18 December 2020: Clinical Research
Characteristics of Nosocomial Infections in Children Screened for SARS-CoV-2 Infection in China
Jun Shen1AE, Jing Sun1AE, Danyang Zhao2AE, Suyun Li3AE, Weiqiang Xiao4AE, Xian Cai1B, Jianjiang Yan1B, Weidong Zhu1B, Qiaozhi Guo2B, Xiulan Wen5B, Jinxia Wu3B, Xuan Shi3B, Daoju Jiang3C, Jing Huang3C, Jiaming Luo1C, Huan Chen6C, Yan Hong1C, Wencheng Ma3D, Guangming Liu3F, Haomei Yang3D, Qiang Wang3F, Yongling Song3F, Jinai Lin1D, Xin Sun7A, Peiqing Li3A*DOI: 10.12659/MSM.928835
Med Sci Monit 2020; 26:e928835
Abstract
BACKGROUND: This study summarizes the characteristics of children screened for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection and reports the case of 1 child who was diagnosed with SARS-CoV-2 infection in Guangzhou Women and Children’s Medical Center and the cases of his family members.
MATERIAL AND METHODS: The medical records of 159 children who were admitted to our hospital from January 23 to March 20, 2020, were retrospectively analyzed. Samples from pharyngeal or/and anal swabs were subjected to reverse-transcription polymerase chain reaction (RT-PCR) testing for SARS-CoV-2 within 12 h of patient admission; a second RT-PCR test was done 24 h after the first test.
RESULTS: Of the 159 patients, 151 patients had epidemiological histories, 14 patients had cluster onset, and 8 patients had no epidemiological history but had symptoms similar to coronavirus disease 2019 (COVID-19). The most common symptom was fever (n=125), followed by respiratory and gastrointestinal symptoms. A 7-year-old boy in a cluster family from Wuhan was confirmed with asymptomatic SARS-CoV-2 infection with ground-glass opacity shadows on his lung computed tomography scan, and his swab RT-PCR test had not turned negative until day 19 of his hospitalization. In patients who did not test positive for SARS-CoV-2, influenza, respiratory syncytial virus, and adenovirus were observed. A total of 158 patients recovered, were discharged, and experienced no abnormalities during follow-up.
CONCLUSIONS: For SARS-CoV-2 nosocomial infections, taking a “standard prevention & contact isolation & droplet isolation & air isolation” strategy can prevent infection effectively. Children with clustered disease need close monitoring.
Keywords: COVID-19, Multiphasic Screening, Pandemics, Pediatrics, Primary Prevention, COVID-19, COVID-19 Nucleic Acid Testing, Child, Child, Preschool, Coronavirus, Cross Infection, Fever, Hospitalization, Hospitals, Medical Records, Patient Discharge, SARS-CoV-2
Background
The novel coronavirus infection named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) by the Coronaviridae Study Group of the International Committee on Taxonomy of Viruses first occurred in China in December 2019 [1]. The World Health Organization named the disease caused by SARS-CoV-2 infection coronavirus disease 2019 (COVID-19) [2]. With the approval of the State Council and as stipulated in the Law of the People’s Republic of China on the Prevention and Control of Infectious Diseases, COVID-19 was included in the Class B of infectious diseases; however, measures for the prevention and control of Class A infectious diseases have been adopted for COVID-19 [3].
There have been various types of reports from Guangzhou, China, on COVID-19, which have improved our understanding of the disease, including reports on the transmission via air-conditioning [4], temporal patterns of viral shedding [5], authenticity of reverse-transcription polymerase chain reaction (RT-PCR) testing [6], and efficacy of chloroquine as a treatment option [7].
It has been reported that from a total of 72 314 cases, fewer than 1% were in children younger than 10 years of age [8]. While the majority of children infected by SARS-CoV-2 have a registered household contact with COVID-19 [9], it was found that children have milder symptoms than adults and infants are vulnerable to infection [10]; also, asymptomatic infections in children are not uncommon [11].
Our hospital center was designated for the screening and treatment of children with COVID-19 in Guangzhou, and has been screening and managing pediatric patients to control the spread of the epidemic in Guangzhou. To the best of our knowledge, there have not been any studies reporting the epidemiology and screening of children from this area. Therefore, to shed light on the situation in Guangzhou, this study sought to delineate the clinical characteristics of the children who were screened for SARS-CoV-2 infection using the “standard prevention & contact isolation & droplet isolation & air isolation” strategy.
Material and Methods
PATIENTS:
This retrospective study included 159 children who were screened for SARS-CoV-2 infection in the Guangzhou Women and Children’s Medical Center from January 23 to March 20, 2020. Children who were younger than 18 years old and met the screening and diagnostic criteria as a suspected case according to the Consensus of Experts in the Diagnosis and Treatment of Children with SARS-CoV-2 Infection in Guangdong Province [12] were selected. The diagnostic criteria of a suspected case included epidemiological history (travel or residence history in Wuhan or in Wuhan’s surrounding areas or in communities with confirmed infection cases within 14 days before the onset of illness; history of contact with patients with SARS-CoV-2 infection (positive RT-PCR test) within 14 days before onset; history of contact with patients with fever or respiratory symptoms from Wuhan, Wuhan’s surrounding areas, or communities with confirmed cases within 14 days before onset; cluster onset and clinical features (fever and/or respiratory symptoms; radiological imaging results characteristic of pneumonia; normal or decreased white blood cells count in the early stages of onset or decreased lymphocyte count). Diagnosis was based on the presence of 1 of the epidemiological histories and 2 of the clinical features. If there was no clear epidemiological history, 3 of the clinical features were considered for a positive diagnosis.
Patients were excluded if 2 pharyngeal or/and anal swab samples taken for viral nucleic acid RT-PCR tests more than 24 h apart after admission were both negative.
This study was approved by the ethics committee of the hospital (No. 2020-25001) and the requirement for informed consent was waived.
STRATEGY AND SCREENING METHOD:
A “standard prevention & contact isolation & droplet isolation & air isolation” strategy was used to control nosocomial infection of SARS-CoV-2 (Supplementary Material). Patients’ pharyngeal or/and anal swab samples were taken within the first 12 h of admission and tested by real-time fluorescent RT-PCR for detection of SARS-CoV-2 nucleic acids. A second RT-PCR test was performed 24 h after the first test.
TREATMENT AFTER SCREENING:
Confirmed cases were transferred to the “confirmed ward”, and severe or critical patients were transferred to the pediatric intensive care unit. Patients were discharged and a 14-day quarantine at home was advised when both RT-PCR tests were negative. Patients were transferred to another specialty ward to continue isolated treatment if both RT-PCR tests were positive.
DATA COLLECTION AND FOLLOW-UP:
Detailed demographic data, clinical characteristics at admission, and hematologic and imaging indicators of the included patients were extracted from the structured electronic medical records system.
All patients were followed up by telephone from 3 days to 3 weeks after discharge. Their family members completed screening tests by viral nucleic acid testing at designated adult hospitals. The follow-up calls collected the subsequent clinical manifestations of the children and family members and the RT-PCR test results of family members at designated adult medical facilities.
STATISTICAL ANALYSIS:
Statistical analyses were performed using SPSS 22.0 (IBM, Armonk, NY, USA). Descriptive statistics were used to interpret the patterns of the clinical characteristics. The
Results
GENERAL PATIENT CHARACTERISTICS:
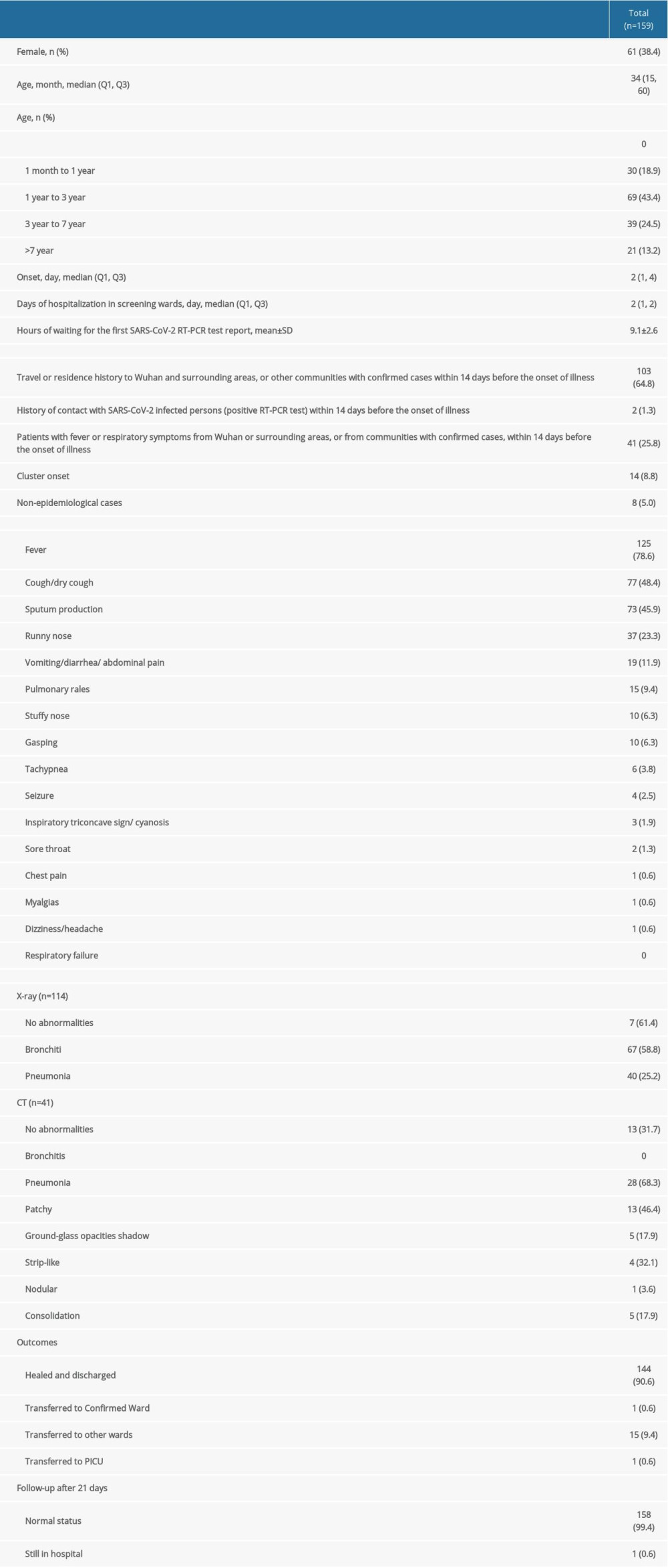
Among the 159 included patients (98 boys and 61 girls), the median age was 34 months (interquartile range: 15, 60); onset occurred an average of 4.79 days after exposure and the average length of hospitalization in the suspected-infection screening wards was 1.61 days (Table 1). The screening flow chart is shown in Figure 1.
EPIDEMIOLOGY:
A total of 64.8% of the study population had travel, residence history of travel, or residence in Wuhan or its surrounding areas or in communities with confirmed cases within 14 days before symptom onset. Among the 2 patients who had a history of contact with infected persons, 1 was confirmed with SARS-CoV-2 infection while the other was found negative by RT-PCR testing. The 25.8% of the population who had history of contact with a patient who had fever or respiratory symptoms from the epidemic area within 14 days before onset tested negative. Fourteen cases had cluster onset and 8 cases had no epidemiological history but had symptoms similar to those of COVID-19. There were 10 families of cluster cases without pathogenic microorganisms detected; however, among them, there were clusters of illnesses in close contact with symptomatic patients in the Hubei epidemic area (Table 1).
Some patients showed unconventional test results and clinical symptoms. Ground-glass opacity (GGO) changes in the chest CT scan was found in a 13-year-old asymptomatic sibling of a patient with confirmed COVID-19 (Figure 2), and she was negative for pharynx and anal swab RT-PCR tests for SARS-CoV-2. Four patients had other detected etiologies, including Staphylococcus humane (sepsis), Klebsiella pneumoniae (pneumonia), Escherichia coli (urinary tract infection), and mumps. There were 10 families of cluster cases without pathogenic microorganisms detected; however, among them, there were clusters of illnesses in close contact with symptomatic patients in the Hubei epidemic area (Table 1).
CLINICAL CHARACTERISTICS:
The clinical manifestation of 159 patients is shown in Table 2. Fever was the most common symptom (n=125), followed by respiratory symptoms (cough=77, sputum=73, and runny nose=37) and gastrointestinal symptoms (vomiting, diarrhea, and abdominal pain). However, a patient with confirmed COVID-19 was asymptomatic, but GGOs were seen in the anterior basal segment of his right lung by CT scanning (Figure 3). No pathogens were detected in 103 patients.
Laboratory evaluation of 57 cases detected non-SARS-CoV-2 etiology, including 2 patients with 2 pathogenic infections (Table 2).
PRESENTATION OF 2 FAMILIES WITH SARS-COV-2 INFECTION:
In family 1, a 7-year-old boy (case A) with a history of a cluster onset family from Wuhan was confirmed with SARS-CoV-2 by RT-PCR from an anus swab. His early throat swab RT-PCR tests were negative and his anus swab did not turn negative until day 19 of his hospitalization. His chest CT scan showed small GGOs in the right lung (Figure 3). Case A with his family members (grandfather, case B; grandmother, case C; father, case D; mother, case E; and sister, case F) settled in Wuhan before the outbreak of COVID-19 disease in December 2019. On January 22, 2020, they took the high-speed train (G77) from Wuhan to their home in Guangzhou and underwent self-quarantine at home. Case C developed fever on February 11, and later regressed without medical treatment. Case B developed fever on February 15, tested positive for SARS-CoV-2 on February 20, and was hospitalized for isolation treatment. The other family members were tested by SARS-CoV-2 RT-PCR throat swab tests the next day. Case C tested negative and was isolated at home for observation. The test was positive in case D, who had no fever, cough or other discomforts, and was hospitalized for isolation. Cases E and F were asymptomatic and negative by the RT-PCR test for SARS-CoV-2. However, case F, a 13-year-old girl, showed a similar GGO shadow as her brother (case A) on her chest CT scan (Figure 2) and tested negative multiple times by pharynx and anal swab RT-PCR tests for SARS-CoV-2. These cases are represented in Figure 3, top panel.
Family 2 had 3 members (cases G–I, Figure 4, bottom panel) who lived in Xiaogan, Hubei, and went to Guangzhou on January 24, 2020. Case G, a 1-year-old boy, was admitted to the hospital on February 14, 2020, for fever. CT examination showed a few patchy shadows in the anterior segment of the right upper lobe. A throat swab was negative by RT-PCR testing for SARS-CoV-2. He and his family members, father (case H) and mother (case I), returned to Xiaogan, Hubei, by car from January 20 to 24, 2020, and had contacted relatives who returned from Wuhan and had no fever, cough, or other symptoms. On January 24, the family drove home from Xiaogan, Hubei to Guangzhou. Case H had fever on the same day, accompanied by fatigue and pain in both lower extremities. His blood tests and chest CT scan were normal on January 24, but ground-glass nodules in the right upper lobe were revealed on a duplicate CT scan on February 9th, and no SARS-CoV-2 RT-PCR test was performed. From February 13, case I had a mild cough and runny nose without fever and was negative for SARS-CoV-2 by a RT-PCR test.
ETIOLOGY OF NON-SARS-COV-2 PATIENTS:
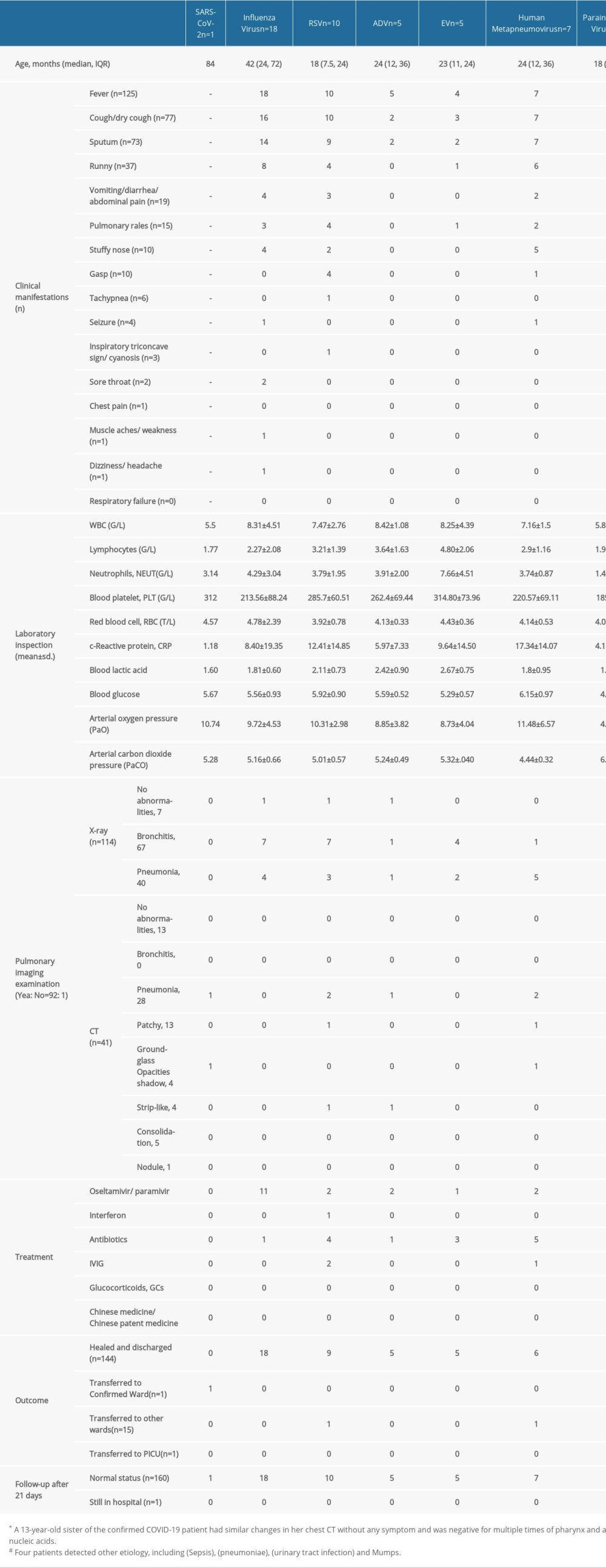
Influenza virus was most common (n=14) in the non-SARS-CoV-2 patients, followed by respiratory syncytial virus and adenovirus. Most patients’ blood cell counts and C-reactive protein levels indicated common viral infection, and the blood cell counts and C-reactive protein levels of patients with bacterial infections were consistent with the changes.
Pulmonary imaging examination was done for 154 patients (96.86%) within 24 h of admission, including 112 X-ray examinations and 42 CT examinations. X-ray results showed 7 patients with no abnormal manifestations, while 62 were diagnosed with bronchitis and 43 were diagnosed with pneumonia. The results of a CT examination showed no abnormalities in 13 patients and pneumonia in 29 patients. GGOs were observed in 4 patients with pneumonia, of which 1 SARS-CoV-2-infected patient presented GGOs in the lateral segment of the right middle lobe, mainly distributed in the periphery of the lung. In 3 other cases with GGOs, 1 case had human metapneumovirus and 2 cases had undetected pathogens. In addition, various CT patterns such as patchy, strip-like, nodular shadow and consolidation were observed.
DIAGNOSIS, TREATMENT, DISTRIBUTION, OUTCOME, AND FOLLOW-UP:
Cases of pneumonia (n=57), bronchitis (n=49), and acute upper respiratory tract infection (n=22) were most common in our study. There were 2 patients with sepsis, 1 with mumps, and 1 with congenital heart disease with Klebsiella pneumoniae infection. All 159 screening patients were treated symptomatically with anti-pathogenic treatment, such as oseltamivir for influenza, azithromycin for mycoplasma pneumonia, and antibiotics. Intravenous immunoglobulins were used in a few patients who had serious medical conditions. Among those who tested negative for SARS-CoV-2, 15 patients were transferred to single rooms in other specialty wards (Figure 4). Except for the 1 patient transferred to the PICU, 158 patients recovered and were discharged by March 20, 2020. Three days after discharge, there were 8 patients with fever (mainly hypothermia) and 30 patients with cough; 7 days after discharge, there were 2 patients with fever and 14 patients with cough; 14 days after discharge, there were no patients with fever and 6 patients with cough; no abnormalities were seen 21 days after discharge. A 7-day follow-up was done for the 2 representative cluster families; family members had mild fever, cough, and diarrhea symptoms initially, but no abnormalities were seen after 21 days. One family’s members (Figure 4, top panel, family 1) who were in close contact with the confirmed person had no symptoms while in isolation at their designated place within 14 days of discharge, and their pharyngeal and anal swabs were negative for multiple consecutive tests.
Discussion
The current study describes the clinical characteristics and management of suspected and confirmed cases of SARS-CoV-2 infection in children in Guangzhou.
The emergence of COVID-19 has attracted global attention, and the WHO has declared the COVID-19 a public health emergency of international concern [13]. Some pediatric patients confirmed with COVID-19 are asymptomatic [14,15]. The basic reproduction number of COVID-19 is affected by many factors [16,17] which might make it difficult to assess the true impact of the pandemic. Also, family members are required to accompany the screening patient during hospitalization, impeding epidemic prevention in the pediatric screening ward [18]. The prevention and control strategy of nosocomial infections for SARS-CoV-2 is “standard prevention & contact isolation & droplet isolation & air isolation”.
Family clusters and close contact with persons with confirmed SARS-CoV-2 are the primary forms of transmission in pediatric infected patients [14,19]. In the current study, among the 159 patients who were screened, 151 patients had epidemiological histories; but the patient confirmed with SARS-CoV-2 was in a cluster family from Wuhan and in close contact with positive patients. There can be transmission from asymptomatic patients and also from patients in the incubation period to other members in a family cluster [14,20]. Therefore, in addition to managing the sources of infection, cutting off the route of transmission requires leaving the environment with a high viral load or implementing terminal disinfection in enclosed spaces.
The patient with confirmed SARS-CoV-2 in our study was asymptomatic, similar to patients in previous studies [14,18]. Compared to adult patients, pediatric patients with SARS-CoV-2 infection had clinically milder symptoms and show fewer alterations in radiological and laboratory testing parameters [15,21–24]. GGOs in lung CT scan changes are commonly seen in infected pediatric patients, whether they were asymptomatic or had mild or severe symptoms [21,22,25]. We found that GGOs on lung CT scan could be seen in patients with SARS-CoV-2 and human metapneumovirus infection and in children without positive pathogens. The CT scan patterns of COVID-19 pneumonia may overlap with other pneumonia types, especially viral pneumonia [26]. Therefore, it is essential to differentiate between symptoms with respect to pneumonia caused by different pathogens, such as adenovirus, respiratory syncytial virus, severe acute respiratory syndrome, bacterial pneumonia, and mycoplasma pneumonia [26,27].
Most of the children admitted to screening wards had an epidemiological history and similar clinical manifestations consistent with laboratory results of viral infections and changes in lung imaging. But only 1 patient who tested negative by pharyngeal swab was confirmed by anal swab RT-PCR for SARS-CoV-2. Patients negative for SARS-CoV-2 infection had influenza virus, respiratory syncytial virus, adenovirus, and other viral infections which were common for the season, with even cluster onset in some families. It was noteworthy that a 13-year-old sister who had close contact with her brother who was confirmed with SARS-CoV-2 infection, had similar changes in her lung CT scan to her brother but tested negative in multiple anal and pharyngeal swab RT-PCR tests. The positive rate of SARS-CoV-2 on CT chest scans in adults was about 60% [23], and in children was close to 35% [25]; moreover, the positive rate is related to the course of sampling and the detection method [28,29]. Interestingly, patients who were RNA-positive and RNA-negative for COVID-19 shared similar clinical symptoms [30]. Therefore, a single negative RT-PCR test result cannot be an exclusion criterion to deem children fit and rid of SARS-CoV-2 infection. Positive SARS-CoV-2 RT-PCR anal swab test results in our confirmed patient continued until day 19 of hospitalization. Viral RNA measurements suggest that viral shedding from the digestive system is greater and lasts longer than that from the respiratory tract; hence rectal swab testing may be more useful than nasopharyngeal swab testing in judging the effectiveness of treatment and determining the timing of termination of quarantine [21]. From our results, we determined that 2 consecutive negative SARS-CoV-2 RT-PCR tests by anal swab could be a criterion to discharge a pediatric patient from the screening ward. Research suggests that the detection of serum IgM and IgG antibodies simultaneously against SARS-CoV-2 in human blood is a valid criterion [29,31], but we did not implement this in our screening patients.
Our study had limitations including the inherent bias of the retrospective nature of the study. Also, our study population size was small, and a variety of tests suggested by other research groups were not performed. Nevertheless, our study is of importance since we showed that consecutive negative tests from anal swabs might be a good indicator for the discharge of patients.
Conclusions
For SARS-CoV-2 nosocomial infections, using the “standard prevention & contact isolation & droplet isolation & air isolation” strategy can prevent the spread of infection to pediatric patients. For clustered onset pediatric patients, a minimum isolation period longer than 14 days during the epidemic or 2 consecutive negative tests with anal swabs more than 24 h apart could determine the timing of termination of quarantine.
Supplementary Material
Standard prevention & contact isolation & droplet isolation & air isolation
1. ORGANIZATION OF SUSPECTED SCREENING WARDS:
The center had designated management department for COVID-19 and clarified responsibilities and set up a dedicated isolation building for suspected and confirmed patients. The isolation building includes one Confirmed Ward and two Screening Wards, the latter of which were described in this article. Nosocomial Infection Prevention strategy in the Screening Wards were standard prevention & contact isolation & droplet isolation & air isolation.
2. AREA DIVISION AND PROTECTIVE MATERIALS: Screening wards are strictly divided into clean areas, semi-contaminated areas and isolation areas. The personal protective equipment (PPE) for staff with corresponding protection levels and disinfection showed in Supplementary Table 1.
Staff Workplace Medical activity Work clothes Waterproof isolation gown Latex gloves Work hat Medical protective mask Protective goggles/mask Protection suit Shoe cover Long sleeve thick rubber gloves Medical staff Suspected/ Screening Wards General medical activities without contacting the patients, non-body fluid exposure risks, such as Inquiry Station, Ward round, Physical Examination etc. √ √ or fabric isolation gown √ √ √ √ √ or Work shoes Medical staff Suspected/ Screening Wards Collection of respiratory samples, venipuncture, handling body fluids and other body fluid spraying actives. √ √ Double √ √ √ or Power-to-air filter respirator √ √ or Work shoes Confirmed Ward All medical activities √ √ if necessary Double √ √ √ or Power-to-air filter respirator √ √ √ or Work shoes Cleaning staff Suspected/ Screening Wads Cleaning, medical waste disposer √ √ or fabric isolation gown √ √ √ √ √ or work shoes, rubber boots √
Figures
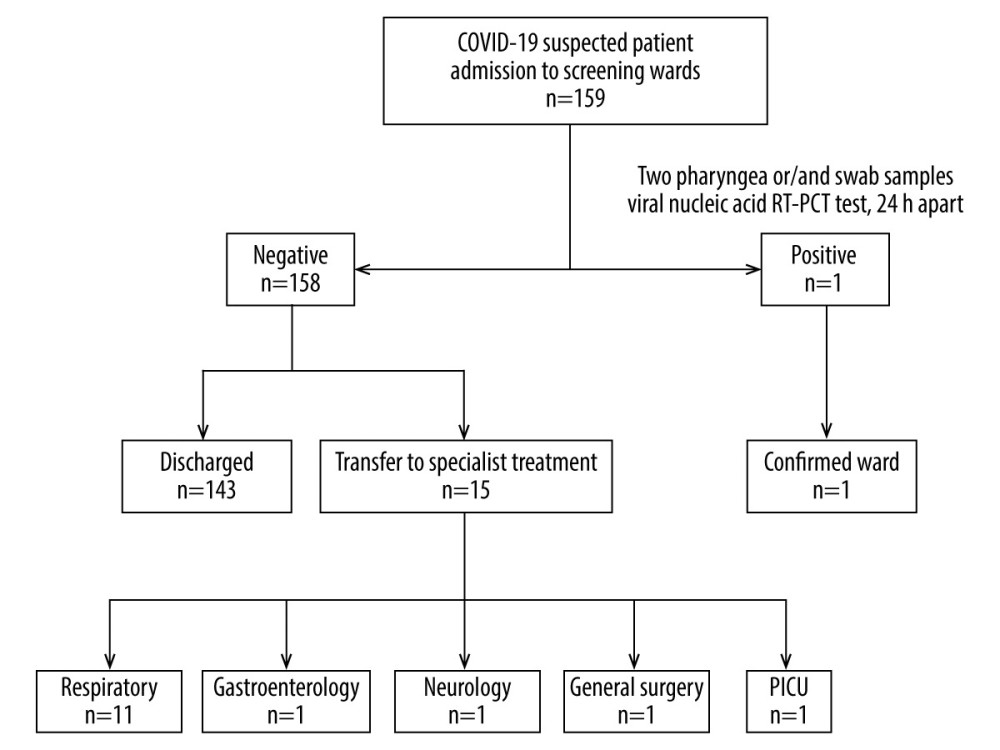 Figure 1. Screening and distribution of suspected patients with COVID-19.
Figure 1. Screening and distribution of suspected patients with COVID-19. 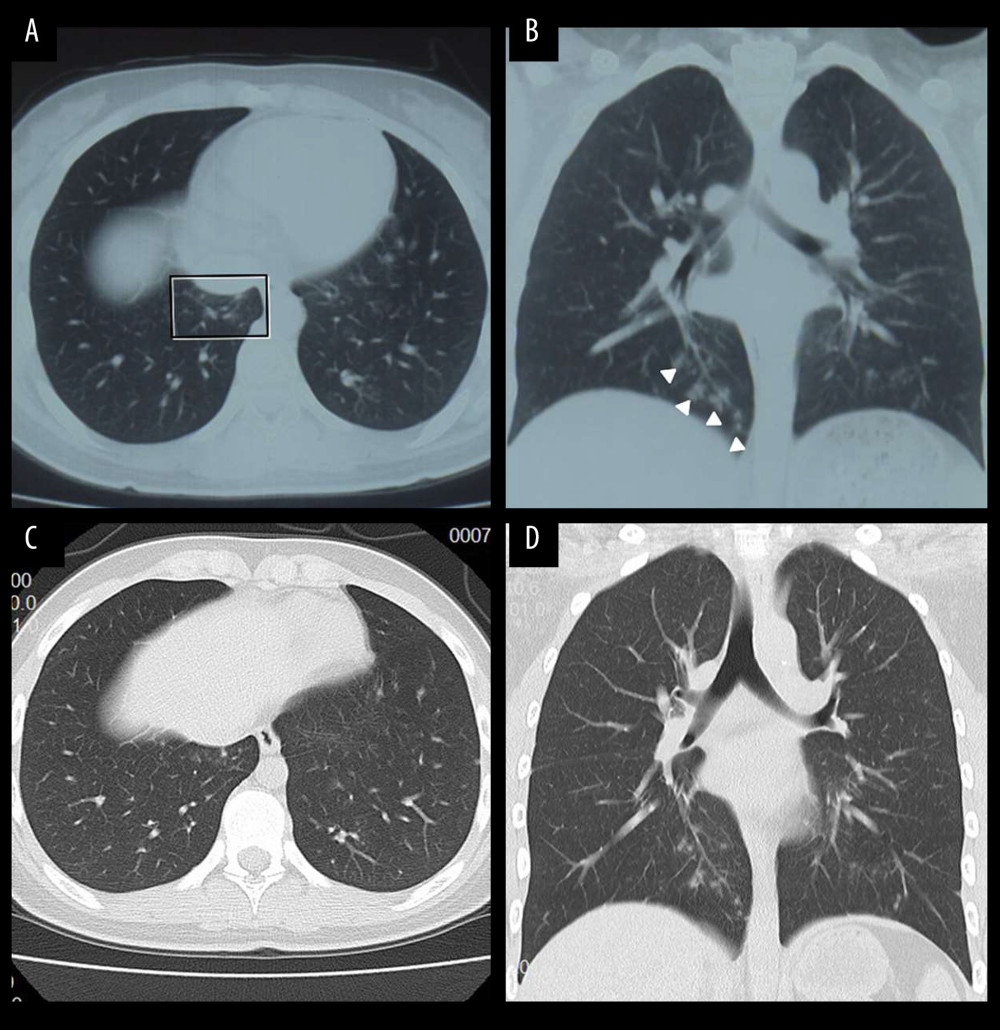 Figure 2. Computed tomography images of a 13-year-old girl (case F from family 1) 2 days after exposure to patients positive for COVID-19 (grandfather and father). (A) Ground-glass opacities and (B) nodules (arrow) were seen in the medial-basal segment of the right lung. Five days later, the ground-glass opacities were (C) absorbed and the nodules were (D) smaller.
Figure 2. Computed tomography images of a 13-year-old girl (case F from family 1) 2 days after exposure to patients positive for COVID-19 (grandfather and father). (A) Ground-glass opacities and (B) nodules (arrow) were seen in the medial-basal segment of the right lung. Five days later, the ground-glass opacities were (C) absorbed and the nodules were (D) smaller. 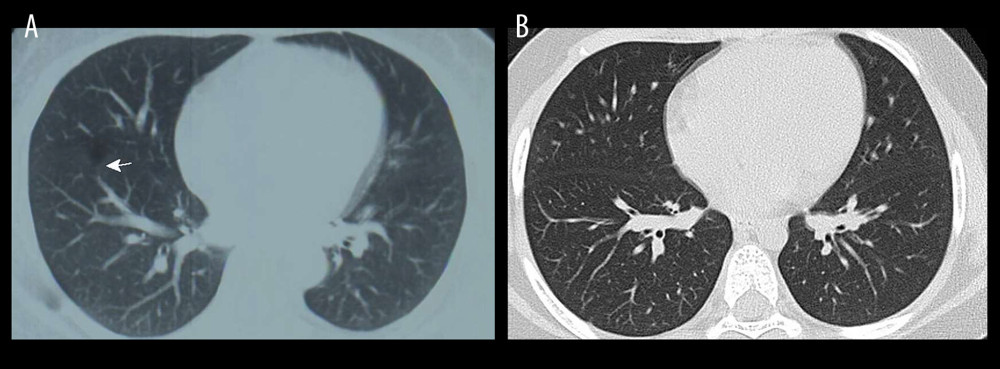 Figure 3. Computed tomography images of a 7-year-old boy (case A from family 1). (A) Ground-glass opacities (arrow) were seen in the anterior basal segment of the right lung. (B) Seven days later, the ground-glass opacities of the right lung were absorbed completely.
Figure 3. Computed tomography images of a 7-year-old boy (case A from family 1). (A) Ground-glass opacities (arrow) were seen in the anterior basal segment of the right lung. (B) Seven days later, the ground-glass opacities of the right lung were absorbed completely. 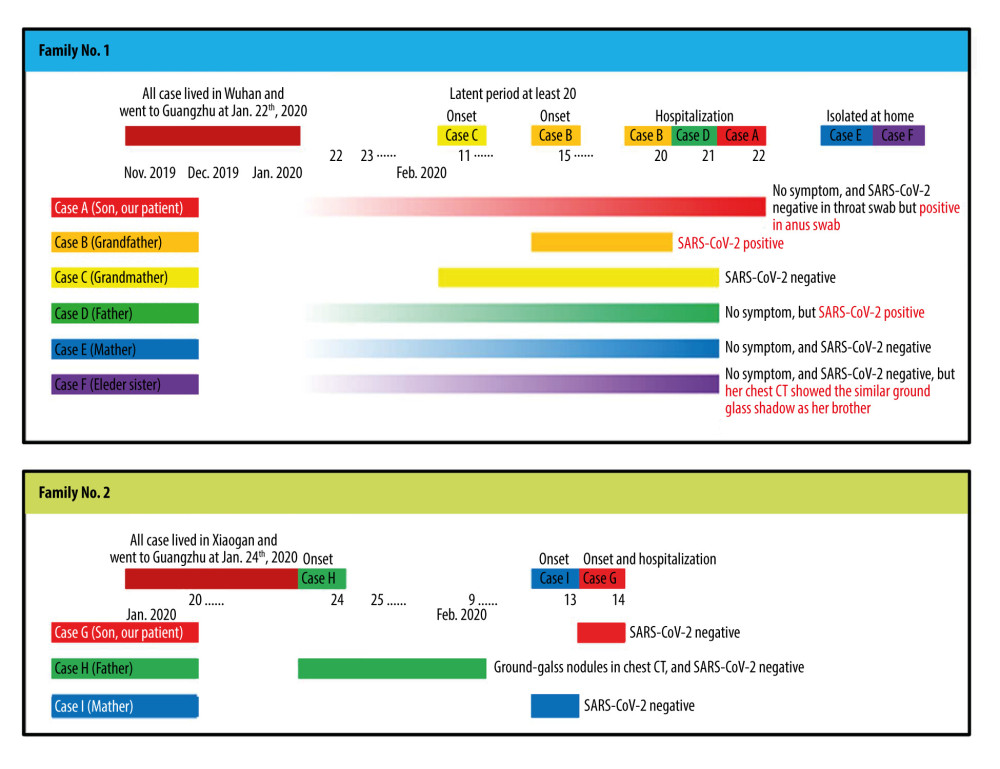 Figure 4. Time-map of onset and diagnosis of the 2 representative families with cluster cases and a history of close contact in Hubei.
Figure 4. Time-map of onset and diagnosis of the 2 representative families with cluster cases and a history of close contact in Hubei. References
1. Coronaviridae Study Group of the International Committee on Taxonomy of Viruses, The species severe acute respiratory syndrome-related coronavirus: Classifying 2019-nCoV and naming it SARS-CoV-2: Nat Microbiol, 2020; 5(4); 536-44
2. World Health Organization: Depression and Other Common Mental Disorders. Global Health Estimates, 2017, Geneva, World Health Organization
3. Announcement of the National Health Commission of the People’s Republic of China, 2020 http://www.nhc.gov.cn/jkj/s7916/202001/44a3b8245e8049d2837a4f27529cd386.shtml
4. Lu J, Gu J, Li K, COVID-19 outbreak associated with air conditioning in restaurant, Guangzhou, China, 2020: Emerg Infect Dis, 2020; 26(7); 1628-31
5. He X, Lau EHY, Wu P, Temporal dynamics in viral shedding and transmissibility of COVID-19: Nat Med, 2020; 26(5); 672-75
6. Li Y, Yao L, Li J, Stability issues of RT-PCR testing of SARS-CoV-2 for hospitalized patients clinically diagnosed with COVID-19: J Med Virol, 2020; 92(7); 903-8
7. Huang M, Tang T, Pang P, Treating COVID-19 with chloroquine: J Molec Cell Biol, 2020; 12(4); 322-25
8. Wu Z, McGoogan JM, Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: Summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention: JAMA, 2020; 323(13); 1239-42
9. Zimmermann P, Curtis N, Coronavirus infections in children including COVID-19: An overview of the epidemiology, clinical features, diagnosis, treatment and prevention options in children: Pediatr Infect Dis J, 2020; 39(5); 355-68
10. Dong Y, Mo X, Hu Y, Epidemiology of COVID-19 among children in China: Pediatrics, 2020; 145(6); e20200702
11. Lu X, Zhang L, Du H, SARS-CoV-2 infection in children: N Engl J Med, 2020; 382(17); 1663-65
12. Pediatric Branch of Guangdong Medical Association, Guangdong Provincial Pediatric Quality Control Center, Pediatric Branch of Guangzhou Medical Association, Center GPQC, Consensus of experts in the diagnosis and treatment of children with SARS-CoV-2 infection in Guangdong Province: Guangdong Med, 2020; 41(3); 217-21
13. Cucinotta D, Vanelli M, WHO declares COVID-19 a pandemic: Acta Biomedica, 2020; 91(1); 157-60
14. Qian G, Yang N, Ma AHY, A COVID-19 Transmission within a family cluster by presymptomatic infectors in China: Clin Infect Dis, 2020; 71(15); 861-62
15. Dong Y, Mo X, Epidemiological characteristics of 2143 pediatric patients with 2019 coronavirus disease in China: Pediatrics, 2020
16. Viceconte G, Petrosillo N, COVID-19 R0: Magic number or conundrum?: Infect Dis Rep, 2020; 12(1); 8516
17. Munster VJ, Koopmans M, van Doremalen N, A novel coronavirus emerging in China – key questions for impact assessment: N Engl J Med, 2020; 382(8); 692-94
18. Kelvin AA, Halperin S, COVID-19 in children: The link in the transmission chain: Lancet Infect Dis, 2020; 20(6); 633-34
19. Ji LN, Chao S, Wang YJ, Clinical features of pediatric patients with COVID-19: A report of two family cluster cases: World J Pediatr, 2020; 16(3); 267-70
20. Ye F, Xu S, Rong Z, Delivery of infection from asymptomatic carriers of COVID-19 in a familial cluster: Clin Infect Dis, 2020; 94; 133-38
21. Xu Y, Li X, Zhu B, Characteristics of pediatric SARS-CoV-2 infection and potential evidence for persistent fecal viral shedding: Nat Med, 2020; 26(4); 502-5
22. Zhou Y, Yang GD, Feng KClinical features and chest CT findings of coronavirus disease 2019 in infants and young children: Zhongguo Dang Dai Er Ke Za Zhi, 2020; 22(3); 215-20 [in Chinese]
23. Ai T, Yang Z, Hou H, Correlation of chest CT and RT-PCR testing in coronavirus disease 2019 (COVID-19) in China: A report of 1014 cases: Radiology, 2020; 296(2); 200642
24. Sinha IP, Harwood R, Semple MG, COVID-19 infection in children: Lancet Respir Med, 2020; 8(5); 446-47
25. Sun D, Li H, Lu XX, Clinical features of severe pediatric patients with coronavirus disease 2019 in Wuhan: A single center’s observational study: World J Pediatr, 2020; 16(3); 251-59
26. Koo HJ, Lim S, Choe J, Radiographic and CT features of viral pneumonia: Radiographics, 2018; 38(3); 719-39
27. Virkki R, Juven T, Rikalainen H, Differentiation of bacterial and viral pneumonia in children: Thorax, 2002; 57(5); 438-41
28. Zeng LK, Tao XW, Yuan WHFirst case of neonate with COVID-19 in China: Zhonghua Er Ke Za Zhi, 2020; 58(4); 279-80 [in Chinese]
29. Tang YW, Schmitz JE, Persing DH, Stratton CW, Laboratory diagnosis of COVID-19: Current issues and challenges: J Clin Microbiol, 2020; 58(6); e00512-20
30. Li YY, Wang WN, Lei YComparison of the clinical characteristics between RNA positive and negative patients clinically diagnosed with 2019 novel coronavirus pneumonia]: Zhonghua Jie He He Hu Xi Za Zhi, 2020; 43(5); 247-30 [in Chinees]
31. Li Z, Yi Y, Luo X, Development and clinical application of a rapid IgM-IgG combined antibody test for SARS-CoV-2 infection diagnosis: J Med Virol, 2020 [Online ahead of print]
Figures
 Figure 1. Screening and distribution of suspected patients with COVID-19.
Figure 1. Screening and distribution of suspected patients with COVID-19. Figure 2. Computed tomography images of a 13-year-old girl (case F from family 1) 2 days after exposure to patients positive for COVID-19 (grandfather and father). (A) Ground-glass opacities and (B) nodules (arrow) were seen in the medial-basal segment of the right lung. Five days later, the ground-glass opacities were (C) absorbed and the nodules were (D) smaller.
Figure 2. Computed tomography images of a 13-year-old girl (case F from family 1) 2 days after exposure to patients positive for COVID-19 (grandfather and father). (A) Ground-glass opacities and (B) nodules (arrow) were seen in the medial-basal segment of the right lung. Five days later, the ground-glass opacities were (C) absorbed and the nodules were (D) smaller. Figure 3. Computed tomography images of a 7-year-old boy (case A from family 1). (A) Ground-glass opacities (arrow) were seen in the anterior basal segment of the right lung. (B) Seven days later, the ground-glass opacities of the right lung were absorbed completely.
Figure 3. Computed tomography images of a 7-year-old boy (case A from family 1). (A) Ground-glass opacities (arrow) were seen in the anterior basal segment of the right lung. (B) Seven days later, the ground-glass opacities of the right lung were absorbed completely. Figure 4. Time-map of onset and diagnosis of the 2 representative families with cluster cases and a history of close contact in Hubei.
Figure 4. Time-map of onset and diagnosis of the 2 representative families with cluster cases and a history of close contact in Hubei. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387