20 January 2021: Meta-Analysis
Association Between Mitochondrial DNA Copy Number and Head and Neck Squamous Cell Carcinoma: A Systematic Review and Dose-Response Meta-Analysis
Zhu Zhu1ABCDEF, Yixiu Liu2B, Didi Wu1C, Hongpeng Wang2ABCDEF*DOI: 10.12659/MSM.928327
Med Sci Monit 2021; 27:e928327
Abstract
BACKGROUND: The association between mitochondrial DNA (mtDNA) copy number and head and neck squamous cell carcinoma (HNSCC) risk remains unclear. Therefore, we aimed to evaluate the relationship between mtDNA copy number and HNSCC risk.
MATERIAL AND METHODS: We searched PubMed, Web of Science, and EMBASE until August 2020. Studies that assessed the association between mtDNA copy number and HNSCC as the outcome of interest were included. We performed a 2-class and dose-response meta-analysis to assess the association between cancer risk and mtDNA.
RESULTS: Eight articles (2 cohort studies and 6 case-control studies) with a total of 3913 patients were included in our meta-analysis. The overall results showed that mean mtDNA copy number level from 9 studies was 0.71 higher in patients with cancer than in non-cancer controls (the standardized mean differences (SMD) 0.71, 95% CI: 0.28–1.15, P<0.001). However, when 4 studies were pooled by dichotomizing mtDNA copy number at the median value into high- and low-content groups, no significant association between mtDNA content and overall cancer risk was found (odds ratio (OR)=0.87, 95% CI: 0.52–1.44, P=0.584). Furthermore, we observed a non-linear association from 3 studies between increased mtDNA copy number levels (P for nonlinearity <0.001).
CONCLUSIONS: The elevated mtDNA copy number could predict the risk of HNSCC as a biomarker. Moreover, there was non-linear relationship of risk between HNSCC and mtDNA copy number.
Keywords: Gene Dosage, Genes, Mitochondrial, review, DNA Copy Number Variations, DNA, Mitochondrial, Squamous Cell Carcinoma of Head and Neck
Background
Head and neck cancer (HNC) mainly consists of carcinomas arising from mucosal surfaces of 4 major anatomical sites: nasal cavity/paranasal sinuses, oral cavity, pharynx, and larynx [1]. According to the latest cancer statistics in 2018, it ranked 7th among causes of cancer-related death, and there were about 700 000 new cases and 350 000 deaths around the world [2]. Studies have revealed that about 58% of patients with head and neck squamous cell carcinoma (HNSCC) are in the advanced stage of disease (stage III~IV) when diagnosed and treated. Recently, comprehensive treatment techniques including surgery, radiotherapy, and chemotherapy have significantly improved; however, there were still 30–40% of patients with distant metastasis within 5 years [1,3,4]. Therefore, it is of profound significance for the treatment of HNSCC to actively explore tumor biomarkers which can be used for molecular diagnosis, prognosis, and targeted therapy.
Mitochondria is semi-autonomous organelle with independent genetic material, which provides the energy source for organisms [5]. Compared to the nuclear genome, mitochondrial DNA (mtDNA) is prone to damage from reactive oxygen species due to lack of protective histones and introns [6–8]. Additionally, alterations of mtDNA through genetic mutations or increased/decreased mtDNA copy number contribute to multiple diseases, such as cardiovascular diseases and carcinomas [9–13]. Once mtDNA damage occurs, the level of mtDNA copy number is altered, resulting in mitochondrial dysfunction, which is considered to be an essential pathogenesis of cancer [11]. To some extent, the mtDNA copy number can reflect the level of mtDNA damage and be an indication of mitochondrial function [14,15]. Many studies have reported the association between the mtDNA copy number and HNSCC risk in peripheral blood leukocytes or tissues, but these studies have not reached consistent conclusions [16–23]. Consequently, we conducted a meta-analysis to comprehensively evaluate whether changes in the mtDNA copy number are related to HNSCC risk. This study will clarify the value of mtDNA copy number as a biomarker and ultimately provide guidance for screening the high-risk HNSCC population and achieve tertiary prevention.
Material and Methods
SEARCH STRATEGY AND STUDY SELECTION:
A comprehensive search of the literature was carried out in PubMed, Web of Science, and EMBASE databases published up to August 2020. The search terms were: “head and neck cancer” (e.g., “head and neck squamous cell carcinoma”, “HNSCC”, “laryngeal squamous cell carcinoma (LSCC)”, “squamous cell carcinoma of the tongue (SCCT)”, “oral squamous cell carcinoma (OSCC)”, “hypopharyngeal squamous cell carcinoma”); “mitochondrial DNA” or “mtDNA”; and “copy number” or “content”. We also searched the reference lists of extracted documents. The flow diagram detailing the database searches and included publications is illustrated in Figure 1.
Published studies were included in our analysis if they met the following criteria: 1) case-control or cohort observational studies conducted on human adults; 2) studies that assessed the association between mtDNA copy number and HNSCC as the outcome of interest; 3) studies that reported the level or distribution of mtDNA copy number in both cancer cases and controls; and 4) studies that reported odds ratio (OR) with the corresponding 95% confidence intervals (95% CI) or other available data for calculating the OR and 95% CI. The exclusion criteria were: 1) letters, editorials, case reports, reviews, meta-analyses, and ecological studies; 2) non-English studies; 3) the mtDNA copy number was used to assess other cancers or without a control population. In case of duplications, the publication with the most complete information available was included in this study.
DATA EXTRACTION AND RISK OF BIAS ASSESSMENT:
Two reviewers (ZZ and YL) independently screened included publications and discrepancies were resolved by consensus or the third reviewer (HW). The following details were extracted: the name of the first author, publication year, cancer type, location of study, study design, source of sample, method used for measurement of mtDNA copy number, sample size, mtDNA level copies, mtDNA gene, nuclear DNA (nDNA) gene, age, sex, smoking, and case/control patients by mtDNA copy number level categorization.
The Newcastle-Ottawa Scale (NOS), which is commonly used to assess the quality of selection, comparability, and outcome/exposure of study participants, was used to evaluate included studies. The maximum score is 9 stars [25]. Discrepancies generated from NOS assessment by 2 independent researchers were resolved by consensus.
STATISTICAL ANALYSIS:
In 2-class meta-analysis, the mean and standard deviation (SD) of mtDNA copy number level was used to estimate the effect size in the HNSCC case group and control group. If not provided, the mean and SD of the mtDNA copy number were evaluated based on median, first quartile, third quartile, and sample size [26,27]. In addition, the pooled risk was compared between high versus low median mtDNA copy number level. If studies reported the association between 3 or more mtDNA copy number categories and HNSCC risk, we identified the possible non-linear association through a 2-stage, random-effects, dose-response meta-analysis. We also conducted through modeling of mtDNA copy number level and restricted cubic splines with 3 knots.
Heterogeneity between studies was analyzed using the I2, where an I2 greater than 50 indicates substantial heterogeneity [28,29]. A random-effects model was performed if a fixed random-effects model was unavailable [28]. When possible, subgroup analysis was used to investigate potential sources of heterogeneity. Furthermore, publication bias was examined by using funnel plots and Egger’s and Begg’s test.
The data were collected and integrated in Excel 2016 (Microsoft Office, Redmond, USA). All statistical analysis was conducted using STATA version 15 (StataCorp LLC, College Station, TX, USA), and a statistical significance was set at
Results
CHARACTERISTICS OF STUDIES AND PATIENTS:
Table 1 and Supplementary Table 1 summarized the main characteristics of the patients and studies included in this comprehensive analysis. Among the 8 included articles, 3 studies were from the USA, 2 were from India, and 3 were from China. DNA was extracted from peripheral blood lymphocytes (PBL), tissues, or saliva, then quantitative reverse transcription PCR amplification was performed for the mtDNA gene and the nuclear gene. All studies were observational, including 6 case-control studies and 2 cohort studies. A total of 3913 patients (1288 cancer cases and 2625 non-cancer controls) were included in the studies. In the case group, 73.3% (934/1274) were male, 57.1% (727/1274) were ever-smoking, and the mean age was 59.6 years. Except for Kim 2004, all studies were considered high-quality (NOS score ≥6). Out of 8 eligible articles, 1 paper (Jiang 2005) evaluated 2 mtDNA genes and were analyzed as 2 studies for level of mtDNA copy number.
META-ANALYSIS OF THE AVERAGE LEVEL OF MTDNA COPY NUMBER:
The first 2-class meta-analysis was performed for comparison of the mtDNA copy number level. In Figure 2, we pooled data from 9 studies to demonstrate the mtDNA copy number level between HNSCC cases and the control group [16–23]. There was a significantly higher level of mtDNA copy number among HNSCC cases (SMD=0.71, 95% CI: 0.28–1.15, P<0.001) based on the random-effects model and a substantial level of heterogeneity was observed (I2=96.8%, P<0.001).
Funnel plots are shown in Supplementary Figure 1. An unexpected shape was observed, indicating evidence of significant bias. However, there was no evidence of bias in the Egger’s test and Begg’s test results (P=0.227 and 0.348, respectively). Results of subgrouping are presented in Table 2. There was a low level of heterogeneity in subgrouping according to region, mtDNA gene, and NOS score.
META-ANALYSIS OF MTDNA COPY NUMBER LEVEL AND HNSCC RISKS:
We conducted the second 2-class meta-analysis to assess the potential association between mtDNA content level and HNSCC. When 4 studies were pooled by dichotomizing mtDNA copy number at the median value into high- and low-content groups, including a total of 2047 participants and 404 with high contents in the case group, no significant association between mtDNA content and overall cancer risk was found (pooled effect size comparing high and low contents; OR=0.87, 95% CI: 0.52–1.44, P=0.584) with substantial heterogeneity (I2=82.5%, P=0.001) (Figure 3) [18–20,23]. Similarly, funnel plots appeared symmetrical, indicating no overt evidence of significant bias (all P>0.50) (Supplementary Figure 1). Furthermore, subgroup analysis showed a low level of heterogeneity in subgrouping according to region, mtDNA gene, and NOS score (Table 2).
LINEAR AND NON-LINEAR DOSE-RESPONSE ANALYSIS:
Three of 8 publications on the association between mtDNA copy number level and HNSCC risk were included for dose-response meta-analysis [19,20,23]. We found a significant non-linear association (P<0.001 for nonlinearity; Figure 4). As shown in Figure 4, there was a reduction in cancer risk between the level of 0–5 mtDNA and after that there was an increase in risk of cancer.
Discussion
We assessed available data from 8 observational studies that reported the association between mtDNA copy number level and HNSCC risk in adults. We found a significant association between higher mtDNA copy number and higher risk of cancer. In addition, there was non-linear relationship of risk between HNSCC and mtDNA copy number.
In the present meta-analysis, we performed 3 pooled evaluations: 1) to evaluate the mtDNA copy number level between HNSCC case and control groups; 2) to evaluate the risk of HNSCC for cases in the high versus the low category of mtDNA copy number by dichotomizing at the median value; and 3) to evaluate the dose-response association between mtDNA copy number and the risk of HNSCC. In the first 2-class meta-analysis, the pooled SMD was 0.71 (95% CI: 0.28–1.15), indicating that the mtDNA copy number was higher in HNSCC patients than in the controls. There was substantial heterogeneity across studies (
Adjusted for potential confounding covariance, He et al. [18], using the median mtDNA copy number as a cutoff, found that individuals with a high mtDNA copy number had significantly higher risk of having oral premalignant lesions than those with a low mtDNA copy number. Wang et al. [19] found a U-shaped association between the mtDNA copy number and HNSCC risk. Interestingly, there was no significant association between mtDNA content and overall HNSCC risk in our second 2-class meta-analysis.
It seems that the possible reason for these differences was the dose-dependent association between mtDNA copy number level and HNSCC risk. The present study found that the relationship between mtDNA copy number level and the risk of HNSCC is a non-linear association (
Although previous studies have demonstrated an association between mtDNA copy number and HNSCC risk, to the best of our knowledge, our systematic review is the first comprehensive quantitative analysis from 3 pooled evaluations [14,15,36]. One of the studies aimed to interpret the relationship between mtDNA copy number and cancer prognosis [15], and others aimed to illustrate the association between mtDNA copy number and cancer risk [14,36]. These 3 studies did not take into account the relationship between dose-dependent mtDNA copy number and HNSCC.
The present study has certain limitations that should be considered. First, we only included a small number of studies, only 3 of 8 publications performing dose-response meta-analysis were included, and our comprehensive analysis could not assess the potential temporal association between mtDNA copy number and HNSCC risk. Second, pathogenic factors for HNSCC include alcohol and tobacco consumption, as well as human papilloma virus infection. However, lack of sufficient information limited our further evaluation of behavioral and clinicopathological characteristics of cancer by mtDNA copy number. In addition, not all studies provided mean and SD for evaluating the mtDNA copy number level between HNSCC case and control groups, and this led a possible bias risk, which limits interpretation of the results. Furthermore, all of the included studies were observational research, which limited the causal inference. Further long-term prospective studies should be performed for determining the mtDNA copy number as a biomarker for predicting HNSCC.
Conclusions
In conclusion, the elevated mtDNA copy number could predict the risk of HNSCC as a biomarker. Moreover, there was a non-linear relation of risk between HNSCC and mtDNA copy number.
Figures
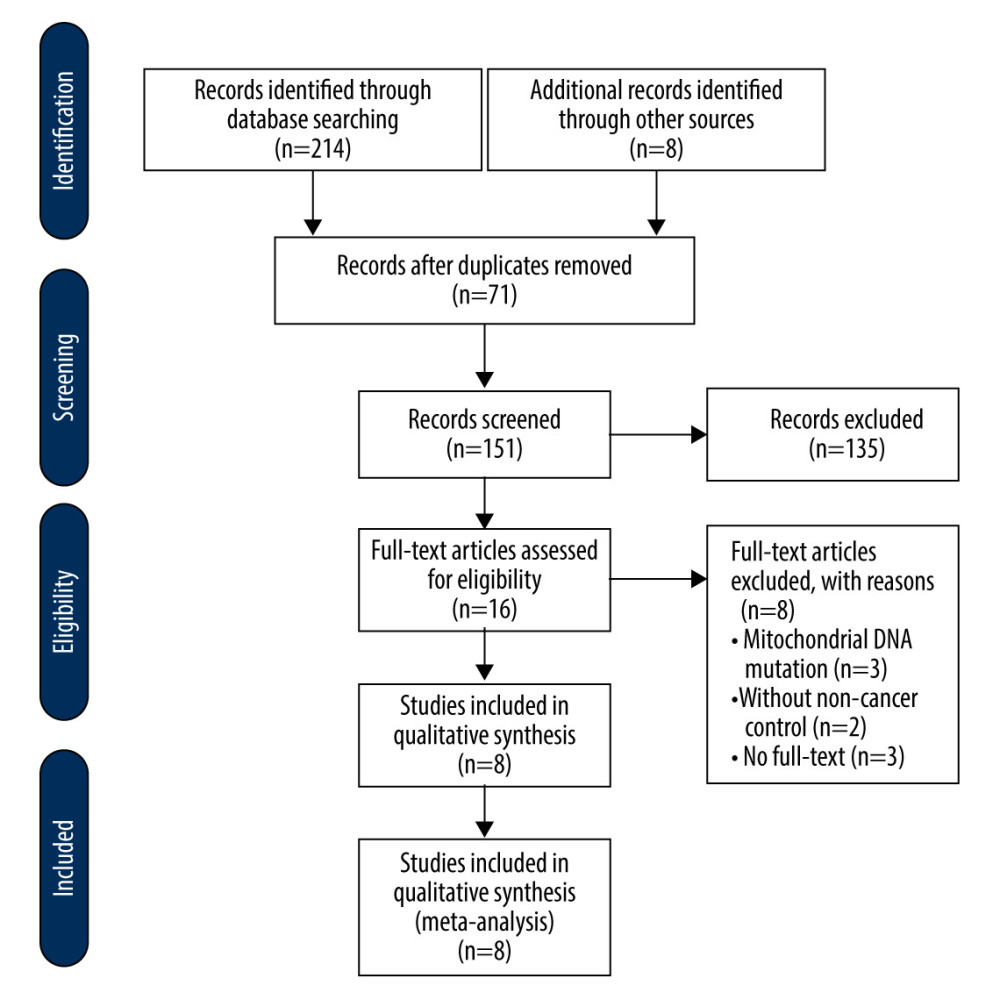 Figure 1. The review flow diagram for identification of study screening and selection.
Figure 1. The review flow diagram for identification of study screening and selection. 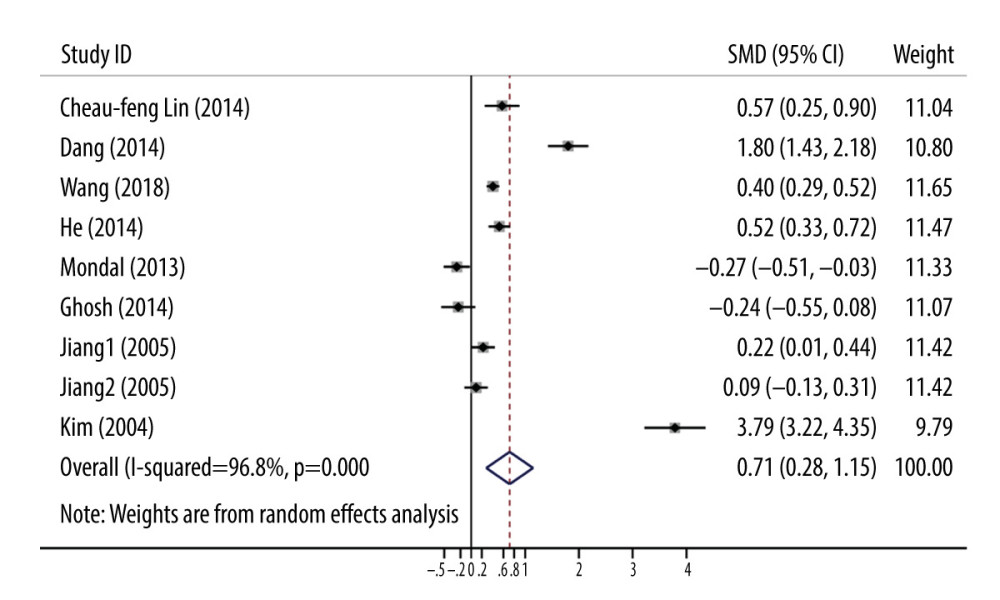 Figure 2. Forest plots of SMD with 95% CI for the levels of mtDNA copy number in head and neck squamous cell carcinoma (HNSCC) cases versus controls.
Figure 2. Forest plots of SMD with 95% CI for the levels of mtDNA copy number in head and neck squamous cell carcinoma (HNSCC) cases versus controls. 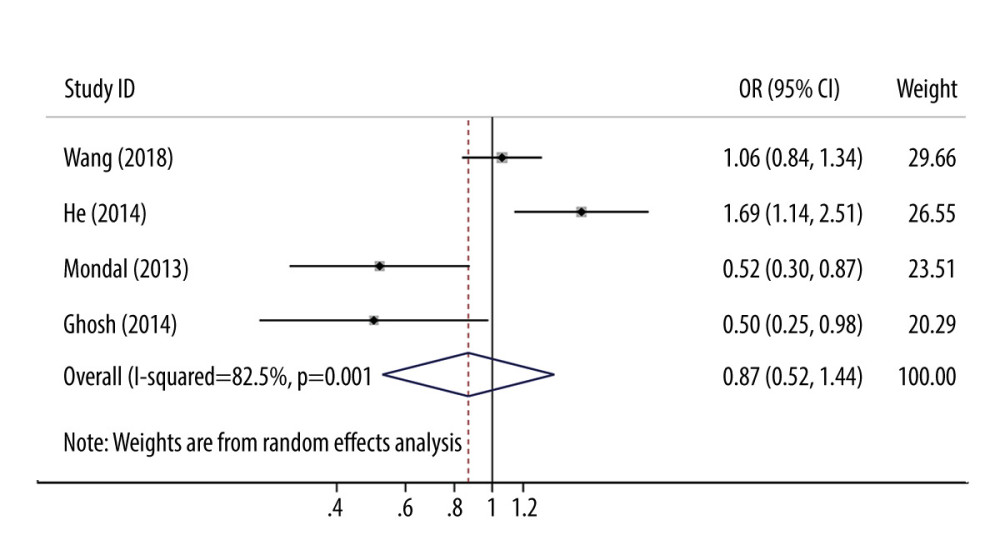 Figure 3. Forest plot presenting OR for head and neck squamous cell carcinoma (HNSCC) in the high versus the low category of mtDNA copy number by dichotomizing at the median value.
Figure 3. Forest plot presenting OR for head and neck squamous cell carcinoma (HNSCC) in the high versus the low category of mtDNA copy number by dichotomizing at the median value. 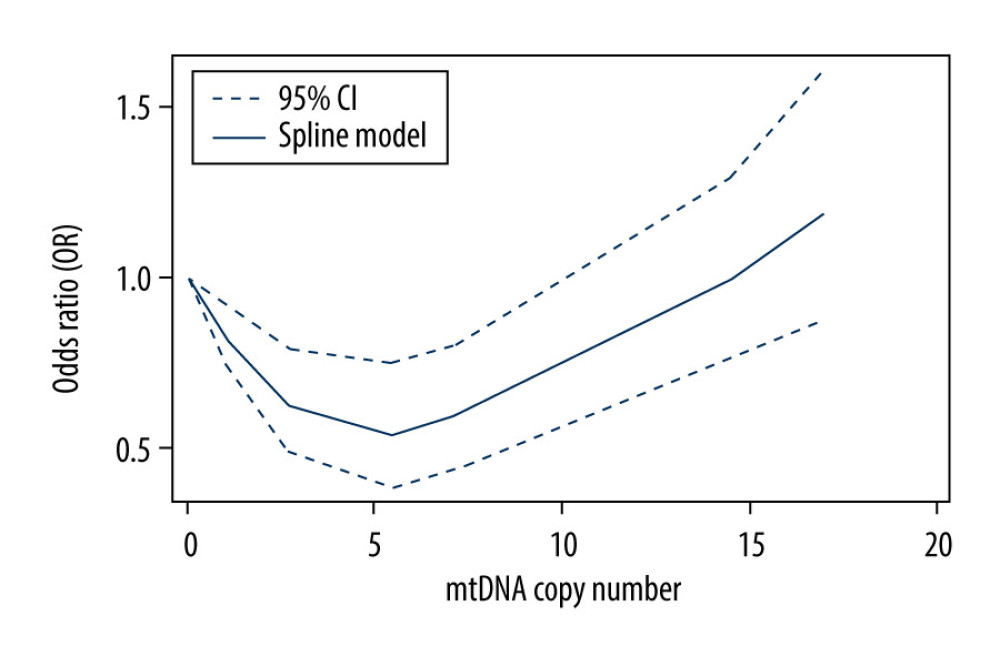 Figure 4. Dose-response association between the mtDNA copy number and head and neck squamous cell carcinoma (HNSCC) risk. mtDNA copy number was modeled with restricted cubic splines in a random-effects dose-response model. Solid line indicates the spline model; dashed lines represent 95% confidence intervals.
Figure 4. Dose-response association between the mtDNA copy number and head and neck squamous cell carcinoma (HNSCC) risk. mtDNA copy number was modeled with restricted cubic splines in a random-effects dose-response model. Solid line indicates the spline model; dashed lines represent 95% confidence intervals. References
1. Leemans CR, Braakhuis BJ, Brakenhoff RH, The molecular biology of head and neck cancer: Nat Rev Cancer, 2011; 11; 9-22
2. Bray F, Ferlay J, Soerjomataram I, Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries: Cancer J Clin, 2018; 68; 394-424
3. Oliva M, Spreafico A, Taberna M, Immune biomarkers of response to immune-checkpoint inhibitors in head and neck squamous cell carcinoma: Ann Oncol, 2019; 30; 57-67
4. Kaidar-Person O, Gil Z, Billan S, Precision medicine in head and neck cancer: Drug Resist Update, 2018; 40; 13-16
5. Fu Y, Tigano M, Sfeir A, Safeguarding mitochondrial genomes in higher eukaryotes: Nat Struct Mol Biol, 2020; 27; 687-95
6. Orekhov AN, Poznyak AV, Sobenin IA, Mitochondrion as a selective target for treatment of atherosclerosis: Role of mitochondrial DNA mutations and defective mitophagy in the pathogenesis of atherosclerosis and chronic inflammation: Curr Neuropharmacol; 2019 [Online ahead of print]
7. Gray K, Kumar S, Figg N, Effects of DNA damage in smooth muscle cells in atherosclerosis: Circ Res, 2015; 116; 816-26
8. Li Y, Huang W, Yu Q, Lower mitochondrial DNA content relates to high-altitude adaptation in Tibetans: Mitochondrial DNA Part A, 2016; 27; 753-57
9. Corsi S, Iodice S, Vigna L, Platelet mitochondrial DNA methylation predicts future cardiovascular outcome in adults with overweight and obesity: Clin Epigenetics, 2020; 12; 29
10. Liu LP, Cheng K, Ning MA, Association between peripheral blood cells mitochondrial DNA content and severity of coronary heart disease: Atherosclerosis, 2017; 261; 105-10
11. Luo Y, Ma J, Lu W, The significance of mitochondrial dysfunction in cancer: Int J Mol Sci, 2020; 21; 5598
12. Mohamed Yusoff AA, Mohd Nasir KN, Haris K, Detection of somatic mutations in the mitochondrial DNA control region D-loop in brain tumors: The first report in Malaysian patients: Oncol Lett, 2017; 14; 5179-88
13. Chang X, Bakay M, Liu Y, Mitochondrial DNA haplogroups and susceptibility to neuroblastoma: J Natl Cancer Inst, 2020; 25; djaa024
14. Hu L, Yao X, Shen Y, Altered mitochondrial DNA copy number contributes to human cancer risk: Evidence from an updated meta-analysis: Sci Rep, 2016; 6; 35859
15. Chen N, Wen S, Sun X, Elevated mitochondrial DNA copy number in peripheral blood and tissue predict the opposite outcome of cancer: A meta-analysis: Sci Rep, 2016; 6; 37404
16. Cheau-Feng Lin F, Jeng YC, Huang TY, Mitochondrial DNA copy number is associated with diagnosis and prognosis of head and neck cancer: Biomarkers, 2014; 19; 269-74
17. Dang S, Qu Y, Wei J, Low copy number of mitochondrial DNA (mtDNA) predicts worse prognosis in early-stage laryngeal cancer patients: Diagn Pathol, 2014; 9; 28
18. He Y, Gong Y, Gu J, Increased leukocyte mitochondrial DNA copy number is associated with oral premalignant lesions: An epidemiology study: Carcinogenesis, 2014; 35; 1760-64
19. Wang L, Lv H, Ji P, Mitochondrial DNA copy number is associated with risk of head and neck squamous cell carcinoma in Chinese population: Cancer Med, 2018; 7; 2776-82
20. Mondal R, Ghosh SK, Choudhury JH, Mitochondrial DNA copy number and risk of oral cancer: A report from Northeast India: PLoS One, 2013; 8; e57771
21. Jiang WW, Masayesva B, Zahurak M, Increased mitochondrial DNA content in saliva associated with head and neck cancer: Clin Cancer Res, 2005; 11; 2486-91
22. Kim MM, Clinger JD, Masayesva BG, Mitochondrial DNA quantity increases with histopathologic grade in premalignant and malignant head and neck lesions: Clin Cancer Res, 2004; 10; 8512-15
23. Ghosh SK, Singh AS, Mondal R, Dysfunction of mitochondria due to environmental carcinogens in nasopharyngeal carcinoma in the ethnic group of Northeast Indian population: Tumour Biol, 2014; 35; 6715-24
24. Moher D, Liberati A, Tetzlaff J, Altman DG, Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement: PLoS Med, 2009; 6; e1000097
25. Yang L, Tang H, Lin X, OPA1-Exon4b binds to mtDNA D-loop for transcriptional and metabolic modulation, independent of mitochondrial fusion: Front Cell Dev Biol, 2020; 8; 180
26. Wan X, Wang W, Liu J, Tong T, Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range: BMC Med Res Methodol, 2014; 14; 135
27. Luo D, Wan X, Liu J, Tong T, Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range: Stat Methods Med Res, 2018; 27; 1785-805
28. Naghshi S, Sadeghi O, Willett WC, Esmaillzadeh A, Dietary intake of total, animal, and plant proteins and risk of all cause, cardiovascular, and cancer mortality: Systematic review and dose-response meta-analysis of prospective cohort studies: BMJ, 2020; 370; m2412
29. Higgins JP, Thompson SG, Deeks JJ, Altman DG, Measuring inconsistency in meta-analyses: BMJ, 2003; 327; 557-60
30. Boyapati RK, Rossi AG, Satsangi J, Ho GT, Gut mucosal DAMPs in IBD: From mechanisms to therapeutic implications: Mucosal Immunol, 2016; 9; 567-82
31. Tabrizi SJ, Flower MD, Ross CA, Wild EJ, Huntington disease: new insights into molecular pathogenesis and therapeutic opportunities: Nat Rev Neurol, 2020; 16(10); 529-46
32. Zhou S, Kachhap S, Sun W, Frequency and phenotypic implications of mitochondrial DNA mutations in human squamous cell cancers of the head and neck: Proc Natl Acad Sci USA, 2007; 104; 7540-45
33. Prior SL, Griffiths AP, Baxter JM, Mitochondrial DNA mutations in oral squamous cell carcinoma: Carcinogenesis, 2006; 27; 945-50
34. Mithani SK, Taube JM, Zhou S, Mitochondrial mutations are a late event in the progression of head and neck squamous cell cancer: Clin Cancer Res, 2007; 13; 4331-35
35. Chatterjee A, Dasgupta S, Sidransky D, Mitochondrial subversion in cancer: Cancer Prev Res (Phila), 2011; 4; 638-54
36. Mi J, Tian G, Liu S, The relationship between altered mitochondrial DNA copy number and cancer risk: A meta-analysis: Sci Rep, 2015; 5; 10039
Figures
 Figure 1. The review flow diagram for identification of study screening and selection.
Figure 1. The review flow diagram for identification of study screening and selection. Figure 2. Forest plots of SMD with 95% CI for the levels of mtDNA copy number in head and neck squamous cell carcinoma (HNSCC) cases versus controls.
Figure 2. Forest plots of SMD with 95% CI for the levels of mtDNA copy number in head and neck squamous cell carcinoma (HNSCC) cases versus controls. Figure 3. Forest plot presenting OR for head and neck squamous cell carcinoma (HNSCC) in the high versus the low category of mtDNA copy number by dichotomizing at the median value.
Figure 3. Forest plot presenting OR for head and neck squamous cell carcinoma (HNSCC) in the high versus the low category of mtDNA copy number by dichotomizing at the median value. Figure 4. Dose-response association between the mtDNA copy number and head and neck squamous cell carcinoma (HNSCC) risk. mtDNA copy number was modeled with restricted cubic splines in a random-effects dose-response model. Solid line indicates the spline model; dashed lines represent 95% confidence intervals.
Figure 4. Dose-response association between the mtDNA copy number and head and neck squamous cell carcinoma (HNSCC) risk. mtDNA copy number was modeled with restricted cubic splines in a random-effects dose-response model. Solid line indicates the spline model; dashed lines represent 95% confidence intervals. Tables
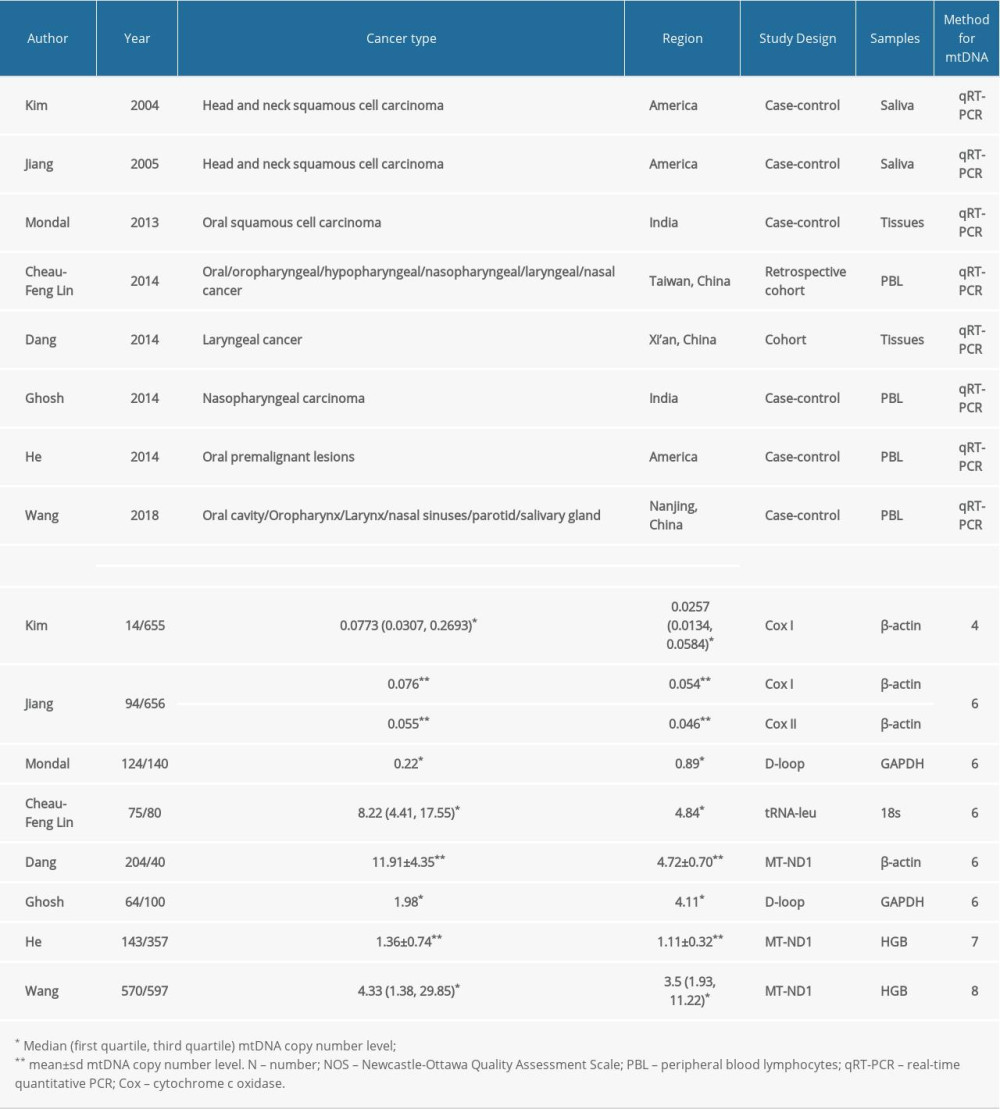 Table 1. The baseline characteristics of included studies.
Table 1. The baseline characteristics of included studies.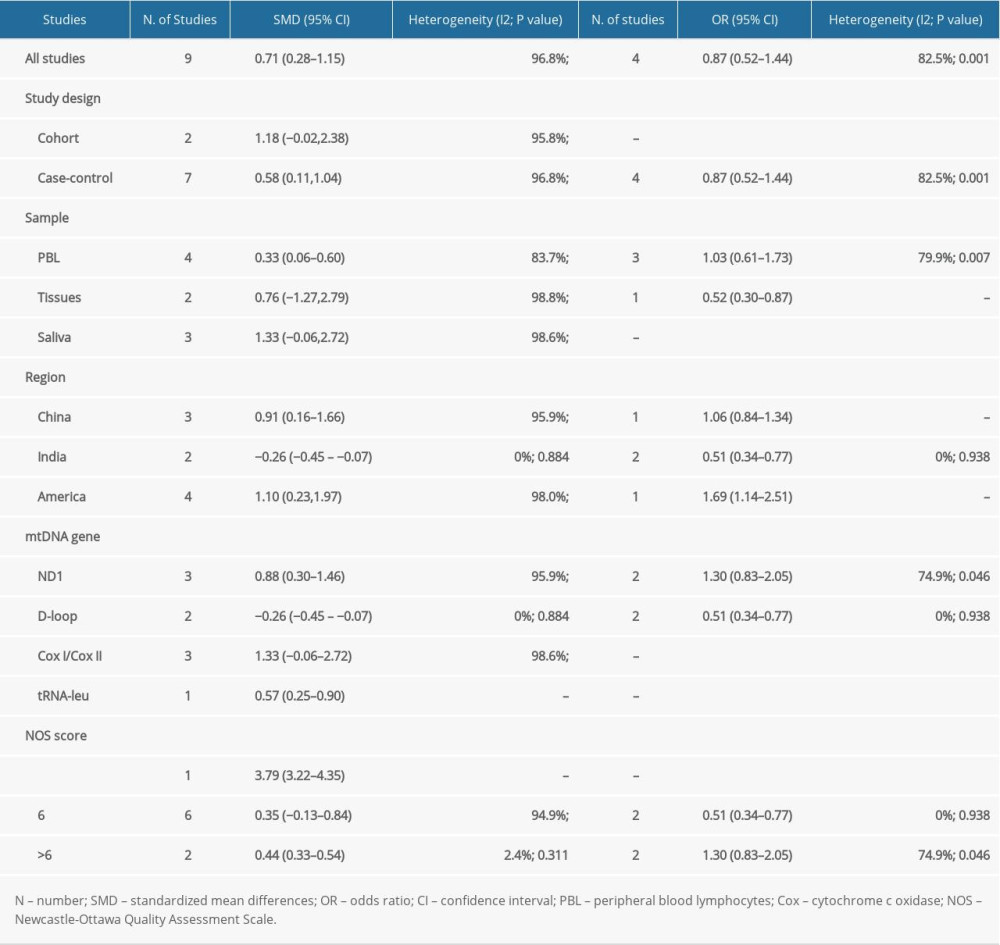 Table 2. Subgroup analyses for the two class meta-analysis.
Table 2. Subgroup analyses for the two class meta-analysis. Table 1. The baseline characteristics of included studies.
Table 1. The baseline characteristics of included studies. Table 2. Subgroup analyses for the two class meta-analysis.
Table 2. Subgroup analyses for the two class meta-analysis.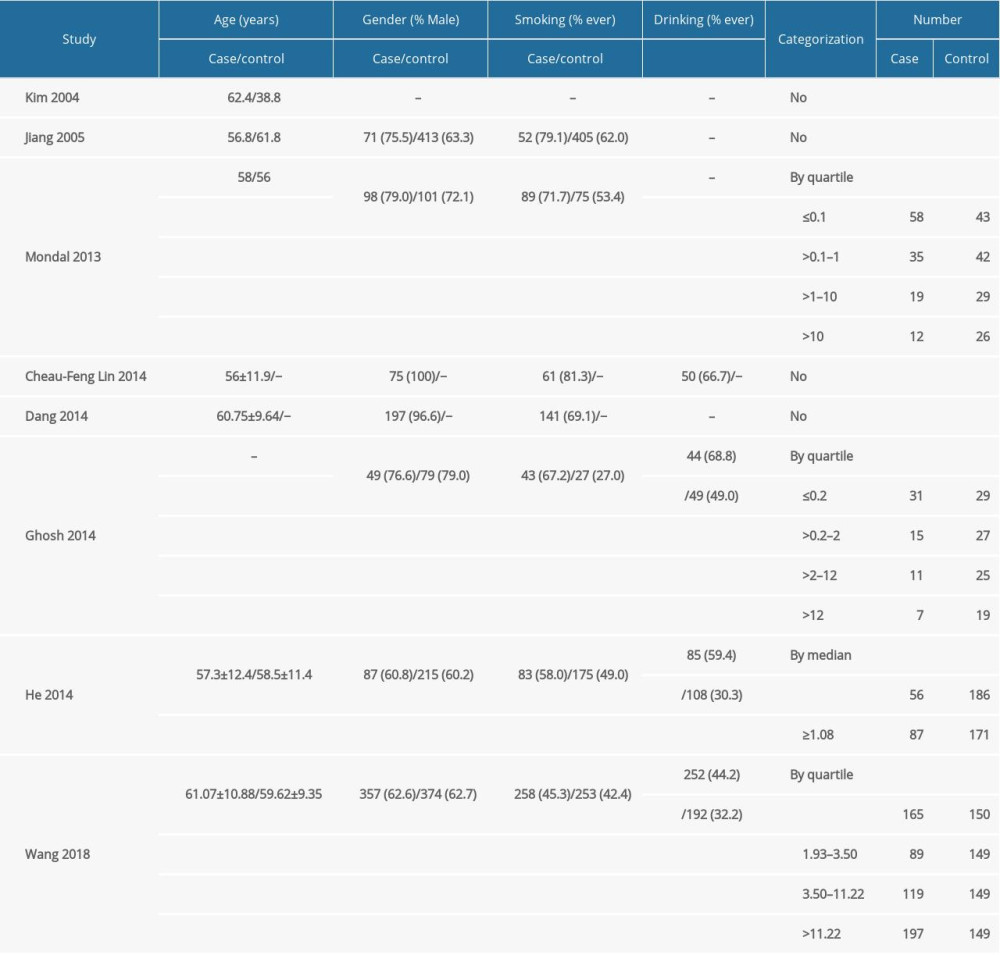 Supplementary Table 1. Supplementary information of included studies.
Supplementary Table 1. Supplementary information of included studies. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








