22 June 2020: Clinical Research
Association of Serum Thyroid Hormones with the Risk and Severity of Chronic Kidney Disease Among 3563 Chinese Adults
Jialin Li1CE, Xi’ai Wu2BD, Minjing Luo1BF, Meihua Yan3BD, Qian Wang1D, Ping Li3AG, Wenquan Niu3CE*DOI: 10.12659/MSM.922910
Med Sci Monit 2020; 26:e922910
Abstract
BACKGROUND: Chronic kidney disease (CKD) is a global health problem with an increasing prevalence. We explored the association of serum thyroid hormones with the risk and severity of CKD among Chinese adults.
MATERIAL AND METHODS: This retrospective study involved 3563 participants. CKD was diagnosed according to the clinical practice guidelines of the 2012 Kidney Disease Improving Global Outcomes guidelines. Effect-size estimates are expressed as odds ratio (OR) and 95% confidence interval (CI).
RESULTS: Given the strong magnitude of correlation, only 3 thyroid hormones were analyzed: free triiodothyronine (FT3), free thyroxin (FT4), and thyroid-stimulating hormone (TSH). After propensity score matching on age, sex, diabetes, and hypertension, per 0.2 pg/mL increase in FT3 was significantly associated with 35–38% reduced risk of CKD at stage 1–4, and per 0.3 ng/dL increase in FT4 was only significantly associated with 21% reduced risk of CKD at stage 5 (OR, 95% CI: 0.79, 0.69–0.89), and per 0.5 μIU/mL increment in TSH increased the risk of CKD stage 5 by 8% (1.08, 1.02–1.14). Importantly, 3 thyroid hormones acted interactively, particularly for the interaction between FT3 and FT4 in predicting CKD at stage 5 (OR, 95% CI: 1.81, 1.30–2.55 for high FT3-low FT4, 17.72, 7.18–43.74 for low FT3-high FT4, and 22.28, 9.68–51.30 for low FT3-low FT4).
CONCLUSIONS: Our findings indicate that serum FT3 can be used as an early-stage biomarker for CKD, and FT4 and TSH can be used as advanced-stage biomarkers among Chinese adults.
Keywords: Health Status Indicators, Renal Insufficiency, Chronic, Thyroid Hormones, Asians, Creatinine, Risk Factors, Severity of Illness Index, Thyroid Function Tests, thyrotropin, thyroxine, Triiodothyronine
Background
Chronic kidney disease (CKD) is a global health problem that has reached epidemic proportions, with an estimated prevalence rate of 8–16% [1]. Currently, CKD is gaining increased attention as a potential driver of cardiovascular and cerebrovascular diseases [2,3]. In China, CKD affects approximately 10.8% of adults [4], resulting in disability and heavy socioeconomic burden [5,6]. There are several known risk factors for CKD, such as diabetes and hypertension [7–9]. Clinical investigations have revealed substantial variation in the onset and progression of CKD that cannot be fully explained by preexisting risk factors [10,11]. Thus, efforts are needed to identify more potential risk factors in the development of CKD.
It is widely recognized that thyroid hormones are of clinical and public health importance for renal physiology and functional development [12,13]. From epidemiological aspects, a nationally representative cohort of U.S. patients with moderate-to-severe CKD showed an inverse association between estimated glomerular filtration rate (eGFR) and the risk of hypothyroidism [14]. In addition, a retrospective cohort study in Taiwanese indicated that higher concentrations of thyroid-stimulating hormone (TSH) were associated with greater risk of subsequent CKD [12]. Moreover, another prospective cohort study in middle-aged and elderly Shanghainese revealed that high free thyroxin (FT4), but not TSH and free triiodothyronine (FT3), was associated with increased risk of incident CKD and rapid eGFR decline [15]. The reasons for these inconsistences are multiple, likely due to heterogeneous study populations, different study designs, or unaccounted-for residual confounders. Moreover, a literature search revealed sparse data directly comparing thyroid hormones and various CKD stages in the current medical literature.
To fill this gap in knowledge and generate more information for future studies, we developed a hypothesis that abnormal serum thyroid hormones are potential risk predictors for CKD among Chinese adults, and tested this hypothesis in a retrospective study by assessing the association of 5 thyroid hormone biomarkers with the risk and severity of CKD, both individually and interactively, via propensity score matching analysis.
Material and Methods
STUDY PARTICIPANTS:
This was a hospital-based retrospective study. All study participants were Han Chinese adults aged 18 to 80 years at the time of enrollment from the Department of Endocrinology and Department of Nephrology at China-Japan Friendship Hospital, and they were consecutively recruited during the period January 2010 to December 2018. The study protocol was approved by the Ethics Committee of China-Japan Friendship Hospital, and was in accordance with the principles of the Declaration of Helsinki. All participants in this study gave their informed written consent.
Initially, 5294 participants were recruited, and 1731 of them were excluded due to the following reasons: (i) under dialysis or after kidney transplantation; (ii) essential relevant information including serum creatinine and urinary albumin-to-creatinine ratio (ACR) was missing; (iii) taking medication affecting thyroid function, such as thyroxine, anti-thyroid drugs, glucocorticoid, antiepileptic and contraceptive drugs prehospitalization; and (iv) being pregnant or having diabetic ketoacidosis, acute cardiovascular events, or other severe disorders including tumors. Thus, there were 3563 eligible patients with complete data in the final analysis.
Among these 3563 eligible patients, including 2396 males and 1167 females, 289 were clinically confirmed to be free of CKD and they formed the control group, while 3274 were diagnosed with CKD and they formed the case group.
DIAGNOSIS OF CKD:
CKD was diagnosed on the basis of either eGFR <60 ml/min/1.73 m2 or the presence of albuminuria according to the clinical practice guidelines of the 2012 Kidney Disease Improving Global Outcomes (KDIGO) [16]. GFR was estimated according to the 2009 CKD Epidemiology Collaboration (CKD-EPI) equation, as confirmed and validated in many previous studies [17–21]. This equation is sex-specific. For females, if serum creatinine (Scr) is ≤0.7 mg/dl, eGFR equals to 144×(Cr/0.7)−0.329×(0.993)age, and if Scr is >0.7 mg/dl, eGFR equals to 144×(Cr/0.7)−1.209×(0.993)age. For males, if Scr is ≤0.9 mg/dl, eGFR equals to 141×(Cr/0.9)−0.411×(0.993)age, and if Scr is >0.9 mg/dl, eGFR equals to 141×(Cr/0.9)−1.209×(0.993)age.
In this present study, we did not attempt to define persistent proteinuria, because a majority of patients had proteinuria measured only once.
CKD STAGES:
Based on the 2012 KDIGO guidelines, CKD patients were classified into 4 categories according to eGFR: stages 1–2 (eGFR ≥60 ml/min/1.73 m2 and urinary ACR ≥30 mg/g), stage 3 (eGFR: 30 to 59 ml/min/1.73 m2), stage 4 (eGFR: 15 to 29 ml/min/1.73 m2), and stage 5 (eGFR <15 ml/min/1.73 m2) [16].
In this study, there were 471, 544, 1214, and 1045 patients being diagnosed to be at CKD stages 1–2, stage 3, stage 4, and stage 5, respectively.
CLINICAL AND BIOCHEMICAL INDEXES:
Hypertension and diabetes were diagnosed at the time of enrollment. Hypertension was defined as systolic blood pressure ≥140 mmHg, diastolic blood pressure ≥90 mmHg, or previous treatment with antihypertensive drugs [22]. Diabetes was defined as fasting plasma glucose ≥7.0 mmol/L [23] or taking hypoglycemic drugs or receiving parenteral insulin therapy.
Peripheral venous blood samples were drawn in the fasting state before admission for clinical treatment. Serum and plasma were separated immediately after centrifugation within 1 h of blood sampling. Serum thyroid hormone concentrations were measured by electrochemiluminescence immunoassay (ECLIA), including total triiodothyronine (T3), total thyroxine (T4), FT3, FT4, and TSH. The reference ranges of T3, T4, FT3, FT4, and TSH are 0.8–2 ng/mL, 5.1–14.1 μg/dL, 2.0–4.4 pg/mL, 0.93–1.7 ng/dL, and 0.27–4.2 μIU/mL, respectively. Creatinine concentrations were measured via the sarcosine oxidase method, and urinary microalbumin was measured by immunoturbidimetry. Urinary ACR was calculated as milligrams of urinary albumin excretion per gram of urinary creatinine. Serum triglycerides (TG), total cholesterol (TC), high-density lipoprotein cholesterol (HDLC), low-density lipoprotein cholesterol (LDLC), hemoglobin A1c (HbA1c), and uric acid (UA) were measured using standard methods. All measurements were completed at the Clinical Laboratory for Endocrinology, China-Japan Friendship Institute of Clinical Medical Sciences.
STATISTICAL ANALYSES:
The χ2 tests for categorical data and Wilcoxon rank sum tests for continuous data were used to assess whether baseline characteristics were different between the 4 CKD stage groups and the control group. Spearman correlation analyses were used to assess the relationship across 5 thyroid hormones due to their skewed distributions. Logistic regression analyses were conducted to assess the association of thyroid hormones with the risk and severity of CKD at a significance level of 5% before and after adjusting for confounders, as well as by applying propensity score matching method to reduce selection bias by equating groups based on confounding factors. Effect-size estimates are expressed as odds ratio (OR) and 95% confidence interval (95% CI).
Prediction accuracy gained by adding significant thyroid hormones was assessed from both discrimination and calibration viewpoints. In this study, net reclassification improvement (NRI) and integrated discrimination improvement (IDI) [24,25] were calculated to judge the discrimination capability of significant thyroid hormones. Calibration capability was evaluated using the −2 log likelihood ratio test, Akaike information criterion (AIC), and Bayesian information criterion (BIC) to see how closely the prediction probability for the addition of significant thyroid hormones reflected the actual observed risk and the global fit of modified risk model [26]. Moreover, the net benefit for the addition was also inspected by decision curve analysis [27], and in this curve, the X-axis denotes thresholds for CKD risk, and the Y-axis denotes net benefits on different thresholds.
Statistical analyses were completed using the STATA software Release 14.1 (Stata Corp, TX, USA). Wherever appropriate, statistics were then adjusted for multiple comparisons using a Bonferroni correction. A P value of less than 0.05 was considered statistically significant.
Results
BASELINE CHARACTERISTICS:
Table 1 shows the baseline characteristics of study participants. CKD patients at stages 1–2, stage 3, and stage 4 were older than controls (P<0.001), but CKD patients at stage 5 were younger (P<0.001). Except for stage 3 (P=0.308), the sex composition differed significantly between CKD patients at different stages and controls (P<0.001). As for thyroid hormones, concentrations of T3, T4, FT3, and FT4 were significantly lower in CKD patients at different stages than in controls (P<0.05); TSH concentrations were significantly lower in CKD patients with stages 1–2 (P<0.05), but significantly higher in CKD patients with stage 4 and stage 5 (P<0.05), than in controls.
CORRELATION ANALYSES:
The correlation plot of 5 thyroid hormones under study is presented in Figure 1. Due to the strong magnitude of correlation between T3 and FT3 (Spearman correlation coefficient r: 0.939, P<0.0001), T4 and FT4 (Spearman correlation coefficient r: 0.711, P<0.0001), only FT3 and FT4 were retained in the following analyses.
RISK PREDICTION FOR CKD:
Prediction of 3 thyroid hormones (FT3, FT4, and TSH) for the risk of CKD at different stages before and after propensity score matching analysis is provided in Table 2. Based on Bonferroni correction for 12 comparisons, associations were considered significant at a P value of less than 0.004. After balancing age, sex, diabetes, and hypertension between cases and controls through propensity score matching analysis, per 0.2 pg/mL increment in serum FT3 was significantly associated with 35–38% reduced risk of CKD at stages 1–4, and the reduction in association with CKD stage 5, albeit marginally significant, was only 2%. With regard to serum FT4, the per 0.3 ng/dL increase was only significantly associated with a 21% reduced risk of CKD at stage 5 (OR: 0.79, 95% CI: 0.69 to 0.89, P<0.001). By contrast, per 0.5 μIU/mL increment in serum TSH increased the risk of CKD stage 5 by 8% (OR: 1.08, 95% CI: 1.02 to 1.14, P=0.003).
PREDICTION ACCURACY ASSESSMENT:
Table 3 shows the prediction accuracy gained by separately adding 3 thyroid hormones aforementioned to the basic model (including age, sex, diabetes, hypertension, TG, TC, HDLC, and UA) for CKD at different stages. From calibration aspects, reduction in both AIC and BIC statistics was greater than 10 after adding each of 3 thyroid hormones to the basic model across all CKD stages. Additionally, likelihood ratio tests revealed statistical significance for FT3 and FT4 at stages 1–4, and for TSH at stages 4–5 at a level of 4%. From discrimination aspects, both NRI and IDI indicated that addition of FT3 to the basic model was significant at stages 1–5, FT4 at stages 3–5, and TSH at stages 1–2 and 4–5 (P <0.004), which was further confirmed by decision curve analysis (Figure 2).
INTERACTION OF THYROID HORMONES:
In view of the significant individual association of 3 thyroid hormones with CKD risk, further interaction exploration was conducted (Table 4). To facilitate interpretation, each thyroid hormone was binarized according to the median value among all study participants, and classified into high and low groups accordingly. To avoid false-positive association, Bonferroni P values of less than 0.004 were considered significant in interaction analysis.
For the interaction between FT3 and FT4, high FT3 and low FT4 (OR: 1.81, 95% CI: 1.30 to 2.55), low FT3 and high FT4 (OR: 17.72, 95% CI: 7.18 to 43.74), and low FT3 and low FT4 (OR: 22.28, 95% CI: 9.68 to 51.30) were associated with the significant risk of CKD at stage 5 in a graded manner. There was also a significant association of low FT3 and low FT4 with CKD at stages 1–2 (OR: 11.93, 95% CI: 4.34 to 32.83) and stage 4 (OR: 10.70, 95% CI: 4.34 to 26.23). For the interaction between FT3 and TSH, there was a significant association of low FT3 and low TSH (OR: 15.93, 95% CI: 6.12 to 41.49), and low FT3 and high TSH (OR: 19.62, 95% CI: 5.88 to 67.53) with CKD at stage 5. Similarly, the interaction between FT4 and TSH was significant for low FT4 and low TSH (OR: 3.59, 95% CI: 1.91 to 6.75), and low FT4 and high TSH (OR: 4.36, 95% CI: 2.38 to 7.96) in association with CKD at stage 5, as well as for low FT4 and high TSH with CKD at stage 4 (OR: 3.24, 95% CI: 1.52 to 6.91).
Discussion
In this retrospective study, we aimed to test the hypothesis that serum thyroid hormones are potential risk predictors for the risk and severity of CKD among Chinese adults. Our findings support this hypothesis that serum FT3 may serve as an early-stage biomarker for CKD, and FT4 and TSH as advanced-stage biomarkers among Chinese adults. Moreover, it is also worth noting that these 3 thyroid hormones may act interactively in predisposition to developing CKD. To the best of our knowledge, this is the first study that has evaluated the association between thyroid hormones and CKD severity among Chinese adults.
The involvement of thyroid hormones in the development of CKD is biologically plausible. It is well known that thyroid hormones play an important role in differentiation, growth, and metabolism, and they are necessary for the normal function of virtually all tissues, including the kidneys [28,29]. Although the molecular mechanisms behind the association between thyroid hormones and CKD are not yet completely understood, it has been reported that thyroid hormones affect renal function via some pre-renal or direct renal effects on cardiac output and the systemic vascular resistance, which further regulates renal blood flow [29–31]. There is also evidence that thyroid hormones affect renal clearance of water load by their effects on GFR [32], and they affect Na reabsorption at the proximal convoluted tubules, primarily by increasing Na/K ATPase activity [33] and tubular potassium permeability [34]. It is thus reasonable to speculate that unfavorable changes in serum thyroid hormones may worsen renal function, which then leads to the development and progression of CKD.
Some studies have examined the association between thyroid hormones and CKD risk, and the results are not often reproducible. For example, in a prospective cohort involving older adults from the Netherlands, there was no detectable association between baseline thyroid hormone concentrations and changes in renal function during follow-up [35]. However, a large prospective study conducted in South Korea showed that normal-to-low levels of FT3 and normal-to-high levels of TSH were associated with an increased risk of incident CKD [36]. By contrast, in a cross-sectional studies from China, TSH was negatively associated with eGFR, and high FT4 was associated with an increased risk of CKD in euthyroid individuals [37]. Another prospective study showed that high FT4, but not TSH and FT3, was associated with an increased risk of incident CKD and rapid eGFR decline in middle-aged and elderly Chinese [15]. Several factors could be behind these conflicting findings. The first factor might be heterogeneity across study populations. Mounting evidence suggests that genetic influences in CKD are polygenic [38], and different populations usually have different genetic profiles and diverse lifestyle patterns [39,40]. This is exemplified by differences between northern and southern Chinese, as wide geographic differences cause various discrepancies due to historical and cultural influences. For instance, the average urinary sodium excretion in northern Chinese is nearly double that in southern Chinese, leading to an average of 7.4 and 6.9 mm Hg increased in systolic and diastolic blood pressure,22 the established risk factor for CKD [8,9]. The second reason might be related to unaccounted residual confounding, which might yield a possible selection bias. The third reason is that the contribution of any individual biomarker to CKD risk is likely to be small, in view of the complex nature of CKD development [41]. Most studies on the association between thyroid hormones and CKD have were conducted in Western countries and among southern Chinese. In this present study, we focused on northern Chinese adults and employed the propensity score matching method to reduce selection bias by equating groups based on age and sex when assessing the association between serum thyroid hormones and the risk and severity of CKD. Our findings revealed that serum FT3 and FT4 are protective factors against CKD susceptibility at different stages, and serum TSH is a risk factor for advanced CKD stages. In clinical practice, thyroid hormones can be easily measured, and thus might be useful in predicting the onset and progression of CKD.
Another important finding of this study is that the 3 thyroid hormones we studied might act in an interactive manner, especially for the interaction between FT3 and FT4 when predicting the risk of CKD stage 5. In most previous studies, thyroid hormones were only investigated individually, and their potential interactions were often overlooked. However, due to multiple subgroups in interaction analysis and the limited number of study participants, especially after propensity score matching, our findings should be considered preliminary and require confirmation in other independent populations.
Several possible limitations should be acknowledged in this study. First, the cross-sectional design precludes further comments on the cause-effect relationship between thyroid hormones and CKD, and all study participants were recruited from one center, requiring further external validation. Second, some unmeasured characteristics of the study participants, such as obesity, might confound the association of thyroid hormones with CKD risk and severity. Third, insufficient sample size or random measurement error may have limited our power to detect phenotype–disease associations. Fourth, all study participants were enrolled from a single hospital, which might have led to population stratification. Fifth, this study involved Chinese adults of Han ethnicity, and extrapolation to other ethnic or racial groups is restricted.
Conclusions
Despite these limitations, our findings indicated that serum FT3 may serve as an early-stage biomarker for CKD, and FT4 and TSH could be used as advanced-stage biomarkers among Chinese adults. Importantly, these thyroid hormones can act interactively in predisposition to the development of CKD. Nevertheless, for practical reasons, we hope that this study will not remain just another endpoint of research instead of beginning to establish background data to further investigate the contributory role of thyroid hormones in the pathogenesis of CKD and as adjuvant therapy to control CKD progression.
Figures
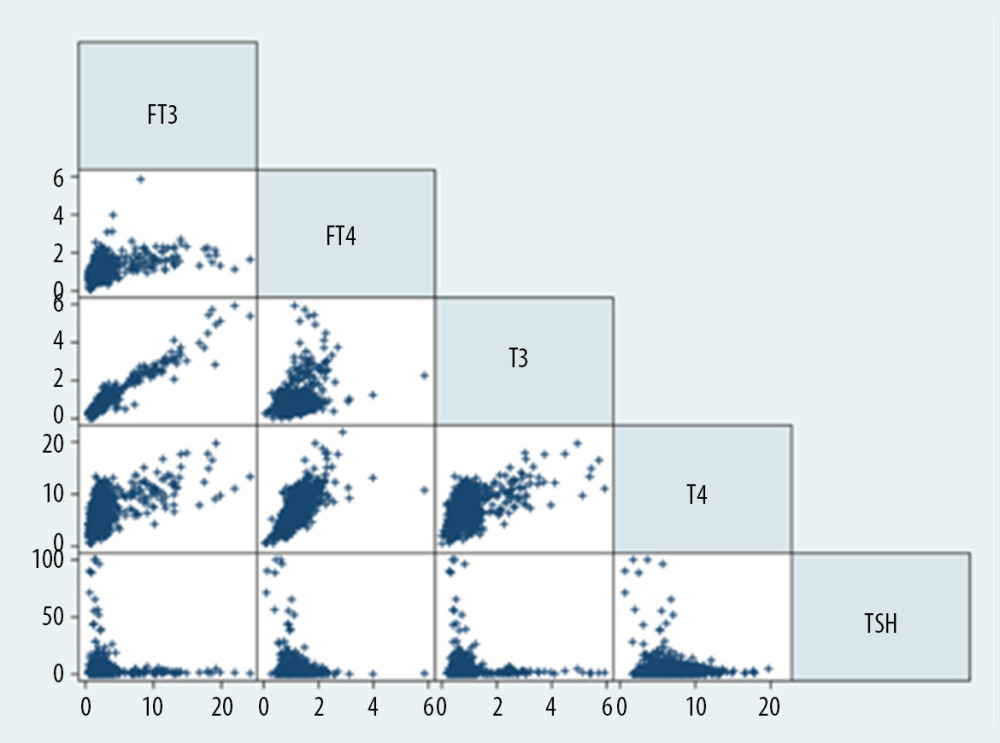 Figure 1. Correlation between total triiodothyronine (T3), total thyroxine (T4), free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) among all study participants.
Figure 1. Correlation between total triiodothyronine (T3), total thyroxine (T4), free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) among all study participants. 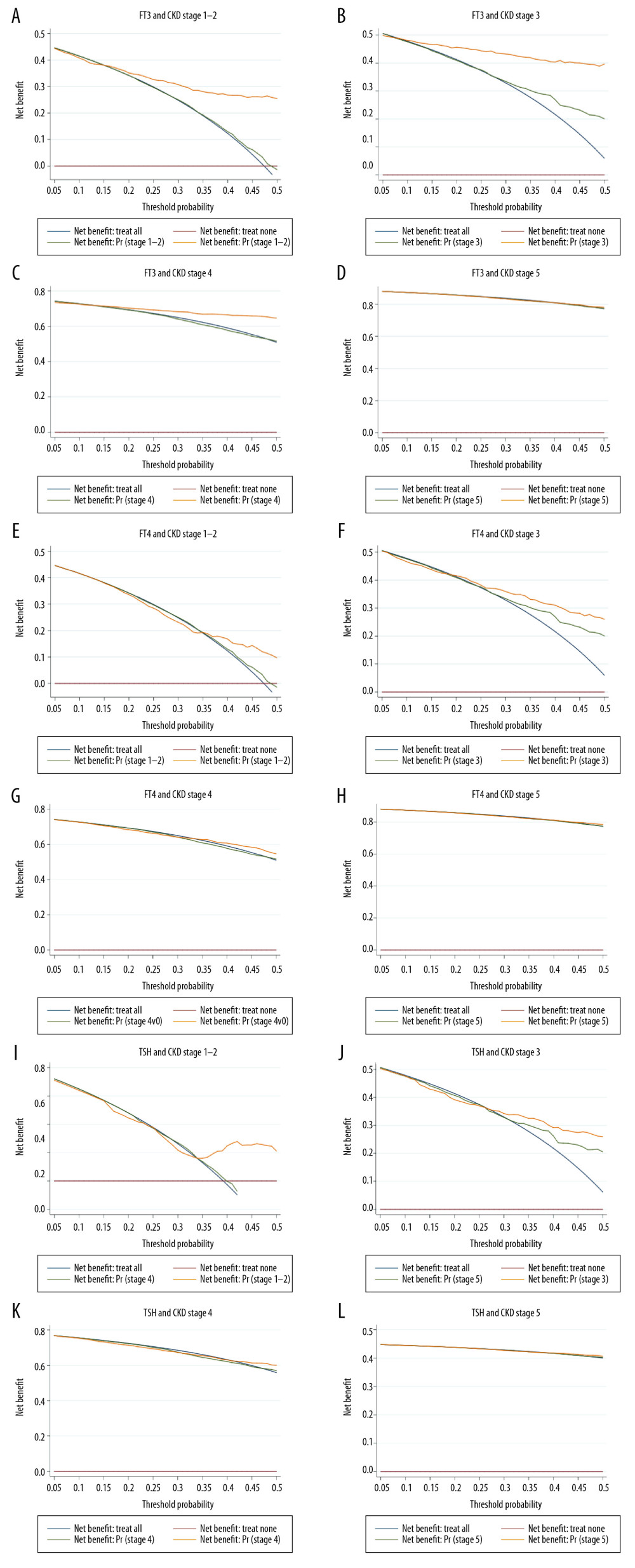 Figure 2. (A–L) Decision curve analysis of adding 3 thyroid hormones (free triiodothyronine or FT3, free thyroxin or FT4, and thyroid-stimulating hormone or TSH) to the basic model in prediction of chronic kidney disease (CKD) at different stages.
Figure 2. (A–L) Decision curve analysis of adding 3 thyroid hormones (free triiodothyronine or FT3, free thyroxin or FT4, and thyroid-stimulating hormone or TSH) to the basic model in prediction of chronic kidney disease (CKD) at different stages. Tables
Table 1. Baseline characteristics of study participants in this retrospective study.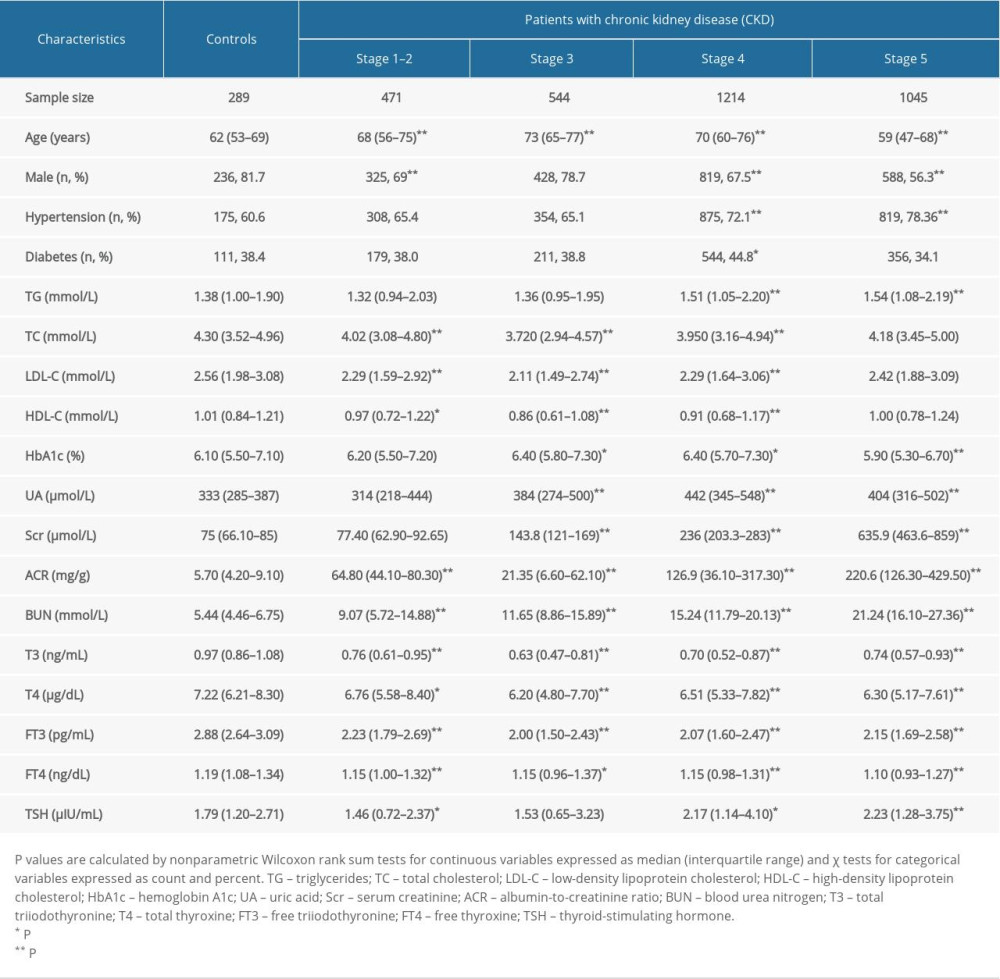 Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages.
Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages.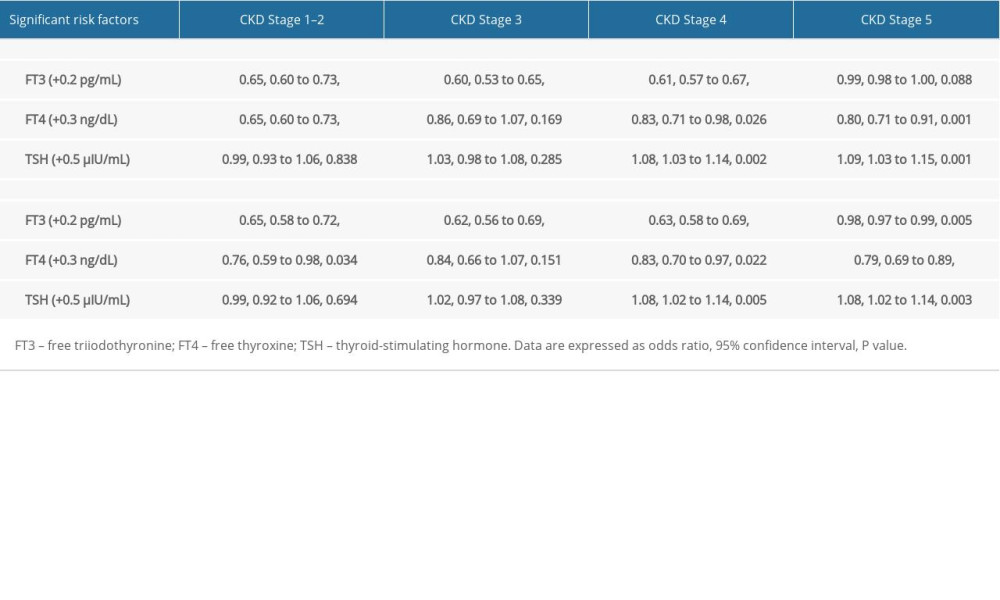 Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages.
Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages.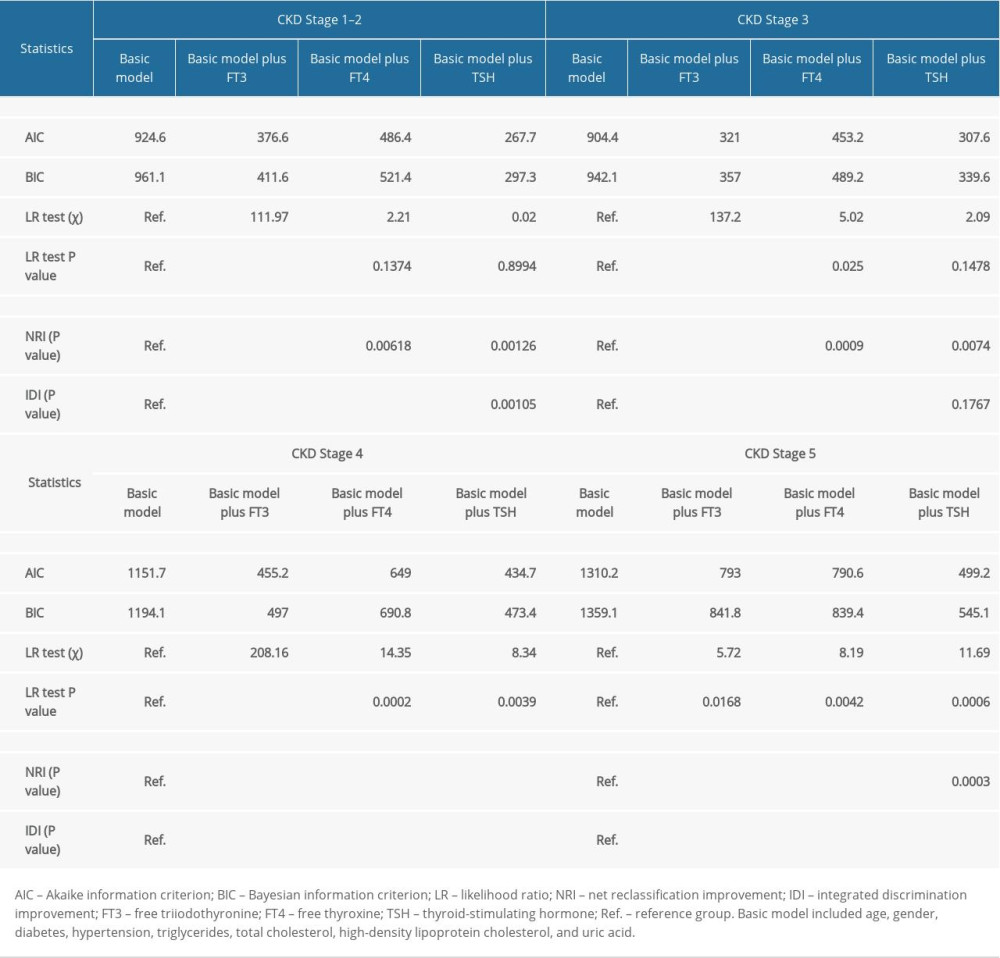 Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages.
Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages.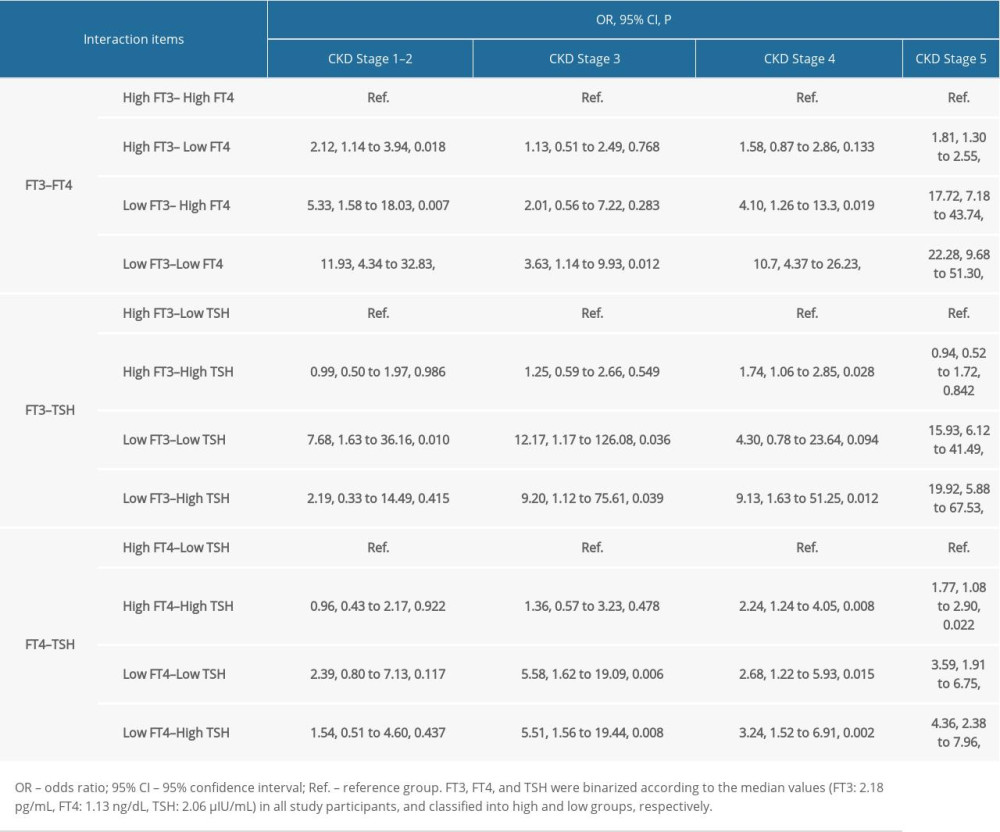
References
1. Jha V, Garcia-Garcia G, Iseki K, Chronic kidney disease: Global dimension and perspectives: Lancet, 2013; 382(9888); 260-72
2. Foley RN, Murray AM, Li S, Chronic kidney disease and the risk for cardiovascular disease, renal replacement, and death in the United States Medicare population, 1998 to 1999: J Am Soc Nephrol, 2005; 16(2); 489-95
3. Perco P, Wilflingseder J, Bernthaler A, Biomarker candidates for cardiovascular disease and bone metabolism disorders in chronic kidney disease: A systems biology perspective: J Cell Mol Med, 2008; 12(4); 1177-87
4. Zhang L, Wang F, Wang L, Prevalence of chronic kidney disease in China: A cross-sectional survey: Lancet, 2012; 379(9818); 815-22
5. Robinson BM, Zhang J, Morgenstern H, Worldwide, mortality risk is high soon after initiation of hemodialysis: Kidney Int, 2014; 85(1); 158-65
6. Saran R, Robinson B, Abbott KC, US Renal Data System 2018 Annual Data Report: Epidemiology of Kidney Disease in the United States: Am J Kidney Dis, 2019; 73(3 Suppl 1); A7-A8
7. Zaman SB, Karim MA, Hossain N, Plasma triglycerides as a risk factor for chronic kidney disease in type 2 diabetes mellitus: Evidence from northeastern Thailand: Diabetes Res Clin Pract, 2018; 138; 238-45
8. James MT, Hemmelgarn BR, Tonelli M, Early recognition and prevention of chronic kidney disease: Lancet, 2010; 375(9722); 1296-309
9. Levey AS, Coresh J, Chronic kidney disease: Lancet, 2012; 379(9811); 165-80
10. Johnson RJ, Wesseling C, Newman LS, Chronic kidney disease of unknown cause in agricultural communities: N Engl J Med, 2019; 380(19); 1843-52
11. Webster AC, Nagler EV, Morton RL, Masson P, Chronic kidney disease: Lancet, 2017; 389(10075); 1238-52
12. Chuang MH, Liao KM, Hung YM, Abnormal thyroid-stimulating hormone and chronic kidney disease in elderly adults in Taipei City: J Am Geriatr Soc, 2016; 64(6); 1267-73
13. Wang X, Zhao X, Huang X, Association of subclinical thyroid dysfunction with chronic kidney disease: A systematic review and meta-analysis: Endocr Res, 2020; 45(1); 41-49
14. Rhee CM, Kalantar-Zadeh K, Streja E, The relationship between thyroid function and estimated glomerular filtration rate in patients with chronic kidney disease: Nephrol Dial Transplant, 2015; 30(2); 282-87
15. Huang X, Ding L, Peng K, Thyroid hormones associate with risk of incident chronic kidney disease and rapid decline in renal function: A prospective investigation: J Transl Med, 2016; 14(1); 336
16. Levin A, Stevens PE, Bilous RW, Kidney disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease: Kidney International Supplement, 2013; 3; 1-150
17. Hsu CY, CKD-EPI eGFR categories were better than MDRD categories for predicting mortality in a range of populations: Ann Intern Med, 2012; 157(10); JC5-12
18. Matsushita K, Mahmoodi BK, Woodward M, Comparison of risk prediction using the CKD-EPI equation and the MDRD study equation for estimated glomerular filtration rate: JAMA, 2012; 307(18); 1941-51
19. Matsushita K, Tonelli M, Lloyd AAlberta Kidney Disease Network, Clinical risk implications of the CKD Epidemiology Collaboration (CKD-EPI) equation compared with the Modification of Diet in Renal Disease (MDRD) Study equation for estimated GFR: Am J Kidney Dis, 2012; 60(2); 241-49
20. Stevens LA, Schmid CH, Greene T, Comparative performance of the CKD Epidemiology Collaboration (CKD-EPI) and the Modification of Diet in Renal Disease (MDRD) Study equations for estimating GFR levels above 60 mL/min/1.73 m2: Am J Kidney Dis, 2010; 56(3); 486-95
21. Levey AS, Stevens LA, Schmid CH, A new equation to estimate glomerular filtration rate: Ann Intern Med, 2009; 150(9); 604-12
22. Chobanian AV, BG , Black HR, Cushman WCNational Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National High Blood Pressure Education Program Coordinating Committee, The seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure: The JNC 7 report: JAMA, 2003; 89; 2560-72
23. American Diabetes Association, Diagnosis and classification of diabetes mellitus: Diabetes Care, 2013; 6(Suppl 1); S67-74
24. Pencina MJ, D’Agostino RB, D’Agostino RB, Vasan RS, Evaluating the added predictive ability of a new marker: From area under the ROC curve to reclassification and beyond: Stat Med, 2008; 7(2); 157-72 discussion 207–12
25. Pencina MJ, D’Agostino RB, Vasan RS, Statistical methods for assessment of added usefulness of new biomarkers: Clin Chem Lab Med, 2010; 8(12); 1703-11
26. Ternes N, Rotolo F, Michiels S, Empirical extensions of the lasso penalty to reduce the false discovery rate in high-dimensional Cox regression models: Stat Med, 2016; 5(15); 2561-73
27. Vickers AJ, Elkin EB, Decision curve analysis: A novel method for evaluating prediction models: Med Decis Making, 2006; 6(6); 565-74
28. Mansourian AR, A review on cardiovascular diseases originated from subclinical hypothyroidism: Pak J Biol Sci, 2012; 5(2); 58-67
29. Basu G, Mohapatra A, Interactions between thyroid disorders and kidney disease: Indian J Endocrinol Metab, 2012; 6(2); 204-13
30. Klein I, Ojamaa K, Thyroid hormone and the cardiovascular system: N Engl J Med, 2001; 344(7); 501-9
31. Vargas F, Moreno JM, Rodriguez-Gomez I, Vascular and renal function in experimental thyroid disorders: Eur J Endocrinol, 2006; 154(2); 197-212
32. Emmanouel DS, Lindheimer MD, Katz AI, Mechanism of impaired water excretion in the hypothyroid rat: J Clin Invest, 1974; 54(4); 926-34
33. Lin HH, Tang MJ, Thyroid hormone upregulates Na,K-ATPase alpha and beta mRNA in primary cultures of proximal tubule cells: Life Sci, 1997; 60(6); 375-82
34. Katz AI, Lindheimer MD, Renal sodium- and potassium-activated adenosine triphosphatase and sodium reabsorption in the hypothyroid rat: J Clin Invest, 1973; 52(4); 796-804
35. Meuwese CL, Gussekloo J, de Craen AJ, Thyroid status and renal function in older persons in the general population: J Clin Endocrinol Metab, 2014; 99(8); 2689-96
36. Zhang Y, Chang Y, Ryu S, Thyroid hormone levels and incident chronic kidney disease in euthyroid individuals: The Kangbuk Samsung Health Study: Int J Epidemiol, 2014; 43(5); 1624-32
37. Wang K, Xie K, Gu L, Association of thyroid function with the estimated glomerular filtration rate in a large Chinese euthyroid population: Kidney Blood Press Res, 2018; 43(4); 1075-83
38. O’Seaghdha CM, Fox CS, Genetics of chronic kidney disease: Nephron Clin Pract, 2011; 118(1); c55-63
39. Lin BM, Nadkarni GN, Tao R, Genetics of chronic kidney disease stages across ancestries: The PAGE study: Front Genet, 2019; 10; 494
40. Rosset S, Tzur S, Behar DM, The population genetics of chronic kidney disease: Insights from the MYH9-APOL1 locus: Nat Rev Nephrol, 2011; 7(6); 313-26
41. Campbell D, Weir MR, Defining, treating, and understanding chronic kidney disease – a complex disorder: J Clin Hypertens (Greenwich), 2015; 17(7); 514-27
Figures
 Figure 1. Correlation between total triiodothyronine (T3), total thyroxine (T4), free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) among all study participants.
Figure 1. Correlation between total triiodothyronine (T3), total thyroxine (T4), free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) among all study participants. Figure 2. (A–L) Decision curve analysis of adding 3 thyroid hormones (free triiodothyronine or FT3, free thyroxin or FT4, and thyroid-stimulating hormone or TSH) to the basic model in prediction of chronic kidney disease (CKD) at different stages.
Figure 2. (A–L) Decision curve analysis of adding 3 thyroid hormones (free triiodothyronine or FT3, free thyroxin or FT4, and thyroid-stimulating hormone or TSH) to the basic model in prediction of chronic kidney disease (CKD) at different stages. Tables
 Table 1. Baseline characteristics of study participants in this retrospective study.
Table 1. Baseline characteristics of study participants in this retrospective study. Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages.
Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages. Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages.
Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages. Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages.
Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages. Table 1. Baseline characteristics of study participants in this retrospective study.
Table 1. Baseline characteristics of study participants in this retrospective study. Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages.
Table 2. Risk prediction of thyroid hormones for chronic kidney disease (CKD) at different stages. Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages.
Table 3. Prediction accuracy gained by adding thyroid hormones to basic model for chronic kidney disease (CKD) at different stages. Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages.
Table 4. Interaction between free triiodothyronine (FT3), free thyroxine (FT4), and thyroid-stimulating hormone (TSH) in prediction of chronic kidney disease (CKD) at different stages. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








