26 January 2023: Clinical Research
Comparison of Postoperative Outcomes of Hand-Sewn Versus Stapled Esophago-jejunal Anastomosis During Total Gastrectomy for Gastric Cancer in 72 Patients: A Retrospective, Single-Center Study in Poland
Karolina MajewskaDOI: 10.12659/MSM.938759
Med Sci Monit 2023; 29:e938759
Abstract
BACKGROUND: Mechanical stapling is a commonly used alternative to hand-sewn technique for esophago-jejunal anastomosis in total gastrectomy (TG). Some studies report reduction in postoperative complications in the stapler group. This retrospective study aimed to compare short- and long-term surgical outcomes between the groups with stapled and hand-sewn esophago-jejunal anastomosis (EJA) during open TG for gastric cancer.
MATERIAL AND METHODS: The study included 72 adult patients with gastric cancer who underwent TG in the Department of Digestive Tract Surgery in Katowice between May 2018 and December 2021. The patients were divided into 2 groups according to the technique of EJA: stapled (44 cases) or hand-sewn (28 cases). We compared the groups in terms of the duration of the surgery, length of hospital stay, and occurrence of complications (focusing on anastomotic leakage, stricture and abdominal abscess).
RESULTS: There were no significant differences in duration of the surgery (P=0.6), blood loss (P=0.7), or length of postoperative hospital stay (P=0.2) among the groups. Early postoperative complications rates were 9.1% (4/44) in the stapler group and 17.9% (5/28) in the hand-sewn group (P=0.27). The most frequent complication was anastomotic leakage, with 2 cases in each group (P=0.76). The mean follow-up time was 1.8±0.9 (0.3-3.6) years. During this period the anastomotic stricture occurred in 7 (15.9%) cases with stapled anastomosis and in 5 (17.9%) cases with hand-sewn anastomosis (P=0.52).
CONCLUSIONS: In this study there were no significant differences in mortality, morbidity, and surgery duration between stapled and hand-sewn esophago-jejunal anastomosis in total gastrectomy.
Keywords: Anastomosis, Surgical, Gastrectomy, Morbidity, Mortality, Stomach Neoplasms, Adult, Humans, Anastomotic Leak, Constriction, Pathologic, Poland, Postoperative Complications
Background
The open total gastrectomy (TG) is one of the methods of curative treatment for advanced gastric cancer [1]. It is a standard procedure applied in node-positive or T2–T4a tumors, when it is essential to achieve sufficient resection margins, in case of pancreatic invasion requiring pancreaticosplenectomy, as well as in some cases of tumors located at the greater curvature of the stomach, if there is a risk of metastasis to the lymph nodes accompanying the left gastroepiploic artery [1]. Some studies reported acceptable results also for minimally invasive gastrectomy, but it is still not recommended in more advanced tumors [1–4]; therefore, open TG remains an important part of gastric cancer surgery.
Several techniques are applied for gastrointestinal tract reconstruction after TG, including jejunal interposition, double tract method, and Roux-en-Y esophago-jejunal anastomosis (EJA) [1]. Some of the most important complications after TG are those associated with EJA, including anastomotic leakage, dehiscence, bleeding, and stenosis [5]. EJA may be performed using traditional hand-sewn technique or mechanical stapling, using linear or circular devices [1]. Although stapled anastomosis is a well-described and commonly used method, there is little recent data regarding the surgical complications of open total gastrectomy with comparison of stapled and hand-sewn esophago-jejunal anastomosis [6]. Some previous studies found a reduction in duration of the surgery, along with lower incidence of anastomotic leakage and higher rate of strictures in the stapler group, while others reported no difference between these 2 techniques [7–10]. A recent meta-analysis showed that hand-sewn and stapled anastomosis have similar surgical outcomes, while staplers reduce the operative time [6], but the recent data about open TG are limited. Only 12 studies were included in the meta-analysis, with 1 recent study on open TG comprising 63 patients [11].
Therefore, this retrospective study from a single center in Poland aimed to compare postoperative outcomes from hand-sewn and stapled esophago-jejunal anastomosis during total gastrectomy in 72 patients with gastric cancer treated with total gastrectomy between May 2018 and December 2021.
Material and Methods
ETHICAL STATEMENT:
This was a retrospective study of patients’ medical records, and all data were fully anonymized before access. Written informed consent was obtained from all participants. All procedures were in accordance with the 1964 Declaration of Helsinki on Medical Research Involving Human Subjects and its subsequent amendments or comparable ethical standards. Our retrospective analysis of patient medical records fell into the category of exempt from Institutional Review Board (IRB) approval according to local regulations [12] and according to the official response from the Ethics Committee (number: PCN/CBN/0052/KB/153/22), details of which were provided to the journal.
BACKGROUND:
Data from 79 consecutive patients who underwent total gastrectomy for gastric cancer at our university medical center between 2018 and 2021 were retrospectively analyzed. The following inclusion criteria were defined:
The exclusion criteria were as follows:
After applying the above inclusion and exclusion criteria, 72 patients were eligible for the analysis.
PATIENTS’ CHARACTERISTICS:
Patients were treated according to the latest available European Society for Medical Oncology (ESMO) guidelines [13]. In 2022 there was a revision of ESMO guidelines with additional recommendations regarding management of gastric cancers [14]. Multidisciplinary treatment included collaboration between the surgeon, gastroenterologist, radiologist, and oncologist. Total gastrectomy was performed by experienced surgeons. Patients were divided into 2 groups according to the method of EJA: (1) EJA performed using a circular stapler or (2) EJA performed with hand suturing. A significance analysis of differences in terms of preoperative, intraoperative and postoperative factors was performed between the 2 groups.
SURGICAL TECHNIQUE:
The decision about the esophago-jejunal anastomosis technique was taken intraoperatively according to surgeon preference. Esophago-jejunal anastomoses were performed by 3 different surgeons. In all patients, restoration of intestinal continuity was made without preserving duodenal passage (DP) of food performing esophagojejunostomy with Roux-Y (RY) configuration. All esophago-jejunal anastomoses were performed using a retrocolic route. The first jejunal loop was cut and the distal jejunal loop was brought up to reach the esophagus. Hand-sewn end-to-end esophago-jejunal anastomosis was performed in 2 layers of 4-0 synthetic absorbable monofilament suture (an inner layer using running suture and a second layer using single sutures) by intussusception of about 2–4 cm of the distal end of the esophagus and esophago-jejunal anastomosis into the jejunum, end-to-end (Figure 1A). The technique of hand-sewn EJA was designed by the surgical team of our Digestive Tract Surgery Department, and the details of the technique are available in the experimental study [15]. The first layer of sutures connected the patients’ full thickness of the esophageal stump with the full thickness of the edge of the jejunal stump, and the second layer connected the esophageal tunica adventitia with the jejunal seromuscular layer. The distance between the second layer of single sutures and the ends of the esophagus and jejunum was about 4 cm, so that a jejunal cuff of 2–4 cm was created. After making the second layer of single sutures, while tying the knots, the part of the esophagus connected with the jejunal stump by the first layer of sutures was slid into the adjacent part of the jejunum, creating a jejunal cuff surrounding the esophagus edge and the EJA. For stapled end-to side esophago-jejunal anastomosis, a circular stapler-anvil method was used (Figure 1B) [16]. The device used for the anastomosis was the Ethicon (Johnson & Johnson) Circular Stapler CDH25B. The anvil was introducted into the esophageal stump, and the purse-string suture was placed around it. The stapler was placed in the jejunal stump. The opening was made in the antimesenteric surface of the jejunum, and then the stapler was attached with the anvil. The number of staples used depended on the esophageal diameter, and number of 25 was applied. In both groups, the jejunal and duodenal stump were closed using linear stapler or hand sutures. The jejuno-jejunal end-to-side anastomosis was performed at least 50 cm distally from EJA in 1 or 2 suture layers (inner layer using running suture and second layer using additional single sutures), using hand-sewn technique (4-0 synthetic absorbable monofilament suture).
ANALYSIS OF PREOPERATIVE AND INTRAOPERATIVE FACTORS:
Data collected on patients included: gender, age, body mass index (BMI), presence of comorbidities, chemotherapy before surgery, laboratory parameters white blood cells (WBC), C-reactive protein (CRP), platelets (PLT), hemoglobin (Hb), American Society of Anesthesiologists Physical Status (ASA-PS) score, intraoperative blood loss, red blood cell concentrate supply, surgery duration, and catecholamine administration. We collected data on the prevalence of diabetes and cardiovascular diseases including hypertension, ischemic heart disease and heart failure. The frequency of respiratory diseases such as asthma or chronic obstructive pulmonary disease was also included. Given speculation that active smoking before surgery may be a cause of postoperative complications [17], regular smoking during the year preceding surgery was included in the analysis to further assess the homogeneity of the study groups.
The ASA-PS scale was used to assess the clinical status of patients before surgery [18]. The indications for blood transfusion, administration of pressor amines, and all intraoperative management were consistent with the ERAS (Enhanced Recovery After Surgery) protocol and NICE (National Institute for Health and Care Excellence) principles [19,20]. The indication for intraoperative red blood cell concentrate transfusion was hemodynamic instability. Catecholamines (norepinephrine, epinephrine, dopamine, dobutamine) were administered during surgery because of hemodynamic instability associated with a decrease in mean arterial pressure or stroke volume.
ANALYSIS OF POSTOPERATIVE COMPLICATIONS AND FOLLOW-UP:
We analyzed the length of patients’ hospital stay (overall and after the surgery), the need for parenteral nutrition (along with its duration), as well as postoperative complications during hospitalization divided as early (<30 days) and late (≥30 days). The complications were categorized using the Clavien-Dindo scale, which is a recognized scale and has been used for years to assess surgical complications [21]. The occurrence of perioperative complications was analyzed, particularly including: anastomotic leakage, abdominal bleeding, infectious complications (suppuration of the wound, abscess, sepsis), eventration, perforation, intra-abdominal fluid collection, cardiopulmonary insufficiency and the need for ICU admission (along with length of ICU stay) due to postoperative complications.
Occurrence of late postoperative complications, particularly anastomotic strictures, as well as the need for rehospitalization or reoperation, was further assessed in the collected follow-up data after the patient’s discharge from the hospital.
Follow-up was conducted based on patient interviews collected between January 2022 and April 2022 (up to 4 attempted interviews at monthly intervals in case of non-response). We additionally included the information about local recurrence of the disease, metastases revealed after discharge, and overall patients’ survival.
STATISTICAL ANALYSIS:
Descriptive analysis was performed. A 95% confidence interval was used. The distribution of quantitative variables was analyzed. Variables with a normal distribution were expressed as means with their standard deviations; variables with a non-normal distribution were given as medians and their interquartile ranges (IQR). Analysis of differences between groups of patients divided according to the method of esophago-jejunal anastomosis (using stapler or manual suturing) was performed. The following factors were considered in the analysis: gender, age, BMI, comorbidities, preoperative chemotherapy, laboratory parameters, ASA-PS scale, operative time, blood loss, need for catecholamines administration and red blood cell concentrate transfusion, length of hospitalization, need for parenteral nutrition, and postoperative complications (including rehospitalizations, reoperations and death). The level of statistical significance was set at
Results
PATIENTS’ CHARACTERISTICS:
The study group consisted of 44 males and 28 females with a mean age of 65±10 (42–85) years; 57 (79.2%) patients were older than 59 years and 12 (16.7%) were over 74 years of age. Hand-sewn anastomosis was performed in 28 (39%) cases, while stapled anastomosis was performed in 44 (61%). All procedures were elective. According to the types and definitions of the gastric surgery provided by the Japanese Gastric Cancer Association, there were 54 (75%) standard TG, 11 (15.3%) extended TG, 5 (6.9%) palliative TG, and 2 (2.8%) completion TG [1]. The characteristics of the patients and their laboratory results are presented in Table 1.
PERIOPERATIVE PARAMETERS AND POSTOPERATIVE COMPLICATIONS:
Perioperative parameters are shown in Table 2. Most patients were in ASA-PS class III (43 patients 59.7%). Early postoperative complications occurred in 14 patients (19.4%). The most frequent complication was an esophago-jejunal anastomosis leakage 4 patients (5.6%). The most common surgical complications were Clavien-Dindo grade IV (6 patients 8.3%). There was 1 case of in-hospital mortality (1.4%) due to the perforation of the duodenum, abscess, and subsequent sepsis. Postoperative complications are presented in Table 3.
HISTOPATHOLOGICAL EXAMINATION:
According to American Joint Committee on Cancer (AJCC) classification [22], most of the patients had cancer stage IA (12 patients 17%), followed by IIB and IIIB (11 and 11 patients respectively 16%, Table 4, Figure 2). The most uncommon was stage IV 2 patients (3%). There were 32 patients with nodal metastases (44%) and 2 (3%) with distal metastases (Table 4).
FOLLOW-UP:
Mean follow-up time was 1.7±0.9 (0.4–3.7) years. During this period, anastomotic stricture occurred in 13 cases (18.1%). Median time after surgery when the stricture appeared was 3.5 months (IQR 8; range 1.5–15 months). The number of patients alive at the end of observation period (01.2022, including interviews and medical records) was 53/72 (73.6%). Twelve patients (17%) died (1 in-hospital) while 7 patients (9.7%) were lost to follow-up. The most common cause of death was cancer progression or its recurrence 7 patients (58.3% of all deaths). Follow-up of the patients is presented in Table 5. Overall disease-specific survival (DSS) after 12 and 24 months was 93.8% and 86.5%, respectively. Overall disease-free survival (DFS) after 12 and 24 months was 81.9% and 73.9%, respectively. DSS and DFS for particular groups are presented in Figures 3 and 4, respectively.
COMPARISON BETWEEN HAND-SEWN AND STAPLED GROUPS:
The groups were very similar to each other. There were no statistically significant differences among the patients’ age, gender, BMI, comorbidities (including hypertension, non-ischemic heart disease, diabetes, asthma, and others), chemotherapy before surgery or laboratory parameters, or ASA-PS scores (P>0.05 for all mentioned variables, Table 1). Perioperative parameters such as duration of surgery, blood loss, catecholamines administration, need for red blood cell concentrate transfusion, and length of hospital stay were also not significantly different between the analyzed groups (P>0.05 in each case, Table 2). This ensured homogeneity of the studied groups and tested as many potential confounding factors as possible.
Early postoperative complications rates were 18.2% (8/44) in the stapled group and 21.4% (6/28) in the hand-sewn group (p=0.48, Table 3). The most frequent complication was anastomotic leakage 2 cases in the stapled group and 2 in the hand-sewn group (4.5% and 7.1%, respectively, P=0.76). There were 3 (11%) admissions to the ICU in the hand-sewn group and 4 (9%) in the stapled group (P=1.0). There were no significant differences regarding response to follow-up (88.6% response in stapled group, 77.8% in hand-sewn group; P=0.21) (Table 5). During the follow-up period, anastomotic stricture occurred in 7 (15.9%) of 44 cases with stapled anastomosis, and in 6 (21.4%) of 28 cases with hand-sewn anastomosis (P=0.52). There were 12 deaths (17%), 6 in each group, with no between-group differences (P=0.32). Disease-specific survival was similar in both groups (88.9% for hand-sewn anastomosis and 70.2% for stapled anastomosis, with no significant difference in follow-up duration; P=0.59) (Figure 3). There were no differences in disease-free survival (68.4% for hand-sewn group and 61.5% for stapled group; P=0.89) (Figure 4).
Discussion
We compared surgical outcomes of hand-sewn and circular stapled esophago-jejunal anastomosis in open total gastrectomy. The groups of patients were fairly homogenous with respect to age, laboratory parameters, cancer staging, and other potentially confounding variables. The main finding of this study is that there were no between-group differences in terms of surgery duration, LOS, and postoperative complications, with particular emphasis on anastomotic leakage, abdominal abscess, and anastomotic strictures in long-term follow-up. Additionally, during the follow-up we assessed the recurrence rate and long-term survival of patients with gastric cancer after TG, and there were no significant differences, which is another factor proving the similarity of these 2 groups.
The length of the procedure, which is associated with anastomosis time, is one of the most important factors influencing the patient’s condition after surgery. Longer surgery and anesthesia puts additional strain on the patient and increases the incidence of postoperative complications [23]. In our study, there was no significant difference between hand-sewn anastomosis and circular stapling anastomosis (
Regardless of the continuous development of anastomotic techniques, esophago-jejunal anastomotic leakage (EJAL) remains one of the most serious complications in total gastrectomy, affecting 4–15% of patients [33]. Several potential risk factors of EJAL were proposed, including advanced age, male sex, anemia, malnourishment, cardiovascular diseases, pulmonary insufficiency, diabetes, smoking, obesity, stage and localization of the tumor, and surgical technique [33]. Considering the EJA method, some comparative studies reported lower leakage rates for stapled anastomosis [7,8,34], with differences also for particular types of staplers, while in other large cohorts the methods were equivalent [25], or even a higher leakage incidence after circular stapled anastomosis was observed [35]. Muneoka et al [36] compared the efficacy of linear and circular stapling in open total gastrectomy, showing that the occurrence of surgical complications was similar in both groups, but the use of a linear stapler improved patients’ nutritional status after the surgery and reduced blood loss. In a review by Umemura et al [35],a linear stapler was superior to a circular stapler in terms of both leakage and stenosis. In our cohort, 4 patients (5.6%) were diagnosed with EJAL, which is an acceptable rate, similar to that reported in the Japanese National Clinical Database (4.4%) [37]. EJAL was associated with longer hospitalization time (over 30 days for each patient) and half of the patients required ICU admission. All patients were above 65 years old with cardiovascular diseases, and 3 of them were overweight. Both stapler and hand-sewn technique in our study seem to provide safe anastomosis in open total gastrectomy. The occurrence of EJAL was not associated with anastomosis technique, tumor staging, preoperative chemotherapy, surgery duration, or combined organ resection, but the sample size was too small for extended analysis of EJAL risk factors. The results are also limited by the fact that we investigated only 1 method of stapled anastomosis, while the linear stapled technique seems to be beneficial in most studies. Therefore, further research should take into account more potential confounding factors not included in this study, but some of them (like surgical technique details, experience of the surgeon, or tension on the anastomosis site) are difficult to assess and may be potential sources of bias.
Overall complications rate in our study was 18.1%, with no significant difference between the analyzed groups (21% for hand-sewn; 16% for stapler group;
Among the long-term complications associated with EJA, anastomotic stricture is one of the most important, as it affects patient’s quality of life and often requires invasive treatment by endoscopic dilation. The frequency of anastomotic strictures in the literature varies from 4.1 to 38% [38–45], with various factors indicated as possibly affecting the stenosis rates. In a study on the efficacy of esophagogastric anastomosis with a circular stapler [38], the overall stricture rate was 38%, with differences reported for the various stapler sizes. A higher stricture risk was observed when a 25-mm stapler was used compared with a 28- or 29-mm device (53% vs 23%, respectively). Moreover, the occurrence of anastomotic leakage was an independent risk factor for stenosis. In a recent analysis, Tyler et al [39] excluded patients with anastomotic leakage as a known risk factor for stenosis, and they observed a 10% stenosis rate (most occurring during the first 100 days after surgery). In our study, symptomatic anastomotic strictures mostly occurred 3.5 months after surgery, in a total of 13 cases (18.1%). In 1 case of stenosis, the postoperative course was complicated by anastomotic leakage. The slightly higher incidence of stenosis might be the result of stapler size used for gastrointestinal tract reconstruction. The most commonly used size of circular stapler in our clinic was 25 mm, followed by 21 mm. The decision about stapler size was made intraoperatively, based on the inner diameter of the patient’s esophagus. In some studies there was no difference in strictures rates, comparing 21-mm and 25-mm [40] or 23–25-mm and 28–33-mm circular staplers [39,41,42]. However, a large Japanese cohort [43], as well as a randomized trial by Fisher et al [44], reported the use of smaller stapler as a risk factor for stenosis. The impact of stapler size on formation of anastomotic strictures was confirmed in a recent meta-analysis [45] in which the mean stricture rate was 31% and it was significantly higher for smaller staplers, comparing 21-mm and 25-mm, as well as 25-mm and 28-mm circular devices. A review on laparoscopic total gastrectomy indicated that the linear stapler technique is superior to circular in terms of anastomotic stenosis [35], which was confirmed in a recent study by Park et al [46]. Moreover, similar results were found for linear staplers in comparison with hand-sewn anastomosis [47]. A meta-analysis by Honda et al [48] revealed a higher incidence of strictures in stapled anastomosis than in hand-sewn anastomosis, but only when the circular stapler diameter was below 30 mm, but in some studies there was no difference [7]. Another study reported superior results of the linear stapler technique, with diameter of anastomosis measured in endoscopy 1.6 cm in the linear group, 1.2 cm in the hand-sewn group, and 1.0 cm in the circular group, without significant difference between the last 2 groups [49]. In that paper, despite the relatively small sizes of staplers used, no difference was found regarding anastomotic stricture, with stenosis rates of 15.9% in the stapler group and 21.4% in the hand-sewn group (
There was no significant difference in hospital mortality between the hand-sewn and stapled anastomosis groups in our study (
It is also worth noting that there is a significant difference in cost between methods of performing anastomosis, which in many clinical centers may be crucial when choosing a particular method. Depending on various factors, the cost of using a stapler compared to the hand-sewn approach may be several hundred euros more expensive [30,32,58]. Taking into account similar clinical outcomes of patients after stapled and traditional EJA, the hand-sewn technique may be a good alternative when a cost-effective approach is needed.
There are some limitations to our research. This was a single-center retrospective study restricted to 72 patients; however, the groups were comparable, with good homogeneity. The relatively short time of observation (3.5 years) limited the number of patients included, but guaranteed similar cancer treatment protocol and surgical technique. The study is also limited to the comparison of only 2 types of anastomoses, as we included those with higher surgeon experience in our center to avoid the factors associated with a learning curve. Anastomosis was also performed by 3 different surgeons, which may have influenced results, although all surgeons had extensive experience in gastric surgery, which should have limited any potential impact. Another limitation is that some possible confounding factors were not taken into account, as these were difficult to assess retrospectively and could create potential risk of bias. Variables such as anastomosis site tension or duration of the anastomosis creation should be taken into account in further prospective comparative studies on gastrointestinal tract anastomoses. The main limitation associated with the retrospective design of our study is the risk of selection bias, as the choice of anastomosis technique was based only on the surgeon’s preference; therefore, randomized controlled trials are needed to confirm these findings. The low incidence of postoperative anastomotic leakage did not allow us to perform analysis of risk factors for this complication, so comparison of leakage incidence between the 2 anastomotic techniques needs to be further performed in larger cohorts, and the incidence of this complication is itself an important outcome. In our study, the anastomosis diameter was not assessed prospectively during endoscopic follow-up for the whole cohort; we assessed only the occurrence of symptomatic strictures (with or without the need for endoscopic dilation), as we believe these are the most important ones, taking into account the impact on patients’ quality of life, nutritional status, and further management, as well as possible subsequent complications.
Conclusions
There were no significant differences in postoperative complications and surgery duration between the hand-sewn and stapler esophago-jejunal anastomosis groups. The results indicate that stapled and hand-sewn anastomoses in open total gastrectomy are equivalent. The postoperative mortality after open total gastrectomy is low, despite the patients’ burden.
Figures
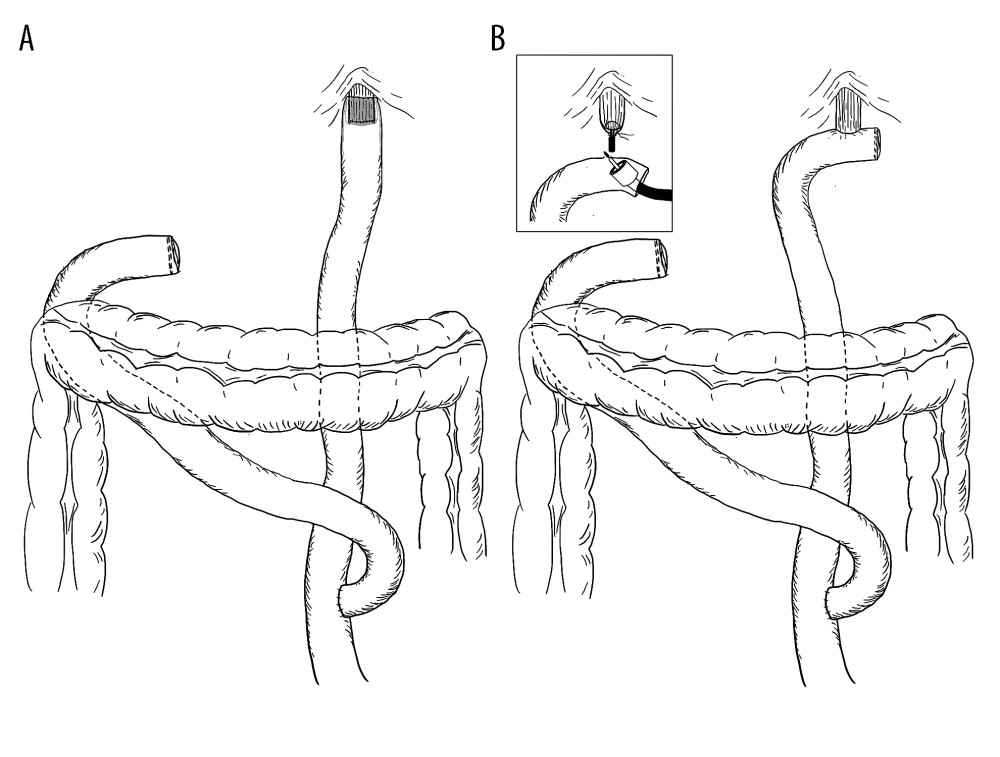 Figure 1. Schematic presentation of gastrointestinal tract reconstruction after total gastrectomy end-to-end hand-sewn esophagojejunostomy (A), end-to-side circular stapled esophagojejunostomy (B). The figure was created by author Karolina Majewska using GoodNotes 5 application, Time Base Technology Limited, © 2011–2022 GoodNotes Limited.
Figure 1. Schematic presentation of gastrointestinal tract reconstruction after total gastrectomy end-to-end hand-sewn esophagojejunostomy (A), end-to-side circular stapled esophagojejunostomy (B). The figure was created by author Karolina Majewska using GoodNotes 5 application, Time Base Technology Limited, © 2011–2022 GoodNotes Limited. 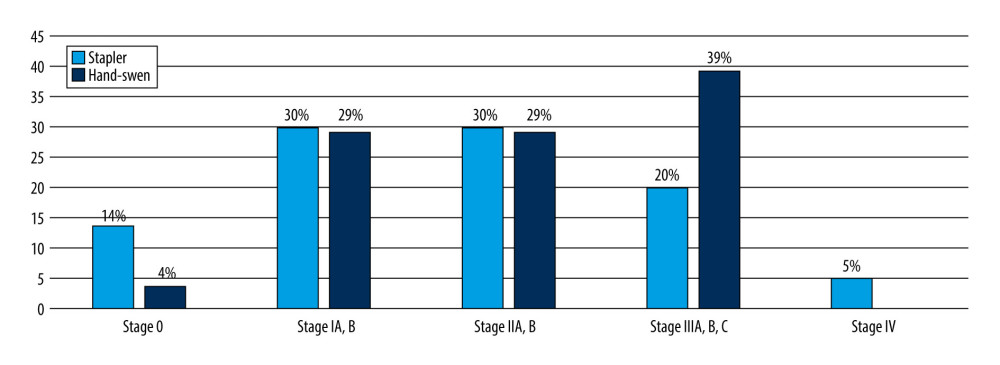 Figure 2. American Joint Committee on Cancer (AJCC) staging comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 2. American Joint Committee on Cancer (AJCC) staging comparison between stapler and hand-sewn esophago-jejunal anastomosis. 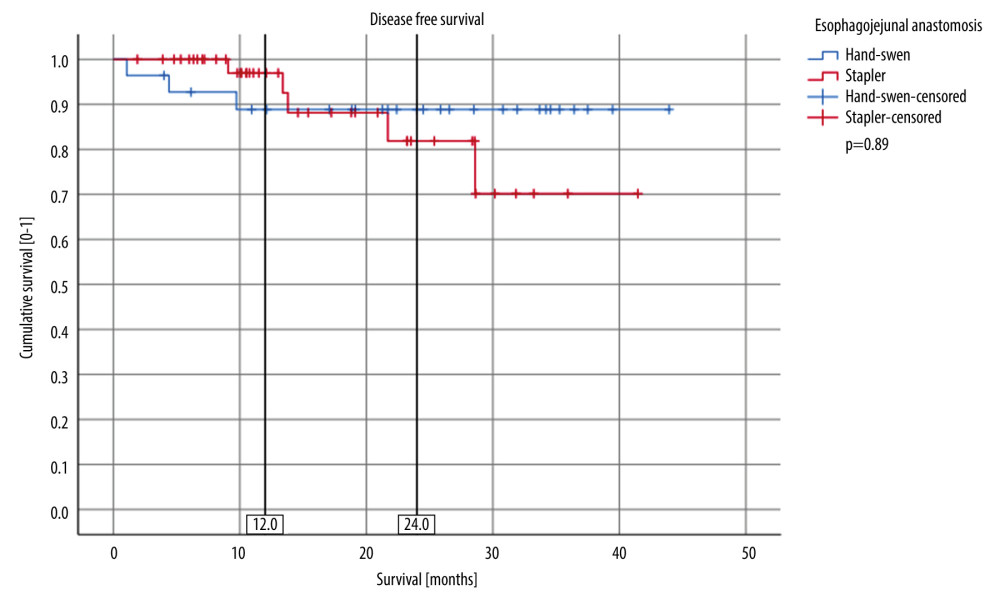 Figure 3. Disease-Specific Survival (DSS) comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 3. Disease-Specific Survival (DSS) comparison between stapler and hand-sewn esophago-jejunal anastomosis. 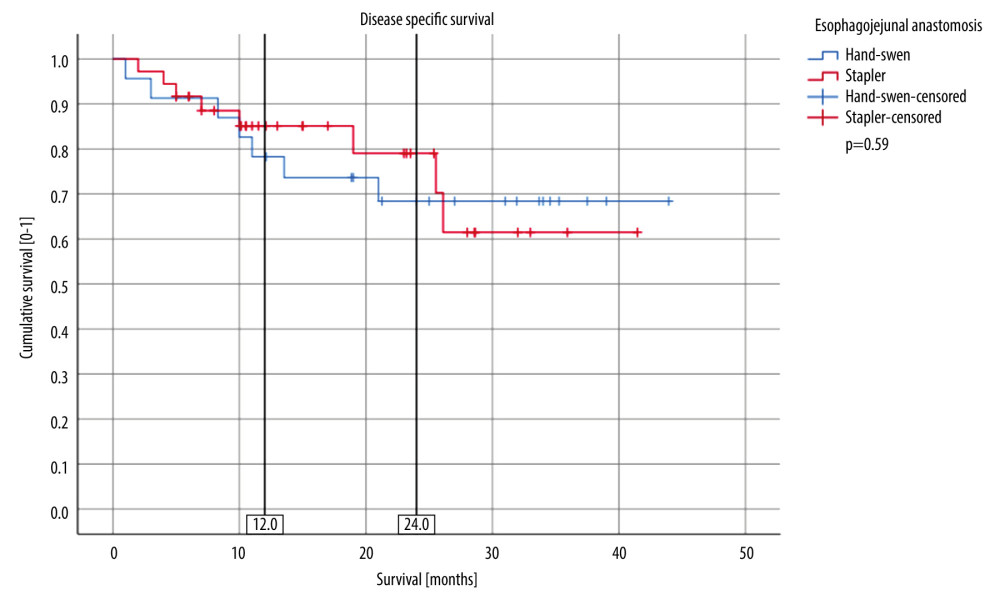 Figure 4. Disease-Free Survival (DFS) comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 4. Disease-Free Survival (DFS) comparison between stapler and hand-sewn esophago-jejunal anastomosis. References
1. : Gastric Cancer, 2021; 24(1); 1-21
2. Sweigert PJ, Eguia E, Nelson MH, Total gastrectomy in patients with gastric adenocarcinoma: Is there an advantage to the minimally invasive approach?: Surgery, 2019; 166(4); 623-31
3. Katai H, Mizusawa J, Katayama H, Single-arm confirmatory trial of laparoscopy-assisted total or proximal gastrectomy with nodal dissection for clinical stage I gastric cancer: Japan Clinical Oncology Group study JCOG1401: Gastric Cancer, 2019; 22(5); 999-1008
4. Kim H-H, Han S-U, Kim M-C, Effect of laparoscopic distal gastrectomy vs open distal gastrectomy on long-term survival among patients with stage I gastric cancer: JAMA Oncol, 2019; 5(4); 506-13
5. Chen K, Di Wu , Pan Y, Totally laparoscopic gastrectomy using intracorporeally stapler or hand-sewn anastomosis for gastric cancer: A single-center experience of 478 consecutive cases and outcomes: World J Surg Oncol, 2016; 14(1); 115
6. Honório FCC, Tustumi F, Pinheiro Filho JEL, Esophagojejunostomy after total gastrectomy: A systematic review and meta-analysis comparing hand-sewn and stapled anastomosis: J Surg Oncol, 2022; 126(1); 161-67
7. Takeyoshi I, Ohwada S, Ogawa T, Esophageal anastomosis following gastrectomy for gastric cancer: Comparison of hand-sewn and stapling technique: Hepatogastroenterology, 2000; 47(34); 1026-29
8. Liu B, Liu Y, Liu J, Feng Z, Comparison of hand-sewn and stapled anastomoses in surgeries of gastrointestinal tumors based on clinical practice of China: World J Surg Onc, 2014; 12(1); 292
9. Fujimoto S, Takahashi M, Endoh F, Stapled or manual suturing in esophagojejunostomy after total gastrectomy: A comparison of outcome in 379 patients: Am J Surg, 1991; 162(3); 256-59
10. Fok M, Ah-Chong AK, Cheng SWK, Wong J, Comparison of a single layer continuous hand-sewn method and circular stapling in 580 oesophageal anastomoses: Br J Surg, 2005; 78(3); 342-45
11. Kolandasamy C, Short term and long term outcomes of stapled versus handsewn oesophagojejunal anastomosis after total gastrectomy: Doctoral dissertation, 2017, Madras Medical College
12. Ministerstwo zdrowia: Rozporządzenie ministra zdrowia i opieki społecznej w sprawie szczegółowych zasad powoływania i finansowania oraz trybu działania komisji bioetycznych Available from: [in Polish]http://isap.sejm.gov.pl/isap.nsf/download.xsp/WDU19990470480/T/D19990480L.pdf
13. Smyth EC, Verheij M, Allum W, Gastric cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up: Ann Oncol, 2016; 27; v38-v49
14. Lordick F, Carneiro F, Cascinu SESMO Guidelines Committee, Gastric cancer: ESMO Clinical Practice Guideline for diagnosis, treatment and follow-up: Ann Oncol, 2022; 33(10); 1005-20
15. Wojtyczka A, Górka Z, Bierzynska-Macyszyn G, Gastrectomy in the rat using two modifications of esophagojejunal anastomosis. General status, local histological changes and relationships to bone density: Eur Surg Res, 1999; 31(6); 497-507
16. Ellison E, Zollinger RM, Total gastrectomy, stapled: Zollinger’s atlas of surgical operations, 2016; 10e, McGraw Hill https://accesssurgery.mhmedical.com/content.aspx?bookid=1755§ionid=119128495
17. Thomsen T, Villebro N, Møller AM, Interventions for preoperative smoking cessation: Cochrane Database Syst Rev, 2014; 2014(3); CD002294
18. Mayhew D, Mendonca V, Murthy BVS, A review of ASA physical status historical perspectives and modern developments: Anaesthesia, 2019; 74(3); 373-79
19. Desiderio J, Trastulli S, D’Andrea V, Parisi A, Enhanced recovery after surgery for gastric cancer (ERAS-GC): Optimizing patient outcome: Transl Gastroenterol Hepatol, 2020; 5; 11
20. National Institute for Health and Care Excellence: Intravenous fluid therapy in adults in hospital, 2017 Available from: https://www.nice.org.uk/guidance/cg174
21. Dindo D, Demartines N, Clavien P-A, Classification of surgical complications: Ann Surg, 2004; 240(2); 205-13
22. Amin MB, Edge SB, Greene FL, Brierley JD: AJCC cancer staging manual, 2017, New York, Springer
23. Cheng H, Clymer JW, Po-Han Chen B, Prolonged operative duration is associated with complications: A systematic review and meta-analysis: J Surg Res, 2018; 229; 134-44
24. Seufert RM, Schmidt-Matthiesen A, Beyer A, Total gastrectomy and oesophagojejunostomy a prospective randomized trial of hand-sutured versus mechanically stapled anastomoses: Br J Surg, 2005; 77(1); 50-52
25. Celis J, Ruiz E, Berrospi F, Payet EMechanical versus manual suture in the jejunal esophageal anastomosis after total gastrectomy in gastric cancer: Rev Gastroenterol Peru, 2001; 21(4); 271-75 [in Spanish]
26. Law S, Fok M, Chu K-M, Wong J, Comparison of hand-sewn and stapled esophagogastric anastomosis after esophageal resection for cancer: Ann Surg, 1997; 226(2); 169-73
27. Liu Q-X, Qiu Y, Deng X-F, Comparison of outcomes following end-to-end hand-sewn and mechanical esophagogastric anastomosis after oesophagectomy for carcinoma: A prospective randomized controlled trial: Eur J Cardiothorac Surg, 2015; 47(3); e118-23
28. Vilela Castro PM, Gonçalves Ribeiro FP, de Freitas Rocha A, Hand-sewn versus stapler esophagogastric anastomosis after esophageal ressection: sistematic review and meta-analysis: Arq Bras Cir Dig, 2014; 27(3); 216-21
29. Seo SH, Kim KH, Kim MC, Comparative study of hand-sutured versus circular stapled anastomosis for gastrojejunostomy in laparoscopy assisted distal gastrectomy: J Gastric Cancer, 2012; 12(2); 120-25
30. Jarry J, Wagner T, de Pommerol M, Laparoscopic Roux-en-Y gastric bypass: Comparison between hand-sewn and mechanical gastrojejunostomy: Updates Surg, 2012; 64(1); 25-30
31. Jiang H-P, Lin L-L, Jiang X, Qiao H-Q, Meta-analysis of hand-sewn versus mechanical gastrojejunal anastomosis during laparoscopic Roux-en-Y gastric bypass for morbid obesity: Int J Surg, 2016; 32; 150-57
32. Wang Z, Wei Y, Liu X, Application value of hand-sewn anastomosis in totally laparoscopic total gastrectomy for gastric cancer: World J Surg Onc, 2021; 19(1); 229
33. Gong W, Li J, Combat with esophagojejunal anastomotic leakage after total gastrectomy for gastric cancer: A critical review of the literature: Int J Surg, 2017; 47; 18-24
34. Kim HS, Kim BS, Lee IS, Comparison of totally laparoscopic total gastrectomy and open total gastrectomy for gastric cancer: J Laparoendosc Adv Surg Tech, 2013; 23(4); 323-31
35. Umemura A, Koeda K, Sasaki A, Totally laparoscopic total gastrectomy for gastric cancer: Literature review and comparison of the procedure of esophagojejunostomy: Asian J Surg, 2015; 38(2); 102-12
36. Muneoka Y, Ohashi M, Makuuchi R, Advantageous short-term outcomes of esophagojejunostomy using a linear stapler following open total gastrectomy compared with a circular stapler: World J Surg, 2021; 45(8); 2501-9
37. Watanabe M, Miyata H, Gotoh M, Total gastrectomy risk model: Ann Surg, 2014; 260(6); 1034-39
38. Hosoi T, Abe T, Uemura N, The impact of circular stapler size on the incidence of cervical anastomotic stricture after esophagectomy: World J Surg, 2019; 43(7); 1746-55
39. Tyler RW, Nair A, Lau M, Hodson J, Incidence of anastomotic stricture after Ivor-Lewis oesophagectomy using a circular stapling device: World J Gastrointest Surg, 2019; 11(11); 407-13
40. Wang J, Yao F, Yao J, 21- versus 25-mm circular staplers for cervical anastomosis: A propensity-matched study: J Surg Res, 2020; 246; 427-34
41. Yendamuri S, Gutierrez L, Oni A, Does circular stapled esophagogastric anastomotic size affect the incidence of postoperative strictures?: J Surg Res, 2011; 165(1); 1-4
42. Tagkalos E, van der Sluis PC, Uzun E, The circular stapled esophagogastric anastomosis in esophagectomy: No differences in anastomotic insufficiency and stricture rates between the 25 mm and 28 mm circular stapler: J Gastrointest Surg, 2021; 25(9); 2242-49
43. Fukagawa T, Gotoda T, Oda I, Stenosis of esophago-jejuno anastomosis after gastric surgery: World J Surg, 2010; 34(8); 1859-63
44. Fisher BL, Atkinson JD, Cottam D, Incidence of gastroenterostomy stenosis in laparoscopic Roux-en-Y gastric bypass using 21- or 25-mm circular stapler: A randomized prospective blinded study: Surg Obes Relat Dis, 2007; 3(2); 176-79
45. Allen W, Wells CI, Greenslade M, Association between circular stapler diameter and stricture rates following gastrointestinal anastomosis: Systematic review and meta-analysis: World J Surg, 2018; 42(10); 3097-105
46. Park KB, Kim EY, Song KY, Esophagojejunal anastomosis after laparoscopic total gastrectomy for gastric cancer: Circular versus linear stapling: J Gastric Cancer, 2019; 19(3); 344-54
47. Deng X-F, Liu Q-X, Zhou D, Hand-sewn vs linearly stapled esophagogastric anastomosis for esophageal cancer: A meta-analysis: World J Gastroenterol, 2015; 21(15); 4757-64
48. Honda M, Kuriyama A, Noma H, Hand-sewn versus mechanical esophagogastric anastomosis after esophagectomy: Ann Surg, 2013; 257(2); 238-48
49. Xu Q-R, Wang K-N, Wang W-P, Linear stapled esophagogastrostomy is more effective than hand-sewn or circular stapler in prevention of anastomotic stricture: A comparative clinical study: J Gastrointest Surg, 2011; 15(6); 915-21
50. Markar SR, Karthikesalingam A, Vyas S, Hand-sewn versus stapled oesophago-gastric anastomosis: Systematic review and meta-analysis: J Gastrointest Surg, 2011; 15(5); 876-84
51. Shannon AB, Straker RJ, Fraker DL, Ninety-day mortality after total gastrectomy for gastric cancer: Surgery, 2021; 170(2); 603-9
52. Li SS, Costantino CL, Mullen JT, Morbidity and mortality of total gastrectomy: A comprehensive analysis of 90-day outcomes: J Gastrointest Surg, 2019; 23(7); 1340-48
53. Iwatsuki M, Yamamoto H, Miyata H, Association of surgeon and hospital volume with postoperative mortality after total gastrectomy for gastric cancer: Data from 71,307 Japanese patients collected from a nationwide web-based data entry system: Gastric Cancer, 2021; 24(2); 526-34
54. van Putten M, Nelen SD, Lemmens VEPP, Overall survival before and after centralization of gastric cancer surgery in the Netherlands: Br J Surg, 2018; 105(13); 1807-15
55. Urschel JD, Blewett CJ, Bennett WF, Handsewn or stapled esophagogastric anastomoses after esophagectomy for cancer: Meta-analysis of randomized controlled trials: Dis tEsophagus, 2001; 14(3–4); 212-17
56. Kim T, Yu W, Chung H, Handsewn versus stapled gastroduodenostomy in patients with gastric cancer: Long-term follow-up of a randomized clinical trial: World J Surg, 2011; 35(5); 1026-29
57. Li Z, Liu Y, Bai B, Surgical and long-term survival outcomes after laparoscopic and open total gastrectomy for locally advanced gastric cancer: a propensity score-matched analysis: World J Surg, 2019; 43(2); 594-603
58. Wang Z, Liu X, Cheng Q, Digestive tract reconstruction of laparoscopic total gastrectomy for gastric cancer: A comparison of the intracorporeal overlap, intracorporeal hand-sewn anastomosis, and extracorporeal anastomosis: J Gastrointest Oncol, 2021; 12(3); 1031-41
Figures
 Figure 1. Schematic presentation of gastrointestinal tract reconstruction after total gastrectomy end-to-end hand-sewn esophagojejunostomy (A), end-to-side circular stapled esophagojejunostomy (B). The figure was created by author Karolina Majewska using GoodNotes 5 application, Time Base Technology Limited, © 2011–2022 GoodNotes Limited.
Figure 1. Schematic presentation of gastrointestinal tract reconstruction after total gastrectomy end-to-end hand-sewn esophagojejunostomy (A), end-to-side circular stapled esophagojejunostomy (B). The figure was created by author Karolina Majewska using GoodNotes 5 application, Time Base Technology Limited, © 2011–2022 GoodNotes Limited. Figure 2. American Joint Committee on Cancer (AJCC) staging comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 2. American Joint Committee on Cancer (AJCC) staging comparison between stapler and hand-sewn esophago-jejunal anastomosis. Figure 3. Disease-Specific Survival (DSS) comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 3. Disease-Specific Survival (DSS) comparison between stapler and hand-sewn esophago-jejunal anastomosis. Figure 4. Disease-Free Survival (DFS) comparison between stapler and hand-sewn esophago-jejunal anastomosis.
Figure 4. Disease-Free Survival (DFS) comparison between stapler and hand-sewn esophago-jejunal anastomosis. Tables
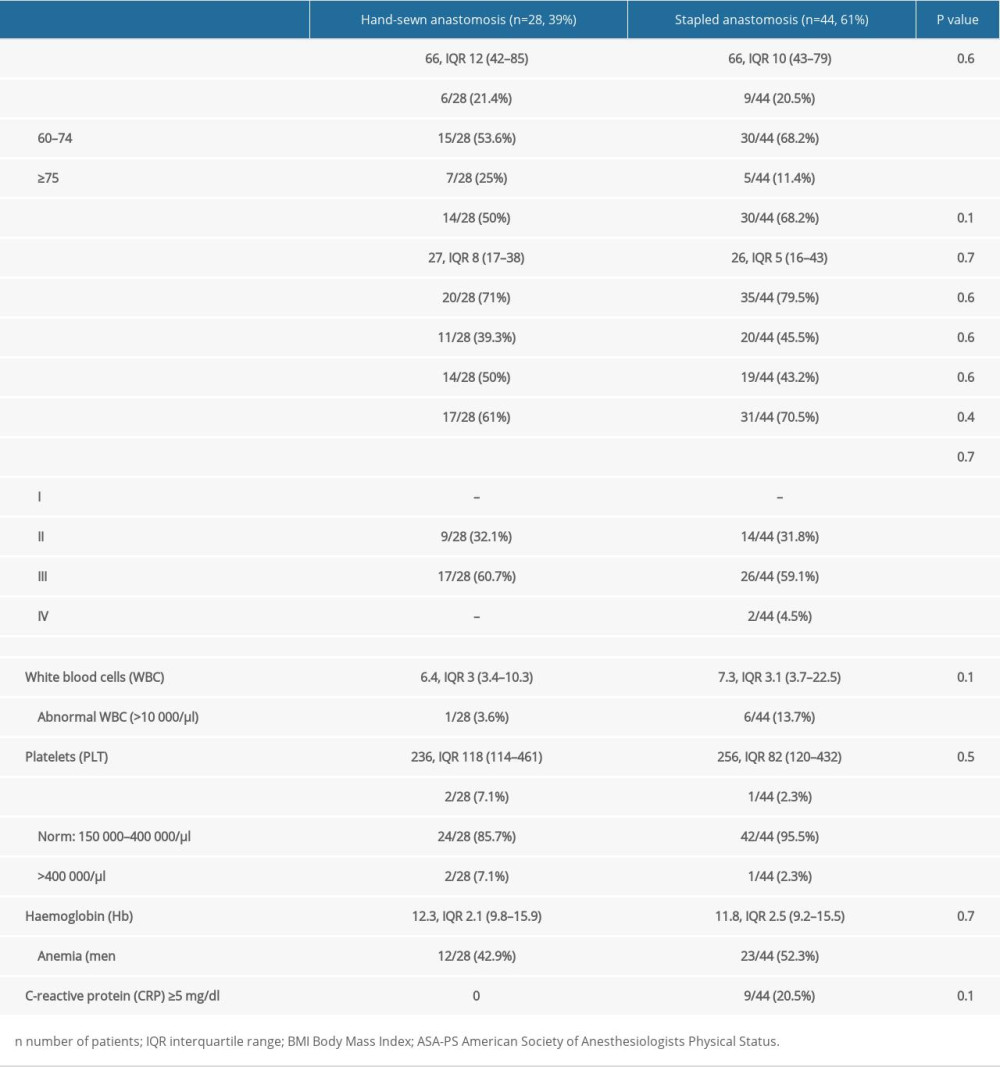 Table 1. The general characteristics of patients.
Table 1. The general characteristics of patients.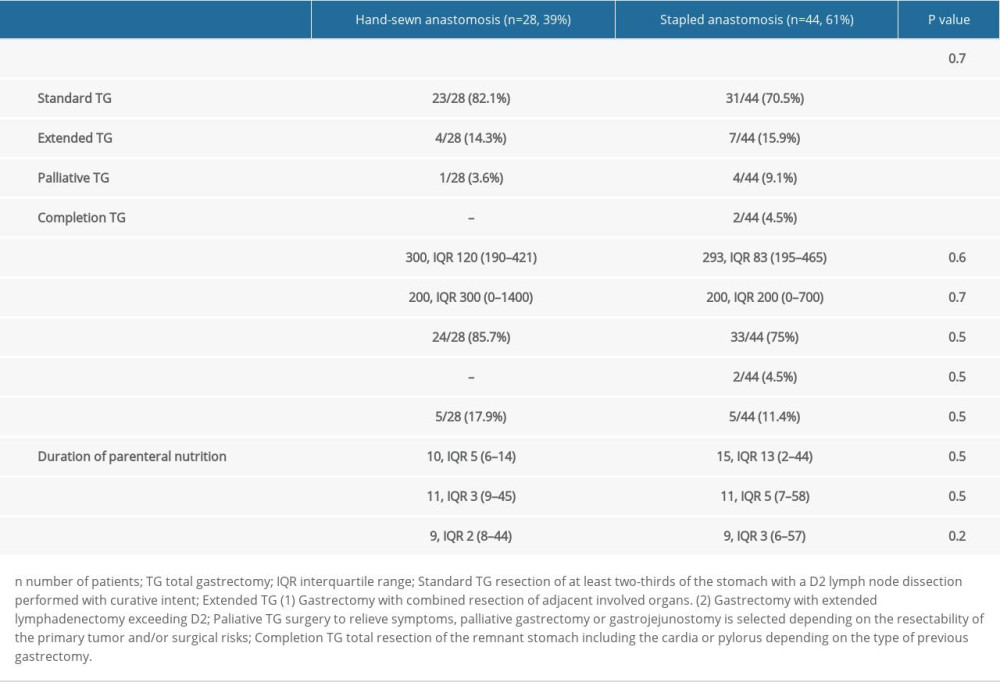 Table 2. Perioperative parameters.
Table 2. Perioperative parameters.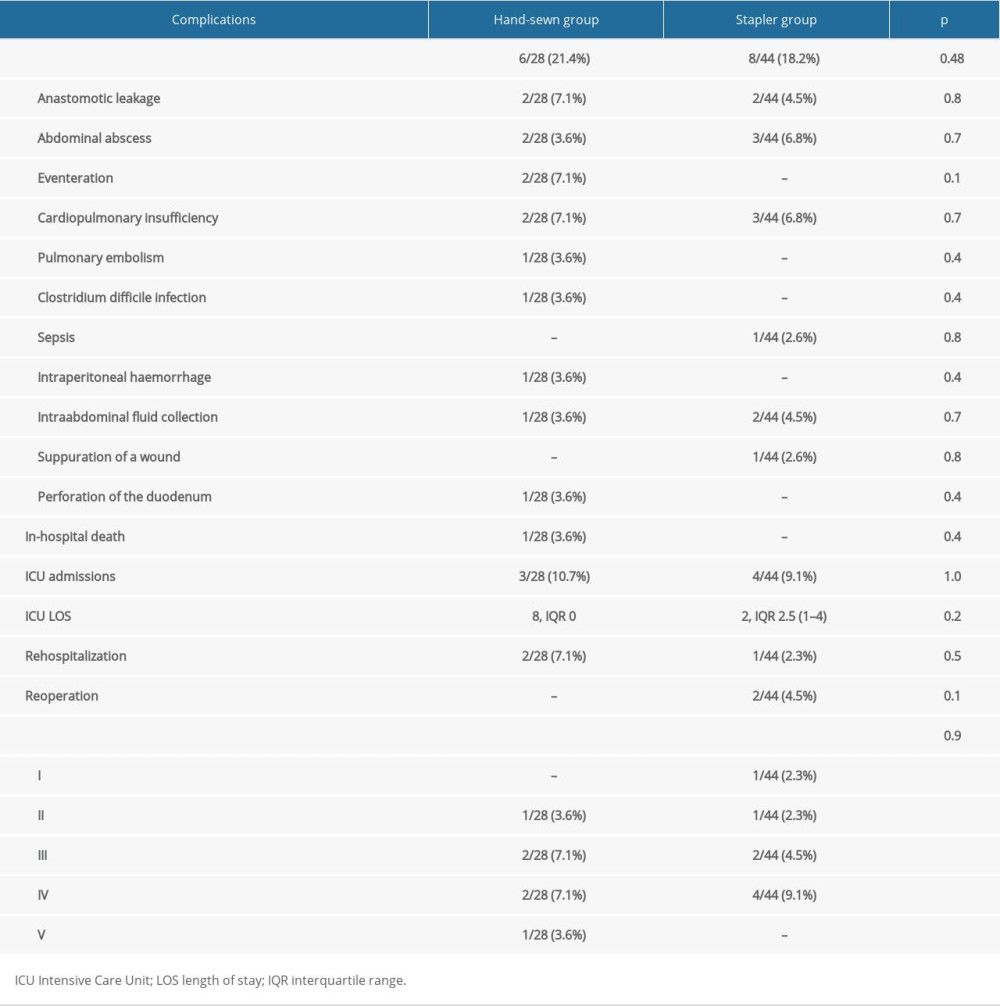 Table 3. Early surgical complications.
Table 3. Early surgical complications.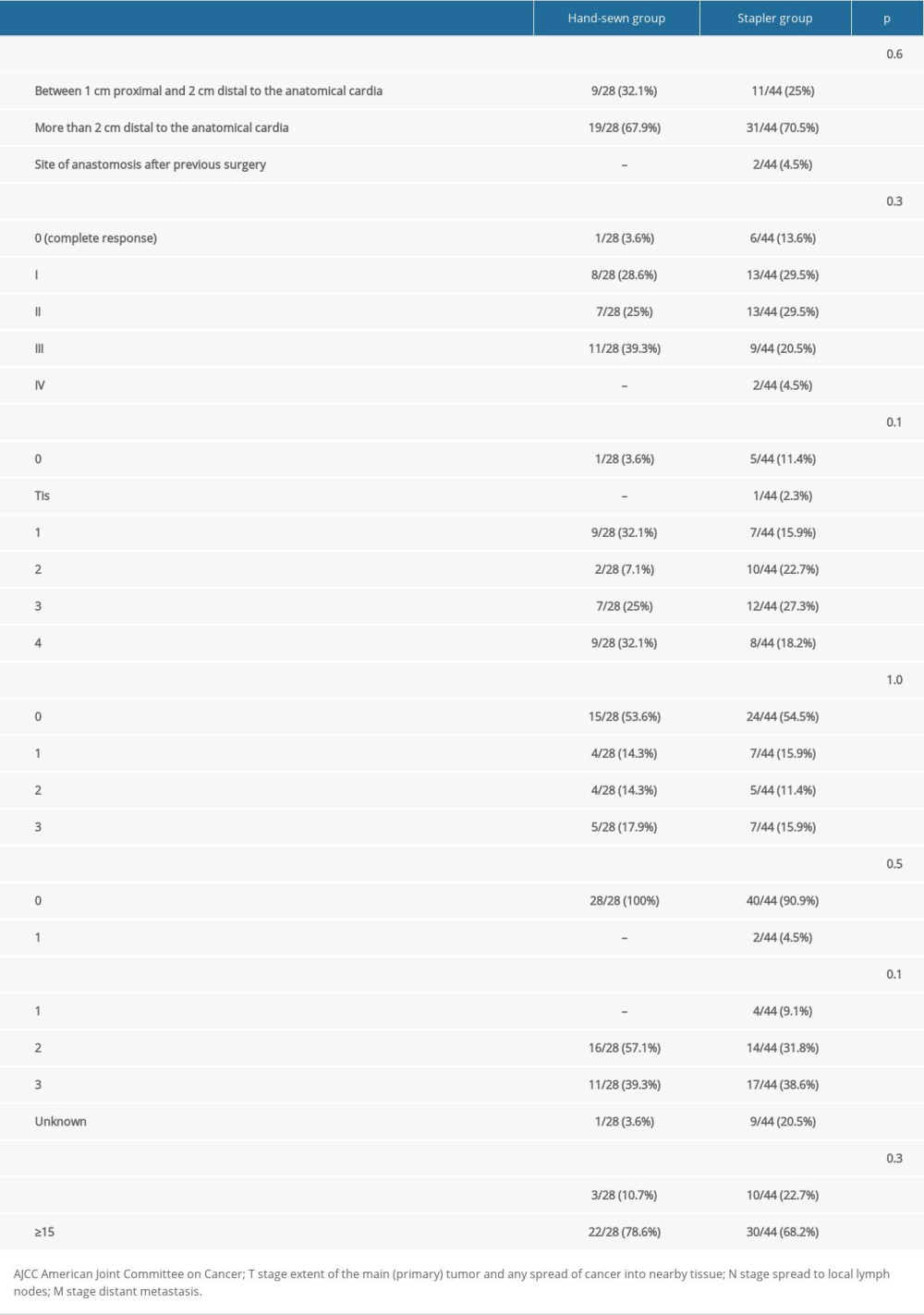 Table 4. Histopathological classification.
Table 4. Histopathological classification.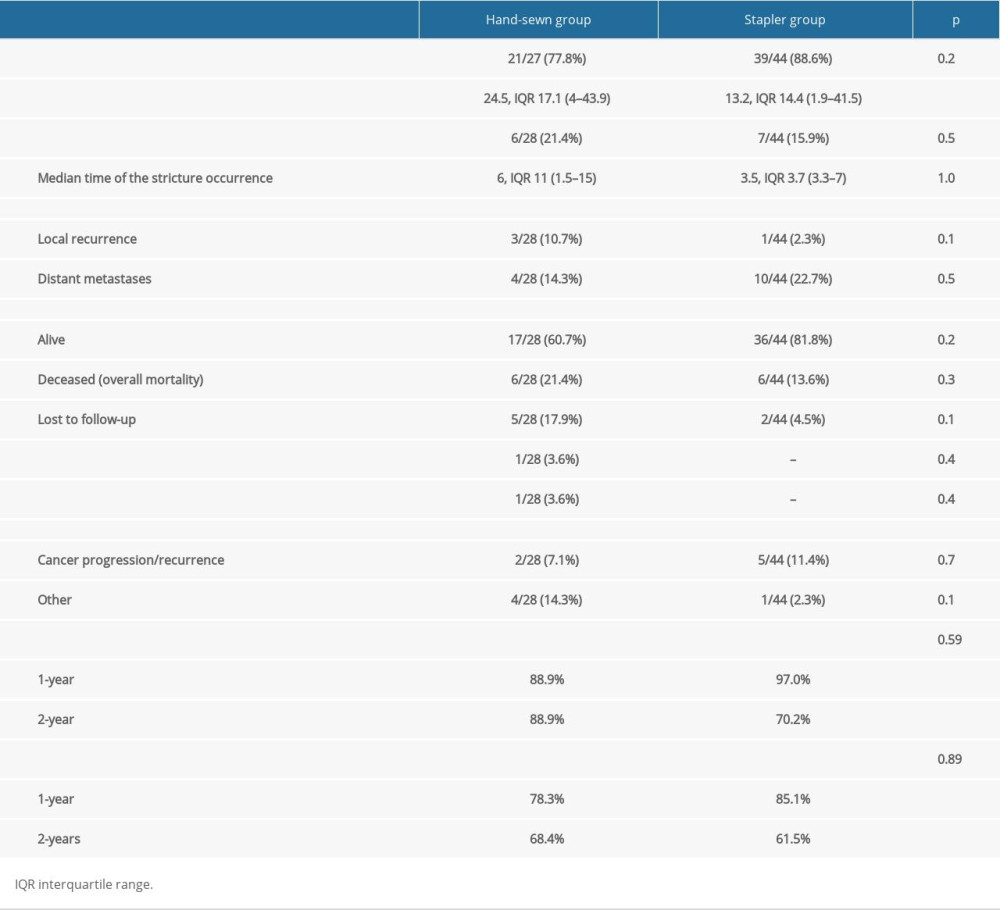 Table 5. Follow-up of the patients.
Table 5. Follow-up of the patients. Table 1. The general characteristics of patients.
Table 1. The general characteristics of patients. Table 2. Perioperative parameters.
Table 2. Perioperative parameters. Table 3. Early surgical complications.
Table 3. Early surgical complications. Table 4. Histopathological classification.
Table 4. Histopathological classification. Table 5. Follow-up of the patients.
Table 5. Follow-up of the patients. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








