuries (68.4%) during the pandemic period, and predicted that behavioral changes at the time of quarantine would decrease the risk of trauma. They stated that the decrease in sports injuries and injuries in children during school closure supports this hypothesis [12]. Similar to the findings of Pellegrini et al, we also found a significant reduction in eye injuries in patients under 18 years and patients over 65 years. However, there was no significant change regarding ED presentation for ocular trauma in the patients aged 19–64 years, who were not in continuous quarantine. As the outdoor activities of patients under 18 years and over 65 years were restricted due to quarantine, the rate of ocular trauma in these age groups might have decreased. The rate of ocular trauma in the patients age 19–64 years did not significantly change. This finding may be attributed to their relatively unrestricted activities and possible domestic violence.
In the present study, 3016 patients were enrolled and the data were compared over a 3-month interval. We observed that 14% of the ED presentations before the pandemic were in the pediatric group, and this rate decreased to 9% during the pandemic period. In a recent study that compared a COVID-free period with the COVID period, the ED presentations of patients under 18 years also significantly decreased during the COVID period [13].
A study by D’Oria et al, while validating a new scoring system for the ophthalmic emergency room, reviewed electronic records of 953 patients who visited between April 1, 2018, and May 30, 2018. During the 2-month period, according to their triage score system, 606 of 953 patients who aplied to ophthalmic emergency room were classified as non-urgent and 347 were urgent. According to their findings, approximately 36% of the patients did not need to be evaluated at the ophthalmic emergency room [14]. In our study, 1161 patients applied to the ED in the 3-month period in 2020 vs 1855 in 2019. There was a marked decrease in ED presentations when the curfew was applied during the pandemic. This may be attributed to the fact that non-urgent cases might have not applied to the ED during the pandemic and some urgent cases might have hesitated to apply due to concern of possible COVID-19 transmission.
Poyser et al reported an overall 53% reduction in emergency eye department attendance during the lockdown period. They compared a 1-month period (March 24, 2020 to April 23, 2020) during the pandemic with the same period in 2019. They also reported a 46% reduction in trauma-related presentations during the lockdown period [15]. In our study, the overall reduction rate was 37.4%. In addition, 2019 was divided into 2 groups as weekdays and weekends, and 2020 as semi-quarantine weekday, semi-quarantine weekend, and full quarantine. In the period 2020, the distribution of the average number of patients was in accordance with the groups, taking into account that the group aged 18 and under and 65 and over were in quarantine. The average number of patients daily, and the number of patients who applied for trauma, infection, pain/burning/stinging, or sudden vision loss decreased significantly, while the change in the average number of patients admitted for other causes was not significant.
An important limitation of this study is that it analyzed the ophthalmic emergency presentations at a single tertiary hospital. The tertiary hospital of Bursa Uludağ University was the only center in the region that did not stop the admission of patients with ophthalmic emergencies and symptoms; all the other hospitals had all stopped giving medical care to ophthalmic patients at times during the pandemic. This fact might have affected the number of ED presentations. The strength of this study is that it evaluated the ophthalmic emergency presentations in different quarantine models in different age groups.
Conclusions
To the best of our knowledge, this simple preliminary study is the first to assess changes in the number and characteristic of admission for ophthalmic emergencies during the pandemic period. Further and more complex studies should be conducted in different countries to develop better organization models and to determine the number of health care personnel required in ophthalmology departments. The role of territorial medicine is also very important to treat emergencies initially and to reduce the number of patients who have to go to large, central hospitals.
Tables
Table 1. The patient groups included in the study in March, April, and May 2019 and 2020.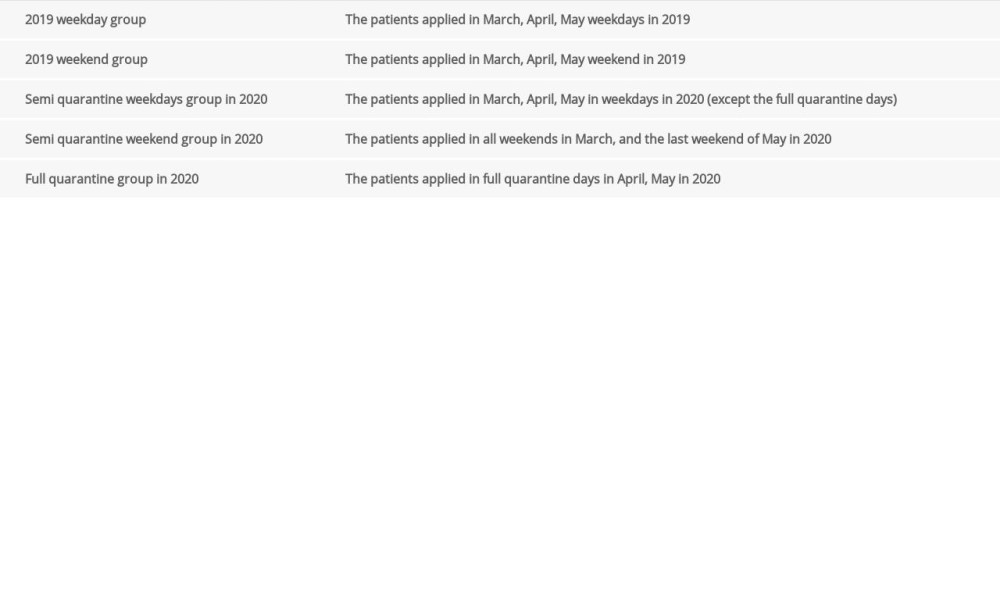 Table 2. The distribution of ophthalmic emergency presentations of different age groups in March, April, and May 2019 vs 2020.
Table 2. The distribution of ophthalmic emergency presentations of different age groups in March, April, and May 2019 vs 2020.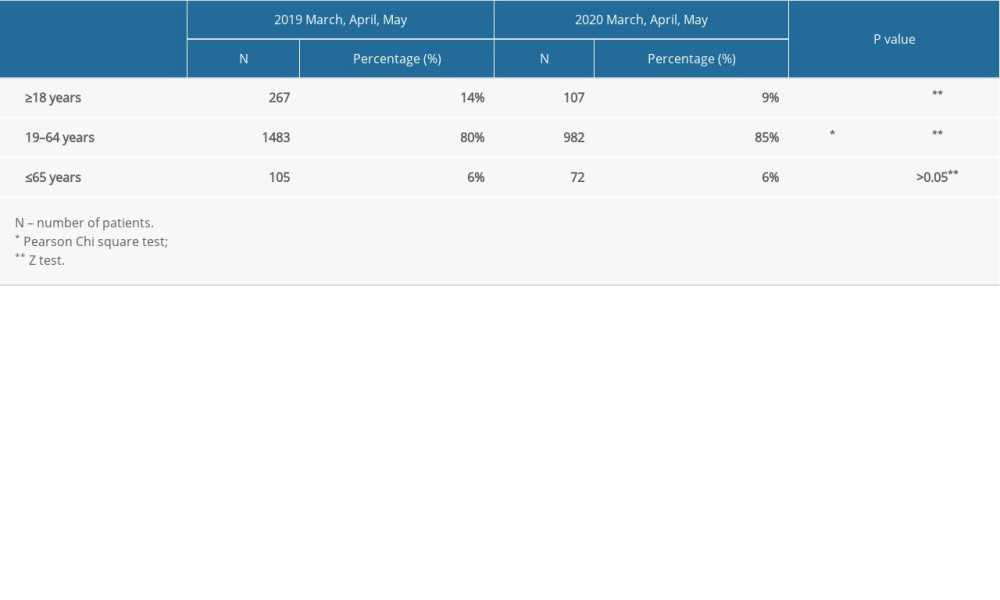 Table 3. The reasons for emergency depatment presentations in March, April, and May in 2019 and 2020.
Table 3. The reasons for emergency depatment presentations in March, April, and May in 2019 and 2020.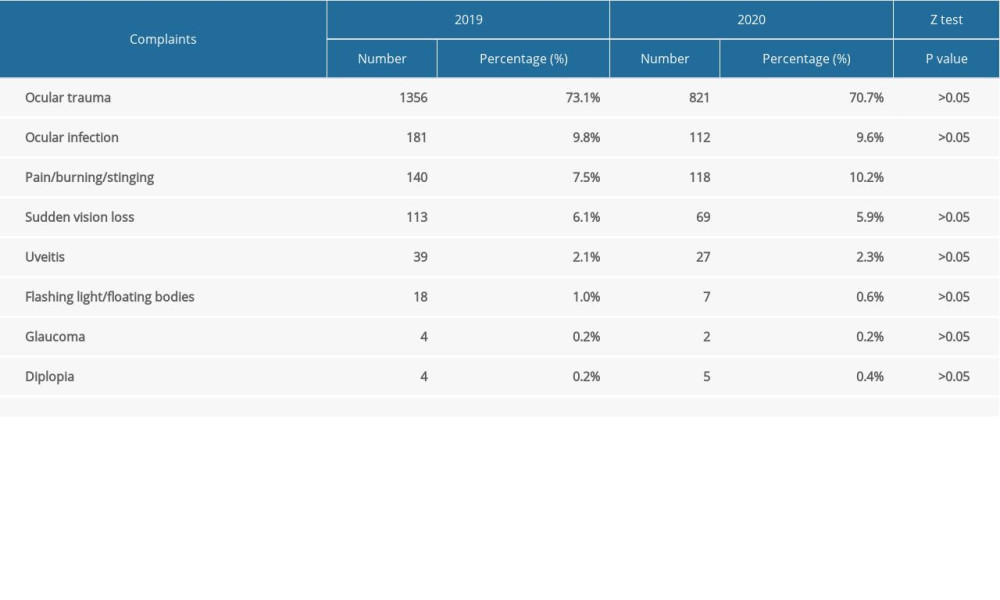 Table 4. The average number of patients in age groups according to quarantine days.
Table 4. The average number of patients in age groups according to quarantine days.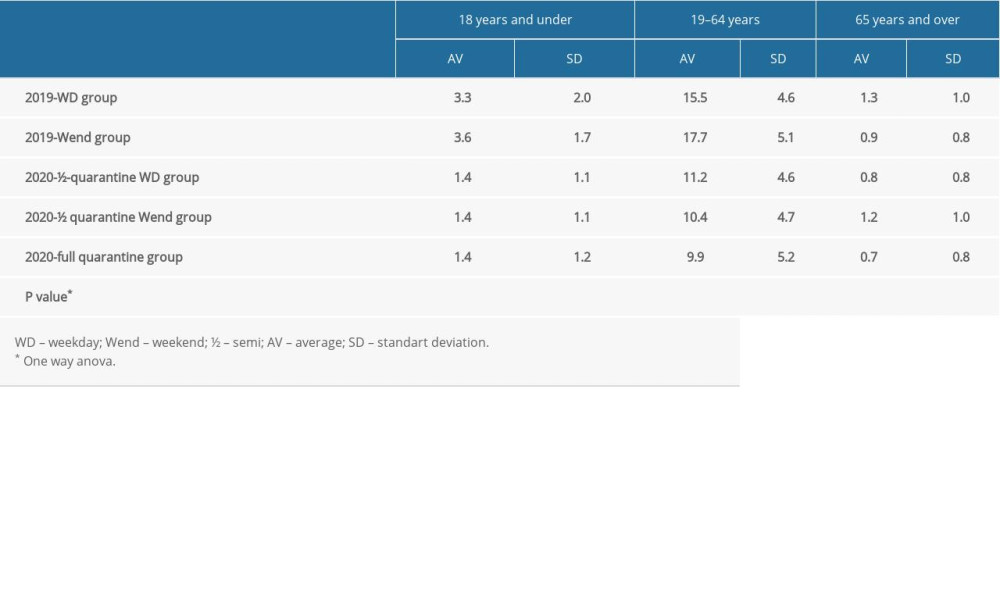 Table 5. The average number of patients who presented to the emergency department with different health problems according to quarantine days.
Table 5. The average number of patients who presented to the emergency department with different health problems according to quarantine days.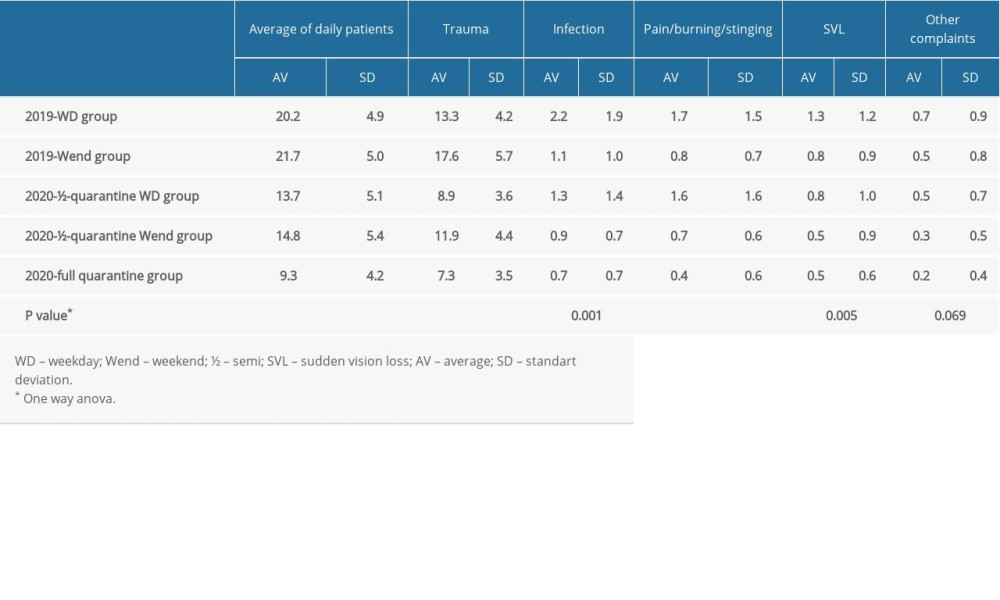
References
1. Channappanavar R, Perlman S, Pathogenic human coronavirus infections: Causes and consequences of cytokine storm and immunopathology: Semin Immunopathol, 2017; 39; 529-39
2. Andrews EE, Ayers KB, Brown KS, No body is expendable: Medical rationing and disability justice during the COVID-19 pandemic: Am Psychol, 2020 [Online ahead of print]
3. Martin-Delgado J, Viteri E, Mula A, Availability of personal protective equipment and diagnostic and treatment facilities for healthcare workers involved in COVID-19 care: A cross-sectional study in Brazil, Colombia, and Ecuador: PLoS One, 2020; 15; e0242185
4. Boškoski I, Gallo C, Wallace MB, Costamagna G, COVID-19 pandemic and personal protective equipment shortage: Protective efficacy comparing masks and scientific methods for respirator reuse: Gastrointest Endosc, 2020; 92; 519-23
5. Actis AG, Brogliatti B, Personal protective equipment in eye examination after the coronavirus pandemic: Everything like before? Minerva Chir, 2020; 75; 203-5
6. Siddiqui O, Manchanda V, Yadav A, Comparison of two real-time polymerase chain reaction assays for the detection of severe acute respiratory syndrome-CoV-2 from combined nasopharyngeal-throat swabs: Indian J Med Microbiol, 2020; 38; 385-89
7. Bennett S, Søreide K, Gholami S, Strategies for the delay of surgery in the management of resectable hepatobiliary malignancies during the COVID-19 pandemic: Curr Oncol, 2020; 27; e501-11
8. Johnson AP, Wohlauer MV, Mouawad NJ, The impact of the COVID-19 pandemic on vascular surgery trainees in the United States: Ann Vasc Surg, 2021; 72; 182-90
9. Müller M, Stöckle U, Trampuz A, Coronavirus pandemic – SARS-CoV-2 in orthopedics and trauma surgery: Z Orthop Unfall, 2021; 159(1); 25-31
10. Wu C, Patel SN, Jenkins TL, Ocular trauma during COVID-19 stay-at-homeorders: A comparative cohort study: Curr Opin Ophthalmol, 2020; 31; 423-26
11. Shah M, Shah S, Patel H, Khanna R, Impact of COVID-19 lock down on ocular trauma in pediatric population: Int J Paeddiatrics Geriatrics, 2020; 3; 27-29
12. Pellegrini M, Roda M, Di Geronimo N, Changing trends of ocular trauma in the time of COVID-19 pandemic: Eye (Lond), 2020; 34; 1248-50
13. Franzolin E, Casati S, Albertini O, Impact of COVID-19 pandemic on Ophthalmic Emergency Department in an Italian tertiary eye centre: Eur J Ophthalmol, 2021 [Online ahead of print]
14. D’Oria F, Bordinone MA, Rizzo T, Validation of a new system for triage of ophthalmic emergencies: The Alphabetical Triage Score for Ophthalmology (ATSO): Int Ophthalmol, 2020; 40; 2291-96
15. Poyser A, Deol SS, Osman L, Impact of COVID-19 pandemic and lockdown on eye emergencies: Eur J Ophthalmol, 2020; 19; 1120672120974944
Tables
 Table 1. The patient groups included in the study in March, April, and May 2019 and 2020.
Table 1. The patient groups included in the study in March, April, and May 2019 and 2020. Table 2. The distribution of ophthalmic emergency presentations of different age groups in March, April, and May 2019 vs 2020.
Table 2. The distribution of ophthalmic emergency presentations of different age groups in March, April, and May 2019 vs 2020. Table 3. The reasons for emergency depatment presentations in March, April, and May in 2019 and 2020.
Table 3. The reasons for emergency depatment presentations in March, April, and May in 2019 and 2020. Table 4. The average number of patients in age groups according to quarantine days.
Table 4. The average number of patients in age groups according to quarantine days. Table 5. The average number of patients who presented to the emergency department with different health problems according to quarantine days.
Table 5. The average number of patients who presented to the emergency department with different health problems according to quarantine days. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








