10 September 2020: Clinical Research
Clinical Outcomes of Atlantoaxial Dislocation Combined with Osteoporosis Using Posterior Atlantoaxial Rod, Screw Fixation, and Posterior Interfacet Fusion: A Retrospective Study of 21 Cases
Qingfeng Shen1BE, Yingpeng Xia1A*, Tiantong Xu1BCDDOI: 10.12659/MSM.925187
Med Sci Monit 2020; 26:e925187
Abstract
BACKGROUND: Surgical procedures on atlantoaxial dislocation combined with osteoporosis remain controversial. This study was established to assess the mid-term clinical outcomes of atlantoaxial dislocation combined with osteoporosis using posterior atlantoaxial rod, screw fixation and posterior interfacet fusion.
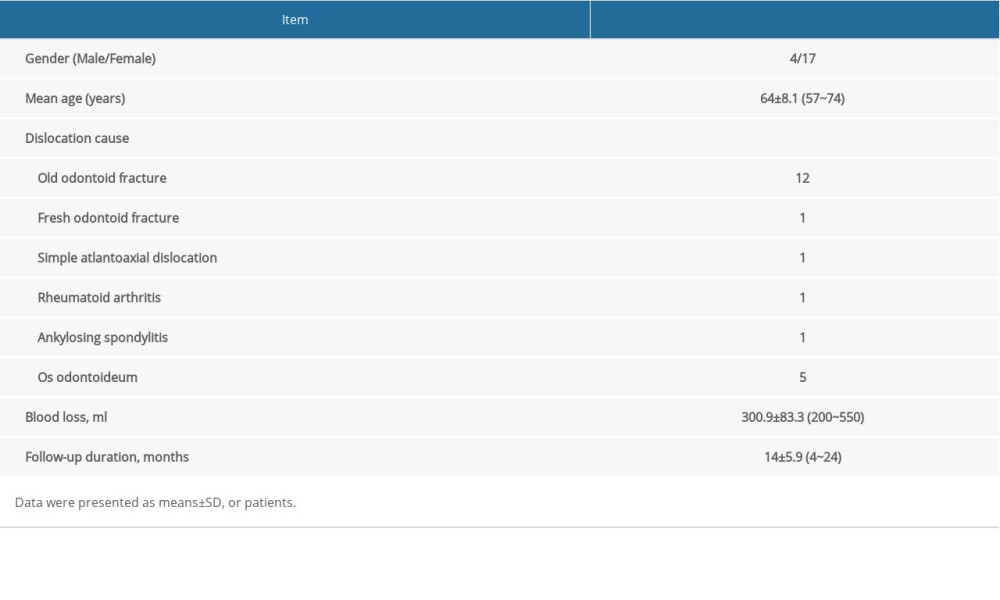
MATERIAL AND METHODS: From January 2017 to January 2020, 21 patients (4 males and 17 females) with coexisting atlantoaxial dislocation and osteoporosis who underwent posterior atlantoaxial rod and screw fixation were included in our study with an average age of 64±8.1 years (range, 57–74 years). The subjective and objective symptoms, together with the neurological function of the patients were measured. Radiography and magnetic resonance imaging (MRI) were performed, Japanese Orthopaedic Association (JOA) score for spinal cord function and VAS score for pain recovery was assessed.
RESULTS: JOA and visual analog scale (VAS) score were significantly improved at 14±5.9 month follow-up compared with pretreatment values. Complete or almost complete anatomical reduction was observed in all 21 patients. All patients had good bony fusion at the final follow-up. No screw-loosening or atlantoaxial redislocation occurred in 21 cases. The only complication was mild numbness in the C2 innervation area of the posterior occipital region in 6 cases, which had no effect on life.
CONCLUSIONS: The results suggested that posterior atlantoaxial rod, screw fixation system, and posterior interfacet fusion could achieve satisfactory initial results for the treatment of atlantoaxial dislocation combined with osteoporosis.
Keywords: Aftercare, Atlanto-Axial Joint, Osteoporosis, Bone Screws, Joint Dislocations, Prostheses and Implants, Spinal Fusion
Background
Atlantoaxial dislocation refers to the loss of a normal anatomical articulation between the articular surface of atlas (C1) and the axis (C2) caused by congenital malformation, trauma, degeneration, inflammation, or surgery, resulting in joint dysfunction and neurological dysfunction [1–3]. The unique position of the odontoid process, rising between the ring of the atlas ventrally, together with the transverse atlantal ligament dorsally and the C1–C2 lateral mass joints are the major factors preventing dislocation of C1–C2 [1], with any disruption in the integrity of these structures predisposing to atlantoaxial dislocation development [4–6]. Although uncommon, atlantoaxial dislocation can be linked with complicated deformities of the cranio-vertebral junction and represent a potential for serious clinical consequences, including respiratory failure, cervical myelopathy, or even death [7,8]. According to the etiology, atlantoaxial dislocation can be classified as traumatic, spontaneous, and congenital [1]. Based on the reducibility, atlantoaxial dislocation can be further divided into reducible and irreducible [2].
The treatment of atlantoaxial dislocation requires reduction and decompression while taking appropriate measures to maintain the stability of the atlantoaxial vertebra. Traditional Gallie, Brooks, Apofix laminar clamps and other techniques are relatively simple to operate, but because of the risk of spinal cord injury and poor biomechanical stability, it is tough to meet the needs of clinical rigid treatment. Since Goel and Laheri [9] reported the posterior atlantoaxial plate and screw fixation system in 1994, the clinical problem that the posterior atlantoaxial fixation is not strong enough and the technical operation is complex and dangerous has been solved. In recent years, many surgeons have used posterior approaches for atlantoaxial dislocation treatment and have achieved good clinical outcomes [10–12].
Earlier studies have indicated that pedicle screw fixation is highly related to the bone mineral density [13–15]. Osteoporotic patients are prone to loosening of internal fixation [16], which leads to non-fusion and failure of operation. In the special field of atlantoaxial joint, once the operation fails, it is even more difficult to perform the revision surgery [17]. Therefore, despite multiple effective surgical approaches and techniques have been developed for atlantoaxial dislocation, pedicle screw fixation remains a challenge for orthopedic surgeons in an osteoporotic spine. As far as we know, reports about the treatment of patients with coexisting atlantoaxial dislocation and osteoporosis are still lacking nowadays.
In view of these situations, this paper retrospectively observed the treatment outcomes of 21 cases of atlantoaxial dislocation with osteoporosis admitted to our hospital from January 2017 to January 2020, the related problems in the treatment were also explored and discussed.
Material and Methods
PATIENT POPULATION:
We retrospectively collected the clinical data of patients with coexisting atlantoaxial dislocation and osteoporosis who underwent posterior atlantoaxial rod and screw fixation from January 2017 to January 2020. This study was approved by the Medical Ethics Committee of our hospital. Written informed consent was obtained from all patients (2020-B01, January 4, 2020).
Inclusion criteria of patients were: 1) reducible atlantoaxial dislocation/instability; 2) presence of neck pain or spinal cord compression; 3) bone mineral density (BMD) T-score <−2.5. Exclusion criteria included: 1) occipito-cervical deformity with stable atlantoaxial joint; 2) BMD T-score above −2.5; 3) patients who had atlantoaxial dislocation combined with other occipito-cervical deformities.
PREOPERATIVE PREPARATION:
After admission, a complete cervical radiographic examination was performed for each patient including MRI and a computed tomography (CT) scan. Before the operation, skull traction was performed for patients who had dislocation on lateral cervical radiographs in extension. Then, the traction was maintained for another week after traction reduction or partial reduction. Bedside lateral x-ray was then performed.
SURGICAL TECHNIQUES:
The patients received general anesthesia through nasal tracheal cannula, and were then placed in a supine position with skull traction. Throughout the sub-occipital posterior median approach, the posterior cervical muscles were dissected to expose the nail point. The screws were positioned under fluoroscopy. The central point of the posterior margin of the inferior articular process on C1 lateral mass was selected as the entry point. Place the 3.5 mm-diameter polyaxial screw (Medtronic Inc., Minneapolis, MN, USA) at an angle of about 15° upward and inward, with a depth of 26–30 mm. C2 pedicle screws were placed with the upper inner edge of the inferior articular process of the axis as the entry point, inclined 20° inward and upward, with a diameter of 3.5–4.0 mm and a length of 22–26 mm (Medtronic Inc., Minneapolis, MN, USA). The C2 laminar screws were placed by 5 mm from the central line of the spinous process and the upper edge of the vertebral lamina respectively, and the screws were extracted from the center point of the lower articular process on the opposite side. The angle of the screws was 25° anteriorly, 8° downwardly, and the length of the screw channel was 26–28 mm (Medtronic Inc., Minneapolis, MN, USA). After that, C2 nerve root was exposed and dissected, the atlantoaxial lateral mass joint was thoroughly exposed, and the ligament tissue of capsule wall attached to the edge of articular process was incised with a sharp knife and then entered the joint cavity. The articular cartilage was scraped by curette, and the joint was completely loosened by prying the articular surface. After the reduction of atlantoaxial joint by depressing the spinous process of the vertebra, a connecting rod of appropriate length and radian was then installed. C-arm x-ray fluoroscopy was used to check the condition of reduction, if unsatisfactory reduction was obtained, the connecting rod needs to be reshaped for further reduction. After satisfactory reduction, the posterior arch of atlas and the lamina of axis were polished. Then the posterior superior iliac crest was exposed, the bone cortex was cut through the bone window with a bone knife, and the cancellous bone granules were extracted from the posterior superior iliac crest with a curette. Next, the bone granules implanted in the atlantoaxial joint cavity were compacted with a bone graft rod (Medtronic Sofamor-Danek, Minneapolis, MN, USA), and the rest were implanted between the posterior arch of atlas and the lamina of axis. Finally, the wounds were rinsed and the incisions were closed. Drainage tube was placed in the incision.
POSTOPERATIVE MANAGEMENT:
All patients received intravenous antibiotics for 24 hours after operation. The drainage tube was removed on the second day. Patients were placed on strict bed rest for 3 days when pain relief and drain removal, and were then allowed to ambulate while wearing a hard cervical collar. Use of a cervical collar was continued until definite bone fusion occurs.
POSTOPERATIVE ASSESSMENT:
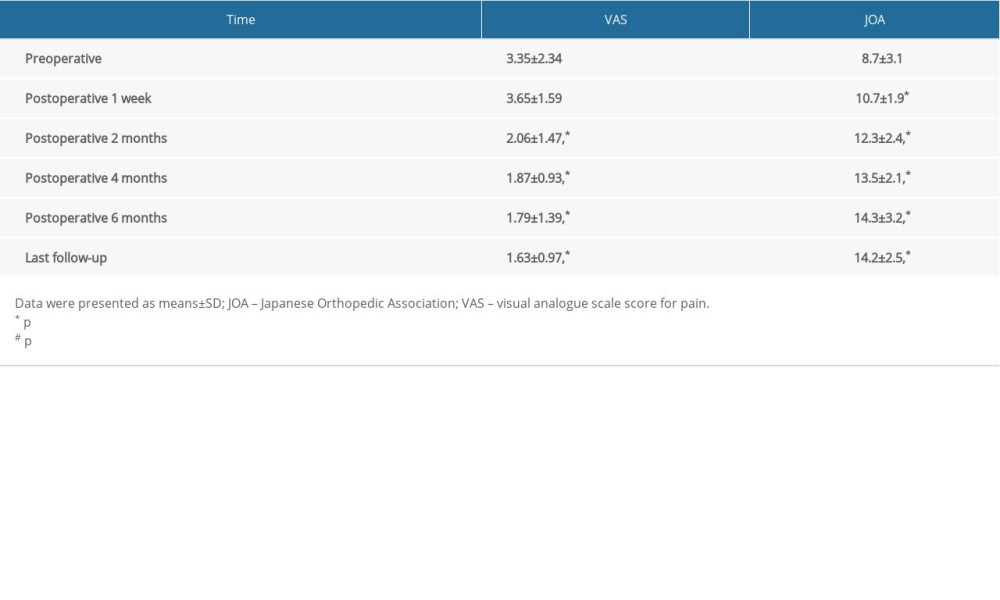
Postoperative x-ray, MRI, and reconstructive CT scan were performed to determine reduction, decompression, status of bone graft, and internal fixation at 7 days, 2, 4, 6, 9, and 12 months after surgery, and annually thereafter. JOA scores and VAS were assessed preoperatively, postoperatively, 1 week, 2, 4, and 6 months after surgery and last follow-up. Bone fusion was confirmed by continuous callus passing the interface between the graft and donor bone bed in CT sagittal reconstruction image.
STATISTICAL ANALYSIS:
The paired
Results
BASELINE DATA:
Four males and 17 females with an average age of 64±8.1 years (range, 57~74 years) were enrolled in our study. The causes of atlantoaxial dislocation were old odontoid fracture (n=12), fresh odontoid fracture (n=1), simple atlantoaxial dislocation (n=1) and rheumatoid arthritis (n=1), ankylosing spondylitis (n=1) and os odontoideum (n=5). Twenty patients had spinal cord compression and limb dysfunction; 1 patient only showed neck pain and limited movement. The BMD T-score of the patients were all less than −2.5 with a minimum value of −3.9. Four patients had osteoporotic fractures in other parts. General information of the patients is listed in Table 1.
FUNCTIONAL OUTCOMES:
The average followed-up time was 14±5.9 months (range, 4~24 months); the functional outcomes of the patients is presented in Table 2. JOA and VAS score were significantly improved at follow-up compared with pretreatment values (all P<0.05). Complete or almost complete anatomical reduction was noticed in all patients. All patients had good bony fusion at the final follow-up. Typical cases are shown in Figures 1 and 2.
COMPLICATIONS:
No fracture of screws or fixing rods was reported. No screw-loosening or atlantoaxial redislocation occurred in the 21 cases. Mild numbness occurred in the C2 innervation area of the posterior occipital region in 6 cases, which had no effect on the patients’ life.
Discussion
Atlantoaxial dislocation is a rare and potentially fatal disturbance of the normal atlantoaxial join [18,19]. At present, with the aggravation of aging and the increasing number of osteoporosis patients, the situation of internal fixation pull-out and surgical failure caused by osteoporosis has become even more prominent. In this study, preoperative skull traction and posterior atlantoaxial rod and screw fixation were used in combination with posterior interfacet fusion, and all cases had bone graft fusion. Improved VAS and JOA score were noticed at postoperative follow-up when compared to preoperative score.
Atlantoaxial dislocation, particularly in the setting of clinical symptoms, typically requires surgical intervention. Despite this consensus, the actual treatment has been less consistent. Several scholars have advocated preoperative skeletal traction to facilitate reduction [20,21], whereas others have used skeletal traction only during the surgical procedure [22,23]. In the current study, skull traction was conducted in patients with severe dislocation, un-reduction or incomplete reduction. Bedside lateral x-ray films were taken under traction and surgery was carried out 1 week later after the observation of dislocation reduction. This method is to reduce the stress of internal fixation and prevent the complications of screw loosening and pull-out caused by excessive stress of internal fixation during operation.
Although there are many kinds of internal fixation methods, including Gallie and Brooks titanium cable, Apofix laminectomy, Magerl screw, and Harms-Goel system (i.e., atlantoaxial pedicle screw and atlantoaxial laminectomy), the posterior atlantoaxial screw technology has become the current mainstream fixation scheme due to its good mechanical properties. In this technique, atlas and axis were respectively placed with screws, and then a strong posterior internal fixation system was formed by connecting the rods. At present, there are 2 main technologies of atlas screw placement: lateral mass screw as well as pedicle screw. Both of them can achieve good postoperative results for patients with normal bone density. However, because of the obvious biomechanical advantage of C1 pedicle screw compared with lateral mass screw [24], all cases in this study received pedicle screw fixation, and long screws should be selected to reach the anterior cortex as much as possible. For patients with posterior arch dysplasia (height <3.5 mm) who cannot complete the complete pedicle screw placement, semi embedded pedicle screw placement was performed to maximize the mechanical stability [25,26]. In cases which C2 pedicle screws cannot be applied due to severe high-riding vertebral artery, theoretically, laminar screws or isthmus screws can be used instead. However, due to the biomechanical advantages of laminar screws, all patients in this group use laminar screws instead. Bicortical laminar screws have achieved good clinical results in patients with normal bone structure [27]. The pedicle screw is fixed through the posterior, middle, and anterior columns of the axis, while the laminar screw is completely located in the posterior column of the axis, and only the posterior structure is fixed which is not strong enough to resist lateral bending of the cervical spine [28]. Therefore, it is necessary to ensure that at least one side has pedicle screws to ensure 3-column fixation and increase the lateral bending strength so as to achieve strong fixation.
Conventional patients with atlantoaxial dislocation can achieve good fusion results only by posterior interlamina fusion [29]. However, for posterior atlantoaxial lamina fusion, only the surface of posterior arch and lamina of atlantoaxial can be used as the bone graft bed, and the surface of the bone graft is cortical bone. Therefore, after fixation and reduction, the bone graft bed should be fully prepared by grinding or biting off the bone cortex and exposing the cancellous bone or blood oozing on the bone surface. In order to increase the certainty of fusion in patients with osteoporosis, posterior interfacet fusion was carried out at least one side at the same time of interbody fusion. Similar to anterior cervical interbody graft, posterior interfacet fusion can be performed between atlantoaxial lateral masses, which bear a certain compression load, and the contact area of the graft is large, so it is more conducive to the fusion of the graft. One study has reviewed 87 patients with atlantoaxial dislocation who underwent atlantoaxial lateral mass fusion, and the success rate of postoperative fusion was as high as 100% [30]. In addition, we reduced the difficulty of reduction by further atlantoaxial release during the operation. At the same time, good release can also reduce the stress of postoperative internal fixation [31], thereby increasing the probability of successful surgery. In this study, C2 nerve root was dissected while the patients underwent atlantoaxial lateral mass joint release and bone graft fusion. Although theoretically C2 nerve root sectioning would cause skin numbness in occipital region, Elliott et al. [32] and Kang et al. [33] suggested that the lateral mass joint cavity could be fully exposed after C2 nerve root sectioning, which was beneficial for screw placement, reduction and even bone graft fusion, and patients would not have related complaints after surgery. Similar to the aforementioned results, only 6 patients complained of mild numbness in the C2 innervation area at the posterior occipital region, which had no effect on their life. For the patients with normal bone, some scholars have doubts about the necessity of external fixation after posterior fixation, but the external fixation fixture can indeed reduce cervical vertebra activity and improve the fusion rate [33]. Therefore, patients in our study were required to wear the cervical brace strictly after operation until there is clear evidence of fusion. Due to the application of posterior interfacet fusion, the strong fusion is generally obtained 2 to 4 months after operation.
C2 nerve root is involved in the composition of occipital small nerve, auricular great nerve and cervical transverse nerve, so we try to keep the integrity of C2 nerve root at least on one side during the operation. In this group, only 5 patients had loose C2 nerve roots on one side and the course was upward, so the C1–C2 joint process could be released and bone graft fusion could be completed without cutting off. In the other 16 patients, C2 nerve roots on both sides significantly affected the release of C1–C2 and the implementation of bone grafting. Therefore, we choose to cut off the C2 nerve root on one side with a smaller diameter to complete the bone graft fusion between the articular processes, keep the integrity of the C2 nerve root on the other side, and did not do the C1–C2 release and bone graft fusion. This study had some limitations. Firstly, the retrospective design had its inherent limitations of such study. Secondly, only 21 patients were observed in our study because of the strict inclusion criteria. The sample size was small, which may have influenced the results in this study. Another limitation in our study was the short follow-up period and lack of a control group. Therefore, further studies with large samples are needed to elucidate the long-term clinical outcomes of patients with coexisting atlantoaxial dislocation and osteoporosis.
Conclusions
Despite the aforementioned limitations, our results proved that preoperative skull traction and posterior atlantoaxial rod and screw fixation combined with posterior interfacet fusion could achieve satisfactory initial results for the treatment of atlantoaxial dislocation combined with osteoporosis.
Figures
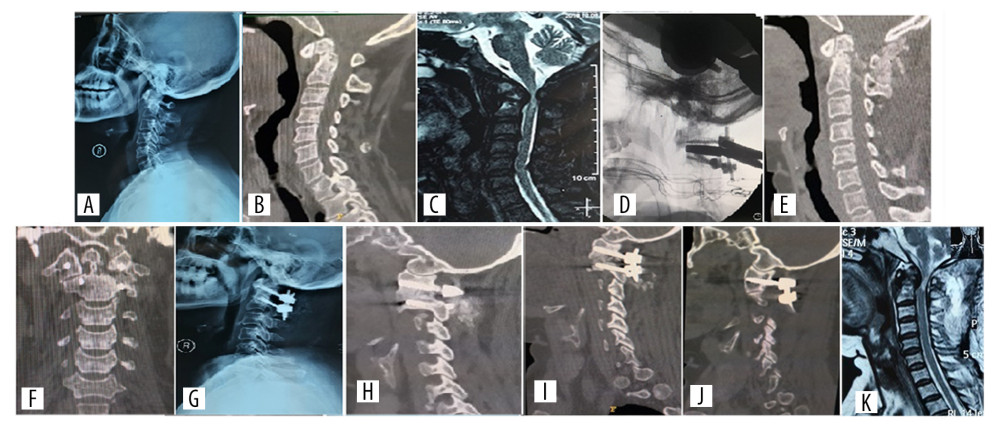 Figure 1. Preoperative, intra-operative, postoperative, 1 week and 9 weeks follow-up radiographs of a patient who had atlantoaxial dislocation caused by an old odontoid fracture treated with posterior atlantoaxial rod and screw fixation. (A–C) X-ray, CT, and MRI before the posterior atlantoaxial rod and screw fixation. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E–G) CT and x-ray at 1 week after operation. (H) CT at 9 weeks after operation showed that strong fusion has been formed between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging.
Figure 1. Preoperative, intra-operative, postoperative, 1 week and 9 weeks follow-up radiographs of a patient who had atlantoaxial dislocation caused by an old odontoid fracture treated with posterior atlantoaxial rod and screw fixation. (A–C) X-ray, CT, and MRI before the posterior atlantoaxial rod and screw fixation. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E–G) CT and x-ray at 1 week after operation. (H) CT at 9 weeks after operation showed that strong fusion has been formed between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging. 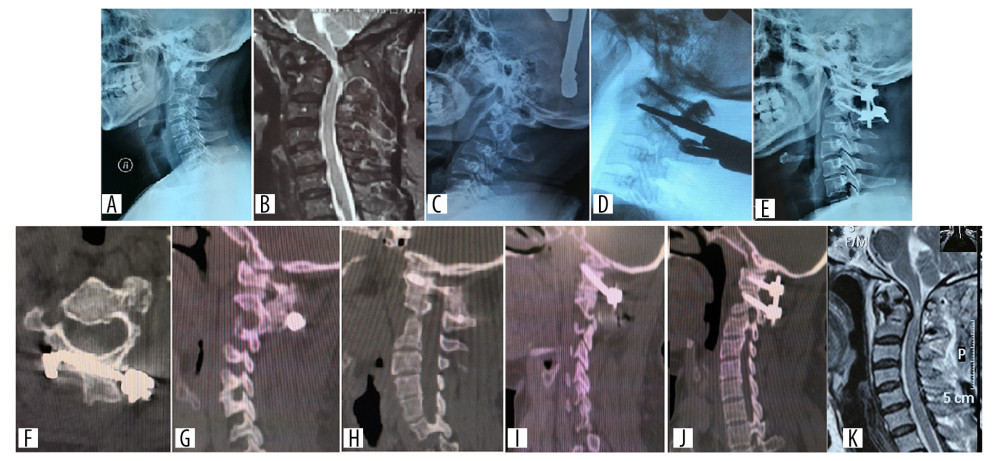 Figure 2. Preoperative, postoperative, 1- and 8-week follow-up radiographs of a patient with anatomical variation and atlantoaxial dislocation caused by an old odontoid fracture, who was treated with C2 bicortical lamina screw fixation. (A, B) X-ray and MRI before the bicortical lamina screw fixation. (C) X-ray imaging showing the reduction of dislocation after skull traction. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E, F) Postoperative x-ray and CT imaging. (G) CT at 1 week after operation. (H) CT at 8 weeks after operation revealed strong fusion between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging.
Figure 2. Preoperative, postoperative, 1- and 8-week follow-up radiographs of a patient with anatomical variation and atlantoaxial dislocation caused by an old odontoid fracture, who was treated with C2 bicortical lamina screw fixation. (A, B) X-ray and MRI before the bicortical lamina screw fixation. (C) X-ray imaging showing the reduction of dislocation after skull traction. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E, F) Postoperative x-ray and CT imaging. (G) CT at 1 week after operation. (H) CT at 8 weeks after operation revealed strong fusion between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging. References
1. Greenberg AD, Atlanto-axial dislocations: Brain, 1968; 91; 655-84
2. Wang S, Wang C, Yan M, Novel surgical classification and treatment strategy for atlantoaxial dislocations: Spine, 2013; 38; E1348-56
3. Xu J, Yin Q, Xia H, New clinical classification system for atlantoaxial dislocation: Orthopedics, 2013; 36; e95-100
4. Gholve PA, Hosalkar HS, Ricchetti ET, Occipitalization of the atlas in children. Morphologic classification, associations, and clinical relevance: J Bone Joint Surg Am, 2007; 89; 571-78
5. Cremers MJ, Bol E, de Roos F, van Gijn J, Risk of sports activities in children with Down’s syndrome and atlantoaxial instability: Lancet, 1993; 342(8870); 511-14
6. Lourie H, Stewart WA, Spontaneous atlantoaxial dislocation. A complication of rheumatoid disease: N Engl J Med, 1961; 265; 677-81
7. Kumar R, Kalra SK, Mahapatra AK, A clinical scoring system for neurological assessment of high cervical myelopathy: Measurements in pediatric patients with congenital atlantoaxial dislocations: Neurosurgery, 2007; 61; 987-93 discussion 993–94
8. Reddy KR, Rao GS, Devi BI, Pulmonary function after surgery for congenital atlantoaxial dislocation: A comparison with surgery for compressive cervical myelopathy and craniotomy: J Neurosurg Anesthesiol, 2009; 21; 196-201
9. Goel A, Laheri V, Plate and screw fixation for atlanto-axial subluxation: Acta Neurochirurgica, 1994; 129; 47-53
10. Yin YH, Tong HY, Qiao GY, Yu XG, Posterior reduction of fixed atlantoaxial dislocation and basilar invagination by atlantoaxial facet joint release and fixation: Aa modified technique with 174 cases: Neurosurgery, 2016; 78; 391-400
11. Guo SL, Zhou DB, Yu XG, Posterior C1–C2 screw and rod instrument for reduction and fixation of basilar invagination with atlantoaxial dislocation: Eur Spine J, 2014; 23; 1666-72
12. Goel A, Kulkarni AG, Sharma P, Reduction of fixed atlantoaxial dislocation in 24 cases: technical note: J Neurosurg Spine, 2005; 2; 505-9
13. Hadjipavlou AG, Nicodemus CL, Al-Hamdan FA, Correlation of bone equivalent mineral density to pull-out resistance of triangulated pedicle screw construct: J Spinal Disord, 1997; 10; 12-19
14. Halvorson TL, Kelley LA, Thomas KA, Effects of bone mineral density on pedicle screw fixation: Spine, 1994; 19; 2415-20
15. Wittenberg RH, Shea M, Swartz DE, Importance of bone mineral density in instrumented spine fusions: Spine, 1991; 16; 647-52
16. Zhang QH, Tan SH, Chou SM, Effects of bone materials on the screw pull-out strength in human spine: Med Eng Phys, 2006; 28; 795-801
17. Tan M, Jiang X, Yi P, Revision surgery of irreducible atlantoaxial dislocation: A retrospective study of 16 cases: Eur Spine J, 2011; 20; 2187-94
18. Jain VK, Atlantoaxial dislocation: Neurol India, 2012; 60; 9-17
19. Yang SY, Boniello AJ, Poorman CE, A review of the diagnosis and treatment of atlantoaxial dislocations: Global Spine J, 2014; 4; 197-210
20. Nordt JC, Stauffer ES, Sequelae of atlantoaxial stabilization in two patients with Down’s syndrome: Spine, 1981; 6; 437-40
21. Hedequist D, Bekelis K, Emans J, Proctor MR, Single stage reduction and stabilization of basilar invagination after failed prior fusion surgery in children with Down’s syndrome: Spine, 2010; 35; E128-33
22. Goel A, Desai KI, Muzumdar DP, Atlantoaxial fixation using plate and screw method: A report of 160 treated patients: Neurosurgery, 2002; 51; 1351-56 discussion 1356–57
23. Wang C, Yan M, Zhou H, Atlantoaxial transarticular screw fixation with morselized autograft and without additional internal fixation: Technical description and report of 57 cases: Spine, 2007; 32; 643-46
24. Fensky F, Kueny RA, Sellenschloh K, Biomechanical advantage of C1 pedicle screws over C1 lateral mass screws: A cadaveric study: Eur Spine J, 2014; 23; 724-31
25. Zhang XL, Huang DG, Wang XD, The feasibility of inserting a C1 pedicle screw in patients with ponticulus posticus: A retrospective analysis of eleven patients: Eur Spine J, 2017; 26; 1058-63
26. Cao L, Yang E, Xu J, “Direct vision” operation of posterior atlantoaxial transpedicular screw fixation for unstable atlantoaxial fractures: A retrospective study: Medicine, 2017; 96; e7054
27. Gorek J, Acaroglu E, Berven S, Constructs incorporating intralaminar C2 screws provide rigid stability for atlantoaxial fixation: Spine, 2005; 30; 1513-18
28. Lapsiwala SB, Anderson PA, Oza A, Resnick DK, Biomechanical comparison of four C1 to C2 rigid fixative techniques: Anterior transarticular, posterior transarticular, C1 to C2 pedicle, and C1 to C2 intralaminar screws: Neurosurgery, 2006; 58; 516-21 discussion 521
29. Elliott RE, Tanweer O, Boah A, Atlantoaxial fusion with screw-rod constructs: Meta-analysis and review of literature: World Neurosurg, 2014; 81; 411-21
30. Ghostine SS, Kaloostian PE, Ordookhanian C, Improving C1–C2 complex fusion rates: An alternate approach: Cureus, 2017; 9; e1887
31. Yin YH, Qiao GY, Yu XG, Posterior realignment of irreducible atlantoaxial dislocation with C1–C2 screw and rod system: A technique of direct reduction and fixation: Spine J, 2013; 13; 1864-71
32. Elliott RE, Kang MM, Smith ML, Frempong-Boadu A, C2 nerve root sectioning in posterior atlantoaxial instrumented fusions: A structured review of literature: World Neurosurg, 2012; 78; 697-708
33. Kang MM, Anderer EG, Elliott RE, C2 nerve root sectioning in posterior C1–2 instrumented fusions: World Neurosurg, 2012; 78; 170-77
Figures
 Figure 1. Preoperative, intra-operative, postoperative, 1 week and 9 weeks follow-up radiographs of a patient who had atlantoaxial dislocation caused by an old odontoid fracture treated with posterior atlantoaxial rod and screw fixation. (A–C) X-ray, CT, and MRI before the posterior atlantoaxial rod and screw fixation. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E–G) CT and x-ray at 1 week after operation. (H) CT at 9 weeks after operation showed that strong fusion has been formed between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging.
Figure 1. Preoperative, intra-operative, postoperative, 1 week and 9 weeks follow-up radiographs of a patient who had atlantoaxial dislocation caused by an old odontoid fracture treated with posterior atlantoaxial rod and screw fixation. (A–C) X-ray, CT, and MRI before the posterior atlantoaxial rod and screw fixation. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E–G) CT and x-ray at 1 week after operation. (H) CT at 9 weeks after operation showed that strong fusion has been formed between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging. Figure 2. Preoperative, postoperative, 1- and 8-week follow-up radiographs of a patient with anatomical variation and atlantoaxial dislocation caused by an old odontoid fracture, who was treated with C2 bicortical lamina screw fixation. (A, B) X-ray and MRI before the bicortical lamina screw fixation. (C) X-ray imaging showing the reduction of dislocation after skull traction. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E, F) Postoperative x-ray and CT imaging. (G) CT at 1 week after operation. (H) CT at 8 weeks after operation revealed strong fusion between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging.
Figure 2. Preoperative, postoperative, 1- and 8-week follow-up radiographs of a patient with anatomical variation and atlantoaxial dislocation caused by an old odontoid fracture, who was treated with C2 bicortical lamina screw fixation. (A, B) X-ray and MRI before the bicortical lamina screw fixation. (C) X-ray imaging showing the reduction of dislocation after skull traction. (D) Intra-operative image of arthrolysis of atlantoaxial lateral mass. (E, F) Postoperative x-ray and CT imaging. (G) CT at 1 week after operation. (H) CT at 8 weeks after operation revealed strong fusion between the lateral mass joints. (I) One week after operation, CT showed the position of C1 pedicle screws on the left and right sides. (J, K) MRI at 1 week after operation showed that the compression of spinal cord has been relieved. CT – computed tomography; MRI – magnetic resonance imaging. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387