31 May 2022: Clinical Research
A Retrospective Study from 2 Tertiary Hospitals in China to Evaluate the Risk Factors for Surgical Site Infections After Abdominal Hysterectomy in 188 Patients
Dong Wang1ABCDEF, Yanhua Chen2ABCDEF*, Jianjun Deng13ABCDG, Guoguang Xiao1BCD, Yaru Li1BCD, Lin Lin4BCD, Yun You5BCDDOI: 10.12659/MSM.936198
Med Sci Monit 2022; 28:e936198
Abstract
BACKGROUND: Surgical site infections in patients after abdominal hysterectomy can increase medical expenses and increase the risk of death in patients. This retrospective study from 2 grade A tertiary hospitals in China aimed to evaluate the risk factors for postoperative surgical site infections (SSIs) in 188 patients undergoing abdominal hysterectomy between September 2013 and June 2021.
MATERIAL AND METHODS: Of the 188 patients, 94 patients with SSIs were classified into the infected group, and 94 patients without SSIs were classified into the control group. Wound drainage was sampled for bacterial isolation and culture.
RESULTS: The suspected risk factors for SSIs after abdominal hysterectomy were body mass index, whether the patient had comorbidities of diabetes mellitus, cancer, or hypoproteinemia, surgical wound classification, whether preoperative skin preparation was performed, whether the patient had chemotherapy, length of incision, amount of blood loss during surgery, duration of surgery, necessity of a second surgery, whether a wound drainage tube was inserted, and whether delayed suturing was used in wound. Of them, body mass index (OR=1.133; 95% CI: 1.012~1.266; P=0.029), more than 3 hours of surgery (OR=0.261; 95% CI: 0.108~0.631; P=0.003), and wound drainage tube insertion (OR=0.223; 95% CI: 0.094~0.531; P=0.001) were the independent risk factors.
CONCLUSIONS: The findings support previous studies and showed that risk factors for SSIs after abdominal hysterectomy included increased patient BMI, increased operation duration, and the number of surgical drainage tubes used.
Keywords: Gynecology, Hysterectomy, Laparotomy, Risk Factors, Surgical Wound Infection, China, Female, Humans, Tertiary Care Centers
Background
Hysterectomy is one of the most common surgical procedures performed for women [1].
A woman’s risk of having a hysterectomy in her lifetime is around 45% [2]. Laparotomy, which requires a wide view of the surgical area and exposure of pelvic anatomy, has been commonly used to treat gynecologic malignant tumors such as uterine, endometrial, and ovarian cancer [3].
A recent study has shown that the incidence rate of surgical site infections after hysterectomy is 6.18–9.61% [4,5]. High body mass index, the amount of blood loss during surgery, low hematocrit levels, and anemia can increase the incidence of surgical site infections after hysterectomy [6]. Among the different types of hysterectomy, laparoscopic hysterectomy results in lower rates of surgical site infections compared with abdominal hysterectomy and vaginal hysterectomy [6]. Surgical site infections not only increase medical expenses, including the surgery and drug costs [7], but also increase the morbidity, mortality, and readmission rates [1]. Therefore, this retrospective study from 2 grade A tertiary hospitals in China aimed to evaluate the risk factors for postoperative surgical site infections in 188 patients undergoing abdominal hysterectomy between September 2013 and June 2021.
Material and Methods
ETHICS APPROVAL:
This study was carried out in accordance with the Declaration of Helsinki. Ethics approval of this study was received from the Medical Ethics Committee of West China Second University Hospital, Sichuan University (No. YXKY2021LSP [178]). Before the research procedures started, the patients were verbally informed of the purpose and significance of this study and were asked to give us voluntary consent to collect their data for this study. The verbal informed consent process was witnessed by the head nurse of the Gynecology Department. Verbal informed consent was obtained from all patients included in this study. The verbal informed process was approved by the Medical Ethics Committee of West China Second University Hospital, Sichuan University. Data collected were confidential and used only by this study.
STUDY SETTING:
A total of 188 patients undergoing abdominal hysterectomy at 2 grade A tertiary hospitals in China between September 2013 and June 2021 were included in this study.
STUDY TOOLS:
Of the 188 patients, 94 patients with surgical site infections were classified into the infected group, and 94 patients without surgical site infections were classified into the control group. Wound drainage samples were inoculated on blood agar plates, MacConkey agar plates, and Sabouraud’s medium produced by Guangzhou Detgerm Microbiological Science, Ltd., China. Bacterial isolation and culture were performed according to the China’s National Guide to Clinical Laboratory Procedures. VITEK® 2 Compact, which is a mass spectrometry microbial identification system produced by bioMérieux France, was used to identify pathogenic bacteria from positive samples.
Surgical wound healing and infection were identified according to surgical wound healing status, hospital statistics [8], and the Identifying Criteria for Nosocomial Infection (Tentative) issued by the National Health Commission of the People’s Republic of China [9].
High-risk factors for surgical site infections in this study were monitored using the following indicators: age, body mass index (BMI), whether the patient had comorbidities of heart disease, hypertension, diabetes mellitus, cancer, malnutrition, anemia, or hypoproteinemia, preoperative white blood cell count and hemoglobin level, surgical wound classification, whether preoperative skin preparation was performed, whether the patient had chemotherapy, prior abdominal surgery or high-dose antibiotic therapy, length of incision, amount of blood loss during surgery, duration of surgery, necessity of a second surgery, whether a wound drainage tube was inserted, and whether delayed suturing was used.
DATA COLLECTION:
Data were collected by the researchers from the patients’ medical records. The researchers had more than 7 years of clinical experience in obstetrics and gynecology and more than 4 years of experience in nosocomial infection control.
STATISTICAL ANALYSIS:
Data were analyzed using SPSS19.0. The incidence of surgical site infections was expressed with n (%). If continuous variables were found to not be normally distributed after normality test in single-factor analysis, then non-parametric tests on 2 independent groups were used. Classified variables were performed with the chi-square (χ2) test. Data with a
Results
CLINICAL DATA OF PATIENTS UNDERGOING ABDOMINAL HYSTERECTOMY:
Symptoms of surgical site infections in the 94 patients after abdominal hysterectomy were as follows: redness, swelling, pain, bleeding, fluid or purulent drainage (or had foul smell) from the incision; serious infection can cause the presence of necrotic tissue in the wound, poor wound healing, or occurrence of a tunneling wound. The average age of the 94 patients with surgical site infections was 46.57±8.86, and the quartiles of their inpatient days were 20 (15.75–24.25) days. Superficial incisional, deep incisional, and organ/space surgical site infection rates were 93.62% (88/94), 5.32% (5/94), and 1.06% (1/94), respectively. Most of the superficial incisional surgical site infections occurred after radical hysterectomy and extrafascial hysterectomy, and wound healing was mainly graded as good; most of the deep incisional surgical site infections occurred after radical hysterectomy and wound healing was mainly graded as fair; and most of the organ/space surgical site infections occurred after extrafascial hysterectomy and wound healing was mainly graded as good, as shown in Table 1.
PATHOGENIC BACTERIA CAUSING SURGICAL SITE INFECTIONS:
Specimens of drainage from infected wounds in the 94 patients after abdominal hysterectomy were delivered for laboratory testing. A total of 99 pathogenic bacteria were isolated. Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Staphylococcus aureus, and Pseudomonas aeruginosa, which accounted for 37.37% (37/99), 19.19% (10/99), 11.11% (11/99), 7.07% (7/99), and 6.06% (6/99), respectively, were the main pathogenic bacteria. Among them, 1 multidrug-resistant Staphylococcus aureus was found. Details are presented in Table 2.
SINGLE-FACTOR ANALYSIS OF POSSIBLE HIGH-RISK FACTORS FOR SURGICAL SITE INFECTIONS IN PATIENTS AFTER ABDOMINAL HYSTERECTOMY:
Single-factor analysis was performed for the possible high-risk factors for surgical site infections in patients after abdominal hysterectomy. The suspected factors influencing surgical site infections in patients after abdominal hysterectomy were BMI, whether the patient had comorbidities of diabetes mellitus, cancer, or hypoproteinemia, surgical wound classification, whether preoperative skin preparation was performed, whether the patient had chemotherapy, length of incision, the amount of blood loss during surgery, duration of surgery, necessity of a second surgery, whether a wound drainage tube was inserted, and whether delayed suturing was used. A statistically significant difference (P<0.1) was found, as shown in Table 3.
MULTIVARIATE ANALYSIS OF POSSIBLE HIGH-RISK FACTORS FOR SURGICAL SITE INFECTIONS IN PATIENTS AFTER ABDOMINAL HYSTERECTOMY:
The suspected factors influencing surgical site infections in the single-factor analysis were considered as the independent variables in the binary logistic regression analysis. The results showed that BMI, more than 3 hours of surgery, and wound drainage tube insertion were the independent factors influencing surgical site infections after abdominal hysterectomy. A statistically significant difference (P<0.05) was found, as shown in Table 4.
Per 0.123 increase in preoperative BMI (
Our results predicted that BMI, more than 3 hours of surgery, and wound drainage tube insertion after surgery are factors influencing surgical site infections in patients after abdominal hysterectomy. The prediction accuracy was 73.40%, indicating a good accuracy and valuable prediction.
Discussion
LIMITATIONS:
This study did not show that the comorbidities of diabetes mellitus, cancer or hypoproteinemia, class III surgical wound, preoperative chemotherapy, preoperative skin preparation, length of incision, blood loss greater than 500 mL during surgery, a second surgery, and delayed suture in wound are the independent factors influencing surgical site infections after abdominal hysterectomy (P>0.05), but this does not mean that they are note possible independent risk factors for surgical site infections. Göksever et al [6] reported that diabetes mellitus, blood loss during surgery, and low hematocrit level were the risk factors for surgical site infections after abdominal hysterectomy. Our study was a retrospective study of 188 cases from 2 hospitals in China, so a small amount of data was collected for this study. We hope the sample size will increase in order to further evaluate the results.
Conclusions
The findings of this study support previous studies and showed that risk factors for surgical site infections after abdominal hysterectomy included increased patient BMI, increased operation duration, and the number of surgical drainage tubes used. Preoperative BMI control in patients, reducing operative time, and avoiding unnecessary wound drainage tube insertion after surgery are recommended to prevent surgical site infections after abdominal hysterectomy.
Tables
Table 1. Superficial incisional, deep incisional, and organ/space surgical site infection rates in patients after abdominal surgery.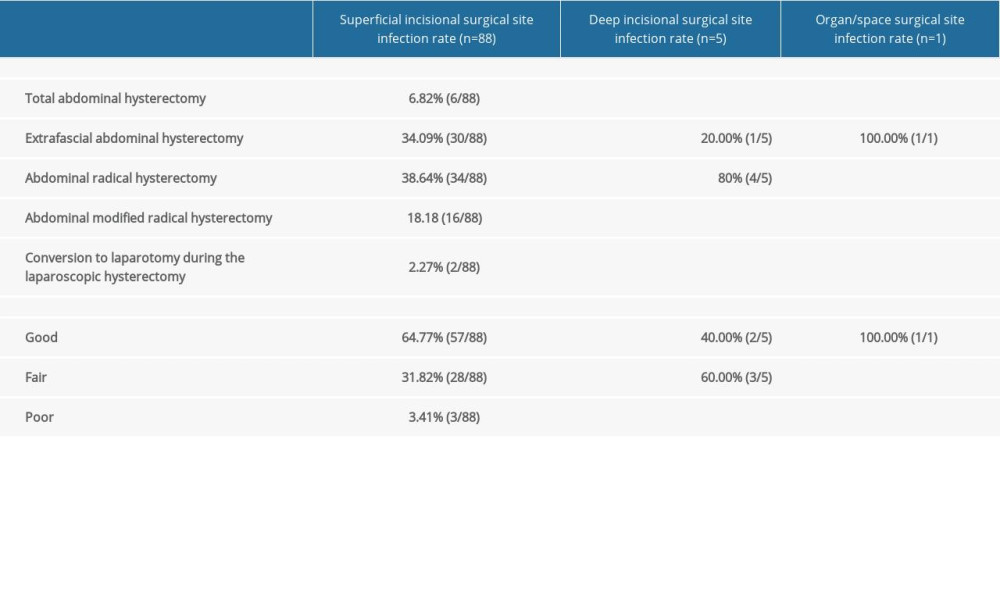 Table 2. Constituent ratio of pathogenic bacteria in infected wounds in patients after abdominal hysterectomy.
Table 2. Constituent ratio of pathogenic bacteria in infected wounds in patients after abdominal hysterectomy.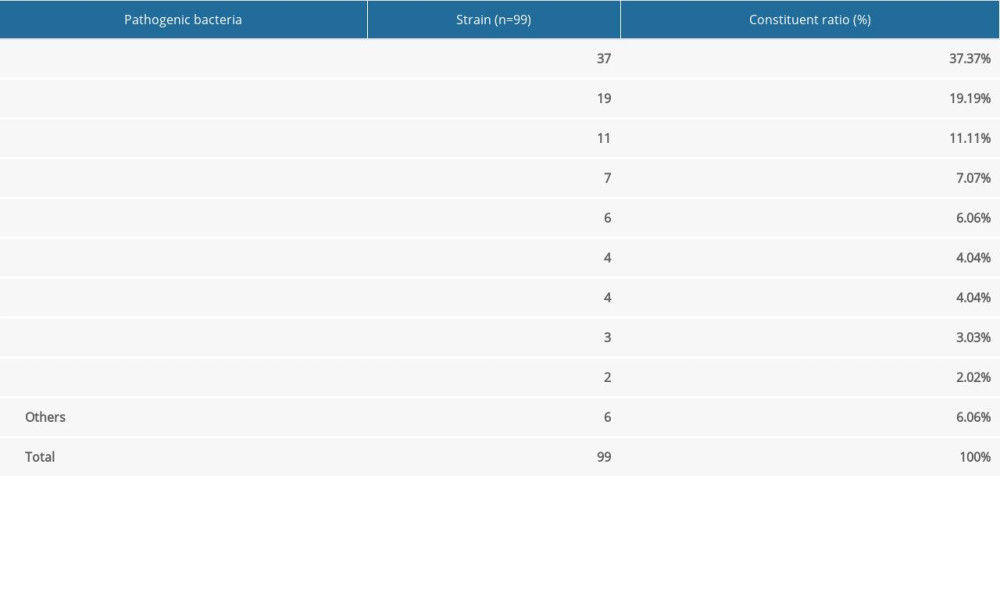 Table 3. Single-factor analysis of possible high-risk factors for surgical site infections in patients after abdominal hysterectomy.
Table 3. Single-factor analysis of possible high-risk factors for surgical site infections in patients after abdominal hysterectomy.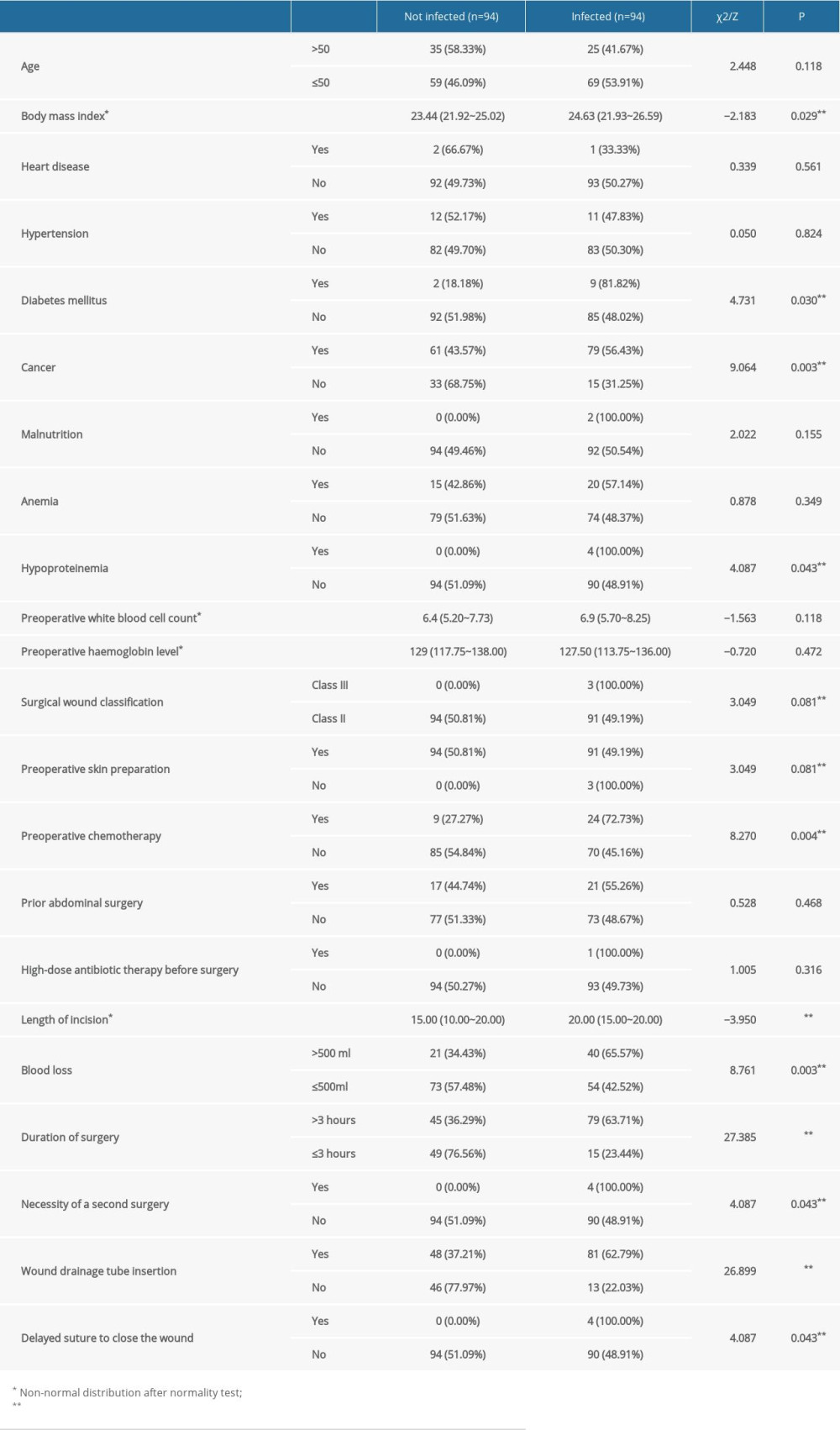 Table 4. Binary logistic regression analysis of high-risk factors for surgical site infections in patients after abdominal hysterectomy.
Table 4. Binary logistic regression analysis of high-risk factors for surgical site infections in patients after abdominal hysterectomy.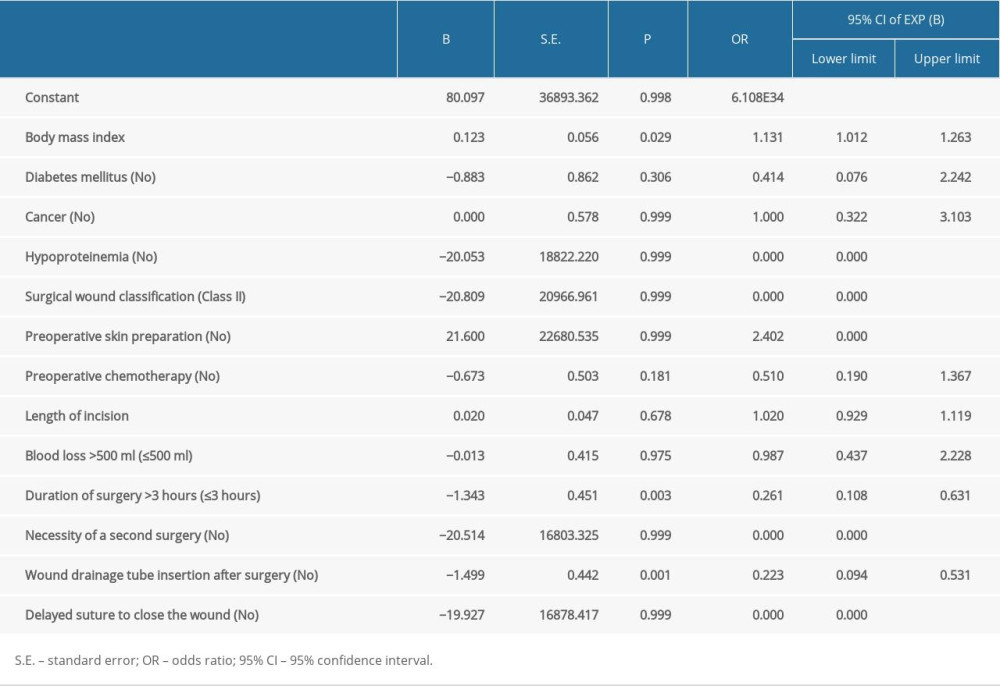
References
1. Burgess A, Fish M, Goldberg S, Surgical-site infection prevention after hysterectomy: Use of a consensus bundle to guide improvement: J Healthc Qual, 2020; 42(4); 188-94
2. Ayeleke RO, Mourad S, Marjoribanks J, Antibiotic prophylaxis for elective hysterectomy: Cochrane Database Syst Rev, 2017; 6(6); CD004637
3. Lu C, Dai W, Zhou A, Choice and thinking on gynecological surgery procedures: Journal of Laparoscopic Surgery, 2008; 13(6); 537-38
4. Zhang G, Cao W, Li C, Risk factors for surgical site infection after total hysterectomy in patients with gynecological malignant tumor: Chinese Journal of Infection Control, 2021; 20(7); 602-6
5. Davidson C, Enns J, Bennett C, Reducing abdominal hysterectomy surgical site infections: A multidisciplinary quality initiative: Am J Infect Control, 2020; 48(11); 1292-97
6. Göksever Çelik H, Çelik E, Risk factors for surgical site infection after hysterectomy: J Infect Dev Ctries, 2017; 11(4); 355-60
7. Wang J, Luo Y, Wang D, Influencing factors of incision infection after gynecological surgery and its impact on medical expenses: Chinese Journal of Clinical Rational Drug Use, 2019; 12(30); 8-10
8. Deng Y, The hospital statistics and the grades of healing of incision: Chinese Medical Record, 2004; 5(9); 38-39
9. , Nosocomial Infection Diagnosis Criteria (Tentative) (Reprint 7): Chinese Journal of Nosocomiology, 2002; 3; 5
10. Steiner HL, Strand EA, Surgical-site infection in gynecologic surgery: Pathophysiology and prevention: Am J Obstet Gynecol, 2017; 217(2); 121-28
11. Wei F, Zhang J, Wei X, Risk factors influencing wound infection after hysterectomy and its prevention measures: Maternal & Child Health Care of China, 2020; 35(3); 442-44
12. Shi L, Gu Q, Zhang F, Predictive factors of surgical site infection after hysterectomy for endometrial carcinoma: A retrospective analysis: BMC Surg, 2021; 21(1); 292
13. Andiman SE, Xu X, Boyce JM, Decreased surgical site infection rate in hysterectomy: Effect of a gynecology-specific bundle: Obstet Gynecol, 2018; 131(6); 991-99
14. Lim CS, Mowers EL, Mahnert N, Risk factors and outcomes for conversion to laparotomy of laparoscopic hysterectomy in benign gynecology: Obstet Gynecol, 2016; 128(6); 1295-305
15. Dotson S, Landa A, Ehrisman J, Secord AA, Safety and feasibility of contained uterine morcellation in women undergoing laparoscopic hysterectomy: Gynecol Oncol Res Pract, 2018; 5; 8
16. Bergstrom J, Aloisi A, Armbruster S, Minimally invasive hysterectomy surgery rates for endometrial cancer performed at National Comprehensive Cancer Network (NCCN) centers: Gynecol Oncol, 2018; 148(3); 480-84
17. Li L, Zhang D, Lin C, Zhang L, Significance of applying single incision laparoscopic surgery to treatment of benign ovarian diseases: Jilin Medical Journal, 2021; 42(5); 1195-97
18. Liu F, Xie J, Tian Y, Comparison of laparoscopic surgery and open abdominal surgery in treatment of gynecological diseases: China Journal of Endoscopy, 2016; 22(9); 57-60
Tables
 Table 1. Superficial incisional, deep incisional, and organ/space surgical site infection rates in patients after abdominal surgery.
Table 1. Superficial incisional, deep incisional, and organ/space surgical site infection rates in patients after abdominal surgery. Table 2. Constituent ratio of pathogenic bacteria in infected wounds in patients after abdominal hysterectomy.
Table 2. Constituent ratio of pathogenic bacteria in infected wounds in patients after abdominal hysterectomy. Table 3. Single-factor analysis of possible high-risk factors for surgical site infections in patients after abdominal hysterectomy.
Table 3. Single-factor analysis of possible high-risk factors for surgical site infections in patients after abdominal hysterectomy. Table 4. Binary logistic regression analysis of high-risk factors for surgical site infections in patients after abdominal hysterectomy.
Table 4. Binary logistic regression analysis of high-risk factors for surgical site infections in patients after abdominal hysterectomy. In Press
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








