06 June 2022: Animal Study
Artificial Dermal Scaffold Loaded with Platelet-Rich Plasma Promotes Wound Healing in Pigs by Favoring Angiogenesis
Zhi-Hao Li12ABEFG, Guo-Feng Wu3AEFG, Hao-Qiang Song4BCDF, Kui Huang5BCD, Bo Wu6BCD, Xiao-Long Xu2BCD, Li-Xin Zhu1AEFG*DOI: 10.12659/MSM.936186
Med Sci Monit 2022; 28:e936186
Abstract
BACKGROUND: The development of artificial dermis provides a new therapeutic method for full-thickness skin defects. However, the slow regeneration of blood vessels in the wound site still cannot be solved perfectly. In our study, we combined platelet-rich plasma (PRP) with Lando® artificial dermal scaffold to promote vascular regeneration and wound healing in pigs.
MATERIAL AND METHODS: First, PRP was compounded with the artificial dermal scaffold. Then, this material was co-cultured with human vascular endothelial cells (HUVECs) and the growth and proliferation of HUVECs were assessed. Bama miniature pigs wound models were fabricated, the materials were transplanted into the skin defect, and wound healing and blood vessel regeneration were assessed by HE staining and CD31 immunohistochemistry.
RESULTS: Scanning electron microscopy (SEM) showed that PRP formed round particles on the surface of the artificial dermis material. Cell co-culture experiments showed that the PRP composite artificial dermal scaffold can promote the growth and proliferation of HUVECs. CCK8 experiments demonstrated that the number of cells in the PRP composites group on days 2, 3, 4, and 5 was higher than that in the material alone group (P<0.01). The results of animal experiments showed that PRP composite artificial dermal material can promote wound healing. Histological staining and immunohistochemical staining indicated that the PRP composites group promoted epithelial tissue thickening and blood vessel regeneration in wounds (P<0.001).
CONCLUSIONS: Our experimental results showed that the artificial dermal scaffold loaded with platelet-rich plasma can promote the revascularization of wounds and accelerated wound healing.
Keywords: Pacemaker, Artificial, platelet-rich plasma, Skin, Artificial, Wound Healing, Animals, endothelial cells, Skin, Swine
Background
Due to the lack of subcutaneous soft tissue, tendon- and/or bone-exposure wounds of the head and extremities are generally difficult to heal, and often require multiple surgeries, which greatly increase the clinical burden [1]. Traditionally, tendon- and/or bone-exposure wounds are usually covered by flap reconstruction. Although some patients can achieve satisfactory clinical results when using flap reconstruction, there are still some uncertainties and drawbacks regarding flap viability, flap bulkiness, and morbidity at the donor site [2]. In recent years, artificial dermal substitutes have been proven effective in the reconstruction of complex soft tissue wounds, even in the presence of exposed tendons or bones [3,4].
Generally, artificial dermis substitutes have a double-layer structure. The upper layer plays a role similar to the skin epidermis and has good waterproof and antibacterial effects, and the bottom layer plays the role of dermis scaffold template by promoting local blood vessel formation and dermal regeneration [5]. Developed by Shenzhen Landu biomaterials Co., Ltd, Lando®, artificial dermis is an acellular dermal substitute that was initially approved by the National Medical Products Administration in 2017 for the dermal repair and reconstruction of non-infected wounds [6]. Clinical results confirmed that the skin graft survival rate and postoperative scar evaluation of this product are better than in the imported control group [7]. However, the slow vascularization rate and the long interval between the first implantation of the artificial dermis and autogenous skin grafting are considered the main drawbacks of such scaffolds used in tendon- and bone-exposure wounds due to the lack of subcutaneous fat, muscle tissue, and vascular tissue [8]. Several efforts – including modification of structural and physicochemical properties of dermal scaffolds, biological scaffold activation with growth factor-releasing systems or gene vectors, and generation of vascularized skin substitutes by seeding scaffolds with vessel-forming cells – have been made to induce vascular growth in scaffolds [9], but thus far there is no simple and established technology for inducing vascular growth of dermal scaffold.
Platelet-rich plasma (PRP) is a high-concentration platelet-oriented plasma obtained from animal or human whole blood via centrifugation [10], containing various growth factors (GFs) such as platelet-derived growth factor (PDGF), transforming growth factor (TGF-β), IGF (insulin-like growth factor), endothelial growth factor (EGF), and vascular endothelial growth factor (VEGF) [11–13]. These GFs derived from PRP can contribute to tissue regeneration and wound healing by promoting cell attachment, migration, differentiation, and extracellular matrix synthesis [14]. Therefore, PRP has been used as a supplement for releasing growth factors in various tissue engineering applications and has been shown to have unique organizational restructuring advantages [15,16].
Therefore, to overcome the difficulty of vascular regeneration in the process of wound repair with the artificial dermal scaffold, we combined PRP with an artificial dermal scaffold to assess its role in promoting vascular regeneration and wound healing in vivo and in vitro.
Material and Methods
ISOLATION OF PRP:
All procedures were approved by the Laboratory Animals Use Committee of Mingzhu Laboratory Animal Technology Co., Ltd. Songshan Lake, Dongguan, China, and all ethical principles related to the care and use of laboratory animals were complied with. The PRP was isolated according to the literature [17]. Blood sample were obtained from Bama miniature pigs. Briefly, an aliquot of 50 mL of peripheral blood and the anticoagulant sodium citrate solution (K2 EDTA, spray-dried, 10.8 mg, BD Vacutainer®) was centrifuged at 300 g for 10 min to remove erythrocytes and leukocytes, then we collected the upper layer and the middle layer. The bottom plasma layer (approximate 1 mL) was collected as PRP after centrifuging again for 15 min at 1200 g.
PREPARATION OF AD/PRP COMPOSITE SCAFFOLD:
The artificial dermal scaffold (AD scaffold) is a cell-free dermal substitute developed by Shenzhen Lando Biomaterials Co., Ltd. It has a double-layer structure in which the upper layer is medical silicone rubber film, and the lower layer is a bovine tendon collagen-chondroitin sulfate scaffold [18]. The manufacturing process of the AD scaffold was as described in the literature [19]: The chondroitin sulfate solution was added to the collagen solution, blended, and we obtained a collagen-chondroitin sulfate composite solution, which was then injected into the mold, freeze-dried, and finally heat dehydrated for cross-linking to obtain a collagen composite layer. The collagen composite layer was bonded to the silicone rubber film and chemically cross-linked, and the excess cross-linking agent was removed by washing with water and packaged to obtain an artificial dermal scaffold. Then, an AD scaffold loaded with PRP (AD/PRP composite scaffold, for short) was created by mixing the artificial dermis and PRP solution of 20 mL for 2 h.
CELL CULTURE:
HUVECs were purchased from Guangzhou Yanshi Technology Co., Ltd. (Guangzhou, China), and grown in α-MEM supplemented with 10% fetal bovine serum (FBS, Gibco, Grand Island, NY) and 1% penicillin-streptomycin solution (Gibco) at 37°C in a humidified 5% CO2/95% air atmosphere. Cells of almost confluent cultures were detached with 0.25% trypsin/EDTA (Gibco). Trypsin was neutralized with 10% FBS containing α-MEM. Cells were resuspended in 10% FBS containing α-MEM after centrifugation at 1000 rpm for 3 min.
CELL ADHESION AND PROLIFERATION:
HUVECs in logarithmic growth phase were used for further study. The cells were digested by trypsin and separately seeded on the AD scaffold and AD/PRP composite scaffold in a 96-well plate with a density of 104 cells/mL. On day 7 of culture, the samples were divided into 2 parts for further study. One part was fixed with 4% paraformaldehyde at room temperature for 1 h. After the fixative samples were washed twice with PBS every 10 min, the cells were sequentially penetrated with 0.1% Triton X-100 (Coolaber, China) for 10 min and blocked with 1% bovine serum albumin (Sigma-Aldrich, America) for 30 min. Subsequently, 5 μg/mL phalloidin-rhodamine (Invitrogen, America) and 4′, 6-diamidino-2-phenylindole (DAPI, Sigma-Aldrich) solution were utilized to stain the cytoskeletons and the cell nuclei, respectively, in a dark room. Finally, a laser scanning confocal microscope (LSCM, Leica, SP8) was used to obtain images of cell adhesion and proliferation at 405/552 nm. For the other part of the samples, gradient dehydration was performed with 50%, 70%, 90%, and 100% ethanol. After freeze-drying, the samples were coated with a thin layer of gold and observed using a scanning electron microscope (SEM) (ZEISS Merlin) at 5 kV with a Schottky Thermal Field Emission (TFE) filament.
CELL COUNTING KIT-8 (CCK8) ASSAY:
The cell proliferation activity was measured by CCK8 assay. Cells were seeded in 96-well plates with a density of 2×103 per well. After the cells had adhered, on days 1, 2, 3, 4, and 5, 10 μL of CCK8 was added to each well for incubation at 37°C for 2 h. The absorbance of each well at 490 nm was recorded using a microplate reader (BioRad, Hercules, CA, USA).
IN VIVO ANIMAL MODEL STUDIES:
All procedures were approved by the Laboratory Animals Use Committee of Mingzhu Laboratory Animal Technology Co., Ltd. Songshan Lake, Dongguan, China, and all ethical principles related to the care and use of laboratory animals were complied with. Three Bama miniature pigs were used. The treatment group was treated with the AD/PRP composite scaffold, and the control group was treated with the AD scaffold alone.
Experimental animals were anesthetized by intravenous injection of propofol to induce anesthesia and tracheal intubation with isoflurane for maintenance. Then, animals were positioned prone on the operating table, with their heads immobilized and shaved. Two round skull exposed-bone wounds with a diameter of 2 cm and periosteum preserved were created above the orbit with a sharp knife under aseptic conditions, and the edges of the 2 wounds were 2 cm apart. We transplanted 2 different scaffolds on the same Bama miniature pig to exclude the influence of the individual. The scaffolds were punctured with a sharp knife to avoid a possible hematoma, trimmed to the same size and shape as the wounds, and secured in position using 3-0 Ethicon® sutures along the borders of the wound. Vaseline gauze dressing was placed over the wound before wrapping in sterile gauze. After these procedures, pigs were placed in individual cages inside the institutional animal facility.
Ten days postoperatively, these animals were anesthetized and immobilized in the same way as above. The packaging dressing was removed, the scaffold layer was ruddy, and the protective silicone layer was loosened, which indicated neo-dermis formation. Then, the silicone layer was peeled off without difficulty. The neo-dermis was covered with a perforated and appropriate autologous split-thickness skin graft, which was harvested from the top of the animal’s head.
On day 30, tissue from the wound site was taken for histopathological analysis. Each sample was completely submerged in 4% paraformaldehyde solution, followed by subsequent storage at 4°C in a refrigerator.
HISTOLOGY ANALYSIS:
Paraffin-embedded samples cut into slices with 5-μm thickness in cross-section were utilized for histological staining. After dewaxing and rehydration, hematoxylin and eosin (H&E) staining was conducted to histologically observe the wound healing. To further evaluate angiogenesis in wound tissue, immunohistochemistry of CD31 was employed.
STATISTICAL ANALYSIS:
SPSS 26.0 software was used for statistical analysis, and the data were recorded as the mean±SD. An independent-sample
Results
CELL ADHESION AND PROLIFERATION IN AD/PRP COMPOSITE SCAFFOLD:
To understand the morphological characteristics and the adhesion and proliferation of HUVECs on the AD scaffold and AD/PRP composite scaffold, the samples were observed by LSCM and SEM. Figure 1A and 1C are the surface morphology of AD scaffold and AD/PRP composite scaffold inoculated with HUVECs under SEM, respectively. The red arrow indicates HUVECs, which are polygonal and adhere and grow well on the surfaces of both scaffolds. In Figure 1C, black arrows display circular granules of different sizes. Figure 1B and 1D show the fluorescence staining results of the AD scaffold and AD/PRP composite scaffold inoculated with HUVECs. The results demonstrate that there are more HUVECs on the surface of the AD/PRP composite scaffold.
EFFECT OF AD/PRP COMPOSITE SCAFFOLD ON HUVECS PROLIFERATION:
We quantitatively compared the ability of the AD scaffold and AD/PRP composite scaffold to promote HUVECs proliferation. Figure 2 shows the results of the CCK8 experiment. On the first day, there was no statistically significant difference between the AD scaffold and AD/PRP scaffold in promoting cell proliferation. On the second day, the effect of the AD/PRP scaffold on promoting cell proliferation was significantly higher than that of the AD scaffold, and the difference was statistically significant (P<0.01). On the third, fourth, and fifth day, the AD/PRP scaffold promoted the proliferation of cells more than that of AD scaffolds. The difference was statistically significant and P was less than 0.001.
AD/PRP COMPOSITE SCAFFOLD ACCELERATES WOUND HEALING IN PIGS:
Skull bone-exposure wounds of Bama miniature pigs were created to evaluate the effect of the composite scaffold. As shown in Figure 3A, on day 0, the wound diameter was 2 cm, with the AD/PRP composite scaffold group on the left side and the AD scaffold group on the right side. On day 10, the wound area on the left side was reduced compared to the wound area on the right side. On day 30, the left wound was significantly smaller than the right wound, with only a small amount of black blood scab. Figure 3B demonstrates the quantitative statistical results of wound healing rate. On the 10th day, the wound healing rate of the treatment group was 67±5%, which was significantly higher than 48±10% of the control group, and the difference was statistically significant. On the 30th day, the wound healing rate of the treatment group was much higher than that of the control group, and the difference was statistically significant, with a P of less than 0.001.
AD/PRP COMPOSITE SCAFFOLD PROMOTES EPITHELIAL TISSUE THICKENING AND VASCULAR REGENERATION:
On the 30th day, most wounds had healed. At this time, granulation tissue underwent remodeling, and epithelial tissue regenerated at the wound site [20]. We assessed the regeneration of epithelial tissue and blood vessels in the wound site by HE staining and CD31 immunohistochemical staining. As shown in Figure 4A, compared with the control group, the epithelial tissue in the treatment group was significantly thickened. Quantitative statistics displayed that the average epithelial thickness in the treatment group was 250 μm, which was higher than the average of 100 μm in the control group, and the difference was statistically significant, with P less than 0.001 (Figure 4C).
Vascular endothelial cells were marked by CD31 to confirm the degree of tissue neovascularization [21]. In Figure 4B, the results of immunohistochemical staining of CD31 in the treatment group and control group showed that the number of positive cells in the treatment group was significantly higher than that in the control group. Figure 4D shows that the vascular regeneration ability of the treatment group was much higher than that of the control group, and the difference was statistically significant.
Discussion
The treatment of complex wounds is always a difficult challenge in clinical practice. To the best of our knowledge, our experiments are the first in vivo validation of the efficacy of platelet-rich plasma-bound artificial dermal scaffold in promoting wound healing in pigs, and these data are important because the skin characteristics of pigs closely match those of humans, providing an experimental basis for further clinical applications.
In this study, we used the Lando® artificial dermal scaffold, previously reported by our research group, as a core scaffold [22]. This material has a double-layer structure. Its upper layer is a medical silicone rubber film acting as a semi-permeable membrane, whose water vapor transmission rate is similar to the normal skin of the human body, better controlling the loss of water from the wound and providing mechanical support for the product suture. The lower layer is a cross-linked collagen-chondroitin sulfate dermal scaffold, with a pore size of about 50–200 μm and porosity of >90%. Studies have shown that porosity is conducive to increased angiogenesis, which in turn promotes tissue regeneration [23].
It was found through in vitro cell culture that this scaffold material was biocompatible and the cells grew and proliferated in the material [19]. This may be related to the cross-linked collagen-chondroitin sulfate of the underlying membrane, in which the carboxyl or phosphate group in chondroitin sulfate interacts with the ɛ-amino group of lysine or the guanidine group of arginine in collagen to improve the film formation process, and to adjust the dermal scaffold biocompatibility, degradation rate, mechanical strength, and the porous structure. Diaz-Gomez et al [24] found that PRP increased the biocompatibility and adhesion of the material. Our results also showed that the cells significantly proliferated in the PRP group, which may be related to PRP proliferation [25].
PRP mainly contains concentrated platelets and various growth factors [26]. Shaolong Zhou et al [27] found that PRP can accelerate wound healing by promoting vascular regeneration. However, for clinically complex wound types, such as those with exposed bone and tendon, it is difficult to adequately meet the needs of wound repair using PRP. Bonding with scaffold materials with certain mechanical strength is required. The artificial dermal scaffold has good biocompatibility [28], suitable mechanical strength (can resist traction and shear forces) [29], and has a porous structure conducive to the progress of cell metabolism [30]. However, the current clinically used artificial dermal materials all have the disadvantage of insufficient vascular regeneration [31]. In theory, PRP combined with artificial dermal scaffold have the mechanical properties of materials needed for complex wound repair and biologically promote vascular regeneration.
The cell experiments indicated that PRP combined with artificial dermal scaffold could promote the proliferation of vascular endothelial cells. It has now been proved that VEGF is abundant in PRP [32], and VEGF has the effect of promoting the proliferation of vascular endothelial cells. The observation of the wound demonstrated that the wound healing rate of the PRP group was significantly higher than that of the control group. Further, HE staining results indicated that the PRP group had a stronger regeneration ability than the control group. Immunohistochemistry demonstrated that PRP combined with artificial dermal scaffold could promote the increase of CD31-positive expression in the wound site. In immunohistochemistry, CD31 is mainly used to evaluate tissue angiogenesis [33]. PRP contains a large amount of cell growth factors and relevant functional proteins. Among them, thrombin can recruit vascular endothelial cells in surrounding tissues, stimulate fibroblast proliferation, and promote new capillary formation [34]. In addition, VEGF is also contained in PRP. VEGF can induce the proliferation and migration of endothelial cells and promote the formation of new blood vessels [35]. Therefore, our experimental results suggest that PRP combined with artificial dermal materials has the effect of promoting vascular regeneration associated with its promotion of vascular endothelial cell proliferation. It has been demonstrated that PRP can increase the cell adhesiveness of scaffold materials [24]. In addition, PRP has a role in recruiting endothelial progenitor cells [36]. Therefore, the effect of PRP combined with an artificial dermal scaffold to promote vascular regeneration may also be related to its increased adhesion and aggregation of endothelial progenitor cells. The main reason for non-healing in diabetes is insufficient vascular regeneration [37], and PRP combined with artificial dermal scaffolds can promote the regeneration of blood vessels. Therefore, we believe that PRP combined with artificial dermal scaffold can promote wound healing in diabetes.
The results suggested that PRP increased the vascularization ability of the artificial dermal scaffold material and thus promoted wound healing. This study only focused on PRP combined with an artificial dermal scaffold to promote vascular regeneration. However, wound healing is the result of multiple biological interactions [38]. The present experiment did not detect collagen regeneration, which needs to be further investigated in future experiments.
Conclusions
In this study, an artificial dermal/PRP scaffold was successfully prepared for wound healing. Artificial dermal scaffold loaded with platelet-rich plasma promoted the revascularization of wounds and accelerated wound healing.
Figures
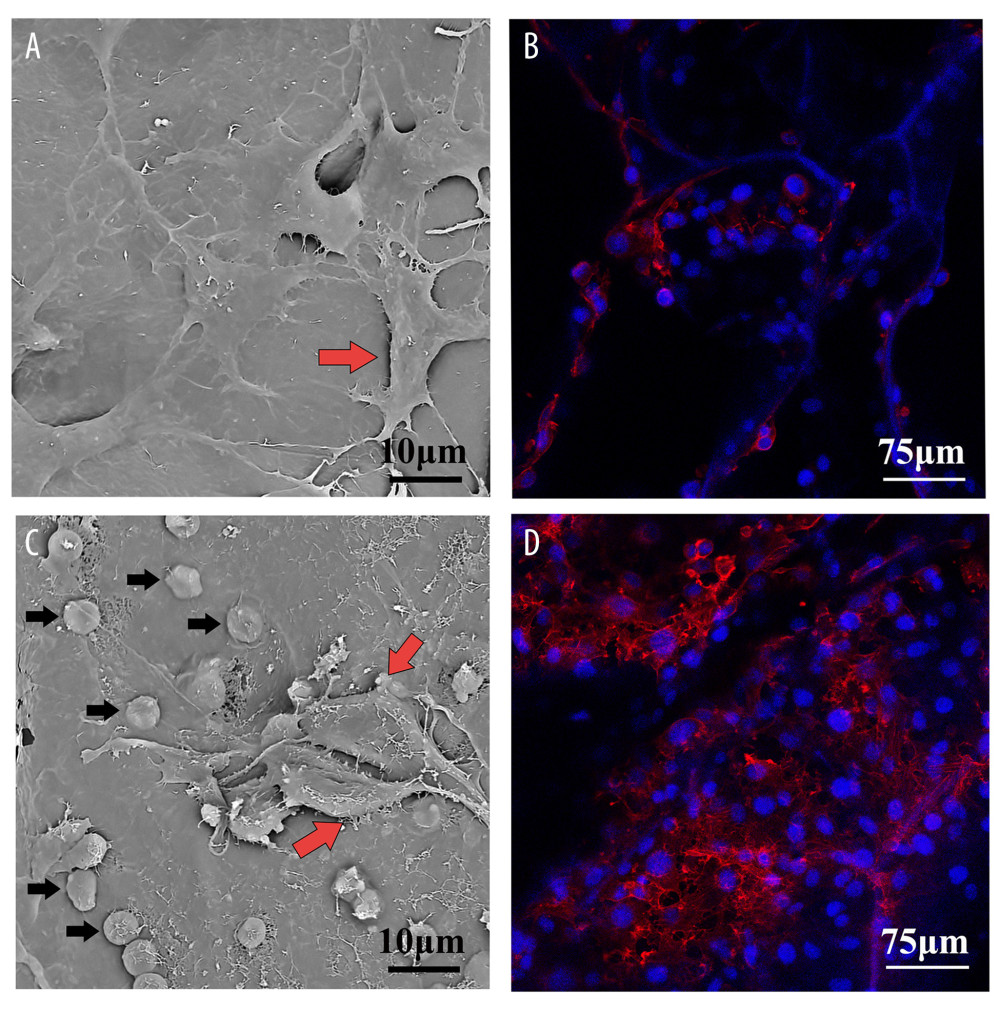 Figure 1. Cell adhesion and proliferation on the surface of the AD scaffold and AD/PRP composite scaffold. (A) The SEM result of HUVECs on AD scaffolds, red arrows point to cells. (B) The fluorescence staining result of HUVECs on AD scaffolds. (C) The SEM result of HUVECs on AD/PRP scaffolds, red arrows point to cells and black arrows point to platelet granules. (D) The fluorescence staining result of HUVECs on AD/PRP scaffolds. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 1. Cell adhesion and proliferation on the surface of the AD scaffold and AD/PRP composite scaffold. (A) The SEM result of HUVECs on AD scaffolds, red arrows point to cells. (B) The fluorescence staining result of HUVECs on AD scaffolds. (C) The SEM result of HUVECs on AD/PRP scaffolds, red arrows point to cells and black arrows point to platelet granules. (D) The fluorescence staining result of HUVECs on AD/PRP scaffolds. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). 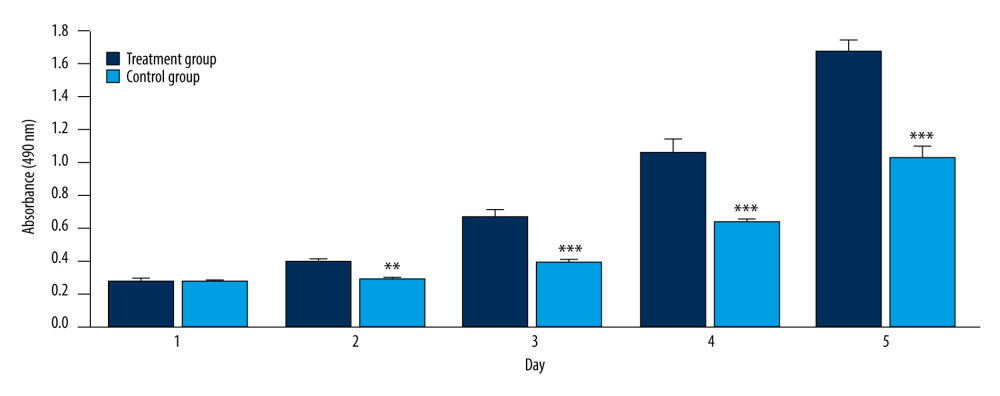 Figure 2. Cell proliferative viability in AD scaffolds and AD/PRP composite scaffolds. ** P<0.01 and *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 2. Cell proliferative viability in AD scaffolds and AD/PRP composite scaffolds. ** P<0.01 and *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). 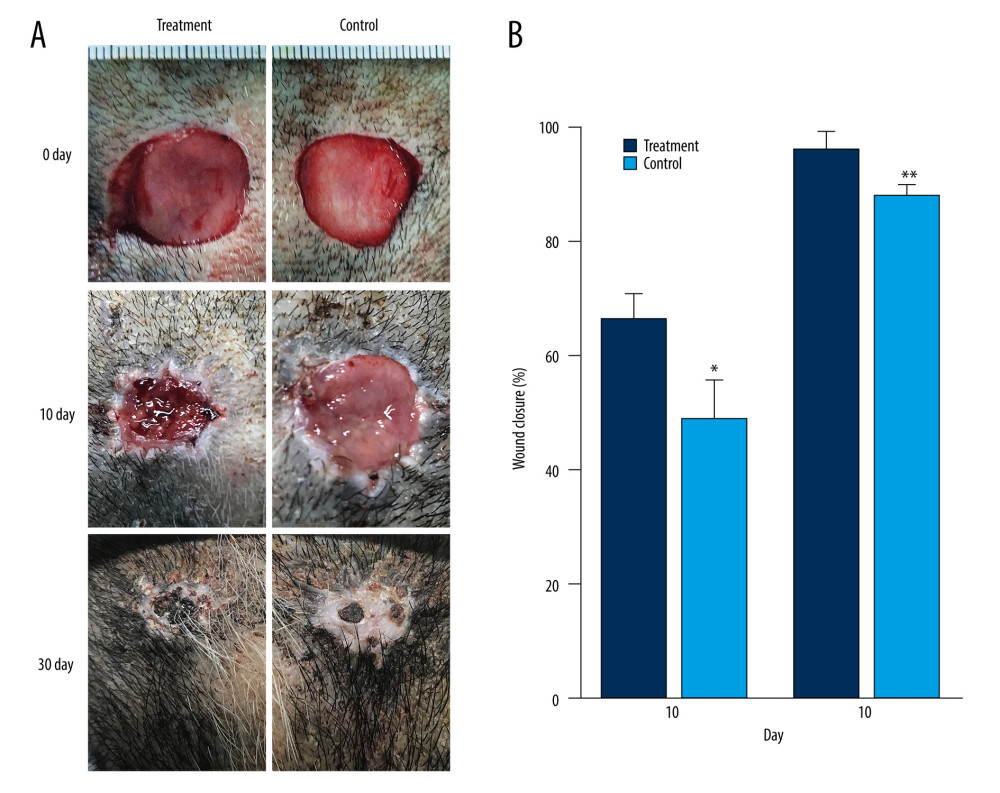 Figure 3. General view of the repair effects in AD scaffolds and AD/PRP composite scaffolds: the treatment group on the left and the control group on the right. (A) Fabrication of skin defect model in pig heads on day 0 and after treatment on day 10 and day 30. (B) Statistical plot of wound healing rate. * P<0.05 and ** P<0.01 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 3. General view of the repair effects in AD scaffolds and AD/PRP composite scaffolds: the treatment group on the left and the control group on the right. (A) Fabrication of skin defect model in pig heads on day 0 and after treatment on day 10 and day 30. (B) Statistical plot of wound healing rate. * P<0.05 and ** P<0.01 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). 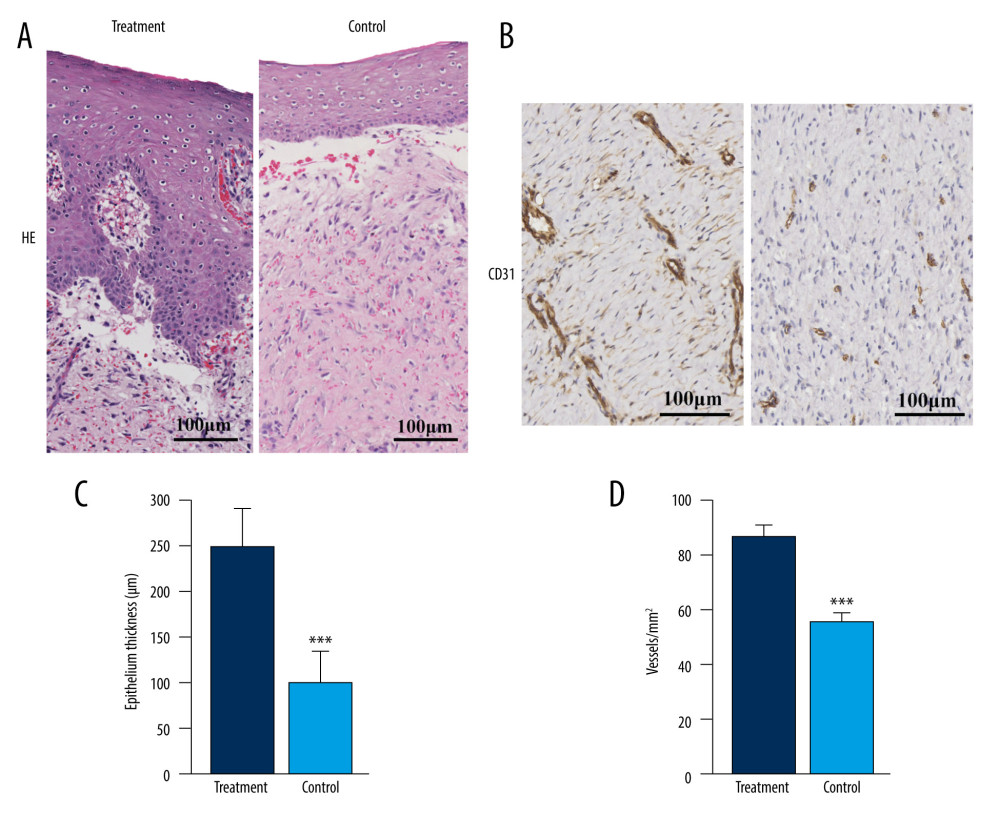 Figure 4. The histological staining results of the AD scaffolds and AD/PRP composite scaffolds. (A) HE staining of skin defect on day 30. (B) CD31 immunohistochemistry staining. (C) Statistical plot of epithelium thickness. (D) Statistical plot of vessels. *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 4. The histological staining results of the AD scaffolds and AD/PRP composite scaffolds. (A) HE staining of skin defect on day 30. (B) CD31 immunohistochemistry staining. (C) Statistical plot of epithelium thickness. (D) Statistical plot of vessels. *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). References
1. Brandi C, Grimaldi L, Nisi G, Treatment with vacuum-assisted closure and cryo-preserved homologous de-epidermalised dermis of complex traumas to the lower limbs with loss of substance, and bones and tendons exposure: J Plast Reconstr Aesthet Surg, 2008; 61(12); 1507-11
2. Hudgins PA, Flap reconstruction in the head and neck: Expected appearance, complications, and recurrent disease: Eur J Radiol, 2002; 44(2); 130-38
3. Nyame TT, Chiang HA, Leavitt T, Tissue-engineered skin substitutes: Plast Reconstr Surg, 2015; 136(6); 1379-88
4. Lucich EA, Rendon JL, Valerio IL, Advances in addressing full-thickness skin defects: A review of dermal and epidermal substitutes: Regen Med, 2018; 13(4); 443-56
5. De Francesco F, Busato A, Mannucci S, Artificial dermal substitutes for tissue regeneration: Comparison of the clinical outcomes and histological findings of two templates: J Int Med Res, 2020; 48(8) 300060520945508
6. Qiu X, Wang J, Wang G, Wen H: J Plast Surg Hand Surg, 2018; 52(4); 204-9
7. Chen G, Tang H, Wang GEvaluate the clinical effectiveness of domestic double layer artificial dermis dressing with autologous split-thickness skin for treatment of wounds with bone or tendon exposure: Chinese Journal of Injury Repair and Wound Healing(Electronic Edition), 2016 [in Chinese]
8. Yeong EK, Yu YC, Chan ZH, Roan TL, Is artificial dermis an effective tool in the treatment of tendon-exposed wounds?: J Burn Care Res, 2013; 34(1); 161-67
9. Frueh FS, Menger MD, Lindenblatt N, Current and emerging vascularization strategies in skin tissue engineering: Crit Rev Biotechnol, 2017; 37(5); 613-25
10. Everts P, Onishi K, Jayaram P, Platelet-rich plasma: New performance understandings and therapeutic considerations in 2020: Int J Mol Sci, 2020; 21(20); 7794
11. Sheean AJ, Anz AW, Bradley JP, Platelet-rich plasma: Fundamentals and clinical applications: Arthroscopy, 2021; 37(9); 2732-34
12. Baria M, Vasileff WK, Miller M, Cellular components and growth factor content of platelet-rich plasma with a customizable commercial system: Am J Sports Med, 2019; 47(5); 1216-22
13. Qian Z, Wang H, Bai Y, Improving chronic diabetic wound healing through an injectable and self-healing hydrogel with platelet-rich plasma release: ACS Appl Mater Interfaces, 2020; 12(50); 55659-74
14. Etulain J, Platelets in wound healing and regenerative medicine: Platelets, 2018; 29(6); 556-68
15. Sadeghi-Ataabadi M, Mostafavi-Pour Z, Vojdani Z, Fabrication and characterization of platelet-rich plasma scaffolds for tissue engineering applications: Mater Sci Eng C Mater Biol Appl, 2017; 71; 372-80
16. Anitua E, Tejero R, Alkhraisat MH, Orive G, Platelet-rich plasma to improve the bio-functionality of biomaterials: BioDrugs, 2013; 27(2); 97-111
17. Dohan Ehrenfest DM, Rasmusson L, Albrektsson T, Classification of platelet concentrates: From pure platelet-rich plasma (P-PRP) to leucocyte- and platelet-rich fibrin (L-PRF): Trends Biotechnol, 2009; 27(3); 158-67
18. Wang W, Zhang L, Sun L, Biocompatibility and immunotoxicology of the preclinical implantation of a collagen-based artificial dermal regeneration matrix: Biomed Environ Sci, 2018; 31(11); 829-42
19. Xu Z, Chen X, Tan R, Preparation and characterization of a gallium-loaded antimicrobial artificial dermal scaffold: Mater Sci Eng C Mater Biol Appl, 2019; 105; 110063
20. Zhao X, Wu H, Guo B, Antibacterial anti-oxidant electroactive injectable hydrogel as self-healing wound dressing with hemostasis and adhesiveness for cutaneous wound healing: Biomaterials, 2017; 122; 34-47
21. Yang J, Chen Z, Pan D, Umbilical cord-derived mesenchymal stem cell-derived exosomes combined pluronic F127 hydrogel promote chronic diabetic wound healing and complete skin regeneration: Int J Nanomedicine, 2020; 15; 5911-26
22. Qiu XW, Wang JHEfficacy of dermal scaffold for promoting repair of acute full-thickness skin defects in pigs: Nan Fang Yi Ke Da Xue Xue Bao, 2018; 38(3); 363-68 [in Chinese]
23. Chimutengwende-Gordon M, Dowling R, Pendegrass C, Blunn G, Determining the porous structure for optimal soft-tissue ingrowth: An in vivo histological study: PLoS One, 2018; 13(10); e0206228
24. Diaz-Gomez L, Alvarez-Lorenzo C, Concheiro A, Biodegradable electrospun nanofibers coated with platelet-rich plasma for cell adhesion and proliferation: Mater Sci Eng C Mater Biol Appl, 2014; 40; 180-88
25. Guo SC, Tao SC, Yin WJ, Exosomes derived from platelet-rich plasma promote the re-epithelization of chronic cutaneous wounds via activation of YAP in a diabetic rat model: Theranostics, 2017; 7(1); 81-96
26. Fernandez-Moure JS, Van Eps JL, Cabrera FJ, Platelet-rich plasma: A biomimetic approach to enhancement of surgical wound healing: J Surg Res, 2017; 207; 33-44
27. Zhou S, Li L, Chen C, Injectable gelatin microspheres loaded with platelet rich plasma improve wound healing by regulating early inflammation: Int J Med Sci, 2021; 18(9); 1910-20
28. Solovieva EV, Teterina AY, Klein OI, Sodium alginate-based composites as a collagen substitute for skin bioengineering: Biomed Mater, 2020; 16(1); 015002
29. Dai NT, Huang WS, Chang FW, Development of a novel pre-vascularized three-dimensional skin substitute using blood plasma gel: Cell Transplant, 2018; 27(10); 1535-47
30. Cheng N, Jeschke MG, Sheikholeslam M, Promotion of dermal regeneration using pullulan/gelatin porous skin substitute: J Tissue Eng Regen Med, 2019; 13(11); 1965-77
31. De Francesco F, Busato A, Mannucci S, Artificial dermal substitutes for tissue regeneration: Comparison of the clinical outcomes and histological findings of two templates: J Int Med Res, 2020; 48(8) 300060520945508
32. Kobayashi E, Fluckiger L, Fujioka-Kobayashi M, Comparative release of growth factors from PRP, PRF, and advanced-PRF: Clin Oral Investig, 2016; 20(9); 2353-60
33. Lertkiatmongkol P, Liao D, Mei H, Endothelial functions of platelet/endothelial cell adhesion molecule-1 (CD31): Curr Opin Hematol, 2016; 23(3); 253-59
34. Carney DH, Mann R, Redin WR, Enhancement of incisional wound healing and neovascularization in normal rats by thrombin and synthetic thrombin receptor-activating peptides: J Clin Invest, 1992; 89(5); 1469-77
35. Genet G, Boye K, Mathivet T, Endophilin-A2 dependent VEGFR2 endocytosis promotes sprouting angiogenesis: Nat Commun, 2019; 10(1); 2350
36. Sidiropoulou S, Papadaki S, Tsouka AN, The effect of platelet-rich plasma on endothelial progenitor cell functionality: Angiology, 2021; 72(8); 776-86
37. Okonkwo UA, DiPietro LA, Diabetes and wound angiogenesis: Int J Mol Sci, 2017; 18(7); 1419
38. Broughton G, Janis JE, Attinger CE, Wound healing: An overview: Plast Reconstr Surg, 2006; 117(7 Suppl); 1e-32e-S
Figures
 Figure 1. Cell adhesion and proliferation on the surface of the AD scaffold and AD/PRP composite scaffold. (A) The SEM result of HUVECs on AD scaffolds, red arrows point to cells. (B) The fluorescence staining result of HUVECs on AD scaffolds. (C) The SEM result of HUVECs on AD/PRP scaffolds, red arrows point to cells and black arrows point to platelet granules. (D) The fluorescence staining result of HUVECs on AD/PRP scaffolds. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 1. Cell adhesion and proliferation on the surface of the AD scaffold and AD/PRP composite scaffold. (A) The SEM result of HUVECs on AD scaffolds, red arrows point to cells. (B) The fluorescence staining result of HUVECs on AD scaffolds. (C) The SEM result of HUVECs on AD/PRP scaffolds, red arrows point to cells and black arrows point to platelet granules. (D) The fluorescence staining result of HUVECs on AD/PRP scaffolds. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). Figure 2. Cell proliferative viability in AD scaffolds and AD/PRP composite scaffolds. ** P<0.01 and *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 2. Cell proliferative viability in AD scaffolds and AD/PRP composite scaffolds. ** P<0.01 and *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). Figure 3. General view of the repair effects in AD scaffolds and AD/PRP composite scaffolds: the treatment group on the left and the control group on the right. (A) Fabrication of skin defect model in pig heads on day 0 and after treatment on day 10 and day 30. (B) Statistical plot of wound healing rate. * P<0.05 and ** P<0.01 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 3. General view of the repair effects in AD scaffolds and AD/PRP composite scaffolds: the treatment group on the left and the control group on the right. (A) Fabrication of skin defect model in pig heads on day 0 and after treatment on day 10 and day 30. (B) Statistical plot of wound healing rate. * P<0.05 and ** P<0.01 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). Figure 4. The histological staining results of the AD scaffolds and AD/PRP composite scaffolds. (A) HE staining of skin defect on day 30. (B) CD31 immunohistochemistry staining. (C) Statistical plot of epithelium thickness. (D) Statistical plot of vessels. *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA).
Figure 4. The histological staining results of the AD scaffolds and AD/PRP composite scaffolds. (A) HE staining of skin defect on day 30. (B) CD31 immunohistochemistry staining. (C) Statistical plot of epithelium thickness. (D) Statistical plot of vessels. *** P<0.001 relative to the control group. Images were processed using Photoshop software (Adobe Photoshop CS6 USA). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








