05 November 2020: Clinical Research
Fibular Neck Osteotomy Approach in Treatment of Posterolateral Tibial Plateau Fractures: A Retrospective Case Series
Lang Chen1ABC, Yuan Xiong1ABD, Chenchen Yan1CD, Wu Zhou1EF, Ze Lin1DF, Zexi He1C, Bobin Mi1FG, Guohui Liu1AFG*DOI: 10.12659/MSM.927370
Med Sci Monit 2020; 26:e927370
Abstract
BACKGROUND: The surgical strategies for posterolateral tibial plateau fractures are still inconsistent. Although a number of operative approaches were previously reported for surgical treatment of fractures of the posterolateral column in the tibial plateau, some approaches fail to provide direct visualization of the articular surface and do not allow enough space to access the posterolateral area of the lateral tibial plateau, thereby leading to unsatisfactory reconstruction of the knee and poor articular activity.
MATERIAL AND METHODS: We retrospectively reviewed records of 21 patients who underwent fibular neck osteotomy approach for posterolateral fractures. Radiographs taken during follow-up were used to evaluate the quality of fracture reduction and lower-limb axis. The Tegner-Lysholm score was used to assess patient functional performance. Complications, including incision infection, osteotomy nonunion, peroneal nerve injury, and fragment displacement, were evaluated.
RESULTS: We included 12 males and 9 females, with an age range of 27-67 years (mean age, 42.43 years). No intraoperative complications or postoperative complications were found. The mean operative duration was 128.05 min (range: 86–167 min). No patients were lost to clinical or radiographic follow-up. All patients had complete follow-up (range: 13–28 months, mean: 19.57 months). Anatomical fracture reduction was achieved in 14 patients. Radiological limb alignment was restored in all patients. The mean Tegner-Lysholm score was 87.07 (range: 74–95) and the average knee society score (KSS) was 91.67 (range: 86–94) at the final follow-up.
CONCLUSIONS: In this retrospective study, the results suggest that the fibular neck osteotomy approach is a good choice for treatment of posterolateral tibial plateau fractures.
Keywords: Knee Injuries, Osteotomy, Tibial Fractures, Fibula, Tomography, X-Ray Computed
Background
Tibial plateau fractures are one of the most challenging articular fractures to treat, and account for approximately 1% of all fractures [1,2]. Posterolateral fractures of the tibial plateau are rarely reported, with an incidence of 7% [3]. In the past, the classic classifications (such as Schatzker and AO) were widely used for tibial plateau fracture, but failed to completely describe the posterolateral part of the tibial plateau. As computerized tomography (CT) scans have become widely used in patients with tibial plateau fracture, tibial plateau fractures have been divided into 4 columns [4], with recognition of the importance of the posterolateral part of the tibial plateau [5].
Recently, increasing attention has been focussed on surgical methods for treating posterolateral tibial plateau fractures [6]. Fixation of the posterolateral fractures is important for knee joint stability and range of motion [7]. Importantly, unsatisfactory reconstruction of intraarticular fractures can lead to posttraumatic osteoarthritis. Various approaches, such as posterolateral and posteromedial approach, posteromedial approach, and transfibular approach, have been used to treat posterolateral fractures [8–10]. Since every approach has its advantages and disadvantages, no approach has been widely accepted by orthopedic surgeons.
Although previous studies reported that the transfibular approach (fibular neck osteotomy or fibular head osteotomy) for visualizing posterolateral articular injury is practical and has no adverse effects [10,11], surgeons are careful about adopting this method owing to the potential for iatrogenic peroneal nerve injury. In addition, the complications associated with fibular neck osteotomy also make surgeons avoid using this approach. However, this approach may be a feasible way to observe the articular surface and achieve precise fracture reduction. The present study evaluated the benefits and limitations of the fibular neck osteotomy approach.
Material and Methods
PATIENTS AND METHODS:
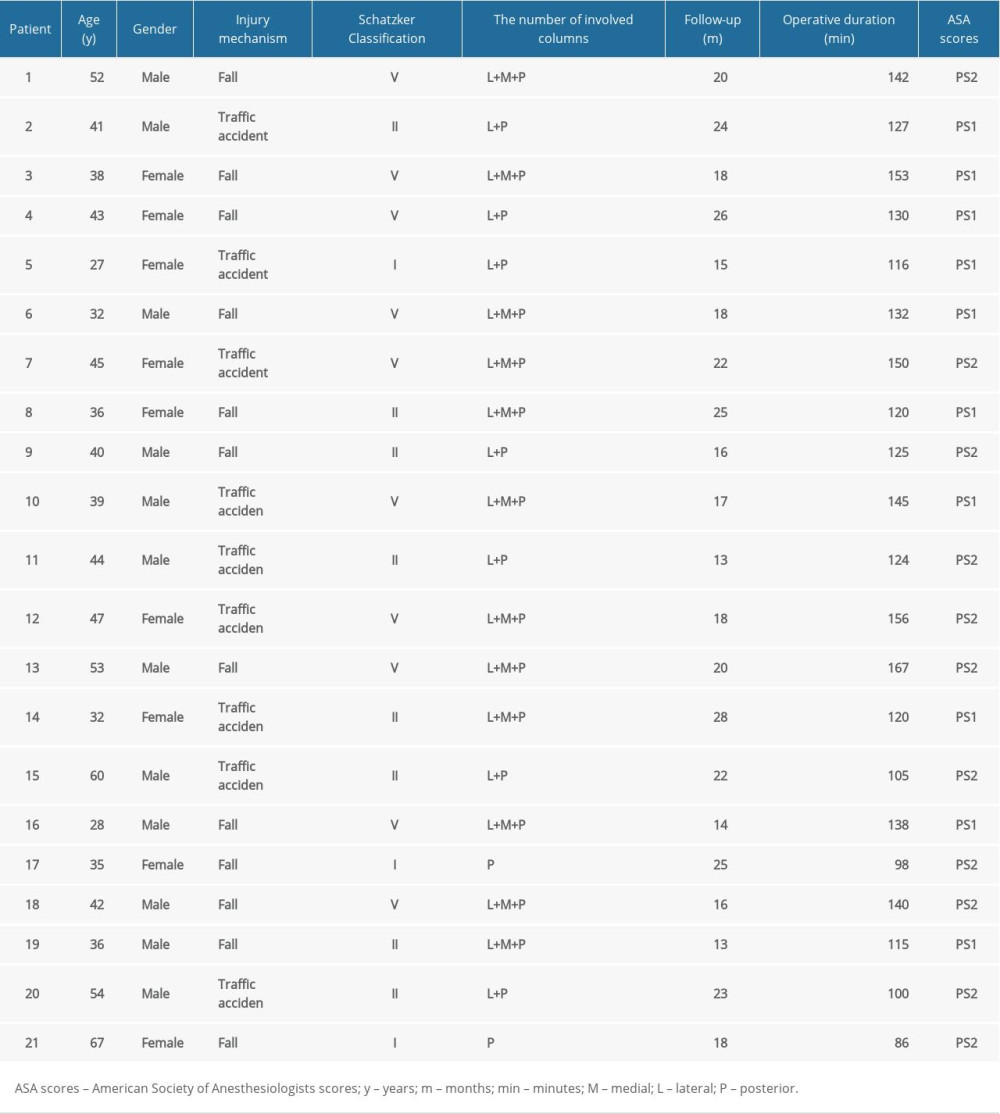
This is a study of case series with level of evidence IV. From October 2016 to January 2019, records of 21 patients who underwent fibular neck osteotomy approach for posterolateral fractures were retrospectively reviewed. The inclusion criteria were: (i) adult patients with fresh closed fractures, (ii) comminuted posterolateral tibial plateau fractures, (iii) knee activity was normal before injury, (iv) no serious vascular and nerve injury, and (v) signed inform consent. The exclusion criteria were: (i) American Society of Anesthesiologists (ASA) scores >PS3, (ii) knee active inflammation, (iii) open fractures or pathological fracture, (iv) osteofascial compartment syndrome, and (v) other types of tibial plateau fracture. There were 12 men and 9 women, with mean age 42.43±10.30 years. The injury mechanism and classification of fractures are listed in Table 1. All surgeries were completed in a university hospital by the same professional surgical team.
SURGICAL TECHNIQUE:
1) Preoperative X-ray and CT imaging of the fracture were necessary for planning the operative strategies of fixation (Figures 1A–1C; 2A, 2B). 2) A prone position (for the isolated posterior column fracture) or lateral decubitus was selected, as appropriate. A tourniquet was used to avoid excessive bleeding and to keep clear surgical visualization during surgery (Figures 1E, 2C). 3) The skin incision started from the inside of the biceps femoris tendon and extending anterolateral tibia to cross over the fibular head, running approximately 6–9 cm distally (Figure 1D). 4) The common peroneal nerve was scrupulously identified and protected. A wire saw was used to cut the fibular neck. (Figures 1F, 1G, 2D). 5) The standard lateral arthrotomy was performed and the hematoma was cleared. Then, the articular surface and posterolateral tibial plateau fracture were fully visualized and reduced (Figues 1H, 2E). 6) Standard reduction approaches inclusive of bone grafting were used. A 3.5-mm lateral proximal tibia plate was used (Figures 1I, 1J, 2F). 7) The fibular neck was fixed with 1 or 2 long cortex screws after fixation of the posterolateral tibial plateau fracture (Figure 1K, 2G).
POSTOPERATIVE ADMINISTRATION AND FOLLOW-UP:
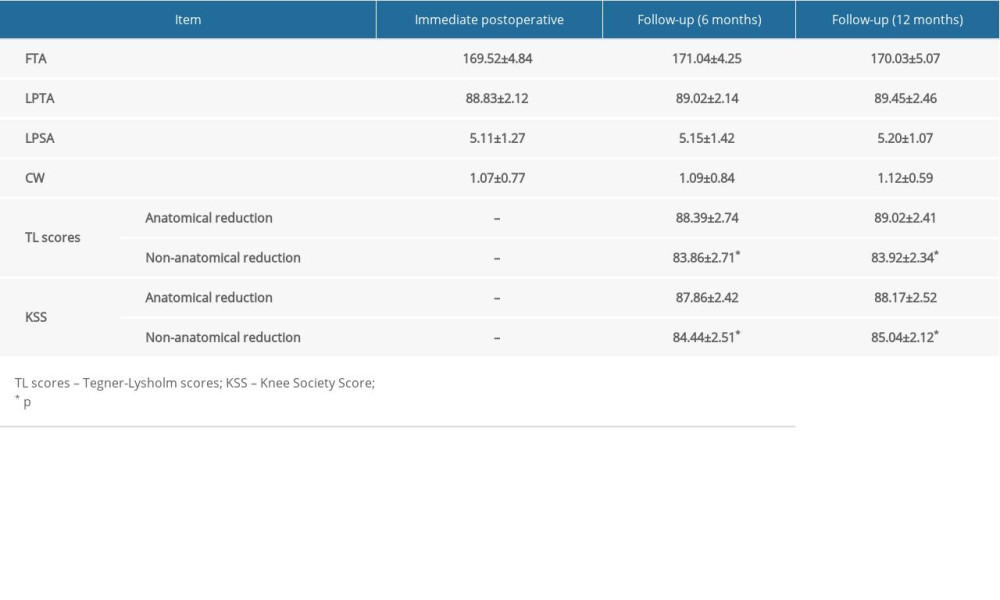
A passive motion machine was used by every participant. The range of motion of the passive motion machine began from 30° flexion and increased in keeping with the tolerance of participants. Active joint motion was encouraged, while partial weight bearing was only allowed starting at 12 weeks postoperatively. Radiographs were taken monthly for the initial 3 months. ROM and X-ray analysis were performed at each visit. Articular reduction criteria were: anatomical, good (<2 mm step), and poor (>2 mm step). Radiological parameters assessed were the femoro-tibial angle (FTA, normal: 180±5°), medial proximal tibial angle (MPTA, normal: 87±5°), lateral posterior slope angle (LPSA, normal: 9±4°), and condylar width (CW, normal: <5 mm compared to opposite side) [12]. Tegner-Lysholm (TL) scores and KSS [13] were assessed during the follow-up visit.
STATISTICAL ANALYSIS:
SPSS (version 16, Chicago, IL) was used to analyze the data. Reduction quality over the follow-up period based on the studied radiological parameters were analyzed using the paired
Results
No intraoperative or postoperative complications associated with this approach were found in this case series. No patients were lost to clinical or radiographic follow-up (Table 1). The mean time of follow-up ranged from 13 to 28 months (mean: 19.57 months). The mean operative duration ranged from 86 to 167 min (mean: 128.05 min). No infection, bone necrosis, neurovascular, or common peroneal nerve injury occurred. All fractures had united. Radiological limb alignment was restored in all patients. In addition, no re-collapse of articular surface or osteotomy nonunion were found.
Fourteen patients achieved anatomical fracture reduction and 7 achieved good fracture reduction. The femoro-tibial axis, MPTA, and condylar width were anatomically restored in all patients. Radiological parameters, including FTA, LPTA, LPSA, and CW, did not significantly change during follow-up (p > 0.05, Table 2). The mean knee arc of motion was 138.14° (range: 125–158°). No flexion contractures or extensor lag was found. The mean Tegner-Lysholm score was 87.07 (range: 74–95) and the mean KSS was 91.67 (range: 86–94) at final follow-up. Patients with non-anatomical articular reduction at the lateral tibia-femoral compartment had significantly lower TL and KSS scores (Table 2).
Discussion
It is widely accepted that it is difficult to perform reduction and fixation of the fibular head and the peroneal nerve for posterolateral tibial plateau fractures [14]. Direct fracture visualization can be obtained by the posteromedial approach and S-shaped approach [15]. However, in our opinion, those 2 methods require massive dissection of soft tissue, in which it is easy to damage the tibial neurovascular bundle. The anterolateral approach is safe and familiar to surgeons but fails to completely meet the requirements of anatomical reduction of posterolateral fractures [16]. Frosch [17] introduced an anterolateral and posterolateral arthrotomy approach, which allowed clear visualization of the joint surface but at the cost of massive damage to the soft tissue and common peroneal nerve. A dual-incisions approach was reported by Carlson [8], which has the advantage of exposing the lateral edge of the tibia instead of the posterior column. Tao [18] reported a novel posterolateral method for posterolateral tibial plateau fractures, without osteotomy or tenotomy, but this approach limits the distal exposure of the fracture. Hu [19] also introduced an anterolateral supra-fibular-head method for the treatment of posterolateral tibial plateau fractures. However, these methods are not appropriate for treatment of a maximum posterior cortex displacement that needs reduction.
We noted that most orthopedic surgeons avoid using the transfibular approach because they think this approach can lead to iatrogenic injury of the common peroneal nerve. However, for some complex posterolateral fragments that are covered by the fibular head, it is difficult to achieve reduction and fixation. In addition, some posterolateral fractures combined with fibular neck fracture are also suited to this approach. The fibular osteotomy was first described by Lobenhoffer [20] to treat posterolateral fracture. This approach has the advantage of providing a good view of the posterolateral corner of the tibia plateau and the disadvantage of extensive trauma to soft tissue of the posterolateral corner. Yu et al. [11] introduced a fibular head osteotomy technique for treatment of posterolateral tibial plateau fracture. They found that this approach provided outstanding visualization, thus facilitating the reduction and internal fixation for posterolateral tibial plateau fracture. Pires [10] reported that the fibular neck osteotomy approach has no adverse effects and is practical for visualizing posterolateral articular injury. In the present study, we used the fibular neck osteotomy approach for the treatment of posterolateral fracture. As the final follow-up results showed, all patients were satisfied with their knee function, and there were no serious complications of the transfibular technique, as reported in previous studies [10,11]. In the present study, none of the patients had common peroneal nerve palsies, fixation loss or nonunion at the osteotomy site, or posterolateral instability of the knee.
Advantages of the fibular neck osteotomy approach include the following: sufficient operation space is provided to avoid neurovascular and large soft tissue injury; providing direct visualization of articular surface to ensure an accurate anatomic reduction, thereby decreasing posttraumatic arthritis risk; and it is a straightforward treatment of some complicated fracture patterns with posterolateral articular displacement. Lateral column fractures extending to the posterior column are the most common posterolateral fracture type and are often associated with serious articular depression [7,21]. Either an extension-valgus or flexion-valgus injury mechanism can cause this two-column-involved fracture type. Obtaining and maintaining anatomic alignment and articular reduction throughout the whole bone union period are the crucial points for achieving satisfactory outcomes in surgical therapy for posterolateral fracture [22]. Based on the results presented in the present study, no significant difference was found in the alignment parameters, such as FTA, LPTA, LPSA, and CW, between immediate and 12-month postoperative measurements. Disadvantages of this method include the following: the common peroneal nerve was more likely to be injured than with the other approaches, and the osteotomy site may have nonunion or fixation loss. However, the disadvantages of this approach can be easily prevented by careful dissection and visualization of the common peroneal nerve and fixation of the fibular osteotomy with a long cortex screw to avoid osteotomy nonunion [10].
To the best of our knowledge, no previous studies have explored the exact size of posterolateral fragments and the extent of collapse of articular surface that indicate orthopedic surgery. In our experience, fragments larger than 3% of the tibial plateau’s articular surface, with an articular collapse of at least 3 mm, more often develop towards osteoarthritis. The classification of posterolateral fracture based on CT should be investigated to help better understand this kind of fracture and provide an ideal approach for the treatment of this kind of fracture.
Limitations to this respective study are that is was based on a single center’s experience, and did not provide long-term follow-up data with randomized controlled groups. Furthermore, the sample was small due to the relative rarity of the relevant fracture pattern, and prospective studies are needed to determine the safety and utility of this approach.
Conclusions
The fibular neck osteotomy approach appears to be a feasible alternative treatment for posterolateral tibial plateau fractures, which can offer direct visualization for articular anatomical reduction and diminish the risk of posttraumatic arthritis. Importantly, the postoperative complications of this approach are limited provided that the common peroneal nerve is carefully protected and the posteromedial neurovascular bundle is avoided.
Figures
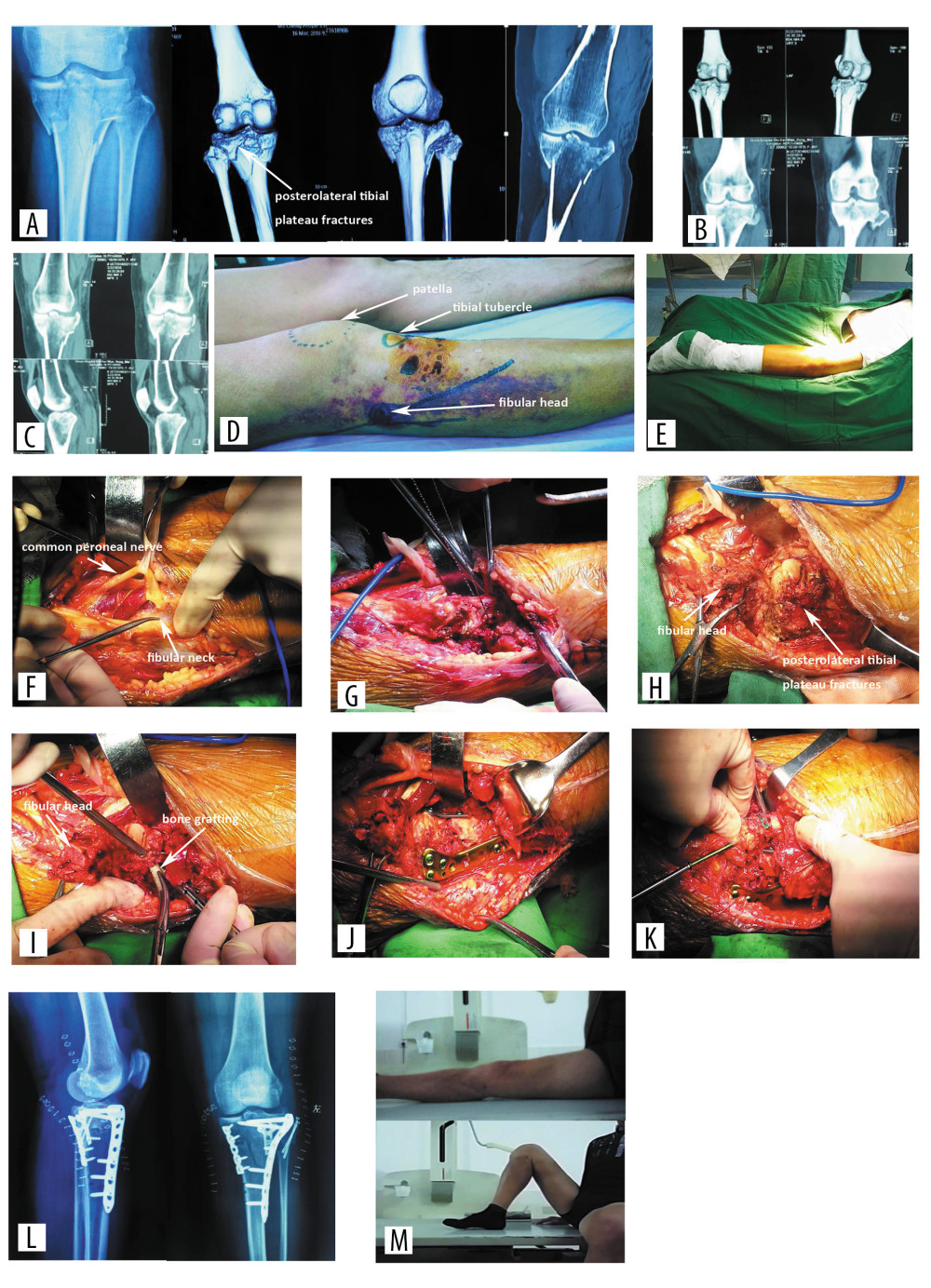 Figure 1. A 52-year-old man with right-sided tibial plateau fractures after a fall (Schatzker V). (A–C) X-ray and CT scan. (D, E) Operative position and approach. (F) The common peroneal nerve was carefully identified and protected. (G) A wire saw was used to cut the fibular neck. (H) Full visualization of the articular surface and posterolateral tibial plateau was achieved. (I) Standard reduction techniques and bone grafting. (J) A 3.5-mm lateral proximal tibia locking compression plate was used. (K) The fibular neck was fixed with 2 long cortex screws. (L) Radiographic image indicating fracture reduction and the internal fixation. (M) The clinical outcome was excellent.
Figure 1. A 52-year-old man with right-sided tibial plateau fractures after a fall (Schatzker V). (A–C) X-ray and CT scan. (D, E) Operative position and approach. (F) The common peroneal nerve was carefully identified and protected. (G) A wire saw was used to cut the fibular neck. (H) Full visualization of the articular surface and posterolateral tibial plateau was achieved. (I) Standard reduction techniques and bone grafting. (J) A 3.5-mm lateral proximal tibia locking compression plate was used. (K) The fibular neck was fixed with 2 long cortex screws. (L) Radiographic image indicating fracture reduction and the internal fixation. (M) The clinical outcome was excellent. 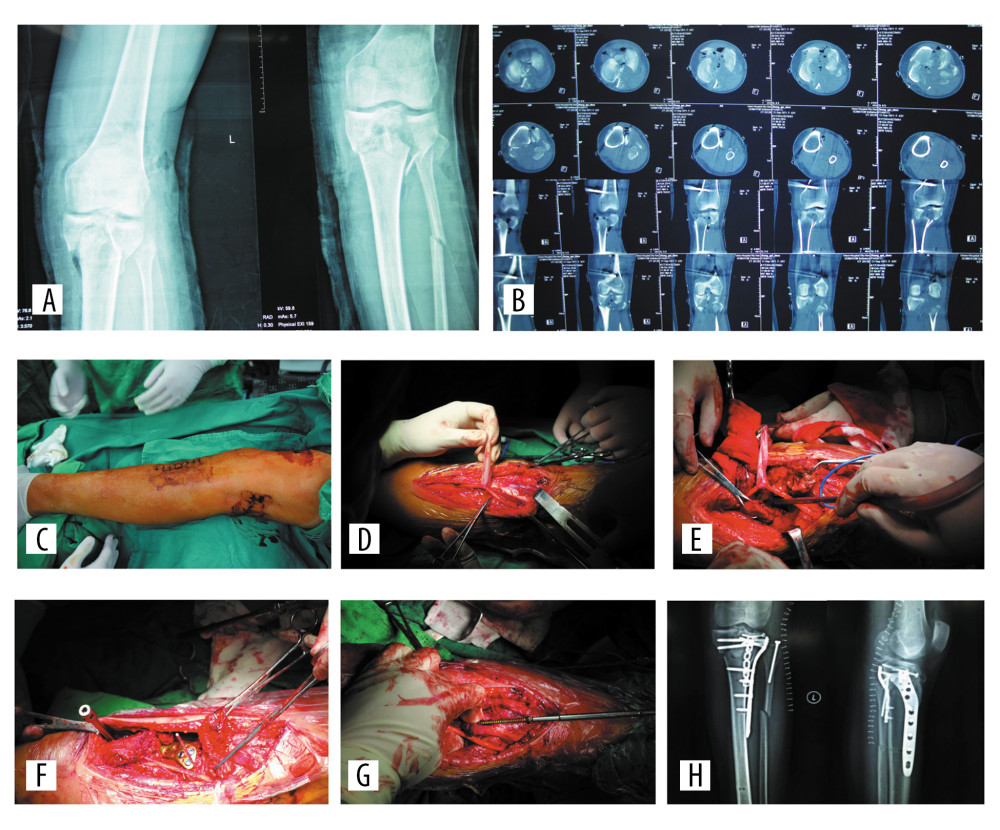 Figure 2. A 43-year-old women with left-sided tibial plateau fractures after a fall (Schatzker V). (A, B) X-ray and CT scan indicated the posterolateral fracture of the tibial plateau and fibular neck fracture. (C) Operative position (lateral position). (D) The common peroneal nerve was carefully identified and protected. (E) The articular surface and posterolateral tibial plateau fracture were fully visualized. (F) A 3.5-mm lateral proximal tibia locking compression plate was used. (G) The fibular neck was fixed with a long cortex screw. (H) Radiographic image indicating fracture reduction and the internal fixation.
Figure 2. A 43-year-old women with left-sided tibial plateau fractures after a fall (Schatzker V). (A, B) X-ray and CT scan indicated the posterolateral fracture of the tibial plateau and fibular neck fracture. (C) Operative position (lateral position). (D) The common peroneal nerve was carefully identified and protected. (E) The articular surface and posterolateral tibial plateau fracture were fully visualized. (F) A 3.5-mm lateral proximal tibia locking compression plate was used. (G) The fibular neck was fixed with a long cortex screw. (H) Radiographic image indicating fracture reduction and the internal fixation. References
1. Urruela AM, Davidovitch R, Karia R, Results following operative treatment of tibial plateau fractures: J Knee Surg, 2013; 26; 161-65
2. Moore TM, Patzakis MJ, Harvey JP, Tibial plateau fractures: definition, demographics, treatment rationale, and long-term results of closed traction management or operative reduction: J Orthop Trauma, 1987; 1; 97-119
3. Partenheimer A, Gosling T, Muller MManagement of bicondylar fractures of the tibial plateau with unilateral fixed-angle plate fixation: Unfallchirurg, 2007; 110; 675-83 [in German]
4. Chang SM, Hu SJ, Zhang YQ, A surgical protocol for bicondylar four-quadrant tibial plateau fractures: Int orthop, 2014; 38; 2559-64
5. Martínez-Rondanelli A, Escobar-González SS, Henao-Alzate A, Martínez-Cano JP, Reliability of a four-column classification for tibial plateau fractures: Int Orthop, 2017; 41(9); 1881-86
6. Zhang P, Lian K, Luo D, A combined approach for the treatment of lateral and posterolateral tibial plateau fractures: Injury, 2016; 47; 2326-30
7. Zhai Q, Luo C, Zhu Y, Morphological characteristics of split-depression fractures of the lateral tibial plateau (Schatzker type II): A computer-tomography-based study: Int Orthop, 2013; 37; 911-17
8. Carlson DA, Bicondylar fracture of the posterior aspect of the tibial plateau. A case report and a modified operative approach: J Bone Joint Surg Am, 1998; 80; 1049-52
9. Bhattacharyya T, McCarty LP, Harris MB, The posterior shearing tibial plateau fracture: treatment and results via a posterior approach: J Orthop Trauma, 2005; 19; 305-10
10. Pires RE, Giordano V, Wajnsztejn A, Complications and outcomes of the transfibular approach for posterolateral fractures of the tibial plateau: Injury, 2016; 47; 2320-25
11. Yu B, Han K, Zhan C, Fibular head osteotomy: A new approach for the treatment of lateral or posterolateral tibial plateau fractures: Knee, 2010; 17; 313-18
12. Barei DP, Nork SE, Mills WJ, Complications associated with internal fixation of high-energy bicondylar tibial plateau fractures utilizing a two-incision technique: J Orthop Trauma, 2004; 18; 649-57
13. Ranawat CS, Insall J, Shine J, Duo-condylar knee arthroplasty: Hospital for special surgery design: Clin Orthop Relat Res, 1976(120); 76-82
14. Garner MR, Warner SJ, Lorich DG, Surgical approaches to posterolateral tibial plateau fractures: J Knee Surg, 2016; 29; 12-20
15. Trickey EL, Rupture of the posterior cruciate ligament of the knee: J Bone Joint Surg Br, 1968; 50; 334-41
16. Zhai Q, Hu C, Luo C, Multi-plate reconstruction for severe bicondylar tibial plateau fractures of young adults: Int Orthop, 2014; 38; 1031-35
17. Frosch KH, Balcarek P, Walde T, A new posterolateral approach without fibula osteotomy for the treatment of tibial plateau fractures: J Orthop Trauma, 2010; 24; 515-20
18. Tao J, Hang DH, Wang QG, The posterolateral shearing tibial plateau fracture: Treatment and results via a modified posterolateral approach: Knee, 2008; 15; 473-79
19. Hu SJ, Chang SM, Zhang YQ, The anterolateral supra-fibular-head approach for plating posterolateral tibial plateau fractures: A novel surgical technique: Injury, 2016; 47; 502-7
20. Lobenhoffer P, Gerich T, Bertram TParticular posteromedial and posterolateral approaches for the treatment of tibial head fractures: Unfallchirurg, 1997; 100; 957-67 [in German]
21. Zhu Y, Meili S, Dong M, Pathoanatomy and incidence of the posterolateral fractures in bicondylar tibial plateau fractures: A clinical computed tomography-based measurement and the associated biomechanical model simulation: Arch Orthop Trauma Surg, 2014; 134; 1369-80
22. Barei DP, Nork SE, Mills WJ, Functional outcomes of severe bicondylar tibial plateau fractures treated with dual incisions and medial and lateral plates: J Bone Joint Surg Am, 2006; 88(8); 1713-21
Figures
 Figure 1. A 52-year-old man with right-sided tibial plateau fractures after a fall (Schatzker V). (A–C) X-ray and CT scan. (D, E) Operative position and approach. (F) The common peroneal nerve was carefully identified and protected. (G) A wire saw was used to cut the fibular neck. (H) Full visualization of the articular surface and posterolateral tibial plateau was achieved. (I) Standard reduction techniques and bone grafting. (J) A 3.5-mm lateral proximal tibia locking compression plate was used. (K) The fibular neck was fixed with 2 long cortex screws. (L) Radiographic image indicating fracture reduction and the internal fixation. (M) The clinical outcome was excellent.
Figure 1. A 52-year-old man with right-sided tibial plateau fractures after a fall (Schatzker V). (A–C) X-ray and CT scan. (D, E) Operative position and approach. (F) The common peroneal nerve was carefully identified and protected. (G) A wire saw was used to cut the fibular neck. (H) Full visualization of the articular surface and posterolateral tibial plateau was achieved. (I) Standard reduction techniques and bone grafting. (J) A 3.5-mm lateral proximal tibia locking compression plate was used. (K) The fibular neck was fixed with 2 long cortex screws. (L) Radiographic image indicating fracture reduction and the internal fixation. (M) The clinical outcome was excellent. Figure 2. A 43-year-old women with left-sided tibial plateau fractures after a fall (Schatzker V). (A, B) X-ray and CT scan indicated the posterolateral fracture of the tibial plateau and fibular neck fracture. (C) Operative position (lateral position). (D) The common peroneal nerve was carefully identified and protected. (E) The articular surface and posterolateral tibial plateau fracture were fully visualized. (F) A 3.5-mm lateral proximal tibia locking compression plate was used. (G) The fibular neck was fixed with a long cortex screw. (H) Radiographic image indicating fracture reduction and the internal fixation.
Figure 2. A 43-year-old women with left-sided tibial plateau fractures after a fall (Schatzker V). (A, B) X-ray and CT scan indicated the posterolateral fracture of the tibial plateau and fibular neck fracture. (C) Operative position (lateral position). (D) The common peroneal nerve was carefully identified and protected. (E) The articular surface and posterolateral tibial plateau fracture were fully visualized. (F) A 3.5-mm lateral proximal tibia locking compression plate was used. (G) The fibular neck was fixed with a long cortex screw. (H) Radiographic image indicating fracture reduction and the internal fixation. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387