05 August 2020: Clinical Research
Are There Lower Complication Rates with Bidirectional Barbed Suture in Total Knee Arthroplasty Incision Closure? A Randomized Clinical Trial
Shuo Feng1ABCDE, Ye Zhang1ABCDE, Feng Zhang2CE, Zhi Yang1AC, Xiang-Yang Chen1ADEF*, Guo-Chun Zha1ADEFDOI: 10.12659/MSM.922783
Med Sci Monit 2020; 26:e922783
Abstract
BACKGROUND: The use of barbed suture in total knee arthroplasty (TKA) remains controversial. We performed a prospective study to investigate the clinical outcomes of bidirectional barbed suture for incision closure in TKA.
MATERIAL AND METHODS: We conducted a single-center, randomized controlled trial to determine the efficiency and safety of barbed suture in TKA at our institution between December 2017 and April 2019. Eligible patients were randomly assigned to different suture methods for skin closure. Randomization was conducted via computerized randomization list. Our primary endpoint was the incidence of wound complications within 3 months of surgery. This trial was registered at ClinicalTrials.gov, number ChiCTR-IPR-17013677.
RESULTS: A total of 582 patients were enrolled, consisting of 193 who received full-layer barbed suture (group A), 195 who received barbed suturing of the joint capsule (group B), and 194 who received suturing of the joint capsule by traditional absorbable suture (group C). The incidence of incision complications in group A (19.7%) was significantly higher than that in group B (7.2%) and C (9.3%) (P<0.0125). The incidence rate for incision complications in group B was similar to that in group C (P>0.0125). The time for incision closure in groups A (13.5±2.0 min) and B (16.1±1.9 min) was significantly shorter than that in group C (25.0±2.0 min) (P<0.001).
CONCLUSIONS: The use of full-thickness bidirectional barbed suture for incision closure after TKA may increase postoperative incision complications, and therefore is not recommended. However, the use of barbed suture for the joint capsule has shown effectiveness, reducing suture time with no increase in incision complications.
Keywords: Arthroplasty, Replacement, Knee, Postoperative Complications, Sutures, Body Mass Index, Follow-Up Studies, Incidence, Joint Capsule, Knee Joint, operative time, Prospective Studies, Surgical Wound, Suture Techniques
Background
Meticulous wound closure is the integral and final step of a successful total knee arthroplasty (TKA). However, its importance is often overlooked. Improper suturing methods may lead to wound-healing problems that could increase the risk of infection. Operative time is a risk factor for postoperative infection, with a 9% increased risk per 15 min increment [1].
The use of knotless, barbed sutures to close the incision and facilitate rapid closure and soft-tissue repair in abdominoplasty and plastic surgery is recommended, as they reduce postoperative incision complications and decrease surgery time in these contexts [2,3]. However, in TKA and unicompartmental knee arthroplasty (UKA), barbed sutures can increase postoperative incision complications, including effusion, superficial infection, deep infection, dehiscence, and skin necrosis [4,5]. Previous studies have used barbed sutures to suture the joint capsule, as well as subcutaneous and intracutaneous tissues, without skin staples to strengthen the suture. The results of these studies indicate that the cutting action generated by barbed suture displacement may cut the skin during knee joint motion. This phenomenon would serve to increase problems with incision healing. To explore the advantages of barbed sutures with improved surgical outcomes, we tested a method of using sutures for the joint capsule and subcutaneous tissues while utilizing staples for the skin.
We hypothesized that the use of bidirectional barbed sutures for the joint capsule, traditional absorbable sutures for subcutaneous tissues, and staples for skin closure would reduce TKA operation time without increasing the incidence of incision healing, compared with the use of full-layer barbed sutures (joint capsule, subcutaneous, and intracutaneous tissues sutured by barbed sutures) or traditional absorbable suture (joint capsule and subcutaneous tissues sutured by absorbable sutures, staples used for skin closure).
Material and Methods
STUDY DESIGN AND PARTICIPANTS:
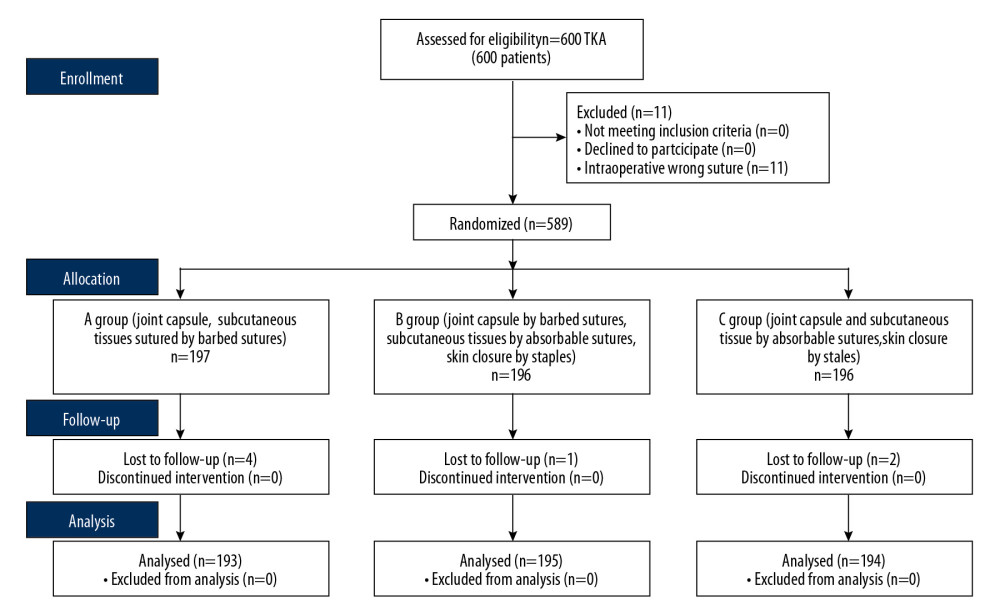
A single-center, randomized controlled trial was conducted to compared the new method with two different wound closure techniques in unilateral primary TKA. The protocol can be accessed in the Chinese Clinical Trial Registry. Acquired informed consent can be viewed in the supplemental content. These procedures comply with the regulations of the Affiliated Hospital of Xuzhou Medical University. Our research complies with the ethical standards of the National Research Council and the 1964 Helsinki Declaration. This study was approved by our institutional review board (XYFY2017-JS004-05). All patients provided informed consent. Our work has been reported in line with Consolidated Standards of Reporting Trials (CONSORT) guidelines. This study is registered at ClinicalTrials.gov, number ChiCTR-IPR-17013677. Figure 1 shows the CONSORT flow diagram.
The inclusion criteria were as follows: (1) patients with knee-joint degenerative arthritis, (2) patients approved for an initial unilateral joint replacement, and (3) patients able to receive surgery performed by a highly qualified operator. The exclusion criteria included the following: (1) patients with neurovascular diseases of the affected limbs, (2) patients with a history of surgery at the operative site, and (3) patients with body mass index (BMI) >30 kg/m2.
RANDOMIZATION AND MASKING:
Based on the selection and exclusion criteria, from December 2017 to January 2019, we prospectively collected clinical data for 600 patients treated with primary total knee arthroplasty. This number reflected the expected number of registrations and exits in our region. Each participant was randomized by lot [1: 1: 1] to one of three suture methods using a concealed block size of 6. The random list was generated by computer. The random envelope method was adopted for grouping concealment. Each grouping scheme was placed into an envelope according to the coding order, and the coding was written on the outside of the envelope, which was saved by the researcher. Before the incision was closed, the nurse selected a random envelope which provided the suture method. The surgeons, nurses, and all other team members were not blinded to the three groups. The Orthopedic Data Center was responsible for treatment allocation and statistical analysis under the supervision of a competent statistician and all analysts were masked to treatment allocation.
SURGICAL PROCEDURE:
All patients were supine on the operating table and under general anesthesia. A tourniquet was used at the base of the thigh during surgery. We used a median incision in the knee joint that extended medially to the side of the patella. A posterior-stabilizing bone cement prosthesis was implanted in all patients using the same joint replacement technique. While the incision was sutured, the knee joint was bent at 45°. A drainage tube was placed in the incision.
Group A: the joint capsule (Stratafix1-0), subcutaneous tissues (Stratafix2-0), and intracutaneous tissues (Stratafix3-0) were sutured using a bi-directional barbed suture. At the end, an extra 4–5 stitches were made to avoid detachment and incision rupture.
Group B: the joint capsule was sutured by bi-directional barbed suture (Stratafix1-0) and subcutaneously sutured using a traditional absorbable suture (Ethicon VICRYL* Plus 2-0). The skin was sutured by staples.
Group C: the joint capsule was sutured by a traditional absorbable suture (Ethicon VICRYL* Plus 1-0), and the subcutaneous tissue was sutured by an absorbable suture (Ethicon VICRYL* Plus 2-0). The skin was sutured by staples.
A mixture of tranexamic acid solution (tranexamic acid 1.5 g in 50 ml of normal saline) was poured into the articular cavity from the drainage tube after the joint capsule was sutured. The joint was then bent and stretched to check for suture closeness. If the liquid outflowed, then intermittent sutures were made at the exudation site. The tourniquet was released after the incision suture and bandaging.
POSTOPERATIVE TREATMENT: All patients underwent the same postoperative management. Patients received a single intravenous (IV) dose of prophylactic antibiotics before the operation and 24 h after surgery. The standard dose was 2 g dicloxacillin or 1.5 g cefuroxime, depending on the patient’s allergy status. The drainage tube was removed 48 h after the operation. Active and passive functional exercise was performed after removal of the drainage tube. Hemoglobin and other blood laboratory tests were conducted 3 days after the operation. Low molecular weight heparin was injected subcutaneously. The dressing was changed every 2 days under strict sterile conditions during the inpatient stay. Superficial infection was defined in accordance with CDC criteria for superficial incisional surgical site infection [6]. A diagnosis of deep infection was based on the MSIS criteria and required operative management and/or IV antibiotics in our cohorts [7]. The patients diagnosed with deep infection and skin margin necrosis were successfully treated with debridement of devitalized tissue, extensive washout, wound vacuum-assisted closure (VAC) therapy and required operative management, 6 weeks of IV antibiotics, and 6 months of oral antibiotic therapy. Superficial infections were all successfully treated with oral antibiotics. We defined hematoma as a palpable mass in the knee cavity requiring surgical removal or decompression [8]. Hematoma was successfully treated with oral antibiotics, wound VAC, and surgical intervention.
DATA COLLECTION:
Preoperative and postoperative clinical data were evaluated by an independent senior surgeon blinded to the patient’s randomization. Incision length, suture time, operation time, hospital stay length, and incision complications (such as effusion, infection, hematoma, and skin necrosis) were recorded. Knee Society Scores (KSS) were collected preoperatively and 3 months postoperatively. No changes were made to trial protocols after the trial commenced.
STATISTICAL ANALYSIS:
Data processing was performed using SPSS 22.0 statistical software, and data were expressed as mean ± standard deviation (x±s). Data were compared between groups using the following analyses: Quantitative data were compared using analysis of variance and nonparametric analysis. Qualitative data were compared using the chi-square test. Data quantification was assessed with the L-S-D test (if the variance is not equal, the corrected Welch’s ANOVA is adopted). Enumeration data were assessed for significance with the chi-square test (α=0.05). P<0.05 indicated statistical significance. Chi-square test for pairwise comparison: corrected inspection level α’=0.0125.
Results
A total of 600 patients (600 TKAs) were invited to take part in this research. Eleven patients were excluded because of an intraoperative wrong suture being used. Seven patients were lost to follow-up. Finally, 582 knees were included for analysis. A total of 193 TKAs were assigned to group A, 195 to group B, and 194 to group C. Figure 1 shows the CONSORT flow diagram.
Group A was composed of 53 males and 140 females, aged 64.8±8.7 years on average, with an average BMI of 24.1±2.7 kg/m2. Preoperative hemoglobin was 133.9±9.3 g/L, and plasma albumin was 39.5±1.7 g/L.
Group B was composed of 49 males and 146 females, 66.0±9.2 years on average, with an average BMI of 24.4±2.9 kg/m2. Preoperative hemoglobin was 135.1±9.7 g/L, and plasma albumin was 39.6±1.7 g/L.
Group C was composed of 54 males and 140 females, aged 65.0±8.7 years on average, with an average BMI of 24.0±2.7 kg/m2. Preoperative hemoglobin was 133.8±8.3 g/L, and plasma albumin was 39.4±1.4 g/L.
No statistically significant differences were observed between the three groups in the preoperative general data, including gender, age, BMI, preoperative hemoglobin, preoperative plasma albumin, or KSS (P>0.05, Table 1). The patients’ details are shown in Table 1.
Preoperative and postoperative (3 months) KSS were compared for the three groups (Table 2). No differences were observed between the groups for preoperative or postoperative clinical and functional knee scores (P>0.05).
Tables 3 and 4 show the clinical outcomes and complications, respectively, in the three groups. The operation times for group A (70.0±4.3 min) and group B (78.2±4.7 min) were significantly less than that for group C (87.1±5.0 min) (P<0.001, Tables 3, 5). The suture speed improved significantly after application of the barbed suture in groups A and B. This difference was statistically significant (P<0.001, Tables 3, 5). No statistically significant differences were observed in the hemoglobin and plasma albumin levels among the three groups 3 days after surgery (P>0.05). There was no statistical difference in length of hospital stay (P>0.05).
Significant differences were noted in the incidence rate of complications between the three groups (P<0.001, Table 4). The rate (19.7%) of complications in group A was higher than those in groups B (7.2%) and C (9.3%). Multiple comparisons showed statistically significant differences (P<0.0125; Table 5). However, no statistically significant differences in the rate of complications were observed between groups B and C (P=0.347; Table 5). Significant differences were observed in superficial infection between the three groups (P=0.008; Table 4). Nineteen patients experienced superficial infection in group A (9.8%). This number was higher than that in group B (six patients with superficial infection, 3.1%) and group C (eight patients, 4.1%). Thus, the results of multiple comparisons showed statistically significant differences between group A and groups B in superficial infection (P<0.0125; Table 5). No differences were found in the incidence rate of other complications, such as effusion, blisters, hematoma, skin edge necrosis, or deep infections, among the three groups (P>0.05; Table 4).
Discussion
The TKA wound is traditionally sutured by intermittent knots using common sutures. However, the knotting is time consuming. Improper suturing may lead to iatrogenic damage and other complications. The pressure of the knotted sutures may be uneven, leading to tissue ischemia. The absorption of large knots may lead to severe local tissue inflammation and potential infectious lesions. TKA offers a high postoperative survival rate and desirable long-term efficacy. However, the highest rates of surgery for the treatment of postoperative wound problems are related to wound infection (21.9%), wound hematoma (13.9%), and wound necrosis (14.3%) [9]. Galat [10] noted that wound complications are inextricably linked to long-term sequelae of TKA. After 5 years, the risks of deep prosthetic infection or infection requiring an additional major surgical treatment reach 6.0% and 5.3%, respectively. Therefore, effective and safe closure of incisions is critical to increase surgical efficiency and prevent infections in patients. With ongoing developments in material biology, progress has been achieved in the improved design of sutures. Barbed sutures have tiny barbs that are uniformly distributed on the surface. This novel suturing device with a self-anchorage system can maintain tissue tension and requires no knotting after the sutures are strained [11,12]. Additionally, no retraction occurs in the sutures following suturing [11,13]. Thus, this approach has been recently introduced for orthopedics.
This analysis showed no significant differences in the incidence rate of complications between the joint capsule barbed suture group (group B, 7.2%) and the traditional absorbable suture group (group C, 9.3%). These numbers are consistent with previous reports by Ting [14] and Gililland [15,16] on the incidence rate of complications in the deep joint capsule tissue caused by barbed sutures. Thus, the incidence rate of complications caused by barbed sutures is not higher than that caused by absorbable sutures for the suturing of the joint capsule and the retinaculum layer. In addition, the suturing tension of the barbed sutures can meet the requirements for postoperative joint functional exercise [15]. However, Campbell [4] and Patel [17] reported that the use of barbed sutures increases the incidence rate of complications when used for subcutaneous tissue and fascia. Our research results were consistent with this trend. Nineteen patients had superficial infections in the full-layer barbed suture group (group A, 9.8%). This number was higher than those in the joint capsule barbed suture group (six patients, 3.1%) and the traditional absorbable suture group (nine patients, 4.1%).These differences may indicate that the increase in superficial infections was associated with the suturing of the intracutaneous and subcutaneous tissue using barbed sutures. To explain this situation, Smith [18] and Williams [19] reported that this phenomenon is common during the period of the initial “learning curve” of new physicians. The barbed suture is excessively tight with a high tension, possibly leading to avascular necrosis of the tissue. Therefore, some scholars [20] have proposed that barbed sutures should not be used to suture the skin and the subcutaneous tissue under high tension following TKA. The skin edges should match, and the vertical mattress pattern suture may be utilized to reduce complications, such as postoperative skin edge necrosis. Thread residues could be left on the body surface when barbed sutures are used to suture such regions as the intracutaneous region. These thread residues may facilitate the growth of bacteria, leading to infection [21,22]. It has been observed that a large range of motion of the knee joint is possible during rehabilitation following TKA. The cutting action generated by barbed suture displacement may increase the risk of wound infection and is common in UKA [5]. Some other scholars [13,22–24] have also proposed that the design of the barbed suture can easily lead to infections if the barbs can trap fiber from the towel and gauze and increase the surface of the sutures. Hence, bacteria can accumulate substantially under the barbs. However, this mechanism has not been analyzed
The incidence rate of postoperative complications in the patients that received the barbed sutures only for the joint capsule (group B) was lower than that in the full-layer barbed suture group (group A). Group B also exhibited efficiency, safety, and effectiveness throughout the procedure. The suture times for the full-layer barbed suture group (group A) (13.5±2.0 min) and joint capsule-only barbed suture group (group B) (16.1±1.9 min) were shorter than that for the traditional absorbable suture group (group C) (25.0±2.0 min). This phenomenon could lead to a difference in the operation time among the three groups, with a result of 7–12 min less operation time in the barbed suture groups. Namba [1] reported that the decrease in surgery time reduces the risk of infection following total knee replacement. A TKA surgery time of more than 210 min significantly increases the risk of infection compared with surgery lasting less than 120 min, and the risk of infection at the deep operation site increases by 9% for each extension of operation time by 15 min (95% confidence interval, 4–13%) [1]. Peersman et al. [25] also evaluated the relationship between the duration of surgery and postoperative infections and found that 127 min is the critical duration for prediction of prosthesis infection following total knee joint replacement. Long TKA surgery duration would also prolong the time that the tourniquet is used and increase the intraoperative dominant blood loss, inevitably reducing blood circulation in the lower limbs. Prolonged reduced blood circulation can promote local ischemia and anoxia of the knee joints, necrosis of adipocytes, declined immunity of the skin and subcutaneous tissues, inhibition of wound healing, and additional complications, such as fat liquefaction and sterile exudation [26,27]. The application of barbed sutures allows rapid closure of incisions, thus helping to decrease operation time, intraoperative dominant blood loss, and infection risk at the operation site [15,18].
This study also has some limitations. First, the use of bidirectional barbed sutures was only assessed for TKA. Therefore, we cannot assume that the complications associated with barbed suture in TKA are similar to those in other plastic surgeries. Second, this study excluded obese patients with BMI values higher than 30 kg/m2 because this condition can increase incision complications [28,29]. Third, although the conclusions should be theoretically credible because the clinical data were collected in a prospective manner with a large number of cases, the follow-up duration was relatively short. Thus, we cannot conclude whether this technique will achieve reliable long-term results. Fourth, this study did not compare the cost of different suture methods. Barbed suture costs more than traditional absorbable suture. However, with the support of domestic health insurance policies, patients may pay only half of the cost or even less. Therefore, the cost for patients who use different suture methods is approximately the same.
Conclusions
We do not recommend the use of full-thickness barbed sutures for primary TKA. Although these barbed sutures can shorten the suture time, they can increase postoperative incision complications. However, the use of bidirectional barbed suture for the joint capsule has shown effectiveness, reducing the suture time with no increase in incision complications.
References
1. Namba RS, Inacio MC, Paxton EW, Risk factors associated with deep surgical site infections after primary total knee arthroplasty: An analysis of 56,216 knees: J Bone Joint Surgery Am, 2013; 95(9); 775-82
2. Lee SW, Nomura E, Tokuhara T, Laparoscopic technique and initial experience with knotless, unidirectional barbed suture closure for staple-conserving, delta-shaped gastroduodenostomy after distal gastrectomy: J Am Coll Surg, 2011; 213(6); e39-45
3. Rosen AD, Use of absorbable running barbed suture and progressive tension technique in abdominoplasty: A novel approach: Plast Reconstr Surg, 2010; 125(3); 1024-27
4. Campbell AL, Patrick DA, Liabaud B, Geller JA, Superficial wound closure complications with barbed sutures following knee arthroplasty: J Arthroplasty, 2014; 29(5); 966-69
5. Chawla H, van der List JP, Fein NB, Barbed suture is associated with increased risk of wound infection after unicompartmental knee arthroplasty: J Arthroplasty, 2016; 31(7); 1561-67
6. Mangram AJ, Horan TC, Pearson ML, Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee: Infect Control Hosp Epidemiol, 1999; 20(4); 250-78 quiz 279–80
7. Parvizi J, Zmistowski B, Berbari EF, New definition for periprosthetic joint infection: from the Workgroup of the Musculoskeletal Infection Society: Clin Orthop Relat Res, 2011; 469(11); 2992-94
8. Idestrup C, Sawhney M, Nix C, Kiss A, The incidence of hematoma formation in patients with continuous femoral catheters following total knee arthroplasty while receiving rivaroxaban as thromboprophylaxis: An observational study: Reg Anesth Pain Med, 2014; 39(5); 414-17
9. Jamsen E, Huhtala H, Puolakka T, Moilanen T, Risk factors for infection after knee arthroplasty. A register-based analysis of 43,149 cases: J Bone Joint Surg Am, 2009; 91(1); 38-47
10. Galat DD, McGovern SC, Larson DR, Surgical treatment of early wound complications following primary total knee arthroplasty: J Bone Joint Surg Am, 2009; 91(1); 48-54
11. Olweny EO, Park SK, Seideman CA, Self-retaining barbed suture for parenchymal repair during laparoscopic partial nephrectomy; Initial clinical experience: BJU Int, 2012; 109(6); 906-9
12. Vakil JJ, O’Reilly MP, Sutter EG, Knee arthrotomy repair with a continuous barbed suture: A biomechanical study: J Arthroplasty, 2011; 26(5); 710-13
13. Shermak MA, Mallalieu J, Chang D, Barbed suture impact on wound closure in body contouring surgery: Plast Reconstr Surg, 2010; 126(5); 1735-41
14. Ting NT, Moric MM, Della Valle CJ, Levine BR, Use of knotless suture for closure of total hip and knee arthroplasties: A prospective, randomized clinical trial: J Arthroplasty, 2012; 27(10); 1783-88
15. Gililland JM, Anderson LA, Barney JK, Barbed versus standard sutures for closure in total knee arthroplasty: A multicenter prospective randomized trial: J Arthroplasty, 2014; 29(9 Suppl); 135-38
16. Gililland JM, Anderson LA, Sun G, Perioperative closure-related complication rates and cost analysis of barbed suture for closure in TKA: Clin Orthop Relat Res, 2012; 470(1); 125-29
17. Patel RM, Cayo M, Patel A, Wound complications in joint arthroplasty: Comparing traditional and modern methods of skin closure: Orthopedics, 2012; 35(5); e641-46
18. Smith EL, DiSegna ST, Shukla PY, Matzkin EG, Barbed versus traditional sutures: Closure time, cost, and wound related outcomes in total joint arthroplasty: J Arthroplasty, 2014; 29(2); 283-87
19. Williams SB, Alemozaffar M, Lei Y, Randomized controlled trial of barbed polyglyconate versus polyglactin suture for robot-assisted laparoscopic prostatectomy anastomosis: technique and outcomes: Eur Urol, 2010; 58(6); 875-81
20. Boopalan PR, Daniel AJ, Chittaranjan SB, Managing skin necrosis and prosthesis subluxation after total knee arthroplasty: J Arthroplasty, 2009; 24(2); 322.e23-7
21. Helling ER, Okpaku A, Wang PT, Levine RA, Complications of facial suspension sutures: Aesthet Surg J, 2007; 27(2); 155-61
22. Hammond DC, Barbed sutures in plastic surgery: A personal experience: Aesthet Surg J, 2013; 33(3 Suppl); 32S-39S
23. Cortez R, Lazcano E, Miller T, Barbed sutures and wound complications in plastic surgery: An analysis of outcomes: Aesthet Surg J, 2015; 35(2); 178-88
24. Hurwitz DJ, Reuben B, Quill barbed sutures in body contouring surgery: A 6-year comparison with running absorbable braided sutures: Aesthet Surg J, 2013; 33(3 Suppl); 44S-56S
25. Peersman G, Laskin R, Davis J, Prolonged operative time correlates with increased infection rate after total knee arthroplasty: HSS J, 2006; 2(1); 70-72
26. Vince K, Chivas D, Droll KP, Wound complications after total knee arthroplasty: J Arthroplasty, 2007; 22(4 Suppl 1); 39-44
27. Vince KG, Abdeen A, Wound problems in total knee arthroplasty: Clin Orthop Relat Res, 2006; 452; 88-90
28. Adhikary SD, Liu WM, Memtsoudis SG, Liu J: J Arthroplasty, 2016; 31(4); 749-53
29. Winiarsky R, Barth P, Lotke P, Total knee arthroplasty in morbidly obese patients: J Bone Joint Surg Am, 1998; 80(12); 1770-74
Figures
Tables
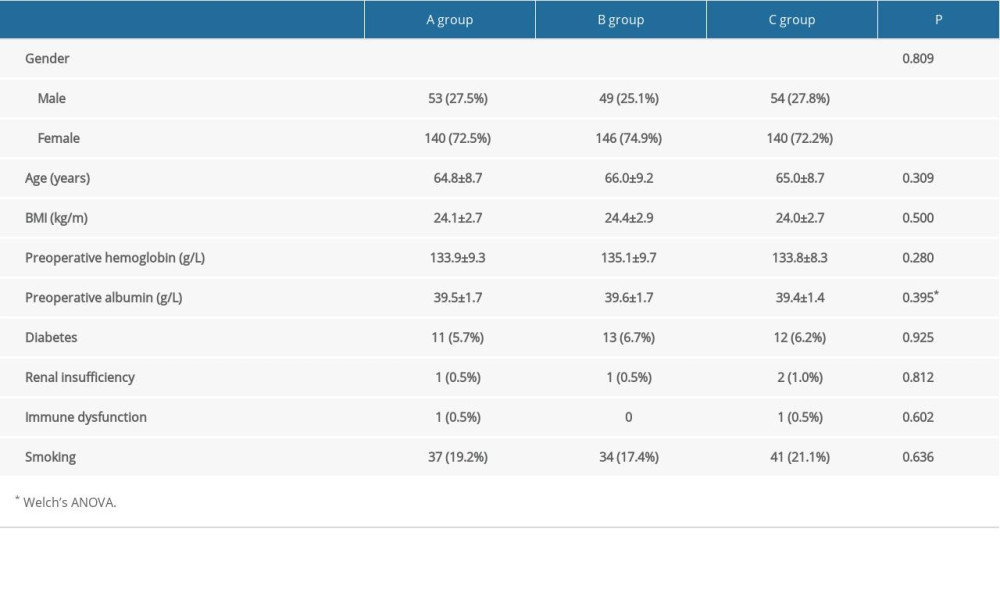 Table 1. Patient demographics of three groups.
Table 1. Patient demographics of three groups.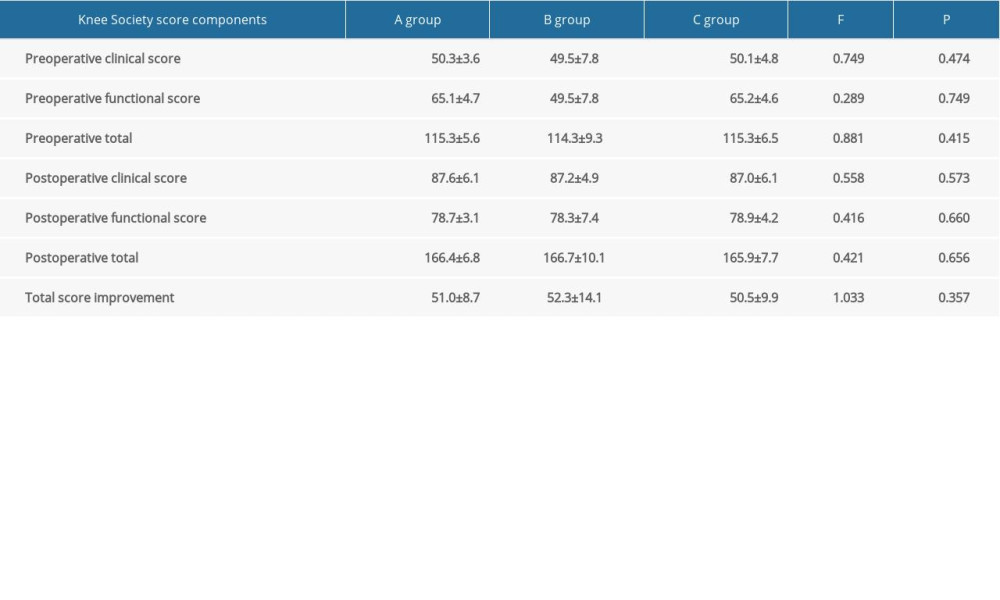 Table 2. Knee Society scores.
Table 2. Knee Society scores.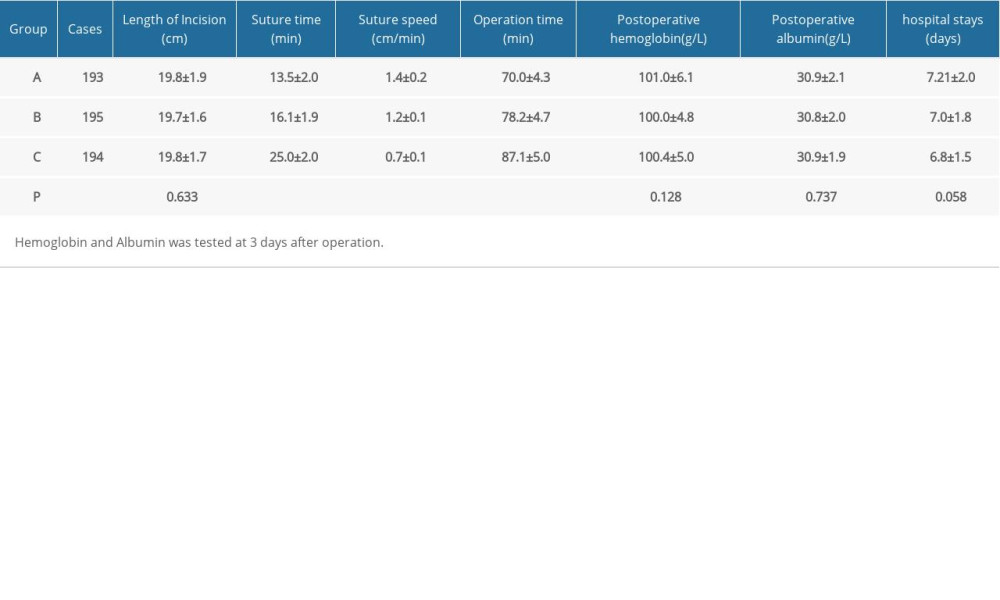 Table 3. Clinical outcomes of three groups.
Table 3. Clinical outcomes of three groups.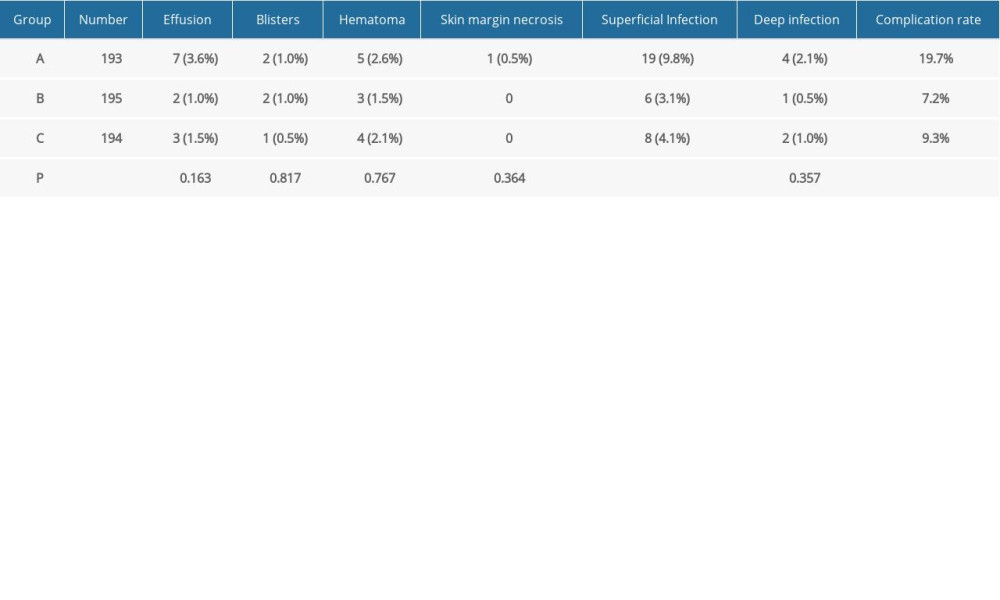 Table 4. Complicatio ns of three groups.
Table 4. Complicatio ns of three groups.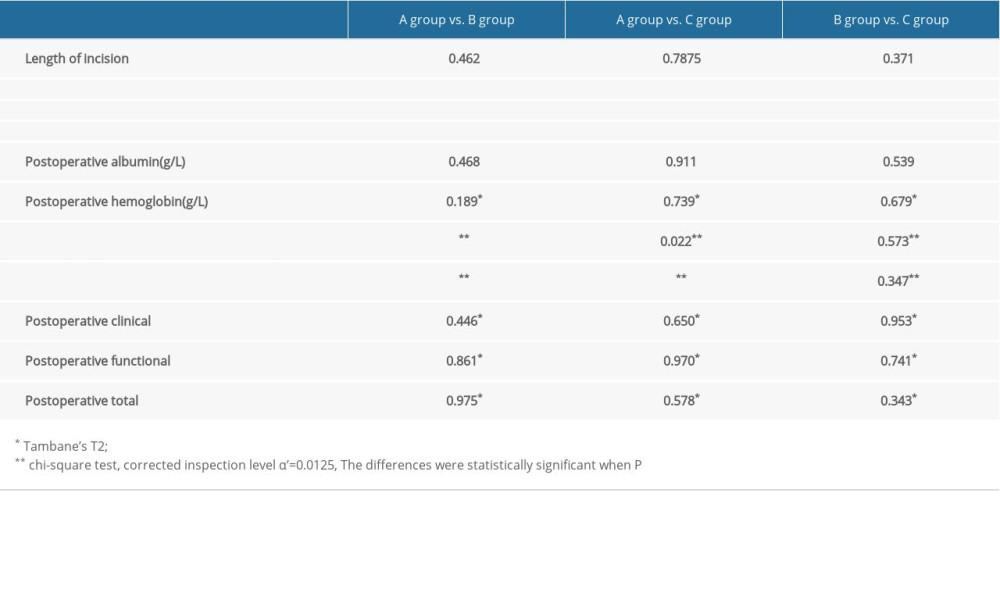 Table 5. Comparison of results.
Table 5. Comparison of results. Table 1. Patient demographics of three groups.
Table 1. Patient demographics of three groups. Table 2. Knee Society scores.
Table 2. Knee Society scores. Table 3. Clinical outcomes of three groups.
Table 3. Clinical outcomes of three groups. Table 4. Complicatio ns of three groups.
Table 4. Complicatio ns of three groups. Table 5. Comparison of results.
Table 5. Comparison of results. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387