29 September 2020: Clinical Research
Use of the Gout Impact Scale to Evaluate Quality of Life in Chinese Subjects with Gout: A Cross-Sectional Study
Peidan Yang12CDE, Zhixin Chen23CDE, Yimin Talia Chen4EF, Minying Liu1BF, Mingying Zhang1BF, Xiangwei Yang1BF, Changsong Lin1ADF, Qiang Xu1ABDEFG*DOI: 10.12659/MSM.925593
Med Sci Monit 2020; 26:e925593
Abstract
BACKGROUND: To use a gout-specific quality of life (QoL) tool, the Gout Impact Scale (GIS), to evaluate characteristics of gout affecting QoL in subjects with gout.
MATERIAL AND METHODS: In this cross-sectional study, 169 individuals with gout completed the 24-item GIS and a general questionnaire regarding gout characteristics. The reliability and validity of the GIS were verified by Cronbach’s a and exploratory factor analysis, respectively. The impact of gout characteristics on the QoL of subjects with gout was assessed by stepwise multiple regression analysis.
RESULTS: The 169 subjects with gout included 149 (88.2%) men and 20 (11.8%) women, of median age 43 years. The reliability of the GIS was appropriate (0.84–0.90), except for Gout Medication Side Effects (0.69) and Unmet Gout Treatment Need (0.59). Exploratory factor analysis showed that construct validity was acceptable, with a cumulative variance contribution rate of 5 common factors of 70.09% and factor loading >0.5 between each pair of items of the GIS. Univariate analysis showed that male sex was positively correlated with Well-being During Attack (p<0.05), and that source of medical expenses, current cigarette use and drinking were significantly correlated with Unmet Gout Treatment Need (p<0.05 each). A family history of gout, gout flares, and attack frequency were significantly correlated with total GIS, Well-being During Attack, and Gout Concern during Attack (p<0.05 each). Multivariate analysis suggested that history of gouty arthritis, acute attack and attack frequency had a considerable impact on QoL (p<0.05 each).
CONCLUSIONS: The GIS showed acceptable reliability and validity in identifying associations between poor QoL and gout characteristics.
Keywords: gout, Health impact assessment, Asians, Cross-Sectional Studies, Quality of Life, Surveys and Questionnaires
Background
Gout is a painful, inflammatory form of arthritis, caused by abnormal metabolism of purines and the resulting accumulation of uric acid crystals within the joints and other tissues [1,2]. Estimates indicate that 1 to 3% of the Chinese population has gout [3], with the incidence rate gradually increasing [4,5]. Individuals with gout experience severe gout flares, chronic recurrent pain, and joint swelling, resulting in a reduction in their quality of life (QoL) [6,7], which is poorer in individuals with gout than in physically and mentally healthy persons [8]. The instruments currently used to assess QoL in subjects with gout include the Short-Form 36-item health status survey (SF-36) [9], the Health Assessment Questionnaire-Disability survey (HAQ-DI) [10], the World Health Organization Health-Related Quality of Life Scale (WHOQOL-BREF) [11], and the Gout Assessment Questionnaire 2.0 (GAQ 2.0) [12]. Studies have tended to use general instruments to evaluate the QoL of subjects with gout, but they are relatively insensitive and do not evaluate the effects of gout and the drugs used to treat it from the subject’s point of view [13]. Furthermore, little is known about Chinese subjects’ awareness of gout, treatment status, and treatment satisfaction.
The present study was designed to assess overall QoL in Chinese subjects with gout and to investigate the association between gout-related variables and QoL in this population. Self-reported outcomes were determined using the Gout Impact Scale (GIS), the main portion of the GAQ2.0 [14], and demographic and clinical characteristics were also collected.
Material and Methods
STUDY DESIGN AND STUDY POPULATION:
This cross-sectional, observational study recruited subjects with gout who were evaluated at the rheumatology clinic of the First Affiliated Hospital of Guangzhou University of Chinese Medicine from March 2018 to June 2019. Subjects were included if (1) they were aged >18 years and met the 2015 ACR-EULAR Gout Classification Criteria [15,16]; (2) they volunteered to complete the questionnaire; and (3) they had good reading comprehension and were able to communicate without difficulty. Subjects were excluded if they had been diagnosed with a mental illness or cognitive disorder. All participants provided written informed consent. The study protocol was approved by the Ethics Committee of the First Affiliated Hospital in Guangzhou University of Chinese Medicine (No. ZYYECK [2018] 172) and conformed to the principles of the Declaration of Helsinki.
QOL ASSESSMENT:
All participants completed the 24-item GIS in Chinese, which allowed them to describe the influence of gout on their QoL. The Chinese version of the GIS, which was copyrighted by Takeda Pharmaceuticals, was provided by Lionbridge Technologies [17]. The 24-item GIS includes 4 items addressing overall concerns about gout, 2 items addressing the side effects of gout medications, 3 items addressing, unmet treatment needs, 11 addressing patient well-being during gout attacks, and 4 items, addressing concerns about gout during goat attacks [18]. The first 3 dimensions assessed the overall effects of gout, whereas the last 2 dimensions evaluated the effects of gout onset. Each item was scored on a Likert 5-point scale [19], with participants rating their responses from “strongly agree” to “strongly disagree”, “all the time” to “never”, and “not at all” to “extremely”. The score for each participant on each dimension of the GIS was calculated. Scores ranged from 0 to 100, with higher scores indicating poorer condition.
DEMOGRAPHIC AND CLINICAL CHARACTERISTICS:
Demographic characteristics were recorded for each subject, including sex, age, body mass index (BMI), educational level, gross monthly income, sources of medical expenses, current cigarette use, and current drinking. Clinical characteristics included disease duration, family history of gout, baseline urate-lowering therapy (ULT), gout flares, and frequency of attacks over 6 months.
DATA COLLECTION:
Patients with gout were informed of the significance and purpose of the research by an investigator. If the participant became confused during the survey process, the investigator was available for consultation. Because this survey included a combination of electronic and paper questionnaires, patients unfamiliar with the operation of electronic devices could complete the questionnaires with the help of family members or the investigator. The content of the questionnaire was examined carefully before analysis. If there were any blank answers, the patient was contacted and asked to clarify the incomplete answers. Two researchers checked the details of the data.
STATISTICAL METHODS:
Demographic and clinical variables were analyzed by descriptive statistical methods. Categorical variables were reported as number and percentage, and continuous variables as median (inter-quartile range, IQR) or mean±standard deviation (SD). Cronbach’s alpha was used to determine the internal consistency of the GIS, with 0.7 or above considered acceptable. Exploratory factor analysis was used to test the construct validity of GIS, with a cumulative variance contribution rate >60% and factor loading >0.5 considered appropriate. A Kaiser-Meyer-Olkin (KMO) value >0.7 and a significance on Bartlett’s sphericity test <0.01 indicated that the data were suitable for factor analysis. Because the GIS score was not normally distributed, factors possibly influencing QoL were assessed by Spearman correlation coefficient analysis, the Mann-Whitney U-test, or the Kruskal-Wallis H-test. Variables found to be statistically significant were subsequently selected as independent variables, with GIS score being the dependent variable. Multiple linear stepwise regression analysis was performed to determine the relationships between significant variables and GIS scores. Each linear regression model used P-P plots and scatter plots to evaluate the residual and normal distribution of the dependent variables. All statistical analyses were performed using SPSS software, with p-values <0.05 being defined as statistically significant.
Results
STUDY CHARACTERISTICS:
Of the 174 subjects with gout recruited, 5 were excluded because of incomplete data or withdrew voluntarily, and 169 patients were analyzed. The effective response rate on the questionnaires was 97%. The 169 patients included 149 (88.2%) men and 20 (11.8%) women, of median age 43 years (IQR: 35–53.5 years) and median disease duration of 36 months (IQR: 12–71 months). At evaluation, 50% of the patients were currently experiencing an acute gout attack. Ninety-three (43.1%) patients had experienced 3 or more acute gout flares during the previous 6 months, and 98 (57.6%) had taken uric acid-lowering drugs. The demographic and clinical characteristics and the mean GIS summary scores of these patients are shown in Table 1.
ASSESSMENT OF QOL IN GOUT:
Median scores on GIS and its subscales ranged from 41.67 (Unmet Gout Treatment Needs) to 87.5 (Gout Concern Overall). These GIS scores indicated that participants had considerable concerns about their gout (87.5±25), the side effects of medications used to treat this condition (75±37.5) and acute gout attacks (75±25). Nevertheless, subjects regarded their drug therapy as effective and their health status during a gout flares as acceptable, as shown by the their scores on the “Unmet Gout Treatment Need” (41.67±11.67) and “Well-being During Attack” (43.18±21.86) subscales, both of which were below the scale mid-points. These results indicate that the overall QoL of Chinese patients with gout was generally moderate or below average (Table 1).
RELIABILITY OF THE GIS:
Evaluations of internal consistency showed that Cronbach’s α was 0.89 overall; 0.90 for the Gout Concern Overall dimension, 0.69 for the Gout Medications Side Effects dimension, 0.59 for the Unmet Gout Treatment Need dimension, 0.91 for the Well-being During Attack dimension, and 0.84 for the Gout Concern During Attack dimension. Thus, reliability was adequate for overall GIS (0.89) and for 3 of the subscales (0.84–0.90) (Table 2).
CONSTRUCT VALIDITY OF GIS:
Evaluation of construct validity showed that the KMO sampling was adequate, with a score of 0.86, and the approximate chi-squared value on Bartlett’s sphericity test was 2905.528 (df=276, p<0.01), indicating that the GIS scores were appropriate for exploratory factor analysis. The result of exploratory factor analysis suggested that 5 common factors with eigenvalues greater than 1 were retained. The cumulative variance contribution rate was 70.09%, and factor loading between each pair of items on the GIS was >0.5, indicating reasonable validity. The 5 principal components explained 32.10%, 17.11%, 9.79%, 5.85%, and 5.24%, respectively, of the variation in total evidence (Table 3).
CORRELATIONS BETWEEN QOL AND GOUT-RELATED VARIABLES:
Correlation analysis showed that male sex was significantly associated with Well-being During Gout Attacks (p=0.01), whereas sources of medical expenses, current cigarette use, and current drinking significantly correlated with Unmet Gout Treatment Need (p<0.05 each). Family history of gout, gout flares, and 6-month frequency of gout attacks were positively associated with Well-being During Attacks (p<0.01 each), Gout Concern During Attacks (p<0.05 each), and overall GIS scores (p<0.01 each) (Table 4).
STEPWISE MULTIPLE LINEAR REGRESSION:
Stepwise multiple linear regression analysis was performed to identify factors significantly associated with total GIS score and score on each subscale. Patients undergoing an acute gout attack were significantly more anxious than those who were not on overall concern about goat (r=7.73, p<0.01) and concern about gout during an attack (r=6.92, p<0.01), indicating that patients with gout flares had poorer QoL. Scores on unmet gout treatment needs were significantly higher in patients with than without frequent gout attacks (r=0.64, p<0.01) and gout flares (r=5.57, p<0.01), as well as being higher in current smokers than non-smokers (r=6.63, p<0.01). Scores on Well-being During Attacks were significantly higher in patients with than without a history of gouty arthritis (r=10.38, p<0.05), in patients who were than were not experiencing attacks (r=0.52, p<0.05) and in those with than without gout relapse (r=8.91, p<0.05), indicating that health status during an attack enhanced patient discontent. History of gout (r=24.43, p<0.05), acute gout attacks (r=31.56, p<0.05), and greater attack frequency (r=1.54, p<0.05) were positively correlated with poorer QoL, as shown by overall GIS scores (Table 5).
Discussion
QoL has been recognized as an important outcome of in subjects with gout, as shown in the UK Department of Health Trial and the Outcome Measures in Rheumatology Clinical Trial (OMERACT) [20,21]. Overall GIS was designed to estimate the influence of gout on mental and social function [22,23] and was the only gout-specific QoL measurement assessed during OMERACT [13], showing satisfactory reliability and validity in subjects with gout. The present cross-sectional study of 169 patients with gout in China used gout-specific QoL measurements to evaluate the association between QoL and gout characteristics. Overall, we observed that patients with gout had moderate or low QoL. Univariate analysis showed that male sex was positively correlated with well-being during an attack. Source of medical expenses, current smoking, and current drinking were significantly related to unmet gout treatment needs. Multiple linear regression analysis of factors associated with overall GIS indicated that history of gouty arthritis, acute gout attack, and attack frequency had significant effects on QoL.
We found that Cronbach’s α on the overall GIS was 0.89, with 3 subscales of the GIS also showing satisfactory internal consistency (0.84~0.90). In contrast, Cronbach’s α on the unmet gout treatment needs (0.59) and side effects of gout medications (0.69) subscales were lower. Similar results were observed in other studies. For example, an observational survey of 147 patients in the U.S.A. found that reliability was sufficient for the overall GIS (0.93) and 3 of its subscales (0.82~0.94), but not for the unmet gout treatment needs (0.62) and side effects of gout medication (0.32) subscales [19]. Another study, involving 308 patients with gout, showed that Cronbach’s α for the GIS was sufficient (0.76–0.94), but not for the side effects of gout medication (0.60) and unmet gout treatment needs (0.65) subscales [12]. Cronbach’s α for the GIS may increase as the number of items increase [24], suggesting that the low Cronbach’s α on the unmet gout treatment needs and side effects of gout medications may be due to their having fewer items (2 and 3, respectively).
The first study using the GIS to investigate the correlation between gout-related features and QoL found that attack frequency and serious pain episodes reduced the QoL of gout patients [8]. In contrast, objective indicators, such as the number of swollen and painful joints during gout flare, blood uric acid concentration, and gouty tophi, were not associated with patient QoL. Physician severity score and acute gout attack were found to correlate positively with total GIS score [18], as did unbearable pain and the severity of acute gouty arthritis [24]. Consistent with the above results, we found that gout flares and attack frequency were significantly associated with poor QoL. Unbearable pain during gout flare and more frequent attacks made patients more worried about physical impairment, loss of ability to work, and the burden of healthcare costs [12]. Patients with gout flares or frequent attacks were found to more likely experience depression and/or anxiety, which had an impact on their mental state [25].
Older men were found to be more susceptible to gouty arthritis, reducing their overall QoL [26,27]. Our findings also suggested that QoL was worse in men than in women during a gout attack. Alternatively, 17-β estradiol in women may regulate purine synthesis and uric acid metabolism, reducing uric acid levels. In contrast, estrogen in men may promote renal uric acid reabsorption and inhibit renal excretion of uric acid. In addition, because men generally participate more in social activities, they are more likely to drink alcohol and eat high-purine foods [28]. More interestingly, we found that current smoking, current alcohol consumption, and source of medical expenses correlated significantly with the Unmet Gout Treatment Need subscale. Alcohol drinking has been reported to play a role in the development of arthritis [29]. Alcohol intake increases purine and blood lactic acid contents, which inhibit renal excretion of uric acid [30]. The association between smoking and gout, however, is unclear. A recent meta-analysis showed that smoking was not involved in the risk of gout, but that continued smoking had negative health impacts on patients with gout [31]. Long disease duration and medical treatment are costly for inpatients and outpatients, especially those increasing the financial burden on gout patients lacking health insurance and reducing their QoL. The European League Against Rheumatism (EULAR) has recommended that pharmacologic therapy should be effectively combined with nonpharmacologic strategies [32]. Biannual serum urate monitoring may be safer and more cost-effective than no monitoring or annual monitoring [33]. Regular serum urate monitoring, along with health education about moderate drinking, smoking, and a low purine diet, may improve treatment compliance and the QoL of patients with acute gout flares [34].
The present study had several limitations. First, this was a single-center, cross-sectional study based on a specified point-in-time. Second, the GIS is a self-reported disease outcome instrument, which may result in recall bias and less objective results. Third, most of the patients with gout were from the clinic of the First Affiliated Hospital of Guangzhou University, a clinic that accepts more patients with severe symptoms. Therefore, patients with less obvious symptoms who did not frequently visit this clinic were not included. Finally, our sample size was relatively small and consisted of Chinese patients, suggesting that our findings may not be applicable to other ethnic groups.
Conclusions
The present study found that the GIS, a gout-specific instrument, had acceptable validity and reliability to reflect the QoL of patients with gout. Overall GIS score showed significant positive correlations with a family history of gout, acute gout flares, and the frequency of gout attacks, indicating that these factors reduce patient QoL. Proper monitoring and health education may strengthen the management of gout.
Tables
Table 1. Baseline characteristics of gout patients.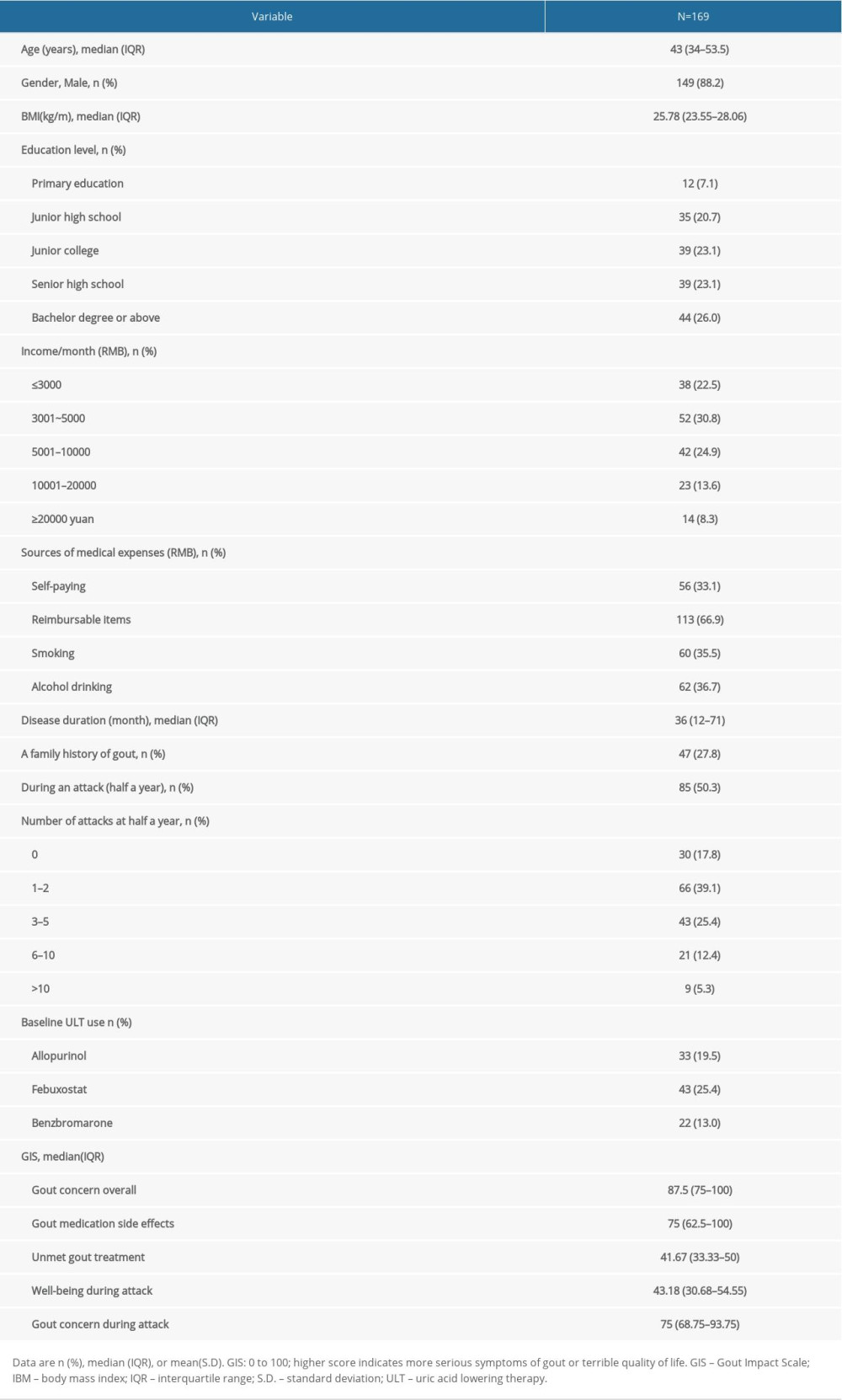 Table 2. Internal consistency analysis of the Gout Impact Scale.
Table 2. Internal consistency analysis of the Gout Impact Scale.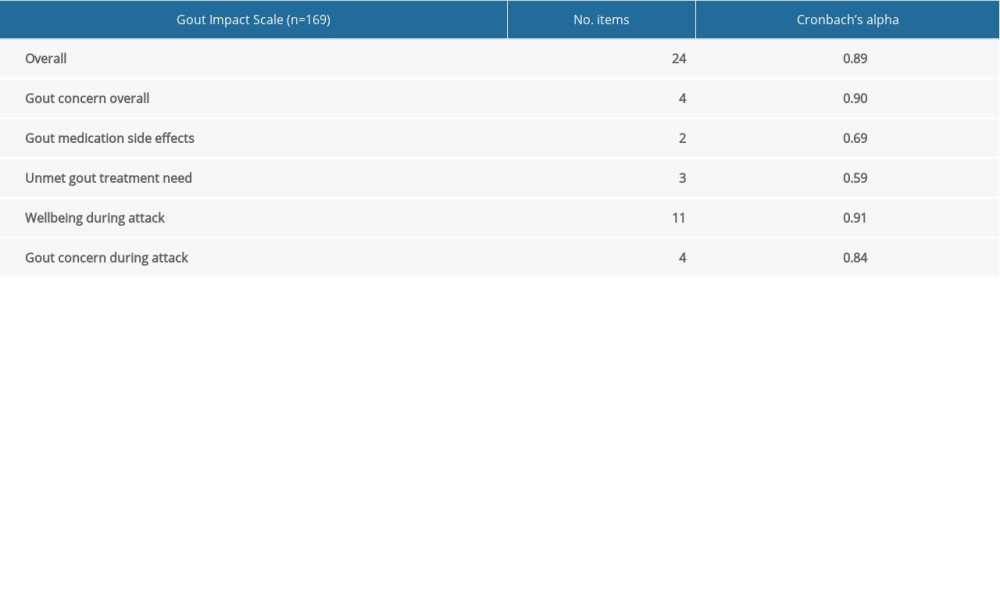 Table 3. Exploratory factor analysis of the Gout Impact Scale.
Table 3. Exploratory factor analysis of the Gout Impact Scale.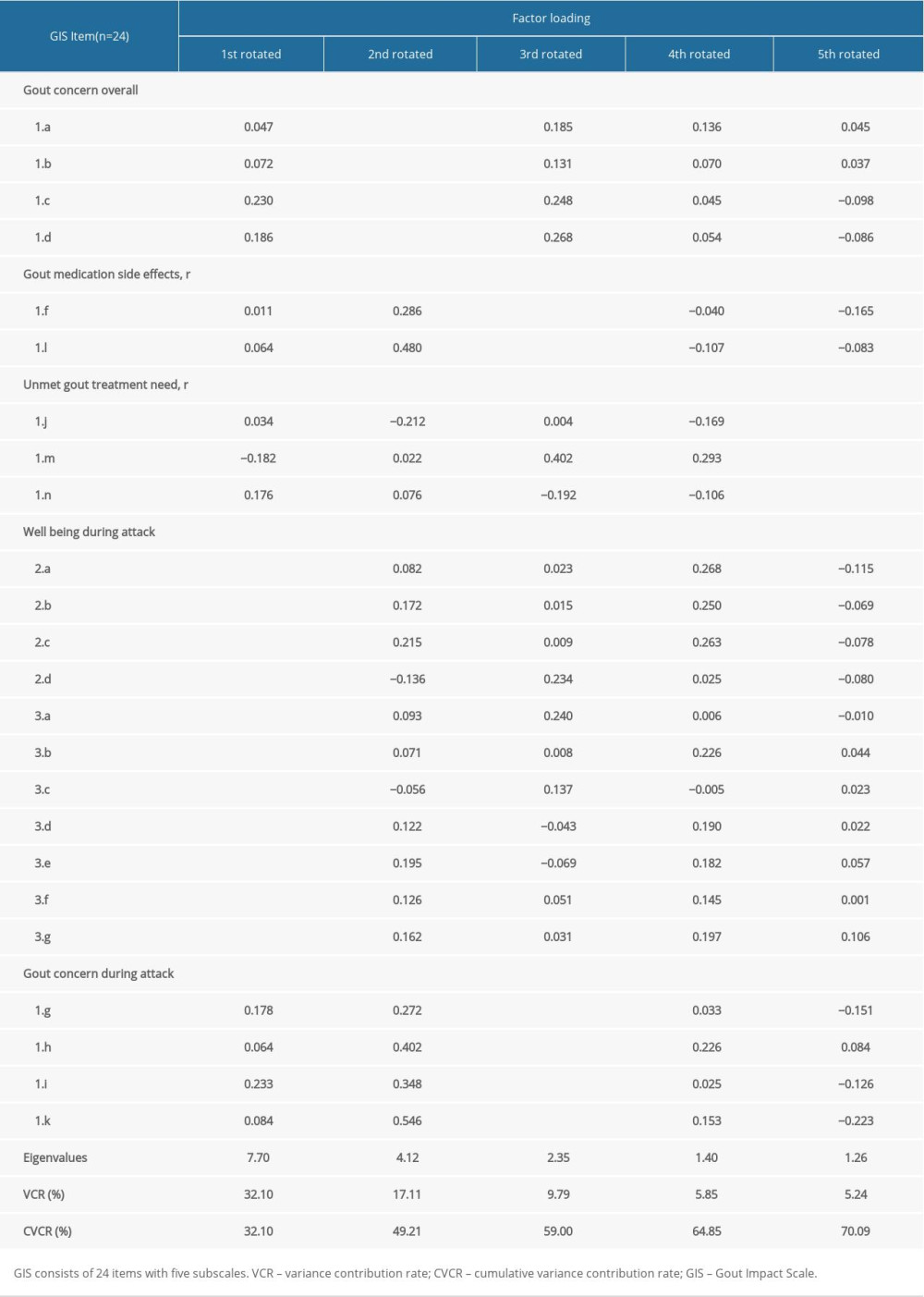 Table 4. Association between the Gout Impact Scale and gout-related features.
Table 4. Association between the Gout Impact Scale and gout-related features.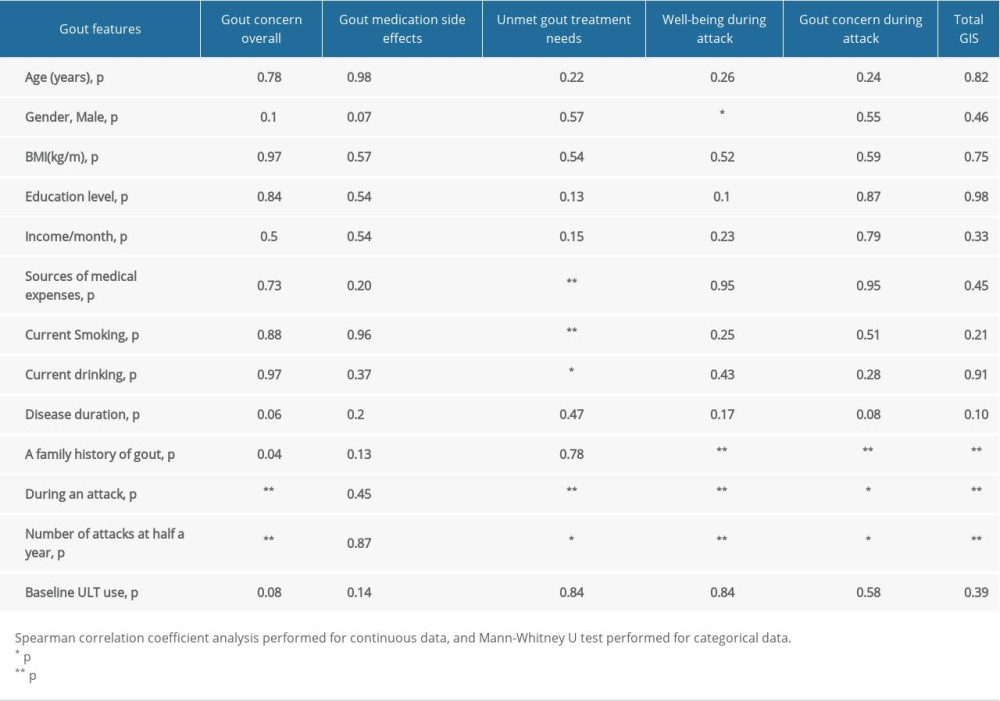 Table 5. Stepwise multiple linear regression analysis of the Gout Impact Scale in gout patients.
Table 5. Stepwise multiple linear regression analysis of the Gout Impact Scale in gout patients.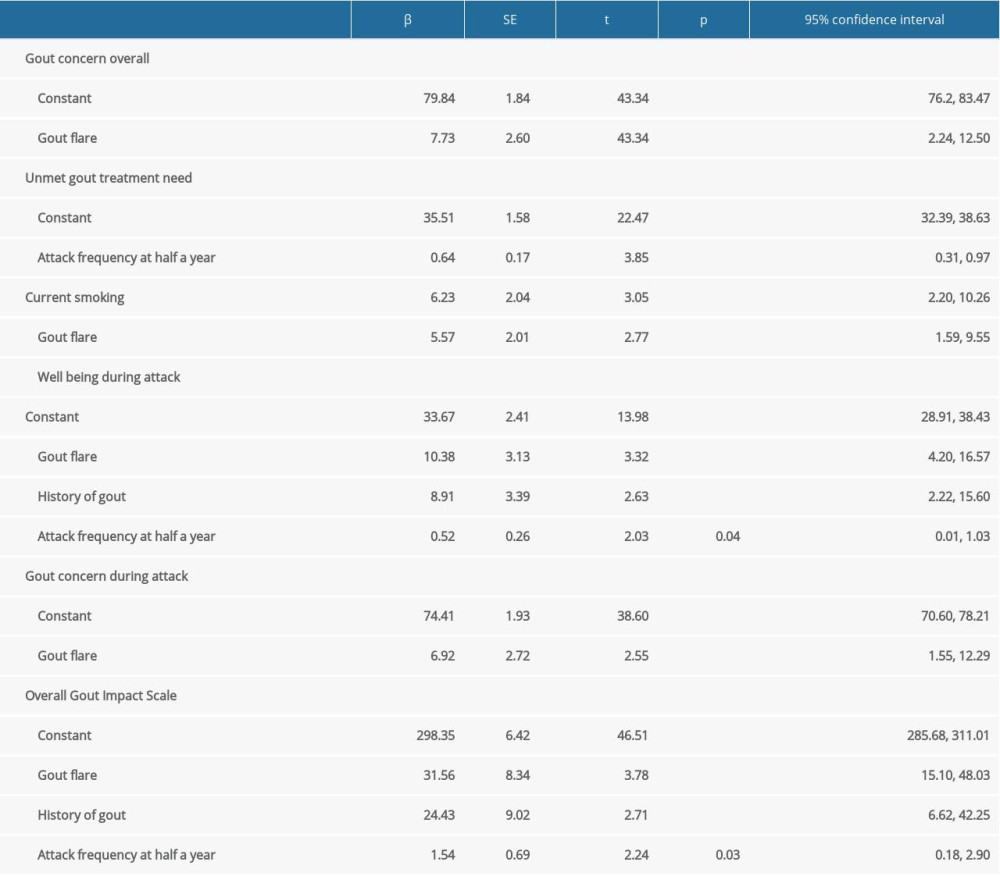
References
1. Choi HK, Mount DB, Reginato AMAmerican College of Physicians; American Physiological Society, Pathogenesis of gout: Ann Intern Med, 2005; 143(7); 499-516
2. Khanna PP, Shiozawa A, Walker V, Health-related quality of life and treatment satisfaction in patients with gout: Results from a cross-sectional study in a managed care setting: Patient Prefer Adherence, 2015; 9; 971-81
3. Singh JA, Bharat A, Khanna D, Racial differences in health-related quality of life and functional ability in patients with gout: Rheumatology (Oxford), 2017; 56(1); 103-12
4. Zhu Y, Pandya BJ, Choi HK, Prevalence of gout and hyperuricemia in the US general population: The National Health and Nutrition Examination Survey 2007–2008: Arthritis Rheum, 2011; 63(10); 3136-41
5. Pai S, Raslan A, Schlesinger N, Gout: Update on current therapeutics: Curr Treat Options Rheumatol, 2015; 1(2); 131-42
6. Kim KY, Schumacher HR, Hunsche E, A literature review of the epidemiology and treatment of acute gout: Clin Ther, 2003; 25(6); 1593-617
7. Terkeltaub R, Update on gout: New therapeutic strategies and options: Nat Rev Rheumatol, 2010; 6(1); 30-38
8. Hirsch JD, Terkeltaub R, Khanna D, Gout disease-specific quality of life and the association with gout characteristics: Patient Relat Outcome Meas, 2010; 2010; 1-8
9. Khanna PP, Perez-Ruiz F, Maranian P, Khanna D, Long-term therapy for chronic gout results in clinically important improvements in the health-related quality of life: Short Form-36 is responsive to change in chronic gout: Rheumatology (Oxford), 2011; 50(4); 740-45
10. Alvarez-Hernández E, Peláez-Ballestas I, Vázquez-Mellado JREUMAIMPACT, Validation of the Health Assessment Questionnaire disability index in patients with gout: Arthritis Rheum, 2008; 59(5); 665-69
11. Chandratre P, Roddy E, Clarson L, Health-related quality of life in gout: A systematic review: Rheumatology (Oxford), 2013; 52(11); 2031-40
12. Hirsch JD, Lee SJ, Terkeltaub R, Evaluation of an instrument assessing influence of gout on health-related quality of life: J Rheumatol, 2008; 35(12); 2406-14
13. Singh JA, Taylor WJ, Simon LS, Patient-reported outcomes in chronic gout: A report from OMERACT 10: J Rheumatol, 2011; 38(7); 1452-57
14. Taylor WJ, Gout measures: Gout Assessment Questionnaire (GAQ, GAQ2.0), and physical measurement of tophi: Arthritis Care Res (Hoboken), 2011; 63(Suppl 11); S59-63
15. Neogi T, Jansen TL, Dalbeth N, 2015 Gout classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative [published correction appears in Ann Rheum Dis. 2016;75(2): 473]: Ann Rheum Dis, 2015; 74(10); 1789-98
16. Choi IA, Kim JH, Lee YJ, Performance of the 2015 American College of Rheumatology/European League against Rheumatism classification criteria for gout in Korean patients with acute arthritis: J Korean Med Sci, 2019; 34(22); e155
17. Wallace B, Khanna D, Aquino-Beaton C, Performance of Gout Impact Scale in a longitudinal observational study of patients with gout: Rheumatology (Oxford), 2016; 55(6); 982-90
18. Chandratre P, Mallen C, Richardson J, Health-related quality of life in gout in primary care: Baseline findings from a cohort study: Semin Arthritis Rheum, 2018; 48(1); 61-69
19. Hickey A, Barker M, McGee H, O’Boyle C, Measuring health-related quality of life in older patient populations: A review of current approaches: Pharmacoeconomics, 2005; 23(10); 971-93
20. Taylor WJ, Colvine K, Gregory K, The Health Assessment Questionnaire Disability Index is a valid measure of physical function in gout: Clin Exp Rheumatol, 2008; 26(4); 620-26
21. Lee W, Teng GG, Kok JC, Validity and reliability of the Gout Impact Scale in a multi-ethnic Asian population: Int J Rheum Dis, 2019; 22(8); 1427-34
22. Scire CA, Manara M, Cimmino MAKING Study Collaborators, Gout impacts on function and health-related quality of life beyond associated risk factors and medical conditions: Results from the KING observational study of the Italian Society for Rheumatology (SIR): Arthritis Res Ther, 2013; 15(5); R101
23. Pao CH, Ko Y, An assessment of the psychometric properties of the Chinese version of the Gout Impact Scale: Curr Med Res Opin, 2020; 36(1); 17-21
24. Fu T, Cao H, Yin R, Associated factors with functional disability and health-related quality of life in Chinese patients with gout: A case-control study: BMC Musculoskelet Disord, 2017; 18(1); 429
25. Prior JA, Mallen CD, Chandratre P, Gout characteristics associate with depression, but not anxiety, in primary care: Baseline findings from a prospective cohort study: Joint Bone Spine, 2016; 83(5); 553-58
26. Kramer HM, Curhan G, The association between gout and nephrolithiasis: The National Health and Nutrition Examination Survey III, 1988–1994: Am J Kidney Dis, 2002; 40(1); 37-42
27. Mikuls TR, Farrar JT, Bilker WB, Gout epidemiology: Results from the UK General Practice Research Database, 1990–1999: Ann Rheum Dis, 2005; 64(2); 267-72
28. Tsai EC, Boyko EJ, Leonetti DL, Fujimoto WY, Low serum testosterone level as a predictor of increased visceral fat in Japanese-American men: Int J Obes Relat Metab Disord, 2000; 24(4); 485-91
29. Towiwat P, Li ZG, The association of vitamin C, alcohol, coffee, tea, milk and yogurt with uric acid and gout: Int J Rheum Dis, 2015; 18(5); 495-501
30. Choi HK, Atkinson K, Karlson EW, Alcohol intake and risk of incident gout in men: A prospective study: Lancet, 2004; 363(9417); 1277-81
31. Jee Y, Jeon C, Sull JW, Association between smoking and gout: A meta-analysis: Clin Rheumatol, 2018; 37(7); 1895-902
32. Zhang W, Doherty M, Bardin TEULAR Standing Committee for International Clinical Studies Including Therapeutics, EULAR evidence based recommendations for gout. Part II: Management. Report of a task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT): Ann Rheum Dis, 2006; 65(10); 1312-24
33. Robinson PC, Dalbeth N, Donovan P, The cost-effectiveness of biannual serum urate (SU) monitoring after reaching target in gout: A health economic analysis comparing SU monitoring [published correction appears in J Rheumatol, 2019; 46(3): 330]: J Rheumatol, 2018; 45(5); 697-704
34. Dore RK, Gout: What primary care physicians want to know: J Clin Rheumatol, 2008; 14(5 Suppl); S47-54
Tables
 Table 1. Baseline characteristics of gout patients.
Table 1. Baseline characteristics of gout patients. Table 2. Internal consistency analysis of the Gout Impact Scale.
Table 2. Internal consistency analysis of the Gout Impact Scale. Table 3. Exploratory factor analysis of the Gout Impact Scale.
Table 3. Exploratory factor analysis of the Gout Impact Scale. Table 4. Association between the Gout Impact Scale and gout-related features.
Table 4. Association between the Gout Impact Scale and gout-related features. Table 5. Stepwise multiple linear regression analysis of the Gout Impact Scale in gout patients.
Table 5. Stepwise multiple linear regression analysis of the Gout Impact Scale in gout patients. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








