26 September 2022: Clinical Research
Factors Associated with Placenta Previa: A Retrospective, Single-Center Study in Turkey
Fatih Mehmet Findik1ABCDEF*DOI: 10.12659/MSM.938023
Med Sci Monit 2022; 28:e938023
Abstract
BACKGROUND: The incidence of placenta previa is gradually increasing. The major risk factor is a history of cesarean section (CS). Such patients may experience severe bleeding during pregnancy and surgery. Patients with placenta previa were classified based on risk factors in this study. This retrospective study from a single center in Turkey aimed to evaluate the factors associated with placenta previa in 151 women.
MATERIAL AND METHODS: Patients with placenta previa were grouped by the presence/absence of prior CS. Group 1 (123 patients) had undergone at least 1 CS, and Group 2 (28 patients) had not undergone CS. The diagnosis of placenta previa was made by ultrasound. Placenta previa was defined as cases where the placenta crossed the internal os. Duration of surgery, bleeding during surgery, and the amounts of erythrocyte suspensions required were compared between groups.
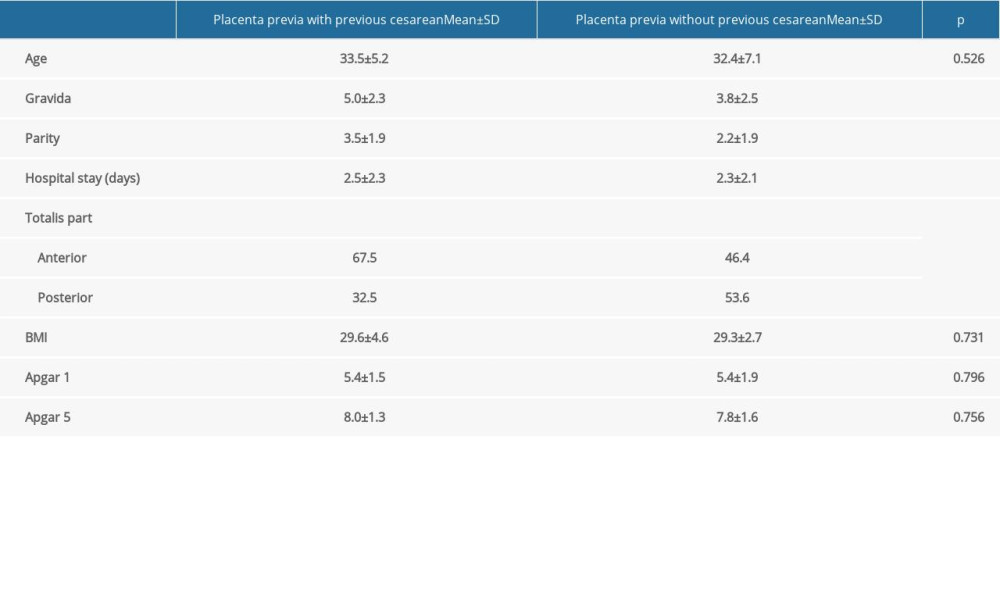
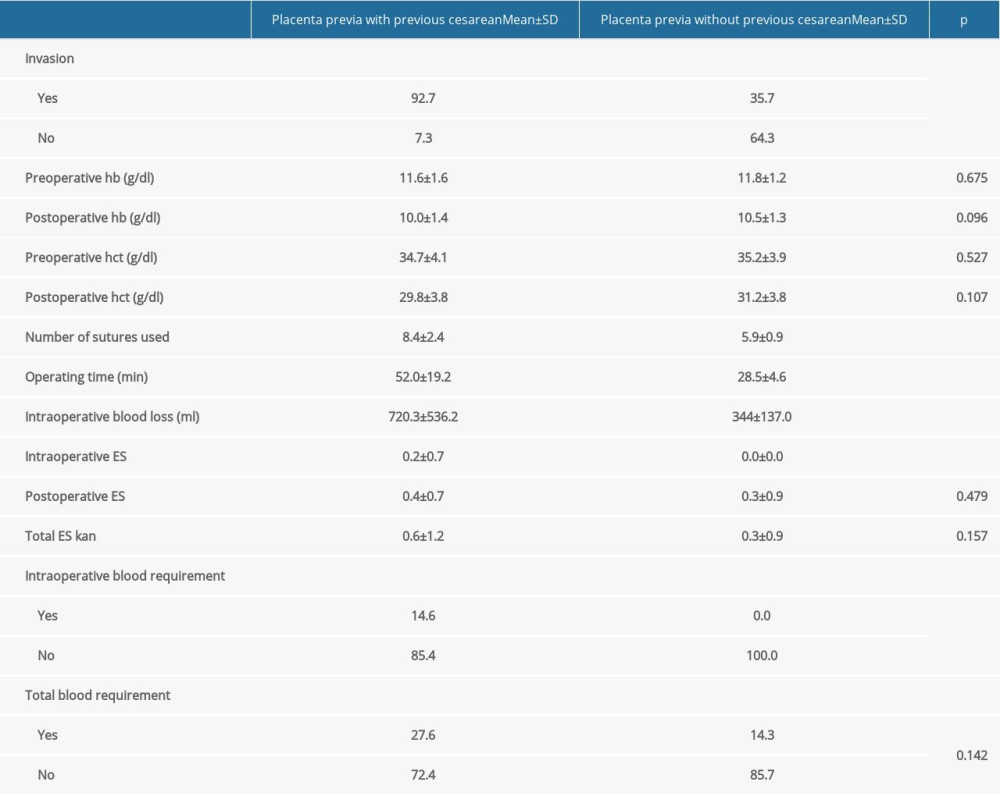
RESULTS: Of Group 1 patients, 67.5% had anterior placenta previa compared to 46.4% in Group 2. The mean duration of surgery was: 52.0±19.2 and 28.5±4.6 min (P<0.001); the number of sutures was 8.4±2.4 and 5.9±0.9 (P<0.001); the bleeding volumes were 720.3±536.2 and 344±137.0 mL (P<0.001); and the amount of erythrocyte suspension administered intraoperatively was 0.2±0.7 and 0.0±0.0 unit (P=0.032).
CONCLUSIONS: Mean duration of surgery, number of sutures, bleeding volume, and intraoperatively applied ES volumes were significantly different between groups. Identification of placenta previa patients who have undergone prior CS is vitally important in terms of preoperative preparation.
Keywords: Cesarean Section, Repeat, Maternal Mortality, Placenta Previa, Cesarean Section, Female, Humans, Placenta, Pregnancy, Risk Factors, Turkey
Background
Placenta previa is diagnosed when the placenta completely covers the internal cervical os. The prevalence rises as cesarean delivery numbers increase, to attain about 0.5% [1–3]. Previous placenta previa and prior cesarean section (CS) are the 2 most significant risk factors [4–7]. However, maternal age, multiparity, smoking, chronic hypertension, multiple gestations, and previous uterine procedures (curettage and myomectomy) are also risk factors [3–9]. Severe bleeding during labor is possible, especially during the third trimester. The other risks include a need for cesarean hysterectomy, preterm delivery, and maternal death [7,10,11]. Patients with a previous cesarean section are more likely to have placental invasion. These patients have a higher risk of antepartum hemorrhage, postpartum hemorrhage, and hysterectomy [6,10]. Transvaginal or transabdominal ultrasonography aid diagnosis [12]. Diagnostic ultrasonography reveals complete closure of the cervical os by the placenta. The present study shows that placenta previa etiologies differ greatly between women who have undergone prior CS and those who have not. This retrospective study from a single center in Turkey aimed to evaluate the factors associated with placenta previa in 151 women.
Material and Methods
INCLUSION AND EXCLUSION CRITERIA:
Patients whose placenta completely covered the cervical os (as revealed by preoperative ultrasonography) were included; those with low-lying placenta and who underwent surgery prior to week 20 were excluded. In addition, patients with multiple pregnancies and comorbidities such as diabetes mellitus, hypertension, and bleeding disorders were excluded from the study.
STATISTICAL ANALYSIS:
Statistical analysis employed SPSS ver. 21.0 for Mac (SPSS, Inc., Chicago, IL, USA). Data are presented as means±standard deviations or as medians with interquartile ranges. The Mann-Whitney U-test or the Fisher exact test was used to compare the groups. A
Results
A total of 151 placenta previa patients underwent operations; 123 patients in Group 1 (with at least 1 prior CS) and 28 in Group 2 (no CS). The mean ages of patients in Groups 1 and 2 were 33.5±5.2 and 32.4±7.1 years, respectively, and were not significantly different. Gravidity was 5.0±2.3 in Group 1 and 3.8±2.5 in Group 2, and thus was significantly different (
Discussion
In our study, the difference between the groups in terms of operation time, numbers of sutures, amount of bleeding, and intraoperatively administered ES volumes was significant. In addition, the hospital stay of Group 1 was significantly longer.
Placenta previa rates have risen dramatically in recent years. In our region, the incidence is 8.1% [14–16]. A previous CS is a major cause of this increase [17]. A placenta previa is more than a diagnosis. A placenta previa can cause hemorrhage during pregnancy and delivery, and maternal mortality. The infant may need to be delivered early, especially in patients with invasive abnormalities. The risk of hysterectomy in such patients is also rather high [2,7,10]. Although placenta previa is diagnosed by ultrasound, placental invasion is not always detectable in patients receiving standard obstetric care [18]. The literature reveals that placental invasion is likely to be associated with prior CS, but no distinction was made based on the patient’s previous method of delivery [19]. Another study reported that the risk of invasion is increased, especially in women who have had a previous cesarean section [6]. In our study, we found a very significant difference in placental invasion between the 2 groups (92.7 and 35.7%,
In another study on antepartum bleeding, the amount of bleeding was higher in the group with high invasion [10]. In this study, no distinction was made according to previous delivery type. The number of cesarean sections was higher in patients in the postpartum bleeding group. In addition, this group had more placental invasion and had more hospitalization days. Placenta previa is known to increase the requirement for blood transfusions and maternal mortality by inducing severe postpartum hemorrhage [20]. In this study, it was found that the amount of bleeding increased significantly when grouped according to the presence of cesarean section. Planned surgical delivery in patients with abnormal (invasive) placenta reduces complications and the need for blood transfusions. In the study, the diagnosis of abnormal invasion was categorized according to whether it was prenatal or intrapartum, but no distinction was made between the groups according to the presence of cesarean section [21]. Prenatal diagnosis of placental invasion minimized bleeding in a UK study. Some patients had never undergone CSs, but this was not considered when measuring bleeding [22]. It is essential to have ESs on standby during CS, as severe bleeding is possible [7,18,22,23]. Massive transfusion was maximally correlated with abnormal placentation in a study of over 690 000 deliveries [24]. Wefound that placental invasion was significantly higher in Group 1, as was the bleeding volume (720.3±536.2 vs 344±137.0 mL;
A 2018 study on placenta previa risk factors reported that a prior CS imparted the highest risk; this increased with the number of previous CSs [25]. When encountering placenta previa cases, it is essential to determine whether the placenta lies anterior or posterior. The risk of hysterectomy was considerably higher in the anterior cases [26]. We found that most placenta were anterior in Group 1 patients, and most were posterior in Group 2 patients (67.5% vs 46.4%,
Our study has some limitations. One of these is the relatively low incidence of placenta previa patients (although its incidence has been increasing recently). As the incidence increases, some of our information on this subject will be updated and some of our information will be renewed. In addition, multicenter studies may support our study and contribute to the literature.
Conclusions
In conclusion, placenta previa patients (who are becoming more common) require careful obstetric care. These patients have a high risk of bleeding and may need hysterectomy during surgery. The need for blood transfusions is also high. We observed that there were significant differences between the groups in terms of duration of surgery, amount of bleeding, amount of ES used, and length of hospital stay. It is essential to ask patients if they have undergone prior CS. In this way, the preoperative preparation process will be carried out according to the needs of the patient. In addition, more specific information about the disease can be given to the patient.
References
1. Ozdemirci S, Akpinar F, Baser E, Effect of the delivery way and number of parity in the subsequent incidence of placenta previa: J Matern Fetal Neonatal Med, 2020; 33(19); 3238-43
2. Cresswell JA, Ronsmans C, Calvert C, Prevalence of placenta praevia by world region: A systematic review and meta-analysis: Trop Med Int Health, 2013; 18(6); 712-24
3. Kollmann M, Gaulhofer J, Lang U, Placenta praevia: Incidence, risk factors and outcome: J Matern Fetal Neonatal Med, 2016; 29(9); 1395-98
4. Lavery JP, Placenta previa: Clin Obstet Gynecol, 1990; 33(3); 414-21
5. Klar M, Michels KB, Cesarean section and placental disorders in subsequent pregnancies – a meta-analysis: J Perinat Med, 2014; 42(5); 571-83
6. Jain V, Bos H, Bujold E, Guideline No. 402: Diagnosis and management of placenta previa: J Obstet Gynaecol Can, 2020; 42(7); 906-17
7. Jauniaux E, Alfirevic Z, Bhide AGRoyal College of Obstetricians and Gynaecologists, Placenta praevia and placenta accreta: Diagnosis and management: Green-top Guideline No. 27a: BJOG, 2019; 126(1); e1-e48
8. Jenabi E, Salimi Z, Bashirian S, The risk factors associated with placenta previa: An umbrella review: Placenta, 2022; 117; 21-27
9. Ananth CV, Savitz DA, Luther ER, Maternal cigarette smoking as a risk factor for placental abruption, placenta previa, and uterine bleeding in pregnancy: Am J Epidemiol, 1996; 144(9); 881-89
10. Long SY, Yang Q, Chi R, Maternal and neonatal outcomes resulting from antepartum hemorrhage in women with placenta previa and its associated risk factors: A single-center retrospective study: Ther Clin Risk Manag, 2021; 12(17); 31-38
11. Solheim KN, Esakoff TF, Little SE, The effect of cesarean delivery rates on the future incidence of placenta previa, placenta accreta, and maternal mortality: J Matern Fetal Neonatal Med, 2011; 24(11); 1341-46
12. Farine D, Fox HE, Jakobson S, Vaginal ultrasound for diagnosis of placenta previa: Am J Obstet Gynecol, 1988; 159(3); 566-69
13. Jauniaux E, Ayres-de-Campos D, Langhoff-Roos JFIGO Placenta Accreta Diagnosis and Management Expert Consensus Panel, FIGO classification for the clinical diagnosis of placenta accreta spectrum disorders: Int J Gynaecol Obstet, 2019; 146(1); 20-24
14. Findik FM, Içen MS, Tunç SY, Evaluation of patients with previous C/S+placenta previa: Totals İn 2017: Dicle Tip Dergisi, 2020; 47(3); 630-37
15. Bowman ZS, Eller AG, Bardsley TR, Risk factors for placenta accreta: A large prospective cohort: Am J Perinatol, 2014; 31(9); 799-804
16. Sallam HF, Shady NW, A sandwich technique (N&H variation technique) to reduce blood loss during cesarean delivery for complete placenta previa: A randomized controlled trial: J Matern Fetal Neonatal Med, 2019; 32(19); 3145-52
17. Wang YL, Su FM, Zhang HY, Aortic balloon occlusion for controlling intraoperative hemorrhage in patients with placenta previa increta/percreta: J Matern Fetal Neonatal Med, 2017; 30(21); 2564-68
18. Bailit JL, Grobman WA, Rice MM, Morbidly adherent placenta treatments and outcomes: Obstet Gynecol, 2015; 125(3); 683-89
19. Hobson SR, Kingdom JC, Murji A, No. 383-screening, diagnosis, and management of placenta accreta spectrum disorders: J Obstet Gynaecol Can, 2019; 41(7); 1035-49
20. Ma Y, Liu R, Zhang J, An analysis of maternal-fetal prognosis in patients with placenta accreta: J Matern Fetal Neonatal Med, 2021; 34(5); 725-31
21. Tikkanen M, Paavonen J, Loukovaara M, Antenatal diagnosis of placenta accreta leads to reduced blood loss: Acta Obstet Gynecol Scand, 2011; 90(10); 1140-46
22. Fitzpatrick KE, Sellers S, Spark P, The management and outcomes of placenta accreta, increta, and percreta in the UK: A population-based descriptive study: BJOG, 2014; 121(1); 62-71
23. Chen M, Liu X, You Y, Internal iliac artery balloon occlusion for placenta previa and suspected placenta accreta: A randomized controlled trial: Obstet Gynecol, 2020; 135(5); 1112-19
24. Mhyre JM, Shilkrut A, Kuklina EV, Massive blood transfusion during hospitalization for delivery in New York State, 1998–2007: Obstet Gynecol, 2013; 122(6); 1288-94
25. Iacovelli A, Liberati M, Khalil A, Risk factors for abnormally invasive placenta: A systematic review and meta-analysis: J Matern Fetal Neonatal Med, 2020; 33(3); 471-81
26. Park HS, Cho HS, Management of massive hemorrhage in pregnant women with placenta previa: Anesth Pain Med, 2020; 15(4); 409-16
27. Baba Y, Matsubara S, Ohkuchi A, Anterior placentation as a risk factor for massive hemorrhage during cesarean section in patients with placenta previa: J Obstet Gynaecol Res, 2014; 40(5); 1243-48
28. Jang DG, We JS, Shin JU, Maternal outcomes according to placental position in placental previa: Int J Med Sci, 2011; 8(5); 439-44
In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387