17 May 2023: Clinical Research
Management of Unstable C1 Fractures Involving the Lateral Mass: Posterior C1–C2 Screw-Rod Fixation and Fusion
Xiaobao Zou1BDE, Haozhi Yang1BC, Chenfu Deng1CF, Junlin Chen1BF, Rencai Ma1CF, Xiangyang Ma1AG*, Hong Xia1ADOI: 10.12659/MSM.938600
Med Sci Monit 2023; 29:e938600
Abstract
BACKGROUND: Although most unstable C1 fractures can be effectively treated either by conservative treatment with external immobilization or by surgical procedure of C1-ring osteosynthesis, those fractures involving the lateral mass are likely to lead to traumatic arthritis and persistent neck pain. Specific reports of treatment of unstable C1 fractures involving the lateral mass are still scarce. We therefore present this report to evaluate the effectiveness of posterior C1-C2 screw-rod fixation and fusion for unstable C1 fractures involving the lateral mass.
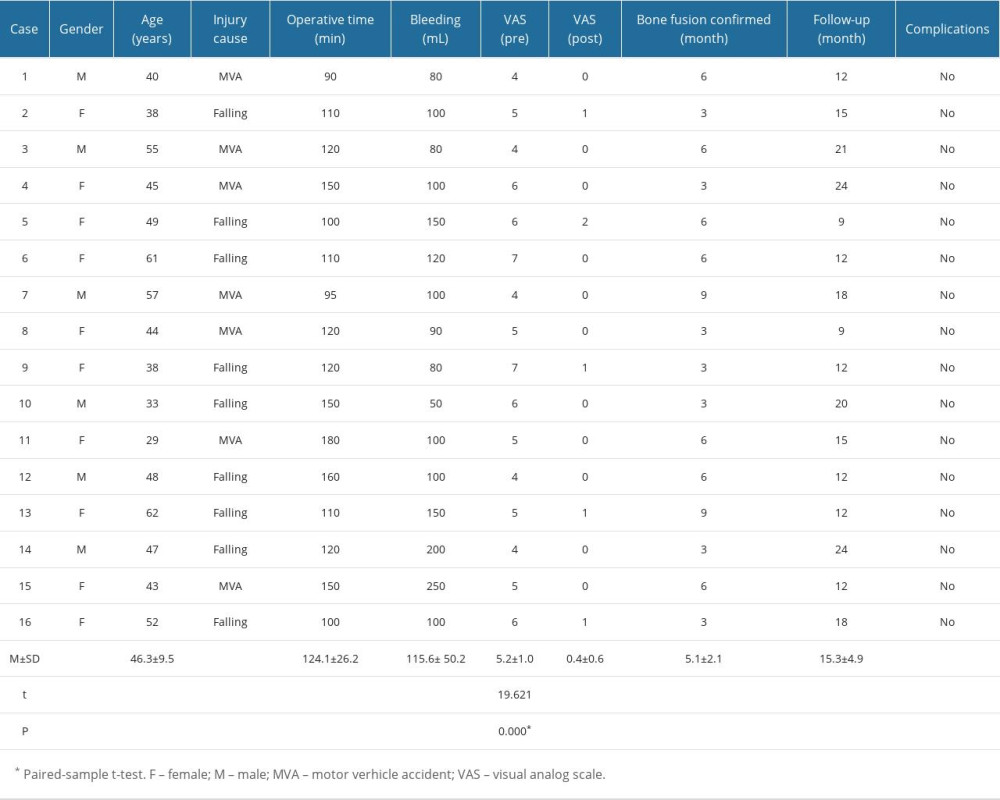
MATERIAL AND METHODS: From June 2009 to June 2016 in our hospital, 16 cases were diagnosed with C1 fractures involving the lateral mass and treated by posterior C1-C2 screw-rod fixation and fusion. The patients’ clinical data were retrospectively analyzed. Preoperative and postoperative images were taken to evaluate cervical sequence, location of screws, and bone fusion. Neurological status and neck pain levels were evaluated clinically on follow-up.
RESULTS: All patients underwent surgery successfully. The mean follow-up duration was 15.3±4.9 months (range 9-24 months). All patients obtained satisfying clinical outcomes with good neck pain alleviation, appropriate screw placement, and reliable bone fusion. None of the patients developed vascular or neurological complications during the operation or follow-up.
CONCLUSIONS: Posterior C1-C2 screw-rod fixation and fusion is an effective management for unstable C1 fractures involving the lateral mass. This operation can provide reliable stabilization and satisfactory bone fusion.
Keywords: Atlas, Internal fracture fixation, Spinal Fractures, Spinal Fusion, Cervical Vertebrae, Bone Screws, Fracture Fixation, Internal, Retrospective Studies, Treatment Outcome, Cervical Atlas, Humans, Male, Female, Adult, Middle Aged
Background
C1 fractures account for 2–13% of all cervical spine fractures and 1–2% of all spinal fractures [1,2]. Although there is a consensus on the treatment of stable C1 fractures, the optimal treatment of unstable C1 fractures is controversial. Nonsurgical management of unstable C1 fractures has poor reduction and high rates of non-union [3]. C1-ring osteosynthesis can provide immediate reduction and preserve C1–C2 motion for fractures of C1 anterior arch and posterior arch [2,4,5]. However, for unstable C1 fractures involving the lateral mass, C1-ring osteosynthesis could not offer ideal reduction of fractures of the lateral mass effectively, which can result in traumatic arthrosis, chronic neck pain, and even atlantoaxial instability [6]. Nevertheless, there are few related reports about the treatment of unstable C1 fractures involving the lateral mass.
In present study, 16 patients with unstable C1 fracture involving the lateral mass who were treated by posterior C1–C2 screw-rod fixation and fusion were selected and the clinical data were retrospectively analyzed to evaluate the effectiveness of this surgical management.
Material and Methods
PATIENT DATA:
From June 2009 to June 2016, 16 consecutive patients with unstable C1 fractures involving the lateral mass, including 6 men and 10 women, were recruited. Posterior C1–C2 screw-rod fixation and fusion was performed on each case. The average age was 46.3±9.5 years (range 29–62 years). The history includes injuries from falls (9 cases) and motor vehicle accidents (7 cases). All patients were conscious and cooperative and presented with neck pain and restricted motion of the cervical spine without neurological symptoms.
Routine preoperative cervical anteroposterior and lateral X-rays, computed tomography (CT) with three-dimensional reconstruction, and magnetic resonance imaging (MRI) of each case were collected. Fractures of the anterior and posterior atlantal arches involving the lateral mass in all patients were confirmed by CT (Figure 1). Transverse atlantal ligament (TAL) injury was found in 10 patients by MRI or CT images, including 3 cases with Dickman type I TAL injury and 7 cases with Dickman type II TAL injury.
SURGICAL PROCEDURE:
Preoperative preparation: Skull traction was performed in each case for 1 week with a weight of 3–4 kg. Intravenous prophylactic broad-spectrum antibiotics were routinely administered 30 minutes before surgery.
Surgical technique: After general anesthesia, the patient was placed in the prone position with moderate cervical flexion. Skull traction was performed, maintaining a weight of 3–4 kg. A longitudinal posterior midline incision was performed from the superoccipital part to the C2 spinous process. The occipital bone, the posterior arch of C1, and the lateral mass of C2 were exposed by subperiosteal dissection. Then, a C1 pedicle screw or a lateral mass screw was inserted, with priority of C1 pedicle screw. The entry points of C1 pedicle screws were ascertained using the C2 lateral mass as a landmark, assuring that they were aligned with the center of the C2 lateral mass and at least 3 mm below the superior rim of the C1 posterior arch [7]. If the C1 posterior arch was too thin and less than 2.0 mm in height, a C1 lateral mass screw was placed according to the technique described by Goel and Harms [8,9]. The C2 pedicle screw was the preferred type of C2 screw. Its entry point was in the superior and medial quadrant of the C2 lateral mass, and screw was inserted under direct sight followed by exposing the upper edge of the C2 lamina and the inner edge of the arch. If the placement of C2 pedicle screws was unsafe due to the anatomical variations, C2 translaminar screws were used instead [10]. After accomplishing the placement of all screws, the patient’s head was raised to restore natural cervical curvature, and then the rods were loaded into the C1 and C2 screw heads on both sides and locked. After good placement of internal fixation and cervical alignment were confirmed by C-arm X-ray, the autogenous bone grafting was performed. A drainage tube was then placed, and the incision was closed layer by layer.
POSTOPERATIVE MANAGEMENT AND FOLLOW-UP:
The drainage tube was removed 48 h after surgery. Cervical X-ray and CT scans were obtained 3 days postoperatively to assess the position of internal fixation. A rigid cervical collar was used for external immobilization for 3 months after surgery. Patients were followed up at 3, 6, 9, and 12 months and then once per year or whenever needed. The level of neck pain was evaluated by visual analog scale (VAS) score. The neurological status also was recorded. All patients underwent cervical X-ray and CT scans at each follow-up. Bone fusion was assessed by CT scan.
STATISTICAL ANALYSIS:
All data are expressed as the mean and standard deviation. The paired-samples
Results
All 16 patients underwent the operation successfully. No neurovascular injury occurred during the procedure. The average operative time was 124.1±26.2 minutes (range 90.0–180.0 minutes), with a mean intraoperative blood loss of 115.6±50.2 mL (range 50.0–250.0 mL). Postoperative X-ray and CT scan revealed proper position of internal fixation in all patients (Figure 2). The average follow-up time was 15.3±4.9 months (range 9.0–24.0 months). A similar level of neurological function was found in all cases. Neck pain was relieved in all patients after operations. Postoperative VAS scores (mean 0.4±0.6; range 0.0–2.0) were significantly lower than preoperative VAS score (mean 5.1±1.0; range 4.0–7.0;
Discussion
The atlas, the first cervical vertebra, is formed by the anterior and posterior arches and the 2 lateral masses without vertebral body and spinous process. Most C1 fractures occur in the ring structure, because the weakest points of C1 are the regions where the anterior and posterior arches connect with the lateral masses [11]. Historically, the integrity of the TAL is the main basis for the judgment of the stability of C1 fractures, and the C1 burst fracture with concomitant injury of TAL are regarded as unstable fracture [2]. In addition, sagittal split lateral mass fractures have also been considered unstable due to the lateral displacement of the fractured lateral mass [12]. However, it is currently considered that all C1 fractures are unstable except for single anterior arch fracture or posterior arch fracture without TAL rupture [13,14], which reveals that the integrity of the TAL is no longer the primary criterion for determining the stability of the C1 fracture. In this study, all patients had fractures of the anterior arch, posterior arch, and unilateral lateral mass, which were considered unstable C1 fractures.
Very few patients with C1 fractures have neurological symptoms because fractures of the C1 ring or lateral mass increase the space of spinal canal that is available for the spinal cord, thereby inhibiting compression [15]. Therefore, the most important management for C1 fractures is stabilization. Previously, conservative treatment with skull traction, followed by external halo-vest immobilization, was commonly recommended for unstable C1 fractures [16]. However, the poor efficacy of restoring fracture and maintaining reduction provided by nonsurgical treatments may lead to a high risk of non-union [3]. Moreover, unstable C1 fractures involving the lateral mass can lead to severe instability of C1–C2, which can result in arthrosis and persistent neck pain [6]. Rransford et al [12] retrospectively analyzed 10 patients with longitudinal split fracture of the C1 lateral mass, and clinical outcomes revealed that 3 patients had delayed upper cervical deformity after external cervical collar or halo-vest immobilization. Dvorak et al [17] prospectively analyzed 22 patients with C1 burst fracture, revealing the failure of preoperative function recovery after nonsurgical treatments, which suggested nonsurgical management was not the optimal option.
Presently, clinical research has shown that C1-ring osteosynthesis is an effective surgical option in treatment of unstable C1 fractures to preserve important C1–C2 motion [2,4,5]. For unstable C1 fractures involving the lateral mass, C1-ring osteosynthesis can restore fractures of the C1 anterior arch and posterior arch, but cannot adequately restore fractures of the lateral mass [6]. Unsatisfactory reduction of fractures of the C1 lateral mass can lead to arthrosis and persistent neck pain, which can result in severe discomfort and even the need for re-fusion surgery. Segal et al [6] performed C1-ring osteosynthesis in 18 patients with unstable C1 fractures and found that 3 had non-union after the operation, 2 of which had C1 lateral mass fractures, indicating that the clinical effect of C1-ring osteosynthesis on unstable C1 fractures involving the lateral mass was not satisfactory. Therefore, C1–C2 fixation and fusion may be a better treatment for unstable C1 fractures involving the lateral mass. With the development of internal fixation devices, posterior screw-rod instruments are widely used in C1–C2 fixation, with excellent biomechanical stability, wide applicability, and high bone fusion rate [18].
In our study, 16 patients with unstable C1 fracture involving the lateral mass were treated by posterior C1–C2 screw-rod fixation and fusion and were followed up to assess the clinical effects. All patients achieved satisfactory bone fusion and alleviation of neck pain without complications during the follow-up. Compared with conservative treatment, this technique could shorten the treatment period, accelerate bone fusion, enabling patients to carry out functional rehabilitation exercise as soon as possible and resuming daily life, regardless of restriction of motor function of the atlantoaxial joint to some extent. Moreover, this technique can effectively avoid complications such as poor reduction and non-union of fracture and reduce the risk of traumatic arthritis and chronic pain due to intraarticular fracture related to C1-ring osteosynthesis. It is worth noting that while our results recommend this technique, it requires an adequate learning curve. In addition, this surgical technique still carries the risk of vascular and nerve damage and must be performed at a center capable of dealing with complications.
Several limitations in the current study should be noted. Firstly, our sample size is rather small. Further research with larger sample sizes and longer follow-up to evaluate the effect of this are needed. Secondly, the data in the present study is retrospective, which affects the reliability of the results. Future prospective studies which add more standardized measures are essential for validation of the results. Lastly, we intend to carry out a comparative study of other therapeutic techniques in the future.
Conclusions
Posterior C1–C2 screw-rod fixation and fusion is an effective surgical option to manage unstable C1 fractures involving the lateral mass. This operation can provide reliable stabilization and satisfactory bone fusion.
Figures
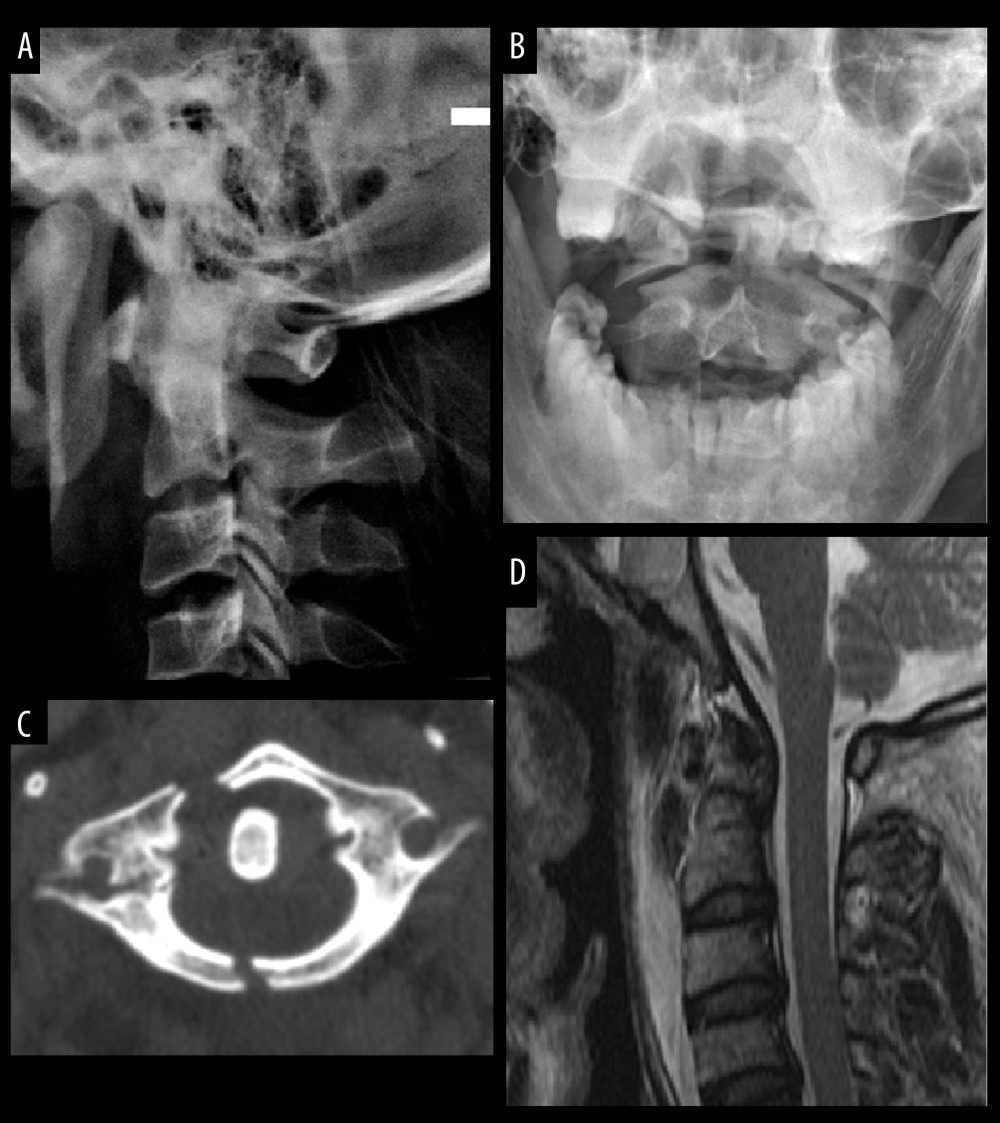 Figure 1. A 40-year-old man with unstable C1 fracture involving right lateral mass. (A, B) Preoperative cervical lateral and mouth-open X-rays showed lateral mass displacement. (C) CT scan showed fractures of C1 anterior and posterior arches and right lateral mass. (D) Preoperative MRI showed no spinal cord compression.
Figure 1. A 40-year-old man with unstable C1 fracture involving right lateral mass. (A, B) Preoperative cervical lateral and mouth-open X-rays showed lateral mass displacement. (C) CT scan showed fractures of C1 anterior and posterior arches and right lateral mass. (D) Preoperative MRI showed no spinal cord compression. 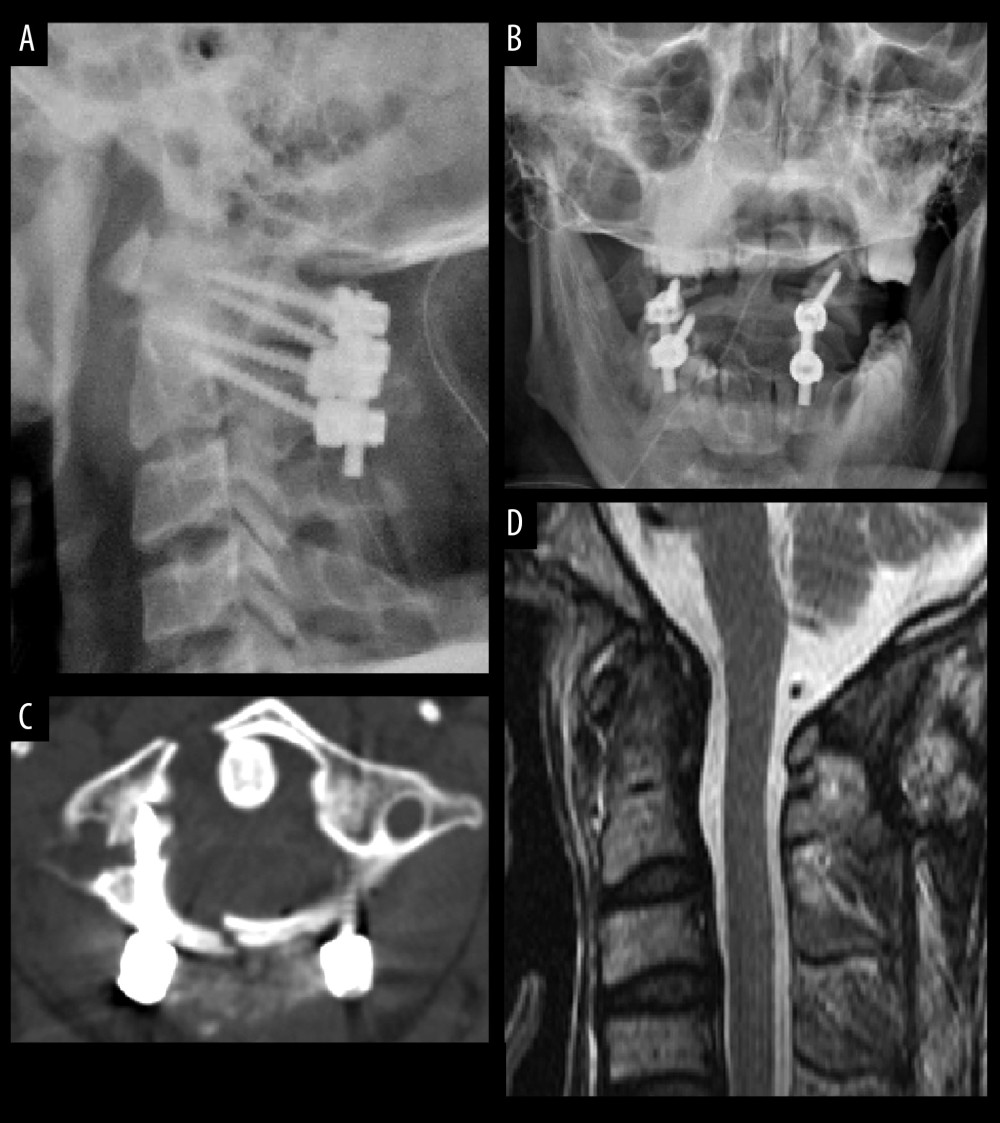 Figure 2. The same patient underwent posterior C1–C2 screw-rod fixation and fusion. (A, B) Postoperative cervical lateral and mouth-open X-rays revealed optimal sequence and position of internal fixation. (C) CT scan revealed correct placement of pedicle screws. (D) Postoperative MRI showed no damage to the spinal cord.
Figure 2. The same patient underwent posterior C1–C2 screw-rod fixation and fusion. (A, B) Postoperative cervical lateral and mouth-open X-rays revealed optimal sequence and position of internal fixation. (C) CT scan revealed correct placement of pedicle screws. (D) Postoperative MRI showed no damage to the spinal cord. 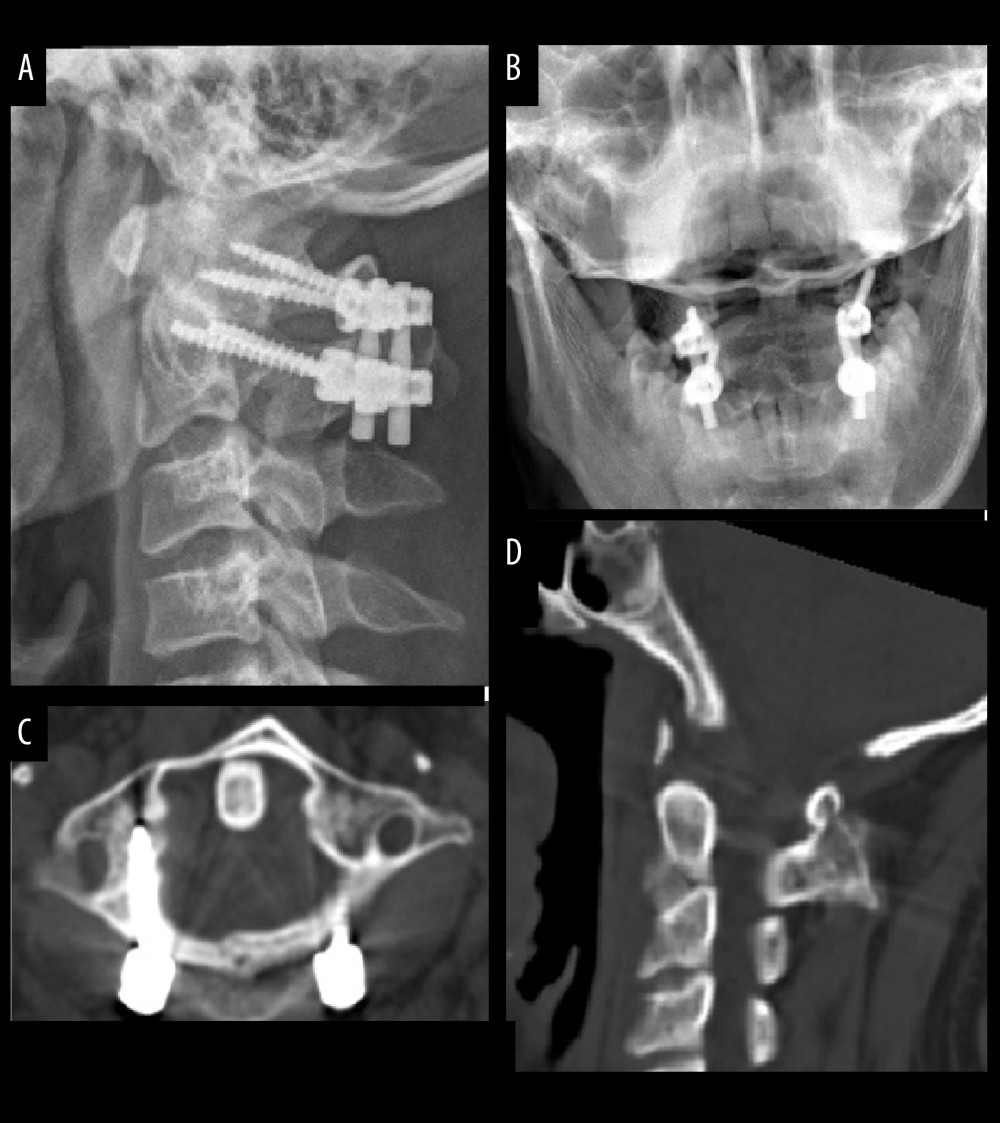 Figure 3. The same patient was followed up 6 months after surgery. (A, B) Cervical lateral and mouth-open X-rays revealed stable fixation and stability of C1–C2. (C, D) CT scans indicated stable location of pedicle screws and solid bone fusion.
Figure 3. The same patient was followed up 6 months after surgery. (A, B) Cervical lateral and mouth-open X-rays revealed stable fixation and stability of C1–C2. (C, D) CT scans indicated stable location of pedicle screws and solid bone fusion. References
1. Matthiessen C, Robinson Y, Epidemiology of atlas fractures – a national registry-based cohort study of 1,537 cases: Spine J, 2015; 15; 2332-37
2. He B, Yan L, Zhao Q, Self-designed posterior atlas polyaxial lateral mass screw-plate fixation for unstable atlas fracture: Spine J, 2014; 14; 2892-96
3. Kim MK, Shin JJ, Comparison of radiological and clinical outcomes after surgical reduction with fixation or halo-vest immobilization for treating unstable atlas fractures: Acta Neurochir (Wien), 2019; 161; 685-93
4. Li L, Teng H, Pan J, Direct posterior C1 lateral mass screws compression reduction and osteosynthesis in the treatment of unstable Jefferson fractures: Spine (Phila Pa 1976), 2011; 36; E1046-51
5. Ma W, Xu N, Hu Y, Unstable atlas fracture treatment by anterior plate C1-ring osteosynthesis using a transoral approach: Eur Spine J, 2013; 22; 2232-39
6. Segal LS, Grimm JO, Stauffer ES, Non-union of fractures of the atlas: J Bone Joint Surg Am, 1987; 69; 1423-34
7. Ma XY, Yin QS, Wu ZH, Anatomic considerations for the pedicle screw placement in the first cervical vertebra: Spine (Phila Pa 1976), 2005; 30(13); 1519-23
8. Goel A, Laheri V, Plate and screw fixation for atlanto-axial subluxation: Acta Neurochir (Wien), 1994; 129; 47-53
9. Harms J, Melcher RP, Posterior C1–C2 fusion with polyaxial screw and rod fixation: Spine (Phila Pa 1976), 2001; 26; 2467-71
10. Ma XY, Yin QS, Wu ZH, C2 anatomy and dimensions relative to translaminar screw placement in an Asian population: Spine (Phila Pa 1976), 2010; 35; 704-8
11. Teo EC, Ng HW, First cervical vertebra (atlas) fracture mechanism studies using finite element method: J Biomech, 2001; 34; 13-21
12. Bransford R, Chapman JR, Bellabarba C, Primary internal fixation of unilateral C1 lateral mass sagittal split fractures: A series of 3 cases: J Spinal Disord Tech, 2011; 24(3); 157-63
13. Lee C, Woodring JH, Unstable Jefferson variant atlas fractures: An unrecognized cervical injury: Am J Neuroradiol, 1991; 12; 1105-10
14. Lee TT, Green BA, Petrin DR, Treatment of stable burst fracture of the atlas (Jefferson fracture) with rigid cervical collar: Spine (Phila Pa 1976), 1998; 23; 1963-67
15. Lleu M, Charles YP, Blondel B, C1 fracture: Analysis of consolidation and complications rates in a prospective multicenter series: Orthop Traumatol Surg Res, 2018; 104; 1049-54
16. Kamal Y, Ortho MS, Khan HA, Atlas and axis injuries role of Halovest: Int J Health Sci (Qassim), 2014; 8; 335-45
17. Dvorak MF, Johnson MG, Boyd M, Long-term health-related quality of life outcomes following Jefferson-type burst fractures of the atlas: J Neurosurg Spine, 2005; 2; 411-17
18. Huang DG, Hao DJ, He BR, Posterior atlantoaxial fixation: A review of all techniques: Spine J, 2015; 15; 2271-81
Figures
 Figure 1. A 40-year-old man with unstable C1 fracture involving right lateral mass. (A, B) Preoperative cervical lateral and mouth-open X-rays showed lateral mass displacement. (C) CT scan showed fractures of C1 anterior and posterior arches and right lateral mass. (D) Preoperative MRI showed no spinal cord compression.
Figure 1. A 40-year-old man with unstable C1 fracture involving right lateral mass. (A, B) Preoperative cervical lateral and mouth-open X-rays showed lateral mass displacement. (C) CT scan showed fractures of C1 anterior and posterior arches and right lateral mass. (D) Preoperative MRI showed no spinal cord compression. Figure 2. The same patient underwent posterior C1–C2 screw-rod fixation and fusion. (A, B) Postoperative cervical lateral and mouth-open X-rays revealed optimal sequence and position of internal fixation. (C) CT scan revealed correct placement of pedicle screws. (D) Postoperative MRI showed no damage to the spinal cord.
Figure 2. The same patient underwent posterior C1–C2 screw-rod fixation and fusion. (A, B) Postoperative cervical lateral and mouth-open X-rays revealed optimal sequence and position of internal fixation. (C) CT scan revealed correct placement of pedicle screws. (D) Postoperative MRI showed no damage to the spinal cord. Figure 3. The same patient was followed up 6 months after surgery. (A, B) Cervical lateral and mouth-open X-rays revealed stable fixation and stability of C1–C2. (C, D) CT scans indicated stable location of pedicle screws and solid bone fusion.
Figure 3. The same patient was followed up 6 months after surgery. (A, B) Cervical lateral and mouth-open X-rays revealed stable fixation and stability of C1–C2. (C, D) CT scans indicated stable location of pedicle screws and solid bone fusion. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387