30 May 2023: Clinical Research
Association Between Serum Vitamin D Levels and Physical Outcomes of Patients Who Underwent Rehabilitation Following Ischemic Stroke
Wojciech BorowiczDOI: 10.12659/MSM.940115
Med Sci Monit 2023; 29:e940115
Abstract
BACKGROUND: Ischemic stroke is the most common cause of disability in adults. Deficiency of vitamin D in patients with cardiovascular diseases is increasing. Only a few studies have assessed the relationship between serum vitamin D levels and functional capacity and degree of disability. This study aimed to evaluate the association between serum vitamin D levels and physical outcomes of 94 patients who underwent physical rehabilitation following ischemic stroke.
MATERIAL AND METHODS: A group of 94 patients was enrolled; however, 80 patients (61.8±6.9 years) were included. They underwent a 6-week rehabilitation using proprioceptive neuromuscular facilitation (PNF, 60 min daily), mirror therapy (MT, 30 min daily), and occupational therapy (OT, 45 min daily). The Barthel Index (BI) and modified Rankin scale (mRS) were used for functional assessments. Laboratory blood tests for serum vitamin D and insulin-like growth factor 1 (IGF-1) levels were conducted.
RESULTS: There was a significant increase in BI scores (median difference=2.0 points [pts]; P<0.001) and IGF levels (median difference=124.6 ng/ml; P<0.001) after rehabilitation. There was a significant decrease in mRS scores (median difference=7.0 pts; P<0.001), but there was no significant difference in vitamin D levels (P=0.40). The effect of age (B=-0.01, P=0.04) and serum vitamin D level (B=-0.02, P=0.01) on the BI score was demonstrated. The effect of body mass index (BMI) results (B=-0.07, P=0.02) on the mRS score was observed.
CONCLUSIONS: Lower serum vitamin D levels and more advanced age may be associated with worse functional outcomes in first-ever ischemic stroke patients.
Keywords: 25-hydroxyvitamin D, functional status, ischemic stroke, neurological rehabilitation, Adult, Humans, Vitamin D, stroke rehabilitation, Vitamins, Vitamin D Deficiency, Stroke
Background
Ischemic stroke causes irreversible brain damage and affects people of all ages on all continents. It is the second leading cause of death [1], and it is the leading cause of disability in people aged over 45 years [2]. Despite significant improvements in primary prevention, stroke continues to affect more than 1.1 million Europeans [3] and Chinese [4] each year, which indicates the severity of the problem.
Established risk factors for ischemic stroke do not explain the occurrence of the disease in one-third of patients [5], warranting further exploration of potential risk factors. Serum vitamin D levels are positively associated with improved cardiovascular health, particularly with a reduced risk of stroke [6]. Recently, there has been an increased prevalence of vitamin D deficiency in patients with cardiovascular diseases, including post-stroke patients [7].
Vitamin D deficiency is described as a co-morbid condition in many diseases such as acute ischemic stroke, neurodevelopmental disorders and intellectual disability, and cardiovascular risk, and it is associated with increased mortality [8,9]. The discovery of the vitamin D receptor (VDR) made it possible to learn more about its effects on extraskeletal organs [10]. The identification of calcitriol (the active form of vitamin D) receptors in various tissues of the human body confirmed the pleiotropic, multidirectional effects of vitamin D [11].
Zhou et al [12], in their systematic review and meta-analysis, confirmed the hypothesis that low vitamin D levels are associated with an increased risk of ischemic stroke, which indicates they are a possible risk factor for stroke. In contrast, higher vitamin D concentrations significantly protect against stroke.
Vitamin D is a well-known neurosteroid hormone that plays an important role in modulating cognitive processes and regulating neurotrophic signaling [13] for neuroprotection, neuromodulation, vascular risk factors for stroke [14–16], and inflammation [17,18]. VitaminD, both from food and that synthesized in the skin, undergoes transformations that result in the formation of 2 metabolites. Hydroxylation to 25-hydroxyvitamin D (25(OH)D), a substrate for the synthesis of the biologically active 1,25 dihydroxyvitamin D (1,25(OH)2D), occurs in liver cells, which takes place in the proximal cells of the kidneys. Both metabolites enter the bloodstream. Although 1,25(OH)2 is a biologically active form of vitamin D, its serum levels do not correlate with the state of the body’s actual supply. A marker of vitamin D content is the measurement of 25(OH)D. The half-life of the circulating metabolite in the blood is approximately 21 days and is the best indicator of the total vitamin D content in the body. In contrast, the 1,25(OH)2 present in serum has a short half-life of approximately 4 hours and determination of its content is not used for assessing vitamin D deficiency.
Many studies in the literature have assessed the relationship between vitamin D in terms of stroke risk [6,19]. Few studies have assessed the relationship between serum vitamin D levels and the functional capacity of patients and the associated degree of disability. Therefore, there was an attempt to assess the relationship between vitamin D levels in patients admitted to rehabilitation and functional outcomes. Therefore, this study aimed to evaluate the association between serum vitamin D levels and physical outcomes of 94 patients who underwent physical rehabilitation following ischemic stroke.
Material and Methods
ETHICAL CONSIDERATIONS:
The study was approved by the Ethics Committee of Wrocław Medical University (permission no. KB-813/2020). The study was conducted in accordance with the Good Clinical Practice Guidelines and the Declaration of Helsinki. Each person was briefed and instructed on the conduct of the experiment before signing the consent to participate. All study participants were informed of the possibility of discontinuing their participation in the project in the case of health problems or for other reasons.
TRIAL REGISTRATION:
The study was conducted as part of the project “Effectiveness of various therapeutic forms and their influence on nervous, muscular and vascular plasticity in patients after ischemic stroke” in collaboration with Dr. Sílvia Rocha-Rodrigues (Research Centre in Physical Activity and Health, Faculty of Sport, University of Porto, Portugal). The project was registered in the International Standard Randomized Controlled Trial Number Registry Platform (registry no. ISRCTN16891871).
PARTICIPANTS:
A group of 94 post-ischemic stroke patients undergoing rehabilitation at the Neurological Rehabilitation Unit of the Wrocław Regional Specialist Hospital were enrolled in the study. Patients were qualified to participate in the research by a team consisting of a physician-specialist in medical rehabilitation, a neurologist, a neurologopedist, a clinical psychologist, and a physiotherapist. Inclusion criteria for the study included first-ever ischemic stroke, time of onset 2 weeks before admission for early neurological rehabilitation, stroke confirmed by magnetic resonance imaging (MRI) or computed tomography (CT), age >18 years, no contraindications to participate in the experiment (consent of attending physician), no neurological comorbidities, and written informed consent of the patient to participate in the study. Exclusion criteria included patients with an infection in the past 2 weeks, patients who took vitamin D and its derivatives or calcium in the past 3 months, patients with liver and kidney disorders, patients with thyroid disorders, patients with aphasia, and patients who did not provide consent. A group of 80 patients met the criterion of participating in 2 follow-up examinations was finally qualified for the study. There were 25 women (31.3%) and 55 men (68.7%) in that group. Patients were provided with proprioceptive neuromuscular facilitation (PNF) and mirror therapy (MT) for 42 days. At 6-week intervals, patients had blood drawn for routine tests and selected biochemical parameters were determined in the remaining blood. All tests and surveys were carried out by the same physician.
MEASUREMENTS:
On the day of admission, all patients underwent standard neurological examination, basic anthropometric measurements, and stroke severity assessment using the National Institutes of Health Stroke Scale (NIHSS). In terms of primary outcomes, functional tests were performed using Barthel Index (BI) and modified Rankin scale (mRS).
BARTHEL INDEX:
The BI is a commonly used scale to assess the level of functional independence in patients undergoing physiotherapy after stroke. The BI measures deficits in self-care, mobility, and sphincter control. Scores ranging from 0 to 20 points are interpreted as follows: ≤4 points – very severe disability; 5–9 points – severe disability; 10–14 points – moderate severity of disability; 15–19 points – mild disability; 20 points – full independence.
MODIFIED RANKIN SCALE:
The mRS is a commonly used tool to assess functional outcome after a stroke. It assigns a score ranging from 0 (no symptoms) to 6 (death), with higher scores indicating more severe disability. The scale is often used to assess a patient’s ability to carry out activities of daily living, such as eating, dressing, and mobility. The mRS has been shown to have good inter-rater reliability and validity, and is widely used in both clinical practice and stroke research.
LABORATORY BLOOD TESTS:
Patients had their blood routinely drawn from the ulnar vein for basic laboratory tests such as complete blood count (CBC) and urinalysis. The following concentrations were determined: vitamin D and IGF-1 levels. The serum levels of those substances were determined on admission to the unit and after 6 weeks of rehabilitation training. Each patient had blood drawn from an ulnar vein, always at the same time, at 6: 30 a.m., on an empty stomach. Laboratory tests were performed at the Scientific Laboratory of the Research and Development Center at the Regional Specialized Hospital in Wrocław. Performing biochemical tests at the same time, using reagents from a single production batch, and ensuring the same measurement conditions was intended to minimize the occurrence of external, random errors that could alter the results of biochemical analyses. The tests were performed in the laboratory on an Alinity ci analyzer using reagents from Abbott (Chicago, Illinois, USA). This is a widely used, standardized immunochemical assay using a chemiluminescent microparticle immunoassay (CMIA) used to quantify 25(OH)D in human serum and plasma on an Alinity ci analyzer. The Alinity ci 25-OH Vitamin D test has been standardized against the National Institute of Standards & Technology Standard Reference Material 2972 (NIST SRM 2972). The test is used as an aid in assessing adequacy of vitamin D levels. It is a one-step immunochemical test with delayed conjugate addition, dedicated to the quantitative determination of 25-hydroxyvitamin D in human serum and plasma using microparticles and a chemiluminescent marker (CMIA). Paramagnetic microparticles coated with anti-vitamin D antibodies and assay diluent are added to the test sample, and the whole mixture was incubated. The 25-hydroxyvitamin D present in the sample was removed from the vitamin D-binding protein and then binds to the anti-vitamin D antibodies, coating the microparticles. A conjugate containing acridine-labeled vitamin D was added to form the reaction mixture. The reaction mixture was incubated. After a wash cycle, the Pre-Trigger Solution and the Trigger Solution that triggers the Trigger Solution reaction were added. The intensity of the signal produced by the chemiluminescence reaction was measured in relative light units (RLU), based on the relationship between the amount of 25-hydroxyvitamin D in the sample and the RLU values measured by the optical system. A normal serum vitamin D level was defined as a 25(OH)D concentration >30 ng/ml. Vitamin D deficiency was defined as a concentration of 25(OH)D <30 ng/ml.
REHABILITATION PROCEDURES:
Once stabilized during the early neurological rehabilitation period, post-ischemic stroke patients may develop a wide variety of disorders, the clinical picture of which will depend on the nature and extent of damaged brain tissues. Movement disorders are one of the most common clinical manifestations. Rehabilitation treatment (rehabilitation training) focuses on regaining motor function to a degree that enables patients to achieve and meet their self-care needs. Patients selected for the project were rehabilitated with neurophysiological methods (PNF and MT) for 5 days a week. Rehabilitation using the PNF method was oriented towards improvement of a specific lost function, not just a structure. The overriding aim of the therapy was to help the patient achieve the highest possible functional level. Each unit of treatment for mobility issues lasted 60 minutes. Moreover, each patient additionally had MT applied daily for 30 minutes. The rehabilitation training was 6 weeks long. Also, each patient had daily one-to-one sessions with a clinical psychologist for 30 minutes and an additional 45 minutes of occupational therapy (OT). For patient safety reasons, blood pressure and heart rate were measured before each kinesitherapy unit. Since patients with diabetes were also included in the study group, electroencephalography (ECG) changes indicative of myocardial hypoxia, which may also occur during exercise, were an absolute precondition for discontinuing the rehabilitation training. The rehabilitation training has always been individually tailored to each patient and their current abilities and needs, taking into account the patient’s capabilities.
SAMPLE SIZE:
The sample size analysis was based on the main objective of the study, which was to assess changes in vitamin D levels before and after 6 weeks of rehabilitation. Before the start of the study, it was assumed that there would be an increase in vitamin D levels. The minimum sample size needed to detect a difference of 20% assuming alpha=5%, power=80% and confidence level=95% is 79 patients. The sample size analysis was performed using the G*Power software. Statistical power analyses were performed using G*Power 3.1
STATISTICAL ANALYSIS:
Statistical analysis was performed using Statistica 13 software (TIBCO, Inc., Palo Alto, USA). Arithmetic means and standard deviations or medians, upper and lower quartiles and the range of variability (minimum and maximum value) were calculated for measurable variables. Prevalence (%) was calculated for qualitative variables. All studied quantitative variables were verified using the Shapiro-Wilk test to determine distribution type. Comparisons between pre- and post-rehabilitation scores were made using non-parametric Wilcoxon test. The level of α=0.05 was used for all comparisons. Moreover, the analysis of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) was performed using a linear regression (univariate model). The unstandardized and standardized regression coefficients, standard error and level of statistical significance were determined. The next step was to develop a multivariate model (stepwise progressive method), taking into account variables whose
Results
PATIENTS’ CHARACTERISTICS:
The study ultimately included 80 patients meeting the participation criterion; the mean age of participants was 61.8±6.9. In this group, 68.7% were men (55 individuals). Table 1 shows the characteristics of the group including age, height, weight, body mass index (BMI), number of days since stroke diagnosis, NIHSS score, sex, smoking, and history of chronic diseases.
OUTCOMES’ CHANGES AFTER REHABILITATION:
Figures 1–4 show a comparison of BI, mRS, vitamin D, and insulin-like growth factor 1 (IGF-1) results before and after rehabilitation. After therapy, there was a statistically significant increase in BI scores (median difference is 2.0 points; P<0.001) and IGF levels (median difference is 124.6 ng/ml; P<0.001). There was also a statistically significant reduction in mRS scores (median difference is 7.0 points; P<0.001). There were no significant differences in vitamin D levels (P=0.40).
VARIABLES AFFECTING OUTCOMES:
Table 2 shows the assessment of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) of post-stroke patients (linear regression analysis in the univariate model). The effect of age (B=−0.01, P=0.04) and serum vitamin D levels (B=−0.02, P=0.01) on BI score was demonstrated. The effect of BMI results (B=−0.07, P=0.02) on mRS score was observed.
Discussion
STUDY LIMITATIONS:
Firstly, a limitation of this study was that the trial was not randomized and it took place at a single center. In the future, it would be advisable to conduct a multicenter study for validation in other cohorts. We cannot directly relate our results to the above studies due to the fact that our study group included only patients after ischemic stroke but not treated with thrombolytic therapy. Future studies, which we plan to expand to a larger patient population, should take this aspect into account. Furthermore, there was no way to exclude errors related to variables that were not measurable in this observational study, such as sun exposure, diet, physical activity, or parathormone levels. No in-depth analysis of nutritional status was carried out and no information on nutritional conditions was collected. Future research should consider whether vitamin D supplementation in patients undergoing rehabilitation improves functional outcomes in ischemic stroke patients. The BI and mRS tools used are recommended for functional assessment and have high inter-rater reliability. Nevertheless, there is no mandatory definition of a good score, and it is the researcher who sets the standards that determine the score. Neither scale takes into account the patient’s mental state, and anxiety or post-stroke depression can affect a patient’s functioning and quality of life. Future studies should also use other objective measurement methods that take into account all aspects of life, both physical and mental.
Conclusions
In conclusion, lower serum vitamin D levels and older age may be associated with worse functional outcome in first-ever ischemic stroke patients. It is urgent to evaluate in a prospective, randomized trial with a placebo group whether vitamin D supplementation in appropriate doses can improve prognosis and functional outcomes in first-ever ischemic stroke patients undergoing rehabilitation treatment.
Figures
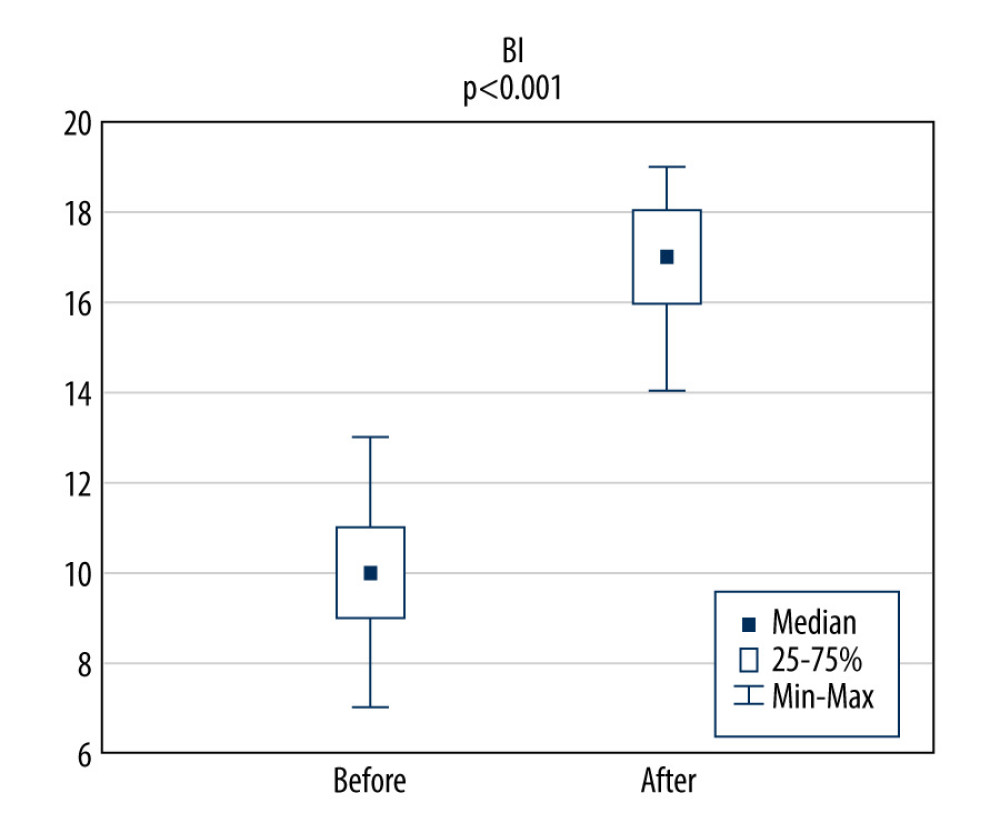 Figure 1. A comparison of BI results before and after rehabilitation. BI – Barthel Index.
Figure 1. A comparison of BI results before and after rehabilitation. BI – Barthel Index. 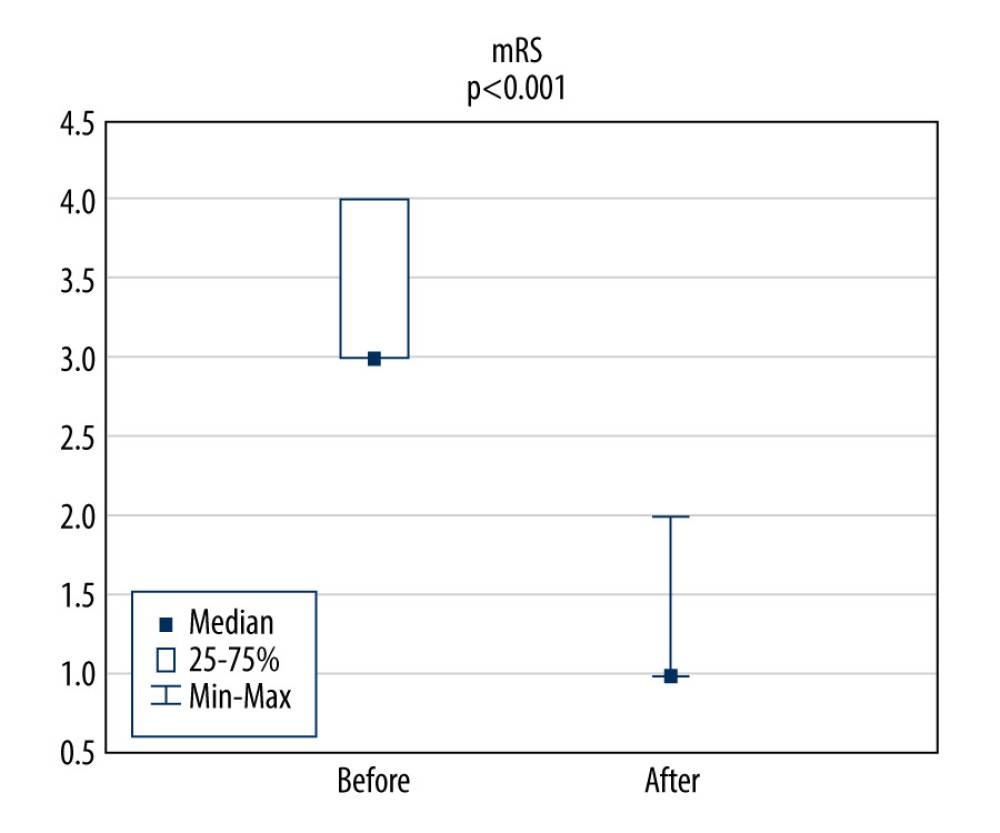 Figure 2. A comparison of mRS results before and after rehabilitation. mRS – modified Rankin scale.
Figure 2. A comparison of mRS results before and after rehabilitation. mRS – modified Rankin scale. 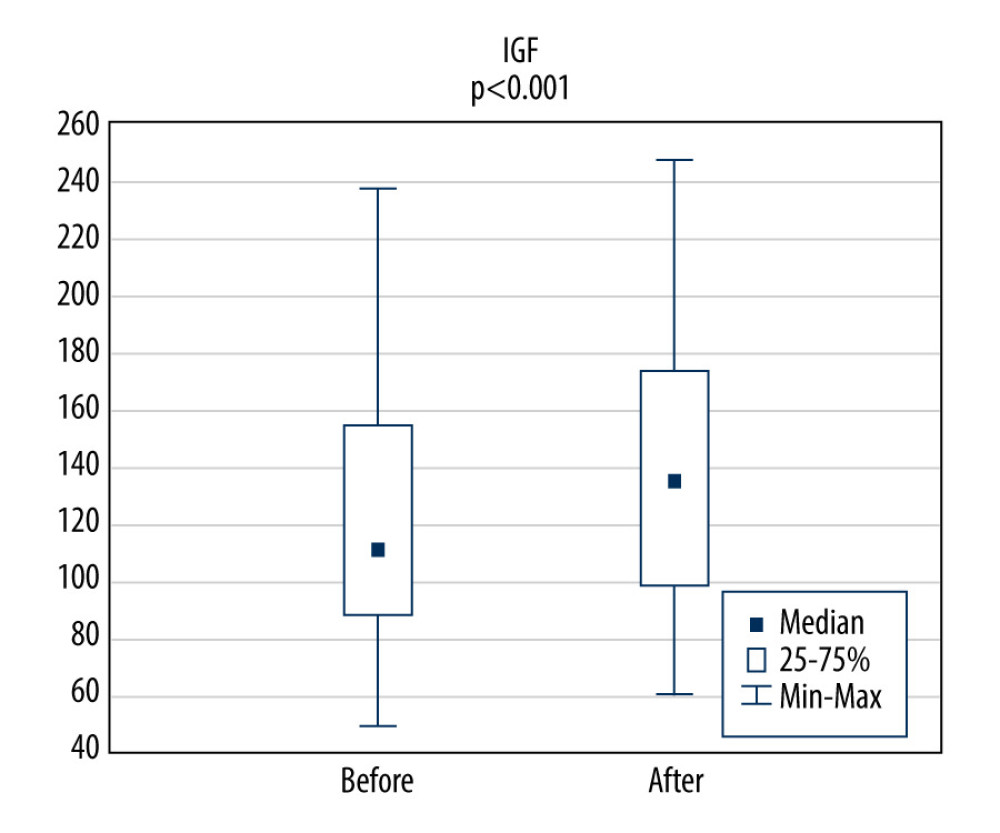 Figure 3. A comparison of IGF results before and after rehabilitation. IGF – insulin-growth factor.
Figure 3. A comparison of IGF results before and after rehabilitation. IGF – insulin-growth factor. 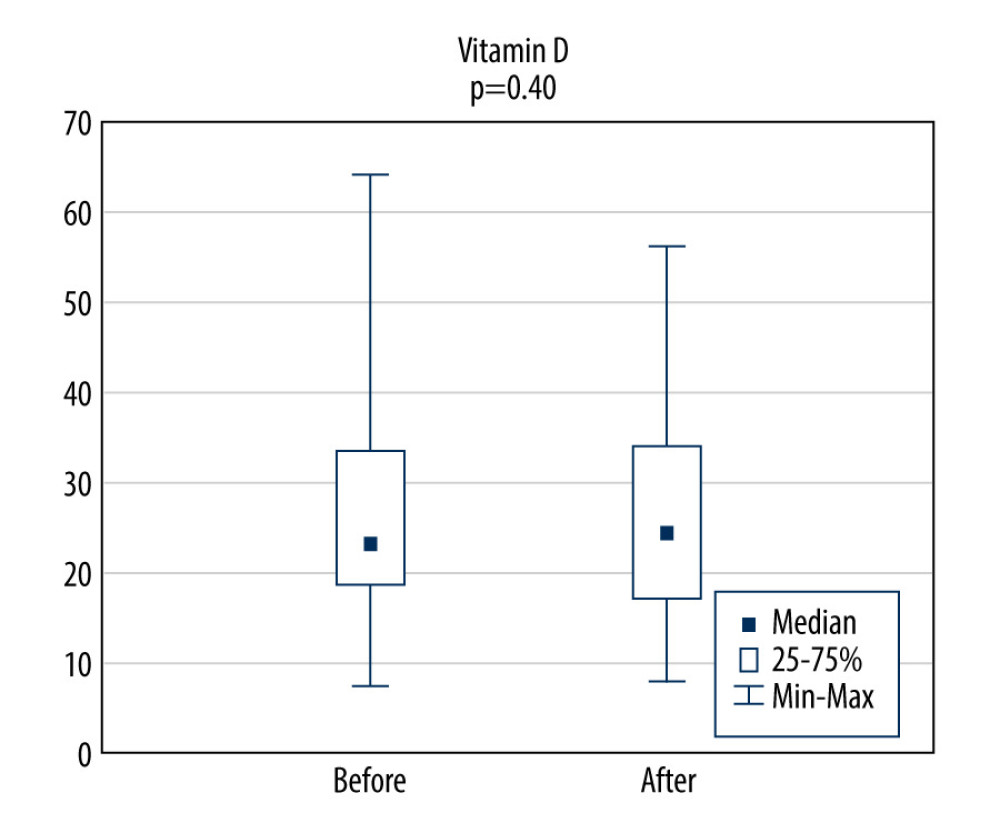 Figure 4. A comparison of vitamin D results before and after rehabilitation.
Figure 4. A comparison of vitamin D results before and after rehabilitation. References
1. Talebi A, Amirabadizadeh A, Nakhaee S, Cerebrovascular disease: How serum phosphorus, vitamin D, and uric acid levels contribute to the ischemic stroke: BMC Neurol, 2020; 20; 116
2. Siotto M, Santoro M, Aprile I, Vitamin D and rehabilitation after stroke: Status of art: Applied Sciences, 2020; 10(6); 1973
3. Béjot Y, Bailly H, Durier J, Giroud M: Presse Med, 2016; 45(12 Pt 2); e391-e98
4. Wang W, Jiang B, Sun H, Prevalence, incidence, and mortality of stroke in China: Results from a nationwide population-based survey of 480687 adults: Circulation, 2017; 135(8); 759-71
5. Ay H, Arsava EM, Andsberg G, Pathogenic ischemic stroke phenotypes in the NINDS-stroke genetics network: Stroke, 2014; 45(12); 3589-96
6. Yarlagadda K, Ma N, Doré S, Vitamin D and stroke: Effects on incidence, severity, and outcome and the potential benefits of supplementation: Front Neurol, 2020; 11; 384
7. Kheiri B, Abdalla A, Osman M, Vitamin D deficiency and risk of cardiovascular diseases: A narrative review: Clin Hypertens, 2018; 24; 9
8. Alfieri DF, Lehmann MF, Oliveira SR, Vitamin D deficiency is associated with acute ischemic stroke, C-reactive protein, and short-term outcome: Metab Brain Dis, 2017; 32(2); 493-502
9. Matyjaszek-Matuszek B, Lenart-Lipińska M, Woźniakowska E, Clinical implications of vitamin D deficiency: Menopause Rev, 2015; 14(2); 75-81
10. Marino R, Misra M, Extra-skeletal effects of vitamin D: Nutrients, 2019; 11(7); 1460
11. Christakos S, Dhawan P, Verstuyf A, Vitamin D: Metabolism, molecular mechanism of action, and pleiotropic effects: Physiol Rev, 2016; 96(1); 365-408
12. Zhou R, Wang M, Huang H, Lower vitamin D status is associated with an increased risk of ischemic stroke: A systematic review and meta-analysis: Nutrients, 2018; 10(3); 277
13. Dicou E, Neurotrophins and neuronal migration in the developing rodent brain: Brain Res Rev, 2009; 60(2); 408-17
14. Aspell N, Lawlor B, O’Sullivan M, Is there a role for vitamin D in supporting cognitive function as we age?: Proc Nutr Soc, 2018; 77(2); 124-34
15. van Schoor NM, Comijs HC, Llewellyn DJ, Lips P, Cross-sectional and longitudinal associations between serum 25-hydroxyvitamin D and cognitive functioning: Int Psychogeriatr, 2016; 28(5); 759-68
16. Wilson VK, Houston DK, Kilpatrick L, Relationship between 25-hydroxyvitamin D and cognitive function in older adults: The health, aging and body composition study: J Am Geriatr Soc, 2014; 62(4); 636-41
17. Balden R, Selvamani A, Sohrabji F, Vitamin D deficiency exacerbates experimental stroke injury and dysregulates ischemia-induced inflammation in adult rats: Endocrinology, 2012; 153(5); 2420-35
18. Di Rosa M, Malaguarnera G, De Gregorio C, Immuno-modulatory effects of vitamin D3 in human monocyte and macrophages: Cell Immunol, 2012; 280(1); 36-43
19. Marek K, Cichoń N, Saluk-Bijak J, The role of vitamin D in stroke prevention and the effects of its supplementation for post-stroke rehabilitation: A narrative review: Nutrients, 2022; 14(13); 2761
20. Wu WX, He DR, Low vitamin D levels are associated with the development of deep venous thromboembolic events in patients with ischemic stroke: Clin Appl Thromb Hemost, 2018; 24(9 Suppl); 69S-75S
21. Manson JE, Cook NR, Lee IM, Vitamin D supplements and prevention of cancer and cardiovascular disease: N Engl J Med, 2019; 380(1); 33-44
22. Zeng YY, Yuan CX, Wu MX, Low vitamin D levels and the long-term functional outcome of stroke up to 5 years: Brain Behav, 2021; 11(10); e2244
23. Markišić M, Pavlović AM, Pavlović DM, The impact of homocysteine, vitamin B12, and vitamin D levels on functional outcome after first-ever ischaemic stroke: Biomed Res Int, 2017; 2017; 5489057
24. Daubail B, Jacquin A, Guilland JC, Serum 25-hydroxyvitamin D predicts severity and prognosis in stroke patients: Eur J Neurol, 2013; 20(1); 57-61
25. Zhang B, Wang Y, Zhong Y, Serum 25-hydroxyvitamin D deficiency predicts poor outcome among acute ischemic stroke patients without hypertension: Neurochem Int, 2018; 118; 91-95
26. Wei ZN, Kuang JG, Vitamin D deficiency in relation to the poor functional outcomes in nondiabetic patients with ischemic stroke: Biosci Rep, 2018; 38(2); BSR20171509
27. Li M, Li C, He J, Zheng X, Study on the relationship between 25-hydroxyvitamin D level and rehabilitation of stroke patients: Folia Neuropathol, 2022; 60(1); 114-21
28. Park KY, Chung PW, Kim YB, Serum vitamin D status as a predictor of prognosis in patients with acute ischemic stroke: Cerebrovasc Dis, 2015; 40(1–2); 73-80
29. Turetsky A, Goddeau RP, Henninger N, Low serum vitamin D is independently associated with larger lesion volumes after ischemic stroke: J Stroke Cerebrovasc Dis, 2015; 24(7); 1555-63
30. Siniscalchi A, Lochner P, Anticoli S, What is the current role for vitamin D and the risk of stroke?: Curr Neurovasc Res, 2019; 16(2); 178-83
31. Daumas A, Daubail B, Legris N, Association between admission serum 25-hydroxyvitamin D levels and functional outcome of thrombolyzed stroke patients: J Stroke Cerebrovasc Dis, 2016; 25(4); 907-13
32. Yalbuzdag SA, Sarifakioglu B, Afsar SI, Is 25(OH)D associated with cognitive impairment and functional improvement in stroke? A retrospective clinical study: J Stroke Cerebrovasc Dis, 2015; 24(7); 1479-86
33. Holick MF, The vitamin D deficiency pandemic: Approaches for diagnosis, treatment and prevention: Rev Endocr Metab Disord, 2017; 18(2); 153-65
34. Braga M, Simmons Z, Norris KC, Vitamin D induces myogenic differentiation in skeletal muscle derived stem cells: Endocr Connect, 2017; 6(3); 139-50
35. Antoniak AE, Greig CA, The effect of combined resistance exercise training and vitamin D3 supplementation on musculoskeletal health and function in older adults: A systematic review and meta-analysis: BMJ Open, 2017; 7(7); e014619
36. Momosaki R, Abo M, Urashima M, Vitamin D supplementation and post-stroke rehabilitation: A randomized, double-blind, placebo-controlled trial: Nutrients, 2019; 11(6); 1295
37. Murphy TH, Corbett D, Plasticity during stroke recovery: From synapse to behaviour: Nat Rev Neurosci, 2009; 10(12); 861-72
Figures
 Figure 1. A comparison of BI results before and after rehabilitation. BI – Barthel Index.
Figure 1. A comparison of BI results before and after rehabilitation. BI – Barthel Index. Figure 2. A comparison of mRS results before and after rehabilitation. mRS – modified Rankin scale.
Figure 2. A comparison of mRS results before and after rehabilitation. mRS – modified Rankin scale. Figure 3. A comparison of IGF results before and after rehabilitation. IGF – insulin-growth factor.
Figure 3. A comparison of IGF results before and after rehabilitation. IGF – insulin-growth factor. Figure 4. A comparison of vitamin D results before and after rehabilitation.
Figure 4. A comparison of vitamin D results before and after rehabilitation. Tables
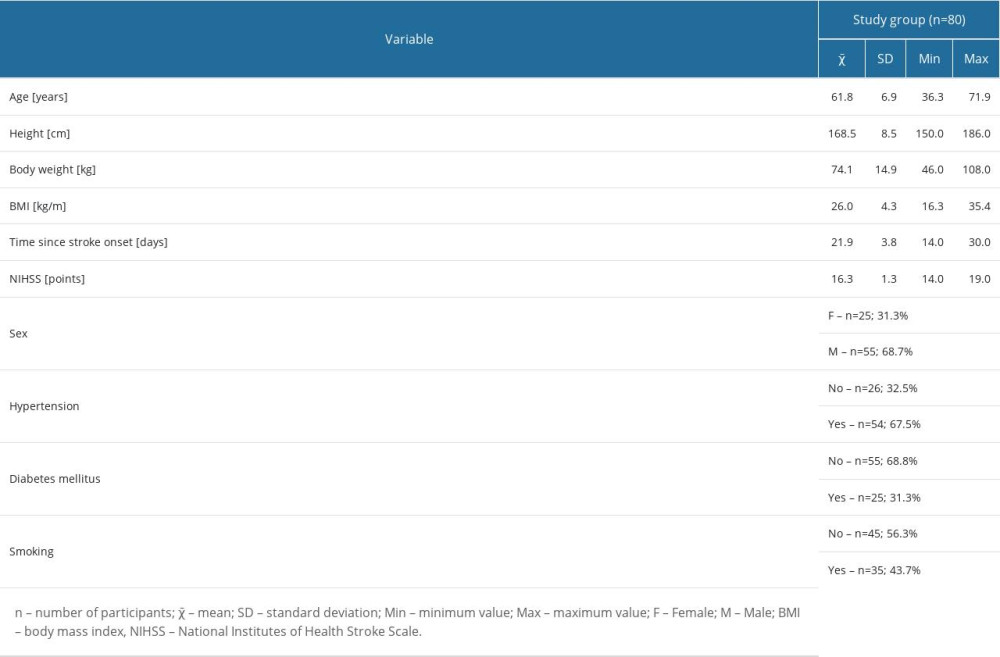 Table 1. Characteristics of the study group.
Table 1. Characteristics of the study group.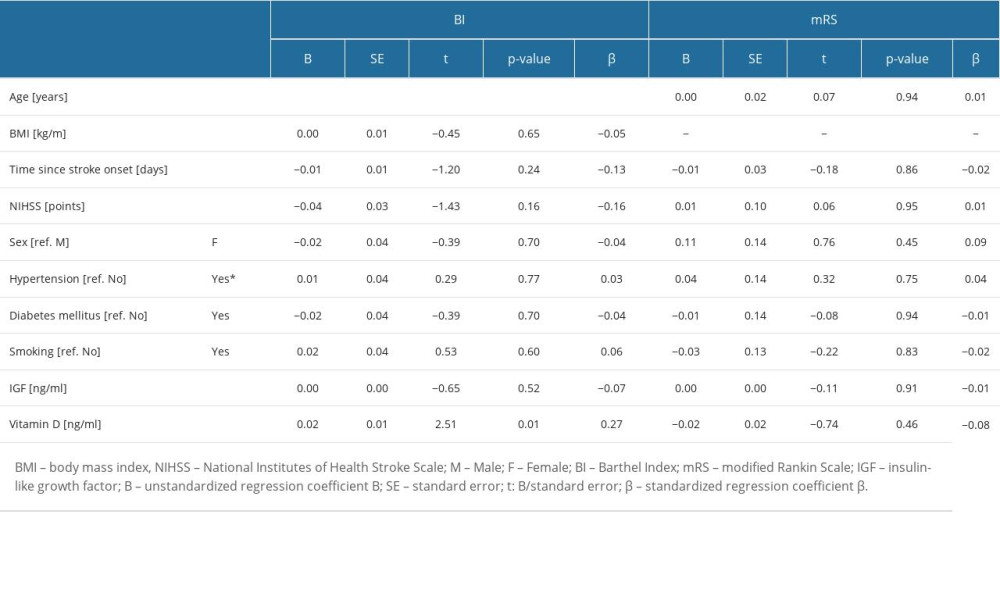 Table 2. The assessment of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) of post-stroke patients.
Table 2. The assessment of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) of post-stroke patients. Table 1. Characteristics of the study group.
Table 1. Characteristics of the study group. Table 2. The assessment of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) of post-stroke patients.
Table 2. The assessment of the impact of selected variables on activities of daily living (BI) and disability/dependence in the daily activities (mRS) of post-stroke patients. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








