12 February 2021: Animal Study
Effects of Betulinic Acid Derivative on Lung Inflammation in a Mouse Model of Chronic Obstructive Pulmonary Disease Induced by Particulate Matter 2.5
Qianyu Yue1BCDE, Xiaoli Deng1BCD, Yuntao Li1BCD, Yunhui Zhang1ADEFG*DOI: 10.12659/MSM.928954
Med Sci Monit 2021; 27:e928954
Abstract
BACKGROUND: Chronic obstructive pulmonary disease (COPD) is mainly induced by the increased content of particulate matter 2.5 (PM2.5) in the atmosphere. This study aimed to evaluate the effects of betulinic acid derivative on lung inflammation in a mouse model of chronic obstructive pulmonary disease induced by particulate matter 2.5.
MATERIAL AND METHODS: The mice were given a PM2.5 (25 μl) suspension for 7 days by the intranasal route to establish a COPD model. The content of TNF-α and IL-6 in the BALF samples was measured by commercially available ELISA kits.
RESULTS: The PM2.5-induced higher LDH and ACP levels were significantly alleviated in mouse lung tissues by treatment with betulinic acid derivative. Treatment with betulinic acid derivative also suppressed PM2.5-induced increase in AKP and ALB levels in mouse lung tissues. Betulinic acid derivative reversed PM2.5-mediated suppression of SOD activity and elevation of NOS level in mouse BALF. Moreover, the PM2.5-induced excessive NO and MDA levels in mouse BALF were significantly reduced (P<0.05) by treatment with betulinic acid derivative. Treatment with betulinic acid derivative improved TNF-α and IL-6 levels in BALF induced by PM2.5 exposure. Betulinic acid derivative inhibited PM2.5-induced acute inflammatory exudate, alveolar septae damage, and inflammatory cell infiltration in lungs of mice.
CONCLUSIONS: In the mouse model of PM2.5-induced COPD, betulinic acid derivative reduced the degree of lung inflammation and downregulated inflammatory mediators. These findings support the need for further in vivo studies and clinical evaluation of betulinic acid derivative in patients with COPD.
Keywords: Anti-Inflammatory Agents, Diterpenes, Particulate Matter, Pulmonary Disease, Chronic Obstructive, Bronchoalveolar Lavage Fluid, Interleukin-6, Pentacyclic Triterpenes
Background
Pulmonary diseases in Chinese people are mainly induced by inhaling air contaminated with particulate matter (PM), which alters lung histology. High PM levels, especially PM2.5 due to human intervention, has led to a rapidly increased mortality rates in patients with respiratory diseases [1]. PM2.5 is particulate matter in the air having particle diameter larger than 2.5 μm. The PM2.5 is harmful mainly because of its ability to adsorb pollutants, heavy toxic elements, viruses, and bacteria from the atmosphere [2,3]. PM2.5 is characterized by its potential to remain in the air for long times and to enter pulmonary tissues after inhalation, which adversely affects human health [2,3]. Mechanistic investigations have shown that elevated levels of reactive oxygen species (ROS) and mediators of inflammation induced by PM2.5 are responsible for pulmonary tissue injury and damage [4–6]. Examination of lung tissues revealed marked damage in patients after inhalation of PM2.5 [7,8].
The COPD is characterized by lung airway blocking due to inflammation and subsequent degradation of pulmonary tissues [9,10]. Generally, COPD is detected in chain cigarette smokers and people frequently exposed to PM2.5 [2–4, 11]. Compounds having anti-inflammatory potential are effective in treatment of respiratory diseases such as COPD [12–15]. Currently available compounds used for COPD treatment have adverse effects such as diarrhea, decrease in body weight, vomiting, and headaches [16–18]. Thus, discovery of drug candidates for treatment of respiratory diseases induced by PM2.5 is immediately required.
Secondary metabolites isolated from diverse plant species are useful for inhibition of many respiratory diseases, including COPD, bronchitis, chronic pneumonia, and asthma [19–21]. Amenable functionalities and several biological activities associated with triterpenes have attracted attention of clinicians globally [22]. Other properties of triterpenes have demonstrated effective anti-inflammatory [23], anti-allergic, and HIV-inhibitory effects [4]. Therefore, this study aimed to evaluate the effects of a betulinic acid derivative on lung inflammation in a mouse model of COPD induced by particulate matter 2.5.
Material and Methods
SYNTHESIS OF DRUG COMPOUND:
The triterpenoid compound betulinic acid was subjected to oxidation using CrO3/H2SO4/acetone to obtain compound 2 (Figure 1). Compound 2 on condensation with H2NNH2 in the presence of KOH delivered the desired hydrazone 3. Reaction of compound 3 with floro-α,β-unsaturated ketone in the presence of a base produced compound 4, which was subsequently reacted with palladium acetate/potassium carbonate using chlorobenzene and molecular sieves to obtain the desired product 5.
ANIMALS:
Fifty adult male mice (8 weeks old; 20–25 body weight) were provided by the Soochow University Animal Center (Suzhou, China). All mice were acclimatized under sterile conditions at 23±1°C and 60% humidity and exposed to 12-h light and dark cycles. Approval for the study was obtained from the Committee for Animal Care, the First People’s Hospital of Yunnan Province, Kunming, 650032, China. The experimental procedures were conducted in accordance with the guidelines issued by the Chinese National Institute of Health.
THE PM2.5 COLLECTION:
Airborne PM2.5 was collected during a 2-week period from an urban region using a Thermo Anderson sampler (Brand; Thermo Fisher Scientific, Inc., Waltham, MA, USA). Partitioning of the membrane filter into 2×2 cm parts was followed by ultrasonic oscillation (at 110 kHz) of the pieces repeated 5 times in ultrapure water at room temperature. After filtration with steel gauze, the filtrate was subjected to centrifugation at 15 000×g for 30 min. The precipitate obtained was kept in physiological saline, subjected to sterilization in an autoclave, and then stored at 4°C.
INDUCTION OF COPD IN MICE:
Mice in the model and treatment groups were given suspension of PM2.5 (25 μl) by intranasal route daily for 7 days. The sham group was administered equal volumes of physiological saline alone. The mice administered PM2.5 suspension were separated into 4 groups of 10 mice each: the model group and 3 betulinic acid treatment groups (at 2-, 5-, and 8-mg/kg doses). Mice were given betulinic acid at 2-, 5-, and 8-mg/kg doses daily for 15 days through intra-gastric route in physiological saline. Mice were monitored for sensitivity, body hair pattern, and respiratory murmur in all 5 groups for 30 days. On day 31, mice were sacrificed using choral hydrate anesthesia to collect bronchoalveolar lavage fluid (BALF) and remove the lungs.
BALF ANALYSIS:
Mice were injected with 1X PBS (1 ml) into the lungs, which was then withdrawn for determination of various cytokines and oxidative markers by standard methodology [13]. The BALF samples were centrifuged at 4°C for 30 min at room temperature. Supernatant was analyzed for SOD activity and presence of malondialdehyde (MDA), lactate dehydrogenase (LDH), alkaline phosphatase (AKP), albumin (ALB), and inducible nitric oxide synthetase (iNOS) levels using ELISA kits. The levels of TNF-α and IL-6 in the BALF samples were measured using commercially available ELISA kits.
HISTOPATHOLOGICAL ANALYSIS OF LUNGS:
Histopathological alterations were examined in upper regions of the left pulmonary lobes using HE staining. Treatment of pulmonary tissues was performed with 10% buffered formalin for 24 h at 25°C to get fixed tissues. Then, dehydration was carried out with gradient ethanol followed by embedding in paraffin and subsequent slicing into thin 3-μm sections. Thin sections were dyed at room temperature after HE staining for 25 min for light microscopy examination of cell infiltration and acute inflammatory exudate.
STATISTICAL ANALYSIS:
The data are presented as the mean±SD of experiments carried out independently in triplicate. Data were analyzed using one-way analysis of variance (ANOVA) followed by least significant difference post hoc testing. SPSS software (SPSS, Inc., Chicago, IL, USA) was used for statistical analysis of the data. Differences were defined as statistically significant at
Results
CHEMISTRY:
Cyclized betulinic acid derivative 5 was synthesized for in vivo evaluation against PM2.5induced COPD in the mouse model taking into consideration diverse biological properties and bioavailability of triterpenoids in living systems. Cyclized betulinic acid derivative 5 was obtained from betulinic acid 1 using a sequence of reactions consisting of oxidation and condensation, followed by acid catalyzed reaction with α,β-unsaturated ketone and, finally, palladium acetate/potassium carbonate-mediated cyclization (Figure 1).
BETULINIC ACID INHIBITS INFLAMMATION IN MICE WITH PM-INDUCED COPD:
Exposure to PM2.5 significantly increased LDH and ACP levels in the mouse lung tissues compared to the sham group (Figure 2). The AKP and ALB levels were also much higher in PM2.5-exposed mice compared to the sham group. The PM2.5-induced LDH and ACP levels were significantly alleviated in mouse lung tissues after treatment with 2-, 5-, and 8-mg/kg doses of betulinic acid. Treatment with 2-, 5-, and 8-mg/kg doses of betulinic acid also suppressed the PM2.5-induced increase in AKP and ALB levels in mouse lung tissues.
BETULINIC ACID INHIBITS PM2.5-INDUCED OXIDATIVE STRESS FACTORS IN MICE:
The activity of SOD in PM2.5-exposed mice was suppressed and that of NOS was promoted compared to sham mice (Figure 3). Betulinic acid reversed the PM2.5-mediated suppression of SOD activity and elevation of NOS level in mouse BALF at 2-, 5-, and 8-mg/kg doses. The NO and MDA levels in BALF of PM2.5-exposed mice were significantly (P<0.05) elevated compared to the sham group. The PM2.5-induced excessive NO and MDA levels in mouse BALF were significantly (P<0.05) reduced by treatment with 2-, 5-, and 8-mg/kg doses of betulinic acid.
BETULINIC ACID ALLEVIATES PM2.5-INDUCED EXCESSIVE CYTOKINE RELEASE IN MICE:
Continued exposure to PM2.5 leads to decreased levels of anti-oxidants in lung tissues, especially in chain smokers [24,25]. The effect of betulinic acid on TNF-α and IL-6 levels in PM2.5-exposed mice were measured at 2-, 5-, and 8-mg/kg doses by ELISA (Figure 4). The BALF of PM2.5-exposed mice showed higher TNF-α and IL-6 levels compared to the sham group. However, betulinic acid treatment of PM2.5-exposed mice at 2-, 5-, and 8-mg/kg doses alleviated TNF-α and IL-6 levels in BALF. The decrease in PM2.5-induced TNF-α and IL-6 levels in mouse BALF was significant at 2 and 5 mg/kg and the effect was the strongest at the 8-mg/kg concentration.
BETULINIC ACID INHIBITS TISSUE DAMAGE AND INFLAMMATION INDUCED BY PM2.5 IN MICE:
The preventive effect of betulinic acid on lung damage induced by PM2.5 in mice was determined by standard methodology [23,24]. Acute inflammatory exudate, increased inflammatory cell infiltration, and damaged alveolar septae were observed in mice exposed to PM2.5 (Figure 5). In the sham mouse group, acute inflammatory exudate, increased inflammatory cell infiltration, and damaged alveolar septae were not observed. Betulinic acid treatment inhibited PM2.5-induced acute inflammatory exudate, alveolar septae damage, and inflammatory cell infiltration in mouse lungs at 2-, 5-, and 8-mg/kg doses. The preventive effect of betulinic acid on PM2.5-induced acute inflammatory exudate, alveolar septae damage, and inflammatory cell infiltration in mouse lungs was strongest at 8-mg/kg doses.
Discussion
Reactive oxygen species are excessively produced in animal lungs by exposure to particulate matter, which is the major factor leading to bronchial alveolar wall thickening [26]. Many respiratory diseases in humans are associated with particulate matter exposure, especially to PM2.5. Pulmonary chronic inflammation induced by PM2.5 is the main cause of several diseases, including pulmonary hypertension and COPD [27]. In developing countries, sharp increases in the incidence of respiratory diseases, including asthma, pneumonia, and COPD, are being caused by increased PM2.5 content in the atmosphere.
Respiratory diseases induced by PM2.5 are a serious health issue globally; therefore, studies to develop treatments, particularly using traditional Chinese medicine, are increasingly being performed [28–30]. Lung inflammation in smokers is inhibited through reduction of chemokine expression by treatment with tuberostemonine [31]. Inflammation of lung airways in house dust mite-mediated asthma patients is inhibited by resveratrol treatment [14]. Improvement in pulmonary function has been reported in a PM2.5-induced mouse model of lung damage by treatment with GubenZhike via inflammatory cell infiltration suppression [32]. The present study showed that PM2.5 promoted aggregation of inflammatory cells, enhanced acute inflammatory exudate, and damaged lung tissues in mice. PM2.5 exposure activates innate immune cells as well as epithelial cells, which subsequently promotes excessive inflammatory cytokine production and elevate antibacterial protein levels [33,34]. The present study found elevated levels of LDH and ACP in the mouse lung tissues exposed to PM2.5. Moreover, AKP and ALB levels in lung tissues of mice were also higher following PM2.5 exposure relative to the sham group. Level of oxidants like MDA, iNOS, TNF-α, and IL-6 also showed significant increases in mouse lung tissues after exposure to PM2.5. Additionally, SOD activity was downregulated in PM2.5-exposed mouse BALF compared to sham mice. However, betulinic acid treatment of PM2.5-exposed mice caused a significant suppression in levels of inflammatory cytokines and inhibited ROS generation in the BALF. Betulinic acid treatment effectively reversed PM2.5-mediated suppression of SOD activity in mouse BALF. In the present study, acute inflammatory exudate, increased inflammatory cell infiltration, and damaged alveolar septae were observed in mice exposed to PM2.5. However, betulinic acid treatment inhibited PM2.5-induced acute inflammatory exudate, alveolar septae damage, and inflammatory cell infiltration in mouse lungs at 2-, 5-, and 8-mg/kg doses.
Conclusions
Betulinic acid inhibits PM2.5-mediated inflammation and damage of lungs through downregulation of inflammatory molecules and increase in anti-oxidative factors. Moreover, betulinic acid treatment inhibited PM2.5-induced acute inflammatory exudate, alveolar septae damage, and inflammatory cell infiltration in mouse lungs. The findings from this study in a mouse model of particulate matter 2.5-induced COPD and lung inflammation support the need for further in vivo studies and clinical evaluation of the effects of betulinic acid derivative in patients with COPD.
Figures
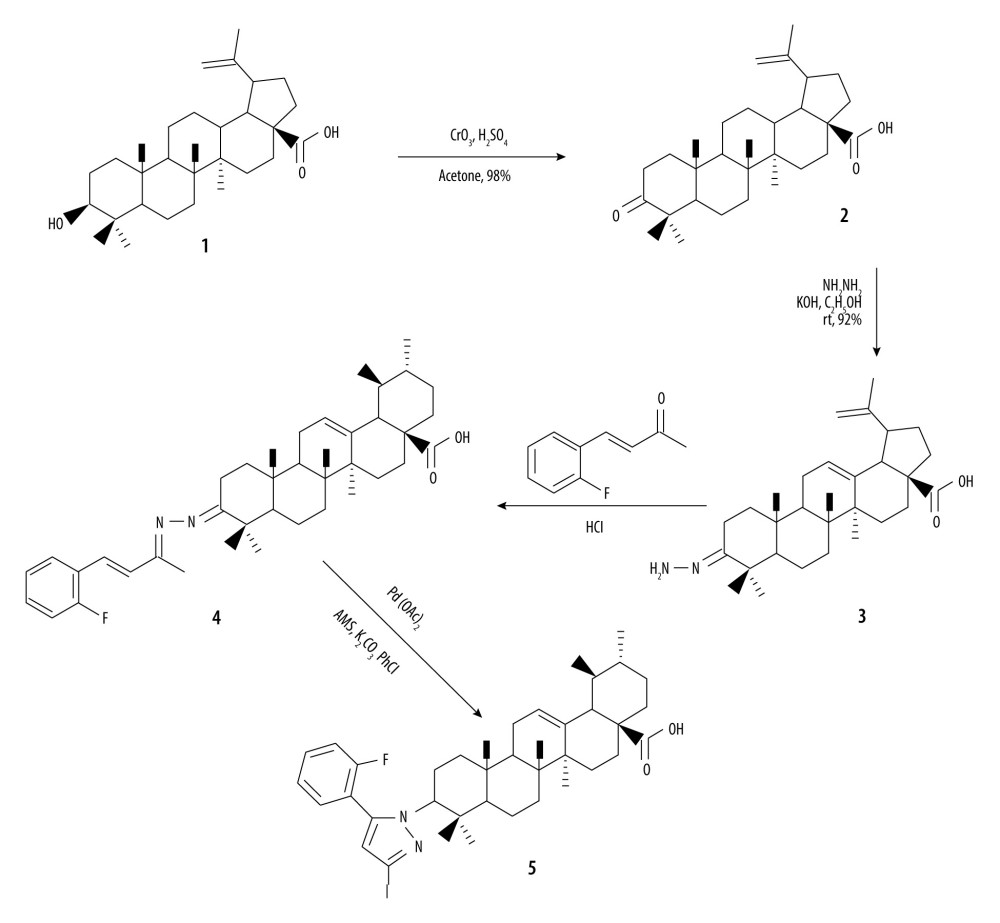 Figure 1. Synthesis of betulinic acid derivative.
Figure 1. Synthesis of betulinic acid derivative. 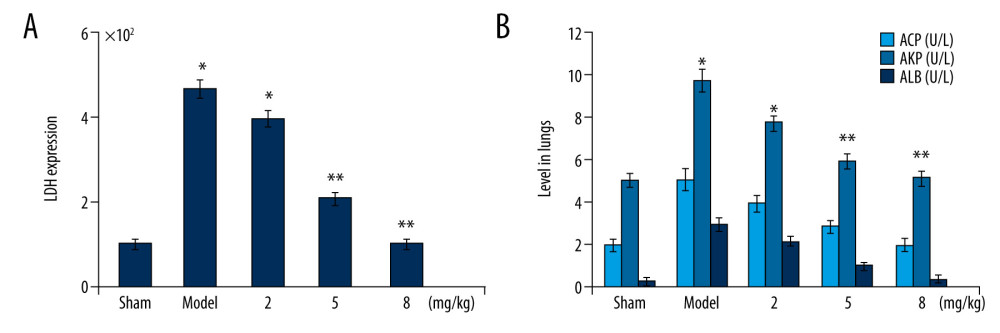 Figure 2. (A, B) Betulinic acid suppresses PM2.5-mediated inflammatory molecules. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The excised lung tissues were assessed using ELISA kits for LDH, AKP, ALB, and ACP levels after completion of treatment. * P<0.05 and ** P<0.02 vs sham group.
Figure 2. (A, B) Betulinic acid suppresses PM2.5-mediated inflammatory molecules. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The excised lung tissues were assessed using ELISA kits for LDH, AKP, ALB, and ACP levels after completion of treatment. * P<0.05 and ** P<0.02 vs sham group. 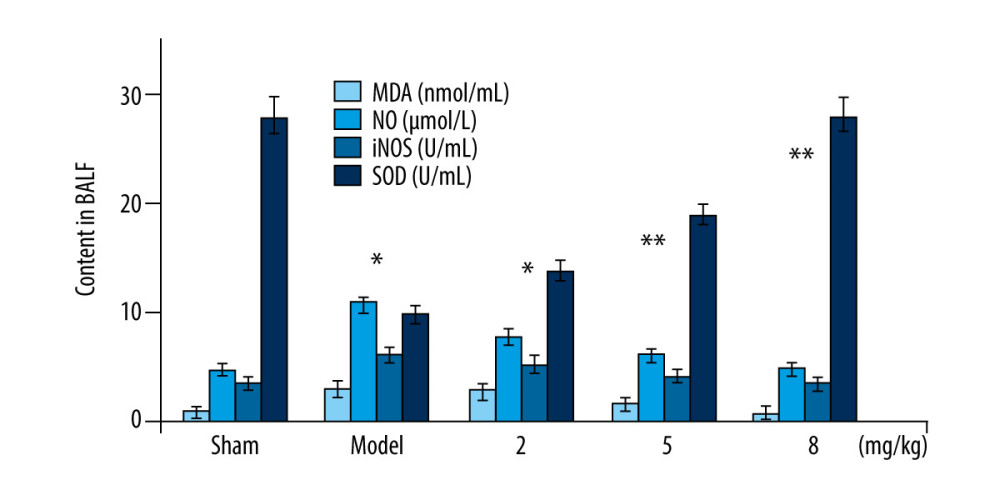 Figure 3. Betulinic acid suppresses PM2.5-mediated promotion of oxidative markers. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were assessed for MDA, NO, NOS, and SOD levels by ELISA. * P<0.05 and ** P<0.02 vs sham group.
Figure 3. Betulinic acid suppresses PM2.5-mediated promotion of oxidative markers. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were assessed for MDA, NO, NOS, and SOD levels by ELISA. * P<0.05 and ** P<0.02 vs sham group. 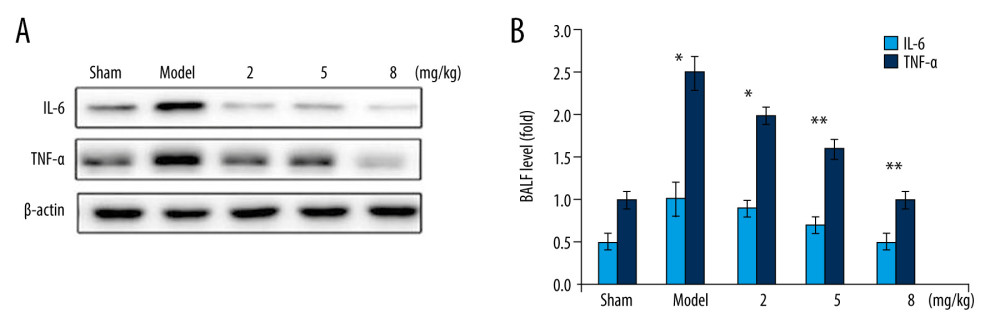 Figure 4. Betulinic acid inhibits PM2.5-mediated production of TNF-α and IL-6 levels in BALF of mice. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were analyzed by (A) western blotting and (B) ELISA assays for TNF-α and IL-6 content. * P<0.05 and ** P<0.02 vs sham group.
Figure 4. Betulinic acid inhibits PM2.5-mediated production of TNF-α and IL-6 levels in BALF of mice. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were analyzed by (A) western blotting and (B) ELISA assays for TNF-α and IL-6 content. * P<0.05 and ** P<0.02 vs sham group. 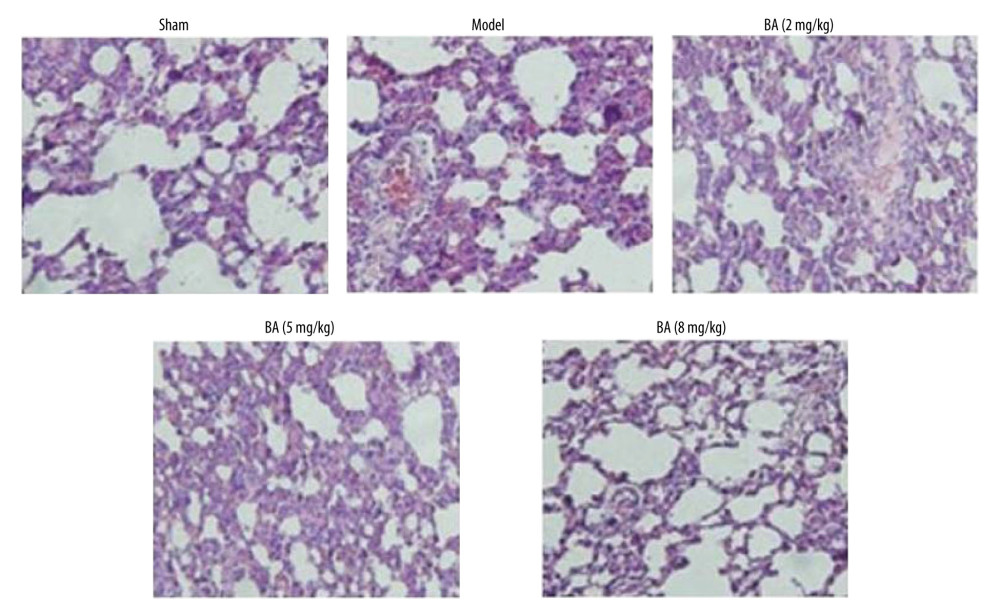 Figure 5. Betulinic acid inhibits PM2.5-induced histological alterations in mouse lungs. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid and pathological alterations were assessed by hematoxylin and eosin staining. Magnification, ×220.
Figure 5. Betulinic acid inhibits PM2.5-induced histological alterations in mouse lungs. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid and pathological alterations were assessed by hematoxylin and eosin staining. Magnification, ×220. References
1. Kaiser J, Air pollution: Evidence mounts that tiny particles can kill: Science, 2000; 289; 22-23
2. Zhao Q, He KB, Ma YLRegional PM pollution in Beijing and surrounding area during summertime: Huan Jing KeXue, 2009; 30; 1873-80 [in Chinese]
3. Pope CA, Burnett RT, Thun MJ, Lung cancer, cardiopulmonary mortality and long term exposure to fine particulate air pollution: JAMA, 2002; 287; 1132-41
4. Kodavanti UP, Jaskot RH, Su WY, Genetic variability in combustion particle induced chronic lung injury: Am J Physiol, 1997; 272; L521-32
5. Tong Y, Ni X, Zhang Y, Study of toxicological mechanism of acidified aerosols: Biol Trace Elem Res, 2002; 85; 149-56
6. Ogino K, Zhang R, Takahashi H, Allergic airway inflame-mation by nasal inoculation of particulate matter (PM2.5) in NC/Nga mice: PLoS One, 2014; 9; e92710
7. Dye JA, Lehmann JR, McGee JK, Acute pulmonary toxicity of particulate matter filter extracts in rats: Coherence with epidemiologic studies in Utah valley residents: Environ Health Perspect, 2001; 109; S395-403
8. Greenwell LL, Moreno T, Jones TP, Richards RJ, Particle induced oxidative damage is ameliorated by pulmonary antioxidants: Free RadicBiol Med, 2002; 32; 898-905
9. Cazzola M, Donner CF, Hanania NA, One hundred years of chronic obstructive pulmonary disease (COPD): Respir Med, 2007; 101; 1049-65
10. Li C, Chen J, Yuan W, Preventive effect of ursolic acid derivative on particulate matter 2.5-induced chronic obstructive pulmonary disease involves suppression of lung inflammation: IUBMB Life, 2020; 72(4); 632-40
11. Kammerl IE, Dann A, Mossina A, Impairment of immunoproteasome function by cigarette smoke and in chronic obstructive pulmonary disease: Am J Respir Crit Care Med, 2016; 193; 1230-41
12. Stefan MS, Rothberg MB, Shieh MS, Association between antibiotic treatment and outcomes in patients hospitalized with acute exacerbation of COPD treated with systemic steroids: Chest, 2013; 143; 82-90
13. Chen J, Zhou H, Wang J, Therapeutic effects of resveratrol in a mouse model of HDM induced allergic asthma: Int Immuno Pharmacol, 2015; 25; 43-48
14. Xiao XQ, Lai J, Luo YLStudy on reversal of effect of double coptis on the resistance of: J Gannan Med Univ, 2016; 36; 190-92 [in Chinese]
15. Zhang FClinical observation on treating ventilator associated pneumonia with the Qingjin Huatan decoction: Clin J Chin Med, 2016; 8; 71-72 [in Chinese]
16. Wright J, Paauw DS, Complications of antibiotic therapy: Med Clin North Am, 2013; 97; 667-79
17. Blumenthal KG, Shenoy ES, Hurwitz S, Effect of a drug allergy educational program and antibiotic prescribing guideline on inpatient clinical providers’ antibiotic prescribing knowledge: J Allergy Clin Immunol Pract, 2014; 2; 407-13
18. Rolain JM, Abat C, Jimeno MT, Do we need new antibiotics?: Clin Microbiol Infect, 2016; 22; 408-15
19. Gao JF, Zhang XY, Experimental observation on germicidal efficacy of a herbal compound disinfectant solution: Chin J Disinfection, 2005; 22; 305-6
20. Chung HS, Hon PM, Lin G, Antitussive activity of Stemona alkaloids from Stemona tuberose: Planta Med, 2003; 69; 914-20
21. Liao JF, Shi CC, Chen SY: J Ethnopharmacol, 1997; 57; 57-62
22. Jäger S, Trojan H, Kopp T, Pentacyclictriterpene distribution in various plantsdrich sources for a new group of multi-potent plant extracts: Molecules, 2009; 14; 2016-31
23. Meng YQ, Liu D, Cai LL, The synthesis of ursolic acid derivatives with cytotoxic activity and investigation of their preliminary mechanism of action: Bioorg Med Chem, 2009; 17; 848-54
24. Ma CM, Cai SQ, Cui JR, The cytotoxic activity of ursolic acid derivatives: Eur J Med Chem, 2005; 40; 582-89
25. Li J, Guo WJ, Yang QY, Effects of ursolic acid and oleanolic acid on human colon carcinoma cell line HCT15, World J: Gastroenterol, 2002; 8; 493-95
26. Driscoll KE, TNFα and MIP 2: Role in particle induced inflammation and regulation by oxidative stress: Toxicol Lett, 2000; 112-13; 177-83
27. Rahman I, Bismas SK, Kode A, Oxidant and antioxidant balance in the airways and airway disease: Eur J Pharmacol, 2006; 533; 222-39
28. Cui S, He ZZ, Zhu ZW, Microfluidic analysis of PM2.5 induced epithelial mesenchymal transition in human bronchial epithelial 16HBE cells: Microfluid Nanofluidics, 2015; 19; 263-72
29. Jing Y, Zhang H, Cai Z, Bufeihuoxue capsule attenuates PM2.5 induced pulmonary inflammation in mice: Evid Based Complement Alternat Med, 2017; 2017 1575793
30. Wang H, Song L, Ju W, The acute airway inflammation induced by PM2.5 exposure and the treatment of essential oils in Balb/c mice: Sci Rep, 2017; 7; 44256
31. Jung KH, Beak H, Park S, The therapeutic effects of tuberostemonine against cigarette smoke induced acute lung inflammation in mice: Eur J Pharmacol, 2016; 774; 80-86
32. Qin YY, Jing Y, Liu YInfluence of GubenZhike Granules on lung function and morphology of lung injury mouse model induced by PM: China J Trad Chin Med Pharm, 2016; 31; 1028-31 [in Chinese]
33. Su WY, Jaskot RH, Richards J, Induction of pulmonary matrilysin expression by combustion and ambient air particles: Am J Physiol Lung Cell Mol Physiol, 2000; 279; L152-60
34. Veranth JM, Kaser EG, Veranth MM, Cytokine responses of human lung cells (BEAS 2B) treated with micron sized and nanoparticles of metal oxides compared to soil dusts: Part Fibre Toxicol, 2007; 4; 2
Figures
 Figure 1. Synthesis of betulinic acid derivative.
Figure 1. Synthesis of betulinic acid derivative. Figure 2. (A, B) Betulinic acid suppresses PM2.5-mediated inflammatory molecules. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The excised lung tissues were assessed using ELISA kits for LDH, AKP, ALB, and ACP levels after completion of treatment. * P<0.05 and ** P<0.02 vs sham group.
Figure 2. (A, B) Betulinic acid suppresses PM2.5-mediated inflammatory molecules. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The excised lung tissues were assessed using ELISA kits for LDH, AKP, ALB, and ACP levels after completion of treatment. * P<0.05 and ** P<0.02 vs sham group. Figure 3. Betulinic acid suppresses PM2.5-mediated promotion of oxidative markers. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were assessed for MDA, NO, NOS, and SOD levels by ELISA. * P<0.05 and ** P<0.02 vs sham group.
Figure 3. Betulinic acid suppresses PM2.5-mediated promotion of oxidative markers. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were assessed for MDA, NO, NOS, and SOD levels by ELISA. * P<0.05 and ** P<0.02 vs sham group. Figure 4. Betulinic acid inhibits PM2.5-mediated production of TNF-α and IL-6 levels in BALF of mice. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were analyzed by (A) western blotting and (B) ELISA assays for TNF-α and IL-6 content. * P<0.05 and ** P<0.02 vs sham group.
Figure 4. Betulinic acid inhibits PM2.5-mediated production of TNF-α and IL-6 levels in BALF of mice. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid. The BALF samples were analyzed by (A) western blotting and (B) ELISA assays for TNF-α and IL-6 content. * P<0.05 and ** P<0.02 vs sham group. Figure 5. Betulinic acid inhibits PM2.5-induced histological alterations in mouse lungs. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid and pathological alterations were assessed by hematoxylin and eosin staining. Magnification, ×220.
Figure 5. Betulinic acid inhibits PM2.5-induced histological alterations in mouse lungs. The PM2.5-exposed mice were treated with 2-, 5-, and 8-mg/kg doses of betulinic acid and pathological alterations were assessed by hematoxylin and eosin staining. Magnification, ×220. In Press
12 Mar 2024 : Database Analysis
Risk Factors of Age-Related Macular Degeneration in a Population-Based Study: Results from SHIP-TREND-1 (St...Med Sci Monit In Press; DOI: 10.12659/MSM.943140
12 Mar 2024 : Clinical Research
Preoperative Blood Transfusion Requirements for Hemorrhoidal Severe Anemia: A Retrospective Study of 128 Pa...Med Sci Monit In Press; DOI: 10.12659/MSM.943126
12 Mar 2024 : Clinical Research
Tissue Inhibitors of Metalloproteinase 1 (TIMP-1) and 3 (TIMP-3) as New Markers of Acute Kidney Injury Afte...Med Sci Monit In Press; DOI: 10.12659/MSM.943500
12 Mar 2024 : Review article
Optimizing Behçet Uveitis Management: A Review of Personalized Immunosuppressive StrategiesMed Sci Monit In Press; DOI: 10.12659/MSM.943240
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








