04 February 2022: Clinical Research
Blood Pressure Rhythm and Blood Pressure Variability as Risk Factors for White Matter Lesions: A Cross-Sectional Study
Dong Zhang1ABCDEF*, Mingli He2ABCDG, Qing He1DEG, Zeheng Li3DEFDOI: 10.12659/MSM.933880
Med Sci Monit 2022; 28:e933880
Abstract
BACKGROUND: White matter lesions are common in the elderly. The aim of this study was to explore the correlation between blood pressure rhythm and blood pressure variability with white matter lesions.
MATERIAL AND METHODS: A total of 144 subjects aged 40 to 80 years underwent MRI scanning to assess the degree of white matter lesions using the Fazekas scale. The regional cerebral blood flow was detected by brain perfusion imaging, and an ambulatory blood pressure monitor was used to measure the circadian blood pressure rhythm. Odds ratio and the 95% confidence interval was computed using logistics regression analysis. The relationship between various factors and blood pressure was calculated by curve simulation.
RESULTS: With the increase of white matter lesions, the regional cerebral blood flow at the lesion decreased gradually. Systolic blood pressure day/night difference ratio (OR=0.815, 95% CI 0.729-0.910), diastolic blood pressure day/night difference ratio (OR=0.895, 95% CI 0.831-0.964), systolic blood pressure coefficient of variation (OR=1.589, 95% CI 1.273-1.983), and diastolic blood pressure coefficient of variation (OR=1.363, 95% CI 1.150-1.616) were significantly associated with Fazekas score (P<0.05 for all).
CONCLUSIONS: Greater blood pressure variability and blood pressure rhythm disorders were associated with lower regional cerebral blood flow in patients with white matter lesions.
Keywords: Blood Pressure Monitors, Hypertension, Leukoencephalopathies, Regional Blood Flow, Adult, Aged, 80 and over, Blood Pressure, Cross-Sectional Studies, Female, Humans, Magnetic Resonance Imaging, Male, Risk Factors, white matter
Background
White matter lesions (WMLs) are a very common condition in the elderly, and may be confirmed only when cognition impairment [1], executive motor function dysfunction, and other symptoms [2] occur due to the progression of lesions. Numerous recent studies have shown that hypertension and aging are important causes of WMLs [3]. In addition to hypertension, both blood pressure rhythm (BPR) [4] and blood pressure variability (BPV) [5] have been shown to markedly increase the residual risk of WMLs.
The elements of blood pressure comprise blood pressure value (BP), BPV, and BPR. Although the impacts of elevated BP on the body have long been recognized, people are now paying close attention to increased BPV and abnormal BPR [6]. A European study demonstrated that the risk of cardiovascular and cerebrovascular events is closely associated with BPV [7], as well as circadian BPR [8]. Empirical studies have also emphasized that WMLs may be due to mild chronic cerebral white matter hypoperfusion caused by cerebral small-vessel lesions [9]. Some risk factors such as hypertension are important causes of such small-vessel lesions [10]. In addition, the increase in BPV has been found to directly induce damages to small perforating vessels in brain tissue, for which adaptive dilatation of the perforator is impaired, causing local chronic hypoperfusion. Subsequently, this leads to a series of cerebral small-vessel diseases [11]. At present, the relevance of BPR disorder and increased BPV to regional cerebral blood flow (rCBF) of WMLs areas remains largely unknown.
Patients with WML often also have hypertension. For patients undergoing treatment for hypertension, the effect of anti-hypertensive drugs and the mode of administration can also significantly affect the features of BP fluctuation. We thus believe that elevated BP is the underlying cause of WMLs [12] and that an increase in BPV due to BPR changes can contribute to the progression of WMLs. Unfortunately, no studies have assessed the interaction between BPR, rCBF, and the degree of WMLs. Therefore, we aimed to explore the use of the 24-h ambulatory blood pressure monitor (ABPM) method to accurately and quickly record the BP of patients throughout the day [13]. The patients’ rCBF at WML areas were recorded using craniocerebral perfusion imaging to explore the more detailed relationship between WMLs, rCBF, BPR and BPV, as well as the possible underlying mechanisms for the progression of WMLs in terms of BPR. We thus hypothesize that: (a) BPR and BPV are negatively correlated with rCBF and cognitive function, and (b) cognitive function is likely to decline as rCBF decreases.
Material and Methods
SUBJECT:
We enrolled 154 patients with various degrees of WMLs. They were enrolled from the Neurology Department of Lianyungang First People’s Hospital between November 2019 and November 2020. All subjects were selected from outpatient or inpatient departments with memory dysfunction and other symptoms as the chief concern. Patients were found to have WMLs and were selected according to the exclusion criteria and inclusion criteria after MRI examination. After learning about the study and signing the informed consent form, they were arranged to be hospitalized for the completion of relevant examinations. Based on the inclusion criteria and exclusion criteria, 8 patients were excluded due to data abnormalities, while 2 cases were excluded due to intolerance to MRI. Finally, we performed statistical analysis of data from 144 patients. Among them, 132 completed 24-h ABPM, and 134 cases completed the cerebral CT perfusion imaging (CTP) examination. The patients underwent brain MRI, cognitive function evaluation, 24-h ABPM, and other examinations. Per performed a cross-sectional observational study to explore the relationship between blood pressure and cerebral blood flow at WMLs. This study was authorized by the Ethics Committee of Lianyungang First People’s Hospital (approval number LW201910180010). All subjects had signed the informed consent form.
INCLUSION CRITERIA:
(1) Ages 40 to 80; (2) Definite white matter lesions found by cranial MRI.
EXCLUSION CRITERIA:
(1) Mental disorder; (2) secondary hypertension (eg, endocrine hypertension, renal hypertension); (3) acute cerebral infarction or previous history of severe cerebral infarction (at admission, NIH Stroke Scale >5, or infarction that can affect cognitive function); (4) Congenital vascular dysplasia; (5) other causes of white matter lesions, eg, autoimmune diseases, hypoxia, and intoxication; (6) allergic to iodine contrast agents; (7) liver and kidney failure; (8) a history of brain surgery; and (9) severe brain atrophy and extensive lacunar infarction.
CTP SCANNING:
We used Siemens dual-source computed tomography for CT examination, and Professional Syngo Software for image processing. We selected 2–3 CBF measurements of interest from bilateral lesion areas at the most prominent level of subcortical and periventricular WMLs based on the MRI scan image. Subsequently, the average value was taken as the CBF value for this side of the lesion area.
MRI SCANNING:
Magnetic resonance imaging type: GE Signa HDxt 3.0T, the U.S.A. All patients were scanned in the same posture.
WMLS ANALYSIS:
To evaluate WMLs in the periventricular and subcortical regions, we used the Fazekas scale for white matter lesions severity rating [14] (range: 0–6). Afterward, the scores from the 2 sections were added to calculate the total score. Periventricular or subcortical white matter high signal score was rated as 0: no lesions; 1: cap or pencil-like thin layer lesions; 2: lesions of smooth halo appearance; 3: irregular periventricular high signal extending to deep white matter. Fazekas grade (0–3) is characterized as follows: Grade 0: no lesions; Grade 1: mild lesions, 0 to 1; Grade 2: moderate lesions, 2 to 3; Grade 3: severe lesions, 4 to 6.
BP RECORD:
After 5 min in bed, the subject’s left brachial artery blood pressure was measured every 3 min using a calibrated electronic sphygmomanometer. Blood pressure was measured 3 times. Subsequently, the mean value was taken as the blood pressure at admission.
After completing all medical examinations, the subjects underwent 24-h ambulatory blood pressure monitoring (Spacelabs Healthcare 90217A, US), where diastolic blood pressure (DBP) and systolic blood pressure (SBP) data were collected at night and during the day. BP was recorded every 20 min between 6: 00 and 22: 00 (daytime), and every 30 min between 22: 00 and 6: 00 the next day (nighttime). We recorded the mean blood pressure and standard deviation (SD) during the daytime and nighttime. BPR is expressed as the rate of a drop in BP at night, blood pressure day/night difference ratio=(daytime BP-nighttime BP)/daytime BP×100. BPV was calculated with the formula: CV=SD/mean BP. During the examination period, subjects were only allowed to perform normal activities required for life, while vigorous exercises or other activities that could cause mental stimulation were prohibited. To prevent subjects from BP fluctuations due to stimulation, no other examinations or operations were allowed during this period. Because the anti-hypertensive treatment of patients is very complex (irregular and unreasonable drug use), it was necessary to maintain their blood pressure state at home and to avoid blood pressure fluctuations caused by sudden withdrawal or change of medication. We did not stop and change the patient’s current anti-hypertensive plan, but we adjusted the anti-hypertensive regimen and made a follow-up plan at discharge.
COGNITIVE FUNCTION ASSESSMENT:
The Montreal Cognitive Assessment Scale (MoCA Scale) was used to evaluate the participants’ cognitive function. During the test, the subject was in a quiet and enclosed room and was examined by a professional psychologist or neurologist [15].
DATA ANALYSIS:
The data are presented as mean±standard deviation, percentage, or interquartile range depending on their corresponding data distribution. Because the sample size was relatively small, there were few subjects with systolic blood pressure day/night difference ratio (SBPDNR) >10. To better reflect the data characteristics of subjects with different blood pressure rhythms, we used the interquartile range based on the SBPDNR to group the baseline data and examination results of patients, and then divided the patients into 2 groups: a lower SBPDNR group (<6.0) and a higher SBPDNR group (≥6.0). Data were tested for normality using the Kolmogorov-Smirnov test. The Mann-Whitney
Results
GENERAL INFORMATION:
We also observed that among the 144 participants, 70 (48.6%) patients exhibited serious WMLs (Fazekas score ≥2) (Table 1). We identified no significant differences in blood lipids, sex, fasting blood glucose, degree of education, coronary heart disease, smoking and alcohol consumption between the groups. However, there were significant differences in age (P=0.020), 24-h mean SBP (P=0.031), 24-h mean SBP (P<0.001), diastolic blood pressure day/night difference ratio (DBPDNR) (P<0.001), night SBP (P<0.001), night DBP (P<0.001), mean subcortical rCBF (P=0.003), mean periventricular rCBF (P=0.002), Fazekas score (P<0.001), and MoCA score (P<0.05) (Table 2).
ANALYSIS OF THE RELATIONSHIP BETWEEN WMLS AND VARIOUS FACTORS:
Our results, based on univariate binary logistic regression analysis of Fazekas score and various factors, revealed that age, 24hSBPCV, 24hDBPCV, SBPDNR, and DBPDNR were correlated with WMLs. In addition, multivariate logistic regression analysis of potential confounding factors, including sex, age, fasting blood glucose, blood lipid, hypertension, and BMI confirmed that factors that had previously been significantly associated still remained statistically correlated. The results of the single-factor multivariate logic analysis on Fazekas score and rCBF showed that a reduction in Fazekas scores led to a gradual increase in the rCBF at the lesion sites. Moreover, we performed a multivariate logistic regression analysis. Our findings indicated that the odds ratio was increased after multiparameter regulation. For subcortical WMLs, Fazekas 0 rCBF was 1.847 times higher than Fazekas 3 rCBF (OR=1.847, 95% CI=1.476–2.310, P<0.001), while for periventricular lesions, Fazekas 0 rCBF was 1.991 times higher than Fazekas3 rCBF (OR=1.991, 95% CI=1.565–2.532, P<0.001) (Table 3).
ANALYZING THE RELATIONSHIP BETWEEN DAY/NIGHT BPR, BPV, AND RCBF:
As shown in Figure 1, we observed that all quadratic simulation curves of SBPDNR, DBPDNR, and rCBF exhibited an inverted “U” shape, indicating that the BP day/night difference ratio was negatively correlated with rCBF and was positively correlated with rCBF at a certain interval. By observing the 2 ends of vertex coordinates, we found that there was a BP day/night difference ratio value corresponding to maintaining a good rCBF. We estimated the approximate corresponding BP day/night difference ratio interval between the rCBF coordinates. The results showed that when subcortical regional cerebral blood flow was 40–50 ml/100 g/min, the corresponding SBPDNR and DBPDNR intervals were 5–20 and 2–15, respectively. Similarly, when the periventricular regional cerebral blood flow was 40–50 ml/100g/min, the corresponding SBPDNR and DBPDNR intervals were 2–20 and −2–17, respectively. The quadratic simulation curves depicted that the BPV coefficient was roughly negatively correlated with rCBF (Figure 2).
RELATIONSHIP BETWEEN COGNITIVE FUNCTION, RCBF, AND BP:
As shown in Figures 3 and 4, the cubic simulation curve of SBPDNR, DBPDNR, and MoCA score revealed an “S” type relationship. Each curve had 2 turning points, whereby there was a relatively stable MoCA score interval between the 2 turning points. Regardless of whether this interval was on SBPDNR or DBPDNR, its median value was approximately 10. The quadratic simulation curve shows that the coefficient of variation of BP was significantly negatively correlated with the MoCA score. Finally, the quadratic simulation curve of MoCA score and rCBF demonstrated that when the subcortical CBF and lateral periventricular CBF were around 55 and 60 ml/100g/min, the MoCA score reached the highest value.
Discussion
This observational study explored the interaction between BPR, BPV, rCBF, and the degree of WMLs. Our results elucidated that both SBPDNR and DBPDNR were significantly correlated with WMLs, suggesting that the BPR may be a protective factor for WMLs. However, BPR and rCBF curves indicate a more complicated relationship between BPR and WMLs.
Some recent studies concluded that WMLs are associated with a decrease in rCBF at the lesions in elderly hypertensive patients [16]. Decreased cerebral perfusion can induce hypoxia and ischemia in both cerebral cortices, thus causing microcirculation disturbance and worsening neurodegenerative changes [17]. This is similar to our conclusions, but it is unclear whether BPR participates in the decreased CBF. To better reflect changes in other data when the BPR changes gradually, we used the interquartile range based on SBPDNR to group the baseline data. Our results (Table 2) showed that patients with weaker BPR or higher BP at night than during the day exhibited higher mean BP throughout the day, and were more likely to develop WMLs, accompanied by more severe cognitive impairment. Similarly, in the intergroup comparison of Q1 and Q3, we found that there were differences in age, nocturnal blood pressure, coefficient of variation of blood pressure, Fazekas score, rCBF and MOCA score between 2 groups. We also noted that the rCBF in the low SBPDNR group was considerably lower compared with that in the high SBPDNR group. We found that the rCBF of Fazekas 0 was obviously higher than that of patients with Fazekas3 in both subcortical and periventricular WMLs (Table 3). A plausible explanation for this is that an increase in BP at night caused by BPR disorder was possibly one of the factors causing the decrease of CBF in WMLs.
In our previous study [18], we found that in terms of WMLs, nocturnal BP increase might be more dangerous than daytime BP increase. A study by Dirk Sander emphasized that circadian SBP changes, especially nocturnal SBP increase, might play a pivotal role in the pathogenesis of WMLs [19]. However, the study did not identify their specific relationship and did not focus on DBP changes. In the present study, we identified that SBPDNR and DBPDNR were protective factors for WMLs. However, Figure 2 illustrates that when SBPDNR gradually approached the normal level (10–20), a gradual increase in rCBF occurred. On the other hand, when SBPDNR gradually shifts from the normal level, a subsequent drop in rCBF was observed. Likewise, a study conducted in China demonstrated a marked increase in WMLs volume in patients with chronic extreme dipper pattern, non-dipper pattern, or reversed-dipper pattern of BP compared to those with dipper pattern of BP [20]. The above-described results indicate that the normal BPR is a protective factor that can postpone the progression of lesions, while BPR disorder can promote the decrease in intracranial rCBF, which can subsequently accelerate the occurrence and development of WMLs.
Besides BPR, the BPV coefficient was negatively correlated with rCBF, indicating that an increase in the BPV coefficient led to a decrease in the rCBF. This outcome concurred with the results of an observational study in China, which reported that excessive SBP variability accelerates cognitive dysfunction and the development of brain WMLs, particularly in elderly patients [21]. It has been shown that high BPV can lead to frequent episodes of hypotension, which may result in cerebral hypoperfusion, thereby causing cerebral small-vessel disease [3], hippocampal atrophy [22], and accelerating cognitive impairment. In this present study, we confirmed the relationship between BPV and local hypoperfusion of WMLs, which is probably based on hypertension and BPR disorder. A study by Tessa van Middelaar found that high SBP and pulse pressure variability are associated with the progression of WMLs; therefore, interventions for variability reduction may be the most effective means for alleviation of WMLs [23]. Here, we verified a possible mechanism in which the increase in BP coefficient of variation leads to a decrease in rCBF, which ultimately promotes the development of WMLs. Therefore, reducing BP fluctuation is imperative for the treatment of hypertension.
Although a close relationship between cognitive dysfunction and WMLs has long been verified by numerous studies [1,24,25], few researchers have explored the relationship between CBF in the diseased area and cognitive function. Liu’s study found that decreased perfusion in the WMLs region caused by posterior cerebral artery stenosis was associated with cognitive decline [21]. However, the sample size of the study was small and there is a lack of research on BP. Our results, based on the relationship of MoCA score with BPR, BPV, and rCBF, revealed that when BPR is normal, cognitive function is relatively stable. As BPV increases, cognitive function also deteriorates, which was in line with the association between BPV and rCBF. Through the study of cognitive function, we indirectly proved the influence of BPR disorder and increased BPV on rCBF, which is a highly overlooked research area.
This study has shown that the most important risk factors for increased white matter lesions with age was hypertension, suggesting that the treatment of hypertension can delay the progression of WMLs [26]. A study published in JAMA documented that after intensive anti-hypertensive treatment in hypertensive patients, the group with a target SBP below 120 mmHg exhibited lower WMLs volume and higher total cerebral blood volume compared to the group with a target SBP below 140 mmHg [27]. Similarly, this study demonstrates that effective anti-hypertensive therapy can significantly mitigate the progress of WMLs. Nevertheless, the specific changes in the patients’ BPR during anti-hypertensive treatment and the relevant influence on the progression of WMLs remain unclear, requiring further exploration. Moreover, no randomized controlled clinical trials have investigated BPR and WMLs. Therefore, treatment strategies that merely reduce BP while ignoring the patients’ own BPR disorder may be inadequate in preventing the progression of WMLs. In addition, only a few researchers have recognized the hazard of the impact of elevated BP at night on the progression of WMLs because most follow-up studies and data acquisitions are conducted during the day, whereas the relevant nighttime data on patients are often not collected. We emphasize that patients often pay more attention to their blood pressure during the day when they are at home and neglect to treat their blood pressure at night. This may have quietly contributed to the progression of WMLs.
There are some inherent limitations in our study. Firstly, the sample size of patients in this study was small, and the fact that they were all selected from the same hospital ward could have biased the study and limit generalization of its results. Second, there should be a reasonable anti-hypertensive program for follow-up observation. Lastly, subsequent studies should include multicenter clinical trials with larger sample sizes and long-term follow-ups to verify the reliability and validity of BPR regulation in preventing and delaying the progression of WMLs. The assessment of white matter lesions with only visual rating scale is another limitation.
Conclusions
The findings of this research provide new clinical evidence that when blood pressure rhythm is disturbed or blood pressure variability is increased, it is likely to promote the progression of WMLs by reducing rCBF, and normal blood pressure rhythm may be a protective factor for WMLs. We thus recommend that patients with WMLs should maintain a normal BPR when controlling hypertension and should pay attention to reducing blood pressure during the day. More importantly, they should also pay attention to the appearance of high blood pressure at night. However, in the process of lowering blood pressure, it is necessary to avoid drastic fluctuations in blood pressure caused by high or low blood pressure.
Figures
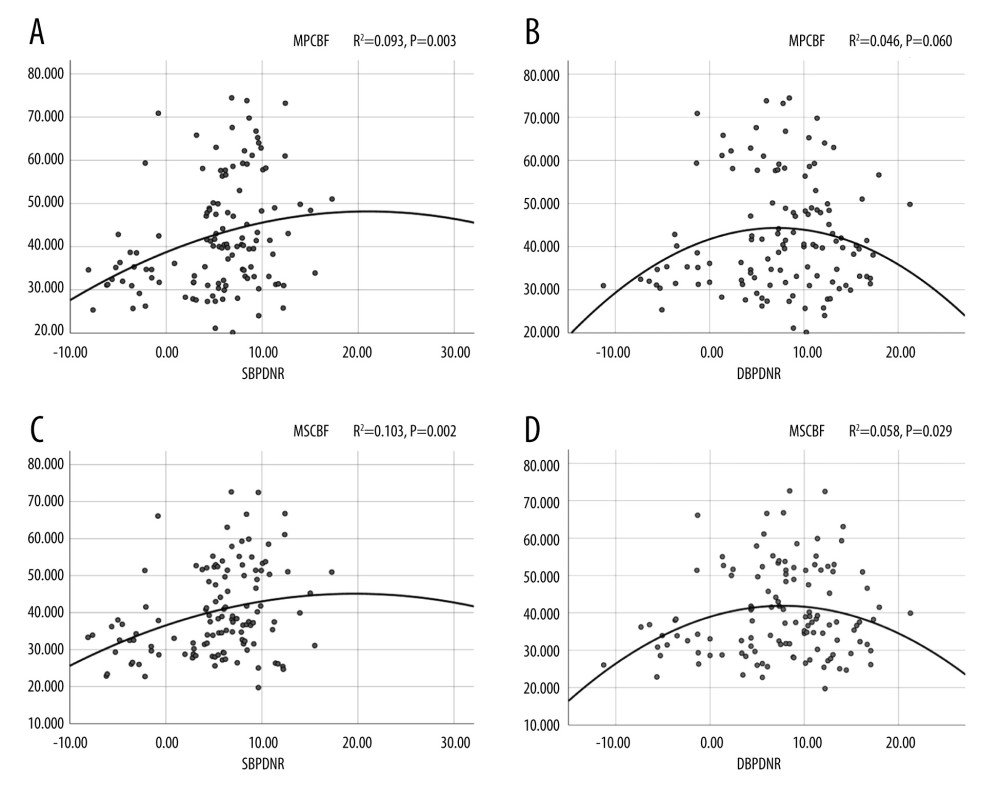 Figure 1. (A–D) Quadratic curve of blood pressure rhythm and rCBF. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 1. (A–D) Quadratic curve of blood pressure rhythm and rCBF. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. 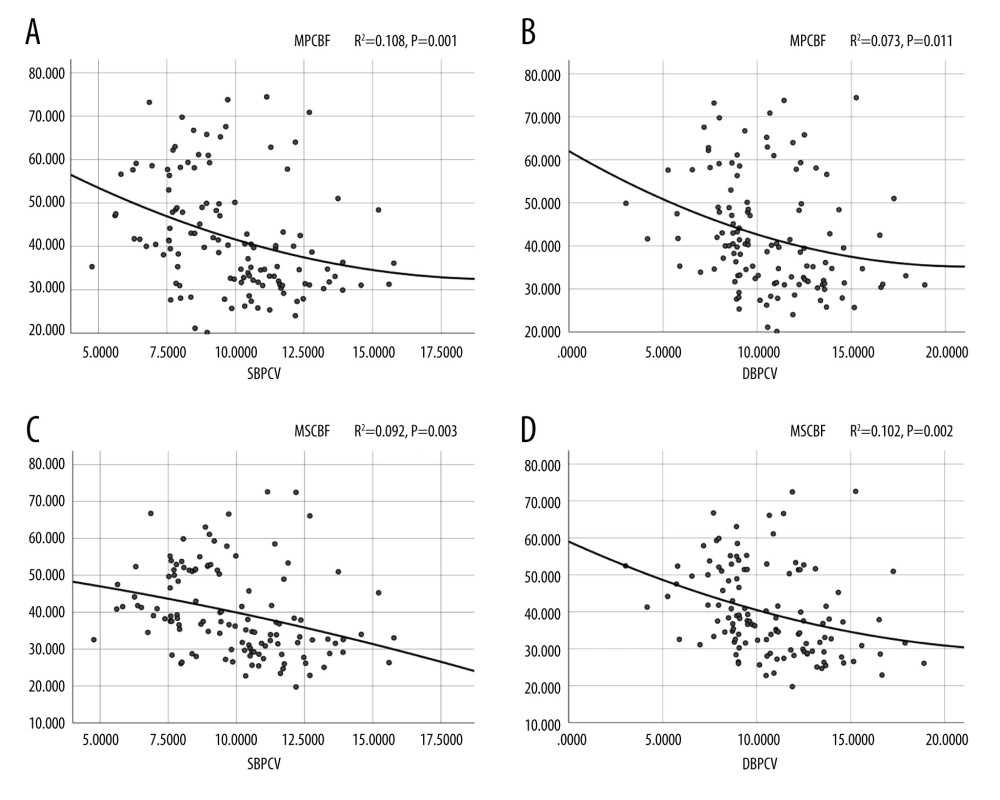 Figure 2. (A–D) Quadratic curve of blood pressure variability coefficient and rCBF. SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 2. (A–D) Quadratic curve of blood pressure variability coefficient and rCBF. SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. 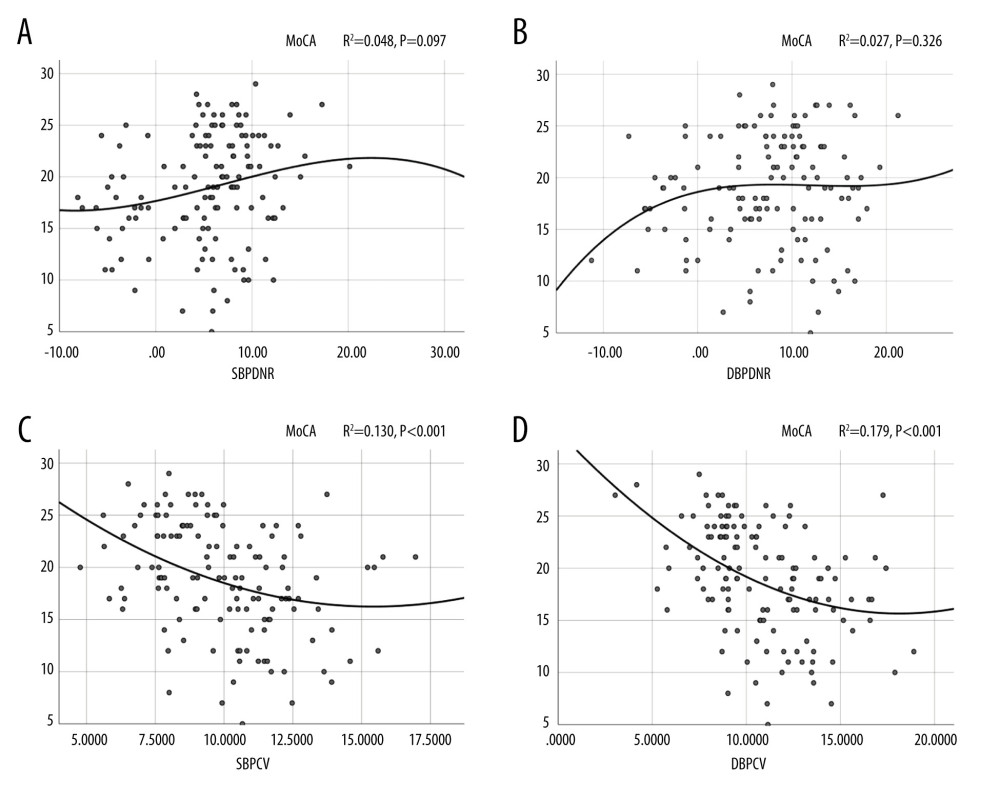 Figure 3. (A–D) Relationship between MoCA and blood pressure. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; SPSS Statistics 26 IBM.
Figure 3. (A–D) Relationship between MoCA and blood pressure. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; SPSS Statistics 26 IBM. 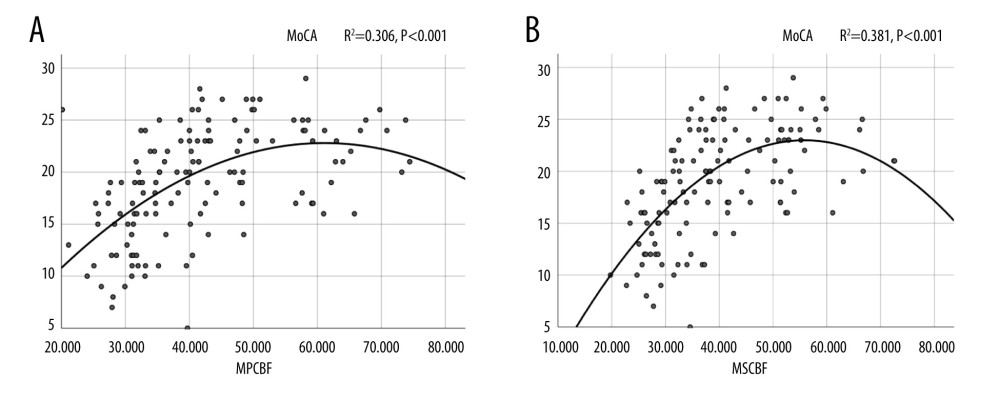 Figure 4. (A, B) Relationship between MoCA and cerebral blood flow. MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 4. (A, B) Relationship between MoCA and cerebral blood flow. MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. References
1. Jokinen H, Goncalves N, Vigario R, Early-stage white matter lesions detected by multispectral MRI segmentation predict progressive cognitive decline: Front Neurosci, 2015; 9; 455
2. Abraham HM, Wolfson L, Moscufo N, Cardiovascular risk factors and small vessel disease of the brain: Blood pressure, white matter lesions, and functional decline in older persons: J Cereb Blood Flow Metab, 2016; 36; 132-42
3. Pantoni L, Cerebral small vessel disease: From pathogenesis and clinical characteristics to therapeutic challenges: Lancet Neurol, 2010; 9; 689-701
4. Hannawi Y, Yanek LR, Kral BG, Hypertension is associated with white matter disruption in apparently healthy middle-aged individuals: Am J Neuroradiol, 2018; 39; 2243-48
5. Kim BJ, Kwon SU, Park JM, Blood pressure variability is associated with white matter lesion growth in intracranial atherosclerosis: Am J Hypertens, 2019; 32; 918-24
6. Erdogan D, Gullu H, Caliskan M, The influence of circadian blood pressure changes on aortic distensibility and left ventricular diastolic function in hypertensive individuals: Int J Cardiovasc Imaging, 2006; 22; 157-65
7. Gosmanova EO, Mikkelsen MK, Molnar MZ, Association of systolic blood pressure variability with mortality, coronary heart disease, stroke, and renal disease: J Am Coll Cardiol, 2016; 68; 1375-86
8. Palatini P, Thijs L, Staessen JA, Predictive value of clinic and ambulatory heart rate for mortality in elderly subjects with systolic hypertension: Arch Intern Med, 2002; 162; 2313-21
9. Kurata M, Okura T, Watanabe S, Higaki J, Association between carotid hemodynamics and asymptomatic white and gray matter lesions in patients with essential hypertension: Hypertens Res, 2005; 28; 797-803
10. Black HR, The burden of cardiovascular disease: following the link from hypertension to myocardial infarction and heart failure: Am J Hypertens, 2003; 16; 4S-6S
11. Caplan LR, Lacunar infarction and small vessel disease: Pathology and pathophysiology: J Stroke, 2015; 17; 2-6
12. Mortamais M, Reynes C, Brickman AM, Spatial distribution of cerebral white matter lesions predicts progression to mild cognitive impairment and dementia: PLoS One, 2013; 8; e56972
13. Cardoso CR, Salles GF, Prognostic importance of ambulatory blood pressure monitoring in resistant hypertension: Is it all that matters?: Curr Hypertens Rep, 2016; 18; 85
14. Fazekas F, Chawluk JB, Alavi A, MR signal abnormalities at 1.5 T in Alzheimer’s dementia and normal aging: Am J Roentgenol, 1987; 149; 351-56
15. Nasreddine ZS, Phillips NA, Bedirian V, The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment: J Am Geriatr Soc, 2005; 53; 695-99
16. van Dalen JW, Mutsaerts H, Nederveen AJ, White matter hyperintensity volume and cerebral perfusion in older individuals with hypertension using arterial spin-labeling: Am J Neuroradiol, 2016; 37; 1824-30
17. Vernieri F, Pasqualetti P, Matteis M, Effect of collateral blood flow and cerebral vasomotor reactivity on the outcome of carotid artery occlusion: Stroke, 2001; 32; 1552-58
18. Zhang D, Zhang J, Zhang B, Association of blood pressure, white matter lesions, and regional cerebral blood flow: Med Sci Monit, 2021; 27; e929958
19. Dirk S, Kerstin W, Jürgen KF, Bastian C, Extent of cerebral white matter lesions is related to changes of circadian blood pressure rhythmicity: Arch Neurol, 2000; 57; 1302-7
20. Zhang H, Cui Y, Zhao Y, Association of circadian rhythm of blood pressure and cerebral small vessel disease in community-based elderly population: J Gerontol A Biol Sci Med Sci, 2019; 74; 1322-30
21. Liu Z, Zhao Y, Zhang H, Excessive variability in systolic blood pressure that is self-measured at home exacerbates the progression of brain white matter lesions and cognitive impairment in the oldest old: Hypertens Res, 2016; 39; 245-53
22. Barnes J, Bartlett JW, van de Pol LA, A meta-analysis of hippocampal atrophy rates in Alzheimer’s disease: Neurobiol Aging, 2009; 30; 1711-23
23. van Middelaar T, Richard E, Moll VCE, Visit-to-visit blood pressure variability and progression of white matter hyperintensities among older people with hypertension: J Am Med Dir Assoc, 2019; 20; 1175-77
24. Silbert LC, Dodge HH, Perkins LG, Trajectory of white matter hyperintensity burden preceding mild cognitive impairment: Neurology, 2012; 79; 741-47
25. Ogama N, Sakurai T, Nakai T, Impact of frontal white matter hyperintensity on instrumental activities of daily living in elderly women with Alzheimer disease and amnestic mild cognitive impairment: PLOS ONE, 2017; 12; e172484
26. Wang T, Li Y, Guo X, Reduced perfusion in normal-appearing white matter in mild to moderate hypertension as revealed by 3D pseudocontinuous arterial spin labeling: J Magn Reson Imaging, 2016; 43; 635-43
27. Nasrallah IM, Pajewski NM, Auchus AP, Association of intensive vs standard blood pressure control with cerebral white matter lesions: JAMA, 2019; 322; 524-34
Figures
 Figure 1. (A–D) Quadratic curve of blood pressure rhythm and rCBF. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 1. (A–D) Quadratic curve of blood pressure rhythm and rCBF. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. Figure 2. (A–D) Quadratic curve of blood pressure variability coefficient and rCBF. SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 2. (A–D) Quadratic curve of blood pressure variability coefficient and rCBF. SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. Figure 3. (A–D) Relationship between MoCA and blood pressure. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; SPSS Statistics 26 IBM.
Figure 3. (A–D) Relationship between MoCA and blood pressure. SBPDNR – systolic blood pressure day/night difference ratio; DBPDNR – diastolic blood pressure day/night difference ratio; SBPCV – systolic blood pressure coefficient of variation; DBPCV – diastolic blood pressure coefficient of variation; SPSS Statistics 26 IBM. Figure 4. (A, B) Relationship between MoCA and cerebral blood flow. MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM.
Figure 4. (A, B) Relationship between MoCA and cerebral blood flow. MPCBF – mean periventricular cerebral blood flow; MSCBF – mean subcortical cerebral blood flow; SPSS Statistics 26 IBM. Tables
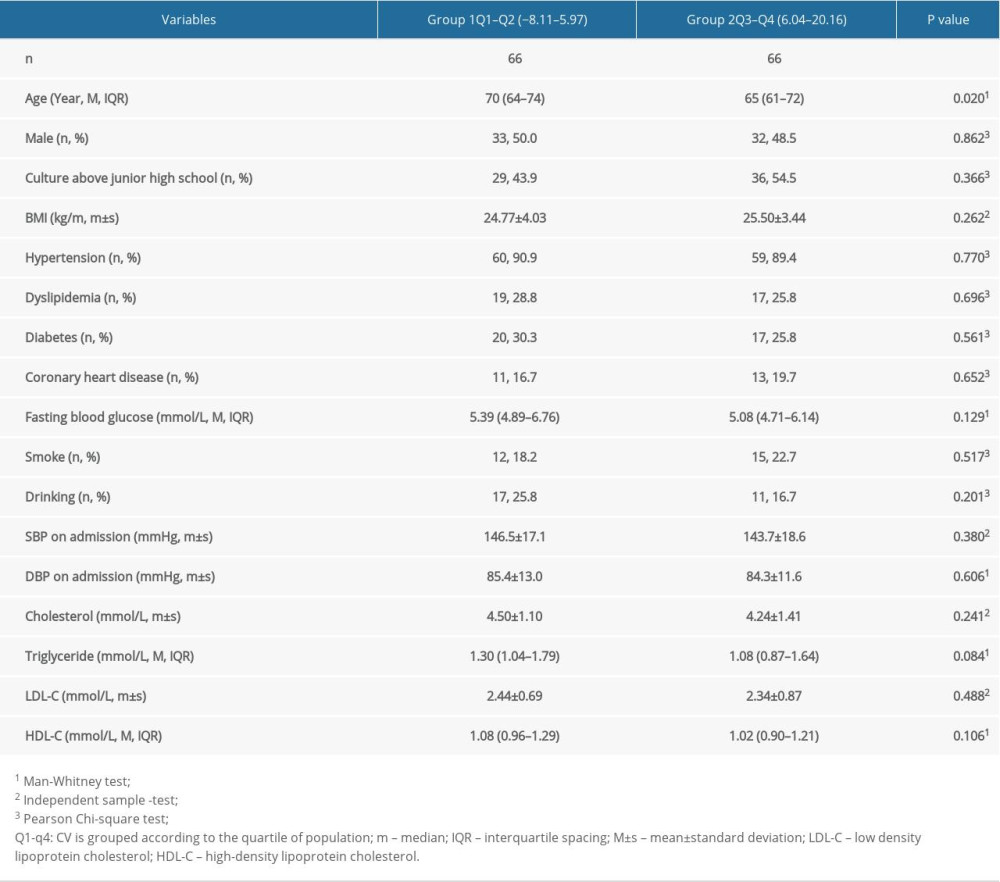 Table 1. Baseline characteristics of patients according to SBP day/night ratio quartile grouping.
Table 1. Baseline characteristics of patients according to SBP day/night ratio quartile grouping.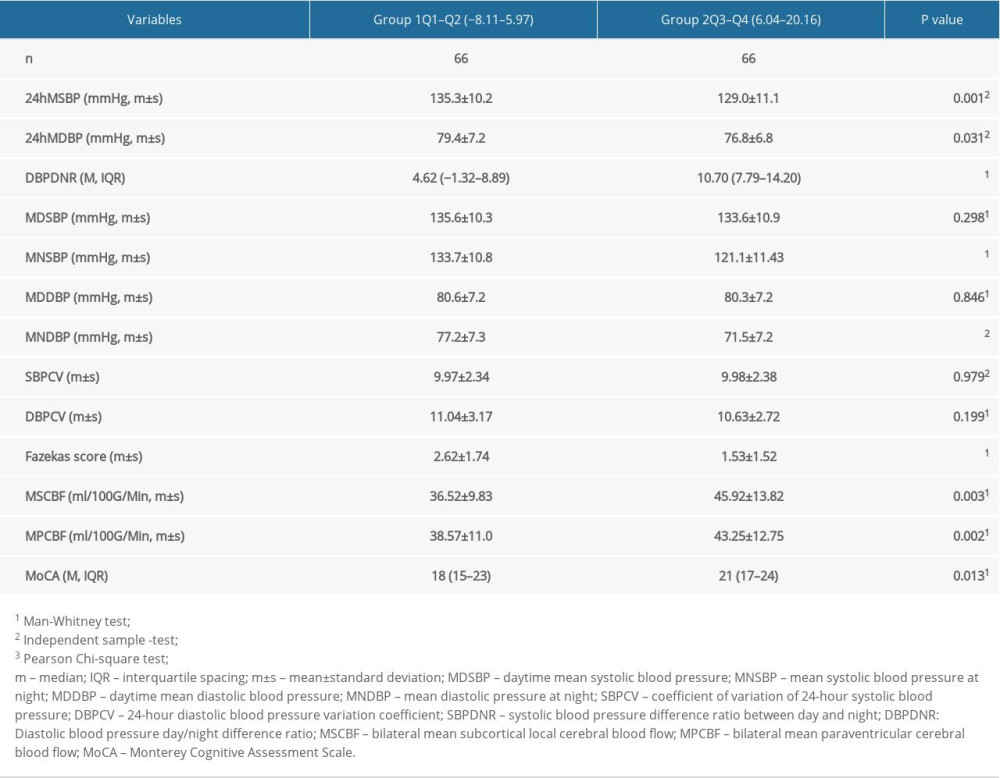 Table 2. Main examination results of patients according to SBP day/night ratio quartile grouping.
Table 2. Main examination results of patients according to SBP day/night ratio quartile grouping.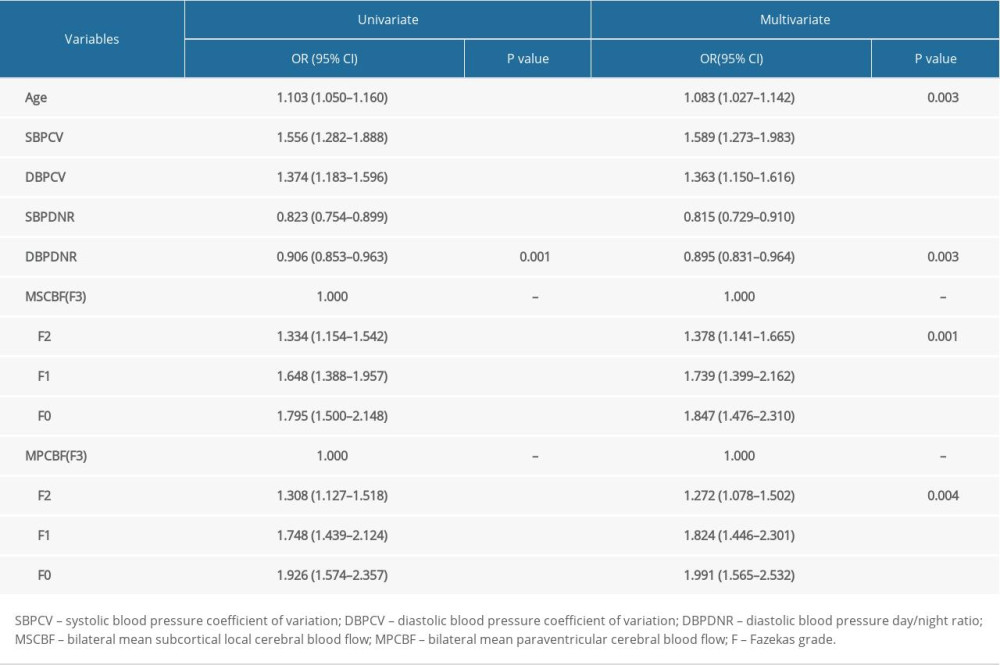 Table 3. Logistic regression analysis of Fazekas grades and various factors.
Table 3. Logistic regression analysis of Fazekas grades and various factors. Table 1. Baseline characteristics of patients according to SBP day/night ratio quartile grouping.
Table 1. Baseline characteristics of patients according to SBP day/night ratio quartile grouping. Table 2. Main examination results of patients according to SBP day/night ratio quartile grouping.
Table 2. Main examination results of patients according to SBP day/night ratio quartile grouping. Table 3. Logistic regression analysis of Fazekas grades and various factors.
Table 3. Logistic regression analysis of Fazekas grades and various factors. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








