03 July 2020: Clinical Research
Risk Factors for Relapse of Childhood B Cell Acute Lymphoblastic Leukemia
Rongrong Zhang1BCDEF, Haiyan Zhu1BCDF, Yufang Yuan1CDEF*, Jiou Zhao2BCD, Xiaochun Yang1BCF, Zhaofang Tian1ACDEFGDOI: 10.12659/MSM.923271
Med Sci Monit 2020; 26:e923271
Abstract
BACKGROUND: B cell acute lymphoblastic leukemia (B-ALL) is the most common type of ALL. This study aimed to explore risk factors for relapse of childhood B-ALL.
MATERIAL AND METHODS: Total of 102 pediatric B-ALL patients were included in this study. B-ALL patients were divided into a relapse group and a non-relapse group. Chemotherapy-induced agranulocytosis time, fusion gene, and minimal residual disease (MRD) were assessed. White blood cell (WBC) count in peripheral blood and risk stratification were evaluated in newly-diagnosed patients. Kaplan-Meier plots were used to evaluate the correlation between risk factors and relapse rates. Multivariate analysis was performed with Cox proportional hazard model to estimate relative risk (RR), 95% confidence interval (95% CI), and hazard ratio (HR). Finally, 99 cases of B-ALL were included in this study.
RESULTS: There were significant differences between the relapse group and the non-relapse group in age (p=0.004), chemotherapy-induced agranulocytopenia (p=0.001), WBC count in peripheral blood of newly diagnosed patients (p=0.016), risk stratification (p=0.000), and MRD at 12th week (p=0.007). Age over 10 years, high-risk stratification, long period of agranulocytopenia, higher WBC counts, and MRD more than 10⁻⁴ were correlated with higher B-ALL relapse rate (p<0.05). Multivariate analysis showed significantly higher relapse rates for age ≥10 years, high-risk stratification, and MRD at 12th week >10⁻⁴, with RR (95% CI) of 4.001 (1.005–15.930), 4.964 (1.050–23.456), and 4.646 (1.383–15.614), respectively.
CONCLUSIONS: Agranulocytopenia ≤7 days, peripheral blood WBC >100×10⁹/L, and MRD at 33rd day >10⁻⁴ were associated with B-ALL relapse. Age ≥10 years, high-risk stratification, and MRD at 12th week >10⁻⁴ were independent risk factors for relapse.
Keywords: Neoplasm, Residual, Precursor Cell Lymphoblastic Leukemia-Lymphoma, Recurrence, Risk Factors, Antineoplastic Combined Chemotherapy Protocols, B-Lymphocytes, Child, Child, Preschool, Chronic Disease, Disease-Free Survival, Flow Cytometry, Leukocyte Count, Precursor B-Cell Lymphoblastic Leukemia-Lymphoma
Background
Childhood acute lymphoblastic leukemia (ALL) is the most prevalent malignancy of childhood, accounting for more than 80% of all childhood ALL and 25% of cancers in childhood [1,2]. With the use of multi-agent chemotherapy strategies, the long-term clinical outcomes of childhood ALL patients have been significantly improved, with an overall survival (OS) rate more than 90% [3]. B cell acute lymphoblastic leukemia (B-ALL) is the most common type of ALL, accounting more than 70% of cases [4]. However, due to the medical discrepancies among different regions and hospitals in China, the cure rate of ALL is significantly lower than in Europe and the USA [5]. Children with ALL usually have cardiopulmonary impairment, neuromuscular dysfunction, and skeletal pathologies, all of which impede physical function [6]. Although, cytotoxic treatment strategies produce higher cure rates of ALL, they cause higher rates of long-term and acute complications [7]. Despite the satisfactory overall prognosis of pediatric ALL patients, there is an urgent need to discover a more effective and less toxic therapeutic approach.
Better diagnostic strategies (e.g., biopsy, bone marrow aspirate examination, and peripheral blood count) have improved the diagnosis of pediatric ALL [8,9]. In the recent years, many risk factors have been found [10,11], such as osteonecrosis, adolescence, hyperlipidemia, ionizing radiation, genetic diseases, and Down syndrome, which can predict the occurrence of ALL. The most common reason for ALL treatment failure is relapse, especially for patients with B-ALL [12]. However, risk factors for relapse of pediatric ALL are unclear.
We conducted a B-ALL childhood-based study to discover the risk factors for pediatric B-ALL, from January 2010 to January 2015. The detailed information for risk factors were collected from the B-ALL children. This study aimed to explore the risk factors for relapse of childhood B-ALL, as well as to optimize disease assessment and therapeutic strategy to enhance the survival rate of B-ALL children.
Material and Methods
SUBJECTS:
We enrolled 102 pediatric B-ALL patients (including 50 males and 52 females, with mean age of 4.68±2.95 years) at the Pediatric Hematological Tumor Ward, the Affiliated Huaian No. 1 People’s Hospital of Nanjing Medical University (Huaian, China) between January 2010 to January 2015. Inclusion criteria were age less than 18 years old, and immunophenotypic analysis, morphological analysis, cytogenetic testing, and molecular biology examination for diagnosing B-ALL were made using the CCLG-2008 protocol of Beijing Children’s Hospital [13]. The exclusion criteria were patients with Down syndrome, death within 15 days of induced remission chemotherapy, failure to cooperate with treatment, and patient undergoing irregular chemotherapy. All of the above patients were followed up to January 2018, guaranteeing all follow-up periods were more than 6 months. The B-ALL patients were divided into a relapse group (n=23) and a non-relapse group (n=76).
This study was approved by the Ethics Committee of Affiliated Huaian No. 1 People’s Hospital of Nanjing Medical University. The informed consents were obtained from parents of all B-ALL children enrolled in this study.
MEASUREMENT:
All B-ALL patients underwent regular treatment according to the CCLG-2008 protocol of Beijing Children’s Hospital [13]. All of the patients received the same treatments in this study. Data on sex and age were collected. The chemotherapy-induced agranulocytosis time was recorded according to the method described in a previous study [14]. The fusion gene expression was analyzed using the method described in a previous study [15]. The minimal residual disease (MRD) was measured using multi-parameter flow cytometry assay in bone marrow samples, which were collected at day 33 (MRD at 33rd day) and at week 12 (MRD at 12th week) of the remission induction [16].
DEFINITION OF RISK FACTORS:
Subjects were subdivided into 3 age groups: age <1 year, 1 year ≤ age <10 years, and age ≥10 years, according to the method described in a previous study [17]. Chemotherapy-induced agranulocytopenia time factor was subdivided into 3 groups: time ≤7 days, 7 days < time ≤21 days, and time >21 days. The WBC count in peripheral blood of newly diagnosed patients was graded into ≤100×109/L and >100×109/L [18]. The risk stratification was divided into 3 levels: lower (standard) risk (leukocyte count <25×109/L), medium risk (25×109/L ≤ leukocyte count <50×109/L), and high-risk (leukocyte count ≥50×109/L) according to the method described in a previous study [19].
OUTCOMES OF B-ALL CHILDREN:
The outcomes of B-ALL patients were divided into relapse, death, loss to follow-up and disease-free survival according to the method described in a previous study [20]. Relapse was defined as return of leukemia after complete remission based on the morphology determination of bone marrow [21]. Loss to follow-up was defined as when the patient could not be contacted due to any reason. Disease-free survival was defined as when the patient not developing relapse or death from B-ALL diagnosis until the date of last follow-up [22]. Disease-free survival was the primary endpoint. Chemotherapy-induced agranulocytopenia time, WBC count of newly diagnosed patients, risk stratification, and fusion gene expression were the secondary endpoints.
CATEGORY OF B-ALL RELAPSE:
In this study, B-ALL relapse was divided into simple bone marrow relapse, extramedullary relapse, and bone marrow combining extramedullary relapse [23]. Simple bone marrow relapse was defined as lymphoblasts more than 25% (≥25%). Extramedullary relapse was defined as recurrence of B-ALL in the central nervous system and/or testis. Bone marrow combined with extramedullary relapse was defined as lymphoblasts more than 5% (≥5%) and recurrence in 1 or more extramedullary locations [24].
STATISTICAL ANALYSIS:
The data were analyzed using professional SPSS statistical software (version: 17.0, SPSS, Inc., Chicago, IL, USA). The numeric variables are presented as mean±standard deviation (SD) and were analyzed with Tukey’s post hoc test validated by ANOVA for comparing measurement data between groups. The categorical variables are presented as “n” or “%” and were analyzed with the
Results
DEMOGRAPHIC CHARACTERISTICS OF CHILDREN WITH B-ALL:
A total of 102 newly-diagnosed B-ALL children were eligible for the study. We excluded 2 patients with therapy-associated death and 1 patient who was lost to follow-up (Figure 1). Therefore, 99 cases of B-ALL, including relapse cases (n=23, 23.23%) and non-relapse cases (n=76, 76.77%) who completed the baseline testing and follow-up were included in the analysis. Among the 23 cases of relapse B-ALL, there were 19 cases of simple bone marrow relapse, 3 cases of central nervous system relapse, and 1 case of testis relapse.
RISK FACTORS FOR RELAPSE OF B-ALL:
In this study, the relapses of patients in the relapse group occurred from 6 months to 48 months after treatment. The results showed that there were significant differences in age (p=0.004), chemotherapy-induced agranulocytopenia time (p=0.001), WBC count in newly diagnosed peripheral blood (p=0.016), risk stratification (p=0.000), and MRD at 12th week (p=0.007) between the relapse group and non-relapse group (Table 1). However, there were no significant differences for sex (p=0.855), bone marrow progenitor cells in newly diagnosed patients (p=0.161), fusion gene (p=0.421), or MRD at 33rd day (p=0.054) between the 2 groups (Table 1). Therefore, age ≥10 years, chemotherapy-induced agranulocytopenia time, WBC count >100×109/L in peripheral blood of newly diagnosed patients, high risk, and MRD >10−4 at 12th week were proven to be risk factors for B-ALL in this study.
AGE MORE THAN 10 YEARS AND HIGH-RISK STRATIFICATION ASSOCIATED WITH HIGHER RELAPSE RATE OF B-ALL:
Kaplan-Meier validated univariate analysis indicated that the relapse rate in the age ≥10 years group was significantly higher compared to that in the age <1 year group and the 1 year ≤ age <10 years group (Figure 2A, p<0.05). However, there were no significant differences for relapse rate between the age <1 year group and the 1 year ≤ age <10 years group (Figure 2A, p>0.05). Kaplan-Meier analysis showed that the relapse rate in the high-risk stratification group was significantly higher compared to that in the standard and intermediate risk stratification groups (Figure 2B, p<0.05). However, there were no significant differences for relapse rate between the standard group and the intermediate risk stratification group (Figure 2B, p>0.05).
SHORTER PERIOD OF AGRANULOCYTOPENIA AND HIGHER WBC COUNTS WERE CORRELATED WITH RELAPSE RATE OF B-ALL:
According to Kaplan-Meier analysis, there were significant differences for relapse rates between time of agranulocytopenia ≤7 days, and time >21 days (Figure 3A, p<0.05), but there were no differences between 7 days < time ≤21 days and >21 days (Figure 3A, p>0.05), or between 7 days < time ≤21 days and time ≤7 days (Figure 3A, p>0.05). Kaplan-Meier dependent univariate analysis also showed that the relapse rate was significantly higher in the peripheral blood of newly diagnosed patients in the WBC count >100×109/L group compared to that in the ≤100×109/L group (Figure 3B, p<0.05).
:
Our results indicated that MRD at 33rd day in the >10−4 group demonstrated significantly higher relapse rate compared to that in MRD at 33rd day in the ≤10−4 group (Figure 4A, p<0.05). Moreover, for the MRD at 12th week, the relapse rate was significantly higher in the >10−4 group compared to that in the ≤10−4 group (Figure 4B, p<0.05). Therefore, MRD is also a risk factor for higher relapse rate for B-ALL.
MULTIVARIATE ANALYSIS FOR ESTIMATING B-ALL RISK FACTORS WITH COX PROPORTIONAL HAZARD MODEL:
In this study, the Cox proportional hazard model was established and used to conduct multivariate analysis for estimating the risk factors of B-ALL, showing that there were significantly higher relapse rates for age ≥10 years, high-risk stratification, and MRD at 12th week >10−4 (Table 2, p<0.05). Meanwhile, the RR (95% CI) for age ≥10 years, high-risk stratification, and MRD at 12th week >10−4 were 4.001 (1.005–15.930), 4.964 (1.050–23.456), and 4.646 (1.383–15.614), respectively (Table 2).
Discussion
B-ALL accounts for more than 80% of all childhood ALL [25]. B-ALL therapeutic strategies such as CAR-T cell immunotherapy have resulted in continuous improvement of B-ALL therapy [26], with many disease-free survival patients, but approximately 15–20% of patients have B-ALL relapse, with poor outcomes and prognosis [25].
The present study explored the risk factors for childhood B-ALL, and discovered that independent risk factors for B-ALL include age ≥10 years, high-risk stratification, and MRD at 12th week >10−4, the RR (95% CI) of which were 4.001 (1.005–15.930), 4.964 (1.050–23.456), and 4.646 (1.383–15.614), respectively. According to the CCLG-2008 protocol of Beijing Children’s Hospital [13], age of B-ALL children <1 year or ≥10 years are risk factors for poor prognosis of ALL. The China National Study reported that the survival rate of ALL was 60–64% in 2005–2009 [27]; prognosis and outcome are affected by physiological and psychosocial factors, biological heterogeneity, and lack of experience and approaches used by medical teams [28]. Our findings showed that B-ALL children age ≥10 years old are at higher risk of relapse of B-ALL, which is also a reason for the poor prognosis. Therefore, the general chemotherapy regimen might be not be effective for treating B-ALL, and therapeutic strategies targeting B-ALL children ≥10 years old should be used in large treatment centers. The high-risk B-ALL children tend to have one or more risk factors for poor prognosis, including infections, difficult to cure, and death. In this study, we found that the higher-risk B-ALL children were more likely to relapse compared to those with standard- or intermediate-risk B-ALL, which is consistent with previous studies [20,29]. The MRD is the source for relapse of ALL; therefore, it is critical to monitor MRD in the therapeutic process. A previous study [30] also reported that relapse rates are higher in B-ALL children who have MRD at 33rd day ≥10−4, which is consistent with the present Kaplan-Meier analysis results. Research outside China indicated that lower levels of MRD can also induce adverse outcomes. However, due to the different standards for assessment methods, estimating time, and predicted values inside and outside China [31], the significance of lower MRD in ALL has not been previously assessed. However, it is sufficiently consistent for monitoring MRD in definition of risk stratification and guidance of clinical therapy worldwide. Therefore, more complete information about MRD in patients is critical for ALL research.
In addition to the 3 independent risk factors detailed above, we also analyzed the roles of agranulocytopenia time in estimating relapse rates using Kaplan-Meier analysis, which is a novelty of our study. According to Kaplan-Meier analysis, there were significant differences in relapse rates between patients with time of agranulocytopenia ≤7 days and those with time >21 days, but we found no significant differences between patients with 7 days < time ≤21 days and >21 days, or between 7 days < time ≤21 days and time ≤7 days. We speculate that a longer time of chemotherapy-induced agranulocytopenia is associated with longer bone marrow suppression and the more sensitivity to chemotherapy, with better chemotherapeutic efficacy. However, long-term agranulocytopenia also increases the risk of infection [32]. Therefore, it would be a promising research direction to assess the chemotherapy-induced agranulocytopenia time and to accurately predict treatment timing for ALL. Furthermore, B-ALL is more likely to relapse in newly diagnosed children with peripheral blood WBC count more than 100×109/L compared to those with less than 100×109/L, which might be associated with the excessive invasion of tumors in multiple organs. Because of the limited number of cases in this study, we only carried out qualitative research on expression of children’s fusion genes, without further quantitative and classified research. However, the relationship between the fusion genes BCR-ABL1, ETV6-RUNX1, TCF3-PBX1, and IKZF1 and children’s ALL recurrence has been also previously studied [24].
Although this study produced some interesting results, there are also some limitations. First, the sample size in this study was small, which might have affected the accuracy of results. Second, this study only qualitatively studied fusion gene expression and did not perform quantitative and classified analyses. Third, the correlation between the risk factors for B-ALL and the overall survival rate was not clarified in this study, and this needs to be explored in future research.
Conclusions
The present 5-year long-term investigation of B-ALL in our center showed that many risk factors can predict the relapse of B-ALL. We found that age ≥10 years, time of agranulocytopenia ≤7 days, high-risk stratification, peripheral blood WBC count >100×109/L, and MRD at 33rd day/12th week >10−4 predicted B-ALL relapse, and age ≥10 years, high-risk stratification, and MRD at 12th week >10−4 were the independent risk factors for relapse. Additionally, accurate estimation of the degree of severity and precise evaluation for risk stratification, together with effective interventions, would help to enhancement of survival rate of B-ALL patients.
Figures
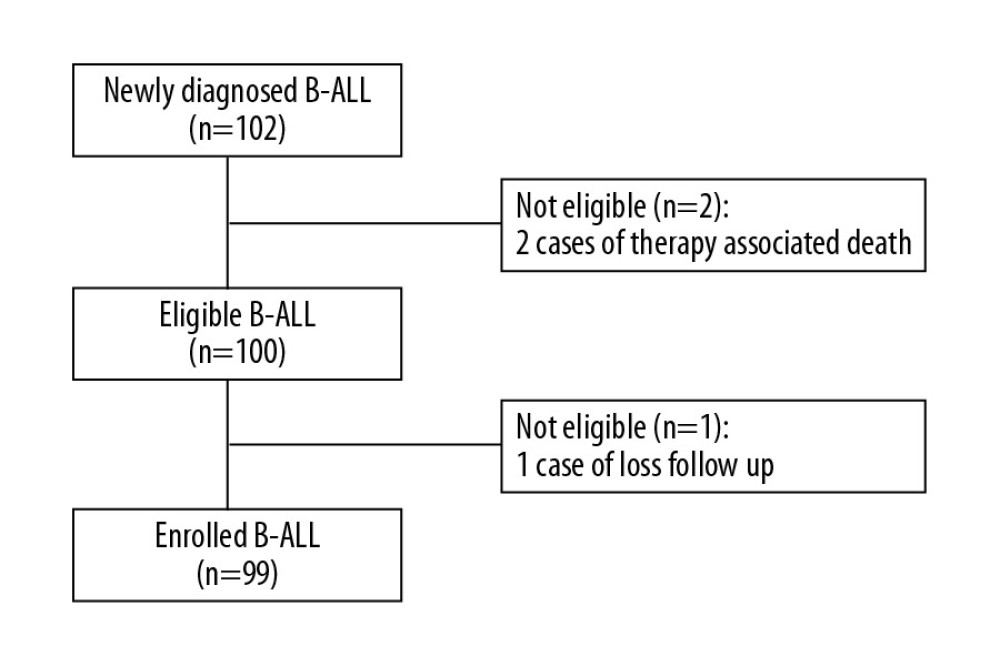 Figure 1. Flow diagram for the included childhood B-ALL cases.
Figure 1. Flow diagram for the included childhood B-ALL cases. 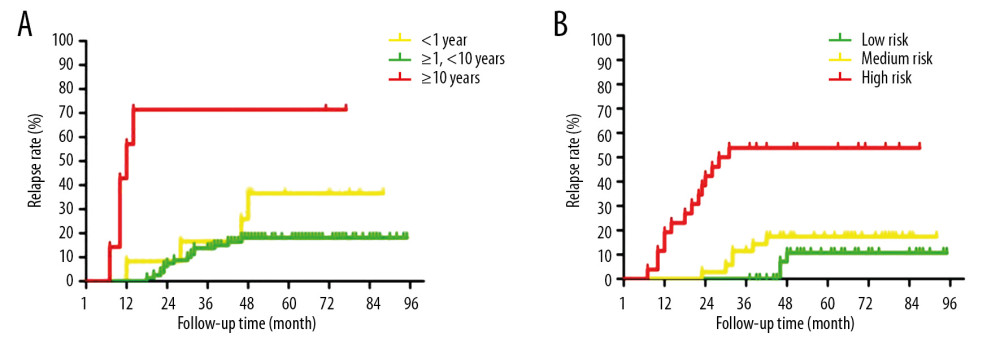 Figure 2. Kaplan-Meier analysis for correlation between relapse rates and age (A) or high-risk stratification (B) of B-ALL patients.
Figure 2. Kaplan-Meier analysis for correlation between relapse rates and age (A) or high-risk stratification (B) of B-ALL patients. 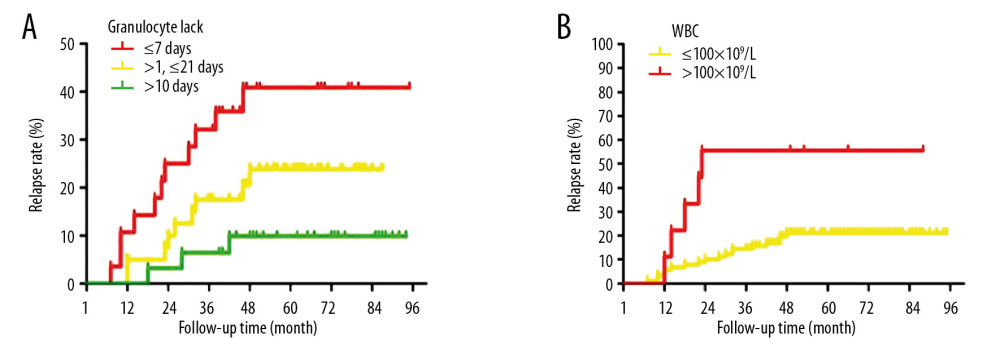 Figure 3. Kaplan-Meier analysis of correlation between relapse rates and time of agranulocytopenia (A) or peripheral blood WBC count in newly-diagnosed patients (B) of B-ALL patients.
Figure 3. Kaplan-Meier analysis of correlation between relapse rates and time of agranulocytopenia (A) or peripheral blood WBC count in newly-diagnosed patients (B) of B-ALL patients. 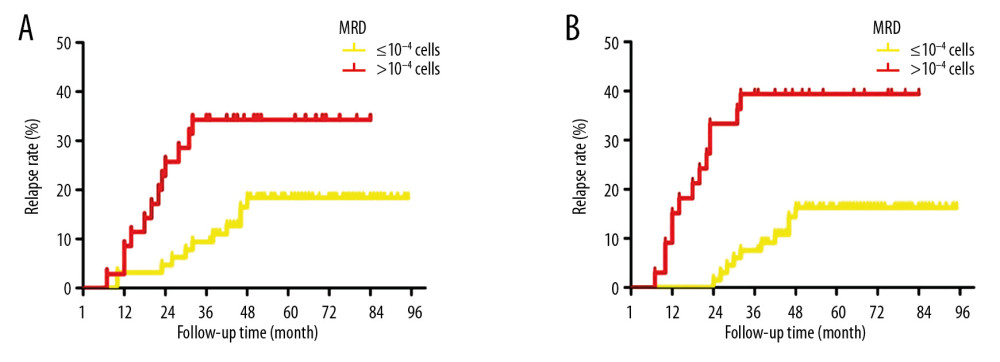 Figure 4. Kaplan-Meier analysis of correlation between relapse rates and MRD at 33rd day (A) or MRD at 12th week (B) in B-ALL patients.
Figure 4. Kaplan-Meier analysis of correlation between relapse rates and MRD at 33rd day (A) or MRD at 12th week (B) in B-ALL patients. References
1. Bhojwani D, Yang JJ, Pui CH, Biology of childhood acute lymphoblastic leukemia: Pediatr Clin North Am, 2015; 62; 47-60
2. Wang Y, Wang X, Tian J, Renal function and plasma methotrexate concentrations predict toxicities in adults receiving high-dose methotrexate: Med Sci Monit, 2018; 24; 7719-26
3. Hunger SP, Loh ML, Whitlock JA, Children’s Oncology Group’s 2013 blueprint for research: Aute lymphoblastic leukemia: Pediatr Blood Cancer, 2013; 60; 957-63
4. Besbes S, Hamadou WS, Boulland ML, Minimal residual disease detection in Tunisian B-acute lymphoblastic leukemia based on immunoglobulin gene rearrangements: Braz J Med Biol Res, 2017; 50; e5426
5. Zheng R, Peng X, Zeng H, Incidence, mortality and survival of childhood cancer in China during 2000–2010 period: A population-based study: Cancer Lett, 2015; 363; 176-80
6. Ness KK, Kaste SC, Zhu L, Skeletal, neuromuscular and fitness impairments among children with newly diagnosed acute lymphoblastic leukemia: Leuk Lymphoma, 2016; 56; 1004-11
7. Oskarsson T, Soerhall S, Arvidson J, Relapsed childhood acute lymphoblastic leukemia in the Nordic countries: Prognostic factors, treatment and outcome: Haematologica, 2016; 101; 68-76
8. Cao W, Liang C, Gen Y, Role of diffusion-weighted imaging for detecting bone marrow infiltration in skull in children with acute lymphoblastic leukemia: Diagn Interv Radiol, 2016; 22; 580-86
9. Hong Y, Zhang J, Guo Q, Diacetyl hexamethylene diamine (CAHB) exerts pro-apoptotic and anti-proliferative function in leukemic T lymphocytes via downregulating PI3K/Akt signaling: Med Sci Monit, 2019; 25; 5211-18
10. Kunstreich M, Kummer S, Laws HJ, Osteonecrosis in children with acute lymphoblastic leukemia: Haematologica, 2016; 101; 1295-305
11. Belson M, Kingsley B, Holmes A, Risk factors for acute leukemia in children: A review: Environ Health Perspect, 2017; 115; 138-45
12. Sakarou M, Eisele L, Duhrsen U, Efficacy of the GMALL-B-ALL/MHL 2002 protocol in Burkitt leukemia/lymphoma and aggressive non-Hodgkin-lymphomas with or without CNS involvement: Eur J Haematol, 2009; 102; 241-50
13. Li SD, Chen YB, Li ZG, Infections during induction therapy of protocol CCLG-2008 in childhood acute lymphoblastic leukemia: A signle-center experience with 256 cases in China: Chin Med J (Endl), 2015; 128; 472-76
14. Wicinski M, Weclewicz MM, Clozapine-induced agranulocytosis/granulocytopenia: Mechanisms and monitoring: Curr Opin Hematol, 2018; 25; 22-28
15. Yaguchi A, Ishibashi T, Terada K, EP300-ZNF384 fusion gene product up-regulates GATA-3 gene expression and induces hematopoietic stem cell gene expression signature in B-cell precursor acute lymphoblastic leukemia cells: Int J Hematol, 2017; 106; 269-81
16. Coustan-Smith E, Song G, Clark C, New markers for minimal residual disease detection in acute lymphoblastic leukemia: Blood, 2011; 117; 6267-76
17. Jaime-Perez JC, Fernandez LT, Jimenez-Castillo RA, Age acts as an adverse independent variable for survival in acute lymphoblastic leukemia, data form a cohort in Northeast Mexico: Clin Lymphoma Myeloma Leuk, 2017; 17; 590-94
18. Isshiki Y, Ohwada C, Sakaida E, CD20 positivity and white and blood cell count predict treatment outcomes in Philadelphia chromosome-negative acute lymphoblastic leukemia patients ineligible for pediatric-inspired chemotherapy: Jpn J Clin Oncol, 2017; 47; 1047-54
19. Pui CH, Carroll WL, Meshinchi S, Biology, risk stratification, and therapy of pediatric acute leukemias: An update: J Clin Oncol, 2011; 29; 551-65
20. Health Quality Ontario, Minimal residual disease evaluation in childhood acute lymphoblastic leukemia: A clinical evidence review: Ont Health Technol Assess Ser, 2016; 16; 1-52
21. Locatelli F, Schrappe M, Bernardo ME, How I treat relapsed childhood acute lymphoblastic leukemia: Blood, 2012; 120; 2807-16
22. Pui CH, Pei D, Raimondi SC, Clinical impact of minimal residual disease in children with different subtypes of acute lymphoblastic leukemia treated with response-adapted therapy: Leukemia, 2017; 31; 333-39
23. Jaime-Perez JC, Pinzon-Uresti MA, Jimenez-Castillo RA, Relapse of childhood acute lymphoblastic leukemia and outcomes at a reference center in Latin America: Organomegaly at diagnosis is a significant clinical predictor: Hematology, 2018; 23; 1-9
24. Ceppi F, Cazzaniga G, Colombini A, Risk factors for relapse in childhood acute lymphoblastic leukemia: Prediction and prevention: Expert Rev Hematol, 2015; 8; 57-70
25. Li Y, Gupta G, Molofsky A, B lymphoblastic leukemia/lymphoma with Burkitt-like morphology and IGH/MYC rearrangement: Report of 3 cases in adult patients: Am J Surg Pathol, 2018; 42; 269-76
26. Davila ML, Brentjens RL, CD-19 targeted CAR T cells as novel cancer immunotherapy for relapsed or refractory B cell acute Lymphoblastic leukemia: Clin Adv Hematol Oncol, 2016; 14; 802-8
27. Zhou Q, Hong D, Lu J, Pediatric medical care system in China has significantly reduced abandonment of acute lymphoblastic leukemia treatment: J Pediatr Hematol Oncol, 2015; 37; 181-84
28. Curran E, Stock W, How I treat acute lymphoblastic leukemia in older adolescents and young adults: Blood, 2015; 125; 3702-10
29. Page KM, Labopin M, Ruggeri A, Factors associated with long-term risk of relapse after unrelated cord blood transplantation in children with acute lymphoblastic leukemia in remission: Biol Blood Marrow Transplant, 2017; 23; 1350-58
30. Horton TM, Whitlock JA, Lu X, Bortezomib reinduction chemotherapy in high-risk ALL in first relapse: A report from the children’s oncology group: Br J Haematol, 2019; 186; 274-85
31. Chen X, Wood BL, Monitoring minimal residual disease in acute leukemia: Technical challenges and interpretive complexities: Blood Rev, 2017; 31; 63-75
32. Faurschou M, Obel M, Baslund B, Long-term risk and outcome of infection-related hospitalization in granulomatosis with polyangiitis: A nationwide population-based cohort study: Scand J Rheumatol, 2018; 47; 475-80
Figures
 Figure 1. Flow diagram for the included childhood B-ALL cases.
Figure 1. Flow diagram for the included childhood B-ALL cases. Figure 2. Kaplan-Meier analysis for correlation between relapse rates and age (A) or high-risk stratification (B) of B-ALL patients.
Figure 2. Kaplan-Meier analysis for correlation between relapse rates and age (A) or high-risk stratification (B) of B-ALL patients. Figure 3. Kaplan-Meier analysis of correlation between relapse rates and time of agranulocytopenia (A) or peripheral blood WBC count in newly-diagnosed patients (B) of B-ALL patients.
Figure 3. Kaplan-Meier analysis of correlation between relapse rates and time of agranulocytopenia (A) or peripheral blood WBC count in newly-diagnosed patients (B) of B-ALL patients. Figure 4. Kaplan-Meier analysis of correlation between relapse rates and MRD at 33rd day (A) or MRD at 12th week (B) in B-ALL patients.
Figure 4. Kaplan-Meier analysis of correlation between relapse rates and MRD at 33rd day (A) or MRD at 12th week (B) in B-ALL patients. Tables
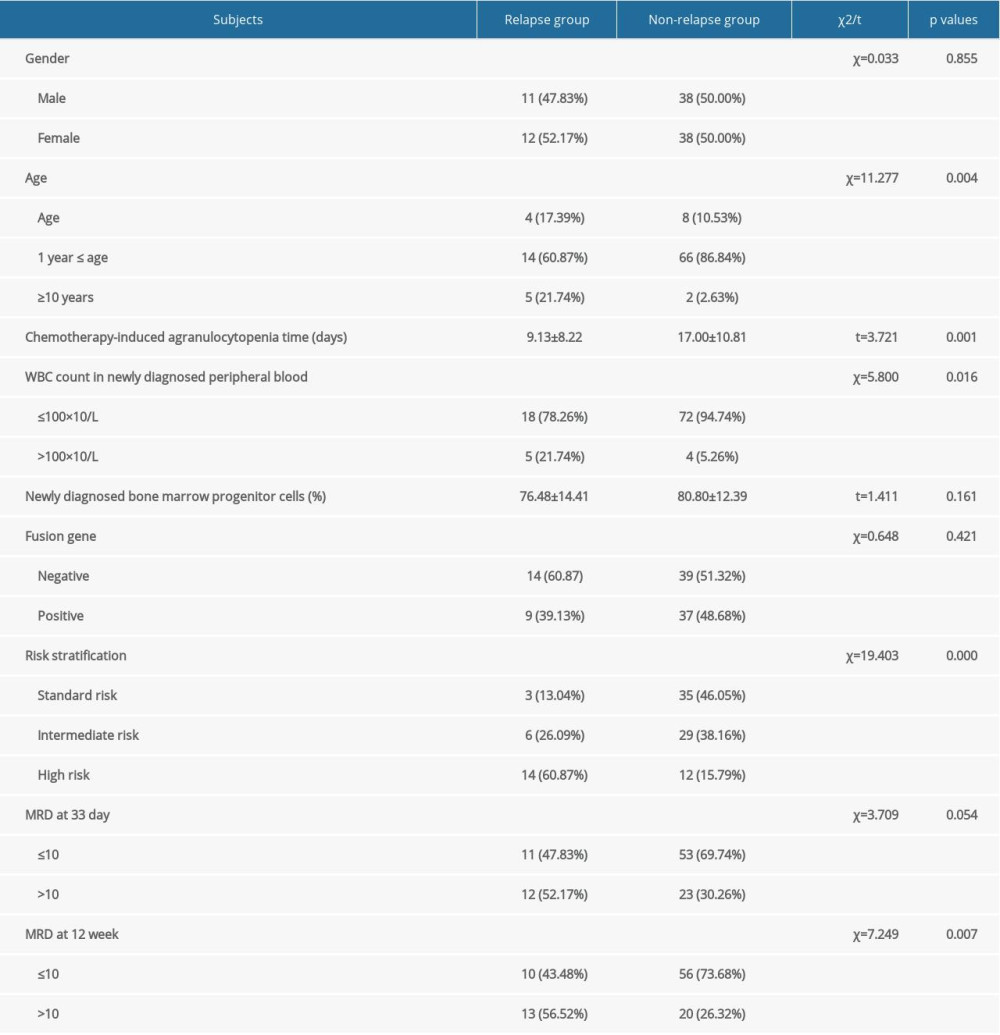 Table 1. Characteristics for the relapse and non-relapse groups of B-ALL patients.
Table 1. Characteristics for the relapse and non-relapse groups of B-ALL patients.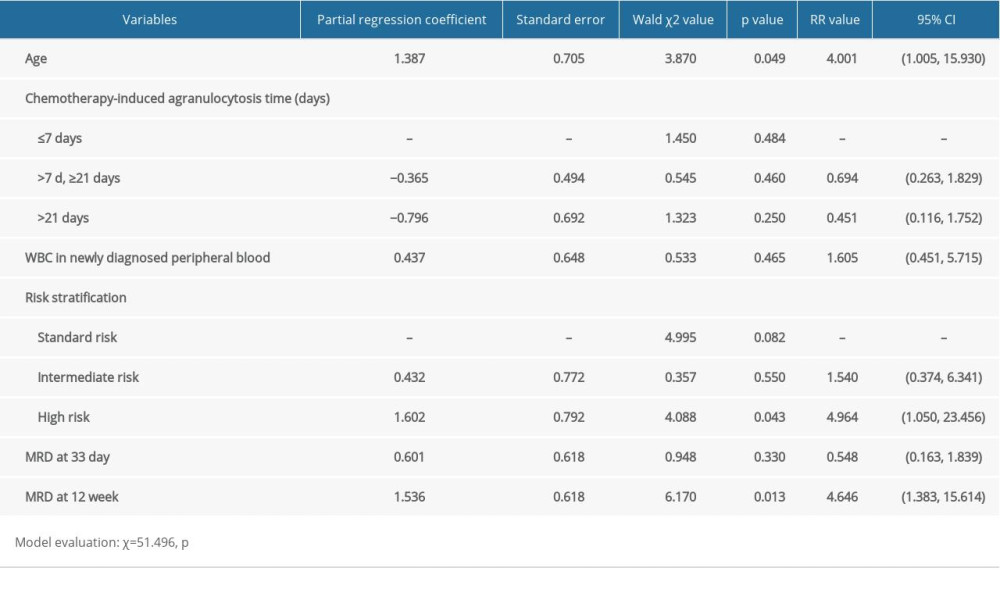 Table 2. Cox regression analysis was conducted to identify risk prognostic factors of relapse in B-ALL children. Model evaluation: χ2=51.496, p<0.001.
Table 2. Cox regression analysis was conducted to identify risk prognostic factors of relapse in B-ALL children. Model evaluation: χ2=51.496, p<0.001. Table 1. Characteristics for the relapse and non-relapse groups of B-ALL patients.
Table 1. Characteristics for the relapse and non-relapse groups of B-ALL patients. Table 2. Cox regression analysis was conducted to identify risk prognostic factors of relapse in B-ALL children. Model evaluation: χ2=51.496, p<0.001.
Table 2. Cox regression analysis was conducted to identify risk prognostic factors of relapse in B-ALL children. Model evaluation: χ2=51.496, p<0.001. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








