26 May 2022: Clinical Research
Evaluation of Patients with Angiographically-Confirmed Coronary Artery Disease to Investigate the Association Between Epicardial Fat Thickness and Atrial Fibrillation
Xiaoxia Xu1ABF, Qina Zhou2CDE, Zhongyuan Ren3BF, Fengdan Wang3BC, Yixin Chen3BD, Hui Sun3ADFG*DOI: 10.12659/MSM.936446
Med Sci Monit 2022; 28:e936446
Abstract
BACKGROUND: Epicardial fat thickness (EFT) is increasingly recognized as an independent risk factor of the presence, severity, and recurrence of atrial fibrillation (AF). We investigated the associations between EFT and AF prevalence and identified its correlation with other risk factors.
MATERIAL AND METHODS: A total of 199 participants who underwent coronary angiography and had confirmed coronary artery disease (CAD) were enrolled in this study. The EFT was measured by echocardiography and the association of EFT with other AF risk factors was evaluated by multivariate logistic regression analysis.
RESULTS: The EFT was significantly higher in patients with comorbidity of AF and CAD than those with CAD alone (6.86±1.96 mm vs 5.91±1.71 mm, P<0.001). Logistic regression analysis indicated that EFT was a predictive factor of the occurrence of AF in CAD, after adjusting for body mass index (BMI), systolic blood pressure (SBP), left circumflex artery (LCX) stenosis, LA diameter, B-type natriuretic peptide (BNP), creatinine (Cr), and blood urea nitrogen (BUN). LA diameter, SBP, and LCX stenosis are also independent risk factors for CAD complicated by AF. Correlation analysis revealed significant positive linear correlations between EFT and BMI (P<0.01), EFT, and LA diameter (P<0.05), as well as positive correlations between LA diameter and BNP, Cr, or BUN.
CONCLUSIONS: Epicardial fat thickness is a strong predictor for AF prevalence in patients with CAD, independent of other AF risk factors such as LA diameter, BMI, and SBP, while LA diameter, SBP, and LCX stenosis are also independent AF risk factors for CAD.
Keywords: Atrial Fibrillation, Coronary Artery Disease, Adipose Tissue, Constriction, Pathologic, Humans, Pericardium, Risk Factors
Background
Atrial fibrillation (AF) is highly prevalent in patients with coronary artery disease (CAD). There is evidence showing that the prevalence of AF in patients with stable CAD is 19% [1], which reaches 28% in acute myocardial infarction patients [2]. Epicardial fat thickness and volume is increasingly recognized as a predictive factor contributing to the occurrence and severity of AF, independent of other AF risk factors, including body mass index and left atrial enlargement [3–5]. Due to the close anatomical proximity with both coronary arteries and myocardium, epicardial fat tissue can promote the development and maintenance of AF and CAD via varied mechanisms, including the paracrine transmission of adipocytokines [6], promoting myocardial fibrosis [6], direct adipocyte infiltration into the atrial myocardium leading to altered atrial electrophysiological substrates [7], blocked inter-atrial conduction [8], sympathovagal imbalance [9], and increased sympathetic activity and innervation [10].
A cross-sectional study measuring epicardial fat thickness (EFT) and pericardial fat thickness (PFT) via transthoracic echocardiography suggested that EFT can be considered as an independent predictor for CAD, while there was no significant association between PFT and CAD [11]. Although EFT has been recognized as an independent predictor for CAD and AF separately, there have been few studies focused on the conditions of the comorbidity of AF and CAD. Nakanishi reported a significant association between peri-atrial epicardial fat volume and new-onset AF in patients with CAD [12], but the epicardial fat volume was defined as the adipose tissue located within the pericardial sac using multidetector computed tomography (MDCT). Furthermore, despite reports that pericardial fat is associated with AF, AF burden, and ablation outcomes of AF [13,14], we should be aware of the essential difference between epicardial fat tissues and pericardial fat tissues, and it is still unclear whether EFT is associated with AF complicated by CAD. This study thus aimed to determine the relationship between EFT and the occurrence of AF in patients with CAD, and the correlation with other risk factors, which involve the location and severity of coronary artery obstruction.
Material and Methods
STUDY DESIGN AND POPULATION:
This retrospective study recruited 199 consecutive adult patients who were admitted to the General Cardiology Department and Cardiac Care Unit (CCU) of Shanghai 10th People’s Hospital between June 2020 and March 2021. The study was approved by the Institutional Review Board of Tongji University School of Medicine. Patients who met all the following criteria were eligible for inclusion: (1) adults aged 18 years and over on the date of consent; (2) Coronary artery disease (CAD): Coronary arteriography (CAG) showing at least 1 stenosis of the great coronary artery ≥50% or typical electrocardiographic changes and elevated myocardium biochemical markers; and (3) Documented AF on an electrocardiogram (ECG) or Holter monitor within the last 24 months (as shown in Figure 1). Patients with CAD complicated by AF were included in the CAD+AF group (n=83), and the CAD group (n=116) consisted of patients with CAD but without AF.
Exclusion criteria were: (1) Patients with AF secondary to other heart diseases, such as valvular heart disease, hypertensive heart disease, hypertrophic obstructive cardiomyopathy, and dilated cardiomyopathy; and (2) Patients with malignant tumors, cardiac valvular disease, mental illnesses, or severe immune system diseases, infectious diseases, hematological diseases, severe impairment of brain, liver or kidney, and multiple organ dysfunction syndromes.
The study was conducted in strict compliance with the principles outlined in the Declaration of Helsinki and was approved by Institutional Ethics Committee of Shanghai Tenth People’s Hospital (permit number: SHSY-IEC-5.0/22K69/P01). All patients provided written informed consent.
CLINICAL DATA AND RISK FACTOR ASSESSMENT:
We recorded baseline data, including age, sex, height, weight, body mass index (BMI), and blood pressure were collected. Any history of diabetes mellitus, hypertension, and smoking status. Fasting blood samples were collected to measure total cholesterol, low-density lipoprotein cholesterol (LDL-C), high-density lipoprotein cholesterol (HDL-C), triglycerides, creatinine, blood urea nitrogen, cardiac troponin T, myoglobin, B-type natriuretic peptide (BNP), creatine (Cr), blood urea nitrogen (BUN), C-reactive protein (CRP), Creatine kinase-MB, hemoglobin A1C, D-dimer, alanine transaminase (ALT), and aspartate aminotransferase (AST) level.
CORONARY ARTERIOGRAPHY (CAG):
Coronary arteriographic data were collected from cardiac catheterization laboratory records.
The digital angiography system used was the Axiom Artis Q ceiling (Siemens, Erlangen, Germany).
We collected data on the percentage of narrowing of the affected coronary vessel, including left anterior descending (LAD), left main artery (LM), left circumflex artery (LCX), and right coronary artery (RCA). The patients with presence of luminal narrowing more than 50% of at least 1 coronary artery on coronary angiography were included in this study. Depending on the severity, the stenosis was classified as mild (<50%), moderate (50~75%), severe (75~90%), and blocking (≥90%). Three-vessel disease were identified as more than 3 coronary arteries with luminal narrowing more than 50% (representitive coronary angiography as shown in Figure 2).
ECHOCARDIOGRAPHY AND EPICARDIAL FAT THICKNESS (EFT) MEASUREMENT:
A cardiac sonographer blinded to all study details using an echocardiography device with frequency probe (2.0–4.5 MHz) (Vivid E9, GE, USA) was used to measure echocardiographic indicators. Measurements, including LA diameter, left ventricular end-diastolic diameter (LVEDD), left ventricular end-systolic diameter (LVESD), and left ventricular ejection fraction were performed according to the current guidelines [15]. On the echocardiogram, epicardial adipose tissue is recognized as the echo-free space between the outer epicardium and visceral pericardium. EAT measurement was performed by EFT measured perpendicularly to the right ventricle free wall in 2D parasternal long-axis and short-axis views at end-systole and end-diastole in 3 cardiac cycles. Maximum EFT for parasternal long-axis view was measured perpendicularly to the aortic annulus, and perpendicularly to the interventricular septum at the papillary muscle level for parasternal short-axis view. The average of measurements at the 3 cycles was determined as the EFT. There is evidence that standard parasternal long-axis and short-axis views provide the most accurate assessment of the EFT thickness of the right ventricle [16]. Representative echocardiographic pictures for EFT measurement were shown in Figure 3 (sinus rhythm) and Figure 4 (AF)
ASSESSMENT OF AF:
The assessment of AF was performed in all patients using the same diagnostic criteria. Prevalent AF was defined based on the presence of any episodes of confirmed atrial flutter or AF on electrocardiography (ECG) or Holter report before this study. The surface 12-lead ECGs and 24-h Holter monitoring from external medical institutions or previous hospital records were also used as evidence of AF. The ECG device used in our institution is Lnno-12-U (SID medical, Shanghai, China), while the Holter device is BI9000 (Biomedical Instruments Co., Ltd. Shenzhen, China). AF symptoms, severity, and duration were evaluated by at least 2 cardiologists. Clinical classifications of atrial fibrillation as stated in the 2014 AHA/ACC/HRS Guideline for the Management of Patients with Atrial Fibrillation [17]: Paroxysmal AF was defined as AF that terminates spontaneously or with intervention within 7 days of onset. Persistent AF was defined as continuous AF sustained >7 days. Long-standing persistent AF was defined as continuous AF >12 months in duration. All patients in the CAD group had AF excluded using ECGs and monitorization.
STATISTICAL ANALYSIS:
All statistical analysis was performed using the IBM SPSS 23. Levene’s test for equality of variances was used to test the distribution of measurement data. The comparison of normally distributed data was performed using the independent-sample
Results
CLINICAL CHARACTERISTICS:
A total of 199 participants were included: 83 patients with CAD complicated with AF (the CAD+AF group) and 116 controls with CAD but without AF (the CAD group). The baseline characteristics of patients are shown in Table 1. Within the CAD+AF group, 48 (57.8%) patients had paroxysmal AF and 35 (42.2%) had persistent AF or long persistent AF.
The patients with CAD complicated by AF were not significantly different from the control subjects regarding age, sex, height, weight, history of DM and hypertension, DBP, LVEDD, LVESD, EF%, CTn-T, myoglobin, CK-MB, CRP, D-dimer, HbA1c, total cholesterol, HDL-C, LDL-C ALT, and AST (P>0.05, Table 1).
However, patients with CAD complicated by AF were more likely to have a history of smoking, higher BMI, higher EFT, larger LA diameter, and higher systolic blood pressure (SBP), BNP, Cr, and BUN than those in the CAD group (P<0.05 for all, Table 1). For instance, patients with AF had significant higher BMI (25.48±3.76 kg/m2 vs 24.44±3.16 kg/m2, P<0.05) and a larger LA diameter (43.12±5.84 mm vs 36.51±4.50 mm, P<0.05) compared to patients without AF. In addition, the EFT at long-axis end-systole in patients in the CAD+AF group was significantly higher than in the CAD group (6.86±1.96 mm vs 5.91±1.71 mm, P<0.001). Differences of other factors are presented in Table 1.
Table 2 lists the comparison of the vessel location and severity of coronary artery stenosis. Patients with AF had a significantly higher percentage of LCX stenosis than patients without AF (40.1% vs 24.1%, P=0.009). Differences in prevalence of other locations of coronary stenosis, including LAD stenosis, RCA stenosis, and 3 vessels, were not statistically significant between the CAD+AF group and the CAD group. There was no significant difference in severity of coronary artery stenosis between the 2 groups.
CORRELATION ANALYSIS BETWEEN VARIABLES:
Table 3 shows the Pearson correlation coefficient analysis between variables before entry into the logistic regression model. There were significantly positive linear correlations between EFT and BMI (P<0.01), as well as EFT and LA diameter (P<0.05), (Figure 5 showing the Scatter plot of LA diameter by EFT).
LA Diameter was shown to be significantly and positively correlated with BMI (
BNP, Cr, and BUN were all positively correlated with each other and were positively correlated with LA diameter, but were negatively correlated with EF%.
MULTIPLE REGRESSION ANALYSIS:
The association between AF and EFT was assessed by multivariate binary logistic regression analysis (Table 4). The occurrence of AF was regarded as a dependent variable, while BMI, SBP, LCX stenosis, EFT (long-axis end-systole), LA diameter, BNP, Cr, and BUN were retained as the covariates in the model. EFT (odds ratio [OR]: 1.327; 95% confidence interval [CI]: 1.1081–1.628; P=0.007), SBP (OR: 0.981; 95% CI: 0.965–0.996; P=0.017), LCX stenosis (OR: 0.377; 95% CI: 0.175–0.814; P=0.013) and LA diameter (OR: 1.320; 95% CI: 1.203–1.447; P<0.001) were identified as independent risk factors for the occurrence of AF in patients CAD.
Discussion
CURRENT EVIDENCE ON EFT AND AF:
Epicardial fat refers to adipose tissue located between the myocardium and visceral pericardium, usually covering the surface of the right ventricle and left ventricular anterior wall and surrounding atrioventricular grooves and interventricular grooves [18,19]. Although mounting evidence supports the association between pericardial fat and AF, we should be aware of the distinction between pericardial fat and epicardial fat, as they differ in anatomy, origin, and biochemistry. Epicardial fat is situated between the myocardium and visceral pericardium, while pericardial fat is located between the visceral pericardium and internal surface of the parietal pericardium [18]. In terms of origin, epicardial fat evolves from the splanchnopleuric mesoderm during embryogenesis, while pericardial fat evolves from the primitive thoracic mesenchyme [20]. From the biochemical aspect, epicardial fat is metabolically active and well supplied with adipokines via paracrine or vasocrine mechanisms [18]. Finally, the function of pericardial fat appears to be completely different from that of epicardial fat.
THE ASSOCIATION OF EPICARDIAL FAT THICKNESS WITH AF:
There is increasing evidence that epicardial fat thickness (EFT) and epicardial fat volume (EFV), as measured by echocardiography, computed tomography (CT), or magnetic resonance image (MRI), are independent risk factors for the presence and severity of atrial fibrillation [3,21,22]. Furthermore, very recent clinical data found that EFT and EFV were significantly associated with AF recurrence after pulmonary vein isolation with at least 1-year follow-up [23], which was consistent with the findings of a systematic review and meta-analysis [24]. Although the Framingham Heart Study, involving 3217 individuals, and another clinical study found that higher pericardial fat volumes were associated with higher prevalence of AF [13,25], these 2 studies defined total pericardial fat volume as adipose tissue within the pericardial sac. A meta-analysis comparing the strength of associations of epicardial, pericardial, abdominal, and overall adiposity with AF that included 63 population studies, found that the associations with AF were stronger in studies that measured epicardial fat, not pericardial fat [26].
However, there is still controversy about the association between EFT and AF. For instance, a large prospective cohort study involving 3905 participants with cardiovascular disease over a 5-year follow-up found out that EFV was significantly associated with the prevalence of AF, but the association is not statistically significant after adjusting for left atrium size [27]. Therefore, EFV was quantified by cardiac CT as the fat within the pericardial sac, but the other studies defined it as pericardial fat volume.
THE ASSOCIATION BETWEEN EFT AND AF IN PATIENTS WITH CAD:
Nakanishi et al assessed the relationship between new-onset AF after AMI and epicardial adipose tissue via multidetector computed tomography (MDCT) during a 3-year follow-up period [12]. They found that peri-atrial EFV was a risk factor independent of LA enlargement for developing new-onset AF in patients with CAD. That was the first study of the association between the epicardial adipose tissue and AF in CAD patients. However, the reliability might have been influenced by the disadvantages of diagnosing CAD using MDCT, which has limitedaccuracy and negative predictive value, especially in relatively low-risk individuals [28] and patients with irregular rhythms. Of note EAT was shown to be an independent predictor for the development of new-onset postoperative AF (POAF) in a study involving 124 patients who underwent coronary artery bypass grafting (CABG) surgery [29].
The present study identified definite CAD via the criterion standard technique of coronary angiography and quantitatively assessed the stenosis severity. We found that the EFT measured by 4 methods from parasternal long-axis and short-axis views at both end-systole and end-diastole in patients with CAD complicated by AF was significantly higher than in the CAD group. Multiple regression analysis showed that EFT was significantly associated with the occurrence of AF in patients with CAD. This association was completely maintained after adjusting for BMI, SBP, LCX stenosis, LA Diameter, BNP, Cr, and BUN. Our results are consistent with those of Nakanishi et al, as mentioned above.
OTHER PREDICTORS:
In the present study, SBP, LCX stenosis, and LA diameter were also shown to be independent risk factors for CAD complicated by AF. Concerning coronary artery stenosis, a study in the Korean population reported that LCX accounting for the infarct-related arteries was associated to early AF occurrence after AMI in patients with enlarged LA, but the association was not significant in patients with non-enlarged LA [30], probably because enlarged LA is vulnerable to small stimuli such as ischemic damage of the left atrium caused by LCX stenosis.
Left atrium (LA) enlargement is the final common consequence of structural remodeling processes resulting in the development and maintenance of AF. Evidence showed that enlarged LA are independent prognostic factors for AF recurrence after successful rhythm control by cardioversion or by catheter ablation [31,32]. Furthermore, LA enlargement, particularly the LA area and volume index measured by echocardiography, was demonstrated to be a significant predictor for the risk of developing silent AF in patients with acute myocardial infarction (AMI) [33]. Consistent with the studies mentioned above, the present study found LA diameter was considerably larger in patients with CAD complicated by AF than in those without AF and was associated with the prevalence of AF in CAD. Although Pearson correlation coefficient analysis in our study confirmed the positive correlation between LA diameter and EFT, LA enlargement and EFT were independent predictors of AF in CAD.
Interestingly, our results indicated that subjects with CAD complicated by AF had lower systolic blood pressure than those who only had CAD. Moreover, we found systolic blood pressure was inversely correlated with AF independent of other AF risks.
AF is known to reduce left ventricular diastolic filling due to loss of atrial kick, leading to a reduction in stroke volume, which can be compensated for by increased heart rate and remains preserved by left ventricular ejection fraction (LVEF). Although there is no direct evidence of how AF affects blood pressure, a recent study reported an increase in systolic blood pressure (SBP) in persistent AF patients who had sinus rhythm restored after electrical cardioversion, compared with before cardioversion, whereas there was no significant change in SBP in patients remaining in AF rhythm [34]. This means the systolic blood pressure can be lowered due to persistent AF. The SBP increase when persistent AF is converted to sinus rhythm can partially explain the inverse correlation of SBP and AF in our findings.
Regarding BMI, our results found that CAD patients who exhibited AF had significantly higher BMI, which is positively correlated with EFT and LA diameter. This finding was consistent with the evidence reporting a significant positive correlation between EFT and BMI in patients with cardiovascular disease [35]. Despite that, we found that BMI could not independently predict AF risk in CAD patients. This can be explained by BMI being a convincing predictor of either AF [36] or CAD [37]. Therefore, it is impossible to estimate AF risk from CAD by BMI. To date, limited data indicate that BMI is associated with LA enlargement [38,39]. Regardless of the intercorrelation among BMI, EFT, and LA diameter, BMI and LA diameter were not excluded as candidate variables because either with or without BMI or LA diameter as one of the candidate variables, there was no significant difference in the results of multivariate logistic regression regarding prediction of AF prevalence.
In addition, we found that patients with CAD complicated by AF had a significantly higher level of BNP, Cr, and BUN compared to CAD patients without AF. Plitt et al reported an association of elevated BNP level with raised AF burden, as evaluated by 1-week ambulatory rhythm monitoring [40]. A systematic review and meta-analysis demonstrated the association of elevated BNP level with increased risk of new-onset AF with acute coronary syndrome (ACS) [41]. These studies can explain the higher level of BNP in patients with comorbidity of CAD and AF rather than CAD alone. A study of 395 patients with stage 3 to 5 chronic kidney disease reported that enlarged LA diameter and hypoalbuminemia were independent predictors of the deterioration of renal function assessed by estimated glomerular filtration rate (eGFR) [42]. Akgul et al [43] recently reported that patients with postoperative atrial fibrillation (PoAF) had higher BUN and Cr compared to the PoAF(−) group. They suggested that BUN and Cr levels were predictors of postoperative atrial fibrillation after off-pump cardiopulmonary bypass grafting surgery. However, they did not investigate the relationship between LA diameter and BUN and Cr levels [44]. Moreover, in the present study, Pearson correlation coefficient analysis indicated that BNP, Cr, and BUN were all positively correlated with each other and positively correlated with LA diameter, but were negatively correlated with LVEF. This is the first study to report a relationship between LA enlargement and high levels of Cr and BUN in patients with CAD complicated by AF.
LIMITATIONS:
Our study has several limitations. Comparison among several different AF subtypes was not conducted in our study. Therefore, more accurate estimation of AF burden using insertable cardiac monitors or at least intermittent rhythm monitoring is needed to determine the relationship between EFT and AF burden and atrial conduction in patients with CAD. Furthermore, we did not assess the mechanisms by which EFT influenced the development and maintenance of AF, including the aspects of fibrosis, inflammation, paracrine effects, infiltration of adipose tissue, atrial electrophysiological properties, and autonomic nervous regulation, as mentioned in other studies [45]. Further studies will be performed for in-depth exploration of mechanisms.
Conclusions
This is the first study to demonstrate that epicardial fat thickness is a strong predictor for AF prevalence in patients with CAD, independent of other AF risk factors such as LA diameter, BMI, and SBP. Additionally, SBP, LCX stenosis, and LA diameter were independent risk factors for AF in CAD patients. We also are the first to find that high levels of Cr and BUN were positively correlated with LA diameter in patients with CAD complicated by AF. Investigations are needed to further clarify the exact causality and underlying mechanisms of increased epicardial fat thickness influencing AF prevalence in patients with CAD.
Figures
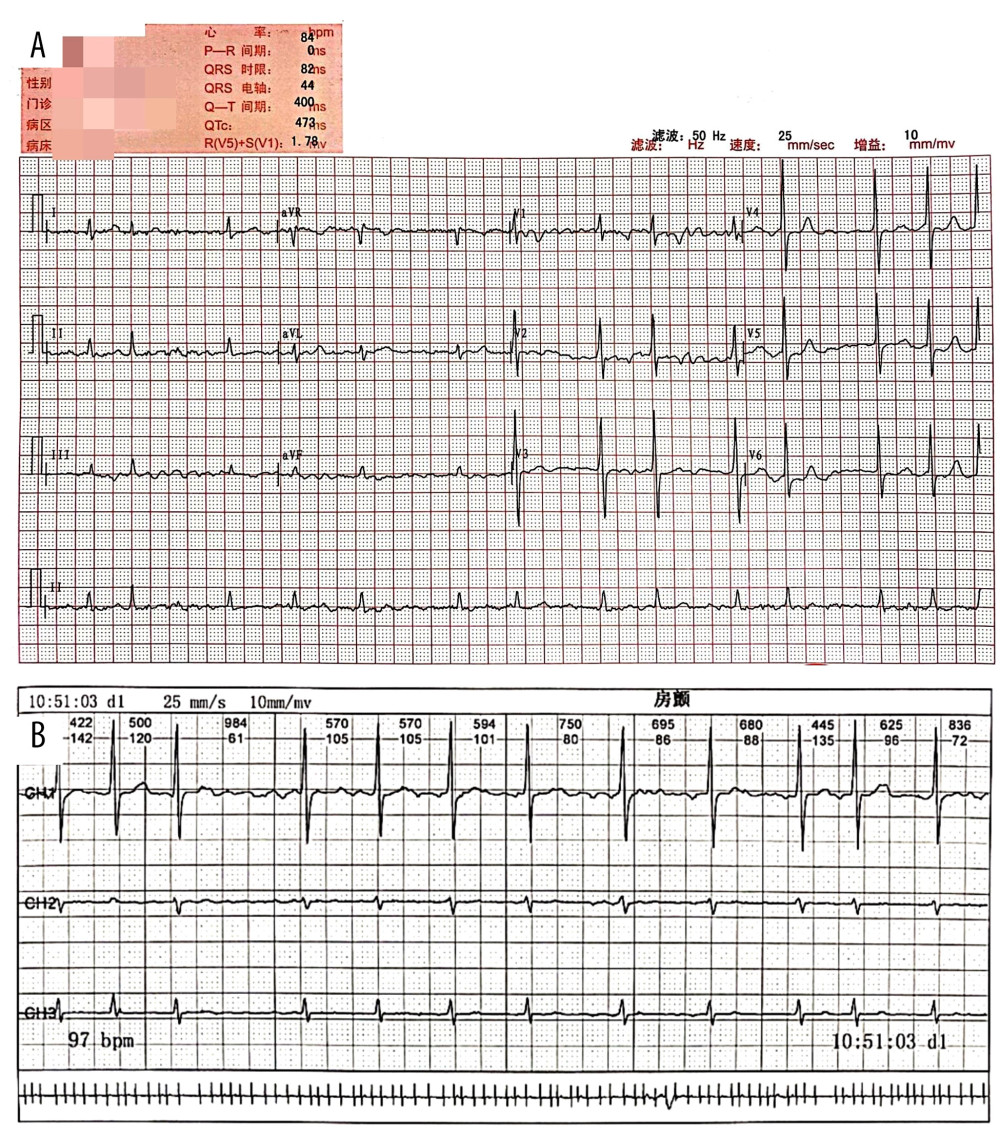 Figure 1. ECG and Holter in the detection of atrial fibrillation. (A) A representative ECG showing atrial fibrillation rhythm from a patient with permanent atrial fibrillation. (B) A selected segment of a representative Holter showing atrial fibrillation rhythm from a patient with paroxysmal atrial fibrillation.
Figure 1. ECG and Holter in the detection of atrial fibrillation. (A) A representative ECG showing atrial fibrillation rhythm from a patient with permanent atrial fibrillation. (B) A selected segment of a representative Holter showing atrial fibrillation rhythm from a patient with paroxysmal atrial fibrillation. 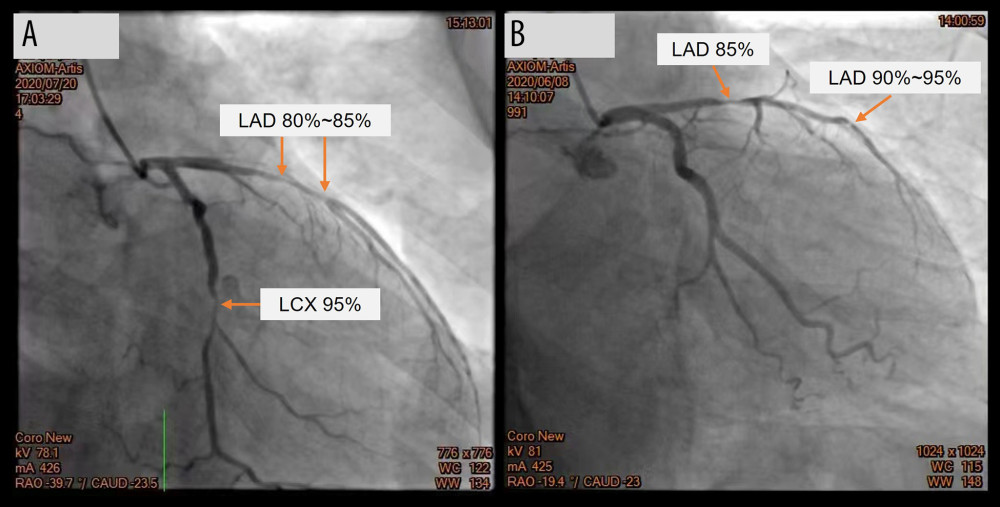 Figure 2. Coronary angiography (CAG) in the detection of coronary artery disease. (A) Shows 80~85% stenosis (red arrow) in the proximal and mid-segment left anterior descending (LAD) and 95% stenosis (red arrow) in the proximal segment of left circumflex artery (LCX). (B) Shows 85% stenosis (red arrow) in the proximal segment of LAD and 90~95% stenosis (red arrow) in the mid-distal segment of LAD.
Figure 2. Coronary angiography (CAG) in the detection of coronary artery disease. (A) Shows 80~85% stenosis (red arrow) in the proximal and mid-segment left anterior descending (LAD) and 95% stenosis (red arrow) in the proximal segment of left circumflex artery (LCX). (B) Shows 85% stenosis (red arrow) in the proximal segment of LAD and 90~95% stenosis (red arrow) in the mid-distal segment of LAD. 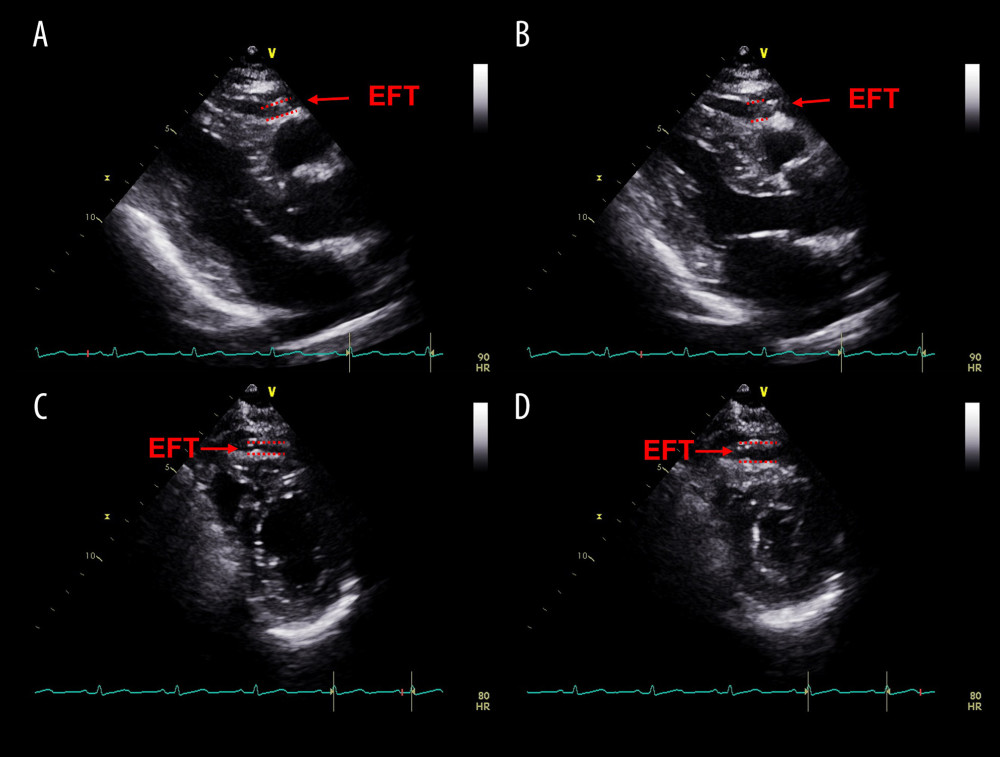 Figure 3. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with sinus rhythm. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view.
Figure 3. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with sinus rhythm. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view. 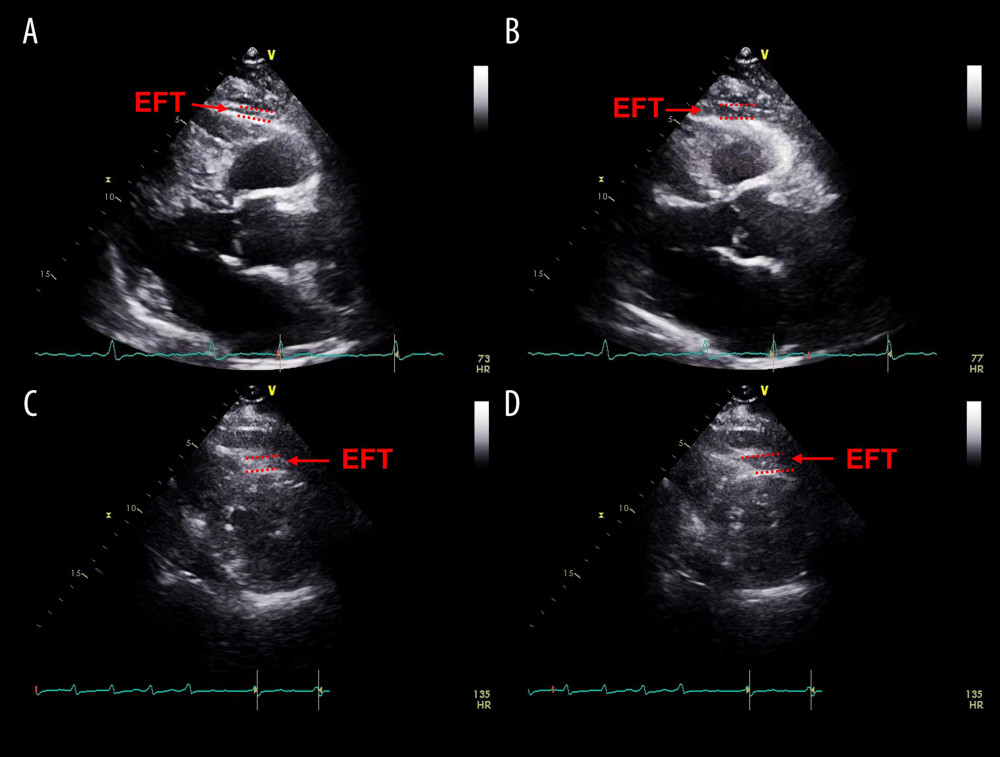 Figure 4. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with atrial fibrillation. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view.
Figure 4. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with atrial fibrillation. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view. 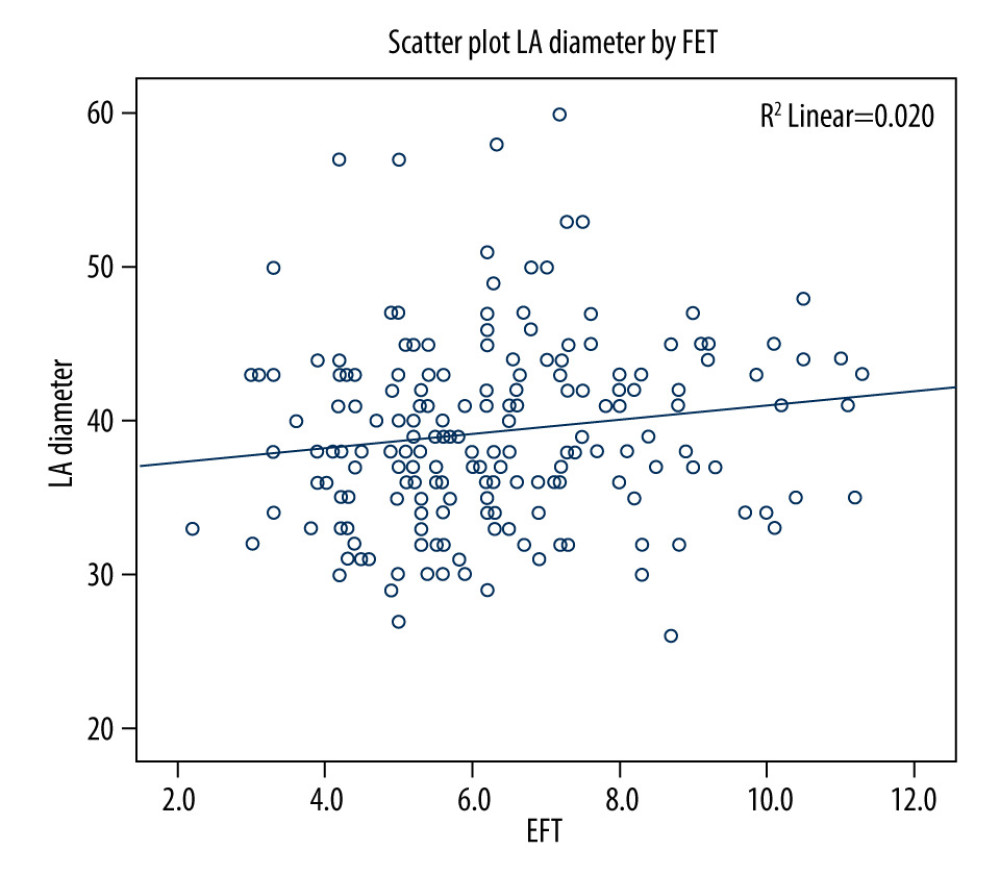 Figure 5. Scatter plot of LA diameter by EFT. There was no apparent correlation between LA diameter and EFT, R2=0.020. EFT – epicardial fat thickness; LA – left atrial.
Figure 5. Scatter plot of LA diameter by EFT. There was no apparent correlation between LA diameter and EFT, R2=0.020. EFT – epicardial fat thickness; LA – left atrial. Tables
Table 1. Comparison of baseline clinical characteristics. Normally distributed variables are described as mean and standard deviation, while non-normally distributed variables are described as median. Categorical characteristics are presented as n (%).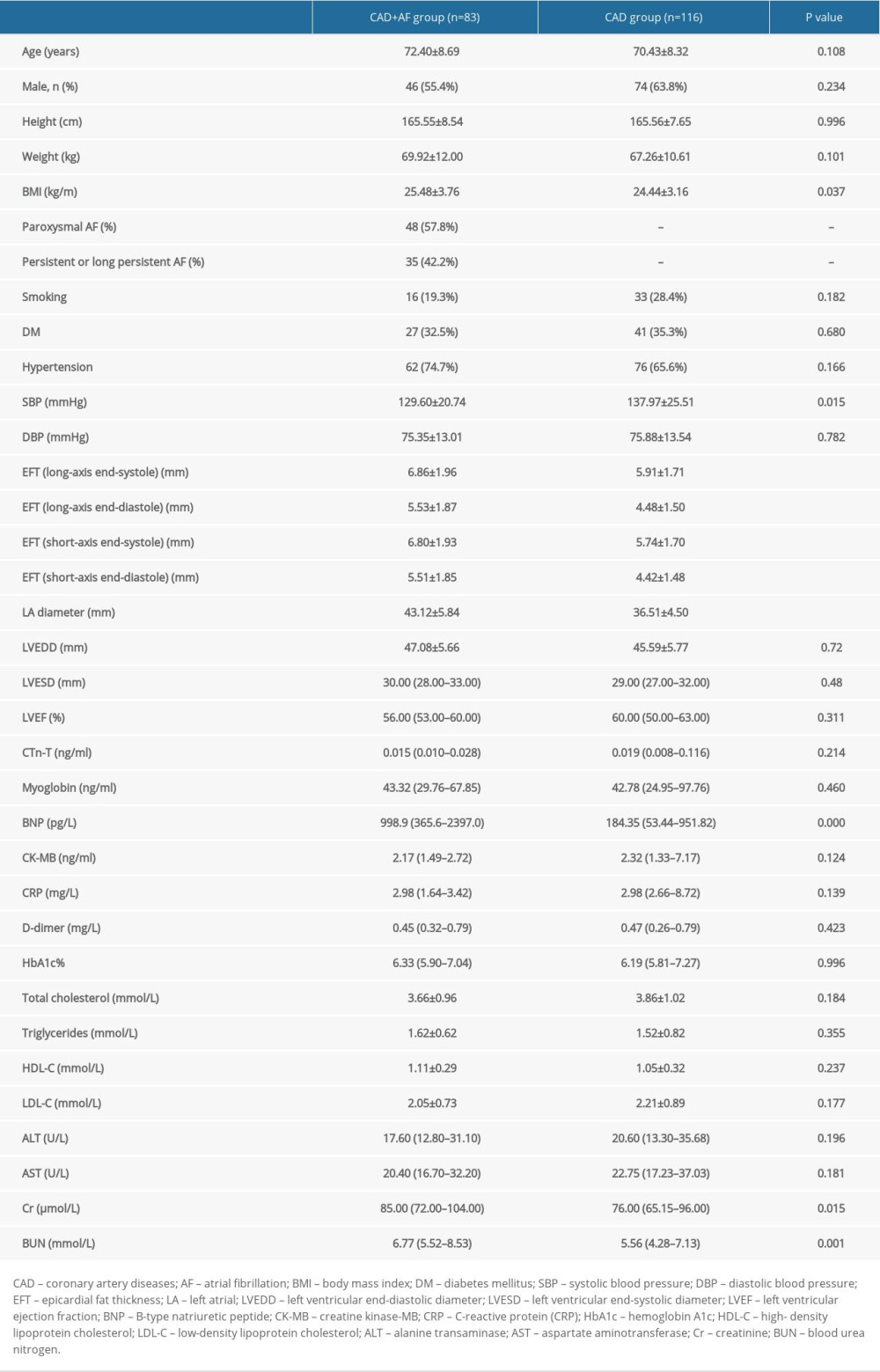 Table 2. The vessel location and severity of coronary artery stenosis.
Table 2. The vessel location and severity of coronary artery stenosis.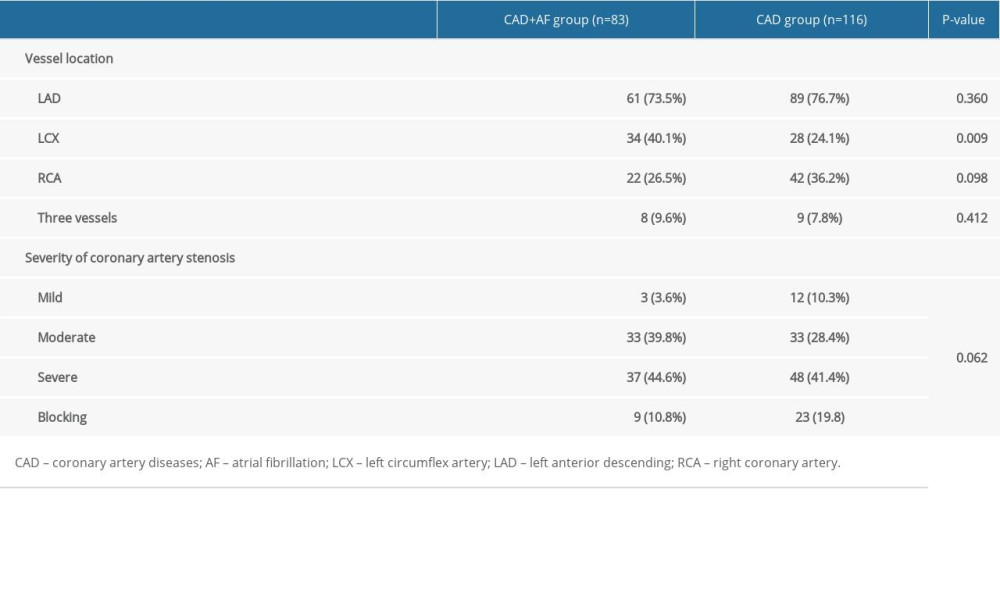 Table 3. Correlation analysis between variables.
Table 3. Correlation analysis between variables.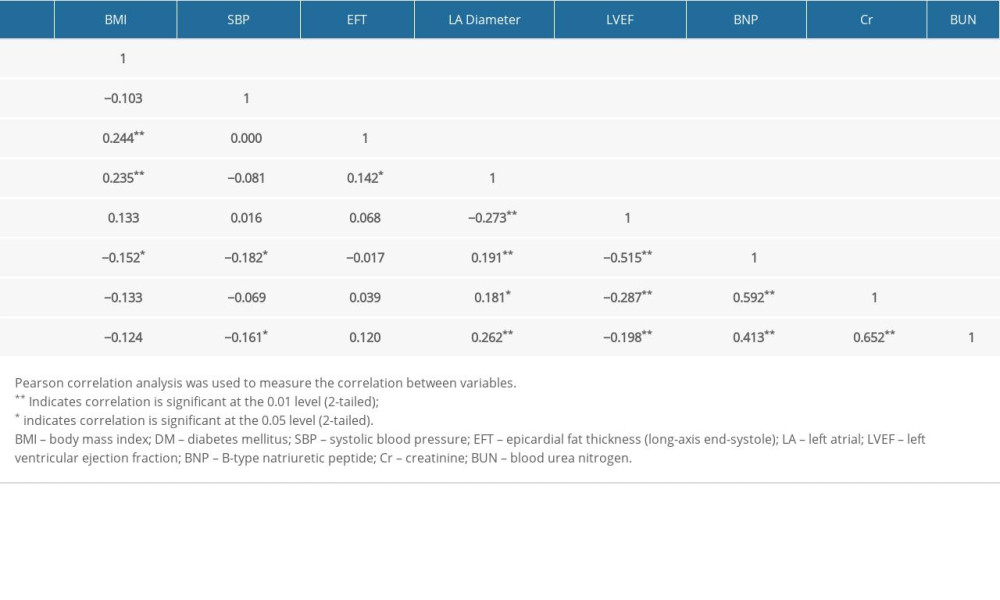 Table 4. Multivariate binary logistic regression analysis among candidate variables.
Table 4. Multivariate binary logistic regression analysis among candidate variables.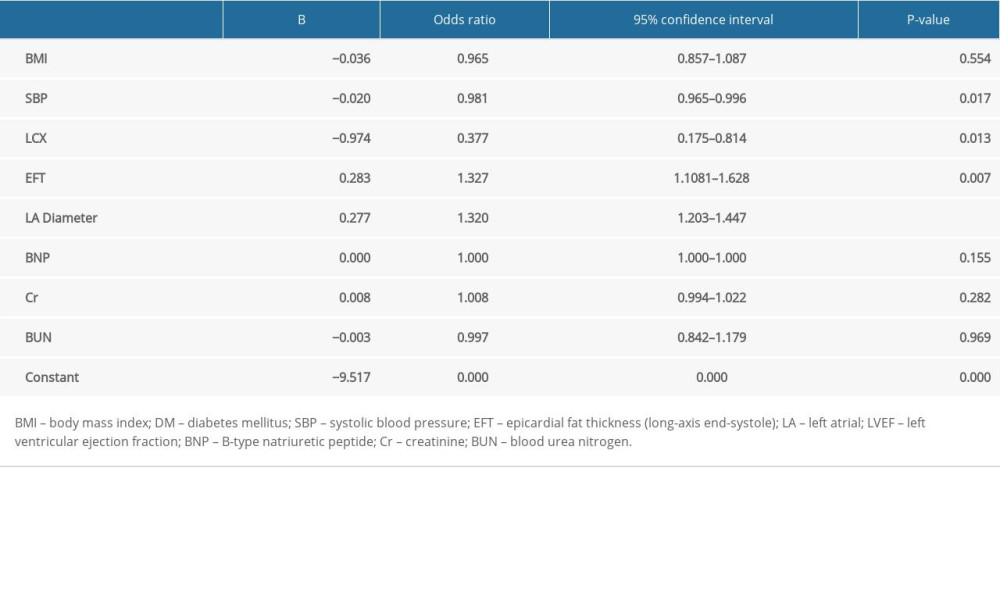
References
1. Zielonka A, Tkaczyszyn M, Mende M, Atrial fibrillation in outpatients with stable coronary artery disease: Results from the multicenter RECENT study: Pol Arch Med Wewn, 2015; 125(3); 162-71
2. Schmitt J, Duray G, Gersh BJ, Hohnloser SH, Atrial fibrillation in acute myocardial infarction: A systematic review of the incidence, clinical features and prognostic implications: Eur Heart J, 2009; 30(9); 1038-45
3. Nakamori S, Nezafat M, Ngo LH, Left atrial epicardial fat volume is associated with atrial fibrillation: A prospective cardiovascular magnetic resonance 3D Dixon study: J Am Heart Assoc, 2018; 7(6); e008232
4. Zhu J, Yang Z, Chen X, A stronger association of epicardial fat volume with non-valvular atrial fibrillation than measures of general obesity in Chinese patients undergoing computed tomography coronary angiography: Diabetes Metab Syndr Obes, 2021; 14; 1223-32
5. Yorgun H, Canpolat U, Aytemir K, Association of epicardial and peri-atrial adiposity with the presence and severity of non-valvular atrial fibrillation: Int J Cardiovasc Imaging, 2015; 31(3); 649-57
6. Ansaldo AM, Montecucco F, Sahebkar A, Epicardial adipose tissue and cardiovascular diseases: Int J Cardiol, 2019; 278; 254-60
7. Zghaib T, Ipek EG, Zahid S, Association of left atrial epicardial adipose tissue with electrogram bipolar voltage and fractionation: Electrophysiologic substrates for atrial fibrillation: Heart Rhythm, 2016; 13(12); 2333-39
8. Jhuo SJ, Hsieh TJ, Tang WH, The association of the amounts of epicardial fat, P wave duration, and PR interval in electrocardiogram: J Electrocardiol, 2018; 51(4); 645-51
9. Balcioğlu AS, Çiçek D, Akinci S, Arrhythmogenic evidence for epicardial adipose tissue: Heart rate variability and turbulence are influenced by epicardial fat thickness: Pacing Clin Electrophysiol, 2015; 38(1); 99-106
10. Romanov A, Minin S, Nikitin N, The relationship between global cardiac and regional left atrial sympathetic innervation and epicardial fat in patients with atrial fibrillation: Ann Nucl Med, 2021; 35(10); 1079-88
11. Ghaderi F, Eshraghi A, Shamloo AS, Mousavi S, Association of epicardial and pericardial fat thickness with coronary artery disease: Electronic Physician, 2016; 8(9); 2982-89
12. Nakanishi K, Fukuda S, Tanaka A, Peri-atrial epicardial adipose tissue is associated with new-onset nonvalvular atrial fibrillation: Circ J, 2012; 76(12); 2748-54
13. Thanassoulis G, Massaro JM, O’Donnell CJ, Pericardial fat is associated with prevalent atrial fibrillation: The Framingham Heart Study: Circ Arrhythm Electrophysiol, 2010; 3(4); 345-50
14. Wong CX, Abed HS, Molaee P, Pericardial fat is associated with atrial fibrillation severity and ablation outcome: J Am Coll Cardiol, 2011; 57(17); 1745-51
15. Lang RM, Badano LP, Mor-Avi V, Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging: J Am Soc Echocardiogr, 2015; 28(1); 1-39e14
16. Eroğlu S, How do we measure epicardial adipose tissue thickness by transthoracic echocardiography?: Anatol J Cardiol, 2015; 15(5); 416-19
17. January CT, Wann LS, Alpert JS, 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society [published correction appears in J Am Coll Cardiol. 2014;64(21):2305–7]: J Am Coll Cardiol, 2014; 64(21); e1-e76
18. Sacks HS, Fain JN, Human epicardial adipose tissue: A review: Am Heart J, 2007; 153; 907-17
19. Lacobellis G, Corradi D, Sharma AM, Epicardial adipose tissue: Anatomic, biomolecular and clinical relationships with the heart. Nature clinical practice: Nat Clin Pract Cardiovasc Med, 2005; 2(10); 536-43
20. Ansaldo AM, Montecucco F, Sahebkar A, Epicardial adipose tissue and cardiovascular diseases: Int J Cardiol, 2019; 278; 254-60
21. Aribas A, Akilli H, Kayrak M, Echocardiographic epicardial fat thickness in patients with paroxysmal atrial fibrillation: Exp Clin Cardiol, 2014; 20; 3574-86
22. Zhu J, Yang Z, Chen X, A stronger association of epicardial fat volume with non-valvular atrial fibrillation than measures of general obesity in chinese patients undergoing computed tomography coronary angiography: Diabetes Metab Syndr Obes, 2021; 14; 1223-32
23. Goldenberg GR, Hamdan A, Barsheshet A, Epicardial fat and the risk of atrial tachy-arrhythmia recurrence post pulmonary vein isolation: A computed tomography study: Int J Cardiovasc Imaging, 2021; 37(9); 2785-90
24. Sepehri Shamloo A, Dagres N, Dinov B, Is epicardial fat tissue associated with atrial fibrillation recurrence after ablation? A systematic review and meta-analysis: Int J Cardiol Heart Vasc, 2019; 22; 132-38
25. Al Chekakie MO, Welles CC, Metoyer R, Pericardial fat is independently associated with human atrial fifibrillation: J Am Coll Cardiol, 2010; 56; 784-88
26. Wong CX, Sun MT, Odutayo A, Associations of epicardial, abdominal, and overall adiposity with atrial fibrillation: Circ Arrhythm Electrophysiol, 2016; 9(12); e004378
27. Mahabadi AA, Lehmann N, Kälsch H, Association of epicardial adipose tissue and left atrial size on non-contrast CT with atrial fibrillation: the Heinz Nixdorf Recall Study: Eur Heart J Cardiovasc Imaging, 2014; 15; 863-69
28. Zaghloul A, Iorgoveanu C, Balakumaran K, Limitations of coronary computed tomography angiography in predicting acute coronary syndrome in a low to intermediate-risk patient with chest pain: Cureus, 2018; 10(5); e2649
29. Gunturk EE, Topuz M, Serhatlioğlu F, Akkaya H, Echocardiographically measured epicardial fat predicts new-onset atrial fibrillation after cardiac surgery: Braz J Cardiovasc Surg, 2020; 35(3); 339-45
30. Hwang HJ, Ha JW, Joung B, Relation of inflammation and left atrial remodeling in atrial fibrillation occurring in early phase of acute myocardial infarction: Int J Cardiol, 2011; 146(1); 28-31
31. Kranert M, Shchetynska-Marinova T, Liebe V, Recurrence of atrial fibrillation in dependence of left atrial volume index: In Vivo, 2020; 34(2); 889-96
32. Njoku A, Kannabhiran M, Arora R, Left atrial volume predicts atrial fibrillation recurrence after radiofrequency ablation: A meta-analysis: Europace, 2018; 20(1); 33-42
33. Stamboul K, Zeller M, Fauchier L, Incidence and prognostic significance of silent atrial fibrillation in acute myocardial infarction: Int J Cardiol, 2014; 174(3); 611-17
34. Olbers J, Jacobson E, Viberg F, Systolic blood pressure increases in patients with atrial fibrillation regaining sinus rhythm after electrical cardioversion: J Clin Hypertens (Greenwich), 2019; 21(3); 363-68
35. Aitken-Buck HM, Moharram M, Babakr AA, Relationship between epicardial adipose tissue thickness and epicardial adipocyte size with increasing body mass index: Adipocyte, 2019; 8(1); 412-20
36. Aune D, Sen A, Schlesinger S, Body mass index, abdominal fatness, fat mass and the risk of atrial fibrillation: A systematic review and dose-response meta-analysis of prospective studies: Eur J Epidemiol, 2017; 32(3); 181-92
37. Mora S, Yanek LR, Moy TF, Interaction of body mass index and Framingham risk score in predicting incident coronary disease in families: Circulation, 2005; 111(15); 1871-76
38. Chen X, Wu M, Xu K, Effects of body mass index and gender on left atrial size in Chinese hypertensive patients: Clin Exp Hypertens, 2020; 42(8); 714-21
39. Huang G, Parikh PB, Malhotra A, Relation of body mass index and gender to left atrial size and atrial fibrillation: Am J Cardiol, 2017; 120(2); 218-22
40. Plitt DC, Chung EH, Mounsey JP, Relation of atrial fibrillation burden and N-terminal pro-brain natriuretic peptide: Am J Cardiol, 2013; 111(9); 1315-18
41. Gao X, Zeng R, Liao P, Relation of N-terminal pro-brain natriuretic peptide and new-onset atrial fibrillation in patients with acute coronary syndrome: A systematic review and meta-analysis: Scand J Clin Lab Invest, 2016; 76(6); 460-64
42. Chen SC, Chang JM, Tsai YC, Left atrial diameter and albumin with renal outcomes in chronic kidney disease: Int J Med Sci, 2013; 10(5); 575-84
43. Akgul E, Parlar AI, Erkul GSA, Investigation of the effect of preoperative hypoalbuminemia, blood urea nitrogen and creatinine levels on postoperative atrial fibrillation on off-pump coronary bypass surgery patients: Heart Surg Forum, 2020; 23(5); E641-46
44. Couselo-Seijas M, Rodríguez-Mañero M, González-Juanatey JR, Eiras S, Updates on epicardial adipose tissue mechanisms on atrial fibrillation: Obes Rev, 2021; 22(9); e13277
Figures
 Figure 1. ECG and Holter in the detection of atrial fibrillation. (A) A representative ECG showing atrial fibrillation rhythm from a patient with permanent atrial fibrillation. (B) A selected segment of a representative Holter showing atrial fibrillation rhythm from a patient with paroxysmal atrial fibrillation.
Figure 1. ECG and Holter in the detection of atrial fibrillation. (A) A representative ECG showing atrial fibrillation rhythm from a patient with permanent atrial fibrillation. (B) A selected segment of a representative Holter showing atrial fibrillation rhythm from a patient with paroxysmal atrial fibrillation. Figure 2. Coronary angiography (CAG) in the detection of coronary artery disease. (A) Shows 80~85% stenosis (red arrow) in the proximal and mid-segment left anterior descending (LAD) and 95% stenosis (red arrow) in the proximal segment of left circumflex artery (LCX). (B) Shows 85% stenosis (red arrow) in the proximal segment of LAD and 90~95% stenosis (red arrow) in the mid-distal segment of LAD.
Figure 2. Coronary angiography (CAG) in the detection of coronary artery disease. (A) Shows 80~85% stenosis (red arrow) in the proximal and mid-segment left anterior descending (LAD) and 95% stenosis (red arrow) in the proximal segment of left circumflex artery (LCX). (B) Shows 85% stenosis (red arrow) in the proximal segment of LAD and 90~95% stenosis (red arrow) in the mid-distal segment of LAD. Figure 3. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with sinus rhythm. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view.
Figure 3. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with sinus rhythm. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view. Figure 4. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with atrial fibrillation. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view.
Figure 4. The measurement of epicardial fat thickness (EFT) by echocardiography in a patient with atrial fibrillation. Epicardial fat appears as an echo-free space between the red dashed lines. (A) EFT measured during end-diastole in the parasternal long-axis view. (B) EFT measured during end-systole in the parasternal long-axis view. (C) EFT measured during end-diastole in the parasternal short-axis view. (D) EFT measured during end-systole in the parasternal short -axis view. Figure 5. Scatter plot of LA diameter by EFT. There was no apparent correlation between LA diameter and EFT, R2=0.020. EFT – epicardial fat thickness; LA – left atrial.
Figure 5. Scatter plot of LA diameter by EFT. There was no apparent correlation between LA diameter and EFT, R2=0.020. EFT – epicardial fat thickness; LA – left atrial. Tables
 Table 1. Comparison of baseline clinical characteristics. Normally distributed variables are described as mean and standard deviation, while non-normally distributed variables are described as median. Categorical characteristics are presented as n (%).
Table 1. Comparison of baseline clinical characteristics. Normally distributed variables are described as mean and standard deviation, while non-normally distributed variables are described as median. Categorical characteristics are presented as n (%). Table 2. The vessel location and severity of coronary artery stenosis.
Table 2. The vessel location and severity of coronary artery stenosis. Table 3. Correlation analysis between variables.
Table 3. Correlation analysis between variables. Table 4. Multivariate binary logistic regression analysis among candidate variables.
Table 4. Multivariate binary logistic regression analysis among candidate variables. Table 1. Comparison of baseline clinical characteristics. Normally distributed variables are described as mean and standard deviation, while non-normally distributed variables are described as median. Categorical characteristics are presented as n (%).
Table 1. Comparison of baseline clinical characteristics. Normally distributed variables are described as mean and standard deviation, while non-normally distributed variables are described as median. Categorical characteristics are presented as n (%). Table 2. The vessel location and severity of coronary artery stenosis.
Table 2. The vessel location and severity of coronary artery stenosis. Table 3. Correlation analysis between variables.
Table 3. Correlation analysis between variables. Table 4. Multivariate binary logistic regression analysis among candidate variables.
Table 4. Multivariate binary logistic regression analysis among candidate variables. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








