09 November 2022: Clinical Research
Retrospective Study from a Single Center on the Efficacy of Pulsed Lavage Following Excision of Burns ≥30% of the Total Body Surface Area in 63 Patients
Jia Wan1ABCDEF, Jia He1BCD, Lu Chen1BC, Le Qiu1DEF, Fei Wang1DEF, Xu-Lin Chen1ADFG*DOI: 10.12659/MSM.937697
Med Sci Monit 2022; 28:e937697
Abstract
BACKGROUND: Ensuring the take rate of skin grafting and reducing the mortality of patients with severe burns have remained big challenges worldwide. This retrospective study from a single center aimed to evaluate the efficacy of pulsed lavage following excision of burns ≥30% of the total body surface area (TBSA) in 63 patients.
MATERIAL AND METHODS: Among 63 patients, the types of burns sustained were severe burns and extremely severe burns (≥30% TBSA). The degrees of the burns were second degree and third degree, and the causes were thermal, chemical, and electric. Patients with early aggressive excision were divided into a pulsed lavage group and control group. The constituent of the lavage fluid was 0.9% physiological saline. The evaluation of wound healing and complications was based on the wound healing rate and time, clinical symptoms, and examination. We determined the take rate of skin grafting, positive rate of postoperative bacterial cultures, changes in perioperative serum C-reactive protein (CRP) and procalcitonin (PCT) levels, and incidence of secondary grafting.
RESULTS: The take rate of skin grafting and the decreased rates of perioperative serum CRP and PCT levels were significantly higher in the pulsed lavage group than in the control group (P<0.05). Moreover, the positive rate of wound postoperative bacterial cultures and mortality in the pulsed lavage group showed remarkably lower levels (P<0.05).
CONCLUSIONS: Pulsed lavage following excision of burns ≥30% TBSA increased the take rate of skin grafting, alleviated the positive rate of postoperative bacterial cultures, decreased serum CRP and PCT levels, and reduced mortality.
Keywords: autografts, Burns, Flushing, Surgical Wound, Humans, Body Surface Area, Therapeutic Irrigation, Skin Transplantation, C-Reactive Protein
Background
Burns are a common clinical disease of sudden trauma, with an annual global incidence of 11 million people. This trauma has become a global public health concern, with high disability and mortality rates [1,2]. As early as the nineteenth century, Sneve, a pioneer of burns, said that “there is no more frightful accident than severe burn of a large area.” A severe systemic response can be caused by a severe burn, which can lead to several complications, such as hypovolemic shock, sepsis, and multiple organ dysfunction syndrome, and can even threaten a patient’s life [3,4]. Severe burn wounds differ from other acute skin lesions with systemic effects because of their complex healing [5]. The necrotic tissue in deep burn wounds can cause excessive local inflammatory response, deepen the progressive damage to the wound, increase the risk of infection, and affect the outcome [6,7].
The guideline for the burned skin evaluation was followed according to the extent of the burns, usually calculated by the percentages of total body surface area (TBSA) burned and the estimated depth of the burns, including superficial burns (first degree), partial thickness burns (second degree), and full thickness burns (third degree) [8]. For severe burns, all patients were resuscitated with Ringer’s lactated fluid and plasma according to the Chinese formula (1.5 mL/[kg·%TBSA] crystalloids and colloids plus 2000 mL of water) during the first 24 h after the burn occurred. However, the fluid resuscitation formula for burns is only an estimate, and the specific fluid treatment plan needs to be determined based on vital signs, urine output, other injuries, and other medical conditions [9]. Aggressive excision and wound closure have been documented to be effective treatments to improve the outcome of severe burns [10]. Aggressive excision is the removal necrotic eschar to develop a vascularized wound bed for autografting. However, some open wound remains, which is a rich pabulum for growth of microorganisms that can cause further inflammatory problems and even invasive infections in the course of this procedure. The failure of skin grafting after excision and infection are the 2 main factors that lead to life-threatening sepsis, which is the most common cause of death in severely burned patients [11,12]. Therefore, how to increase the take rate of grafting and reduce the incidence of infection after aggressive excision is a big challenge for surgeons [13].
Pulsed lavage is a high-pressure irrigation technique to primarily debride wounds [14,15]. Its principle involves the separation of the bacteria and dirt on the wound surface from the tissue by the vibration of a pulsed liquid flow during debridement. The flow and pressure of flushing can be controlled, and a clear surgical vision is facilitated by the pulsed irrigator. In addition, the lavage fluid can be sucked automatically during the flushing process [16,17]. Pulsed lavage irrigation has been widely used in orthopedic procedures, such as knee surgery, to reduce the postoperative infection rate [18]. For example, Nikfarjam et al confirmed that pulsed irrigation of laparotomy wounds in operations exceeding 2 h reduced surgical site infections after major hepatobiliary pancreatic surgery [19]. Surgical site infections appear to be reduced with pulsatile lavage irrigation of wounds before skin closure in patients undergoing prolonged intraabdominal surgeries [20]. Ahn et al confirmed pulsed irrigation was more effective than bulb syringe irrigation in the posterior muscle layer [21]. Bath et al also found pulsed irrigation was more effective than bulb syringe irrigation in the posterior muscle layer [22]. Fei et al confirmed that a pulsed lavage group, closed drainage group, and iodine lavage group all showed much better postoperative infection prevention than the saline lavage group [23].
It is speculated that effective cleansing of the wound bed with a technique such as pulsed lavage to remove excess organisms might alleviate some of these issues in severely burned patients. Further, it may better prepare the wound bed for successful autografting. However, little information on its clinical effectiveness in severe burn patients undergoing aggressive excision is available. In the present study, the effects of pulsed lavage during early excision on the infection control, autografting, and mortality of severely burned patients were investigated. Therefore, this retrospective study from a single center aimed to evaluate the efficacy of pulsed lavage following excision of burns ≥30% of the TBSA in 63 patients.
Material and Methods
PATIENTS:
The study was conducted at the Burns Centre of Anhui Medical University Hospital and covered the period from 2017 to 2020. Inclusion criteria were age 3 years to 80 years old and burn size ≥30% TBSA. Exclusion criteria were as follows: pregnancy or lactation; cerebral hemorrhage; serious mental conditions; history of malignant tumor; autoimmune disease; hemophilia; or patients with coagulopathy caused by systemic diseases. A total of 63 burn patients who underwent early excision and grafting were retrospectively enrolled in the study. This study was approved by the Medical Ethics Committee of the First Affiliated Hospital of Anhui Medical University, and informed consent was waived because the study was retrospective in design.
All patients were resuscitated with Ringer’s lactated fluid and plasma according to the Chinese formula (1.5 mL/[kg·%TBSA] crystalloids and colloids plus 2000 mL of water) during the first 24 h after the burn; the formula was modified according to the response of each patient. Before the initial excision and skin grafting, the wounds were treated by changing the dressing daily and topically applying silver sulfadiazine. Then, 2 to 10 days after thermal injury, patients with stable physiological parameters underwent aggressive excisions and skin grafting at the initial surgery, during which the deep burn wounds on the extremities were always excised first. The 63 patients were divided into 2 groups: the pulsed lavage group (n=30) and control (n=33) group.
PROCEDURES OF PULSED LAVAGE AND CONVENTIONAL IRRIGATION:
Before surgical treatment, the burn wounds of all patients were disinfected at the surgery sites, and different surgical methods were selected by assessing the depth of the burn wounds. During the surgical treatment, fascial excision was performed for full-thickness burns, and the necrotic tissue was excised down to the deep fascia. Tangential excision was performed for deep partial-thickness burns; that is, the necrotic tissue was removed with dermatome, and the normal dermis and adipose tissue were preserved. Bleeding points on the wounds were treated by electrocoagulation or ligation hemostasis methods after aggressive excision. Before the excised burn wounds were covered with autografts or allografts, the wounds were rinsed using different flushing modes in the 2 groups. The procedures were performed under strict aseptic operating conditions.
PULSED LAVAGE GROUP:
As shown in Figure 1, the pulsed irrigator (electric pulse flushing suction apparatus) consisted of a host machine, built-in power supply, negative pressure tube, inlet pipe, outlet pipe, and flushing nozzle with an aspirator. The pulsed irrigator (APEXPULSETM) was made by Apex Tools & Orthopedics Company, Guangzhou, China. The lavage fluid was 0.9% physiological saline (Foshan Shuanghe Pharmaceutical Co., Ltd., Guangzhou, China).
To facilitate the flushing, patients were placed on the operating table in the best position, a sterile basin was kept below the wounds, and the table was covered with waterproof sheeting. The total volume of irrigating solution (0.9% physiological saline) depended on the situation of the wounds [23]. The volume generally was not less than 6000 mL for patients with severe burns. The pulsed irrigator was divided into 2 levels (high/low), according to the frequency of flushing. The pulsed irrigators were connected to the negative pressure devices by a negative pressure tube and ensured that the flushing nozzles were held vertically in total circumferential contact with the wound surface. The devices were started when the surgeon pulled the trigger. The pulsed irrigators were applied to the wounds with pulsed lavage at 10 to 15 pounds per square inch (psi) of pressure, and the angles were modified according to the actual burn situation. The area of the wounds under the flushing nozzles were subjected to negative pressure, which separated the bacteria from the normal tissue. Meanwhile, the built-in negative-pressure suction tube sucked away the waste liquid. The flushing nozzles were kept on another area, and the pulse irrigator was restarted. These steps were repeated in the sequences from the deep to the shallow part of the wounds. The entire surface of the wounds was covered in this manner. The specific treatment process is shown in Figures 2–4.
CONTROL GROUP:
The conventional method, which is called pouring flush, was applied to the control group. Similar to in the pulsed lavage group, under strict aseptic conditions, patients were placed on the operating table in the best position, a sterile basin was kept below the wounds, and the table was covered with waterproof sheeting. The lavage fluid (0.9% physiological saline) was poured over the surgical site perpendicularly over the wound surface at 30 cm away by the surgeons. The wound dirt was wiped off with a sterile gauze during rinsing.
WOUND COVERAGE:
After being rinsed, the wounds were further hemostasized by electrocoagulation. Based on the burned and donor area, different skin grafting methods were used to cover the wound, such as stamped autograft, meshed skin grafting, microskin autografting, and Meek technique skin grafting. Finally, the wound was pressure-bandaged with sterile gauze.
DATA COLLECTION:
The demographic data were retrieved from the electric medical record system. The take rate of skin grafting, positive rate of postoperative bacterial cultures, changes in the perioperative inflammation-related markers (serum CRP and PCT levels), incidence of secondary grafting, and mortality were collected and analyzed to determine whether pulsed lavage had a positive effect on early excision and wound closure.
STATISTICAL ANALYSIS:
Statistical analysis was performed using SPSS software (version 26.0). The measurement data are expressed as mean±SD. The independent-sample
Results
DEMOGRAPHIC DATA OF PATIENTS:
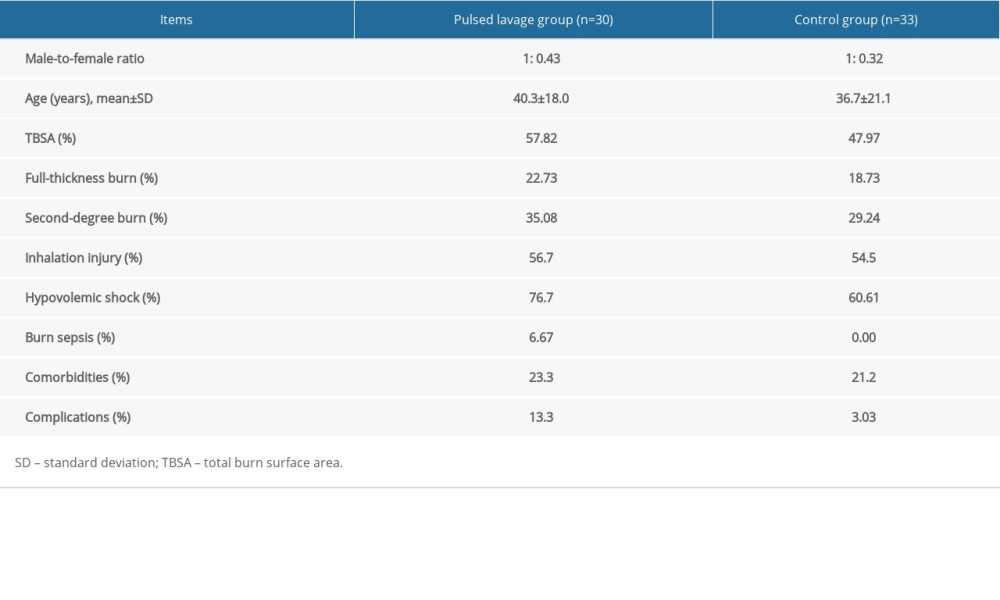
The demographic data of the patients are shown in Table 1. In the pulsed lavage group, there were 21 male and 9 female patients. On admission, they were aged 40.3±18.0 years, and the mean BSA burned was 57.8%. The mean burn areas of partial-thickness and full-thickness were 35.1% and 22.7%, respectively. Seventeen patients had inhalation injury, 23 patients had hypovolemic shock, and only 1 patient had burn sepsis on admission. In the control group, there were 25 male and 8 female patients. On admission, they were aged 36.7±21.1 years, and the mean BSA burned was 48.0%. The mean burn areas of partial-thickness and full-thickness were 29.2% and 18.7%, respectively. Eighteen patients had inhalation injury, 20 patients had hypovolemic shock, and no patient had burn sepsis on admission.
No statistical differences were found in sex, age, burn area and depth, inhalation injury, hypovolemic shock, burn sepsis, and other comorbidities between the 2 groups (all
TAKE RATE OF SKIN GRAFTING:
The take rate of skin grafting is one of the most reliable indices of the effectiveness of the healing of burn wounds [6]. As shown in Figure 5, the take rate of skin grafting was significantly higher in the pulsed lavage group than in the control group (84.93±8.59 vs 74.40±11.74, P<0.05).
POSITIVE RATE OF POSTOPERATIVE BACTERIAL CULTURES:
During burn wound treatment, inhibition of bacterial growth is important for wound healing effects [24]. Hence, the positive rate of postoperative bacterial cultures was compared between the pulsed lavage and control groups. The positive rate of the postoperative bacterial cultures of the 2 groups was calculated as follows:
Positive rate of postoperative bacterial cultures (%) = number of positive postoperative bacterial cultures / total number of patients in each group.
As shown in Figure 6, the positive rate of the postoperative bacterial cultures was significantly lower in the pulsed lavage group than in the control group (6.67% vs 36.4%, P<0.05).
CHANGES OF THE PERIOPERATIVE SERUM CRP LEVELS:
CRP is an indicator parameter that is widely used for inflammation [25]. To assess whether the systemic inflammatory response differed in the 2 groups, the perioperative serum CRP levels were examined by the immunoturbidimetry method using a Beckman AU5800 biochemical analyzer. Before surgery, no significant difference was found in the preoperative serum CRP levels between the 2 groups (166.77±46.68 mg/L vs 145.03±38.98 mg/L, P>0.05). After surgery, no significant difference was found in the serum CRP levels between the 2 groups (123.18±43.21 mg/L vs135.45±32.93 mg/L, P>0.05).
To assess the changes in serum CRP levels, the decreased rates were compared between the pulsed lavage and control groups. The decreased rates of both groups were calculated as follows:
Decreased rates(%) = (preoperative serum CRP level – postoperative serum CRP level) / preoperative serum CRP level.
As shown in Figure 7, the decreased rates (%) were significantly higher in the pulsed lavage group than in the control group (24.07±24.18 vs 4.18±17.36, P<0.05).
CHANGES OF THE PERIOPERATIVE SERUM PCT LEVELS:
PCT is a useful parameter to characterize systemic inflammation, infection, and sepsis. The serum PCT level increases in cases of sepsis and in severe systemic inflammatory reactions [26]. Hence, the perioperative serum PCT levels were examined by the method of enzyme-linked fluorescent immunoassay using a VIDAS30 fluorescence immunoassay analyzer. Before surgery, no significant difference was found in the preoperative serum PCT levels between the 2 groups (3.54±7.34 ng/L vs 8.48±10.27 ng/L, P>0.05). After surgery, the serum PCT level was significantly lower in the pulsed lavage group than in the control group (0.72±0.67 ng/L vs 4.46±5.06 ng/L, P<0.05).
To assess the changes in serum PCT levels, the decreased rates were compared between the pulsed lavage and control groups. The decreased rates were calculated in the same way as the decreased rates of serum CRP. As shown in Figure 8, the decreased rates were significantly higher in the pulsed lavage group than in the control group (57.60±30.34 vs 35.27±33.73, P<0.05).
INCIDENCE OF UNPLANNED REOPERATION OF SKIN GRAFTING:
To assess the recovery of the patients, the unplanned reoperation of skin grafting in both groups was analyzed. The unplanned reoperation of skin grafting was calculated as follows:
Unplanned reoperation of skin grafting (%) = number of unplanned reoperation / total number of patients in each group.
As shown in Figure 9, no significant difference was found between the 2 groups (20.0% vs 33.3%, P>0.05).
MORTALITY:
No deaths occurred during the period of treatment in the pulsed lavage group. The mortality was significantly lower in the pulsed lavage group than in the control group (0% vs 12.1%,
Discussion
Severe burn is one of the extremely serious forms of trauma with high mortality and has been associated with severe pain, distress, and reduced quality of life for the patients [27]. As mentioned in previous studies, the core links of burn treatment are anti-infective, anti-shock, and wound treatment of burn patients. Severe burn wounds differ from other acute wounds by the nature of their size, depth, and systemic effects, which are complicated to heal. Therefore, the treatment of burn wounds plays a vital role in wound healing, which influences the prognosis and quality of life of patients. Recent studies have noted that the advancement in burn treatment with early excision and grafting after resuscitation reduces the risk of infection and accelerates the healing of burn wounds by comparing the patients who underwent delayed excision and grafting [13]. However, the treatment approach that can improve the quality of wound healing remains a tough challenge in the clinical field for surgeons. Patients with severe burns are at higher risk of developing infection, and autograft grafting of severe burns is limited by insufficient supply [28]. Thus, controlling the extent of infection and increasing the take rate of grafting play a significant role in burn treatment research. Performing surgical debridement is particularly important, which is the basis of burn treatment, and thorough wound irrigation is one of the most significant debridement methods to promote the recovery of severe burns.
To solve this issue, wound irrigation was applied in the clinic. In the present study, we compared 2 methods of wound irrigation (pulsed lavage and conventional irrigation), aiming to evaluate the efficacy of pulsed lavage following excision of burns ≥30% TBSA. Given the numerous and complex factors that were difficult to control in the development of burn treatment, inclusion and exclusion criteria were applied. Comparative results indicated that pulsed lavage on the burn wounds after early excision had a more positive effect on the recovery of severe burn patients than conventional irrigation.
Almost all surgeons use some form of wound irrigation at the end of surgery. Pulsed lavage, as a relatively novel irrigation technique, has been suggested in recent studies to provide a potential benefit in reducing surgical site infections, thereby accelerating wound healing [29]. In the course of surgical procedures, pulsed lavage has been widely used in many fields, including major hepatobiliary pancreatic surgeries, intraabdominal surgeries, and spinal surgeries [19–22]. However, in the present study, we aimed to evaluate the efficacy of pulsed lavage following excision of burns ≥30% TBSA, which is different from previous studies in the field of treatment. The results of this study may prove valuable in the further wound treatment of severe burns.
The functions of wound irrigation are as follows: the blood and dirt on the wound surface are washed away for easy observation, the remaining bacteria are removed to lower the susceptibility to infection, and the original color of the tissue is exposed to determine whether the tissue is alive or not [30].
In the present study, after early excision and hemostasis of the surgical procedure, the conventional irrigation method was applied to the control group. The lavage fluid was poured directly into the wound surface to wash away dirt, blood clots, and other substances through the fluidity of the liquid. This conventional method cannot carry away bacteria. Several studies have reported that the whole irrigation process is complex, such that the bacteria can easily invade it. In addition, the lavage fluid cannot be continuously flushed, the angles of irrigation are difficult to control, the irrigation pressure cannot be guaranteed, and the blind angles cannot be flushed. If the sites of irrigation need to be changed, the position of patients need to be changed repeatedly. This process may aggravate the injury, destroy the biological barrier, and make the patient more susceptible to infection [31].
In the pulsed lavage group, the pulsed irrigators were applied to the wound debridement after early excision. The pulsed irrigator is a common device applied in surgical debridement, which is relatively uncommon for burns. This device is suitable for rinsing the wounds caused by a vascular, neurogenic, and pressure ulcer or trauma, and the technique is slightly modified from the conventional irrigation. In this study, the take rate of skin grafting was significantly higher in the pulsed lavage group than in the control group. In addition, the rate of postoperative bacterial cultures of wound surface was markedly lower in the pulsed lavage group than in the control group, which confirmed that the pulsed lavage had completely overcome the defects of conventional irrigation.
The principle of a pulsed irrigator is to use the high-pressure gas of eddy current principle to press out the water. By using the pulsed irrigator, the liquid becomes pulse flows, in which the lavage fluid and compressed air are mixed to form a liquid mist. In the pulsed lavage technique, the pulsed fluid flow has pressurization and decompression periods which can loosen the dirt, blood clots, and bacteria. These particles can be easily discharged by generating shock changes of different frequencies and strengths, leading to a more thorough rinsing with the help of the “bouncing effect” [32]. Meanwhile, the effects of the pulsed fluid flow cause the microdeformation of cells and stimulate granulation tissue formation. In our practice, different irrigation joints were selected according to the various sites of the burn wounds. Hence, pulsed lavage was more flexible and effective for surgeons to rinse burn wounds with more complete debridement. This process leads to a lower rate of infection and higher take rate of skin grafting than the conventional irrigation [33].
In addition to the indicators in vitro of the wound surface, the inflammatory indicators in vivo of severe burn patients were observed. CRP and PCT are 2 well-documented indicators of infection [26]. Changes in the perioperative serum CRP and PCT levels were recorded, and the decreased rates were compared between the 2 groups. In the present study, the decreased rates of the serum CRP and PCT levels were significantly higher in the pulsed lavage group than in the control group.
CRP is a protein that can react with pneumococcal C polysaccharides to form a complex. CRP is an indicator of inflammatory activity in the acute phase, which increases rapidly within hours after the onset of various diseases, such as acute inflammation, tissue damage, myocardial infarction, surgery, burn trauma, and radiation injury. This protein has a tendency to increase exponentially [34]. In general, the serum CRP levels reflect the severity of tissue injury and infection and the degree of inflammatory response [35]. The percent change in serum CRP has been demonstrated to serve as a more accurate marker of infection risk than an absolute threshold value [36]. PCT is also an acute-phase protein that can be used to predict the systemic inflammation and the bacterial infections of patients. The serum PCT levels increase during severe bacterial, fungal, and parasitic infections, sepsis, systemic inflammatory response syndrome, and multiple organ dysfunction syndrome. This protein reflects the extent of the systemic inflammatory response, and the increase in serum PCT levels usually appears in severe shock and multiple organ dysfunction syndrome [28]. In this study, serum CRP and PCT levels rose rapidly within a very short time after the severe burns. The patients responded relatively to the different methods of the wound irrigation after early excision and grafting. The serum CRP and PCT levels decreased, and they decreased more rapidly in the pulsed lavage group than in the control group. Therefore, statistically, the results demonstrated a more rapid decrease in the systemic inflammation response with pulsed lavage, thereby helping promote the physical functioning of the patients to recover better and faster.
Severe burn wounds, generally caused by local thermal exposures, lead to life-threatening systemic effects. Previous studies have shown that the prognostic indicators, which included the incidence of secondary skin grafting and the rate of mortality in burn patients, were associated with numerous factors, such as age, TBSA (or burn index), inhalation injury, and surgical management [37]. Lower rates of secondary skin grafting and mortality are characteristics of better recovery for patients. Furthermore, mortality is the most important and intuitive outcome reflecting the effect of treatment [38]. In the present study, there were no deaths in the pulsed lavage group, and the mortality rate was markedly lower in the pulsed lavage group than in the control group.
However, no significant difference was found in the incidence of secondary skin grafting between the pulsed lavage and control groups. Many factors affect the occurrence of secondary skin grafting. The main reason for the absence of a statistically significant difference can be due to an insufficient sample size. In the future, we will continuously update the reference data and deeply explore this aspect.
Since 2017, considerable practical experience with the application of pulsed lavage has been gained in our burn center. The advantages of pulsed lavage for the treatment of burn wounds are summarized as follows. First, the pulsed fluid flow of the pulse irrigator can rinse the wound surface quickly and thoroughly and focus on removing the residual necrotic tissue and bacteria. Second, the wasted liquid can collect in time while being flushed by the pulsed irrigators, which can reduce the risk of infection by carrying away the bacteria and dirt immediately. Meanwhile, the rinsing time and the whole operation time can be shortened, reducing the risk of the operation. Third, the pressure of pulsed lavage is controllable for surgeons, and this process is safe and reliable. Pulsed lavage reduces the secondary damage to the surrounding normal tissue.
During the pulsed lavage, whether the pressure of flushing is appropriate should be given attention. In standard practice, this process can remove the dirt and bacteria on the wound surface but does not damage the cells and normal tissues. The wound should be rinsed with a sufficient quantity of fluid and a certain impact to achieve a better effect. However, wounds need adequate hemostasis before pulsed lavage to prevent blood coagulation or damage to the exposed nerve endings [39].
The main limitations of this study were as follows. First, this was only a retrospective study. An open, prospective, randomized controlled study is needed to compare the efficacy of pulsed lavage in the treatment of burns of over 30% TBSA. Second, the sample size was only 63 during 2017 to 2020 due to the limited number of patients with severe burns. In our opinion, a larger sample size would yield more reliable data. Third, although no statistical differences were found in the baseline parameters, such as sex, age, burn area and depth, inhalation injury, hypovolemic shock, and burn sepsis, between the 2 groups, selection bias was difficult to avoid.
Conclusions
The clinical experience by comparing the wound treatment by using pulsed lavage and conventional irrigation in severe burns at the Anhui Medical University Hospital Burn Center indicated that pulsed lavage following excision of burns over 30% TBSA increased the take rate of skin grafting, alleviated the positive rate of postoperative bacterial cultures, decreased serum CRP and PCT levels, and reduced mortality.
Figures
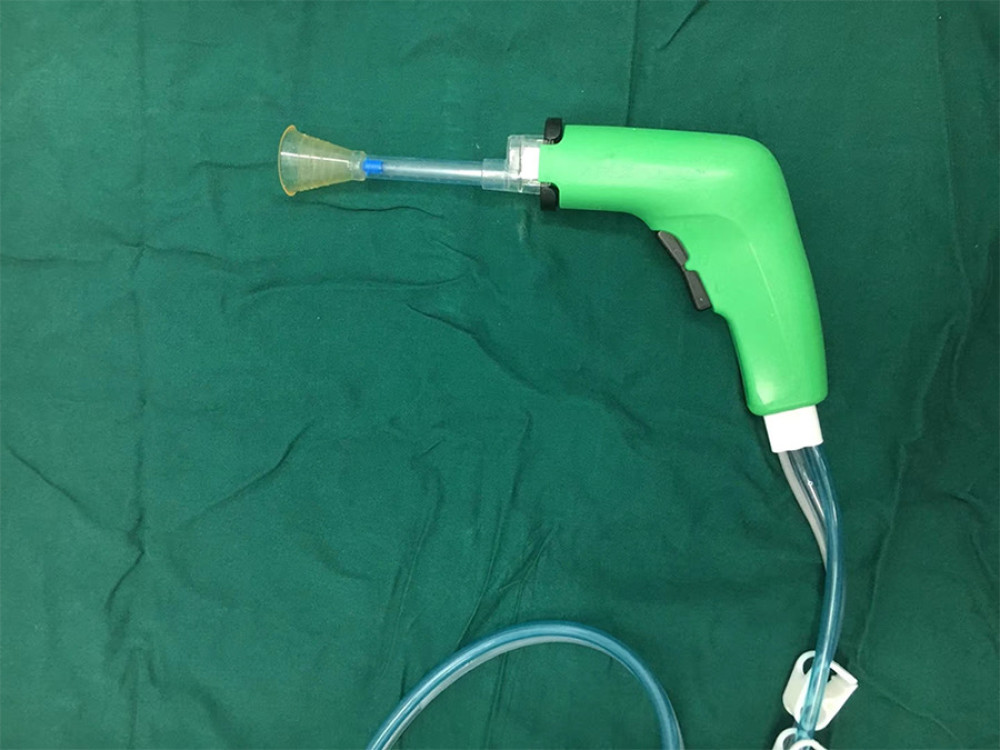 Figure 1. A photograph of the pulsed irrigator (electric pulse flushing suction apparatus).
Figure 1. A photograph of the pulsed irrigator (electric pulse flushing suction apparatus). 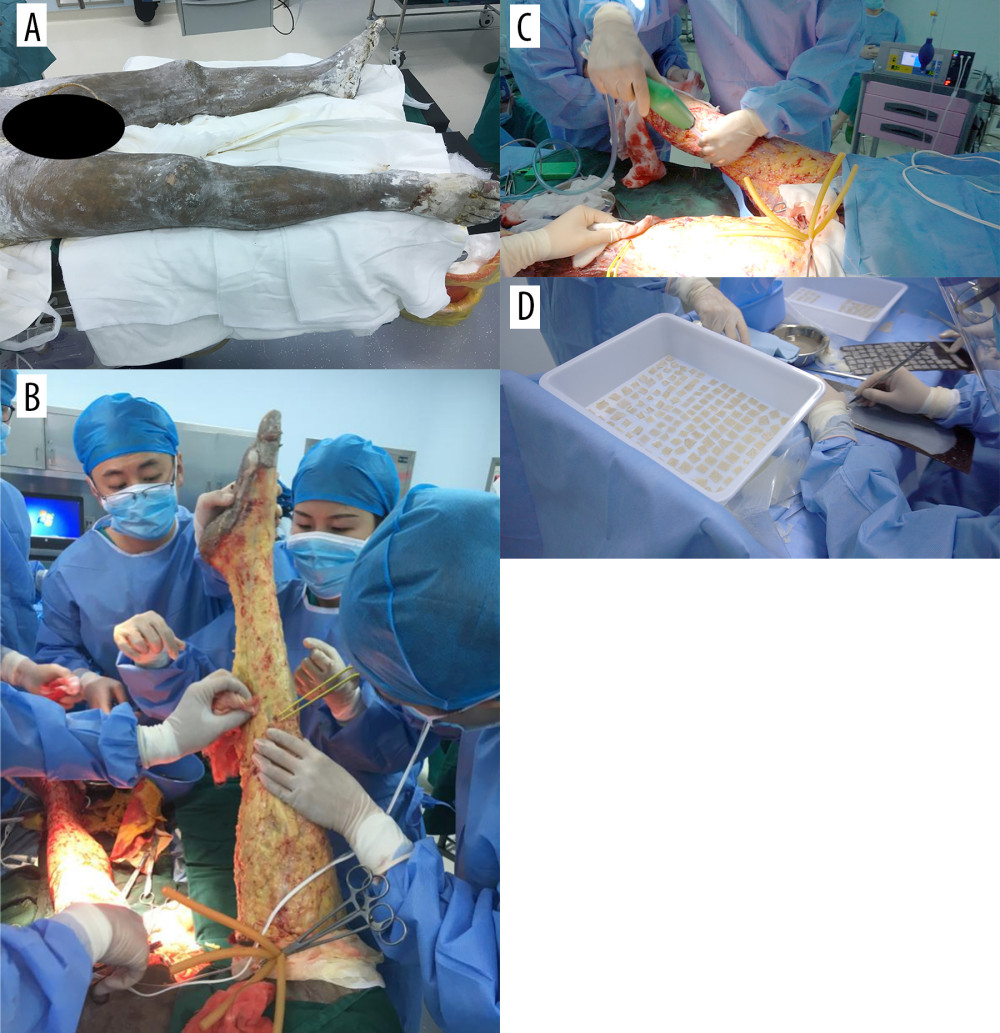 Figure 2. Pulsed lavage application of severe burns. (A) A 49-year-old male patient with a 60% total burn surface area (TBSA) burn. The surgical procedure was performed on the sixth day after the burn, during which 40% TBSA of full-thickness burn eschar was found on both lower extremities before the operation. (B) The wounds of both lower extremities were excised to the level of the normal adipose tissue or the fascia, and electrocoagulation or ligation hemostasis methods were applied after aggressive excision. (C) The pulsed irrigator was applied to rinse the wound surface with flexible angles. (D) The stamped autograft method was used to cover the wound, according to the condition of the wounds.
Figure 2. Pulsed lavage application of severe burns. (A) A 49-year-old male patient with a 60% total burn surface area (TBSA) burn. The surgical procedure was performed on the sixth day after the burn, during which 40% TBSA of full-thickness burn eschar was found on both lower extremities before the operation. (B) The wounds of both lower extremities were excised to the level of the normal adipose tissue or the fascia, and electrocoagulation or ligation hemostasis methods were applied after aggressive excision. (C) The pulsed irrigator was applied to rinse the wound surface with flexible angles. (D) The stamped autograft method was used to cover the wound, according to the condition of the wounds. 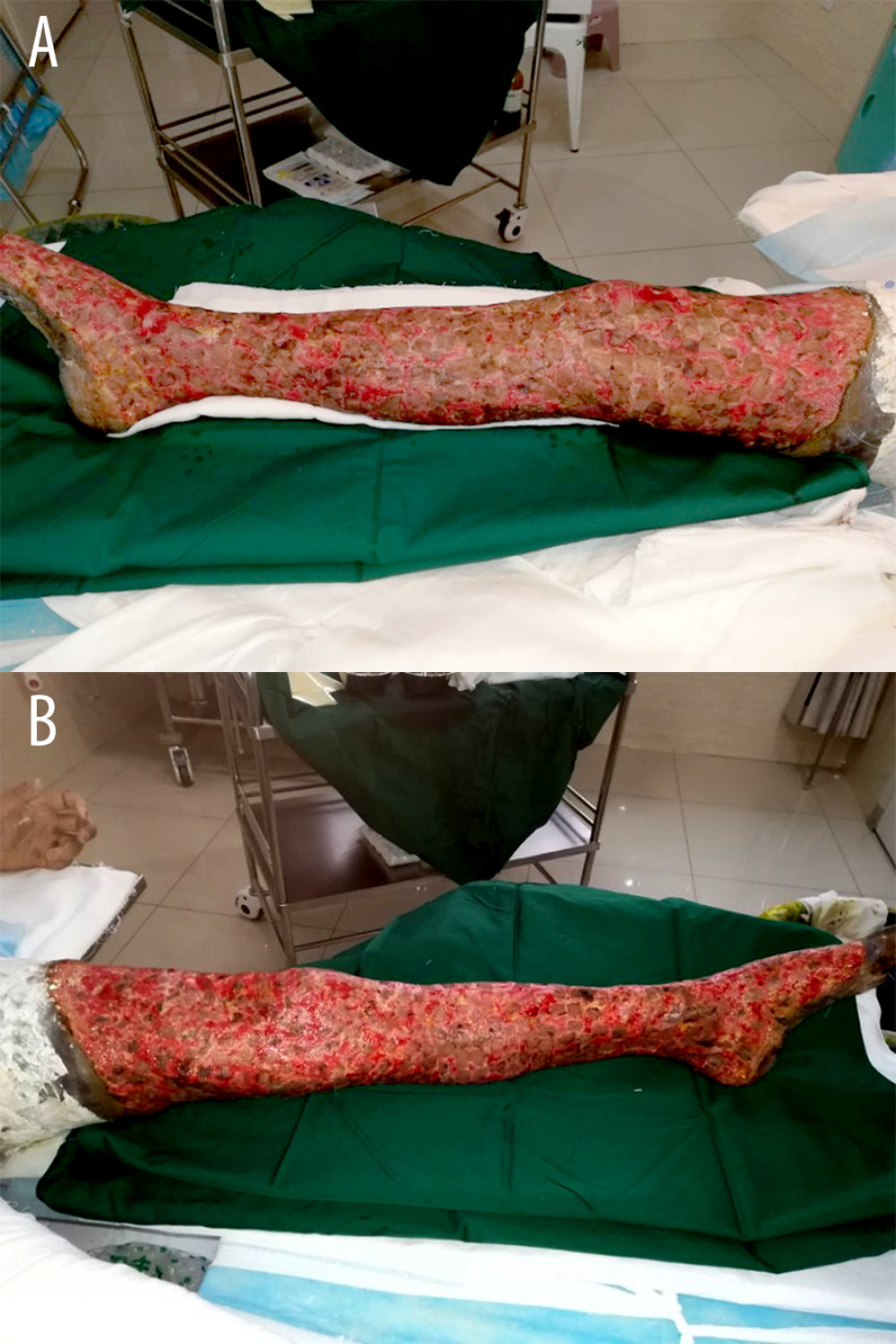 Figure 3. Skin graft 1 week after the operation. (A, B) The skin grafts took well 1 week after the operation, and the take rate of skin grafting was almost 100%.
Figure 3. Skin graft 1 week after the operation. (A, B) The skin grafts took well 1 week after the operation, and the take rate of skin grafting was almost 100%. 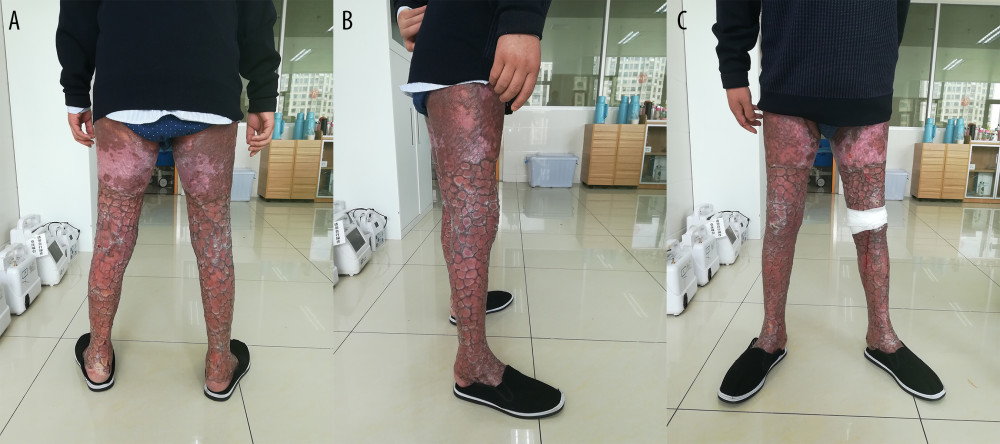 Figure 4. Follow-up at 6 months after discharge. (A–C) Six months after discharge, the autografts remained stable, and the patient could walk by himself without a walking stick.
Figure 4. Follow-up at 6 months after discharge. (A–C) Six months after discharge, the autografts remained stable, and the patient could walk by himself without a walking stick. 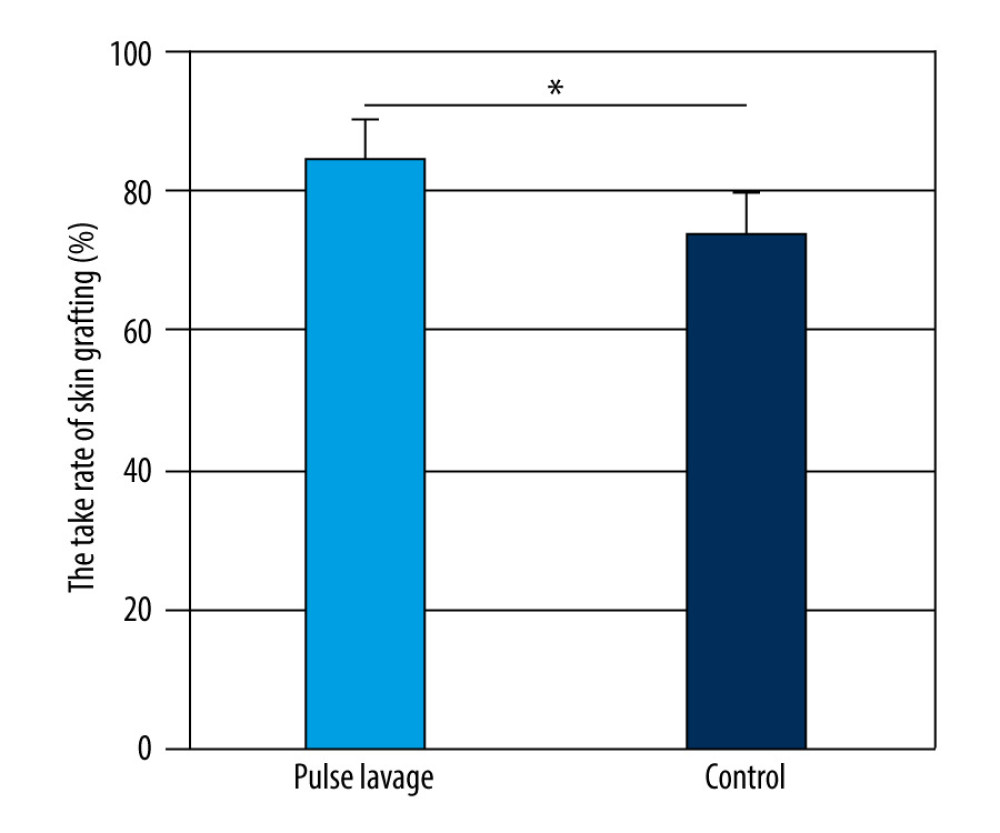 Figure 5. The take rate of skin grafting of the 2 groups. The take rate of skin grafting was significantly higher in the pulsed lavage group than that in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 5. The take rate of skin grafting of the 2 groups. The take rate of skin grafting was significantly higher in the pulsed lavage group than that in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. 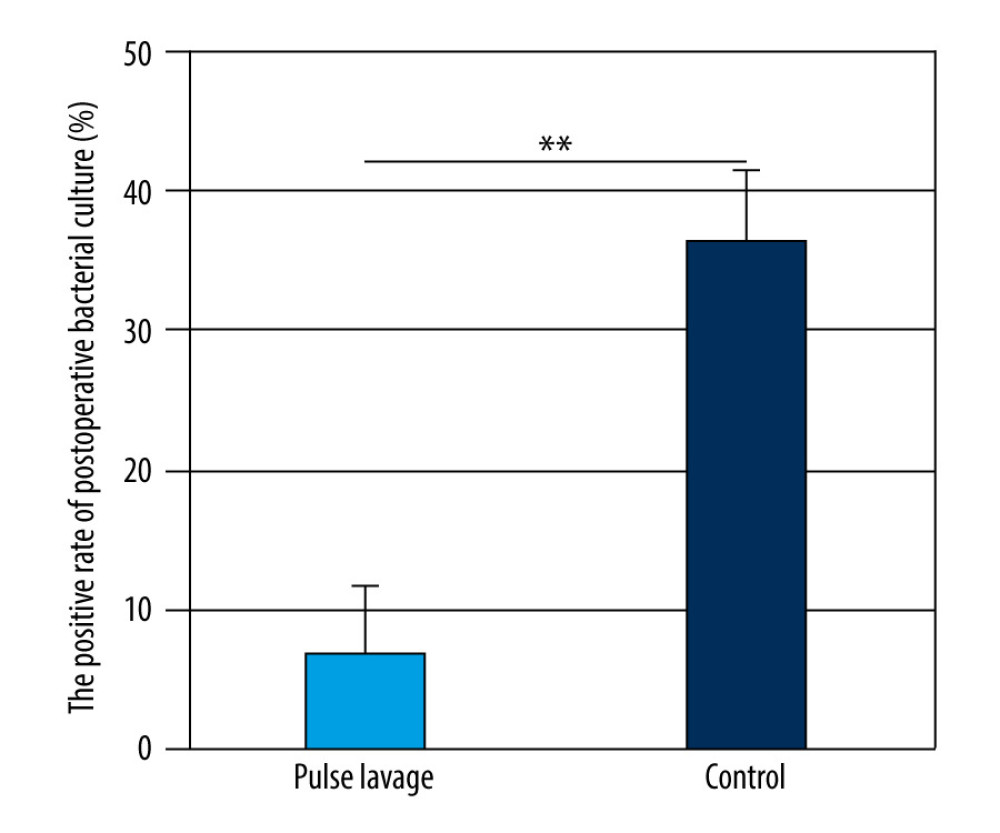 Figure 6. The positive rate of postoperative bacterial cultures of the 2 groups. The positive rate of postoperative bacterial cultures of the pulsed lavage group was significantly lower than that in the control group, with ** P<0.01. Microsoft Excel (version 2209) was used for figure creation.
Figure 6. The positive rate of postoperative bacterial cultures of the 2 groups. The positive rate of postoperative bacterial cultures of the pulsed lavage group was significantly lower than that in the control group, with ** P<0.01. Microsoft Excel (version 2209) was used for figure creation. 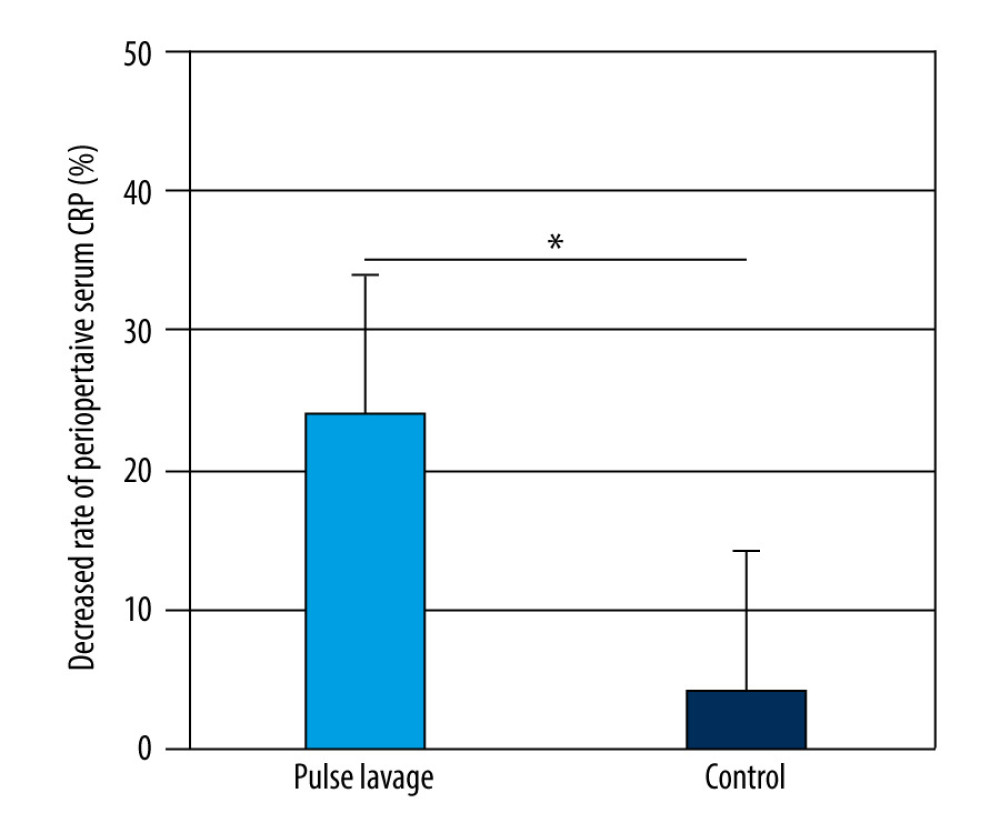 Figure 7. Decreased rates of serum C-reactive protein (CRP) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 7. Decreased rates of serum C-reactive protein (CRP) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. 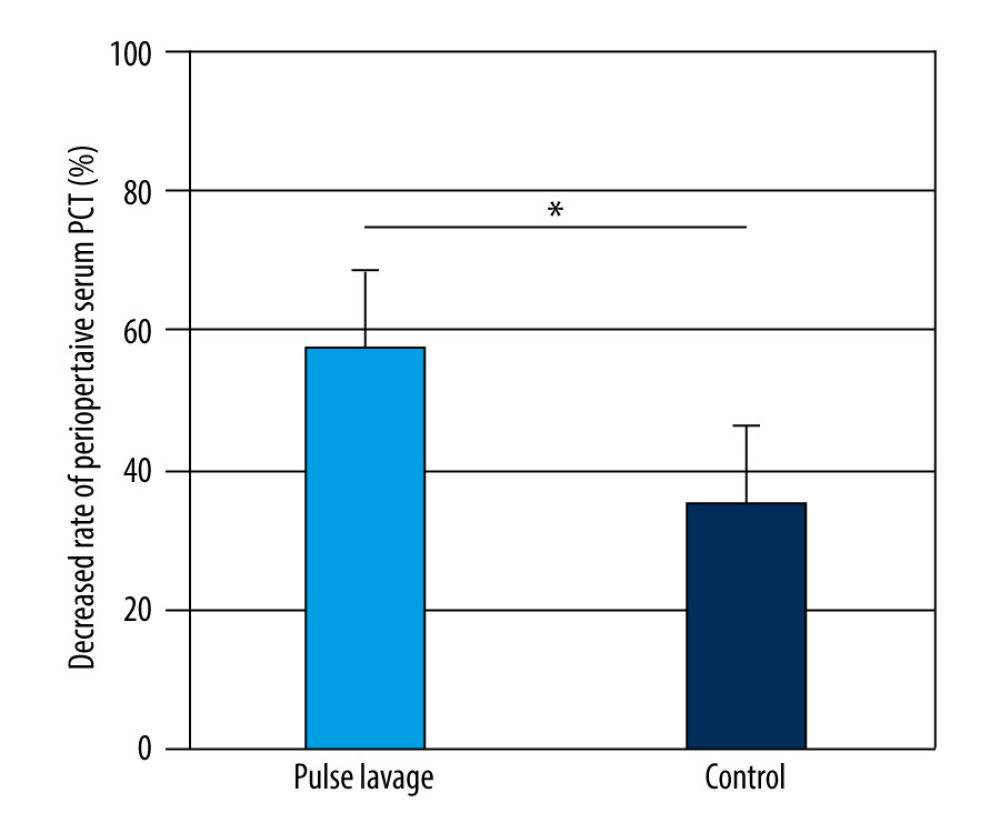 Figure 8. Decreased rates of serum procalcitonin (PCT) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 8. Decreased rates of serum procalcitonin (PCT) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. 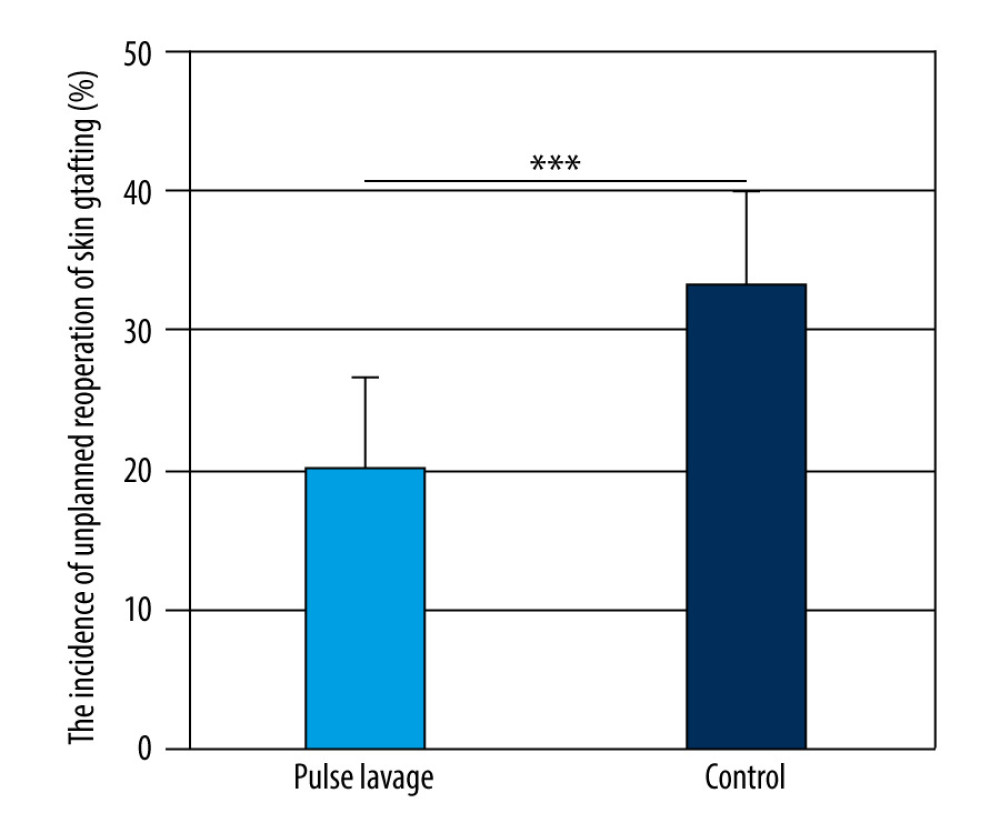 Figure 9. The incidence of unplanned reoperation of skin grafting of the 2 groups. There was no significant difference between the 2 groups, with *** P>0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 9. The incidence of unplanned reoperation of skin grafting of the 2 groups. There was no significant difference between the 2 groups, with *** P>0.05. Microsoft Excel (version 2209) was used for figure creation. References
1. Friston D, Laycock H, Nagy I, Want EJ, Microdialysis workflow for metabotyping superficial pathologies: Application to burn injury: Anal Chem, 2019; 91(10); 6541-48
2. Tian H, Wang L, Xie W, Epidemiologic and clinical characteristics of severe burn patients: Results of a retrospective multicenter study in China, 2011–2015: Burns Trauma, 2018; 6; 14
3. Brandenburg KS, Weaver AJ, Karna SLR: Sci Rep, 2019; 9(1); 13627
4. Zhang P, Zou B, Liou YC, Huang C, The pathogenesis and diagnosis of sepsis post burn injury: Burns Trauma, 2021; 9; tkaa047
5. Khan A, Xu M, Wang T: Biosci Rep, 2019; 39(6); BSR20190504
6. Tapking C, Popp D, Herndon DN, Cardiac dysfunction in severely burned patients: Current understanding of etiology, pathophysiology, and treatment: Shock, 2020; 53(6); 669-78
7. Hofmann E, Fink J, Eberl A, A novel human ex vivo skin model to study early local responses to burn injuries: Sci Rep, 2021; 11(1); 364
8. Schaefer TJ, Szymanski KD: Burn evaluation and management, 2022, StatPearls, Treasure Island (FL)
9. Ben DF, Ma B, Chen XL, Burn injuries caused by ship fire: A 12-year study in Shanghai: Burns, 2010; 36(4); 576-80
10. Tompkins RG, Survival from burns in the new millennium: 70 years’ experience from a single institution: Ann Surg, 2015; 261(2); 263-68
11. Russell CD, Schwarze J, The role of pro-resolution lipid mediators in infectious disease: Immunology, 2014; 141(2); 166-73
12. Cartotto R, Topical antimicrobial agents for pediatric burns: Burns Trauma, 2017; 5; 33
13. Farhan N, Jeffery S, Diagnosing burn wounds infection: The practice gap & advances with moleculight bacterial imaging: Diagnostics (Basel), 2021; 11(2); 268
14. Golz A, Yun J, Garbis N, Salazar D, The effect of pulsed lavage irrigation on suture knot security: J Orthop Surg (Hong Kong), 2020; 28(1); 2309499019888129
15. Huljev DDebridement-crucial procedure in the treatment of chronic wounds: Acta Med Croatica, 2013; 67(Suppl 1); 63-69 [in Croatian]
16. Ratto N, Arrigoni C, Rosso F, Total knee arthroplasty and infection: How surgeons can reduce the risks: EFORT Open Rev, 2016; 1(9); 339-44
17. Yang Z, Dai S, Treatment of infection with improved pulsed lavage: Wounds, 2013; 25(9); 251-55
18. Poilvache H, Ruiz-Sorribas A, Sakoulas G: Front Med (Lausanne), 2020; 7; 527
19. Nikfarjam M, Weinberg L, Fink MA, Pressurized pulse irrigation with saline reduces surgical-site infections following major hepatobiliary and pancreatic surgery: Randomized controlled trial: World J Surg, 2014; 38(2); 447-55
20. Nikfarjam M, Kimchi ET, Gusani NJ, Reduction of surgical site infections by use of pulsatile lavage irrigation after prolonged intra-abdominal surgical procedures: Am J Surg, 2009; 198(3); 381-86
21. Ahn DK, Lee S, Moon SH, Bulb syringe and pulsed irrigation: Which is more effective to remove bacteria in spine surgeries?: Clin Spine Surg, 2016; 29(1); 34-37
22. Bath MF, Powell J, Ismail I, Machesney MR, Use of pulsed lavage reduces the rate of surgical site infection after laparotomy: J Surg Res, 2021; 266; 300-5
23. Fei J, Gu JH, Comparison of lavage techniques for preventing incision infection following posterior lumbar interbody fusion: Med Sci Monit, 2017; 23; 3010-18
24. Oba J, Okabe M, Yoshida T, Hyperdry human amniotic membrane application as a wound dressing for a full-thickness skin excision after a third-degree burn injury: Burns Trauma, 2020; 8; tkaa014
25. Hofmaenner DA, Steiger P, Schuepbach RA, Safety of enzymatic debridement in extensive burns larger than 15% total body surface area: Burns, 2021; 47(4); 796-804
26. Peschanski N, Chenevier-Gobeaux C, Mzabi L, Prognostic value of PCT in septic emergency patients: Ann Intensive Care, 2016; 6(1); 47
27. Lami FH, Al Naser RK, Epidemiological characteristics of burn injuries in Iraq: A burn hospital-based study: Burns, 2019; 45(2); 479-83
28. Ma Z, Han J, Chang B: ACS Infect Dis, 2017; 3(11); 820-32
29. Bath MF, Suresh R, Davies J, Machesney MR, Does pulsed lavage reduce the risk of surgical site infection? A systematic review and meta-analysis: J Hosp Infect, 2021; 118; 32-39
30. Anghel EL, DeFazio MV, Barker JC, Current concepts in debridement: science and strategies: Plast Reconstr Surg, 2016; 138(3 Suppl); 82S-93S
31. Shetty R, Barreto E, Paul KM, Suction assisted pulse lavage: randomised controlled studies comparing its efficacy with conventional dressings in healing of chronic wounds: Int Wound J, 2014; 11(1); 55-63
32. Mundy LR, Gage MJ, Yoon RS, Liporace FA, Comparing the speed of irrigation between pulsatile lavage versus gravity irrigation: An ex-vivo experimental investigation: Patient Saf Surg, 2017; 11; 7
33. Norman G, Atkinson RA, Smith TA, Intracavity lavage and wound irrigation for prevention of surgical site infection: Cochrane Database Syst Rev, 2017; 10; CD012234
34. Dvorak JE, Ladhani HA, Claridge JA, Review of sepsis in burn patients in 2020: Surg Infect (Larchmt), 2021; 22(1); 37-43
35. Gao N, Yan C, Zhang G, Changes of serum procalcitonin (PCT), C-reactive protein (CRP), interleukin-17 (IL-17), interleukin-6 (IL-6), high mobility group protein-B1 (HMGB1) and D-dimer in patients with severe acute pancreatitis treated with continuous renal replacement therapy (CRRT) and its clinical significance: Med Sci Monit, 2018; 24; 5881-86
36. Stambough JB, Curtin BM, Odum SM, Does change in ESR and CRP guide the timing of two-stage arthroplasty reimplantation?: Clin Orthop Relat Res, 2019; 477(2); 364-71
37. Puthumana JS, Ngaage LM, Borrelli MR, Risk factors for cooking-related burn injuries in children, WHO Global Burn Registry: Bull World Health Organ, 2021; 99(6); 439-45
38. Du Y, Lv GZ, Yu S, Wang D, Tan Q, Long-term medical treatment of patients with severe burns at exposed sites: World J Clin Cases, 2020; 8(16); 3515-26
39. Lu J, Deegan AJ, Cheng Y, OCT-based angiography and surface topography in burn-damaged skin: Lasers Surg Med, 2021; 53(6); 849-60
Figures
 Figure 1. A photograph of the pulsed irrigator (electric pulse flushing suction apparatus).
Figure 1. A photograph of the pulsed irrigator (electric pulse flushing suction apparatus). Figure 2. Pulsed lavage application of severe burns. (A) A 49-year-old male patient with a 60% total burn surface area (TBSA) burn. The surgical procedure was performed on the sixth day after the burn, during which 40% TBSA of full-thickness burn eschar was found on both lower extremities before the operation. (B) The wounds of both lower extremities were excised to the level of the normal adipose tissue or the fascia, and electrocoagulation or ligation hemostasis methods were applied after aggressive excision. (C) The pulsed irrigator was applied to rinse the wound surface with flexible angles. (D) The stamped autograft method was used to cover the wound, according to the condition of the wounds.
Figure 2. Pulsed lavage application of severe burns. (A) A 49-year-old male patient with a 60% total burn surface area (TBSA) burn. The surgical procedure was performed on the sixth day after the burn, during which 40% TBSA of full-thickness burn eschar was found on both lower extremities before the operation. (B) The wounds of both lower extremities were excised to the level of the normal adipose tissue or the fascia, and electrocoagulation or ligation hemostasis methods were applied after aggressive excision. (C) The pulsed irrigator was applied to rinse the wound surface with flexible angles. (D) The stamped autograft method was used to cover the wound, according to the condition of the wounds. Figure 3. Skin graft 1 week after the operation. (A, B) The skin grafts took well 1 week after the operation, and the take rate of skin grafting was almost 100%.
Figure 3. Skin graft 1 week after the operation. (A, B) The skin grafts took well 1 week after the operation, and the take rate of skin grafting was almost 100%. Figure 4. Follow-up at 6 months after discharge. (A–C) Six months after discharge, the autografts remained stable, and the patient could walk by himself without a walking stick.
Figure 4. Follow-up at 6 months after discharge. (A–C) Six months after discharge, the autografts remained stable, and the patient could walk by himself without a walking stick. Figure 5. The take rate of skin grafting of the 2 groups. The take rate of skin grafting was significantly higher in the pulsed lavage group than that in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 5. The take rate of skin grafting of the 2 groups. The take rate of skin grafting was significantly higher in the pulsed lavage group than that in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. Figure 6. The positive rate of postoperative bacterial cultures of the 2 groups. The positive rate of postoperative bacterial cultures of the pulsed lavage group was significantly lower than that in the control group, with ** P<0.01. Microsoft Excel (version 2209) was used for figure creation.
Figure 6. The positive rate of postoperative bacterial cultures of the 2 groups. The positive rate of postoperative bacterial cultures of the pulsed lavage group was significantly lower than that in the control group, with ** P<0.01. Microsoft Excel (version 2209) was used for figure creation. Figure 7. Decreased rates of serum C-reactive protein (CRP) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 7. Decreased rates of serum C-reactive protein (CRP) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. Figure 8. Decreased rates of serum procalcitonin (PCT) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 8. Decreased rates of serum procalcitonin (PCT) of the 2 groups. The decreased rates in the pulsed lavage group were significantly higher than those in the control group, with * P<0.05. Microsoft Excel (version 2209) was used for figure creation. Figure 9. The incidence of unplanned reoperation of skin grafting of the 2 groups. There was no significant difference between the 2 groups, with *** P>0.05. Microsoft Excel (version 2209) was used for figure creation.
Figure 9. The incidence of unplanned reoperation of skin grafting of the 2 groups. There was no significant difference between the 2 groups, with *** P>0.05. Microsoft Excel (version 2209) was used for figure creation. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387