30 June 2023: Lab/In Vitro Research
Comparison of Composite Resin (Duo-Shade) Shade Guide with Vita Ceramic Shades Before and After Chemical and Autoclave Sterilization
Shekhar GuptaDOI: 10.12659/MSM.940949
Med Sci Monit 2023; 29:e940949
Abstract
BACKGROUND: This study aimed to compare a composite resin (Duo-Shade) shade guide with Vita ceramic shades before/after chemical and autoclave sterilization.
MATERIAL AND METHODS: Color values (L*a*b*) were recorded directly from shade tabs of prefabricated composite resin (Brilliant NG Universal Duo-Shade) and ceramic (Vita classic) shade guide with a calibrated spectrophotometer (Vita Easy Shade Advance 4.0). Seventy-two composite resin disk samples with 6 different shades (A1/B1, A2/B2, A3/D3, A3.5/B3, A4/C4, and C2/C3) (n=12 each) were divided into 2 groups (Gp) – Gp A (Autoclave) and Gp C (Chemical) (15 cycles) – to assess their influence on respective shades. Mean values calculated the color differences (ΔE) while differences in color values (L*a*b*) were graded on the National Bureau of Standards (NBS) 6-grade scale and assessed for Clinical Acceptance/Perceptible Threshold (CAT), (CPT). All differences were considered significant if the color difference ΔE was ≥3.3.
RESULTS: Only 2 out of 12 Shade tabs (C2C3, A4C4) of composite resin matched to Vita shade tab C2 and C4 (ΔE ≤3.3). Both groups showed notable color differences after respective sterilization protocols, with color differences in Gp A significantly higher than Gp C (DE ³3.3). Within groups, all shades in Gp A showed remarkably different color changes, with shade C2C3 and A1B1 being denoted as clinically unacceptable.
CONCLUSIONS: Manufacturer-provided shade guides do not match ceramic shades as claimed and chemical sterilization using 10% Deconex was associated with less color changes than with autoclave sterilization.
Keywords: Ceramics, Color, Composite Resins, nanocomposites, Sterilization
Background
Specific skills to apply the knowledge of dental material sciences into clinical application ensures successful, long lasting, and comprehensive esthetic treatment results. The ban on dental amalgam in many Scandinavian countries [1] increased the demand for tooth-colored restorative resins which had revolutionary advances in resin particle sizes (Nano), filler size/type, loading, and clinical techniques [2]. Despite the availability of a vast commercial product range of composite resin with improved optical properties (color, translucency, opalescence, fluorescence) and improved mechanical properties [3], dentist dissatisfaction with composite shades from provided (prefabricated) composite shade guides (CSG) has also been widely reported [4]. Shade discrepancies are especially common between completed restoration shade (polymerized) and the reciprocal shade on the shade tab after finishing/polishing. Shade matching not only involves an understanding of color science and surface characteristics, but more importantly one must understand the limitations of the human eye and the restorative materials used. Polychromatic tooth structure, difficulty of the human eye to match shades, the effect of the background, and the light under which a shade is observed add to the complexity of shade matching. The color of a completed composite restoration has been reported to be influenced by a wide range of extrinsic and intrinsic factors. Factors affecting shade matching that are likely to be neglected in clinical practice include geometric attributes (gloss, haze, contrast ratio) [5], surface finish/polish [6], background color base (transmitted/reflected/opaque/artificial) [7], method of selecting shade (accurate versus inaccurate) [8], shade guide representing tooth colors accurately, and consistent designations of shades within/between various composite brands [9]. Shade mismatch between the composite brand and its supplied CSG led to the development of new clinical techniques (e.g., incremental layering technique, interposing glycerin gel between enamel and dentin) [10,11] and distributed enamel and dentin composite shades/shade guide tabs [12]. The present dental composite global market ($24.7 million USD) is predicted to double ($59 million USD) by the year 2031 [13], and a bigger diversity in different composite products and their respective shade guides has already been created, which has led to confusion among practicing dentists [14,15]. These authors have concluded that the manufacturer’s shade guides lack total shade representation of natural teeth, which is based on the view that each tooth has a wider shade distribution within different layers (enamel, dentin and restorations). The discrepancy between composite restorations and their respective CSG was also linked to shade guides being made of different material and thickness than the marketed composite [16]. With patients returning to replace the restorations, citing shade discrepancy as a main reason, many authors concurred, preparing and using a customized CSG from the same composite material [17]. Advantage of individually fabricated shade guides of composite resin restoration includes the shade guide being of the same material (lot, brand, specification, manufacturing date, storage), and the possibility to create more clinical shade options by varying different characteristics (thickness, surface structure, glaze) [18,19]. The drawbacks of such an approach included material wastage, time consumption, and durability of shades in terms of routine and regular disinfection of customized shade tabs. Composite restoration kits that provide respective CSG and those clinicians who have improvised to customize their own shade guides represent just a small percentage of this problem.
The large majority of the composite manufacturers do not supply any CSG, but instead rely on using the Vita (classical) shade guide as a standard for instilling various shades within the commercial product [20]. The communication between the manufacturers and the clinicians for composite shades is dependent upon trust in the Vita ceramic guide system, despite the fact that Vita shade guides are made of dental porcelain with different optical properties than composite. However, the durability of the vita classical shade guide standard can be gauged by the fact that there have been few changes (mostly in arrangement and increased number of vita shades, from the previous 16 shades to the current 26 plus 3 bleach shades in the Vita 3D master shade guide) in the Vitapan classical during the last 50 years [21]. The Vita classical shade guide was introduced in the year 1927 (Vita Zahnfabrik in Bad Sackingen, Germany) and continues to be the most globally accepted and used shade guide, mainly because of its reliability to match natural tooth colors and their varied shades [7,9]. Clinical determination of color/shade selection has been traditionally visual, which although being subjective in nature has been considered precise, especially with experienced clinicians [20]. A major concern with composite manufacturers has been the lack of a standard resin composite shade nomenclature in the literature [22]. As a result, the current picture of CSG is that they do not match the restorations they represent [20]. Various tactical claims by manufacturers in that their composite/acrylic resin color corresponds to ceramic color standards [23] have been found to be dissimilar to Vita shades [18,24]. To meet the demands of clinicians and patients, many brands (eg, Inspiro, Miris2) have developed prefabricated anatomic laminate shade guide/tabs (dual-shade) that present an underlying dentin with an overlying layer of the corresponding enamel. A composite resin dual-shade guide has an enamel layer that overlies the layer of dentin, with both having different shades, thus mimicking the natural tooth. While this new approach allows direct visual comparison with enamel or dentine, the operator still has to decide what thickness of each layer will be appropriate to obtain the desired shade. With advances in sensitive color-measuring instruments like colorimeters/spectrophotometers and rigorous standards in visual acceptable threshold (VAT) and visual perceptible threshold (VPT) [25], clear guidelines [National Bureau of Standards (NBS) unit for critical remarks of color differences] [22,26] have been established that determine a composite shade to be clinically acceptable or not.
In the last 23 years, since the turn of the century, there have been more than 60 epidemics reported, with COVID-19 being the biggest and the deadliest [27]. Infection control has now become a serious and a major criterion of patient and personal safety. A large number of varied microorganisms inhabit the oral cavity, many of which are potentially lethal and can spread rapidly through contact. Periodontal bleeding can occur on touch from a probe, thus exposing blood, while saliva harbors a wide variety of bacteria and viruses. To minimize cross-infection while treating dental disease, strict infection control is mandatory, which usually achieved by sterilization or disinfection. Autoclaving is considered the standard for achieving complete sterilization of dental instruments, while many other instruments and materials cannot be autoclaved and therefore rely on surface disinfection with chemical sterilizers (phenols, iodophors, and chlorine containing compounds). All shade guides have been keyed as a non-critical instrument [28] in guidelines with infection control, but because they come in contact with the patient’s skin/mucosa, they are considered contaminated. In addition to the above-mentioned likely neglected factors that affect shade selection in composites, routine clinical use of CSG tabs (prefabricated or custom made) causes color changes after certain cycles of sterilization or disinfection. For any shade-selection procedure, it is mandatory to keep the shade tab under the patient’s lips and close to the natural teeth so as to determine the shade difference. Since each shade tab has to be put into the oral cavity, sterilization of the shade guide is mandatory. Sterilization procedures (chemical and autoclave) may be one of the main reasons for altered shades of CSG, which eventually cause shade mismatch, since the CSG does not represent the shade that it actually should; which may also spare the manufacturers from being criticized for not providing correct shades. A recently introduced second-generation nanocomposite resin system [Brilliant™ NG Universal Duo-Shade (Coltene Altstättan, Switzerland)] has introduced a new Duo-Shade system that claims to obtain 2 different vita shades from a single syringe (after 24 h of curing). The manufacturer provides 6 syringes (tones) (A1/B1, A2/B2, A3/D3, A3.5/B3, A4/C4, and C2/C3 for enamel and dentin each) that claim to cover an overall 12 different vita shades in the Vita classical shade guide system. The manufacturer provides 2 different prefabricated shade guides [shade A1/B1, A2/B2, A3/D3 having 8 tabs and shade A3.5/B3, A4/C4 and C2/C3 (enamel/dentin) having 6 shade tabs]. This approach of 2 shades within a single syringe and 2 different shade guides is novel and may overcome the drawbacks of the layering technique. This study intends to investigate whether the individual shade tabs of this composite resin system correspond to their respective vita classical shade tabs and whether the shades were compatible with the infection control measures (chemical and autoclave) the manufacturer recommends. We hypothesized that being 2 different materials (ceramic and plastic), the CRS will not correspond to that of vita classical shade guide and that both sterilization protocols will alter the shade over time. Alternately, the null hypothesis would state that there should be no differences between the composite and corresponding vita shade guide tabs, and that 15 cycles of the 2 sterilization methods would not change the color of the shade tabs. Therefore, this study aimed to compare dual-shade composite resin shade guides with vita ceramic shades following chemical sterilization and autoclave sterilization.
Material and Methods
ETHICS:
Academic practices and policies of the college and the affiliated university require all research projects have to be approved by the concerned ethics authority before commencing. Therefore, this study was duly approved by the Ethics Committee of the College of Dentistry at the Jazan University under Ethics Committee reference number CODJU – 2214F.
STUDY DESIGN:
This in vitro study used an experimental comparative approach, which was conducted during the first quarter of the year 2023. The study was designed in 2 different sample/measure stages. The first sample measure involved a direct comparison of shade guide tabs, while the second sample measure required preparation of testing samples according to specifications followed by intervention in the form of 2 different sterilization protocols followed by measuring the color differences.
OPERATIONAL DEFINITIONS:
“Shade” was operationally defined for this research project as a term that describes a particular hue or variation of the primary hue, such as a bluish shade of green color. “Shade guide” is a term that will define a set of simulated teeth (prefabricated or custom made) used to select a particular shade for a restoration. “Shade tab or tab” is a term that describes a material strip that is attached to or projecting from a holder and is used for identification and to provide information about the color of the product. A shade guide may have multiple tabs categorized according to shades, brightness, or hue.
SAMPLE PREPARATION, SELECTION, AND GROUPING:
Calculated sample size for both measures was based on a power analysis [power of 0.8 at a significance level of 0.05 (β=0.2)] [29]. The sample size for both measures was decided accordingly to be 6 samples for each shade tab irrespective of the number of shades present in a shade guide.
SAMPLE/MEASURE 1 (COLOR DIFFERENCES BETWEEN CSG AND VITA SHADE GUIDES):
The 2 shade guides used for comparison of color differences were that for a direct composite (Brilliant™ NG Universal Duo-shade, Coltene Altstättan, Switzerland) against the standard vita classical (VITA Zahnfabrik H. Rauter GmbH, Germany) shade guide (specifications and features in Table 1). The composite kit had 2 shade guides (shade A1/B1, A2/B2, A3/D3 having 8 tabs and shade A3.5/B3, A4/C4, and C2/C3 having 6 shade tabs). For vita classical shade guide, 2 tabs from 6 different shade guides (less than 1 year of exclusive research usages) that would correspond to the respective shade tabs of CSG (A1, A2, A3, A3.5, A4, B1, B2, B3, C2, C3, C4, D3) were collected for comparison. All vita shade guides/tabs were cleaned and sterilized by chemical disinfection as per the manufacturer’s recommendations.
SAMPLE/MEASURE 2 (COLOR DIFFERENCES AFTER STERILIZATION PROTOCOL/15 CYCLES):
The specimens for the experimental procedure were made up of the material direct composite restoration kit (Table 1). A hollow cylindrical mold (polytetrafluoroethylene) (10 mm outer and 8 mm inner diameter) with vertical height of 4 mm was used to standardize the samples. The thickness of the specimens was based on the thickness of standard thickness of vita shade guide tabs (3.5 to 4 mm). A clear glass plate was used on one side to standardize the base or the non-testing surface [30]. For each specimen the respective cartridge of the composite kit was packed into the mold using a gold-plated composite packing instrument followed by covering the top surface (testing) with a Mylar strip over which a glass plate was placed. Excess material at the top was extruded by placing a weight of 1 kg for 30 s. The glass plate on either side allowed light curing to be done for each increment both from above and from bottom. Light curing was accomplished by a light curing unit (Dentsply QHL 75 Model No 503; SN. 503-20865; Dentsply Caulk Milford USA) (intensity setting of 400 mW/cm2) for 30 s (Dentin/enamel A1/B1, A2/B2, A3/D3) and 40 s (Brilliant NG Dentin/enamel A3.5/B3, C2/C3, A4/C4) depending upon the shades, as recommended by the manufacturer. A radiometer was used to verify the output of the curing unit. The head of the light curing unit was kept at a standard distance of 1 mm away from the glass slide, with standardization achieved by a rubber stopper (1 mm) attached to the surface of glass slides. Once samples were cured, they were removed from their respective molds. Finishing of each specimen was carried out as per manufacturer’s recommendations, which was a 3-stage procedure: coarse finishing, followed by fine finishing (40 μm and 15 μm diamond), and finally polishing (Diatech Composite polisher). A standard speed of 5000 to 15 000 rpm was followed as per recommendations. Each specimen was marked with a notch on the sides of the bottom surface. The samples were then stored at room temperature in light-proof containers for 24 h before testing for color parameters.
GROUP DISTRIBUTION:
A total of 72 samples (Sample/Measure 2) (4 mm thick composite resin disks) fabricated from 6 different shade tones (A1/B1, A2/B2, A3/D3, A3.5/B3, A4/C4 and C2/C3) with each tone represented by 12 samples each, were divided into 2 experimental groups (Gp) – Gp A (autoclave) and Gp C (chemical) – based on the sterilization protocol. After recording the baseline color values (CIE L*a*b*), the specimens in both groups were subjected to their respective cycles of sterilization. For specimens in Gp A, a steam autoclave (Tuttnauer Model T-Max-10; SN-14060015) at the manufacturer’s recommended temperature (132°C/270°F), pressure (313 KPa) and time (27 min) followed by drying was performed for each cycle (15 cycles) with a gap of 24 h. For specimens in GP C, the resin disks were liberally sprayed with Deconex solution (lot: 128745, Borer Chemie, Switzerland), followed by wrapping in an airtight container for 3 min. Handling of materials followed strict adherence to infection control measures and manufacturer’s recommendations.
MEASURES, DATA COLLECTION, EVALUATION, AND ANALYSIS:
Color value measurements were standardized by measuring with a spectrophotometer (SPM) (Vita Easy Shade Advance 4.0, Model Number: DEASYAS4, VITA Zahnfabrik H. Rauter GmbH & Co. Germany). To minimize variations due to changing positions of SPM, an index (silicone) that had an opening which corresponded to SPM tip diameter was used for both samples/measures (1 and 2). All shade tabs/specimens were centered using gradations so that the middle portion of the shade tab/specimen would be in line with the SPM tip. To minimize the effect of external light/illuminant and background, all measurements were made in a calibration box (0 calibration standard) that provided a white background. Before measuring color of shade tabs/specimens on each day (baseline and 15 cycles), the SPM was calibrated with its supplied tool and instructions. Each color measured was expressed in values according to the CIELAB parameters (L*, a* and b*) where L* is lightness/darkness (100/0: completely white/completely black), a* (red-green) and b* is yellow-blue chromatic coordinates. Values for coordinates a* and b* can be either positive (+) or negative (−), with positive values representing the color more towards red (a*) or yellow (b*) shade and a negative value indicating more towards green (a*) or blue (b*) [a*=green (−a), and red (+a) axis, and b*=blue (−b), and yellow (+b) axis] [31]. For both samples (1 and 2), an average was calculated from 3 measurements for each coordinate.
STATISTICAL ANALYSIS:
For sample 1 (prefabricated composite shade guide corresponding to vita classical shade guide), mean (average) values and standard deviations were obtained for each shade tab in both shade guides (3 independent measurements) of CIELAB values (L*, a*, b*). The differences of each value for each corresponding shade guide were expressed as delta E (ΔE), which was calculated according to the equation [31,32]:
Where L1, a1, and b1 represent color values of one shade and L2, a2 and b2 that of the other shade guide tab [11]. For measure 2 (differences between Gp A and Gp C), the differences for each CIELAB color value (L*, a* and b*) were calculated in terms of differences between baseline and the value of the color values obtained on the particular cycle (day 1, day 2…. Day 15). Each difference in color value (ΔL*, Δa*, Δb*) was obtained from corresponding differences (L*1–L*2, a1*-a2*, b1*-b2*), which were the differences between time periods (day 1 and day 2) [7,8,11]. The overall difference in color ΔE was then calculated using the equation mentioned above. This delta E* represented the magnitude of color difference between each specimen without indicating the direction towards which the color differed. Various levels of differences for each color coordinate (ΔL*, Δa*, Δb*) were denoted using National Bureau of Standards (NBS) unit for critical remarks of color differences [(0.0 to 0.5 – almost the same); 0.5 to 1.5 – slightly different; 1.5 to 3.0 – perceivably different; 3.0 to 6.0 – remarkably different; 6.0 to 12.0 – extremely marked different; ≥12.0 – different color)] [26,31]. For verifying the clinical significance of obtained magnitude of color differences (ΔE) on the clinical acceptability/perceptibility threshold (CAT/CPT), a value of ΔE less than 1 was considered as not appreciable, between 1 and 3.3 or less as appreciable by skilled operators only and therefore clinically acceptable, while more than 3.3 could be appreciated by anyone (layman) and therefore was clinically unacceptable [32].
Results
SAMPLE/MEASURE 1 (COLOR DIFFERENCES BETWEEN CSG AND VITA SHADE GUIDES):
The mean values with standard deviations of measured color (L*, a* and b*) for 6 different shades of CSG as marketed by the manufacturer and the corresponding color coordinate values for each individual corresponding shade (A1, A2, A3, A3.5, A4, B1, B2, B3, C2, C3, C4, D3) tab of the vita classical shade guide are shown in Table 2. The color coordinate L* which represents the value (brightness/darkness) was found to be highest in shade A1B1 for CSG (M=74.10±1.39), which was lower than the corresponding A1 (M=79.53±2.29) and B1 (M=79.42±1.29) on the vita shade guide. For coordinate L*, shade C2 (M=70.10±2.59) and C4 (M=64.91±1.71), used in CSG tab C2C3 and A4C4, were the only 2 shades whose mean values corresponded to the vita shade values [VC2 (M=70.67±1.57) and VC4 (M=64.06±1.29)] (Table 2). For color coordinate a* (red–green) and b* (blue–yellow), the values between the 2 shade guides corresponded, although the direction in CSG shade tabs did not match that of vita shades. The values for color coordinates a* indicate that the composite shade tabs A2B2 (M=1.10±0.35), A3D3 (M=−0.25±0.09) and A3.5B3 (M=1.49±0.78) were more towards red. For color coordinate b*, CSG shades A1B1, A2B2, A3D3, and A3.5B3 were more towards yellow than the corresponding vita guide. Composite shade A3.5B3 demonstrated highest values for color coordinate b* (+) (M=35.10±2.41). The magnitude of color differences as expressed in the NBS standard units demonstrated that color values of shade C2C3 and A4C4 matched closely to the corresponding vita shades (C2, C3 and C4) with slight differences from vita A4. On the NBS unit scale for color differences, the values for CSG C2C3 (ΔE=0.47 with vita C2) and A4C4 (ΔE=0.36 with vita A4) were only found to be less (ΔE=0.5), which denotes the shades to be same. At the same time, these 2 composite shades (C2C3 and A4B4) were found to be perceivably different (ΔE=1.5 to 3.0) on the NBS unit scale for vita shade A4 and C3. The remaining composite shade guide tabs (A1/B1, A2/B2, A3/D3, A3.5/B3) with values for ΔE ranging between 3 to 6 (NBS units) were denoted as remarkably different from the corresponding vita shades. On the clinical acceptance/perceptible threshold composite shades, A1/B1, A2/B2, A3/D3, A3.5/B3 had color difference score (ΔE ≥3.3) with their corresponding vita shades and were denoted to be appreciable by anyone (layman), which is considered clinically unacceptable, while composite shade C2C3 and A4C4 had color difference values (ΔE ≤0.5) against corresponding vita shades C2 and C4, which denotes similar shade or no color difference on the scale. The color difference (ΔE) of these 2 shades with corresponding vita shade C3 and A4 was denoted clinically acceptable since the differences can be perceived only by skilled operators (ΔE=1.0 to 3.3).
SAMPLE/MEASURE 2 (COLOR DIFFERENCES AFTER STERILIZATION PROTOCOL/15 CYCLES):
The ability of composite shade tabs to maintain their original shades after 15 cycles of autoclaving and chemical sterilization is presented in Table 3. Overall results indicate that composite resin samples in Gp C showed less changes in the magnitude of color differences (ΔE ≤3.3) than the samples in Gp A. All shades in Gp A (within the group) demonstrated a significant change in color values (L*, a*, b*) immediately after the first cycle of autoclaving, with highest changes being observed in shade C2C3 (ΔE=1.84) on the first cycle (Figure 1). The shade samples that had the least changes at the first day were in Gp C [C2C3 (ΔE=0.23)] (Figure 2). On the NBS unit scale for color differences, shade A3D3 in GpC denoted perceivably different color changes (ΔE=1.5 to 3.0) between the 3rd and 12th cycles of chemical sterilization, which later increased to remarkably different (ΔE=3.0 to 6.0) between 13th and 15th cycle (Table 3, Figure 2). On the contrary, all shade samples in Gp A were denoted to have remarkably different shades (ΔE=3.0 to 6.0) in early autoclave cycles, with shade C2C3 showing such a change at the first cycle of autoclave sterilization. On the CAT/CPT scale for color difference, the shade tab A1B1 and C2C3 showed color difference values that were clinically unacceptable (ΔE ≥3.3) (Figure 1).
Discussion
COLOR DIFFERENCES BETWEEN COMPOSITE AND VITA SHADE GUIDES:
A dental shade is basically a set of shade standards that is used to identify the closest possible shade of the tooth to be replaced/restored. One of the primary requirements of an ideal shade guide is to have and represent the full natural color spectrum of human dentition, which also must be logically arranged in an ordered way in 1 or more attributes (value, chroma, hue) or coordinates of color (L*, a*, b*) [19]. The shades in the composite kit used in this study have been blended in a proportion that is not revealed by the manufacturer. Both shades have been supplied in a single syringe with no barrier separating them within the cartridge, which means that the 2 corresponding vita-shaded composites are mixed as a single dispensable composite, as opposed to the layered concept in which enamel and dentin are supplied separately. The vita classical shade guide has 4 groups (A, B, C, D) with each group having 4 subdivision (1,2,3,4) shade tabs, thus making a total of 16 shades. Each of the groups in the vita shade guide are assigned according to the dominant hue, and each subdivision (1,2,3,4) demonstrates a logical increase in the chroma with subsequent reduction of the value [35]. Such logical distribution is not present with the CSG used in this study, although it provides 2 different shade guides that are based on 6 shades. Three shades have been assigned to each shade guide with a number of shade tabs (8 and 6) different between shade guides 1 and 2, respectively.
The results obtained for different color coordinates (L*, a*, b*) for the vita shades fall in the range of values reported in earlier studies [20,21,32], thus adding to the reliability and validity of the vitapan classic shade guide color spectrum using a spectrophotometer. When precombined shades of the composite shade guide were compared with individual shade tabs of the vita classical shade guide, the color differences (ΔE) in shade C2C3 and A4C4 were found to closely match with vita C2 and C4 shades. Since the shades are combined in the composite shade guide, it cannot be established whether the matching effect was due to C2, C3, A4, or C4 component of composite resin. In total, 12 shades of composite were matched with 12 shades of vita classic, out of which only 2 shades match (16%). Paravina et al reported finding only 4.2% of shades were clinical acceptability [36]. However, in their study there were 6 different types of composite resins studied, which explains the difference in observed results. The results of the present study show that the mean values for color coordinate L* in the composite resin shade guide (L*range 64 to 74) were lower than the corresponding vita shades (L*64 to 79) except for individual shades C2 and C4. Similar differences in color coordinate were also reported in studies by Swift et al [37] and Ikeda et al [38]. The reduction in value (brightness) can be explained by the inherent optical properties of the components between resin and ceramics [20]. The use of nano-filler particles (size range 8000 to 30 000 nanometers) create a mismatch in refractive index between the resin matrix and filler, with filler particles scattering the light, creating a reduction of brightness and translucency [20,39]. Although the bis-GMA resin matrix has a similar refractive index to that of the silica filler, the addition of TEGDMA increases this refractive index of resin [40,41]. All combinations used in the composite resin system are of 2 different hues (b*) of the vita ceramic shade guide (A=red and brown, B=red and yellow, C=grey, D=red and grey). Since vita shades A, B, and D contains 2 different hues, the combination of A1B1 in the composite shade guide reflects a mix of 4 different hues, which also explains the matching of color coordinates for composite shade containing vita C shade. Since the vita C shade contains a single hue (grey), the combination with another shade will cause less changes in value, which are reflected by less L* changes in composite shade tabs C2C3 and A4C4. Analysis of color coordinate a* and b* shows that the values in only 2 composite shade tabs (A1B1, A3D3) were negative b (more towards the green axis), while 6 out of 12 corresponding vita shades have b* values towards red (+). Shades which were clinically denoted as unacceptable (clinical acceptance/perceptible threshold) showed greater variations in values of a* and b*. The decrease in b* values has also been attributed to the basic photoinitiator contained in visible light cure resins, which is camphorquinone [42]. This photoinitiator also controls the yellowness of the composite and, when activated (blue light), there are changes in b* (decrease) level, while the camphorquinone becomes invisible [43]. In conclusion, our results agree with the reports of Paravina et al and Wee et al, showing that restorative composite resin manufacturers declare that their composite resin shades are similar to vita shades (classical) without these shades necessarily correlating to them [18,24].
Clinical observations in the past have also concluded that value, chroma, and hue of various esthetic composites do not clinically match keyed vita shades [44]. Whether manufacturers prepare their shade guides from the same composite or use different shades has also been a subject of contention [45]. Earlier studies have reported that the materials for the composite shade guides are different [46] while others have reported they are prepared from the same composite resin [47]. One of the composite resin manufacturers (Tokuyama, Japan) supplies prefabricated molds with the kit so that clinicians are able to fabricate custom shade guides for the kit [11].
COLOR DIFFERENCES AFTER STERILIZATION PROTOCOL/15 CYCLES:
Manufacturers for all CSG recommend both chemical sterilization and autoclaving, although detailed instructions regarding the frequency are usually absent. It has been reported that most shade guides are disinfected without following the manufacturer’s instructions [48]. The results from our study show that both measures of infection control (chemical and autoclave) caused significant color differences for all coordinates (L*, a*, b*), with a color difference (ΔE) most evident when autoclaving was used. Our results are applicable to the fact that the manufacturers make composite shade guides from the same composite kit, which is why this study fabricated specimens accordingly. Two composite resin shades in Gp A (A1B1, C2C3) at the end of 15 autoclave cycles had color differences (ΔE ≥3.3) denoted as clinically unacceptable since these differences could be appreciated by anyone. For shade A1B1, the higher color differences were observed at the 12th autoclave cycle, while the color differences in shade C2C3 were observed after just 2 autoclave cycles. All other shades in Gp A at the end of 15 cycles also had color differences (ΔE ≥1.0 to 3.3), which could be only appreciated by skilled operators. Generally, in an autoclave there are 3 phases (heating, exposure, and cooling) which involve rapid temperature changes. This brings about expansion and contraction of the composite resin depending upon its linear thermal expansion coefficient (LTEC) [49]. Within the composite body, the resin matrix and the filler have discrepancies in LTEC, which result in uneven expansion/contraction within the components of the composite resin [50]. The interface between the matrix and the filler is thus fatigued, making the interface more prone to debonding. Dissolution of surface organic matrix has also been reported to affect most dental materials, including composites [51]. Since both processes are present within the composite body, the overall result is lower contact angles and deeper filler exposition [52]. This process results in an overall change of surface morphology (roughness), which becomes prone to color changes by deposition [51]. Steam sterilization has been reported to cause significant changes in micromorphology and wettability of bulk composites (Filtek Bulk Fill and Filtek Z350XT) [51,52]. The values for color changes observed in Gp C are in agreement with those reported by Jeong et al [53], who observed noticeable but acceptable (ΔE*=2.2 and 2.3) changes after 10-day immersion of resin shades in distilled water. Different studies have reported color changes in composite resin materials and have concluded that they are more susceptible to optical and chemical changes than other restorative materials (ceramics and metals) [44,54,55]. Water sorption with subsequent staining has also been reported to contribute to color changes in composite resin, especially if the resin contains higher amounts of TEGDMA [56].
STRENGTH AND LIMITATIONS OF THE STUDY:
The present study is unique in that most previous studies that assessed the color changes due to sterilization have involved either ceramics or unfilled resin. The limitations of the study include: not having used the prefabricated shade guide for evaluation of color changes after sterilization, only 1 brand investigated and 1 thickness (4 mm) assessed, not using more sensitive measuring tools like CIEDE2000, difference in geometry of the composite specimen, which may not be as exact as that of vita shade guide tab, and inherent limitations associated with spectrophotometer use.
Conclusions
This study, within its own limitations, concludes that CSG supplied by the manufacturer with composite kit does not simulate the shades of the vita classic shade guide. Various shades in CSG undergo significant color changes during sterilization with an autoclave, causing color changes that are clinically unacceptable. Clinicians using prefabricated CSG should routinely use chemical sterilization while avoiding frequent autoclaving. This study recommends clinicians fabricate their own custom shade guide from a particular lot, and keep the prefabricate CSG as a reference while using a customized shade guide on patients. Consistent with the above, clinicians should compare the customized shade guide after sterilization cycles with the prefabricated CSG for color changes.
Figures
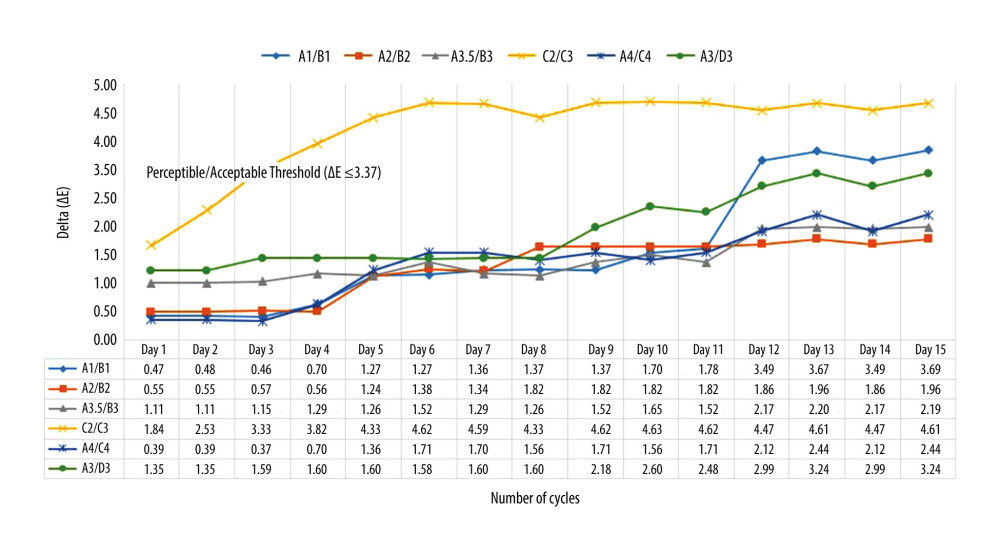 Figure 1. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group A (autoclave disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation).
Figure 1. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group A (autoclave disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation). 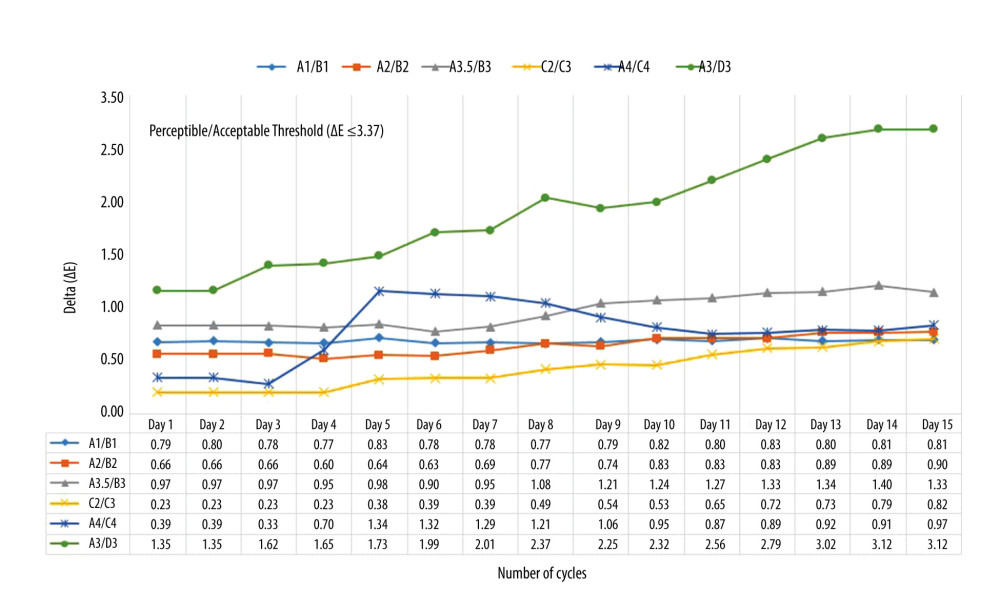 Figure 2. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group C (chemical disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation).
Figure 2. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group C (chemical disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation). Tables
Table 1. Test material with distribution of groups according to sterilization method.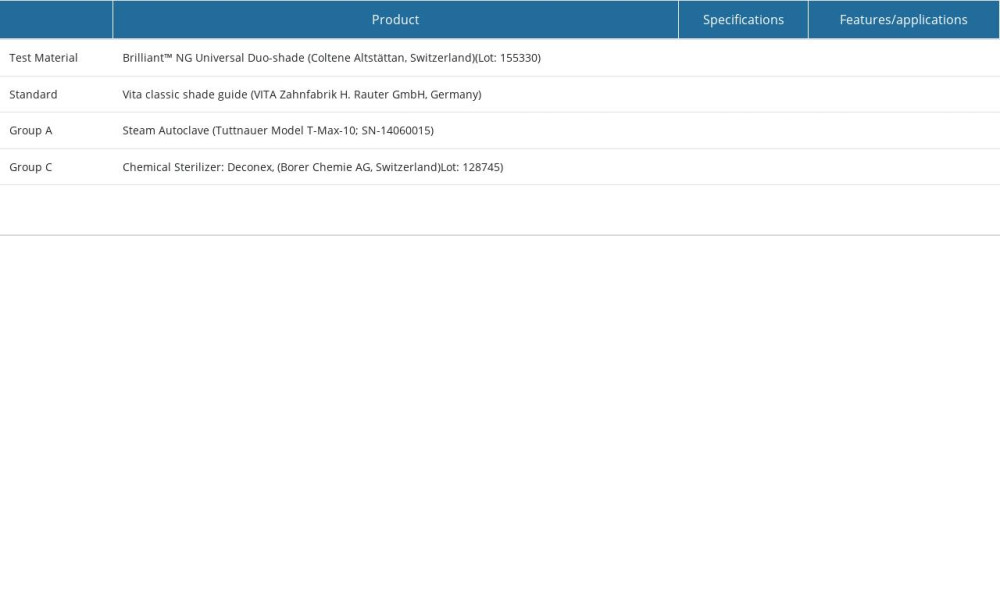 Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs.
Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs.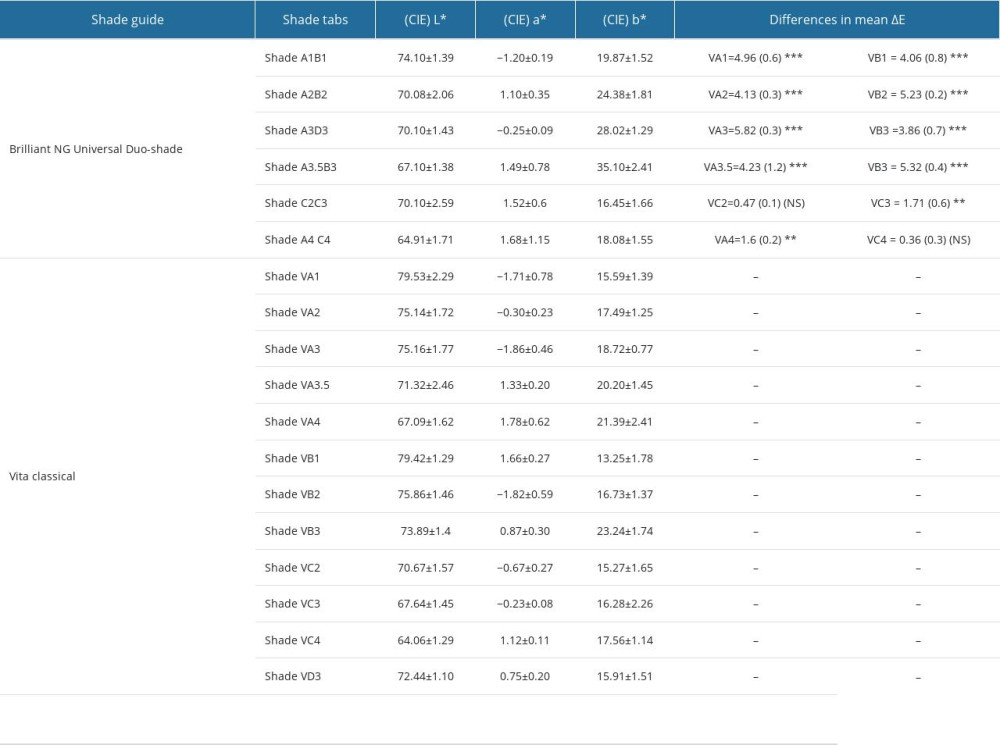 Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave).
Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave).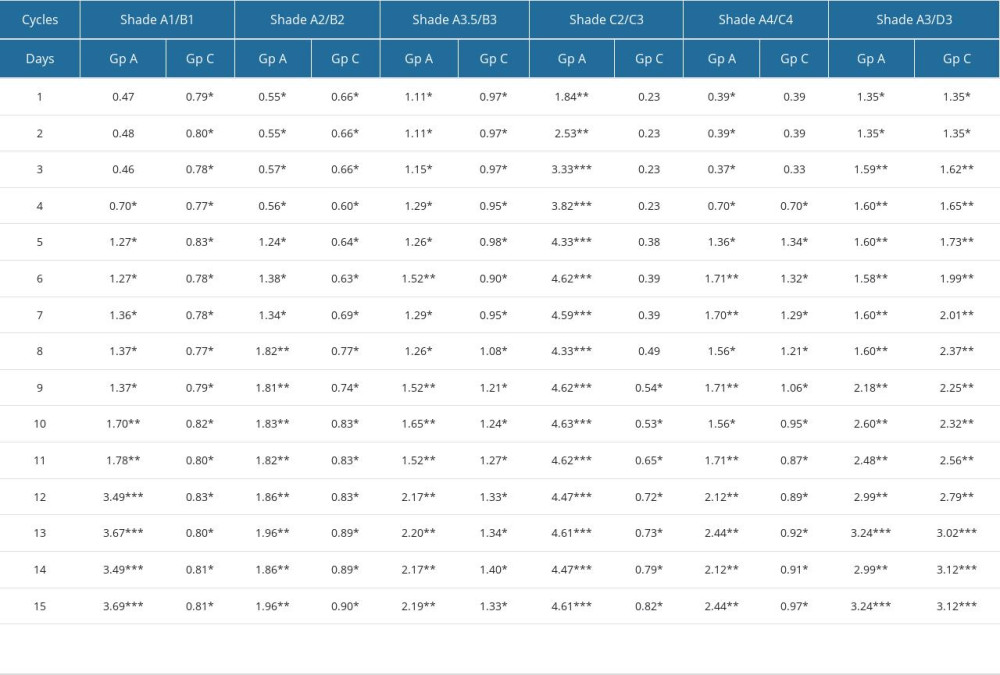
References
1. Norwegian Ministry of the Environment: Amendment of Regulations of 1 June 2004 no 922. Relating to Restrictions on the Use of Chemicals and Other Products Hazardous to Health and the Environment, 2008, Oslo, Norway, Norwegian Ministry of the Environment Available at: https://www.regjeringen.no/globalassets/upload/md/vedlegg/forskrifter/product_regulation_amendment_071214.pdf
2. Mikhail SS, Schricker SR, Azer SS, Optical characteristics of contemporary dental composite resin materials: J Dent, 2013; 41(9); 771-78
3. Aguilar FG, da Roberti Garcia LF, Cruvinel DR, Color and opacity of composites protected with surface sealants and submitted to artificial accelerated aging: Eur J Dent, 2012; 6; 24-33
4. Sarac D, Sarac YS, Kulunk S, The effect of polishing techniques on the surface roughness and color change of composite resins: J Prosthet Dent, 2006; 96(1); 33-40
5. Carrillo-Marcos A, Salazar-Correa G, Castro-Ramirez L, The microhardness and surface roughness assessment of bulk-fill resin composites treated with and without the application of an oxygen-inhibited layer and a polishing system: An in vitro study: Polymers, 2022; 14(15); 3053
6. Lee YK, Lim BS, Kim CW, Effect of surface conditions on the color of dental resin composites: J Biomed Mater Res, 2002; 63; 657-63
7. Iyer RS, Babani VR, Yaman P, Dennison J, Color match using instrumental and visual methods for single, group, and multi-shade composite resins: J Esthet Restor Dent, 2021; 33(2); 394-400
8. Kim BJ, Lee YK, Influence of the shade designation on the color difference between the same shade-designated resin composites by the brand: Dent Mater, 2009; 25(9); 1148-54
9. Chu SJ, Trushkowsky RD, Paravina RD, Dental color matching instruments and systems. Review of clinical and research aspects: J Dent, 2010; 38(Suppl 2); e2-16
10. Ardu S, Krejci I, Biomimetic direct composite stratification technique for the restoration of anterior teeth: Quintessence Int, 2006; 37; 167-7
11. Magne P, Bruzi G, Carvalho AO, Evaluation of an anatomic dual-laminate composite resin shade guide: J Dent, 2013; 41; e80-86
12. Chu SJ, Clinical color match of porcelain visual shade matching systems: J Esthet Restor Dent, 2005; 6; 358 [commentary]
13. Dental Composites Market: Global Analysis Report, 2031 Available at: https://www.transparencymarketresearch.com/dental-composites-market.html
14. Gomez-Polo C, Gomez-Polo M, Martinez Vazquez de Parga JA, CeleminVinuela A, Study of the most frequent natural tooth colors in the Spanish population using spectrophotometry: J Adv Prosthodont, 2015; 7(6); 413-22
15. Paolone G, Orsini G, Manauta J, Composite shade guides and color matching: Int J Esthet Dent, 2014; 9(2); 164-82
16. Prabu PS, Prabu NM, Kumar M, Abhirami M, Shade variance in ceramic restoration and shade tab: An in vitro study: J Pharm Bioallied Sci, 2012; 4(Suppl 2); S139-41
17. Robertson TM, Heymann HO, Swift EJ: Sturdevant’s art & science of operative dentistry, 2002; 484, St Louis, CV Mosby
18. Paravina RD, Performance assessment of dental shade guides: J Dent, 2009; 37(Suppl 1); e15-20
19. Todorov R, Peev T, Zlatev S, Shade guides used in the dental practice: Journal of IMAB – Annual Proceeding Scientific Papers, 2020; 26(2); 3168-73
20. Floriani F, Brandfon BA, Sawczuk NJ, Color difference between the vita classical shade guide and composite veneers using the dual-layer technique: J Clin Exp Dent, 2022; 14(8); e615
21. : Vita shade guide Website: http://vident.com/products/shade-management/vita-classical-previously-the-luminvacuum-shade-guide/
22. Jouhar R, Ahmed MA, Khurshid Z, An overview of shade selection in clinical dentistry: Appl Sci, 2022; 12(14); 6841
23. Baratieri LN, Araujo E, Monteiro S, Color in natural teeth and direct resin composite restorations: Essential aspects: Eur J Esthet Dent, 2007; 2(2); 172-86
24. Wee AG, Kang EY, Jere D, Beck FM, Clinical color match of porcelain visual shade-matching systems: J Esthet Restor Dent, 2005; 17; 351-57
25. Ghinea R, Pérez MM, Herrera LJ, Color difference thresholds in dental ceramics: J Dent, 2010; 38(Suppl 2); e57-64
26. Nimeroff I, Colorimetry: Natl Bureau Stand Monogr, 1968; 47; 104
27. Mattoo KA, Jain S, Managing prosthodontic (geriatric) patients during the SARS-CoV-2 pandemic: J Int Oral Health, 2020; 12; S69-75
28. Al Makramani BMA, Al Sanabani F, Mattoo KA, Reviewing infection control in prosthodontic practice with a case of herpes simplex in the times of a corona virus pandemic: Ann Romanian Soc Cell Biol, 2021; 25(6); 10898-904
29. Silva FP, Faria-e-Silva AL, Moraes RR, Effect of thermally deposited siloxane-methacrylate coating on bonding to glass fibre posts: Int Endod J, 2018; 51; 78-85
30. Browning WD, Contreras-Bulnes R, Brackett MG, Brackett WW, Color differences: Polymerized composite and corresponding Vitapan Classical shade tab: J Dent, 2009; 37; e34-39
31. Pande N, Kulkarni S, Jaiswal P, Chahande J, Comparative evaluation of the effect of three medications on the color stability of two commercially available acrylic resin denture teeth after thermocycling–An in vitro study: Indian J Multidiscip Dent, 2019; 9(1); 9
32. Schmeling M, Sartori N, Monteiro S, Baratieri L, Color stability of shade guides after autoclave sterilization: Int J Periodontics Restorative Dent, 2014; 34(5); 689-93
33. Fahmy MM, Maglad SA, Color stability of shade guides after disinfection and autoclave sterilization: J Am Sci, 2015; 11(12); 89-95
34. Browning WD, Chan DC, Blalock JS, Brackett MG, A comparison of human raters and an intra-oral spectrophotometer: Oper Dent, 2009; 34; 337-43
35. Udiljak Z, Illes D, Knezovic Zlataric D, Celic R, Effect of clinical experience on the shade matching accuracy in different dental occupational groups: Acta Stomatol Croat, 2018; 52(2); 132-39
36. Paravina RD, Kimura M, Powers JM, Color computability of resin composites of identical shade designation: Quintessence Int, 2006; 37; 713-19
37. Swift EJ, Hammel S, Lund PS, Colorimetric evaluation of vita shade resin composites: Int J Prosthodont, 1994; 7; 356-61
38. Ikeda T, Nakanishi A, Yamamoto T, Sano H, Color differences and color changes in Vita Shade tooth-colored restorative materials: Am J Dent, 2003; 16; 381-84
39. Mitra SB, Wu D, Holmes BN, An application of nanotechnology in advanced dental materials: JADA, 2003; 134; 1382-90
40. Rawls HR, Upshaw JE, Restorative resins: Phillips’s science of dental materials, 2003; 399-441, Philadelphia, WB Saunders
41. Kaizer MR, Diesel PG, Mallmann A, Jacques LB, Ageing of silorane-based and methacrylate-based composite resins: Effects on translucency: J Dent, 2012; 40(Suppl 1); e64-71
42. Shortall AC, How light source and product shade influence cure depth for a contemporary composite: J Oral Rehabil, 2005; 32; 906-11
43. Menon A, Ganapathy DM, Mallikarjuna AV, Factors that influence the colour stability of composite resins: Drug Invent Today, 2019; 11(3); 744-49
44. Yap AU, Tan KB, Bhole S, Comparison of aesthetic properties of toothcolored restorative materials: Oper Dent, 1997; 22; 167-72
45. Al Moaleem MM, Alkhayrat FM, Madkhali HA, Subjective differences between dentists and patients about relative quality of metal ceramic restorations placed in the esthetic zone: J Contemp Dent Pract, 2017; 18(2); 112-16
46. Wieder S, Custom shade guide system for composite resins: J Esthet Dent, 1990; 2(1); 10-12
47. Terry DA, Color matching with composite resin: A synchronized shade comparison: Pract Proced Aesthet Dent, 2003; 15(7); 515-28
48. Rutala WA, Weber DJ, Disinfection and sterilization in health care facilities: What clinicians need to know: Clin Infect Dis, 2004; 39; 702-9
49. Nascimento AS, Rodrigues JFB, Torres RHN, Physicomechanical and thermal analysis of bulk-fill and conventional composites: Braz Oral Res, 2019; 33; e008
50. Buruiana T, Melinte V, Popa ID, Buruiana EC, New urethane oligodimethacrylates with quaternary alkylammonium for formulating dental composites: J Mater Sci Mater Med, 2014; 25(4); 1183-94
51. Nascimento AS, Lima DB, Fook MVL, de Albuquerque MS, Physicomechanical characterization and biological evaluation of bulk-fill composite resin: Braz Oral Res, 2018; 25(32); e107
52. De Sousa-Lima RX, De Sousa Santos K, De Azevedo Silva LJ, Can sterilization methods influence surface properties of resin composites? A purpose for previewing bias in laboratory bacterial adhesion tests: Microsc Res Tech, 2022; 85(3); 1101-7
53. Jeong TS, Kang HS, Kim SK, The effect of resin shades on microhardness, polymerization shrinkage, and color change of dental composite resins: Dent Mater J, 2009; 28(4); 438-45
54. Gürdal P, Akdeniz BG, Hakan-Sen B, The effects of mouthrinses on microhardness and colour stability of aesthetic restorative materials: J Oral Rehabil, 2002; 29; 895-901
55. Yap AU, Tan SH, Wee SS, Chemical degradation of composite restoratives: J Oral Rehabil, 2001; 28; 1015-21
56. Domingos PA, Garcia PP, Oliveira AL, Palma-Dibb RG, Composite resin color stability: Influence of light sources and immersion media: J Appl Oral Sci, 2011; 19; 204-11
Figures
 Figure 1. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group A (autoclave disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation).
Figure 1. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group A (autoclave disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation). Figure 2. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group C (chemical disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation).
Figure 2. Graphical presentation showing comparative differences in mean delta values ΔE within the composite shade tabs in group C (chemical disinfection). Figure created using MS Excel sheet, version 20H2 (OS build 19042,1466), Windows 11 Pro, Microsoft Corporation). Tables
 Table 1. Test material with distribution of groups according to sterilization method.
Table 1. Test material with distribution of groups according to sterilization method. Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs.
Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs. Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave).
Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave). Table 1. Test material with distribution of groups according to sterilization method.
Table 1. Test material with distribution of groups according to sterilization method. Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs.
Table 2. Mean and standard deviation for CIE color coordinates for L*, a* and b* values and their relative degree of color differences (ΔE) between stock Composite shade guide and Vita Classical shade guide tabs. Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave).
Table 3. Comparative differences in magnitude (mean) of color value (ΔE) calculated from CIE color coordinates (L*, a* and b*) for duo-shade composite between Group C (Chemical Disinfectant) and Group A (Autoclave). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








