08 August 2020: Clinical Research
Systematic Understanding of Mechanism of Yi-Qi-Huo-Xue Decoction Against Intracerebral Hemorrhagic Stroke Using a Network Pharmacology Approach
Jian Li1ABF, Ming Ye1D, Jueming Gao1B, Yeqing Zhang2C, Qiyong Zhu2AG, Weibang Liang3AEFG*DOI: 10.12659/MSM.921849
Med Sci Monit 2020; 26:e921849
Abstract
BACKGROUND: Intracerebral hemorrhage (ICH), a fatal type of stroke, profoundly affects public health. Yi-Qi-Huo-Xue decoction (YQHXD), a traditional Chinese medicine (TCM) prescription, is verified to be an efficient method to treat ICH stroke among the Chinese population. Nevertheless, the pharmacological mechanisms of YQHXD have been unclear.
MATERIAL AND METHODS: We used a strategy based on network pharmacology to explore the possible multi-component, multi-target, and multi-pathway pattern of YQHXD in treating ICH. First, candidate targets for YQHXD were identified using the Traditional Chinese Medicine Systems Pharmacology Database and Analysis Platform (TCMSP). Then, these candidate YQHXD targets were used in combination with the known targets for the treatment of ICH stroke to construct the core network (cPPI) using data on protein–protein interaction (PPI). We calculated 5 topological parameters for identification of the main hubs. Pathway enrichment and GO biological process enrichment analyses were performed after the incorporation of the main hubs into ClueGO.
RESULTS: In total, 55 candidate YQHXD targets for ICH were recognized to be the major hubs in accordance with their topological importance. As suggested by enrichment analysis, the YQHXD targets for ICH were roughly classified into several biological processes (related to redox equilibrium, cell–cell communication, adhesion and collagen biosynthesis, cytokine generation, lymphocyte differentiation and activation, neurocyte apoptosis and development, neuroendocrine system, and vascular development) and related pathways (VEGF, mTOR, NF-κB, RAS/MAPK, JAK/STAT and cytokine–cytokine receptors interaction), indicating those mechanisms underlying the therapeutic effect of YQHXD.
CONCLUSIONS: The present results may serve as a pharmacological framework for TCM studies in the future, helping to promote the use of YQHXD in clinical treatment of ICH.
Keywords: Cerebral Hemorrhage, Pharmacologic Actions, Stroke, gene ontology, hemorrhagic stroke, Protein Interaction Maps
Background
Intracerebral hemorrhagic (ICH) stroke is a fatal disorder associated with high morbidity and mortality rates, accounting for about 15% of all stroke-related mortality [1,2]. Post-ICH cerebral damage is a dynamic process involving a series of complicated pathological pathways, with metabolic and biochemical events. Such events are classified as blood flow decline, free radical injury, apoptosis of neurons, vasogenic and cytotoxic edema, hemorrhagic neuroinflammation, and brain herniation, as well as intracranial hypertension, leading to serious cerebral damage as a result of repeated strokes [3–9]. However, surgical treatment to remove a hematoma cannot significantly improve the long-term prognosis, and there is also no efficient treatment to manage hemorrhagic stroke [10,11].
For thousands of years, traditional Chinese medicine has played an important part in maintaining health. In TCM clinical practice, formulas that integrate distinct botanical, mineral, or animal medicines are commonly used in treating different diseases [12–15]. Yi-Qi-Huo-Xue decoction (YQHXD) has been frequently used in TCM for the treatment of ICH stroke. It consist of a combination of 11 herbal medicines: Astragali Radix (Huangqi, HQ), Angelicae Sinensis Radix (Danggui, DG), Persicae Semen (Taoren, TR), Carthami Flos (Honghua, HH), Pheretima (Dilong, DL), Paeoniae Radix Rubra (Chishao, CS), Chuanxiong Rhizoma (Chuanxiong, CX), Angelicae Dahuricae Radix (Baizhi, BZ), Glycyrrhizae Radix et Rhizoma (Gancao, GC), Asari Radix Et Rhizoma (Xixin, XX), and Hirudo (Shuizhi, SZ). YQHXD I a protocol prescription formulated by the Neurosurgery Department of Jiangsu Provincial Hospital of TCM in accordance with the classical theories of TCM. YQHXD plays an important role in the treatment of ICH through promoting hematoma absorption, mitigating neuroinflammation, and alleviating nerve injury (related data are currently under submission). Some single herbs in the YQHXD prescription are important in other TCM formulas used to treat ICH, like DL and CS in Liangxue Tongyu Prescription [16], as well as SZ in Poxue Huayu and Tianjing Busui Decoction [17]. However, the clinical efficacy and pharmacological effects of YQHXD on ICH have been largely unknown.
For most TCM medicines, their efficacy is usually modulated through various pathways and targets, since there are complex active ingredients in TCM. As a result, it is difficult to precisely determine these active ingredients by conventional methods, making it urgently needed to formulate new and suitable approaches. Historically,
We used a comprehensive approach combined with active compound prediction based on a series of pharmacokinetic parameters, mining of multiple drug targets, and network analysis (by using these databases), to elucidate the synergistic effects and underlying mechanisms of YQHXD on ICH stroke.
Material and Methods
MINING KNOWN ICH STROKE-RELATED TARGETS:
Five publically accessible databases – DrugBank, MalaCards, Online Mendelian Inheritance in Man (OMIM), Genetic Association Database (GAD), and Therapeutic Target Database (TTD) – as well as related references, were retrieved to find targets for ICH stroke [21] using the keywords ‘intracranial hemorrhage’ and ‘hemorrhagic stroke’. As a result, 1558 ICH stroke-related featured targets were extracted (shown in Supplementary Table 1).
COMPOUNDS IN YQHXD:
We collected compounds of all ingredients in YQHXD from TCMSP as well as relevant studies, which produced a total of 1194 compounds in YQHXD. There were 87, 125, 66, 189, 119, 189, 223, 192, and 280 compounds in HQ, DG, TR, HH, CS, CX, BZ, XX, and GC, respectively. Nevertheless, no compounds were detected from the DL except for lumbrokinase and SZ except for hirudin.
ORAL BIOAVAILABILITY (OB) AND DRUG-LIKENESS SCREENING:
OB is the percent of the drug reaching systemic circulation after oral administration, and it also represents the ADME convergence process. A high OB value can be an important index for determining the drug-like properties of diverse bioactive molecules [22]. Drug-likeness qualitatively assesses compound structural similarity to a variety of clinical medicines using the DrugBank database. It is also a qualitative way to estimate the extent of “drug-likeness” for a typical molecule during drug design, which facilitates the optimization of pharmacokinetic and pharmaceutical characters such as solubility and chemical stability [23]. In line with the TCMSP database recommendations, an OB of 30%, together with a drug-likeness index of 0.18 (mean value for all molecules within the DrugBank database) [24], was used as the cut-off value for selecting candidate compounds [25]. In this study, these cut-off values helped to efficiently and maximally collect data from YQHXD using the least components, and the pharmacokinetic data reported may account for this [26]. In addition, additional compounds, such as lumbrokinase, hirudin, calarene, oleic acid, caffeic acid, and linolenic acid, were first excluded in accordance with the above screening criteria. However, they were then identified to be possible compounds for analyses, as indicated by the widely accepted pharmacological activities [27–32].
DRUG TARGET PREDICTION FOR YQHXD:
Identifying the target is a key step during the development of medicines. In this study, we used the systematic medicine targeting method of Yu et al. [33], which can precisely identify putative targets for medicinal compositions. The present systemic medicine targeting approach was conducted on 2 levels, and it represents a systemic target-predicting approach to integrate several algorithms. (1) The HIT database was applied in collection and retrieval of the drug-target interactions verified in experiments. (2) The SysDT model was used to predict the putative compound targets that have not been validated in experiments, and high sensitivity, specificity, and consistency were attained in the prediction of drug-target interactions [33].
PPI NETWORK ESTABLISHMENT:
The BisoGenet plugin of Cytoscape was used to analyze the PPI network through combining the data presented in 6 PPI datasets, including the Biological General Repository for Interaction Datasets (BGRID), Database of Interacting Proteins (DIP), Biomolecular Interaction Network Database (BIND), Human Protein Reference Database (HPRD), Molecular Interaction Database (MID), and InAct. Supplementary Table 2 summarizes details about these PPI data sets. Cytoscape software was subsequently used for the establishment and visualization of 2 PPI networks by enrolling putative YQHXD targets as well as defined ICH-related targets, followed by constructing a core PPI (cPPI) network by merging the above 2 networks based on PPI intersection data.
NETWORK TOPOLOGICAL CHARACTERISTICS ANALYSIS:
The following 5 parameters were calculated to analyze the topological characteristics of all nodes in the cPPI network with the Cytoscape plugin cytohubba [34]: ‘degree’, ‘betweenness’, ‘closeness’, ‘radiality’, and ‘stress’. The definitions and corresponding computational formulas for these parameters were reported in previous studies, and they represent the network-based node topological importance, in which higher quantitative values indicate greater importance.
GENE ONTOLOGY (GO) AND PATHWAY ENRICHMENT ANALYSES:
A total of 335 candidate targets for YQHXD were obtained thorough GO analysis using Omicshare [35] to examine their effects in 3 categories: Molecular Function (MF), Biological Processes (BP), and Cell Component (CC). P<0.05 was the significance threshold to identify those enriched GO terms in hypergeometric testing.
The enrichment analyses for those 16 putative YQHXD targets for ICH stroke were reflected using ClueGO [36], which is the Cytoscape plugin used to visualize non-repetitive biological terms of great gene clusters within the network grouped functionally. The results were categorized into 2 large clusters: biological processes/molecular functions, and the signal transduction pathways. In addition, the ClueGO network was constructed using kappa statistics to present the associations among terms based on related gene similarity.
Results
CANDIDATE COMPOUND SCREENING FOR YQHXD:
Finally, a total of 182 active ingredients were extracted from YQHXD and were identified as significant by selecting OB combined with assessing the drug-likeness. We found 59 compounds that had relatively low OB or drug-likeness value, exhibited great pharmacological effects, and were herbal medicinal components (identified in previous studies), and these were the putative active ingredients. At last, 241 compounds were collected from 11 herbs, which were identified to be the “candidate compounds” (Supplementary Table 3). Specifically, the candidate compound numbers of DG, HQ, HH, TR, CX, CS, XX, BZ, SZ, GC, and DL were 5, 20, 28, 20, 20, 26, 17, 53, 1, 97, and 1, respectively. Among them, 28 were detected in more than 1 herb in YQHXD, and they were verified to possess a variety of biological effects. For example, beta-sitosterol was distributed among 5 herbs (TR, DG, BZ, CS, and HH), and it has strong antioxidant, anti-platelet, anti-inflammation, and anti-tumor activities [37]. Similarly, quercetin, stigmasterol, oleic acid, and kaempferol, which were detected in at least 3 YQHXD herbs, possessed numerous pharmacological activities, and they were involved in regulating several physiopathological processes, like blood-brain barrier (BBB) dysfunction, ICH, immune response, and inflammation [38–41].
PUTATIVE TARGET PREDICTION FOR YQHXD:
Generally, TCM formulas exert great therapeutic and preventive efficacy in complex diseases, and they totally depend on the synergy of different compounds and targets. As a result, therapeutic targets should be further investigated, apart from illustrating the possible active ingredients of YQHXD. In this study, pharmacological, chemical, and genomic data were integrated to predict the putative compound targets. A total of 261 putative targets were predicted for those 338 compounds (Supplementary Table 4). The numbers of putative targets linked by HQ, DG, TR, HH, CS, CX, BZ, XX, GC, SZ, and DL were 229, 73, 72, 277, 154, 93, 135, 125, 240, 2, and 4, respectively. Obvious overlaps were observed in 11 herbs, although each herb has different targets. This means that different components in YQHXD can exert congenerous effects, probably by regulating similar targets. For instance, both CX and BZ are proved to affect the occurrence and development of multiple cerebral injury by decreasing BBB leakage and brain edema, reducing neuron loss, activating microglia and astrocytes, and increasing neural stem cells (NSCs) proliferation [42,43].
To better investigate the effects of candidate targets involved in different MFs, CC, and BPs, we conducted preliminary GO analysis using Omicshare, the DAVID-based public database. We found that the candidate targets were responsive to various stimuli (e.g., inflammatory, chemical factors, hormone, and ROS), biological adhesion, immune systems, inflammation, cell proliferation, and metabolism, and all these participate in the ICH stroke pathological process (Figure 1) [3,44–47].
To comprehensively understand the component-target network in YQHXD systemically and holistically, Cytoscape was utilized to establish a network map, including 5798 edges and 626 nodes (Figure 2). Specifically, the node degree stood for the target or edge number related to the node based on topological analysis. A total of 145 possible components were found in the as-established network to have a median of ≥17 degrees. Of these, quercetin, kaempferol, and luteolin acted on 166, 74, and 68 targets, respectively, and they were then recognized to be the vital active components of YQHXD. Quercetin promotes behavioral and neuronal recovery through inhibiting apoptosis and inflammatory response [48] and protects against cerebral edema and oxidative stress (OS) [49], and this in turn regulates ICH stroke. These results can explain the multiple effects of TCM herbs.
COLLECTION OF KNOWN ICH-RELATED TARGETS:
ICH has been recognized as polygenic genetic disorder, and its pathogenesis may be revealed through investigating the interactions between genes and between genes and the environment. We collected 1558 targets related to ICH based on those 5 available resources. In addition, 199 of our detected putative YQHXD targets were recognized as the targets related to ICH (or therapeutic medicines), which suggests the formula has potential therapeutic effects (Supplementary Table 5).
To examine the underlying pharmacological effects of YQHXD on ICH, those 199 targets underwent KEGG and GO enrichment analyses (Figure 3A, 3B). A series of related targets were found to independently belong to coagulation cascade (33/199), death (109/199), oxidative stress (54/199), immune response (102/199), BBB destruction (43/199), neurotransmitter (24/199), cell proliferation (100/199), and differentiation (119/199), as well as metal ion overload (21/199), suggesting YQHXD compounds were likely to participate in multiple pathogenesis mechanisms of ICH, including apoptosis, immune function, neurologic function, thrombosis, and oxidative stress. For example, coagulation factor VII (F7) and prothrombin (F2) have been recognized to be the critical coagulation factors during the process of thrombosis, which are triggered by injury in various reactions, resulting in thrombosis generation by causing coagulum development, and multiple compounds in YQHXD appear to modulate coagulation factors for their subsequent effects.
DETERMINATION OF POTENTIAL ANTI-ICH TARGETS IN YQHXD:
Recent evidence from network biology reveals the absence of complete functional isolation between proteins and genes. Instead, they function in interconnected pathways and molecular networks on multiple levels. Since the basis of most life processes involves PPI networks, relevant studies may reveal the properties and behaviors of biological molecules. Therefore, PPI data of these genes were first used to establish a putative target network (529 nodes and 39798 edges) and a well-defined ICH-associated target network (2317 nodes and 287016 edges). These 2 networks were then merged to obtain the core protein–protein interaction (cPPI) network, which consisted of 16232 edges and 241 nodes, with the final aim to reveal the pharmacological effect of YQHXD on ICH. Then, these possible YQHXD targets for ICH stroke were identified based on cPPI topological features. As reported previously, a node whose degree exceeds the median value (136) for all nodes within the network is identified as the hub node [50]. As a result, there were 119 hubs in the cPPI network for YQHXD against ICH stroke. Using the widely applied plugin cytohubba, 5 topological features – ‘degree’, ‘betweenness’, ‘closeness’, ‘radiality’, and ‘stress’ – were selected to identify the main hubs. In this network of significant targets, the median values of ‘degree’, ‘betweenness’, ‘closeness’, ‘radiality’, and ‘stress’ were calculated as 175, 145.06518, 207.85, 2.74583, and 8616, respectively. Therefore, 55 candidate targets (main hubs in the cPPI network), with ‘degree’ >175, ‘betweenness’ >145.06518, ‘closeness’ >207.85, ‘radiality’>2.74583, and ‘stress’>8616 were identified. Figure 3 shows the flow chart of screening the candidate targets. Supplementary Table 6 displays details about cPPI topological characteristics and 55 candidate targets.
ENRICHMENT ANALYSIS ON CANDIDATE TARGETS FOR YQHXD AGAINST ICH:
To illustrate the possible effects of these 55 candidate targets, the associations between different functional groups and the potential scientific connotations in the biological networks were identified using the Cytoscape plugin ClueGO, and were then divided into GO biological process and the signaling pathway (Figure 4), which were mainly involved in regulating redox equilibrium, cell–cell communication, adhesion and collagen biosynthesis (BBB), cytokine generation, lymphocyte differentiation and activation, cell apoptosis and development (neurocytes), neuroendocrine system, and vascular development. The KEGG pathways were mainly associated with neurotrophin, autophagy, lymphocyte differentiation, and immuno-inflammatory responses. According to the P value of enriched pathways and their correlation with ICH stroke, 6 representative signal pathways most attracted our interest: VEGF, mTOR, NF-κB, RAS/MAPK, JAK/STAT, and cytokine–cytokine receptors interaction. These KEGG pathways are associated with the intrinsic mechanism of ICH, which indicates that the pathological process of this disease is extremely complex, and this may serve as a critical anti-ICK stroke pharmacological mechanism in YQHXD. Our results suggest a new strategy for pharmacological treatment of ICH stroke.
Discussion
In this study, the anti-ICH stroke mechanism underlying the effect of YQHXD was explored using network pharmacology through data mining and subsequent computational modeling. It was noteworthy that our findings partially elucidate the complex anti-ICH mechanism in the YQHXD formula, and they provide insight into the integrated understanding of the therapeutic efficacy and pharmaceutical activity of YQHXD. First, a total of 182 active ingredients were extracted from YQHXD, and these were shown to be significant by screening OB (≥30%) combined with assessing the drug-likeness (≥0.18). Thereafter, these possible YQHXD targets were mined using the TCMSP database. PPI data were used to construct the core PPI network (cPPI) associated with the correlations of 338 putative YQHXD targets acquired by the systemic drug targeting method with the1558 known anti-ICH stroke targets. Then, 55 candidate anti-ICH targets of YQHXD were identified as the pivotal hub genes in the cPPI network according to the specific topological importance (with ‘stress’ >8616, ‘radiality’ >2.74583, ‘closeness’ >207.85, ‘betweenness’ >145.06518, and ‘degree’ >175).
In addition, GO and KEGG pathway analyses were carried out to demonstrate the candidate target biological significance after the pivotal hub genes were incorporated into ClueGO.
ICH injury is classified into 2 stages: primary and secondary. Primary injury starts from hemorrhage and ultimately results from cerebral vascular damage [51]. Secondary injury can occur in various pathological pathways, including oxidative stress (OS), inflammation, BBB disruption, blood cytotoxicity, necrosis and apoptosis of neurons, excitotoxicity, autophagy, and endoplasmic reticulum stress (ERS), and this inevitably results in the death of neurons [52]. Among the 55 candidate targets mined in YQHXD to treat ICH stroke, some exerted vital inducing roles (risk factors) in the above-mentioned pathological processes, whereas some reversed the pathological changes in some diseases (protective factors). Cytokines such as ILs, TNF, IFN, and TGFB1 have been verified to be important factors of secondary neuronal injury and neurological dysfunction after hemorrhage, which affect the activation and function of multiple immune cells to regulate the synthesis of multiple cells (e.g., white blood cells and endothelial cells), surface adhesion molecules (e.g., ICAM1 and CDH1), and the release of inflammatory metabolites and oxygen free radicals, changing BBB function and integrity, and thus jointly affecting the disease process. In contrast, TNF-α, IL-6, and IL-1β seem to aggravate cerebral injury, while TGFB1, IL-10, and IFN are neuroprotective [53–56]. In addition, MMPs (e.g., MMP2 and MMP9) are associated with hemorrhagic transformation after thrombolysis following cerebral infarction and BBB injury, and are closely associated with poor prognosis in post-ICH stroke [57,58]. NOS3, CAT, and SOD1 are important antioxidant enzymes in the body that can scavenge multiple reactive nitrogen species (RNS) and reactive oxygen species (ROS), thus protecting tissue and local lesion neurons from OS injury, and their activities and upregulated expression contribute to disease recovery [59–61]. Signaling molecules such as TLR4, STAT3, JUN, FOS, and mTOR have been verified to be significantly upregulated in local ICH lesions, which promotes the occurrence of pathological changes like inflammatory response (combined with multiple cytokines and downstream PTGS2 synthesis) and local neuron apoptosis (through affecting Akt- or MAPKs-mediated caspases cascade reaction, HSP5-mediated ERS, and the downstream level of apoptin BCL2L1) [62–64]. The GSK-3β/β-catenin (CTNNB1) pathway has been verified to participate in maintaining the viability of neurons (CCND1- and CDKN2A-mediated), and upregulates BDNF and VEGF to promote angiogenesis, neurogenesis, and BBB repair (KDR- and EGFR-mediated) in ICH [65,66].
The present study is the first to use network pharmacology to investigate the anti-ICH pharmacological mechanism underlying the effect of YQHXD. This study elucidates the anti-ICH mechanism of YQHXD in accordance with the “multi-target, multi-component, and multi-pathway” concept. YQHXD is suggested to exert a comprehensive role in ICH through modulating the redox balance, intercellular adhesion and communication, cytokine production, collagen synthesis, activation and differentiation of leukocytes, development and apoptosis of neurons, and development of vascular and neuroendocrine systems via corresponding pathways (JAK/STAT, mTOR, VEGF, RAS/MAPK, NF-κB, and interactions of cytokine–cytokine receptors). These 6 signal transduction pathways are verified to participate in the diverse pathological changes mentioned above [3,67–73]. Additionally, lymphocytes and cytokines are reported in numerous studies to play important roles in ICH progression [74–76]. The present findings suggest that several critical signaling pathways are involved in lymphocyte activation, differentiation, and proliferation.
In summary, this study focused on 3 aspects. Firstly, the common anti-ICH targets of YQHXD were mainly enriched in the development of blood vessels, BBB (intercellular adhesion and communication, collagen metabolism), and intracellular pathological changes in redox balance. Secondly, in line with the enrichment analysis, the regulatory effects of YQHXD on the differentiation and activation of lymphocytes and cytokine production were responsible for the primary anti-ICH therapeutic mechanisms (inflammatory and immune responses). Thirdly, neuroprotection and neuroendocrine regulation were identified as the crucial effects of YQHXD in the treatment of ICH stroke.
Nonetheless, some limitations should be noted in this study. First of all, certain metabolic and prototype compounds of YQHXD herbs were ignored due to the insufficient data acquired from the available laboratory results and databases. In addition, clinical trials and animal assays to validate our results are lacking for the time being. Additionally, it is difficult to directly evaluate some crucial active ingredients and specific targets collected due to the chemical and conceptual complexity of TCM medications. More research is needed to discover the metabolic and prototype compounds from YQHXD on the basis of pharmacokinetic and pharmacodynamics experiments. Compound interactions can be classified as antagonism and synergy. More systemic studies are needed to study the synergy of multiple components in YQHXD in a dose-dependent manner. The candidate compound targets of YQHXD should be enriched to identify numerous signaling pathways to explore the intrinsic complex anti-ICH mechanism of YQHXD.
Conclusions
The present study illustrates the systemic “multi-compound and multi-target” efficacy of YQHXD against ICH. In addition, proteins, genes and pathways possibly related to biological processes were selected and examined. Moreover, this study also provides a theoretical basis to determine the synergistic effects of TCM in treating diseases and the role of systematic network pharmacology in elucidating the potential mechanisms of action of TCMs. However, as this study was based on data mining and data analysis, further validation studies are needed.
Supplementary Data
Supplementary Table 1. The known ICH-related targets.
Supplementary Table 2. Details about the 6 available protein–protein interaction databases.
Supplementary Table 3. All candidate YQHXD compounds.
Supplementary Table 4. All putative YQHXD targets.
Supplementary Table 5. 199 shared putative YQHXD targets with the known ICH-related targets.
Supplementary Table 6. Topological features for each node/hub/main hub of YQHXD to treat ICH stroke.
Supplementary/raw data available from the corresponding author on request.
Figures
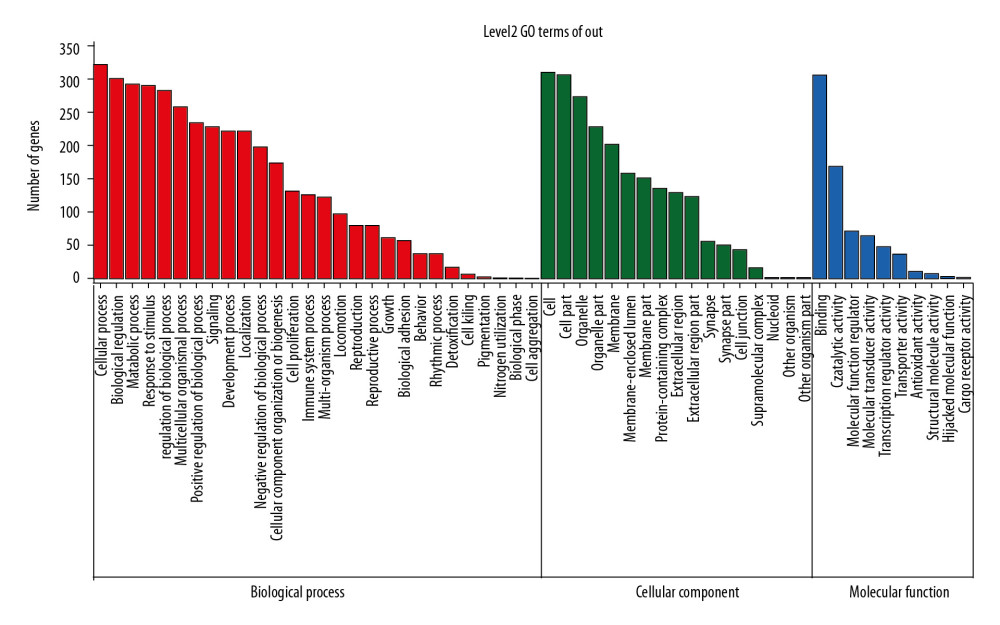 Figure 1. Gene ontology analysis of the putative targets of YQHXD. Candidate targets for YQHXD were analyzed based on Omicshare to shed more light on their possible roles in diverse biological processes (denoted in red), molecular function (denoted in blue), and cell component (denoted in green). The significance threshold was set at P≤0.05, and those GO terms enriched were identified by hypergeometric test. Thereafter, those terms in the same category were ranked based on their P-values, with those on the left being of higher significance. The gene number involved in each term is presented in the y-axis.
Figure 1. Gene ontology analysis of the putative targets of YQHXD. Candidate targets for YQHXD were analyzed based on Omicshare to shed more light on their possible roles in diverse biological processes (denoted in red), molecular function (denoted in blue), and cell component (denoted in green). The significance threshold was set at P≤0.05, and those GO terms enriched were identified by hypergeometric test. Thereafter, those terms in the same category were ranked based on their P-values, with those on the left being of higher significance. The gene number involved in each term is presented in the y-axis. 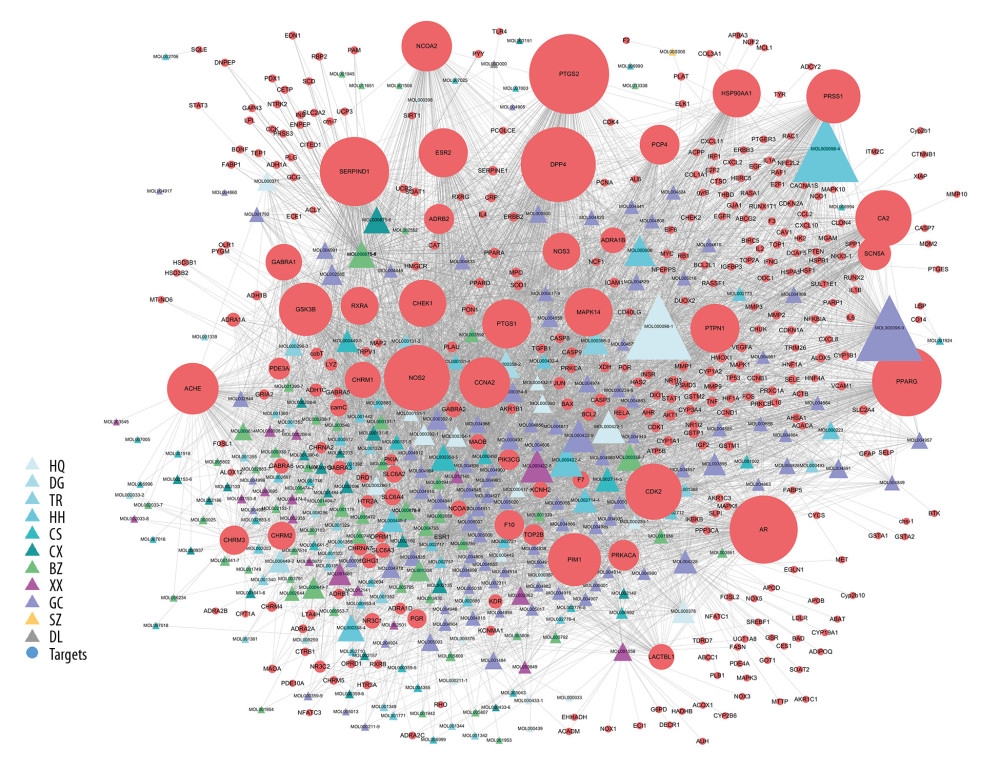 Figure 2. Construction of the YQHXD compound-putative target network. The active compounds (compounds ID) collected based on diverse herbal medicines were linked with corresponding candidate targets to construct the compound-target network, in which a node indicates an active compound (the various colored triangles stand for diverse herbal medicines) and the target (red dot). HQ – Astragali Radix; DG – Angelicae Sinensis Radix; TR – Persicae Semen; HH – Carthami Flos; DL – Pheretima; CS – Paeoniae Radix Rubra; CX – Chuanxiong Rhizoma; BZ – Angelicae Dahuricae Radix; XX – Asari Radix Et Rhizoma; SZ – Hirudo; GC – Glycyrrhizae Radix et Rhizoma.
Figure 2. Construction of the YQHXD compound-putative target network. The active compounds (compounds ID) collected based on diverse herbal medicines were linked with corresponding candidate targets to construct the compound-target network, in which a node indicates an active compound (the various colored triangles stand for diverse herbal medicines) and the target (red dot). HQ – Astragali Radix; DG – Angelicae Sinensis Radix; TR – Persicae Semen; HH – Carthami Flos; DL – Pheretima; CS – Paeoniae Radix Rubra; CX – Chuanxiong Rhizoma; BZ – Angelicae Dahuricae Radix; XX – Asari Radix Et Rhizoma; SZ – Hirudo; GC – Glycyrrhizae Radix et Rhizoma. 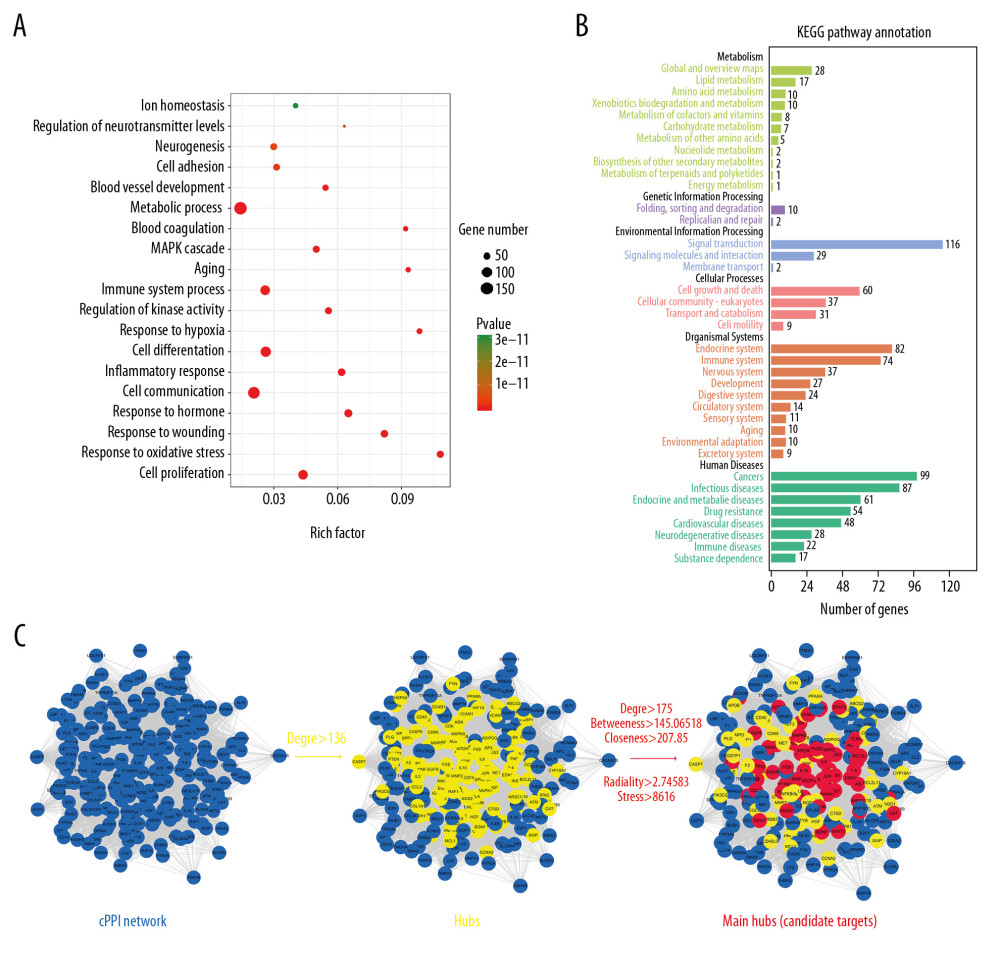 Figure 3. Candidate targets identification. YQHXD shared 199 candidate targets with the identified targets for ICH related to the pathological process. The targets that overlapped were identified based on Omicshare and show their roles in various GO (A) and KEGG (B) terms. The significance threshold was set at P≤0.05, and the terms enriched were identified by hypergeometric test. (C) Flow chart showing the process of selecting potential targets. In the cPPI network, hubs with higher degree than the median among all network nodes were extracted. In addition, main hubs (candidate targets) were mined by calculating 5 topological features.
Figure 3. Candidate targets identification. YQHXD shared 199 candidate targets with the identified targets for ICH related to the pathological process. The targets that overlapped were identified based on Omicshare and show their roles in various GO (A) and KEGG (B) terms. The significance threshold was set at P≤0.05, and the terms enriched were identified by hypergeometric test. (C) Flow chart showing the process of selecting potential targets. In the cPPI network, hubs with higher degree than the median among all network nodes were extracted. In addition, main hubs (candidate targets) were mined by calculating 5 topological features. 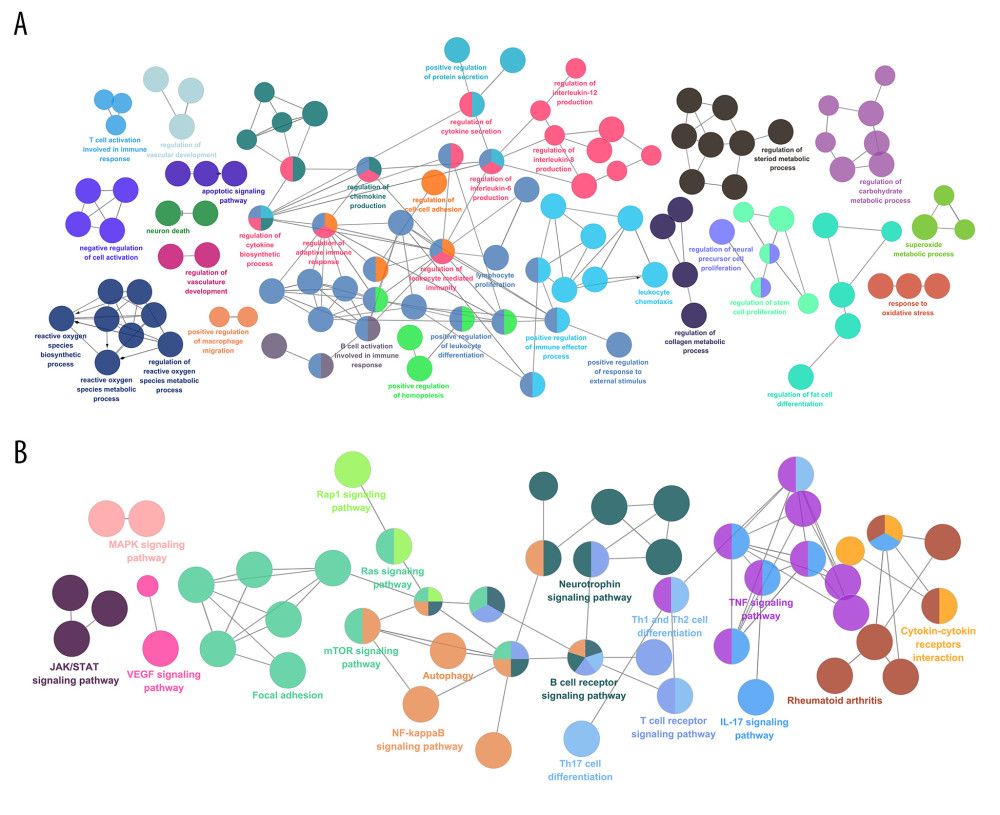 Figure 4. Enrichment analysis based on ClueGO and labeling of vital terms of the group. Partial overlaps were observed in groups that are functionally related. Typical interactions among biological processes or pathways are enriched (P<0.05) across the major targets of YQHXD. (A) Possible enriched targets of YQHXD in typical biological processes. (B) Possible enriched targets of YQHXD in typical signaling pathways.
Figure 4. Enrichment analysis based on ClueGO and labeling of vital terms of the group. Partial overlaps were observed in groups that are functionally related. Typical interactions among biological processes or pathways are enriched (P<0.05) across the major targets of YQHXD. (A) Possible enriched targets of YQHXD in typical biological processes. (B) Possible enriched targets of YQHXD in typical signaling pathways. References
1. Steiner T, Al-Shahi Salman R, Beer REuropean Stroke Ortganisation, European Stroke Organisation (ESO) guidelines for the management of spontaneous intracerebral hemorrhage: Int J Stroke, 2014; 9(7); 840-55
2. van Asch CJ, Luitse MJ, Rinkel GJ, Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: A systematic review and meta-analysis: Lancet Neurol, 2010; 9(2); 167-76
3. Zhou Y, Wang Y, Wang J, Inflammation in intracerebral hemorrhage: From mechanisms to clinical translation: Progr Neurobiol, 2014; 115; 25-44
4. Hegde A, Prasad GL, Rao S, Predictors of outcome in spontaneous intracerebral hemorrhage-role of oxidative stress biomarkers: World Neurosurg, 2018; 120; 601
5. Zhou T, Wang H, Shen J, The p35/CDK5 signaling is regulated by p75NTR in neuronal apoptosis after intracerebral hemorrhage: J Cell Physiol, 2019 [Online ahead of print]
6. Peng WJ, Li Q, Tang JH, The risk factors and prognosis of delayed perihematomal edema in patients with spontaneous intracerebral hemorrhage: CNS Neurosci Ther, 2019; 25(10); 1189-94
7. Xu M, Lin J, Wang D, Cardiac troponin and cerebral herniation in acute intracerebral hemorrhage: Brain Behav, 2017; 7(6); e00697
8. Napier J, Rose L, Adeoye O, Modulating acute neuroinflammation in intracerebral hemorrhage: The potential promise of currently approved medications for multiple sclerosis: Immunopharmacol Immunotoxicol, 2019; 41(1); 7-15
9. Chen CJ, Ding D, Ironside NERICH Investigators, Intracranial pressure monitoring in patients with spontaneous intracerebral hemorrhage: J Neurosurg, 2019 [Online ahead of print]
10. Gross BA, Intracerebral hemorrhage surgery: Improving patient selection and outcome: World Neurosurg, 2016; 91; 642-43
11. Flaherty ML, Beck J, Surgery for intracerebral hemorrhage: Moving forward or making circles?: Stroke, 2013; 44(10); 2953-54
12. Hao P, Jiang F, Cheng J, Traditional Chinese Medicine for cardiovascular disease: Evidence and potential mechanisms: J Am Coll Cardiol, 2017; 69(24); 2952-66
13. Zhang L, Schuppan D, Traditional Chinese Medicine (TCM) for fibrotic liver disease: Hope and hype: J Hepatol, 2014; 61(1); 166-68
14. Li XM, Brown L, Efficacy and mechanisms of action of traditional Chinese medicines for treating asthma and allergy: J Allergy Clin Immunol, 2009; 123(2); 297-306 quiz 307–8
15. Gong X, Sucher NJ, Stroke therapy in Traditional Chinese Medicine (TCM): Prospects for drug discovery and development: Phytomedicine, 2002; 9(5); 478-84
16. Li X, Huang X, Tang Y, Assessing the pharmacological and therapeutic efficacy of Traditional Chinese Medicine liangxue tongyu prescription for intracerebral hemorrhagic stroke in neurological disease models: Front Pharmacol, 2018; 9; 1169
17. Ren J, Zhou X, Wang J, Poxue Huayu and Tianjing Busui decoction for cerebral hemorrhage (upregulation of neurotrophic factor expression): Upregulation of neurotrophic factor expression: Neural Regen Res, 2013; 8(22); 2039-49
18. Terstappen GC, Schlupen C, Raggiaschi R, Gaviraghi G, Target deconvolution strategies in drug discovery: Nat Rev Drug Discov, 2007; 6(11); 891-903
19. Zhang GB, Li QY, Chen QL, Su SB, Network pharmacology: A new approach for chinese herbal medicine research: Evid Based Complement Alternat Med, 2013; 2013 621423
20. Xu T, Ma C, Fan S, Systematic understanding of the mechanism of baicalin against ischemic stroke through a network pharmacology approach: Evid Based Complement Alternat Med, 2018; 2018 2582843
21. Walsh KB, Zhang X, Zhu X, Intracerebral hemorrhage induces inflammatory gene expression in peripheral blood: Global transcriptional profiling in intracerebral hemorrhage patients: DNA Cell Biol, 2019; 38(7); 660-69
22. Xu X, Zhang W, Huang C, A novel chemometric method for the prediction of human oral bioavailability: Int J Mol Sci, 2012; 13(6); 6964-82
23. Tian S, Wang J, Li Y, Drug-likeness analysis of traditional Chinese medicines: Prediction of drug-likeness using machine learning approaches: Mol Pharm, 2012; 9(10); 2875-86
24. Wang X, Xu X, Tao W, A systems biology approach to uncovering pharmacological synergy in herbal medicines with applications to cardiovascular disease: Evid Based Complement Alternat Med, 2012; 2012 519031
25. Wang S, Wang H, Lu Y, Tianfoshen oral liquid: A CFDA approved clinical Traditional Chinese Medicine, normalizes major cellular pathways disordered during colorectal carcinogenesis: Oncotarget, 2017; 8(9); 14549-69
26. Tao W, Xu X, Wang X, Network pharmacology-based prediction of the active ingredients and potential targets of Chinese herbal Radix Curcumae formula for application to cardiovascular disease: J Ethnopharmacol, 2013; 145(1); 1-10
27. Wang YH, Chen KM, Chiu PS, Lumbrokinase attenuates myocardial ischemia-reperfusion injury by inhibiting TLR4 signaling: J Mol Cell Cardiol, 2016; 99; 113-22
28. Karabiyikoglu M, Hua Y, Keep RF, Intracerebral hirudin injection attenuates ischemic damage and neurologic deficits without altering local cerebral blood flow: J Cereb Blood Flow Metab, 2004; 24(2); 159-66
29. Bourourou M, Heurteaux C, Blondeau N, Alpha-linolenic acid given as enteral or parenteral nutritional intervention against sensorimotor and cognitive deficits in a mouse model of ischemic stroke: Neuropharmacology, 2016; 108; 60-72
30. Liang G, Shi B, Luo W, Yang J, The protective effect of caffeic acid on global cerebral ischemia-reperfusion injury in rats: Behav Brain Funct, 2015; 11; 18
31. Song J, Kim YS, Lee DH, Neuroprotective effects of oleic acid in rodent models of cerebral ischaemia: Sci Rep, 2019; 9(1); 10732
32. Govindarajan M, Rajeswary M, Benelli G, δ-cadinene, calarene and δ-4-carene from kadsura heteroclita essential oil as novel larvicides against malaria, dengue and filariasis mosquitoes: Comb Chem High Throughput Screen, 2016; 19(7); 565-71
33. Yu H, Chen J, Xu X, A systematic prediction of multiple drug-target interactions from chemical, genomic, and pharmacological data: PLoS One, 2012; 7(5); e37608
34. Chin CH, Chen SH, Wu HH, cytoHubba: Identifying hub objects and sub-networks from complex interactome: BMC Syst Biol, 2014; 8(Suppl 4); S11
35. Su M, Guo C, Liu M, Therapeutic targets of vitamin C on liver injury and associated biological mechanisms: A study of network pharmacology: Int Immunopharmacol, 2019; 66; 383-87
36. Bindea G, Mlecnik B, Hackl H, ClueGO: A Cytoscape plug-in to decipher functionally grouped gene ontology and pathway annotation networks: Bioinformatics, 2009; 25(8); 1091-93
37. Bin Sayeed MS, Ameen SS, Beta-Sitosterol: A promising but orphan nutraceutical to fight against cancer: Nutr Cancer, 2015; 67(8); 1214-20
38. Galho AR, Cordeiro MF, Ribeiro SA, Protective role of free and quercetin-loaded nanoemulsion against damage induced by intracerebral haemorrhage in rats: Nanotechnology, 2016; 27(17); 175101
39. Antwi AO, Obiri DD, Osafo N, Stigmasterol modulates allergic airway inflammation in guinea pig model of ovalbumin-induced asthma: Mediators Inflamm, 2017; 2017 2953930
40. Yang YL, Cheng X, Li WH, Kaempferol attenuates LPS-induced striatum injury in mice involving anti-neuroinflammation, maintaining BBB integrity, and down-regulating the HMGB1/TLR4 pathway: Int J Mol Sci, 2019; 20(3); 491
41. Sales-Campos H, Souza PR, Peghini BC, An overview of the modulatory effects of oleic acid in health and disease: Mini Rev Med Chem, 2013; 13(2); 201-10
42. Liu ZK, Ng CF, Shiu HT, Neuroprotective effect of Da Chuanxiong Formula against cognitive and motor deficits in a rat controlled cortical impact model of traumatic brain injury: J Ethnopharmacol, 2018; 217; 11-22
43. Lili W, Yehong S, Qi Y: Fitoterapia, 2013; 85; 144-53
44. Hu X, Tao C, Gan Q, Oxidative stress in intracerebral hemorrhage: Sources, mechanisms, and therapeutic targets: Oxid Med Cell Longev, 2016; 2016 3215391
45. Sheth KN, Rosand J, Targeting the immune system in intracerebral hemorrhage: JAMA Neurol, 2014; 71(9); 1083-84
46. Lin X, Tang Y, Sun B, Cerebral glucose metabolism: Influence on perihematomal edema formation after intracerebral hemorrhage in cat models: Acta Radiol, 2010; 51(5); 549-54
47. Wang HC, Lin WC, Lin YJ, The association between serum adhesion molecules and outcome in acute spontaneous intracerebral hemorrhage: Crit Care, 2011; 15(6); R284
48. Zhang Y, Yi B, Ma J, Quercetin promotes neuronal and behavioral recovery by suppressing inflammatory response and apoptosis in a rat model of intracerebral hemorrhage: Neurochem Res, 2015; 40(1); 195-203
49. Dong YS, Wang JL, Feng DY, Protective effect of quercetin against oxidative stress and brain edema in an experimental rat model of subarachnoid hemorrhage: Int J Med Sci, 2014; 11(3); 282-90
50. Li S, Zhang ZQ, Wu LJ, Understanding ZHENG in Traditional Chinese Medicine in the context of neuro-endocrine-immune network: IET Syst Biol, 2007; 1(1); 51-60
51. Qureshi AI, Mendelow AD, Hanley DF, Intracerebral haemorrhage: Lancet, 2009; 373(9675); 1632-44
52. Ren C, Guingab-Cagmat J, Kobeissy F, A neuroproteomic and systems biology analysis of rat brain post intracerebral hemorrhagic stroke: Brain Res Bull, 2014; 102; 46-56
53. Ye L, Gao L, Cheng H, Inflammatory profiles of the interleukin family and network in cerebral hemorrhage: Cell Mol Neurobiol, 2018; 38(7); 1321-33
54. Gris T, Laplante P, Thebault PCanadian Critical Care Translational Biology Group, Innate immunity activation in the early brain injury period following subarachnoid hemorrhage: J Neuroinflamm, 2019; 16(1); 253
55. Jiang C, Wang Y, Hu Q, Immune changes in peripheral blood and hematoma of patients with intracerebral hemorrhage: FASEB J, 2020; 34(2); 2774-91
56. Yang JT, Lee TH, Lee IN, Dexamethasone inhibits ICAM-1 and MMP-9 expression and reduces brain edema in intracerebral hemorrhagic rats: Acta Neurochir (Wien), 2011; 153(11); 2197-203
57. Dang B, Duan X, Wang Z, A therapeutic target of cerebral hemorrhagic stroke: Matrix metalloproteinase-9: Curr Drug Targets, 2017; 18(12); 1358-66
58. Hernandez-Guillamon M, Martinez-Saez E, Delgado P, MMP-2/MMP-9 plasma level and brain expression in cerebral amyloid angiopathy-associated hemorrhagic stroke: Brain Pathol, 2012; 22(2); 133-41
59. Wu J, Hua Y, Keep RF, Oxidative brain injury from extravasated erythrocytes after intracerebral hemorrhage: Brain Res, 2002; 953(1–2); 45-52
60. Sugiyama T, Imai T, Nakamura S, A novel Nrf2 activator, RS9, attenuates secondary brain injury after intracerebral hemorrhage in sub-acute phase: Brain Res, 2018; 1701; 137-45
61. Xie RX, Li DW, Liu XC, Carnosine attenuates brain oxidative stress and apoptosis after intracerebral hemorrhage in rats: Neurochem Res, 2017; 42(2); 541-51
62. Liu DL, Zhao LX, Zhang S, Du JR, Peroxiredoxin 1-mediated activation of TLR4/NF-kappaB pathway contributes to neuroinflammatory injury in intracerebral hemorrhage: Int Immunopharmacol, 2016; 41; 82-89
63. Lan X, Han X, Li Q, Wang J, (−)-Epicatechin, a natural flavonoid compound, protects astrocytes against hemoglobin toxicity via Nrf2 and AP-1 signaling pathways: Mol Neurobiol, 2017; 54(10); 7898-907
64. Wang Z, Fang L, Shi H, Yang Z, miR-181b regulates ER stress induced neuron death through targeting Heat Shock Protein A5 following intracerebral haemorrhage: Immunol Lett, 2019; 206; 1-10
65. Zhao Y, Wei ZZ, Zhang J, GSK-3beta inhibition induced neuroprotection, regeneration, and functional recovery after intracerebral hemorrhagic stroke: Cell Transplant, 2017; 26(3); 395-407
66. Senn R, Elkind MS, Montaner J, Potential role of blood biomarkers in the management of nontraumatic intracerebral hemorrhage: Cerebrovasc Dis, 2014; 38(6); 395-409
67. Jung S, Moon KS, Jung TY, Possible pathophysiological role of vascular endothelial growth factor (VEGF) and matrix metalloproteinases (MMPs) in metastatic brain tumor-associated intracerebral hemorrhage: J Neurooncol, 2006; 76(3); 257-63
68. Xu S, Wu Q, Guo G, Ding X, The protective effects of urocortin1 against intracerebral hemorrhage by activating JNK1/2 and p38 phosphorylation and further increasing VEGF via corticotropin-releasing factor receptor 2: Neurosci Lett, 2015; 589; 31-36
69. Wang JP, Zhang MY, Role for target of rapamycin (mTOR) signal pathway in regulating neuronal injury after intracerebral hemorrhage: Cell Physiol Biochem, 2017; 41(1); 145-53
70. Zhang Z, Liu Y, Huang Q, NF-kappaB activation and cell death after intracerebral hemorrhage in patients: Neurol Sci, 2014; 35(7); 1097-102
71. Shen X, Ma L, Dong W, Autophagy regulates intracerebral hemorrhage induced neural damage via apoptosis and NF-kappaB pathway: Neurochem Int, 2016; 96; 100-12
72. Chen S, Zhao L, Sherchan P, Activation of melanocortin receptor 4 with RO27-3225 attenuates neuroinflammation through AMPK/JNK/p38 MAPK pathway after intracerebral hemorrhage in mice: J Neuroinflammation, 2018; 15(1); 106
73. Gong L, Manaenko A, Fan R, Osteopontin attenuates inflammation via JAK2/STAT1 pathway in hyperglycemic rats after intracerebral hemorrhage: Neuropharmacology, 2018; 138; 160-69
74. Liu S, Liu X, Chen S, Neutrophil-lymphocyte ratio predicts the outcome of intracerebral hemorrhage: A meta-analysis: Medicine, 2019; 98(26); e16211
75. Rolland WB, Lekic T, Krafft PR, Fingolimod reduces cerebral lymphocyte infiltration in experimental models of rodent intracerebral hemorrhage: Exp Neurol, 2013; 241; 45-55
76. Zhang F, Ren Y, Fu W, Predictive accuracy of neutrophil-to-lymphocyte ratio on long-term outcome in patients with spontaneous intracerebral hemorrhage: World Neurosurg, 2019; 125; e651-57
Figures
 Figure 1. Gene ontology analysis of the putative targets of YQHXD. Candidate targets for YQHXD were analyzed based on Omicshare to shed more light on their possible roles in diverse biological processes (denoted in red), molecular function (denoted in blue), and cell component (denoted in green). The significance threshold was set at P≤0.05, and those GO terms enriched were identified by hypergeometric test. Thereafter, those terms in the same category were ranked based on their P-values, with those on the left being of higher significance. The gene number involved in each term is presented in the y-axis.
Figure 1. Gene ontology analysis of the putative targets of YQHXD. Candidate targets for YQHXD were analyzed based on Omicshare to shed more light on their possible roles in diverse biological processes (denoted in red), molecular function (denoted in blue), and cell component (denoted in green). The significance threshold was set at P≤0.05, and those GO terms enriched were identified by hypergeometric test. Thereafter, those terms in the same category were ranked based on their P-values, with those on the left being of higher significance. The gene number involved in each term is presented in the y-axis. Figure 2. Construction of the YQHXD compound-putative target network. The active compounds (compounds ID) collected based on diverse herbal medicines were linked with corresponding candidate targets to construct the compound-target network, in which a node indicates an active compound (the various colored triangles stand for diverse herbal medicines) and the target (red dot). HQ – Astragali Radix; DG – Angelicae Sinensis Radix; TR – Persicae Semen; HH – Carthami Flos; DL – Pheretima; CS – Paeoniae Radix Rubra; CX – Chuanxiong Rhizoma; BZ – Angelicae Dahuricae Radix; XX – Asari Radix Et Rhizoma; SZ – Hirudo; GC – Glycyrrhizae Radix et Rhizoma.
Figure 2. Construction of the YQHXD compound-putative target network. The active compounds (compounds ID) collected based on diverse herbal medicines were linked with corresponding candidate targets to construct the compound-target network, in which a node indicates an active compound (the various colored triangles stand for diverse herbal medicines) and the target (red dot). HQ – Astragali Radix; DG – Angelicae Sinensis Radix; TR – Persicae Semen; HH – Carthami Flos; DL – Pheretima; CS – Paeoniae Radix Rubra; CX – Chuanxiong Rhizoma; BZ – Angelicae Dahuricae Radix; XX – Asari Radix Et Rhizoma; SZ – Hirudo; GC – Glycyrrhizae Radix et Rhizoma. Figure 3. Candidate targets identification. YQHXD shared 199 candidate targets with the identified targets for ICH related to the pathological process. The targets that overlapped were identified based on Omicshare and show their roles in various GO (A) and KEGG (B) terms. The significance threshold was set at P≤0.05, and the terms enriched were identified by hypergeometric test. (C) Flow chart showing the process of selecting potential targets. In the cPPI network, hubs with higher degree than the median among all network nodes were extracted. In addition, main hubs (candidate targets) were mined by calculating 5 topological features.
Figure 3. Candidate targets identification. YQHXD shared 199 candidate targets with the identified targets for ICH related to the pathological process. The targets that overlapped were identified based on Omicshare and show their roles in various GO (A) and KEGG (B) terms. The significance threshold was set at P≤0.05, and the terms enriched were identified by hypergeometric test. (C) Flow chart showing the process of selecting potential targets. In the cPPI network, hubs with higher degree than the median among all network nodes were extracted. In addition, main hubs (candidate targets) were mined by calculating 5 topological features. Figure 4. Enrichment analysis based on ClueGO and labeling of vital terms of the group. Partial overlaps were observed in groups that are functionally related. Typical interactions among biological processes or pathways are enriched (P<0.05) across the major targets of YQHXD. (A) Possible enriched targets of YQHXD in typical biological processes. (B) Possible enriched targets of YQHXD in typical signaling pathways.
Figure 4. Enrichment analysis based on ClueGO and labeling of vital terms of the group. Partial overlaps were observed in groups that are functionally related. Typical interactions among biological processes or pathways are enriched (P<0.05) across the major targets of YQHXD. (A) Possible enriched targets of YQHXD in typical biological processes. (B) Possible enriched targets of YQHXD in typical signaling pathways. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








