19 April 2022: Clinical Research
Factors Associated with Non-Adherence for Prescribed Treatment in 201 Patients with Multidrug-Resistant and Rifampicin-Resistant Tuberculosis in Anhui Province, China
Qing-Qing Zhu1BCDE, Jie Wang23BCDE, Napoleon Bellua Sam4F, Jie Luo5F, Jie Liu1A, Hai-Feng Pan23A*DOI: 10.12659/MSM.935334
Med Sci Monit 2022; 28:e935334
Abstract
BACKGROUND: This study aimed to investigate the factors associated with non-adherence of prescribed treatment in patients with multidrug-resistant and rifampicin-resistant tuberculosis (MDR/RR-TB) in Anhui Province, China.
MATERIAL AND METHODS: A cross-sectional survey was conducted in each designated hospital between March 2020 and May 2021. A structured questionnaire was designed to collect categorical characteristics and the historical data of the study participants. Non-adherence was determined from patient medical records and face-to-face interviews using the questionnaire at each designated hospital for MDR/RR-TB.
RESULTS: A total of 201 patients with confirmed sputum cultures positive for MDR/RR-TB were enrolled, 27.4% of whom were non-adherent to MDR/RR-TB treatment. In Anhui, MDR patients had a high incidence of adverse events, of which gastrointestinal reactions accounted for the majority. Absence of other chronic diseases (odds ratio (OR) 0.401; 95% confidence interval (CI) 0.203-0.791) and having no drug discontinuation (OR 0.040; 95% CI 0.018-0.091) were protective predictors of adherence. Patients with MDR/RR-TB with secondary education level and above and monthly family income of $309.4 USD or higher were more likely to follow the guidelines. Those who received anti-tuberculosis treatment and those who lived in suburban areas were less likely to adhere to the treatment. Binary-logistic regression indicated that the risk factor of non-adherence was drug discontinuation.
CONCLUSIONS: Low education level, place of residence, poor financial conditions, presence of other chronic diseases, discontinuation of medication, and frequency of anti-tuberculosis treatments were influential factors of adherence to MDR/RR-TB treatment.
Keywords: Antitubercular Agents, medication adherence, Patient Compliance, Risk Factors, China, Cross-Sectional Studies, Humans, Odds Ratio, Rifampin, Tuberculosis, Multidrug-Resistant
Background
Tuberculosis is a major public health problem worldwide, especially in Asia and Africa, regions that account for the highest mortality among the communicable diseases worldwide. There, mortality from tuberculosis exceeds that of HIV/AIDS and accounted for 1.5 million deaths in 2018 [1]. China is 1 of the 8 countries from these regions and accounts for two-thirds of the global total of tuberculosis cases [1]. In 2013, of the 0.48 million new cases of multi-drug resistant rifampicin-resistant tuberculosis (MDR/RR-TB) worldwide, 0.21 million related deaths occurred [2]. In 2019, the global tuberculosis incidence rate was 130/100 000, and China ranked third among 30 countries, with a high burden of new cases (8.4% of new cases globally). It was estimated that about 3.3% of new cases and 18% of patients who were treated were resistant to rifampin. The countries with the highest estimated number of patients with rifampin resistance to tuberculosis are India (124 000, 27% globally), China (65 000, 14% globally), and Russia (39 000, 8% globally). Nevertheless, the diagnosis and successful treatment of MDR/RR-TB occurred were where the underperformance was greatest. Each of the 16 cities in Anhui Province, China, has set up a designated hospital for MDR/RR-TB, which is responsible for the detection, treatment, and management of patients. The center for disease control and prevention (CDC) of each city cooperates with the designated hospitals to supervise patients’ standardized treatment and ensure treatment adherence. Adherence to MDR/RR-TB treatment is the most vital requirement for efficient tuberculosis control [3]. Therefore, research on the influencing factors of tuberculosis treatment adherence is essential for discovering potential influencing factors and intervening to improve the cure rate and survival rate of patients. In recent years, Anhui Province has gradually promoted the control of MDR/RR-TB. Initially, the Global Fund MDR tuberculosis prevention and treatment program was implemented in Fuyang and Anqing in 2012, and by 2016, province-wide coverage of MDR tuberculosis treatment and management was achieved (the treatment requirements for RR-TB are the same as those for MDR-TB). In 2017, the program management of standardized treatment of patients with MDR/RR-TB was given an impetus across the province, but the number of patients in treatment and the success rate of treatment were still undesirable.
Treatment adherence in patients with MDR/RR-TB is correlated with various factors, including insufficient awareness of MDR/RR-TB [3], the occurrence and management of adverse reactions to anti-tuberculosis drugs, implementation of treatment guidelines [4], family economic status, and management of supervised medication administration. Compared with the treatment effect in patients with tuberculosis who are drug sensitive, the treatment effect in patients with MDR/RR-TB is much worse [5]. This may be because MDR/RR-TB requires a long treatment duration, which requires continuous treatment for 18 to 20 months [6], there are many kinds of therapeutic drugs, which are difficult to obtain [7,8], there is a high incidence of adverse reactions [9–11], and most families cannot afford drugs owing to the high cost of outpatient examination and hospitalization [9,10,12–14]. Fang et al investigated the adherence to tuberculosis treatment in Anhui Province [15] and identified several related factors, including marital status, annual income, medical personnel supervision, and patient knowledge about anti-tuberculosis treatment. However, they recruited the drug-sensitive tuberculosis population [15], whereas we selected patients with drug-resistant tuberculosis to describe the non-adherence to MDR/RR-TB treatment.
Although MDR/RR-TB has been included in the scope of the National Reimbursement for Major Diseases, there are still many drugs that are scarce, expensive, and cannot be reimbursed within the range of medical insurance, greatly reducing the treatment adherence of patients with MDR/RR-TB. The result is the spread and prevalence of MDR/RR-TB, which causes great harm to the society. Since 2016, one municipal medical institution was designated as an MDR/RR-TB hospital in each prefecture-level city and was made responsible for the diagnosis and inpatient and outpatient follow-up treatment of MDR/RR-TB in the city. Each city’s CDC tuberculosis control staff are responsible for the supervision and management of patients with MDR/RR-TB in their jurisdiction.
Therefore, this study aimed to investigate the factors associated with non-adherence for prescribed treatment in patients with MDR/RR-TB in Anhui Province, China.
Material and Methods
STUDY PARTICIPANTS:
This study was conducted in Anhui Province from March 2020 to May 2021. As the eighth largest province in China, Anhui consists of 16 municipalities and 104 counties (districts) with a total population of more than 60 million (Figure 1). A stratified sampling method was used based on the geographical distribution of Anhui Province. The province was divided into 3 zones, namely southern, central, and northern, with enormous interzonal variation. Representative cities were selected by the per capita gross domestic product (GDP), and 25 patients with MDR/RR-TB were selected in each city by simple random sampling. A total of 8 municipalities (including Anqing, Tongling, Maanshan, Hefei, Huainan, Bengbu, Fuyang, and Huaibei) were selected as study sites after considering the registration and management of MDR/RR-TB patients and the level of GDP per capita in each municipality. The survey was conducted on patients with MDR/RR-TB who registered chronologically at the designated hospitals for MDR/RR-TB in each municipality from January 1, 2017, onward. This survey ensured that no cases of death outcomes were included. This study recruited 201 patients and continued its investigations after the treatment period of the patients was over. The diagnosis of resistance in these patients was detected by the supervision of the treatment carried out.
STUDY METHODS:
A structured questionnaire was designed, and the in-depth interviews were conducted by trained investigators. All participants were interviewed face-to-face at the local designated hospital by using the self-designed survey tool, which included demographic and socio-economic information of the participants, MDR/RR-TB-related medical seeking behavior, history of unhealthy behaviors and disease, and the knowledge of MDR/RR-TB. Information related to patient treatment was entered into the China Tuberculosis Information Management System in accordance with the requirements of the China CDC. The structured questionnaire was designed based on the consultation of experienced doctors and extensive relevant literature review.
The rate of incorporation of patients with MDR/RR-TB into treatment and the rate of successful treatment were recorded as the relevant indicators in this study.
RELEVANT DEFINITIONS:
Body mass index (BMI) was calculated by taking a person’s weight in kg divided by their height in m2, or BMI=kg/m2 [16]. In this study, a BMI less than 18.4 was defined as underweight and above 24.0 was considered obese. A BMI in the range of 18.5 to 23.9 was considered normal.
DATA ANALYSIS:
The data was captured using Epidata 3.1 and exported to SPSS 23.0 (IBM Corp, Armonk, NY, USA) for statistical analysis. Quantitative data was described by χ̄±standard deviation, and qualitative data was expressed as rates or percentages. The chi-square test was used to analyze the association of each variable with adherence to MDR/RR-TB treatment. A binary-logistic regression model was used to further assess the impact of variables on adherence. The odds ratio (OR) with 95% confidence interval (CI) was used to measure the magnitude of association. A
Results
GENERAL INFORMATION:
A total of 201 patients were recruited during the study period. The male to female ratio was 2.9: 1. The age of the respondents ranged from 34 to 67 years, with a mean age of 50.5±16.4 years. The mean height of the patients was 169±7.0 cm, and the mean weight was 60.8±10.7 kg. With regards to education level, 86.1% had high school or technical secondary school education or lower. Concerning patients’ work, 22.7% were working on farms, 21.1% were unemployed, 18.0% were migrant workers. Almost all patients (97.5%) had health insurance. The percentage of respondents who lived in urban areas was 45.8%, while 37.8% lived in the countryside. Nearly 60% of the patients had 2 to 3 family members.
KNOWLEDGE OF MDR/RR-TB:
Patients who knew all of the 9 items about MDR/RR-TB on the survey were defined as having a good mastery and high rate knowledge; not knowing all answers was regarded as a low awareness rate. The questions in Table 1 were open and multi-selective, not dichotomous choices. Consequently, the percentage of those who knew all of the 9 items about MDR/RR-TB was 16.9%. The awareness rate of MDR/RR for each article is shown in Table 1.
STATUS OF TREATMENT:
A total of 72.6% of the patients had good treatment compliance; 90.5% had received anti-tuberculous treatment more than once. The total cost of this MDR/RR-TB hospitalization was a minimum of $154.7 USD and a maximum of $27 846, with a median of $1574. Of the adverse reactions that occurred in 63.7% of patients with MDR/RR-TB, most were gastrointestinal reactions. Of the patients who experienced adverse reactions, 67.8% were given efficient treatment.
ANALYSIS OF TREATMENT ADHERENCE AND ITS INFLUENCING FACTORS:
Adherence was compared among different subgroups using the chi-square test. It was found that education level, place of residence, household monthly income, presence of other chronic diseases, discontinuation of medication, and the frequency of anti-tuberculosis treatments were factors influencing adherence of patients with MDR/RR-TB (Table 2).
The variables with significant differences in Table 2 were extracted and the ORs and 95% CIs were calculated separately for them (Table 3).
Binary-logistic regression analysis revealed that drug discontinuation was a barrier to adherence to MDR/RR-TB treatment (Table 4).
Discussion
Providing efficient treatment is a key step in stopping the spread of MDR/RR-TB. However, treatment that lasts for 18 to 20 months makes it difficult for patients to maintain adherence. In our study, 72.6% of the patients adhered to the MDR/RR-TB treatment. A previous report defined adherence and the differences in the way drug-sensitive and drug-resistant tuberculosis patients are managed in registries, treatment cycles and methods, and national policies; poor adherence was defined as a missed dose of medication [15]. The study revealed that factors such as marital status, annual income, tuberculosis knowledge, and medical staff visits affect drug-sensitive patients [15]. However, our study showed that low education level, place of residence, poor financial conditions, presence of other chronic diseases, discontinuation of medication, and frequency of anti-tuberculosis treatments were major influential factors of adherence to MDR/RR-TB treatment. Therefore, there are differences in the study population and findings between the 2 studies. Prior to the standardization of MDR/RR-TB treatment, many patients experienced more than 1 anti-tuberculosis treatment or non-standardized treatment with a failed outcome, possibly because drug sensitivity testing was not performed. These were the main factors found to influence treatment adherence in the results of the univariate analysis of the present study and were partially comparable to the results of similar studies [3,4,7,9–14,17–22]. Due to the low literacy rate, this segment of patients might have a relatively insufficient understanding of physicians’ advice and knowledge of tuberculosis prevention and control; therefore, they might not have a good grasp of the hazards of drug-resistant tuberculosis and the importance of standardized treatment during the consultation. MDR/RR-TB treatment regimens in this study included at least 4 effective anti-tuberculosis drugs, the costs of medication were relatively high, and there were some items not covered by health insurance. The 2-year-long treatment cycle imposed a heavy financial burden on patients. It was therefore difficult for patients who were living in a low-income family to afford the whole cycle of treatment. In 2020, the average annual salary of employed persons in urban private units in Anhui Province was $8134 USD, and salaries in rural areas were significantly lower than this. For some unemployed patients, it caused a greater financial burden. Patients with drug-resistant pulmonary tuberculosis were included in the reimbursement of chronic and special disease medical insurance. The proportion of inpatient treatment reimbursement was relatively high, and the proportion of outpatient treatment reimbursement was not high, and therefore, the economic burden of patients was great. As reported in other study, financial hardship was a major factor affecting treatment adherence in patients with MDR/RR [9,10,12–15]. In the province’s 16 cities, each city had only 1 designated hospital for MDR/RR-TB, usually a municipal general hospital; therefore, it was more challenging for patients with MDR/RR-TB living in counties and rural areas to find medical services than for those living in cities. Consequently, this was 1 possible reason accounting for non-adherence. Patients with comorbidity of other chronic diseases, discontinuation of medication during treatment, and a high frequency of previous anti-tuberculosis treatments were in poor general health, and the state of their diseases were more complex. Thus, they were more prone to be affected by other factors. Compared with the patients with drug-resistant tuberculosis alone who were in anti-tuberculosis treatment for the first time, the above-mentioned patients could obviously not totally adhere to the treatment.
Drug discontinuation is a significant factor affecting adherence, and it is necessary to urge patients to adhere to the course of medication. Drug discontinuation means interruption of treatment, which promotes the growth and reproduction of drug-resistant tuberculosis bacteria. Notably, the impact of drug discontinuation on patient adherence was extremely significant and easily contributed to the prevalence of drug-resistant bacteria.
Considering the above factors affecting treatment adherence of patients with MDR/RR-TB, the following approaches have been considered to enhance treatment adherence and control the drug-resistant tuberculosis epidemic.
Firstly, greater importance should be given to the advocacy of tuberculosis-related knowledge [3,12,15,17,19]. While guiding patients, physicians should emphasize the dangers of MDR/RR-TB and the possible consequences of unregulated treatment. Supervising administrators should highlight the infectiousness of drug-resistant tuberculosis during household follow-up visits and supervision of medication administration. Patients should be proactively informed about how to protect their family members from being infected. At the same time, care should be given to the physical and mental health of patients, and adverse reactions occurring during taking anti-tuberculosis drugs should be recorded. Once adverse events happen, timely treatment at the designated hospital should be provided to prevent adverse consequences. For patients who have had multiple anti-tuberculosis treatments, it is even more essential to strengthen communication interventions and psychological counseling, as necessary. As for patients with low literacy, more attention to tailoring methods and approaches for this population is important. Patient mastery of relevant knowledge should be assessed, and for patients who do not master it well, the information must be promoted, emphasized, and communicated several times. Tools such as brochures should be made and distributed in an easy-to-understand way using drawings, flow charts, and slogans for different types of target groups, with concise and easy-to-remember content.
Secondly, efforts to minimize the financial burden of patient treatment by taking advantage of the central financial tuberculosis program, financial subsidies, and related expenditure reductions were provided to drug-resistant patients. Applying to the finance department for more investment and to the health insurance department for further increase in reimbursement ratio and increasing the types of anti-tuberculosis drugs covered by medical insurance reimbursement would be urgently required to improve adherence. Government investment and policy protection were the crucial points to promoting tuberculosis prevention and control [1,13,23,24]. Through multisectoral means, we could expand the free packages to reduce the financial burden for the poor, such as writing off the costs of transport and supplementary nutrition involved in treatment. All of the above might facilitate regular treatment, improve patient adherence, and increase the cure rate.
Thirdly, the strengthening of adverse drug reaction monitoring cannot be ignored. There are various kinds of anti-tuberculosis drugs that have a high incidence of adverse reactions. The adverse effects were not a risk factor affecting adherence in this study; however, many studies have reported that patients had an interruption of therapy due to adverse effects [9–11,18]. Clinicians and supervisory administrators should strengthen patient awareness of the timely detection of adverse drug reactions, have patients sign a written informed consent for anti-tuberculosis treatment before drug administration, and inform patients in detail of the types of possible adverse reactions that might occur and the clinical manifestations and symptoms. When an adverse reaction occurs, patients must communicate with their doctors as soon as possible. Regular review was also a means of detecting adverse drug reactions. Adverse effects might be mitigated by changes in the way medication is taken; for example, reducing gastrointestinal reactions might be achieved by gradually increasing the dose and adjusting the time of medication or by taking it with juice, yogurt, and other beverages. If the effects are not relieved or serious adverse reactions occur and the patient could not tolerate them, the treatment regimen should be adjusted; however, the principle of drug combination might not be changed. It is of primary importance to ensure early, regular, whole-course, appropriate, and combined drug use.
Generally, MDR/RR-TB is characterized by a long treatment cycle, high cost, and a high rate of adverse events. The adherence of participants in the present study was affected by a range of factors. In the course of routine tuberculosis control, we must enhance awareness of prevention and control and take various measures to decrease non-adherence according to the above-mentioned factors and improve the cure rate to control the tuberculosis epidemic.
This study had some limitations. Firstly, the information collected on the questionnaire was mainly obtained from patients’ subjective recall; therefore, recall bias was inevitable. Secondly, the sample size was relatively small, which may weaken the robustness of the conclusions.
Conclusions
The findings of this study indicated that 27.4% of the participants did not adhere to MDR/RR-TB therapy. The influencing factors for non-adherence include education level, place of residence, monthly household income, presence of other chronic diseases, drug discontinuation, and multiple anti-tuberculosis treatments.
Tables
Table 1. Patient awareness of multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis.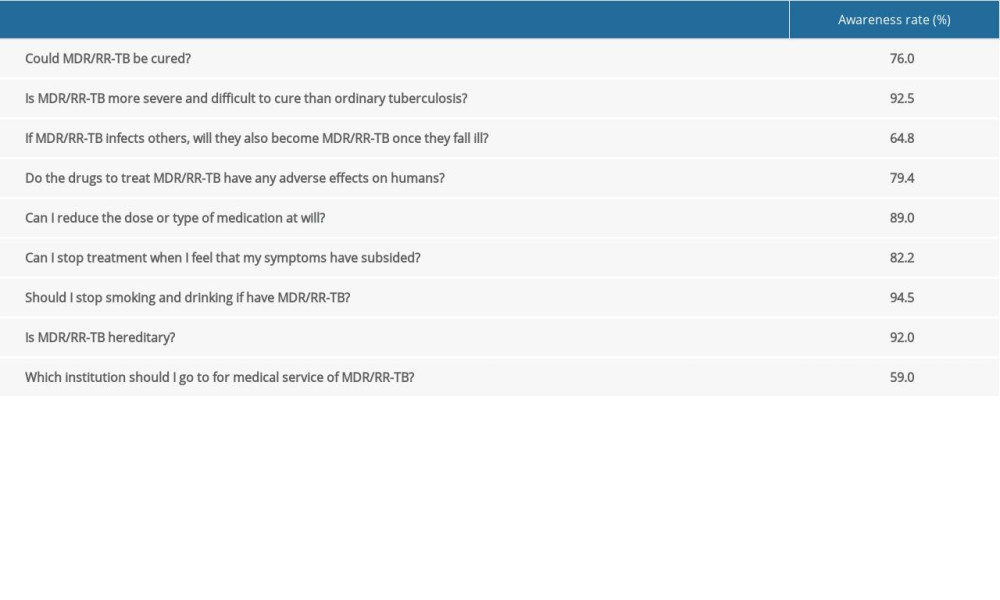 Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.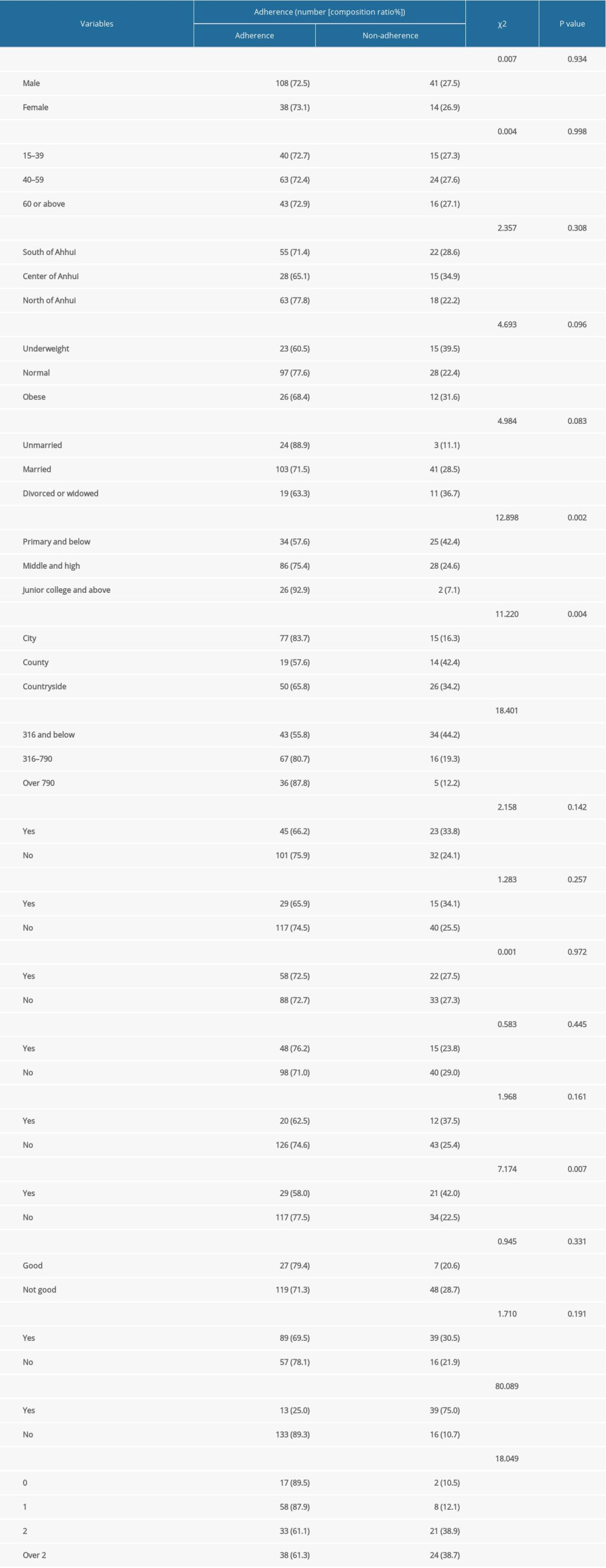 Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable.
Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable.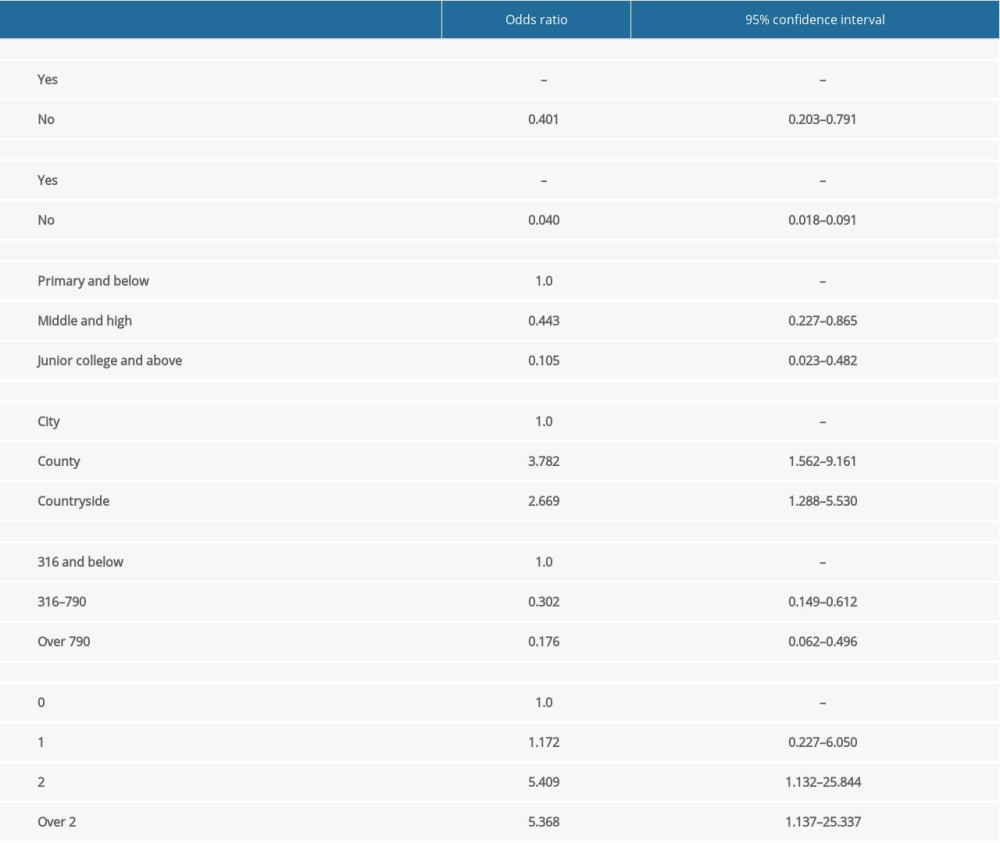 Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.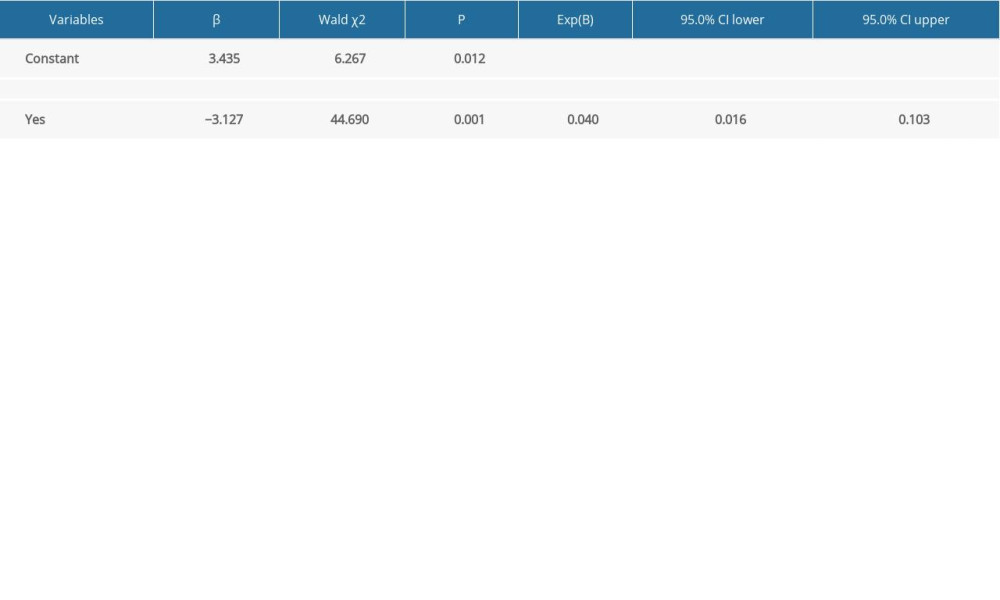
References
1. Harding E, WHO global progress report on tuberculosis elimination: Lancet Respir Med, 2020; 8(1); 19
2. Zumla A, George A, Sharma V, The WHO 2014 global tuberculosis report – further to go: Lancet Glob Health, 2015; 3(1); e10-12
3. Zhou C, Chu J, Liu J, Adherence to tuberculosis treatment among migrant pulmonary tuberculosis patients in Shandong, China: A quantitative survey study: PLoS One, 2012; 7(12); e52334
4. Usmanova R, Parpieva N, Davtyan H, Treatment compliance of multidrug resistant tuberculosis in Uzbekistan: Does practice follow policy?: Int J Environ Res Public Health, 2021; 18(8); 4071
5. Ashwath P, Sannejal AD, A quest to the therapeutic arsenal: Novel strategies to combat multidrug-resistant bacteria: Curr Gene Ther, 2021 [Online ahead of print]
6. Korenromp EL, Glaziou P, Fitzpatrick C, Implementing the global plan to stop TB, 2011–2015 – optimizing allocations and the Global Fund’s contribution: A scenario projections study: PLoS One, 2012; 7(6); e38816
7. Hu D, Liu X, Chen J, Direct observation and adherence to tuberculosis treatment in Chongqing, China: A descriptive study: Health Policy Plan, 2008; 23(1); 43-55
8. Gunther G, van Leth F, Alexandru S, Multidrug-resistant tuberculosis in Europe, 2010–2011: Emerg Infect Dis, 2015; 21(3); 409-16
9. Wang Y, Chen H, Huang Z, Drug non-adherence and reasons among multidrug-resistant tuberculosis patients in Guizhou, China: A cross-sectional study: Patient Prefer Adherence, 2019; 13; 1641-53
10. Xing W, Zhang R, Jiang W, Adherence to multidrug resistant tuberculosis treatment and case management in Chongqing, China – a mixed method research study: Infect Drug Resist, 2021; 14; 999-1012
11. Gelmanova IY, Keshavjee S, Golubchikova VT, Barriers to successful tuberculosis treatment in Tomsk, Russian Federation: Non-adherence, default and the acquisition of multidrug resistance: Bull World Health Organ, 2007; 85(9); 703-11
12. Ibrahim LM, Hadejia IS, Nguku P, Factors associated with interruption of treatment among pulmonary tuberculosis patients in Plateau State, Nigeria. 2011: Pan Afr Med J, 2014; 17; 78
13. Zhou C, Chu J, Geng H, Pulmonary tuberculosis among migrants in Shandong, China: Factors associated with treatment delay: BMJ Open, 2014; 4(12); e005805
14. Zhou C, Tobe RG, Chu J, Detection delay of pulmonary tuberculosis patients among migrants in China: A cross-sectional study: Int J Tuberc Lung Dis, 2012; 16(12); 1630-36
15. Fang XH, Shen HH, Hu WQ, Prevalence of and factors influencing anti-tuberculosis treatment non-adherence among patients with pulmonary tuberculosis: A cross-sectional study in Anhui Province, Eastern China: Med Sci Monit, 2019; 25; 1928-35
16. Weir CB, Jan A: BMI classification percentile and cut off points, 2021, StatPearls
17. Tang Y, Zhao M, Wang Y, Non-adherence to anti-tuberculosis treatment among internal migrants with pulmonary tuberculosis in Shenzhen, China: A cross-sectional study: BMC Public Health, 2015; 15; 474
18. Franke MF, Appleton SC, Bayona J, Risk factors and mortality associated with default from multidrug-resistant tuberculosis treatment: Clin Infect Dis, 2008; 46(12); 1844-51
19. Driver CR, Matus SP, Bayuga S, Factors associated with tuberculosis treatment interruption in New York City: J Public Health Manag Pract, 2005; 11(4); 361-68
20. Cutfield T, Mowlem L, Paynter J, Treatment and outcomes of multidrug-resistant tuberculosis in Auckland 1995–2018: Intern Med J, 2021 [Online ahead of print]
21. Fregona G, Cosme LB, Moreira CMM, Risk factors associated with multidrug-resistant tuberculosis in Espirito Santo, Brazil: Rev Saude Publica, 2017; 51; 41
22. Holtz TH, Lancaster J, Laserson KF, Risk factors associated with default from multidrug-resistant tuberculosis treatment, South Africa, 1999–2001: Int J Tuberc Lung Dis, 2006; 10(6); 649-55
23. Bastos ML, Cosme LB, Fregona G, Treatment outcomes of MDR-tuberculosis patients in Brazil: A retrospective cohort analysis: BMC Infect Dis, 2017; 17(1); 718
24. d’Arc Lyra Batista J, de Fatima Pessoa Militao de Albuquerque M, Smoking increases the risk of relapse after successful tuberculosis treatment: Int J Epidemiol, 2008; 37(4); 841-51
Tables
 Table 1. Patient awareness of multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis.
Table 1. Patient awareness of multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis. Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment. Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable.
Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable. Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment. Table 1. Patient awareness of multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis.
Table 1. Patient awareness of multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis. Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 2. Univariate analysis of the risk factors for non-adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment. Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable.
Table 3. Univariate analysis of influencing factors for multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis non-adherence and odds ratio value with 95% CI of each variable. Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment.
Table 4. Multi-factor logistic regression analysis of factors affecting patients’ adherence to multidrug-resistant tuberculosis and rifampicin-resistant tuberculosis treatment. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387