23 September 2020: Clinical Research
Evaluation of Factors Associated with Anxiety and Depression in Chinese Visiting Scholars in the United States During the COVID-19 Pandemic Assessed by Online Questionnaires
Yanjie Zhao12ABE*, Ping Wang3ADE, Jiangping Wu1BD, Ruibin Wang4DF, Qingkun Song5ACFGDOI: 10.12659/MSM.926602
Med Sci Monit 2020; 26:e926602
Abstract
BACKGROUND: This study aimed to use online questionnaires to evaluate the factors associated with anxiety and depression in Chinese visiting scholars in the United States during the COVID-19 pandemic.
MATERIAL AND METHODS: Using a cross-sectional design, 311 Chinese scholars visiting 41 states in the United States were interviewed on 20 and 21 April 2020 through WeChat using the Patient Health Questionnaire-9 (PHQ-9) and the Generalized Anxiety Disorder-7 (GAD-7) questionnaire.
RESULTS: Of these 311 visiting scholars, 69 (22.2%) reported no symptoms of anxiety or depression, whereas 63 (20.3%) reported severe anxiety and 67 (21.5%) reported severe depression. Risk of anxiety was 93% higher in visiting scholars with than without accompanying parents in the US (odds ratio [OR], 1.93; 95% confidence interval [CI], 1.01–3.68) and was 1.72-fold (95% CI, 1.04–2.84) higher in those experiencing stress about family members with COVID-19. Stresses about personal security and return to China on schedule were associated with 1.73-fold (95% CI, 1.03–2.92) and 3.00-fold (95% CI, 1.51–5.95) higher risks of anxiety, respectively. Risks of depression were 1.86-fold (95% CI, 1.14–3.05), 1.84-fold (95% CI, 1.10–3.07), and 3.45-fold (95% CI, 1.72–6.92) higher in visiting Chinese scholars who were than were not experiencing stresses about financial support, personal security and return to China on schedule, respectively.
CONCLUSIONS: Chinese scholars visiting the United States during the COVID-19 pandemic experienced severe psychological distress. Surveys that include larger numbers of visiting scholars are warranted.
Keywords: Anxiety, COVID-19, Depression, Betacoronavirus, COVID-19, Coronavirus Infections, Cross-Sectional Studies, International Educational Exchange, Marriage, Pandemics, Parents, Pneumonia, Viral, Psychological Tests, Risk, SARS-CoV-2, Stress, Psychological, Surveys and Questionnaires, United States, young adult
Background
Since December 2019, the outbreak of COVID-19 has infected more than 6.7 million people in 188 countries/regions worldwide, including more than 1.9 million in the United States (US). To date, more than 393 000 people worldwide have died of this disease. The World Health Organization (WHO) announced a pandemic outbreak of COVID-19 on 11 March 2020 [1].
Infectious disease pandemics are frequently associated with mental health problems. For example, the mental health of medical staff and vulnerable populations was affected during the SARS epidemic [2]. The COVID-19 pandemic has increased consultations with psychiatry professionals and has prompted evaluations of mental health among the general population, healthcare workers and vulnerable populations [3]. Psychological assistance services, including internet-, telephone-, and application-based counseling or intervention, have been widely used in response to the COVID-19 outbreak in China [4]. On 2 February 2020, the State Council of China announced the commencement of nationwide psychological assistance hotlines [5].
Economic burden, family support, social support, and social capital have all been reported to affect mental health status [6]. Social isolation, including social exclusion and low social capital, also leads to psychological problems [7,8]. People with greater informal social support were found to be more likely to recover from symptoms of psychosis [9]. Many studies have focused on the mental health of medical staff, the general population, and self-isolated individuals [10–14]. Chinese scholars visiting the United States to conduct research have experienced social isolation, lack of family support, and stresses from the COVID-19 pandemic. To our knowledge, this is the first study to assess the mental health of Chinese scholars visiting the US during the COVID-19 pandemic.
WeChat in China is similar to Twitter in the US and is often used as a tool for medical research [15]. At present, more than one billion individuals in China utilize WeChat on their smartphones [15]. Questionnaires were administered to Chinese scholars visiting the US via WeChat on their smartphones. The symptoms of depression were assessed using the Chinese versions of the Patient Health Questionnaire-9 (PHQ-9), a valid and reliable tool to screen for depression [16], whereas the symptoms of anxiety were assessed using the Generalized Anxiety Disorder-7 (GAD-7) questionnaire, an effective and reliable tool to screen for anxiety [17]. Both the PHQ-0 and the GAD-7 are widely used in psychology research in China.
Material and Methods
ETHICAL APPROVAL:
This study was approved by the Ethics Committee of Beijing Shijitan Hospital, Capital Medical University (SJTKY11-JY-2020(1). All subjects provided informed consent electronically prior to taking the survey. The informed consent page presented 2 options (yes/no). The subjects selecting yes were eligible to respond to the questionnaire and could quit the process at any time.
STUDY DESIGN:
This was a cross-sectional study involving 311 visiting scholars across the US who were screened on the Internet for anxiety and depression on 20 and 21 April 2020. Independent variables included demographic factors, family members staying in the US with the visiting scholars, and sources of stress.
SUBJECTS:
To be eligible, visiting scholars had to have permanent jobs in China, receive funding support for their research visit to the US, and stay in the US during the COVID-19 pandemic. Chinese undergraduate and postgraduate students who were studying in the US and visiting scholars who had returned to China at the time of the interview were excluded from the survey. The subjects were aged from 18 to 60 years and received the questionnaire in April 2020. Participants were surveyed through WeChat by snowball sampling or chain-referral sampling, with the study participants recruiting other participants whom they knew were visiting from China. The internet-based anonymous and self-rated questionnaires were designed by Wenjuan Application (
DEFINITIONS OF ANXIETY AND DEPRESSION:
The symptoms of depression and anxiety were evaluated using the Chinese versions of the validated PHQ-9 (range, 0–27) [16] and GAD-7 (range, 0–21) [17], respectively. Scores of 0–4 on the PHQ-9 were defined as normal, whereas scores of 5–9, 10–14, and 15–27 were defined as indicating mild, moderate, and severe depression, respectively [16]. Scores of 0–4 on the GAD-7 were defined as normal, whereas scores of 5–9, 10–14, and 15–21 were defined as indicating mild, moderate, and severe anxiety, respectively [17].
COVARIATES:
The demographic data included age, sex, marital status (married, unmarried and others), professional title (junior, moderate, sub-senior and senior levels), level of education (bachelor’s, master’s and doctoral degrees) and field of study (science, engineering, medicine and arts). Other factors recorded included the time since arrival in the US for the current research visit (<3, <6, <9, <12 and ≥12 months), the time to the end of the research visit (<3, <6, <9, <12 and ≥12 months), and the states in the US being visited. The family members (parents, children, and spouse) visiting the US with these scholars and their sources of stress (shortage of resources, fiancé or fiancée remaining in China, family members infected by COVID-19, security in the US, returning to China on time, and interruption of the research visit) were also recorded.
STATISTICAL ANALYSIS:
All statistical analyses were performed using IBM SPSS Statistics software 23.0 (IBM SPSS Software). Correlations of anxiety and depression scores with age groups, time since arrival in the US, time to the end of the research visit, and professional and educational levels were analyzed by Spearman correlation tests. Differences in anxiety and depression scores among fields of study were analyzed by Kruskal-Wallis tests, and differences in anxiety and depression scores between sexes, between those who were and were not accompanied by family members, and among sources of stress were analyzed by Mann-Whitney U tests. Factors with p-values <0.05 on univariate analysis were included in the multivariate analysis, under ordinal logistic regression with the dependent variables being no, mild, moderate, and severe anxiety and depression. All tests were two-sided, with significance defined as a p-value <0.05.
Results
PARTICIPANTS:
A total of 311 scholars visiting 41 states participated in the survey (Figure 1). The 9 states without a responding visiting scholar were Alabama, Alaska, Arizona, Idaho, Maine, New Hampshire, North Dakota, Vermont, and Wyoming. More than 95% of the visiting scholars were aged under 50 years. Ninety-nine (31.8%) visiting scholars were women and 212 (68.2%) were men; of these, 259 (83.3%) were married and 46 (14.8%) were unmarried. Of these visiting scholars, 227 (73.0%) had been in the US longer than 6 months and 219 (70.5%) were due to return to China in less than 6 months. Of the 311 visiting scholars, 94 (30.2%), 61 (19.6%), 63 (20.3%), and 93 (29.9%) were studying science, engineering, medicine, and the arts, respectively. In addition, 190 (61.1%) responders had at least a sub-senior position professionally, and 216 (69.5%) had obtained a doctoral degree.
DISTRIBUTION OF ANXIETY AND DEPRESSION AND THEIR RELATIONSHIP WITH BASELINE CHARACTERISTICS:
The median anxiety score was 7.0, with 25th percentile and 75th percentiles of 4.0 and 14.0, respectively (Figure 2A). Of the 311 visiting scholars, 85 (27.3%), 107 (34.4%), 56 (18.0%), and 63 (20.3%) reported no, mild, moderate, and severe anxiety, respectively (Figure 2B). The median depression score was 7.0, with 25th percentile and 75th percentiles of 3.0 and 13.0, respectively (Figure 3A). In addition, 104 (33.4%), 87 (28.0%), 53 (17.0%), and 67 (21.5%) of these scholars had no, mild, moderate, and severe depression, respectively (Figure 3B). Analysis showed that 191 (61.5%) participants had both anxiety and depression, 35 (11.2%) had anxiety alone, 16 (5.1%) had depression alone, and 69 (22.2%) had neither anxiety nor depression.
Median anxiety score was significantly lower in visiting scholars aged ≤30 years than those aged >30 years (5.50 vs. 7.0) and was significantly lower in unmarried than in married participants (6.00 vs. 7.00, p=0.04) (Table 1). The time to the end of the research visit was negatively correlated with anxiety score, with median anxiety score being significantly higher in scholars with <3 months than in those with ≥3 months to the end of their research visit (9.00 vs. 7.00, p=0.002). Senior professionals had a median anxiety score of 8.00, with professional title levels being positively correlated with anxiety score (p=0.013). Anxiety score was unrelated to sex, length of stay in the US, field of study, or educational level.
The time to the end of the research visit was also negatively correlated with depression score, with median depression score being significantly higher in scholars with <3 months than in those with ≥3 months to the end of their research visit (9.00
CORRELATION BETWEEN FACTORS AND ANXIETY AND DEPRESSION SCORES:
Visiting scholars staying in the US with family members had similar anxiety and depression scores as those staying in the US without family members (Table 1). Participants visiting with parents in the US had a significantly higher median anxiety score than those visiting without parents (p=0.007, Table 2). Moreover, scholars visiting the US with children were more likely to have higher anxiety scores than those visiting without children (p=0.041). Visiting scholars experiencing stress in the US had significantly higher anxiety (7.00 vs. 2.00) and depression (8.00 vs. 2.00) scores than those without stress (p<0.001 each). Participants with stresses such as shortage of resources, financial difficulties, security, infection with COVID-19, and returning to China on schedule had higher anxiety and depression scores than those without these stresses (p<0.05 each). However, stress associated with possible interruption of the research visit was not associated with anxiety or depression score (p>0.05).
Staying in the US with parents was associated with a 1.93-fold higher risk of anxiety (p=0.047, Table 3). Stresses associated with COVID-19 infection, security in the US, and returning to China on schedule were associated with 1.72-fold, 1.73-fold, and 3.00-fold higher risks of anxiety, respectively (p<0.05 each). Stresses associated with financial difficulties, security in the US, and returning to China on schedule were associated with 86%, 84%, and 245% higher risks of depression, respectively (p<0.05 each).
Discussion
To our knowledge, this is the first mental health survey of international visiting scholars during the COVID-19 pandemic and the first to assess factors associated with increased anxiety and depression. COVID-19, the most infectious disease since the Spanish flu, has been described as a once-in-a-century pathogen. Mass disasters, such as earthquakes, floods, tsunamis, hurricanes, and infectious diseases, have been reported to influence mental disorders [18]. International visiting scholars are regarded as more vulnerable and face more challenges than the general population.
International visiting scholars were found to have more serious mental health problems than the medical staff in Wuhan, China, during the COVID-19 pandemic between January and February 2020 [4,10]. This survey found that 20.3% and 21.5% of visiting scholars had symptoms of severe anxiety and severe depression, respectively, compared with 6.0% and 7.3%, respectively, of the medical staff in Wuhan [4]. Moreover, 27.3% of participants in this survey had no symptoms of anxiety and 33.4% had no symptoms of depression, compared with 51.4% and 40.0%, respectively of the medical staff in Wuhan [4]. Staff members in Wuhan reported excessive tension, fatigue, hyperactivity, frustration, and self-blame over patients’ deaths and worried about themselves and their families being infected. However, they worked on a regular rotation and received professional crisis intervention from psychological teams, who guided them in self-regulation. Also, these staff members received support from their colleagues, relatives and friends; their contributions were affirmed and their safety was guaranteed [19]. In contrast, the safety of these visiting scholars was not guaranteed and they were socially isolated, with many lacking family and social support [20]. Visiting scholars in the US were easily neglected during the pandemic and could not easily access professional psychological help, resulting in serious psychological distress.
Visiting scholars over 30 years old and those who were married had higher anxiety scores than those who were younger or unmarried. In contrast, a previous study found that the mental health stability rate was lower in subjects aged 18–29 years (39.8%) than in those aged 30–84 years (57.2%) [21]. That study found that for young people, occupational status, especially being employed, was of major importance in the development of stable mental health [21]. All respondents in our study had stable jobs, which may have been responsible for the more stable mental health of participants aged <30 years.
Being accompanied by parents was associated with a 1.93-fold risk of anxiety. A study in Singapore showed that 52.6% of the caregivers of the elderly (≥60 years) had psychological distress [22] and experienced multiple negative physical, emotional, social, and financial stressors due to the increased demands in care-giving [23,24]. In addition to the above pressures, visiting scholars also worried about their parents becoming infected with COVID-19, because the elderly have had the highest mortality rate from COVID-19 infection [25]. Alternatively, they might be more dependent on their parents, with impeded or depressed creative consciousness, with these individuals having not completed the process of separation-individualization [26]. This may have made it more difficult for these individuals to tolerate loneliness and to increase symptoms of anxiety when experiencing danger, threat, or uncertainty [26].
Uncertainty was the main reason for anxiety [27,28]. International flights, including to China, were canceled widely, and Chinese visiting scholars did not have the opportunity to return to China. They were uncertain about their security and personal safety in the US. Thus, people closer to their scheduled return time were more anxious than those who expected to stay longer in the US. Similar to the general population [12,29], the stress of being infected with COVID-19 was also a main reason for anxiety, and financial distress was a main reason for depression. Financial hardship is strongly associated with depression [30,31], and financial stress was found to be the strongest direct predictor of symptoms of depression [32].
The rates of anxiety and depression among Chinese visiting scholars in the US was high, even higher than that of frontline medical staff in Wuhan, China, during the COVID-19 outbreak, who were ranked as the being at the highest need of psychological intervention. Vulnerable and easily overlooked groups need urgent psychological crisis intervention to avoid extreme events, such as suicide, self-injury, impulsive behavior, and group psychological crisis events [19]. On 27 April 2020, the Consulate-General of the People’s Republic of China in San Francisco initiated a free online consultation platform for overseas Chinese, including consultation about COVID-19 and mental health [33]. A wide range of evidence-based Internet programs are currently available for disease prevention and treatment [34]. Subjects who continue to experience anxiety and depression after 2 weeks can schedule psychiatric interviews and, if necessary, can be treated with drugs or can return to China [19]. On 9 May 2020, the Embassy of the People’s Republic of China in the US announced that international students experiencing difficulties in the US, including visiting scholars, can register to take temporary flights back to China [35].
This study had several limitations. First, selection bias may have occurred because most of the participating scholars were recruited through the snowball sampling method by WeChat, suggesting that those who completed the survey may have been more interested in mental health-related topics. A survey covering more visiting scholars should be implemented to illustrate the general situation. Second, although the recruited visiting scholars were from 41 states in the US, the numbers among states were unbalanced and some deviations may have occurred. Finally, this survey did not include insomnia severity. Anxiety levels have been reported significantly higher in individuals who did than did not report symptoms of insomnia [36].
Conclusions
Chinese scholars visiting the US during the COVID-19 pandemic experienced serious mental disorders, including anxiety and depression. To relieve their anxiety and depression, visiting scholars should be encouraged to access online psychological intervention services and psychological assistance hotlines. Surveys focusing on larger numbers of visiting scholars should be performed.
Figures
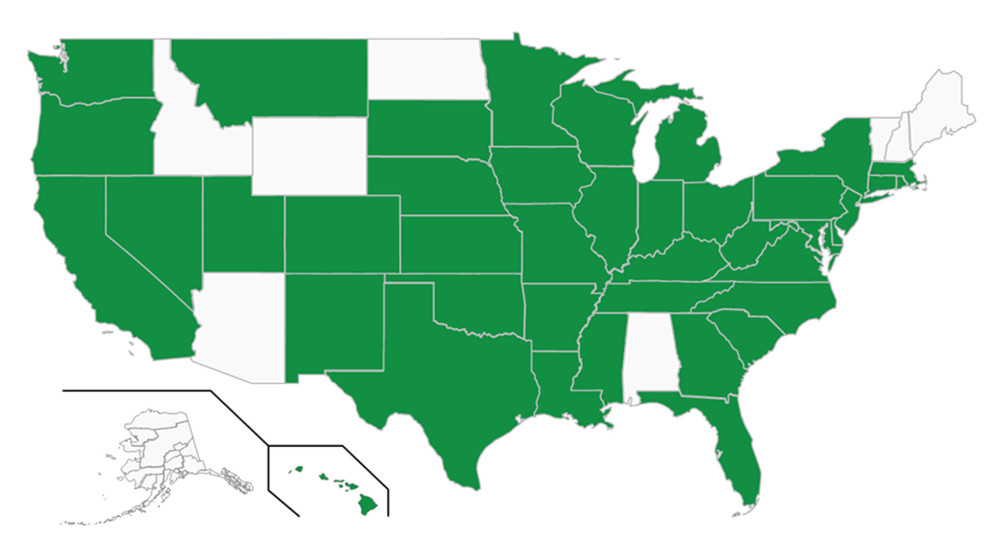 Figure 1. Map of the United States, showing the numbers of Chinese scholars visiting each state.
Figure 1. Map of the United States, showing the numbers of Chinese scholars visiting each state. 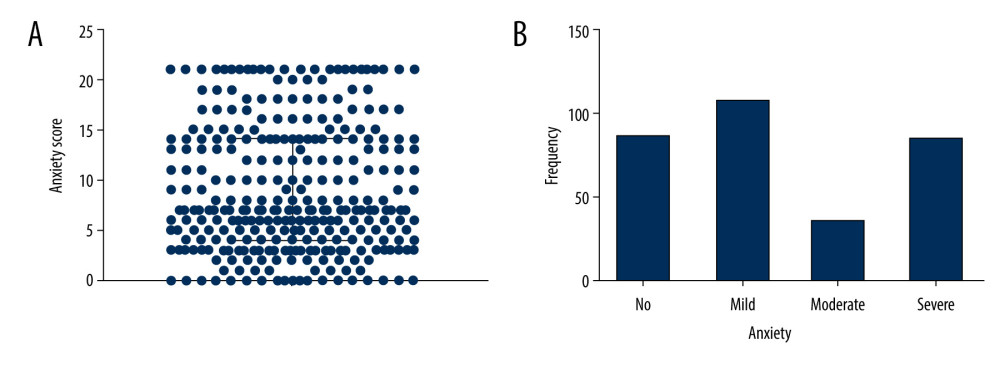 Figure 2. Status of anxiety among visiting scholars in the United States. (A) Distribution of anxiety scores, (B) frequency of anxiety levels.
Figure 2. Status of anxiety among visiting scholars in the United States. (A) Distribution of anxiety scores, (B) frequency of anxiety levels. 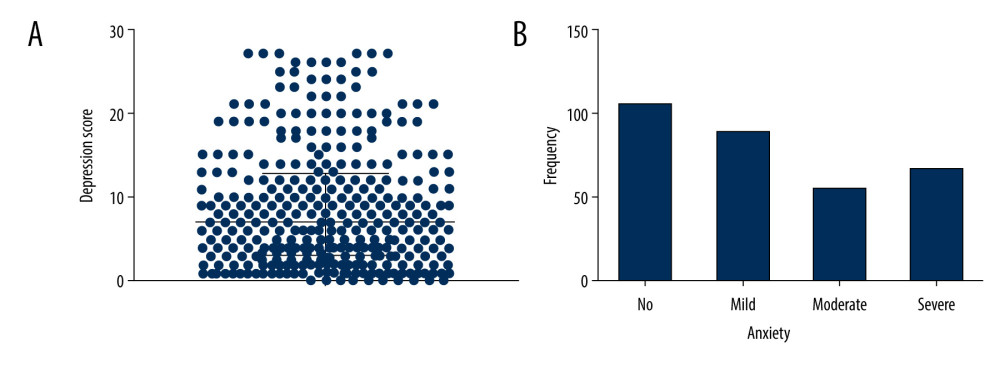 Figure 3. Status of depression among visiting scholars in the United States. (A) Distribution of depression scores, (B) frequency of depression levels.
Figure 3. Status of depression among visiting scholars in the United States. (A) Distribution of depression scores, (B) frequency of depression levels. References
1. Quinn GP, Vadaparampil ST, Malo T, Oncologists’ use of patient educational materials about cancer and fertility preservation: Psychooncology, 2012; 21(11); 1244-49
2. Wu P, Fang Y, Guan Z, The psychological impact of the SARS epidemic on hospital employees in China: Exposure, risk perception, and altruistic acceptance of risk: Can J Psychiatry, 2009; 54(5); 302-11
3. Rajkumar RP, COVID-19 and mental health: A review of the existing literature: Asian J Psychiatr, 2020; 52; 102066
4. Lai J, Ma S, Wang Y, Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019: JAMA Netw Open, 2020; 3(3); e203976
5. : The State Council of China A notification to set up nationwide psychological assistance hotlines against the 2019-nCoV outbreak Published February 2, 2020. Available at [URL]: http://www.gov.cn/xinwen/2020-02/02/content_5473937.htm
6. Cucinotta D, Vanelli M, WHO declares COVID-19 a pandemic: Acta Biomed, 2020; 91(1); 157-60
7. Wadia R, Social capital and sleep quality in those who self-isolate: Br Dent J, 2020; 228(8); 595
8. Wright N, Stickley T, Concepts of social inclusion, exclusion and mental health: A review of the international literature: J Psychiatr Ment Health Nurs, 2013; 20(1); 71-81
9. Smyth N, Siriwardhana C, Hotopf M, Hatch SL, Social networks, social support and psychiatric symptoms: Social determinants and associations within a multicultural community population: Soc Psychiatry Psychiatr Epidemiol, 2015; 50(7); 1111-20
10. Kang L, Ma S, Chen M, Impact on mental health and perceptions of psychological care among medical and nursing staff in Wuhan during the 2019 novel coronavirus disease outbreak: A cross-sectional study: Brain Behav Immun, 2020; 87; 11-17
11. Li Z, Ge J, Yang M, Vicarious traumatization in the general public, members, and non-members of medical teams aiding in COVID-19 control: Brain Behav Immun, 2020; 88; 916-19
12. Wang C, Pan R, Wan X, Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China: Int J Environ Res Public Health, 2020; 17(5); 1729
13. Xiao H, Zhang Y, Kong D, Social capital and sleep quality in individuals who self-isolated for 14 days during the coronavirus disease 2019 (COVID-19) outbreak in January 2020 in China: Med Sci Monit, 2020; 26; e923921
14. Xiao H, Zhang Y, Kong D, The effects of social support on sleep quality of medical staff treating patients with coronavirus disease 2019 (COVID-19) in January and February 2020 in China: Med Sci Monit, 2020; 26; e923549
15. Montag C, Becker B, Gan C, The multipurpose application WeChat: A review on recent research: Front Psychol, 2018; 9; 2247
16. Zhang YL, Liang W, Chen ZM, Validity and reliability of Patient Health Questionnaire-9 and Patient Health Questionnaire-2 to screen for depression among college students in China: Asia Pac Psychiatry, 2013; 5(4); 268-75
17. He XH, Li CB, Qian J, Reliability and validity of generalized anxiety scale in general hospitals: Shanghai Arch Psychiatry, 2010; 22(4); 200-3
18. Mondal R, Sarkar S, Banerjee I, Acute stress-related psychological impact in children following devastating natural disaster, the Sikkim earthquake (2011), India: J Neurosci Rural Pract, 2013; 4(Suppl 1); S19-23
19. Ma N, Ma H, Li LJ, Reading and analysis of the guiding principles of emergent psychological crisis intervention in the COVID-19: Chinese J Psychiatry, 2020; 53(2); 95-98
20. Filion N, Fenelon A, Boudreaux M, Immigration, citizenship, and the mental health of adolescents: PLoS One, 2018; 13(5); e0196859
21. Winzer R, Sorjonen K, Lindberg L, What predicts stable mental health in the 18–29 age group compared to older age groups? Results from the Stockholm Public Health Cohort 2002–2014: Int J Environ Res Public Health, 2018; 15(12); 2859
22. Sambasivam R, Liu J, Vaingankar JA, The hidden patient: Chronic physical morbidity, psychological distress, and quality of life in caregivers of older adults: Psychogeriatrics, 2019; 19(1); 65-72
23. Hudson P, Trauer T, Kelly B, Reducing the psychological distress of family caregivers of home-based palliative care patients: Short-term effects from a randomised controlled trial: Psychooncology, 2013; 22(9); 1987-93
24. Hudson P, Trauer T, Kelly B, Reducing the psychological distress of family caregivers of home-based palliative care patients: Longer term effects from a randomised controlled trial: Psychooncology, 2015; 24(1); 19-24
25. Fauci AS, Lane HC, Redfield RR, Covid-19 – navigating the uncharted: N Engl J Med, 2020; 382(13); 1268-69
26. Yalom ID: Existential psychotherapy, 2020, New York, Basic books, US
27. Ma Q, Qiu W, Fu H, Sun X, Uncertain is worse: Modulation of anxiety on pain anticipation by intensity uncertainty: Evidence from the ERP study: Neuroreport, 2018; 29(12); 1023-29
28. Putwain DW, Pescod M, Is reducing uncertain control the key to successful test anxiety intervention for secondary school students? Findings from a randomized control trial: Sch Psychol Q, 2018; 33(2); 283-92
29. Dowdall N, Ward CL, Lund C, The association between neighbourhood-level deprivation and depression: Evidence from the South African National Income Dynamics Study: BMC Psychiatry, 2017; 17(1); 395
30. Butterworth P, Rodgers B, Windsor TD, Financial hardship, socio-economic position and depression: Results from the PATH Through Life Survey: Soc Sci Med, 2009; 69(2); 229-37
31. Weaver A, Taylor RJ, Chatters LM, Himle JA, Depressive symptoms and psychological distress among rural African Americans: The role of material hardship and self-rated health: J Affect Disord, 2018; 236; 207-10
32. Schulz AJ, Israel BA, Zenk SN, Psychosocial stress and social support as mediators of relationships between income, length of residence and depressive symptoms among African American women on Detroit’s eastside: Soc Sci Med, 2006; 62(2); 510-22
33. : Overseas Chinese can consult COVID-19 through a free online medical consultation platform, the Consulate-General of the People’s Republic of China in San Francisco Available at [URL]: http://www.chinaconsulatesf.org/chn/lsbf/hqxx/t1757250.htm
34. Rogers MA, Lemmen K, Kramer R, Internet-delivered health interventions that work: Systematic review of meta-analyses and evaluation of website availability: J Med Internet Res, 2017; 19(3); e90
35. : International students experiencing difficulties in the United States, including visiting scholars, can register to take a temporary flight back to China, Embassy of People’s Republic of China in the United States of America Available at [URL]: http://www.chinaembassy.org/chn/lszj/zytz/t1777393.htm?from=groupmessage&isappinstalled=0
36. Bragantini D, Sivertsen B, Gehrman P, Differences in anxiety levels among symptoms of insomnia. The HUNT study: Sleep Health, 2019; 5(4); 370-75
Figures
 Figure 1. Map of the United States, showing the numbers of Chinese scholars visiting each state.
Figure 1. Map of the United States, showing the numbers of Chinese scholars visiting each state. Figure 2. Status of anxiety among visiting scholars in the United States. (A) Distribution of anxiety scores, (B) frequency of anxiety levels.
Figure 2. Status of anxiety among visiting scholars in the United States. (A) Distribution of anxiety scores, (B) frequency of anxiety levels. Figure 3. Status of depression among visiting scholars in the United States. (A) Distribution of depression scores, (B) frequency of depression levels.
Figure 3. Status of depression among visiting scholars in the United States. (A) Distribution of depression scores, (B) frequency of depression levels. Tables
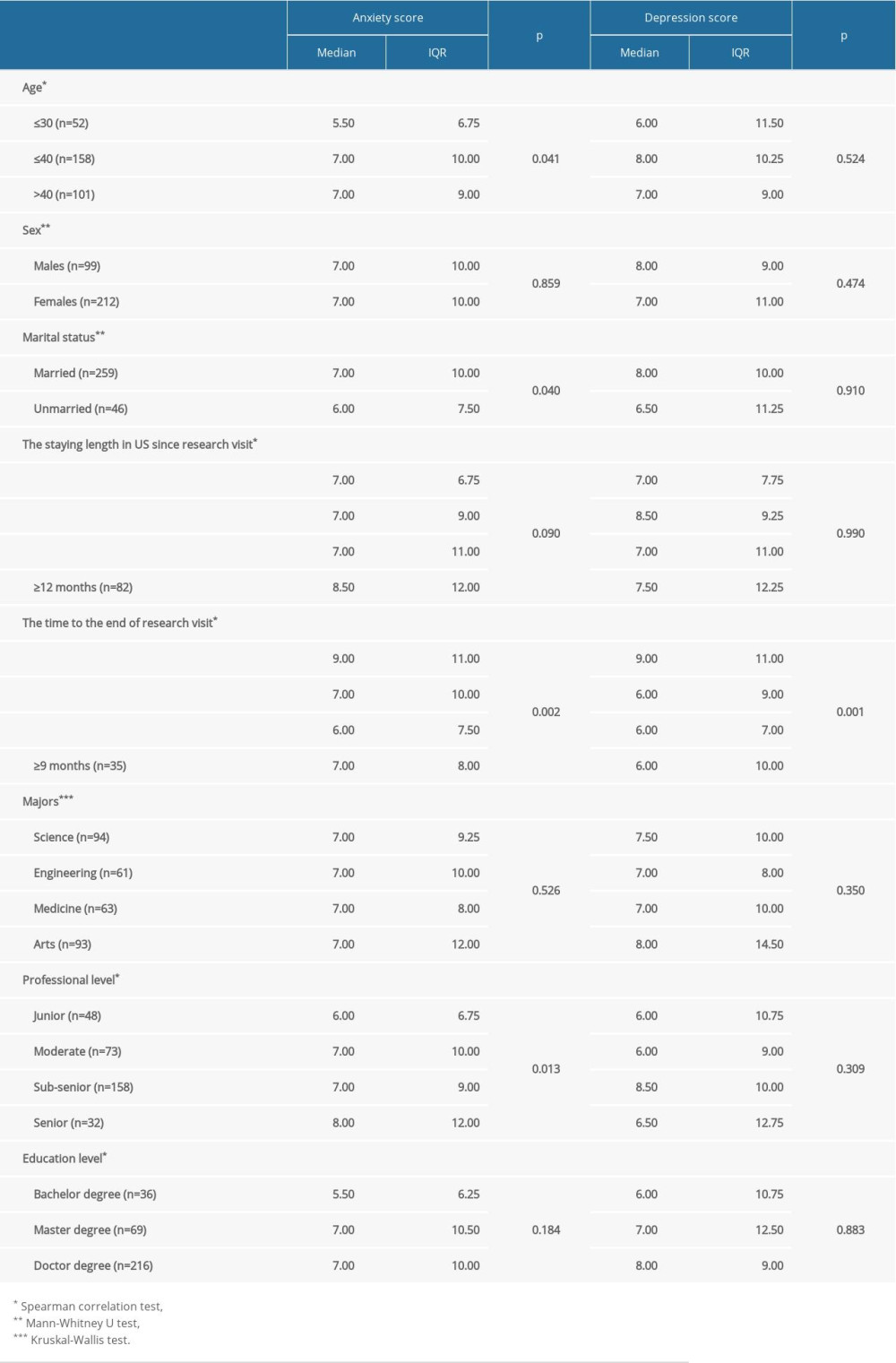 Table 1. Relationships between subject characteristics and anxiety and depression scores.
Table 1. Relationships between subject characteristics and anxiety and depression scores.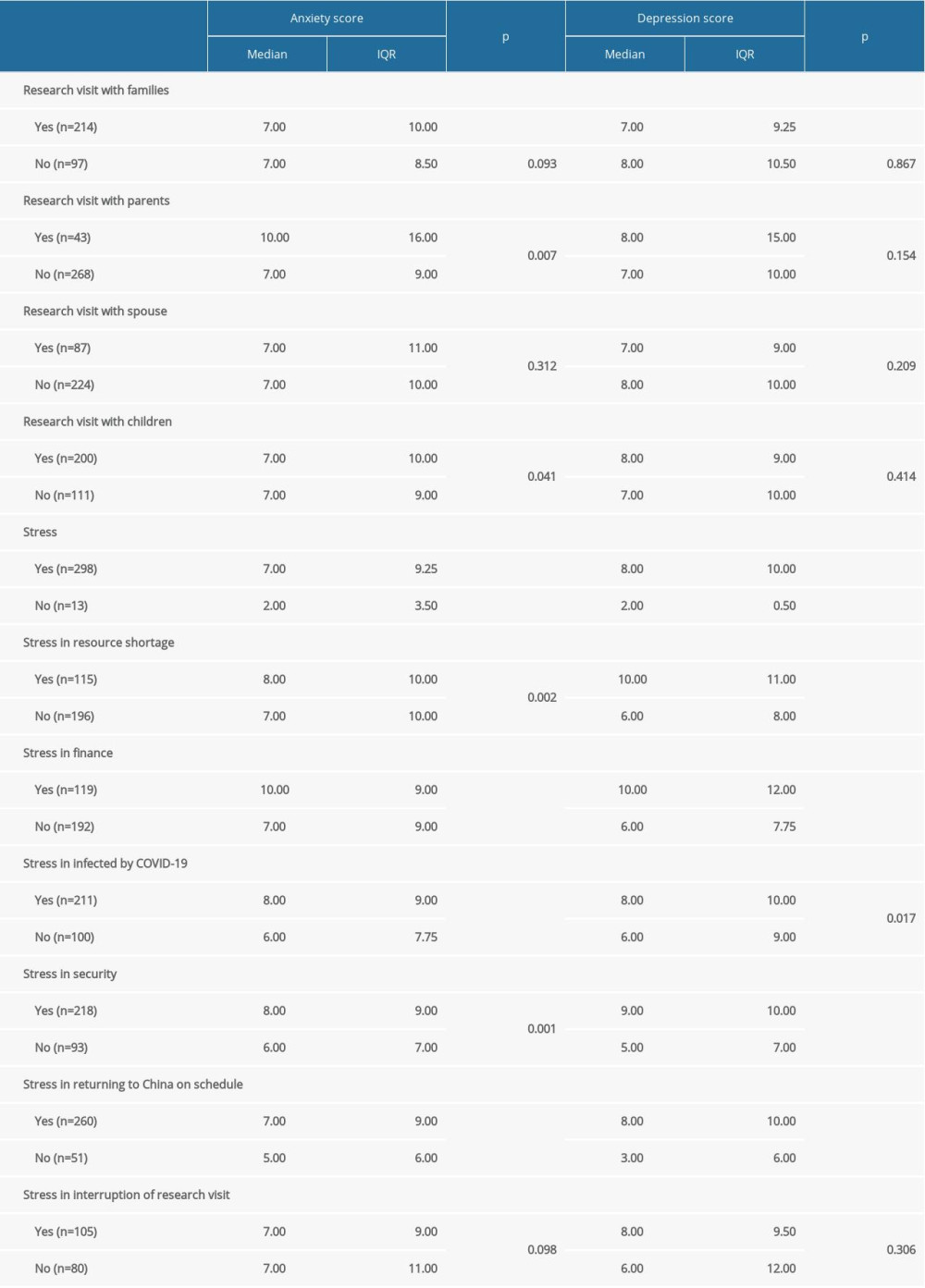 Table 2. Correlations of factors with anxiety and depression scores.
Table 2. Correlations of factors with anxiety and depression scores.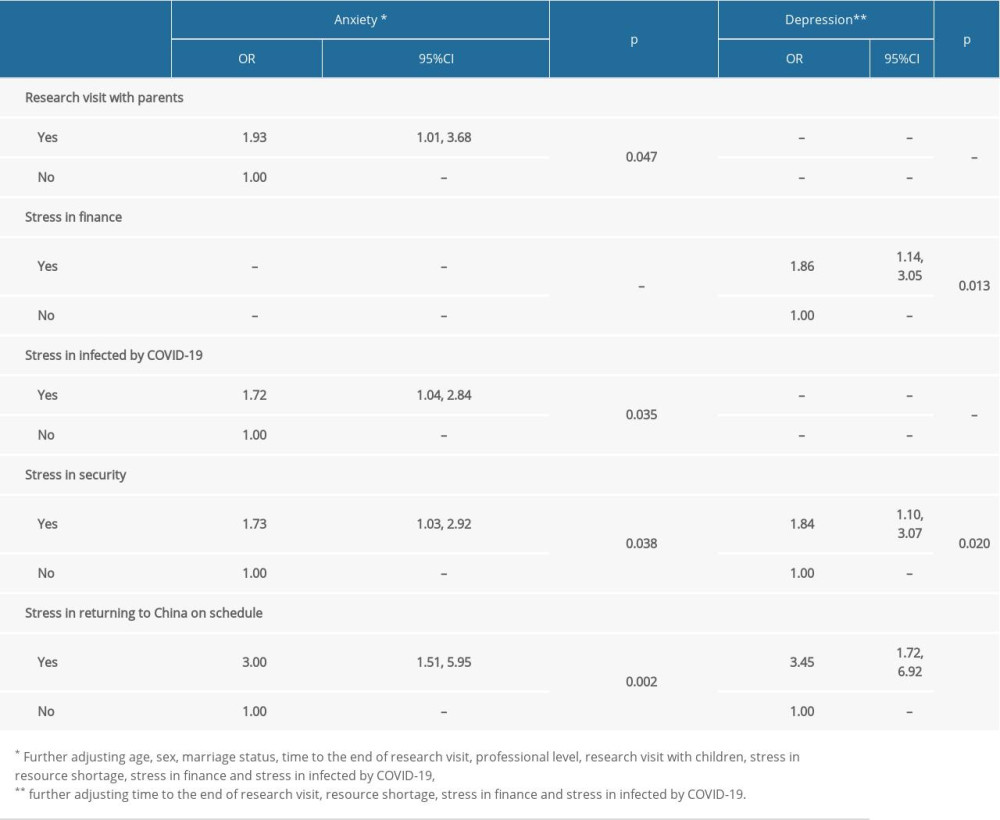 Table 3. Multivariate ordinal logistic regression analysis of factors significantly associated with anxiety and depression.
Table 3. Multivariate ordinal logistic regression analysis of factors significantly associated with anxiety and depression. Table 1. Relationships between subject characteristics and anxiety and depression scores.
Table 1. Relationships between subject characteristics and anxiety and depression scores. Table 2. Correlations of factors with anxiety and depression scores.
Table 2. Correlations of factors with anxiety and depression scores. Table 3. Multivariate ordinal logistic regression analysis of factors significantly associated with anxiety and depression.
Table 3. Multivariate ordinal logistic regression analysis of factors significantly associated with anxiety and depression. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








