18 January 2023: Database Analysis
Assessment of Hospital Volume in the Surgical Management of Endometrial and Ovarian Cancer: A Polish Population-Based Study
Szymon Piątek1ACEF*, Filip Urbański2BC, Sabina Karczmarz3CE, Artur Prusaczyk13DE, Piotr Sobiczewski1EF, Magdalena Bogdan4E, Mariusz Gujski5EF, Mariusz BidzińskiDOI: 10.12659/MSM.938776
Med Sci Monit 2023; 29:e938776
Abstract
BACKGROUND: Surgery is a cornerstone in management of ovarian and endometrial cancer. The European Society of Gynecological Oncology introduced quality indicators to improve management of these cancers. The optimal annual number of surgeries per unit was established for high-quality surgical treatment.
MATERIAL AND METHODS: The database of the National Health Fund on surgical management of endometrial and ovarian cancer was analyzed. Patients treated between 2017 and 2020 were included. Departments where patients underwent surgery were divided according to number of surgeries performed per year in endometrial cancer: ≥80, 79-50, 49-20, 19-0; and ovarian cancer: ≥100, 99-50, 49-20, 19-0. Optimal number of surgeries per center was defined as at least 100 and 80 surgeries per year in ovarian and endometrial cancer, respectively.
RESULTS: Totally, there were 22 325 surgeries in 316 units and 10 381 surgeries in 251 units due to endometrial and ovarian cancer, respectively. Most surgeries in endometrial cancer (n=15 077; 67.5%) and ovarian cancer (n=9642; 92.88%) were performed in departments that did not meet optimal criteria in number of surgeries. Between 2017 and 2019, an increasing trend in number of surgeries per year in endometrial and ovarian cancer was found. In 2020, there was a decrease in the number of surgeries by 7.8% (n=453) and 8.6% (n=234) in endometrial and ovarian cancer, respectively.
CONCLUSIONS: In Poland, surgical treatment of ovarian and endometrial cancer is decentralized. Most cancer patients underwent surgery in low-volume general gynecologic departments. The COVID-19 pandemic impaired cancer management, leading to a decreased number of surgeries.
Keywords: Endometrial Neoplasms, Ovarian Neoplasms, Quality Indicators, Health Care, Surgery Department, Hospital, Humans, Female, Poland, Pandemics, COVID-19, Hospitals
Background
Endometrial and ovarian cancers are leading in incidence among gynecological malignancies in North America and Europe [1]. In total, in those regions, the estimated number of new cases of endometrial and ovarian cancer in 2020 were 198 453 and 93 323, respectively [1]. Survival improvement remains the main goal of anticancer treatment. Today, targeted therapies are in the spotlight, and numerous studies confirmed their efficacy in clinical practice [2,3]. However, surgery remains the main treatment method in primary endometrial and ovarian cancer.
In Poland, the survival rate in endometrial and ovarian cancer is one of the lowest in Europe [4,5]. The low survival rate in Eastern Europe was noted in the European Society of Gynecological Oncology/European Society Radiation Oncology European Society of Pathology (ESGO/ESTRO/ESP) endometrial cancer guidelines in 2021 [6]. Concin et al suggested that the worse survival compared with that of Western and Northern Europe may result from a more aggressive type of cancer occurring in this part of Europe [6]. However, it also may be caused by more advanced stages, low healthcare expenditure, or a poorly organized healthcare system. Bradley et al found that lower survival in cancer patients is more associated with the lack of access to quality care and not biological differences between tumors [7]. It has been shown that centralization of oncological treatment improves patients’ survival in both ovarian and endometrial cancer [8–10]. In the ESGO quality indicators in endometrial cancer and advanced ovarian cancer, the number of surgical procedures performed per center is a principle indicator [11,12]. In endometrial cancer, the optimal and minimal number of surgeries per year were 80 and 50, respectively [11]; while in ovarian cancer, at least 100 surgeries of advanced cases per year was established as the optimal number [12].
Healthcare in Poland is potentially fully accessible for patients, but ultimately it does not guarantee the availability of healthcare of a standardized quality. Currently, a vast minority of hospitals in Poland have a quality certificate from the Ministry of Health [13]. Among approximately 1200 hospitals, 164 (13.6%) providers are certified.
The aim of this study was to assess how many surgeries in endometrial and ovarian cancer in Poland are performed in accordance with the ESGO qualitative index regarding the number of surgeries.
Material and Methods
DATA SOURCE:
Healthcare in Poland is provided by the National Health Fund (Narodowy Fundusz Zdrowia [NFZ]), which finances health services for all Poles. However, in 2021, 90% of Polish citizens (34 062 250 of 37 907 700) were registered as “insured” in the National Health Fund database [14,15]. Data on the surgical management of 13 types of cancer in every publicly funded hospital are available on the site of the National Health Fund (https://ezdrowie.gov.pl/portal/home/badania-i-dane/zdrowe-dane); instructions on how to access the data are presented step by step in Figure 1. Diagnoses and surgical procedures were recorded according to the International Classification of Disease, Tenth Revision (ICD-10) and International Classification of Disease, Ninth Revision, Clinical Modification (ICD-9-CM), respectively. Among gynecological malignancies, data on endometrial (C54) and ovarian (C56) cancer were available; they included number of cancer patients treated surgically, number of units providing surgical treatment, and duration of hospital stay. Completeness of data is mandatory for healthcare reimbursement.
Analyzed data did not include patients and units outside the system of the National Health Fund. Although the number of commercially treated patients remained unknown, they constituted a small group of patients and omitting them should not affect presented data.
National Cancer Registry collects data on cancer incidence and mortality in Poland. Reporting every new case of cancer to the National Cancer Registry and National Health Fund is mandatory and required by Polish law.
STUDY CONSTRUCTION:
From National Health Fund database, data on patients with endometrial and ovarian cancer treated surgically between 2017 and 2020 were retrieved. The number of patients undergoing surgery was related to the total number of newly diagnosed cases reported by the National Cancer Registry. Among all hospitals registered by the National Health Fund, a distinction was made between cancer centers and university/teaching hospitals. All units were divided according the number of surgeries performed per year. The optimal number of surgeries per center was defined as at least 80 and 100 surgeries per year in endometrial and ovarian cancer, respectively. Those were regarded as high-volume centers. Other (suboptimal) units were divided according to the number of surgeries, as follows, for endometrial cancer: 79-50/year (middle volume), 49-20/year (low volume), and 19-0/year (very low volume); and for ovarian cancer: 99-50/year (middle volume), 49-20/year (low volume), and 19-0/year (very low volume).
This article presents crude numbers and percentages.
Results
ENDOMETRIAL CANCER:
Among 316 units that provided surgical treatment for endometrial cancer, most (86.4%; n=274) were general gynecology departments, while university units and cancer centers constituted 8.2% (n= 26) and 5.4% (n=17), respectively. A total of 10 947 (49%) surgeries for endometrial cancer were performed in general gynecologic departments, while 5693 (25.5%) and 5685 (25.5%) of 22 325 endometrial cancer surgeries were performed in teaching hospitals and cancer centers, respectively. Units that met the ESGO quality indicator in optimal number of surgeries constituted 4.35% (11/253) in 2017, 5.2% (13/249) in 2018, 5.7% (14/245) in 2019, and 4% (10/249) in 2020 (Table 2). Most surgeries (15 077; 67.5%) were performed in departments that did not meet the optimal criteria in number of surgeries, and nearly half of the patients (10 676; 47.8%) were treated in units that did not fulfill the minimum ESGO requirement (low and very low volume). Between 2017 and 2019, 6 of 26 (23%) teaching/university units and 7 of 17 (41.2%) cancer centers met ESGO criteria for the optimal number of surgeries.
OVARIAN CANCER:
A total of 3172 (30.56%) patients with ovarian cancer underwent surgery in cancer centers, 3251 (31.32%) patients in university departments, and 3958 patients (38.13%) in general gynecologic units. Only 839 of 10 381 (8.08%) patients were treated surgically in units with at least 100 surgeries per year, while 9642 (92.88%) patients underwent surgeries in units that met suboptimal criteria regarding the number of surgeries (Table 3). Of those, 2894 (27.88%) ovarian cancer patients underwent surgery in very low-volume units (<20 surgeries per year). Between 2017 and 2019, none of the 26 teaching/university hospitals and only 3 of 17 (17.65%) cancer center units met the criteria for the optimal number of surgeries in ovarian cancer.
Discussion
The survival rates of patients with ovarian and endometrial cancer in Poland were found to be some of the lowest in Europe. Poland had one of the highest age-standardized death rates from ovarian cancer, which reached 6.45%, compared with 5.19% in the European Union and 4.85% in the United States [4]. Between 1990 and 2017, Poland had an increasing trend in endometrial cancer age-standardized mortality rate, with +0.512% (95% CI: 0.333–0.692%) per year [5]. Our results showed that decentralized treatment in units with suboptimal volumes of surgeries may be one of the reasons. Other possible explanations include more advanced staging, prevalence of unfavorable histopathologic and molecular subtypes, and comorbidities. In Poland, no national quality indicators have been developed so far; therefore, we decided to use ESGO quality indicators as a benchmark. The number of surgeries performed in units is an easily measurable indicator, which allows a direct comparison between departments. Numerous gynecologic wards providing surgical treatment facilitates access to healthcare; however, this leads to the dispersion of surgical treatment. Most patients with ovarian (92.88%) and endometrial (67.5%) cancer underwent surgeries in units with suboptimal volume. The optimal number of operations is a cornerstone for high-quality surgical treatment. It also allows appropriate training for doctors during gynecologic oncology fellowship.
The centralization of oncological treatment improves survival with a simultaneous reduction in complications [16]. In Italy, most surgeries for ovarian cancer were performed by general gynecologists, but their oncological results were worse than those of gynecologic oncologists [17]. Recently, similar observations were reported by Jochum et al during the International Gynecologic Cancer Society Congress in New York [18]. An analysis of a French registry, including the 29 879 ovarian cancer patients who underwent surgery between 2013 and 2019, showed that most of them were operated in low-volume hospitals. The volume of the hospitals was an independent risk factor, and the difference in overall survival was 63 versus 53 months between high- and low-volume centers, respectively. They concluded that high-volume centers are expected to improve the prognosis of ovarian cancer; moreover, adequate management of comorbidities and postoperative complications are expected in high-volume centers. Although centralization of treatment can cause barriers related to long travel, improvements in oncological outcome fully justifies the development of high-volume centers [17,19].
The absence of quality control may lead to low system value. Cancer treatment without quality verification can lead to a poor level of care and may contribute to poor outcomes in cancer treatment. Even the implementation of new drugs (immunotherapy, targeted therapies) may not lead to improved survival if surgical treatment remains below the quality criteria. Actually, in Poland, some gynecologic oncology subunits were established within obstetrics and gynecologic departments. The oncological surgeries in endometrial and ovarian cancers were highly valued by the National Health Fund and could be performed without limit. This leads to easy access to oncologic treatment; however, the medical staff were not prepared for cancer management. Doctors had to share time between oncologic and obstetric care. Even specialists in gynecologic oncology had obstetrical duties in these departments. Finally, upgrading oncologic surgical skills was not obligatory.
Experienced and well-educated healthcare professionals are of key importance in cancer management but are insufficient to ensure high-quality care. Readiness to implement pro-quality changes is not only the issue of obstetricians and gynecologists and gynecologic oncologists, but also of decision makers, including the National Health Fund. Recently, the COVID-19 pandemic and the migration crisis related to the military conflict in Ukraine showed that healthcare flexibility in Poland is high and the implementation of quick changes is possible.
Treatment in suboptimal volume centers cannot be synonymous with suboptimal surgery. Some units had a significant number of surgeries, but they did not exceed the thresholds established by the ESGO. The cut-off levels for the optimal number of operations were set arbitrarily by ESGO experts. The lack of a methodology on how the number of optimal number of surgeries was determined is a burden for the ESGO qualitative indicators.
The COVID-19 pandemic had a negative impact on healthcare system worldwide, including limited access to healthcare professionals. It resulted in the reduction in the number of surgeries in 2020. Although the Polish data on the number of new cases in 2020 are not yet published, a reduced number of new cases can be expected. However, this will not reflect a decreasing incidence trend. It might be expected that the pandemic impaired survival rates in cancer patients. However, paradoxically, there may be an improvement in survival, because some advanced patients may have died without a diagnosis of cancer due to limited access to healthcare. This trend may be more pronounced in countries with a high number of excess deaths, such as Poland, where 60 687 excess deaths were recorded [20].
A limitation of our study is the lack of clinical data. Complications after surgery and readmissions were not compared between units. Finally, survival data were not available for these patients. Therefore, it cannot be concluded that prognosis is related to surgical volume of the department.
Conclusions
In Poland, surgical treatment of ovarian and endometrial cancer is decentralized. Most patients with cancer undergo surgery in low-volume general gynecologic departments. The decentralization of surgical treatment may have arisen from the easier access to surgery, shorter waiting time for surgery, or proximity to the place of residence. However, the extent of surgery in low-volume hospitals may be naturally limited due to the lack of intensive care units and the avoidance of potential complications. It may have negative consequences, especially in patients with ovarian cancer, in which optimal debulking is the key factor of potential success.
Tables
Table 1. New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23].![New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23].](https://jours.isi-science.com/imageXml.php?i=t1-medscimonit-29-e938776.jpg&idArt=938776&w=1000) Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020.
Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020.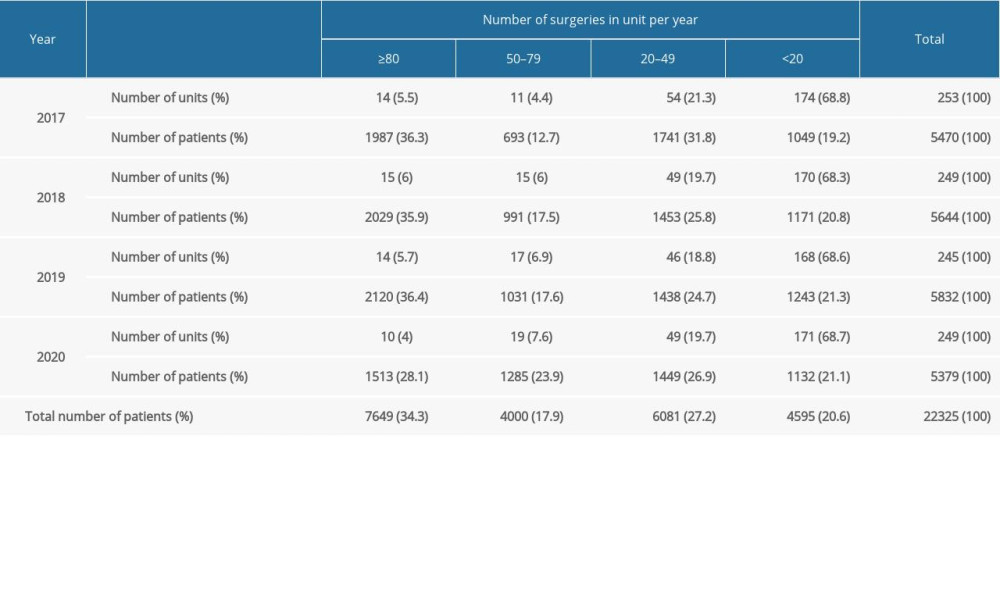 Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020.
Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020.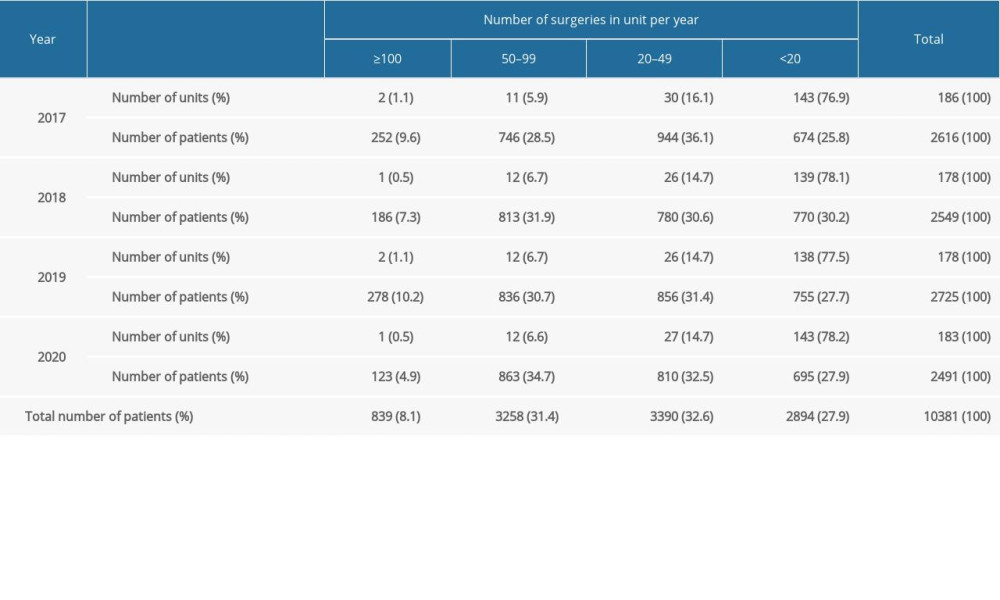 Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis.
Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis.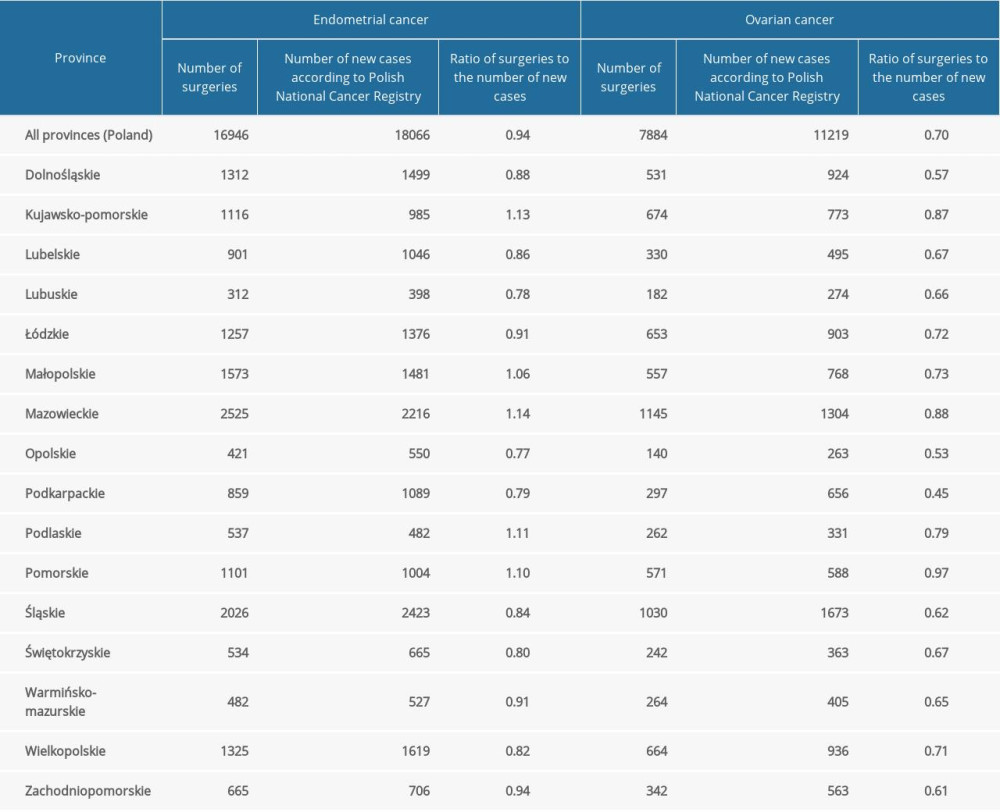
References
1. Ferlay J, Colombet M, Bray F: Cancer incidence in five continents, CI5plus: IARC CancerBase No. 9 [Internet], Lyon, France, International Agency for Research on Cancer Available from: https://gco.iarc.fr/today/online-analysis-table
2. Musacchio L, Boccia SM, Caruso G, Immune checkpoint inhibitors: A promising choice for endometrial cancer patients?: J Clin Med, 2020; 9(6); 1721
3. Washington CR, Moore KN, PARP inhibitors in the treatment of ovarian cancer: A review: Curr Opin Obstet Gynecol, 2021; 33(1); 1-6
4. Malvezzi M, Carioli G, Rodriguez T, Global trends and predictions in ovarian cancer mortality: Ann Oncol, 2016; 27(11); 2017-25
5. Zhang S, Gong T-T, Liu F-H, Global, regional, and national burden of endometrial cancer, 1990–2017: Results from the global burden of disease study, 2017: Front Oncol, 2019; 9; 1440
6. Concin N, Matias-Guiu X, Vergote I, ESGO/ESTRO/ESP guidelines for the management of patients with endometrial carcinoma: Radiother Oncol, 2021; 154; 327-53
7. Bradley CJ, Given CW, Roberts C, Disparities in cancer diagnosis and survival: Cancer, 2001; 91(1); 178-88
8. Woo YL, Kyrgiou M, Bryant A, Centralisation of services for gynaecological cancers – a Cochrane systematic review: Gynecol Oncol, 2012; 126(2); 286-90
9. Eggink FA, Vermue MC, Van der Spek C, The impact of centralization of services on treatment delay in ovarian cancer: A study on process quality: Int J Qual Health Care, 2017; 29(6); 810-16
10. Christie J, Centralized, specialist care for gynecologic cancer patients: Cancer Nurs, 2016; 39(1); 82-83
11. Concin N, Planchamp F, Abu-Rustum NR, European Society of Gynaecological Oncology quality indicators for the surgical treatment of endometrial carcinoma: Int J Gynecol Cancer, 2021; 31(12); 1508-29
12. Fotopoulou C, Concin N, Planchamp F, Quality indicators for advanced ovarian cancer surgery from the European Society of Gynaecological Oncology (ESGO): 2020 update: Int J Gynecol Cancer, 2020; 30(4); 436-40
13. Data of Polish Ministry of Health, List of hospitals with accreditation: Status on 2022-09-30 Available on line: https://dane.gov.pl/pl/dataset/2699
14. , National Health Fund activity report for the third quarter of 2021: Sprawozdanie z działalności Narodowego Funduszu Zdrowia za III kwartał 2021 roku, zal._do_uchwaly_nr_37._czesc_opisowa https://www.nfz.gov.pl/zarzadzenia-prezesa/uchwaly-rady-nfz/uchwala-nr-372021iv,6586.html
15. Cierniak-Piotrowska M, Dąbrowska A, Stelmach K: Population. Size and structure and vital statistics in Poland by territorial division in 2021 Available on line: https://stat.gov.pl/en/topics/population/population/population-size-and-structure-and-vital-statistics-in-poland-by-territorial-division-in-2021-as-of-31-december,3,31.html
16. Birkmeyer JD, Sun Y, Wong SL, Stukel TA, Hospital volume and late survival after cancer surgery: Ann Surg, 2007; 245(5); 777-83
17. Mandato VD, Torricelli F, Uccella S, An Italian National Survey on Ovarian Cancer Treatment at first diagnosis. There’s none so deaf as those who will not hear: J Cancer, 2021; 12(15); 4443-54
18. Jochum F, Hamy A-S, Laas E, Impact of comorbidities, postoperative complications and center volume on overall survival in real life cohort of 29879 patients
19. Stitzenberg KB, Sigurdson ER, Egleston BL, Centralization of cancer surgery: Implications for patient access to optimal care: J Clin Oncol, 2009; 27(28); 4671-78
20. World Health Organization: Global excess deaths associated with COVID-19 Available from: https://www.who.int/data/sets/global-excess-deaths-associated-with-covid-19-modelled-estimates
21. Didkowska J, Wojciechowska U, Czaderny K: Cancer in Poland 2017, 2019, Warsaw
22. Wojciechowska U, Didkowska J, Michałek I: Cancer in Poland 2018, 2020, Warsaw
23. Didkowska J, Wojciechowska U, Olasek P: Cancer in Poland 2019, 2021, Warsaw
Tables
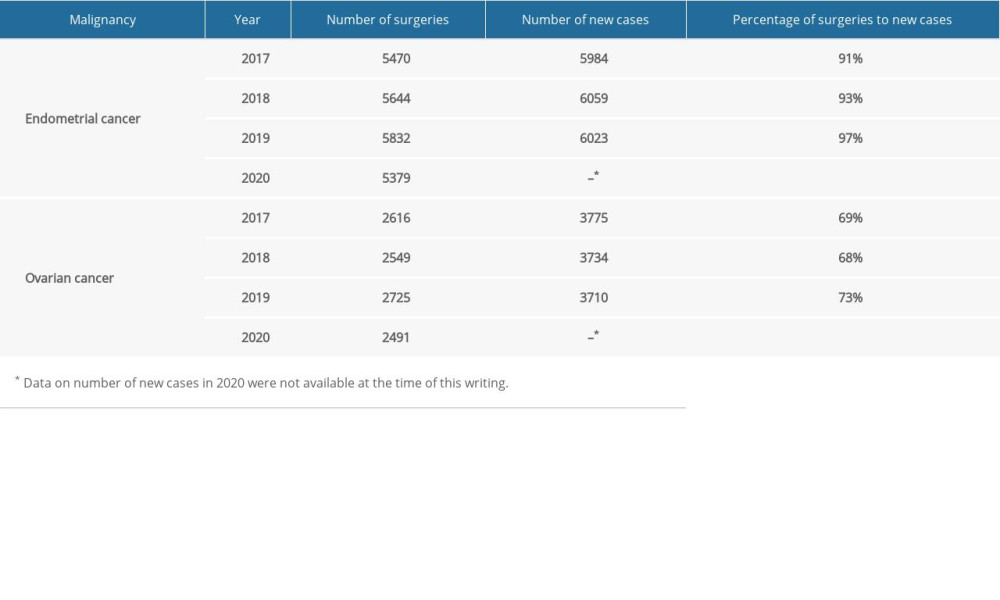 Table 1. New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23].
Table 1. New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23]. Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020.
Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020. Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020.
Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020. Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis.
Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis. Table 1. New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23].
Table 1. New cases and surgeries for endometrial and ovarian cancer. The number of new cases was retrieved from annual reports “Cancer in Poland” [21–23]. Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020.
Table 2. Surgical treatment of endometrial cancer in Poland from 2017 to 2020. Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020.
Table 3. Surgical treatment of ovarian cancer in Poland from 2017 to 2020. Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis.
Table 4. Ratio of number of surgeries and number of new cases in Poland between 2017 and 2019: an inter-region analysis. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387









