03 December 2021: Clinical Research
Impact of H-Type Hypertension on Pericarotid Adipose Tissue and Plaque Characteristics Based on Computed Tomography (CT) Angiography: A Propensity Score Matching Study
Ying Liu1ABEF, Lun Xu2ACD, Yan Gu1ADG*, Yonggang Zhang1DF, Chongchang Miao1BDDOI: 10.12659/MSM.933351
Med Sci Monit 2021; 27:e933351
Abstract
BACKGROUND: We analyzed the correlation among the inflammatory changes in pericarotid adipose tissue (PCAT), plaque characteristics, and H-type hypertension on CT angiography (CTA) and explored the utility of CTA in the prevention and treatment of carotid atherosclerosis.
MATERIAL AND METHODS: A total of 135 patients who underwent head and neck CTA to investigate carotid artery atherosclerosis were retrospectively analyzed. The plaque characteristic parameters (plaque burden and remodeling index), PCAT attenuation value, and net enhancement value around the carotid artery, where the plaques were located, were recorded, and confounding factors were matched by propensity score analysis. A paired t test was used to compare the differences in fat tissue inflammatory changes and plaque characteristic parameters between the 2 groups, and logistic regression analysis was used to evaluate the relationship between plaque characteristics and the attenuation values and net enhancement values of PCAT. The correlation coefficient was calculated between type H hypertension and plaque risk grade.
RESULTS: The results of the experiment indicate that PCAT attenuation values and net enhancement values gradually increased as the degree of hypertension increased. Compared with those of patients in the normal Hcy group, these values increased more clearly in patients with high Hcy (HHcy) (r=0.641, P<0.001, r=0.581, P<0.001), although, regardless of whether the Hcy value increased, there were significant differences between the groups. However, this effect was more pronounced in patients with H-type hypertension. Logistic regression analysis of risk factors for carotid atherosclerotic plaque suggests that Hcy (OR=1.391, 95% CI 1.146-1.689, P=0.001), PCAT attenuation values (OR=1.212, 95% CI 1.074-1.367, P=0.002), and net enhancement values (OR=1.201, 95% CI 1.042-1.383, P=0.011) were independent risk factors for plaque vulnerability.
CONCLUSIONS: Our results suggest that H-type hypertension is significantly associated with PCAT attenuation and net enhancement and that PCAT net enhancement values are useful in predicting plaque risk as attenuation.
Keywords: computed tomography angiography, Hypertension, MRAP Protein, Human, Plaque, Atherosclerotic, Adipose Tissue, Female, Humans, Male, propensity score, Risk Factors
Background
In recent years, the incidence of H-type hypertension has been increasing; this type of hypertension is not only an independent risk factor for atherosclerosis (AS) but is also a risk factor for inducing cardiovascular and cerebrovascular events [1]. H-type hypertension is a common clinical hypertension type that refers to primary hypertension accompanied by hyperhomocysteinemia (HHcy) [2]; that is, the Hcy level is increased to >10 μmol/L. H-type hypertension is one of the independent risk factors for AS [2,3]. An increasing number of studies have pointed out that hypertension and high Hcy have a significant synergistic effect in the process of inducing stroke [4] and then induce a variety of cardiovascular and cerebrovascular diseases [5]. Cerebrovascular events caused by AS are the main cause of acute cerebral infarction, especially in carotid AS [6].
AS is a pathological change caused by chronic progressive arterial and periarterial fatty inflammation, which plays an important role in the occurrence and development of cardiovascular and cerebrovascular diseases. In recent years, PCAT has become the focus of cardiovascular research because of its special anatomical structure and pathological phenotypic changes. Similar to the coronary artery, the carotid artery shares a microenvironment with its surrounding adipose tissue, and the existence of a bidirectional signaling pathway [7]. Physiologically, PCAT is mainly composed of beige-colored adipose cells, shows an anti-inflammatory phenotype [8,9], and has a protective effect on the cardiovascular and cerebrovascular systems. However, in the pathological state, its microenvironment is a proinflammatory phenotype [10], with infiltration of inflammatory cells and cytokines [11,12], which can induce and promote the progression of cardiovascular and cerebrovascular diseases. Marwan et al [13] demonstrated that PCAT inflammation can lead to vascular endothelial injury and AS by grafting visceral fat and subcutaneous fat around the common carotid artery in apolipoprotein E-deficient mice. Significant progress has been made in the study of the association between PCAT inflammation and coronary atherosclerotic disease, but medical imaging studies of PCAT are relatively rare. Carotid AS is not only an important parameter reflecting systemic AS, but is also closely related to the occurrence of cerebrovascular events such as white matter damage and stroke.
Homocysteine is a metabolite of methionine and has been considered to be a biological marker of cardiovascular diseases for many years [14]. Recent studies [15] have established that HHcy is associated with the development of atherosclerosis vascular disease, and excessive homocysteine impedes intimal cell functions, which induces AS and is understood to be a multifactorial process. There are reports [16] that the level of homocysteine has a positive correlation with AS. HHcy is also closely associated with lipid metabolism, but there is scant information on the effect on perivascular adipose tissue.
PVAT inflammation can contribute to AS. Dysfunctional PVAT secretes adipocytokines (such as interleukin-6), which can diffuse directly into the vessel wall, leading to chronic vascular remodeling [17]. The adipose tissue in chronic systemic inflammation inhibits lipid accumulation, which changes the adipose cell phenotype, promoting oxidation and fibrosis [18]. In conclusion, PVAT secretes the more proinflammatory type of fat cell factors (such as resistin, leptin, and chemotactic protein), instead of the vascular protection factors.
Goeller et al [18] conducted a retrospective, single-center, case-control study comparing the CCTA of 19 patients with acute coronary syndrome and 16 patients with stable coronary heart disease, and found that the high attenuation of right pericoronary artery fat was associated with increased cardiac mortality, consistent with the results of Antonopoulos et al [19]. Baradaran et al [20] used a similar method to study pericoronary fat to measure the CT attenuation value of PCAT, and found that ipsilateral PCAT attenuation was increased in patients with stroke or transient ischemic attack, and the fat density around the stenosis segment of the internal carotid artery was significantly higher than that around the non-stenosed segment, regardless of whether the patients had symptoms. However, it should be pointed out that the above studies assessed the general population, no studies have been conducted on people with H-type hypertension, and data on the changes in PCAT inflammation are still lacking. In practice, common carotid artery bifurcation occurs in atherosclerotic plaques, and increasing PCAT attenuation occurs around the carotid artery atherosclerotic lesions surrounding the fat infiltration with inflammation. The degree of PCAT attenuation increases with the carotid artery net reinforcement value and represents the activity of local inflammation. In this study, we explored the hypothesis of an association among changes in PCAT inflammation, plaque characteristics, and H-type hypertension.
Material and Methods
GENERAL DATA:
This study protocol was approved by the Ethics Committee of our hospital (KY-20210416001-01).
WE enrolled 135 patients with carotid atherosclerotic plaque formation who underwent head and neck CTA examination in Lianyungang First People’s Hospital from October 2020 to March 2021, including 104 males and 31 females, mean age 68.07±9.74. Clinical signs, medical history, and clinical laboratory results of the patients were recorded. The data collected included sex, age, blood pressure, blood glucose, triglyceride (TG), cholesterol (TC), low-density lipoprotein (LDL), high-density lipoprotein (HDL), lipoprotein A, homocysteine (Hcy), history of stroke, and smoking history. According to whether the Hcy level was more than or equal to 10 μmol/L, the patients were divided into a high Hcy group and a normal Hcy group and then divided into 4 subgroups (grade 0, grade 1, grade 2, and grade 3) according to presence of hypertension and hypertension grade. Grade 0 is normal blood pressure (systolic blood pressure <140 mmHg and diastolic blood pressure <90 mmHg); Grade 1 is systolic blood pressure 140~159 mmHg or diastolic blood pressure of 90~99 mmHg; Grade 2 is systolic blood pressure of 160~179 mmHg or diastolic blood pressure of 100~109 mmHg; Grade 3 is systolic blood pressure ≥180 mmHg or diastolic blood pressure ≥110 mmHg.
RELEVANT CLINICAL RISK FACTORS AND RESEARCH INDEX DEFINITIONS:
The demographic characteristics and atherosclerosis-related risk factors of enrolled patients were collected. The risk factors included:
1. IMAGE ANALYSIS AND OBSERVATION OF CAROTID ARTERY CTA:
A GPACS system was used to analyze the segments with plaques at the common carotid artery bifurcation, and unified window width and window level were used for measurement (WW=800 and WL=300).
2. PCAT MEASUREMENT: Segments of the plaque at the bifurcation of the common carotid artery were selected to slide the cursor from the proximal segment to the distal segment, and the maximum cross-sectional area of the plaque was selected as the fat measurement point. Two regions of interest (ROIs) were established in the perivascular fat on the same axial section (area ≥1 mm2), and the mean value was taken as the attenuation value (Figures 1, 2). Accurate registration was performed between the base phase and the enhancement phase on the GPACS system. After matching, the ROI of the same region as the contrast period was placed in the same position in the adipose tissue to measure the base Hounsfield unit values. The net enhancement value is the difference between the Hounsfield element value obtained after enhancement and the ROI of the base phase. The placement of the ROI for each subject depended on the location of carotid plaque and the location of PCAT. The fat attenuation value of the same position before and after contrast agent injection was measured, and the net enhancement value was calculated. All fat density measurements are reported in HU units.
The site of ROIs placement was determined by the maximum cross-sectional area of the plaque and location of the PVAT pads. ROIs were drawn carefully with placing at least 1 mm from the adventitia. The results were re-checked by another researcher.
PLAQUE ANALYSIS:
The GPACS system was used to outline the plaque features. The segments of the plaque at the common carotid artery bifurcation were selected. The sliding cursor was used from the near segment to the far segment to select the maximum cross-sectional area of the plaque as the plaque measurement point to record the plaque features. Plaque area (PA), vascular area (LA), reference lumen area (RLA). The plaque burden (PB) (PB=PA/LA×100%) and remodeling index (RI) (RI=LA/RLA) were calculated. The reference sites were the proximal end of the plaque at the carotid bifurcation and the distal end without plaque, and the vascular area at the reference site was the mean of the sum of the luminal area at the proximal end and the distal end without plaque. For the same patch, different measurement points selected led to great differences in the measured values. Therefore, the maximum cross-sectional area of the patch was uniformly selected as the measurement point in this study.
PLAQUE RISK GRADING:
According to IVUS – VH and Underhill’s CAS risk scoring system [21], plaque score, and rupture risk were predicted as follows: PB< 40% was a low-risk plaque with a score of 1; PB > was 40% and had no lipid core, which was a low-risk plaque with a score of 1; PB >40% and lipid core <20% were medium- and low-risk plaques with a score of 2; 20%≤ lipid core <40%, indicating medium-high-risk plaques, scoring 3 points; and a lipid core ≥40% was considered high-risk plaques, with a score of 4. The proximity of nodular calcification in the plaque and even intrusion into the lumen were also risk factors, and the corresponding score was added as 1. The lipid core is the area of low density in the plaque with a CT value <30 HU. The evaluation of plaque vulnerability was: low-risk plaques were stable plaques, and medium- and low-risk to high-risk plaques were vulnerable plaques. Among them, medium- and low-risk plaques and medium- and high-risk plaques were predicted to be classified as low-, medium-, and high-rupture risk vulnerable plaques.
STATISTICAL ANALYSIS:
To explore the differences in fat and plaque characteristics around the carotid artery in patients with H-type hypertension, we first evaluated whether there were differences in perivascular inflammation in the plaque area at the common carotid artery bifurcation in each group. We used the independent-sample
Results
COMPARISON OF BASELINE CHARACTERISTICS BETWEEN THE 2 GROUPS AFTER PROPENSITY SCORE MATCHING:
We screened 1290 patient with head and neck CTA examination. Of 769 patients with atherosclerotic plaques at unilateral or bilateral carotid artery bifurcation, we excluded 56 patients with carotid artery occlusion, 249 patients with incomplete medical history, 1 patient with carotid artery dissection, 16 patients with malignant tumor history, and 1 patient with poor image quality, for a total of 181 case. Forty-six patients were excluded after propensity scoring. A total of 135 patient met the inclusion criteria, with an average age of 68.07 years and 23% of whom were female. According to the >10 μmol/L Hcy level, 67 patients in the high Hcy group and 68 patients in the normal group were divided into 2 groups (Table 1). Table 1 lists the main characteristics of the entire study cohort. There were no significance differences in the comparison of covariates between the 2 groups (P>0.05).
COMPARISON OF FAT CHARACTERISTICS AROUND THE CAROTID ARTERY AFTER PROPENSITY SCORE MATCHING:
PCAT attenuation and net reinforcement values with the gradual increase of hypertension grade. Figure 3 shows the carotid plaques surrounding adipose tissue attenuation and distribution patterns of reinforced net value of the high Hcy and normal groups, and compared with normal group, the high Hcy group fat tissue attenuation and net reinforcement value increased more significantly (P<0.001).
COMPARISON OF PLAQUE CHARACTERISTICS AND PLAQUE GRADING BETWEEN THE 2 GROUPS AFTER PROPENSITY SCORE MATCHING:
Correlation coefficient between hypertension grade and plaque grade was r=0.307, P<0.05. Patients in the high Hcy group had a stronger correlation than those in the normal group (r=0.294, P<0.05 vs r=0.267, P<0.05), while the hypertension grade showed a very weak correlation with plaque load and remodeling index. The correlation coefficients were r=0.032 and r=0.063, P>0.05, respectively, which were not statistically significant (Figure 4).
Spearman correlation analysis was calculated for the changes in PCAT inflammation and plaque vulnerability, and the correlation coefficient between the attenuation value of PCAT and plaque grade was r=0.605,
RISK FACTOR ANALYSIS OF PLAQUE VULNERABILITY:
According to plaque classification, the plaques were divided into 2 groups: stable plaques and vulnerable plaques. Factors including sex, age, blood pressure, blood glucose, TGs, TC, LDL, HDL, lipoprotein A, Hcy, history of stroke and smoking, PA, LA, PB and RI were included to construct an ordered logistic regression model. One-way ANOVA was performed for these risk factors (Table 2). The results showed that the effect of Hcy on plaque vulnerability was statistically significant (OR=1.391, 95% CI 1.146–1.689, P=0.001). The effect of PCAT attenuation on plaque vulnerability was statistically significant (OR=1.212, 95% CI 1.074–1.367, P=0.002). The net enhancement value of PCAT had a statistically significant effect on plaque vulnerability (OR=1.201, 95% CI 1.042–1.383, P=0.011). There was a significant difference between the carotid fat attenuation value and net enhancement value between the 2 groups (P<0.001) (Table 3).
Discussion
We used routine head and neck CTA examinations and showed that with an increase in blood pressure in patients in the high Hcy group, the PCAT attenuation values and net enhancement values increased, more clearly when compared to that in patients in the normal Hcy group. When the Hcy value increased, there were significant differences, but in the H group of patients with high blood pressure, this increase was more pronounced (r=0.641,
Similar to pericoronal fat, PCAT inflammation causes the accumulation of lipid gradients to change from lipophilic to hydrophilic [9] CTA examination showed increased fat attenuation, and an enhanced scan showed slightly uneven enhancement; that is, there was a net enhancement value. Recent research data support the role of perivascular fat density change as a surrogate marker of local inflammation [17] and confirm that PCAT has metabolic and immune activity, which is not only related to AS but also associated with hypertension and hyperHcy. In conclusion, our results are important because we found that inflammatory activity in carotid atherosclerotic diseases may be associated with H-type hypertension.
In this study, we further analyzed the characteristics of carotid bifurcation plaques. The site most commonly involved with carotid atherosclerotic plaques is the carotid bifurcation, and this distribution pattern is related to hemodynamics. Vortexes easily form when blood flow passes through vascular bifurcations or plaques, and the shear force is weakened accordingly. Carotid atherosclerotic plaques, especially lipid plaques, tend to develop at positions where blood flow shear force is relatively low. Vortexes easily form at vascular bifurcations or plaques, which can cause vasoconstriction, platelet aggregation and inflammation, thus triggering the rupture of vulnerable plaques. At present, the characteristics of vulnerable plaques are considered to include thin fibrous caps, large lipid cores, intraplaque bleeding, intraplaque neovascularization and inflammatory cell infiltration [22,23]. In this study, although no significant differences were found between H-type hypertension patients and the other subgroups in terms of plaque load and vascular remodeling, there was a significant correlation between hypertension grade and plaque grade (r=0.307,
We also performed Spearman correlation analysis on changes in pericarotid adipose tissue inflammation and plaque rupture risk grade. The attenuation value and net enhancement value of pericarotid adipose tissue were significantly correlated with plaque grade (r=0.605 and 0.644 respectively,
Finally, we performed regression analysis of the risk factors for carotid atherosclerotic plaque and found that Hcy, PCAT attenuation, and net enhancement value were independent risk factors for plaque risk. Currently, many studies have confirmed that increased perivascular fat attenuation is significantly correlated with plaque vulnerability [8]. Saba et al [24] found that the degree of carotid plaque enhancement is positively correlated with the attenuation of perivascular fat; that is, the density of PCAT can be used as an indirect marker of plaque stability. In this study, we found that the PCAT net enhancement value was as valuable as the PCAT attenuation value in assessing the risk of plaque rupture. Thus, the present evidence seems to suggest that the net enhancement value of PCAT is as relevant to the development of AS, as its attenuation value or that it may be a potential marker of plaque vulnerability.
Blood pressure variability (BPV) has been recognized as a predictor for brain vascular lesions, which can influence brain structure and function [25]. It plays an important role on the onset and course of cognitive impairment and dementia [26]. Long-term BPV is associated with cardiovascular and cerebrovascular events like stroke and myocardial infarction [27], independent of mean blood pressure. Meanwhile, BPV increases with elevation of blood pressure and is associated with target-organ damage independent of absolute blood pressure in hypertension [28]. It is easy to find the target-organ damage in the retina, kidneys, heart, brain, and vasculature by medical methods [27]. A study found that long-term BPV was a risk factor of cardiovascular and cerebrovascular events in high-risk populations [29]. Future research should explore their effects on carotid atherosclerosis and carotid morphological characteristics.
Yuting Tan et al [30] found that H-type hypertension is closely related to the degree of plaque enhancement and is an independent risk factor for plaque vulnerability using contrast-enhanced ultrasound. These results are similar to the results of our study. In patients with H-type hypertension accompanied by carotid atherosclerotic plaque formation, inflammation of the pericarotid adipose tissue showed increased attenuation with varying degrees of intensification, and this local inflammation may be independent of other systemic inflammation. Through further validation, these markers may become indicators for the early prevention and treatment of stroke in patients with H-type hypertension with carotid AS. The use of noninvasive imaging techniques to assess changes in PCAT inflammation in patients with type H hypertension can more accurately assess local inflammation and potentially providing a basis for more targeted treatment. In addition, these findings confirm that increased fat attenuation and net enhancement around carotid plaques in patients with type H hypertension on CT are associated with histopathological perivascular fat inflammation, which can be detected around “culprit” plaques before they contribute to ischemic events.
Limitations of this study include the following: (1) It was a retrospective, single-center study with a small sample size; (2) There is inevitable selection bias; and (3) The measurement of PCAT density on CT may be affected by the change of ROI position. To ensure that the ROIs were evenly distributed, we chose the location of the largest carotid bifurcation plaque (ie, the level of the degree of carotid stenosis was the most serious) to establish each ROI, but as a result of the anatomy of the carotid artery, fat positions around the positions of the ROIs were placed slightly differently, which may have affected local adipose tissue attenuation values and net reinforcement value measurement. Therefore, there will be future challenges in determining specific thresholds or ranges in plaque rupture risk assessment.
In future studies, the risk factors for plaque rupture should be further analyzed in people with different types of hypertension to investigate different interventional methods for people with different etiologies. In addition, this study was a single-center, retrospective study, and the sample size should be further expanded to provide more powerful data for use in clinical practice.
type hypertension is an important risk factor for ischemic stroke, which is not only significantly associated with the risk of recurrence of ischemic stroke, but is also associated with high-risk vulnerable plaques. Therefore, the early diagnosis and intervention of fat inflammation around carotid plaque in H-type hypertension patients may become a novel marker for the prevention and treatment of first-episode and recurrent ischemic stroke.
Conclusions
In patients with carotid AS investigated by CTA, H-type hypertension is significantly associated with PCAT attenuation and net enhancement. Our results indicate that PCAT net enhancement values have utility in predicting plaque risk as PVAT attenuation.
Figures
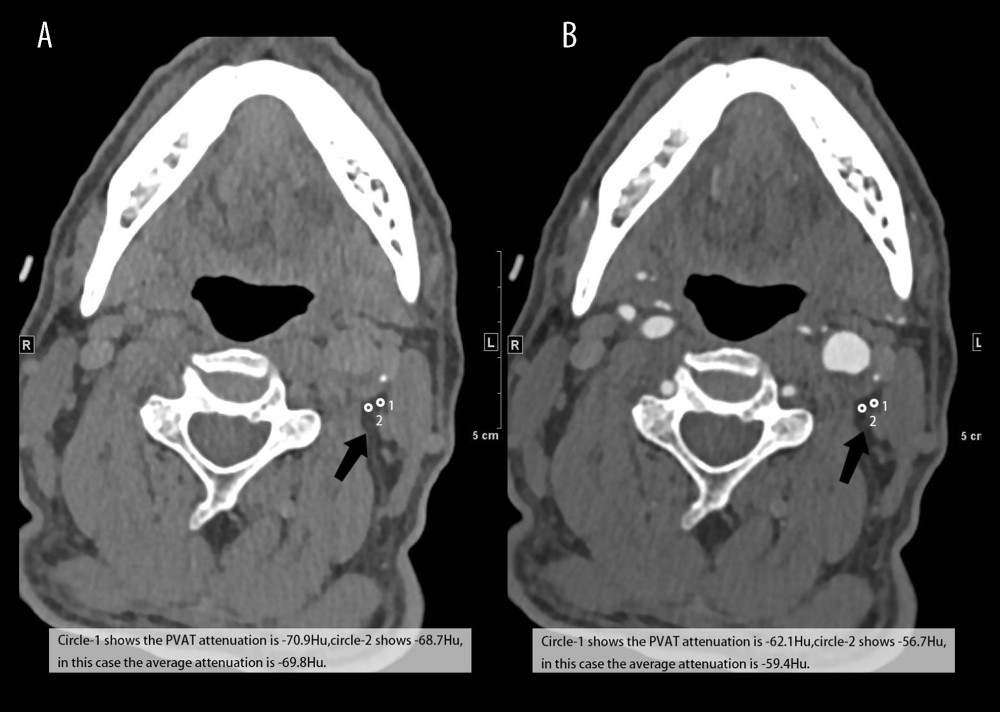 Figure 1. A 61-year-old man in the HHcy group with left carotid low-density plaque with a nodular calcification (high-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −69.8 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −58.4 HU with a net enhancement value of 11.4 HU.
Figure 1. A 61-year-old man in the HHcy group with left carotid low-density plaque with a nodular calcification (high-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −69.8 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −58.4 HU with a net enhancement value of 11.4 HU. 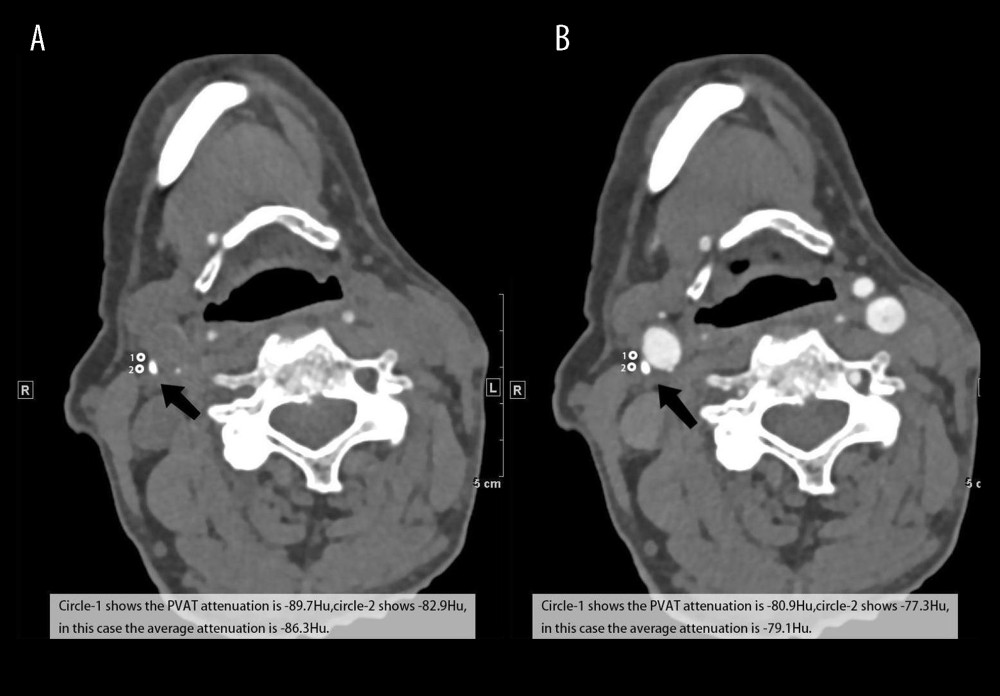 Figure 2. A 75-year-old man matched in the normal group with right carotid calcific plaque (low-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −86.3 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −79.1 HU with a net enhancement value of 7.2 HU.
Figure 2. A 75-year-old man matched in the normal group with right carotid calcific plaque (low-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −86.3 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −79.1 HU with a net enhancement value of 7.2 HU. 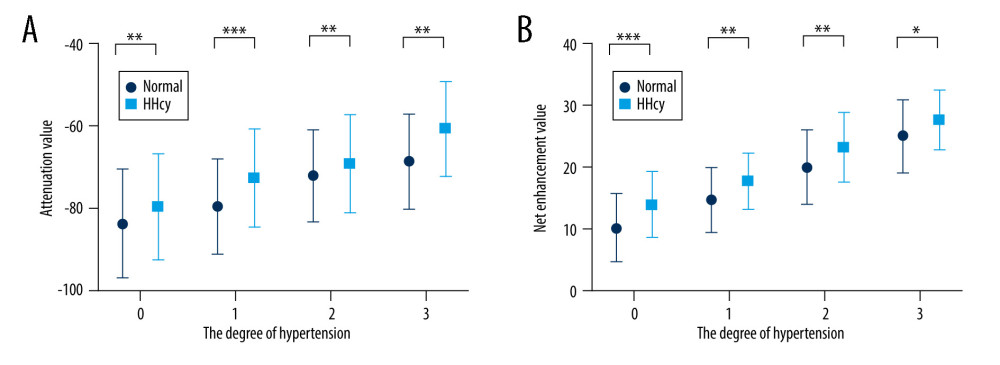 Figure 3. (A) Paired t test was used to compare the difference in PCAT attenuation values of different hypertension grades between the normal group and the high Hcy group. (B) The paired t test was used to compare the differences in the net enhancement value of PCAT in different hypertension grades between the normal group and the high Hcy group. (*P<0.05; ** P<0.002; *** P<0.001).
Figure 3. (A) Paired t test was used to compare the difference in PCAT attenuation values of different hypertension grades between the normal group and the high Hcy group. (B) The paired t test was used to compare the differences in the net enhancement value of PCAT in different hypertension grades between the normal group and the high Hcy group. (*P<0.05; ** P<0.002; *** P<0.001). 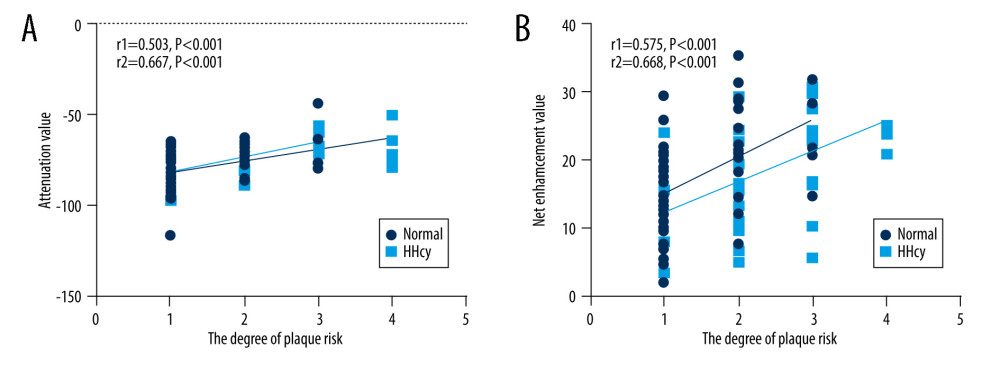 Figure 4. (A) Spearman correlation analysis was performed on the attenuation value of peripheral carotid fat and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.503, P<0.001), and the blue dots represent the HHcy group (r2=0.667, P<0.001). (B) Spearman correlation analysis was performed on the net enhancement value of PCAT and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.575, P<0.001), and the blue dots represent the HHcy group (r2=0.668, P<0.001).
Figure 4. (A) Spearman correlation analysis was performed on the attenuation value of peripheral carotid fat and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.503, P<0.001), and the blue dots represent the HHcy group (r2=0.667, P<0.001). (B) Spearman correlation analysis was performed on the net enhancement value of PCAT and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.575, P<0.001), and the blue dots represent the HHcy group (r2=0.668, P<0.001). References
1. Zhou F, Hou D, Wang Y, Evaluation of H-type hypertension prevalence and its influence on the risk of increased carotid intima-media thickness among a high-risk stroke population in Hainan Province, China: Medicine (Baltimore), 2020; 99; e21953
2. Zhang J, Liu Y, Wang A, Association between H-type hypertension and asymptomatic extracranial artery stenosis: Sci Rep, 2018; 8(1); 1328
3. Akoumianakis I, Akawi N, Antoniades C, Exploring the crosstalk between adipose tissue and the cardiovascular system: Korean Circ J, 2017; 47(5); 670-85
4. Li T, Zhu J, Fang Q, Association of H-type hypertension with stroke severity and prognosis: Biomed Res Int, 2018; 2018; 8725908
5. Ganguly P, Alam SF, Role of homocysteine in the development of cardiovascular disease: Nutr J, 2015; 14; 6
6. Marnane M, Prendeville S, McDonnell C, Plaque inflammation and unstable morphology are associated with early stroke recurrence in symptomatic carotid stenosis: Stroke, 2014; 45; 801-6
7. Antonopoulos AS, Margaritis M, Verheule S, Mutual regulation of epicardial adipose tissue and myocardial redox state by PPAR-γ/adiponectin signalling: Circ Res, 2016; 118; 842-55
8. Goeller M, Achenbach S, Cadet S, Pericoronary adipose tissue computed tomography attenuation and high-risk plaque characteristics in acute coronary syndrome compared with stable coronary artery disease: JAMA Cardiol, 2018; 3(9); 858-63
9. Lin A, Dey D, Wong DTL, Perivascular adipose tissue and coronary atherosclerosis: From biology to imaging phenotyping: Curr Atheroscler Rep, 2019; 21; 47
10. Ridker PM, Everett BM, Thuren T, Antiinflammatory therapy with canakinumab for atherosclerotic disease: N Engl J Med, 2017; 377(12); 1119-31
11. Fuster JJ, Ouchi N, Gokce N, Obesity-induced changes in adipose tissue microenvironment and their impact on cardiovascular disease: Circ Res, 2016; 118; 1786-807
12. Park SY, Kim KH, Seo KW, Resistin derived from diabetic perivascular adipose tissue up-regulates vascular expression of osteopontin via the AP-1 signalling pathway: J Pathol, 2014; 232; 87-97
13. Marwan M, Hell M, Schuhbäck A, Gauss S, CT attenuation of pericoronary adipose tissue in normal versus atherosclerotic coronary segments as defined by intravascular ultrasound: J Comput Assist Tomogr, 2017; 41(5); 762-67
14. Haloul M, Vinjamuri SJ, Naquiallah D, Hyperhomocysteinemia and low folate and vitamin B12 are associated with vascular dysfunction and impaired nitric oxide sensitivity in morbidly obese patients: Nutrients, 2020; 12; 2014
15. Kang S, Rosenson RS, Analytic approaches for the treatment of hyperhomocysteinemia and its impact on vascular disease: Cardiovasc Drug Ther, 2018; 32; 233-40
16. Kim J, Kim H, Roh H, Kwon Y, Causes of hyperhomocysteinemia and its pathological significance: Arch Pharm Res, 2018; 41; 372-83
17. Antoniades C, Shirodaria C, Detecting coronary inflammation with perivascular fat attenuation imaging: JACC Cardiovasc Imaging, 2019; 12; 2011-14
18. Goeller M, Achenbach S, Cadet S, Pericoronary adipose tissue computed tomography attenuation and high-risk plaque characteristics in acute coronary syndrome compared with stable coronary artery disease: JAMA Cardiol, 2018; 3; 858-63
19. Antonopoulos AS, Sanna F, Sabharwal N, Detecting human coronary inflammation by imaging perivascular fat: Sci Transl Med, 2017; 9(398); eaal2658
20. Baradaran H, Myneni PK, Patel P, Association between carotid artery perivascular fat density and cerebrovascular ischemic events: J Am Heart Assoc, 2018; 7; e010383
21. Underhill HR, Hatsukami TS, Cai J, A noninvasive imaging approach to assess plaque severity: The carotid atherosclerosis score: Am J Neuroradiol, 2010; 31; 1068-75
22. Ferencik M, Hoffmann U, High-risk coronary plaque on computed tomography angiography: Time to recognize a new imaging risk factor: Circ Cardiovasc Imaging, 2018; 11; e007288
23. Williams MC, Moss AJ, Dweck M, Coronary artery plaque characteristics associated with adverse outcomes in the SCOT-HEART Study: J Am Coll Cardiol, 2019; 73; 291-301
24. Saba L, Zucca S, Gupta A, Perivascular fat density and contrast plaque enhancement: Does a correlation exist?: Am J Neuroradiol, 2020; 41; 1460-65
25. Lattanzi S, Vernieri F, Silvestrini M, Blood pressure variability and neurocognitive functioning: J Clin Hypertens, 2018; 20; 645-47
26. Tully PJ, Yano Y, Launer LJ, Association between blood pressure variability and cerebral small-vessel disease: A systematic review and meta-analysis: J Am Heart Assoc, 2020; 9; e13841
27. Mena LJ, Felix VG, Melgarejo JD, Maestre GE, 24-hour blood pressure variability assessed by average real variability: A systematic review and meta-analysis: J Am Heart Assoc, 2017; 6(10); e006895
28. Lattanzi S, Vernieri F, Silvestrini M, Blood pressure variability and neurocognitive functioning: J Clin Hypertens, 2018; 20; 645-47
29. Ma Y, Song A, Viswanathan A, Blood pressure variability and cerebral small vessel disease: A systematic review and meta-analysis of population-based cohorts: Stroke, 2020; 51; 82-89
30. Tan Y, Nie F, Wu G, Impact of H-type hypertension on intraplaque neovascularization assessed by contrast-enhanced ultrasound: J Atheroscler Thromb, 2021 [Online ahead of print]
Figures
 Figure 1. A 61-year-old man in the HHcy group with left carotid low-density plaque with a nodular calcification (high-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −69.8 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −58.4 HU with a net enhancement value of 11.4 HU.
Figure 1. A 61-year-old man in the HHcy group with left carotid low-density plaque with a nodular calcification (high-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −69.8 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −58.4 HU with a net enhancement value of 11.4 HU. Figure 2. A 75-year-old man matched in the normal group with right carotid calcific plaque (low-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −86.3 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −79.1 HU with a net enhancement value of 7.2 HU.
Figure 2. A 75-year-old man matched in the normal group with right carotid calcific plaque (low-risk plaque). The basal scan (A) shows the average fat tissue (white circle) of −86.3 HU, whereas the postcontrast scan (B) shows the average fat tissue density (white circle) value of −79.1 HU with a net enhancement value of 7.2 HU. Figure 3. (A) Paired t test was used to compare the difference in PCAT attenuation values of different hypertension grades between the normal group and the high Hcy group. (B) The paired t test was used to compare the differences in the net enhancement value of PCAT in different hypertension grades between the normal group and the high Hcy group. (*P<0.05; ** P<0.002; *** P<0.001).
Figure 3. (A) Paired t test was used to compare the difference in PCAT attenuation values of different hypertension grades between the normal group and the high Hcy group. (B) The paired t test was used to compare the differences in the net enhancement value of PCAT in different hypertension grades between the normal group and the high Hcy group. (*P<0.05; ** P<0.002; *** P<0.001). Figure 4. (A) Spearman correlation analysis was performed on the attenuation value of peripheral carotid fat and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.503, P<0.001), and the blue dots represent the HHcy group (r2=0.667, P<0.001). (B) Spearman correlation analysis was performed on the net enhancement value of PCAT and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.575, P<0.001), and the blue dots represent the HHcy group (r2=0.668, P<0.001).
Figure 4. (A) Spearman correlation analysis was performed on the attenuation value of peripheral carotid fat and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.503, P<0.001), and the blue dots represent the HHcy group (r2=0.667, P<0.001). (B) Spearman correlation analysis was performed on the net enhancement value of PCAT and plaque risk classification. The gray dots represent the normal Hcy group (r1=0.575, P<0.001), and the blue dots represent the HHcy group (r2=0.668, P<0.001). Tables
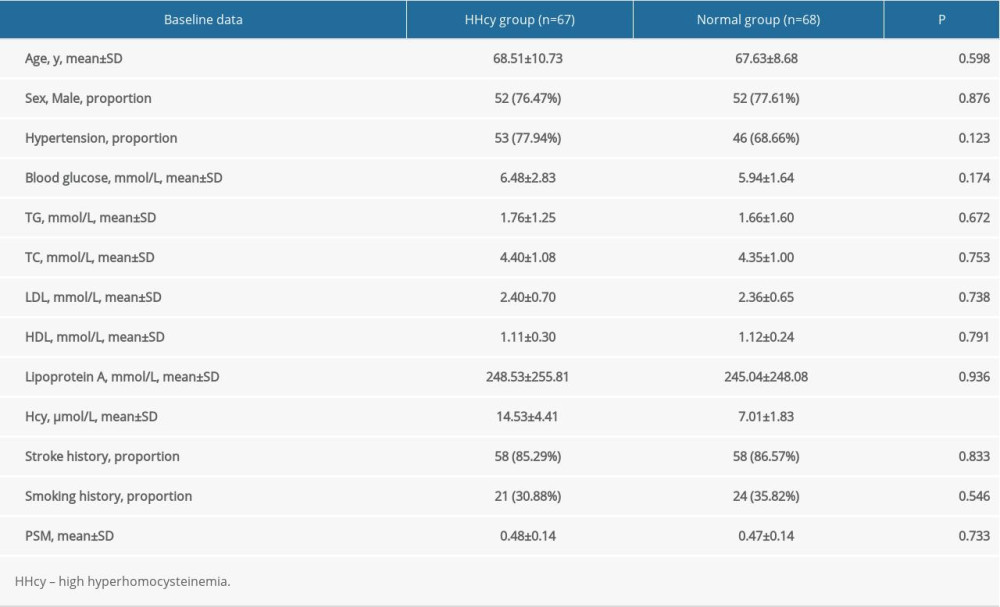 Table 1. Comparison of baseline data between the normal group and the HHcy group.
Table 1. Comparison of baseline data between the normal group and the HHcy group.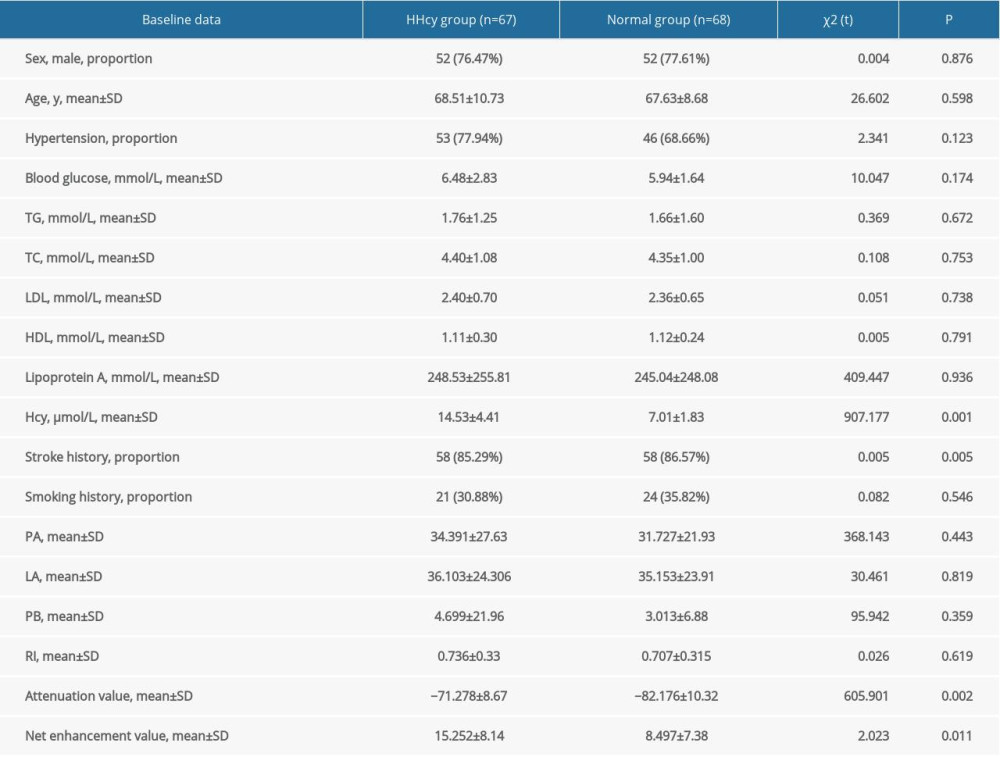 Table 2. one-way analysis of variance of risk factors for plaque vulnerability.
Table 2. one-way analysis of variance of risk factors for plaque vulnerability.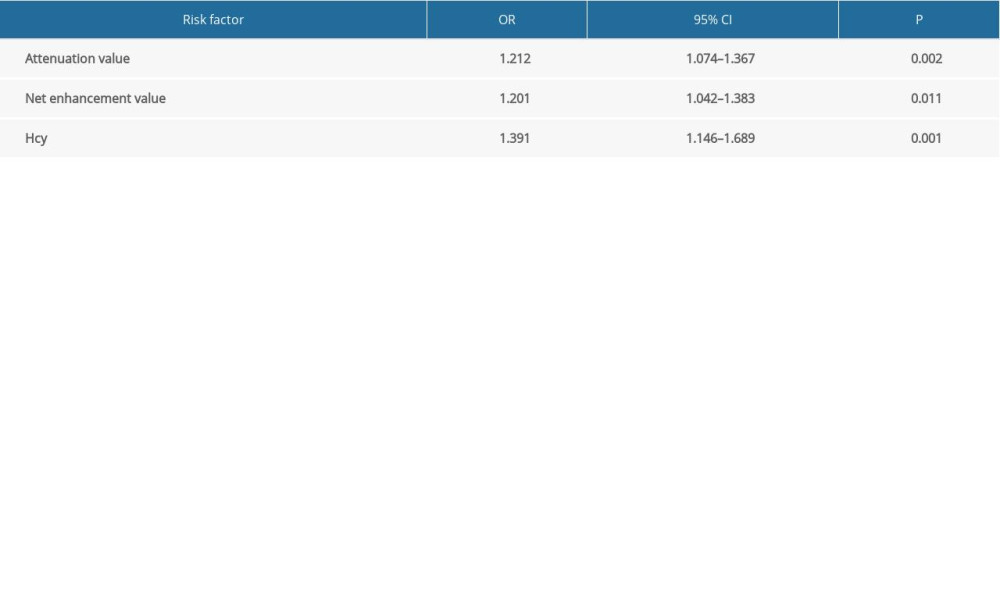 Table 3. Regression analysis of risk factors for plaque vulnerability.
Table 3. Regression analysis of risk factors for plaque vulnerability. Table 1. Comparison of baseline data between the normal group and the HHcy group.
Table 1. Comparison of baseline data between the normal group and the HHcy group. Table 2. one-way analysis of variance of risk factors for plaque vulnerability.
Table 2. one-way analysis of variance of risk factors for plaque vulnerability. Table 3. Regression analysis of risk factors for plaque vulnerability.
Table 3. Regression analysis of risk factors for plaque vulnerability. In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








