23 December 2020: Clinical Research
Safety and Efficacy of Therapeutic Erythrocytapheresis Treatment in Chronic Mountain Sickness Patients in Shigatse, Tibet, China
Mingyuan NiuBCD, Shekhar SinghEF, Ma MiB, Pian BianB, Zhuoga DejiAB, Duoji MimaA, Xiankai LiACEGDOI: 10.12659/MSM.927853
Med Sci Monit 2020; 26:e927853
Abstract
BACKGROUND: Therapeutic erythrocytapheresis (TEA) is a medical technology that separates erythrocytes from whole blood and has been used in various hematological conditions. However, reports on the use of TEA to treat chronic mountain sickness (CMS) are lacking. The aim of the present study was to evaluate the efficacy, safety, and use of TEA in treatment of CMS.
MATERIAL AND METHODS: A total of 32 patients living in the Shigatse area of Tibet (altitude 4000 m) who had CMS were treated with TEA. Clinical data, CMS score, Borg dyspnea score, 6-min walking test score, and NYHA classification values were collected prior to and after TEA therapy.
RESULTS: TEA treatment significantly increased SpO₂ (93.8±2.6 vs. 80.5±5.8%, P<0.001) and decreased red blood cell (5.77±0.70 vs. 7.48±0.67×10¹²/L, P<0.001), hematocrit (53.8±5.6 vs. 69.2±4.8%, P<0.001) and hemoglobin (178±16 vs. 236±14 g/L, P<0.001). Significantly lower systolic and diastolic blood pressure were also noted (P<0.001). Echocardiography showed higher left ventricle diameter (4.6±0.4 vs. 4.4±0.5 cm, P<0.01). TEA markedly decreased CMS scores (0.45±0.85 vs. 7.58±2.31, P<0.001), Borg dyspnea scale scores (0.48±0.73 vs. 0.88±0.81, P<0.001), and NYHA classification scores (P<0.05). Additionally, there was marked improvement in the 6-min walking test scores (578.5±83.1 vs. 550.4±79.0 m, P<0.001). The procedure was well tolerated, with no complications.
CONCLUSIONS: Our novel approach of treating CMS patients with TEA safely and effectively reduced erythrocytosis, which remains a fundamental challenge in CMS patients.
Keywords: Altitude Sickness, Cytapheresis, Polycythemia, Chronic Disease, Electrocardiography, Severity of Illness Index, Tibet, vital signs
Background
Chronic mountain sickness (CMS), or Monge’s disease, is a clinical syndrome caused by long-term living at high altitudes of more than 2500 meters. It is characterized by excessive erythrocytosis (Hb ≥190 g/L in female patients, Hb ≥210g/L in male patients) and severe hypoxemia [1]. The prevalence of CMS is variable among different populations living at different high altitudes and has been reported to be above 30% in plateau regions [2]. The Qinghai-Tibetan plateau is the highest and largest plateau in the world, with a population of >60 million. CMS is a common condition here, with incidence rates of 2.43–37.5% (at elevations 3000–4700 m), and increases with elevation. Compared to native Tibetans, CMS is more prevalent in Han male immigrants (17.8%) [3–6]. CMS not only seriously affects the health and quality of life of plateau residents, but also leads to chronic pulmonary hypertension via various cellular and molecular mechanisms [7–11]; it can cause increased ventricular afterload and finally lead to the development of life-threatening right-heart failure [12–15]. In addition, the excessive erythrocytosis of CMS increases the viscosity of blood, making it thick and sticky, which significantly increases the risk of thrombosis, leading to diseases such as myocardial infarction, pulmonary embolism, and cerebral infarction, resulting in multiorgan dysfunction and death.
Therefore, it is imperative to accurately evaluate and establish effective treatment methods for CMS. Several pharmacological approaches have been employed [1,16–18] but there is no specific medicine suitable for treatment. Phlebotomy is another frequent practice for treating CMS, in which certain volume of whole blood is removed. However, this technique not only decreases red blood mass and hemoglobin, but also causes loss of platelets, albumin, coagulation factor, and leucocytes and results in iron deficiency and volemic imbalance. Therefore, phlebotomy remains impractical for long-term management of CMS [1].
Therapeutic erythrocytapheresis (TEA) has been used as an alternative therapy to treat polycythemia rubra vera and hemochromatosis. It is a sophisticated form of phlebotomy in which cell separators remove red blood cells only, sparing platelets, albumin, and coagulation factors [19–21]. Thus, in the present study, we for the first time used TEA to treat CMS patients. The purpose of this study was to collect clinical data of patients with CMS in the Shigatse area of Tibet at an average altitude of 4000 m and to evaluate the safety and efficacy of TEA in CMS patients.
Material and Methods
STUDY DESIGN:
This was a single-center, self-control study. All participants diagnosed with CMS and who received TEA were continuously enrolled from March to December 2018 while attending the Cardiology Department of Shigatse People’s Hospital, Tibet, China.
The study was approved by the Human Research Ethics Committee of Shigatse People’s Hospital. All participants provided written informed consent.
STUDY POPULATION:
CMS is diagnosed when Hb is ≥190 g/L in females and ≥210 g/L in males due to chronic erythrocytosis and with severe hypoxemia. Demographic data, medical history, and smoking status were collected through questionnaire. SpO2, red blood cells, hemoglobin and hematocrit, blood pressure, liver and renal function, cardiac biomarkers, and electrolytes were regularly tested within 2 days before and after TEA. Echocardiography, 6-min walking test, the New York Heart Association (NYHA) classification, Borg dyspnea scale, and Qinghai CMS score were strictly evaluated and confirmed by 2 independent physicians before and after TEA.
Exclusion criteria were: 1) age ≤18 or ≥70 years; 2) NYHA functional class IV heart failure or severe liver or renal dysfunction; 3) cannot tolerate TEA or unable to complete the 6-min walking test; 4) coagulation disorders or high risk of bleeding; and 5) pregnant or lactating women.
TREATMENT PROCEDURE:
The TEA technique was performed using a COBE® spectra™(TERUMO BCT) instrument and disposable closed tubes. Room temperature was kept at 25–26°C and all patients were placed in supine position. Two accesses were established on superficial veins connected to tubes, one on the left hand and the other on the right. One tube was used for outflow and the other for inflow. The COBE system software calculated exchange volume according to sex, height, weight, and hematocrit of patients. After removal of RBC, the plasma was returned with 0.9% saline as fluid compensation. Intraoperative heparin was used for anticoagulation. During the TEA procedure, the blood flow was 50–60 ml/min, circulating volume was 2500–3000 ml, and the collection time was limited to 1–2 h. Blood pressure, SpO2, and heart rate were monitored throughout.
STATISTICAL ANALYSIS:
All analyses were performed with SPSS, version 13.0 (Chicago, IL, USA). Continuous variables are expressed as mean±SD and discrete variables as percentages. The differences in continuous variables between groups were examined by paired-samples
Results
We enrolled a total of 32 participants diagnosed with CMS, consisting of 5 Han immigrants (15.6%) and 27 native Tibetans (84.4%), living in the Shigatse area of Tibet at an average altitude of 4000 m. Most (96.7%) of the participants were male. The average age of the participating patients was 44 years. Most of the participants had a history of smoking (78.1%), averaging 20 cigarettes per day. The most common disease history of participants was hyperuricemia (78.1%), hypertension (46.9%), and dyslipidemia (28.1%). Two patients had history of stroke and 3 patients had history of COPD (Table 1).
An average of 1457±207 ml blood was taken out during the TEA procedure during a period of about 2 h (Table 2).
Table 3 shows the vital signs and laboratory results before and after TEA treatment. There was significant reduction in concentration of red blood cells, hemoglobin, and hematocrit after TEA treatment (
Table 4 illustrates the echocardiographic measurement of the patients with CMS before and after TEA treatment. Except for the change in left ventricle diameter (4.4±0.5
Table 5 shows the efficacy of TEA therapy in CMS patients. The Borg dyspnea scale and Qinghai CMS score decreased significantly (both
Discussion
STUDY LIMITATIONS:
The major drawback of this study is its small sample size. Wider acceptance and use as a safe and effective treatment need further larger-scale study. Additionally, patients from remote mountain areas were at times unable to be followed up regularly; therefore, we could not monitor them for long periods or record any long-term adverse effects. Additional research with a larger population is essential.
Conclusions
In conclusion, this study shows that TEA is an efficient and safe treatment of CMS, which not only decrease excessive erythrocytosis but also preserves the important blood components in CMS patients. Therefore, in the future, it is likely that TEA could be used as primary treatment for CMS.
Tables
Table 1. Baseline characteristics of the participants.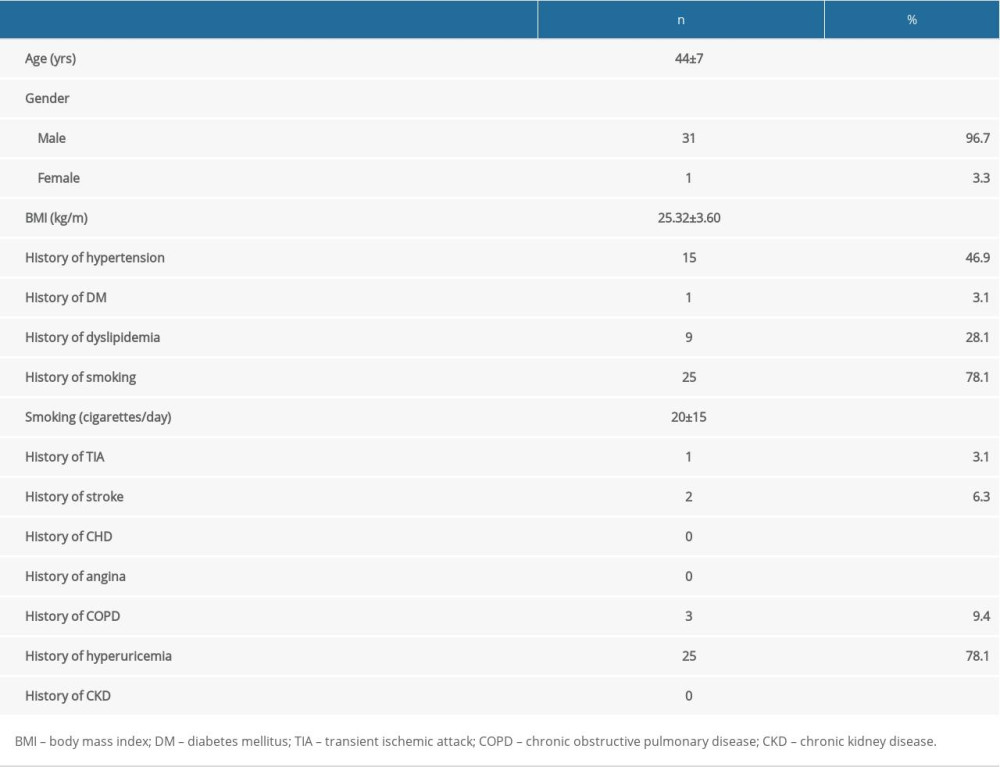 Table 2. Parameters of the TEA procedure.
Table 2. Parameters of the TEA procedure.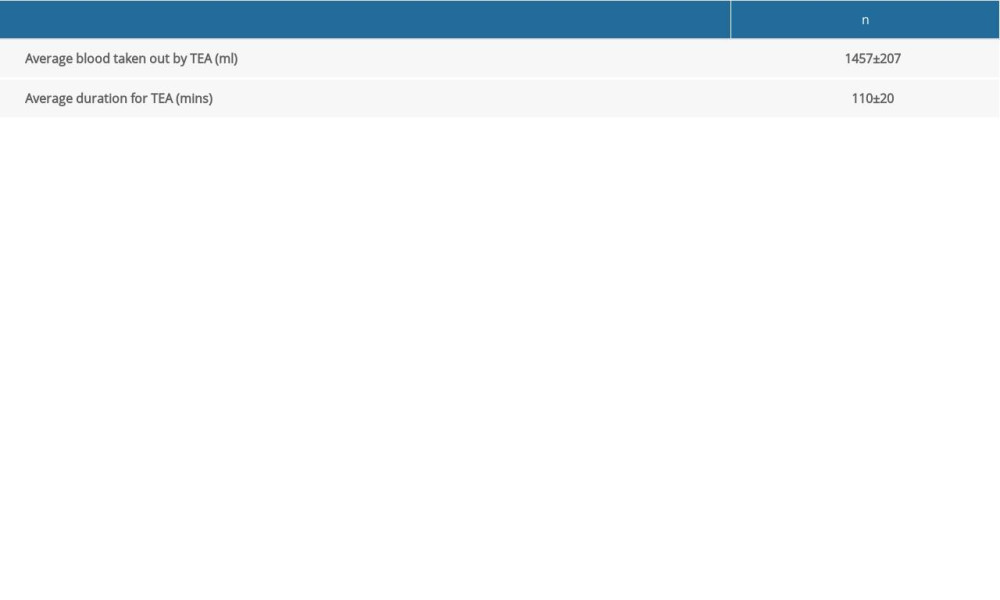 Table 3. Vital signs and laboratory results of CMS patients before and after TEA treatment.
Table 3. Vital signs and laboratory results of CMS patients before and after TEA treatment.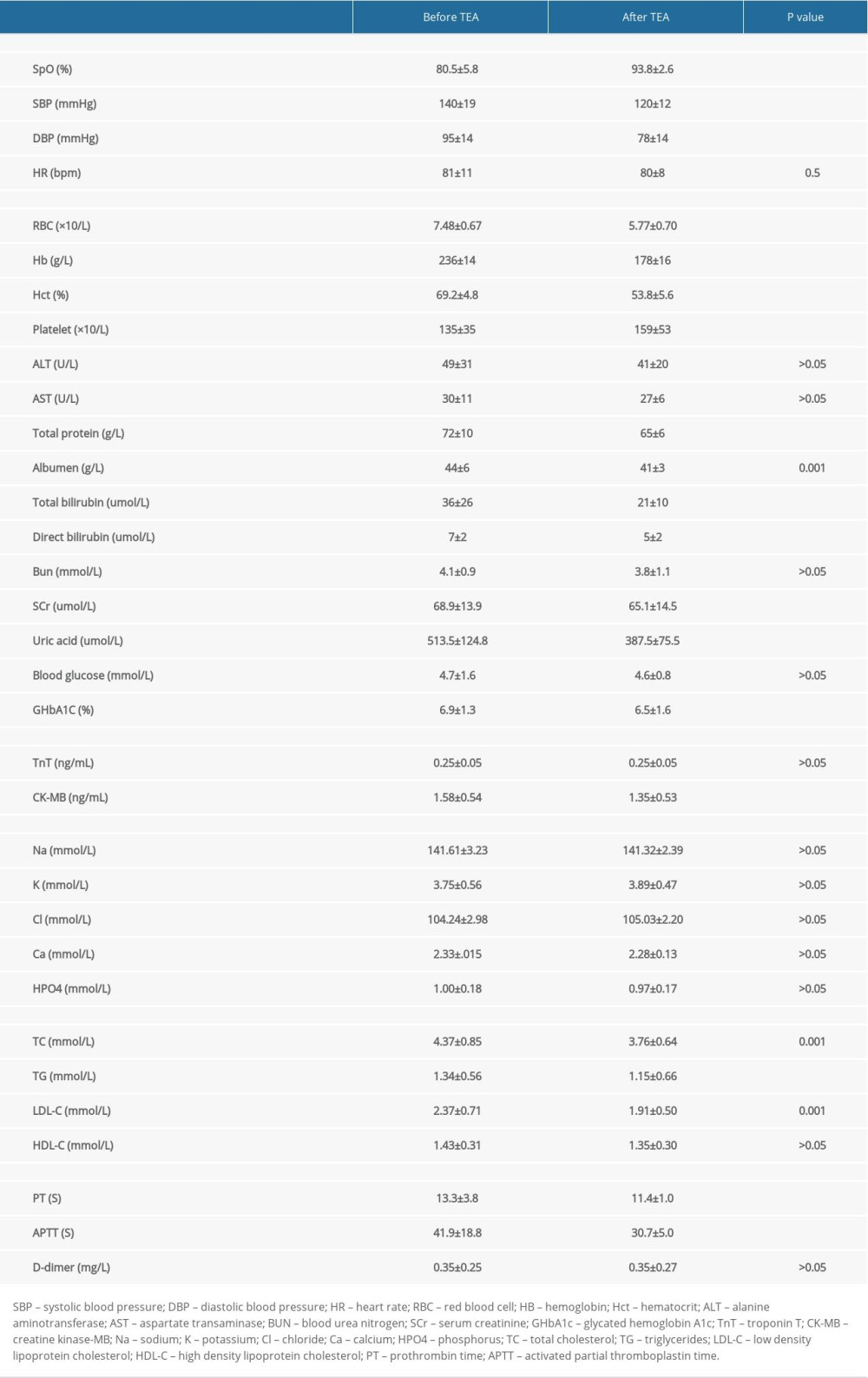 Table 4. Echocardiographic measurement in CMS patient before and after TEA.
Table 4. Echocardiographic measurement in CMS patient before and after TEA.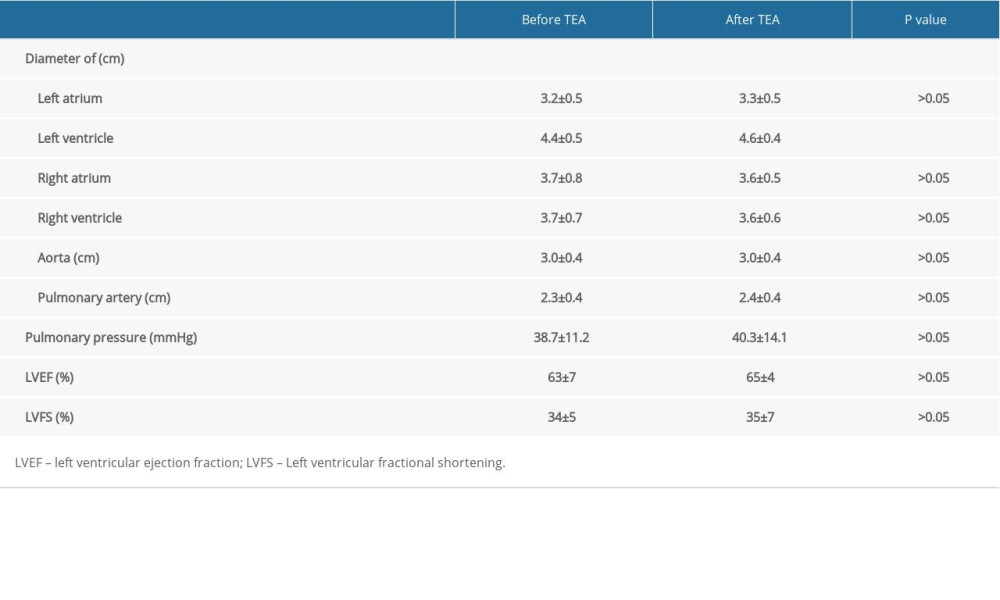 Table 5. Evaluation of severity of CMS before and after TEA treatment.
Table 5. Evaluation of severity of CMS before and after TEA treatment.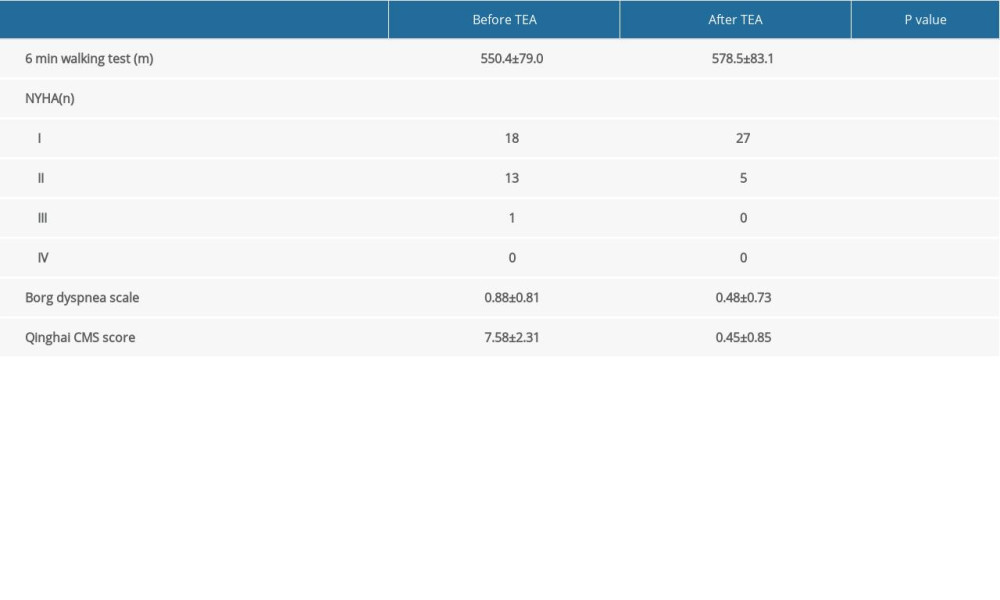
References
1. Villafuerte FC, Corante N, Chronic mountain sickness: Clinical aspects, etiology, management, and treatment: High Alt Med Biol, 2016; 17; 61-69
2. Gonzales GF, Rubio J, Gasco M, Chronic mountain sickness score was related with health status score but not with hemoglobin levels at high altitudes: Respir Physiol Neurobiol, 2013; 188; 152-60
3. Jiang C, Chen J, Liu F, Chronic mountain sickness in Chinese Han males who migrated to the Qinghai-Tibetan plateau: Application and evaluation of diagnostic criteria for chronic mountain sickness: BMC Public Health, 2014; 14; 1-11
4. Li C, Li X, Liu J, Investigation of the differences between the Tibetan and Han populations in the hemoglobin–oxygen affinity of red blood cells and in the adaptation to high-altitude environments: Hematology, 2018; 23; 309-13
5. Fan X, Ma L, Zhang Z, Associations of high-altitude polycythemia with polymorphisms in PIK3CD and COL4A3 in Tibetan populations: Hum Genomics, 2018; 12; 1-9
6. Jiang C, Liu F, Luo Y, Gene expression profiling of high altitude polycythemia in Han Chinese migrating to the Qinghai-Tibetan plateau: Mol Med Rep, 2012; 5; 287-93
7. Grimminger J, Richter M, Tello K, Thin air resulting in high pressure: Mountain sickness and hypoxia-induced pulmonary hypertension: Can Respir J, 2017; 2017 8381653
8. Dunham-Snary KJ, Wu D, Sykes EA, Hypoxic pulmonary vasoconstriction: From molecular mechanisms to medicine: Chest, 2017; 151; 181-92
9. Wilkins MR, Ghofrani HA, Weissmann N, Pathophysiology and treatment of high-altitude pulmonary vascular disease: Circulation, 2015; 131; 582-90
10. Murray AJ, Montgomery HE, Feelisch M, Metabolic adjustment to high-altitude hypoxia: From genetic signals to physiological implications: Biochem Soc Trans, 2018; 46; 599-607
11. Neupane M, Swenson ER, High-altitude pulmonary vascular diseases: Adv Pulm Hypertens, 2017; 15; 149-57
12. Naeije R, Dedobbeleer C, Pulmonary hypertension and the right ventricle in hypoxia: Exp Physiol, 2013; 98; 1247-56
13. León-Velarde F, Villafuerte FC, Richalet JP, Chronic mountain sickness and the heart: Prog Cardiovasc Dis, 2010; 52; 540-49
14. Naeije R, Altitude and the right heart: Rev Mal Respir, 2018; 35; 441-51
15. Schreier DA, Hacker TA, Hunter K, Impact of increased hematocrit on right ventricular afterload in response to chronic hypoxia: J Appl Physiol, 2014; 117; 833-39
16. Sharma S, Gralla J, Ordonez JG, Acetazolamide and N-acetylcysteine in the treatment of chronic mountain sickness (Monge’s disease): Respir Physiol Neurobiol, 2017; 246; 1-8
17. Richalet JP, Rivera-Ch M, Maignan M, Acetazolamide for Monge’s disease: Efficiency and tolerance of 6-month treatment: Am J Respir Crit Care Med, 2008; 177; 1370-76
18. Cui J, Gao L, Yang H, Potential beneficial effects of oral administration of isoflavones in patients with chronic mountain sickness: Exp Ther Med, 2013; 7; 275-79
19. Itam KP, Okafor IM, Use of apheresis in the treatment of Haematological conditions: World Scientific News, 2016; 50; 250-65
20. Wijermans P, van Egmond L, Ypma P, Isovolemic erythrocytapheresis technique as an alternative to conventional phlebotomy in patients with polycythemia rubra vera and hemochromatosis: Transfus Apher Sci, 2009; 40; 137
21. Sundic T, Hervig T, Hannisdal S, Erythrocytapheresis compared with whole blood phlebotomy for the treatment of hereditary haemochromatosis: Blood Transfus, 2014; 12(Suppl 1); 7-12
22. Evers D, Kerkhoffs J-L, Van Egmond L, The efficiency of therapeutic erythrocytapheresis compared to phlebotomy: A mathematical tool for predicting response in hereditary hemochromatosis, polycythemia vera, and secondary erythrocytosis: J Clin Apher, 2014; 29; 133-38
23. Al-Rahal N, AlHamza F, Therapeutic erythrocytapheresis versus traditional phlebotomy in the treatment of patients with erythrocytosis: Int J Adv Res, 2016; 4; 509-15
24. Liu H, Liu H, Shen J, A clinical analysis of erythrocytapheresis for the treatment of polycythemia: Transfus Apher Sci, 2013; 48; 229-33
25. Teofili L, Valentini CG, Rossi E, De Stefano V, Indications and use of therapeutic phlebotomy in polycythemia vera: Which role for erythrocytapheresis?: Leukemia, 2019; 33; 279-81
26. Zhao Y, Zhang Z, Liu L, Associations of high altitude polycythemia with polymorphisms in EPAS1, ITGA6 and ERBB4 in Chinese Han and Tibetan populations: Oncotarget, 2017; 8; 86736-46
27. West JB, Physiological effects of chronic hypoxia: N Engl J Med, 2017; 376; 1965-71
28. Wright AD, Beazley MF, Bradwell AR, Medroxyprogesterone at high altitude. The effects on blood gases, cerebral regional oxygenation, and acute mountain sickness: Wilderness Environ Med, 2004; 15; 25-31
29. Plata R, Cornejo A, Arratia C, Angiotensin-converting-enzyme inhibition therapy in altitude polycythaemia: A prospective randomised trial: Lancet, 2002; 359; 663-66
Tables
 Table 1. Baseline characteristics of the participants.
Table 1. Baseline characteristics of the participants. Table 2. Parameters of the TEA procedure.
Table 2. Parameters of the TEA procedure. Table 3. Vital signs and laboratory results of CMS patients before and after TEA treatment.
Table 3. Vital signs and laboratory results of CMS patients before and after TEA treatment. Table 4. Echocardiographic measurement in CMS patient before and after TEA.
Table 4. Echocardiographic measurement in CMS patient before and after TEA. Table 5. Evaluation of severity of CMS before and after TEA treatment.
Table 5. Evaluation of severity of CMS before and after TEA treatment. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








