25 February 2021: Database Analysis
Combining Blood-Based Biomarkers to Predict Mortality of Sepsis at Arrival at the Emergency Department
Yinjing Xie1CE, Binbin Li2BC, Ying Lin1BD, Fei Shi2AG*, Weibu Chen1AF, Wenyuan Wu1F, Wenjia Zhang1B, Yun Fei1D, Shiqing Zou1D, Can Yao2CDOI: 10.12659/MSM.929527
Med Sci Monit 2021; 27:e929527
Abstract
BACKGROUND: Our aim was to determine a useful combination of blood biomarkers that can predict 28-day mortality of sepsis upon arrival at the Emergency Department (ED).
MATERIAL AND METHODS: Based on Sepsis-3.0, 90 sepsis patients were enrolled and divided into survivor and nonsurvivor groups with day 28 as the study end point. After comparing the demographic data and clinical characteristics of patients, we evaluated the predictive validity of a combination of markers including interleukin-6 (IL-6), procalcitonin (PCT), and lactate at arrival at the ED. Independent risk factors were found by using univariate and multivariate logistic regression analyses, and the prognostic value of markers was determined by the area under the curve (AUC) of the receiver operating characteristic (ROC) curve.
RESULTS: There were 67 (74.4%) survivors and 23 (25.6%) nonsurvivors. The levels of IL-6 (survivors vs nonsurvivors: median 205.30 vs 3499.00 pg/mL, P=0.012) and lactate (survivors vs. nonsurvivors: median 2.37 vs 5.77 mmol/L, P=0.003) were significantly lower in survivor group compared with the nonsurvivor group. Markers including IL-6, PCT, lactate, and neutrophil-to-white blood cell ratio (NWR) were independent risk factors in predicting 28-day mortality due to sepsis. The combination of these 4 markers provided the best predictive performance for 28-day mortality of patients with sepsis, on arrival at the ED (AUC of 0.823, 95% confidence interval [CI] 0.723–0.924), and its accuracy, specificity, and sensitivity were 74.4% (95% CI 64.0–82.8%), 91% (95% CI 80.9–96.3%), and 65% (95% CI 42.8–82.8%), respectively.
CONCLUSIONS: The combination of IL-6, PCT, lactate, and NWR measurements is a potential predictor of 28-day mortality for patients with sepsis, at arrival at the ED. Further research is needed to confirm our findings.
Keywords: C-Reactive Protein, Interleukin-6, Lactic Acid, Mortality, Sepsis, Area Under Curve, Emergency Service, Hospital, Logistic Models, procalcitonin, ROC Curve, Risk Factors, Sensitivity and Specificity
Background
Sepsis is a large clinical and public health burden throughout the world. Its social and economic consequence have been largely underestimated [1]. Locations that are the least equipped to prevent, identify, or treat sepsis have the highest burden [2]. Early detection and timely treatment of sepsis are crucially important for both the patients and society in general.
Research has shown that a quick Sequential (sepsis-related) Organ Failure Assessment (qSOFA) score ≥2 was an independent factor for 30-day mortality due to sepsis [3]. However, other studies have indicated that qSOFA has a low sensitivity for predicting outcomes [4]. Sepsis arises from complex reactions to systemic inflammation, which involves elevated levels of a variety of blood-based biomarkers including immune cells and cytokines, such as white blood cells (WBCs) and interleukin-6 (IL-6), and acute response proteins, such as procalcitonin (PCT) and high-sensitivity C-reactive protein (hs-CRP) [5]. We aimed to identify an effective combination of markers that can help predict 28-day mortality of sepsis as early as patients’ arrival at the Emergency Department (ED).
Increasing numbers of investigators have begun searching for reliable biomarkers or combinations of biomarkers to predict sepsis-related mortality [6]. Although several studies have evaluated the predictive value of the qSOFA score and some biomarkers such as hs-CRP and PCT or their combinations, most focused on the points in time when patients enter or are already in the Intensive Care Unit (ICU) [7,8]. In this study, we gathered indicators within the first 2 h of patients’ arrival at the ED to identify a useful combination of biomarkers to predict 28-day mortality of sepsis at the time of arrival at the ED. We selected several markers that are widely used in clinical practice and have results that are quick and easy to obtain.
Material and Methods
PATIENTS:
We conducted this retrospective study on patients with suspected sepsis admitted to the ED at Shenzhen People’s Hospital, the second clinical medical college of Jinan University, or the first affiliated hospital of Southern University of Science and Technology from December 2017 to April 2019, with the approval of the Ethics Committee of Shenzhen People’s Hospital and the Second Clinical Medical College of Jinan University (No. LL-KT-201705001) and informed consent waived.
STUDY POPULATION:
We collected data on adult patients who were aged above 18 years and were examined by a physician for assessment and diagnosis of sepsis based on Sepsis-3.0 criteria when they presented to the ED. As shown in Figure 1, patients were excluded from the study if they were pregnant, were younger than 18 years old, had experienced traumatic injury, had cancer, required immediate surgical intervention, had been resuscitated from cardiopulmonary arrest, had a do-not-resuscitate status, or had undergone major surgery in the previous 30 days or antibacterial therapy in the 5 days prior to ED arrival. We gathered the qSOFA scores of patients at their arrival at the ED by using altered mental status, systolic blood pressure ≤100, and respiratory rate ≥22 [9].
DATA COLLECTION:
The following information was required: baseline information (age, sex, weight, and height), comorbidities, intervention of mechanical ventilator, use of vasopressors, length of hospital and ICU stays in days, mortality in 28 days, and clinical indicators such as mean arterial blood pressure. Furthermore, blood indicators including PCT, hs-CRP, IL-6, and lactate levels; WBC count; and neutrophil-to-WBC ratio (NWR) were collected from patients with suspected sepsis at arrival at the ED. All samples were assessed in the Laboratory Department of Shenzhen People’s Hospital, following manufacturers’ instructions. PCT, hs-CRP, IL-6, and lactate were measured from plasma, and WBC count was measured from whole blood.
STATISTICAL EVALUATION:
Data were evaluated using Statistical Package for Social Sciences (SPSS) software, version 19.0 (SPSS Inc., Chicago, IL). Normally distributed continuous variables are reported as means (standard deviation [SD]), while nonnormally distributed variables are reported as medians (interquartile range [IQR]). We used the chi-squared test to compare categorical variables, and we used independent 2-sample testing to compare continuous variables. Univariate and multivariate logistic regression analyses were used for determining independent effects for 28-day mortality, and the model selection strategy was to add all the variables whose likelihood ratio test P-value <0.05 (forward, likelihood ratio, entry criteria: 0.10, exclusion criteria: 0.15). We used receiver operating characteristic (ROC) curves to assess the association of biomarkers with 28-day mortality [10]. P<0.05 was considered significant. We used Matthews correlation coefficient (MCC) to evaluate the predictive model, with MCC worst value=– and best value=+1 [11].
Results
BASELINE CHARACTERISTICS AND OUTCOMES:
After screening for eligibility, a total of 90 patients with sepsis were enrolled and divided into the survivor group (n=67, 44 men and 23 women) and the nonsurvivor group (n=23, 14 men and 9 women) according to 28-day mortality. The total 28-day mortality was 25.6% in this study. As shown in Table 1, there was no statistical difference between the 2 groups based on age, sex, mean arterial blood pressure, pathogen, etiology, and duration of hospital stay. The baseline characteristics of patients revealed that nonsurvivors had a higher burden of hypertension and hemiplegic stroke. The SOFA scores of nonsurvivors were significantly higher than those of survivors.
COMPARISON OF BLOOD-BASED BIOMARKERS AND QSOFA SCORE BETWEEN SURVIVOR AND NONSURVIVOR GROUPS:
Compared with the nonsurvivor group, the survivor groups had significantly lower levels of IL-6 (survivors vs nonsurvivors: median 205.30 vs 3499.00 pg/mL, P=0.012) and lactate (survivors vs nonsurvivors: median 2.37 vs 5.77 mmol/L, P=0.003). As shown in Table 2, there were no statistical differences in levels of hs-CRP, PCT, WBC count, NWR, and the qSOFA score (P=0.235, 0.681, 0.459, 0.103, 0.856, respectively) between the 2 groups.
LOGISTIC REGRESSION ANALYSIS OF BIOMARKERS FOR 28-DAY MORTALITY:
The levels of NWR (odds ratio [OR]=0.009; 95% confidence interval [CI]: 0.000–1.052; P=0.052), IL-6 (OR=1.000; 95% CI: 1.000–1.001; P=0.009), PCT (OR=0.981; 95% CI: 0.965–0.097; P=0.019), and lactate (OR=1.309; 95% CI: 1.038–1.651; P=0.023) had significant predictive ability for 28-day mortality of sepsis, indicating that NWR, IL-6, PCT, and lactate are independent risk factors (Table 3). Other variables, including hs-CRP, WBC count, and the qSOFA score, were not potential predictors of 28-day mortality in this study.
ROC CURVE ANALYSIS OF BIOMARKERS FOR PREDICTING 28-DAY MORTALITY:
Results of ROC curve analysis are shown in Table 4 and Figure 2. With regard to the ability of these biomarkers to predict the 28-day mortality of sepsis, the cutoff value was 2580.50 pg/mL for IL-6, with 56.5% sensitivity and 86.6% specificity (AUC 0.675, 95% CI 0.534–0.816, P=0.013), and 5.385 mmol/L for lactate, with 52.5% sensitivity and 94.0% specificity (AUC 0.710, 95% CI 0.568–0.852, P=0.003). The remaining biomarkers, including hs-CRP, PCT, WBC count, NWR, and the qSOFA score, had no significant value in predictive performance. Combinations were then evaluated to improve predictive performance, and the combination of IL-6, PCT, lactate, and NWR (AUC 0.823, 95% CI 0.723–0.924, P<0.001) was found to have a higher value in predicting 28-day mortality of sepsis at the very early phase, with accuracy, specificity, and sensitivity of 74.4% (95% CI 64.0–82.8%), 91% (95% CI 80.9–96.3%), and 65% (95% CI 42.8–82.8%), respectively. The MCC was +0.58.
Discussion
The qSOFA score and 6 laboratory variables for patients with suspected sepsis at arrival at the ED were evaluated in our study. The results preliminarily showed that a novel combination of IL-6, PCT, lactate, and NWR was a predictor for 28-day mortality of sepsis at arrival at the ED. This combination, based on 4 blood-based biomarkers, is easily gathered within the first 2 h after a patient’s arrival at the ED. Therefore, it may play a significant role in early risk assessment and timely intervention for patients with sepsis. However, our study did not show that the qSOFA score was an independent risk factor to predict 28-day mortality at arrival at the ED.
The effectiveness of IL-6 to predict sepsis mortality has been addressed in several previous research [12,13]. As a pleiotropic cytokine, IL-6 is expressed by different kinds of cells in response to infections and tissue injuries at a very early phase (usually within 2 h), and it is one of the crucial parts in the systemic infection reaction to sepsis [14,15]. Elevated IL-6 levels in serum have been detected in sepsis and are related to a high risk of mortality [16]. For adults without any inflammation, the IL-6 concentration in blood ranges from 0.2 to 7.8 pg/mL; however, for patients with sepsis, it may rise to 1600 pg/mL or even higher [17]. In this study, IL-6 levels were significantly higher in nonsurvivors than in survivors. Furthermore, IL-6 was shown to be an independent factor to predict 28-day mortality for patients with sepsis. These results are in line with a previous study [18]. With the cutoff value for IL-6 set at 2580.50 pg/mL, it has a sensitivity of 56.5% and a moderate specificity of 86.6% (AUC=0.675) for predicting 28-day mortality of sepsis. Although the AUC of IL-6 was not high, the results indicated that IL-6 is a potential predictive biomarker for 28-mortality of sepsis patients. Combining it with another biomarker may improve the predictive power.
In addition to IL-6, lactate was another biomarker that increased significantly in nonsurvivors compared with survivors in this study. Lactate is a notable biomarker in defining septic shock in Sepsis-3.0. Elevated lactate levels have been shown to be an independent risk factor and a useful index for 28-day mortality of sepsis in a previous study [19]. Even when tested within the first 2 h after patients’ arrival at the ED, the levels of lactate in nonsurvivors were significantly higher than in survivors. Moreover, lactate was one of the independent risk factors in our study. Setting the cutoff value at 5.385 mmol/L yielded a sensitivity of 52.2% and a high specificity of 94.0% (AUC=0.710) for predicting 28-day mortality of sepsis. These results were supported by prior findings of an association between lactate and mortality related to sepsis [20].
PCT is a polypeptide precursor of the calcitonin hormone whose main role is to control of the concentrations of calcium in blood. Under normal conditions, PCT is produced by the thyroid C-cells and is present at an extremely low level in the blood (<0.05 ng/mL). However, during infectious and inflammatory stimuli, especially sepsis, many kinds of cells are triggered by cytokines and chemokines to synthesize and release PCT [21]. Several studies have determined the predictive ability of PCT in sepsis and found that PCT kinetics over the first 72 h were associated with in-hospital and ICU mortality of patients with sepsis [22,23]. Our findings show that PCT is an independent risk factor of 28-day mortality of sepsis, which is supported by previous research [24,25].
High-sensitivity CRP is an acute-phase protein and is widely known as a marker in response to inflammation. During acute-phase inflammation, hs-CRP levels increase significantly, and they are used to aid the diagnosis of sepsis [26]. Previous studies showed that hs-CRP begins to rise within 6-8 h of infection [23]. In this study, we recorded the hs-CRP levels of patients with sepsis within in the first 2 h after their arrival at the ED. Some patients may have been in the early phase of sepsis, when the hs-CRP had not begun to rise.
WBC and neutrophil counts are traditional laboratory variables for patients with infections. These indicators are readily measured and routinely performed in hospital laboratories. The circulation of neutrophils is altered by inflammatory stimuli, such as sepsis. After infection, neutrophils move from the marginal to the circulation pool, and large amounts of immature neutrophils enter the circulation. These factors can cause an elevated neutrophil percentage [27]. Although there was no significant difference for WBC count and NWR in a comparison of survivors and nonsurvivors, NWR was found to be an independent risk factor. Several previous studies showed that the neutrophil-to-lymphocyte ratio was a predictor for mortality of sepsis [28,29]. Our findings were generally consistent with those previous reports in terms of an increased neutrophil percentage.
In the development of a new definition for sepsis, the qSOFA score has been demonstrated to be a key factor in identifying sepsis associated with a risk of death or longer ICU stay [30]. Various studies have determined that the qSOFA score is a useful predictor for mortality of ICU patients [31,32]. However, in our study, the qSOFA score was not an independent risk factor in predicting 28-day mortality of sepsis at arrival at the ED, and no difference was found in comparing the survivors with the nonsurvivors. This outcome may be due to the qSOFA scores reflecting the status of patients with the first 2 h after their arrival at the ED. Some of the patients may have been in the early phase of sepsis, at which point they had not yet developed symptoms such as altered consciousness, hypotension, and short breath. Consequently, the above factors may result in reduced sensitivity of qSOFA score in predicting 28-day mortality in our study.
There are also limitations in our research. First, we used a retrospective study design, and policy and other systemic changes could have caused coding practices to vary over time, resulting in bias. Second, because it was a single-center study, the results may not be applicable to other centers. Third, the sample size was small, which inevitably led to limited statistical power. Therefore, further study with multiple centers and a large sample size is necessary to confirm the results.
Conclusions
In conclusion, our study investigated a novel combination of lactate, PCT, IL-6, and NWR to predict 28-day mortality in patients with sepsis at arrival at the ED. This combination can be readily and quickly measured in the ED, and it may be a simple but reliable predictor of sepsis. Future research is needed to determine the prognostic potential of the combination in patients with sepsis, within 2 h of their ED arrival.
Figures
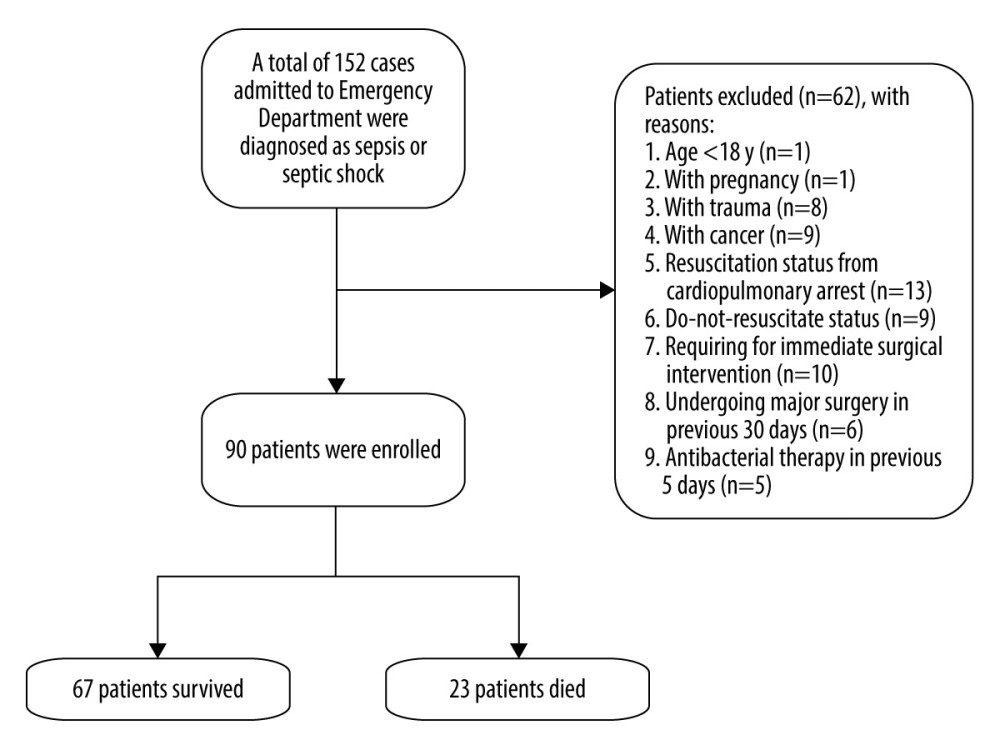 Figure 1. Participant screening and enrollment in the study.
Figure 1. Participant screening and enrollment in the study. 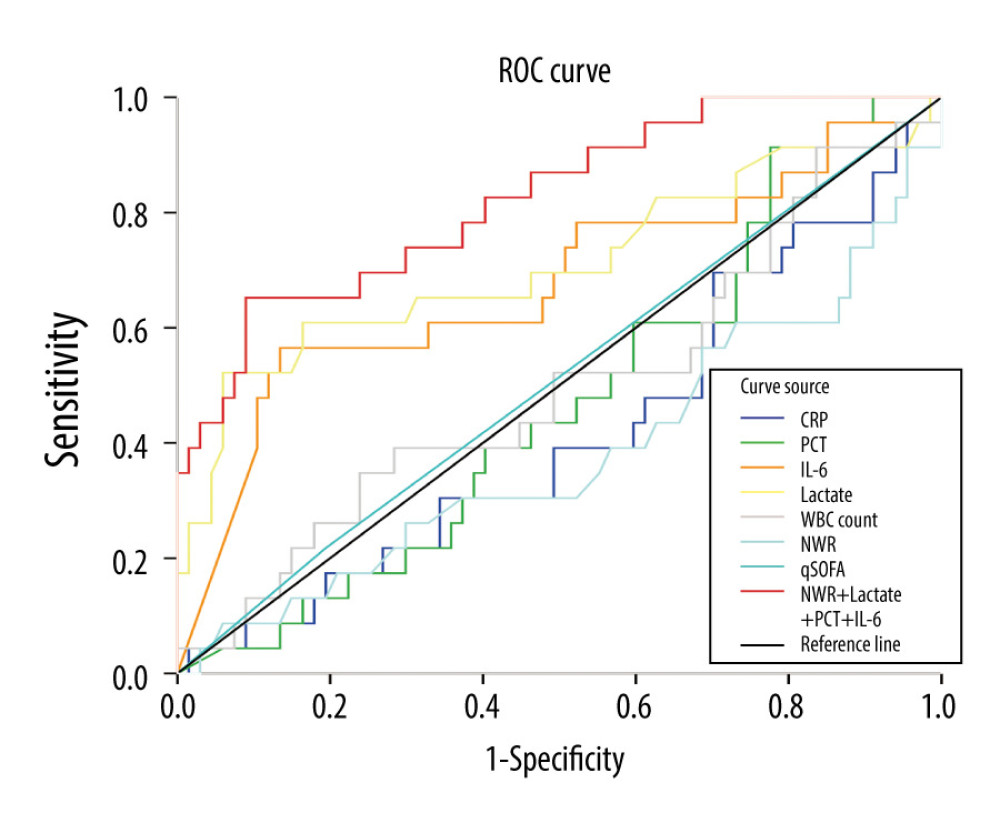 Figure 2. The receiver operating characteristic (ROC) curves of the selected markers for predicting 28-day mortality of sepsis patients on arrival at the Emergency Department. The ROC curves for single markers and their combination included the following areas: high-sensitivity C-reactive protein (hs-CRP), 0.417; procalcitonin (PCT), 0.471; interleukin-6 (IL-6), 0.675; lactate, 0.710; white blood cell (WBC) count, 0.497; neutrophil-to-WBC ratio (NWR), 0.383; quick Sequential (sepsis-related) Organ Failure Assessment score (qSOFA), 0.512; combination of NWR, IL-6, PCT, and lactate, 0.823.
Figure 2. The receiver operating characteristic (ROC) curves of the selected markers for predicting 28-day mortality of sepsis patients on arrival at the Emergency Department. The ROC curves for single markers and their combination included the following areas: high-sensitivity C-reactive protein (hs-CRP), 0.417; procalcitonin (PCT), 0.471; interleukin-6 (IL-6), 0.675; lactate, 0.710; white blood cell (WBC) count, 0.497; neutrophil-to-WBC ratio (NWR), 0.383; quick Sequential (sepsis-related) Organ Failure Assessment score (qSOFA), 0.512; combination of NWR, IL-6, PCT, and lactate, 0.823. References
1. Luhr R, Cao Y, Söderquist B, Cajander S, Trends in sepsis mortality over time in randomised sepsis trials: A systematic literature review and meta-analysis of mortality in the control arm, 2002–2016: Crit Care, 2019; 23(1); 241
2. Rudd KE, Johnson SC, Agesa KM, Global, regional, and national sepsis incidence and mortality, 1990–2017: Analysis for the Global Burden of Disease Study: Lancet, 2020; 395(2); 200-11
3. Abdullah S, Grand J, Sijapati A, qSOFA is a useful prognostic factor for 30-day mortality in infected patients fulfilling the SIRS criteria for sepsis: Am J Emerg Med, 2020; 38(3); 512-16
4. Kim KS, Suh GJ, Kim K, Quick Sepsis-related Organ Failure Assessment score is not sensitive enough to predict 28-day mortality in emergency department patients with sepsis: A retrospective review: Clin Exp Emerg Med, 2019; 6(4); 77-83
5. Liu Y, Han N, Li Q, Li Z, Regulatory mechanisms underlying sepsis progression in patients with tumor necrosis factor-α genetic variations: Exp Ther Med, 2016; 12(5); 323-28
6. Wang J, Sun Y, Teng S, Li K, Prediction of sepsis mortality using metabolite biomarkers in the blood: A meta-analysis of death-related pathways and prospective validation: BMC Med, 2020; 18(6); 83
7. Fernando SM, Tran A, Taljaard M, Prognostic accuracy of the quick Sequential Organ Failure Assessment for mortality in patients with suspected infection: A systematic review and meta-analysis: Ann Intern Med, 2018; 168(7); 266-75
8. Raith EP, Udy AA, Bailey M, Prognostic accuracy of the SOFA score, SIRS criteria, and qSOFA score for in-hospital mortality among adults with suspected infection admitted to the intensive care unit: JAMA, 2017; 317(8); 290-300
9. Angus DC, Seymour CW, Coopersmith CM, A framework for the development and interpretation of different sepsis definitions and clinical criteria: Crit Care Med, 2016; 44(9); e113-21
10. Habibzadeh F, Habibzadeh P, Yadollahie M, On determining the most appropriate test cut-off value: The case of tests with continuous results: Biochem Med (Zagreb), 2016; 26(10); 297-307
11. Chicco D, Jurman G, Survival prediction of patients with sepsis from age, sex, and septic episode number alone: Sci Rep, 2020; 10(11); 17156
12. Jekarl DW, Lee SY, Lee J, Procalcitonin as a diagnostic marker and IL-6 as a prognostic marker for sepsis: Diagn Microbiol Infect Dis, 2013; 75(12); 342-47
13. Miguel-Bayarri V, Casanoves-Laparra EB, Pallás-Beneyto L, Prognostic value of the biomarkers procalcitonin, interleukin-6 and C-reactive protein in severe sepsis: Med Intensiva, 2012; 36(13); 556-62
14. Ganesan P, Shanmugam P, Sattar SB, Shankar SL, Evaluation of IL-6, CRP and hs-CRP as early markers of neonatal sepsis: J Clin Diagn Res, 2016; 10(14); DC13-17
15. Takahashi W, Nakada TA, Yazaki M, Oda S, Interleukin-6 levels act as a diagnostic marker for infection and a prognostic marker in patients with organ dysfunction in Intensive Care Units: Shock, 2016; 46(15); 254-60
16. Georgescu AM, Grigorescu BL, Chirteş IR, The relevance of coding gene polymorphysms of cytokines and cellular receptors in sepsis: J Crit Care Med (Targu Mures), 2017; 3(16); 5-11
17. Thompson DK, Huffman KM, Kraus WE, Kraus VB, Critical appraisal of four IL-6 immunoassays: PLoS One, 2012; 7(17); e30659
18. Djordjevic D, Pejovic J, Surbatovic M, Prognostic value and daily trend of interleukin-6, neutrophil CD64 expression, C-reactive protein and lipopolysaccharide-binding protein in critically ill patients: Reliable predictors of outcome or not?: J Med Biochem, 2015; 34(18); 431-39
19. Shapiro NI, Trzeciak S, Hollander JE, A prospective, multicenter derivation of a biomarker panel to assess risk of organ dysfunction, shock, and death in Emergency Department patients with suspected sepsis: Crit Care Med, 2009; 37(19); 96-104
20. Song YH, Shin TG, Kang MJ, Predicting factors associated with clinical deterioration of sepsis patients with intermediate levels of serum lactate: Shock, 2012; 38(20); 249-54
21. Assicot M, Gendrel D, Carsin H, High serum procalcitonin concentrations in patients with sepsis and infection: Lancet, 1993; 341(21); 515-18
22. Schuetz P, Amin DN, Greenwald JL, Role of procalcitonin in managing adult patients with respiratory tract infections: Chest, 2012; 141(22); 1063-73
23. Zhang Y, Khalid S, Jiang L, Diagnostic and predictive performance of biomarkers in patients with sepsis in an intensive care unit: J Int Med Res, 2019; 47(23); 44-58
24. Andriolo BN, Andriolo RB, Salomão R, Atallah ÁN, Effectiveness and safety of procalcitonin evaluation for reducing mortality in adults with sepsis, severe sepsis or septic shock: Cochrane Database Syst Rev, 2017; 1(24); CD010959
25. Mustafić S, Brkić S, Prnjavorac B, Diagnostic and prognostic value of procalcitonin in patients with sepsis: Med Glas (Zenica), 2018; 15(25); 93-100
26. Kofoed K, Andersen O, Kronborg G, Use of plasma C-reactive protein, procalcitonin, neutrophils, macrophage migration inhibitory factor, soluble urokinase-type plasminogen activator receptor, and soluble triggering receptor expressed on myeloid cells-1 in combination to diagnose infections: A prospective study: Crit Care, 2007; 11(26); R38
27. Martins EC, Silveira LDF, Viegas K, Neutrophil-lymphocyte ratio in the early diagnosis of sepsis in an intensive care unit: A case-control study: Rev Bras Ter Intensiva, 2019; 31(27); 64-70
28. Fuss J, Voloboyeva A, Poliovyj V, Prognostic value of using neutrophil-lymphocyte ratio in patients with burn injury for the diagnosis of sepsis and bacteraemia: Pol Przegl Chir, 2018; 90(28); 13-16
29. Ni J, Wang H, Li Y, Neutrophil to lymphocyte ratio (NLR) as a prognostic marker for in-hospital mortality of patients with sepsis: A secondary analysis based on a single-center, retrospective, cohort study: Medicine (Baltimore), 2019; 98(29); e18029
30. Seymour CW, Liu VX, Iwashyna TJ, Assessment of clinical criteria for sepsis: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3): JAMA, 2016; 315(30); 762-74
31. Godinjak A, Iglica A, Rama A, Predictive value of SAPS II and APACHE II scoring systems for patient outcome in a medical intensive care unit: Acta Med Acad, 2016; 45(31); 97-103
32. Innocenti F, Tozzi C, Donnini C, SOFA score in septic patients. Incremental prognostic value over age, comorbidities, and parameters of sepsis severity: Intern Emerg Med, 2018; 13(32); 405-12
Figures
 Figure 1. Participant screening and enrollment in the study.
Figure 1. Participant screening and enrollment in the study. Figure 2. The receiver operating characteristic (ROC) curves of the selected markers for predicting 28-day mortality of sepsis patients on arrival at the Emergency Department. The ROC curves for single markers and their combination included the following areas: high-sensitivity C-reactive protein (hs-CRP), 0.417; procalcitonin (PCT), 0.471; interleukin-6 (IL-6), 0.675; lactate, 0.710; white blood cell (WBC) count, 0.497; neutrophil-to-WBC ratio (NWR), 0.383; quick Sequential (sepsis-related) Organ Failure Assessment score (qSOFA), 0.512; combination of NWR, IL-6, PCT, and lactate, 0.823.
Figure 2. The receiver operating characteristic (ROC) curves of the selected markers for predicting 28-day mortality of sepsis patients on arrival at the Emergency Department. The ROC curves for single markers and their combination included the following areas: high-sensitivity C-reactive protein (hs-CRP), 0.417; procalcitonin (PCT), 0.471; interleukin-6 (IL-6), 0.675; lactate, 0.710; white blood cell (WBC) count, 0.497; neutrophil-to-WBC ratio (NWR), 0.383; quick Sequential (sepsis-related) Organ Failure Assessment score (qSOFA), 0.512; combination of NWR, IL-6, PCT, and lactate, 0.823. Tables
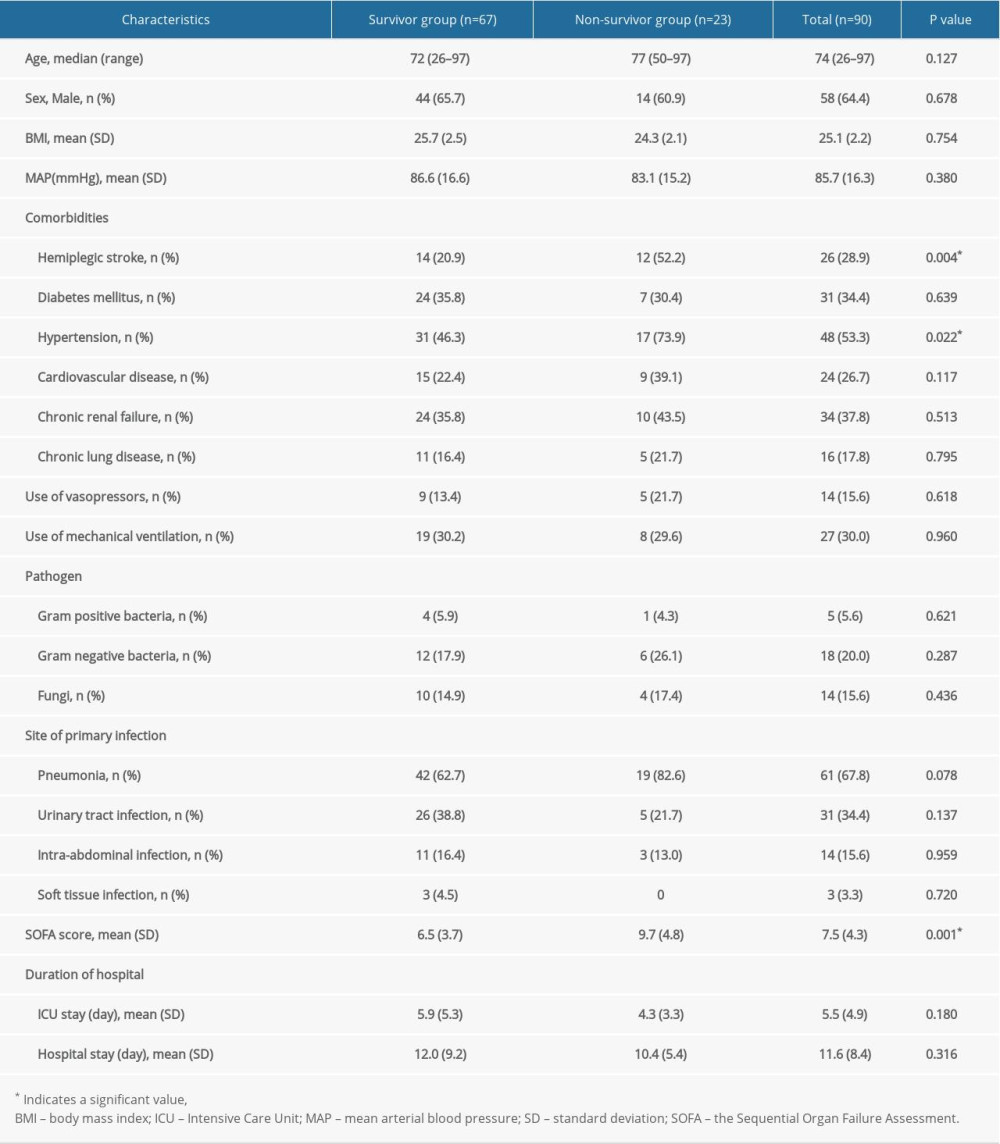 Table 1. Demographic characteristics.
Table 1. Demographic characteristics.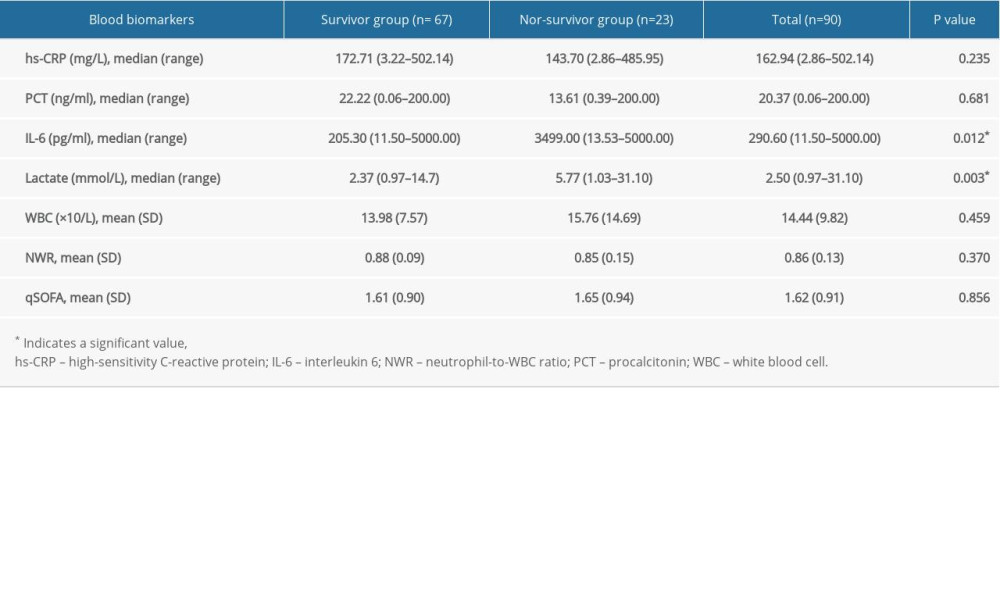 Table 2. Blood biomarkers by study group.
Table 2. Blood biomarkers by study group.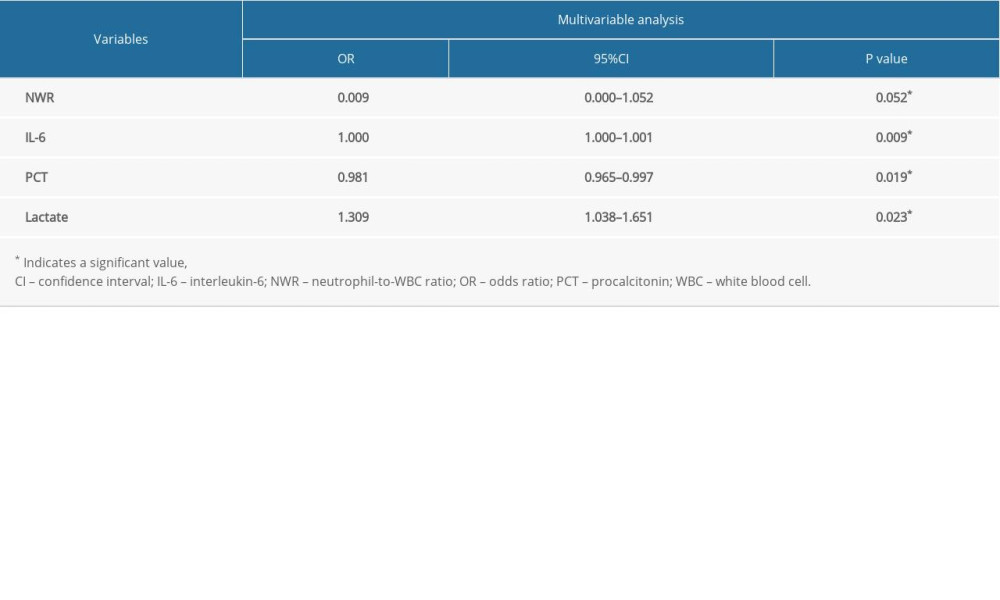 Table 3. The logistic regression analysis of blood-based biomarkers for predicting 28-day mortality in patients with sepsis or septic shock.
Table 3. The logistic regression analysis of blood-based biomarkers for predicting 28-day mortality in patients with sepsis or septic shock.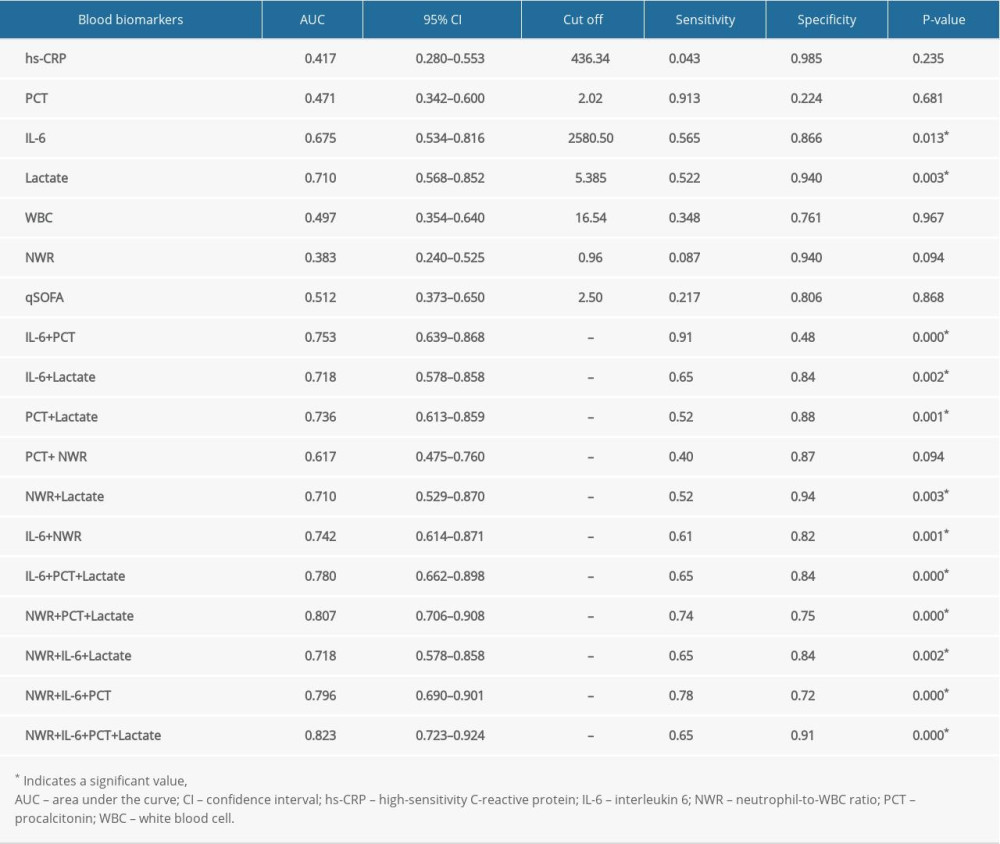 Table 4. Prognostic value of clinical parameters.
Table 4. Prognostic value of clinical parameters. Table 1. Demographic characteristics.
Table 1. Demographic characteristics. Table 2. Blood biomarkers by study group.
Table 2. Blood biomarkers by study group. Table 3. The logistic regression analysis of blood-based biomarkers for predicting 28-day mortality in patients with sepsis or septic shock.
Table 3. The logistic regression analysis of blood-based biomarkers for predicting 28-day mortality in patients with sepsis or septic shock. Table 4. Prognostic value of clinical parameters.
Table 4. Prognostic value of clinical parameters. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








