17 May 2022: Database Analysis
Relationship Between C-Reactive Protein and Respiratory Diseases in Patients with Type 2 Diabetic Retinopathy
Kejia Chen1BCDEF, Jiamin Yan1BDF, Ling Wu1AD, Xingbo Gu1ACDEG*DOI: 10.12659/MSM.935807
Med Sci Monit 2022; 28:e935807
Abstract
BACKGROUND: The aim of this study was to explore the relationship between C-reactive protein (CRP) and respiratory diseases in patients with diabetic retinopathy.
MATERIAL AND METHODS: We identified 855 patients with diabetic retinopathy who met the inclusion criteria from the “Diabetes Complications Data Set” in the National Population Health Data Center. We divided patients into 3 groups according to CRP tertiles: Q1 (<0.3 mg/dL), Q2 (0.3-0.35 mg/dL), and Q3 (>0.35 mg/dL). A multivariate logistic regression model was used to evaluate the relationship between CRP and respiratory diseases. The area under the receiver operating characteristic (ROC) curve was used to investigate the independent predictive effect of CRP on respiratory diseases.
RESULTS: Of the 855 patients with diabetic retinopathy, 137 (16%) had respiratory diseases. Prevalence of respiratory diseases gradually increased with an increase in CRP level (P for trend=0.001). With CRP as a continuous variable in the logistic regression model adjusted for confounding factors (model 3), the odds ratio (OR) per 1 standard deviation increment of CRP was 1.25 (95% CI 1.07-1.45, P=0.004). When the lowest CRP tertile group was used as the reference group, the OR of the highest CRP tertile group was 1.99 (95% CI 1.22-1.3.26, P=0.006). Adding CRP to the risk factor model increased the area under the ROC curve (0.68 vs 0.65, P=0.017). Subgroup analysis showed that the relationship between CRP and respiratory diseases had no potential heterogeneity among subgroups.
CONCLUSIONS: CRP can be used as an effective biomarker in predicting risk of respiratory diseases in patients with diabetic retinopathy.
Keywords: C-Reactive Protein, Diabetic Retinopathy, Respiratory Tract Diseases, Diabetes Mellitus, Type 2, Humans, ROC Curve
Background
Type 2 diabetes mellitus is characterized by hyperglycemia, insulin resistance, and relative insulin deficiency [1]. In 2015, the estimated number of patients with type 2 diabetes worldwide reached 392 million (equivalent to approximately 6% of the world’s population), including patients in developed and developing countries [2]. Guidelines for the prevention and treatment of type 2 diabetes mellitus in China show that the prevalence is increasing yearly and reached 11.2% in 2017. Type 2 diabetes mellitus has the second highest prevalence of chronic diseases after hypertension. In addition, its comorbidities have contributed to the increased disease burden and social burden of Chinese residents. Diabetic retinopathy is a medical condition in which the retina is damaged by diabetes. It is one of the leading causes of blindness in developed countries. In the United States, diabetic retinopathy is one of the leading causes of blindness in people aged 20 to 64 years, accounting for 12% of all new cases of blindness each year [3]. A previous study showed that the longer the duration of diabetes, the higher the chance of diabetic retinopathy occurring as a complication [4].
The mechanism of diabetes comorbidity is as follows. Hemodynamic and metabolic disturbances caused by the metabolism lead to impaired functions of macrovascular, microvascular, and inflammatory factors [5]. In recent years, many studies have shown that metabolic glucose abnormalities share a common pathophysiological background with respiratory diseases [6]. The risk of asthma, chronic obstructive pulmonary disease (COPD), lung injury, and respiratory infections in patients with diabetes is significantly increased [7]. C-reactive protein (CRP) is a cyclic pentameric protein found in plasma, and its concentration increases with inflammation [8]. Studies have suggested that hyperglycemia may stimulate the release of inflammatory cytokines [9]. As an inflammatory marker in clinical practice, CRP is sensitive and nonspecific [10]. Moreover, it can be used as a sensitive indicator for the diagnosis and efficacy evaluation of respiratory infections [11]. Nevertheless, the relationship between CRP and respiratory diseases remains unclear in patients with type 2 diabetes mellitus and the complication of retinopathy. In addition, normal concentrations of CRP in healthy adults range from 0 to 0.8 mg/dL, whereas there are few studies on the CRP range in patients with type 2 diabetes mellitus retinopathy (especially those with respiratory diseases as a primary outcome indicator). Therefore, this study aimed to explore the relationship between CRP levels and respiratory diseases in patients with type 2 diabetes mellitus retinopathy.
Material and Methods
ETHICS:
This study was based on publicly available data from the “Diabetes Complications Data Set” in the National Population Health Data Center and did not involve interaction with human participants or the use of personally identifiable information. The study did not require informed consent, and the author obtained a data use agreement from the National Clinical Medical Science Data Center (301 Hospital).
Results
For the 855 patients with diabetic retinopathy included in this study, the mean age was 56.7 years (SD, 10.6 years). Men accounted for 64.1%. The average level of BMI was 26.5 kg/m2 (SD, 3.4 kg/m2). A total of 648 patients had hypertension (75.7%), 157 had hyperlipidemia (18.3%), 505 had atherosclerosis (85.8%), 87 had stroke (10.1%), 53 had arrhythmia (6.1%), and 258 had lower extremity arteries (30.1%). In the group of patients with respiratory diseases, the levels of alkaline phosphatase, creatinine, uric acid, and CRP were significantly higher than those in the patient group without respiratory diseases. The serum albumin level was higher in the group of patients without respiratory diseases (Table 1).
Among the 855 patients with diabetic retinopathy, 137 patients had respiratory diseases (16.0%). The median level of CRP was 0.32 mg/dL (0.19–0.40, IQR). Figure 2 shows that the overall prevalence of respiratory diseases tended to increase significantly with the increase of CRP level (
Table 2 shows the odds ratios (ORs) and 95% confidence intervals (CIs) of the relationship between CRP and respiratory diseases under different logistic regression models. In the logistic regression model adjusted for confounding factors (model 3), the CRP level increased by 1 SD and the OR value was 1.25 (95% CI 1.07–1.45,
When adding CRP level to multivariate models including age, sex, hypertension, hyperlipidemia, atherosclerosis, stroke, serum albumin, creatinine, and total cholesterol, the ROC AUC before and after were 0.65 (95% CI 0.62–0.67) and 0.68 (95% CI 0.65–0.70), respectively. The difference was statistically significant when comparing the area under the curve (
Figure 4 shows the results when CRP and respiratory disease were analyzed in subgroups according to age, sex, BMI, hypertension, hyperlipidemia, stroke, coronary heart disease, atherosclerosis, and lower extremity artery disease. CRP level was significantly associated with respiratory diseases in most subgroups. However, no significant direct interaction of CRP level with any subgroup variables was found (
Discussion
The major findings of the present study were that CRP level was an independent risk factor for respiratory diseases in patients with diabetic retinopathy. CRP levels were significantly positively correlated with the prevalence of respiratory diseases after adjusting for potential confounding factors. Patients with CRP levels in the highest tertile group (Q3: >0.35 mg/dL) had 1.99 times the risk of respiratory disease than the lowest tertile group (Q1: <0.30 mg/dL). This association did not change under different models and subgroup analyses. In addition, the model’s ability to predict respiratory diseases was improved by adding CRP level to the well-defined risk factor models for patients with diabetic retinopathy.
Although a few studies on the relationship between CRP and respiratory-related diseases have been reported [14], there are very few studies on the relationship between CRP and the respiratory system in patients with diabetic retinopathy, and in particular, no relevant studies with larger sample sizes have been reported in a Chinese patient population. The studies related to type 2 diabetes have simply linked type 2 diabetes with respiratory diseases or linked type 2 diabetic retinopathy with respiratory diseases. Meanwhile, there is a lack of studies about the relationship between CRP and respiratory diseases in type 2 diabetic retinopathy [15–17]. Therefore, the present study can fill the gaps in this area of research to a certain extent, thus providing localized evidence to support the prevention and treatment strategies in related fields. Our research results also confirm that there is an independent positive correlation between CRP levels and respiratory diseases in patients with diabetic retinopathy in China. Furthermore, CRP can be used as a potential biomarker of respiratory diseases in patients with type 2 diabetic retinopathy.
At present, the exact mechanism by which elevated CRP levels cause respiratory disease remains unclear. One of the manifestations of chronic respiratory diseases is skeletal muscle dysfunction and emaciation [18]. As the duration of the disease increases, the patient loses exercise endurance, thereby exhibiting fatigue and dyspnea at the lowest level of exertion [19]. It has been proposed that these symptoms constitute an independent process that leads to the systemic inflammatory burden of the disease [20]. As an acute phase protein, CRP is released by hepatocytes, and its elevation can be a sign of the severity of systemic inflammation [21]. It has been shown that as CRP levels increase, muscle activity increases, and walking distance decreases within 6 min [22]. Therefore, the prognosis of these patients can be indirectly reflected by CRP levels measured under stable conditions.
There were several limitations in this study. First, as an observational study, the results did not explain the causal relationship between the 2 variables but only speculated on its possible correlation to a certain extent. Second, data on CRP levels at the time of patient admission were used in this study, and CRP levels can change over time. This prevented the assessment of relationship between changes in CRP levels over time and respiratory diseases. Third, we collected only total respiratory disease outcomes and could not explain the relationship of CRP with specific respiratory diseases, such as COPD and other clinical outcomes. Fourth, patients excluded from the study due to lack of CRP measurement results may differ in some characteristics from those selected, which may have caused research bias. Fifth, previous studies have confirmed a strong association between CRP and diabetic retinopathy [23]. The degree of diabetic retinopathy in the patients may affect the level of CRP. The stage of diabetic retinopathy may be an important confounding factor in this study. Unfortunately, the variable of diabetic retinopathy stage was not collected in this dataset. Sixth, although as many covariates as possible that affect the relationship between CRP and respiratory diseases were collected, there are still other important confounding factors, including smoking, air pollution, and occupational exposure, that could not be collected. Finally, this study was conducted in a single center with a high level of clinical diagnosis and treatment, and people with various characteristics may not have been included as research participants. Therefore, the results of this study need to be further confirmed by a multicenter study.
Conclusions
Elevated CRP levels are independently associated with respiratory disease in patients with type 2 diabetic retinopathy. CRP can be used as an effective biomarker in the prediction of respiratory disease risk in patients with type 2 diabetic retinopathy. The potential mechanisms involved in the relationship between CRP and respiratory diseases need to be determined through further research.
Figures
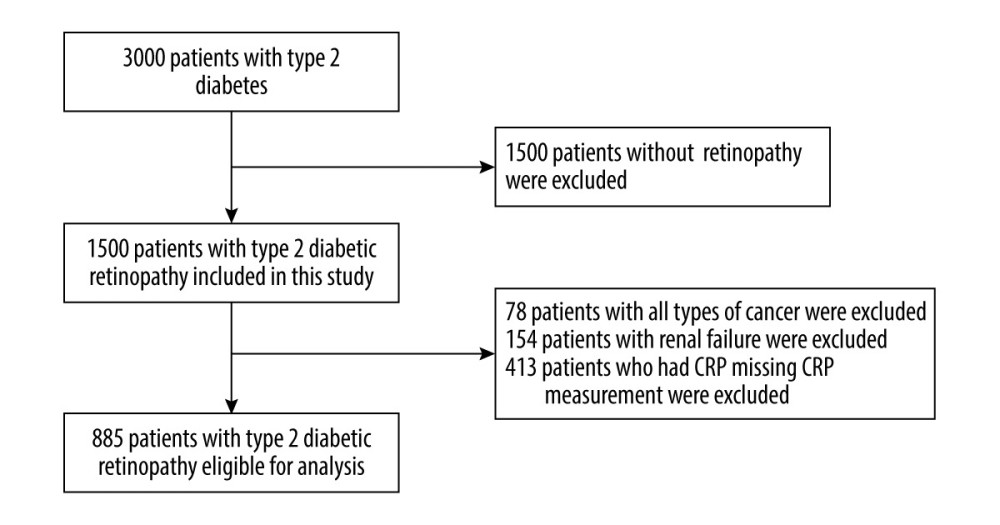 Figure 1. Patient flow chart.
Figure 1. Patient flow chart. 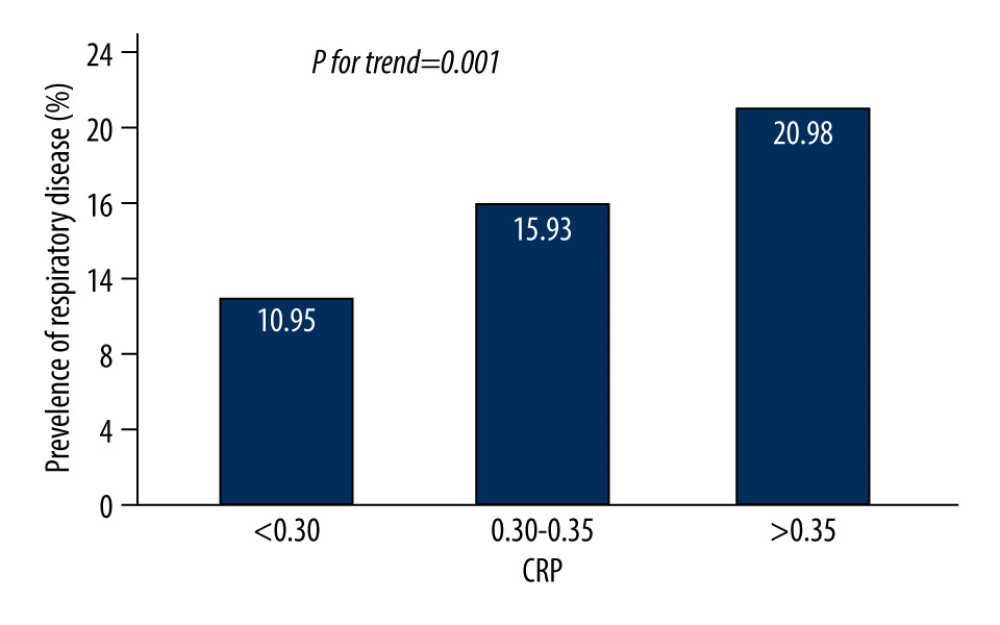 Figure 2. Prevalence of respiratory diseases based on the tertiles of C-reactive protein in patients with type 2 diabetic retinopathy.
Figure 2. Prevalence of respiratory diseases based on the tertiles of C-reactive protein in patients with type 2 diabetic retinopathy. 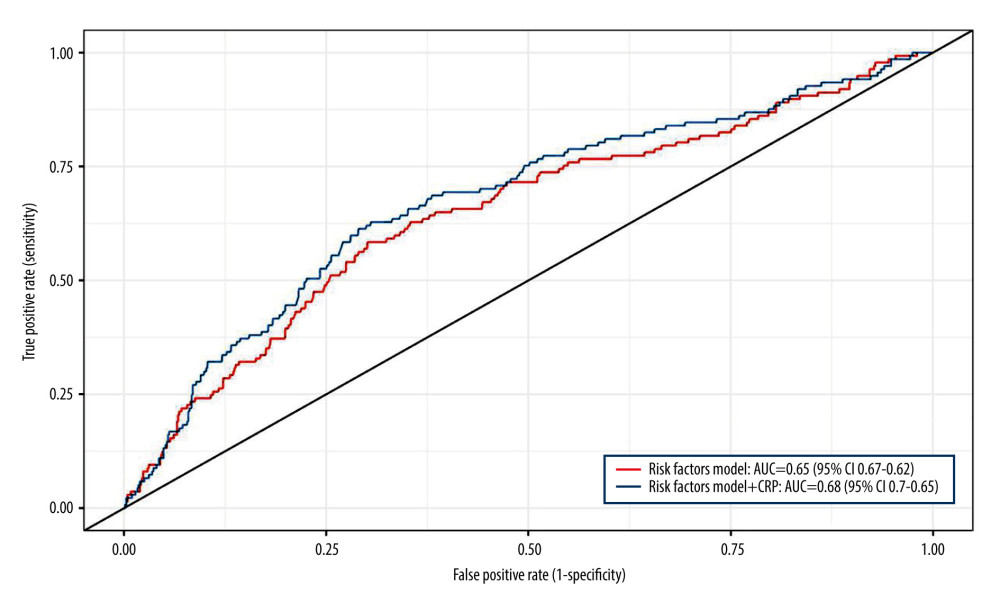 Figure 3. The area under the receiver operating characteristic curve of C-reactive protein in the prediction of respiratory diseases among patients with type 2 diabetic retinopathy.
Figure 3. The area under the receiver operating characteristic curve of C-reactive protein in the prediction of respiratory diseases among patients with type 2 diabetic retinopathy. 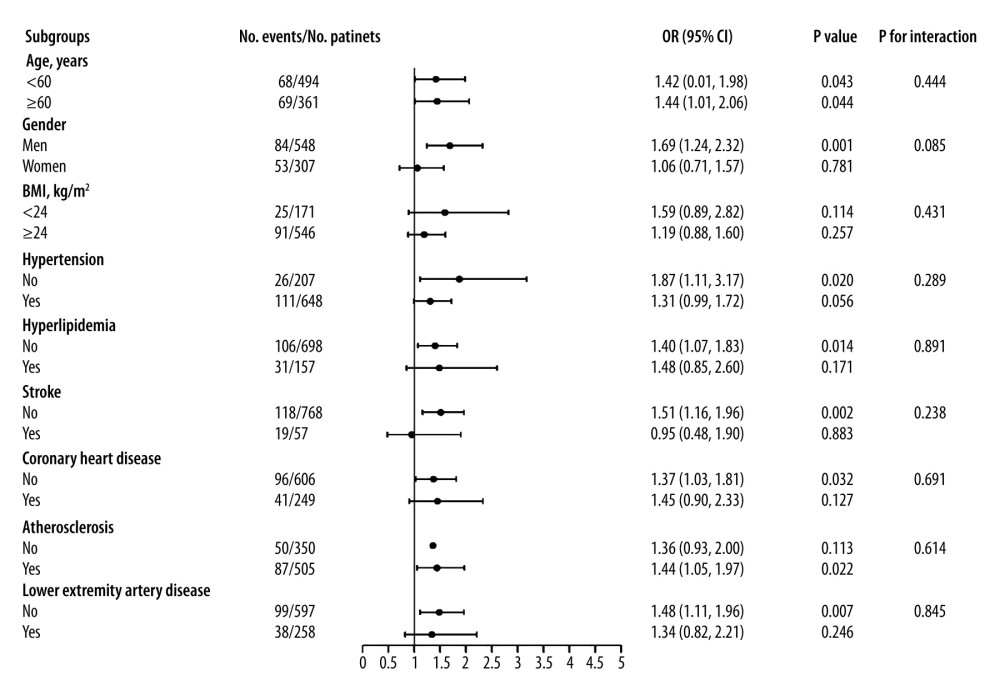 Figure 4. Forest plots of the odds ratios and 95% confidence intervals of C-reactive protein and respiratory diseases in subgroup analyses.
Figure 4. Forest plots of the odds ratios and 95% confidence intervals of C-reactive protein and respiratory diseases in subgroup analyses. References
1. Surampudi PN, John-Kalarickal J, Fonseca VA, Emerging concepts in the pathophysiology of type 2 diabetes mellitus: Mt Sinai J Med, 2009; 76(3); 216-26
2. Reddy KS, Global Burden of Disease Study 2015 provides GPS for global health 2030: Lancet, 2016; 388(10053); 1448-49
3. Engelgau MM, Geiss LS, Saaddine JB, The evolving diabetes burden in the United States: Ann Intern Med, 2004; 140(11); 945-50
4. Pan C-W, Wang S, Wang P, Diabetic retinopathy and health-related quality of life among Chinese with known type 2 diabetes mellitus: Qual Life Res, 2018; 27(8); 2087-93
5. Cade WT, Diabetes-related microvascular and macrovascular diseases in the physical therapy setting: Phys Ther, 2008; 88(11); 1322-35
6. Visca D, Pignatti P, Spanevello A, Relationship between diabetes and respiratory diseases – clinical and therapeutic aspects: Pharmacol Res, 2018; 137; 230-35
7. Sevenoaks MJ, Stockley RA, Chronic Obstructive Pulmonary Disease, inflammation and co-morbidity – a common inflammatory phenotype?: Respir Res, 2006; 7(1); 1-9
8. Pepys MB, Hirschfield GM, C-reactive protein: A critical update: J Clin Invest, 2003; 111(12); 1805-12
9. Haidet J, Cifarelli V, Trucco M, Luppi P, C-peptide reduces pro-inflammatory cytokine secretion in LPS-stimulated U937 monocytes in condition of hyperglycemia: J Inflamm Res, 2012; 61(1); 27-35
10. Korppi M, Non-specific host response markers in the differentiation between pneumococcal and viral pneumonia: What is the most accurate combination?: Pediatr Int, 2004; 46(5); 545-50
11. Deron S, C-reactive protein: An inflammatory biomarker in clinical practice: The Journal of Lancaster General Hospital, 2007; 2(2); 63
12. Idiopathic B, Endocrinopathies D, Report of the expert committee on the diagnosis and classification of diabetes mellitus: Diabetes Care, 2003; 26; S5-20
13. Wilkinson C, Ferris FL, Klein RE, Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales: Ophthalmology, 2003; 110(9); 1677-82
14. Gallego M, Pomares X, Capilla S, C-reactive protein in outpatients with acute exacerbation of COPD: Its relationship with microbial etiology and severity: Int J Chron Obstruct Pulmon Dis, 2016; 11; 2633
15. Meteran H, Backer V, Kyvik KO, Comorbidity between chronic obstructive pulmonary disease and type 2 diabetes: A nation-wide cohort twin study: Respir Med, 2015; 109(8); 1026-30
16. Malte Rasmussen S, Brok J, Backer V, Association between chronic obstructive pulmonary disease and type 2 diabetes: A systematic review and meta-analysis: COPD: J Chronic Obstr Pulm Dis, 2018; 15(5); 526-35
17. Lee CTC, Mao IC, Lin CH, Chronic obstructive pulmonary disease: A risk factor for type 2 diabetes: A nationwide population-based study: Eur J Clin Invest, 2013; 43(11); 1113-19
18. Wouters EF, Creutzberg EC, Schols AM, Systemic effects in COPD: Chest, 2002; 121(5); 127S-30S
19. Sin DD, Wu L, Man SP, The relationship between reduced lung function and cardiovascular mortality: A population-based study and a systematic review of the literature: Chest, 2005; 127(6); 1952-59
20. Maltais F, Skeletal muscles in chronic airflow obstruction: Why bother?: Am J Respir, 2003; 168(8); 916-17
21. Ghobadi H, Fouladi N, Beukaghazadeh K, Ansarin K, Association of high sensitive CRP level and COPD assessment test scores with clinically important predictive outcomes in stable COPD patients: Tanaffos, 2015; 14(1); 34
22. Sugawara K, Takahashi H, Kasai C, Effects of nutritional supplementation combined with low-intensity exercise in malnourished patients with COPD: Respir Med, 2010; 104(12); 1883-89
23. Song J, Chen S, Liu X, Relationship between C-reactive protein level and diabetic retinopathy: A systematic review and meta-analysis: PLoS One, 2015; 10(12); e0144406
Figures
 Figure 1. Patient flow chart.
Figure 1. Patient flow chart. Figure 2. Prevalence of respiratory diseases based on the tertiles of C-reactive protein in patients with type 2 diabetic retinopathy.
Figure 2. Prevalence of respiratory diseases based on the tertiles of C-reactive protein in patients with type 2 diabetic retinopathy. Figure 3. The area under the receiver operating characteristic curve of C-reactive protein in the prediction of respiratory diseases among patients with type 2 diabetic retinopathy.
Figure 3. The area under the receiver operating characteristic curve of C-reactive protein in the prediction of respiratory diseases among patients with type 2 diabetic retinopathy. Figure 4. Forest plots of the odds ratios and 95% confidence intervals of C-reactive protein and respiratory diseases in subgroup analyses.
Figure 4. Forest plots of the odds ratios and 95% confidence intervals of C-reactive protein and respiratory diseases in subgroup analyses. Tables
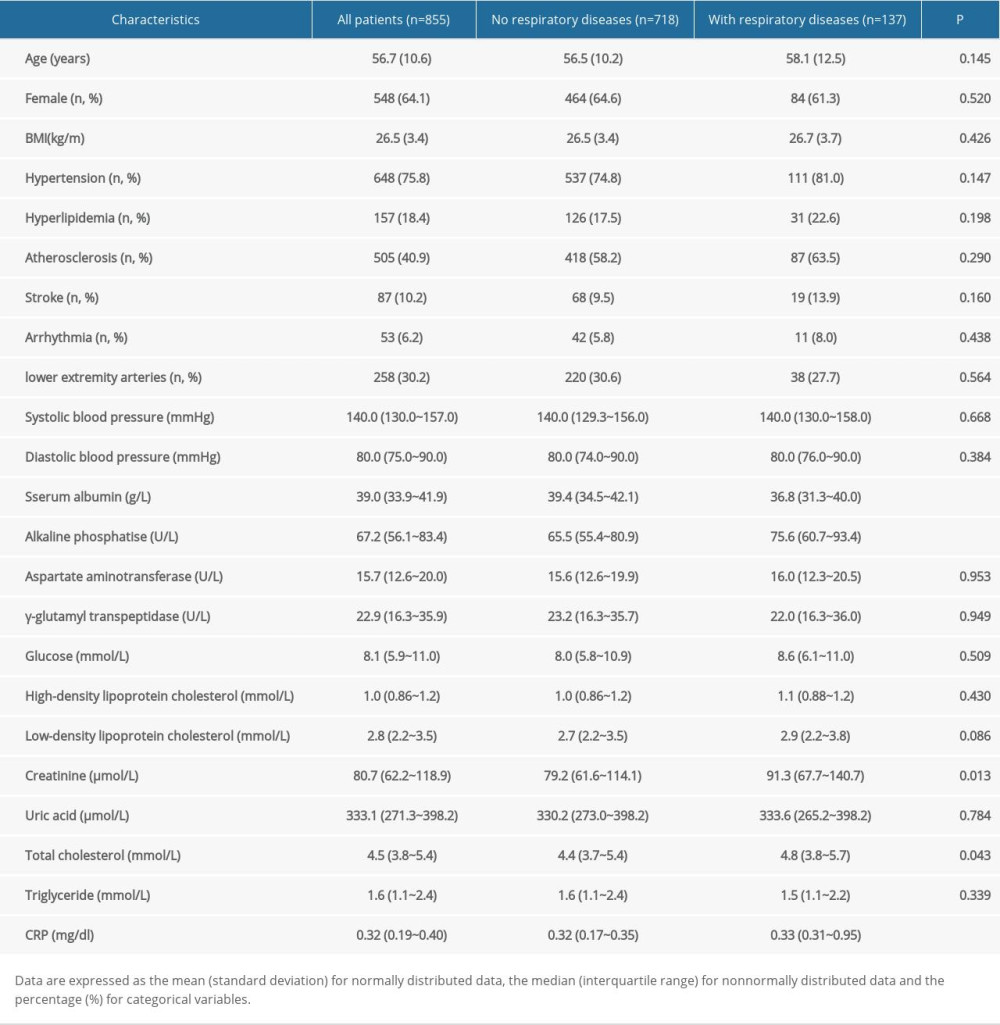 Table 1. Characteristics of patients with diabetic retinopathy.
Table 1. Characteristics of patients with diabetic retinopathy.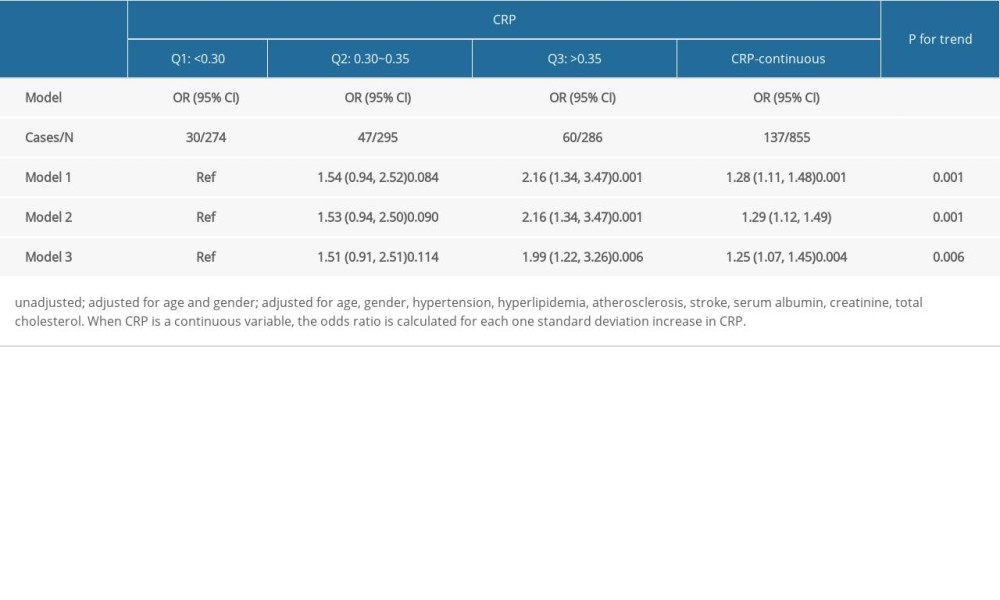 Table 2. Odds ratios and 95% confidence intervals of respiratory diseases according to tertiles of C-reactive protein levels among patients with type 2 diabetic retinopathy.
Table 2. Odds ratios and 95% confidence intervals of respiratory diseases according to tertiles of C-reactive protein levels among patients with type 2 diabetic retinopathy. Table 1. Characteristics of patients with diabetic retinopathy.
Table 1. Characteristics of patients with diabetic retinopathy. Table 2. Odds ratios and 95% confidence intervals of respiratory diseases according to tertiles of C-reactive protein levels among patients with type 2 diabetic retinopathy.
Table 2. Odds ratios and 95% confidence intervals of respiratory diseases according to tertiles of C-reactive protein levels among patients with type 2 diabetic retinopathy. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








