03 January 2021: Clinical Research
Influenza-Associated Encephalopathy and Acute Necrotizing Encephalopathy in Children: A Retrospective Single-Center Study
Yongling Song1ACE, Suyun Li1B, Weiqiang Xiao2BD, Jun Shen3D, Wencheng Ma1D, Qiang Wang1F, Haomei Yang1F, Guangming Liu1F, Yan Hong3F, Peiqing Li1AG*, Sida Yang4AGDOI: 10.12659/MSM.928374
Med Sci Monit 2021; 27:e928374
Abstract
BACKGROUND: Although influenza primarily affects the respiratory system, it can cause severe neurological complications, especially in younger children, but knowledge about the early indicators of acute necrotizing encephalopathy (ANE) is limited. The main purpose of this article is to summarize the clinical characteristics, diagnosis, and treatment of neurological complications of influenza in children, and to identify factors associated with ANE.
MATERIAL AND METHODS: This was a retrospective study of children with confirmed influenza with neurological complications treated between 01/2014 and 12/2019 at Guangzhou Women and Children’s Medical Center. A receiver operating characteristics curve analysis was performed to determine the prognostic value of selected variables.
RESULTS: Sixty-three children with IAE (n=33) and ANE (n=30) were included. Compared with the IAE group, the ANE group showed higher proportions of fever and acute disturbance of consciousness, higher alanine aminotransferase, higher aspartate aminotransferase, higher creatinine kinase, higher procalcitonin, higher cerebrospinal fluid (CSF) protein, and lower CSF white blood cells (all P<0.05). The areas under the curve (AUCs) for procalcitonin and CSF proteins, used to differentiate IAE and ANE, were 0.790 and 0.736, respectively. The sensitivity and specificity of PCT >4.25 ng/ml to predict ANE were 73.3% and 100.0%, respectively. The sensitivity and specificity of CSF protein >0.48 g/L to predict ANE were 76.7% and 69.7%, respectively. Thirteen (43.3%) children with ANE and none with IAE died (P<0.0001).
CONCLUSIONS: High levels of CSF protein and serum procalcitonin might be used as early indicators for ANE. All children admitted with neurological findings, especially during the influenza season, should be evaluated for influenza-related neurological complications.
Keywords: Child, Encephalitis, Influenza, Human, Brain Diseases, Brain Injuries, Child, Preschool, Electroencephalography, ROC Curve, Risk Factors
Background
Influenza in children is a major cause of morbidity and mortality worldwide. Annual epidemics in adults and children are associated with an estimated 3–5 million cases of severe illness, and about 290 000 to 650 000 deaths [1]. Influenza infection is seasonal in temperate countries, with peaks during the winter months, but it has sustained activity throughout the year in tropical climates. Influenza is a single-stranded RNA virus and a member of the Orthomyxoviridae family. Influenza A and B are the dominant circulating viruses, while influenza C is believed to cause mild infection [2,3]. Minor genetic variations (antigenic drift) are the cause of seasonal variation. Major large-scale reassortments generate novel strains (antigenic shift) with little or no pre-existing immunity in the human population, leading to pandemic strains [2,3]. Transmission occurs via respiratory droplets and fomites [2]. The incubation period is 1–4 days [2]. The populations with increased risk for complicated or severe disease course include all children aged 6–59 months, children who have chronic pulmonary (including asthma) or cardiovascular (except isolated hypertension), renal, hepatic, neurologic, hematologic, or metabolic disorders (including diabetes mellitus), children with immunosuppression due to medications or disease, such as HIV infection, children and adolescents (aged 6 months to 18 years) who are receiving long-term aspirin therapy and who might be at risk for Reye syndrome after influenza virus infection, adolescents who are or will be pregnant during the influenza season, residents of long-term care facilities, and children with morbid obesity [2,4].
Nervous system injury caused by influenza is one of the main causes of death caused by influenza among children, and the fatality rate is as high as 30% [5]. Neurological symptoms of brain injury usually appear on the same day or several days after the onset of cold symptoms, with convulsions and changes in consciousness the most common. The common types of nervous system injury caused by influenza are influenza-associated encephalopathy (IAE) [6], Reye’s syndrome, Guillain-Barré syndrome, hemorrhagic shock encephalopathy syndrome [7], and acute necrotizing encephalopathy (ANE) [6,8], among which ANE is the most serious [8].
Currently, there is a lack of early diagnosis indicators of influenza-associated nervous system injury, leading to delays for the early diagnosis of critical cases, resulting in poor prognosis and mortality [9]. No clinical symptoms and signs are specific to ANE, and the exact pathogenesis and risk factors of ANE are still poorly understood, but involve a cytokine storm [10]. Shock, multiorgan failure (MOF), and disseminated intravascular coagulation (DIC) are common [11–13]. Central nervous system injury may manifest as seizures, impaired consciousness, and focal neurological deficits [11,14–19]. The laboratory findings include hyperammonemia, hypoglycemia, lactic acidosis, high cerebrospinal fluid (CSF) protein levels, and decreased platelets [11,14,20–22]. Yamamoto et al. [23] suggested a score to predict the prognosis of ANE based on shock, brain stem lesions, age >4 years, low platelets, and elevated CSF proteins. Wong et al. [8] proposed a score based on radiological features (hemorrhage, cavitation, brain stem lesions, and white matter lesions). Nevertheless, those models included different variables and yield different prognostic values.
Therefore, the aim of the present study was to summarize the clinical characteristics, diagnosis, and treatment of neurological complications of influenza in children, and to identify factors associated with ANE. The results could allow for the early diagnosis of ANE and better patient prognosis.
Material and Methods
STUDY DESIGN AND PATIENTS:
This was a retrospective study of children with confirmed influenza with neurological complications treated between January 2014 and December 2019 at Guangzhou Women and Children’s Medical Center. The study was approved by the ethics committee of Guangzhou Women and Children’s Medical Center (Sui Fuer Kelun [2019] No. 38201). The need for individual consent was waived by the committee.
The inclusion criteria were: 1) <14 years of age; 2) positive real-time PCR detection of influenza virus in nasal and pharyngeal swabs; and 3) presence of symptoms and signs of nervous system injury, such as seizures, rapid cognitive impairment, mental changes, loss of consciousness, or coma. The exclusion criteria were: 1) co-infection with other infections such as herpes simplex virus, cytomegalovirus, or bacteria; 2) with serious comorbidities such as immune deficiency, metabolic disorders, trauma, cerebrovascular disease, or brain tumor; 3) congenital neurological malformation or syndrome; or 4) any inherited condition affecting the neurological functions.
DIAGNOSTIC CRITERIA:
IAE was defined as the presence of altered mental status, including behavioral changes, with no evidence of inflammation of the CNS [24]. The specific IAE diagnostic criteria were [25,26]: 1) acute onset and positive swab for the influenza virus; 2) accompanied by neurological symptoms such as seizures, rapid cognitive impairment, mental changes, loss of consciousness, or coma; 3) most CSF white blood cells are normal with a slight increase in CSF protein; 4) imaging supports encephalopathy, including cerebral edema, hemorrhage, bilateral thalamic lesions, or other imaging changes; and 5) the electroencephalogram (EEG) is normal.
The ANE diagnostic criteria were [27]: 1) acute onset, positive swab for the influenza virus; (2) the onset of influenza symptoms is quickly followed by neurological symptoms such as convulsions, acute disturbance of consciousness, altered mental status, and coma; 3) CSF white blood cell count is normal, and protein is normal or elevated; 4) imaging shows multiple symmetric lesions in the thalamus, brainstem, cerebellum medulla, inner capsule, putamen, and other parts; 5) serum transaminase is increased, accompanied by hyperammonemia or hypoglycemia; and 6) exclusion of brain dysfunction caused by other diseases.
All patients were divided into the IAE and ANE groups.
DATA COLLECTION:
Nasopharyngeal swabs were tested on the day of admission for syncytial virus, adenovirus, influenza A and B, parainfluenza virus, swine influenza virus, human metapneumovirus, and rhinovirus. Blood culture was performed to rule out septicemia due to fungus or bacteria. Clinical data (age, sex, fever, respiratory symptoms, headache, vomiting, convulsions, and disturbance of consciousness), laboratory results (blood routine, biochemical, CSF routine, biochemical, etiology, and culture), and imaging results (head magnetic resonance imaging (MRI) or computed tomography (CT)) from the medical charts. All radiographic examinations were performed by pediatric radiologists with at least 10 years of experience. The CT or MRI images were re-checked by the investigators to confirm the diagnosis of ANE or IAE. The main radiological criteria included abnormal signal, signal alteration, and enhancement.
OUTCOMES:
The prognosis was divided into 3 categories: 1) recovery without sequelae; 2) residual sequelae referring to neurological damage of encephalopathy over 6 months when the cause of the disease is stable, with the exception of neurological dysfunction caused by other diseases; and 3) death.
STATISTICAL METHOD:
SPSS 22.0 (IBM Corp., Armonk, NY, USA) was used for data analysis. The continuous data were non-normally distributed; they were presented as medians (interquartile range) and analyzed using the Mann-Whitney U-test. Categorical data were presented as numbers and rates and analyzed using the chi-square test or Fisher’s exact test, as appropriate. A receiver operating characteristic (ROC) curve analysis was applied to determine the performance of quantitative results of laboratory test to differentiate diagnosis IAE and ANE. Two-sided (except for the chi-square test)
Results
CHARACTERISTICS OF PATIENTS:
Over the 6-year period, 2124 hospitalized patients had a respiratory specimen positive for seasonal influenza A or B, of whom 63 (2.96%) had neurological complications, including 27 males (57.1%) and 36 females (42.9%). The median age was 4 years (2–11 years), among which 42 (66.7%) were ≤5 years old, and 21 cases (33.3%) were >5 years old. None of the children had received the flu vaccine. Influenza symptoms onset was 2 (1–13) days prior to the first onset of neurological symptoms, and the average time from onset to diagnosis was 5 (2–15) days. The most common clinical symptoms on admission were fever, acute disturbance of consciousness, convulsions, and vomiting. The demographic and clinical characteristics of the children are shown in Table 1. The distribution of the frequency of neurological complications in children with influenza during the 2014–2019 period is shown in Figure 1. Neurological complications in children with influenza mostly occurred from December to March, as shown in Figure 2. Moreover, there was no significant difference between the ANE group and the IAE group in the distribution over time.
According to the clinical symptoms, laboratory examination, and imaging examination, the cases were divided into the IAE (n=33) and ANE (n=30) groups. There were more children with fever >39°C in the ANE group (80.0% vs. 48.5%, P=0.02) and with acute disturbance of consciousness (93.3% vs. 18.2%, P<0.0001) (Table 1). All patients were treated with γ-globulin, methylprednisolone, and oseltamivir. More patients with ANE required mechanical ventilation (56.7% vs. 11.8%, P=0.0004). Six children in the ANE group in this study experienced cardiac arrest; none had such complications in the IAE group (P=0.009).
LABORATORY TESTS:
Compared with the IAE group, the ANE group showed higher alanine aminotransferase (ALT) (26 vs. 17 U/L, P=0.01), higher aspartate aminotransferase (AST) (50 vs. 40 U/L, P=0.049), higher creatinine kinase (CK) (170 vs. 105 U/L, P=0.03), higher procalcitonin (PCT) (6.8 vs. 3.2 ng/ml, P<0.0001), higher CSF protein (0.68 vs. 0.31 g/l, P=0.001), and lower CSF white blood cells (5 vs. 10×106/L, P=0.02) (Table 1). The CSF culture was negative in all patients. There was no difference in influenza A vs. B between the 2 groups (P=0.07). Tests for other common respiratory viruses were all negative.
ROC ANALYSIS:
Since PCT and CSF proteins were significantly higher in the ANE group compared with the IAE group, ROC curves were constructed to determine their ability to predict ANE (Figure 3). The areas under the curve (AUCs) for PCT and CSF proteins were 0.790 and 0.736, respectively. The sensitivity and specificity of PCT >4.25 ng/ml to predict ANE were 73.3% and 100.0%, respectively. The sensitivity and specificity of CSF protein >0.48 g/L to predict ANE were 76.7% and 69.7%, respectively (Table 2).
IMAGING AND EEG:
In this study, 4 children failed to complete cranial imaging examinations due to unstable conditions, while other children underwent cranial CT or MRI examination. The typical cranial MRI manifestations of ANE were bilateral thalamus, basal ganglia, medulla bulbus, pontine, and cerebellum symmetric high signals (Figure 4). Cranial MRI of children with IAE showed a variety of manifestations, as shown in Figure 5, without specificity, which could be manifested as scattered abnormal signal shadows and edema in the cerebral hemisphere, and no obvious abnormalities were observed in some children. The EEG of the ANE group showed diffuse slow-wave activity, while the EEG of the IAE group was normal.
TREATMENT AND OUTCOME:
After admission, all severely ill children were routinely monitored and actively treated with fever management and function support. Immediately after diagnosis, oseltamivir antiviral therapy was given, along with methylprednisolone (10 mg/kg/d), γ-globulin (1 g/kg/d for 2 days), and anti-inflammatory therapy. Among them, 21 children with central respiratory failure were given endotracheal intubation ventilator-assisted ventilation. Mannitol, concentrated sodium, cranial pressure lowering, and nutrition support were also given. The patients with ANE and central respiratory failure and severe coma were given plasma exchange.
After active rescue and treatment, in the IAE group, 22 (66.7%) patients recovered, 11 (33.3%) had sequelae, and none died. In the ANE group, 3 (10.0%) children recovered, 14 (46.7%) had sequelae, and 13 (43.3%) died. The differences between the 2 groups were significant (P<0.0001) (Table 3). Three children in the ANE group survived after plasma exchange.
Discussion
Neurological complications caused by influenza are serious conditions, mainly occurring in young children and with high morbidity and mortality rates [5]. H1N1 is a well-documented infectious disease causing a wide range of neurologic dysfunction that includes acute necrotizing encephalopathy, which is one of the most devastating forms of H1N1 infection and is a rare but serious complication of the disease [41]. This article summarized the clinical characteristics and prognosis of 63 children with influenza and neurological complications. The results indicate that high levels of CSF protein and serum procalcitonin might be used as early indicators for ANE. All children admitted with neurological findings, especially during the influenza season, should be evaluated for influenza-related neurological complications.
In this study, most children (n=42, 66.7%) with neurological complications were under the age of 5 years, consistent with the study by Lafond et al. [28]. According to the literature, most children who die of influenza have comorbidities such as congenital cardiovascular disease, neurological disease, lung disease, chromosome disease, or a genetic defect disease, cancer, and diabetes, among others [6,29–31,42,43]. On the other hand, all children in this study had no comorbidities and were previously healthy children, suggesting that influenza may still cause serious neurological complications in healthy children. The high-incidence season of this disease is from December to March of each year, which is consistent with the high-incidence season of influenza [32]. However, our study found that June was also the high-incidence IAE season, which may be related to the peak of influenza in Guangdong in June in recent years. This may be related to the rainy weather in Guangdong, which needs further study. The National Immunization Program of China does not cover seasonal influenza vaccine; therefore, it is necessary to pay attention to the prevention and control of influenza in healthy preschoolers during the high-incidence period of influenza.
The main clinical manifestations of the children in this study were fever, convulsions, disturbance of consciousness, and vomiting. Notably, the respiratory symptoms of these children were relatively mild, with only mild respiratory symptoms or no respiratory symptoms, suggesting that neurological symptoms may be the first or main symptom of IAE. The literature reports that IAE is mainly due to type A influenza virus [33,34], and influenza A (H1N1) is the most common virus in ANE [35,41], but this study suggested only a trend toward a higher frequency of influenza type B in children with ANE. The reason for this discrepancy might be related to the different types of influenza virus circulating each year and in each region, which needs to be further studied by increasing the sample size. Nevertheless, in clinical practice, we should also be aware that nervous system damage can still occur with influenza virus B.
Cranial MRI displays characteristic lesions and plays an important role in the diagnosis and clinical classification of neurological complications of influenza. It has been previously reported that typical cranial MRI in children with ANE is characterized by bilateral thalamus, basal ganglia, medulla oblong, and pons symmetric abnormalities [36,37,41], which is consistent with this study. Cranial MRI in children with ANE is specific and can assist in the early diagnosis of the disease. This is supported by Wong et al. [8], who designed a prediction model solely relying on MRI features.
ANE is a serious neurological complication of influenza in children, with a fatality rate as high as 30% [31]. In this study, the levels of CSF protein and procalcitonin in the ANE group were significantly higher than those in the IAE group. ROC curve analysis suggested that elevated CSF protein and procalcitonin could be used as indicators to predict the severity of neurological damage caused by influenza in children. Thus, the prognosis could be improved by the early measurement of PCT and cerebrospinal fluid protein to identify ANE. This is supported by Yamamoto et al. [23], who designed a prognostic model that included CSF protein levels. Nevertheless, prediction and prognostic models still need to be refined.
At present, there is no specific treatment for nervous system complications caused by influenza [38]. The various treatment schemes suggested in the literature include antiviral, corticosteroid, IVIG, hypothermia, and therapeutic plasma exchange [39,40]. The positive effect of antiviral therapy, including oseltamivir, in reducing the neurological complications of influenza and improving prognosis is unclear. Nevertheless, early intervention with antiviral therapy should inhibit viral replication and thus reduce the inflammatory response and prevent the cytokine storm. In this study, all patients were treated with oseltamivir antiviral therapy, as well as hormones and supporting treatment, but there were still 13 deaths and 25 children had sequelae, and the mortality and sequelae rates of the ANE group were higher than those of the IAE group. Three children with ANE were treated with hormone and propionate, and plasmapheresis was performed at the same time. All 3 children survived, so plasma replacement is feasible for selected children with ANE, but whether it actually changed their final outcome is unknown.
This study has some limitations. First, this was a single-center study with a limited number of patients. Second, this was a retrospective analysis, with a lack of long-term evaluation of the children. In addition, the data that could be analyzed were limited to those routinely gathered and available in the charts. In addition, because of the small number of patients, no reliable multivariable analysis and modeling could be performed. Finally, no control groups were included, mainly because patients with influenza without complications seldom come to the hospital. Additional studies are still necessary to address these issues.
Conclusions
In conclusion, influenza-associated neurological complications should be given priority when admitting children <5 years of age for influenza because of the risk of morbidity and mortality. Children with fever, convulsions, and consciousness disorder should be highly suspected of IAE. The prognosis of IAE is better than that of ANE, but early diagnosis and treatment might improve the prognosis. CSF protein and PCT could be used to predict ANE. Future studies with a larger population are needed for a better understanding of the prevalence and pathogenesis of ANE, for the detection of biomarkers of neurological involvement and disease severity, and for investigation of long-term outcomes.
Figures
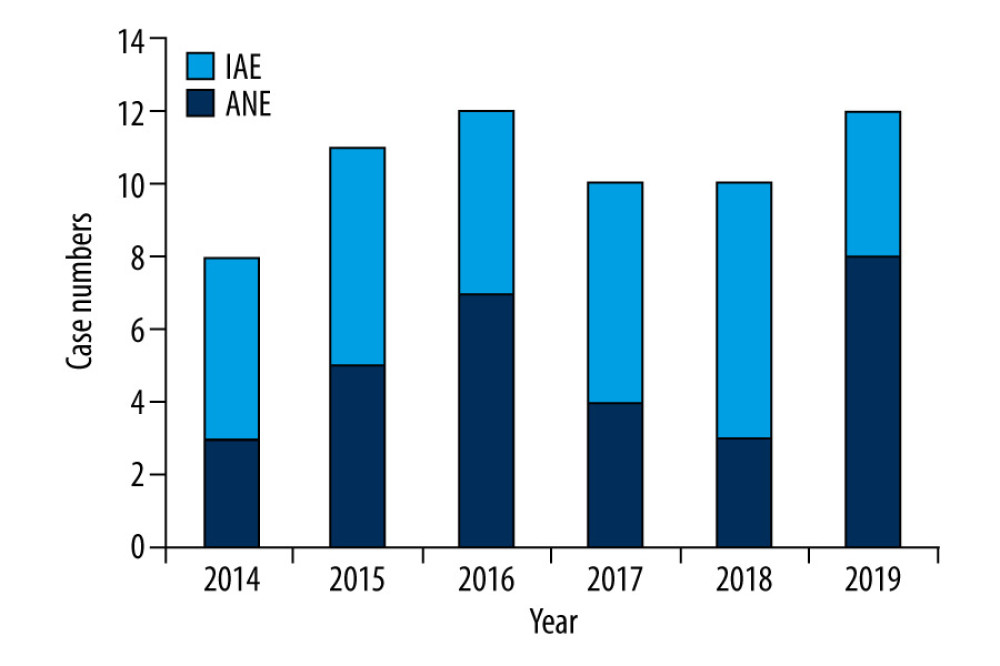 Figure 1. Distribution of the neurological complications in children with influenza during 2014–2019.
Figure 1. Distribution of the neurological complications in children with influenza during 2014–2019. 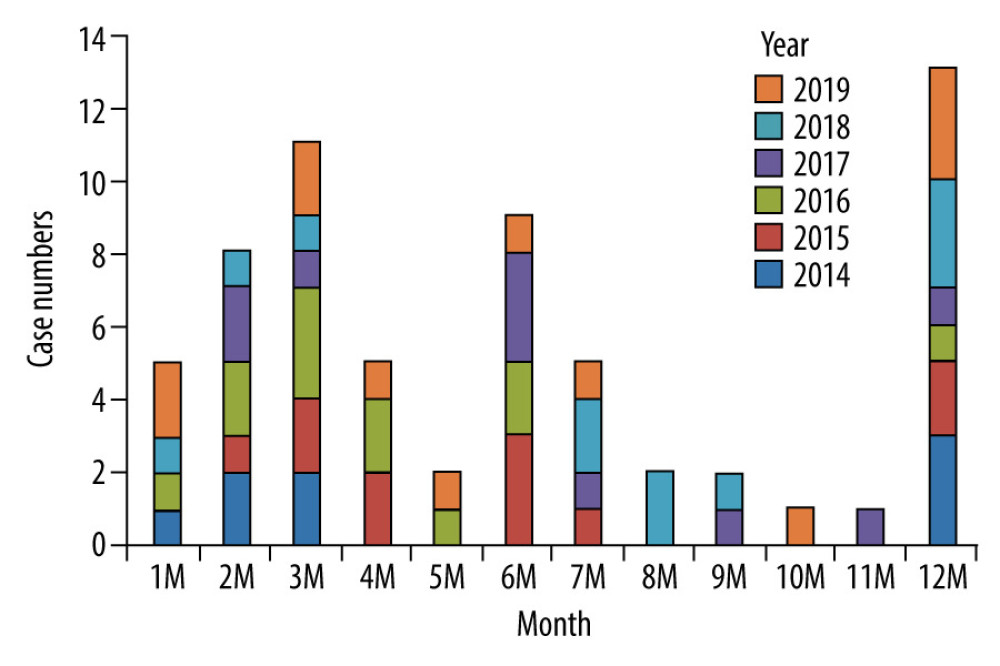 Figure 2. Epidemic trend of brain injury caused by influenza in 2014–2019.
Figure 2. Epidemic trend of brain injury caused by influenza in 2014–2019. 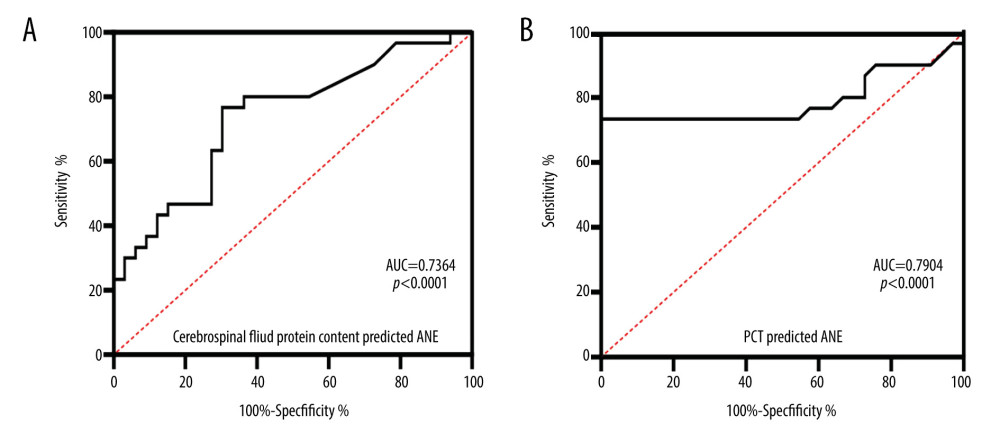 Figure 3. Using ROC curve analysis of PCT and cerebrospinal fluid protein to differentiate ANE from IAE.
Figure 3. Using ROC curve analysis of PCT and cerebrospinal fluid protein to differentiate ANE from IAE. 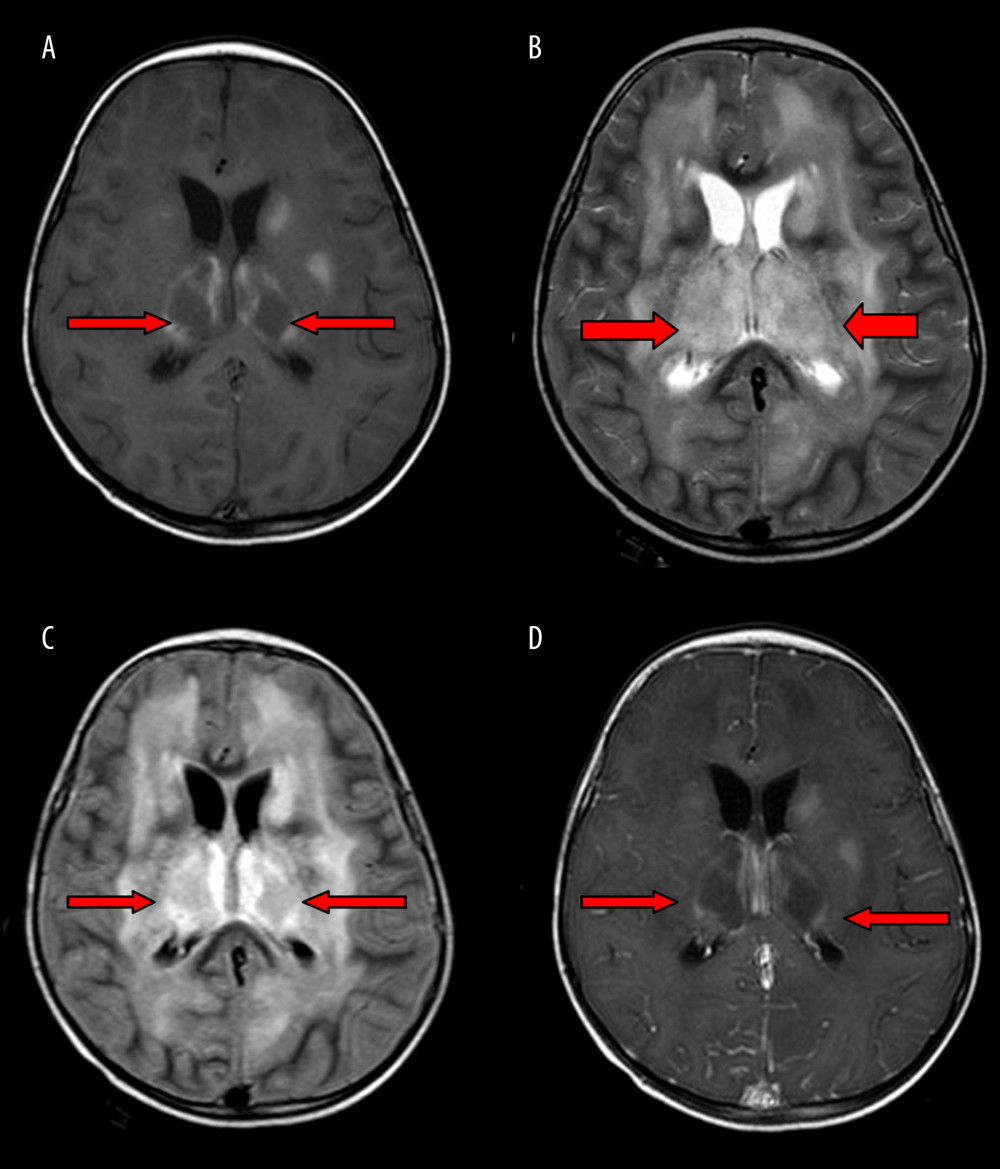 Figure 4. A 3-year-old boy with acute necrotizing encephalitis, with fever for 2 days and convulsion once. The thalamus was swollen. Symmetrical and multifocal involvement was observed in bilateral thalamus and paraventricular (A. T1WI; B. T2WI; C. T2WI-FLAIR), and no enhancement was observed in all lesions (D) (T1WI contrast enhancement). Axial T1WI (A) showed the tricolor pattern in thalamic lesions.
Figure 4. A 3-year-old boy with acute necrotizing encephalitis, with fever for 2 days and convulsion once. The thalamus was swollen. Symmetrical and multifocal involvement was observed in bilateral thalamus and paraventricular (A. T1WI; B. T2WI; C. T2WI-FLAIR), and no enhancement was observed in all lesions (D) (T1WI contrast enhancement). Axial T1WI (A) showed the tricolor pattern in thalamic lesions. 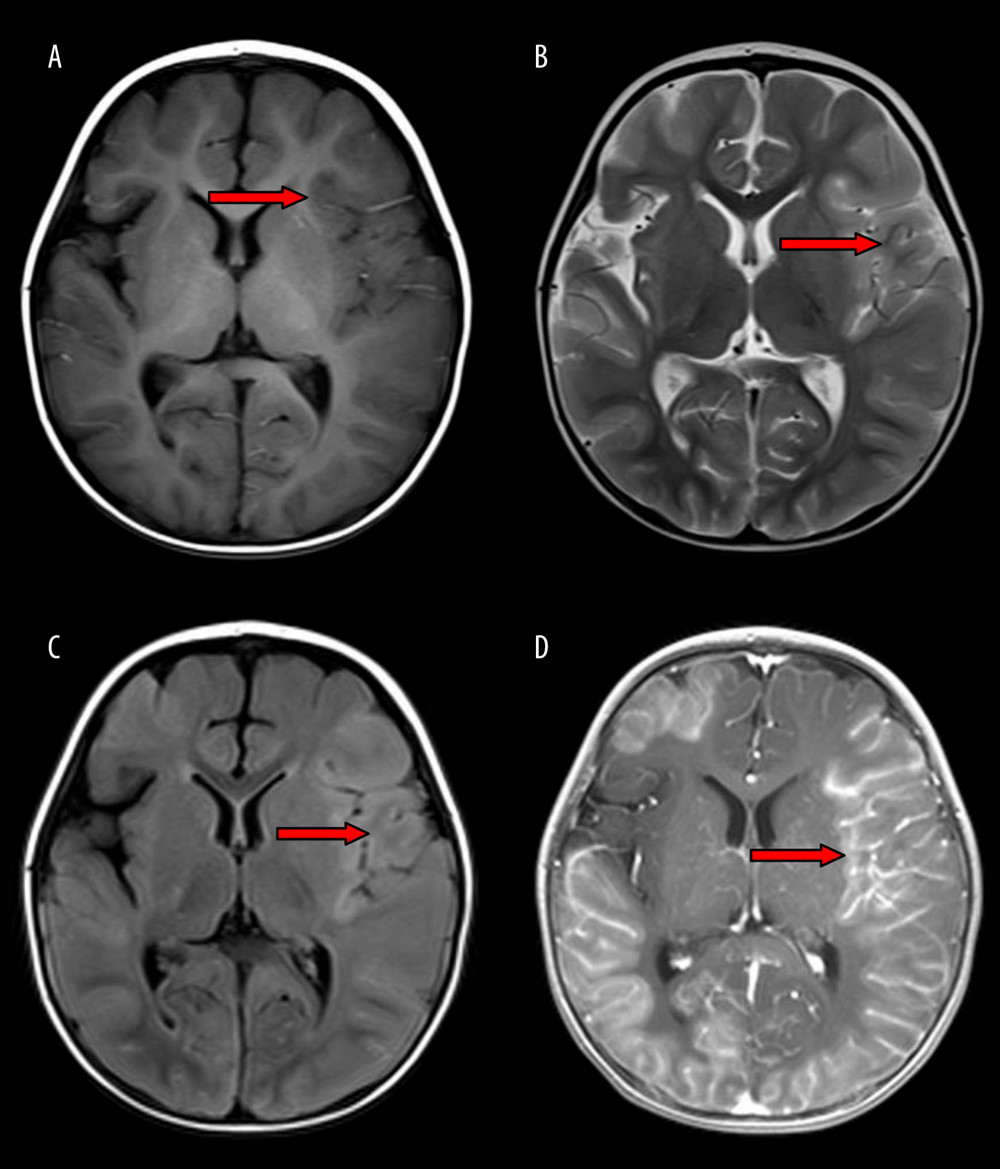 Figure 5. A 11-month-old girl with influenza-associated encephalopathy (IAE), with fever for 2 days, no convulsion. Multiple gyrus swelling and abnormal signals were observed in bilateral cerebral hemispheres, with low signal on T1WI (A) and high signal on T2WI (B) and T2WI-FLAIR (C), more obviously on the left side. Diffuse enhancement was observed on T1WI contrast enhancement (D) in lesions of the gyrus and pia meninges.
Figure 5. A 11-month-old girl with influenza-associated encephalopathy (IAE), with fever for 2 days, no convulsion. Multiple gyrus swelling and abnormal signals were observed in bilateral cerebral hemispheres, with low signal on T1WI (A) and high signal on T2WI (B) and T2WI-FLAIR (C), more obviously on the left side. Diffuse enhancement was observed on T1WI contrast enhancement (D) in lesions of the gyrus and pia meninges. References
1. Grohskopf LA, Alyanak E, Broder KR, Prevention and control of seasonal influenza with vaccines: recommendations of the Advisory Committee on Immunization Practices – United States, 2019–20 Influenza Season: MMWR Recomm Rep, 2019; 68; 1-21
2. Treanor JJ, Influenza (Including avian influenza and swine influenza): Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases, 2015, New York, Saunders
3. Kash JC, Taubenberger JK, The role of viral, host, and secondary bacterial factors in influenza pathogenesis: Am J Pathol, 2015; 185; 1528-36
4. Yildizdas D, Kendirli T, Arslankoylu AE, Neurological complications of pandemic influenza (H1N1) in children: Eur J Pediatr, 2011; 170; 779-88
5. Akins PT, Belko J, Uyeki TM, H1N1 encephalitis with malignant edema and review of neurologic complications from influenza: Neurocrit Care, 2010; 13; 396-406
6. Morishima T, Togashi T, Yokota S, Encephalitis and encephalopathy associated with an influenza epidemic in Japan: Clin Infect Dis, 2002; 35; 512-17
7. Takahashi M, Yamada T, Nakashita Y, Influenza virus-induced encephalopathy: Clinicopathologic study of an autopsied case: Pediatr Int, 2000; 42; 204-14
8. Wong AM, Simon EM, Zimmerman RA, Acute necrotizing encephalopathy of childhood: Correlation of MR findings and clinical outcome: Am J Neuroradiol, 2006; 27; 1919-23
9. Ekstrand JJ, Neurologic complications of influenza: Semin Pediatr Neurol, 2012; 19; 96-100
10. Wu X, Wu W, Pan W, Acute necrotizing encephalopathy: An underrecognized clinicoradiologic disorder: Mediators Inflamm, 2015; 2015 792578
11. Seo HE, Hwang SK, Choe BH, Clinical spectrum and prognostic factors of acute necrotizing encephalopathy in children: J Korean Med Sci, 2010; 25; 449-53
12. Kim YN, You SJ, A case of acute necrotizing encephalopathy associated with parainfluenza virus infection: Korean J Pediatr, 2012; 55; 147-50
13. Okumura A, Mizuguchi M, Kidokoro H, Outcome of acute necrotizing encephalopathy in relation to treatment with corticosteroids and gammaglobulin: Brain Dev, 2009; 31; 221-27
14. San Millan B, Teijeira S, Penin C, Acute necrotizing encephalopathy of childhood: Report of a Spanish case: Pediatr Neurol, 2007; 37; 438-41
15. Tabarki B, Thabet F, Al Shafi S, Acute necrotizing encephalopathy associated with enterovirus infection: Brain Dev, 2013; 35; 454-57
16. Vargas WS, Merchant S, Solomon G, Favorable outcomes in acute necrotizing encephalopathy in a child treated with hypothermia: Pediatr Neurol, 2012; 46; 387-89
17. Lyon JB, Remigio C, Milligan T, Deline C, Acute necrotizing encephalopathy in a child with H1N1 influenza infection: Pediatr Radiol, 2010; 40; 200-5
18. Aydin H, Ozgul E, Agildere AM, Acute necrotizing encephalopathy secondary to diphtheria, tetanus toxoid and whole-cell pertussis vaccination: Diffusion-weighted imaging and proton MR spectroscopy findings: Pediatr Radiol, 2010; 40; 1281-84
19. Okumura A, Mizuguchi M, Aiba H, Delirious behavior in children with acute necrotizing encephalopathy: Brain Dev, 2009; 31; 594-99
20. Ohsaka M, Houkin K, Takigami M, Koyanagi I, Acute necrotizing encephalopathy associated with human herpesvirus-6 infection: Pediatr Neurol, 2006; 34; 160-63
21. Mastroyianni SD, Voudris KA, Katsarou E, Acute necrotizing encephalopathy associated with parainfluenza virus in a Caucasian child: J Child Neurol, 2003; 18; 570-72
22. Kim JH, Kim IO, Lim MK, Acute necrotizing encephalopathy in Korean infants and children: Imaging findings and diverse clinical outcome: Korean J Radiol, 2004; 5; 171-77
23. Yamamoto H, Okumura A, Natsume J, A severity score for acute necrotizing encephalopathy: Brain Dev, 2015; 37; 322-27
24. Goenka A, Michael BD, Ledger E, Neurological manifestations of influenza infection in children and adults: Results of a National British Surveillance Study: Clin Infect Dis, 2014; 58; 775-84
25. Sugaya N, Influenza-associated encephalopathy in Japan: Semin Pediatr Infect Dis, 2002; 13; 79-84
26. Shiomi MPathogenesis of acute encephalitis and acute encephalopathy: Nihon Rinsho, 2011; 69; 399-408 [in Japanese]
27. Howard A, Uyeki TM, Fergie J, Influenza-associated acute necrotizing encephalopathy in siblings: J Pediatric Infect Dis Soc, 2018; 7; e172-77
28. Lafond KE, Nair H, Rasooly MH, Global role and burden of influenza in pediatric respiratory hospitalizations, 1982–2012: A systematic analysis: PLoS Med, 2016; 13; e1001977
29. Halasa NB, Update on the 2009 pandemic influenza A H1N1 in children: Curr Opin Pediatr, 2010; 22; 83-87
30. Flannery B, Reynolds SB, Blanton L, Influenza vaccine effectiveness against pediatric deaths: 2010–2014: Pediatrics, 2017; 139; e20164244
31. Newland JG, Laurich VM, Rosenquist AW, Neurologic complications in children hospitalized with influenza: Characteristics, incidence, and risk factors: J Pediatr, 2007; 150; 306-10
32. Britton PN, Blyth CC, Macartney K, The spectrum and burden of influenza-associated neurological disease in children: Combined encephalitis and influenza sentinel site surveillance from Australia, 2013–2015: Clin Infect Dis, 2017; 65; 653-60
33. To KF, Chan PK, Chan KF, Pathology of fatal human infection associated with avian influenza A H5N1 virus: J Med Virol, 2001; 63; 242-46
34. Rothberg MB, Pekow PS, Liu F, Potentially inappropriate medication use in hospitalized elders: J Hosp Med, 2008; 3; 91-102
35. Surana P, Tang S, McDougall M, Neurological complications of pandemic influenza A H1N1 2009 infection: European case series and review: Eur J Pediatr, 2011; 170; 1007-15
36. Kimura S, Ohtuki N, Nezu A, Clinical and radiological variability of influenza-related encephalopathy or encephalitis: Acta Paediatr Jpn, 1998; 40; 264-70
37. Voudris KA, Skaardoutsou A, Haronitis I, Brain MRI findings in influenza A – associated acute necrotizing encephalopathy of childhood: Eur J Paediatr Neurol, 2001; 5; 199-202
38. Khandaker G, Zurynski Y, Buttery J, Neurologic complications of influenza A(H1N1)pdm09: Surveillance in 6 pediatric hospitals: Neurology, 2012; 79; 1474-81
39. Mizuguchi M, Yamanouchi H, Ichiyama T, Shiomi M, Acute encephalopathy associated with influenza and other viral infections: Acta Neurol Scand, 2007; 115; 45-56
40. Kawashima H, Togashi T, Yamanaka G, Efficacy of plasma exchange and methylprednisolone pulse therapy on influenza-associated encephalopathy: J Infect, 2005; 51; E53-56
41. Turgut M, Sagirogluo S, Suboccipital decompressive craniectomy in a case of complex Chiari malformation complicated with influenza A (H1N1) necrotizing encephalopathy: Childs Nerv Syst, 2020; 36; 1335-36
42. Çiftçi E, Tuygun N, Özdemir H, Clinical and epidemiological features of Turkish children with 2009 pandemic influenza A (H1N1) infection: Experience from multiple tertiary paediatric centres in Turkey: Scand J Infect Dis, 2011; 43; 923-29
43. Teke T, Coskun R, Sungur M, 2009 H1N1 influenza and experience in three critical care units: Int J Med Sci, 2011; 8; 270-77
Figures
 Figure 1. Distribution of the neurological complications in children with influenza during 2014–2019.
Figure 1. Distribution of the neurological complications in children with influenza during 2014–2019. Figure 2. Epidemic trend of brain injury caused by influenza in 2014–2019.
Figure 2. Epidemic trend of brain injury caused by influenza in 2014–2019. Figure 3. Using ROC curve analysis of PCT and cerebrospinal fluid protein to differentiate ANE from IAE.
Figure 3. Using ROC curve analysis of PCT and cerebrospinal fluid protein to differentiate ANE from IAE. Figure 4. A 3-year-old boy with acute necrotizing encephalitis, with fever for 2 days and convulsion once. The thalamus was swollen. Symmetrical and multifocal involvement was observed in bilateral thalamus and paraventricular (A. T1WI; B. T2WI; C. T2WI-FLAIR), and no enhancement was observed in all lesions (D) (T1WI contrast enhancement). Axial T1WI (A) showed the tricolor pattern in thalamic lesions.
Figure 4. A 3-year-old boy with acute necrotizing encephalitis, with fever for 2 days and convulsion once. The thalamus was swollen. Symmetrical and multifocal involvement was observed in bilateral thalamus and paraventricular (A. T1WI; B. T2WI; C. T2WI-FLAIR), and no enhancement was observed in all lesions (D) (T1WI contrast enhancement). Axial T1WI (A) showed the tricolor pattern in thalamic lesions. Figure 5. A 11-month-old girl with influenza-associated encephalopathy (IAE), with fever for 2 days, no convulsion. Multiple gyrus swelling and abnormal signals were observed in bilateral cerebral hemispheres, with low signal on T1WI (A) and high signal on T2WI (B) and T2WI-FLAIR (C), more obviously on the left side. Diffuse enhancement was observed on T1WI contrast enhancement (D) in lesions of the gyrus and pia meninges.
Figure 5. A 11-month-old girl with influenza-associated encephalopathy (IAE), with fever for 2 days, no convulsion. Multiple gyrus swelling and abnormal signals were observed in bilateral cerebral hemispheres, with low signal on T1WI (A) and high signal on T2WI (B) and T2WI-FLAIR (C), more obviously on the left side. Diffuse enhancement was observed on T1WI contrast enhancement (D) in lesions of the gyrus and pia meninges. Tables
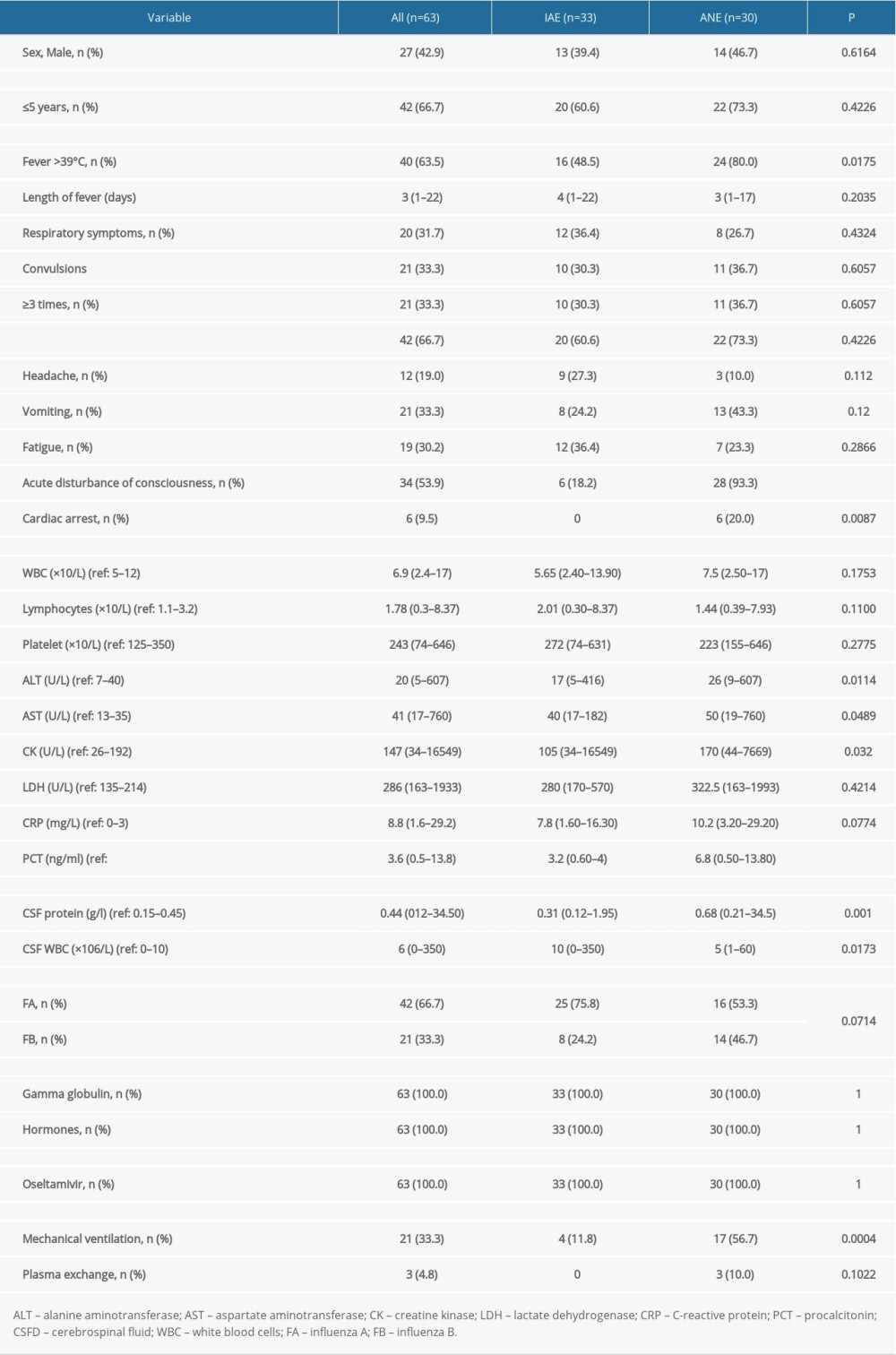 Table 1. Demographic and clinical features of influenza with neurological complications.
Table 1. Demographic and clinical features of influenza with neurological complications.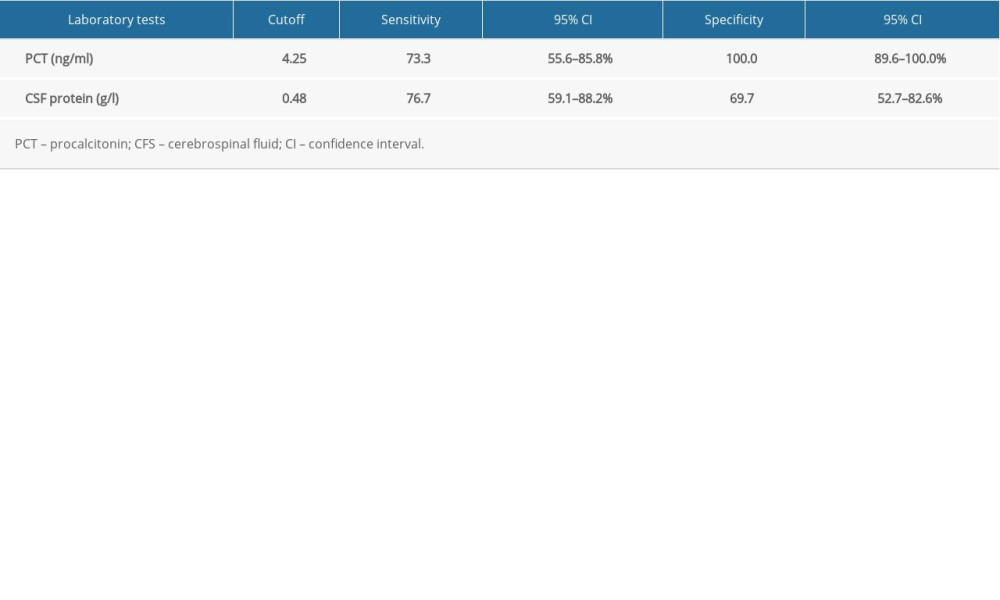 Table 2. Analysis of risk factors for ANE.
Table 2. Analysis of risk factors for ANE.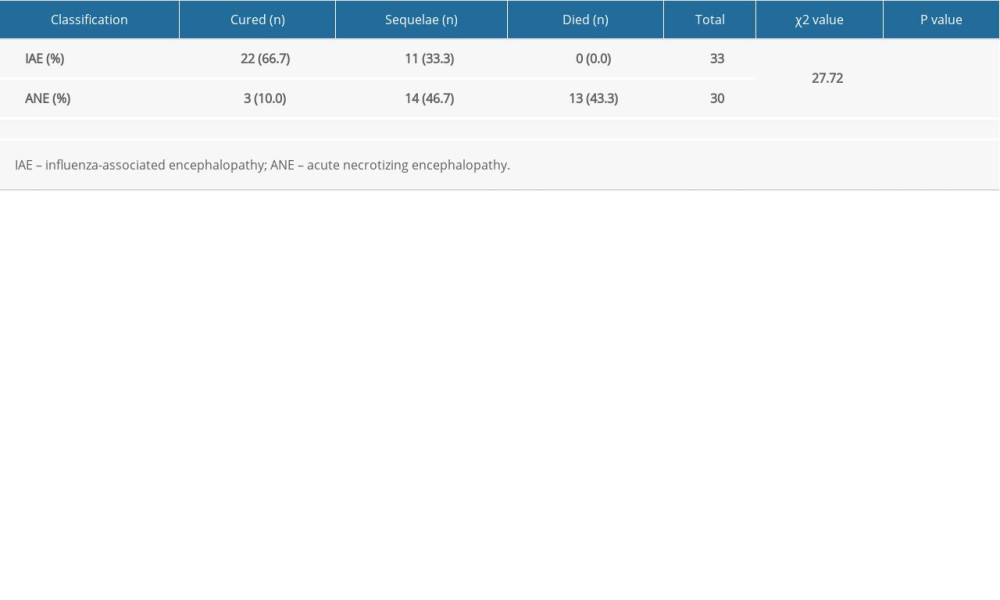 Table 3. Comparison of prognosis between IAE group and ANE group.
Table 3. Comparison of prognosis between IAE group and ANE group. Table 1. Demographic and clinical features of influenza with neurological complications.
Table 1. Demographic and clinical features of influenza with neurological complications. Table 2. Analysis of risk factors for ANE.
Table 2. Analysis of risk factors for ANE. Table 3. Comparison of prognosis between IAE group and ANE group.
Table 3. Comparison of prognosis between IAE group and ANE group. In Press
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








