27 March 2022: Clinical Research
A Faster, Novel Technique to Detect COVID-19 Neutralizing Antibodies
Wei-Huai ChiuDOI: 10.12659/MSM.935812
Med Sci Monit 2022; 28:e935812
Abstract
BACKGROUND: The COVID-19 pandemic has spread globally in a short period of time. It is known that antibody (nAb) level can effectively predict vaccine efficacy, which leads to the exploration of vaccine trials for efficacy assessment. Thus, the current study aimed to develop a platform to quantify nAb levels faster, at lower cost, and with better efficiency.
MATERIAL AND METHODS: A total of 69 sera samples were collected for the research, 28 of which were from unvaccinated participants. The other 27 samples and the remaining 14 samples were from the participants who had received the first and second dose, respectively, of AZ vaccine 1 month before. With cPass assays (Genscript cPass nAb ELISA assay) used as a criterion standard and lateral flow immunoassay kit (Healgen Scientific - LFIA test kit) coupled with a spectrometer (LFIA+S) for checking each specimen, we aimed to detect the presence of neutralizing antibodies in sera and to confirm the relationship between the inhibition rate from cPass assays and the nAb index from the LFIA+S.
RESULTS: Data analysis of the research were taken from the certified ELISA and LFIA+S, which indicated a high consistency (Pearson’s r =0.864; ICC=0.90138) between the 2 methods.
CONCLUSIONS: The dataset demonstrated that LFIA+S was affordable, had a strong correlation with results of the cPass nAbs detection kit, and has potential clinical applications, with an exclusive feature that allows non-experts to use it with ease. It is believed that the proposed platform can be promoted in the near future.
Keywords: Antibodies, Neutralizing, COVID-19, Self Efficacy, Spectrum Analysis, Antibodies, Viral, COVID-19, Humans, Immunoassay, Pandemics, SARS-CoV-2
Background
Since the initial outbreak was reported, COVID-19 has been identified as a public health issue and has caused millions of infections and deaths globally [1–4]. However, there is a broad agreement that eliminating the virus is no longer feasible [5–7]. Increasing the vaccination rate has been recognized as the most effective measure against the global pandemic. Therefore, critical issues such as rapid evaluation of the efficacy of the vaccine are of urgent concern [8–10]. Recently, it has been reported that levels of neutralizing antibodies (nAbs) are highly predictive of immune protection from symptomatic SARS-CoV-2 infection. This is because nAbs can inhibit the interaction between the receptor-binding domain of the spike-1 protein (S1-RBD) and human angiotensin-converting enzyme 2 (h-ACE2) [11,12]. Currently, there are 2 standard methods available for nAbs detection. One is the 50% plaque reduction neutralization test (
On the other hand, the paper-based SARS-CoV-2 Neutralizing Antibody Test Kit (Healgen Scientific - LFIA test kit, Healgen Scientific, LLC, Houston, USA) shows several advantages, such as low cost, short processing time, and ease of use (it can be used by a non-expert), which make LFIA an ideal commercial kit to detect the nAbs [23,24]. However, as the LFIA test provides only qualitative results, the determination of nAbs level relies on the experimental operator’s subjective cognition. Therefore, a novel platform that integrates LFIA with a portable spectrometer (LFIA+S) was proposed in this research to increase sensitivity and accuracy. Furthermore, the detection method was upgraded from qualitative level to semi-quantitative level [25,26].
To determine if LFIA+S is a highly reliable method for nAbs detection, statistical analyses were performed to compare the effects of the proposed integrated platform and the normal criterion standard cPass neutralization antibody assay [27]. We found that LFIA+S results are strongly correlated with those of cPass and LFIA+S only costs around US $5 per test, which is affordable for general clinics or areas with insufficient medical care. Our aim was to provide a highly reliable platform to make it easier to detect the level l of nAbs for COVID-19 vaccine efficacy.
Material and Methods
ETHICS APPROVAL:
The protocol for this research was approved by the Institutional Review Board (IRB) of MacKay Memorial Hospital (IRB No: 21MMHIS141e) and Kaohsiung Medical University Chung-Ho Memorial Hospital (IRB No: KMUHIRB-F(I)-20200141). All of the participants understood the purpose of the study and agreed to sign the participant consent form prior to their participation.
SERUM SAMPLES:
A total of 69 serum samples were studied in a retrospective cohort study from June 2021 to November 2021. Results of the observational study conducted with medical personnel of MacKay Memorial Hospital and Kaohsiung Medical University Chung-Ho Memorial Hospital were included in this study. Among them, 28 serum samples were collected from the people who had not received vaccination yet; the other 27 sera and 14 sera were obtained from people who had received the first and second dose, respectively, of the AZ vaccine 1 month earlier, before the experiment.
SPECTRAL ANALYSIS SYSTEM:
The spectral analysis platform is equipped with a cassette designed for the LFIA test kit to detect the absorbance spectrum. The spectral chip provides high spectral resolution (3–5 nm), the results of which were demonstrated with a certain wavelength range (300 to 1100 nm). The real-time spectrum is used as the experimental reference for the primary absorbance wavelengths, which was to detect the use of this platform from 500 nm to 600 nm and 680 nm.
SARS-COV-2 NEUTRALIZING ANTIBODY LATERAL FLOW IMMUNOASSAY AND DETECTION (LFIA TEST KIT):
A commercially available SARS-CoV-2 Neutralizing Antibody Test Kit (Healgen Scientific – LFIA test kit, Healgen Scientific, LLC, Houston, USA) was used to detect the presence of neutralizing antibodies in sera. First, 25 μL of serum sample was loaded and mixed with 2 drops of the diluted buffer in the well for 10 min. The loaded test solutions can be driven through a conjugated pad by capillary force. As a competitive assay, the presence of neutralizing antibodies can be detected based on the signal intensity at the test line (T-line) and the control line (C-line), as shown in (Figure 1). This is because the neutralizing antibodies can inhibit the binding between the hACE-2 proteins (coated at T-line) and S1-RBD proteins (conjugated to colloidal gold nanoparticles and stored in a conjugation pad). In other words, the increase in neutralizing antibodies within a serum sample could lead to less binding of hACE-2 and S1-RBD/gold nanoparticles and make the T-line lighter. The testing results were considered invalid if the C-line did not appear during the 20-min waiting time.
NOVEL TECHNIQUE PLATFORM OF LATERAL FLOW IMMUNOASSAY COUPLED WITH SPECTROMETER:
In this research, a patent-pending testing platform was designed to demonstrate/display the result of LFIA, as shown in Figure 2. A specifically designed optical system was installed on the platform to reveal the absorbance spectrum of the gold nanoparticles (Figure 3) displayed on the test kit (T-line). The absorbance intensity (ΔA) of the gold nanoparticles can be calculated by the following formula and was later used to quantify the amounts of neutralizing antibodies in sera:
The signal intensity of the T and C-line can be calculated as ΔA T-line and ΔA C-line, respectively. The value of nAb can be derived by comparing the ΔA value of both test and control line:
The amount of neutralizing antibody is proportional to the nAb value. Then, nAb value was transferred to the cPass ELISA inhibition percentage with a regression fitting curve. The formula of the regression curve is:
We compared the inhibition percentage derived from nAb with the cPass ELISA results.
SARS-COV-2 NEUTRALIZING ANTIBODY ELISA TEST:
A commercial FDA-approved SARS-CoV-2 neutralizing antibody ELISA kit (Genscript cPass neutralization antibody assay) as a criterion standard was compared with the LFIA kit. Serum samples and positive and negative controls were first diluted 10 times and individually mixed with a volume ratio of 1: 1 HRP-RBD solution. The mixed samples were then incubated at 37°C for 30 min. We loaded 100 μL of each mixed sample to a microplate well pre-coated with hACE-2 proteins. The microplate was then incubated at 37°C for 30 min and washed with washing buffer 4 times. We added 100 μL of TMB (3, 3′, 5, 5′-Tetramethylbenzidine) substrate solution to each well in the microplate and then incubated it in the dark at room temperature for 15 min to start the enzymatic reaction. We added 50 μL of stop solution to each well, and the microplate was then read by an ELISA reader (Tecan Sunrise™). Since the neutralizing antibodies inhibit the bindings between RBD and hACE-2 proteins, the lower the optical density (O.D.) at 450 nm, the more neutralizing antibody there is. The absorbance of positive control must be less than 0.3, and the absorbance of negative control must be more than 1. The inhibition percentage is obtained from the following formula:
The serum samples with less than 30% inhibition percentage were identified as negative cases.
T TEST:
A 2-tailed
RECEIVER OPERATING CHARACTERISTIC CURVE:
The receiver operating characteristic (ROC) is an effective way to evaluate the overall accuracy of the proposed LFIA+S method by calculating the area under the curve (AUC). In general, the value of AUC ranges from 0 to 1, where a values of 0.9 to 1 reflect an outstanding result, values of 0.8 to 0.9 is considered excellent, and 0.8 to 0.7 is acceptable.
PEARSON’S R:
Pearson’s r was used to evaluate the correlation between cPass ELISA and LFIA+S. Pearson’s r between 0 to 0.25 was the absence of correlation, Pearson’s r between 0.25 and 0.5 was poor correlation, Pearson’s r between 0.5 and 0.75 was moderate to good correlation, and Pearson’s r between 0.75 and 1 was very good to excellent correlation.
BLAND-ALTMAN ANALYSIS:
Bland-Altman analysis was used to evaluate the agreement between cPass ELISA and LFIA+S. The upper limit of the 95% confidence interval was defined by adding 1.96 times standard deviations (SD) to the mean difference between these 2 methods; the lower limit of the 95% confidence interval was defined by subtracting the 1.96 times SDs from the mean difference. Data with 95% confidence interval were agreements between these 2 methods.
INTERCLASS CORRELATION ANALYSIS:
We used intraclass correlation coefficient (ICC) analysis to estimate the reliability between cPass ELISA and the proposed LFIA+S. Coefficient of ICC below 0.5 was poor reliability, coefficient between 0.5 and 0.75 was moderate reliability, coefficient between 0.75 and 0.9 was good reliability, and coefficient above 0.9 was excellent reliability.
Results
The results are shown in Figure 4. The increasing concentration of neutralizing antibodies could replace the S-RBD and bind with h-ACE2, which leads to a lighter color of the T-line. However, no obvious relationship was found between the antibody concentration and C-line color. Therefore, 4 categories were defined based on the visual observation: T-line deeper than C-line (negative), T-line as deep as C-line (weak positive), T-line lighter than C-line (medium positive), and T-line fade away (high positive).
In addition, absorbance was utilized to reveal the spectrum result of the test kits. The spectral peak intensity ranges from 520 nm to 540 nm and depended on the colloidal gold, which is a determining marker for S-RBD. Figure 5 illustrates the results of the spectral observation, which once again confirms that the deeper the color of the T-line (HPOS), the higher the absorbance of the colloidal gold, and the C-line (NEG) does not consistently change with concentration variation.
After scanning the test kits with a spectrometer, an nAb index was calculated by a spectral result formula. To evaluate the diagnostic ability of nAb, we first considered those specimens with an inhibition rate greater than 30% in the cPass kit as positive samples, and we viewed the others as negative samples. We used the
We performed both cPass assays and lateral flow test for each specimen. To confirm the relationship between the inhibition rate from cPass assays and the nAb index from lateral flow test, we performed linear regression analysis, showing a correlation coefficient of 0.864 (Figure 8).
We converted the inhibition percentage of cPass ELISA and LFIA+S. The Bland-Altman analysis showed a 94.2% (65 out of 69) confidence interval between cPass ELISA and LFIA+S (Figure 9). ICC analysis showed excellent reliability between the cPass and LFIA+S, and the coefficient was 0.90138, greater than 0.9 (Figure 10). With the information above, we are more confident that LFIA+S is a reliable solution to predict nAbs.
Discussion
With the outbreak of the COVID-19 pandemic and the threat of SARS-CoV-2 virus variants, there have been more reinfection cases [1,5,28,29]. Even fully vaccinated people still have a high risk of getting infections. It is a necessity that the vaccine effectiveness (VE) be tested, which can be analyzed by neutralizing antibody level (nAb level). As a result, it is important to detect the nAb level in sera after being vaccinated [7,30,31]. In currently used detection methods,
The LFIA+S method proposed in the current study is believed to be a more convenient way to get the nAb result. It takes only 3 min to perform, and it is easy to carry out because of the small size of the kit. In the current research, the LFIA+S method could significantly differentiate between the positive and negative sera at
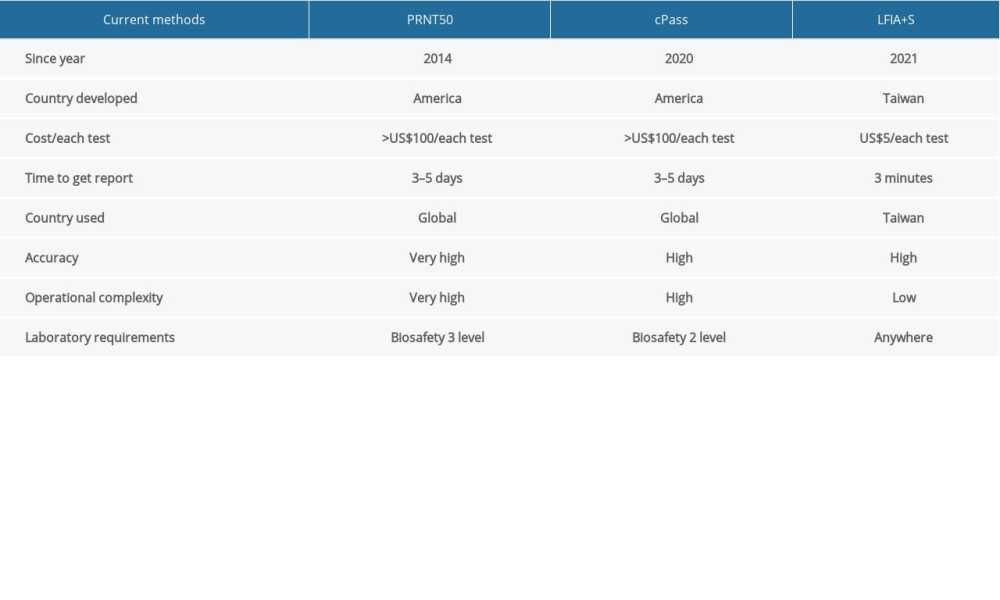
Table 1 provides a simplified comparison and analysis. The results of the statistical analyses show that LFIA+S has an accuracy highly similar to that of cPass in the detection of nAb, and also has high specificity and sensitivity. Our results show that LFIA+S has great potential to be a new reliable method for quantifying nAb.
This current study has several limitations. The first limitation was the design of the optical platform; all the databases we established for comparing the concentration of gold nanoparticles to absorption spectrum information can only be conducted using the LFIA test kit produced by Healgen Scientific. In other words, using testing kits of other brands requires rebuilding the database. To assess all brands will require a significant storage space that makes real-time data and cloud computing impractical. Furthermore, it the number of collected samples should be larger; the insufficient sample size turned out to be the primary obstacle to fine-tuning the platform sensitivity. In the future, it will be essential that more vaccinated people be recruited so as to provide medical institutions with more valid data on vaccine efficacy.
Conclusions
As COVID-19 vaccine coverage increases, it is essential to investigate whether the vaccine efficacy is sufficient to prevent spread of the pandemic. In reality, the existing methods for detecting nAbs level,
Figures
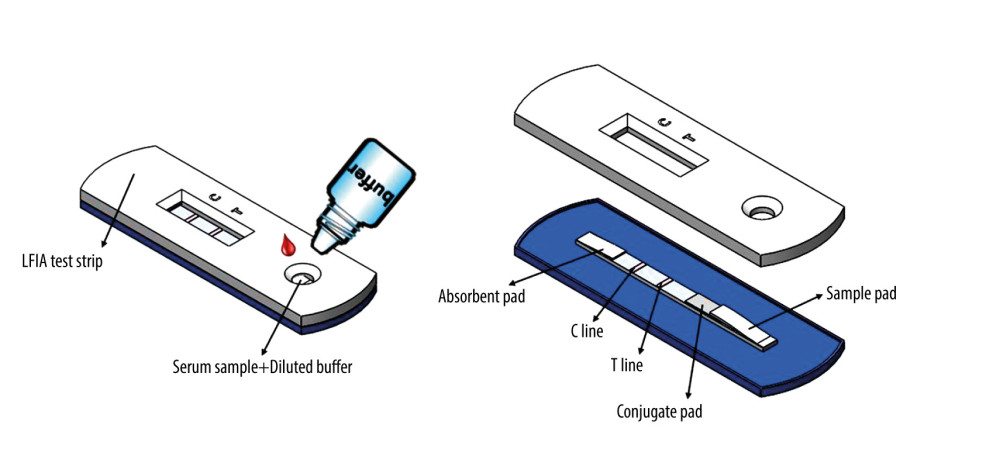 Figure 1. Lateral flow immunoassay test strip with C-line and T-line.
Figure 1. Lateral flow immunoassay test strip with C-line and T-line.  Figure 2. Lateral flow immunoassay+portable spectrometer (LFIA+S).
Figure 2. Lateral flow immunoassay+portable spectrometer (LFIA+S). 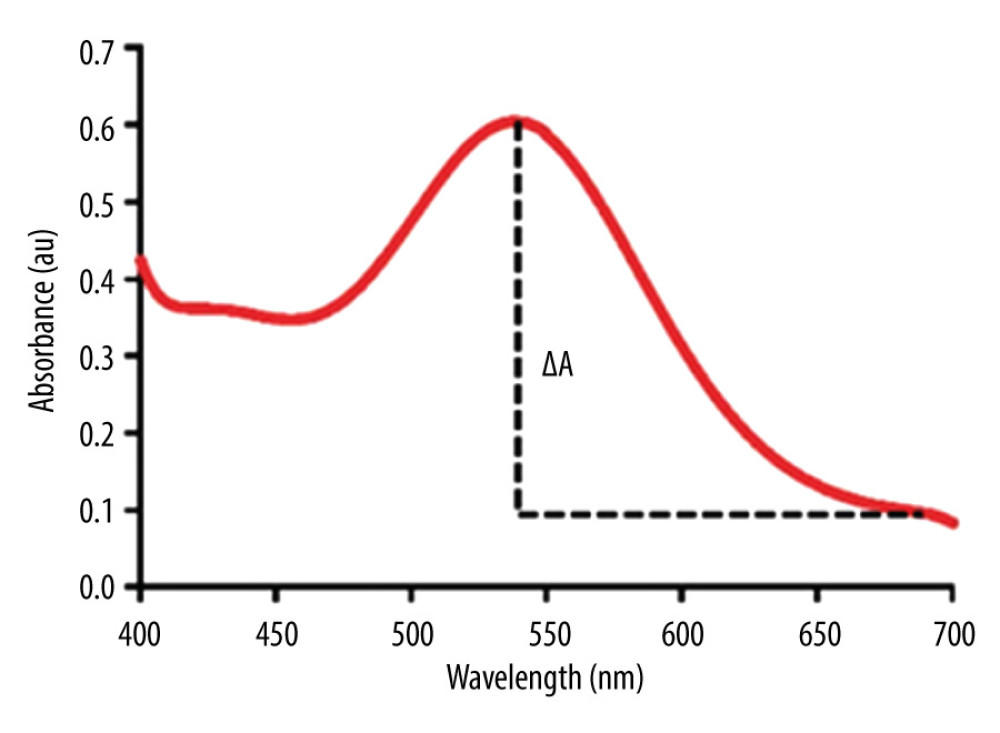 Figure 3. Absorbance spectrum of gold nanoparticles.
Figure 3. Absorbance spectrum of gold nanoparticles. 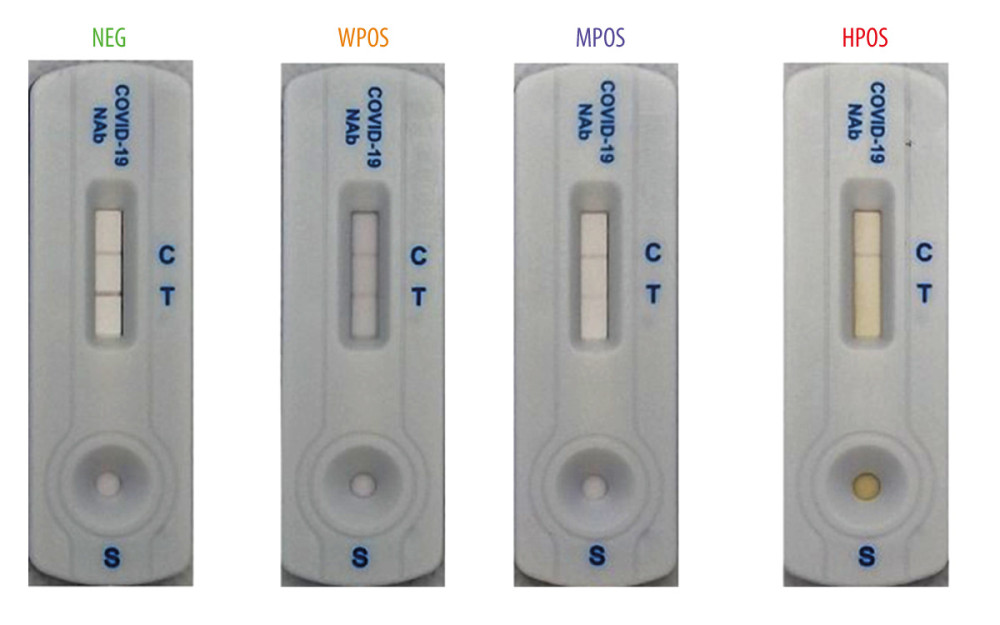 Figure 4. Results of the competitive test kit from different concentration of neutralizing antibodies specimen. From left to right: negative (NEG), weak positive (WPOS), medium positive (MPOS), and high positive (HPOS).
Figure 4. Results of the competitive test kit from different concentration of neutralizing antibodies specimen. From left to right: negative (NEG), weak positive (WPOS), medium positive (MPOS), and high positive (HPOS). 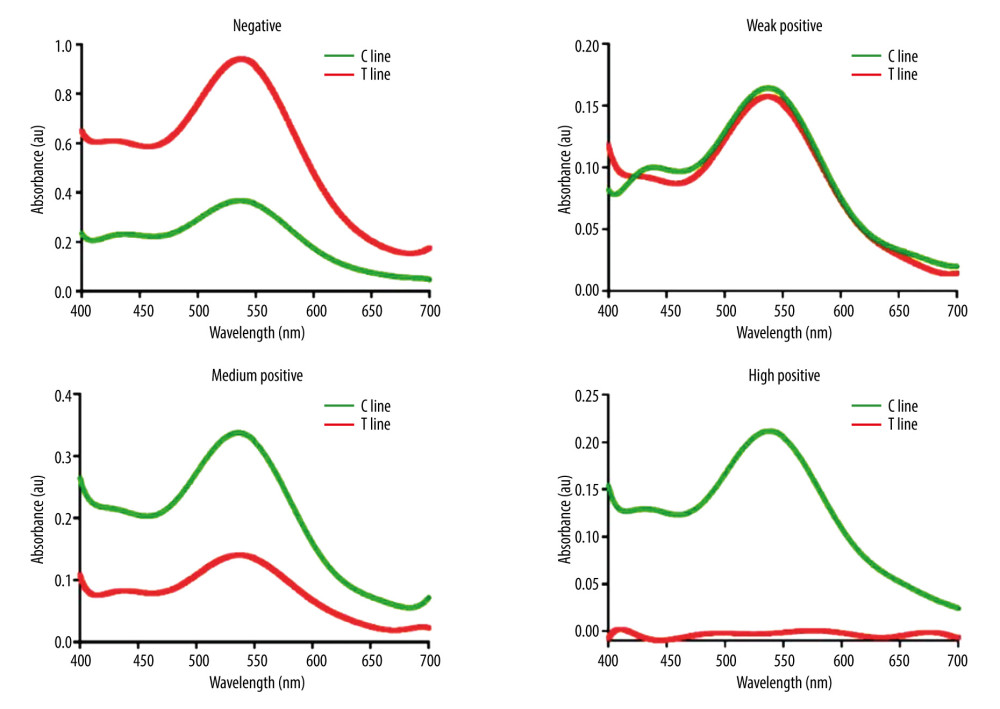 Figure 5. Spectral results of the competitive test kit from different concentration of neutralizing antibodies specimen. Spectrum of C-line shown with green lines. Spectrum of T-line shown with red lines.
Figure 5. Spectral results of the competitive test kit from different concentration of neutralizing antibodies specimen. Spectrum of C-line shown with green lines. Spectrum of T-line shown with red lines. 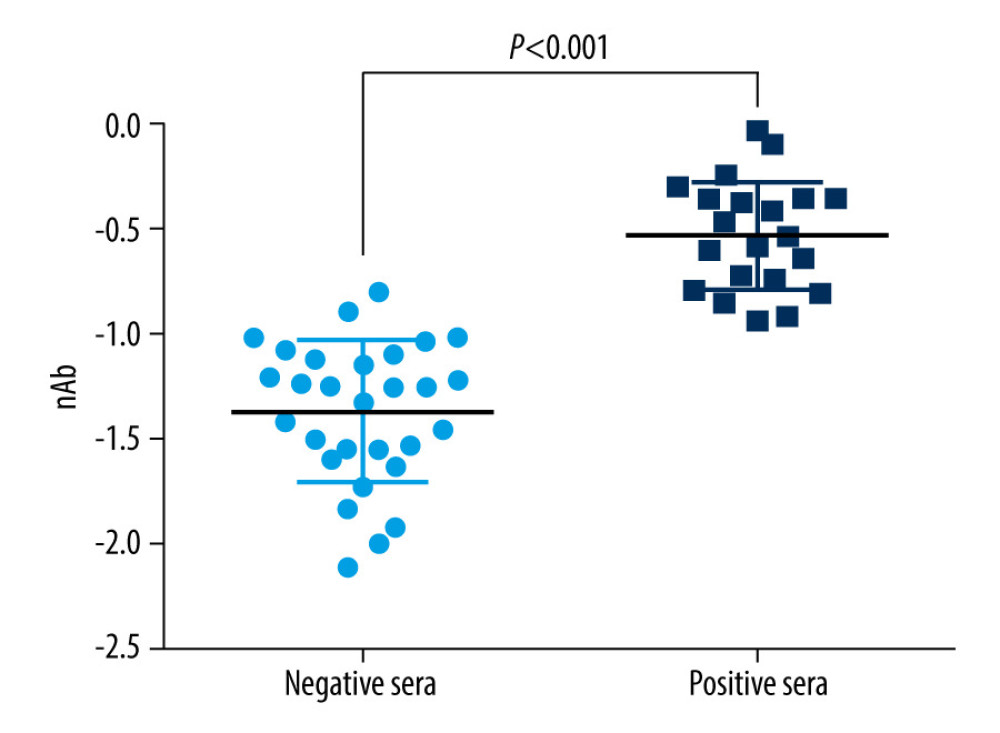 Figure 6. The t test nAb results of negative and positive sera are significantly different (P value <0.001).
Figure 6. The t test nAb results of negative and positive sera are significantly different (P value <0.001). 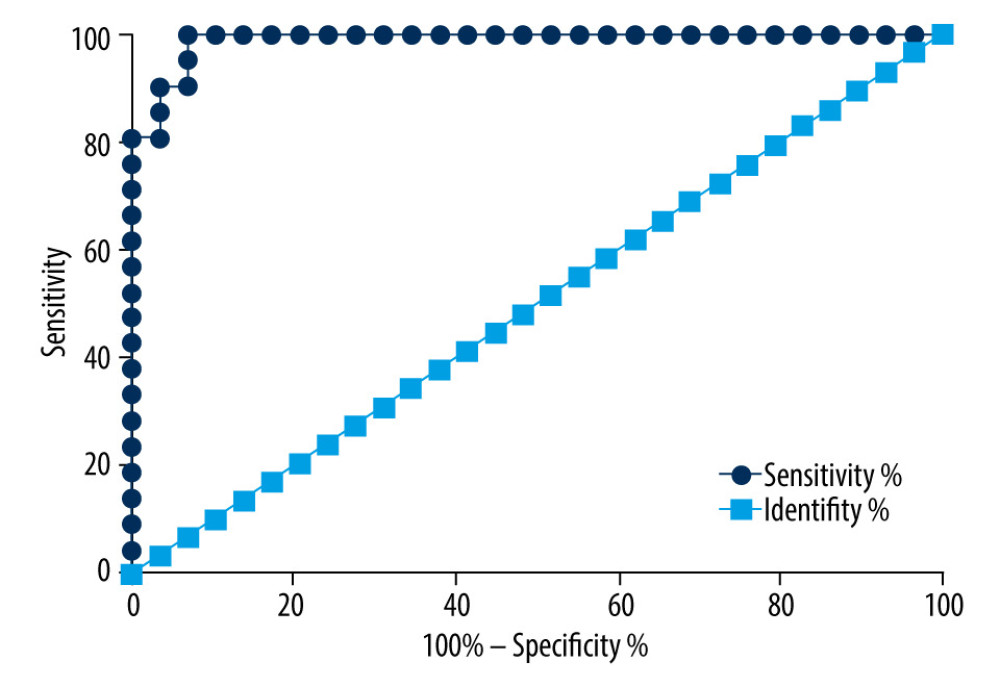 Figure 7. ROC curve for index nAb. The area under the curve is 0.9901.
Figure 7. ROC curve for index nAb. The area under the curve is 0.9901. 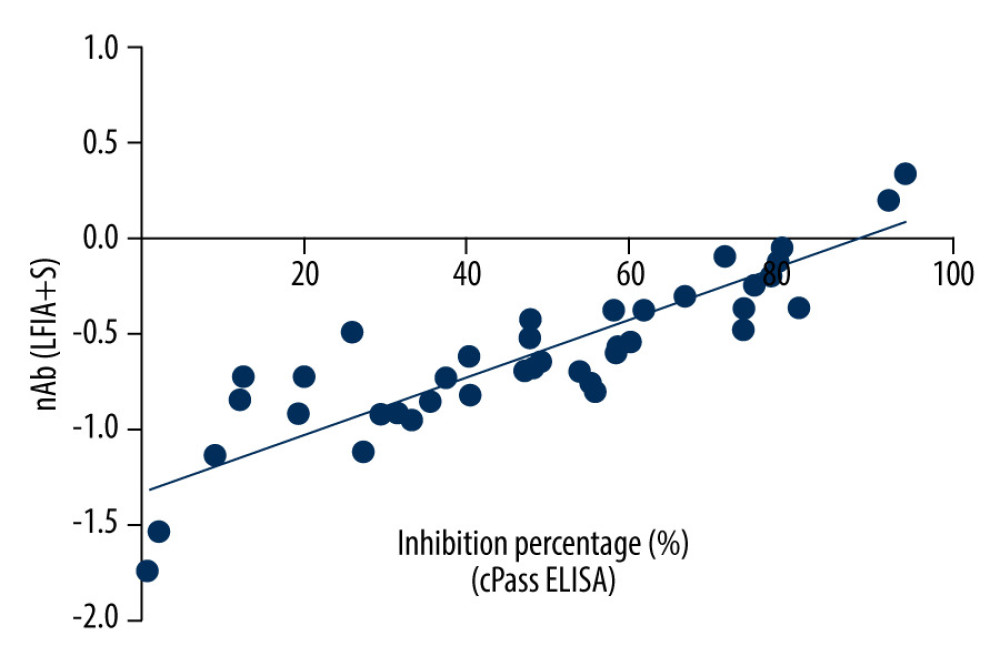 Figure 8. The linear regression fitting between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 8. The linear regression fitting between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. 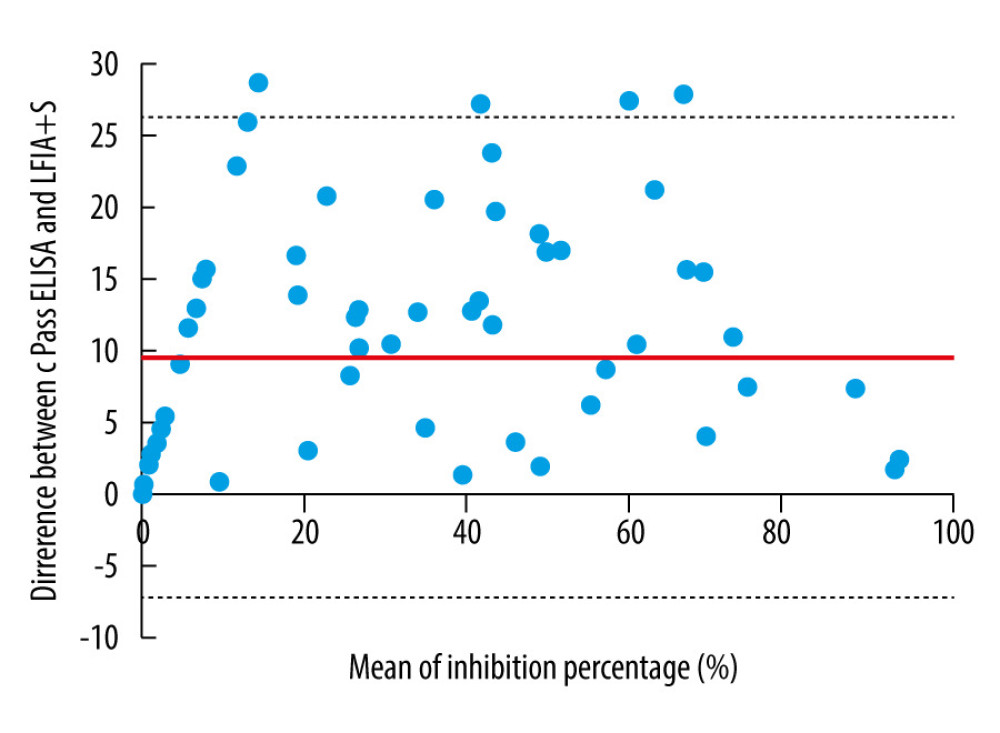 Figure 9. The Bland-Altman analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 9. The Bland-Altman analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. 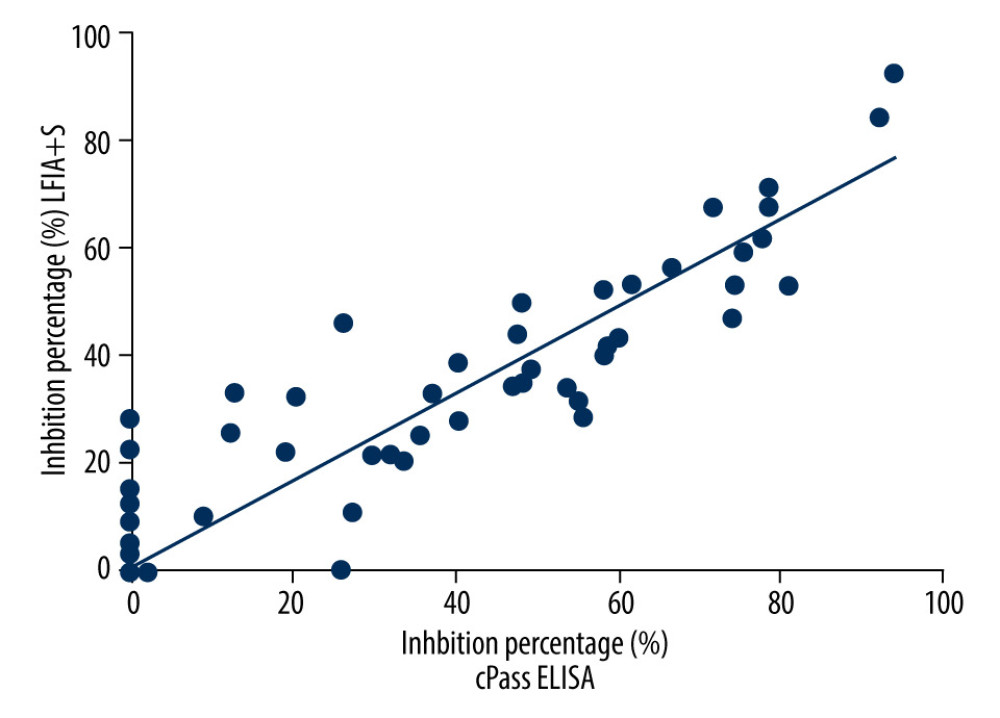 Figure 10. The interclass correlation analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 10. The interclass correlation analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. References
1. Al-Rohaimi AH, Al Otaibi F, Novel SARS-CoV-2 outbreak and COVID19 disease; A systemic review on the global pandemic: Genes Dis, 2020; 7(4); 491-501
2. Su YJ, Chang CW, Chen MJ, Lai YC, Impact of COVID-19 on liver: World J Clin Cases, 2021; 9(27); 7998-8007
3. Bolcato M, Aurilio MT, Aprile A, Take-home messages from the COVID-19 pandemic: strengths and pitfalls of the Italian National Health Service from a medico-legal point of view: Healthcare, 2021; 9(1); 17
4. Perrone MA, Feola A, Pieri M, The effects of reduced physical activity on the lipid profile in patients with high cardiovascular risk during COVID-19 lockdown: Int J Environ Res Public Health, 2021; 18(16); 8858
5. GeurtsvanKessel CH, Okba NMA, Igloi Z, An evaluation of COVID-19 serological assays informs future diagnostics and exposure assessment: Nat Commun, 2020; 11(1); 3436
6. Hansen CH, Michlmayr D, Gubbels SM, Assessment of protection against reinfection with SARS-CoV-2 among 4 million PCR-tested individuals in Denmark in 2020: A population-level observational study: Lancet, 2021; 397(10280); 1204-12
7. Bolcato M, Rodriguez D, Feola A, COVID-19 Pandemic and equal access to vaccines: Vaccines, 2021; 9(6); 538
8. Thomas SJ, Moreira ED, Kitchin N, Six month safety and efficacy of the BNT162b2 mRNA COVID-19 vaccine: medRxiv, 2021; 2021 21261159
9. Baraniuk C, What do we know about China’s COVID-19 vaccines?: BMJ, 2021; 373; n912
10. Ju B, Zhang Q, Ge J, Human neutralizing antibodies elicited by SARS-CoV-2 infection: Nature, 2020; 584(7819); 115-19
11. Haas EJ, Angulo FJ, McLaughlin JM, Impact and effectiveness of mRNA BNT162b2 vaccine against SARS-CoV-2 infections and COVID-19 cases, hospitalisations, and deaths following a nationwide vaccination campaign in Israel: An observational study using national surveillance data: Lancet, 2021; 397(10287); 1819-29
12. Khoury DS, Cromer D, Reynaldi A, Neutralizing antibody levels are highly predictive of immune protection from symptomatic SARS-CoV-2 infection: Nat Med, 2021; 27(7); 1205-11
13. Frenck RW, Klein NP, Kitchin N, Safety, immunogenicity, and efficacy of the BNT162b2 COVID-19 vaccine in adolescents: N Engl J Med, 2021; 385(3); 239-50
14. Bewley KR, Coombes NS, Gagnon L, Quantification of SARS-CoV-2 neutralizing antibody by wild-type plaque reduction neutralization, microneutralization and pseudotyped virus neutralization assays: Nat Protoc, 2021; 16(6); 3114-40
15. Xie X, Nielsen MC, Muruato AE, Evaluation of a SARS-CoV-2 lateral flow assay using the plaque reduction neutralization test: Diagn Microbiol Infect Dis, 2021; 99(2); 115248
16. Taylor SC, Hurst B, Charlton CL, A new SARS-CoV-2 dual-purpose serology test: Highly accurate infection tracing and neutralizing antibody response detection: J Clin Microbiol, 2021; 59(4); e02438-20
17. Jung K, Shin S, Nam M, Performance evaluation of three automated quantitative immunoassays and their correlation with a surrogate virus neutralization test in coronavirus disease 19 patients and pre-pandemic controls: J Clin Lab Anal, 2021; 35(9); e23921
18. Jung J, Rajapakshe D, Julien C, Devaraj S, Analytical and clinical performance of cPass neutralizing antibodies assay: Clin Biochem, 2021; 98; 70-73
19. Lau EHY, Tsang OTY, Hui DSC, Neutralizing antibody titres in SARS-CoV-2 infections: Nat Commun, 2021; 12(1); 63
20. Papenburg J, Cheng MP, Corsini R, Evaluation of a commercial culture-free neutralization antibody detection kit for severe acute respiratory syndrome-related coronavirus-2 and comparison with an antireceptor-binding domain enzyme-linked immunosorbent assay: Open Forum Infect Dis, 2021; 8(6); ofab220
21. Nandakumar V, Profaizer T, Lozier BK, Evaluation of a surrogate enzyme-linked immunosorbent assay-based severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) cPass neutralization antibody detection assay and correlation with immunoglobulin G commercial serology assays: Arch Pathol Lab Med, 2021; 145(10); 1212-20
22. Jung BK, Yoon J, Bae J-Y, Performance evaluation of the BZ COVID-19 neutralizing antibody test for the culture-free and rapid detection of SARS-CoV-2 neutralizing antibodies: Diagnostics, 2021; 11(12); 2193
23. Bao H, Yuan M, Xiao C, Development of a signal-enhanced LFIA based on tyramine-induced AuNPs aggregation for sensitive detection of danofloxacin: Food Chem, 2022; 375; 131875
24. Hnasko RM, Jackson ES, Lin AV, A rapid and sensitive lateral flow immunoassay (LFIA) for the detection of gluten in foods: Food Chem, 2021; 355; 129514
25. Chen P-Y, Ko C-H, Wang CJ, The early detection of immunoglobulins via optical-based lateral flow immunoassay platform in COVID-19 pandemic: PLoS One, 2021; 16(7); e0254486
26. Hung KF, Hung CH, Hong C, Quantitative spectrochip-coupled lateral flow immunoassay demonstrates clinical potential for overcoming coronavirus disease 2019 pandemic screening challenges: Micromachines (Basel), 2021; 12(3); 321
27. Zou KH, O’Malley AJ, Mauri L, Receiver-operating characteristic analysis for evaluating diagnostic tests and predictive models: Circulation, 2007; 115(5); 654-57
28. Tan ST, Chen TH, Yang HW, Su YJ, Changes in poisoning during the COVID-19 pandemic worldwide: Am J Emerg Med, 2021 [Online ahead of print]
29. Su YJ, Lai YC, Comparison of clinical characteristics of coronavirus disease (COVID-19) and severe acute respiratory syndrome (SARS) as experienced in Taiwan: Travel Med Infect Dis, 2020; 36; 101625
30. Bartsch SM, O’Shea KJ, Ferguson MC, Vaccine efficacy needed for a COVID-19 coronavirus vaccine to prevent or stop an epidemic as the sole intervention: Am J Prev Med, 2020; 59(4); 493-503
31. Edara VV, Hudson WH, Xie X, Neutralizing antibodies against SARS-CoV-2 variants after infection and vaccination: JAMA, 2021; 325(18); 1896-98
32. Girardin RC, Dupuis AP, Payne AF, Temporal analysis of serial donations reveals decrease in neutralizing capacity and justifies revised qualifying criteria for coronavirus disease 2019 convalescent plasma: J Infect Dis, 2021; 223(5); 743-51
33. Xu L, Li D, Ramadan S, Li Y, Klein N, Facile biosensors for rapid detection of COVID-19: Biosens Bioelectron, 2020; 170; 112673
34. Miyakawa K, Jeremiah SS, Kato H, Rapid detection of neutralizing antibodies to SARS-CoV-2 variants in post-vaccination sera: J Mol Cell Biol, 2022; 13(12); 918-20
35. Moriyama S, Adachi Y, Sato T, Temporal maturation of neutralizing antibodies in COVID-19 convalescent individuals improves potency and breadth to circulating SARS-CoV-2 variants: Immunity, 2021; 54(8); 1841-1852.e4
Figures
 Figure 1. Lateral flow immunoassay test strip with C-line and T-line.
Figure 1. Lateral flow immunoassay test strip with C-line and T-line. Figure 2. Lateral flow immunoassay+portable spectrometer (LFIA+S).
Figure 2. Lateral flow immunoassay+portable spectrometer (LFIA+S). Figure 3. Absorbance spectrum of gold nanoparticles.
Figure 3. Absorbance spectrum of gold nanoparticles. Figure 4. Results of the competitive test kit from different concentration of neutralizing antibodies specimen. From left to right: negative (NEG), weak positive (WPOS), medium positive (MPOS), and high positive (HPOS).
Figure 4. Results of the competitive test kit from different concentration of neutralizing antibodies specimen. From left to right: negative (NEG), weak positive (WPOS), medium positive (MPOS), and high positive (HPOS). Figure 5. Spectral results of the competitive test kit from different concentration of neutralizing antibodies specimen. Spectrum of C-line shown with green lines. Spectrum of T-line shown with red lines.
Figure 5. Spectral results of the competitive test kit from different concentration of neutralizing antibodies specimen. Spectrum of C-line shown with green lines. Spectrum of T-line shown with red lines. Figure 6. The t test nAb results of negative and positive sera are significantly different (P value <0.001).
Figure 6. The t test nAb results of negative and positive sera are significantly different (P value <0.001). Figure 7. ROC curve for index nAb. The area under the curve is 0.9901.
Figure 7. ROC curve for index nAb. The area under the curve is 0.9901. Figure 8. The linear regression fitting between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 8. The linear regression fitting between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. Figure 9. The Bland-Altman analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 9. The Bland-Altman analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. Figure 10. The interclass correlation analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage.
Figure 10. The interclass correlation analysis between cPass ELISA inhibition percentage and LFIA+S inhibition percentage. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387