03 August 2020: Animal Study
Retinoic Acid-Platinum (II) Complex [RT-Pt(II)] Protects Against Rheumatoid Arthritis in Mice via MEK/Nuclear Factor kappa B (NF-κB) Pathway Downregulation
Ziqiang Cui1BCDE, Yaping Lin2BCD, Yuhong Liu3BCEF, Ling Cao3BDE, Li Cui3ACDEF*DOI: 10.12659/MSM.924787
Med Sci Monit 2020; 26:e924787
Abstract
BACKGROUND: Rheumatoid arthritis (RA) is an inflammatory disorder that is present in approximately 1% of the world’s population. This study was aimed to investigate the effect of retinoic acid-platinum (II) complex [RT-Pt(II)] on rheumatoid arthritis (RA) and to explore the mechanism involved.
MATERIAL AND METHODS: MH7A cell viability was determined by MTT assay and apoptosis was assessed using FACSCalibur flow cytometry. RT-PCR and Western blot assays were used for assessment of mRNA and proteins levels.
RESULTS: Treatment of rheumatoid arthritis with RT-Pt(II) significantly reduced the levels of IL‑1β, IL-6, IL-8, MMP-1, and MMP-13 in synovial fluid of mice in a dose-dependent manner. The expression of iNOS and COX-2 mRNA and protein in rheumatoid arthritis rats was also significantly inhibited by treatment with RT-Pt(II). The TNF-α-induced proliferation of MH7A cells was alleviated by RT-Pt(II) treatment in a concentration-dependent manner. Moreover, RT-Pt(II) treatment induced apoptosis and caused arrest of cell cycle in MH7A cells. The activation of MEK/NF-κB pathway was downregulated by RT-Pt(II) treatment in MH7A cells.
CONCLUSIONS: In summary, the present study demonstrated that RT-Pt(II) inhibits TNF-α-induced inflammatory response, suppresses cell viability, and induces apoptosis in rheumatoid arthritis synovial cells. Moreover, RT-Pt(II) exhibited its effect through targeting the MEK/NF-κB pathway. Therefore, RT-Pt(II) can be used for the development of treatments for rheumatoid arthritis.
Keywords: Anti-Inflammatory Agents, Keratin-16, Rheumatic Fever, Antirheumatic Agents, Arthritis, Rheumatoid, Cell Line, Coordination Complexes, Cyclooxygenase 2, Gene Expression Regulation, Interleukin-6, Interleukin-8, Matrix Metalloproteinase 13, Nitric Oxide Synthase Type II, Platinum Compounds, Synovial Fluid, synoviocytes, Tretinoin
Background
Rheumatoid arthritis (RA) affects more than 1% of the world’s population and is an inflammation-related disorder [1–3]. In China, RA is more prevalent in women than in men and is diagnosed in ~0.50% of the population [4]. The main symptoms in rheumatoid arthritis patients are joint deformation and stiffness, swelling of joints, and cartilaginous tissue destruction [5,6]. RA is believed to be induced by a combination of environmental factors, hereditary, and immunity disorders, but its pathogenesis not yet understood [7]. The treatment for RA-mediated joint decomposition generally aims to delay loss of movement associated with the disorder [8]. The articular cartilage erosion is caused directly by the hyperplastic synovial tissues in patients with RA. The synovial fibroblasts possess proliferation ability similar to those of tumors, resulting in the formation of synovial hyperplasia [9,10]. These fibroblasts mainly contribute to the pathogenesis of RA by aggregating in hyperplastic synovium [9,10]. The accumulation of inflammatory cytokines and over-production of MMPs act as mediators for development of joint inflammation, which subsequently damages joints [10]. Recent studies have mainly focused on synovial fibroblast proliferation inhibition to explore the pathogenesis and for development of RA treatment [11–13]. Thus, targeting proliferation and activating apoptosis of the synovial tissues is the most common aim for treatment of RA [14]. Although there has been significant progress in RA therapeutic strategies, the efficacy remains unsatisfactory. Thus, effective and novel therapies to treat RA are urgently needed. Multiple disorders, including chronic inflammatory disorder, cardiovascular disease, and aging, are associated with oxidative stress. In humans, a well-established antioxidant system consisting of enzymes and antioxidant compounds perform repair and re-synthesis of damaged tissues [15]. The pathology of RA has been found to be very closely involved in oxidative responses in animal models [16]. Among many factors, TNF-α and IL-1β play a prominent role in the progression of RA [17]. The studies have demonstrated that COX-2 and COX-1 are involved in the development of inflammation [18,19]. The COX enzyme is very useful for the formation of prostaglandins and it aggravates cellular inflammation [18,19]. Rheumatoid arthritis involves chronic inflammatory responses and synovial hyperplasia, leading to degradation of connecting bones and cartilages at joints [20–22]. It is a chronic inflammatory disorder damaging many peripheral joints, followed by extra-articular decomposition [23]. The patients experience chronic pain, numbness, gain weight, joints swelling, and loss movement, and there is a burning sensation in the muscles [24]. The present study investigated the role of retinoic acid-platinum (II) complex [RT-Pt(II)] in the treatment of RA and explored the underlying molecular mechanism.
Material and Methods
CELL CULTURE:
Rheumatoid arthritis synovial MH7A cells were provided by the Cell Bank of the Chinese Academy of Sciences (Shanghai, China). Cells were incubated for 24 h in RPMI-1640 medium mixed with FBS (10%) plus a mixture of antibiotics-penicillin and streptomycin (100 μg/ml) in an atmosphere of 5% CO2 at 37°C. To induce RA, RT-Pt(II)-treated cells incubated for 48 h were stimulated at 37°C with 10 ng/ml concentration of TNF-α for 24 h.
VIABILITY ASSAY:
MH7A cells (3×105 cells/well) put in 96-well plates and treated with RT-Pt(II) at 0.25, 0.5, 1.0, 2.0, 4.0, 8.0, and 12 μM doses. Cells were incubated for 48 h, followed by stimulation for 24 h with TNF-α at 37°C to induce RA. Then, MTT solution at 0.5 mg/ml concentration was added to each well and cells were then incubated for 4 h. Formazan crystals in the wells were dissolved by adding 120 μl DMSO. Absorbance was recorded at 587 nm for viability measurement using a microplate reader.
APOPTOSIS ASSAY:
Cells (2×105 cells/well) in 96-well plates were treated with 4 and 12 μM doses of RT-Pt(II). Then, 10 ng/ml of TNF-α was added to wells and cells were incubated for 24 h. Cells were washed in PBS and treated with 400 μl binding buffer and then dyed for 40 min in the dark at 4°C using 5 μl Annexin V-FITC. Cell staining with propidium iodide (10 μl) was carried out for 20 min in the dark at room temperature to detect apoptotic changes. FACSCalibur flow cytometry was used for cell apoptosis detection and FlowJo software was used for analysis of apoptosis.
ELISA:
Cells treated with 4 and 12 μM RT-Pt(II) were stimulated with 10 ng/ml TNF-α for 24 h. The cell culture was centrifuged at 1550 g and 4°C for 15 min to obtain the supernatants. The levels of cytokines – IL-1β (Ab100562), IL-6 (Ab46027), IL-8 (Ab46032), MMP-1 (Ab100603), and MMP-13 (Ab100605) – were assessed using commercially available ELISA kits (Abcam, Cambridge, UK).
REVERSE TRANSCRIPTION QUANTITATIVE POLYMERASE CHAIN REACTION (RT-QPCR):
The RNA from RT-Pt(II)-treated cells was obtained using TRIzol® reagent. The PrimeScript™ RT kit (Takara Bio, Inc., Otsu, Japan) was used for synthesis of cDNA. To perform qPCR, the SYBR® Premix Ex Taq™ II was used. The procedure involved: amplification for 10 min at 93°C, then 38 cycles for 12 s at 93°C and for 25 s at 70°C, followed by 2 min at 76°C. The PCR samples were analyzed for gene expression by 2−ΔΔCq method [26] using GAPDH as control. The primers were:
WESTERN BLOT ANALYSIS:
After treatment with 4 and 12 μM RT-Pt(II), cells were stimulated with 10 ng/ml TNF-α for 24 h. Protein extraction from cells was performed using RIPA buffer and quantified by BCA assay. The protein resolution was achieved on 10% SDS-PAGE by loading 25-μg samples per lane. Proteins were transferred to PVDF membranes blocked with 5% non-fat milk plus 0.1% Tween-20 for 1.5 h. Incubation with anti-p-Mek1/2, anti-p-p65, anti-iNOS, anti-COX-2, anti-Bax, and anti-β-actin primary antibodies (Cell Signaling Technology, Inc., Danvers, MA, USA) was performed overnight at 4°C. Then, incubation with secondary antibodies was carried out at room temperature for 2.5 h. The immunoblots were assessed using a chemiluminescence kit (Cell Signaling Technology, Inc.) and quantified by Gel-Pro Analyzer (version 6.3; Media Cybernetics, Inc., Rockville, MD, USA).
EXPERIMENTAL ANIMALS:
We obtained 40 Sprague-Dawley rats (weighing 260–320 g) from the Animal Center of Shandong University (Shandong, China). The rats were individually caged in sterile cages in the Animal Center with 65% humidity and 23±2°C and 12/12-h light/dark cycles. The rats were given free access to laboratory food and water. The experimental protocols were conducted in accordance with the guidelines issued by the Animal Care and Use Committee, NIH, China. The study was approved by Yan’an University Affiliated Hospital, approval number 202004-0028.
ESTABLISHMENT OF RA MODEL AND TREATMENT:
A previously reported established protocol was used for development of rheumatoid arthritis in rats [11]. After acclimatization in the laboratory, the rats were intraperitoneally injected with 50 mg/kg sodium pentobarbital. Then, Freund’s adjuvant (Sigma-Aldrich, St. Louis, MO, USA) was injected between the 2nd and 3rd toes. The rats developed inflammatory swelling in the right ankle, and inflammation in the nodes of the forelimbs, ears, and tail. The rats were separated into 4 groups of 10 animals each. Rats in the model RA and control groups were given normal saline, and rats in the 2 treatment groups received 2 or 5 mg/kg RT-Pt(II) intragastrically as a single dose.
DETERMINATION OF ARTHRITIC SCORE:
The rats were evaluated for arthritis score microscopically on the 7th, 14th, and 21st days of treatment. Arthritis development in entire paw and digits was scored 11–15 points, arthritis in >2 joints was scored 6–10 points, arthritis formation in 2 joints was scored 1–5 points, and no arthritis was scored 0 points.
OXIDATIVE STRESS MEASUREMENT:
The RA rats were treated with 2 and 5 mg/kg doses of RT-Pt(II), and blood samples from peripheral vessels were collected on day 21 after treatment. The samples were subjected to centrifugation at 2500 g and 4°C for 15 min. The malondialdehyde level and catalase, glutathione peroxidase, and superoxide dismutase activities in the supernatants were analyzed using commercial kits (Beijing Boaosen Biotechnology, Beijing, China).
STATISTICAL ANALYSIS:
The data are expressed as mean±standard deviations of triplicate measurements. Statistical analysis of the data was performed using SPSS 16.0 software (SPSS, Inc., Chicago, IL, USA). For determination of statistically significant differences, the
Results
INHIBITION OF TNF-α-MEDIATED UPREGULATION OF CELLULAR PROLIFERATION BY RT-PT(II):
The TNF-α treatment significantly (P<0.05) increased the proliferative ability of MH7A cells compared to the unstimulated control group (Figure 1). However, RT-Pt(II) exposure alleviated TNF-α-mediated enhancement of MH7A cell proliferative ability in a concentration-dependent manner. The increased proliferative ability mediated by TNF-α was significantly (P<0.02) alleviated by RT-Pt(II) exposure at doses of 0.25 to 12 μM. The inhibition of TNF-α-mediated proliferative ability of cells was alleviated completely by exposure to 12 μM RT-Pt(II) for 48 h.
RT-PT(II) REVERSED THE INHIBITORY EFFECT OF TNF-α ON CELL APOPTOSIS:
The TNF-α treatment of MH7A cells suppressed apoptotic death compared to non-stimulated control cells (Figure 2A). However, RT-Pt(II) treatment at 4 and 12 μM significantly (P<0.05) reversed the apoptosis-inhibiting effect of TNF-α in MH7A cells. The TNF-α-mediated MH7A cell apoptosis suppression was alleviated completely by 12 μM RT-Pt(II) at 72 h. In TNF-α-stimulated MH7A cells, the Bcl-2 level was markedly elevated relative to non-stimulated control cells (Figure 2B). There was TNF-α-mediated downregulation of Bax in MH7A cells. However, RT-Pt(II) exposure at 4 and 12 μM reversed the elevation of Bcl-2 and downregulation of Bax by TNF-α stimulation in MH7A cells.
RT-PT(II) INHIBITED TNF-α-MEDIATED INFLAMMATORY CYTOKINES:
In TNF-α-stimulated MH7A cells, a marked elevation of matrix metalloproteinase-1/-13 and interleukins-1b/-6/-8 levels was observed compared to control cells (Figure 3). The RT-Pt(II) treatment at 4 and 12 μM concentrations markedly suppressed TNF-α-mediated elevation of these factors. The TNF-α mediated promotion of cytokines was alleviated completely on exposure to 12 μM RT-Pt(II).
RT-PT(II) SUPPRESSED TNF-α-INDUCED INOS AND COX-2 EXPRESSION:
In TNF-α-exposed MH7A cells, the level of iNOS was much higher relative to non-stimulated control cells (Figure 4). The COX-2 in TNF-α-exposed cells was also over-expressed relative to non-stimulated control cells. Treatment with 4 and 12 μM RT-Pt(II) alleviated upregulation of iNOS and COX-2 in TNF-α-exposed MH7A cells. The TNF-α-mediated iNOS/COX-2 upregulation was alleviated completely by treatment with 12 μM RT-Pt(II).
RT-PT(II) ALLEVIATES TNF-α-INDUCED MEK/NF-κB ACTIVATION:
In TNF-α-exposed MH7A cells, the p-MEK/1/2 expression was markedly higher relative to the control cells (Figure 5). The TNF-α exposure also caused marked elevation of p-p65 expression in MH7A cells. In RT-Pt(II)-pre-treated cells, the TNF-α-mediated elevation of p-MEK/1/2 expression was markedly reversed. Additionally, RT-Pt(II) pretreatment also reversed TNF-α-mediated elevation of p-p65 expression in MH7A cells.
RT-PT(II) INHIBITS ARTHRITIC SCORE IN RA RATS:
In RA rats, the arthritic score was much higher relative to the normal control rats on days 7, 14, and 21 (Figure 6). The RT-Pt(II) treatment of the RA rats significantly (P<0.01) reduced arthritic score relative to the RA group. The reduction of arthritic score by RT-Pt(II) treatment was more prominent in the 2 mg/kg group compared to the 5 mg/kg group.
REGULATION OF NF-κB P65 AND INTERLEUKINS-1β/-6 BY RT-PT(II):
The NF-κB p65 level on day 21 was much higher in RA rats relative to the normal group (Figure 7). Moreover, interleukins-1β/-6 levels were also elevated in RA rats relative to normal group. However, RT-Pt(II) treatment of the rats at 2 and 5 mg/kg doses reversed RA-induced higher expression of NF-κB p65. The RT-Pt(II) treatment also suppressed RA-mediated increased activities of interleukins-1β/-6 in the rats on day 21.
RT-PT(II) TREATMENT OF RA RATS SUPPRESSED COX-2:
In RA rats, assessment of COX-2 expression showed markedly higher level relative to the normal group (Figure 8). The RT-Pt(II) at 2 and 5 mg/kg doses significantly (P<0.05) reversed RA-mediated elevation of COX-2 expression on day 21. The COX-2 expression suppression by RT-Pt(II) was more prominent in the 5 mg/kg treatment group compared to the 2 mg/kg group.
Discussion
The present study demonstrated that RT-Pt(II) inhibits RA-mediated inflammatory responses
Retinoic acid is well known for its role in multiple physiological pathways, including inflammation, embryogenesis, cell differentiation/proliferation, and morphogenesis [25]. It exhibits an immunomodulatory effect [26], acts as an antitumor agent, and has been used to treat inflammatory diseases of the skin [27–29] and acute promyelocytic leukemia [30]. In rheumatoid arthritis, which is a typical autoimmune disorder, retinoic acid has been demonstrated to exhibit a therapeutic role in the animal models [31–34]. Therefore, the present study hypothesized that RT-Pt(II) may have therapeutic importance for the treatment of rheumatoid arthritis. Synovial hyperplasia and pathogenesis of RA is mainly associated with synovial fibroblasts [10–13]. These cells are involved in the inflammatory processes and angiogenesis, which subsequently result in decomposition of joint bones and cartilages [35,36]. The present study evaluated RT-Pt(II) as an anti-proliferative molecule against MH7A cells
Research on RA pathogenesis has revealed involvement of various cytokines (e.g., TNF-α and IL-6). Studies have proved that biological agents which target TNF-α and IL-6 cytokines are more potent than conventional antirheumatic drugs used for the management of disease [41–44]. In the RA cell model, iNOS and COX-2 levels were found to be markedly upregulated relative to normal cells [28,40]. In the present study, a marked elevation of interleukins-1β/-6/-8 and matrix metalloproteinase-1/-13 was observed in MH7A cells by TNF-α induction. However, pretreatment of MH7A cells with RT-Pt(II) alleviated TNF-α induced upregulation of cytokines. The TNF-α-mediated cytokine upregulation was significantly alleviated by RT-Pt(II) pretreatment at 12 μM. The RT-Pt(II) pretreatment reversed upregulation of iNOS expression and inhibited TNF-α-stimulated COX-2 overexpression in MH7A cells. It is reported that inhibition of the MEK/NF-κB pathway in inflammatory disorders has a protective effect [45]. In the present study, RT-Pt(II) pretreatment suppressed TNF-α-mediated activation of the MEK/NF-κB pathway. These findings suggest that RT-Pt(II) alleviates RA by targeting the MEK/NF-κB pathway.
Conclusions
Thus RT-Pt(II) inhibited RA induced by TNF-α
Figures
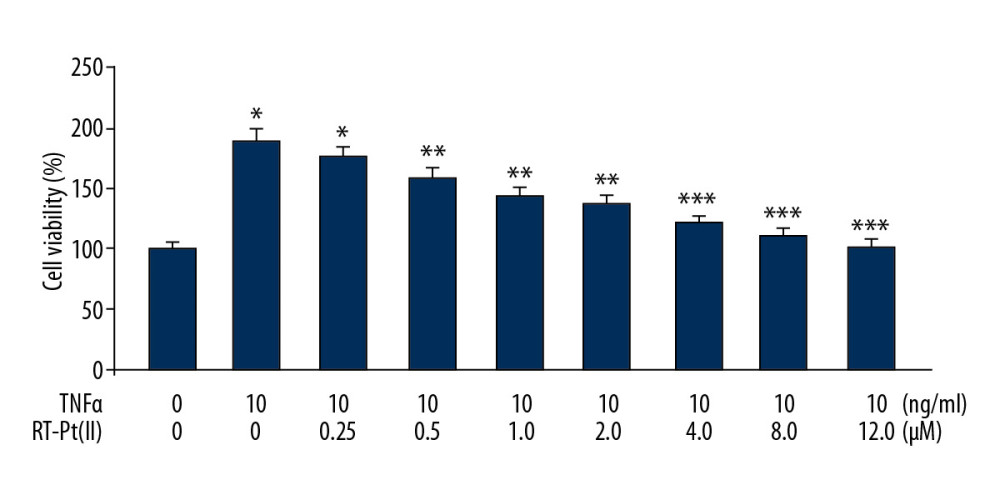 Figure 1. Effect of RT-Pt(II) on proliferation up-regulation by TNF-α in vitro. The RT-Pt(II) exposed cells at 0.25 to 12 μM concentration for 48 h were treated with TNF-α. The changes in proliferative abilities were measured at 72 h of exposure to RT-Pt(II) by MTT assay. * P<0.05, ** P<0.02 and ** P<0.01 vs. TNF-α stimulated cells.
Figure 1. Effect of RT-Pt(II) on proliferation up-regulation by TNF-α in vitro. The RT-Pt(II) exposed cells at 0.25 to 12 μM concentration for 48 h were treated with TNF-α. The changes in proliferative abilities were measured at 72 h of exposure to RT-Pt(II) by MTT assay. * P<0.05, ** P<0.02 and ** P<0.01 vs. TNF-α stimulated cells. 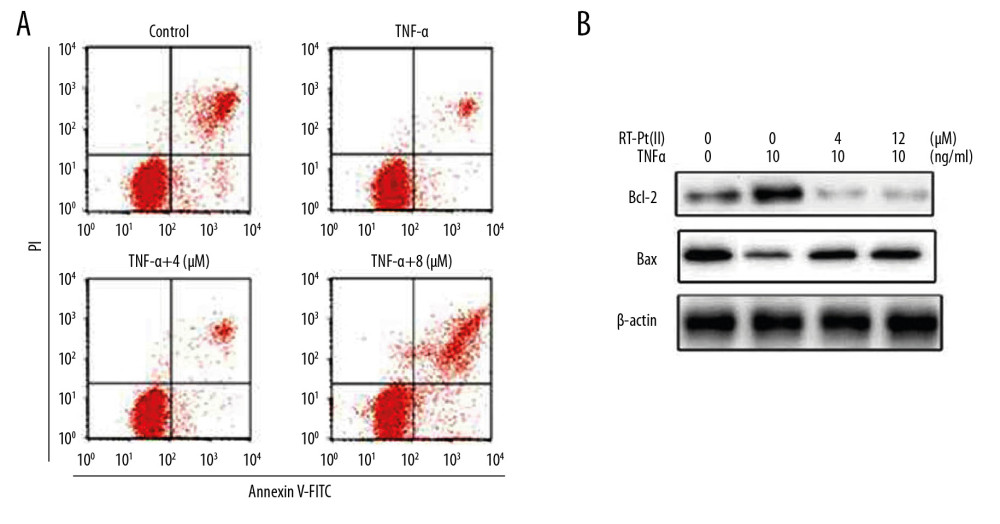 Figure 2. Effect of RT-Pt(II) on MH7A cell apoptosis. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations were treated with TNF-α at 48 h. (A) The cellular apoptosis at 72 h of RT-Pt(II) treatment was analyzed by flow cytometry. (B) The protein expression at 72 h of RT-Pt(II) treatment was assessed by western blotting.
Figure 2. Effect of RT-Pt(II) on MH7A cell apoptosis. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations were treated with TNF-α at 48 h. (A) The cellular apoptosis at 72 h of RT-Pt(II) treatment was analyzed by flow cytometry. (B) The protein expression at 72 h of RT-Pt(II) treatment was assessed by western blotting. 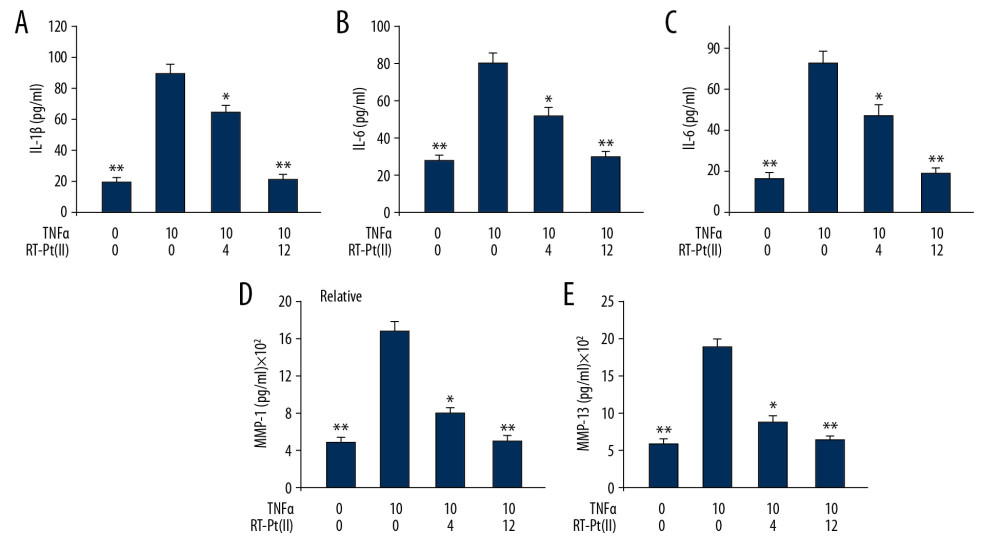 Figure 3. (A–E) Effect RT-Pt(II) on matrix metalloproteinase-1/-13 and interleukins-1β/-6/-8 levels. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations for 48 h were treated with TNF-α. The level of proteins was detected using ELISA assays at 72 h of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. TNF-α treated control
Figure 3. (A–E) Effect RT-Pt(II) on matrix metalloproteinase-1/-13 and interleukins-1β/-6/-8 levels. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations for 48 h were treated with TNF-α. The level of proteins was detected using ELISA assays at 72 h of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. TNF-α treated control 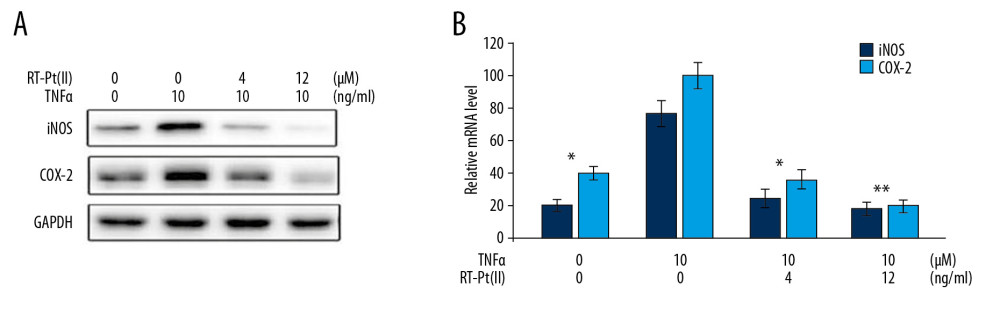 Figure 4. Effect of RT-Pt(II) on iNOS/COX-2 in TNF-α exposed cells. The RT-Pt(II) treated cells at 4 and 12 μM concentrations for 48 h were exposed to TNF-α. (A) The protein levels were measured at 72 h of RT-Pt(II) treatment by western blotting. (B) In RT-Pt(II) treated cells mRNA levels were analyzed at 72 h using RT-PCR. * P<0.02 and ** P<0.01 vs. TNF-α treated cells.
Figure 4. Effect of RT-Pt(II) on iNOS/COX-2 in TNF-α exposed cells. The RT-Pt(II) treated cells at 4 and 12 μM concentrations for 48 h were exposed to TNF-α. (A) The protein levels were measured at 72 h of RT-Pt(II) treatment by western blotting. (B) In RT-Pt(II) treated cells mRNA levels were analyzed at 72 h using RT-PCR. * P<0.02 and ** P<0.01 vs. TNF-α treated cells. 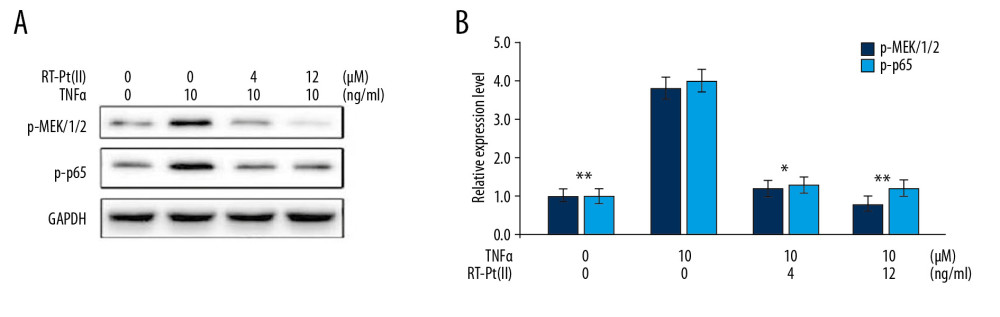 Figure 5. Effect of RT-Pt(II) on MEK/NF-κB phosphorylation. The RT-Pt(II) exposed cells at 4 to 12 μM were treated with TNF-α at 48 h of exposure. (A) The measurement of phosphorylation for MEK/NF-κB (p-665) was performed by western blotting at 72 h of RT-Pt(II) treatment. (B) Semi-quantification of the data * P<0.02 and ** P<0.01 vs. TNF-α treated cells.
Figure 5. Effect of RT-Pt(II) on MEK/NF-κB phosphorylation. The RT-Pt(II) exposed cells at 4 to 12 μM were treated with TNF-α at 48 h of exposure. (A) The measurement of phosphorylation for MEK/NF-κB (p-665) was performed by western blotting at 72 h of RT-Pt(II) treatment. (B) Semi-quantification of the data * P<0.02 and ** P<0.01 vs. TNF-α treated cells. 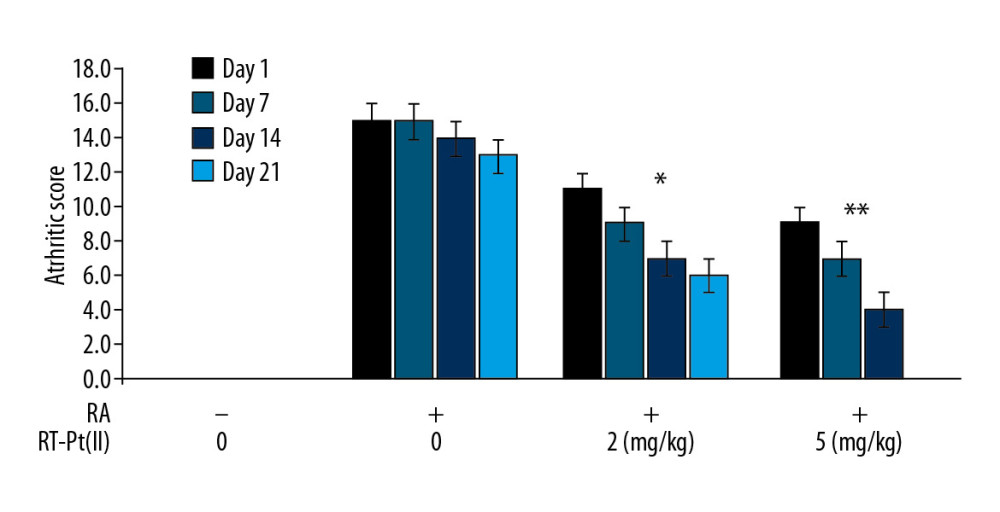 Figure 6. Effect of RT-Pt(II) on arthritic score. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were macroscopically assessed for arthritic score on days 0, 7, 14 and 21 of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 6. Effect of RT-Pt(II) on arthritic score. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were macroscopically assessed for arthritic score on days 0, 7, 14 and 21 of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats. 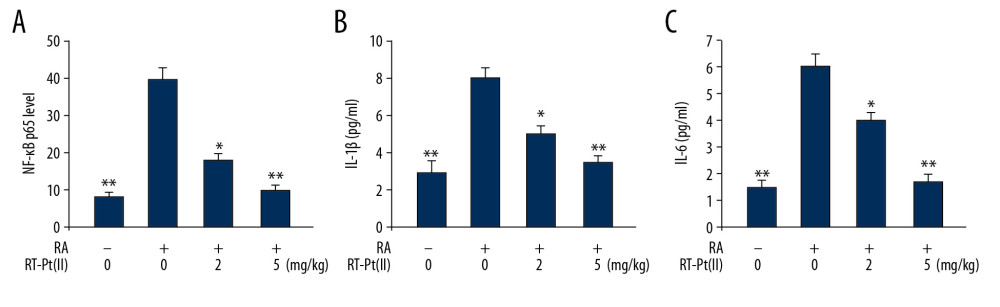 Figure 7. Effect of RT-Pt(II) on NF-κB p65 level, interleukins-1β/-6 and MMP-1/-13 activities. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for (A) NF-κB p65 level and activities of (B) IL-1β and (C) IL-6 on day 21 of the treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 7. Effect of RT-Pt(II) on NF-κB p65 level, interleukins-1β/-6 and MMP-1/-13 activities. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for (A) NF-κB p65 level and activities of (B) IL-1β and (C) IL-6 on day 21 of the treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats. 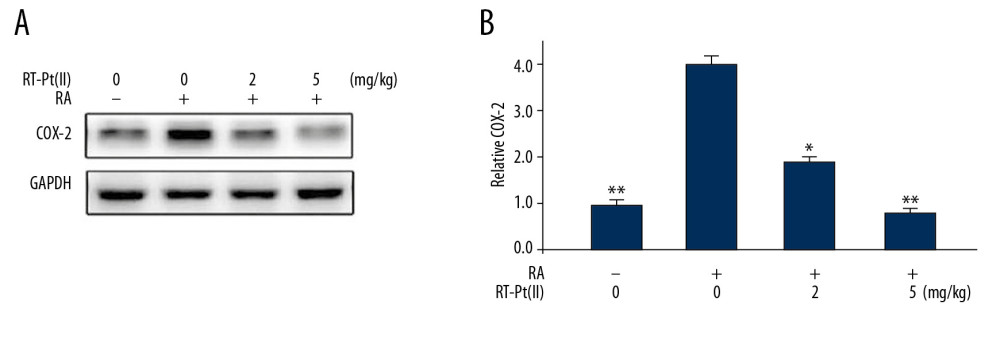 Figure 8. Effect of RT-Pt(II) on COX-2 level in RA rats. (A) The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for COX-2 level on day 21 of the treatment. (B) Semi-quantified data. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 8. Effect of RT-Pt(II) on COX-2 level in RA rats. (A) The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for COX-2 level on day 21 of the treatment. (B) Semi-quantified data. * P<0.02 and ** P<0.01 vs. untreated RA rats. References
1. Smolen JS, Aletaha D, McInnes IB, Rheumatoid arthritis: Lancet, 2016; 388; 2023-38
2. Challal S, Minichiello E, Boissier MC, Semerano L, Cachexia and adiposity in rheumatoid arthritis. Relevance for disease management and clinical outcomes: Joint Bone Spine, 2016; 83; 127-33
3. Ji L, Geng Y, Zhou W, Zhang Z, A study on relationship among apoptosis rates, number of peripheral T cell subtypes and disease activity in rheumatoid arthritis: Int J Rheum Dis, 2016; 19; 167-71
4. Symmons DP, Epidemiology of rheumatoid arthritis: Determinants of onset, persistence and outcome: Best Pract Res Clin Rheumatol, 2002; 16; 707-22
5. Sun J, Yan P, Chen Y, MicroRNA-26b inhibits cell proliferation and cytokine secretion in human RASF cells via the Wnt/GSK-3β/β-catenin pathway: Diagn Pathol, 2015; 10; 72
6. Van Der Geest KS, Smigielska-Czepiel K, Park JA, SF Treg cells transcribing high levels of Bcl-2 and microRNA-21 demonstrate limited apoptosis in RA: Rheumatology (Oxford), 2015; 54; 950-58
7. Xu WD, Zhang M, Zhang YJ, Ye DQ, IL-33 in rheumatoid arthritis: Potential role in pathogenesis and therapy: Hum Immunol, 2013; 74; 1057-60
8. Wang K, Zhao L, Liu X, Differential co-expression analysis of rheumatoid arthritis with microarray data: Mol Med Rep, 2014; 10; 2421-26
9. Song YJ, Li G, He JH, Bioinformatics-based identification of microRNA-regulated and rheumatoid arthritis-associated genes: PLoS One, 2015; 10; e0137551
10. Huber LC, Distler O, Tarner I, Synovial fibroblasts: Key players in rheumatoid arthritis: Rheumatology (Oxford), 2006; 45; 669-75
11. Lowin T, Straub RH, Synovial fibroblasts integrate inflammatory and neuroendocrine stimuli to drive rheumatoid arthritis: Expert Rev Clin Immunol, 2015; 11; 1069-71
12. McInnes IB, Schett G, Pathogenetic insights from the treatment of rheumatoid arthritis: Lancet, 2017; 389; 2328-37
13. Edhayan G, Ohara RA, Stinson WA, Inflammatory properties of inhibitor of DNA binding 1 secreted by synovial fibroblasts in rheumatoid arthritis: Arthritis Res Ther, 2016; 18; 87
14. Liu H, Pope RM, The role of apoptosis in rheumatoid arthritis: Curr Opin Pharmacol, 2003; 3; 317-22
15. Radhakrishnan A, Tudawe D, Chakravarthi S, Effect of γ-tocotrienol in counteracting oxidative stress and joint damage in collagen-induced arthritis in rats: Exp Ther Med, 2014; 7; 1408-14
16. Shahmohamadnejad S, Vaisi-Raygani A, Shakiba Y, Association between butyrylcholinesterase activity and phenotypes, paraoxonase192 rs662 gene polymorphism and their enzymatic activity with severity of rheumatoid arthritis: Correlation with systemic inflammatory markers and oxidative stress, preliminary report: Clin Biochem, 2015; 48; 63-69
17. Lu QY, Han QH, Li X, Analysis of differentially expressed genes between rheumatoid arthritis and osteoarthritis based on the gene co-expression network: Mol Med Rep, 2014; 10; 119-24
18. Mederle K, Meurer M, Castrop H, Hocherl K, Inhibition of COX-1 attenuates the formation of thromboxane A2 and ameliorates the acute decrease in glomerular filtration rate in endotoxemic mice: Am J Physiol Renal Physiol, 2015; 309; F332-40
19. Choi YJ, Lee WS, Lee EG, Sulforaphane inhibits IL-1β-induced proliferation of rheumatoid arthritis synovial fibroblasts and the production of MMPs, COX-2, and PGE2: Inflammation, 2014; 37; 1496-503
20. Luo L, Hu L, He LEffect of moxibustion on ultrastructure of synovial cells in rheumatoid arthritis rats: Zhen Ci Yan Jiu, 2011; 36; 105-9 [in Chinese]
21. Pope RM, Apoptosis as a therapeutic tool in rheumatoid arthritis: Nat Rev Immunol, 2002; 2; 527-35
22. Huang H, Xiao Y, Lin H, Increased phosphorylation of ezrin/radixin/moesin proteins contributes to proliferation of rheumatoid fibroblast-like synoviocytes: Rheumatology (Oxford), 2011; 50; 1045-53
23. Zheng G, Wang L, Jia X, Application of high frequency color Doppler ultrasound in the monitoring of rheumatoid arthritis treatment: Exp Ther Med, 2014; 8; 1807-12
24. Almoallim HM, Alharbi LA, Rheumatoid arthritis in Saudi Arabia: Saudi Med J, 2014; 35; 1442-54
25. Mark M, Ghyselinck NB, Chambon P, Retinoic acid signalling in the development of branchial arches: Curr Opin Genet Dev, 2004; 14; 591-98
26. Pino-Lagos K, Benson MJ, Noelle RJ, Retinoic acid in the immune system: Ann NY Acad Sci, 2008; 1143; 170-87
27. Peck GL, Olsen TG, Yoder FW, Prolonged remissions of cystic and conglobate acne with 13-cis-retinoic acid: N Engl J Med, 1979; 300; 329-33
28. Ward A, Brogden RN, Heel RC, Etretinate. A review of its pharmacological properties and therapeutic efficacy in psoriasis and other skin disorders: Drugs, 1983; 26; 9-43
29. Kwok S-K, Park M-K, Cho M-L, Retinoic acid attenuates rheumatoid inflammation in mice: J Immunol, 2012; 189(2); 1062-71
30. Huang ME, Ye YC, Chen SR, Use of all-trans retinoic acid in the treatment of acute promyelocytic leukemia: Blood, 1988; 72; 567-72
31. Brinckerhoff CE, Coffey JW, Sullivan AC, Inflammation and collagenase production in rats with adjuvant arthritis reduced with 13-cisretinoic acid: Science, 1983; 221; 756-58
32. Kuwabara K, Shudo K, Hori Y, Novel synthetic retinoic acid inhibits rat collagen arthritis and differentially affects serum immunoglobulin subclass levels: FEBS Lett, 1996; 378; 153-56
33. Beehler BC, Hei YJ, Chen S, Inhibition of disease progression by a novel retinoid antagonist in animal models of arthritis: J Rheumatol, 2003; 30; 355-63
34. Nozaki Y, Yamagata T, Sugiyama M, Anti-inflammatory effect of all-trans-retinoic acid in inflammatory arthritis: Clin Immunol, 2006; 119; 272-79
35. Gerlag DM, Tak PP, Novel approaches for the treatment of rheumatoid arthritis: Lessons from the evaluation of synovial biomarkers in clinical trials: Best Pract Res Clin Rheumatol, 2008; 22; 311-23
36. Szekanecz Z, Koch AE, Angiogenesis and its targeting in rheumatoid arthritis: Vascul Pharmacol, 2009; 51; 1-7
37. Zheng YQ, Wei W, Zhu L, Liu JX, Effects and mechanisms of Paeoniflorin, a bioactive glucoside from peony root, on adjuvant arthritis in rats: Inflamm Res, 2007; 56; 182-88
38. Sultana F, Rasool M, A novel therapeutic approach targeting rheumatoid arthritis by combined administration of morin, a dietary flavanol and non-steroidal anti-inflammatory drug indomethacin with reference to pro-inflammatory cytokines, inflammatory enzymes, RANKL and transcription factors: Chem Biol Interact, 2015; 230; 58-70
39. Orita K, Hiramoto K, Kobayashi H, Inducible nitric oxide synthase (iNOS) and α-melanocyte-stimulating hormones of iNOS origin play important roles in the allergic reactions of atopic dermatitis in mice: Exp Dermatol, 2011; 20; 911-14
40. Yao RB, Zhao ZM, Zhao LJ, Cai H, Sinomenine inhibits the inflammatory responses of human fibroblast-like synoviocytes via the TLR4/MyD88/NF-κB signaling pathway in rheumatoid arthritis: Pharmazie, 2017; 72; 355-60
41. Lipsky PE, van der Heijde DM, St Clair EW, Antitumor necrosis factor trial in rheumatoid arthritis with Concomitant Therapy Study Group. Infliximab and methotrexate in the treatment of rheumatoid arthritis: N Engl J Med, 2000; 343; 1594-602
42. Klareskog L, van der Heijde D, de Jager JPTEMPO (Trial of Etanercept and Methotrexate with Radiographic Patient Outcomes) study investigators, Therapeutic effect of the combination of etanercept and methotrexate compared with each treatment alone in patients with rheumatoid arthritis: double-blind randomised controlled trial: Lancet, 2004; 363; 675-81
43. Breedveld FC, Weisman MH, Kavanaugh AF, The PREMIER study: A multicenter, randomized, double-blind clinical trial of combination therapy with adalimumab plus methotrexate versus methotrexate alone or adalimumab alone in patients with early, aggressive rheumatoid arthritis who had not had previous methotrexate treatment: Arthritis Rheum, 2006; 54; 26-37
44. Singh JA, Beg S, Lopez-Olivo MA, Tocilizumab for rheumatoid arthritis: Cochrane Database Syst Rev, 2010(7); CD008331
45. Vo VA, Lee JW, Chang JE, Avicularin inhibits lipopolysaccharide-induced inflammatory response by suppressing ERK phosphorylation in RAW 264.7 macrophages: Biomol Ther (Seoul), 2012; 20; 532-37
Figures
 Figure 1. Effect of RT-Pt(II) on proliferation up-regulation by TNF-α in vitro. The RT-Pt(II) exposed cells at 0.25 to 12 μM concentration for 48 h were treated with TNF-α. The changes in proliferative abilities were measured at 72 h of exposure to RT-Pt(II) by MTT assay. * P<0.05, ** P<0.02 and ** P<0.01 vs. TNF-α stimulated cells.
Figure 1. Effect of RT-Pt(II) on proliferation up-regulation by TNF-α in vitro. The RT-Pt(II) exposed cells at 0.25 to 12 μM concentration for 48 h were treated with TNF-α. The changes in proliferative abilities were measured at 72 h of exposure to RT-Pt(II) by MTT assay. * P<0.05, ** P<0.02 and ** P<0.01 vs. TNF-α stimulated cells. Figure 2. Effect of RT-Pt(II) on MH7A cell apoptosis. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations were treated with TNF-α at 48 h. (A) The cellular apoptosis at 72 h of RT-Pt(II) treatment was analyzed by flow cytometry. (B) The protein expression at 72 h of RT-Pt(II) treatment was assessed by western blotting.
Figure 2. Effect of RT-Pt(II) on MH7A cell apoptosis. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations were treated with TNF-α at 48 h. (A) The cellular apoptosis at 72 h of RT-Pt(II) treatment was analyzed by flow cytometry. (B) The protein expression at 72 h of RT-Pt(II) treatment was assessed by western blotting. Figure 3. (A–E) Effect RT-Pt(II) on matrix metalloproteinase-1/-13 and interleukins-1β/-6/-8 levels. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations for 48 h were treated with TNF-α. The level of proteins was detected using ELISA assays at 72 h of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. TNF-α treated control
Figure 3. (A–E) Effect RT-Pt(II) on matrix metalloproteinase-1/-13 and interleukins-1β/-6/-8 levels. The RT-Pt(II) exposed cells at 4 and 12 μM concentrations for 48 h were treated with TNF-α. The level of proteins was detected using ELISA assays at 72 h of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. TNF-α treated control Figure 4. Effect of RT-Pt(II) on iNOS/COX-2 in TNF-α exposed cells. The RT-Pt(II) treated cells at 4 and 12 μM concentrations for 48 h were exposed to TNF-α. (A) The protein levels were measured at 72 h of RT-Pt(II) treatment by western blotting. (B) In RT-Pt(II) treated cells mRNA levels were analyzed at 72 h using RT-PCR. * P<0.02 and ** P<0.01 vs. TNF-α treated cells.
Figure 4. Effect of RT-Pt(II) on iNOS/COX-2 in TNF-α exposed cells. The RT-Pt(II) treated cells at 4 and 12 μM concentrations for 48 h were exposed to TNF-α. (A) The protein levels were measured at 72 h of RT-Pt(II) treatment by western blotting. (B) In RT-Pt(II) treated cells mRNA levels were analyzed at 72 h using RT-PCR. * P<0.02 and ** P<0.01 vs. TNF-α treated cells. Figure 5. Effect of RT-Pt(II) on MEK/NF-κB phosphorylation. The RT-Pt(II) exposed cells at 4 to 12 μM were treated with TNF-α at 48 h of exposure. (A) The measurement of phosphorylation for MEK/NF-κB (p-665) was performed by western blotting at 72 h of RT-Pt(II) treatment. (B) Semi-quantification of the data * P<0.02 and ** P<0.01 vs. TNF-α treated cells.
Figure 5. Effect of RT-Pt(II) on MEK/NF-κB phosphorylation. The RT-Pt(II) exposed cells at 4 to 12 μM were treated with TNF-α at 48 h of exposure. (A) The measurement of phosphorylation for MEK/NF-κB (p-665) was performed by western blotting at 72 h of RT-Pt(II) treatment. (B) Semi-quantification of the data * P<0.02 and ** P<0.01 vs. TNF-α treated cells. Figure 6. Effect of RT-Pt(II) on arthritic score. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were macroscopically assessed for arthritic score on days 0, 7, 14 and 21 of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 6. Effect of RT-Pt(II) on arthritic score. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were macroscopically assessed for arthritic score on days 0, 7, 14 and 21 of RT-Pt(II) treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats. Figure 7. Effect of RT-Pt(II) on NF-κB p65 level, interleukins-1β/-6 and MMP-1/-13 activities. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for (A) NF-κB p65 level and activities of (B) IL-1β and (C) IL-6 on day 21 of the treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 7. Effect of RT-Pt(II) on NF-κB p65 level, interleukins-1β/-6 and MMP-1/-13 activities. The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for (A) NF-κB p65 level and activities of (B) IL-1β and (C) IL-6 on day 21 of the treatment. * P<0.02 and ** P<0.01 vs. untreated RA rats. Figure 8. Effect of RT-Pt(II) on COX-2 level in RA rats. (A) The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for COX-2 level on day 21 of the treatment. (B) Semi-quantified data. * P<0.02 and ** P<0.01 vs. untreated RA rats.
Figure 8. Effect of RT-Pt(II) on COX-2 level in RA rats. (A) The RA rats untreated or treated with RT-Pt(II) at 2 mg/kg and 5 mg/kg doses were assessed for COX-2 level on day 21 of the treatment. (B) Semi-quantified data. * P<0.02 and ** P<0.01 vs. untreated RA rats. In Press
11 Mar 2024 : Clinical Research
Enhancement of Frozen-Thawed Human Sperm Quality with Zinc as a Cryoprotective AdditiveMed Sci Monit In Press; DOI: 10.12659/MSM.942946
12 Mar 2024 : Database Analysis
Risk Factors of Age-Related Macular Degeneration in a Population-Based Study: Results from SHIP-TREND-1 (St...Med Sci Monit In Press; DOI: 10.12659/MSM.943140
12 Mar 2024 : Clinical Research
Preoperative Blood Transfusion Requirements for Hemorrhoidal Severe Anemia: A Retrospective Study of 128 Pa...Med Sci Monit In Press; DOI: 10.12659/MSM.943126
12 Mar 2024 : Clinical Research
Tissue Inhibitors of Metalloproteinase 1 (TIMP-1) and 3 (TIMP-3) as New Markers of Acute Kidney Injury Afte...Med Sci Monit In Press; DOI: 10.12659/MSM.943500
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








