19 December 2020: Database Analysis
Clinical Characteristics and Risk Factors in Coronavirus Disease 2019 Patients with Liver Injury
Dali Zhang1ABCE*, Zhenyu Zhu1BDF, Jingfeng Bi2C, Danni Feng1F, Lijuan Zhang1CD, Hongling Liu1DE, Yinjie Gao1ADFGDOI: 10.12659/MSM.928849
Med Sci Monit 2020; 26:e928849
Abstract
BACKGROUND: Emerging studies noted that liver injury in coronavirus disease 2019 (COVID-19) patients may be induced by virus-mediated inflammation, which was confirmed by liver pathology. The aim of this study was to observe clinical characteristics and explore risk factors in COVID-19 patients with liver injury.
MATERIAL AND METHODS: In this retrospective study, 40 confirmed COVID-19 patients with normal alanine transaminase (ALT) on admission were divided into a group of normal ALT patients whose ALT was always less than 40 U/l during hospitalization and a group of elevated ALT patients whose ALT was at least once more than 40 U/l after admission. Clinical data, especially virus-induced inflammatory parameters, were analyzed for risk factors and predictive value. The Mann-Whitney U test and t test for comparing means and logistic regression were performed for analysis of risk factors. Area under the ROC curve was used for predictive values.
RESULTS: Sixteen of 40 (40.0%) patients developed elevated ALT, many of them with more severe COVID-19. The highest ALT level was 101 U/l. The risk factors for liver injury were C-reactive protein (CRP), interleukin 6 (IL6), erythrocyte sedimentation rate (ESR), CD8+T cell count, and severity of disease, and CRP (OR 1.13, 95% CI 1.045–1.222, p=0.002) was the independent risk factor.
CONCLUSIONS: Liver injury in COVID-19 patients was mild and associated with inflammatory markers, especially CRP, which suggests that liver injury may be induced by virus-mediated inflammation in COVID-19 patients.
Keywords: COVID-19, drug-induced liver injury, Systemic Inflammatory Response Syndrome, Alanine Transaminase, Aspartate Aminotransferases, Blood Sedimentation, C-Reactive Protein, COVID-19, Coronavirus, Hospitalization, Interleukin-6, Liver, Lymphocyte Count, ROC Curve, Risk Factors, SARS-CoV-2
Background
Coronavirus disease 2019 (COVID-19) is caused by a novel coronavirus which was identified as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) [1]. The World Health Organization (WHO) has reported millions of confirmed cases and deaths worldwide. We are facing an unprecedent challenge of the catastrophe at this pivotal moment.
Recent studies showed 14–53% of COVID-19 patients experienced different degrees of liver injury [1–6], which is associated with inflammatory cytokine storm. Wang et al. provided pathological evidence that abundant SARS-CoV-2 viral particles were observed in cytoplasm of hepatocytes in COVID-19 cases [7]. In light of this, the virus-induced inflammation might be the main mechanism of liver injury. C-reactive protein (CRP), a classical maker of immune-mediated inflammation, which is high in COVID-19 patients with liver injury, supports this hypothesis [8], but whether such inflammatory markers have predictive values is unknown. Thus, we retrospectively analyzed COVID-19 patients treated at our hospital to explore risk factors and observe clinical characteristics in COVID-19 patients with liver injury.
Material and Methods
STUDY DESIGN AND PATIENTS:
This was a retrospective single-center cohort study of COVID-19 patients who had been admitted to a referral hospital from January 20, 2020 to March 30, 2020. Throat swab samples were collected for testing SARS-CoV-2 RNA. All cases were confirmed at least twice to have positive results of real-time reverse-transcriptase polymerase chain reaction (RT-PCR) and diagnosed with COVID-19 according to the criteria of guidance [9]. Informed consents were obtained and the study was approved by the Hospital Ethics Review Board and complied with the Declaration of Helsinki.
The clinical classifications of COVID19 are mild, moderate, severe, and critical (see supplementary appendix). Except for 13 patients who had abnormal liver function on admission, 40 patients were divided into 2 groups based on alanine transaminase (ALT) level: 1) patients with ALT always less than 40 U/l after admission (normal ALT), and 2) patients with ALT at least once more than 40 U/l during hospitalization (elevated ALT). The definition of acute kidney injury (AKI) [10] and acute cardiac injury (ACI) [11] are provided in the Supplementary Appendix.
DATA COLLECTION:
We collected data on epidemiology, past medical history, clinical features, laboratory, treatment, and outcomes from hospital electronic medical records. Laboratory tests mainly included white blood cell (WBC), neutrophil, lymphocyte, ALT, aspartate aminotransferase (AST), albumin (ALB), total bilirubin (TBil), alkaline phosphatase (ALP), gamma-glutamyl transpeptidase (GGT), interleukin 6 (IL-6), erythrocyte sedimentation rate (ESR), procalcitonin (PCT), CRP, total T lymphocyte cell, CD4 T lymphocyte cell, and CD8 T lymphocyte cell counts.
STATISTICAL ANALYSIS:
Continuous variables were described using mean, median, and interquartile range (IQR) values, and categorical variables were described as frequency rates and percentages. Continuous variables that were normally distributed were assessed using t tests for comparing means, while non-normally distributed data were assesses using the Mann-Whitney U test. Proportions for categorical variables were compared using the chi-square test. Logistic regression analysis was performed for risk factors, and area under the ROC curve was used for predictive values.
Results
DEMOGRAPHIC AND CLINICAL CHARACTERISTICS OF COVID-19 PATIENTS:
A total of 53 patients with COVID-19 were enrolled from January 20, 2020 to March 30, 2020, including 31 males and 22 females. The median age was 41.58±3.943 years old. Twenty-four patients had normal ALT, and 29 had elevated ALT, which included 13 patients with elevated ALT on admission and the remaining 16 patients had elevated ALT after admission. Sixteen patients experienced severe COVID-19, and most (81.3%) of them presented with ALT elevation (Supplementary Table 1).
CLINICAL CHARACTERISTIC IN COVID-19 PATIENTS WITH ELEVATED ALT:
Among those confirmed cases, 13 patients who had abnormal liver function on admission were excluded, and data from 40 patients were analyzed. Twenty-four patients had normal ALT and 16 had elevated ALT. Twenty-one patients were male with a mean age of 46.38±3.105 years. Some patients had coexisting medical conditions: 7 patients had hypertension, 4 had diabetes mellitus, and 1 had cardiac disease. No patients had liver disease or kidney disease (Table 1).
Among 16 patients with high ALT, the median time of first elevated ALT was 10.5 days after admission, and the highest level was 101 U/l (Figure 1A), which presented as mild liver injury.
Compared with normal liver function patients, liver injury patients had more severe COVID-19 cases (P=0.025) (Figure 1B), higher level of CRP (P=0.000), IL6 (P=0.021), ESR (P=0.02), creatinine (CRE) (P=0.033), and PCT(p=0.059), and lower level of CD8+T lymphocytes (P=0.013) (Table 1).
COMPLICATION, TREATMENTS, AND OUTCOMES IN COVID-19 PATIENTS WITH ELEVATED ALT:
There were no differences in WBC count, neutrophils count, or procalcitonin level between patients with and without liver injury. That is to say, there was no difference in bacterial infection between the 2 groups. Liver injury patients experienced more severe COVID-19, they were more likely to have received glucocorticoid (P=0.037) and immunoglobin (P=0.001), accompanied by antibacterial (P=0.006) therapy to prevent potential bacterial coinfection. No difference in receiving antiviral therapy was seen in the 2 groups patients, with most receiving lopinavir (31/40 cases) (Table 2). Two patients developed acute kidney injury, 3 developed acute cardiac injury, and there were no complications of septic shock or acute respiratory distress syndrome (ARDS). Up to April 11, 2020, there were 39 patients discharged and 1 death. The dynamic laboratory changes also showed liver injury patients had higher levels of CRP, IL6, and PCT during different stages of disease development (Figure 2). After treatment, these indicators improved (Figure 2).
RISK FACTORS FOR COVID-19 PATIENTS WITH LIVER INJURY:
Logistic regression analysis was performed for risk factors of liver injury based on the significantly different variables. Univariate logistic regression analysis indicated that baseline CRP (P=0.001), IL6 (P=0.011), ESR (P=0.010), and CD8+ T cell (P=0.022) were risk factors for liver injury, while stepwise multivariate logistic regression showed that CRP (P=0.002) was an independent risk factor for liver injury in COVID-19 patients (Table 3).
PREDICTIVE VALUE OF CRP FOR COVID-19 PATIENTS WITH LIVER INJURY:
To test the predictive value of CRP in liver injury patients, we performed ROC curve analysis. Result showed that the area under the ROC curve was 0.89 (95% CI: 0.766–1, P=0.000), a cutoff value 20.9 mg/l, sensitivity in detecting liver injury was 80% and specificity was 91.7% (Figure 3).
Discussion
The pandemic of COVID-19 has posed a threat to public health as SARS-CoV-2 spreads all over the world. Large-scale cases studies reported that extra-pulmonary damage occurs in COVID-19 patients, such as liver damage [8]. Recent studies showed that SARS-CoV-2 viral particles were present and replicated in hepatocytes, but whether liver damage was secondary to SARS-CoV-2 infection and whether inflammatory markers have predictive value in liver injury are unknown.
This retrospective cohort study focused on the natural course of liver injury. All patients had normal liver function on admission and 16 of them developed elevated ALT during hospitalization. This study documented the clinical features and the risk factors of the COVID-19 patients with liver injury. The incidence of liver injury was 40%, which is consistent with other studies [8,12]. We found liver injury mainly presented as mild or medium elevation of ALT, which was associated with COVID-19 severity. Inflammatory parameters such as IL6, ESR, and CRP were independent risk factors for liver injury. Using a cutoff value of baseline CRP more than 20.9 mg/l, COVID-19 patients were susceptible to have liver injury at a median follow-up of 10.5 days.
Currently, the likely mechanisms of liver injury in COVID-19 are virus-induced damage and drug-induced liver injury. Many studies considered it was induced by multiple factors [5,13,14]. In our study, the risk factors for liver injury were inflammatory markers, such as CRP, IL6, ESR, and the independent risk factor was an inflammatory marker, CRP, which means immune-mediated inflammation plays an important role. Recent studies confirmed that SARS-CoV-2 viral particles were not only observed in hepatocytes, but also replicate with abundant overactivated T lymphocytes infiltrated of liver tissue from severe COVID-19 patients [7,15,16]. Hence, virus-mediated inflammation might be involved in the development of liver injury in COVID-19 patients.
CRP is an acute-phase protein; hepatic production is induced by IL-6, and CRP is used as a systemic inflammatory marker in many diseases, such as COVID-19, infections, myocardial disease, and non-alcoholic fatty liver disease [17–19]. Recent studies found that CRP was significantly higher in metabolic-associated fatty liver disease (MAFLD), which is associated with COVID-19 severity [20,21]. This may partially account for why CRP was high in COVID-19 patients with liver injury [8,22]. Wang et al. reported that CRP levels were 19.5 mg/l and 9.8 mg/l in patients with abnormal and normal liver function, respectively, but the difference was not significant (
Liver injury is associated with COVID-19 severity. Virus-induced overactive immune-mediated inflammation, which is characterized by overwhelming release of inflammatory factors, leads to pulmonary injury and extra-pulmonary organ damage including the liver, heart, and kidneys. In our study, we had patients with liver injury, AKI, and ACI. Liver injury patients had higher levels of inflammation indicators such as CRP, IL6, and ESR, and lower levels of immune cells such as CD8+T lymphocytes. The occurrence of liver injury was associated to the progression of the disease, involving a dynamic process. These findings are consistent with those of other studies [2,23].
Our study has limitations, including the modest sample size, and the fact that CRP level may affected by confounding factors, suggesting that a stratified analysis would be better. Despite these limitations, our study showed that CRP level may play a role in liver injury in COVID-19 patients. Patients with MAFLD or SARS-CoV-2 infection all have high CRP levels and are prone to liver injury. The predictive value of CRP needs to be verified in a large-scale case study.
Conclusions
Liver injury in COVID-19 patients was mild and associated with inflammatory markers, especially CRP. Our study revealed that COVID-19 patients can have liver injury secondary to immune-mediated inflammation caused by SARS-CoV-2 infection. COVID-19 patients with high CRP levels should be carefully assessed and monitored for liver injury.
Supplementary Data
Methods
CLINICAL CLASSIFICATIONS:
The clinical classifications are as follows: (1) Mild, mild clinical symptoms, and imaging shows no pneumonia (2) Moderate, with fever, respiratory tract symptoms, and imaging shows pneumonia. (3) Severe, meet any of the following: a) respiratory distress, respiratory rate ≥30 beats/min; b) in the resting state, means oxygen saturation ≤93%; c) arterial blood oxygen partial pressure/oxygen concentration ≤300 mmHg (1 mmHg=0.133kPa). (4) Critical, one of the following conditions: a) respiratory failure occurs and requires mechanical ventilation; b) Shock occurs; c) ICU admission is required for combined organ failure.
DISCHARGE STANDARD DETERMINATION:
Discharge standard determination are as follows: (1) Body temperature return to normal at least more than 3 days. (2) Respiratory symptoms improved significantly. (3) Chest CT images reveal significant absorption of bilateral ground glass opacity. (4) At least two negative results on RT-PCR assay of pharyngeal swab specimens (24 hour interval).
ACUTE KIDNEY INJURY (AKI):
AKI was defined as either an increase in serum creatinine (SCr) by ≥0.3 mg/dl (≥26.5 μmol/L) within 48 hr or increase in SCr to ≥1.5 times of baseline within previous 7 days according to the Kidney Disease: Improving Global Outcomes definition.
ACUTE CARDIAC INJURY (ACI):
ACI was defined if the serum levels of cardiac biomarkers (e.g., troponin I) were above the 99th percentile upper reference limit or new abnormalities were shown in electrocardiography and echocardiography.
Figures
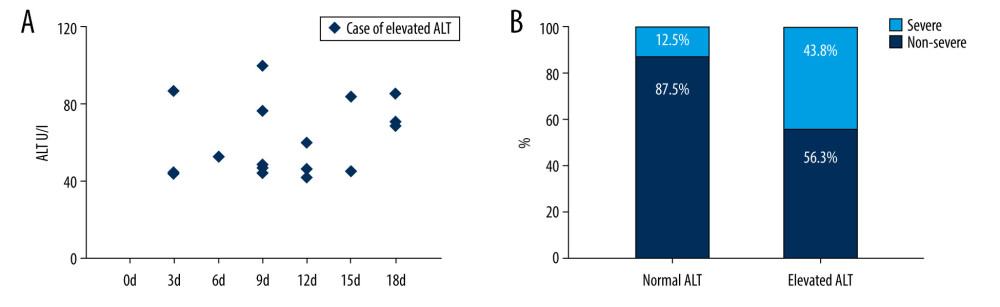 Figure 1. First time of ALT elevation onset day and COVID-19 patient severity with liver injury. (A) First time elevated ALT cases (n=16) on different days after admission. (B) Severity of COVID-19 patients and liver injury.
Figure 1. First time of ALT elevation onset day and COVID-19 patient severity with liver injury. (A) First time elevated ALT cases (n=16) on different days after admission. (B) Severity of COVID-19 patients and liver injury. 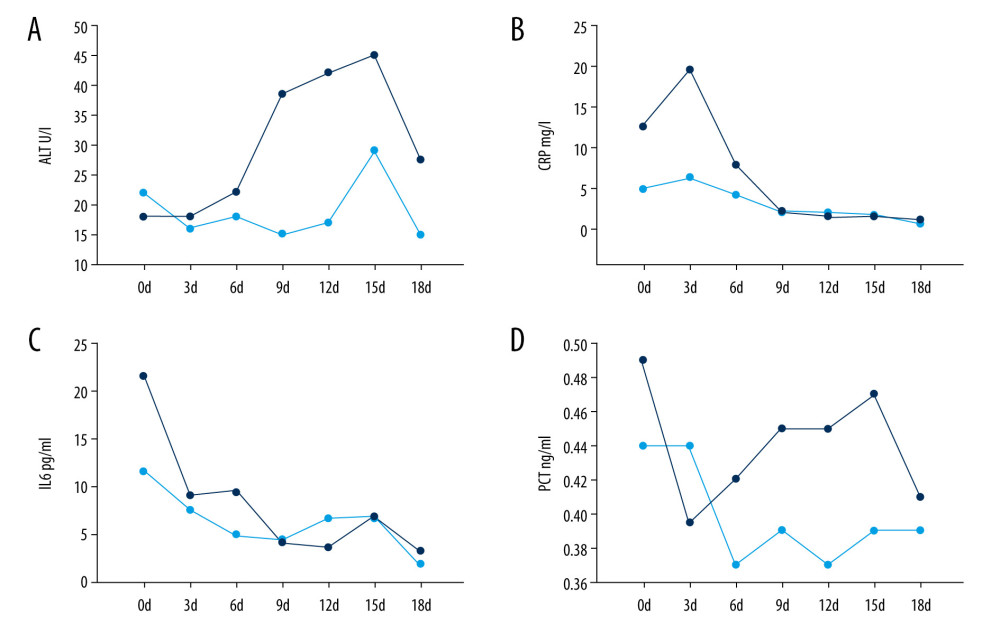 Figure 2. Dynamic profile of laboratory parameters in COVID-19 patients with liver injury. Dynamic Profile of ALT (A), CRP (B), IL6 (C), and PCT (D) in 39 patients (not including 1 death). Green line represents normal ALT group, while clay color represents the elevated ALT group.
Figure 2. Dynamic profile of laboratory parameters in COVID-19 patients with liver injury. Dynamic Profile of ALT (A), CRP (B), IL6 (C), and PCT (D) in 39 patients (not including 1 death). Green line represents normal ALT group, while clay color represents the elevated ALT group. 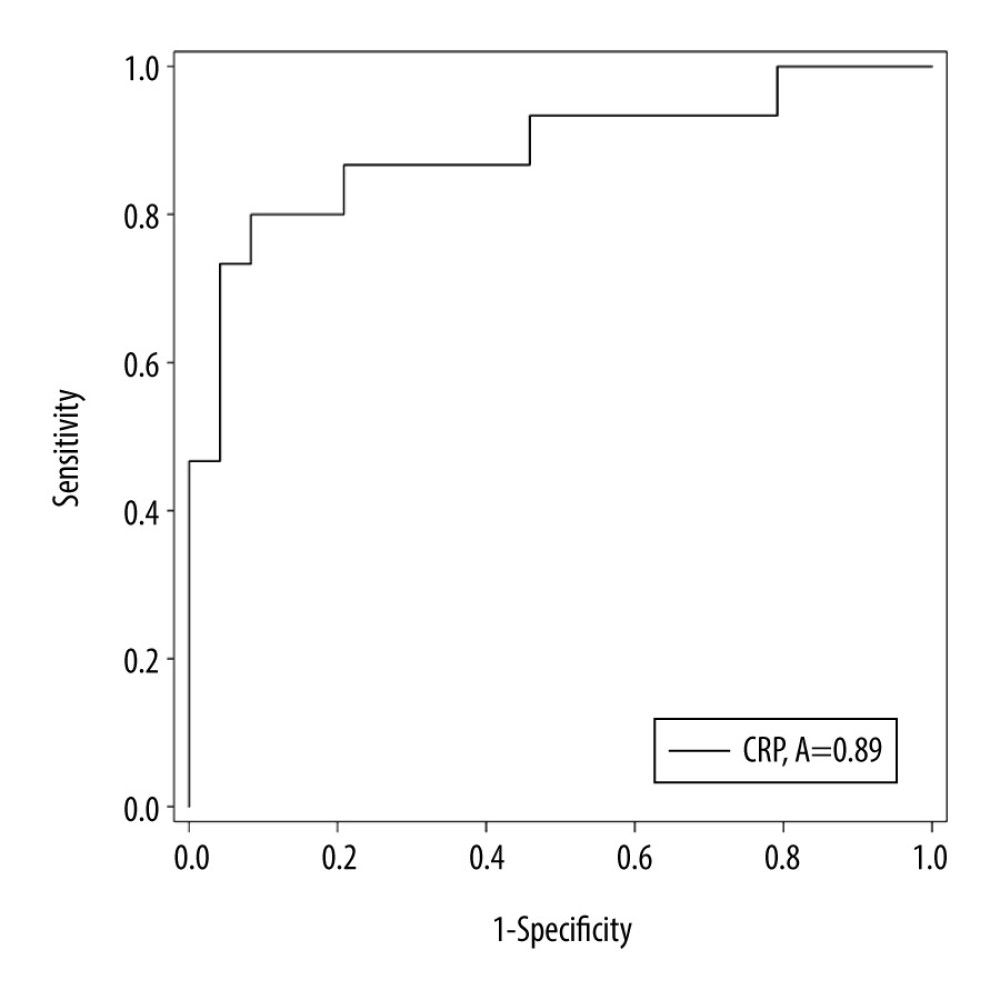 Figure 3. Predictive value of CRP in COVID-19 patients with liver injury. Predictive value for elevated ALT. Cutoff value of CRP was more than 20.9 mg/l on admission, the sensitivity for elevated ALT was 80% and specificity was 91.7% (area under the ROC curve=0.886, 95% CI: 0.766–1, P=0.000).
Figure 3. Predictive value of CRP in COVID-19 patients with liver injury. Predictive value for elevated ALT. Cutoff value of CRP was more than 20.9 mg/l on admission, the sensitivity for elevated ALT was 80% and specificity was 91.7% (area under the ROC curve=0.886, 95% CI: 0.766–1, P=0.000). References
1. International Committee on Taxonomy of Viruses Available from URLhttps://talk.ictvonline.org/
2. Guan WJ, Ni ZY, Hu Y, China Medical Treatment Expert Group for Covid-19: Clinical Characteristics of Coronavirus Disease 2019 in China: N Engl J Med, 2020; 382(18); 1708-20
3. Xu L, Liu J, Lu M, Liver injury during highly pathogenic human coronavirus infections: Liver Int, 2020; 40(5); 998-1004
4. Zhang C, Shi L, Wang F-S, Liver injury in COVID-19: Management and challenges: Lancet Gastroenterol Hepatol, 2020; 5; 428-30
5. Wong GL, Wong VW, Thompson A, Management of patients with liver derangement during the COVID-19 pandemic: An Asia-Pacific position statement: Lancet Gastroenterol Hepatol, 2020; 5; 776-87
6. Yip TC, Lui GC, Wong VW, Liver injury is independently associated with adverse clinical outcomes in patients with COVID-19: Gut, 2020 [Online ahead of print]
7. Wang Y, Liu S, Liu H, SARS-CoV-2 infection of the liver directly contributes to hepatic impairment in patients with COVID-19: J Hepatol, 2020; 73(4); 807-16
8. Zhu N, Zhang D, Wang W, A novel coronavirus from patients with pneumonia in China, 2019: N Engl J Med, 2020; 382; 727-33
9. : Guidance for Corona Virus Disease 2019: Prevention, Control, Diagnosis and Management, 2020, People’s Medical Publishing House
10. Khwaja A, KDIGO clinical practice guidelines for acute kidney injury: Nephron Clin Pract, 2012; 120; c179-84
11. Huang C, Wang Y, Li X, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China: Lancet, 2020; 395; 497-506
12. Chen N, Zhou M, Dong X, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study: Lancet, 2020; 395; 507-13
13. Bertolini A, van de Peppel IP, Bodewes FAJA, Abnormal liver function tests in patients with COVID-19: Relevance and potential pathogenesis: Hepatology, 2020; 72(5); 1864-72
14. Jothimani D, Venugopal R, Abedin MF, COVID-19 and the liver: J Hepatol, 2020; 73; 1231-40
15. Polakos NK, Cornejo JC, Murray DA, Kupffer cell-dependent hepatitis occurs during influenza infection: Am J Pathol, 2006; 168; 1169-78 quiz 404–5
16. Xu Z, Shi L, Wang Y, Pathological findings of COVID-19 associated with acute respiratory distress syndrome: Lancet Respir Med, 2020; 8; 420-22
17. Bi X, Loo YT, Ponnalagu S, Henry CJ, Obesity is an independent determinant of elevated C-reactive protein in healthy women but not men: Biomarkers, 2019; 24; 64-69
18. Nigam P, Bhatt SP, Misra A, Non-alcoholic fatty liver disease is closely associated with sub-clinical inflammation: A case-control study on Asian Indians in North India: PLoS One, 2013; 8; e49286
19. Xie H, Zhao J, Lian N, Clinical characteristics of non-ICU hospitalized patients with coronavirus disease 2019 and liver injury: A retrospective study: Liver Int, 2020; 40; 1321-26
20. Zhou YJ, Zheng KI, Wang XB, Metabolic-associated fatty liver disease is associated with severity of COVID-19: Liver Int, 2020; 40(9); 2160-63
21. Gao F, Zheng KI, Wang XB, Metabolic associated fatty liver disease increases coronavirus disease 2019 disease severity in nondiabetic patients: J Gastroenterol Hepatol, 2020 [Online ahead of print]
22. Gao L, Jiang D, Wen XS, Prognostic value of NT-proBNP in patients with severe COVID-19: Respir Res, 2020; 21; 83
23. Qin C, Zhou L, Hu Z, Dysregulation of immune response in patients with coronavirus 2019 (COVID-19) in Wuhan, China: Clin Infect Dis, 2020; 71(15); 762-68
Figures
 Figure 1. First time of ALT elevation onset day and COVID-19 patient severity with liver injury. (A) First time elevated ALT cases (n=16) on different days after admission. (B) Severity of COVID-19 patients and liver injury.
Figure 1. First time of ALT elevation onset day and COVID-19 patient severity with liver injury. (A) First time elevated ALT cases (n=16) on different days after admission. (B) Severity of COVID-19 patients and liver injury. Figure 2. Dynamic profile of laboratory parameters in COVID-19 patients with liver injury. Dynamic Profile of ALT (A), CRP (B), IL6 (C), and PCT (D) in 39 patients (not including 1 death). Green line represents normal ALT group, while clay color represents the elevated ALT group.
Figure 2. Dynamic profile of laboratory parameters in COVID-19 patients with liver injury. Dynamic Profile of ALT (A), CRP (B), IL6 (C), and PCT (D) in 39 patients (not including 1 death). Green line represents normal ALT group, while clay color represents the elevated ALT group. Figure 3. Predictive value of CRP in COVID-19 patients with liver injury. Predictive value for elevated ALT. Cutoff value of CRP was more than 20.9 mg/l on admission, the sensitivity for elevated ALT was 80% and specificity was 91.7% (area under the ROC curve=0.886, 95% CI: 0.766–1, P=0.000).
Figure 3. Predictive value of CRP in COVID-19 patients with liver injury. Predictive value for elevated ALT. Cutoff value of CRP was more than 20.9 mg/l on admission, the sensitivity for elevated ALT was 80% and specificity was 91.7% (area under the ROC curve=0.886, 95% CI: 0.766–1, P=0.000). Tables
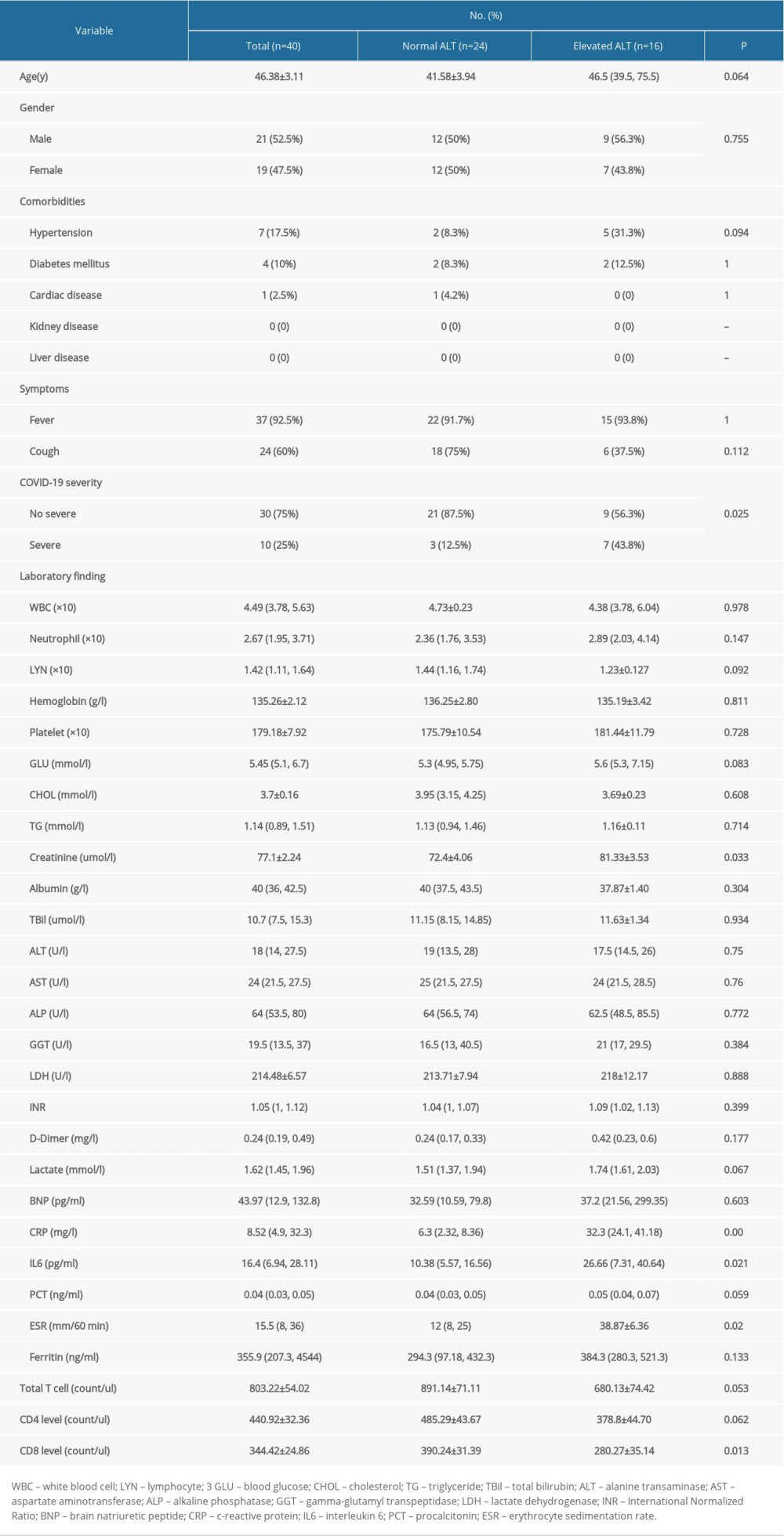 Table 1. Clinical characteristics of COVID-19 patients with liver injury.
Table 1. Clinical characteristics of COVID-19 patients with liver injury.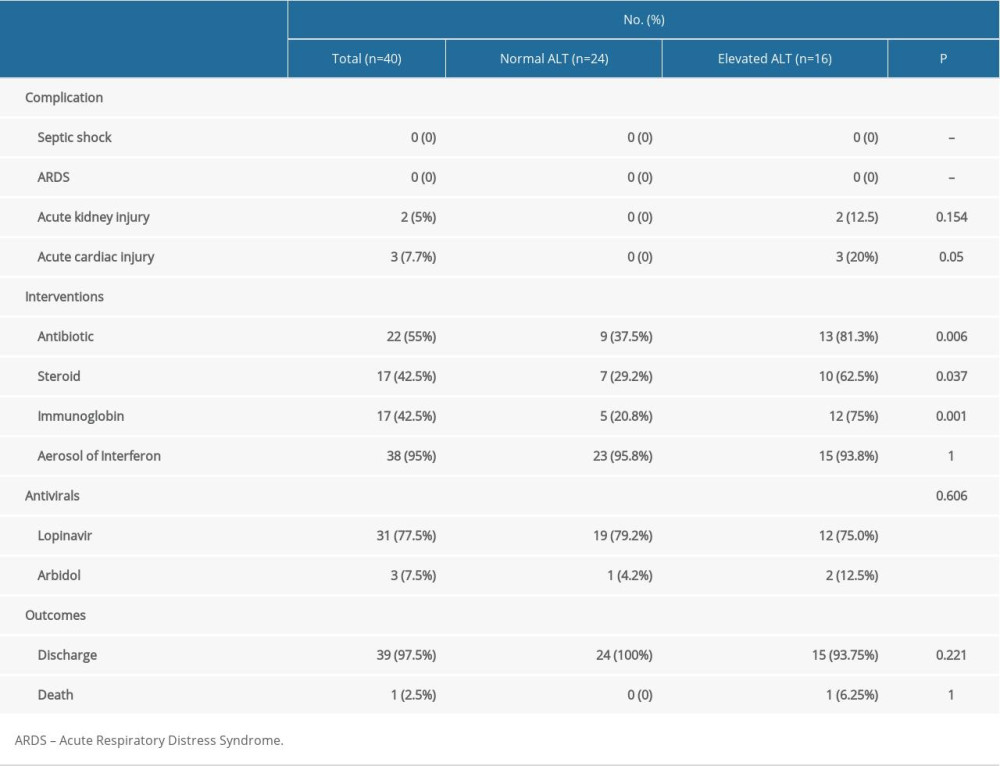 Table 2. Complications, interventions, and outcomes of COVID-19 patients.
Table 2. Complications, interventions, and outcomes of COVID-19 patients.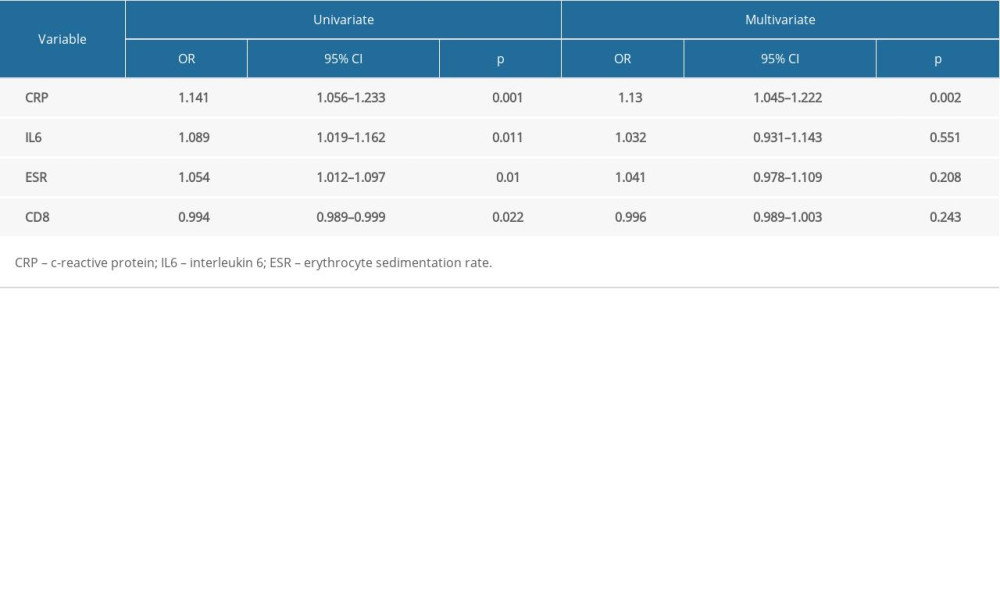 Table 3. Regression analysis for risk in COVID-19 patients with liver injury.
Table 3. Regression analysis for risk in COVID-19 patients with liver injury. Table 1. Clinical characteristics of COVID-19 patients with liver injury.
Table 1. Clinical characteristics of COVID-19 patients with liver injury. Table 2. Complications, interventions, and outcomes of COVID-19 patients.
Table 2. Complications, interventions, and outcomes of COVID-19 patients. Table 3. Regression analysis for risk in COVID-19 patients with liver injury.
Table 3. Regression analysis for risk in COVID-19 patients with liver injury. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








