18 June 2022: Review Articles
Narrative Review of the Mechanism of Hip Prosthesis Dislocation and Methods to Reduce the Risk of Dislocation
Maciej Kostewicz1ABEF*, Grzegorz SzczęsnyDOI: 10.12659/MSM.935665
Med Sci Monit 2022; 28:e935665
Abstract
ABSTRACT: Total hip arthroplasty (THA) is one of the most effective surgical procedures. It improves quality of life, increases range of motion, and reduces pain in patients with hip joint degeneration. THA allows patients to return to everyday social and professional activities. Therefore, today it is the best approach to treatment of several chronic conditions affecting the hip joint, including advanced degenerative diseases, avascular necrosis, and some traumatic events. The aim of this study was to present the mechanism of hip prosthesis dislocation, associated risk factors, and the factors reducing the risk of dislocation, as well as its consequences and methods of risk minimization. Hip dislocation is a common complication following THA. It is responsible for up to 2% to 3% failures of primary replacements, increasing even to 10% in extreme cases of patients highly predisposed to this condition. In most cases, technical errors during implant placement are responsible for the incidence. The measures taken to prevent complications include activities aimed at correct implant insertion and the selection of the most appropriate type of implant for the patient, depending on individual needs. We summarized the current knowledge of implant dislocation to help surgeons understand the changes in biomechanics of the hip after its replacement and the impact of each particular element that participates in it. This knowledge can enable a surgeon choose the most favorable surgical method and the most appropriate implant to reduce the risk of implant dislocation.
Keywords: Arthroplasty, Replacement, Hip, Hip Dislocation, Hip Joint, Hip Prosthesis, Humans, Joint Dislocations, Prosthesis Failure, Quality of Life, Reoperation, Risk Factors
Background
Total hip arthroplasty (THA) is one of the most effective orthopedic procedures. It relieves pain, restores joint mobility, and improves patient quality of life. It allows patients to return to their everyday social and professional activities. Consequently, today it is the best approach to treat several chronic conditions affecting the hip, including advanced degenerative diseases, avascular necrosis, and some traumatic events [1].
Nevertheless, despite the various unquestionable benefits, THA is not free from complications, with dislocation being among the most frequent, responsible for 1.4% to 5.0% of primary THA. Although much effort has been devoted to dislocation prevention, the percentage of dislocations that leads to adverse sequelae after revision procedures is even higher, reaching up to 25% [2].
Dislocation, whose problem lies within the loss of contact between the prosthetic head and its acetabulum, is due to an extreme position of the joint caused by the impact of excessive mechanical forces on the involved lower limb. It can occur with or without implant loosening, periprosthetic fractures, and infection [1].
The aim of the paper was to summarize the mechanism of hip endoprosthesis dislocation, the risk factors, and the factors preventing it, as well as its consequences and methods of risk minimization.
Mechanisms of Dislocation
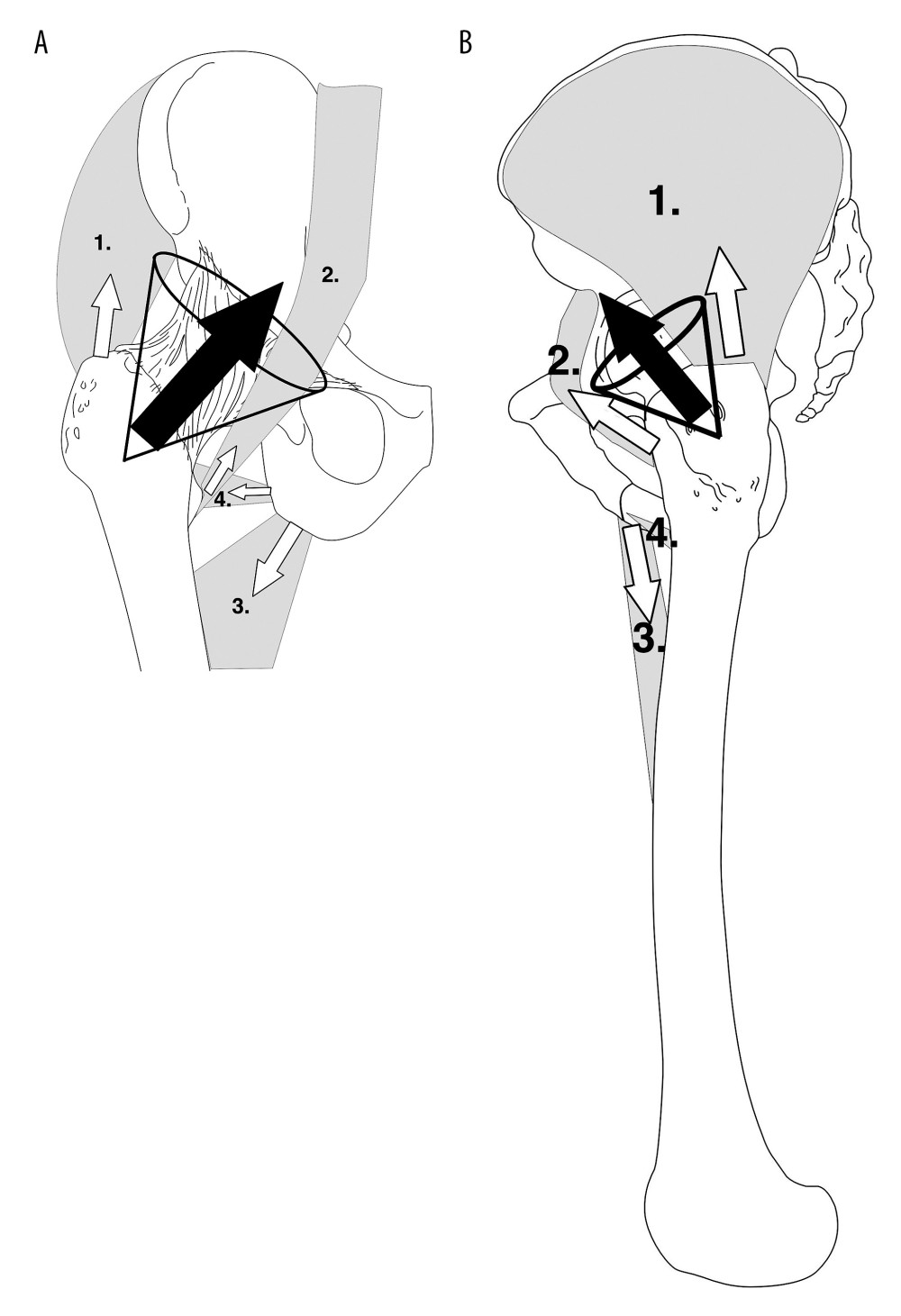
Dislocation occurs when forces acting over the implant in a detrimental direction reach amplitudes that overcome those keeping it intact. It usually takes place as a consequence of unintended external forces that act on a limb placed in an unfavorable position. However, it can also be due to excessive, uncoordinated muscle contractions, such as during epileptic seizures [2,3]. Anatomically, the durability of the articular capsule, which is strengthened by several ligaments, namely the iliofemoral, pubofemoral, and ischiofemoral ligaments, and that of the head of the femur, prevent joint dislocation. After arthroplasty, the postoperative scar formed around the joint partly takes over the function of these ligaments. The scar is supported by negative pressure in the joint cavity, imposing suction force of the value proportional to the contact surface between adherent parts of the prosthesis, and the net force of muscles acting on the pelvic girdle that protects implant integrity (Figure 1A, 1B). The implant is far more prone to dislocation than the anatomical hip owing to the deficiency of the femoral head ligament and the far lower durability of the scar than of the joint capsule and the ligaments supporting it. It is especially prone to dislocation shortly after the procedure, when maturation of the scar is not complete [4].
The amplitude of the net force that stabilizes the hip is highest when its vector is parallel to the acetabular axis. Under such conditions, it presses the prosthetic head toward the acetabulum, protecting it from dislocation. However, when it acts at the same angle, it distributes 2 component forces: the first acting parallel, and the second acting perpendicular to it. The first force presses the head against the acetabulum, supporting its stability, whereas the second force promotes dislocation. The amplitude of the second force is proportional to the sine value of this angle.
Anatomical distribution of the femoral muscles indicates that standing on both legs with the thighs abducted and internally rotated generates net force, which acts almost approximately on the acetabular axis, in both the frontal and the sagittal planes. Thus, in this position, dislocation of the prosthesis is unlikely. However, when the hip is flexed and externally rotated, its distal attachments move anteriorly, changing the direction of their vectors. Consequently, the vector of the net force runs obliquely, generating component force that promotes dislocation. Several routinely performed everyday activities involve limb adjustment in positions that provoke dislocation, including forbidden ones. These include sitting in a cross-legged position, deep squats with heels down, high amplitude swings, and external rotations of maximally abducted and flexed hips. Inappropriate alignment of an artificial prosthetic acetabulum, namely inclination above 70°, retroversion, and too deep positioning, relocates its axis, leading to generation of the component force that dislocates the implant. Therefore, even a relatively small muscular contraction can result in dislocation. Additionally, in those cases, skew distribution of forces acting on the acetabulum contributes to faster loosening and tear-off and fragmentation of its polyethylene insert [2].
Positioning of the Acetabulum
Inappropriate positioning of the acetabulum is the most frequent iatrogenic causative factor of dislocation [5–7]. Based on decade-long observations, the parameters of the optimal positioning of the acetabulum have been defined. They include 45±5° inclination, 15±10° anteversion, and restoring anatomical axis of the joint by its proper location in terms of depth and height [7]. Deviation by more than 3 mm in height and medialization above 5 mm result in asymmetric distribution of mechanical loads, contributing to dislocation [8]. Thus, too steep (inclination above 70°) positioning of the acetabulum with too high (above 30°) or too small (less than 10°) anteversion are recognized as the causative factors of dislocation; especially, when they are associated with its excessive medialization [9].
It is noteworthy that attentiveness to the recommended parameters reduced the incidence of dislocations, loosening of the acetabulum, and acetabular displacement. Therefore, they are generally accepted and widely applied. However, despite their unquestionable usefulness, they do not exclude the risk of dislocation owing to the negative impact of other factors.
Muscular Disorders Favoring Dislocations
Muscular imbalance due to muscle dysfunction or inappropriate coordination of the muscle groups affecting the hip results in inappropriate mechanical loads exerted on the prosthesis. Muscular imbalance can be due to changes in muscle length, such as elongation or shortening, as a consequence of altered anatomical positions of muscular attachments, or by muscles being stretched or relaxed, which leads to their relative mechanical insufficiency. Surgical release of muscular attachments can result in their absolute insufficiency, if not healed. Muscular fibrosis and denervation can also impair their function, usually because of excessively brutal or inappropriate surgical techniques [10,11].
Several analyses revealed that the posterior approach to hip replacement requiring release of external rotators and the posterior aspect of joint capsule increases the risk of dislocation in comparison to lateral, anterolateral, and anterior approaches. The meta-analysis comparing over 13 000 primary hip arthroplasties showed that dislocations complicate 3.23% of procedures performed using the posterior approach, but only 0.55% and 2.18% of those performed using the lateral and anterolateral approaches, respectively. Nevertheless, the percentage of dislocations can be decreased to 0.7% after anatomical reconstruction of the posterior joint capsule and external rotators [12]. In several studies, postoperative reconstruction of the joint capsule reduced the number of dislocations by almost 90% [13,14]. The lateral approach leads to an increased risk of functional weakening of abductors owing to partial detachment of the medial gluteal muscle and the greater trochanter, being responsible for 36% of postoperative dislocations [15]. It has been established that dislocation of the greater trochanter above 1 cm is connected with a 6-fold increased risk in prosthesis dislocation [16].
Inappropriate Positioning of the Stem
In most cases, inappropriate positioning of the stem leads to an excessive anteversion, too deep placement, or varus deformity [10,17]. Excessive anteversion draws back the axis of the prosthetic neck from the acetabular axis, while a too deep placement weakens the muscles whose proximal and distal attachments converge, and varus deformity can lead to the conflict between the medial aspect of the remaining femoral neck and the lesser trochanter with ischial tuberosity which, forming a 2-sided lever, can dislocate the prosthesis in a forcedly adducted and internally rotated limb.
It has been established that the lowest risk of dislocation occurs when the stem is positioned in 10° to 15° anteversion and at an appropriate depth to support it on the Adam’s arch and to restore the calve line [18]. Inappropriate anteversion results in conflict between the stem and the cup and between bony prominences of the pelvis and femur, provoking conflicts that disrupt the balance between elements of the prosthesis and aggravating the risk of its dislocation and loosing. It is far more important in non-cemented prostheses, since the fixation of their acetabula pivots much more on the balance of forces that press it directly into its pelvic lodge. It has been noticed that the anteversion of the stem has to correspond with the anteversion of the acetabulum, summarized by the term “combined anteversion” [19]. This combined anteversion has been primarily assessed with values varying between 25° and 35° in men and up to 45° in women [20], and is currently qualified as 25° to 45° (mean 35°). The easiest way to implant a prosthesis according to those requirements is to implant primarily the stem with required anteversion, compensating the combined anteversion by strictly defined positioning of the acetabulum with computer navigation [21]. Implant setting also entails the risk of complications. Cemented stems have twice the lower risk of periprosthetic fractures than cementless ones [22].
Impact of Stiffness of the Lumbar Spine
A limited range of motion of the lumbosacral spine enforces increased compensatory overloads of the hip, thus being one of the risk factors for endoprosthesis dislocation. A limited range of pelvic tilt during typical everyday activities, including those requiring flexion and extension of the hip (sitting on the chair, standing), reinforces a compensatory range of motion in the prosthesis, which can contribute to its dislocation. Thus, hip arthroplasties performed in patients with ankylosing spondylitis have an extremely high risk of dislocation and loosening of the prosthesis in comparison to those in patients with osteoarthritis [23,24].
One study conducted in a sample of 1000 patients 1 year after primary THA showed that the patients who sustained dislocations had a substantially decreased range of motion in the lumbar spine and sacral slope, while, during standing and sitting, the differences between the involved and the uninvolved lower limb were significantly lower. The results indicated that 92% of patients with dislocations previously underwent surgeries of the lumbar spine, including spine fusions [25]. Analogous results have been obtained from the analysis of the biomechanical reasons for late prosthetic dislocations, in which the study found that the decrease of sacral tilt while changing the body position from standing to sitting forces a decrease in the range of hip motion by 0.9° per each 1.0° of limited spine mobility. The above findings explain the mechanism of late dislocations in patients with decreased spine mobility.
Pelvic retroversion predisposes patients to anterior dislocations, forcing hyperextension of the hip, while standing and anteversion predisposes to posterior dislocations due to excessive flexion in the sitting position [26]. It has been assessed that spondylodesis is the greatest independent risk factor for dislocations of hip prostheses during the first 6 months after arthroplasty [27].
Patient-Dependent Factors that Predispose to THA Dislocation
The patient-dependent factors that predispose patients to dislocation are shown in Table 1. Secondary injuries due to patient noncompliance with postoperative recommendations markedly increase the risk of dislocations. This is especially common in the early postoperative period, when an immature scar provides weak mechanical support of joint congruence. Dislocation can occur from leg crossing, squatting, and even performing movements in an excessive range of motion. During the first 3 months after surgery, inordinate movements increase the risk of dislocation owing to insufficient scar resistance [28]. However, an excessive scar formed around the joint can contribute to dislocation, levering the prosthetic’s head from the acetabulum during contracture of muscles adjacent to the trochanteric area. This usually occurs in cases of repeated surgical interventions. Thus, revision procedures have a significantly higher risk of dislocations, reaching up to 28% of performed procedures. It is most prominent in wide tissue injuries, both traumatic and iatrogenic, that heal leaving an excessive scar and heterotopic ossification [29]. Deficits of skeletal tissues of the acetabulum and the proximal end of the femur form another group of risk factors for displacement [10].
In such cases, education of patients focused on elimination of movements leading to dislocation, carried out by an experienced physiotherapist, can reduce the risk of complication.
Dislocations can also occur in late periods after arthroplasty. Unfortunate events, such as falls, stumbling, and even car accidents, can result in dislocations and associated soft-tissue injuries [30]. Locomotor disability, including stiffness of the adjacent joints of the affected limb, contractures, and impairments of the visual and vestibular systems, hearing, and proprioception, increase the incidence risk [31]. Other factors include neurologic (paresis and cerebral palsy, Parkinson disease, myasthenia), metabolic (diabetes, hypoglycemia), cardiologic (stroke, arrhythmia, cardiac arrest) and many other disorders that predispose a patient to secondary injuries [32–34]. Patients with neuromuscular disorders are prone to dislocations due to an imbalance of particular groups of muscles, especially flexors and pronators. Additional risk factors for these patients include cognitive disorders, weakened muscle strength, impaired coordination and balance, and lack of the possibility to control the patient’s activity that may culminate in dislocation of the prosthesis [5,35,36].
A very specific group of patients predisposed to dislocations includes vigorously physically active individuals, who do sport and undertake risky activities. The generation of much higher loads increases prosthesis wear, implant loss, and the risk of dislocation. Nevertheless, an appropriate selection of an implant that would be adequate for this particular group (low-friction working elements, head diameter 32 mm) and patient education eliminates the risk of this complication to the value of that in patients with low activity [37].
The unpredictable and often also irrational behavior of alcohol and drug abusers and mentally ill patients increases the risk of implant dislocation and periprosthetic fractures [37,38]. In those groups, both complications are the most frequent reasons for revision procedures [3,39]. Very strict preoperative planning, precise implant positioning, and careful postoperative care combined with an intensive rehabilitation program and education allow patients to reduce the risk of dislocations to an accepted level [40].
Patients with soft-tissue imbalance, joint deformities around the hips, and bilateral pathological hips seem to be more predisposed to implant dislocation. Recently identified risk factors include preoperative hip adduction deformity combined with limb lengthening of 2 cm postoperatively, knee valgus combined with pelvic obliquity deformity, and bilateral pathology of the hip that require arthroplasty. If the procedure is planned carefully and has proper postoperative management, dislocation after THA can be prevented [41].
Patients with Crowe type IV developmental dysplasia of the hip are at a high risk of dislocation after THA. Nevertheless, in those cases, implantations of an implant with higher size of the femoral head (28 instead of 22 mm) reduces the risk of dislocation. Risk can be lowered by improvement of the strength of the abductors in properly planned preoperative and postoperative rehabilitation [42].
Recently, obesity, especially morbid obesity, has been identified as one of the factors that increase the risk of dislocation. The relationship between body mass index (BMI) and the degree of THA instability, with a BMI of 40 kg/m2 and higher, is noticeable. The circumference of the thigh, not the BMI itself, is a factor that directly reduces the stability of the joint. Moreover, the rate of THA dislocation in women with obesity is higher than that in men with obesity owing to the differences in fat deposition (women store fat mainly around the hips and thighs, whereas in men it is mostly distributed at the abdomen) [34,43].
Factors Preventing Hip Prosthesis Dislocation
Anatomically, the hip is protected from dislocation by active and passive stabilizers. Active stabilizers are the joint capsule and the pubofemoral, ischiofemoral, and iliofemoral ligaments supporting it. Additionally, the femoral head is powered by its own ligament and suction, which is the effect of negative pressure in the joint cavity during dislocation. Active stabilizers form muscles of the pelvic girdle [44,45]. Their net force presses the head of the prosthesis to its acetabulum, increasing congruency of the joint.
Surgical procedures deprive joints of some of the abovementioned elements. The surgical approach requires dissection, excision, and removal or release of the joint capsule and its ligaments and ligaments of the femoral head, and non-physiological limb movements overstretch muscles of the pelvic ring. The forthcoming fibrosis impairs their contractility, decreasing their strength [46,47]. Several recently introduced techniques preserve anatomical structures with a limited surgical intervention and reconstruction of joint capsule and muscle attachments [48,49]. However, the question of whether it is able to reduce the risk of complications is still controversial [50]. The range of iatrogenic lesions highly depends on the selected surgical approach, patient’s constitution-related factors (obesity), previously performed interventions (scarring), and an excessive (even brutal) surgical technique. Unfortunately, even the most delicate, tissue-protecting technique does not guarantee preservation of anatomical structures. This especially concerns advanced stiffness of the hip, its wide scarring after previously performed procedures and injuries, and the question of when it is necessary to restore biomechanics in dysplastic high hip dislocations with the formation of the secondary acetabulum [51].
An inappropriate size of the prosthetic head can increase the risk of dislocation and accelerate the damage of its acetabulum. Unquestionably, heads with a greater diameter decrease the risk of dislocation, providing higher congruency. At the same time, however, they decrease the range of motion, jeopardizing implant levering in extreme joint positions [52].
Outcomes of Hip Prosthesis Dislocation
Dislocation leads to severe consequences. It can cause vast soft-tissue injury, including scar formation around the joint and the remainders of its capsule, muscles, and their attachments, contributing to bone fractures, the loss of bone, and the integrity and stability of the implant. When repositioned, deprivation of stabilizers can easily reoccur. The consequences of dislocation also include avulsion fractures, vast scarring, and heterotopic ossification [29,53].
Preoperative Planning
Careful preoperative planning, the use of the most suitable implant and surgical approach for the particular case, and an adequate postoperative rehabilitation program combined with education of patients play the most important role in prevention of dislocation.
Several meta-analyses determined that the most effective and least risky surgical approaches are suitable minimally invasive implantation techniques that preserve soft tissues and have implants with bigger diameters of the head [54], as their dislocation requires a bigger force to destabilize the implant [55,56]. Therefore, bipolar prostheses and prostheses with large heads are less prone to dislocation [57]. Hence, they are commonly implanted in patients with neuromuscular disorders [58,59]. Their additional advantage is an increased surface of the contact area between working parts, decreasing the net loading over the surface (pressure), thus minimizing the risk of their abrasion, fragmentation, and creep. Abrasion and fragmentation of a polyethylene insert compromise the congruity of an implant, decreasing its resistance to dislocation. Under such circumstances, the implant should be replaced as soon as possible. Unfortunately, in THA, a higher diameter of the head decreases the range of motion in joints. Its impingement with the acetabular edge in extreme joint positions can lever the head, leading to dislocation.
Heads of higher diameter (eg, 32 mm) conflict with the acetabulum easier than smaller ones (28 mm). Moreover, their application imposes the use of polyethylene inserts of a smaller thickness, jeopardizing its durability [60–62]. Therefore, according to Kelley et al [63], each size of the head should be assigned to an accurate diameter of the acetabulum. Thus, heads of 22 mm diameter could be used with an acetabulum with a diameter up to 50 mm; heads of 26 mm in diameter are suitable with acetabular head diameters of 52 of 54 mm; heads of 28 mm in diameter are suitable with acetabular head diameters of 56 to 60 mm; and a head diameter of 32 mm requires an acetabulum with a diameter greater than 62 mm. Also noteworthy, the relationship between the diameter of the prosthesis head and the width of the neck of its stem should be preserved, as a combination of a small head with a wide neck of the stem increases the risk of implant dislocation [64].
The most common complication of THA is dislocation manifested by instability of the prosthesis, which requires further revision procedures. To avoid the risk of instability, the concept of dual mobility of hip prostheses has been developed. Multiple studies have shown that dual mobility has a statistically significant lower incidence of dislocations, when compared to standard THA. Its use is particularly promising in patients at high risk of femoral neck fractures. Dual mobility is less expensive and more usable than standard THA bearings [6,65].
Conclusions
In conclusion, the idea of implant choice individualization involving the selection of implants that would be most suitable for a patient undergoing THA and his or her activity level and expectations is becoming increasingly popular. A careful biomechanical analysis has shown that widely accepted rules of the recommended implant selection and implantation do not exclude the conflict between its elements or between the femur and the pelvis. The “safety area” introduced by Lewinnek (inclination 40±10° and anteversion 15±10°) of acetabulum positioning does not exclude the risk of ischiofemoral conflict, despite the fact that its placement outside this zone is responsible for up to 70% of dislocations [66]. A careful and delicate preparation of tissues, preserving muscles and their attachments, avoiding the release of muscle attachments and osteotomies, and their careful reattachments and stabilization avoid later dysfunctions leading to dislocation. Muscular insufficiency, when present, as well as joint congruency could be improved by the correction of an implant offset. Proper postoperative care focused on elaboration and strengthening of the desired locomotor habits, patient education on implant displacement and adequate preventive measures, risk minimization, and the negative impact of concomitant diseases that increase the risk of additional injuries can prevent this complication.
References
1. Gausden EB, Parhar HS, Popper JE, Risk factors for early dislocation following primary elective total hip arthroplasty: J Arthroplasty, 2018; 33(5); 1567-71
2. Lu Y, Xiao H, Xue F, Causes of and treatment options for dislocation following total hip arthroplasty: Exp Ther Med, 2019; 18(3); 1715-22
3. Rondon AJ, Tan TL, Schlitt PK, Total joint arthroplasty in patients with Parkinson’s disease: Survivorship, outcomes, and reasons for failure: J Arthroplasty, 2018; 33(4); 1028-32
4. Talbot NJ, Brown JH, Treble NJ, Early dislocation after total hip arthroplasty: Are postoperative restrictions necessary?: J Arthroplasty, 2002; 17(8); 1006-8
5. Cabanela ME, Weber M, Total hip arthroplasty in patients with neuromuscular disease: Instr Course Lect, 2000; 49; 163-68
6. Pituckanotai K, Arirachakaran A, Tuchinda H, Risk of revision and dislocation in single, dual mobility and large femoral head total hip arthroplasty: Systematic review and network meta-analysis: Eur J Orthop Surg Traumatol, 2018; 28(3); 445-55
7. Bhaskar D, Rajpura A, Board T, Current concepts in acetabular positioning in total hip arthroplasty: Indian J Orthop, 2017; 51(4); 386-96
8. Meermans G, Doorn JV, Kats JJ, Restoration of the centre of rotation in primary total hip arthroplasty: The influence of acetabular floor depth and reaming technique: Bone Joint J, 2016; 98-B; 1597-603
9. Fessy MH, Putman S, Viste A, What are the risk factors for dislocation in primary total hip arthroplasty? A multicenter case-control study of 128 unstable and 438 stable hips: Orthop Traumatol Surg Res, 2017; 103(5); 663-68
10. Dargel J, Oppermann J, Brüggemann GP, Eysel P, Dislocation following total hip replacement: Dtsch Arztebl Int, 2014; 111(51–52); 884-90
11. Wang T, Shao L, Xu W, Comparison of morphological changes of gluteus medius and abductor strength for total hip arthroplasty via posterior and modified direct lateral approaches: Int Orthop, 2019; 43(11); 2467-75
12. Masonis JL, Bourne RB, Surgical approach, abductor function, and total hip arthroplasty dislocation: Clin Orthop Relat Res, 2002; 405; 46-53
13. Prietzel T, Hammer N, Schleifenbaum SThe impact of capsular repair on the dislocation rate after primary total hip arthroplasty: A retrospective analysis of 1972 cases: Z Orthop Unfall, 2014; 152(2); 130-43 [in German]
14. Jurkutat J, Zajonz D, Sommer G, The impact of capsular repair on the risk for dislocation after revision total hip arthroplasty – a retrospective cohort-study of 259 cases: BMC Musculoskelet Disord, 2018; 19(1); 314
15. Perka C, Haschke F, Tohtz SDislocation after total hip arthroplasty: Z Orthop Unfall, 2012; 150(2); 89-105 [in German]
16. Patel PD, Potts A, Froimson MI, The dislocating hip arthroplasty: Prevention and treatment: J Arthroplasty, 2007; 22(4 Suppl 1); 86-90
17. Al-Amiry B, Mahmood S, Krupic F, Sayed-Noor A, Leg lengthening and femoral-offset reduction after total hip arthroplasty: Where is the problem – stem or cup positioning?: Acta Radiol, 2017; 58(9); 1125-31
18. Spina M, Scalvi A, Periprosthetic fractures of the proximal femur within first year of the index hip prosthesis: Acta Biomed, 2020; 91(3); e2020060
19. McKibbin B, Anatomical factors in the stability of the hip joint in the newborn: J Bone Joint Surg Br, 1970; 52(1); 148-59
20. Ranawat CS, Maynard MJ, Modern techniques of cemented total hip arthroplasty: Tech Orthopedics, 1991; 6; 17-25
21. Dorr LD, Malik A, Dastane M, Wan Z, Combined anteversion technique for total hip arthroplasty: Clin Orthop Relat Res, 2009; 467(1); 119-27
22. Bissias C, Kaspiris A, Kalogeropoulos A, Factors affecting the incidence of postoperative periprosthetic fractures following primary and revision hip arthroplasty: A systematic review and meta-analysis: J Orthop Surg Res, 2021; 16(1); 15
23. Saglam Y, Ozturk I, Cakmak MF, Total hip arthroplasty in patients with ankylosing spondylitis: Midterm radiologic and functional results: Acta Orthop Traumatol Turc, 2016; 50(4); 443-47
24. Kumar A, Nagai H, Oakley J, Short to long term outcomes of 154 cemented total hip arthroplasties in ankylosing spondylitis: J Clin Orthop Trauma, 2020; 14; 34-39
25. Esposito CI, Carroll KM, Sculco PK, Total hip arthroplasty patients with fixed spinopelvic alignment are at higher risk of hip dislocation: J Arthroplasty, 2018; 33(5); 1449-54
26. Heckmann N, McKnight B, Stefl M, Late dislocation following total hip arthroplasty: Spinopelvic imbalance as a causative factor: J Bone Joint Surg Am, 2018; 100(21); 1845-53
27. Gausden EB, Parhar HS, Popper JE, Risk factors for early dislocation following primary elective total hip arthroplasty: J Arthroplasty, 2018; 33; 1567-71
28. Lu Y, Xiao H, Xue F, Causes of and treatment options for dislocation following total hip arthroplasty: Exp Ther Med, 2019; 18(3); 1715-22
29. Zeckey C, Hildebrand F, Frink M, Krettek C, Heterotopic ossifications following implant surgery-epidemiology, therapeutical approaches and current concepts: Semin Immunopathol, 2011; 33(3); 273-86
30. Sanders S, Tejwani N, Egol KA, Traumatic hip dislocation – a review: Bull NYU Hosp Jt Dis, 2010; 68(2); 91-96
31. Queally JM, Abdulkarim A, Mulhall KJ, Total hip replacement in patients with neurological conditions: J Bone Joint Surg Br, 2009; 91(10); 1267-73
32. Soong M, Rubash HE, Macaulay W, Dislocation after total hip arthroplasty: J Am Acad Orthop Surg, 2004; 12(5); 314-21
33. Cho YJ, Lee CH, Chun YS, Rhyu KH, Outcome after cementless total hip arthroplasty for arthritic hip in patients with residual poliomyelitis: A case series: Hip Int, 2016; 26(5); 458-61
34. Kunutsor SK, Barrett MC, Beswick AD, Risk factors for dislocation after primary total hip replacement: Meta-analysis of 125 studies involving approximately five million hip replacements: Lancet Rheumatol, 2019; 1(2); e111-21
35. Fackler CD, Poss R, Dislocation in total hip arthroplasties: Clin Orthop Relat Res, 1980; 151; 169-78
36. Herrmann S, Kluess D, Kaehler M, A novel approach for dynamic testing of total hip dislocation under physiological conditions: PLoS One, 2015; 10(12); e0145798
37. Krismer M, Sports activities after total hip arthroplasty: EFORT Open Rev, 2017; 2(5); 189-94
38. Aziz KT, Best MJ, Naseer Z, The association of delirium with perioperative complications in primary elective total hip arthroplasty: Clin Orthop Surg, 2018; 10(3); 286-91
39. Kheir MM, Kheir YNP, Tan TL, Increased complications for schizophrenia and bipolar disorder patients undergoing total joint arthroplasty: J Arthroplasty, 2018; 33(5); 1462-66
40. Tsai CH, Muo CH, Hung CH, Disorder-related risk factors for revision total hip arthroplasty after hip hemiarthroplasty in displaced femoral neck fracture patients: A nationwide population-based cohort study: J Orthop Surg Res, 2016; 11(1); 66
41. Liu Q, Cheng X, Yan D, Zhou Y, Plain radiography findings to predict dislocation after total hip arthroplasty: J Orthop Translat, 2019; 18; 1-6
42. Ding ZC, Zeng WN, Mou P, Risk of dislocation after total hip arthroplasty in patients with Crowe type IV developmental dysplasia of the hip: Orthop Surg, 2020; 12(2); 589-600
43. Elkins JM, Daniel M, Pedersen DR, Morbid obesity may increase dislocation in total hip patients: A biomechanical analysis: Clin Orthop Relat Res, 2013; 471(3); 971-80
44. Safran MR, Lopomo N, Zaffagnini S, In vitro analysis of peri-articular soft tissues passive constraining effect on hip kinematics and joint stability: Knee Surg Sports Traumatol Arthrosc, 2013; 21(7); 1655-63
45. Fetto JF, A dynamic model of hip joint biomechanics: The contribution of soft tissues: Adv Orthop, 2019; 2019; 5804642
46. Bergin PF, Doppelt JD, Kephart CJ, Comparison of minimally invasive direct anterior versus posterior total hip arthroplasty based on inflammation and muscle damage markers: J Bone Joint Surg Am, 2011; 93(15); 1392-98
47. Shi XT, Li CF, Han Y, Total hip arthroplasty for Crowe type IV hip dysplasia: Surgical techniques and postoperative complications: Orthop Surg, 2019; 11(6); 966-73
48. Berry DJ, Berger RA, Callaghan JJ, Symposium: Minimally invasive total hip arthroplasty: J Bone Joint Surg, 2003; 85(11); 2235-46
49. Xie J, Zhang H, Wang L, Comparison of supercapsular percutaneously assisted approach total hip versus conventional posterior approach for total hip arthroplasty: A prospective, randomized controlled trial: J Orthop Surg Res, 2017; 12(1); 138
50. Blom AW, Hunt LP, Matharu GS, The effect of surgical approach in total hip replacement on outcomes: An analysis of 723,904 elective operations from the National Joint Registry for England, Wales, Northern Ireland and the Isle of Man: BMC Med, 2020; 18(1); 242
51. Greber EM, Pelt CE, Gililland JM, Challenges in total hip arthroplasty in the setting of developmental dysplasia of the hip: J Arthroplasty, 2017; 32; S38-44
52. Schmidt AH, Leighton R, Parvizi J, Optimal arthroplasty for femoral neck fractures: is total hip arthroplasty the answer?: J Orthop Trauma, 2009; 23(6); 428-33
53. Li L, Xiang S, Wang B, Dead muscle tissue promotes dystrophic calcification by lowering circulating TGF-β1 level: Bone Joint Res, 2020; 9(11); 742-50
54. Pincus D, Jenkinson R, Paterson M, Association between surgical approach and major surgical complications in patients undergoing total hip arthroplasty: JAMA, 2020; 323(11); 1070-76
55. Ertaş ES, Tokgözoğlu AM, Dislocation after total hip arthroplasty: Does head size really matter?: Hip Int, 2021; 31(3); 320-27
56. Miettinen SSA, Mäkinen TJ, Laaksonen I, Dislocation of large-diameter head metal-on-metal total hip arthroplasty and hip resurfacing arthroplasty: Hip Int, 2019; 29(3); 253-61
57. Fahad S, Nawaz Khan MZ, Aqueel T, Hashmi P, Comparison of bipolar hemiarthroplasty and total hip arthroplasty with dual mobility cup in the treatment of old active patients with displaced neck of femur fracture: A retrospective cohort study: Ann Med Surg (Lond), 2019; 45; 62-65
58. Park KS, Seon JK, Lee KB, Yoon TR, Total hip arthroplasty using large-diameter metal-on-metal articulation in patients with neuromuscular weakness: J Arthroplasty, 2014; 29(4); 797-801
59. Liu Y, Sun J, Wang TEffectiveness of total hip arthroplasty in the treatment of involved hips in patients with ankylosing spondylitis: Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi, 2017; 31(1); 25-30 [in Chinese]
60. Crowninshield RD, Maloney WJ, Wentz DH, Biomechanics of large femoral heads: What they do and don’t do: Clin Orthop Relat Res, 2004; 429; 102-7
61. Stroh DA, Issa K, Johnson AJ, Reduced dislocation rates and excellent functional outcomes with large-diameter femoral heads: J Arthroplasty, 2013; 28(8); 1415-20
62. Kung PL, Ries MD, Effect of femoral head size and abductors on dislocation after revision THA: Clin Orthop Relat Res, 2007; 465; 170-74
63. Kelley SS, Lachiewicz PF, Hickman JM, Paterno SM, Relationship of femoral head and acetabular size to the prevalence of dislocation: Clin Orthop Relat Res, 1998; 355; 163-70
64. Kotwal RS, Ganapathi M, John A, Outcome of treatment for dislocation after primary total hip replacement: J Bone Joint Surg Br, 2009; 91(3); 321-26
65. Cuthbert R, Wong J, Mitchell P, Kumar Jaiswal P, Dual mobility in primary total hip arthroplasty: Current concepts: EFORT Open Rev, 2019; 4(11); 640-46
66. Lewinnek GE, Lewis JL, Tarr R, Dislocations after total hip-replacement arthroplasties: J Bone Joint Surg Am, 1978; 60(2); 217-20
In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387