13 May 2022: Clinical Research
Safety and Efficacy of Sufentanil and Fentanyl Analgesia in Patients with Traumatic Brain Injury: A Retrospective Study
Wenhan XiaDOI: 10.12659/MSM.934611
Med Sci Monit 2022; 28:e934611
Abstract
BACKGROUND: This study aimed to retrospectively assess and compare the safety and efficacy of sufentanil and fentanyl in the treatment of patients with traumatic brain injury.
MATERIAL AND METHODS: A total of 85 patients with traumatic brain injury from June 2016 to September 2018 were included in this study, and were enrolled into a sufentanil group and a fentanyl group according to different treatment methods. The patients in both groups were assessed with the Critical care Pain Observation Tool (CPOT) for analgesic score, and Richmond Agitation-Sedation Scale (RASS) for sedation score.
RESULTS: The scores of CPOT and RASS in the 2 groups were significantly lower than before treatment (P<0.05), but there was no significant difference between the 2 groups (P>0.05). The heart rate (HR), rate of spontaneous respiration (RR), and mean arterial pressure (MAP) of the 2 groups were significantly lower than before treatment (P<0.05), and the RR of the sufentanil group was significantly lower than that of the fentanyl group at all time points after treatment (P<0.001).
CONCLUSIONS: Sufentanil has a rapid onset of effect, and it is safe, stable, and effective for patients with traumatic brain injury in the intensive care unit (ICU). Compared with fentanyl, sufentanil can also effectively shorten mechanical ventilation time, time to obtain satisfactory sedation and analgesia, and the length of hospitalization in the ICU.
Keywords: Analgesia, Brain Injuries, Traumatic, Fentanyl, Sufentanil, Humans, Pain
Background
In recent years, analgesia and sedation have become a significant part of overall treatment in the ICU [1]. The 2013 American ICU guidelines for adult patients with pain, agitation, and delirium proposed an analgesic-first sedation strategy, and reiterated the importance of analgesic treatment in the ICU [2]. The guidelines recommended intravenous administration of opioids as the first-line option for treatment of non-neuropathic pain in critically ill patients. In addition, the ideal opioids should have the advantages of fast onset, easy regulation, lower dosage, less accumulation of metabolites, and low cost.
Fentanyl was first introduced into European clinical practice as an analgesic in 1963. Its analgesic effect is about 75 ~ 100 times of that of morphine. It is a powerful narcotic analgesic and has been listed in the World Health Organization and the list of essential drugs in China. The pharmacological effects of fentanyl are similar to morphine, mainly including analgesia, sedation, and anesthesia, and can reduce the stress response of endocrine metabolism. In addition to analgesic and sedative effects, fentanyl can also be used for anesthesia to reduce stress reaction. Therefore, fentanyl is widely used in the treatment of critically ill patients in the ICU.
Sufentanil, as a potent fat-soluble opioid sedative, has been widely applied in the induction of clinical general anesthesia, intraoperative maintenance, and postoperative analgesia due to its clear analgesic effect and stable safety [3,4]. The potency of sufentanil is about 500 times that of morphine. Its binding to the receptor has the characteristics of saturation, reversibility, and specificity. Sufentanil is twice as lipophilic as fentanyl and easily passes through the cell membrane and blood-brain barrier. Therefore, sufentanil can quickly spread and distribute in various tissues in the body, and the analgesic effect is faster. Thus, sufentanil can quickly and widely exert its maximum efficacy after intravenous administration. A large number of clinical trials have confirmed that sufentanil has the characteristics of rapid onset, no histamine release, and stable cardiovascular system function. Compared with the equivalent dose of fentanyl, sufentanil has rapid onset, less changes in hormone level and hemodynamics caused by surgical stress, and less adverse reactions of respiratory depression [5,6]. In vitro, sufentanil preconditioning has a protective effect on liver ischemia-reperfusion injury by inhibiting inflammation [7]. In young patients undergoing general anesthesia, the combination of sufentanil and dexmedetomidine can significantly reduce the incidence of postoperative delirium [8]. In addition, the drug is also used for postoperative analgesia, artificial respiration, general anesthesia, and compound anesthesia.
However, due to the complex and critical condition of patients with traumatic brain injury, the long time required for analgesia, the easy accumulation of analgesic sedative drugs, and the diverse individual differences, current information on use of sufentanil for analgesia and sedation in the ICU is still insufficient [9]. Although there are many clinical studies on fentanyl, there are few studies comparing sufentanil and fentanyl. Therefore, we collected the clinical information of patients with brain trauma in the ICU, and retrospectively evaluated and compared the safety and effectiveness of sufentanil and fentanyl in clinical treatment, so as to further explore the utility of sufentanil.
Material and Methods
THERAPEUTIC METHODS:
All patients were given active primary disease treatment and symptomatic support treatment. In the sufentanil group, patients were intravenously injected with 0.1 μg/kg sufentanil (Humanwell Pharma Co., Ltd., Yichang, Hubei, China, 1 ml: 50 μg), and then switched to a micro-syringe pump to continuously pump the 0.1 μg/(kg·h) sufentanil, and the CPOT score was used to record the analgesia score every 10 min. If the CPOT score was >2, the dosage of sufentanil was increased at the rate of 0.05 μg/(kg·h) until the CPOT score was <2. In the fentanyl group, 1.0 μg/kg fentanyl (Humanwell Pharma Co., Ltd., Yichang, Hubei, China, 10 ml: 500 μg) was injected intravenously, and then switched to a micro-syringe pump to continuously pump the 1.0 μg/(kg·h) fentanyl, and the CPOT score was used to record the analgesia score every 5 min. If the CPOT score was >2, the dosage of fentanyl was increased at the rate of 0.5 μg/(kg·h) until the CPOT score was <2. All patients in the 2 groups were given 1.0 mg/kg propofol (Corden Pharma Co., Ltd., Treviglio, Bergamo, Italy, 1 ml: 20 mg) for analgesia at the same time, and injected within 30~60 s to reduce the impact on hemodynamics, and then switched to a micro-syringe pump to continuously pump propofol 0.5 mg/(kg·h). These 2 drugs are fentanyl group analgesics. The mechanism of action of fentanyl drugs is similar to that of opioids such as morphine. They mainly reduce or relieve pain by stereospecific binding with opioid receptors to excite them. The potency of fentanyl is 100~180 times that of morphine, and the potency of sufentanil is about 500 times that of morphine.
EVALUATION OF CLINICAL INDICATORS:
The acute physiology and chronic health evaluation (APACHE II) scoring system were recorded in 2 groups, and the scores of CPOT and RASS were observed and recorded before treatment and 0, 0.5, 1, 6, 12, 18, 24, and 48 h after obtaining satisfactory sedation and analgesia in the 2 groups. In addition, the indicators of HR, RR, MAP, propofol dose, time to obtain satisfactory sedation and analgesia, mechanical ventilation time, length and cost of hospitalization in ICU, and adverse reactions (eg, respiratory inhibition, skeletal myotonia, pruritus, nausea and vomiting, hypotension, and bradycardia) were further observed and recorded.
SAMPLE SIZE:
We used 2 sets of repeated measurement formulas in clinical studies to estimate the sample size:
In the formula, the n represents the sample size of each group. The σ stands for standard deviation. The p represents the number of observations before treatment for each subject. The r represents the number of observations after treatment for each subject. The ρ is taken as constant 0.65. The δ stands for clinically significant difference. On the basis of previous research, the primary endpoint variable was HR and it was used to calculate the smallest required sample size. We used a minimal clinical significant change in HR of 1.0 bpm and a standard deviation of 2.3 bpm. With α level of 0.05, β level of 0.05, p value of 1, and r value of 6, the smallest required sample size per group was 39 patients. Therefore, we a selected similar clinical sample size when looking for cases and enrolling patients. A total of 85 patients with traumatic brain injury who were admitted to the ICU of Jiangxi Provincial People’s Hospital Affiliated to Nanchang University from June 2016 to September 2018 were included in this study. They were enrolled into 2 groups according to different treatment methods. The patients were enrolled into either the sufentanil group (n=42) or the fentanyl group (n=43). Pregnant women and patients with the severe liver and kidney failure, opioid allergy, and alcohol abuse were excluded. The current study was approved by the Ethics Committee of the Jiangxi Provincial People’s Hospital Affiliated to Nanchang University (No. 2016060) and the informed consent forms were signed by the family members of involved individuals.
STATISTICAL ANALYSIS:
The data were analyzed using SPSS 22.0 statistical software (IBM Corp., Armonk, NY, USA). The measurement data were expressed as mean±standard deviation (x±s). The intra-group and inter-group mean were compared by independent-sample
Results
DEMOGRAPHIC DATA AND BASIC INFORMATION BEFORE TREATMENT:
Table 1 shows the demographic data and basic information of patients in the 2 groups before treatment. There was no significant difference in the indicators of gender, age, weight, APACHE II, alanine aminotransferase (ALT), aspartate aminotransferase (AST), creatinine (Cr), Glasgow scale (GCS), and blood urea nitrogen (BUN) between the 2 groups (P all >0.05).
SCORES OF CPOT AND RASS BEFORE AND AFTER TREATMENT:
Figure 1A and 1B show that scores of CPOT and RASS in the 2 groups were significantly lower than before treatment (P<0.05), but there was no significant difference between the 2 groups (P>0.05).
HR, RR, AND MAP BEFORE AND AFTER TREATMENT:
Figure 2A–2C show that the HR, RR, and MAP of the 2 groups were significantly lower than before treatment (P<0.05), and the RR of the sufentanil group was significantly lower than that of the fentanyl group at all time points after treatment (P<0.001). However, there was no significant difference in HR and MAP between the 2 groups at any time points (P>0.05).
TIME TO OBTAIN SATISFACTORY SEDATION AND ANALGESIA, MECHANICAL VENTILATION TIME, LENGTH AND COST OF HOSPITALIZATION IN ICU, AND ADVERSE REACTIONS:
As shown in Table 2, compared with the fentanyl group, the sufentanil group had shorter mechanical ventilation time, time to obtain satisfactory sedation and analgesia, and length of hospitalization in ICU (P<0.001). However, there was no significant difference in cost of hospitalization in the ICU and adverse reactions between the 2 groups (P>0.05).
Discussion
As an opioid μ receptor agonist and a commonly used analgesic in clinical practice, sufentanil is synthesized synthetically and has strong analgesic effect and little effect on hemodynamics [10]. Compared with other analgesics such as fentanyl, sufentanil is more lipophilic and has a faster onset of action, which allows it to cross the blood-brain barrier and obtain the effect of pain relief in a shorter time. Moreover, sufentanil also has the advantages of short half-life, fast metabolic rate, and steady hemodynamic stability [11,12]. Meanwhile, enough oxygen can be supplied to the heart muscle, and the maximum efficacy can be obtained within a few minutes after intravenous administration of sufentanil [13,14]. Hence, sufentanil has more profound clinical significance in the treatment of patients with traumatic brain injury in the ICU.
Sufentanil has been widely used in Belgium, Luxembourg, and other countries in Europe for long-term analgesia and sedation of patients on mechanical ventilation, and obtained considerable results [15]. At present, there are few studies on the analgesic effect of sufentanil in ICU patients with brain trauma. Sufentanil and fentanyl were selected as the basic analgesic drugs in this experiment to explore the efficacy and clinical utility of these 2 analgesic drugs combined with sedation in ICU patients with brain trauma.
As a reliable pain assessment tool for ICU patients, the CPOT score is widely used in the ICU. In addition, the 2013 American ICU guidelines for adult patients with pain, agitation, and delirium also recommend use of the RASS score to assess the quality and depth of sedation. The results of this study showed that when sufentanil and fentanyl were used for analgesia in patients with traumatic brain injury in ICU, the CPOT and RASS scores were significantly reduced, and both groups obtained satisfactory sedation and analgesia effects. Moreover, the frequency of spontaneous breathing in the sufentanil group was significantly reduced at all time points after treatment, which suggests that sufentanil can increase the synchronization of human and machine in patients with mechanical ventilation and make breathing more stable [16]. The sufentanil group obtained satisfactory sedative and analgesic effects faster, which may be related to the lipophilicity of sufentanil, which is about twice that of fentanyl, and it passes more easily and faster through the blood-brain barrier, so it has a sedative effect stronger than fentanyl.
Only a few previous studies have compared the clinical utility of sufentanil and fentanyl [17,18]. Butterworth [18] found that sufentanil produced a quicker extubation than did fentanyl (geometric mean 12.2 vs 14.2 h), but found no association between time of mechanical ventilation and ICU or hospital length of stay, which disagrees with our study results and expectations. Shortening the time of mechanical ventilation did not shorten the length of hospital stay. We consider that this situation is due to the differences in nursing process and discharge standards. The patients selected in this study were all patients with brain trauma. Controlled hypothermia may be used during the treatment, which can affect the pharmacokinetics and pharmacodynamics of the drugs studied, and may limit the universality of this study. Sufentanil has also been found to be useful for treatment of ICU patients as a part of sedative management. Considering the properties of sufentanil described earlier, the search for an analgesic stabilizing the hemodynamics of patients naturally focused on this agent. Numerous inconveniences associated with the use of morphine and fentanyl as well as the painful procedure additionally contributed to the further quest for other solutions for analgesic sedation in intensive therapy [19,20]. Our study found that there was no correlation between length and cost of hospitalization in the ICU. Although fentanyl has a price advantage over sufentanil, the literature demonstrates that the apparent economic effects achieved with fentanyl are quickly eliminated by the required supplementary treatment and treatment of complications [21]. As Cheng [22] has pointed out and Arom [23] have shown, the process of care and intermediate outcomes (eg, chest tube drainage and arrhythmias) may have a greater effect on cost and hospital length of stay than does choice of anesthetic. This suggests that further efforts to decrease the already short ventilation time might have minimal effects on decreasing hospital direct variable costs. As with all opioids, sufentanil can cause adverse effects, but some of them behave differently due to their specific molecular structure. Compared with fentanyl, sufentanil is associated with significantly less nausea and vomiting. Moreover, euphoric symptoms are also less common and less severe due to the limited effects on dopaminergic structures of the nucleus accumbens and lateral tegmental field. Likewise, it has less effect on cerebral flow compared to fentanyl. The most common complication associated with single doses of sufentanil is bradycardia; however, it should be stressed that it is usually caused by administering it too rapidly. There was no significant difference in adverse reactions between the 2 groups, which may have been related to the small sample size included in our study. Cerebral trauma patients in the ICU are often complicated with hemodynamic disorders, which is also a direct factor leading to the prolongation of mechanical ventilation time and hospitalization time. Since the dawn of its clinical use, sufentanil has become the preferred intravenous opioid under conditions of hemodynamic disturbances [24]. Its standard doses induce slight dilation of arteries, which results from its effect on the vasomotor center and increased capacity of peripheral venous vessels [25,26]. However, no direct negative impact on the dynamics of myocardial contraction has been observed, and the consumption of oxygen is decreased and the basic rhythm is slowed. The beneficial hemodynamic reaction following sufentanil administration persists even in cases of extremely potent autonomic system stimuli [27–30]. Its beneficial effects are also noted in patients with existing ischemic myocardial abnormalities [28]. Intravenous injection of sufentanil resulted in its transfer to surrounding tissues (the half-time of rapid distribution is 1.4 min). However, at the administration site, the increase of its level is quite slow, taking 3–6 minutes to achieve its maximum effect, and the high concentration lasts for a relatively long time after a single administration (the half-time of slow distribution is 17.7 min). The analgesic effect lasts for 30–50 min. This can also explain why there were significant differences in the time to achieve satisfactory sedative and analgesic effects between the 2 groups.
Ultimately, several shortcomings of this study still need to be recognized and pointed out. Firstly, this was a retrospective study with relatively weak evidence level, and further higher-level studies (such as prospective studies and randomized controlled studies) still need to be conducted. Secondly, to further assess the safety and efficacy of sufentanil in the treatment of patients with traumatic brain injury in the ICU, a larger sample size and multi-center prospective studies are still needed.
Conclusions
Sufentanil has a rapid onset of effect, and it is safe, stable, and effective for patients with traumatic brain injury in the ICU. Compared with fentanyl, sufentanil can also effectively shorten mechanical ventilation time, time to obtain satisfactory sedation and analgesia, and the length of hospitalization in the ICU.
Figures
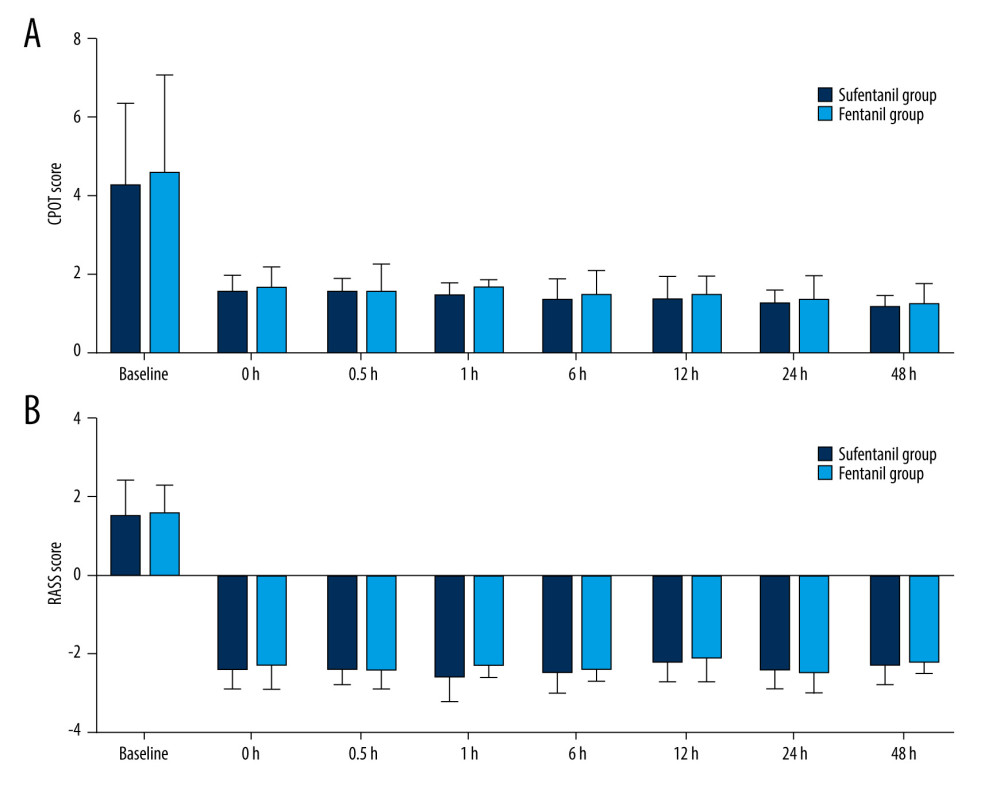 Figure 1. (A, B) The CPOT score, RASS sore in 2 groups were significantly lower than before treatment (P<0.05). (Made using GraphPad Prism 9).
Figure 1. (A, B) The CPOT score, RASS sore in 2 groups were significantly lower than before treatment (P<0.05). (Made using GraphPad Prism 9). 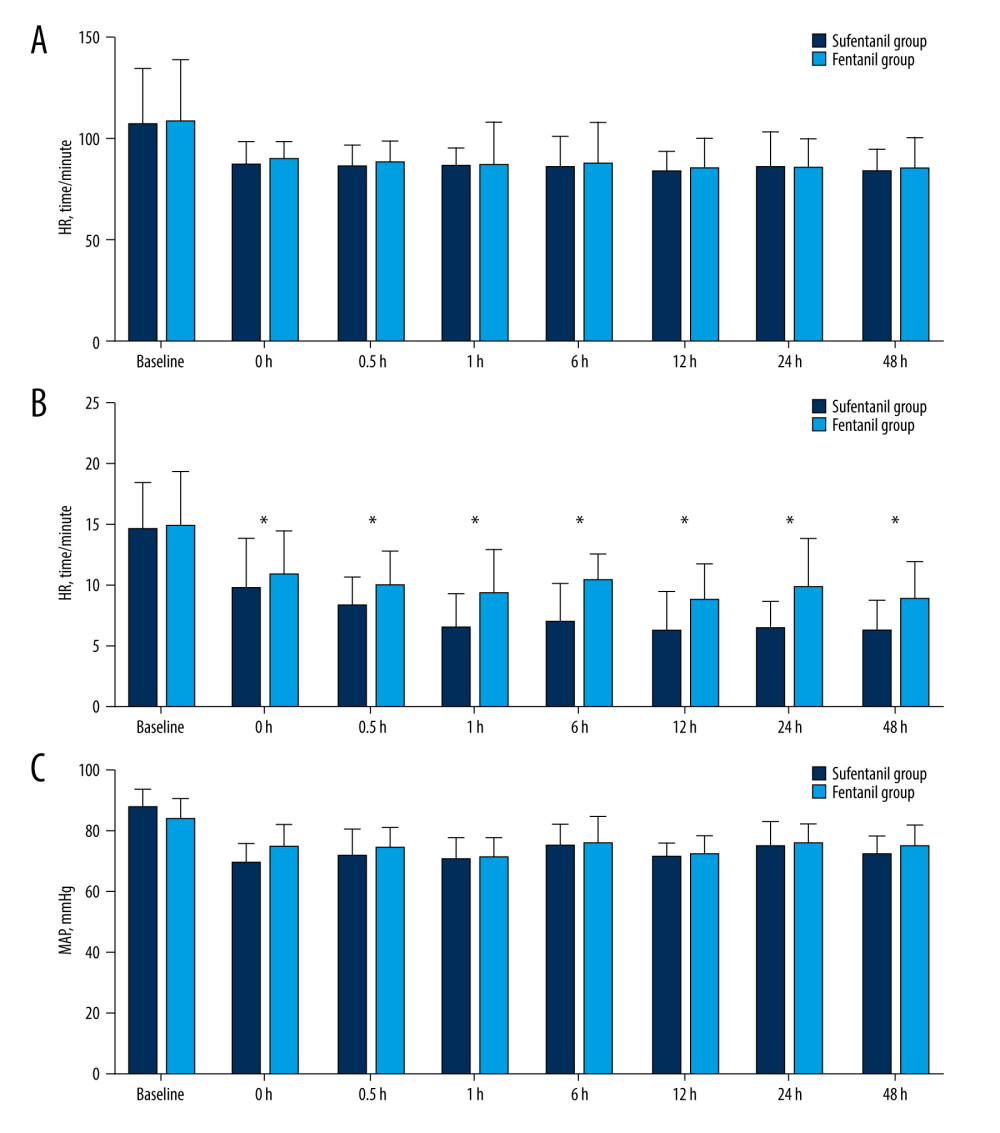 Figure 2. (A–C) HR, RR, and MAP in 2 groups were significantly lower than before treatment (P<0.05).* Comparison between sufentanil group and fentanil group, P<0.001. (Made using GraphPad Prism 9).
Figure 2. (A–C) HR, RR, and MAP in 2 groups were significantly lower than before treatment (P<0.05).* Comparison between sufentanil group and fentanil group, P<0.001. (Made using GraphPad Prism 9). References
1. Gao J, Wei L, Xu G, Effects of dexmedetomidine vs sufentanil during percutaneous tracheostomy for traumatic brain injury patients: A prospective randomized controlled trial: Medicine, 2019; 98; e17012
2. Celis-Rodriguez E, Diaz Cortes JC, Cardenas Bolivar YR, Evidence-based clinical practice guidelines for the management of sedoanalgesia and delirium in critically ill adult patients: Med Intensive (Engl Ed), 2020; 44; 171-84
3. Benahmed-Canat A, Plaisant F, Riche B, Postsurgery analgesic and sedative drug use in a French neonatal intensive care unit: A single-center retrospective cohort study: Archiv Pediatr, 2019; 26; 145-50
4. Nies RJ, Muller C, Pfister R, Monitoring of sedation depth in intensive care unit by therapeutic drug monitoring? A prospective observation study of medical intensive care patients: J Intensive Care, 2018; 6; 62
5. Misailidi N, Papoutsis I, Nikolaou P, Fentanyls continue to replace heroin in the drug arena: The cases of ocfentanil and carfentanil: Forensic Toxicol, 2018; 36; 12-32
6. Zhang ZP, Tang W, Drug metabolism in drug discovery and development: Acta Pharm Sin B, 2018; 8; 721-32
7. Lian Y-H, Fang J, Zhou H-D, Sufentanil preconditioning protects against hepatic ischemia-reperfusion injury by suppressing inflammation: Med Sci Monit, 2019; 25; 2265-73
8. Liu L, Yuan Q, Wang Y, Effects of dexmedetomidine combined with sufentanil on postoperative delirium in young patients after general anesthesia: Med Sci Monit, 2018; 24; 8925-32
9. Roberts DJ, Hall RI, Kramer AH, Sedation for critically ill adults with severe traumatic brain injury: A systematic review of randomized controlled trials: Crit Care Med, 2011; 39; 2743-51
10. Zhi M, Diao Y, Liu S, Sufentanil versus fentanyl for pain relief in labor involving combined spinal-epidural analgesia: A systematic review and meta-analysis of randomized controlled trials: Eur J Clin Pharmacol, 2020; 76; 501-6
11. Han L, Su Y, Xiong H, Oxycodone versus sufentanil in adult patient-controlled intravenous analgesia after abdominal surgery: A prospective, randomized, double-blinded, multiple-center clinical trial: Medicine, 2018; 97; e11552
12. Wang JM, Xu F, Peng G, Efficacy and safety of sufentanil-propofol versus remifentanil-propofol as anesthesia in patients undergoing craniotomy: A meta-analysis: World Neurosurg, 2018; 119; e598-e606
13. Blancher M, Maignan M, Clape C, Intranasal sufentanil versus intravenous morphine for acute severe trauma pain: A double-blind randomized non-inferiority study: PLoS Med, 2019; 16; e1002849
14. Liu M, Li Z, Wang S, Application via mechanical dropper alleviates sufentanil-induced cough: A prospective, randomized, single-blinded trial: Trials, 2019; 20; 170
15. Roelants F, Lavand’homme P, Clonidine versus sufentanil as an adjuvant to ropivacaine in patient-controlled epidural labour analgesia: A randomised double-blind trial: Eur J Anaesthesiol, 2015; 32; 805-11
16. Wilwerth M, Majcher JL, Van der Linden P, Spinal fentanyl vs. sufentanil for post-operative analgesia after C-section: A double-blinded randomised trial: Acta Anaesthesiol Scand, 2016; 60; 1306-13
17. Royston D, Remifentanil in cardiac surgery: Eur J Anaesthesiol Suppl, 1995; 10; 77-79
18. Butterworth J, James R, Do shorter-acting neuromuscular blocking drugs or opioids associate with reduced Intensive Care Unit or hospital lengths of stay after coronary artery bypass surgery?: Anesthesiology, 1988; 88; 1437-46
19. Payen JF, Chanques G, Current practices in sedation and analgesia for mechanically ventilated critically ill patients: A prospective multicenter patient-based study: Anesthesiology, 2007; 106; 687-95
20. Maciejewski Dl, Sedacja analgetyczna z zastosowaniem sufentanylu jako nowy standard postępowania w intensywnej terapii: Anestezjol Intens Ter, 2008; 3(Suppl 1); 21-22 [in Polish]
21. Engoren M, Luther G, A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia: Anesth Analg, 2001; 93; 859-64
22. Cheng DC, Fast track cardiac surgery pathways: Early extubation, process of care, and cost containment: Anesthesiology, 1998; 88; 1429-33
23. Arom KV, Emery RW, Petersen RJ, Schwartz M, Costeffectiveness and predictors of early extubation: Ann Thorac Surg, 1995; 60; 127-32
24. Bovill JG, Sebel PS, Stanley TH, Opioid analgesics in anesthesia: With special reference to their use in cardiovascular anesthesia: Anesthesiology, 1984; 61; 731-55
25. Fukuda K: Opioids in: Anaesthesia, 2009, Philadephia, Churchil Livingstone
26. Ebert TJ, Ficke DJ, Arain SR, Vasodilation from sufentanil in humans: Anesth Analg, 2005; 101; 1677-80
27. Wilhelm W, Kreuer S, The place for short-acting opioids: Special emphasis on remifentanil: Crit Care, 2008; 12(Suppl 3); 5
28. Bhavsar R, Sloth E, Folkersen L, Sufentanil preserves hemodynamics and left ventricular function in patients with ischemic heart disease: Acta Anaesthesiol Scand, 2011; 55; 1002-9
29. Liao X, Yang QY, Xue FS, Bolus dose remifentanil and sufentanil blunting cardiovascular intubation responses in children: A randomized, doubleblind comparison: Eur J Anaesthesiol, 2009; 26; 73-80
30. Lemoine S, Zhu L, Massetti M, Continuous administration of remifentanil and sufentanil induces cardioprotection in human myocardium, in vitro: Acta Anaesthesiol Scand, 2011; 55; 758-64
Figures
 Figure 1. (A, B) The CPOT score, RASS sore in 2 groups were significantly lower than before treatment (P<0.05). (Made using GraphPad Prism 9).
Figure 1. (A, B) The CPOT score, RASS sore in 2 groups were significantly lower than before treatment (P<0.05). (Made using GraphPad Prism 9). Figure 2. (A–C) HR, RR, and MAP in 2 groups were significantly lower than before treatment (P<0.05).* Comparison between sufentanil group and fentanil group, P<0.001. (Made using GraphPad Prism 9).
Figure 2. (A–C) HR, RR, and MAP in 2 groups were significantly lower than before treatment (P<0.05).* Comparison between sufentanil group and fentanil group, P<0.001. (Made using GraphPad Prism 9). Tables
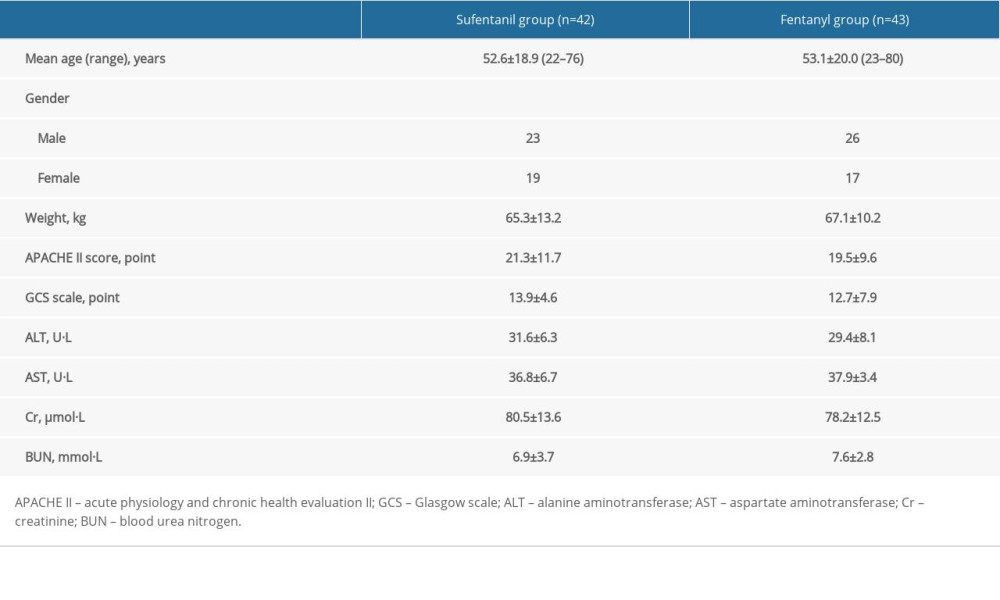 Table 1. Demographic data and basic information before treatment.
Table 1. Demographic data and basic information before treatment.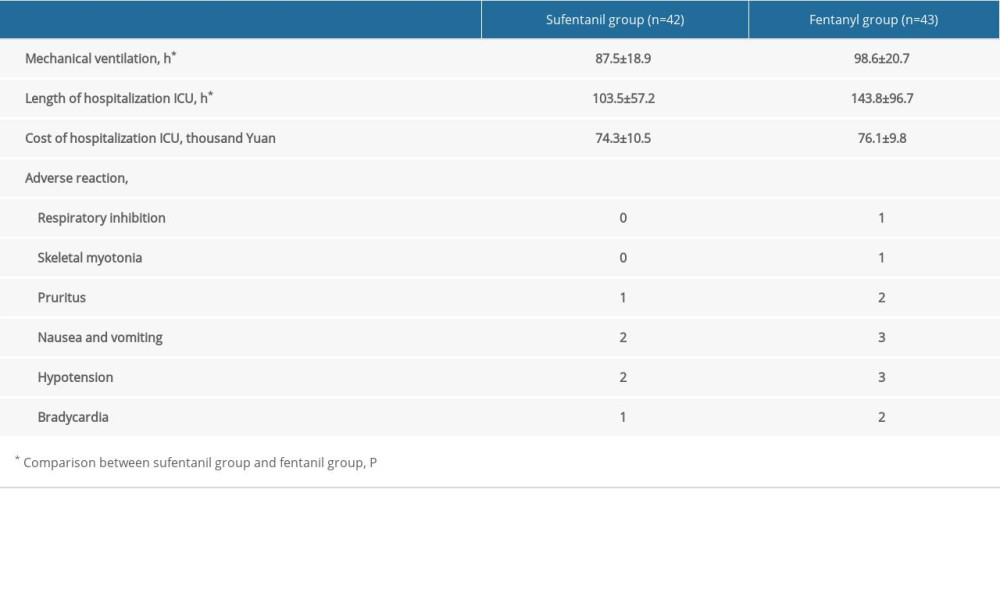 Table 2. Time to obtain satisfactory sedation and analgesia, mechanical ventilation time, and length and cost of hospitalization in the ICU.
Table 2. Time to obtain satisfactory sedation and analgesia, mechanical ventilation time, and length and cost of hospitalization in the ICU. Table 1. Demographic data and basic information before treatment.
Table 1. Demographic data and basic information before treatment. Table 2. Time to obtain satisfactory sedation and analgesia, mechanical ventilation time, and length and cost of hospitalization in the ICU.
Table 2. Time to obtain satisfactory sedation and analgesia, mechanical ventilation time, and length and cost of hospitalization in the ICU. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








