14 November 2022: Clinical Research
Characteristics and Treatment of Pediatric Tracheobronchial Foreign Bodies: A Retrospective Analysis of 715 Cases
Shang Yan1ACEF, Peng Jiang1BCD, Guowei Chen1EF, Yongchao Chen1BD, Hongguang Pan1DE, Lan Li1AC, Nan Zeng2ABG*DOI: 10.12659/MSM.937928
Med Sci Monit 2022; 28:e937928
Abstract
BACKGROUND: This study aimed to analyze the clinical characteristics of tracheobronchial foreign bodies in children in Shenzhen and to explore the diagnosis and treatment methods for special cases.
MATERIAL AND METHODS: This study included a total of 715 children who were diagnosed with tracheobronchial foreign bodies at Shenzhen Children’s Hospital between October 2016 and October 2021. Data on sex, age, inducement, symptoms, foreign body type, foreign body location, foreign body retention time, foreign body history, and complications were recorded and analyzed.
RESULTS: Tracheal foreign bodies were found to occur primarily in children aged 0-2 years (90.6%). The overall incidence rates were 69.1% and 30.9% in boys and girls, respectively. Among them, 42.5% of the foreign bodies were detected in the left bronchus and 45.6% in the right bronchus. Inducements included playing while eating (n=398, 55.7%) and also crying (n=209, 29.2%). Operations were performed on 710 (99.3%) children, including 80 (11.2%) immediate surgeries and 2 tracheotomies. One child had no vital signs upon admission and died after emergency foreign body removal. All of the other children who underwent surgery recovered well postoperatively.
CONCLUSIONS: This study presents the characteristics and methods of diagnosis and treatment of tracheobronchial foreign bodies in pediatric patients in Shenzhen. Tracheobronchial foreign bodies are a major cause of accidental injury in infants and young children. In critical cases, airways should be immediately and rapidly cleared with multidisciplinary collaboration. In addition, public safety awareness should be strengthened, particularly among parents, teachers, and other child caregivers, to reduce and prevent instances of tracheobronchial foreign body accidents in children.
Keywords: Bronchial Diseases, Pediatric Emergency Medicine, Tracheal Diseases, Infant, Male, Female, Child, Humans, Child, Preschool, Bronchoscopy, Foreign Bodies, Bronchi, Trachea
Background
Foreign bodies lodged in the tracheas and bronchi of children are a common emergency in pediatric otolaryngology. A lack of timely and effective diagnosis and treatment can result in serious consequences and even death [1]. Previous studies have demonstrated that tracheobronchial foreign bodies are a major cause of accidental injury in children [2–4]. It is important to strengthen guardians’ awareness of safety measures for the prevention of these accidents and to provide timely diagnoses and treatment to reduce the mortality rate. Our understanding of this condition is gradually deepening, and its incidence and mortality rates have been significantly reduced [1,5,6]. This study aimed to analyze the characteristics of tracheobronchial foreign bodies in children in Shenzhen to provide references for clinical diagnosis, treatment, and prevention.
Material and Methods
CLINICAL DATA:
This study included a total of 715 children diagnosed with tracheobronchial foreign bodies at Shenzhen Children’s Hospital between October 2016 and October 2021. It is the only pediatric hospital in Shenzhen and serves approximately 2 650 000 children. This consisted of 494 (69.1%) boys and 221 (30.9%) girls, with an age range of 6 months to 14 years (average age, 1.54±1.79 years). Among them, 626 (87.6%) had a history of tracheobronchial foreign bodies. The longest history was 6 months, and the shortest was 1 hour. The number of children admitted within 1 day of accident occurrence was the largest (n=296, 41.7%). The foreign body retention times of children of different ages are presented in Table 1.
METHODS:
The children in this study either had a history of foreign bodies or were diagnosed when foreign bodies were detected in the trachea or bronchi via neck and chest computed tomography (CT) or fiberoptic bronchoscopy. Children with foreign bodies in the main airway or bilateral bronchi, or those with inspiratory dyspnea in calm state, underwent immediate surgery as soon as possible to remove the foreign body. Children with unilateral bronchial foreign bodies in a generally stable state underwent foreign body removal via emergency surgery after a preoperative examination. For those with underlying diseases or in poor general condition, a preoperative examination was conducted if possible, and then surgical treatment was performed after their general state was stable and surgery under general anesthesia was tolerable. For all the children in our sample, sex, age, inducement, symptoms, foreign body location, foreign body type, complications, foreign body history, foreign body retention time, and surgical methods used were recorded. Data were analyzed using the SPSS software for Windows, v. 26.0 (IBM Corp., Armonk, N.Y., USA). Data are expressed as median (interquartile) and percentages. The study complied with the principles of the Declaration of Helsinki on Biomedical Research Involving Human Subjects and was approved by the Ethics Review Board of Shenzhen Children’s Hospital (protocol number 202204102). Written informed consent was obtained from each child’s parent or supervisor.
Results
INDUCEMENTS AND CLINICAL MANIFESTATIONS:
The main inducements of tracheal foreign bodies included playing while eating and also crying. There were 398 (55.7%) cases of playing, 209 (29.2%) cases of crying, 42 (5.8%) cases of quiet state, 15 (2.1%) cases of falling, and 51 (7.2%) of unknown cause. The clinical manifestations were mainly recurrent coughing and wheezing. Coughing was detected in all 715 (100%) children, wheezing in 673 (94.1%), laryngeal obstruction in 29 (4.1%), fever in 41 (5.7%), and cyanosis in 36 (5.0%) children. The main clinical sign in auscultation was asymmetrical breathing sounds between the lungs. The rest were weakened or absent breathing sounds on the affected side (n=608, 85.0%); dry rales, wet rales, and/or coarse breathing sounds (n=446, 62.4%); and glottic flapping sounds (n=12, 1.7%). In 29 (4.1%) of the children, no obvious positive signs were heard. The majority of patients underwent a neck and chest CT scan (686, 95.9%), except for 29 children with inspiratory dyspnea in calm state, who received immediate surgery with no CT examination.
FOREIGN BODY LOCATION AND TYPE:
Among them, the foreign bodies were located in the left bronchus in 42.5% (n=304) of the patients, right bronchus in 45.6% (n=326), bilateral bronchi in 1.1% (n=8), and main airway in 10.8% (n=77).
Plant-type foreign bodies accounted for 83.6% (n=598), which included nuts (n=528, 73.8%) and fruits and vegetables (n=70, 9.8%). Among the plant-type foreign bodies, peanuts were the most common (n=278, 46.5%, Figure 1), followed by melon seeds (n=111, 18.6%, Figure 2), walnuts (n=38, 6.4%), Chinese chestnuts (n=22, 3.7%), and other nuts (n=79, 13.2%). Beans accounted for 6.0% (n=36) and other fruits and vegetables for 5.7% (n=34). Animal-type foreign bodies were detected in 46 (6.4%) children. These were mainly bone fragments (n=5, 10.9%). Other food types were detected in 7 (1.0%) children. Plastic and metal foreign bodies accounted for 9.0% (n=64), including 11 (1.5%) cases of plastic toys (Figure 3), 6 (0.8%) cases of pen heads (Figure 4), 6 (0.8%) cases of pen caps, 6 (0.8%) cases of diode bulbs, and 5 (0.7%) cases of whistles.
SURGICAL METHODS AND TRACHEAL FOREIGN BODY-RELATED COMPLICATIONS:
The foreign bodies in 710 (99.3%) of the children were removed by rigid bronchoscopy under general anesthesia; 630 (88.1%) patients underwent urgent surgery with a wait time less than 12 hours and 80 (11.2%) patients underwent immediate surgery with a wait time less than 30 minutes. Preoperatively, intramuscular injection of atropine was routinely administered, and ventilation was controlled during surgery using a high-frequency jet ventilator (ZHONGYI, China). The foreign bodies of the remaining 5 children were coughed up before surgery. This was confirmed by CT re-examination. Immediate surgery was performed on 80 (11.2%) children with inspiratory dyspnea in calm state, bilateral bronchial foreign bodies, or main airway foreign bodies. Without preoperative examination or preoperative fasting, the foreign bodies were surgically removed immediately. Among the 80 children, 5 had main airway foreign bodies. One child with a bronchial foreign body had a history of foreign body inhalation of 2 weeks to 3 months (bone fragments, n=4; shelled melon seeds, n=1). In those children whose breathing was confirmed to be even and stable, the foreign bodies were removed by general emergency surgery after preoperative examination and sufficient preoperative fasting. In 2 children, the glottis could not be passed through when clamping the foreign bodies during surgery; after tracheotomy, the foreign bodies were removed through the tracheal incision. The first of these cases was a 3-year-old boy who had accidentally inhaled a cylindrical plastic pen cap, which was stuck in the left bronchus. The second case was a 9-year-old boy who had accidentally inhaled a plastic pen head, which was stuck in the right bronchus. In both cases, the trachea was successfully blocked 10 days after surgery, and the tracheal stoma was blocked 2 days later. In the sample studied, complications included pneumonia (n=648, 90.6%), obstructive emphysema (n=511, 71.5%), and atelectasis (n=55, 7.7%). Rarer complications included pulmonary bullae (n=1, 0.14%), inflammatory pleural effusion (n=1, 0.14%), pneumothorax with mediastinal emphysema (n=1, 0.14%), and mediastinal hernia (n=1, 0.14%).
TREATMENT OUTCOMES:
A 1-year-old boy choked on grapefruit flesh for 1 hour and had no vital signs during the ambulance ride to the hospital. The patient was connected to life support and sent for emergency surgery to remove the foreign body. Despite the successful removal, he could not be revived, and his death was declared after transfer to the Pediatric Intensive Care Unit (PICU).
Intraoperative tracheotomy was performed in 2 children in whom the foreign bodies could not pass through the glottis, and the tracheal cannulas were removed after 10 days.
An 11-month-old boy with hepatic failure and a history of tracheostomy presented with dyspnea after choking on a walnut. Urgent examination revealed a foreign body in the main airway, pneumothorax, mediastinal emphysema, pneumonia, and laryngeal hyperplasia. With multidisciplinary collaboration, the foreign body was removed in immediate surgery, the laryngeal granuloma was resected, and the tracheal cannula was replaced. The patient was then transferred to the PICU. The volume of the pneumothorax was small, so thoracentesis was not performed. After surgery, the patient’s condition became stable, and the pneumothorax and mediastinal emphysema disappeared spontaneously.
A 1-year-old boy was hospitalized in the Department of Infectious Diseases due to herpangina and recurrent pulmonary infections. CT examination revealed a foreign body in the right bronchus, obstructive emphysema, and mediastinal hernia. With the assistance of thoracic surgery, the peanut in the bronchus was successfully removed by rigid bronchoscopy. The postoperative condition was stable. Postoperative CT revealed that the obstructive emphysema and mediastinal hernia were relieved.
A foreign body was detected in the left bronchus of a 1-year-old boy being treated with fiberoptic bronchoscopy for pneumonia and inflammatory pleural effusion in the Department of Internal Medicine at our hospital. After attempts to remove the foreign body by fiberoptic bronchoscopy were unsuccessful, it was successfully removed by rigid bronchoscopy performed under general anesthesia. After the surgery, medical treatment was continued, and the pleural effusion was self-absorbed.
A 1-year-old boy choked on a black soy bean for 7 days. CT examination revealed a foreign body in the left bronchus, obstructive emphysema, and pulmonary bullae, which were surgically treated. The surgery was successful, and the child was discharged after the foreign body removal. At 1-month follow-up, the pulmonary bullae had spontaneously disappeared. In this study, all but 1 child recovered well after surgery. The mortality rate was 0.14% (n=1).
Discussion
AGE AND SEX DISTRIBUTION:
This study comprised 494 (69.1%) boys and 221 (30.9%) girls (a ratio of 2.24: 1), indicating that the incidence of tracheobronchial foreign bodies is significantly higher in boys than in girls. This is consistent with most previous reports [9–11]. The age of occurrence ranged from 6 months to 14 years, with the highest risk in those aged 1–2 years and an average age of 1.54±1.79 years. There was no difference in the highest risk age for boys and girls, which is, again, in line with previous reports [12]. Sex differences in incidence rates may be related to differences in the physical and psychological development of boys and girls, as well as differences in the parenting of different genders and the sex ratio of the city’s population. According to the China’s National Bureau of Statistics in 2020, the male-to-female ratio in Shenzhen was 122.43: 100. Combined with some previous studies on digestive and otorhinolaryngeal foreign bodies, the proportion of boys is usually slightly higher than that of girls or there is no significant difference [13–20]. Gender differences in psychological development in children aged 1–3 years old do not seem to put boys at such a higher risk than girls. Therefore, differences in physiological development may also be an important reason for the obvious gender difference, and may be related to the gender differences in the development of mastication, swallowing coordination and laryngeal protection.
Th main limitation in our study is that we did not provide evidence that laryngotracheal development occurs earlier in girls than in boys. Further studies should compare sex differences in masticatory development, swallowing coordination, and laryngeal protection investigate whether there are sex differences in laryngotracheal development.
RETENTION TIME AND LOCATION OF FOREIGN BODIES:
There are many factors affecting the retention time of foreign bodies, including the age of the child, type of foreign body, and educational level of guardians [21]. The specific distributions in this study are presented in Table 1. Children younger than 1 year old and older than 6 years old have shorter foreign body retention times, perhaps because the guardians pay the greatest attention to children under 1 year old, and children above 6 years old can clearly express their discomfort and foreign body history.
Thin-slice CT is the best means of locating foreign bodies, and its accuracy can be as high as 99.4% [22–24]. We found the distribution of foreign bodies in the trachea to be slightly higher on the right, which is consistent with previous reports [25–27]. The reason for this may be related to the larger angle between the right main bronchus and main airway, which can increase the likelihood of foreign bodies entering the right side [28]. However, we found that the incidence of foreign bodies in the left bronchus of boys was higher (n=222, 44.9%) than that in girls (n=82, 37.1%). Sex differences in physiological development may make it more difficult for foreign bodies in girls to enter the airway and more likely to stay in the right bronchus after entering the airway.
FOREIGN BODY TYPE:
The most frequently seen foreign body types in this study were plant-type foreign bodies, among which peanuts and melon seeds were the most common, which is consistent with a previous report [29]. This is strongly related to dietary habits in the region studied. A study by Hongguang et al [30] on the types of tracheal foreign bodies observed in our hospital between 2004 and 2008 found a higher incidence of other nuts, such as Chinese chestnuts, pine nuts, pecans, and especially walnuts, which increased from no cases to 38 cases (5.3%). This is related to the acceleration of economic development and the current large-scale popularization of various nuts that used to be expensive. Among plastic and metal foreign bodies, the increase in cases of diode bulbs is related to the current popularity of diode bulbs.
COMPLICATIONS OF TRACHEOBRONCHIAL FOREIGN BODIES:
In this study, 511 (71.5%) children experienced obstructive emphysema, and 55 (7.7%) had atelectasis. When children with no known history of foreign bodies present with comorbid long-term pulmonary infection, it is important to be vigilant against endogenous foreign bodies. Previous reports have suggested that almost all plastic bronchitis is accompanied by atelectasis or pulmonary consolidation [31, 32]. In this study, the cases of obstructive emphysema and atelectasis were spontaneously relieved after the foreign bodies were removed. Another common complication was bronchopneumonia, which was seen in 648 (90.6%) of the children, with only 67 (9.4%) having no obvious pneumonia on CT examination; 27 of this latter group suffered from main airway foreign bodies. Since this is apparent, there is generally a shorter period of foreign body incarceration, reducing local intrapulmonary stimulation caused by foreign bodies like plastic, metal, and bone fragments. Rarer complications observed in this study were pulmonary bulla (n=1, 0.14%), pleural effusion (n=1, 0.14%), pneumothorax with mediastinal emphysema (n=1, 0.14%), and mediastinal hernia (n=1, 0.14%), all of which appeared before surgery, with mild symptoms. After evaluation of their condition and surgical risk, their foreign bodies were removed via rigid bronchoscopy under general anesthesia, and these conditions were alleviated spontaneously without surgical intervention.
SURGICAL METHODS:
In this study, all but 2 children were treated with foreign body removal
When the foreign body was found to be a nut, such as a peanut, located in a unilateral bronchus, and there was a small gap between the foreign body and tracheal wall, a rigid bronchoscope of appropriate size was guided to the upper part of the foreign body. The tracheoscope was rotated and pushed in slowly, which caused the foreign body to enter the bronchoscope. The mucus on the surface of the foreign body would then cause it to adhere to the bronchoscope wall. The foreign body could then be removed by slowly withdrawing the bronchoscope. This method avoided crushing the foreign body with forceps and shortened the surgical duration; however, this method has the potential to push the foreign body deeper into the airway.
For foreign bodies with holes, such as pen heads, those with large holes can be pulled out by opening the foreign body forceps after passing through the hole in the occlusal state and withdrawing from the airway using the bronchoscope (Figure 5). Plastic toys or ornaments with small holes could be pulled out by passing a long metal guidewire with a bent head through the hole, clamping the tail end of the foreign body, and subsequently withdrawing it from the airway with the bronchoscope (Figure 6).
Diode bulbs have 2 lead frames, which are relatively sharp and not usually in a straight line. Therefore, they can easily damage the tracheal wall and glottis when clamped during surgery. If there was difficulty removing these, we would sometimes break them into smaller parts, removing the lead frames after breaking.
For the foreign bodies located in the segmental bronchus and below the segmental bronchus, digestive endoscopic biopsy forceps for children were used. The head of these forceps is smaller than that of foreign body forceps, and the guidewire can be bent. Using an endoscope for visualization by assistants, the biopsy forceps were directed into the deep bronchus along the rigid bronchoscope to clamp the foreign body. This method requires highly proficient assistants; otherwise, the foreign bodies may be pushed deeper.
Conclusions
This study objectively analyzes the characteristics, diagnosis, and treatment of tracheobronchial foreign bodies in Shenzhen. Tracheobronchial foreign bodies are a common but serious form of injury in infants and young children. For critical cases, treatment should be immediately and rapidly given with multidisciplinary collaboration, and a personalized treatment plan should be rapidly developed to avoid further deterioration. Further study is needed, and public awareness needs to be strengthened to reduce the incidence of tracheobronchial foreign bodies in children.
Figures
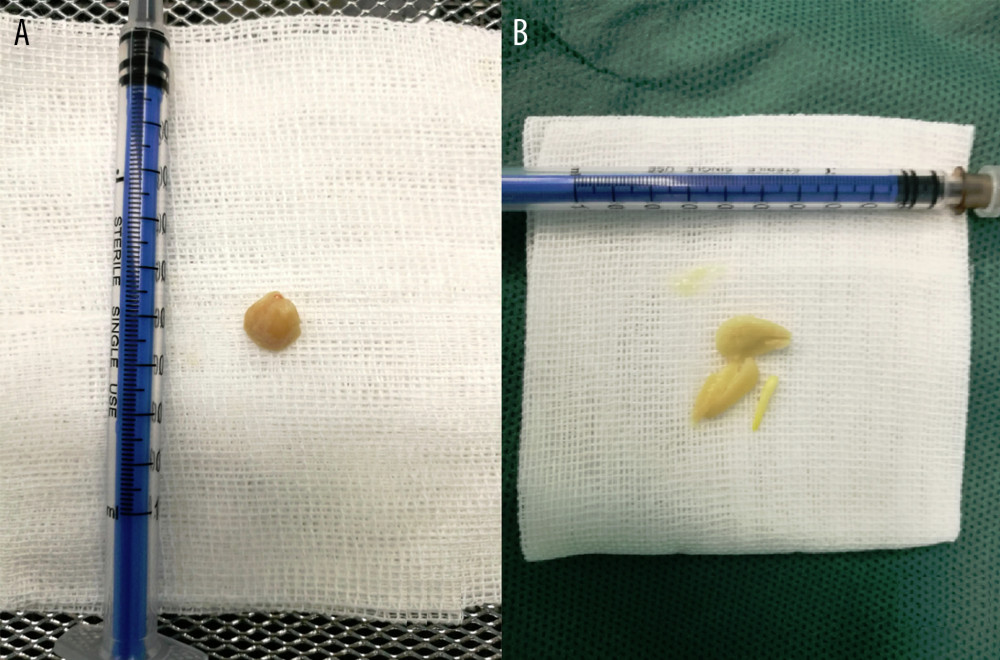 Figure 1. Both (A) and (B) are peanuts removed from the bronchus.
Figure 1. Both (A) and (B) are peanuts removed from the bronchus. 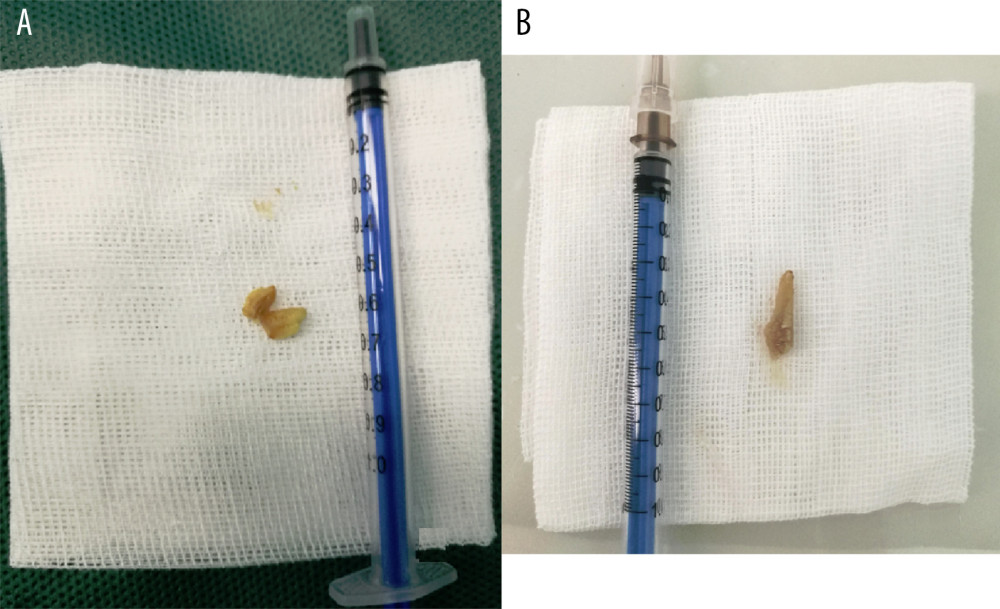 Figure 2. Both (A) and (B) are melon seeds removed from the bronchus.
Figure 2. Both (A) and (B) are melon seeds removed from the bronchus. 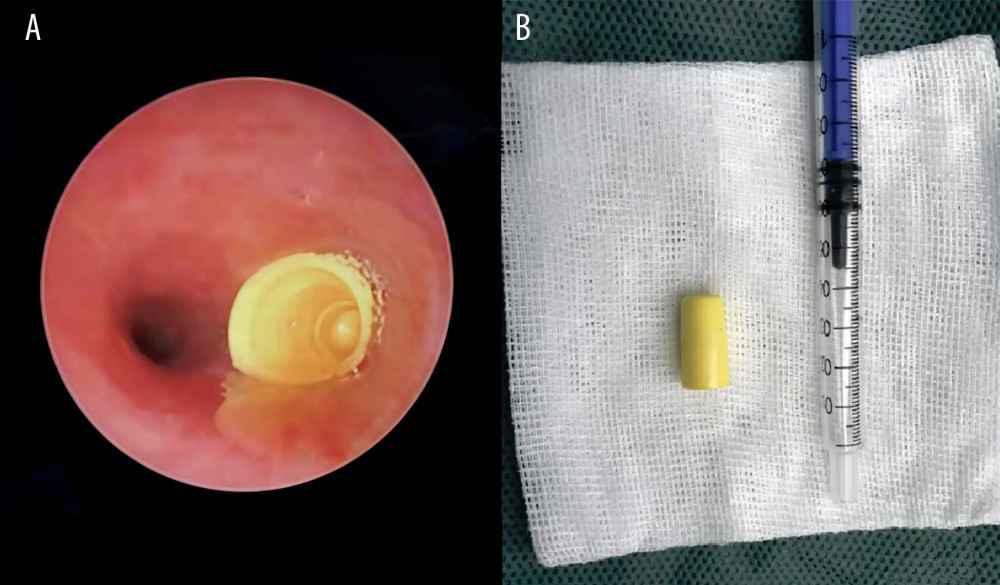 Figure 3. (A) Intraoperative photograph of a plastic toy located in right bronchus. (B) Postoperative photograph of the plastic toy.
Figure 3. (A) Intraoperative photograph of a plastic toy located in right bronchus. (B) Postoperative photograph of the plastic toy. 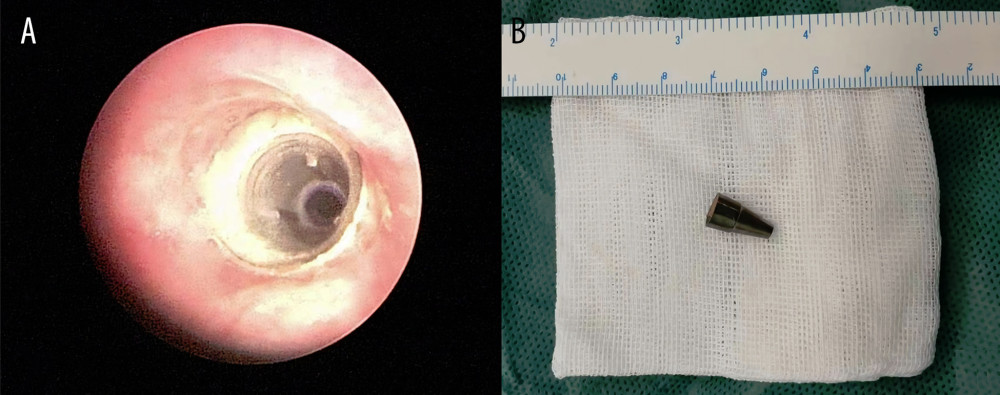 Figure 4. (A) Intraoperative photograph of a pen head located in right bronchus. (B) Postoperative photograph of the pen head.
Figure 4. (A) Intraoperative photograph of a pen head located in right bronchus. (B) Postoperative photograph of the pen head. 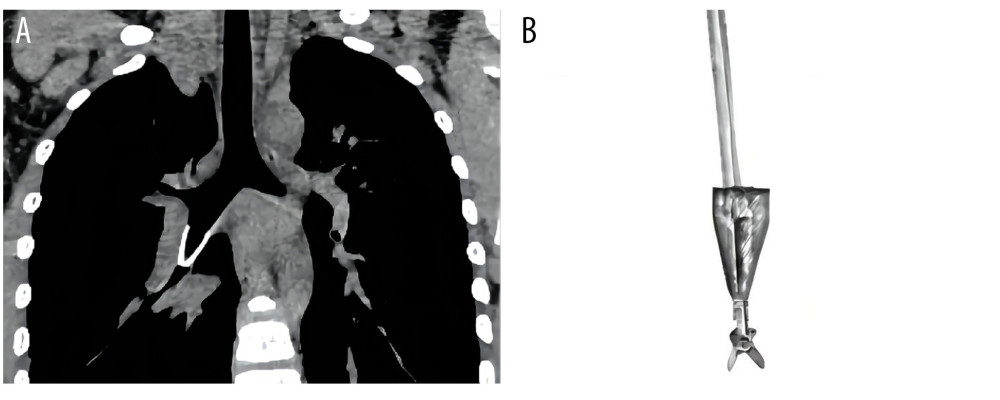 Figure 5. (A) A pen head with large holes located in right bronchus. (B) Opening the foreign body forceps after passing through the hole in the occlusal state (Photoshop, 2020, Adobe).
Figure 5. (A) A pen head with large holes located in right bronchus. (B) Opening the foreign body forceps after passing through the hole in the occlusal state (Photoshop, 2020, Adobe). 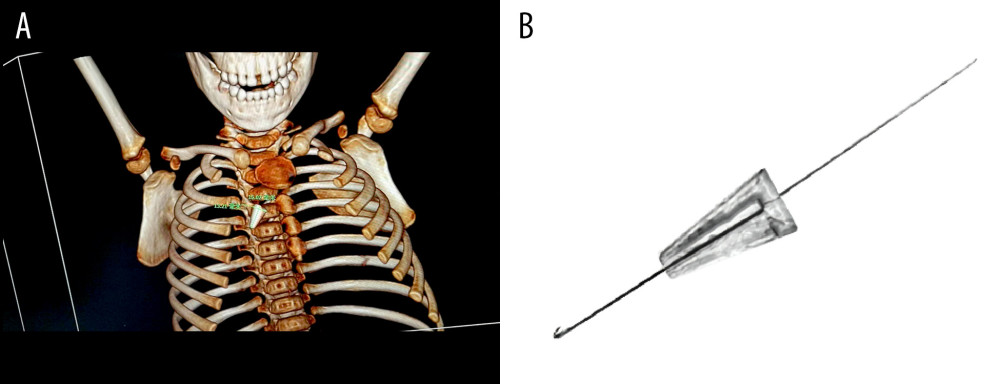 Figure 6. (A) A tapered plastic ornament located in right bronchus. (B) Passing a long metal guidewire with a bent head through the hole, clamping the tail end of the foreign body (Photoshop, 2020, Adobe).
Figure 6. (A) A tapered plastic ornament located in right bronchus. (B) Passing a long metal guidewire with a bent head through the hole, clamping the tail end of the foreign body (Photoshop, 2020, Adobe). References
1. Powers KF, Reese AD, Carr MM, Pediatric bronchoscopy for airway foreign bodies in the ACS NSQIP-P: Morbidity and mortality 2014–2019: Laryngoscope, 2022 [Online ahead of print]
2. Wu X, Wu L, Chen Z, Zhou Y, Fatal choking in infants and children treated in a pediatric intensive care unit: A 7-year experience: Int J Pediatr Otorhinolaryngol, 2018; 110; 67-69
3. Foltran F, Ballali S, Rodriguez H, Inhaled foreign bodies in children: A global perspective on their epidemiological, clinical, and preventive aspects: Pediatr Pulmonol, 2013; 48(4); 344-51
4. Eren S, Balci AE, Dikici B, Foreign body aspiration in children: Experience of 1160 cases: Ann Trop Paediatr, 2003; 23(1); 31-37
5. Zhang J, Zhang YMHow to reduce the incidence of complication and mortality in pediatric tracheobronchial foreign body patients: Zhonghua Er Bi Yan Hou Ke Za Zhi, 2004; 39(11); 658-62 [in Chinese]
6. Johnson K, Linnaus M, Notrica D, Airway foreign bodies in pediatric patients: Anatomic location of foreign body affects complications and outcomes: Pediatr Surg Int, 2017; 33(1); 59-64
7. Committee on Injury, Violence, and Poison Prevention, Prevention of choking among children: Pediatrics, 2010; 125(3); 601-7
8. Lorenzoni G, Lanera C, Azzolina D, Assessing school-based intervention strategies to foster the prevention of choking injuries in children: The results of the CHOP (CHOking Prevention) trial: Health Soc Care Community, 2021; 29(6); 1858-67
9. Cheng J, Liu B, Farjat AE, Routh J, National estimations of airway foreign bodies in children in the United States, 2000 to 2009: Clin Otolaryngol, 2019; 44(3); 235-39
10. Gregori D, Salerni L, Scarinzi C, Foreign bodies in the upper airways causing complications and requiring hospitalization in children aged 0–14 years: Results from the ESFBI study: Eur Arch Otorhinolaryngol, 2008; 265(8); 971-78
11. Wanstreet T, Ramadan J, Carr MM, Airway foreign bodies in pediatric patients: An analysis of composition and age via HCUP KID: Int J Pediatr Otorhinolaryngol, 2021; 142; 110559
12. Ding G, Wu B, Vinturache A, Tracheobronchial foreign body aspiration in children: A retrospective single-center cross-sectional study: Medicine (Baltimore), 2020; 99(22); e20480
13. Chinski A, Foltran F, Gregori D, Foreign bodies in children: A comparison between Argentina and Europe: Int J Pediatr Otorhinolaryngol, 2012; 76(Suppl 1); S76-79
14. Sarafoleanu C, Ballali S, Gregori D, Retrospective study on Romanian foreign bodies injuries in children: Int J Pediatr Otorhinolaryngol, 2012; 76(Suppl 1); S73-75
15. Yan S, Zeng N, Chen G, Presentation and management of nasal foreign bodies in a Chinese metro area: Medicine (Baltimore), 2021; 100(16); e25626
16. Ngo A, Ng KC, Sim TP, Otorhinolaryngeal foreign bodies in children presenting to the Emergency Department: Singapore Med J, 2005; 46(4); 172-78
17. Eskander AE, Sawires HK, Ebeid BA, Foreign body ingestion in Egyptian children: A 10-year experience of endoscopic intervention in a tertiary hospital: Minerva Pediatr, 2019; 71(5); 443-48
18. Leskova J, Stichhauer R, Preis J, Foreign body ingestion in children: Rozhl Chir, 2019; 98(9); 370-74
19. Wood ML, Potnuru PP, Nair S, Inpatient pediatric foreign body ingestion: National estimates and resource utilization: J Pediatr Gastroenterol Nutr, 2021; 73(1); 37-41
20. Orsagh-Yentis D, McAdams RJ, Roberts KJ, McKenzie LB, Foreign-body ingestions of young children treated in US Emergency Departments: 1995–2015: Pediatrics, 2019; 143(5); e20181988
21. Zhou J, Shang WY, Huang ZH, Influential factors for visit time for tracheobronchial foreign bodies in pediatrics: Eur Arch Otorhinolaryngol, 2020; 277(2); 505-9
22. Hegde SV, Hui PK, Lee EY, Tracheobronchial foreign bodies in children: Imaging assessment: Semin Ultrasound CT MR, 2015; 36(1); 8-20
23. Liang J, Hu J, Chang H, Tracheobronchial foreign bodies in children – a retrospective study of 2,000 cases in Northwestern China: Ther Clin Risk Manag, 2015; 11; 1291-95
24. Wang Y, Sun Y, Zhang H, Comprehensive analysis of the diagnosis and treatment of tracheobronchial foreign bodies in children: Ear Nose Throat J, 2021 [Online ahead of print]
25. Chouhan M, Sharma S, Tracheobronchial foreign bodies: The importance of timely intervention and appropriate collaboration: Indian J Otolaryngol Head Neck Surg, 2019; 71(Suppl 1); 972-75
26. Haddadi S, Marzban S, Nemati S, Tracheobronchial foreign-bodies in children; A 7 year retrospective study: Iran J Otorhinolaryngol, 2015; 27(82); 377-85
27. Sumanth TJ, Bokare BD, Mahore DM, Management of tracheobronchial foreign bodies: A retrospective and prospective study: Indian J Otolaryngol Head Neck Surg, 2014; 66(Suppl 1); 60-64
28. Experts consensus on diagnosis and treatment of tracheobronchial foreign bodies in children: Zhonghua Er Bi Yan Hou Tou Jing Wai Ke Za Zhi, 2018; 53(5); 325-38 [in Chinese]
29. Gang W, Zhengxia P, Hongbo L, Diagnosis and treatment of tracheobronchial foreign bodies in 1024 children: J Pediatr Surg, 2012; 47(11); 2004-10
30. Pan H, Li L, Liang Z, Wu ZClinical analysis on 368 children cases with tracheobronchial foreign body: Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi, 2010; 24(12); 544-46 [in Chinese]
31. Ntiamoah P, Mukhopadhyay S, Ghosh S, Mehta AC, Recycling plastic: Diagnosis and management of plastic bronchitis among adults: Eur Respir Rev, 2021; 30(161); 210096
32. Huang JJ, Yang XQ, Zhuo ZQ, Yuan L, Clinical characteristics of plastic bronchitis in children: A retrospective analysis of 43 cases: Respir Res, 2022; 23(1); 51
Figures
 Figure 1. Both (A) and (B) are peanuts removed from the bronchus.
Figure 1. Both (A) and (B) are peanuts removed from the bronchus. Figure 2. Both (A) and (B) are melon seeds removed from the bronchus.
Figure 2. Both (A) and (B) are melon seeds removed from the bronchus. Figure 3. (A) Intraoperative photograph of a plastic toy located in right bronchus. (B) Postoperative photograph of the plastic toy.
Figure 3. (A) Intraoperative photograph of a plastic toy located in right bronchus. (B) Postoperative photograph of the plastic toy. Figure 4. (A) Intraoperative photograph of a pen head located in right bronchus. (B) Postoperative photograph of the pen head.
Figure 4. (A) Intraoperative photograph of a pen head located in right bronchus. (B) Postoperative photograph of the pen head. Figure 5. (A) A pen head with large holes located in right bronchus. (B) Opening the foreign body forceps after passing through the hole in the occlusal state (Photoshop, 2020, Adobe).
Figure 5. (A) A pen head with large holes located in right bronchus. (B) Opening the foreign body forceps after passing through the hole in the occlusal state (Photoshop, 2020, Adobe). Figure 6. (A) A tapered plastic ornament located in right bronchus. (B) Passing a long metal guidewire with a bent head through the hole, clamping the tail end of the foreign body (Photoshop, 2020, Adobe).
Figure 6. (A) A tapered plastic ornament located in right bronchus. (B) Passing a long metal guidewire with a bent head through the hole, clamping the tail end of the foreign body (Photoshop, 2020, Adobe). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387









![Comparision of foreign body retention time in different age groups [n (%)].](https://jours.isi-science.com/imageXml.php?i=t1-medscimonit-28-e937928.jpg&idArt=937928&w=1000)