11 August 2021: Clinical Research
Using the Diaphragm as a Tracking Surrogate in CyberKnife Synchrony Treatment
Guo-quan Li1A, Jing Yang1A, Yan Wang2C, Mengjun Qiu3B, Zeyu Ding1D, Sheng Zhang1E, Sheng-li Yang1G, Zhenjun Peng4F*DOI: 10.12659/MSM.930139
Med Sci Monit 2021; 27:e930139
Abstract
BACKGROUND: In this study, we assessed the usefulness of diaphragm surrogate tracking in the design of a respiratory model for CyberKnife Synchrony treatment of lung tumors.
MATERIAL AND METHODS: Twenty-four patients with lung cancer who underwent stereotactic body radiotherapy with CyberKnife between April and November 2019 were enrolled. Simulation plans for each patient were designed using Xsight lung tracking (XLT) and diaphragm tracking (DT) methods, and tumor visualization tests were performed. The offset consistency at each respiratory phase was analyzed. The relative distance along the alignment center of the superior-inferior (SI) axis in the 2 projections (dxAB), uncertainty (%), and average standard error (AvgStdErr)/maximum standard error (MAXStdErr) were also analyzed.
RESULTS: Bland-Altman analyses revealed that the average differences±standard deviation (SD) between XLT and DT tracking methods were 0.4±2.9 mm, 0.3±4.35 mm, and -1.8±6.8 mm for the SI, left-right (LR), and anterior-posterior (AP) directions, respectively. These results indicated high consistency in the SI and LR directions and poor consistency in the AP direction. Uncertainty differed significantly between XLT and DT (22.813±5.721% vs 9.384±3.799%; t=-5.236; P=0.0008), but we found no significant differences in dxAB, AvgStdErr, or MAXStdErr.
CONCLUSIONS: In the majority of cases, motion tracking by XLT and DT was consistent and synchronized in the SI directions, but not in the LR and AP directions. With a boundary margin of 0.3±4.35 mm and 1.8±6.8 mm for the LR and AP directions, DT may contribute to better implementation of CyberKnife Synchrony treatment in patients with lung tumors near the diaphragm that cannot be seen in tumor visualization tests.
Keywords: Imaging, Three-Dimensional, Medical Oncology, Radiation Oncology, Radiosurgery, Radiotherapy, Diaphragm, Feasibility Studies, Margins of Excision, Movement, Radiotherapy Planning, Computer-Assisted, Tomography, X-Ray Computed
Background
In patients undergo radiotherapy, radiation often results in radionecrosis in various vital organs, including the lungs and liver [1–3]. Stereotactic body radiation therapy (SBRT) has been shown to improve tumor control in patients with early-stage inoperable lung and liver cancers at 2–3 years of follow-up while causing minimal toxicity [4–6]. However, respiratory motion imposes significant challenges for SBRT in the chest and abdomen.
The CyberKnife Synchrony respiratory tracking system provides real-time motion management solutions, including Xsight lung tracking (XLT) and fiducial tracking (FT), which are based on the tracking of the lung tumor and implanted fiducials, respectively. According to the manufacturer’s recommendations, the XLT method requires the tumor density to be significantly higher than that of the surrounding nonmalignant lung tissue in the X-ray image acquired by the CyberKnife image system, and the minimum diameter of the tumor to be greater than 1.5 cm in all directions [7]. For the XLT method, a tumor visualization test (TVT) should be performed before radiation, which is a limiting factor for clinical application of the XLT method. Bahig et al [8] performed TVT on 133 patients and found that the test failed in 45 (34%) patients. In these cases, the FT method seemed to be a feasible alternative.
Nevertheless, the implantation of fiducials may increase the risk of pneumothorax. Additionally, the displacement and deformation between fiducials and the target may lead to errors and subsequent treatment discontinuation. The reported risk of pneumothorax or pulmonary hemorrhage after percutaneous implantation ranged from 13% to 45% [9–12]. The displacement or abandonment of fiducials may also compromise the tracking accuracy. Studies have shown an implantation failure rate of 16%, with displacement and rotation error rates also being relatively high [13,14]. Therefore, in view of the above limitations, spine tracking has been proposed for the treatment of tumors near the spine [15]. However, the internal target volume may involve a large volume of nonmalignant tissue due to tumor motion, which could increase the risk of toxicity. Hence, the development of novel methods to overcome the limitations of XLT and FT while minimizing the exposure volume remains an unmet clinical need. Yang et al [16] found a good motion correlation between the diaphragm and liver tumor in superior-inferior (SI) and anterior-posterior (AP) directions using magnetic resonance imaging, suggesting that the diaphragm could be used as a reliable surrogate target for tracking liver tumors [17–20]. Previous studies have also shown a correlation between diaphragm motion and lung tumor motion by directly evaluating both using either 4-dimensional or fluoroscopic images [21–24].
However, to the best of our knowledge, there are no published reports on using the novel CyberKnife technique to track diaphragm motion as a surrogate marker for lung tumor radiotherapies. In this study, we investigated the feasibility of using diaphragm tracking (DT) as a surrogate in CyberKnife Synchrony treatment. We also compared the performance of DT and XLT in the development of a Synchrony respiration model.
Material and Methods
CLINICAL DATA:
The present study included patients who underwent SBRT with CyberKnife between April 2019 and November 2019 at the Cancer Center of the Union Hospital of Huazhong University of Science and Technology. A total of 24 patients (14 with lung cancer, 6 with lung metastasis of liver cancer, and 4 with lung metastasis of colon cancer) with a planning target volume 34.27 cm3 (13.04–95.25 cm3) were enrolled. The inclusion criteria were (1) a tracking volume minimum diameter of ≥1.5 cm in all directions if the XLT method was used and a clearly visible tumor on the images of A and B X-ray tubes; (2) the treatment site was the middle and lower lung and the simulated computed tomography (CT) image contained a complete and clear diaphragm; and (3) patients had a junior high school education or more and were able to complete the respiratory training and CyberKnife simulation. The patient characteristics are detailed in Table 1. The study protocol was approved by the Ethics Committee of Union Hospital of Huazhong University of Science and Technology (IEC S852). Written informed consent was obtained from each patient.
EQUIPMENT INFORMATION:
The following equipment was used in this study: American Accuray Company CyberKnife VSI (with standard treatment couch), treatment plan system MultiPlan 5.2.1, and treatment execution system CyberKnife 10.5.
RESPIRATORY TRAINING:
To ensure the accuracy and efficiency of SBRT, all patients received respiratory training before CT scanning and treatment. A custom-made breathing training platform was used to ensure regularly breathing following a voice prompt. For consistency, all patients were trained and evaluated by the same investigator.
CT SCAN AND CYBERKNIFE SIMULATION PLAN:
CT images (slice thickness: 1.5 mm, tube current: 400 mA, tube voltage: 120 kVp) were obtained on a Philips Brilliance BigBore CT simulator (Philips Healthcare, Netherlands). The scan range was 15 cm above and below the tumor area, including all the surrounding organs at risk. The CT images were transferred to the MultiPlan (version 5.2.1, Accuray Inc., Sunnyvale, CA, USA) treatment planning system. The gross tumor volume was contoured by the same experienced oncologist. During XLT treatment, the tracking volume (solid structure of the tumor lesion) was used as the reference object in the Synchrony system. According to the manufacturer’s instructions, the tracking volume was identified from end-expiration breath-hold CT images close to the inner edge of solid lung lesions; cloudy and blurred parts were excluded [25]. The tracking volumes of solid tumor lesions (for XLT) and diaphragm (for DT, the diaphragm volume from diaphragmatic dome to 1.5 cm below) were reported. The tracking volumes were contoured by the same experienced medical physicist. For all enrolled patients, CyberKnife simulation plans were designed based on XLT and DT methods.
TUMOR VISUALIZATION TEST:
For consistency, the same experienced radiation oncologist visually identified the tumor and/or diaphragm using the CyberKnife treatment system for all patients enrolled in this study. TVT was performed based on simulation plans to establish the correlation between internal tracking volume and external breathing profile. Initially, the spine X-ray images were used to generate digitally reconstructed radiographs (DRRs) with less than 1 mm of translation offset. Subsequently, the image center was moved from the spine center to the tracking volume center for breathing modeling. The first step to manually build a Synchrony model was to align each patient near the center of the respiratory cycle. Centering the range of respiratory motion reduced the likelihood of treatment interruptions caused by out-of-bound errors. Next, the remaining Synchrony dataset was acquired 1 model point at a time. The user-defined respiratory phase selection was used to acquire both the peak and valley model points (full inspiration/expiration) and either the center inhale or center exhale model point (the midpoint of the respiratory cycle). The translational offsets of the center inhale or center exhale image were reviewed in the Synchrony model (mm) table. If the values were close to zero, it was not necessary to move the couch. If the values were high for 1 or more axes, the couch was moved to center the range of respiratory motion. The translational offsets of the center inhale/exhale image were entered to the couch position (mm) textboxes. Next the model points were collected according to the breathing phase sequence, as shown in Figure 1.
CORRELATION ERROR:
The standard deviation (SD) in the Synchrony correlation model accurately indicated the total difference between the curve of the Synchrony model and each model point representing each correlation image. The SD was used to evaluate the quality of the model, and the SD was obtained using the following formula:
where
DATA EXTRACTION:
We collected both XLT and DT in the same visit, and for TVT, screenshots of each breath phase point were saved in the treatment execution system once. The phase points of each breath were recorded for 60 s until all the optimal models of 8 effective breath phase points were collected. After XLT and DT were executed, XLT and DT data of the screenshot interface were extracted. The offset value, dxAB, uncertainty, and average standard error (AvgStdErr)/maximum standard error (MAXStdErr) of each breathing phase point were obtained according to the recorded information in the treatment execution system.
Tracking with the XLT system provided the association between the observed target position and the position recorded in the DRR images; target offsets were calculated using the DRR images as a reference. The dxAB (mm) parameter was used to assess the relative distance along the alignment center SI axis in the 2 projections (for camera A and camera B of the X-ray imaging system). The SI axis was used because it was common to both projections. The XLT algorithm was used to calculate the dxAB value for every image. The uncertainty (%) parameter was used to assess the calculated detection uncertainty value for the XLT algorithm. Detection uncertainty values higher than the uncertainty threshold parameter indicated the presence of uncertainty errors.
STATISTICAL ANALYSIS:
SPSS statistical software was used for all statistical analyses. The measurement data were expressed as means±SD, and the Bland-Altman method was used to compare the translation offset in the 2 methods. The
Results
BLAND-ALTMAN CONSISTENCY ANALYSIS:
The SD between XLT and DT tracking methods were 0.4±2.9 mm, 0.3±4.35 mm, and −1.8±6.8 mm for SI, left-right (LR), and AP directions, respectively. The mean SD in the AP direction was larger than −1.8 mm, indicating a low consistency between the 2 methods in this direction (Figure 2A–2C).
ANALYSIS OF SYNCHRONICITY:
We analyzed all respiratory phase points for all patients enrolled in this study and plotted the phase point graphs of 2 patients. Although the migration synchronization of the 8 respiratory phase points required to establish the model was good in the SI direction, it was poor in the LR and AP directions (Figures 3, 4).
QUALITY OF THE MODEL:
We compared the Synchrony model quality parameters between XLT and DT, including dxAB, uncertainty, and AvgStdErr/MAXStdErr. Uncertainty differed significantly between XLT and DT (22.813±5.721% vs 9.384±3.799%; t=−5.236; P=0.0008), whereas no significant differences in dxAB (mm), AvgStdErr, or MAXStdErr were observed (P>0.05, Table 2).
Discussion
Respiratory movements involve the rhythmic contraction and expansion of the chest mediated by the contraction and relaxation of the respiratory muscles [26,27]. During radiotherapy in patients with tumors in the chest and abdomen, such as early-stage lung cancer, liver cancer, and pancreatic cancer, respiratory movements lead to irregular movements of the radiation target areas [28,29]. Because the CyberKnife can synchronously track the dynamic changes in the target area, it is a powerful tool for stereotactic radiotherapy and delivery of high-dose hypofractionated radiation. In this study, we developed a DT method to treat tumors located adjacent to the diaphragm and found a high consistency between DT and XLT in the SI direction. Previous studies have shown a good correlation between the diaphragm and liver tumors in SI and AP directions and indicated that the movement amplitude in the mediolateral direction was small and likely clinically irrelevant [16,17]. Based on the linear model, Cerviño et al [23] and Zhou et al [24] reported that the per-phase position, mean position, and excursion estimation errors were 1.12±0.99 mm, 0.97±0.88 mm, and 0.79±0.67 mm, respectively. Intrafractional per-phase tumor position estimation error, mean position error, and excursion error were within 3 mm, 95%, 96%, and 99% of the time, respectively. In our patients, the results provided by DT and XLT were not consistent or synchronized in the LR direction, corroborating the findings of Yang et al [16]. We compared the motion between the diaphragm and the tumor by breathing phase matching and found that the maximum directional mean deviation was −1.8 mm. These results were similar to those of Zhou et al [24], indicating that the use of the diaphragm as a tracking surrogate in the CyberKnife tracking module provides similar performance to that of the movement of the tumor itself in the SI direction.
We also compared the offsets of the respiratory phase points during the modeling and found that most offsets provided sinusoidal curves, consistent with previous findings [30,31]. The offset fitting curve of the diaphragm as a tracking surrogate resembled a sine wave for the SI direction, while no specific trend was observed for the other 2 directions. In 2-dimensional plane images, the diaphragm was clearly visible on the 45° oblique angle orthogonal image of the CyberKnife (Figure 5A, 5B). In this study, the tracking outline of the diaphragm was defined as the outline of the diaphragmatic parietal region. Due to the unique arc-shaped structure of the diaphragm in 2-dimensional images and the position change in the LR and AP directions, the ability of the CyberKnife tracking system to recognize respiratory deformations in the diaphragm may be limited. Furthermore, as shown in (Figure 5C, 5D), the tumor often rotates during respiratory movements [32]; such rotational motions (eg, spiral and rolling motions) cannot be simulated in the DT method.
In this study, we also evaluated the reliability of the system in identifying the diaphragm by comparing tracking parameters in the DT and XLT methods. To ensure the consistency of the model evaluation conditions, we provided breathing training for all patients at the beginning of the study. All patients requiring respiratory management received breathing training at our institution to ensure that they could breathe smoothly and evenly during the treatment, thereby reducing respiratory errors and baseline deviation [31]. Studies have shown that the uncertainty (%) of respiratory models designed using the DT method is significantly lower than that of models designed using the XLT method, while dxABs do not differ significantly between the 2 models. One possible explanation for higher uncertainty (%) in the results provided by the XLT method is that the tumor profiles in one of the images were masked by surrounding impenetrable structures because of smaller tumor diameters or gray-scale profile similarities. The tracking algorithm used in the DT method improved tumor identification owing to the large scope of the diaphragm outline and the large difference in the gray scale of the diaphragm in 2-dimensional images. Although the DT-based model exhibited a slightly higher SD and maximum SD than the XLT-based model, the differences were not statistically significant, indicating that the tumor position predicted by the model was not significantly different from that of the actual diaphragm.
There are several limitations to this study. First, we did not specifically analyze the distance relationship between the XLT and the diaphragm; hence, we were unable to determine the impact of the distance between the diaphragm and the tumor on the respiratory movement. Second, due to the small cohort size, our findings need to be confirmed in future large-cohort studies.
Conclusions
In summary, we performed tumor tracking using the XLT and DT methods. We found that the motion tracking was consistent and synchronized in the SI direction, but not in LR and AP direction. With a boundary margin of 0.3±4.35 mm and 1.8±6.8 mm for the LR and AP directions, DT may contribute to better implementation of CyberKnife Synchrony treatment in patients with lung tumors near the diaphragm that are not visible in TVT. However, more caution is needed for tumors with large motions in the AP direction.
Figures
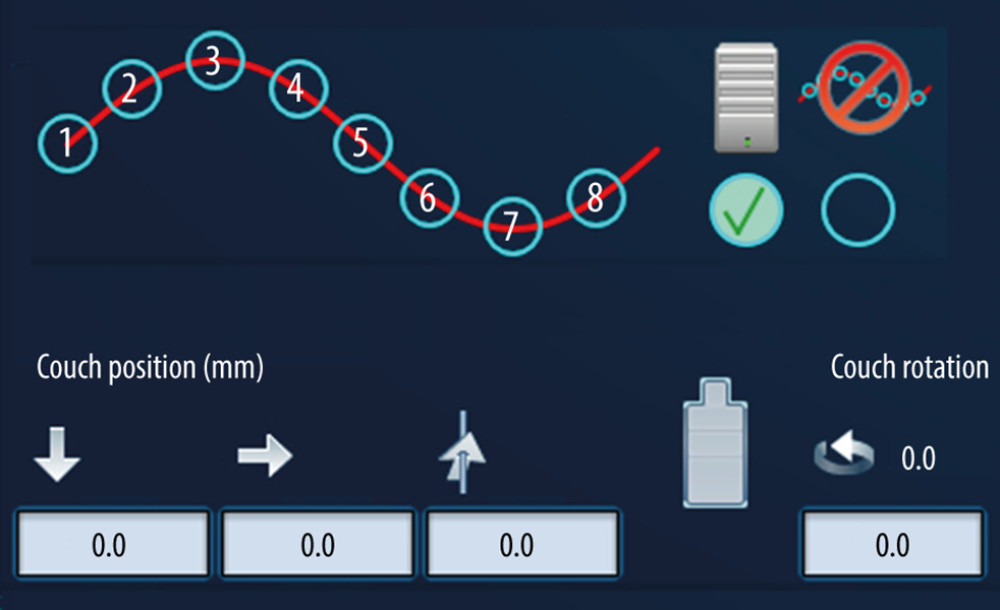 Figure 1. Sampling sequence during respiration
Figure 1. Sampling sequence during respiration 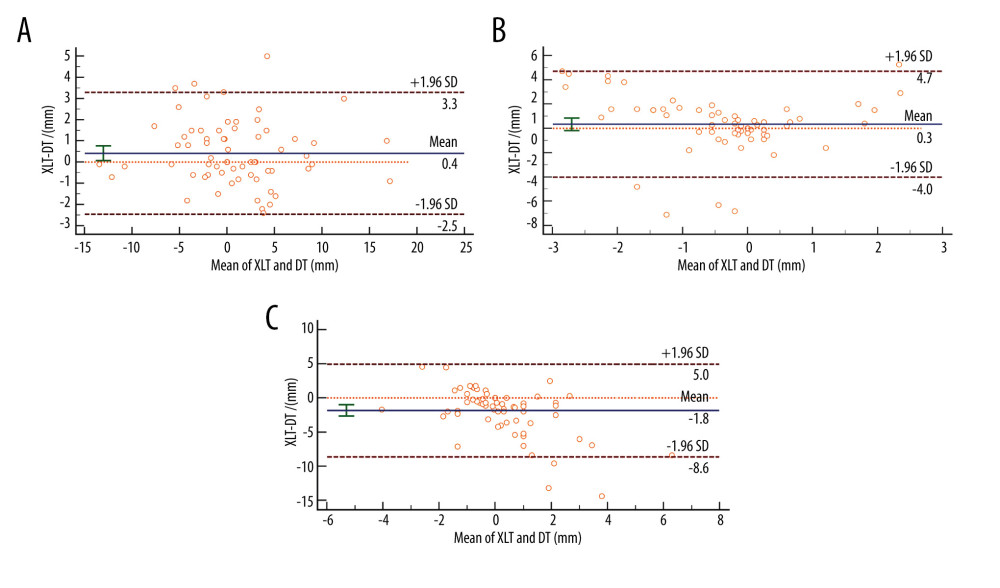 Figure 2. Bland-Altman analysis the offset values between the Xsight lung tracking (XLT) and diaphragm tracking (DT) methods. Consistency analysis of XLT and DT in the (A) superior-inferior, (B) left-right, and (C) anterior-posterior directions.
Figure 2. Bland-Altman analysis the offset values between the Xsight lung tracking (XLT) and diaphragm tracking (DT) methods. Consistency analysis of XLT and DT in the (A) superior-inferior, (B) left-right, and (C) anterior-posterior directions. 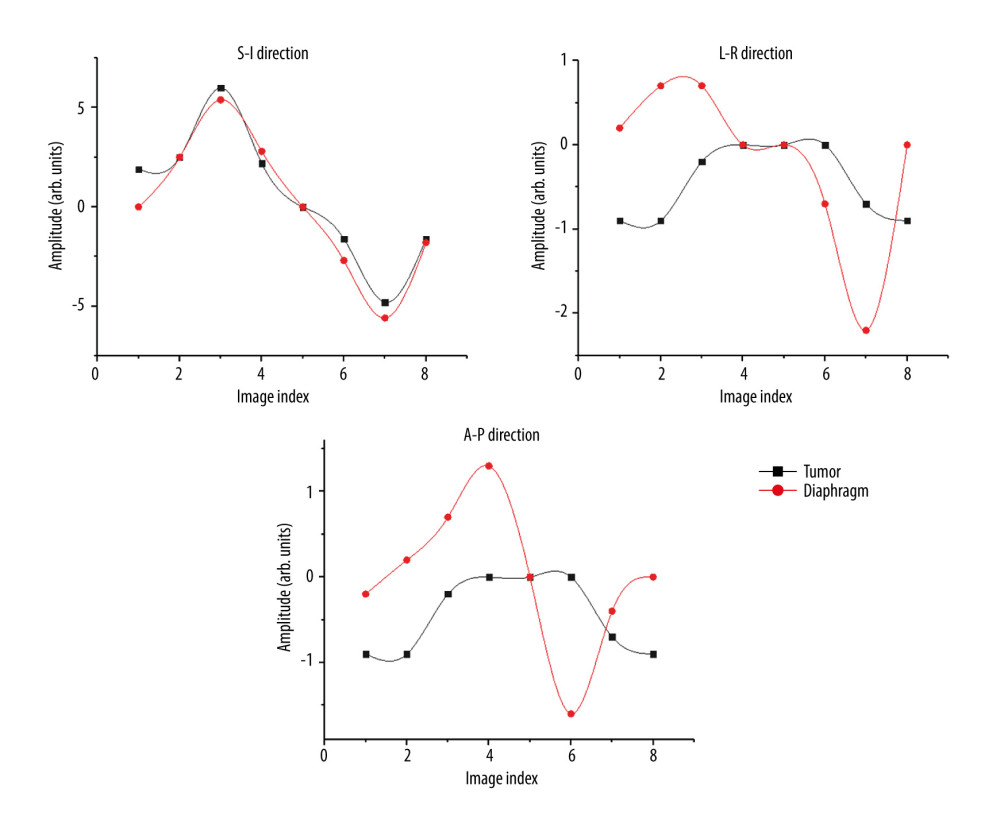 Figure 3. Synchronicity of the 3 translational offsets in patient 1: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior.
Figure 3. Synchronicity of the 3 translational offsets in patient 1: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior. 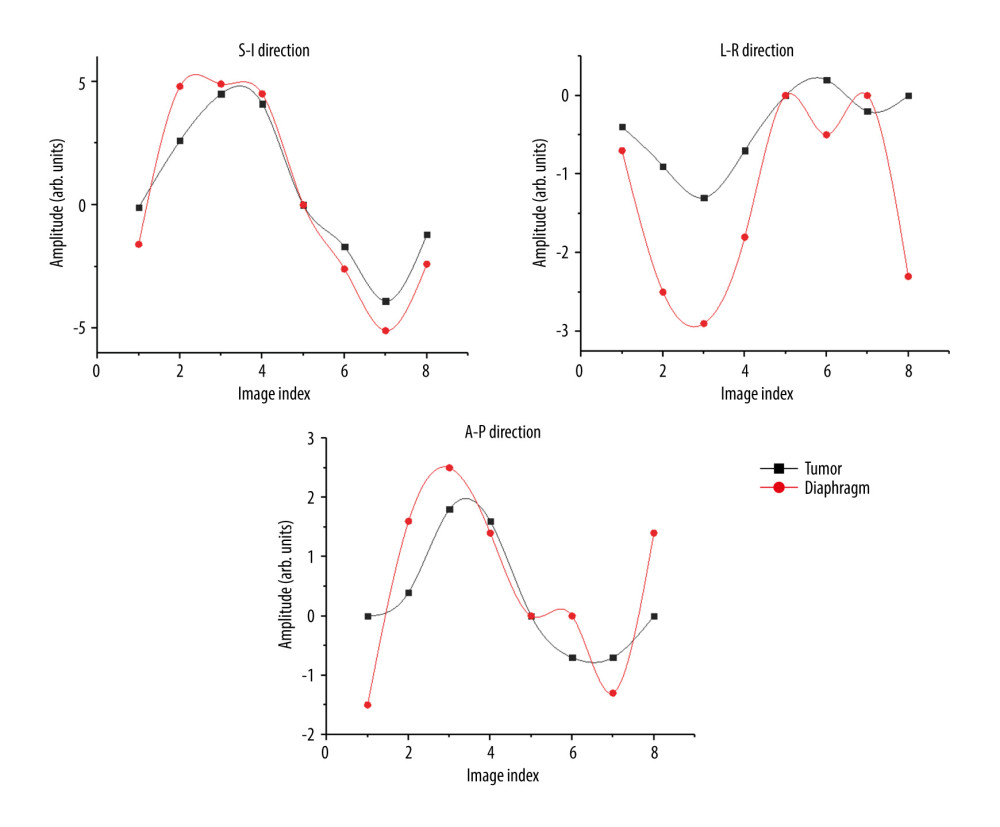 Figure 4. Synchronicity of the 3 translational offsets in patient 2: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior.
Figure 4. Synchronicity of the 3 translational offsets in patient 2: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior. 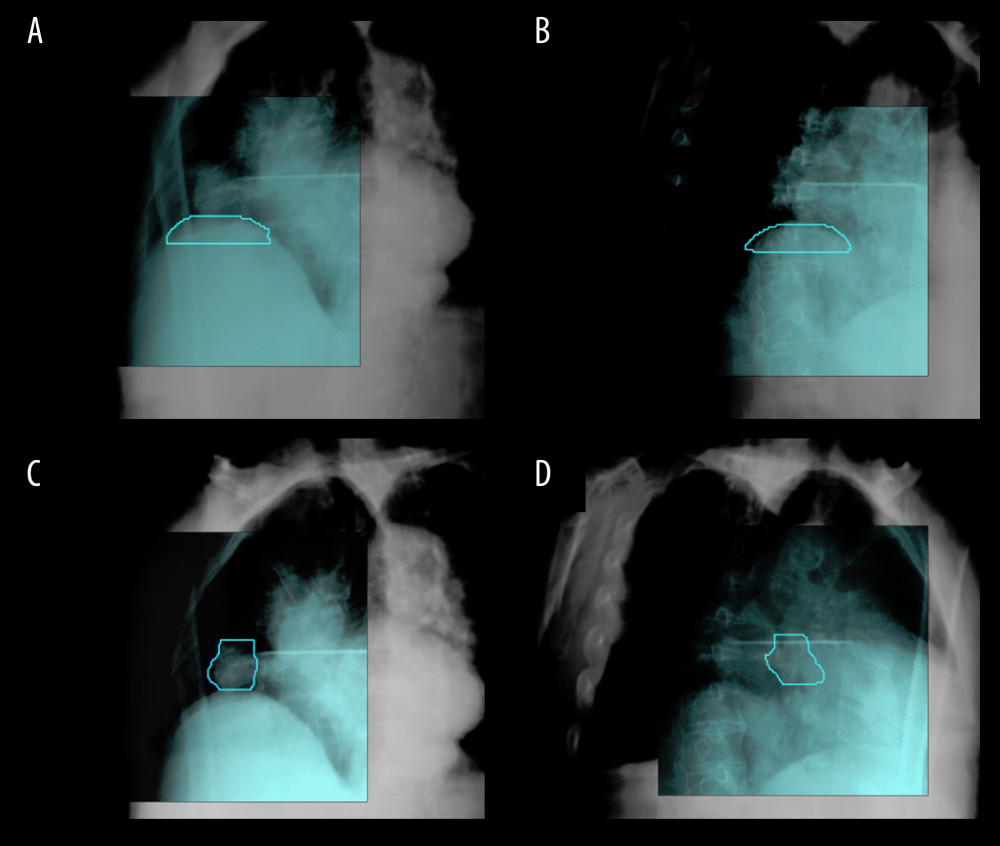 Figure 5. Tracking-guided images using (A, B) diaphragm tracking (DT) and (C, D) Xsight lung tracking (XLT).
Figure 5. Tracking-guided images using (A, B) diaphragm tracking (DT) and (C, D) Xsight lung tracking (XLT). References
1. Pan CC, Kavanagh BD, Dawson LA, Radiation-associated liver injury: Int J Radiat Oncol Biol Phys, 2010; 76(3 Suppl); S94-100
2. Okubo M, Itonaga T, Saito T, Predicting risk factors for radiation pneumonitis after stereotactic body radiation therapy for primary or metastatic lung tumours: Br J Radiol, 2017; 90(1073); 20160508
3. Giridhar P, Mallick S, Rath GK, Julka PK, Radiation induced lung injury: Prediction, assessment and management: Asian Pac J Cancer Prev, 2015; 16(7); 2613-17
4. Videtic GMM, Donington J, Giuliani M, Stereotactic body radiation therapy for early-stage non-small cell lung cancer: Executive summary of an ASTRO evidence-based guideline: Pract Radiat Oncol, 2017; 7(5); 295-301
5. Goodman KA, Kavanagh BD, Stereotactic body radiotherapy for liver metastases: Semin Radiat Oncol, 2017; 27(3); 240-46
6. Temming S, Kocher M, Stoelben E, Risk-adapted robotic stereotactic body radiation therapy for inoperable early-stage non-small-cell lung cancer: Strahlenther Onkol, 2017; 194(2); 91-97
7. Nakayama M, Nishimura H, Mayahara H, Clinical log data analysis for assessing the accuracy of the CyberKnife fiducial-free lung tumor tracking system: Pract Radiat Oncol, 2018; 8(2); e63-70
8. Bahig H, Campeau MP, Vu T, Predictive parameters of CyberKnife fiducial-less (XSight Lung) applicability for treatment of early non-small cell lung cancer: A single-center experience: Int J Radiat Oncol Biol Phys, 2013; 87(3); 583-89
9. Trumm CG, Häußler SM, Muacevic A, CT Fluoroscopy-guided percutaneous fiducial marker placement for CyberKnife stereotactic radiosurgery: Technical results and complications in 222 consecutive procedures: J Vasc Interv Radiol, 2014; 25(5); 760-68
10. van der Voort van Zyp NC, Prevost JB, Hoogeman MS, Stereotactic radiotherapy with real-time tumor tracking for non-small cell lung cancer: Clinical outcome: Radiother Oncol, 2009; 91(3); 296-300
11. Pennathur A, Luketich JD, Heron DE, Stereotactic radiosurgery for the treatment of stage I non-small cell lung cancer in high-risk patients: J Thorac Cardiovasc Surg, 2009; 137(3); 597-604
12. Bhagat N, Fidelman N, Durack JC, Complications associated with the percutaneous insertion of fiducial markers in the thorax: Cardiovasc Intervent Radiol, 2010; 33(6); 1186-91
13. Holmes OE, Gratton J, Szanto J, Reducing errors in prostate tracking with an improved fiducial implantation protocol for CyberKnife based stereotactic body radiotherapy (SBRT): J Radiosurg SBRT, 2018; 5(3); 217-27
14. Scher N, Bollet M, Bouilhol G, Safety and efficacy of fiducial marker implantation for robotic stereotactic body radiation therapy with fiducial tracking: Radiat Oncol, 2019; 14(1); 167
15. Khadige M, Salleron J, Marchesi V: J Thorac Dis, 2018; 10(8); 4976-84
16. Yang J, Cai J, Wang H, Is diaphragm motion a good surrogate for liver tumor motion?: Int J Radiat Oncol Biol Phys, 2014; 90(4); 952-58
17. Chan MK, Lee V, Chiang CL, Lipiodol versus diaphragm in 4D-CBCT-guided stereotactic radiotherapy of hepatocellular carcinomas: Strahlenther Onkol, 2016; 192(2); 92-101
18. Kirilova A, Lockwood G, Choi P, Three-dimensional motion of liver tumors using cine-magnetic resonance imaging: Int J Radiat Oncol Biol Phys, 2008; 71(4); 1189-95
19. Huijskens SC, van Dijk I, Visser J, Predictive value of pediatric respiratory-induced diaphragm motion quantified using pre-treatment 4DCT and CBCTs: Radiat Oncol, 2018; 13(1); 198
20. Li G, Wei J, Huang H, Automatic assessment of average diaphragm motion trajectory from 4DCT images through machine learning: Biomed Phys Eng Express, 2015; 1(4); 045015
21. Lin T, Cerviño LI, Tang X, Fluoroscopic tumor tracking for image-guided lung cancer radiotherapy: Phys Med Biol, 2009; 54; 981
22. Liu HH, Balter P, Tutt T, Assessing respiration-induced tumor motion and internal target volume using four-dimensional computed tomography for radiotherapy of lung cancer: Int J Radiat Oncol, 2007; 68; 531-40
23. Cerviño LI, Chao AKY, Sandhu A, Jiang SB, The diaphragm as an anatomic surrogate for lung tumor motion: Phys Med Biol, 2009; 54; 3529
24. Zhou D, Quan H, Yan D, A feasibility study of intrafractional tumor motion estimation based on 4D-CBCT using diaphragm as surrogate: J Appl Clin Med Phys, 2018; 19(5); 525-31
25. Li GQ, Wang Y, Qiu MJ, Optimized CyberKnife lung treatment: Effect of fractionated tracking volume change on tracking results: Dis Markers, 2020; 2020; 9298263
26. Chen D, Xie H, Zhang S, Gu L, Lung respiration motion modeling: A sparse motion field presentation method using biplane x-ray images: Phys Med Biol, 2017; 62(19); 7855-73
27. Fuerst B, Mansi T, Carnis F, Patient-specific biomechanical model for the prediction of lung motion from 4-D CT images: IEEE Trans Med Imaging, 2015; 34(2); 599-607
28. Yoganathan SA, Maria Das KJ, Agarwal A, Kumar S, Magnitude, impact, and management of respiration-induced target motion in radiotherapy treatment: A comprehensive review: J Med Phys, 2017; 42(3); 101-15
29. Bhasin DK, Rana SS, Jahagirdar S, Nagi B, Does the pancreas move with respiration?: J Gastroenterol Hepatol, 2006; 21(9); 1424-27
30. Hertanto A, Zhang Q, Hu YC, Dzyubak O, Reduction of irregular breathing artifacts in respiration-correlated CT images using a respiratory motion model: Med Phys, 2012; 39(6); 3070-79
31. Liang Z, Liu H, Xue J, Evaluation of the intra- and interfractional tumor motion and variability by fiducial-based real-time tracking in liver stereotactic body radiation therapy: J Appl Clin Med Phys, 2018; 19(3); 94-100
32. Huang CY, Tehrani JN, Ng JA, Six degrees-of-freedom prostate and lung tumor motion measurements using kilovoltage intrafraction monitoring: Int J Radiat Oncol Biol Phys, 2015; 91(2); 368-75
Figures
 Figure 1. Sampling sequence during respiration
Figure 1. Sampling sequence during respiration Figure 2. Bland-Altman analysis the offset values between the Xsight lung tracking (XLT) and diaphragm tracking (DT) methods. Consistency analysis of XLT and DT in the (A) superior-inferior, (B) left-right, and (C) anterior-posterior directions.
Figure 2. Bland-Altman analysis the offset values between the Xsight lung tracking (XLT) and diaphragm tracking (DT) methods. Consistency analysis of XLT and DT in the (A) superior-inferior, (B) left-right, and (C) anterior-posterior directions. Figure 3. Synchronicity of the 3 translational offsets in patient 1: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior.
Figure 3. Synchronicity of the 3 translational offsets in patient 1: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior. Figure 4. Synchronicity of the 3 translational offsets in patient 2: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior.
Figure 4. Synchronicity of the 3 translational offsets in patient 2: S-I – superior-inferior; L-R – left-right; and A-P – anterior-posterior. Figure 5. Tracking-guided images using (A, B) diaphragm tracking (DT) and (C, D) Xsight lung tracking (XLT).
Figure 5. Tracking-guided images using (A, B) diaphragm tracking (DT) and (C, D) Xsight lung tracking (XLT). Tables
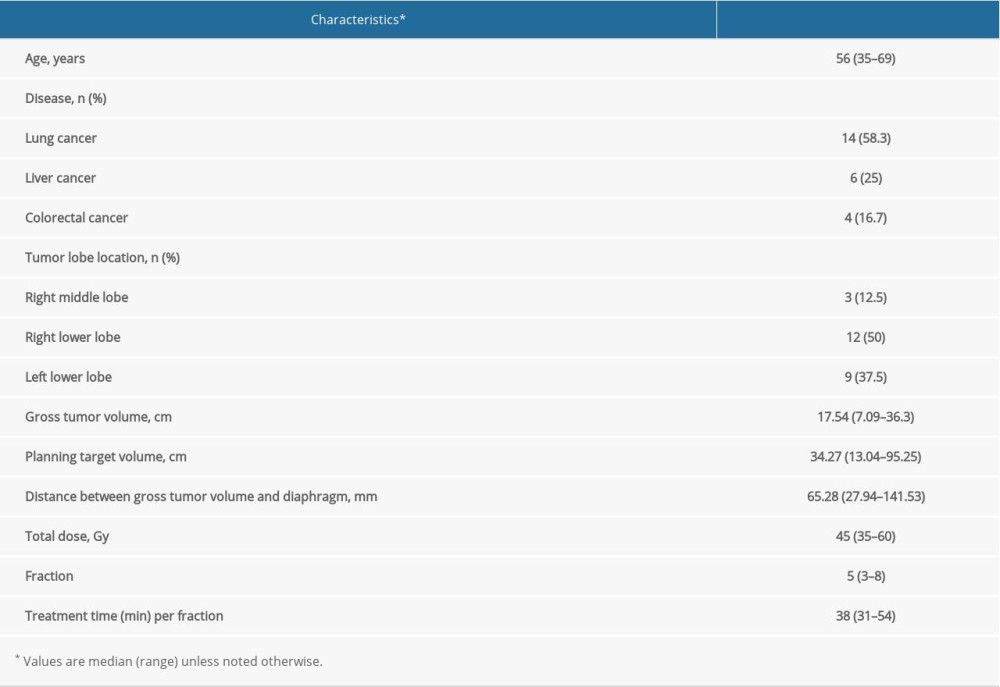 Table 1. Patient characteristics (N=24).
Table 1. Patient characteristics (N=24).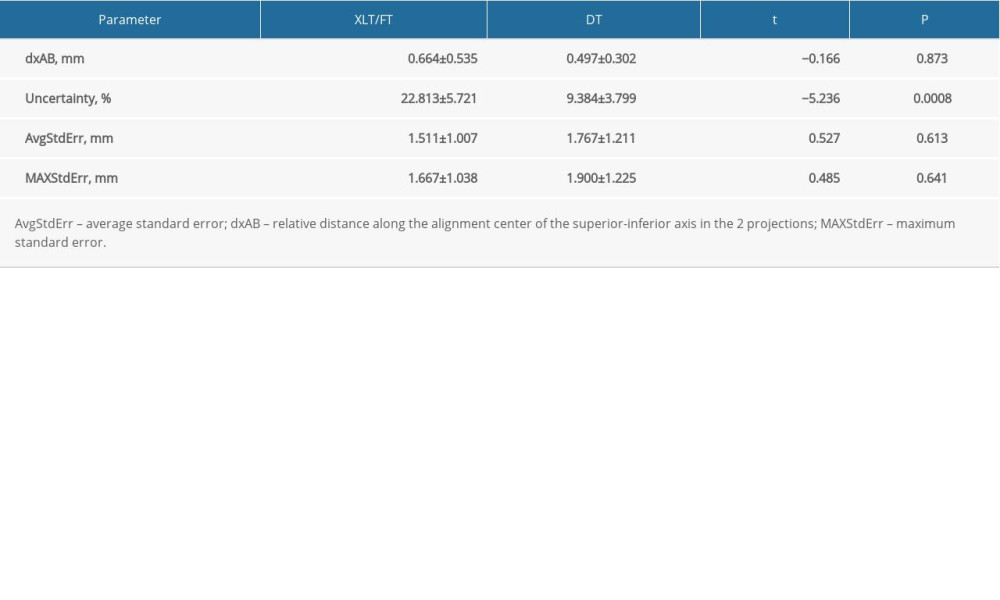 Table 2. Comparison of Synchrony model quality parameters between Xsight lung tracking/fiducial tracking (XLT/FT) and diaphragm tracking (DT) (N=24).
Table 2. Comparison of Synchrony model quality parameters between Xsight lung tracking/fiducial tracking (XLT/FT) and diaphragm tracking (DT) (N=24). Table 1. Patient characteristics (N=24).
Table 1. Patient characteristics (N=24). Table 2. Comparison of Synchrony model quality parameters between Xsight lung tracking/fiducial tracking (XLT/FT) and diaphragm tracking (DT) (N=24).
Table 2. Comparison of Synchrony model quality parameters between Xsight lung tracking/fiducial tracking (XLT/FT) and diaphragm tracking (DT) (N=24). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








