06 October 2022: Clinical Research
Anterior Talofibular Ligament All-Inside Arthroscopic Reconstruction with InternalBrace™ for Chronic Lateral Ankle Instability
Guang-Long Zeng1ABG, Li-Min Cai2CD, QingXiang Xie1EF, Hao-Bo Huang1E, Yong-Cong Li3F, Bo-Yuan Su1ABG*DOI: 10.12659/MSM.937699
Med Sci Monit 2022; 28:e937699
Abstract
BACKGROUND: Anterior talofibular ligament (ATFL) is the most easily injured or even broken of ankle sprain. Patients who fail to receive conservative treatment, resulting in persistent ankle swelling, painful and functional decline that it is so-called chronic lateral ankle instability (CLAI). It makes sense to investigate all-inside arthroscopic reconstruction of ATFL with InternalBrace™ for CLAI.
MATERIAL AND METHODS: We included 108 patients who underwent all-inside arthroscopic ATFL reconstruction with InternalBrace™ for CLAI from January 2018 to April 2020 through a retrospective study. Patients age ranged from 19 to 58 years (mean 35.6±8.7 years). Several elements are used to evaluate the clinical consequences of ankle function, including the American Orthopedic Foot and Ankle Society (AOFAS), Japanese Society for Surgery of the Foot Ankle-Hindfoot (JSSF), Kofoed, Tegner scores and complications, and the tilt angle of talus (TT) and the anterior displacement of talus (ADT) with stressing radiographs were taken to measure in follow-ups.
RESULTS: All 108 patients had all-inside arthroscopic procedures performed smoothly without serious complications. During the follow-up period (26.7±2.6 months on average), no recurrence of ankle instability and other serious complications happened. The AOFAS, JSSF, Kofoed, and Tegner scores significantly increased as time went by postoperatively, which proved statistically significant (P<0.01). Regarding stress-radiographic measurements, TT significantly decreased from (9.5±1.1)° preoperatively to (2.6±0.6)° at the latest follow-up (P<0.01), while ADT significantly decreased from (9.5±1.0) mm preoperatively to (2.6±0.6) mm at the latest examination (P<0.01).
CONCLUSIONS: All-inside arthroscopic ATFL reconstruction with the InternalBrace™ for CLAI is beneficial for ankle stability, allowing earlier return to activities.
Keywords: Arthroscopy, Joint Instability, Lateral Ligament, Ankle, Adult, Ankle, Ankle Joint, Humans, Middle Aged, young adult
Background
Ankle sport injuries account for 10–15% of all sports injuries, often leading to injury or even rupture of the anterior talofibular ligament (ATFL) [1,2]. Chronic lateral ankle instability (CLAI) symptoms occur in up to 40% of patients with ankle sprains. The main manifestations of CLAI are frequent fear of walking at night, persistent ankle swelling and pain, relaxation or stiffness, and chronic lateral ankle instability caused by decreased function [3,4]. When conservative treatment fails, articular cartilage damage due to articular kinematic changes can occur. Surgery can restore ankle stability and function [5]. For CLAI patients with a short course of disease and mild injury, ligament continuity still exists. Anatomical suture repair of ligaments is advocated; for some patients with severe injuries, open lateral ligament reconstruction is recommended, using autologous or allogeneic tendons for anatomical reconstruction of the anterior talofibular ligament and calcaneofibular ligament [6–8]. With the continuous development of minimally invasive techniques, the treatment of CLAI under total arthroscopy has been favored by most scholars. However, at present, repair of the ATFL stump with a suture anchor under total arthroscopy uses knot pulling fixation, which is prone to irritation of surrounding soft tissue or knot release. Since the ligature is not absorbable, rejection reaction, wound infection, and pain may occur after surgery. In anatomical reconstruction, most of which needs to sacrifice the autologous tendon, lateral ligament reconstruction using split peroneus brevis tendon provides satisfying functional outcomes and excellent subjective results, but it can lead to joint stiffness [9]. Major surgical trauma, long tendon-bone healing time, and long recovery time of weight-bearing walking cause serious troubles to patients and doctors. Minimally invasive concepts and sports needs are developing rapidly, and promotion of patient recovery and restoring motor function earlier with total arthroscopic surgery have received increasing attention [10]. The advantage of arthroscope InternalBrace™ (Arthrex, Naples, FL, USA) reconstruction treatment for CLAI is that it conforms to the biomechanical structural characteristics, reconstruction strength is sufficient without sacrificing the autologous tendon, and it can maintain lateral stability of the ankle joint. Therefore, the present study evaluated the feasibility and safety of InternalBrace™ reconstruction treatment of anterior talofibular ligament under total arthroscopy for CLAI patients, and analyzed its clinical effects.
Material and Methods
ETHICS STATEMENT:
Ethics approval and the details of patient informed consent were given by the Medical Ethics Committee of Dongguan Hospital of Traditional Chinese Medicine (reference number PJ [2021] No. 25).
MATERIAL:
We performed retrospective analysis of clinical data of 108 patients randomly selected in the Dongguan Hospital of Traditional Chinese Medicine for CLAI from January 2018 to April 2020.
Inclusion criteria were: age 19–58 years, repeated painful ankle sprains and failure to respond to conservative treatment for 6 months, unstable walking, and limited sensorimotor function. Preoperative X-ray examination (SIEMENS MULTIX Impact, Shanghai, China) of the anterior drawer and varus stress of the ankle was performed to measure the tilt angle of the talus and anterior talar translation (anterior talar translation >9 mm or distance forward compared with the healthy side >5 mm. In the talus tilt test, the talus tilt angle was >10° or tilt angle compared with the healthy side >3°). Patients with MRI examination (UNITED IMAGING uMR 780, Shanghai, China), indicating an anterior talofibular ligament of third-degree injury and examination under ankle arthroscopy confirming an anterior talofibular ligament of third-degree injuries will be included in the study.
Exclusion criteria were: not consistent with the diagnosis of anterior talofibular ligament injury; associated peri-ankle fractures; revision surgery; existence of ankle malformation or severe ankle disease; and patients who are not suitable for surgery due to infectious or chronic wasting diseases.
We included 108 CLAI patients, including 70 males and 38 females; aged 19–58 (35.6±8.7); 27 cases of left side injuries and 81 cases of right-side injuries, all of which were unilateral closed injuries. The course of the disease ranged from 6 to 18 months (10.1±2.6), and the follow-up period was at least 2 years (26.7±2.6), as shown in Table 1.
All patients underwent physical examinations before surgery. Stress ankle X-ray radiography was combined with MRI to evaluate CLAI diagnosis. The physical examination focused on relaxation of the ankle front drawer test and stress ankle X-ray radiograph, including ankle varus stress and front traction test, both conforming to the diagnosis of CLAI, and at the same time eliminating related fracture diseases. The relaxation degree of the ankle drawer test was decreased, and a preoperative MRI of the ankle suggested third-degree injuries of the anterior talofibular ligament, as shown in Figure 1. The X-ray examination of the tilt angle of the talus and anterior talar translation and MRI of the ankle were taken in follow-ups.
SURGICAL TECHNIQUES:
All operations were performed by the same team of foot and ankle surgeons. Preoperative computed tomography (CT) showed no ankle joint fracture and MRI showed ATFL ligament III injury (Figure 2A, 2B). All patients underwent combined spinal and epidural anesthesia or general anesthesia. After successful anesthesia, patients were placed in supine position with a triangular cushion under the ipsilateral knee joint and an air pressure tourniquet on the thigh. During the whole operation, the ankle joint remained in a neutral dorsiflexion position, which can improve the visibility and operating degree of the anterior talofibular ligament during the operation. First, 2 portals were identified for arthroscopy (Arthrex, Naples, FL, USA): the visual portal was the medial midline portal, and the operational portal was the anterolateral auxiliary portal. The medial midline portal was located at the lateral edge of the tibialis anterior tendon (Figure 3A, 3B). Compared with the anteromedial portal, the field of vision of the anterior talofibular ligament under arthroscopy was increased. The anterolateral auxiliary portal was located lateral to the third peroneal muscle, 1.0–1.5 cm in front of the peroneal tip. Attention was paid to avoiding the superficial peroneal nerve. The portal was not only close to the anterior talofibular ligament, but also conducive to avoiding the inferior extensor retinaculum. If cartilage damage or osteophyte formation was found during the operation, this portal could be fully used for cleaning, microfracture, bone grafting, and other operations after the injury of the anterior talofibular ligament was fully evaluated. Under the guidance of arthroscopy, the bone hole (anterior talofibular ligament fibula attachment) was first drilled with a 2.7-mm diameter drill at a proximal angle and level with the lateral edge of the foot. Then, with a 3.5-mm tap, placed clockwise one compound absorbable screw-in knot-free anchor (Arthrex, Naples, FL, USA) with suture (4.75×19.1 mm, with 1 blue suture). Videos are shown in Figure 3C. Next, at the anterior talofibular ligament talus attachment, a 3.4-mm hole was drilled from the upper part of the anterior talofibular ligament to the posteriorly medial part into the talus (non-articular surface, 45° to the lateral edge of foot). We passed the 2 ends of the high-strength fiber cable strap through its composite absorbable screw-in knot-free anchor (Arthrex, Naples, FL, USA) line hole (4.75mm×19.1mm) and screwed it clockwise into the talus bone tunnel. This process required light tapping with a hammer to screw it in. Note that a hemostatic forceps should be placed between the talus and the high-strength fiber cable strap when the InternalBrace™ was screwed into the talus (see videos as shown in Figure 3D). Then, we adjusted the tension of the suture, put the ankle in dorsiflex and eversion posture, and tightened the suture. We screwed the second anchor with the suture into the talus check point of the anterior talofibular ligament using an extrusion screw, and postoperative MRI showed the location of the InternalBrace™ (Figure 2C, 2D). Finally, we sutured the wound, covered it with sterile dressings, and bound it with elastic bandages.
POSTOPERATIVE TREATMENT:
Postoperative rehabilitation was conducted under the guidance of another team of professional rehabilitation physiotherapists and all patients were treated with a short leg cast to maintain a neutral ankle position. Bedside muscle contraction exercise was carried out on the second postoperative day. Two weeks after surgery, the cast was removed and the ankle brace was used for partial weight-bearing and systematic active rehabilitation exercise. Endurance and balance exercises were performed from 6 weeks after surgery until ankle function was restored.
POSTOPERATIVE ASSESSMENT:
All observation indicators were evaluated by the blind method. Postoperative follow-up data of patients were uniformly collected by the department recorder, and complications such as recurrence of lateral ankle instability, rejection reaction, and wound infection during the follow-up were recorded. Intraoperative blood loss and operation time were recorded.
Anterior talar translation and tilt angle, as well as Tegner activity level scores at 6, 12, and 24 months after surgery, were counted to evaluate the clinical results. Postoperatively, the time to return to sports activities was defined in terms of the patient’s return to the desired sports program [11]. AOFAS, Kofoed, and JSSF scoring systems score from aspects of pain level, ankle function, and force line, with a higher score indicating better ankle function recovery.
AOFAS scoring system scores from pain degree, ankle joint function and force line [12] were: excellent: 90–100; good: 75–89; fair: 50–74; poor: <50. Kofoed scoring system scores considering pain, function and activity [13] were: excellent: 85–100; good: 75–85; fair: 70–74; poor: <70. JSSF scoring system scores were based on pain (40), function (50), and alignment (10), with a total score of 100 [14]. The higher the above 3 scores, the better the ankle function recovery.
Tegner scores from the sport level on a scale of 0 to 10. A higher score means a higher level of activity [15].
Surgical duration was recorded in minutes from cutaneous incision to cutaneous suture.
Distance of anterior talar translation (mm): A forward force of about 1.5 kg was applied to the foot after plantar flexion of 10° on the affected side, and then lateral X-ray radiography was performed for the ankle joint. The distance of anterior talar translation is the shortest distance between the posterior lip of the articular surface of the distal tibia and the articular surface of the talus fornix [16]. To assess the inclination angle of the talus (°), anteroposterior X-ray radiography was performed after applying an inversion force of about 1.5 kg to the ankle joint. The inclination angle of the talus is the included angle between the articular surface of the distal tibia and the trochlear articular surface of the talus [16].
STATISTICAL ANALYSIS:
Measurement data were expressed by mean±standard deviation. The Shapiro-Wilk normality test was first performed to check for normal distributions. Sample size estimation was done in G*Power software (Germany) based on the AOFAS scores in a previous study [17]. Allocation of the 108 patients was calculated to provide 90% power (actual power 0.953) to test the hypothesis regarding the validated patient-reported outcome measure (AOFAS). The 95% confidence interval (a type-I error rate of 0.05) was used to analyze whether there was a difference in the AOFAS. Ten-point differences in the AOFAS [18] were recorded as the minimal clinically important change score (MCID), and the estimated dropout rate was 15%. We included 120 patients in the study and 108 patients completed the final follow-up. SPSS 20.0 for Mac OSX (SPSS, Inc, Chicago, IL, USA) was used for statistical processing and one-way analysis of variance or the t test was used. The chi-square test was used for count data. P<0.05 indicated statistically significant differences.
Results
All the surgeries were successfully completed within 20–50 min, with an average of (35.1±7.0) min. The operation time of the first 54 patients was slightly longer, 25–50 (38.6±6.0) min, and that of the subsequent 54 patients was 20–45 (31.6±6.2) min. The difference was statistically significant (
All patients were followed up for more than 2 years, with an average of (26.7±2.6) months. According to X-ray examination of the tilt angle of the talus and anterior talar translation and MRI examination of ankle, no recurrence of ankle instability occurred after surgery. AOFAS, Kofoed JSSF, and Tegner scores of 108 cases are significantly improved after surgery (
Image data evaluation imaging measurement results of 108 patients are shown in Table 3. The talus tilt angle was significantly decreased at the 2-year follow-up (
Discussion
With the development of minimally invasive concepts and arthroscopic techniques, surgeries under all-inside arthroscopy have been in urgent need. We believe that a less invasive procedure that can further decrease postoperative recovery time in people who love sports will be of increased interest in the future [9]. The most important finding of the present study is that both effectively restore the ankle function and satisfy the need of sports function in CLAI.
Rupture or severe injury of the lateral ligament of the ankle are the root of the mechanical instability of the lateral ankle joint in CLAI, which should be restored by surgery as much as possible. Currently, minimally invasive arthroscopy is popular [19]. As for non-anatomical reconstruction, the commonly used method is Evans, which can provide certain lateral stability of the ankle, but damages the original structure and is prone to many surgical complications [20]. In this study, reconstruction with InternalBrace™ augmentation was used, which can preserve the original structure and provide effective stability. In terms of anatomical reconstruction, the classic Broström method [21,22] performs contraction and overlapping sutures on the residual end of the injured ligament. Although the efficacy is satisfactory, the strength will decrease with time. Moreover, repair of the ATFL stump with wire anchor nails is pulling fixation with knots, which is likely to cause irritation and inflammatory response and may gradually become loose or fall off due to the creep effect. In this study, InternalBrace™ was used to reconstruct the ATFL, which can provide long-term lateral stability and sufficient strength, and can allow early out-of-bed rehabilitation. Some scholars have used autologous or allogeneic grafts for ligament reconstruction [23,24], which conforms to the biomechanics of the normal ankle and does not damage the normal tissues and ligaments around the ankle, with few complications and high efficacy [25–29]. If an autologous tendon is used for reconstruction, self-tendon tissue will be needed, and patient compliance will be reduced. InternalBrace™ reconstruction is based on absorbable knotless suture anchors. It is screwed in by rotation and fixed by the closing method without knots. The suture knot has less stimulation, which effectively reduces the relevant risks borne by the patient and the operator and is easier for the patient to accept.
My previous studies were reviewed, and the efficacy of total arthroscopic ATFL repair with anchors and InternalBrace™ reconstruction in the treatment of CLAI was compared through a prospective comparative study. In the present study, 72 patients were followed up. The greatest advantage of arthroscopy is achieving the maximum release in a limited operating space. Under arthroscopy, the anterior part is the subextensor retinaculum, the medial part is the talar neck adjacent to the talar body, the lateral part is the peroneal muscle and subcutaneous tissue, and the posterior part is the lateral anterior surface of the talar body. In most cases, the superficial peroneal nerve is prone to be injured by percutaneous enhanced repair of ATFL using Broström method under arthroscopy [30]. Although the lateral approach of arthroscopy is very close to the superficial peroneal nerve and its branches, we found only 1 case of temporary dorsal foot numbness, who self-recovered shortly after surgery. There were only 2 arthroscopic approaches in our study. Through a minimally invasive cutaneous incision and minimal subcutaneous lysis, the invasiveness of the surgical reconstruction was greatly reduced, contributing to reduced trauma, short surgical duration, less intraoperative bleeding, and low complication rate. At the last follow-up after surgery, the anterior translation, inclination angle, AOFAS, JSSF, Kofoed, and Tegner scores of the talus were significantly improved compared with those before surgery, reflecting the relative advantages of minimally invasive arthroscopy.
As is known, simply improving the activities of daily living cannot fully satisfy most patients with CLAI. Meeting the desire to engage in sports and “returning to sports” are the ultimate goal, and is the current focus of sports medicine. At present, the definition of “returning to sports” has not been unified. It is a mixed process of internal causes, external causes, and time. The common causes include patients’ love of sports before the injury, increase in age after injury, pressure from different aspects, and enthusiasm for rehabilitation exercise, which lead to adverse effects [29,31,32]. “Successfully recovering their desired sports (although they may not achieve the desired sports performance)” was proposed at the “First Global Sports Physiotherapy Conference” in 2016 [11]. This definition of “returning to sports” is more practical. Considering the interaction between patients’ expectations and time lapse, individualized assessment of motor function is necessary [33].
Arthroscopically assisted augmentation for ATFL repair with an InternalBrace™ is a simple, minimally invasive, and rapid procedure that provides additional initial stability and protection to anatomic ATFL repair. Adding InternalBrace™ as an augmentation to a modified Broström-Gould procedure makes early active weight-bearing exercise possible. In addition, an early range of motion was found effective for rehabilitation after ligament reconstruction [34], which is similar to our study. During the follow-up of this study, 98 cases returned to sports, accounting for 91.59%, of which the time of returning to sports was 5.5±0.9 months, meeting the sports demand of most CLAI patients.
During arthroscopic preparation, the individual anatomy and pathology of the patients can be addressed more precisely, and therefore repair and augmentation can be performed at the exact fibular and talar footprint. The arthroscopic InternalBraceTM reconstruction we used can effectively add a margin of safety to the lateral stability of the ankle. The repair was designed without knots, which can reduce soft-tissue irritation, decrease the loosening of knots, effectively prevent secondary injury of ligaments, and allow patients to recover early and more actively. Additionally, it has been reported by some scholars that excessive tension of the InternalBrace™ may lead to stiffness and decrease the mobility of the ankle [35]. When the anchor is placed at the talar insertion point, controlling the tension becomes essential and directly affects recovery of ankle function after surgery. Our method is to use hemostatic forceps when the ankle is in back extension. The hemostatic forceps should be placed between the talus and the high-strength fiber cable strap when the InternalBrace™ is screwed into the talus. Talar anchor pull-out often occurs during arthroscopic enhanced repair, resulting in failure of surgery [36]. The above techniques can reduce this risk. InternalBrace™ reconstruction can preserve the original local anatomical structure of the ankle to the maximum extent, without sacrificing the autologous tendon, and significantly reducing iatrogenic trauma. The InternalBrace™ mimics the biomechanical characteristics of the lateral ankle and has bionic elasticity. The anchor head ring is used as a pulley to allow the high-strength fiber cable strap to slide on the ring and ensure proper tension in the bone tunnel, so that the suture anchor can firmly fix the ligament or high-strength fiber cable strap on the bony structure and promote tendon-bone healing, providing better ankle stability. Total arthroscopic InternalBrace™ reconstruction of the anterior talofibular ligament for CLAI can effectively maintain the anatomical structure of the ankle, recover ankle function, and facilitate earlier return to sports.
However, this study has some limitations. First and foremost, we did not perform a matched-pair study. Secondly, learning curves are required for surgeries under all-inside arthroscopy. Skilled surgical techniques are also required to maximize the strengths of arthroscopy while minimizing the risks. Because the superficial peroneal nerve is close to the anterolateral assisted approach of ankle arthroscopy, nerve stimulation or damage occurs easily during the operation. If continuous ultrasound or MRI examinations can be performed during the repair of ATFL, it is more conducive to analysis.
Conclusions
All-inside ATFL reconstruction with an InternalBrace™ under arthroscopy has significant superiority in ankle stability after surgery which allows early rehabilitation, and can restore the ankle function and satisfy the need for sports function in CLAI.
Figures
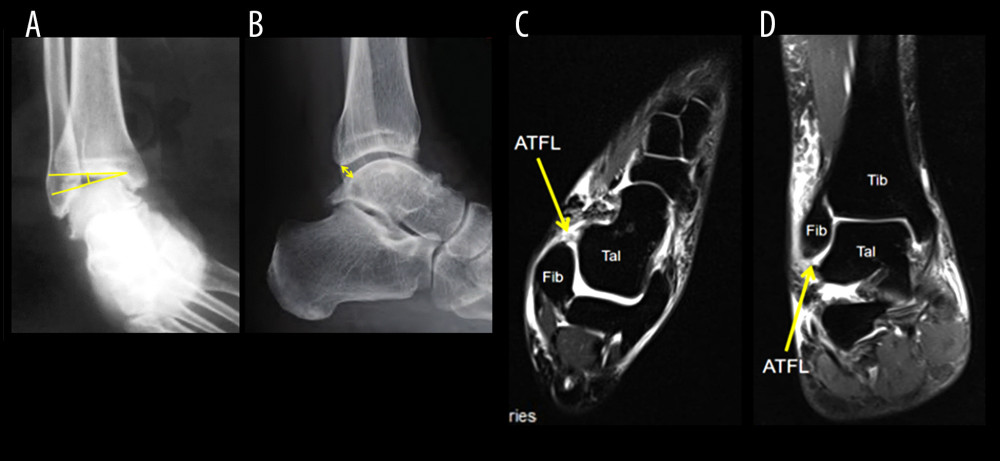 Figure 1. Preoperative examination of ankle stress radiographs and MRI showed anterior talofibular ligament III injury. (A) The tibiotalar tilt angle on varus stress radiographs; (B) Anterior translation of the talus on anterior drawer stress radiographs; (C) MRI cross-sectional manifestation; (D) MRI coronal manifestation. Fib – fibulare; Tal – talus; Tib – tibia; ATFL – anterior talofibular ligament.
Figure 1. Preoperative examination of ankle stress radiographs and MRI showed anterior talofibular ligament III injury. (A) The tibiotalar tilt angle on varus stress radiographs; (B) Anterior translation of the talus on anterior drawer stress radiographs; (C) MRI cross-sectional manifestation; (D) MRI coronal manifestation. Fib – fibulare; Tal – talus; Tib – tibia; ATFL – anterior talofibular ligament. 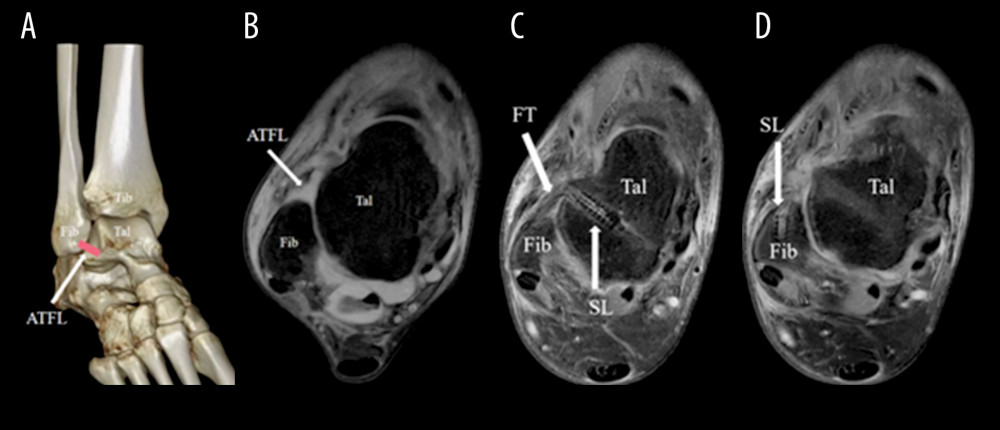 Figure 2. Preoperative and postoperative images of a 25-year-old male patient with right CLAI treated with InternalBrace™. (A) Preoperative computed tomography showed no fracture of ankle joint. (B) Preoperative MRI showed ATFL ligament III injury. (C, D) Postoperative MRI cross-sectional manifestation showed the location of InternalBrace™. Tib – tibia; Fib – fibulare; Tal – talus; ATFL – anterior talofibular ligament. TA – tibialis anterior; FT – FiberTape; SL – SwiveLock.
Figure 2. Preoperative and postoperative images of a 25-year-old male patient with right CLAI treated with InternalBrace™. (A) Preoperative computed tomography showed no fracture of ankle joint. (B) Preoperative MRI showed ATFL ligament III injury. (C, D) Postoperative MRI cross-sectional manifestation showed the location of InternalBrace™. Tib – tibia; Fib – fibulare; Tal – talus; ATFL – anterior talofibular ligament. TA – tibialis anterior; FT – FiberTape; SL – SwiveLock. 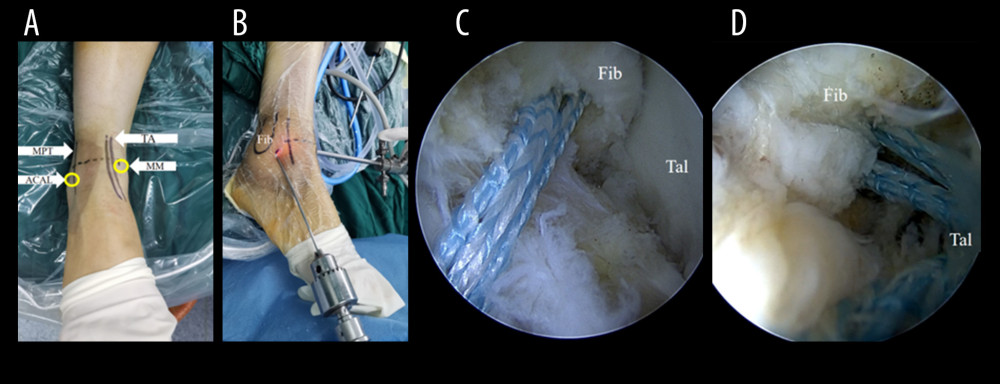 Figure 3. Intraoperative Images of a 25-year-old male patient with right CLAI treated with InternalBraceTM. (A, B) Location of arthroscopic approach. (C) Drill and place an SwiveLock with FiberTape at the fibular footprint ATFL. (D) Complete ATFL ligament reconstruction with InternalBraceTM and check the lateral stability of ankle joint with arthroscopy. TA – tibialis anterior; MPT – musculus peronaeus tertius; MM – medial midline approach; ACAL – accessory anterolateral approach.
Figure 3. Intraoperative Images of a 25-year-old male patient with right CLAI treated with InternalBraceTM. (A, B) Location of arthroscopic approach. (C) Drill and place an SwiveLock with FiberTape at the fibular footprint ATFL. (D) Complete ATFL ligament reconstruction with InternalBraceTM and check the lateral stability of ankle joint with arthroscopy. TA – tibialis anterior; MPT – musculus peronaeus tertius; MM – medial midline approach; ACAL – accessory anterolateral approach. Tables
Table 1. Basic descriptive characteristics of the study group.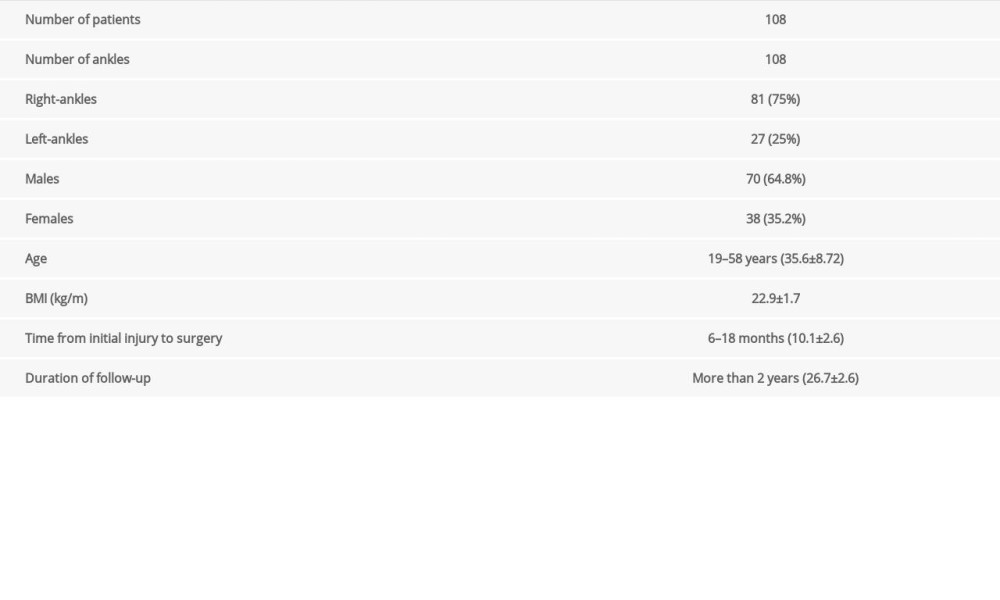 Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s).
Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s).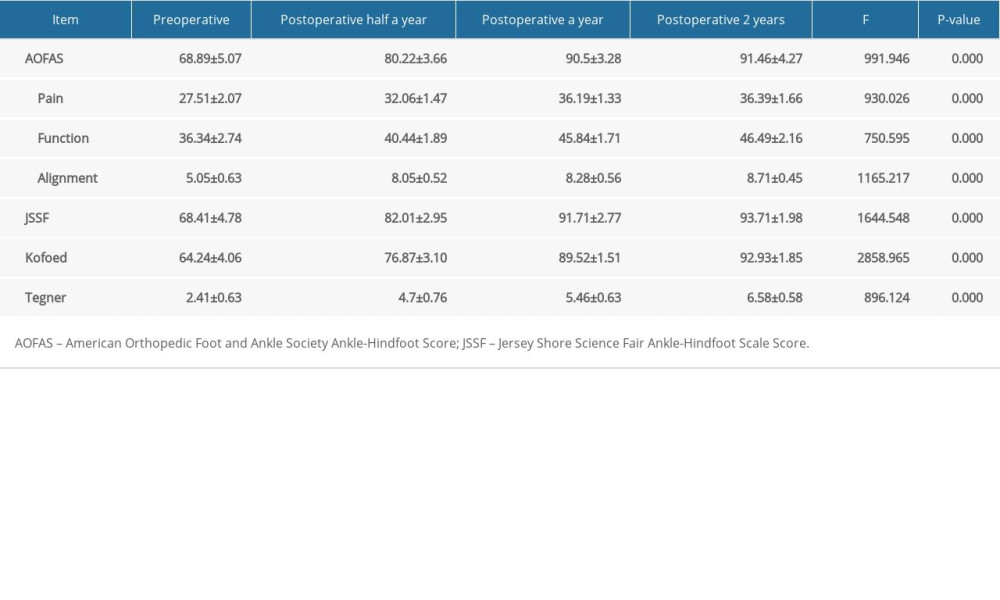 Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s).
Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s).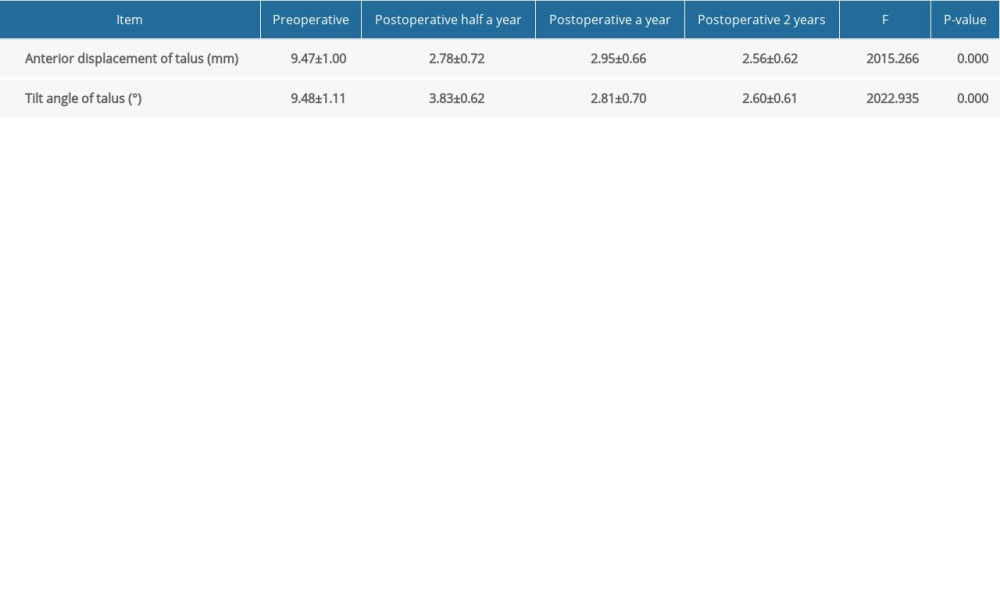
References
1. Hua Y, Chen S, Li Y, Combination of modified Broström procedure with ankle arthroscopy for chronic ankle instability accompanied by intra-articular symptoms: Arthroscopy, 2010; 26(4); 524-28
2. Bonnel F, Toullec E, Mabit C, Chronic ankle instability: Biomechanics and pathomechanics of ligaments injury and associated lesions: Orthop Traumatol Surg Res, 2010; 96(4); 424-32
3. Rezaninová J, Hrazdira L, Moc Králová D, Advanced conservative treatment of complete acute rupture of the lateral ankle ligaments: Verifying by stabilometry: Foot Ankle Surg, 2018; 24; 65-70
4. Choi HJ, Kim DW, Modified Broström procedure using distal fibular periosteal flap augmentation vs anatomic reconstruction using a free tendon allograft in patients who are not candidates for standard repair: Foot Ankle Int, 2017; 38(11); 1207-14
5. Cho BK, Kim YM, Shon HC, A ligament reattachment technique for high-demand athletes with chronic ankle instability: J Foot Ankle Surg, 2015; 54(1); 7-12
6. Yasui Y, Murawski CD, Wollstein A, Operative treatment of lateral ankle instability: JBJS Rev, 2016; 4(5); e6
7. Tourné Y, Mabit C, Lateral ligament reconstruction procedures for the ankle: Orthop Traumatol Surg Res, 2017; 103(1S); S171-81
8. Hu CY, Lee KB, Song EK, Comparison of bone tunnel and suture anchor techniques in the modified Broström procedure for chronic lateral ankle instability: Am J Sports Med, 2013; 41(8); 1877-84
9. Ventura A, Legnani C, Corradini C, Borgo E, Lateral ligament reconstruction and augmented direct anatomical repair restore ligament laxity in patients suffering from chronic ankle instability up to 15 years from surgery: Knee Surg Sports Traumatol Arthrosc, 2020; 28(1); 202-7
10. Mercer NP, Azam MT, Davalos N, Anterior talofibular ligament augmentation with internal brace in the office setting: Arthrosc Tech, 2022; 11(4); e545-e50
11. Ardern CL, Glasgow P, Schneiders A, 2016 Consensus statement on return to sport from the First World Congress in Sports Physical Therapy, Bern: Br J Sports Med, 2016; 50(14); 853-64
12. Kitaoka HB, Alexander IJ, Adelaar RS, Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes: Foot Ankle Int, 1994; 15(7); 349-53
13. Murnaghan JM, Warnock DS, Henderson SA, Total ankle replacement. Early experiences with STAR prosthesis: Ulster Med J, 2005; 74(1); 9-13
14. Niki H, Aoki H, Inokuchi S, Development and reliability of a standard rating system for outcome measurement of foot and ankle disorders I: Development of standard rating system: J Orthop Sci, 2005; 10(5); 457-65
15. Tegner Y, Lysholm J, Rating systems in the evaluation of knee ligament injuries: Clin Orthop Relat Res, 1985(198); 43-49
16. Tarczyńska M, Sekuła P, Gawęda K, Stress radiography in the diagnosis and assessment of the outcomes of surgical treatment of chronic anterolateral ankle instability: Acta Radiol, 2020; 61(6); 783-88
17. Ulku TK, Kocaoglu B, Tok O, Arthroscopic suture-tape internal bracing is safe as arthroscopic modified Broström repair in the treatment of chronic ankle instability: Knee Surg Sports Traumatol Arthrosc, 2020; 28(1); 227-32
18. Hou ZC, Su T, Ao YF, Arthroscopic modified Broström procedure achieves faster return to sports than open procedure for chronic ankle instability: Knee Surg Sports Traumatol Arthrosc, 2022; 30(10); 3570-78
19. Knupp M, Lang TH, Zwicky L, Chronic ankle instability (medial and lateral): Clin Sports Med, 2015; 34(4); 679-88
20. Evans DL, Recurrent instability of the ankle; A method of surgical treatment: Proc R Soc Med, 1953; 46(5); 343-44
21. Yang ZY, Hu Y, Diagnosis and repair of chronic ankle instability: Chinese Journal of Tissue Engineering Research, 2014; 18; 9
22. Pintore E, Cipollaro L, Pintore R, Extensor retinaculum flap and fibular periosteum ligamentoplasty after failed surgery for chronic lateral ankle instability: Foot Ankle Int, 2020; 41(12); 1546-52
23. Krips R, van Dijk CN, Halasi PT, Long-term outcome of anatomical reconstruction versus tenodesis for the treatment of chronic anterolateral instability of the ankle joint: a multicenter study: Foot Ankle Int, 2001; 22(5); 415-21
24. Guelfi M, Vega J, Malagelada F, Dalmau-Pastor M, The arthroscopic all-inside ankle lateral collateral ligament repair is a safe and reproducible technique: Knee Surg Sports Traumatol Arthrosc, 2020; 28(1); 63-69
25. Noailles T, Lopes R, Padiolleau G, Non-anatomical or direct anatomical repair of chronic lateral instability of the ankle: A systematic review of the literature after at least 10 years of follow-up: Foot Ankle Surg, 2018; 24(2); 80-85
26. Song B, Li C, Chen N, All-arthroscopic anatomical reconstruction of anterior talofibular ligament using semitendinosus autografts: Int Orthop, 2017; 41; 975-82
27. Maffulli N, Del Buono A, Maffulli GD, Isolated anterior talofibular ligament Broström repair for chronic lateral ankle instability: 9-year follow-up: Am J Sports Med, 2013; 41(4); 858-64
28. Feller J, Webster KE, Return to sport following anterior cruciate ligament reconstruction: Int Orthop, 2013; 37(2); 285-90
29. Tassignon B, Verschueren J, Delahunt E, Criteria-based return to sport decision-making following lateral ankle sprain injury: A systematic review and narrative synthesis: Sports Med, 2019; 49(4); 601-19
30. Matsui K, Burgesson B, Takao MESSKA AFAS Ankle Instability Group, Minimally invasive surgical treatment for chronic ankle instability: A systematic review: Knee Surg Sports Traumatol Arthrosc, 2016; 24(4); 1040-48
31. Maffulli N, Del Buono A, Maffulli GD, Isolated anterior talofibular ligament Broström repair for chronic lateral ankle instability: 9-year follow-up: Am J Sports Med, 2013; 41(4); 858-64
32. Feller J, Webster KE, Return to sport following anterior cruciate ligament reconstruction: Int Orthop, 2013; 37(2); 285-90
33. Xue XA, Tao WC, Chen ZYInfluencing factors of return to sport after all-inside arthroscopic lateral collateral ligament repair for chronic ankle instability: Zhonghua Yi Xue Za Zhi, 2021; 101(37); 2975-81 [in Chinese]
34. Schuh R, Benca E, Willegger M, Comparison of Broström technique, suture anchor repair, and tape augmentation for reconstruction of the anterior talofibular ligament: Knee Surg Sports Traumatol Arthrosc, 2016; 24(4); 1101-7
35. Willegger M, Schuh R, Arthroscopically assisted tape augmentation for anterior talofibular ligament repair: Arthrosc Tech, 2020; 9(6); e809-e16
36. Willegger M, Benca E, Hirtler L, Biomechanical stability of tape augmentation for anterior talofibular ligament (ATFL) repair compared to the native ATFL: Knee Surg Sports Traumatol Arthrosc, 2016; 24(4); 1015-21
Figures
 Figure 1. Preoperative examination of ankle stress radiographs and MRI showed anterior talofibular ligament III injury. (A) The tibiotalar tilt angle on varus stress radiographs; (B) Anterior translation of the talus on anterior drawer stress radiographs; (C) MRI cross-sectional manifestation; (D) MRI coronal manifestation. Fib – fibulare; Tal – talus; Tib – tibia; ATFL – anterior talofibular ligament.
Figure 1. Preoperative examination of ankle stress radiographs and MRI showed anterior talofibular ligament III injury. (A) The tibiotalar tilt angle on varus stress radiographs; (B) Anterior translation of the talus on anterior drawer stress radiographs; (C) MRI cross-sectional manifestation; (D) MRI coronal manifestation. Fib – fibulare; Tal – talus; Tib – tibia; ATFL – anterior talofibular ligament. Figure 2. Preoperative and postoperative images of a 25-year-old male patient with right CLAI treated with InternalBrace™. (A) Preoperative computed tomography showed no fracture of ankle joint. (B) Preoperative MRI showed ATFL ligament III injury. (C, D) Postoperative MRI cross-sectional manifestation showed the location of InternalBrace™. Tib – tibia; Fib – fibulare; Tal – talus; ATFL – anterior talofibular ligament. TA – tibialis anterior; FT – FiberTape; SL – SwiveLock.
Figure 2. Preoperative and postoperative images of a 25-year-old male patient with right CLAI treated with InternalBrace™. (A) Preoperative computed tomography showed no fracture of ankle joint. (B) Preoperative MRI showed ATFL ligament III injury. (C, D) Postoperative MRI cross-sectional manifestation showed the location of InternalBrace™. Tib – tibia; Fib – fibulare; Tal – talus; ATFL – anterior talofibular ligament. TA – tibialis anterior; FT – FiberTape; SL – SwiveLock. Figure 3. Intraoperative Images of a 25-year-old male patient with right CLAI treated with InternalBraceTM. (A, B) Location of arthroscopic approach. (C) Drill and place an SwiveLock with FiberTape at the fibular footprint ATFL. (D) Complete ATFL ligament reconstruction with InternalBraceTM and check the lateral stability of ankle joint with arthroscopy. TA – tibialis anterior; MPT – musculus peronaeus tertius; MM – medial midline approach; ACAL – accessory anterolateral approach.
Figure 3. Intraoperative Images of a 25-year-old male patient with right CLAI treated with InternalBraceTM. (A, B) Location of arthroscopic approach. (C) Drill and place an SwiveLock with FiberTape at the fibular footprint ATFL. (D) Complete ATFL ligament reconstruction with InternalBraceTM and check the lateral stability of ankle joint with arthroscopy. TA – tibialis anterior; MPT – musculus peronaeus tertius; MM – medial midline approach; ACAL – accessory anterolateral approach. Tables
 Table 1. Basic descriptive characteristics of the study group.
Table 1. Basic descriptive characteristics of the study group. Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s).
Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s). Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s).
Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s). Table 1. Basic descriptive characteristics of the study group.
Table 1. Basic descriptive characteristics of the study group. Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s).
Table 2. Results and comparison of AOFAS, Kofoed, JSSF, Tegner scores at different times among patients (χ̄±s). Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s).
Table 3. Results and comparison of the tilt angle of talus and the anterior displacement of talus at different times among patients (χ̄±s). In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








