12 January 2022: Clinical Research
Retrospective Study of Surgical Outcomes in 60 Patients with Crohn Disease from a Single Center in Poland
Karolina Majewska1BCDEF*, Cezary Rusinowski1BCD, Beata JabłońskaDOI: 10.12659/MSM.934463
Med Sci Monit 2022; 28:e934463
Abstract
BACKGROUND: In Crohn disease (CD), pharmacotherapy with nutritional support is the treatment of choice. However, complications and a lack of response to drugs are indications for surgery. The aim of this study was to present indications for surgery and methods of surgical treatment of CD and to analyze the postoperative morbidity and mortality risk factors.
MATERIAL AND METHODS: This was a retrospective analysis of adult patients who underwent surgery for CD between January 2015 and January 2019. Sixty of 457 patients (13%) hospitalized for CD required surgical treatment. The parameters age, sex, body mass index, duration, behavior and location of the disease, pharmacotherapy, indications for surgery, type and duration of surgery, perioperative complications, and laboratory tests results were analyzed.
RESULTS: Most procedures (90%) were elective. The most common indications for surgery were fistulae and strictures. The most frequently performed procedure was right hemicolectomy (60%). Thirty-two percent of patients had postoperative complications. Perianal disease (P=0.002) and penetrating behavior (P=0.01) were associated with more surgeries. Stricturing and penetrating behavior was more frequent in patients with ileal/ileocecal involvement than in those with CD affecting the colon (P=0.039). Patients with smoking history had a significantly lower age at first surgery (P=0.02). The use of anti-TNF medications appeared to extend time between diagnosis and first surgery (P=0.014).
CONCLUSIONS: Although the analysis did not reveal any risk factors for perioperative complications, perianal manifestations, penetrating disease type, ileal/ileocecal involvement, and smoking may be associated with risk of earlier surgery or multiple surgeries.
Keywords: Crohn Disease, general surgery, Postoperative Complications, Adult, Age Factors, Body Mass Index, Female, Humans, Male, operative time, Poland, Risk Factors, Sex Factors
Background
Crohn disease (CD) is a chronic inflammatory disease that can affect any part of the gastrointestinal tract. Pharmacotherapy, including corticosteroids, immunomodulators (6-mercaptopurine, azathioprine, methotrexate), tumor necrosis factor (TNF) inhibitors (infliximab, adalimumab), and other biologicals (vedolizumab, ustekinumab) along with nutritional support (oral nutrition supplements, enteral nutrition, exclusive enteral nutrition, parenteral nutrition) is the treatment of choice for CD [1–3]. Current strategies aim for deep, long-lasting remission with mucosal healing. Main goals include preventing complications and disease progression and restoring quality of life because curative, causal therapy is not yet available [1–5].
Despite optimal pharmacotherapy, many patients have complications, such as obstruction, fistulae, or abscesses, which are indications for surgical intervention [6]. The 10-year risk of major abdominal surgery for CD decreased from 46.5% to 26.2% during recent decades [7]. There have been consistent improvements in surgical treatment of CD over the years. Since the surgery for CD has become more specialized and less invasive, it can be considered not only as a last resort but also as an alternative to pharmacotherapy [8,9].
The chronic nature of CD is the reason a vast number of patients have many risk factors for perioperative complications. According to several studies [10–14], age, preoperative weight loss, malnutrition, low albumin level, elevated C-reactive protein (CRP) level, disease duration, penetrating behavior, duration of surgery, open surgery, previous resection, and use of steroids or anti-TNF medications are associated with an increased risk of complications. However, rates of complications vary widely (17.6% to 40.9%) in different studies [10–13], and the safety of preoperative anti-TNF therapy is still debated. In 2020, the European Crohn’s and Colitis Organisation (ECCO) guidelines on surgical treatment of CD stated that cessation of anti-TNF therapy prior to surgery is not mandatory [6]; however, this recommendation remains controversial [15]. Some recent meta-analyses reported an association between biological treatment and perioperative complications, while another found no difference in risk [16–18].
The aim of this study was to present the most common indications for surgery and the methods and results of surgical treatment of CD in our referral hospital. We also analyzed the prevalence of postoperative morbidity and mortality risk factors as well as correlations between obtained data and the rate of perioperative complications.
Material and Methods
ETHICS STATEMENT:
This was a retrospective study of medical records, and all patients gave their written informed consent for data management. According to the opinion of the Ethics Committee and local legislation, no additional approval was required due to the anonymous and non-interventional design of the project.
STUDY POPULATION:
The data were obtained from the medical records of patients with CD who underwent surgery between January 2015 and January 2019 in the Department of Digestive Tract Surgery, University Clinical Center, Medical University of Silesia in Katowice. Sixty adult patients with CD confirmed by ileocolonoscopy with multiple biopsy specimens or by histopathological examination of the specimen removed during previous surgery were included in the study. The small intestine involvement was assessed with magnetic resonance imaging (MRI) or computed tomography (CT). We excluded 9 patients with CD who had surgery only to restore bowel continuity.
ANALYZED PARAMETERS:
The patients were classified according to the Montreal Classification for CD [19]. For each patient, we determined current age at diagnosis (A), location (L), and behavior (B) status. The analyzed parameters were the following: age, sex, clinical features (locations and behavior of the disease, body mass index (BMI), age at diagnosis, disease duration, presence of abscesses or fistulae, smoking habit, CD pharmacotherapy, comorbidities (diabetes, hypertension, asthma, ischemic heart disease), surgical characteristics (age at first surgery, time between diagnosis and first surgery, number of surgeries, indications, American Society of Anesthesiologists (ASA) class, duration, type of surgery, technique and position of the anastomosis, need of ostomy creation, size of removed specimen, blood loss, presence and type of early (0–30 days after the surgery) and late (>30 days) perioperative complications, need of reoperation, mortality, and time of hospitalization before and after surgery. We also analyzed results of laboratory tests at admission day: white blood cells (WBC), platelets, hemoglobin, protein, albumin, and CRP levels.
STATISTICAL ANALYSIS:
The statistical analyses were performed using the program Statistica 13.3. Continuous variables were reported as mean and standard deviation. Qualitative variables were expressed as absolute values and percentages. The Mann-Whitney U test or Kruskal-Wallis test and chi-squared test or Fisher’s exact test were used to compare between-group differences for quantitative and qualitative variables, respectively. Analyzed dependent variables were age at first surgery, time from diagnosis to first surgery, number of surgeries due to CD, and length of hospitalization. The distribution of quantitative variables was verified with the Shapiro-Wilk test. Odds ratios (OR) with their 95% confidence intervals (CI) were calculated, if applicable. Pearson’s correlation or Spearman’s rank correlation was used to find associations between continuous variables. A
We performed univariate analysis for morbidity and mortality risk factors using the chi-squared test and Mann-Whitney U test. Analyzed dependent variables were death within 30 days after surgery, occurrence of complications, and occurrence of severe complications (classified as Clavien-Dindo grade ≥III). Multivariate analysis with logistic regression model was considered for independent variables with a
The results were divided into 4 sections: study population characteristics, laboratory tests results, surgical characteristics, and associative analysis.
Results
STUDY POPULATION CHARACTERISTICS:
Forty-eight percent (n=29) of 60 patients were women. The mean age was 38±10.41 (21–75) years. According to the Montreal classification, the most common location was ileocolic. The most frequent behavior was stricturing and penetrating (B2+B3), with only 11.9% (n=7) of patients having non-stricturing, non-penetrating CD, but 42.9% of them (n=3) had concomitant perianal disease. Patients’ general clinical characteristics are detailed in Table 1.
LABORATORY TESTS:
Thirty percent (n=21) of patients had increased WBC levels, and 43% (n=26) had increased platelet levels. Nineteen patients (31.7%) were underweight. Approximately 50% (n=31) of patients had anemia. Mild anemia was most common (n=21), but moderate and severe anemia occurred more often in women than in men (Figure 1); however, the difference was not significant (P=0.363). Albumin levels were decreased in 42.4% of patients (14/33), and CRP levels were elevated in 73.6% of patients (39/53). Detailed results of laboratory tests are described in Table 2.
SURGICAL CHARACTERISTICS:
Sixty-eight percent of patients had the first surgery due to CD before the age of 40 years (Figure 2A). Most patients (70%, n=30) required surgery during first 5 years from diagnosis (Figure 2B). Mean time between diagnosis and first surgery was 4.5 years (±4.5). Sixty percent (n=36) of patients already had surgery for CD before 2015. Thirty percent (n=18) of patients had more than 1 previous surgery. The most common indications for surgery were fistula, stricture, strictures with intermittent ileus, and abscess (Table 3). Ten percent (n=6) of surgeries were urgent, with indications of perforation (n=2), abscess (n=2), and obstruction (n=2).
The right hemicolectomy was the most frequent procedure in our patients. The main procedures are listed in Table 3. The additional procedures were abscess drainage (n=9), surgical treatment of fistulae (n=6), marsupialization of an ovarian cyst (n=3), hernia repair (n=2), splenectomy (n=1), partial gastrectomy (n=1), and cholecystectomy (n=1).
The total number of patients who had partial resection of the ileum or jejunum was 43 (72%). There were 3 resections of the jejunum, with an average length of removed specimen of 73.3 cm (range, 10–100 cm). The ileal resections were performed as main procedures or during hemicolectomy, with an average length of removed intestine of 41.6 cm (range, 5–150 cm).
Intestinal anastomoses were created in 60% of patients (n=36), while 33% (n=20) of patients required ostomy creation. All created ostomies were end enterostomies. The types of enterostomies and anastomoses are listed in Table 3.
The complications rate was 31.7% (n=19). The complication details are presented in Table 4. Reoperation was essential in 15% (n=9) of patients. Ten percent (n=6) of patients had another surgery to restore bowel continuity.
ASSOCIATIVE ANALYSIS:
The analysis of disease behavior according to the Montreal classification showed that perianal disease was associated with more surgeries (OR 8.85, 95% CI 1.05–74.5, P=0.002). Also, the mean age at first surgery was lower (31±6.5) in patients with anal lesions than in patients without perianal disease (35±10.3), but the difference was not significant (P=0.33). Time from diagnosis to first surgery was associated with disease behavior (P=0.02, Kruskal-Wallis test), and the difference was significant between groups with B1 and B3 (P=0.02, Mann-Whitney U test) and between groups with B2 and B3 (P=0.048), but not between groups with B1 and B2 (Figure 2C). Penetrating-type disease was associated with the shortest average time between diagnosis and first surgery (3.4±4.7). Moreover, patients with penetrating disease had significantly more surgeries (OR 3.8, 95% CI 1.19–12.14, P=0.01) than other patients. Non-stricturing, non-penetrating behavior (B1) was more frequent in patients with colitis type (L2) than in those with ileitis or ileocolitis (L1, L3) type (33.3% and 8.2% respectively, OR 5.63, 95% CI 1.01–31.5, P=0.03). CD diagnosis at an older age was associated with shorter time between diagnosis and first surgery (Spearman’s correlation: r=−0.4, P=0.008; linear regression: R2=0.11, b=−0.32, P=0.03).
The patients with smoking history (36.7%, n=22) had a higher rate of postoperative complications (40.9%, n=9) than did nonsmokers (26.3%, n=10), but the difference was not significant (OR 1.94, 95% CI 0.64–5.91,
The use of anti-TNF medications (adalimumab, infliximab) appeared to extend the time between diagnosis and first surgery (
Several variables were associated with duration of hospitalization by Spearman’s correlation. Patients with lower hemoglobin (r=−0.393,
The patients who needed ostomy creation (n=15) had significantly higher CRP levels at admission (P=0.008, CRP median 120.5 mg/L, Figure 3A) and more previous surgeries (P=0.015) than did patients without ostomy (n=36, CRP median 14.44 mg/L). The necessity of ostomy creation was associated with longer hospitalization (P=0.007). The average time of hospitalization among patients with ostomy was 22±27 days, while it was 11±6 days in patients without ostomy.
According to the results of Spearman’s correlation, higher CRP levels were associated with lower albumin (r=−0.051, P=0.002), lower hemoglobin (r=−0.491, P=0.0001), and lower BMI (r=−0.313, P=0.02). In linear regression analysis, only correlations between CRP and albumin (R2=0.33, b=−0.57, P=0.0005) and between CRP and Hb (R2=0.14, b=−0.38, P=0.005) were significant.(Figure 3B).
No variables were significantly associated with the occurrence of perioperative complications in the bivariate analysis. The analysis of mortality risk factors was not performed as there were no deaths within 30 days after surgery.
Discussion
The analysis of the 60 patients with CD included in this study showed that despite the latest improvements in CD medical management, surgery still remains crucial for a significant number of patients with certain complications. The results of the study confirm the results of many other studies in the literature.
Men and women are affected equally by CD, which was observed in adult epidemiological studies [20,21], retrospective analyses [22,23], and in the present study (men/women=31/29). The mean age at diagnosis (31 years) in the present study was similar to that mentioned in the literature [10,24,25], with the most common Montreal class of A2 (17–40 years).
It is a common knowledge that terminal ileum and ileocecal involvement (Montreal class L3) is the most frequent location of CD. However, the percentage of ileocolic location varied from 23.5% to 75.7% in several studies [10,23,25,26] and 78.9% in the present study. This may be due to the differences in disease duration among patients. A Danish population-based inception cohort study [26] showed changes in disease location (increasing percentage of L3) and behavior progression from B1 Montreal class to either B2 or B3 in the course of the disease. The progression of disease behavior in that study was associated with the risk of surgery, and this may be the reason that, despite a relatively high proportion of non-stricturing, non-penetrating behavior (B1) at diagnosis, most patients requiring surgical treatment are assessed as B2 or B3. Out of the 60 patients undergoing surgery in our hospital, only 11.9% had non-stricturing, non-penetrating behavior, and it was more frequent in patients with the colitis type than in those with the ileitis or ileocolitis type (33.3% and 8.3%, respectively). Similar results were found in a population-based cohort study from Minnesota [27].
The mean time between diagnosis and first surgery among our patients was 4.5 years, with 70% of patients requiring surgery during the first 5 years from diagnosis. These results are comparable to those reported in the literature [22,24]; however, overall risk of surgery within 5 years from diagnosis varies (24% to 77%) in different studies [7,27–30]. This may be due to a disparity in the number of patients with each disease type and improvements in CD management. The highest resection rate (77%) was observed in a population-based cohort of 907 patients diagnosed with primary ileocecal CD between 1955 and 1989 [28], while in other studies (more recent and including all CD locations) it was up to 38%, and the risk of major abdominal surgery decreased between decades. In our present study, the average time from diagnosis to first surgery was 7 years for colitis and 4.1 years for ileocolitis and ileitis.
Intestinal stenosis and fistulae tend to be the main indications for surgery [22,23,29]. In the present study, stricture (19%), intermittent ileus (16%), ileus (9%), and fistulae (36%) were 80% of all indications for surgery, which correspond to those mentioned in the literature. Consequently, intestinal resections (especially ileal resection or right hemicolectomy, which accounted for 60% in the present study) and surgery for perianal fistulae remain the most common procedures [23,27,31].
According to the ECCO evidence-based consensus on the diagnosis and management of CD, smoking, penetrating and stricturing disease behavior, ileal disease, jejunal disease, and young age at diagnosis are risk factors for surgery [32].
In our study, patients with a smoking history had a higher rate of postoperative complications and significantly lower age at first surgery. Some studies do not reveal an association between smoking and complication rate [31], but the impact of tobacco use on disease activity, higher risk of structuring and fistulizing behavior, and early postoperative recurrence is well described [33–36]. Moreover, it has been proven that smoking cessation reduces progression to B2/B3 disease and the risk of surgery [36]. Despite the fact that smoking is strongly forbidden in CD, as many as 21.7% of patients undergoing surgery in our hospital and 12% to 36.9% of patients in several studies were smokers [23,25,27,37].
The analysis showed that patients with penetrating disease had the shortest time from diagnosis to first surgery. Perianal lesions and penetrating disease were the risk factors for a higher number of surgeries, which was consistent with the literature [25]. Some studies have also reported a positive association between penetrating disease type and the complication rate [24,31].
Patients with perianal disease had also lower age at first surgery, with an average of 30.4 years in comparison to 35.7 years among patients without perianal lesions. The difference was similar in a retrospective analysis carried out between 2005 and 2014 in which patients with perianal disease were an average of 34 years of age and those without were 39 [22]. Also, the postoperative recurrence rate in patients with anal lesions and in patients with juvenile-onset disease was significantly higher in a Japanese study analyzing the postoperative course of 168 patients [25]. In our study, an older age at diagnosis was associated with shorter time between diagnosis and first surgery.
There is a considerable debate in the literature as to whether the risk of surgery has decreased in the era of biological therapy. Some studies have reported a decrease in surgical risk [30,38], while others have reported no difference [39]. Anti-TNF treatment was described as a factor which leads to significant reduction of surgical requirements [40]. A Japanese study [25] identified biological therapy as a postoperative recurrence suppressor. The association between preoperative anti-TNF therapy and morbidity after surgery remains unclear in older [41–44] and more recent studies [16–18,45]. According to the recent ECCO guidelines, cessation of anti-TNF therapy prior to surgery is not mandatory [6], but this is still questioned [15]. In our department, 31.7% of patients received biological treatment before surgery. Use of anti-TNF medications (adalimumab, infliximab) appeared to extend the time between diagnosis and first surgery (from 3.5 to 6.4 years,
The occurrence of symptoms, such as abdominal pain, decreased food intake, and diarrhea, is the reason patients with CD are particularly prone to weight loss and malnutrition, which is an important risk factor for postoperative complications [46]. In our study, more than a third of patients were underweight. The disturbed iron metabolism due to chronic inflammation and rectal bleeding lead to anemia [47], which affected up to 51.7% of patients in the present study.
Patients undergoing surgery for CD have fairly high rates of postoperative complications, ranging from 23% to 51.3% in the literature (31.7% in the present study) [10,12,48–51]. Analysis of risk factors for septic complications after surgery for CD shows various complication rates, from 10.6 to 30.7% [51], depending on the number of identified risk factors among patients, namely low albumin level, low hemoglobin level, and elevated CRP. We did not find an association between these factors and complications, which may have been due to the limited number of observations.
According to a recent study by Gklavas et al [11], patients are more likely to have postoperative complications if they had a previous surgery for CD. Our results were the same as those of a Korean retrospective analysis [31]in that there was no association between previous laparotomy and an increased risk of postoperative complications. We did not observe postoperative mortality, but the literature reports mortality rates from 0.6% in elective to 3.6% in emergent surgeries for CD [52].
Limitations of the study are the small number of patients and retrospective design, which resulted in the study containing variables that could not be controlled. However, the study is important for assessing the current role of surgery in CD and to evaluate the results of surgical treatment in our referral hospital.
Conclusions
Despite recent improvements in CD pharmacotherapy, 13% of patients hospitalized for CD required surgical intervention, with the most commonly performed procedure being right hemicolectomy. The mean time between CD diagnosis and first surgery was shorter than 5 years, and most patients had more than 1 surgery for CD. Perianal manifestations, penetrating disease type, ileal/ileocecal involvement, and cigarette smoking may be associated with the risk of earlier surgery or multiple surgeries. The necessity of ostomy creation was most common in patients with higher CRP levels and many previous surgeries. Additional efforts are needed to prevent the occurrence of intestinal stenosis, fistulae, and abscesses, which were the main reasons for surgery. Perioperative complications occurred in 32% of patients. Owing to the high prevalence of anemia, hypoalbuminemia, and underweight among patients with CD, nutritional therapies should be an important point of preoperative management as they may improve postoperative outcomes.
Figures
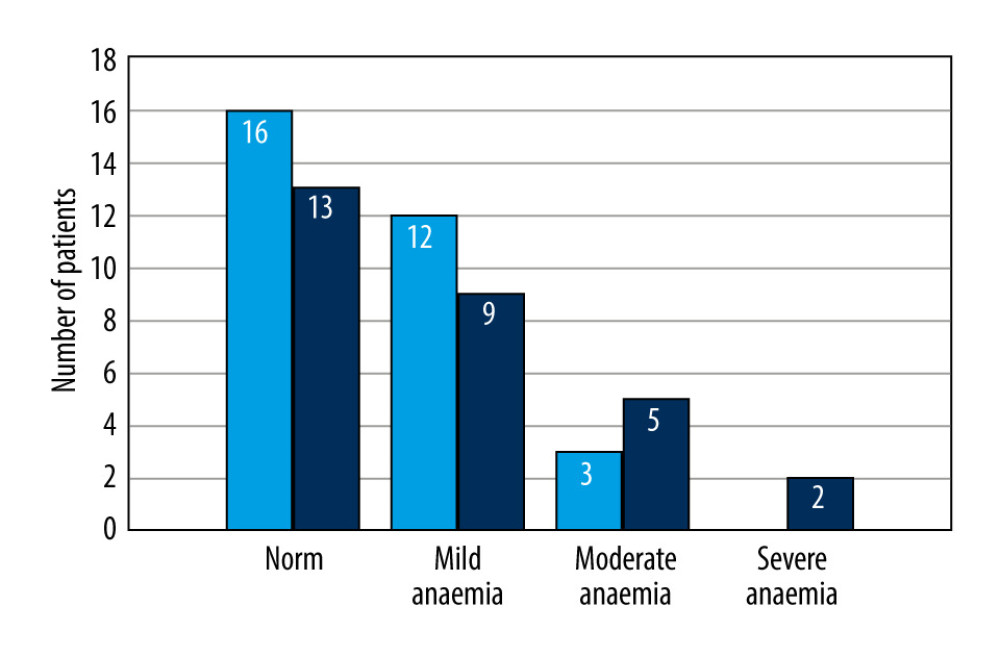 Figure 1. Occurrence of different anemia levels in women (light blue) and men (deep blue) with Chron disease. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 1. Occurrence of different anemia levels in women (light blue) and men (deep blue) with Chron disease. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). 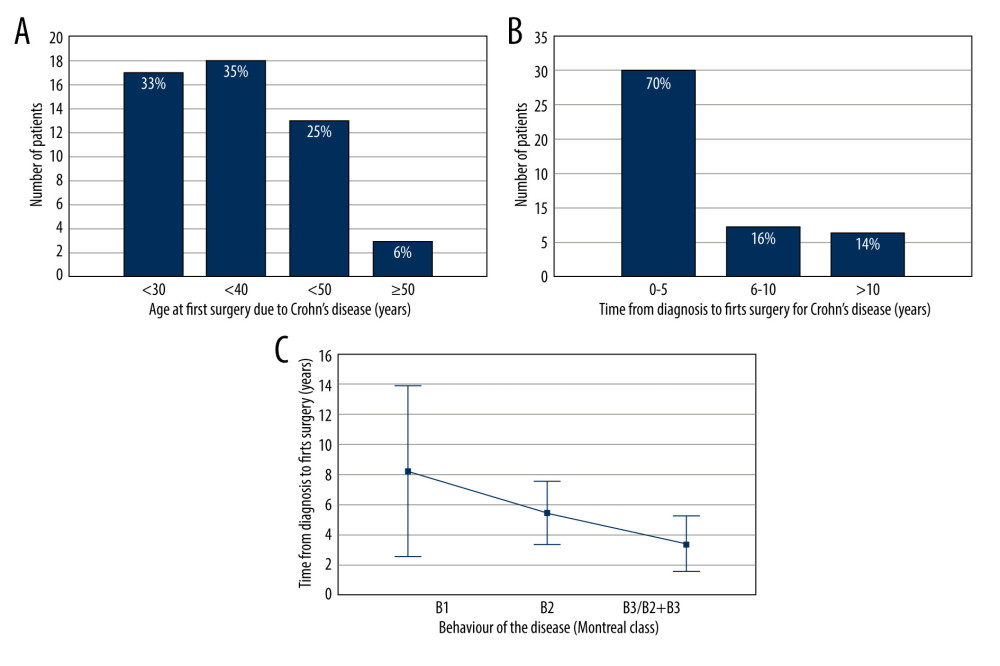 Figure 2. First surgery for Crohn disease: patients’ characteristics. (A) Patient stratification depending on age at first surgery. (B) Patient stratification depending on time between diagnosis and first surgery. (C) Correlation between time from diagnosis to first surgery and disease behavior according to the Montreal classification. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 2. First surgery for Crohn disease: patients’ characteristics. (A) Patient stratification depending on age at first surgery. (B) Patient stratification depending on time between diagnosis and first surgery. (C) Correlation between time from diagnosis to first surgery and disease behavior according to the Montreal classification. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). 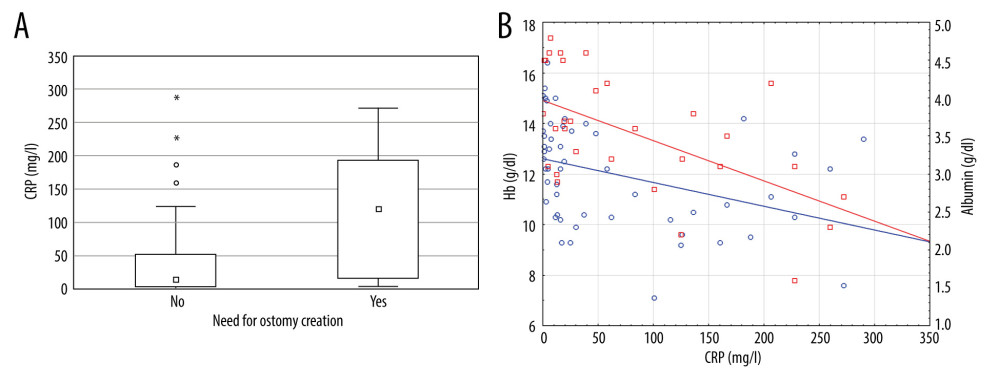 Figure 3. Laboratory parameters in patients with Crohn disease. (A) Need of ostomy creation depending on C-reactive protein (CRP) level. (B) Correlations between CRP and hemoglobin (blue) and albumin (red) levels. (□ median, □ 25–75%, ⌶ non-outlier interval, ° outlier, * extremes). Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 3. Laboratory parameters in patients with Crohn disease. (A) Need of ostomy creation depending on C-reactive protein (CRP) level. (B) Correlations between CRP and hemoglobin (blue) and albumin (red) levels. (□ median, □ 25–75%, ⌶ non-outlier interval, ° outlier, * extremes). Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). References
1. Torres J, Bonovas S, Doherty G, ECCO guidelines on therapeutics in Crohn’s disease: Medical treatment: J Crohns Colitis, 2020; 14(1); 4-22
2. Grass F, Pache B, Martin D, Hahnloser D, Preoperative nutritional conditioning of Crohn’s patients – systematic review of current evidence and practice: Nutrients, 2017; 9(6); 562
3. Lamb CA, Kennedy NA, Raine T, British Society of Gastroenterology consensus guidelines on the management of inflammatory bowel disease in adults [published correction appears in Gut. 2021;70(4): 1]: Gut, 2019; 68(Suppl 3); s1-s106
4. Turner D, Ricciuto A, Lewis A, STRIDE-II: An update on the selecting therapeutic targets in inflammatory bowel disease (STRIDE) initiative of the international organization for the study of IBD (IOIBD): Determining therapeutic goals for treat-to-target strategies in IBD: Gastroenterology, 2021; 160(5); 1570-83
5. Parra RS, Chebli JMF, Amarante HMBS, Quality of life, work productivity impairment and healthcare resources in inflammatory bowel diseases in Brazil: World J Gastroenterol, 2019; 25(38); 5862-82
6. Adamina M, Bonovas S, Raine T, ECCO guidelines on therapeutics in Crohn’s disease: Surgical treatment: J Crohns Colitis, 2020; 14(2); 155-68
7. Tsai L, Ma C, Dulai PS, Contemporary risk of surgery in patients with ulcerative colitis and Crohn’s disease: A Meta-analysis of population-based cohorts: Clin Gastroenterol Hepatol, 2021; 19(10); 2031-45e11
8. Bemelman WA, Allez M, The surgical intervention: Earlier or never?: Best Practice & Research Clinoical Gastroenterology, 2014; 28(3); 497-503
9. Stevens TW, Haasnoot ML, D’Haens GR, Laparoscopic ileocaecal resection versus infliximab for terminal ileitis in Crohn’s disease: Retrospective long-term follow-up of the LIR!C trial: Lancet Gastroenterol Hepatol, 2020; 5(10); 900-7
10. Saad Hossne R, Sassaki LY, Meira JD, Campos LM, Analysis of risk factors and postoperative complications in patients with Crohn’s disease: Arq Gastroenterol, 2018; 55(3); 252-57
11. Gklavas A, Poulaki A, Dellaportas D, Papaconstantinou I, Risk factors for postoperative complications after elective ileocolic resection for Crohn’s disease: A retrospective study: Ann Gastroenterol, 2020; 33(6); 645-55
12. Galata C, Kienle P, Weiss C, Risk factors for early postoperative complications in patients with Crohn’s disease after colorectal surgery other than ileocecal resection or right hemicolectomy: Int J Colorectal Dis, 2019; 34; 293-300
13. Moghadamyeghaneh Z, Carmichael JC, Mills SD, Outcomes of bowel resection in patients with Crohn’s disease: Am Surg, 2015; 81(10); 1021-27
14. Kühn F, Nixdorf M, Schwandner F, Klar ERisk factors for early surgery and surgical complications in Crohn’s disease: Zentralbl Chir, 2018; 143(6); 596-602 [in German]
15. Soop M, Hancock L, Davies J, Anti-TNF therapy before intestinal surgery for Crohn’s disease and the risks of postoperative complications: J Crohns Colitis, 2021; 15(10); 1777
16. Lin YS, Cheng SW, Wang YH, Systematic review with meta-analysis: Risk of post-operative complications associated with pre-operative exposure to anti-tumour necrosis factor agents for Crohn’s disease: Aliment Pharmacol Ther, 2019; 49(8); 966-77
17. Waterland P, Athanasiou T, Patel H, Post-operative abdominal complications in Crohn’s disease in the biological era: Systematic review and meta-analysis: World J Gastrointest Surg, 2016; 8(3); 274-83
18. Xu YY, Yang LS, An P, Meta-analysis: the influence of reoperative infliximab use on postoperative complications of Crohn’s disease: Inflamm Bowel Dis, 2019; 25; 261-69
19. Satsangi J, Silverberg MS, Vermeire S, Colombel JF, The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications: Gut, 2006; 55(6); 749-53
20. Kappelman MD, Rifas-Shiman SL, Kleinman K, The prevalence and geographic distribution of Crohn’s Disease and ulcerative colitis in the United States: Clin Gastroenterol Hepatol, 2007; 5(12); 1424-29
21. Herrinton LJ, Liu L, Lafata JE, Estimation of the period prevalence of inflammatory bowel disease among nine health plans using computerized diagnoses and outpatient pharmacy dispensings: Inflamm Bowel Dis, 2007; 13(4); 451-61
22. Kuehn F, Nixdorf M, Klar E, The role of surgery in Crohn’s disease: Single center experience from 2005–2014: Gastroenterology, 2015; 148(4); 1167-68
23. Hefaiedh R, Sabbeh M, Miloudi N, Surgical treatment of Crohn’s disease: Indications, results and predictive factors of recurrence and morbidity: Tunis Med, 2015; 93(6); 356-60
24. Hong Z, Ren J, Li Y, Delayed diagnosis is associated with early and emergency need for first Crohn’s disease-related intestinal surgery: Med Sci Monit, 2017; 23; 4841-46
25. Kusaka J, Shiga H, Kuroha M, Risk factors associated with postoperative recurrence and repeat surgery in Japanese patients with Crohn’s disease: Int J Colorectal Dis, 2017; 32(10); 1407-13
26. Lo B, Vester-Andersen MK, Vind I, Changes in disease behavior and location in patients with crohn’s disease after seven years of follow-up: A Danish population-based inception cohort: J Crohns Colitis, 2018; 12(3); 265-72
27. Peyrin-Biroulet L, Harmsen WS, Tremaine WJ, Surgery in a population-based cohort of Crohn’s disease from Olmsted County, Minnesota (1970–2004): Am J Gastroenterol, 2012; 107(11); 1693-701
28. Bernell O, Lapidus A, Hellers G, Risk factors for surgery and recurrence in 907 patients with primary ileocaecal Crohn’s disease: Br J Surg, 2000; 87(12); 1697-701
29. Toh JWT, Wang N, Young CJ, Major abdominal and perianal surgery in Crohn’s disease: Long-term follow-up of Australian patients with Crohn’s disease: Dis Colon Rectum, 2018; 61(1); 67-76
30. Frolkis AD, Dykeman J, Negrón ME, Risk of surgery for inflammatory bowel diseases has decreased over time: A systematic review and meta-analysis of population-based studies: Gastroenterology, 2013; 145(5); 996-1006
31. Yang SS, Yu CS, Yoon YS, Risk factors for complications after bowel surgery in Korean patients with Crohn’s disease: J Korean Surg Soc, 2012; 83(3); 141-48
32. Gionchetti P, Dignass A, Danese S: J Crohns Colitis, 2017; 11(2); 135-49
33. To N, Gracie DJ, Ford AC, Systematic review with meta-analysis: The adverse effects of tobacco smoking on the natural history of Crohn’s disease: Aliment Pharmacol Ther, 2016; 43(5); 549-61
34. Nunes T, Etchevers MJ, García-Sánchez V, Impact of smoking cessation on the clinical course of Crohn’s disease under current therapeutic algorithms: A multicenter prospective study: Am J Gastroenterol, 2016; 111(3); 411-19
35. Lakatos PL, Vegh Z, Lovasz BD, Is current smoking still an important environmental factor in inflammatory bowel diseases? Results from a population-based incident cohort: Inflamm Bowel Dis, 2013; 19(5); 1010-17
36. Lawrance IC, Murray K, Batman B, Crohn’s disease and smoking: Is it ever too late to quit?: J Crohns Colitis, 2013; 7(12); e665-71
37. Mosli M, Sabbahi H, Alyousef H, Risk stratification of patients with Crohn’s disease: A retrospective analysis of clinical decision making and its impact on long-term outcome: Dig Dis, 2018; 36(1); 49-55
38. Rungoe C, Langholz E, Andersson M, Changes in medical treatment and surgery rates in inflammatory bowel disease: A nationwide cohort study 1979–2011: Gut, 2014; 63(10); 1607-16
39. Slattery E, Keegan D, Hyland J, Surgery, Crohn’s disease, and the biological era: Has there been an impact?: J Clin Gastroenterol, 2011; 45(8); 691-93
40. Liu W, Zhou W, Xiang J, Lémann index at diagnosis predicts the risk of early surgery in Crohn’s disease: Dis Colon Rectum, 2018; 61(2); 207-13
41. Nørgård BM, Nielsen J, Qvist N, Pre-operative use of anti-TNF-α agents and the risk of post-operative complications in patients with Crohn’s disease – a nationwide cohort study: Aliment Pharmacol Ther, 2013; 37(2); 214-24
42. Syed A, Cross RK, Flasar MH, Anti-tumor necrosis factor therapy is associated with infections after abdominal surgery in Crohn’s disease patients: Am J Gastroenterol, 2013; 108(4); 583-93
43. Billioud V, Ford AC, Tedesco ED, Preoperative use of anti-TNF therapy and postoperative complications in inflammatory bowel diseases: A meta-analysis: J Crohns Colitis, 2013; 7(11); 853-67
44. Rizzo G, Armuzzi A, Pugliese D, Anti-TNF-alpha therapies do not increase early postoperative complications in patients with inflammatory bowel disease. An Italian single-center experience: Int J Colorectal Dis, 2011; 26(11); 1435-44
45. Brouquet A, Maggiori L, Zerbib P, Anti-TNF therapy is associated with an increased risk of postoperative morbidity after surgery for ileocolonic Crohn disease: Results of a prospective nationwide cohort: Ann Surg, 2018; 267(2); 221-28
46. Ladd MR, Garcia AV, Leeds IL, Malnutrition increases the risk of 30-day complications after surgery in pediatric patients with Crohn disease: J Pediatr Surg, 2018; 53(11); 2336-45
47. Baumgart DC, Sandborn WJ, Crohn’s disease: Lancet, 2012; 380(9853); 1590-605
48. Gutiérrez A, Rivero M, Martín-Arranz MD, Perioperative management and early complications after intestinal resection with ileocolonic anastomosis in Crohn’s disease: Analysis from the PRACTICROHN study: Gastroenterol Rep (Oxf), 2019; 7(3); 168-75
49. 2015 European Society of Coloproctology (ESCP) collaborating group, Patients with Crohn’s disease have longer post-operative in-hospital stay than patients with colon cancer but no difference in complications’ rate: World J Gastrointest Surg, 2019; 11(5); 261-70
50. Dreznik Y, Horesh N, Gutman M, Preoperative nutritional optimization for Crohn’s disease patients can improve surgical outcome: Dig Surg, 2018; 35; 442-47
51. Ghoneima AS, Flashman K, Dawe V, High risk of septic complications following surgery for Crohn’s disease in patients with preoperative anaemia, hypoalbuminemia and high CRP: Int J Colorectal Dis, 2019; 34; 2185-88
52. Singh S, Al-Darmaki A, Frolkis AD, postoperative mortality among patients with inflammatory bowel diseases: A systematic review and meta-analysis of population-based studies: Gastroenterology, 2015; 149(4); 928-37
Figures
 Figure 1. Occurrence of different anemia levels in women (light blue) and men (deep blue) with Chron disease. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 1. Occurrence of different anemia levels in women (light blue) and men (deep blue) with Chron disease. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). Figure 2. First surgery for Crohn disease: patients’ characteristics. (A) Patient stratification depending on age at first surgery. (B) Patient stratification depending on time between diagnosis and first surgery. (C) Correlation between time from diagnosis to first surgery and disease behavior according to the Montreal classification. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 2. First surgery for Crohn disease: patients’ characteristics. (A) Patient stratification depending on age at first surgery. (B) Patient stratification depending on time between diagnosis and first surgery. (C) Correlation between time from diagnosis to first surgery and disease behavior according to the Montreal classification. Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). Figure 3. Laboratory parameters in patients with Crohn disease. (A) Need of ostomy creation depending on C-reactive protein (CRP) level. (B) Correlations between CRP and hemoglobin (blue) and albumin (red) levels. (□ median, □ 25–75%, ⌶ non-outlier interval, ° outlier, * extremes). Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc).
Figure 3. Laboratory parameters in patients with Crohn disease. (A) Need of ostomy creation depending on C-reactive protein (CRP) level. (B) Correlations between CRP and hemoglobin (blue) and albumin (red) levels. (□ median, □ 25–75%, ⌶ non-outlier interval, ° outlier, * extremes). Figure were created using the program Statistica (version 13.3, 1984–2017 TIBCO Software Inc). Tables
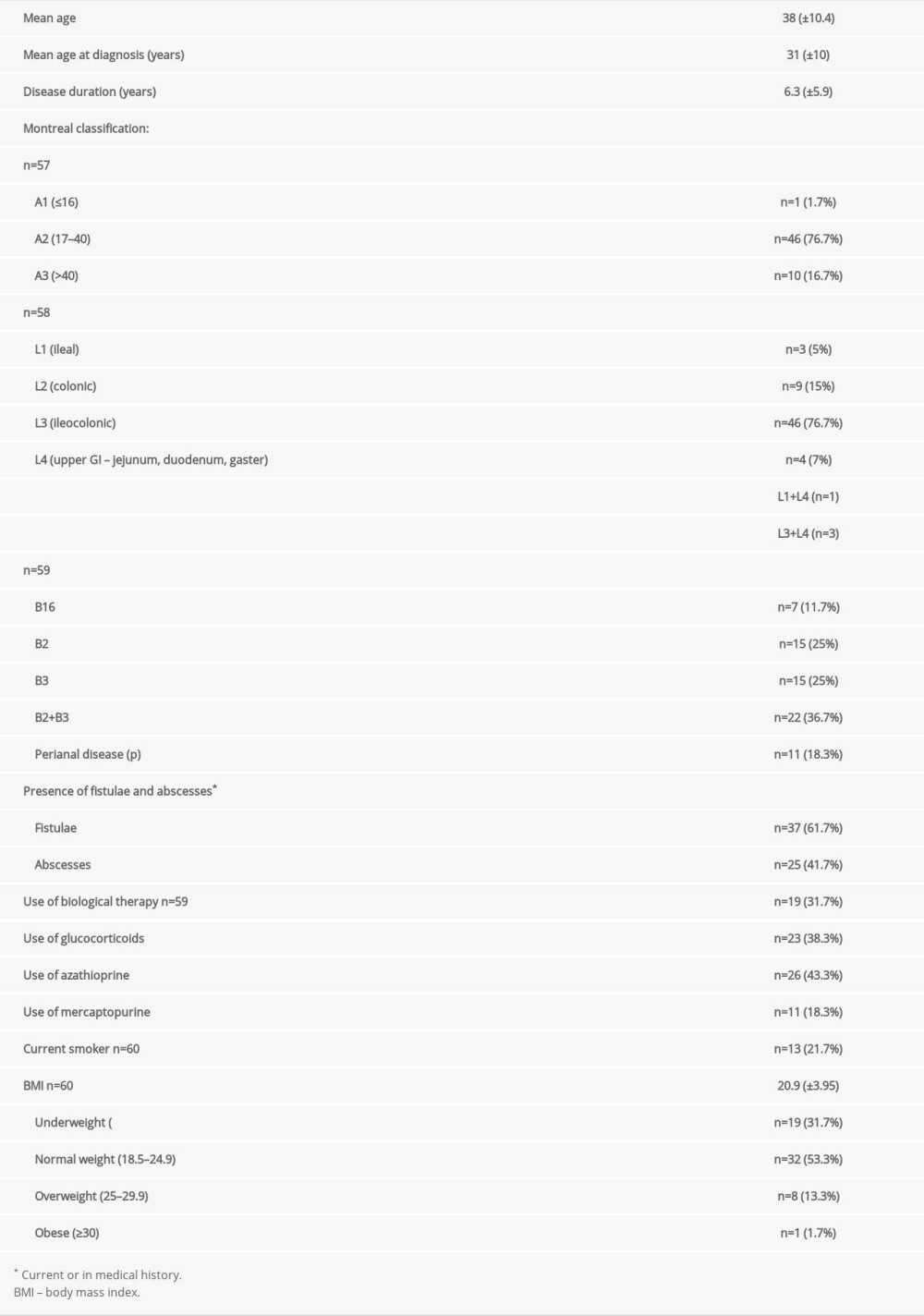 Table 1. The general patient clinical characteristics.
Table 1. The general patient clinical characteristics.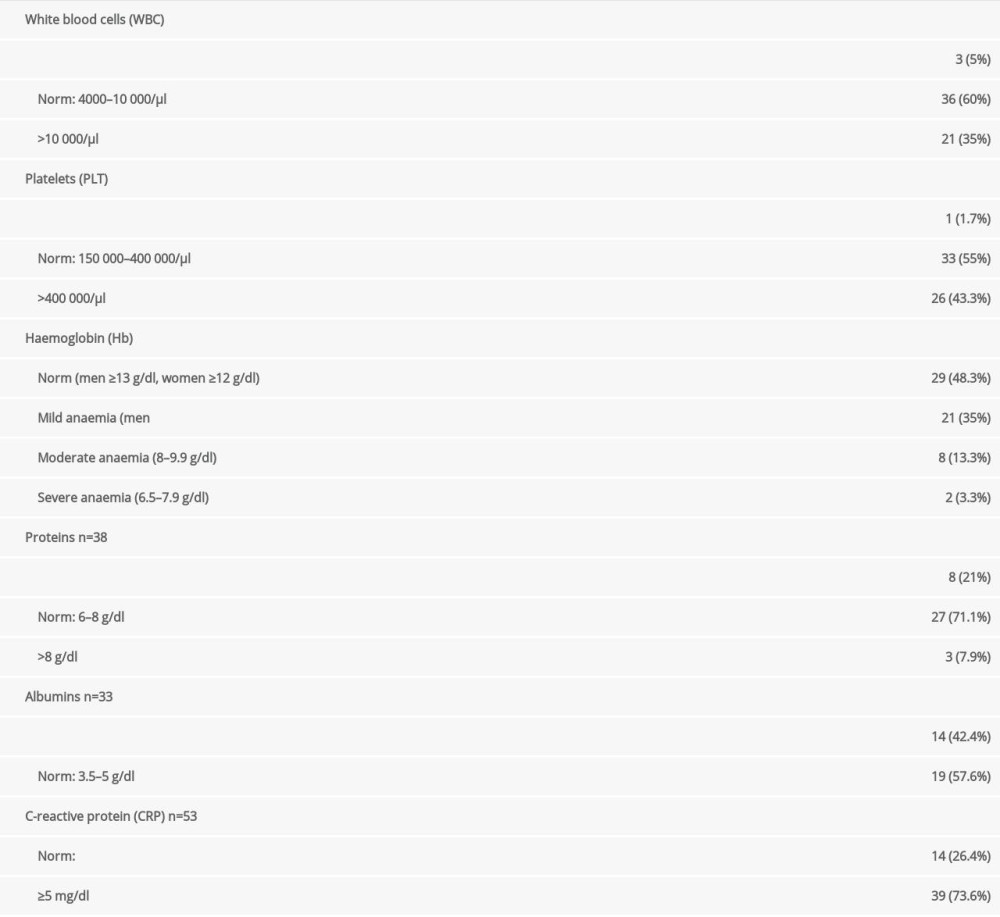 Table 2. Laboratory tests results.
Table 2. Laboratory tests results.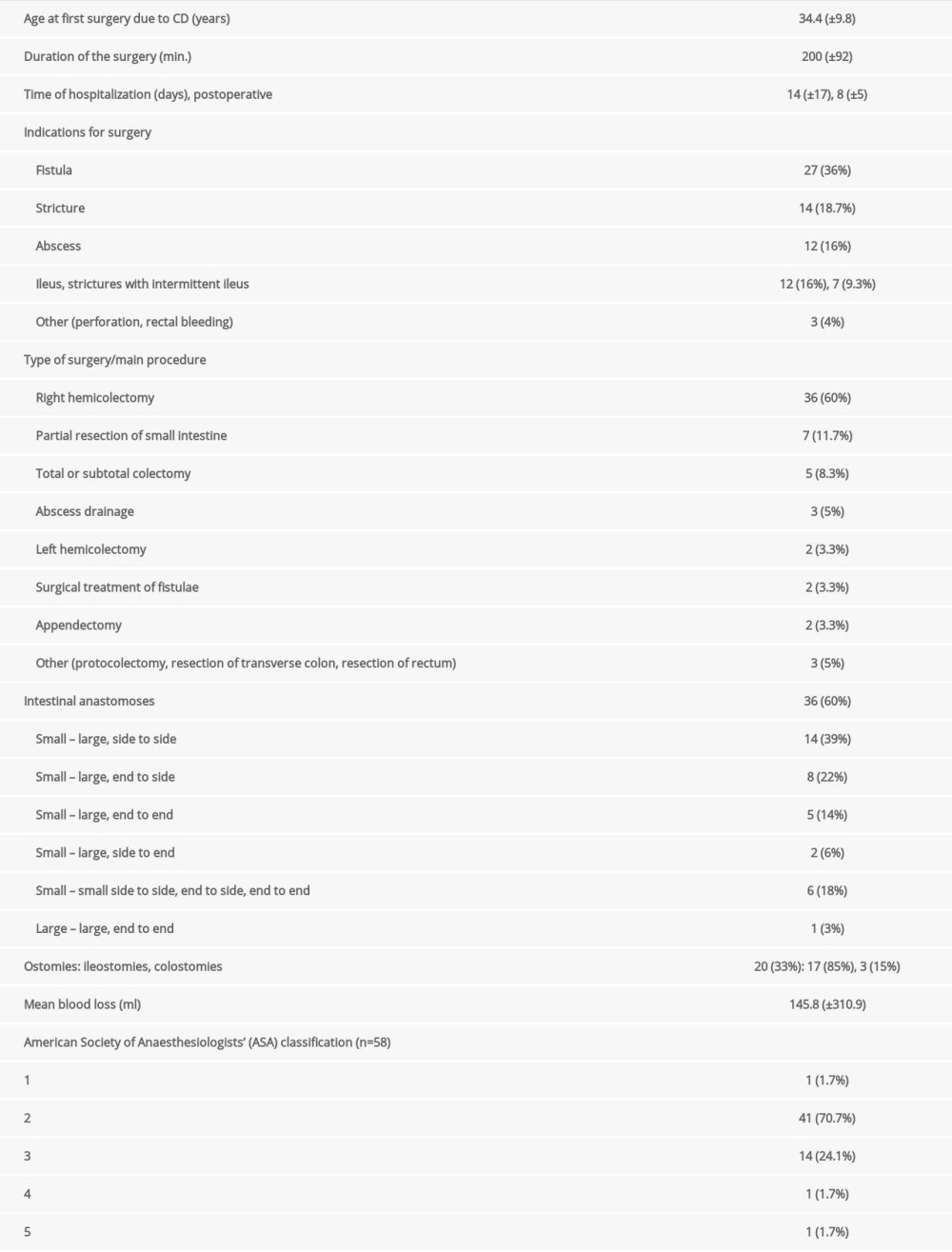 Table 3. Surgical characteristics of the patients.
Table 3. Surgical characteristics of the patients.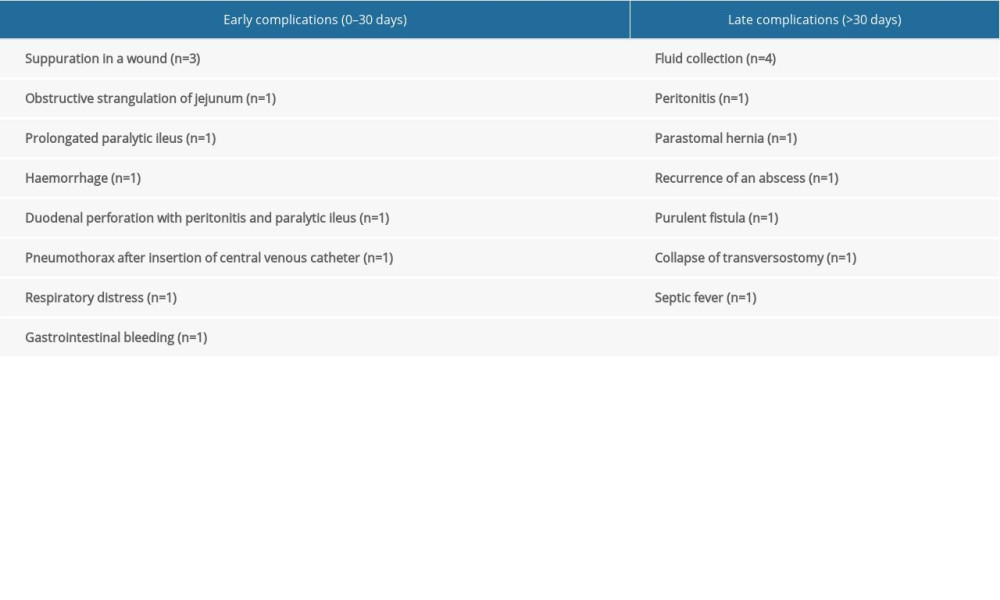 Table 4. Surgical complications.
Table 4. Surgical complications. Table 1. The general patient clinical characteristics.
Table 1. The general patient clinical characteristics. Table 2. Laboratory tests results.
Table 2. Laboratory tests results. Table 3. Surgical characteristics of the patients.
Table 3. Surgical characteristics of the patients. Table 4. Surgical complications.
Table 4. Surgical complications. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








